Abstract
Hypodermoclysis is the continuous subcutaneous infusion of a parenteral solution into dermal tissue, which is typically associated with skin lesions and cosmetic issues in the majority of patients. Scarring and pigmentation are two of the potential skin lesions after hypodermoclysis. The way skin diseases and cosmetic issues are treated has altered dramatically as a result of laser technology. This is the first article to our knowledge that describes the treatment of pigmentation and scarring produced by Hypodermoclysis cutaneous damage by using laser treatment. It was vital to select the appropriate endpoint, technology, and configuration parameters. The lesion was completely resolved after five months of treatment with four laser sessions. The first session used a fractional Er-Yag laser to perform cold ablation. The remaining sessions used 1064 and 585 nm Nd-Yag Q-switch lasers to operate in the nanosecond region. To minimize the danger of post-inflammatory hyperpigmentation (PIH), the treated region was prepped between laser treatments with 4% hydroquinone (HQ) cream. Our protocol may reduce scars and pigmentation while minimizing adverse effects and downtime.
1. Introduction
Hypodermoclysis (HDC) is the continuous subcutaneous infusion of a parenteral solution into the dermal tissue. It can be used for both short- and long-term parenteral medication delivery. Depending on the time frame and type of infused fluid, HDC is associated with varying degrees of tissue disruption, primarily cutaneous injury. The majority of the literature focuses on clinical complications of HDC, such as sepsis and tissue necrosis [1,2]. However, reports of cosmetic skin lesions and complications after HDC and subcutaneous infusion have primarily focused on type I diabetes patients who use insulin pumps [3,4,5]. Furthermore, these reports were purely observational, with no discussion of treatment options [6]. Our review of the literature revealed that no reports on laser treatment for pigmentation or scarring caused by hypodermoclysis had been published. It is well known that cutaneous injury from various causes can result in abnormal pigmentation, either hypo or hyperpigmentation, and resistant scarring. Lasers are commonly used to treat skin pigmentation and scarring [7,8,9]. The laser technologies available for the treatment of skin lesions have undergone a revolution in the last decade [10]. Most laser technologies available rely on their effect on either selective photothermolysis or photoacoustic properties [11]. Experts usually design a protocol that includes various laser technologies and settings that target different chromophores [12,13].
2. Case Report
A 28-year-old middle-eastern man came to the center with visible pigmentation and scarring on the lower-right abdominal quadrant. The patient’s medical history reveals that he is otherwise healthy and has type III Fitzpatrick skin. According to the patient’s reported history, the skin lesion is approximately 23 years old and developed following HDC treatment as a child with an unknown medication; the patient believed it was an antibiotic, but could not provide any additional details or contact information for the facility or provider.
2.1. Lesion Assessment
The lesion was assessed using the Vancouver scale for scar assessment, along with photographic assessment [14,15]. The assessment was conducted by two different investigators when possible and the average values were reported. The patient was not included in the assessment process. The initial scar score was a total of 6, as follows: Vascularity: 0, Pigmentation: 3, Pliability: 2, and Height: 1.
We devised a protocol to address pigmentation and scarring while improving skin texture in areas that received subcutaneous infusion. The lasers used in the protocol included an erbium-doped yttrium aluminum garnet (Er-Yag) fractional laser (Fotona Dynamis, Fotona Inc., Ljubljana, Slovenia), a 1064 nm Crystal Nd-Yag Q-switch nanosecond laser, and a Q-switched 595-nm neodymium-doped yttrium aluminum garnet (Nd-Yag) laser with low fluence (Spectra, Lutronic Aesthetics, Gyeonggi-do, Korea). Only after performing test patches and receiving signed consents did the treatment begin. The protocol is divided into two stages: preparation and treatment. Before and aftercare instructions were given to the patient. The treatment’s goal was to smooth the texture and even out the pigmented lesion so that it blended in better with the surrounding skin.
2.2. Preparation Phase
4% HQ cream was applied daily on the targeted area for two weeks before the sole Er-Yag laser treatment in phase one, but repeated before and after Q-switched 595-nm Nd-Yag in stage two of the treatment phase.
2.3. Treatment Phase
This phase consists of the actual laser treatment and is divided into two stages.
3. Stage One
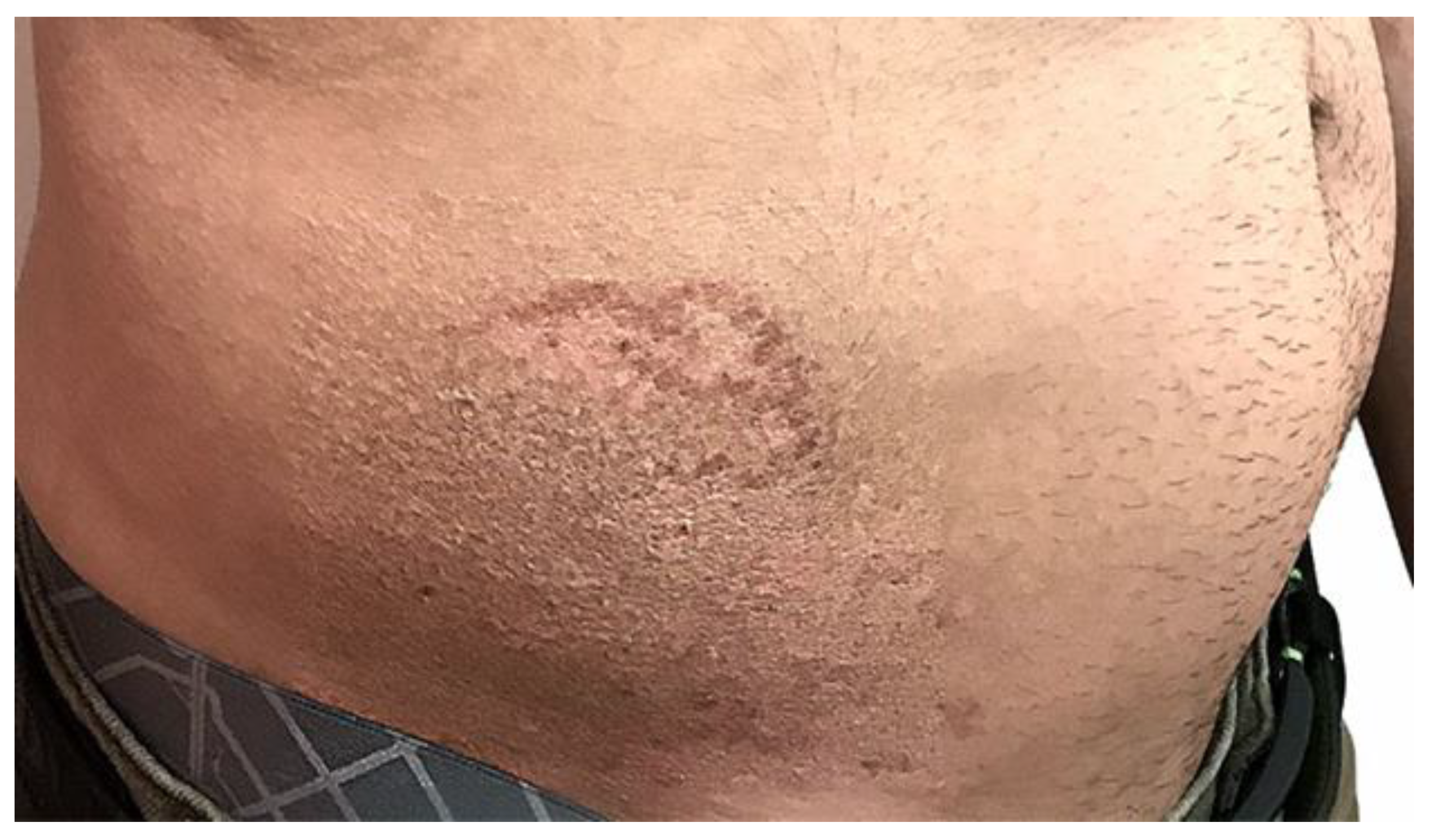
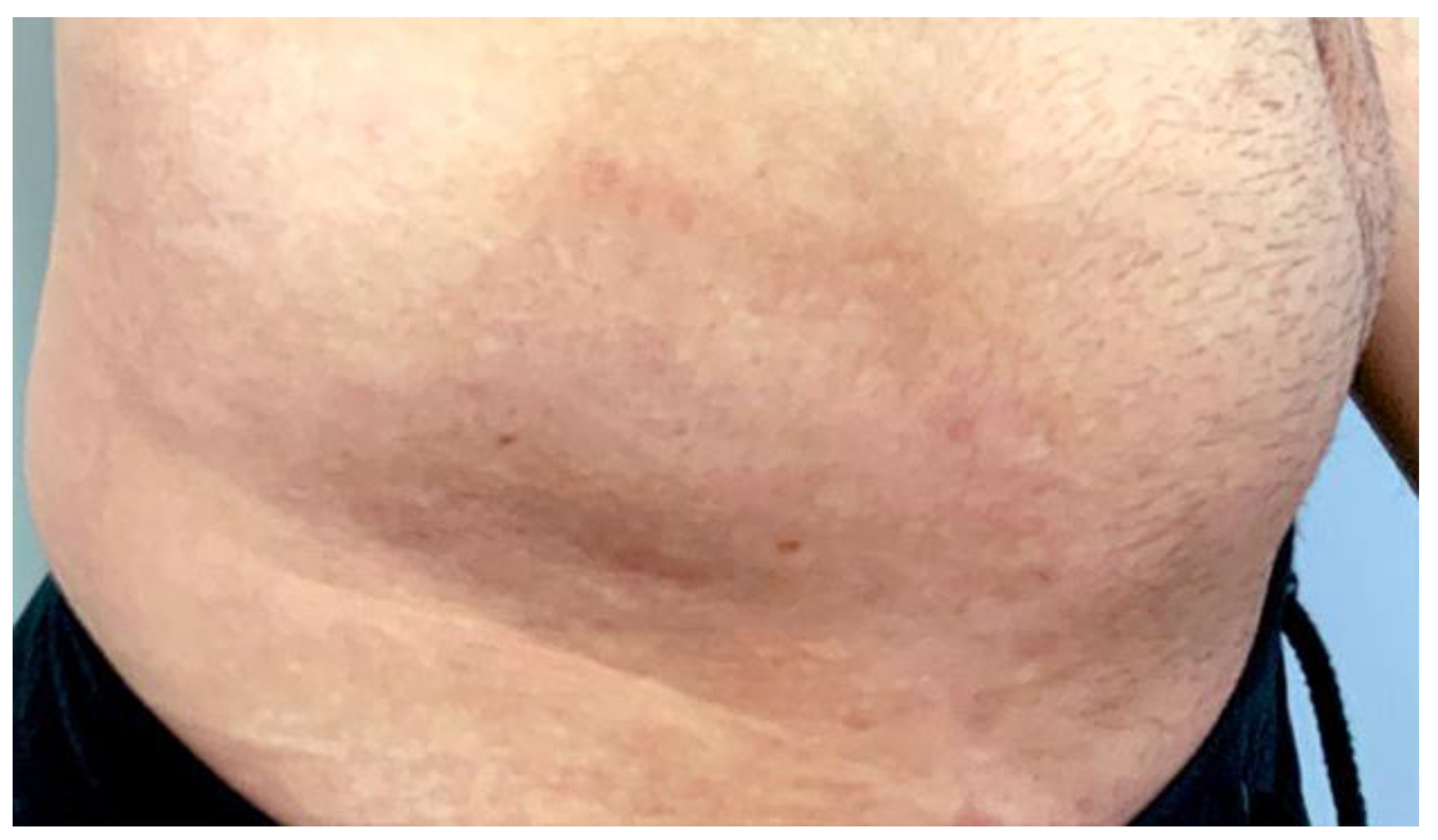
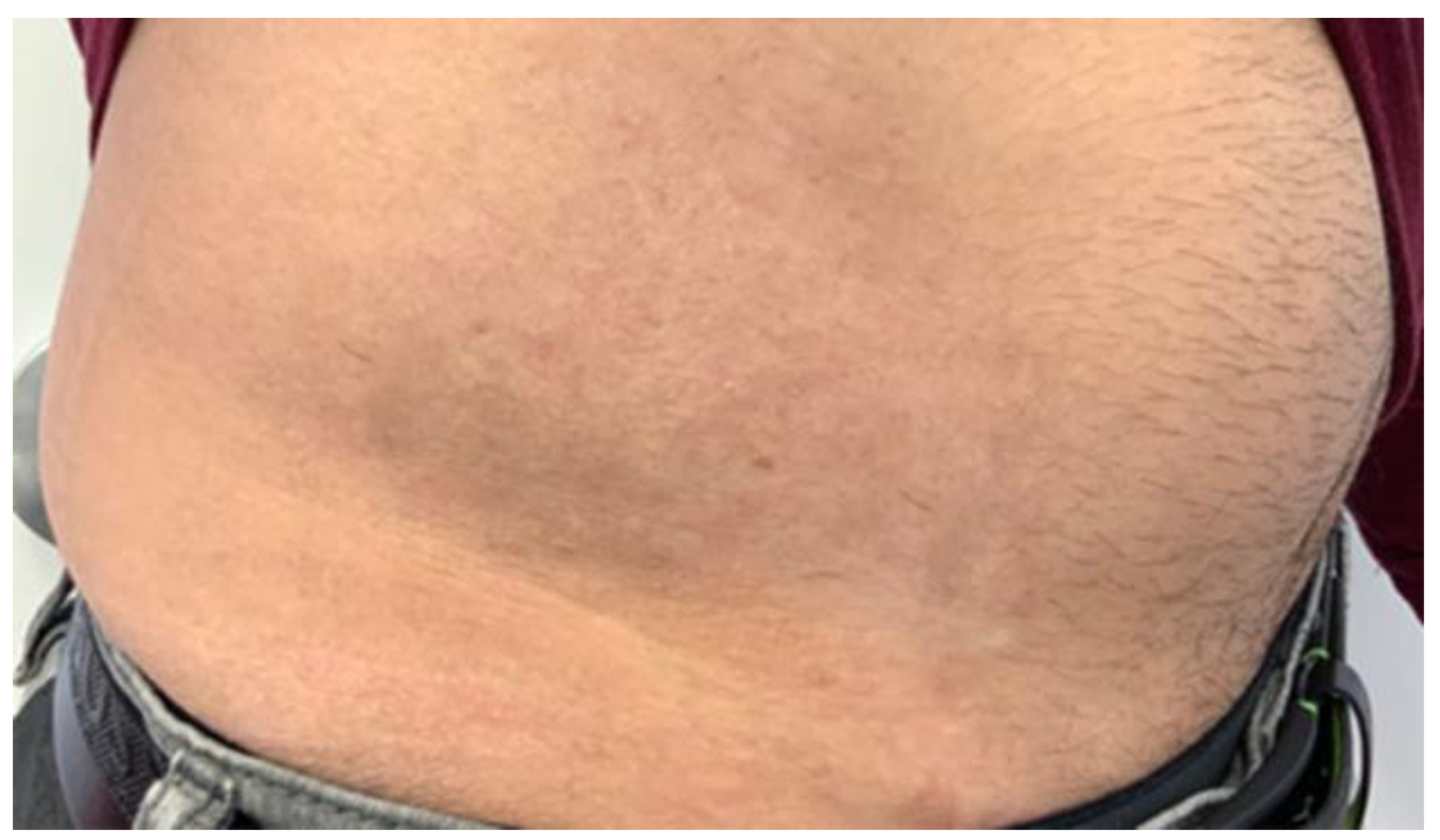
To resurface the skin, fractional Er-Yag was used. Figure 1 and Figure 2 show the lesion before and after the Fotona Er-Yag laser treatment, respectively. The laser was programmed to ablate the epidermis (50 μm) and a portion of the dermis, the papillary dermis, at 260 μm. The fractional handpiece was used with a short pulse mode, the fluence was 90 J/cm2, and the frequency was set to level six. These settings provided 310 μm treatment. The endpoint was either pinpoint bleeding, petechiae or the visual elimination of lesions.
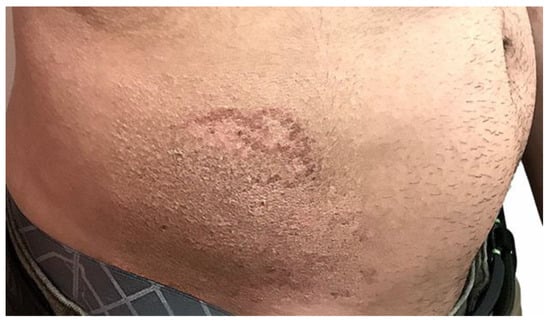
Figure 1.
Shows a photographic examination of the lesion prior to beginning treatment.
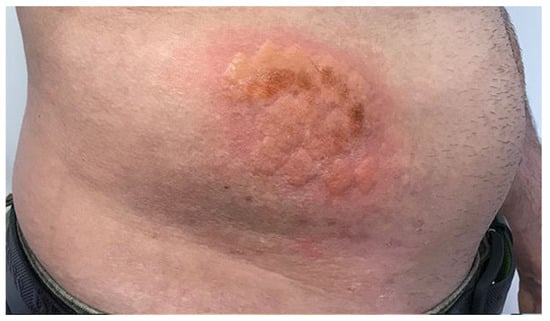
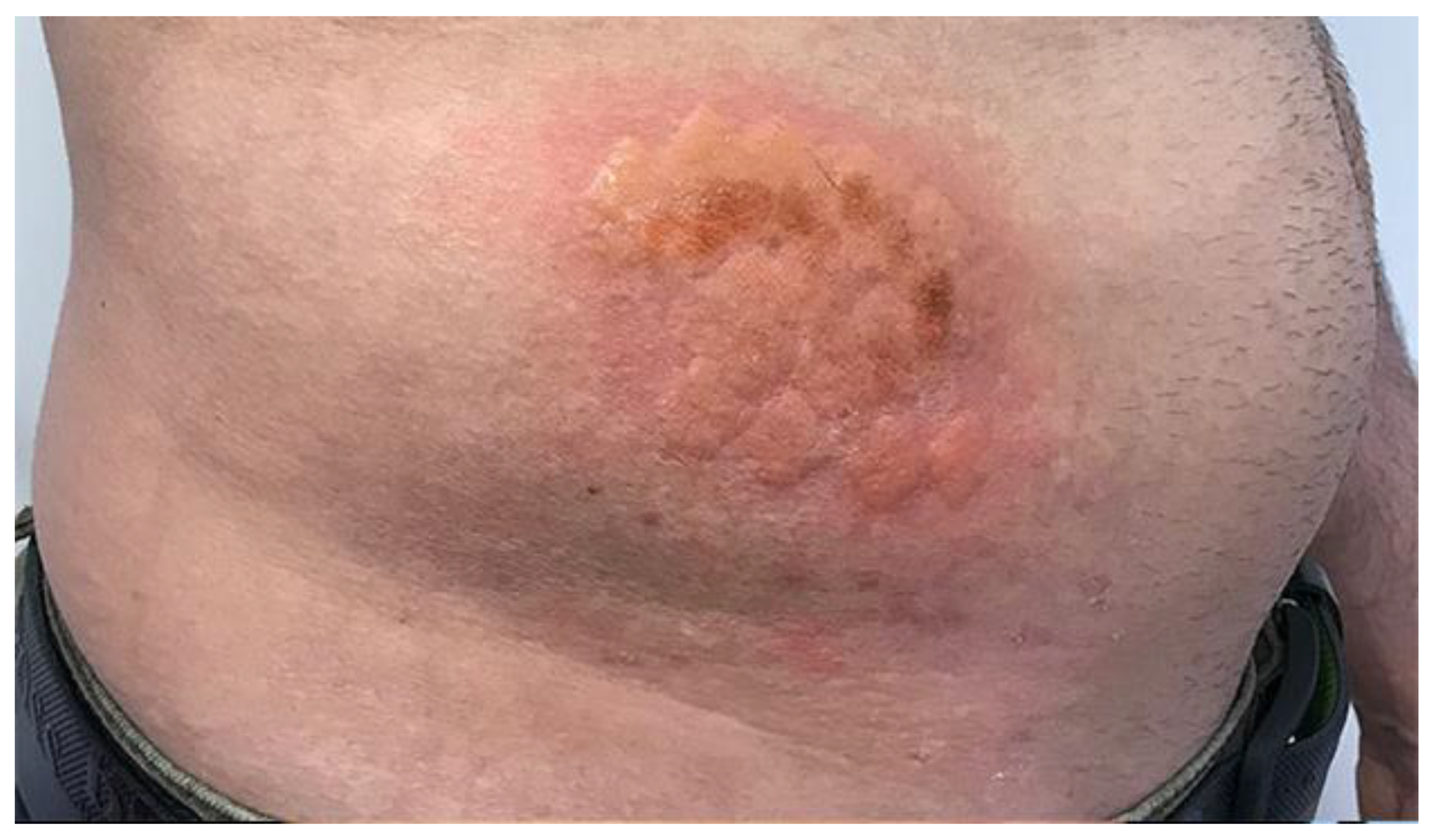
Figure 2.
Shows a photographic examination of the lesion directly after Er-Yag laser treatment.
4. Stage Two
The targeted skin lesions were treated with a series of three nanosecond laser sessions four months apart, six weeks after the first Er-Yag laser treatment (Figure 3, Figure 4 and Figure 5). Each session includes one pass of 1064 nm nanosecond laser, one pass of 585 nm nanosecond laser, and a light 10-micron peel with the Er-Yag in micro-short mode. The patient was instructed to apply the 4% HQ cream two weeks following each session. The treatment’s goal was to resurface the skin, improve the lesion area texture, pliability and alleviate hyperpigmentation to make it less visible against the background skin. Figure 4, Figure 5 and Figure 6 depict the skin lesion four weeks after each treatment in stage two. The irradiated area was covered with a thin layer of OTC antibiotic ointment (Polysporin®, Johnson & Johnson Inc. Markham, ON, Canada), then with a thick layer of a multipurpose healing ointment (AQUAPHOR®, Beiersdorf Inc. Wilton, CT, USA). We used non-woven gauze sponges for dressing purposes. The post-treatment guidelines, including dressing changing and cleaning instruction, were explained to the patient and handed a printed form.
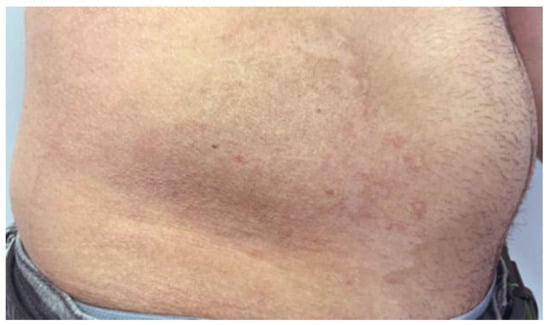
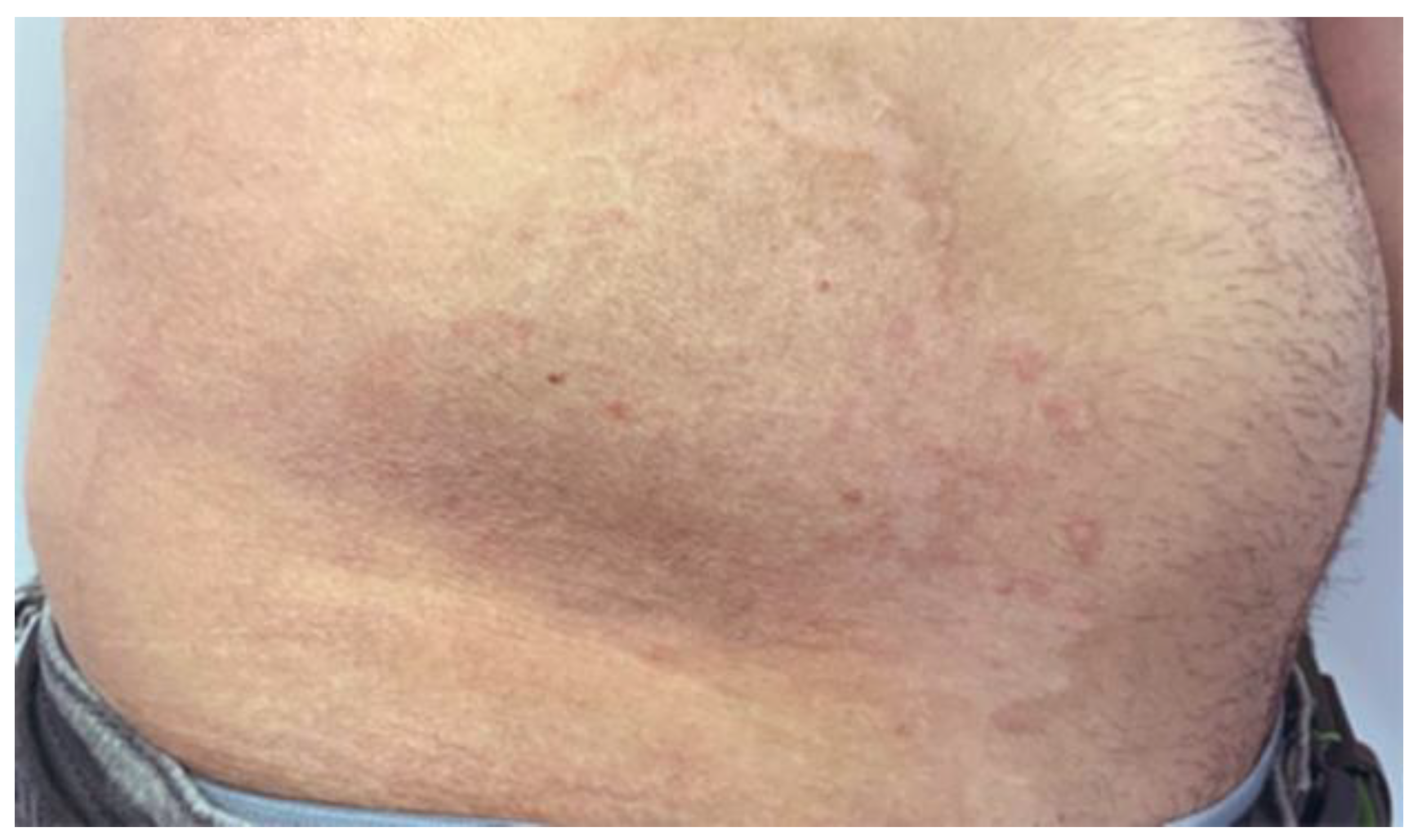
Figure 3.
Shows a photographic examination of the lesion directly the first 1064 and 595 Nd-Yag Q-switch nanosecond laser.
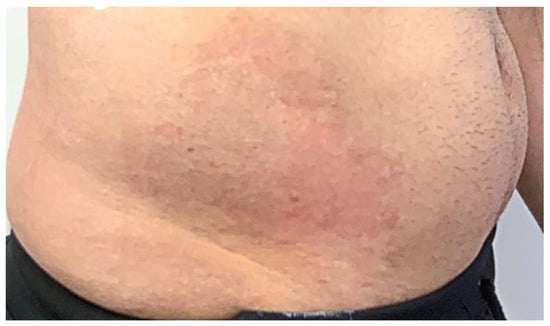
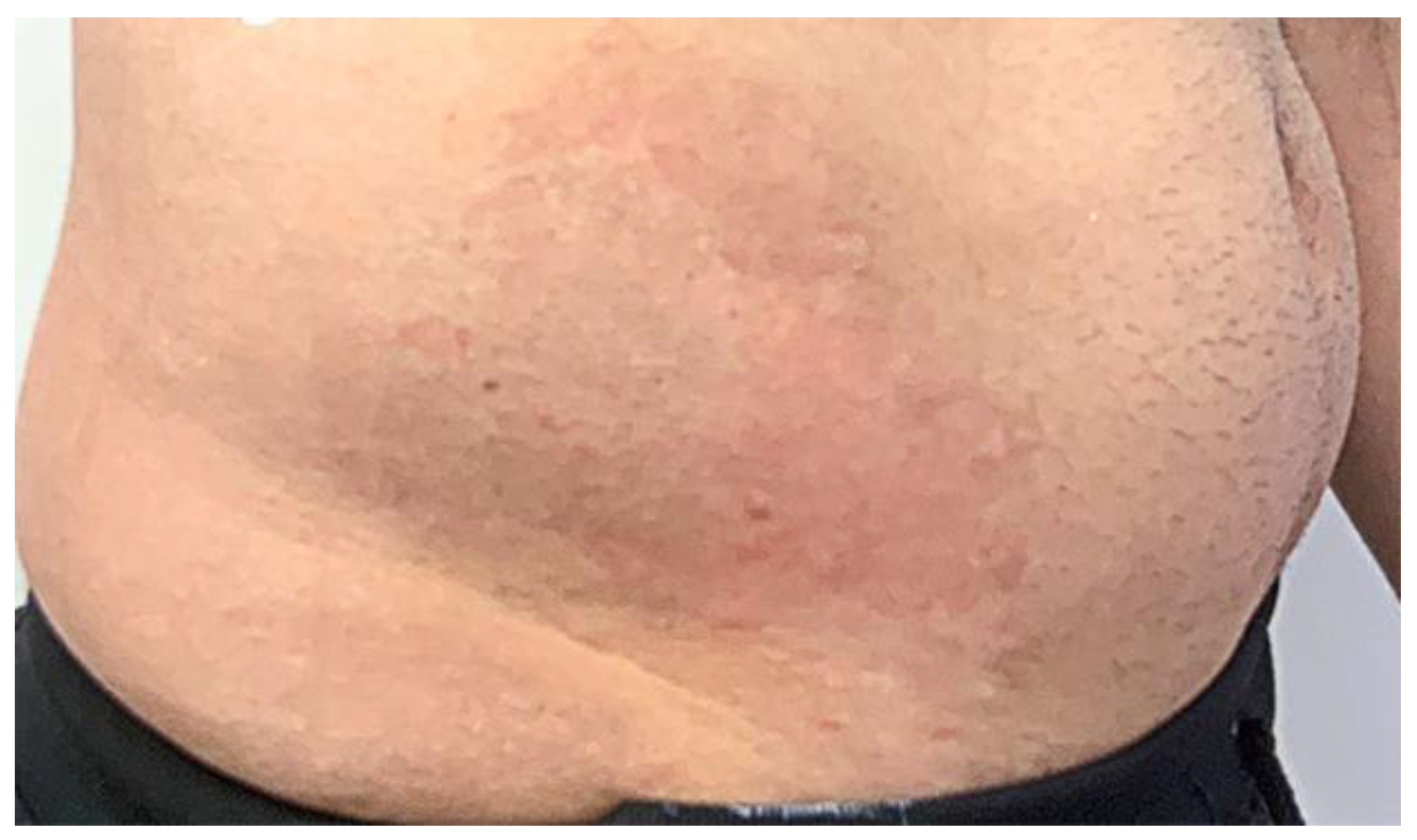
Figure 4.
Shows a photographic examination of the lesion directly the second 1064 and 595 Nd-Yag Q-switch nanosecond laser.
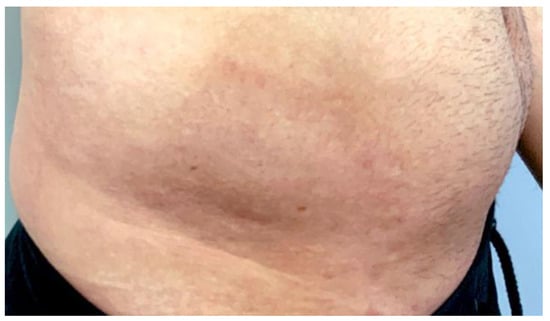
Figure 5.
Shows a photographic examination of the lesion directly the third 1064 and 595 Nd-Yag Q-switch nanosecond laser.
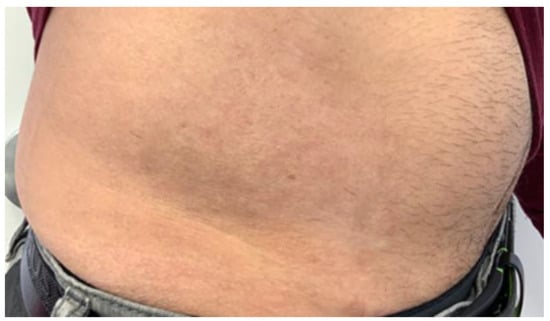
Figure 6.
Shows a photographic examination of the lesion four months after the third 1064 and 595 Nd-Yag Q-switch nanosecond laser treatment.
5. Discussion
Several systematic and non-systematic reviews on scar and hyperpigmentation laser treatment have been published. In their data reporting and comparison, the majority of these reviews did not include the cause of the skin lesion [16,17]. The unanimous conclusion was that more research in the form of randomized trials is required. To the best of our knowledge, this is the first report that discusses the treatment of pigmentation and scarring that is specifically caused by HDC cutaneous injury. There are numerous cosmetic and surgical applications for lasers [12,18,19]. The application of a single laser may differ depending on the pulse width, fluence, and spot size. For example, a millisecond Alexandrite 755 nm laser can be used for laser hair removal. However, it is primarily used for tattoo and pigmentation removal in the picosecond range (4–8). Most lasers use a similar mechanism of action based on photothermolysis [20]. This phenomenon describes the transformation of photon energy into thermal energy via a selective medium known as a chromophore. The laser type and wavelength should be selected based on the patient’s skin type, lesion depths, and targeted chromophores that contribute to the photothermolysis process. Melanin with the highest absorbance, haemoglobin with the highest absorbance, and water with the highest absorbance are the three main chromophores that are targeted in cosmetic procedures. The high affinity of the laser to the chromophores results in the selectivity of any laser treatment. For example, highly pigmented lesions absorb more laser energy than surrounding skin cells. Photoacoustic properties are another mechanism of action that some lasers have. Lasers with very short pulse widths, such as those in the nanosecond and picosecond ranges, can generate powerful acoustic waves. As a result, the pigment particles (melanin or ink) are broken down into smaller ones. The small pigment particles are then removed via lymph drainage and phagocytosis [17,21]. Thermal relaxation, which goes hand in hand with pulse width, is an important concept to consider when considering laser treatment. Thermal energy accumulates in the targeted chromophores during laser exposure, and they are unable to contain the thermal energy for themselves. As a result, thermal energy spreads to bystander cells and tissues. The shorter the thermal relaxation time, the greater the affinity between the laser and the chromophores [22,23]. As a result, when targeting a lesion with high laser affinity, we should use lower fluency and shorter pulse width to avoid side effects like skin burns and post-inflammatory hyperpigmentation (PIH).
The light emitted by the Er-Yag solid-state laser has a wavelength of 2940 nm and has a high affinity for the water molecule, about 15 times that of CO2. As a result, when exposed to Er-Yag irradiation, the skin tissue vaporized instantly. The ability to perform highly precise ablation with little or no coagulation is the main advantage of Er-Yag in short pulse mode. The property enables us to perform controlled skin ablation while transferring less thermal energy to the surrounding tissues. As a result, cold ablations have a higher safety profile than other ablation lasers, such as CO2. The long-pulse mode allows for more coagulation and ablation. Cold ablation is used to remove dermal and epidermal layers, whereas hot ablation rejuvenates the skin.
During the first stage, we used the Er-Yag in Fractional mode. The fluence was set to 90 J/cm2 with a short pulse width and a turbo level six (stacking). This setting allows for precise cold ablation down to 310 μm. The goal of this treatment is to remove the epidermal lesion and a portion of the dermal lesion. Any patient with Fitzpatrick skin type III or higher goes through a preparation period in which they apply HQ cream, a tyrosine kinase inhibitor, to reduce the risk of rebound pigmentation and PIH. The elimination of visible lesion or the presence of pinpoint bleeding was used to determine the endpoint for Er-Yag laser treatment. After cleansing the area with sterilized normal saline, it developed a yellow tint, indicating ablation of the midpapillary dermis, which is bordered by localized erythema. The treated area was covered with a thin layer of triple antibiotic ointment (Polymyxin B Sulfate 10,000 units, Bacitracin Zinc 500 units, Gramicidin 0.25 mg), then a thick layer of a purified anhydrous lanoline and a layer of (Aquaphor).
The second stage aimed to remove the pigmented lesion and restore the skin’s even tone. The gold standard for pigmentation lesion management is the crystal Nd-Yag 1064 nm laser with nanosecond pulse width. The Nd-Yag laser was used with a collimated handpiece, a pulse width of 5–7 ns, a spot size of 7 mm, and a fluence of 1 J/cm2. The 595 nm Nd-Yag treatment aims to target vascularization and reduce redness. The fluence was set to 0.35 J/cm2 with the 5 mm gold toning handpiece.
Figure 3 shows a significant improvement in scarring and pigmentation in the treated area. However, after speaking with the patient, we decided to use the Q-switch nanosecond laser to reduce redness and improve skin tone and color. Figure 4, Figure 5 and Figure 6 show significant improvement in skin redness and texture following each session. Figure 6’s final results were satisfactory to the patient. The final Vancouver scar score in the last follow up visit was 1 as follows: Vascularity: 0, Pigmentation: 0, Pliability: 1, and Height: 0.
6. Conclusions
Laser technology has changed the way skin lesions and dermatological disorders are treated. Choosing the right endpoint, technology, and settings was critical. The total resolution of the lesion was achieved in five months, during which the lesion was treated with four laser sessions. The first session involved cold ablation with an Er-Yag fractional laser. The remaining sessions were carried out in the nanosecond range using 1064 and 595 nm Nd-Yag Q-switch lasers. To reduce the risk of PIH, the treated area underwent a preparation phase between each laser treatment, which included the application of 4% HQ cream. In this case report, our protocol demonstrated promising results in reducing scarring and pigmentation with minimal side effects and downtime. However, treatment parameters and intervals should be customized for each patient.
Author Contributions
Conceptualization, K.A., A.A., S.T., D.O.; validation, K.A., A.A., S.T., D.O.; investigation, K.A., A.A., S.T., D.O.; resources, K.A., A.A., S.T., D.O.; writing—original draft, K.A., D.O.; writing—review and editing, K.A., A.A., S.T., D.O.; visualization, K.A., A.A., S.T., D.O.; supervision, K.A., D.O.; project administration, K.A., A.A., S.T., D.O. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
This case report did not require an ethical approval.
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
All data collected during this study is reported in this manuscript. No other data were created or analyzed in this study. Data sharing is not applicable to this article.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Marks, L.R.; Nolan, N.S.; Liang, S.Y.; Durkin, M.J.; Weimer, M.B. Infectious Complications of Injection Drug Use. Med. Clin. 2022, 106, 187–200. [Google Scholar] [CrossRef]
- Robertson, R.; Broers, B.; Harris, M. Injecting drug use, the skin and vasculature. Addiction 2021, 116, 1914–1924. [Google Scholar] [CrossRef] [PubMed]
- Richardson, T.; Kerr, D. Skin-related complications of insulin therapy. Am. J. Clin. Dermatol. 2003, 4, 661–667. [Google Scholar] [CrossRef]
- Binder, E.; Lange, O.; Edlinger, M.; Meraner, D.; Abt, D.; Moser, C.; Steichen, E.; Hofer, S.E. Frequency of dermatological side effects of continuous subcutaneous insulin infusion in children and adolescents with type 1 diabetes. Exp. Clin. Endocrinol. Diabetes 2015, 123, 260–264. [Google Scholar] [CrossRef]
- Berg, A.K.; Olsen, B.S.; Thyssen, J.P.; Zachariae, C.; Simonsen, A.B.; Pilgaard, K.; Svensson, J. High frequencies of dermatological complications in children using insulin pumps or sensors. Pediatric Diabetes 2018, 19, 733–740. [Google Scholar] [CrossRef]
- Conwell, L.S.; Pope, E.; Artiles, A.M.; Mohanta, A.; Daneman, A.; Daneman, D. Dermatological complications of continuous subcutaneous insulin infusion in children and adolescents. J. Pediatrics 2008, 152, 622–628. [Google Scholar] [CrossRef]
- Al Hallak, K.; Tomi, S.; Omran, D. Q-switch nanosecond laser as innovative and instant management for bruises discoloration, a case report. J. Cosmet. Laser Ther. 2021, 23, 19–23. [Google Scholar] [CrossRef]
- Ogawa, R. The Most Current Algorithms for the Treatment and Prevention of Hypertrophic Scars and Keloids: A 2020 Update of the Algorithms Published 10 Years Ago. Plast. Reconstr. Surg. 2022, 149, 79e–94e. [Google Scholar] [CrossRef] [PubMed]
- Sarkar, R.; Choubey, V.; Devadasan, S. Hyperpigmentary Skin Disorders. Atlas Dermatol. Dermatopathol. Venereol. Inflamm. Dermatoses 2022, 11, 223. [Google Scholar]
- Nestor, M.S.; Fischer, D.; Arnold, D.; Matin, T.; Jones, J.L. Lasers and Aesthetic Devices: Skin Resurfacing, Tattoo Removal, and Body Contouring. In Tips and Tricks in Plastic Surgery; Springer: Cham, Switzerland, 2022; pp. 541–552. [Google Scholar]
- Gaffey, M.M.; Johnson, A.B. Laser Treatment of Pigmented Lesions; StatPearls: Treasure Island, FL, USA, 2020. [Google Scholar]
- Alhallak, K.; Omran, D.; Tomi, S.; Abdulhafid, A. Skin, Light and their Interactions, an In-Depth Review for Modern Light-Based Skin Therapies. J. Clin. Derm. Ther. 2021, 7, 2. [Google Scholar] [CrossRef]
- Jagdeo, J.; Austin, E.; Mamalis, A.; Wong, C.; Ho, D.; Siegel, D.M. Light-emitting diodes in dermatology: A systematic review of randomized controlled trials. Lasers Surg. Med. 2018, 50, 613–628. [Google Scholar] [CrossRef]
- Busche, M.N.; Thraen, A.-C.J.; Gohritz, A.; Rennekampff, H.-O.; Vogt, P.M. Burn scar evaluation using the cutometer® MPA 580 in comparison to “patient and observer scar assessment scale” and “vancouver scar scale”. J. Burn. Care Res. 2018, 39, 516–526. [Google Scholar] [CrossRef]
- Moran, B.; Humphrey, S.; Seal, A.; Berkowitz, J.; Zloty, D. Photographic assessment of postsurgical facial scars epidermally sutured with rapidly absorbable polyglactin 910 or nylon: A randomized clinical trial. J. Am. Acad. Dermatol. 2020, 83, 1395–1399. [Google Scholar] [CrossRef]
- Oosterhoff, T.C.; Beekman, V.K.; van der List, J.P.; Niessen, F.B. Laser treatment of specific scar characteristics in hypertrophic scars and keloid: A systematic review. J. Plast. Reconstr. Aesthetic Surg. 2021, 74, 48–64. [Google Scholar] [CrossRef] [PubMed]
- Wu, D.C.; Goldman, M.P.; Wat, H.; Chan, H.H. A systematic review of picosecond laser in dermatology: Evidence and recommendations. Lasers Surg. Med. 2021, 53, 9–49. [Google Scholar] [CrossRef]
- Conforti, C.; Vezzoni, R.; Giuffrida, R.; Fai, A.; Fadda, S.; Marangi, G.F.; Persichetti, P.; Piccolo, D.; Segreto, F.; Zalaudek, I.; et al. An overview on the role of CO2 laser in general dermatology. Dermatol. Ther. 2021, 34, e14692. [Google Scholar] [CrossRef]
- Passeron, T.; Genedy, R.; Salah, L.; Fusade, T.; Kositratna, G.; Laubach, H.J.; Marini, L.; Badawi, A. Laser treatment of hyperpigmented lesions: Position statement of the European Society of Laser in Dermatology. J. Eur. Acad. Dermatol. Venereol. 2019, 33, 987–1005. [Google Scholar] [CrossRef]
- Fratila, A.; Gauglitz, G.; Strohbücker, A.; Radu, D. Selective photothermolysis of spider veins and reticular varices with the long-pulsed Nd: YAG laser. Phlebologie 2020, 49, 16–22. [Google Scholar]
- Ungaksornpairote, C.; Manuskiatti, W.; Junsuwan, N.; Wanitphakdeedecha, R. A prospective, split-face, randomized study comparing picosecond to Q-switched Nd: YAG laser for treatment of epidermal and dermal pigmented lesions in Asians. Dermatol. Surg. 2020, 46, 1671–1675. [Google Scholar] [CrossRef] [PubMed]
- Beyzaee, A.M.; Patil, A.; Goldust, M.; Moslemi, M.; Kazeminejad, A.; Rokni, G.R. Comparative Efficacy of Fractional CO2 Laser and Q-Switched Nd: YAG Laser in Combination Therapy with Tranexamic Acid in Refractory Melasma: Results of a Prospective Clinical Trial. Cosmetics 2021, 8, 37. [Google Scholar] [CrossRef]
- Robredo, I.G.C. Q-switched 1064 nm Nd: YAG laser in treating axillary hyperpigmentation in Filipino women with skin types IV–V. J. Drugs Dermatol. 2020, 19, 66–69. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).