Phosphatidylethanol for Monitoring Alcohol Use in Liver Transplant Candidates: An Observational Study
Abstract
1. Introduction
2. Methods
2.1. Study Design
2.2. Study Population and Procedure
2.3. Biomarker Assessment
2.4. Statistical Analysis
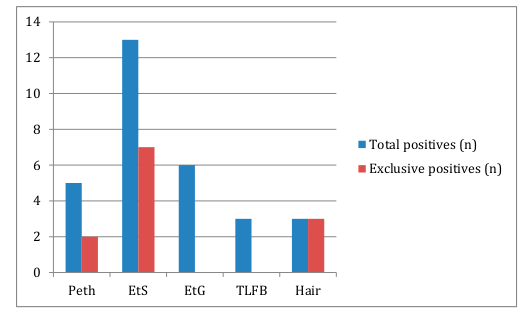
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Burra, P.; Senzolo, M.; Adam, R.; Delvart, V.; Karam, V.; Germani, G.; Neuberger, J.; ELITA; ELTR Liver Transplant Centers. Liver Transplantation for Alcoholic Liver Disease in Europe: A Study from the ELTR (European Liver Transplant Registry). Am. J. Transpl. 2010, 10, 138–148. [Google Scholar] [CrossRef] [PubMed]
- Burroughs, A.-K.; Sabin, C.; Rolles, K.; Delvart, V.; Karam, V.; Buckels, J.; O’Grady, J.G.; Castaing, D.; Klempnauer, J.; Jamieson, N.V.; et al. 3-month and 12-month mortality after first liver transplant in adults in Europe: Predictive models for outcome. Lancet 2006, 367, 225–232. [Google Scholar] [CrossRef]
- Marroni, N.P.; Fleck, A.M., Jr.; Fernandes, S.A.; Galant, L.H.; Mucenic, M.; Meine, M.H.D.M.; Mariante-Neto, G.; Brandão, A.B.D.M. Liver transplantation and alcoholic liver disease: History, controversies, and considerations. World J. Gastroenterol. 2018, 24, 2785–2805. [Google Scholar] [CrossRef] [PubMed]
- Kotlyar, D.S.; Burke, A.; Campbell, M.S.; Weinrieb, R.M. A Critical Review of Candidacy for Orthotopic Liver Transplantation in Alcoholic Liver Disease. Am. J. Gastroenterol. 2008, 103, 734–743. [Google Scholar] [CrossRef] [PubMed]
- Testino, G.; Leone, S. Acute alcoholic hepatitis: A literature review and proposal of treatment. Minerva Med. 2017, 109, 290–299. [Google Scholar]
- Frazier, T.H.; Stocker, A.M.; Kershner, N.A.; Marsano, L.S.; McClain, C.J. Treatment of alcoholic liver disease. Adv. Gastroenterol. 2010, 4, 63–81. [Google Scholar] [CrossRef]
- Jaurigue, M.M.; Cappell, M.S. Therapy for alcoholic liver disease. World J. Gastroenterol. 2014, 20, 2143–2158. [Google Scholar] [CrossRef]
- Marroni, N.P. Management of alcohol recurrence before and after liver transplantation. Clin. Res. Hepatol. Gastroenterol. 2015, 39, S109–S114. [Google Scholar] [CrossRef]
- Dew, M.A.; DiMartini, A.F.; Steel, J.; Dabbs, A.D.V.; Myaskovsky, L.; Unruh, M.; Greenhouse, J. Meta-analysis of risk for relapse to substance use after transplantation of the liver or other solid organs. Liver Transpl. 2008, 14, 159–172. [Google Scholar] [CrossRef]
- Testino, G. Alcohol and liver transplantation: The six-month abstinence rule is not a dogma. Transpl. Int. 2016, 29, 953–954. [Google Scholar] [CrossRef]
- Testino, G.; Burra, P.; Bonino, F.; Piani, F.; Sumberaz, A.; Peressutti, R.; Castiglione, A.G.; Patussi, V.; Fanucchi, T.; Ancarani, O.; et al. Acute alcoholic hepatitis, end stage alcoholic liver disease and liver transplantation: An Italian position statement. World J. Gastroenterol. 2014, 20, 14642–14651. [Google Scholar] [CrossRef]
- Saunders, J.B.; Whitfield, J.B.; Conigrave, K. Diagnostic tests for alcohol consumption. Alcohol Alcohol. 1995, 30, 13–26. [Google Scholar]
- Hock, B.; Schwarz, M.; Domke, I.; Grunert, V.P.; Wuertemberger, M.; Schiemann, U.; Horster, S.; Limmer, C.; Stecker, G.; Soyka, M. Validity of carbohydrate-deficient transferrin (%CDT), γ-glutamyltransferase (γ-GT) and mean corpuscular erythrocyte volume (MCV) as biomarkers for chronic alcohol abuse: A study in patients with alcohol dependence and liver disorders of non-alcoholic and alcoholic origin. Addiction 2005, 100, 1477–1486. [Google Scholar] [PubMed]
- Conigrave, K.M.; Degenhardt, L.J.; Whitfield, J.B.; Saunders, J.B.; Helander, A.; Tabakoff, B.; WHO/ISBRA Study Group. CDT, GGT, and AST as markers of alcohol use: The WHO/ISBRA collaborative project. Alcohol. Clin. Exp. Res. 2002, 26, 332–339. [Google Scholar] [CrossRef] [PubMed]
- Barrio, P.; Teixidor, L.; Rico, N.; Bruguera, P.; Ortega, L.; Bedini, J.L.; Gual, A. Urine Ethyl Glucuronide Unraveling the Reality of Abstinence Monitoring in a Routine Outpatient Setting: A Cross-Sectional Comparison with Ethanol, Self Report and Clinical Judgment. Eur. Addict. Res. 2016, 22, 243–248. [Google Scholar] [CrossRef] [PubMed]
- Staufer, K.; Andresen, H.; Vettorazzi, E.; Tobias, N.; Nashan, B.; Sterneck, M. Urinary ethyl glucuronide as a novel screening tool in patients pre- and post-liver transplantation improves detection of alcohol consumption. Hepatology 2011, 54, 1640–1649. [Google Scholar] [CrossRef] [PubMed]
- Stewart, S.H.; Koch, D.G.; Burgess, D.M.; Willner, I.R.; Reuben, A. Sensitivity and specificity of urinary ethyl glucuronide and ethyl sulfate in liver disease patients. Alcohol. Clin. Exp. Res. 2012, 37, 150–155. [Google Scholar] [CrossRef] [PubMed]
- Simons, J.S.; Wills, T.A.; Emery, N.N.; Marks, R.M. Quantifying alcohol consumption: Self-report, transdermal assessment, and prediction of dependence symptoms. Addict. Behav. 2015, 50, 205–212. [Google Scholar] [CrossRef]
- Wurst, F.M.; Thon, N.; Yegles, M.; Schrück, A.; Preuss, U.W.; Weinmann, W. Ethanol metabolites: Their role in the assessment of alcohol intake. Alcohol. Clin. Exp. Res. 2015, 39, 2060–2072. [Google Scholar] [CrossRef]
- Allen, J.P.; Wurst, F.M.; Thon, N.; Litten, R.Z. Assessing the drinking status of liver transplant patients with alcoholic liver disease. Liver Transpl. 2013, 19, 369–376. [Google Scholar] [CrossRef]
- Stewart, S.H.; Reuben, A.; Brzezinski, W.A.; Koch, D.G.; Basile, J.; Randall, P.K.; Miller, P.M. Preliminary Evaluation of Phosphatidylethanol and Alcohol Consumption in Patients with Liver Disease and Hypertension. Alcohol Alcohol. 2009, 44, 464–467. [Google Scholar] [CrossRef] [PubMed]
- Stewart, S.H.; Koch, D.G.; Willner, I.R.; Anton, R.F.; Reuben, A. Validation of Blood Phosphatidylethanol as an Alcohol Consumption Biomarker in Patients with Chronic Liver Disease. Alcohol. Clin. Exp. Res. 2014, 38, 1706–1711. [Google Scholar] [CrossRef] [PubMed]
- Andresen-Streichert, H.; Beres, Y.; Weinmann, W.; Schröck, A.; Müller, A.; Skopp, G.; Pischke, S.; Vettorazzi, E.; Lohse, A.; Nashan, B.; et al. Improved detection of alcohol consumption using the novel marker phosphatidylethanol in the transplant setting: Results of a prospective study. Transpl. Int. 2017, 30, 611–620. [Google Scholar] [CrossRef] [PubMed]
- Fleming, M.F.; Smith, M.J.; Oslakovic, E.; Lucey, M.R.; Vue, J.X.; Al-Saden, P.; Levitsky, J. Phosphatidylethanol Detects Moderate-to-Heavy Alcohol Use in Liver Transplant Recipients. Alcohol. Clin. Exp. Res. 2017, 41, 857–862. [Google Scholar] [CrossRef] [PubMed]
- Bohn, M.J.; Babor, T.F.; Kranzler, H.R. The Alcohol Use Disorders Identification Test (AUDIT): Validation of a screening instrument for use in medical settings. J. Stud. Alcohol 1995, 56, 423–432. [Google Scholar] [CrossRef] [PubMed]
- Sobell, L.C.; Sobell, M.B. Timeline Follow-Back. In Measuring Alcohol Consumption; Humana Press: Totowa, NJ, USA, 1992; pp. 41–72. [Google Scholar]
- Barrio, P.; Wurst, F.M.; Gual, A. New Alcohol Biomarkers. New challenges. Alcohol Alcohol. 2018, 53, 762–763. [Google Scholar] [CrossRef]
- Reisfield, G.M.; Teitelbaum, S.A.; Large, S.O.; Jones, J.; Morrison, D.G.; Lewis, B. The roles of phosphatidylethanol (PEth), ethyl glucuronide (EtG), and ethyl sulfate (EtS) in identifying alcohol consumption among participants in professionals’ health programs. Drug Test. Anal. 2020, 12, 1102–1108. [Google Scholar] [CrossRef]
- Musshoff, F.; Albermann, E.; Madea, B. Ethyl glucuronide and ethyl sulfate in urine after consumption of various beverages and foods—Misleading results? Int. J. Leg. Med. 2010, 124, 623–630. [Google Scholar] [CrossRef]
- Stachel, N.; Skopp, G. Formation and inhibition of ethyl glucuronide and ethyl sulfate. Forensic Sci. Int. 2016, 265, 61–64. [Google Scholar] [CrossRef]
- Lindenger, C.; Castedal, M.; Schult, A.; Åberg, F. Long-term survival and predictors of relapse and survival after liver transplantation for alcoholic liver disease. Scand. J. Gastroenterol. 2018, 53, 1553–1561. [Google Scholar] [CrossRef]
- Rice, J.P.; Eickhoff, J.; Agni, R.; Ghufran, A.; Brahmbhatt, R.; Lucey, M.R. Abusive drinking after liver transplantation is associated with allograft loss and advanced allograft fibrosis. Liver Transpl. 2013, 19, 1377–1386. [Google Scholar] [CrossRef] [PubMed]
- Zemore, S.E. The effect of social desirability on reported motivation, substance use severity, and treatment attendance. J. Subst. Abus. Treat. 2012, 42, 400–412. [Google Scholar] [CrossRef] [PubMed]
- Lopez Pelayo, H.; Altamirano, J.; Lopez, E.; Barrio, P.; Lopez, A.; Gual, A.; Lligoña, A. Role of Alcohol and Drug Detection by Regular Urine Sample Testing in pre-transplant evaluation for Alcohol Liver Disease. Adicciones 2018, 20, 1121. [Google Scholar] [CrossRef]
- Reisfield, G.M.; Goldberger, B.A.; Crews, B.O.; Pesce, A.J.; Wilson, G.R.; Teitelbaum, S.A.; Bertholf, R.L. Ethyl glucuronide, ethyl sulfate, and ethanol in urine after sustained exposure to an ethanol-based hand sanitizer. J. Anal. Toxicol. 2011, 35, 85–91. [Google Scholar] [CrossRef]
- Liu, Y.; Zhang, X.; Li, J.; Huang, Z.; Lin, Z.; Wang, J.; Zhang, C.; Rao, Y. Stability of Ethyl Glucuronide, Ethyl Sulfate, Phosphatidylethanols and Fatty Acid Ethyl Esters in Postmortem Human Blood. J. Anal. Toxicol. 2018, 42, 346–352. [Google Scholar] [CrossRef]
- Barrio, P.; Mondon, S.; Teixidor, L.; Ortega, L.; Vieta, E.; Gual, A. One Year Clinical Correlates of EtG Positive Urine Screening in Alcohol-Dependent Patients: A Survival Analysis. Alcohol Alcohol. 2017, 52, 460–465. [Google Scholar] [CrossRef]


| Variable | AUDIT negative (score <8) | AUDIT positive (score ≥8) |
|---|---|---|
| Sex (% men) | 83.3 | 87.5 |
| Age (years) | 56.8 | 53.6 |
| ASAT (mean (SD)) | 47.6 (20) UI/L | 34.6 (4) UI/L |
| ALAT (mean (SD)) | 34.9 (25) UI/L | 33 (28) UI/L |
| GGT (mean (SD)) | 89.9 (86) UI/L | 75.6 (11) UI/L |
| EtG positive (%) | 2.4% | 62.5% |
| EtS positive (%) | 19.5% | 62.5% |
| PeTH positive (%) | 7.1% | 25% |
| HEtG positive (%) | 3.4% | 66.7% |
| TLFB positive (%) | 0% | 37.5% |
| All biomarkers negative (%) | 76.2% | 37.5% |
| Other drugs used (%) | 11.9% | 25% |
| VHC (%) | 28.6% | 25% |
| Biomarker | Characteristics | References |
|---|---|---|
| EtG | Obtained from urine. Sensible to urine infections and reduced kidney function. Suitable for abstinence monitoring. Time-frame of detection up to a few days. Cut-off 0.5 mg/L | [15,16,17,19,20,27,28,29,30] |
| EtS | Obtained from urine. Sensible to urine infections and reduced kidney function. Suitable for abstinence monitoring. Time-frame of detection up to a few days. Cut-off 0.05 mg/L. | [17,19,20,31,32,33] |
| PeTH | Obtained from dried blood spots. Suitable for abstinence and heavy drinking monitoring. Timeframe of detection from days to weeks. Cut-off 20 ng/mL | [19,21,22,23,24] |
| HEtG | Obtained from hair. Sensible to contamination and extraction methods. Suitable for abstinence monitoring over long periods of time. Timeframe of detection from weeks to months. Cut-off 7 pg/mL. | [19] |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Barrio, P.; Gual, A.; Lligoña, A.; Teixidor, L.; Weinmann, W.; Yegles, M.; Wurst, F.M. Phosphatidylethanol for Monitoring Alcohol Use in Liver Transplant Candidates: An Observational Study. J. Clin. Med. 2020, 9, 3060. https://doi.org/10.3390/jcm9093060
Barrio P, Gual A, Lligoña A, Teixidor L, Weinmann W, Yegles M, Wurst FM. Phosphatidylethanol for Monitoring Alcohol Use in Liver Transplant Candidates: An Observational Study. Journal of Clinical Medicine. 2020; 9(9):3060. https://doi.org/10.3390/jcm9093060
Chicago/Turabian StyleBarrio, Pablo, Antoni Gual, Anna Lligoña, Lidia Teixidor, Wolfgang Weinmann, Michel Yegles, and Friedrich M. Wurst. 2020. "Phosphatidylethanol for Monitoring Alcohol Use in Liver Transplant Candidates: An Observational Study" Journal of Clinical Medicine 9, no. 9: 3060. https://doi.org/10.3390/jcm9093060
APA StyleBarrio, P., Gual, A., Lligoña, A., Teixidor, L., Weinmann, W., Yegles, M., & Wurst, F. M. (2020). Phosphatidylethanol for Monitoring Alcohol Use in Liver Transplant Candidates: An Observational Study. Journal of Clinical Medicine, 9(9), 3060. https://doi.org/10.3390/jcm9093060






