The Impact of the 2019 European Guideline for Cardiovascular Risk Management: A Cross-Sectional Study in General Practice
Abstract
1. Introduction
2. Methods
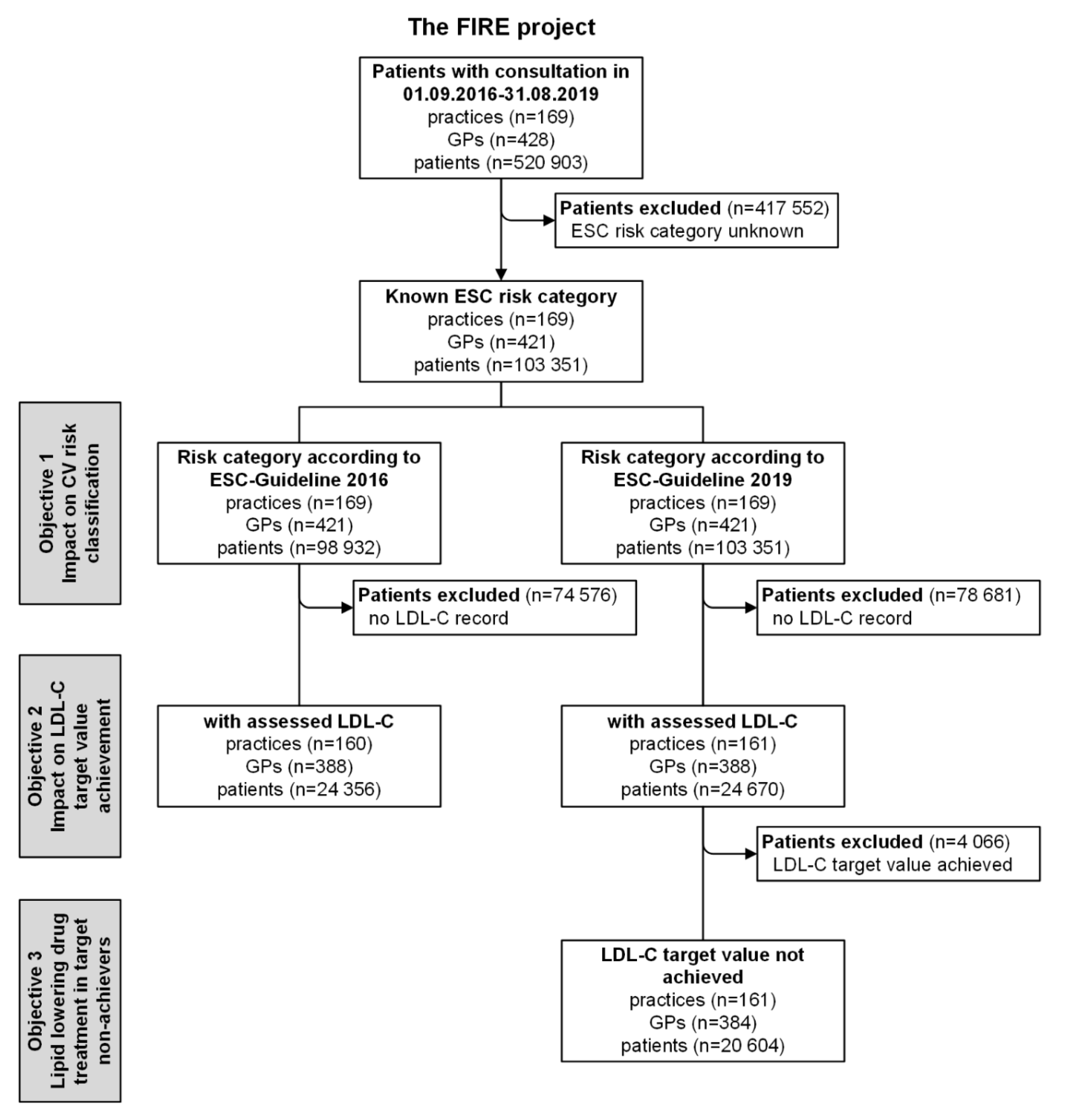
2.1. Study Design, Setting, and Participants
2.2. Implementation of CV Risk Classification
2.3. Database Query and Variables
2.4. Data Analysis
3. Results
3.1. Characteristics of Patients
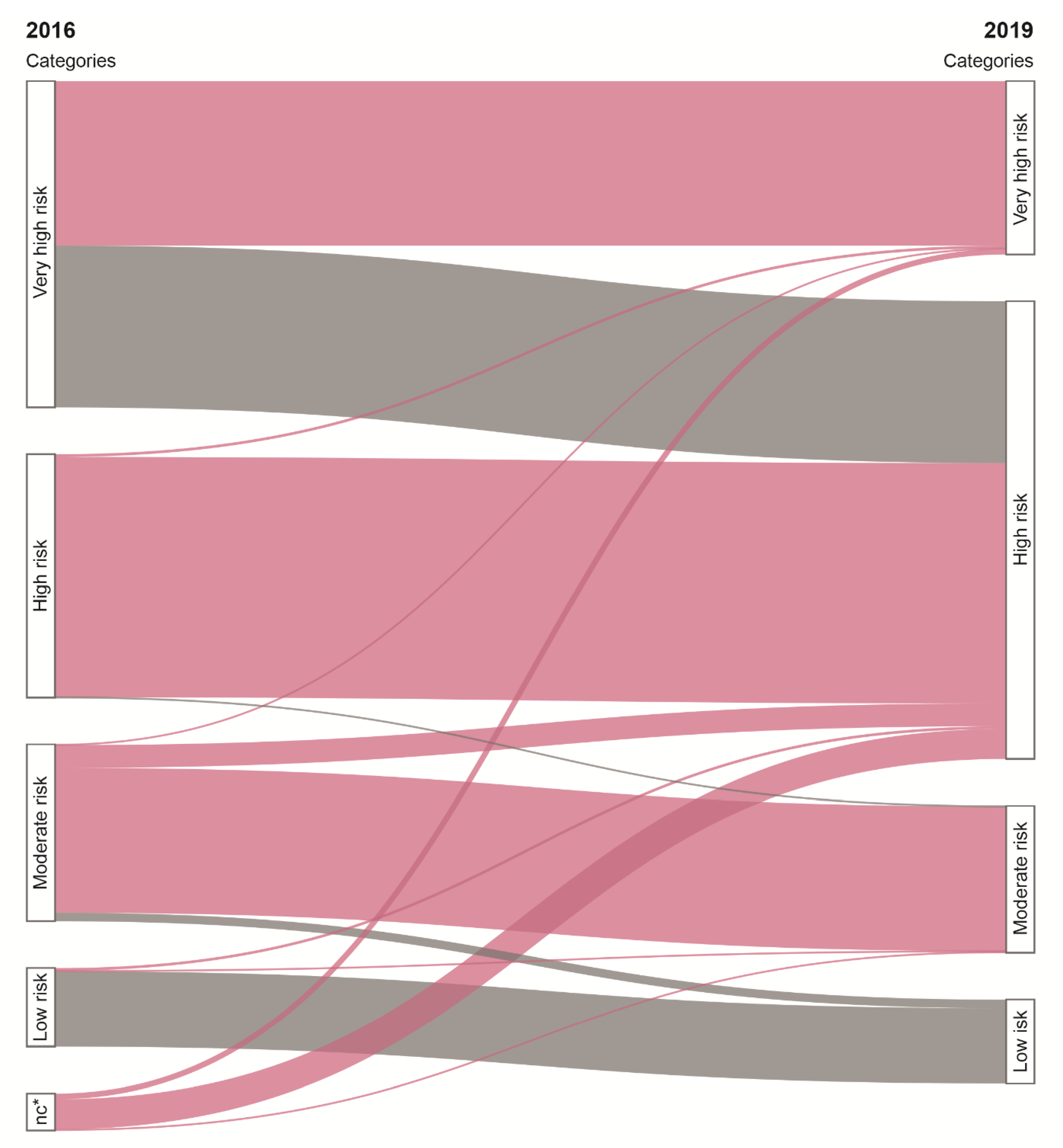
3.2. Impact of Guideline Update on Risk Classification and LDL-C Target Values
3.3. Impact of Guideline Update on LDL-C Target Value Achievement
3.4. Lipid-Lowering Treatment in LDL-C Target Non-Achievers
4. Discussion
Strength and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Data Sharing
References
- Townsend, N.; Wilson, L.; Bhatnagar, P.; Wickramasinghe, K.; Rayner, M.; Nichols, M. Cardiovascular disease in europe: Epidemiological update 2016. Eur. Heart J. 2016, 37, 3232–3245. [Google Scholar] [CrossRef] [PubMed]
- Damen, J.A.; Hooft, L.; Schuit, E.; Debray, T.P.; Collins, G.S.; Tzoulaki, I.; Lassale, C.M.; Siontis, G.C.; Chiocchia, V.; Roberts, C.; et al. Prediction models for cardiovascular disease risk in the general population: Systematic review. BMJ 2016, 353, 2416. [Google Scholar] [CrossRef] [PubMed]
- Wilson, P.W. Established risk factors and coronary artery disease: The framingham study. Am. J. Hypertens 1994, 7, 7–12. [Google Scholar] [CrossRef] [PubMed]
- Mach, F.; Baigent, C.; Catapano, A.L.; Koskinas, K.C.; Casula, M.; Badimon, L.; Chapman, M.J.; De Backer, G.G.; Delgado, V.; Ference, B.A.; et al. 2019 ESC/EAS guidelines for the management of dyslipidaemias: Lipid modification to reduce cardiovascular risk. Eur. Heart J. 2019, 41, 111–188. [Google Scholar] [CrossRef]
- Piepoli, M.F.; Hoes, A.W.; Agewall, S.; Albus, C.; Brotons, C.; Catapano, A.L.; Cooney, M.T.; Corra, U.; Cosyns, B.; Deaton, C.; et al. 2016 european guidelines on cardiovascular disease prevention in clinical practice: The sixth joint task force of the european society of cardiology and other societies on cardiovascular disease prevention in clinical practice (constituted by representatives of 10 societies and by invited experts)developed with the special contribution of the european association for cardiovascular prevention & rehabilitation (eacpr). Eur. Heart J. 2016, 37, 2315–2381. [Google Scholar]
- Chmiel, C.; Bhend, H.; Senn, O.; Zoller, M.; Rosemann, T.; Group, F.S. The fire project a milestone for research in primary care in switzerland. Swiss Med. Wkly. 2011, 141, w13142. [Google Scholar]
- Association, F.S.M. Online Query Tool of the Swiss Physician Statistics [online-abfragetool der fmh-ärztestatistik]. Available online: http://aerztestatistik.myfmh2.fmh.ch (accessed on 26 February 2020).
- Conroy, R.M.; Pyorala, K.; Fitzgerald, A.P.; Sans, S.; Menotti, A.; De Backer, G.; De Bacquer, D.; Ducimetiere, P.; Jousilahti, P.; Keil, U.; et al. Estimation of ten-year risk of fatal cardiovascular disease in europe: The score project. Eur. Heart J. 2003, 24, 987–1003. [Google Scholar] [CrossRef]
- Bell, K.J.L.; Hayen, A.; Irwig, L.; Takahashi, O.; Ohde, S.; Glasziou, P. When to remeasure cardiovascular risk in untreated people at low and intermediate risk: Observational study. BMJ 2013, 346, 1895. [Google Scholar] [CrossRef]
- Cosentino, F.; Grant, P.J.; Aboyans, V.; Bailey, C.J.; Ceriello, A.; Delgado, V.; Federici, M.; Filippatos, G.; Grobbee, D.E.; Hansen, T.B.; et al. 2019 ESC guidelines on diabetes, pre-diabetes, and cardiovascular diseases developed in collaboration with the easd: The task force for diabetes, pre-diabetes, and cardiovascular diseases of the european society of cardiology (ESC) and the european association for the study of diabetes (easd). Eur. Heart J. 2019, 41, 255–323. [Google Scholar]
- WONCA, I.C.C. International Classification of Primary Care—ICPC-2; Springer: Berlin/Heidelberg, Germany, 1998. [Google Scholar]
- WHO Collaborating Centre for Drug Statistics Methodology. Atc-Structure and Principles. Available online: https://www.whocc.no/atc/structure_and_principles/ (accessed on 9 July 2019).
- Stone, N.J.; Robinson, J.G.; Lichtenstein, A.H.; Bairey Merz, C.N.; Blum, C.B.; Eckel, R.H.; Goldberg, A.C.; Gordon, D.; Levy, D.; Lloyd-Jones, D.M.; et al. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: A report of the american college of cardiology/american heart association task force on practice guidelines. J. Am. Coll. Cardiol. 2014, 63, 2889–2934. [Google Scholar] [CrossRef]
- R Core Team. R: A Language and Environment for Statistical Computing; R Foundation for Statistical Computing: Vienna, Austria, 2019. [Google Scholar]
- Byrne, P.; Cullinan, J.; Smith, S.M. Statins for primary prevention of cardiovascular disease. BMJ 2019, 367, l5674. [Google Scholar] [CrossRef]
- Mihaylova, B.; Emberson, J.; Blackwell, L.; Keech, A.; Simes, J.; Barnes, E.H.; Voysey, M.; Gray, A.; Collins, R.; Baigent, C. The effects of lowering ldl cholesterol with statin therapy in people at low risk of vascular disease: Meta-analysis of individual data from 27 randomised trials. Lancet 2012, 380, 581–590. [Google Scholar] [PubMed]
- Presta, V.; Figliuzzi, I.; Miceli, F.; Coluccia, R.; Fogacci, F.; Cicero, A.F.G.; Ferrucci, A.; Borghi, C.; Volpe, M.; Tocci, G.; et al. Achievement of low density lipoprotein (LDL) cholesterol targets in primary and secondary prevention: Analysis of a large real practice database in italy. Atherosclerosis 2019, 285, 40–48. [Google Scholar] [CrossRef] [PubMed]
- Fox, K.M.; Tai, M.H.; Kostev, K.; Hatz, M.; Qian, Y.; Laufs, U. Treatment patterns and low-density lipoprotein cholesterol (LDL-C) goal attainment among patients receiving high- or moderate-intensity statins. Clin. Res. Cardiol. 2018, 107, 380–388. [Google Scholar] [CrossRef] [PubMed]
- Arca, M.; Ansell, D.; Averna, M.; Fanelli, F.; Gorcyca, K.; Iorga, S.R.; Maggioni, A.P.; Paizis, G.; Tomic, R.; Catapano, A.L. Statin utilization and lipid goal attainment in high or very-high cardiovascular risk patients: Insights from italian general practice. Atherosclerosis 2018, 271, 120–127. [Google Scholar] [CrossRef]
- Saxon, D.R.; Eckel, R.H. Statin intolerance: A literature review and management strategies. Prog. Cardiovasc. Dis. 2016, 59, 153–164. [Google Scholar] [CrossRef]
- Zhao, Z.; Du, S.; Shen, S.; Luo, P.; Ding, S.; Wang, G.; Wang, L. Comparative efficacy and safety of lipid-lowering agents in patients with hypercholesterolemia: A frequentist network meta-analysis. Med. 2019, 98, e14400. [Google Scholar] [CrossRef]
- Schmidt, A.F.; Pearce, L.S.; Wilkins, J.T.; Overington, J.P.; Hingorani, A.D.; Casas, J.P. Pcsk9 monoclonal antibodies for the primary and secondary prevention of cardiovascular disease. Cochrane Database Syst. Rev. 2017, 4, CD011748. [Google Scholar] [CrossRef]
- Khan, S.U.; Talluri, S.; Riaz, H.; Rahman, H.; Nasir, F.; Bin Riaz, I.; Sattur, S.; Ahmed, H.; Kaluski, E.; Krasuski, R. A bayesian network meta-analysis of pcsk9 inhibitors, statins and ezetimibe with or without statins for cardiovascular outcomes. Eur. J. Prev. Cardiol. 2018, 25, 844–853. [Google Scholar] [CrossRef]
- Yu, S.; Zolfaghari, K.; Rascati, K.L.; Copeland, L.A.; Godley, P.J.; McNeal, C. Guidelines impact cholesterol management. J. Clin. Lipidol. 2019, 13, 432–442. [Google Scholar] [CrossRef]
- Superko, H.R.; Williams, P.T.; Dansinger, M.; Schaefer, E. Trends in low-density lipoprotein-cholesterol blood values between 2012 and 2017 suggest sluggish adoption of the recent 2013 treatment guidelines. Clin. Cardiol. 2019, 42, 101–110. [Google Scholar] [CrossRef] [PubMed]
- Okerson, T.; Patel, J.; DiMario, S.; Burton, T.; Seare, J.; Harrison, D.J. Effect of 2013 acc/aha blood cholesterol guidelines on statin treatment patterns and low-density lipoprotein cholesterol in atherosclerotic cardiovascular disease patients. J. Am. Heart Assoc. 2017, 6, e004909. [Google Scholar] [CrossRef]
- Byrne, P.; Cullinan, J.; Gillespie, P.; Perera, R.; Smith, S.M. Statins for primary prevention of cardiovascular disease: Modelling guidelines and patient preferences based on an irish cohort. Br. J. Gen. Pract. 2019, 69, e373–e380. [Google Scholar] [CrossRef] [PubMed]
- Lugtenberg, M.; Zegers-van Schaick, J.M.; Westert, G.P.; Burgers, J.S. Why don’t physicians adhere to guideline recommendations in practice? An analysis of barriers among dutch general practitioners. Implement. Sci. 2009, 4, 54. [Google Scholar] [CrossRef] [PubMed]
- Mahtta, D.; Rodriguez, F.; Jneid, H.; Levine, G.N.; Virani, S.S. Improving adherence to cardiovascular guidelines: Realistic transition from paper to patient. Expert Rev. Cardiovasc. Ther. 2020, 18, 41–51. [Google Scholar] [CrossRef] [PubMed]
- Djalali, S.; Ursprung, N.; Rosemann, T.; Senn, O.; Tandjung, R. Undirected health it implementation in ambulatory care favors paper-based workarounds and limits health data exchange. Int. J. Med. Inform. 2015, 84, 920–932. [Google Scholar] [CrossRef]
- Hostettler, S.; Kraft, E. Fmh-ärztestatistik 2017—aktuelle zahlen. Schweiz. Ärztezeitung 2018, 99, 408–413. [Google Scholar]
- Wolfson, J.; Vock, D.M.; Bandyopadhyay, S.; Kottke, T.; Vazquez-Benitez, G.; Johnson, P.; Adomavicius, G.; O’Connor, P.J. Use and customization of risk scores for predicting cardiovascular events using electronic health record data. J. Am. Heart Assoc. 2017, 6, e003670. [Google Scholar] [CrossRef]

| 2016 Guideline | ||||
|---|---|---|---|---|
| Patient Characteristics | Low Risk | Moderate Risk | High Risk | Very High Risk |
| (n = 9461) | (n = 21,138) | (n = 29,176) | (n = 39,157) | |
| Median age (IQR) | 47 (44–51) | 58 (53–63) | 69 (53–81) | 72 (61–81) |
| % female | 75.7 | 38.6 | 57.0 | 42.6 |
| % with an LDL-C measurement | 9.9 | 16.1 | 19.1 | 36.9 |
| median LDL-C (IQR) mmol/L | 3.1 (2.5–3.8) | 3.3 (2.7–4) | 3.0 (2.3–3.9) | 2.3 (1.8–3.1) |
| Morbidities | ||||
| s % with previous CVD | 0.0 | 0.0 | 0.0 | 27.8 |
| % with severe CKD | 0.0 | 0.0 | 0.0 | 10.2 |
| % with moderate CKD | 0.0 | 0.0 | 57.9 | 25.1 |
| % with diabetes | 0.0 | 0.0 | 23.6 | 74.2 |
| % with dyslipidemia | 53.5 | 68.7 | 32.5 | 39.8 |
| % with hypertension | 11.7 | 22.3 | 43.4 | 67.2 |
| % with obesity | 15.7 | 16.3 | 12.5 | 25.5 |
| Lipid-lowering drugs | ||||
| % no treatment | 97.6 | 93.3 | 80.0 | 52.2 |
| % statin only | 2.1 | 6.0 | 18.3 | 42.7 |
| % statin and ezetimibe | 0.18 | 0.46 | 1.37 | 4.52 |
| % ezetimibe only | 0.11 | 0.19 | 0.33 | 0.49 |
| % statin and PCSK-9 inhibitors | 0.00 | 0.00 | 0.03 | 0.06 |
| % PCSK-9 inhibitors only | 0.00 | 0.00 | 0.01 | 0.02 |
| 2019 Guideline | ||||
| Patient Characteristics | Low Risk | Moderate Risk | High Risk | Very High Risk |
| (n = 10,094) | (n = 17,583) | (n = 54,876) | (n = 20,798) | |
| Median age (IQR) | 48 (44–52) | 58 (53–62) | 68 (56–78) | 74 (66–83) |
| % female | 74.8 | 38.9 | 51.8 | 38.7 |
| % with an LDL-C measurement | 9.0 | 13.5 | 24.6 | 37.9 |
| median LDL-C (IQR) mmol/L | 3.1 (2.5–3.6) | 3.2 (2.6–3.8) | 2.9 (2.1–3.7) | 2.2 (1.7–3) |
| Morbidities | ||||
| % with previous CVD | 0.0 | 0.0 | 0.0 | 52.4 |
| % with severe CKD | 0.0 | 0.0 | 0.0 | 19.1 |
| % with moderate CKD | 0.0 | 0.0 | 36.8 | 31.5 |
| % with diabetes | 0.0 | 0.0 | 47.9 | 46.4 |
| % with dyslipidemia | 52.2 | 67.0 | 38.5 | 48.1 |
| % with hypertension | 10.8 | 22.7 | 45.4 | 78.6 |
| % with obesity | 14.9 | 16.9 | 15.4 | 29.8 |
| Lipid-lowering drugs | ||||
| % no treatment | 98.0 | 94.2 | 74.6 | 42.2 |
| % statin only | 1.8 | 5.3 | 23.4 | 50.5 |
| % statin and ezetimibe | 0.11 | 0.39 | 1.61 | 6.63 |
| % ezetimibe only | 0.09 | 0.15 | 0.38 | 0.60 |
| % statin and PCSK-9 inhibitors | 0.00 | 0.00 | 0.02 | 0.12 |
| % PCSK-9 inhibitors only | 0.00 | 0.01 | 0.01 | 0.04 |
| 2019 | ||||
|---|---|---|---|---|
| Patient Characteristics | Low Risk | Moderate Risk | High Risk | Very High Risk |
| (n = 475) | (n = 1769) | (n = 11,551) | (n = 6809) | |
| Median age (IQR) | 49 (45–53) | 59 (55–63) | 67 (57–76) | 72 (64–79) |
| % female | 81.3 | 41.0 | 51.5 | 35.5 |
| median LDL-C (IQR) in mmol/L | 3.6 (3.3–4.0) | 3.5 (3.1–4.0) | 3.1 (2.5–3.9) | 2.4 (1.9–3.2) |
| Median distance to LDL-C target (IQR) in mmol/L | 0.6 (0.3–1.0) | 0.9 (0.5–1.4) | 1.3 (0.7–2.1) | 1.0 (0.5–1.8) |
| Lipid-lowering drugs | ||||
| % no treatment | 93.3 | 89.1 | 58.5 | 28.9 |
| % statin only | 5.3 | 10.1 | 37.7 | 58.7 |
| % statin and ezetimibe | 0.84 | 0.45 | 3.05 | 11.4 |
| % ezetimibe only | 0.63 | 0.40 | 0.74 | 0.84 |
| % statin and PCSK-9 inhibitors | 0.00 | 0.00 | 0.06 | 0.22 |
| % PCSK-9 inhibitors only | 0.00 | 0.00 | 0.02 | 0.07 |
| Statin treatment intensity | ||||
| % high | 1.5 | 2.3 | 12.0 | 33.8 |
| % moderate | 2.9 | 6.9 | 23.7 | 29.9 |
| % low | 0.2 | 0.5 | 1.7 | 2.1 |
| % missing | 1.5 | 0.9 | 3.3 | 4.4 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Meier, R.; Rachamin, Y.; Rosemann, T.; Markun, S. The Impact of the 2019 European Guideline for Cardiovascular Risk Management: A Cross-Sectional Study in General Practice. J. Clin. Med. 2020, 9, 2140. https://doi.org/10.3390/jcm9072140
Meier R, Rachamin Y, Rosemann T, Markun S. The Impact of the 2019 European Guideline for Cardiovascular Risk Management: A Cross-Sectional Study in General Practice. Journal of Clinical Medicine. 2020; 9(7):2140. https://doi.org/10.3390/jcm9072140
Chicago/Turabian StyleMeier, Rahel, Yael Rachamin, Thomas Rosemann, and Stefan Markun. 2020. "The Impact of the 2019 European Guideline for Cardiovascular Risk Management: A Cross-Sectional Study in General Practice" Journal of Clinical Medicine 9, no. 7: 2140. https://doi.org/10.3390/jcm9072140
APA StyleMeier, R., Rachamin, Y., Rosemann, T., & Markun, S. (2020). The Impact of the 2019 European Guideline for Cardiovascular Risk Management: A Cross-Sectional Study in General Practice. Journal of Clinical Medicine, 9(7), 2140. https://doi.org/10.3390/jcm9072140






