β-Ti Alloys for Orthopedic and Dental Applications: A Review of Progress on Improvement of Properties through Surface Modification
Abstract
:1. Introduction
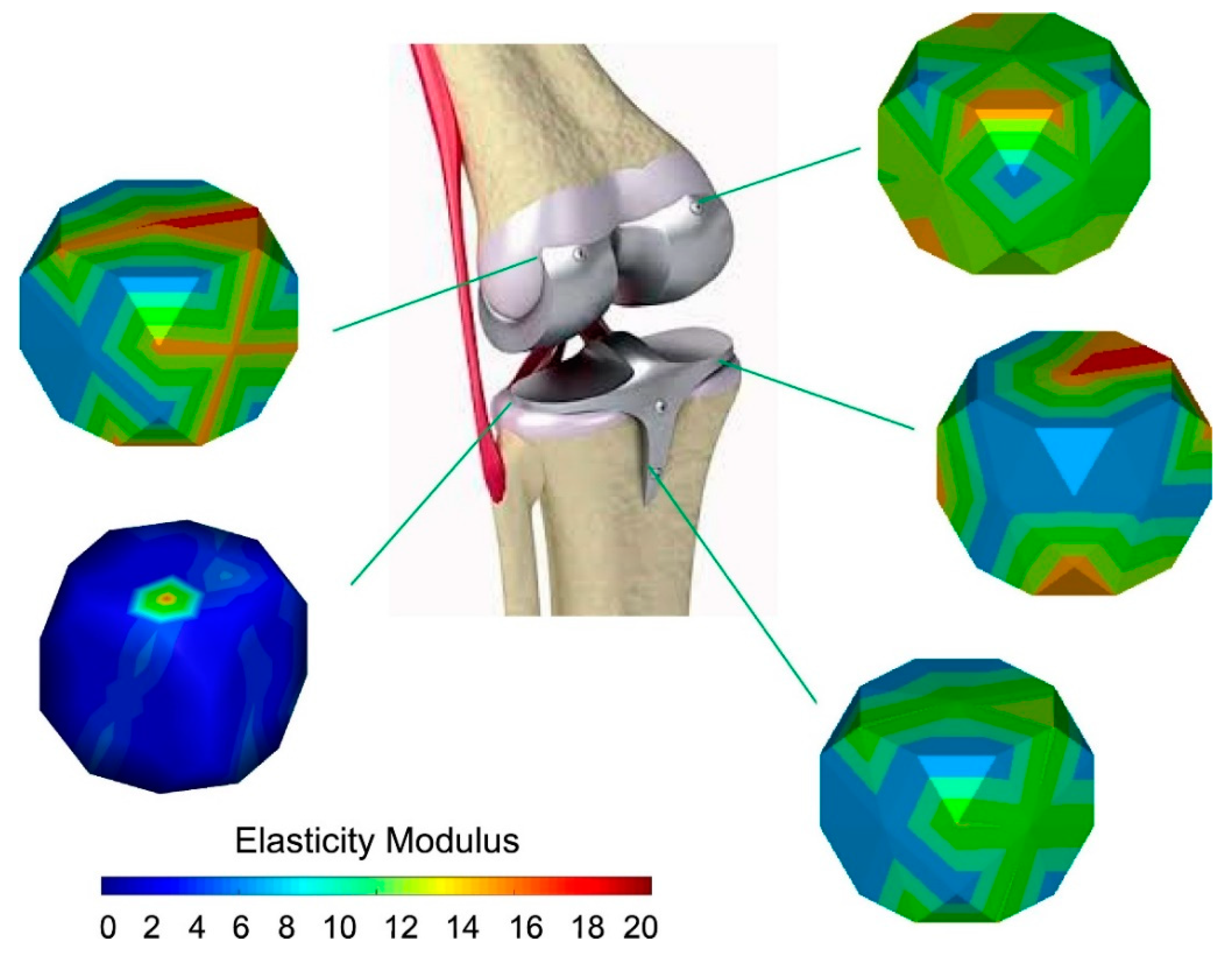
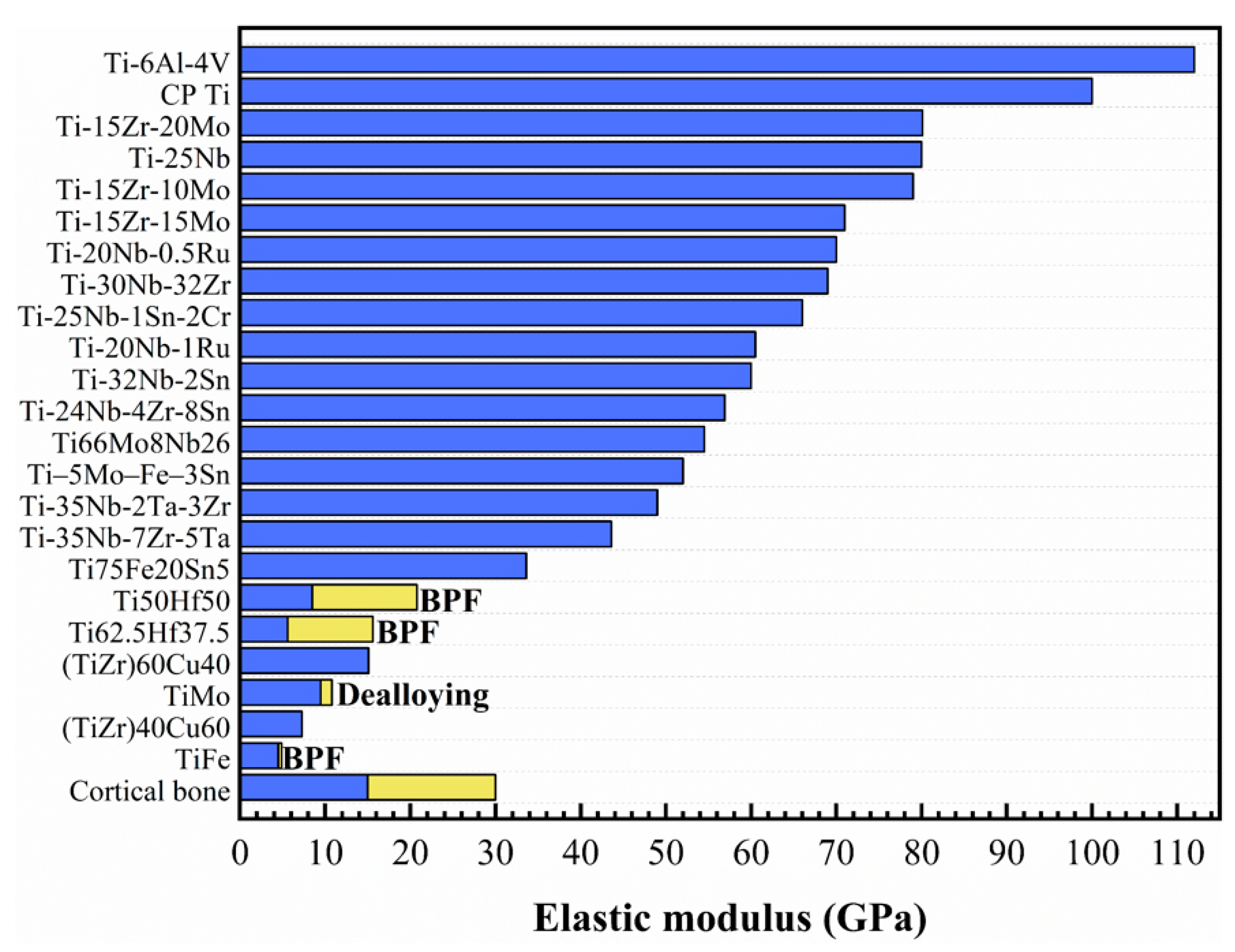
2. Elastic Modulus
3. Hardness
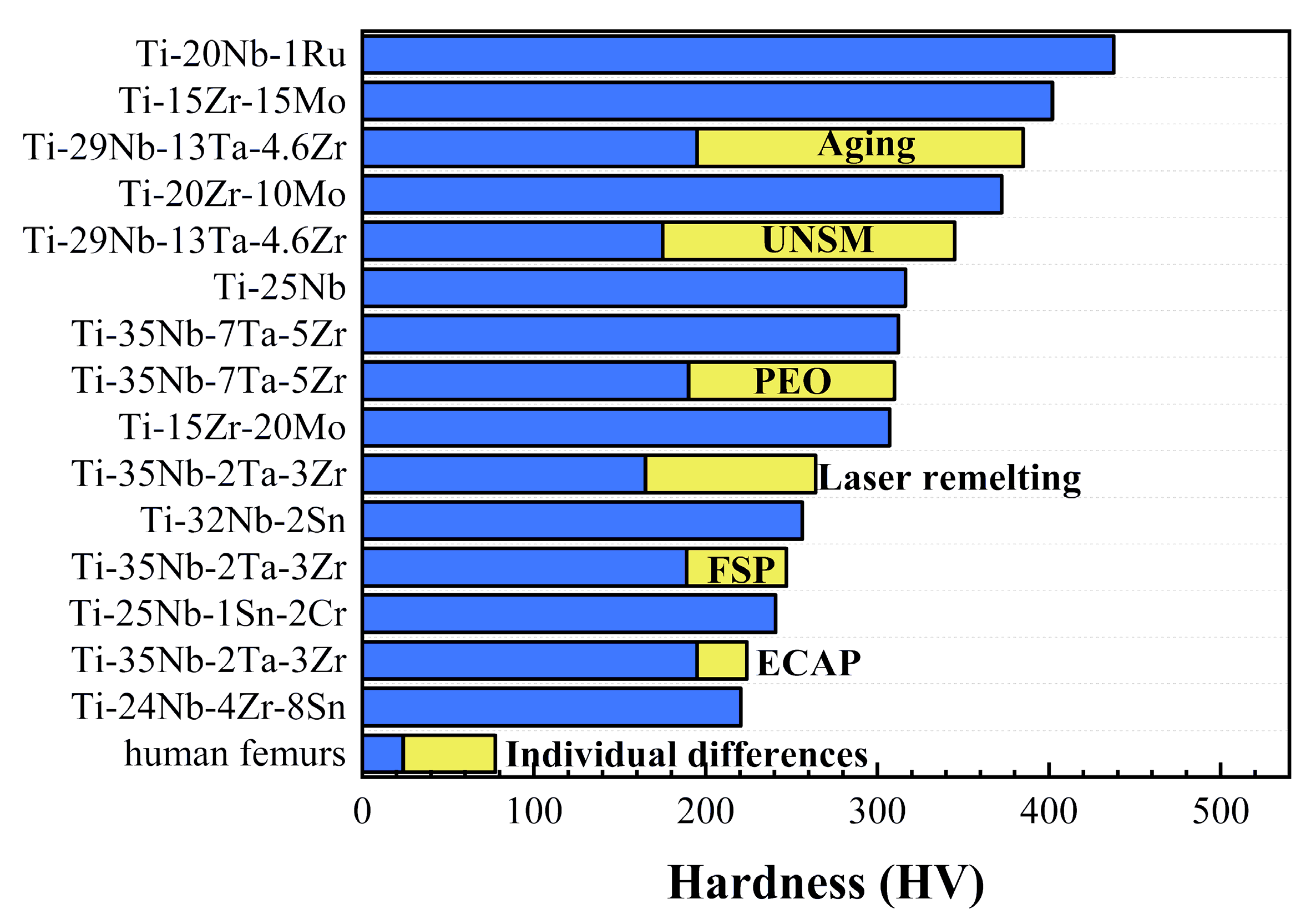
4. Wear Resistance
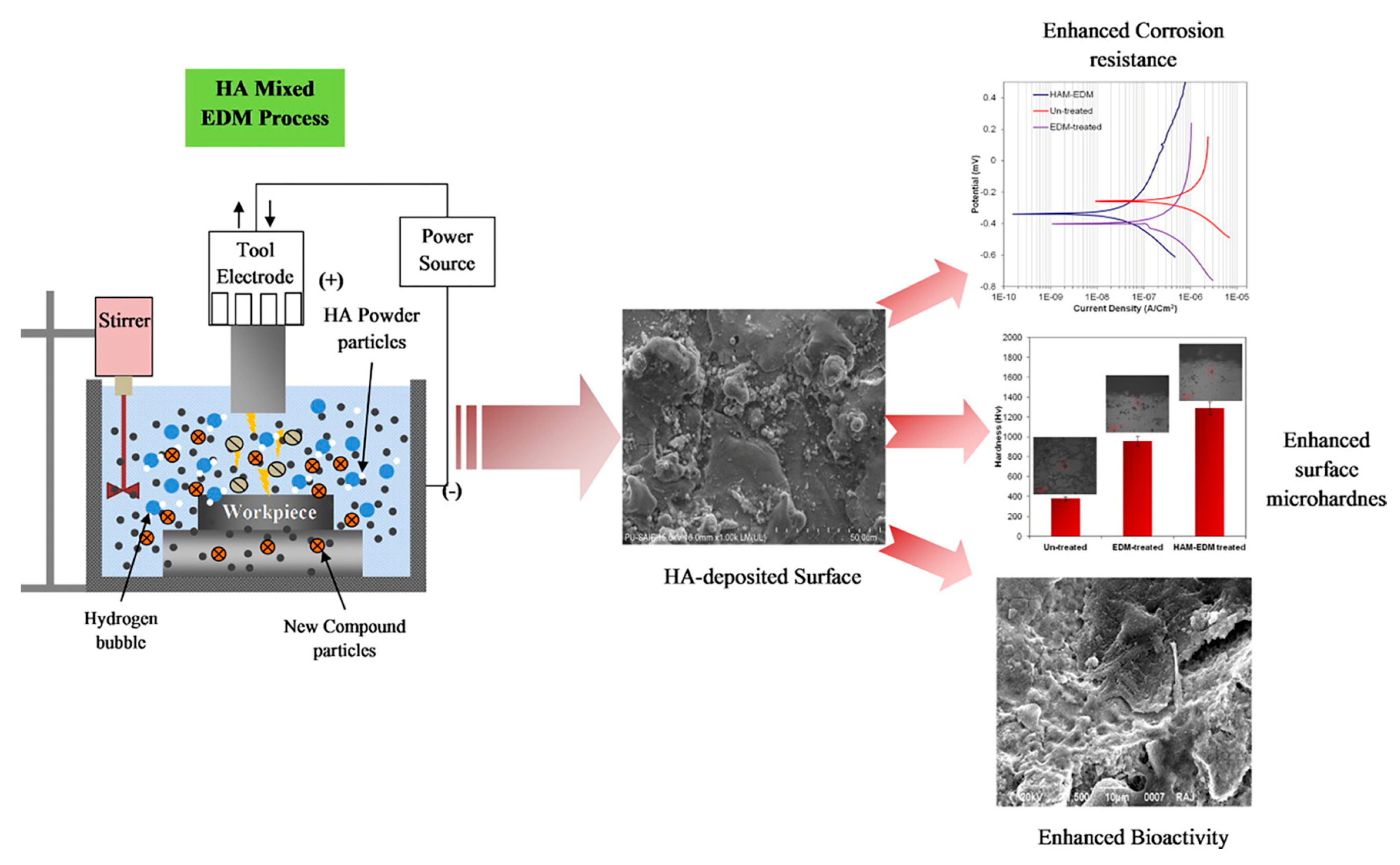
5. Corrosion Resistance
6. Biological Response
6.1. Antibacterial Property
6.2. Bone Regeneration
7. Shortcomings and Prospects
8. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Zhang, L.C.; Chen, L.Y. A Review on Biomedical Titanium Alloys: Recent Progress and Prospect. Adv. Eng. Mater. 2019, 21, 1801215. [Google Scholar] [CrossRef] [Green Version]
- Raji, S.A.; Popoola AP, I.; Pityana, S.L.; Popoola, O.M. Characteristic effects of alloying elements on β solidifying titanium aluminides: A review. Heliyon 2020, 6, e04463. [Google Scholar] [CrossRef]
- Rossi, M.C.; Amado, J.M.; Tobar, M.J.; Vicente, A.; Yañez, A.; Amigó, V. Effect of alloying elements on laser surface modification of powder metallurgy to improve surface mechanical properties of beta titanium alloys for biomedical application. J. Mater. Res. Technol. 2021, 14, 1222–1234. [Google Scholar] [CrossRef]
- Pitchi, C.S.; Priyadarshini, A.; Sana, G.; Narala, S.K.R. A review on alloy composition and synthesis of β-Titanium alloys for biomedical applications. Mater. Today Proc. 2020, 26, 3297–3304. [Google Scholar] [CrossRef]
- Goldberg, J. An Evaluation of Beta Titanium Alloys for Use in Orthodontic Appliances. J. Dent. Res. 1979, 58, 593–599. [Google Scholar] [CrossRef]
- Liu, S.; Liu, W.; Liu, J.; Liu, J.; Zhang, L.; Tang, Y.; Zhang, L.-C.; Wang, L. Compressive properties and microstructure evolution in NiTiNb alloy with mesh eutectic phase. Mater. Sci. Eng. A 2021, 801, 140434. [Google Scholar] [CrossRef]
- Geetha, M.; Singh, A.K.; Asokamani, R.; Gogia, A.K. Ti based biomaterials, the ultimate choice for orthopaedic implants—A review. Prog. Mater. Sci. 2009, 54, 397–425. [Google Scholar] [CrossRef]
- Bolzoni, L.; Ruiz-Navas, E.M.; Gordo, E. Investigation of the factors influencing the tensile behaviour of PM Ti–3Al–2.5V alloy. Mater. Sci. Eng. A 2014, 609, 266–272. [Google Scholar] [CrossRef] [Green Version]
- Semlitsch, M.F.; Weber, H.; Streicher, R.M.; Schön, R. Joint replacement components made of hot-forged and surface-treated Ti-6Al-7Nb alloy. Biomaterials 1992, 13, 781–788. [Google Scholar] [CrossRef]
- He, G.; Liu, H.; Tan, Q.; Ni, J. Diffusion bonding of Ti–2.5Al–2.5Mo–2.5Zr and Co–Cr–Mo alloys. J. Alloys Compd. 2011, 509, 7324–7329. [Google Scholar] [CrossRef]
- Kwon, Y.M.; An, S.; Yeo, I.; Tirumala, V.; Chen, W.; Klemt, C. Radiographic Risk Factors Associated With Adverse Local Tissue Reaction in Head-Neck Taper Corrosion of Primary Metal-on-Polyethylene Total Hip Arthroplasty. J. Am. Acad. Orthop. Surg. 2021, 29, 353–360. [Google Scholar] [CrossRef]
- Sak, A.; Moskalewicz, T.; Zimowski, S.; Cieniek, L.; Dubiel, B.; Radziszewska, A.; Kot, M.; Lukaszczyk, A. Influence of polyetheretherketone coatings on the Ti-13Nb-13Zr titanium alloy’s bio-tribological properties and corrosion resistance. Mater. Sci. Eng. C Mater. Biol. Appl. 2016, 63, 52–61. [Google Scholar] [CrossRef]
- Liu, Y.J.; Li, S.J.; Wang, H.L.; Hou, W.T.; Hao, Y.L.; Yang, R.; Sercombe, T.B.; Zhang, L.C. Microstructure, defects and mechanical behavior of beta-type titanium porous structures manufactured by electron beam melting and selective laser melting. Acta Mater. 2016, 113, 56–67. [Google Scholar] [CrossRef] [Green Version]
- Liu, Y.; Li, S.; Hou, W.; Wang, S.; Hao, Y.; Yang, R.; Sercombe, T.B.; Zhang, L.-C. Electron Beam Melted Beta-type Ti–24Nb–4Zr–8Sn Porous Structures With High Strength-to-Modulus Ratio. J. Mater. Sci. Technol. 2016, 32, 505–508. [Google Scholar] [CrossRef] [Green Version]
- Ho, W.F.; Ju, C.P.; Chern Lin, J.H. Structure and properties of cast binary Ti–Mo alloys. Biomaterials 1999, 20, 2115–2122. [Google Scholar] [CrossRef]
- Zha, S. Study on the Microstructure and Property of New β-Ti28Nb24.5Zr Alloy for Biomedic Applications. Master’s Thesis, Tianjin University, Tianjin, China, 2006. [Google Scholar]
- Zhu, C.; Lv, Y.; Qian, C.; Ding, Z.; Jiao, T.; Gu, X.; Lu, E.; Wang, L.; Zhang, F. Microstructures, mechanical, and biological properties of a novel Ti-6V-4V/zinc surface nanocomposite prepared by friction stir processing. Int. J. Nanomed. 2018, 13, 1881. [Google Scholar] [CrossRef] [Green Version]
- Wang, L.; Xie, L.; Lv, Y.; Zhang, L.-C.; Chen, L.; Meng, Q.; Qu, J.; Zhang, D.; Lu, W. Microstructure evolution and superelastic behavior in Ti-35Nb-2Ta-3Zr alloy processed by friction stir processing. Acta Mater. 2017, 131, 499–510. [Google Scholar] [CrossRef] [Green Version]
- Hafeez, N.; Liu, J.; Wang, L.; Wei, D.; Tang, Y.; Lu, W.; Zhang, L.-C. Superelastic response of low-modulus porous beta-type Ti-35Nb-2Ta-3Zr alloy fabricated by laser powder bed fusion. Addit. Manuf. 2020, 34, 101264. [Google Scholar] [CrossRef]
- Raza, D.; Kumar, G.; Uzair, M.; Singh, M.K.; Sultan, D.; Kumar, R. Development and heat treatment of β-phase titanium alloy for orthopedic application. Mater. Today Proc. 2021. [Google Scholar] [CrossRef]
- Karre, R.; Dey, S.R. Progress in Development of Beta Titanium Alloys for Biomedical Applications. In Encyclopedia of Smart Materials; Elsevier: Amsterdam, The Netherlands, 2019; Volume 5, pp. 512–527. [Google Scholar] [CrossRef]
- Liu, S.; Liu, J.; Wang, L.; Ma, R.L.W.; Zhong, Y.; Lu, W.; Zhang, L.C. Superelastic behavior of in-situ eutectic-reaction manufactured high strength 3D porous NiTi-Nb scaffold. Scr. Mater. 2020, 181, 121–126. [Google Scholar]
- Xie, K.Y.; Wang, Y.; Zhao, Y.; Chang, L.; Wang, G.; Chen, Z.; Cao, Y.; Liao, X.; Lavernia, E.J.; Valiev, R.Z.; et al. Nanocrystalline beta-Ti alloy with high hardness, low Young’s modulus and excellent in vitro biocompatibility for biomedical applications. Mater Sci. Eng. C Mater. Biol. Appl. 2013, 33, 3530–3536. [Google Scholar] [CrossRef]
- Singleton, R.C.; Pharr, G.M.; Nyman, J.S. Increased tissue-level storage modulus and hardness with age in male cortical bone and its association with decreased fracture toughness. Bone 2021, 148, 115949. [Google Scholar] [CrossRef]
- Callioglu, S.; Acar, P. Design of beta-Titanium microstructures for implant materials. Mater. Sci. Eng. C Mater. Biol. Appl. 2020, 110, 110715. [Google Scholar] [CrossRef] [PubMed]
- Dearnley, P.A.; Dahm, K.L.; Çimenoǧlu, H. The corrosion–wear behaviour of thermally oxidised CP-Ti and Ti–6Al–4V. Wear 2004, 256, 469–479. [Google Scholar] [CrossRef]
- Niinomi, M.; Kuroda, D.; Fukunaga, K.-I.; Morinaga, M.; Kato, Y.; Yashiro, T.; Suzuki, A. Corrosion wear fracture of new β type biomedical titanium alloys. Mater. Sci. Eng. A 1999, 263, 193–199. [Google Scholar] [CrossRef]
- Kaur, S.; Ghadirinejad, K.; Oskouei, R.H. An Overview on the Tribological Performance of Titanium Alloys with Surface Modifications for Biomedical Applications. Lubricants 2019, 7, 65. [Google Scholar] [CrossRef] [Green Version]
- Bahl, S.; Suwas, S.; Chatterjee, K. Comprehensive review on alloy design, processing, and performance of β Titanium alloys as biomedical materials. Int. Mater. Rev. 2020, 66, 114–139. [Google Scholar] [CrossRef]
- Torrento, J.E.; Grandini, C.R.; Sousa, T.S.P.; Rocha, L.A.; Gonçalves, T.M.; Sottovia, L.; Rangel, E.C.; Cruz, N.C.; Correa, D.R.N. Bulk and surface design of MAO-treated Ti-15Zr-15Mo-Ag alloys for potential use as biofunctional implants. Mater. Lett. 2020, 269, 127661. [Google Scholar] [CrossRef]
- Liu, S.; Wang, Q.; Liu, W.; Tang, Y.; Liu, J.; Zhang, H.; Liu, X.; Liu, J.; Yang, J.; Zhang, L.C.; et al. Multi-scale hybrid modified coatings on titanium implants for non-cytotoxicity and antibacterial properties. Nanoscale 2021, 13, 10587–10599. [Google Scholar] [CrossRef] [PubMed]
- Kandavalli, S.R.; Wang, Q.; Ebrahimi, M.; Gode, C.; Djavanroodi, F.; Attarilar, S.; Liu, S. A Brief Review on the Evolution of Metallic Dental Implants: History, Design, and Application. Front. Mater. 2021, 8, 140. [Google Scholar] [CrossRef]
- Attarilar, S.; Yang, J.; Ebrahimi, M.; Wang, Q.; Liu, J.; Tang, Y.; Yang, J. The Toxicity Phenomenon and the Related Occurrence in Metal and Metal Oxide Nanoparticles: A Brief Review From the Biomedical Perspective. Front. Bioeng. Biotechnol. 2020, 8, 822. [Google Scholar] [CrossRef]
- Çaha, I.; Alves, A.C.; Rocha, L.A.; Toptan, F. A Review on Bio-functionalization of β-Ti Alloys. J. Bio-Tribo-Corros. 2020, 6, 1–31. [Google Scholar] [CrossRef]
- Wang, Q.; Zhou, P.; Liu, S.; Attarilar, S.; Ma, R.L.; Zhong, Y.; Wang, L. Multi-Scale Surface Treatments of Titanium Implants for Rapid Osseointegration: A Review. Nanomater 2020, 10, 1244. [Google Scholar] [CrossRef]
- Wang, Q.; Wu, L.; Liu, S.; Cao, P.; Yang, J.; Wang, L. Nanostructured Titanium Alloys Surface Modification Technology for Antibacterial and Osteogenic Properties. Curr. Nanosci. 2021, 17, 175–193. [Google Scholar] [CrossRef]
- Zhang, L.-C.; Chen, L.-Y.; Wang, L. Surface Modification of Titanium and Titanium Alloys: Technologies, Developments, and Future Interests. Adv. Eng. Mater. 2020, 22, 1901258. [Google Scholar] [CrossRef]
- Kurup, A.; Dhatrak, P.; Khasnis, N. Surface modification techniques of titanium and titanium alloys for biomedical dental applications: A review. Mater. Today Proc. 2021, 39, 84–90. [Google Scholar] [CrossRef]
- Liang, S. Review of the Design of Titanium Alloys with Low Elastic Modulus as Implant Materials. Adv. Eng. Mater. 2020, 22, 2000555. [Google Scholar] [CrossRef]
- Okulov, I.V.; Okulov, A.V.; Soldatov, I.V.; Luthringer, B.; Willumeit-Romer, R.; Wada, T.; Kato, H.; Weissmuller, J.; Markmann, J. Open porous dealloying-based biomaterials as a novel biomaterial platform. Mater. Sci. Eng. C Mater. Biol. Appl. 2018, 88, 95–103. [Google Scholar] [CrossRef] [PubMed]
- Luthringer, B.J.; Ali, F.; Akaichi, H.; Feyerabend, F.; Ebel, T.; Willumeit, R. Production, characterisation, and cytocompatibility of porous titanium-based particulate scaffolds. J. Mater. Sci. Mater. Med. 2013, 24, 2337–2358. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Prashanth, K.; Zhuravleva, K.; Okulov, I.; Calin, M.; Eckert, J.; Gebert, A. Mechanical and Corrosion Behavior of New Generation Ti-45Nb Porous Alloys Implant Devices. Technologies 2016, 4, 33. [Google Scholar] [CrossRef] [Green Version]
- Okulov, I.V.; Weissmuller, J.; Markmann, J. Dealloying-based interpenetrating-phase nanocomposites matching the elastic behavior of human bone. Sci. Rep. 2017, 7, 20. [Google Scholar] [CrossRef]
- Okulov, A.V.; Volegov, A.S.; Weissmüller, J.; Markmann, J.; Okulov, I.V. Dealloying-based metal-polymer composites for biomedical applications. Scr. Mater. 2018, 146, 290–294. [Google Scholar] [CrossRef]
- Liu, J.; Tang, Y.; Liu, J.; Wang, L. Research progress in titanium alloy in the field of orthopaedic implants. J. Mater. Eng. 2021, 49, 11–15. [Google Scholar]
- Okulov, I.V.; Okulov, A.V.; Volegov, A.S.; Markmann, J. Tuning microstructure and mechanical properties of open porous TiNb and TiFe alloys by optimization of dealloying parameters. Scr. Mater. 2018, 154, 68–72. [Google Scholar] [CrossRef]
- Berger, S.A.; Okulov, I.V. Open Porous α + β Titanium Alloy by Liquid Metal Dealloying for Biomedical Applications. Metals 2020, 10, 1450. [Google Scholar] [CrossRef]
- Li, P.; Zhang, H.; Tong, T.; He, Z. The rapidly solidified β-type Ti–Fe–Sn alloys with high specific strength and low elastic modulus. J. Alloys Compd. 2019, 786, 986–994. [Google Scholar] [CrossRef]
- Xu, Y.; Gao, J.; Huang, Y.; Rainforth, W.M. A low-cost metastable beta Ti alloy with high elastic admissible strain and enhanced ductility for orthopaedic application. J. Alloys Compd. 2020, 835, 155391. [Google Scholar] [CrossRef]
- Li, P.; Ma, X.; Tong, T.; Wang, Y. Microstructural and mechanical properties of β-type Ti–Mo–Nb biomedical alloys with low elastic modulus. J. Alloys Compd. 2020, 815, 152412. [Google Scholar] [CrossRef]
- Guo, X.; Zhang, C.; Tian, Q.; Yu, D. Liquid metals dealloying as a general approach for the selective extraction of metals and the fabrication of nanoporous metals: A review. Mater. Today Commun. 2021, 26, 102007. [Google Scholar] [CrossRef]
- Okulov, I.V.; Joo, S.H.; Okulov, A.V.; Volegov, A.S.; Luthringer, B.; Willumeit-Romer, R.; Zhang, L.; Madler, L.; Eckert, J.; Kato, H. Surface Functionalization of Biomedical Ti-6Al-7Nb Alloy by Liquid Metal Dealloying. Nanomater 2020, 10, 1479. [Google Scholar] [CrossRef]
- Okulov, I.V.; Wilmers, J.; Joo, S.-H.; Bargmann, S.; Kim, H.S.; Kato, H. Anomalous compliance of interpenetrating-phase composite of Ti and Mg synthesized by liquid metal dealloying. Scr. Mater. 2021, 194, 113660. [Google Scholar] [CrossRef]
- Zhu, Y.; Wang, X.; Wang, L.; Fu, Y.; Qin, J.; Lu, W.; Zhang, D. Influence of forging deformation and heat treatment on microstructure of Ti–xNb–3Zr–2Ta alloys. Mater. Sci. Eng. C 2012, 32, 126–132. [Google Scholar] [CrossRef]
- Zhang, T.; Liu, C.-T. Design of titanium alloys by additive manufacturing: A critical review. Adv. Powder Mater. 2021. [Google Scholar] [CrossRef]
- Wang, L.; Qu, J.; Chen, L.; Meng, Q.; Zhang, L.-C.; Qin, J.; Zhang, D.; Lu, W. Investigation of Deformation Mechanisms in β-Type Ti-35Nb-2Ta-3Zr Alloy via FSP Leading to Surface Strengthening. Metall. Mater. Trans. A 2015, 46, 4813–4818. [Google Scholar] [CrossRef]
- Niinomi, M. Fatigue performance and cyto-toxicity of low rigidity titanium alloy, Ti–29Nb–13Ta–4.6Zr. Biomaterials 2003, 24, 2673–2683. [Google Scholar] [CrossRef]
- Zhang, T.; Fan, Q.; Ma, X.; Wang, W.; Wang, K.; Shen, P.; Yang, J.; Wang, L. Effect of laser remelting on microstructural evolution and mechanical properties of Ti-35Nb-2Ta-3Zr alloy. Mater. Lett. 2019, 253, 310–313. [Google Scholar] [CrossRef]
- Lin, Z.; Wang, L.; Xue, X.; Lu, W.; Qin, J.; Zhang, D. Microstructure evolution and mechanical properties of a Ti-35Nb-3Zr-2Ta biomedical alloy processed by equal channel angular pressing (ECAP). Mater. Sci. Eng. C Mater. Biol. Appl. 2013, 33, 4551–4561. [Google Scholar] [CrossRef]
- Liu, R.; Yuan, S.; Lin, N.; Zeng, Q.; Wang, Z.; Wu, Y. Application of ultrasonic nanocrystal surface modification (UNSM) technique for surface strengthening of titanium and titanium alloys: A mini review. J. Mater. Res. Technol. 2021, 11, 351–377. [Google Scholar] [CrossRef]
- Wang, L.; Wang, Y.; Huang, W.; Liu, J.; Tang, Y.; Zhang, L.; Fu, Y.; Zhang, L.-C.; Lu, W. Tensile and superelastic behaviors of Ti-35Nb-2Ta-3Zr with gradient structure. Mater. Des. 2020, 194, 108961. [Google Scholar] [CrossRef]
- Niinomi, M.; Nakai, M. Titanium-Based Biomaterials for Preventing Stress Shielding between Implant Devices and Bone. Int. J. Biomater. 2011, 2011, 836587. [Google Scholar] [CrossRef] [Green Version]
- Kuroda, D.; Niinomi, M.; Morinaga, M.; Kato, Y.; Yashiro, T. Design and mechanical properties of new β type titanium alloys for implant materials. Mater. Sci. Eng. A 1998, 243, 244–249. [Google Scholar] [CrossRef]
- Niinomi, M.; Nakai, M.; Hieda, J. Development of new metallic alloys for biomedical applications. Acta Biomater. 2012, 8, 3888–3903. [Google Scholar] [CrossRef] [PubMed]
- Lee, Y.-S.; Niinomi, M.; Nakai, M.; Narita, K.; Cho, K.; Liu, H. Wear transition of solid-solution-strengthened Ti–29Nb–13Ta–4.6Zr alloys by interstitial oxygen for biomedical applications. J. Mech. Behav. Biomed. Mater. 2015, 51, 398–408. [Google Scholar] [CrossRef]
- Makuch, N.; Kulka, M.; Dziarski, P.; Przestacki, D. Laser surface alloying of commercially pure titanium with boron and carbon. Opt. Lasers Eng. 2014, 57, 64–81. [Google Scholar] [CrossRef]
- Gao, Q.; Yan, H.; Qin, Y.; Zhang, P.; Guo, J.; Chen, Z.; Yu, Z. Laser cladding Ti-Ni/TiN/TiW+TiS/WS2 self-lubricating wear resistant composite coating on Ti-6Al-4V alloy. Opt. Laser Technol. 2019, 113, 182–191. [Google Scholar] [CrossRef]
- Kheradmandfard, M.; Kashani-Bozorg, S.F.; Kim, C.L.; Hanzaki, A.Z.; Pyoun, Y.S.; Kim, J.H.; Amanov, A.; Kim, D.E. Nanostructured beta-type titanium alloy fabricated by ultrasonic nanocrystal surface modification. Ultrason. Sonochem. 2017, 39, 698–706. [Google Scholar] [CrossRef] [PubMed]
- Chauhan, A.S.; Jha, J.S.; Telrandhe, S.; Srinivas, V.; Gokhale, A.A.; Mishra, S.K. Laser surface treatment of α-β titanium alloy to develop a β -rich phase with very high hardness. J. Mater. Process. Technol. 2021, 288, 116873. [Google Scholar] [CrossRef]
- Molinari, A.; Straffelini, G.; Tesi, B.; Bacci, T. Dry sliding wear mechanisms of the Ti6Al4V alloy. Wear 1997, 208, 105–112. [Google Scholar] [CrossRef]
- Cui, W.-F.; Niu, F.-J.; Tan, Y.-L.; Qin, G.-W. Microstructure and tribocorrosion performance of nanocrystalline TiN graded coating on biomedical titanium alloy. Trans. Nonferrous Met. Soc. China 2019, 29, 1026–1035. [Google Scholar] [CrossRef]
- Graves, A.; Norgren, S.; Wan, W.; Singh, S.; Kritikos, M.; Xiao, C.; Crawforth, P.; Jackson, M. On the mechanism of crater wear in a high strength metastable β titanium alloy. Wear 2021, 484, 203998. [Google Scholar] [CrossRef]
- Majumdar, P.; Singh, S.B.; Chakraborty, M. Wear properties of Ti–13Zr–13Nb (wt.%) near β titanium alloy containing 0.5wt.% boron in dry condition, Hank’s solution and bovine serum. Mater. Sci. Eng. C 2010, 30, 1065–1075. [Google Scholar] [CrossRef]
- Mehdi, M.; Farokhzadeh, K.; Edrisy, A. Dry sliding wear behavior of superelastic Ti–10V–2Fe–3Al β-titanium alloy. Wear 2016, 350, 10–20. [Google Scholar] [CrossRef]
- Weng, Z.; Gu, K.; Cui, C.; Cai, H.; Liu, X.; Wang, J. Microstructure evolution and wear behavior of titanium alloy under cryogenic dry sliding wear condition. Mater. Charact. 2020, 165, 110385. [Google Scholar] [CrossRef]
- Li, X.X.; Zhou, Y.; Ji, X.L.; Li, Y.X.; Wang, S.Q. Effects of sliding velocity on tribo-oxides and wear behavior of Ti–6Al–4V alloy. Tribol. Int. 2015, 91, 228–234. [Google Scholar] [CrossRef]
- Huang, C.; Zhang, Y.; Vilar, R.; Shen, J. Dry sliding wear behavior of laser clad TiVCrAlSi high entropy alloy coatings on Ti–6Al–4V substrate. Mater. Des. 2012, 41, 338–343. [Google Scholar] [CrossRef]
- Tong, X.; Sun, Q.; Zhang, D.; Wang, K.; Dai, Y.; Shi, Z.; Li, Y.; Dargusch, M.; Huang, S.; Ma, J.; et al. Impact of scandium on mechanical properties, corrosion behavior, friction and wear performance, and cytotoxicity of a beta-type Ti-24Nb-38Zr-2Mo alloy for orthopedic applications. Acta Biomater. 2021, 134, 791–803. [Google Scholar] [CrossRef] [PubMed]
- Nakai, M.; Iwasaki, T.; Ueki, K. Differences in the effect of surface texturing on the wear loss of β-type Ti–Nb–Ta–Zr and (α+β)-type Ti–6Al–4V ELI alloys in contact with zirconia in physiological saline solution. J. Mech. Behav. Biomed. Mater. 2021, 124, 104808. [Google Scholar] [CrossRef]
- Jiang, X.; Dai, Y.; Xiang, Q.; Liu, J.; Yang, F.; Zhang, D. Microstructure and wear behavior of inductive nitriding layer in Ti–25Nb–3Zr–2Sn–3Mo alloys. Surf. Coat. Technol. 2021, 427, 127835. [Google Scholar] [CrossRef]
- Hua, K.; Zhang, Y.; Zhang, F.; Kou, H.; Li, X.; Wu, H.; Wang, H. Microstructure refinement and enhanced wear-resistance modulated by stress relaxation processing in a metastable β titanium alloy. Mater. Charact. 2021, 181, 111505. [Google Scholar] [CrossRef]
- Kheradmandfard, M.; Kashani-Bozorg, S.F.; Lee, J.S.; Kim, C.-L.; Hanzaki, A.Z.; Pyun, Y.-S.; Cho, S.-W.; Amanov, A.; Kim, D.-E. Significant improvement in cell adhesion and wear resistance of biomedical β-type titanium alloy through ultrasonic nanocrystal surface modification. J. Alloys Compd. 2018, 762, 941–949. [Google Scholar] [CrossRef]
- Zhang, Y.; Chu, K.; He, S.; Wang, B.; Zhu, W.; Ren, F. Fabrication of high strength, antibacterial and biocompatible Ti-5Mo-5Ag alloy for medical and surgical implant applications. Mater. Sci. Eng. C Mater. Biol. Appl. 2020, 106, 110165. [Google Scholar] [CrossRef] [PubMed]
- Jawed, S.F.; Rabadia, C.D.; Liu, Y.J.; Wang, L.Q.; Li, Y.H.; Zhang, X.H.; Zhang, L.C. Mechanical characterization and deformation behavior of β-stabilized Ti-Nb-Sn-Cr alloys. J. Alloys Compd. 2019, 792, 684–693. [Google Scholar] [CrossRef]
- Dias Corpa Tardelli, J.; Bolfarini, C.; Candido Dos Reis, A. Comparative analysis of corrosion resistance between beta titanium and Ti-6Al-4V alloys: A systematic review. J. Trace Elem. Med. Biol. 2020, 62, 126618. [Google Scholar] [CrossRef] [PubMed]
- Moretti, B.; Pesce, V.; Maccagnano, G.; Vicenti, G.; Lovreglio, P.; Soleo, L.; Apostoli, P. Peripheral neuropathy after hip replacement failure: Is vanadium the culprit? Lancet 2012, 379, 1676. [Google Scholar] [CrossRef]
- Mirza, A.; King, A.; Troakes, C.; Exley, C. Aluminium in brain tissue in familial Alzheimer’s disease. J. Trace Elem. Med. Biol. 2017, 40, 30–36. [Google Scholar] [CrossRef] [Green Version]
- Bansal, P.; Singh, G.; Sidhu, H.S. Improvement of surface properties and corrosion resistance of Ti13Nb13Zr titanium alloy by plasma-sprayed HA/ZnO coatings for biomedical applications. Mater. Chem. Phys. 2021, 257, 123738. [Google Scholar] [CrossRef]
- Vlcak, P.; Fojt, J.; Koller, J.; Drahokoupil, J.; Smola, V. Surface pre-treatments of Ti-Nb-Zr-Ta beta titanium alloy: The effect of chemical, electrochemical and ion sputter etching on morphology, residual stress, corrosion stability and the MG-63 cell response. Results Phys. 2021, 28, 104613. [Google Scholar] [CrossRef]
- Abd-elrhman, Y.; Gepreel, M.A.H.; Abdel-Moniem, A.; Kobayashi, S. Compatibility assessment of new V-free low-cost Ti–4.7Mo–4.5Fe alloy for some biomedical applications. Mater. Des. 2016, 97, 445–453. [Google Scholar] [CrossRef]
- Assis, S.L.D.; Wolynec, S.; Costa, I. Corrosion characterization of titanium alloys by electrochemical techniques. Electrochim. Acta 2006, 51, 1815–1819. [Google Scholar] [CrossRef]
- Jin, L.; Cui, W.-F.; Song, X.; Liu, G.; Zhou, L. Effects of surface nanocrystallization on corrosion resistance of β-type titanium alloy. Trans. Nonferrous Met. Soc. China 2014, 24, 2529–2535. [Google Scholar] [CrossRef]
- Prakash, C.; Uddin, M.S. Surface modification of β-phase Ti implant by hydroaxyapatite mixed electric discharge machining to enhance the corrosion resistance and in-vitro bioactivity. Surf. Coat. Technol. 2017, 326, 134–145. [Google Scholar] [CrossRef]
- Chen, L.; Wei, K.; Qu, Y.; Li, T.; Chang, B.; Liao, B.; Xue, W. Characterization of plasma electrolytic oxidation film on biomedical high niobium-containing β-titanium alloy. Surf. Coat. Technol. 2018, 352, 295–301. [Google Scholar] [CrossRef]
- Wang, C.; Ma, F.; Liu, P.; Chen, J.; Liu, X.; Zhang, K.; Li, W.; Han, Q. The influence of alloy elements in Ti 6Al 4V and Ti 35Nb 2Ta 3Zr on the structure, morphology and properties of MAO coatings. Vacuum 2018, 157, 229–236. [Google Scholar] [CrossRef]
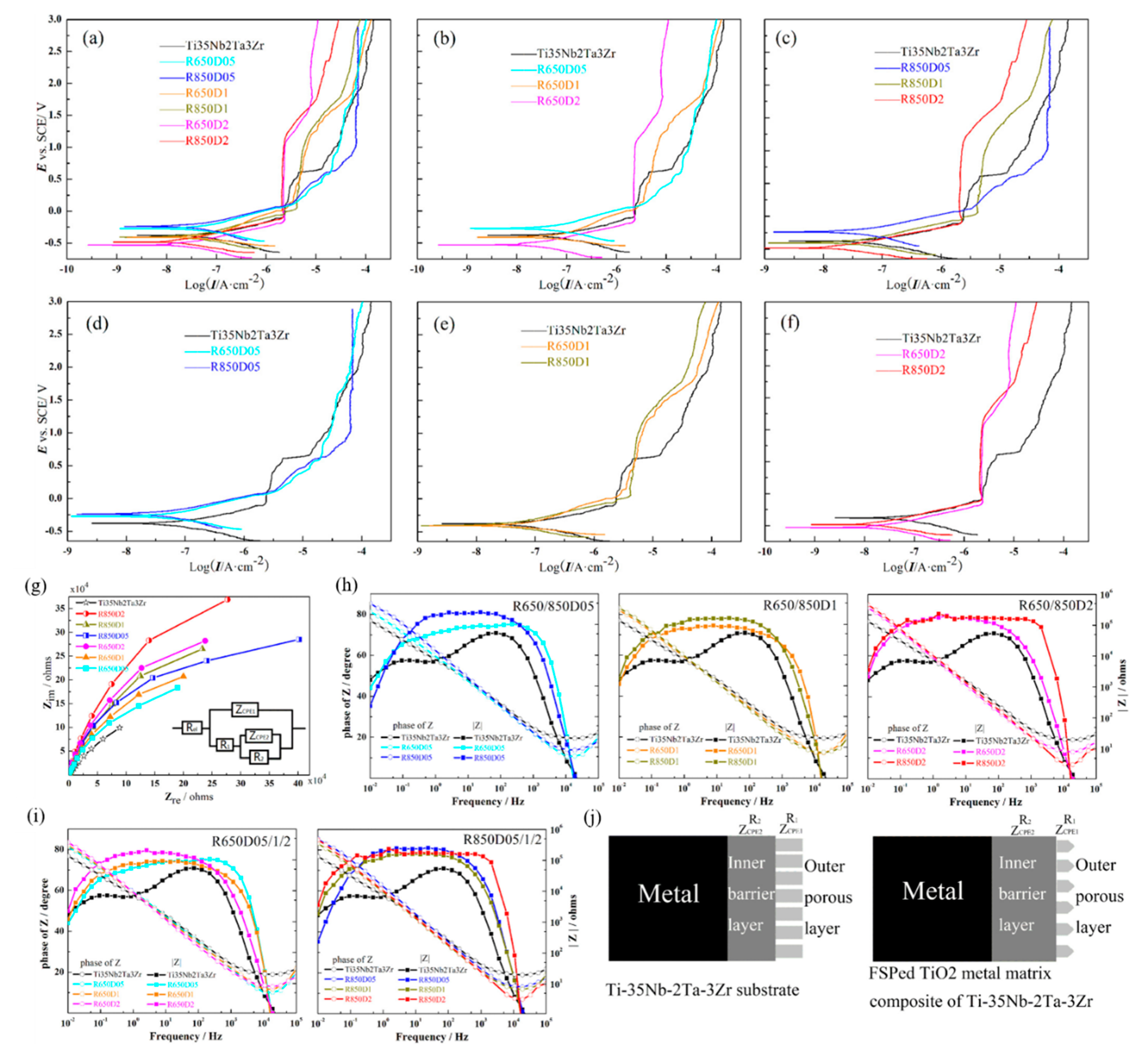
- Gu, H.; Ding, Z.; Yang, Z.; Yu, W.; Zhang, W.; Lu, W.; Zhang, L.-C.; Wang, K.; Wang, L.; Fu, Y.-f. Microstructure evolution and electrochemical properties of TiO2/Ti-35Nb-2Ta-3Zr micro/nano-composites fabricated by friction stir processing. Mater. Des. 2019, 169, 107680. [Google Scholar] [CrossRef]
- Liu, C.-F.; Li, S.-J.; Hou, W.-T.; Hao, Y.-L.; Huang, H.-H. Enhancing corrosion resistance and biocompatibility of interconnected porous β-type Ti-24Nb-4Zr-8Sn alloy scaffold through alkaline treatment and type I collagen immobilization. Appl. Surf. Sci. 2019, 476, 325–334. [Google Scholar] [CrossRef]
- Pina, V.G.; Dalmau, A.; Devesa, F.; Amigo, V.; Munoz, A.I. Tribocorrosion behavior of beta titanium biomedical alloys in phosphate buffer saline solution. J. Mech. Behav. Biomed. Mater. 2015, 46, 59–68. [Google Scholar] [CrossRef]
- Bahl, S.; Das, S.; Suwas, S.; Chatterjee, K. Engineering the next-generation tin containing beta titanium alloys with high strength and low modulus for orthopedic applications. J. Mech. Behav. Biomed. Mater. 2018, 78, 124–133. [Google Scholar] [CrossRef] [Green Version]
- Diomidis, N.; Mischler, S.; More, N.S.; Roy, M.; Paul, S.N. Fretting-corrosion behavior of β titanium alloys in simulated synovial fluid. Wear 2011, 271, 1093–1102. [Google Scholar] [CrossRef]
- Yuan, Z.; He, Y.; Lin, C.; Liu, P.; Cai, K. Antibacterial surface design of biomedical titanium materials for orthopedic applications. J. Mater. Sci. Technol. 2021, 78, 51–67. [Google Scholar] [CrossRef]
- Cai, D.; Zhao, X.; Yang, L.; Wang, R.; Qin, G.; Chen, D.-F.; Zhang, E. A novel biomedical titanium alloy with high antibacterial property and low elastic modulus. J. Mater. Sci. Technol. 2021, 81, 13–25. [Google Scholar] [CrossRef]
- Chang, X.; Smith, G.C.; Quinn, J.; Carson, L.; Chan, C.W.; Lee, S. Optimization of anti-wear and anti-bacterial properties of beta TiNb alloy via controlling duty cycle in open-air laser nitriding. J. Mech. Behav. Biomed. Mater. 2020, 110, 103913. [Google Scholar] [CrossRef]
- Lubov Donaghy, C.; McFadden, R.; Kelaini, S.; Carson, L.; Margariti, A.; Chan, C.-W. Creating an antibacterial surface on beta TNZT alloys for hip implant applications by laser nitriding. Opt. Laser Technol. 2020, 121, 105793. [Google Scholar] [CrossRef]
- Shi, A.; Cai, D.; Hu, J.; Zhao, X.; Qin, G.; Han, Y.; Zhang, E. Development of a low elastic modulus and antibacterial Ti-13Nb-13Zr-5Cu titanium alloy by microstructure controlling. Mater. Sci. Eng. C Mater. Biol. Appl. 2021, 126, 112116. [Google Scholar] [CrossRef]
- Liu, H.; Liu, R.; Ullah, I.; Zhang, S.; Sun, Z.; Ren, L.; Yang, K. Rough surface of copper-bearing titanium alloy with multifunctions of osteogenic ability and antibacterial activity. J. Mater. Sci. Technol. 2020, 48, 130–139. [Google Scholar] [CrossRef]
- Kaur, M.; Singh, K. Review on titanium and titanium based alloys as biomaterials for orthopaedic applications. Mater. Sci. Eng. C Mater. Biol. Appl. 2019, 102, 844–862. [Google Scholar] [CrossRef]
- Sidhu, S.S.; Singh, H.; Gepreel, M.A.H. A review on alloy design, biological response, and strengthening of β-titanium alloys as biomaterials. Mater. Sci. Eng. C Biomim. Mater. Sens. Syst. 2021, 121, 111661. [Google Scholar] [CrossRef]
- Zhao, D.; Liang, H.; Han, C.; Li, J.; Liu, J.; Zhou, K.; Yang, C.; Wei, Q. 3D printing of a titanium-tantalum Gyroid scaffold with superb elastic admissible strain, bioactivity and in-situ bone regeneration capability. Addit. Manuf. 2021, 47, 102223. [Google Scholar] [CrossRef]
- Liang, H.; Zhao, D.; Feng, X.; Ma, L.; Deng, X.; Han, C.; Wei, Q.; Yang, C. 3D-printed porous titanium scaffolds incorporating niobium for high bone regeneration capacity. Mater. Des. 2020, 194, 108890. [Google Scholar] [CrossRef]
- Jirka, I.; Vandrovcova, M.; Frank, O.; Tolde, Z.; Plsek, J.; Luxbacher, T.; Bacakova, L.; Stary, V. On the role of Nb-related sites of an oxidized beta-TiNb alloy surface in its interaction with osteoblast-like MG-63 cells. Mater. Sci. Eng. C Mater. Biol. Appl. 2013, 33, 1636–1645. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Chen, T.; Hu, J.; Li, S.; Zou, Q.; Li, Y.; Jiang, N.; Li, H.; Li, J. Modified surface morphology of a novel Ti-24Nb-4Zr-7.9Sn titanium alloy via anodic oxidation for enhanced interfacial biocompatibility and osseointegration. Colloids Surf. B Biointerfaces 2016, 144, 265–275. [Google Scholar] [CrossRef]
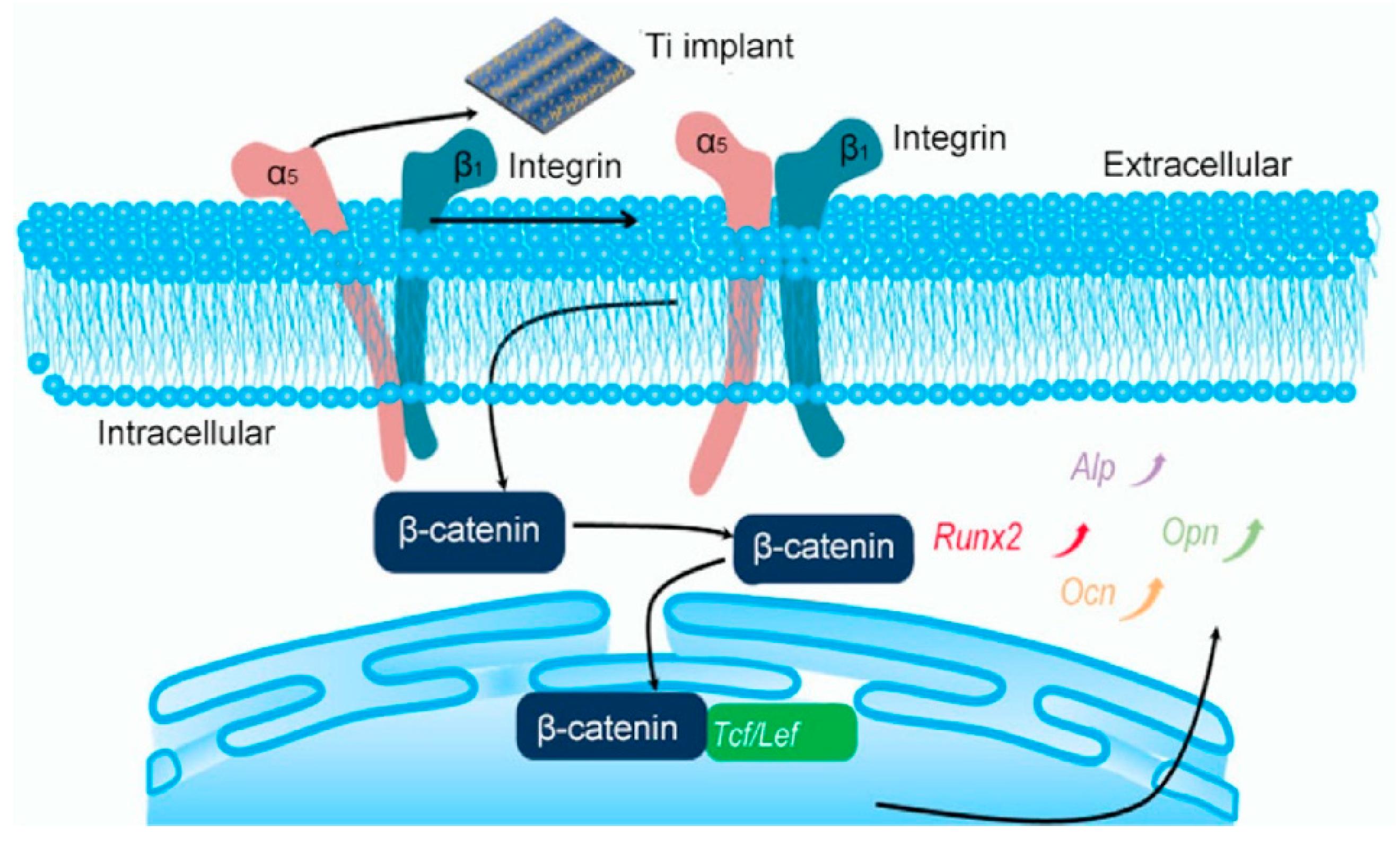
- Fu, J.; Liu, X.; Tan, L.; Cui, Z.; Liang, Y.; Li, Z.; Zhu, S.; Zheng, Y.; Kwok Yeung, K.W.; Chu, P.K.; et al. Modulation of the mechanosensing of mesenchymal stem cells by laser-induced patterning for the acceleration of tissue reconstruction through the Wnt/beta-catenin signaling pathway activation. Acta Biomater. 2020, 101, 152–167. [Google Scholar] [CrossRef] [PubMed]
| Materials | Type | Advantages | Disadvantages | Applications | Clinical Surgery | Ref. |
|---|---|---|---|---|---|---|
| CP Ti | α | Good biocompatibility | Low strength and poor wear resistance | Dental implants | √ | [7] |
| Ti–3Al–2.5V | α + β | Good strength and corrosion resistance | Toxicity elements (Al, V) | Dental implants | √ | [8] |
| Ti-6Al-4V (TC4) | α + β | Excellent strength and corrosion resistance | High elastic modulus, toxicity elements (Al, V), and poor wear resistance | Bone fixation plates and stem of artificial hip joints | √ | [1] |
| Ti–6Al–7Nb | α + β | Good wear resistance | Toxicity element (Al) | Dental prostheses knee, wrist, and femoral stems, fasteners, fixation plates, and screws | √ | [9] |
| Ti–5Al–2.5Fe | α + β | Good wear resistance | Toxicity element (Al) | Hip prostheses | √ | [1] |
| Ti-2.5Al-2.5Mo-2.5Zr (TAMZ) | α + β | High compatibility, toughness, fatigue resistance | Toxicity element (Al) | Hip stems, endosseous, subperiosteal, or transosteal implants in dentistry | √ | [10] |
| Ti-12Mo-6Zr-2Fe (TMZF) | β | Low elastic modulus, high fracture toughness, good wear resistance, and corrosion resistance | Head-neck taper fretting and corrosion, flexural rigidity | Femoral neck shaft, acetabular implant, and femoral stems | √ | [11] |
| Ti-13Nb-13Zr | near β | Low elastic modulus, low density, paramagnetic properties, low thermal conductivity | Low hardness and resistance | Head and acetabulum of hip endoprostheses | √ | [12] |
| Ti-24Nb-4Zr-8Sn (Ti2448) | β | High biocompatibility and mechanical properties | Low wear resistance | Artificial hip joints and dental roots | √ | [13,14] |
| Ti-15Mo | β | More biocompatible, lower modulus, better processability | Lower strength | Femoral hip implant components | √ | [15] |
| Ti-28Nb-24.5Zr | β | Low elastic modulus, high strength and toughness, excellent mechanical properties and biocompatibility | Poor wear property | Surgical and orthopedic implants | √ | [16] |
| Material | Preparation Process | Coefficient of Friction | Wear Loss | Mechanism | Ref. | ||
|---|---|---|---|---|---|---|---|
| Before | After | Before | After | ||||
| Ti-24Nb-38Zr-2Mo | cold crucible levitation melting + cold rolling + solution treatment | 1.25 | 1.10 | 1.3 mg | 0.9 mg | plowing and some indication of abrasive wear | [78] |
| Ti-24Nb-38Zr-2Mo-0.1Sc | cold crucible levitation melting + cold rolling + solution treatment | 1.20 | 0.90 | 1.0 mg | 0.5 mg | plowing and some indication of abrasive wear | [78,79] |
| Ti-35Nb-2Ta-3Zr | hybrid surface modification | 0.6 | 0.15 | / | / | abrasive wear + adhesive wear | [31] |
| Ti-13Zr-13Nb-0.5B | melting + heat treatment + hot rolling + solid solution + water quenching | 0.42 | 0.4 | / | / | microcutting; abrasive wear | [73] |
| Ti-29Nb-13Ta-4.6Zr | Picosecond + laser processing | / | / | 0.00102 mm3 | 0.00014 mm3 | wear debris containment effect and loading pressure | [79,80] |
| Ti-25Nb-3Zr-2Sn-3Mo | vacuum induction nitriding | 0.65 | 0.25 | 0.2 mm3 | 0.0007 mm3 | abrasive wear (rod-shaped TiN0.3 phase and soft β matrix) | [80] |
| Ti-5Al-5Mo-5V-3Cr-0.5Fe | vacuum arc melting + forging + stress relaxation | 0.57 | 0.45 | 0.073 mm3 | 0.034 mm3 | small amount of adhesive wear and slight abrasion wear | [81] |
| Ti-29Nb-13Ta-4.6Zr | solution-treated + water quenching + UNSM | / | / | 0.00102 mm3 | 0.00014 mm3 | increased surface hardness + nanoscale lamellar grains + α precipitates | [82] |
| Ti-30Nb-4Sn | laser nitriding | 0.70 | 0.18 | / | / | three-body abrasive wear | [83] |
| Ti-10V-2Fe-3Al | hot-rolled + heat treatment | 0.6 | 0.6 | / | / | oxidation + superelasticity | [74] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Shao, L.; Du, Y.; Dai, K.; Wu, H.; Wang, Q.; Liu, J.; Tang, Y.; Wang, L. β-Ti Alloys for Orthopedic and Dental Applications: A Review of Progress on Improvement of Properties through Surface Modification. Coatings 2021, 11, 1446. https://doi.org/10.3390/coatings11121446
Shao L, Du Y, Dai K, Wu H, Wang Q, Liu J, Tang Y, Wang L. β-Ti Alloys for Orthopedic and Dental Applications: A Review of Progress on Improvement of Properties through Surface Modification. Coatings. 2021; 11(12):1446. https://doi.org/10.3390/coatings11121446
Chicago/Turabian StyleShao, Longfei, Yiheng Du, Kun Dai, Hong Wu, Qingge Wang, Jia Liu, Yujin Tang, and Liqiang Wang. 2021. "β-Ti Alloys for Orthopedic and Dental Applications: A Review of Progress on Improvement of Properties through Surface Modification" Coatings 11, no. 12: 1446. https://doi.org/10.3390/coatings11121446
APA StyleShao, L., Du, Y., Dai, K., Wu, H., Wang, Q., Liu, J., Tang, Y., & Wang, L. (2021). β-Ti Alloys for Orthopedic and Dental Applications: A Review of Progress on Improvement of Properties through Surface Modification. Coatings, 11(12), 1446. https://doi.org/10.3390/coatings11121446








