Rescue Blankets-Transmission and Reflectivity of Electromagnetic Radiation
Abstract
1. Introduction
2. Factors Influencing Electromagnetic Measurements with Rescue Sheets
2.1. Ultraviolet (UV) Radiation
2.2. Infrared (IR) Radiation
2.3. Thermal Imaging
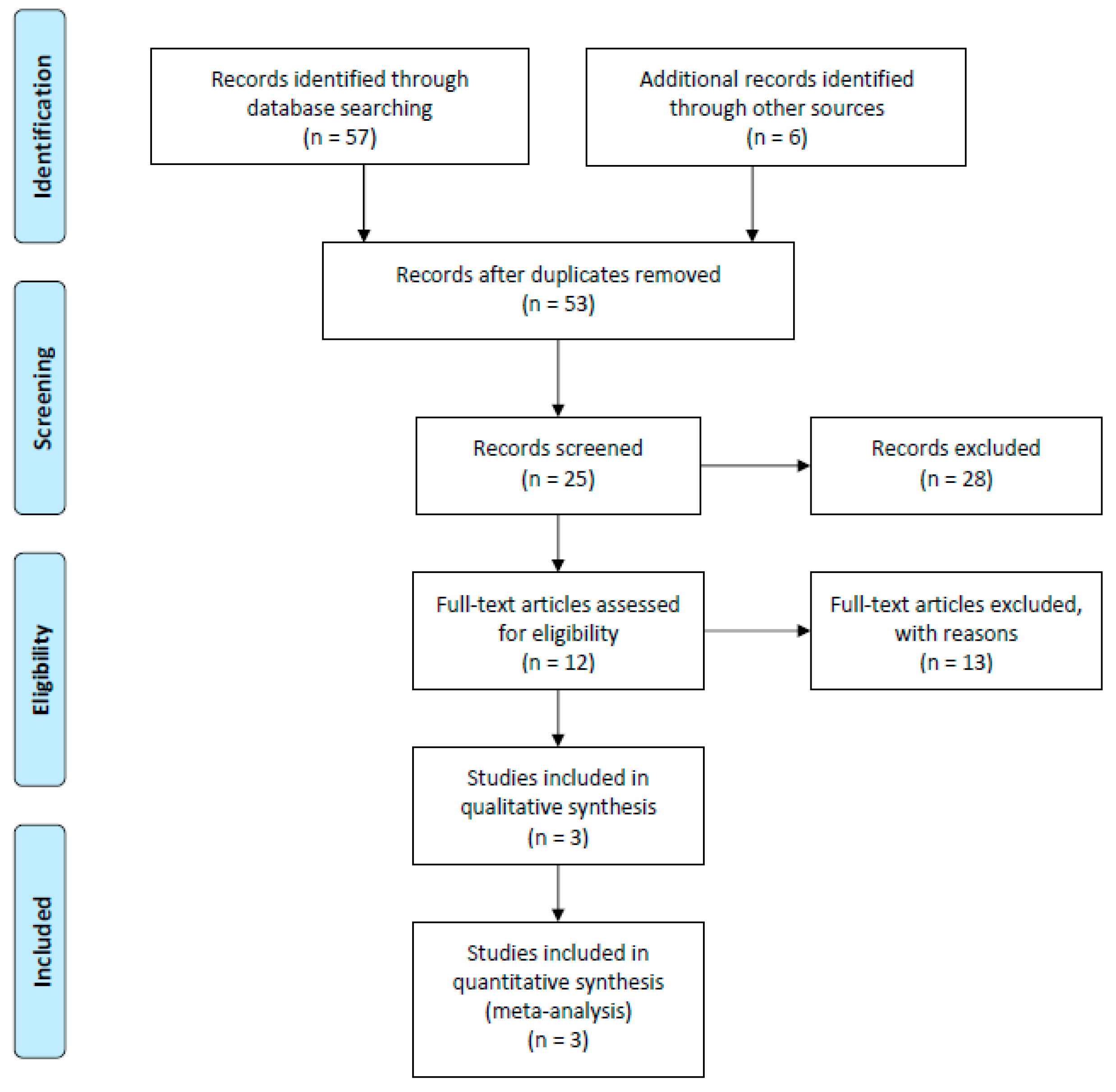
3. Materials and Methods
3.1. Measurement of Heat Loss by Rescue Blankets According to Surface Color
3.2. Optometric Measurement of Transparency with UV Radiation, HEV Light and Visible Light
3.3. Thermographic Measurement of IR Radiation from Rescue Blankets
4. Results and Discussion
4.1. Measurement of Heat Loss by Rescue Blankets According to Surface Color
4.2. Optometric Measurement of Transparency with UV Radiation, HEV Light and Visible Light
4.3. Thermographic Measurement of IR Radiation from Rescue Blankets
5. Implications
6. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Mommsen, P.; Andruszkow, H.; Frömke, C.; Zeckey, C.; Wagner, U.; van Griensven, M.; Frink, M.; Krettek, C.; Hildebrand, F. Effects of accidental hypothermia on posttraumatic complications and outcome in multiple trauma patients. Injury 2013, 44, 86–90. [Google Scholar] [CrossRef]
- Gerecht, R. The lethal triad. Hypothermia, acidosis & coagulopathy create a deadly cycle for trauma patients. JEMS 2014, 39, 56–60. [Google Scholar] [PubMed]
- Brugger, H.; Putzer, G.; Paal, P. Accidental hypothermia. Anaesthesist 2013, 62, 624–631. [Google Scholar] [CrossRef] [PubMed]
- Zasa, M.; Flowers, N.; Zideman, D.; Hodgetts, T.J.; Harris, T. A torso model comparison of temperature preservation devices for use in the prehospital environment. Emerg. Med. J. 2016, 33, 418–422. [Google Scholar] [CrossRef] [PubMed]
- Leung, E.M.; Colorado Escobar, M.; Stiubianu, G.T.; Jim, S.R.; Vyatskikh, A.L.; Feng, Z.; Garner, N.; Patel, P.; Naughton, K.L.; Follador, M.; et al. A dynamic thermoregulatory material inspired by squid skin. Nat. Commun. 2019, 10, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Allen, P.B.; Salyer, S.W.; Dubick, M.A.; Holcomb, J.B.; Blackbourne, L.H. Preventing hypothermia: Comparison of current devices used by the US Army in an in vitro warmed fluid model. J. Trauma 2010, 69, 154–161. [Google Scholar] [CrossRef]
- Tikuisis, P.; Giesbrecht, G.G. Prediction of shivering heat production from core and mean skin temperatures. Eur. J. Appl. Physiol. Occup. Physiol. 1999, 79, 221–229. [Google Scholar] [CrossRef] [PubMed]
- Haverkamp, F.J.C.; Giesbrecht, G.G.; Tan, E.C.T.H. The prehospital management of hypothermia—An up-to-date overview. Injury 2018, 49, 149–164. [Google Scholar] [CrossRef]
- Henriksson, O.; Lundgren, P.J.; Kuklane, K.; Holmér, I.; Giesbrecht, G.G.; Naredi, P.; Bjornstig, U. Protection against cold in prehospital care: Wet clothing removal or addition of a vapor barrier. Wilderness Environ. Med. 2015, 26, 11–20. [Google Scholar] [CrossRef]
- Chadwick, S.; Gibson, A. Hypothermia and the use of space blankets: A literature review. Accid. Emerg. Nurs. 1997, 5, 122–125. [Google Scholar] [CrossRef]
- Henriksson, O.; Lundgren, J.P.; Kuklane, K.; Holmér, I.; Bjornstig, U. Protection against cold in prehospital care-thermal insulation properties of blankets and rescue bags in different wind conditions. Prehosp. Disaster Med. 2009, 24, 408–415. [Google Scholar] [CrossRef] [PubMed]
- Isser, M.; Kranebitter, H.; Kühn, E.; Lederer, W. High-energy visible light transparency and ultraviolet ray transmission of metallized rescue sheets. Sci. Rep. 2019, 9, 1–6. [Google Scholar] [CrossRef]
- International Commission on Non-Ionizing Radiation Protection. ICNIRP statement—Protection of workers against ultraviolet radiation. Health Phys. 2010, 99, 66–87. [Google Scholar] [CrossRef] [PubMed]
- Izadi, M.; Jonaidi-Jafari, N.; Pourazizi, M.; Alemzadeh-Ansari, M.H.; Hoseinpourfard, M.J. Photokeratitis induced by ultraviolet radiation in travelers: A major health problem. J. Postgrad. Med. 2018, 64, 40–46. [Google Scholar] [PubMed]
- Sliney, D.H. How light reaches the eye and its components. Int. J. Toxicol. 2002, 21, 501–509. [Google Scholar] [CrossRef] [PubMed]
- Viennot, L.; Décamp, N. Which Side to Put the Survival Blanket? Analysis and Suggestions for Activities with Students. Published by the MUSE Group (More Understanding with Simple Experiments) in the Physics Education Division (PED) of the European Physical Society (EPS). Available online: https://cdn.ymaws.com/www.eps.org/resource/collection/016775D4-8888-474D-887F-3E33AEA5E6D0/EPSPED_SurvivalBlanket.pdf (accessed on 30 March 2020).
- Besson, U. Paradoxes of thermal radiation. Eur. J. Phys. 2009, 30, 995–1007. [Google Scholar] [CrossRef]
- Boyer, T.H. Thermodynamics of the harmonic oscillator: Wien’s displacement law and the Planck spectrum. Am. J. Phys. 2003, 71, 866–870. [Google Scholar] [CrossRef]
- Sonnier, R.; Ferry, L.; Gallard, B.; Boudenne, A.; Lavaud, F. Controlled Emissivity Coatings to Delay Ignition of Polyethylene. Materials 2015, 8, 6935–6949. [Google Scholar] [CrossRef]
- FLIR. Drone Education Lab for Thermal Applications. Available online: https://www.flir.com/suas/delta/ (accessed on 12 February 2020).
- Zenmuse, X.T. TECHN. DATEN User Manual. Available online: http://www.dji.com/product/zenmuse-xt (accessed on 12 February 2020).
- Council Directive 93/42/EEC. Medical Devices. Available online: https://cemarking.net/medical-devices-directive/ (accessed on 10 January 2019).
- Isser, M.; Kranebitter, H.; Fink, H.; Wiedermann, F.J.; Lederer, W. High tensile strength increases multifunctional use of survival blankets in wilderness emergencies. Wilderness Environ. Med. 2020, in press. [Google Scholar]
- Isser, M.; Kranebitter, H.; Kofler, A.; Groemer, G.; Wiedermann, F.J.; Lederer, W. Rescue blankets hamper thermal imaging by infrared cameras. Appl. Compos. Mater. 2020, in press. [Google Scholar]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; PRISMA Group. Reprint-preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. Phys. Ther. 2009, 89, 873–880. [Google Scholar] [CrossRef] [PubMed]
- Renström, B. Space or rescue blanket—A bluff? Arct. Med. Res. 1992, 51, 212–213. [Google Scholar]

© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kranebitter, H.; Wallner, B.; Klinger, A.; Isser, M.; Wiedermann, F.J.; Lederer, W. Rescue Blankets-Transmission and Reflectivity of Electromagnetic Radiation. Coatings 2020, 10, 375. https://doi.org/10.3390/coatings10040375
Kranebitter H, Wallner B, Klinger A, Isser M, Wiedermann FJ, Lederer W. Rescue Blankets-Transmission and Reflectivity of Electromagnetic Radiation. Coatings. 2020; 10(4):375. https://doi.org/10.3390/coatings10040375
Chicago/Turabian StyleKranebitter, Hannah, Bernd Wallner, Andreas Klinger, Markus Isser, Franz J. Wiedermann, and Wolfgang Lederer. 2020. "Rescue Blankets-Transmission and Reflectivity of Electromagnetic Radiation" Coatings 10, no. 4: 375. https://doi.org/10.3390/coatings10040375
APA StyleKranebitter, H., Wallner, B., Klinger, A., Isser, M., Wiedermann, F. J., & Lederer, W. (2020). Rescue Blankets-Transmission and Reflectivity of Electromagnetic Radiation. Coatings, 10(4), 375. https://doi.org/10.3390/coatings10040375




