Functional Progression in Patients with Interstitial Lung Disease Resulted Positive to Antisynthetase Antibodies: A Multicenter, Retrospective Analysis
Abstract
1. Introduction
2. Methods
2.1. Study Design
2.2. Pulmonary Function Tests
2.3. Statistical Analysis
3. Results
3.1. Differences between Anti-Jo1-Positive and Negative Subgroups at Baseline
3.2. Differences between Anti-Jo1 Positive and Negative Subgroups During Follow-Up
4. Discussion
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Lundberg, I.E.; Tjärnlund, A.; Bottai, M.; Werth, V.P.; Pilkington, C.; Visser, M.; Alfredsson, L.; Amato, A.A.; Barohn, R.J.; Liang, M.H.; et al. 2017 European League Against Rheumatism/American College of Rheumatology classification criteria for adult and juvenile idiopathic inflammatory myopathies and their major subgroups. Ann. Rheum. Dis. 2017, 76, 1955–1964. [Google Scholar] [CrossRef] [PubMed]
- Cavagna, L.; Trallero-Araguás, E.; Meloni, F.; Cavazzana, I.; Rojas-Serrano, J.; Feist, E.; Zanframundo, G.; Morandi, V.; Meyer, A.; Da Silva, J.A.P.; et al. Influence of Antisynthetase Antibodies Specificities on Antisynthetase Syndrome Clinical Spectrum Time Course. J. Clin. Med. 2019, 8, 2013. [Google Scholar] [CrossRef] [PubMed]
- Ghirardello, A.; Doria, A. New insights in myositis-specific autoantibodies. Curr. Opin. Rheumatol. 2018, 30, 614–622. [Google Scholar] [CrossRef]
- La Corte, R.; Monaco, A.L.; Locaputo, A.; Dolzani, F.; Trotta, F. In patients with antisynthetase syndrome the occurrence of anti-Ro/SSA antibodies causes a more severe interstitial lung disease. Autoimmunity 2006, 39, 249–253. [Google Scholar] [CrossRef]
- Bauhammer, J.; Blank, N.; Max, R.; Lorenz, H.-M.; Wagner, U.; Krause, D.; Fiehn, C. Rituximab in the treatment of Jo1 antibody–associated antisynthetase syndrome: Anti-Ro52 positivity as a marker for severity and treatment response. J. Rheumatol. 2016, 43, 1566–1574. [Google Scholar] [CrossRef] [PubMed]
- Zamora, A.C.; Hoskote, S.S.; Abascal-Bolado, B.; White, D.; Cox, C.W.; Ryu, J.H.; Moua, T. Clinical features and outcomes of interstitial lung disease in anti-Jo-1 positive antisynthetase syndrome. Respir. Med. 2016, 118, 39–45. [Google Scholar] [CrossRef]
- Johnson, C.; Connors, G.R.; Oaks, J.; Han, S.; Truong, A.; Richardson, B.; Lechtzin, N.; Mammen, A.L.; Casciola-Rosen, L.; Christopher-Stine, L.; et al. Clinical and pathologic differences in interstitial lung disease based on antisynthetase antibody type. Respir. Med. 2014, 108, 1542–1548. [Google Scholar] [CrossRef]
- Andersson, H.; Aalokken, T.M.; Gunther, A.; Mynarek, G.K.; Garen, T.; Lund, M.B.; Molberg, O. Pulmonary involvement in the antisynthetase syndrome: A comparative cross-sectional study. J. Rheumatol. 2016, 43, 1107–1113. [Google Scholar] [CrossRef][Green Version]
- Trallero-Araguás, E.; Grau-Junyent, J.M.; Labirua-Iturburu, A.; García-Hernández, F.J.; Monteagudo-Jiménez, M.; Fraile-Rodriguez, G.; Les-Bujanda, I.; Rodriguez-Carballeira, M.; Sáez-Comet, L.; Selva-O’Callaghan, A. Clinical manifestations and long-term outcome of anti-Jo1 antisynthetase patients in a large cohort of Spanish patients from the GEAS-IIM group. Semin. Arthritis Rheum. 2016, 46, 225–231. [Google Scholar] [CrossRef]
- González-Pérez, M.I.; Mejía-Hurtado, J.G.; Pérez-Román, D.I.; Buendía-Roldán, I.; Mejía, M.; Falfán-Valencia, R.; Mateos-Toledo, H.N.; Rojas-Serrano, J. Evolution of pulmonary function in a cohort of patients with interstitial lung disease and positive for antisynthetase antibodies. J. Rheumatol. 2020, 47, 415–423. [Google Scholar] [CrossRef]
- Cavagna, L.; Nuño, L.; Scirè, C.A.; Govoni, M.; Longo, F.J.L.; Franceschini, F.; Neri, R.; Castañeda, S.; Giraldo, W.A.S.; Caporali, R.; et al. Clinical spectrum time course in anti jo-1 positive antisynthetase syndrome: Results from an international retrospective multicenter study. Medicine 2015, 94, e1144. [Google Scholar] [CrossRef] [PubMed]
- Pinal-Fernandez, I.; Casal-Dominguez, M.; Huapaya, J.A.; Albayda, J.; Paik, J.J.; Johnson, C.; Silhan, L.; Christopher-Stine, L.; Mammen, A.L.; Danoff, S.K. A longitudinal cohort study of the anti-synthetase syndrome: Increased severity of interstitial lung disease in black patients and patients with anti-PL7 and anti-PL12 autoantibodies. Rheumatology 2017, 56, 999–1007. [Google Scholar] [CrossRef]
- Aggarwal, R.; Cassidy, E.; Fertig, N.; Koontz, D.C.; Lucas, M.; Ascherman, D.P.; Oddis, C.V. Patients with non-Jo-1 anti-tRNA-synthetase autoantibodies have worse survival than Jo-1 positive patients. Ann. Rheum. Dis. 2014, 73, 227–232. [Google Scholar] [CrossRef] [PubMed]
- Liu, H.; Xie, S.; Liang, T.; Ma, L.; Sun, H.; Dai, H.; Wang, C. Prognostic factors of interstitial lung disease progression at sequential HRCT in anti-synthetase syndrome. Eur. Radiol. 2019, 29, 5349–5357. [Google Scholar] [CrossRef] [PubMed]
- González-Gay, M.A.; Montecucco, C.; Selva-O’Callaghan, A.; Trallero-Araguas, E.; Molberg, O.; Andersson, H.; Rojas-Serrano, J.; Perez-Roman, D.I.; Bauhammer, J.; Fiehn, C.; et al. Timing of onset affects arthritis presentation pattern in antisynthetase syndrome. Clin. Exp. Rheumatol. 2018, 36, 44–49. [Google Scholar]
- Goh, N.S.; Hoyles, R.K.; Denton, C.P.; Hansell, D.M.; Renzoni, E.A.; Maher, T.M.; Nicholson, A.G.; Wells, A.U. Short-term pulmonary function trends are predictive of mortality in interstitial lung disease associated with systemic sclerosis. Arthritis Rheumatol. 2017, 69, 1670–1678. [Google Scholar] [CrossRef]
- Collard, H.R.; Moore, B.B.; Flaherty, K.R.; Brown, K.K.; Kaner, R.J.; King, T.E., Jr.; Lasky, J.A.; Loyd, J.E.; Noth, I.; Olman, M.A.; et al. Acute exacerbations of idiopathic pulmonary fibrosis. Am. J. Respir. Crit. Care Med. 2007, 176, 636–643. [Google Scholar] [CrossRef]
- Miller, M.R. General considerations for lung function testing. Eur. Respir. J. 2005, 26, 153–161. [Google Scholar] [CrossRef]
- Graham, B.L.; Brusasco, V.; Burgos, F.; Cooper, B.G.; Jensen, R.; Kendrick, A.; MacIntyre, N.R.; Thompson, B.R.; Wanger, J. 2017 ERS/ATS standards for single-breath carbon monoxide uptake in the lung. Eur. Respir. J. 2017, 49, 1600016. [Google Scholar] [CrossRef]
- American Thoracic Society. Guidelines for the six-minute walk test. Am. J. Respir. Crit. Care Med. 2002, 166, 111–117. [Google Scholar] [CrossRef]
- Barba, T.; Fort, R.; Cottin, V.; Provencher, S.; Durieu, I.; Jardel, S.; Hot, A.; Reynaud, Q.; Lega, J.-C. Treatment of idiopathic inflammatory myositis associated interstitial lung disease: A systematic review and meta-analysis. Autoimmun. Rev. 2019, 18, 113–122. [Google Scholar] [CrossRef] [PubMed]
- Marie, I.; Josse, S.; Decaux, O.; Dominique, S.; Diot, E.; Landron, C.; Roblot, P.; Jouneau, S.; Hatron, P.Y.; Tiev, K.P.; et al. Comparison of long-term outcome between anti-Jo1- and anti-PL7/PL12 positive patients with antisynthetase syndrome. Autoimmun. Rev. 2012, 11, 739–745. [Google Scholar] [CrossRef] [PubMed]
- Hervier, B.; Devilliers, H.; Stanciu, R.; Meyer, A.; Uzunhan, Y.; Masseau, A.; Dubucquoi, S.; Hatron, P.-Y.; Musset, L.; Wallaert, B.; et al. Hierarchical cluster and survival analyses of antisynthetase syndrome: Phenotype and outcome are correlated with anti-tRNA synthetase antibody specificity. Autoimmun. Rev. 2012, 12, 210–217. [Google Scholar] [CrossRef] [PubMed]
- Tomonaga, M.; Sakamoto, N.; Ishimatsu, Y.; Kakugawa, T.; Harada, T.; Nakashima, S.; Hara, A.; Hara, S.; Horai, Y.; Kawakami, A.; et al. Comparison of pulmonary involvement between patients expressing anti-PL-7 and anti-Jo-1 antibodies. Lung 2015, 193, 79–83. [Google Scholar] [CrossRef] [PubMed]
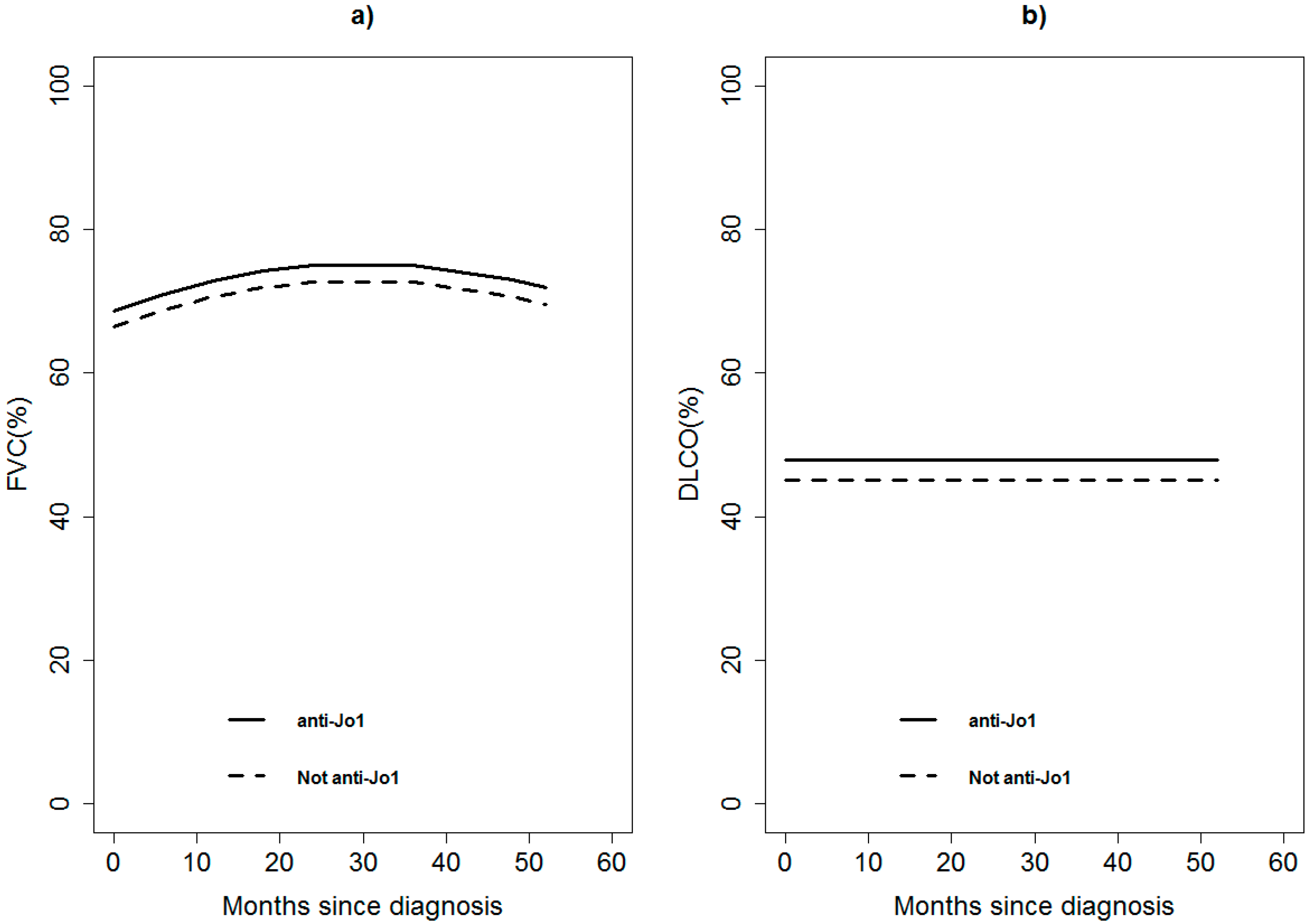
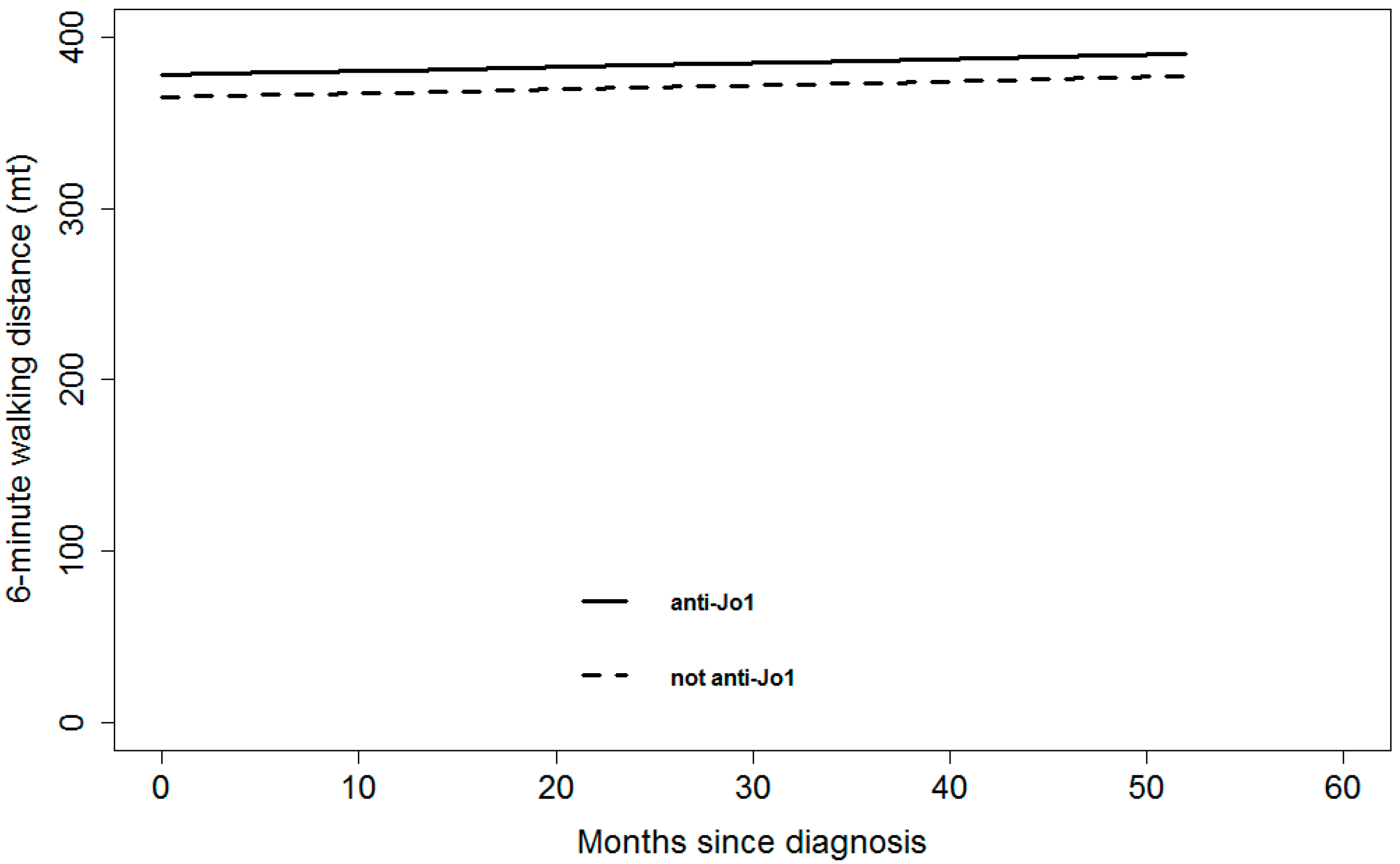
| Parameters | General Population | Jo1 | Non Jo1 | P |
|---|---|---|---|---|
| N | 57 | 32 | 25 | |
| sex = F (%) | 39 (68.4) | 20 (62.5) | 19 (76.0) | 0.391 |
| Age of development of respiratory symptoms (median (IQR)) | 63 (50,70) | 61 (51,70) | 65 (50,69) | 0.843 |
| Age of diagnosis ASS (median (IQR)) | 65.5 (52,71) | 61 (52,71) | 66 (55,71) | 0.723 |
| Delay on diagnosis in months (median (IQR)) | 7 (2,20) | 6 (1,16) | 10 (3,20) | 0.095 |
| Smoking status—active smoker or former smoker (%) | 15 (27.8) | 6 (20.0) | 9 (37.5) | 0.223 |
| Coexistance of other autoimmune diseases (%) | 16 (28.1) | 7 (21.9) | 9 (36.0) | 0.373 |
| Antibodies | General Population | Jo1 | Non Jo1 | P |
| ANA (%) | 31 (60.8) | 16 (57.1) | 15 (65.2) | 0.58 |
| Anti-SSA/Ro 52+ (%) | 26 (56.5) | 10 (40.0) | 16 (76.2) | 0.019 |
| Symptoms | General Population | Jo1 | Non Jo1 | P |
| Exertional dyspnea (%) | 46 (83.6) | 25 (80.6) | 21 (87.5) | 0.716 |
| Dyspnea at rest (%) | 17 (29.8) | 10 (31.2) | 7 (28.0) | 1 |
| Cough (%) | 30 (53.6) | 15 (46.9) | 15 (62.5) | 0.288 |
| Chest pain (%) | 3 (5.4) | 2 (6.2) | 1 (4.2) | 1 |
| Raynaud’s phenomenon (%) | 9 (16.1) | 2 (6.2) | 7 (29.2) | 0.03 |
| Fever (%) | 15 (26.8) | 6 (18.8) | 9 (37.5) | 0.138 |
| Mechanic’s hands (%) | 3 (5.6) | 2 (6.2) | 1 (4.5) | 1 |
| Joint involvement (%) | 23 (40.4) | 13 (40.6) | 10 (40.0) | 1 |
| Muscle involvement (%) | 17 (29.8) | 11 (34.4) | 6 (24.0) | 0.561 |
| Skin lesions (%) | 11 (19.3) | 4 (12.5) | 7 (28.0) | 0.184 |
| GI tract symptoms (%) | 4 (7.0) | 3 (9.4) | 1 (4.0) | 0.623 |
| Systemic symptoms (%) | 15 (26.3) | 7 (21.9) | 8 (32.0) | 0.546 |
| Chronic onset of respiratory symptoms (%) | 27 (49.1) | 14 (46.7) | 13 (52.0) | 789 |
| Respiratory symptoms as first onset of ASS (%) | 42 (75.0) | 22 (71.0) | 20 (80.0) | 0.542 |
| General Population | Jo1 | Non Jo1 | P | |
| TLC (%) (median (IQR)) | 77% (66,88) | 79% (74,88) | 74 (61,88) | 0.265 |
| FVC (%) (median (IQR)) | 80 (59,92,5) | 78% (60,92) | 81 (58,92) | 0.941 |
| VC (%) (median (IQR)) | 77% (60,92) | 78% (66,92) | 60 (58,88) | 0.295 |
| DLCO (%) (median (IQR)) | 46% (37,57) | 43% (37,52) | 52 (34,58) | 0.7 |
| IT (%) (median (IQR)) | 80.5 (77,86.5) | 80% (77,84) | 81 (75,86) | 0.887 |
| Walking test (m) (median (IQR)) | 352 (299,460) | 385 (319,490) | 342 (281,412) | 0.334 |
| Walking test (% minimal SaO2) (median (IQR)) | 92 (88,94) | 92 (89,94) | 92 (87,95) | 0.815 |
| Walking test (% median SaO2) (median (IQR)) | 92 (89,96) | 92 (90,96) | 92 (88,96) | 0.776 |
| General Population | Jo1 | Non Jo1 | P | |
| Corticosteroids (%) | 50 (90.9) | 29 (90.6) | 21 (91.3) | 1 |
| Immunosuppressant | 27 (50.9) | 19 (59.4) | 8 (38.1) | 0.166 |
| Cyclosporin A | 4 | 3 | 1 | |
| Azathioprine | 8 | 4 | 4 | |
| Methotrexate | 4 | 3 | 1 | |
| Cyclophosphamide | 8 | 7 | 1 | |
| Cyclosporin A + cyclophosphamide | 2 | 1 | 1 | |
| Rituximab | 1 | 1 | - | |
| Oxygen therapy (%) | 15 (27.8) | 9 (28.1) | 6 (27.3) | 1 |
| Clinical Features During Follow Up | Jo1 | NonJo1 | P |
|---|---|---|---|
| N | 29 | 18 | |
| Raynaud’s phenomenon (%) | 1 (3.4) | 0 (0.0) | 1.000 |
| Fever (%) | 1 (3.4) | 0 (0.0) | 1.000 |
| Mechanic’s hands (%) | 3 (10.7) | 3 (16.7) | 0.666 |
| Joint pain (%) | 5 (17.9) | 6 (33.3) | 0.296 |
| Muscle pain (%) | 3 (10.7) | 3 (16.7) | 0.666 |
| Skin lesions (%) | 4 (14.3) | 2 (11.1) | 1.000 |
| Systemic symptoms (%) | 3 (10.7) | 2 (11.8) | 1.000 |
| Acute exacerbation of respiratory symptoms (%) | 8 (29.6) | 5 (29.4) | 1.000 |
| FVC (%) | DLCO (%) | |||
|---|---|---|---|---|
| Variables | Estimate (95%Confidence Interval) | P-Value | Estimate (95% Confidence Interval) | P-Value |
| anti-Jo1 vs. non-anti-Jo1 | 2.31 (−14.13;18.74) | 0.7813 | 2.70 (−7.46;16.86) | 0.7051 |
| Anti-SSA/Ro52+ Yes vs. No | 7.05 (−8.10;22.20) | 0.3579 | 3.49 (−10.27;17.26) | 0.6153 |
| Acute onset vs. chronic | 3.64 (−10.76;18.03) | 0.6072 | 0.63 (−12.29;13.55) | 0.9230 |
| Delay in diagnosis (>1 year vs. within 1 years) | 5.58 (−11.00;22.17) | 0.5058 | 0.66 (−14.18;15.51) | 0.9296 |
| Immunosuppressant treatment (Yes vs. No) | 8.03 (−12.56;28.61) | 0.4409 | −2.85 (−19.14;13.43) | 0.7286 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dei, G.; Rebora, P.; Catalano, M.; Sebastiani, M.; Faverio, P.; Pozzi, M.R.; Manfredi, A.; Cameli, P.; Salton, F.; Salvarani, C.; et al. Functional Progression in Patients with Interstitial Lung Disease Resulted Positive to Antisynthetase Antibodies: A Multicenter, Retrospective Analysis. J. Clin. Med. 2020, 9, 3033. https://doi.org/10.3390/jcm9093033
Dei G, Rebora P, Catalano M, Sebastiani M, Faverio P, Pozzi MR, Manfredi A, Cameli P, Salton F, Salvarani C, et al. Functional Progression in Patients with Interstitial Lung Disease Resulted Positive to Antisynthetase Antibodies: A Multicenter, Retrospective Analysis. Journal of Clinical Medicine. 2020; 9(9):3033. https://doi.org/10.3390/jcm9093033
Chicago/Turabian StyleDei, Giulia, Paola Rebora, Martina Catalano, Marco Sebastiani, Paola Faverio, Maria Rosa Pozzi, Andreina Manfredi, Paolo Cameli, Francesco Salton, Carlo Salvarani, and et al. 2020. "Functional Progression in Patients with Interstitial Lung Disease Resulted Positive to Antisynthetase Antibodies: A Multicenter, Retrospective Analysis" Journal of Clinical Medicine 9, no. 9: 3033. https://doi.org/10.3390/jcm9093033
APA StyleDei, G., Rebora, P., Catalano, M., Sebastiani, M., Faverio, P., Pozzi, M. R., Manfredi, A., Cameli, P., Salton, F., Salvarani, C., Cavagna, L., Confalonieri, M., Bargagli, E., Luppi, F., & Pesci, A. (2020). Functional Progression in Patients with Interstitial Lung Disease Resulted Positive to Antisynthetase Antibodies: A Multicenter, Retrospective Analysis. Journal of Clinical Medicine, 9(9), 3033. https://doi.org/10.3390/jcm9093033









