A Potential Mechanism of Tumor Progression during Systemic Infections Via the Hepatocyte Growth Factor (HGF)/c-Met Signaling Pathway
Abstract
1. Introduction
2. Experimental Section
2.1. Materials/Patients and Methods
2.1.1. Clinical Study
2.1.2. Animal Study
Mice and Cell Line
Animal Model
Flow Cytometric Analysis of c-Met Expression
Measurement of Cytokines
Establishment of c-Met Knockdown Cells
Western Blotting
Evaluation of Tumor Growth in Liver Metastasis
Ethics
Statistical Analysis
3. Results
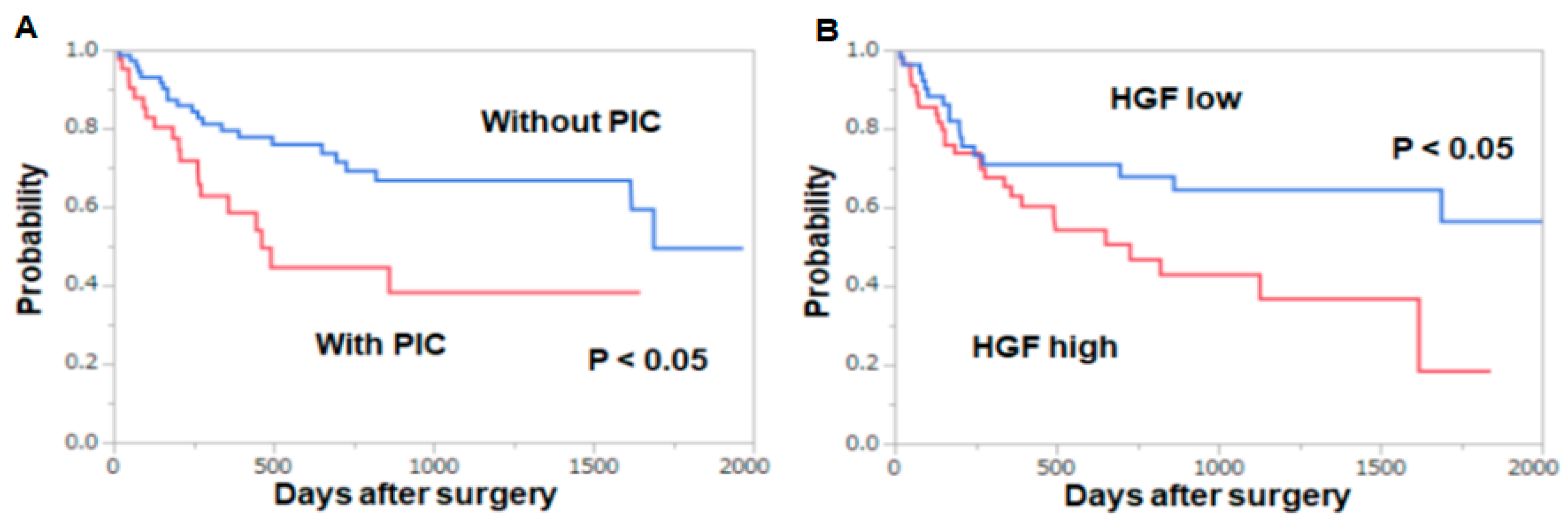
3.1. Clinical Study
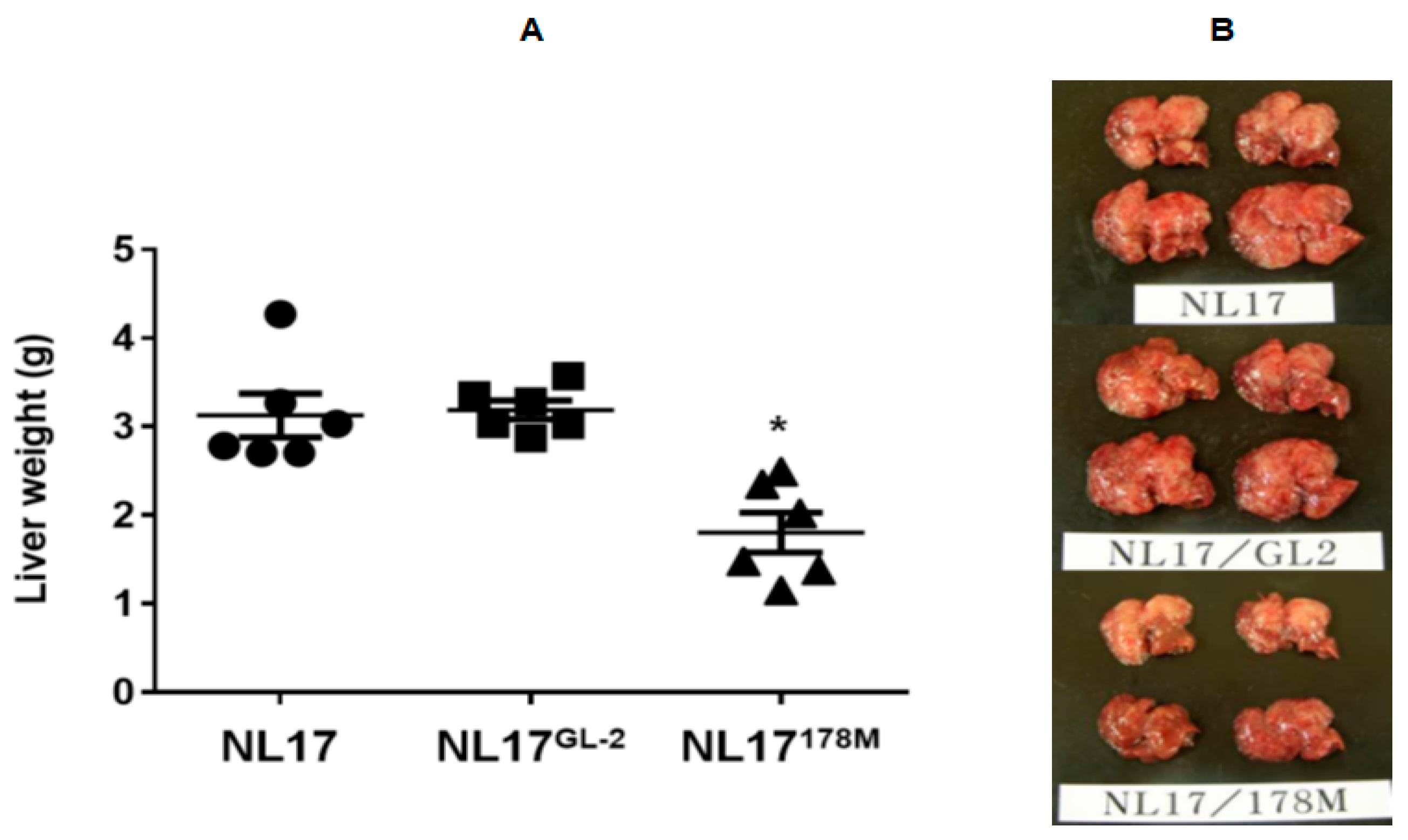
3.2. Animal Study
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Tsujimoto, H.; Ichikura, T.; Ono, S.; Sugasawa, H.; Hiraki, S.; Sakamoto, N.; Yaguchi, Y.; Yoshida, K.; Matsumoto, Y.; Hase, K. Impact of postoperative infection on long-term survival after potentially curative resection for gastric cancer. Ann. Surg. Oncol. 2009, 16, 311–318. [Google Scholar] [CrossRef] [PubMed]
- Tsujimoto, H.; Ueno, H.; Hashiguchi, Y.; Ono, S.; Ichikura, T.; Hase, K. Postoperative infections are associated with adverse outcome after resection with curative intent for colorectal cancer. Oncol. Lett. 2010, 1, 119–125. [Google Scholar] [CrossRef]
- Lagarde, S.M.; de Boer, J.D.; ten Kate, F.J.; Busch, O.R.; Obertop, H.; van Lanschot, J.J. Postoperative complications after esophagectomy for adenocarcinoma of the esophagus are related to timing of death due to recurrence. Ann. Surg. 2008, 247, 71–76. [Google Scholar] [CrossRef] [PubMed]
- Shimada, H.; Fukagawa, T.; Haga, Y.; Oba, K. Does postoperative morbidity worsen the oncological outcome after radical surgery for gastrointestinal cancers? A systematic review of the literature. Ann. Gastroenterol. Surg. 2017, 1, 11–23. [Google Scholar] [CrossRef] [PubMed]
- Shen, W.H.; Zhou, J.H.; Broussard, S.R.; Freund, G.G.; Dantzer, R.; Kelley, K.W. Proinflammatory cytokines block growth of breast cancer cells by impairing signals from a growth factor receptor. Cancer Res. 2002, 62, 4746–4756. [Google Scholar] [PubMed]
- Shankar, J.; Messenberg, A.; Chan, J.; Underhill, T.M.; Foster, L.J.; Nabi, I.R. Pseudopodial actin dynamics control epithelial-mesenchymal transition in metastatic cancer cells. Cancer Res. 2010, 70, 3780–3790. [Google Scholar] [CrossRef]
- Zhang, Y.W.; Su, Y.; Volpert, O.V.; Vande Woude, G.F. Hepatocyte growth factor/scatter factor mediates angiogenesis through positive VEGF and negative thrombospondin 1 regulation. Proc. Natl. Acad. Sci. USA 2003, 100, 12718–12723. [Google Scholar] [CrossRef]
- Sawada, K.; Radjabi, A.R.; Shinomiya, N.; Kistner, E.; Kenny, H.; Becker, A.R.; Turkyilmaz, M.A.; Salgia, R.; Yamada, S.D.; Vande Woude, G.F.; et al. c-Met overexpression is a prognostic factor in ovarian cancer and an effective target for inhibition of peritoneal dissemination and invasion. Cancer Res. 2007, 67, 1670–1679. [Google Scholar] [CrossRef]
- Matsumoto, Y.; Tsujimoto, H.; Ono, S.; Shinomiya, N.; Miyazaki, H.; Hiraki, S.; Takahata, R.; Yoshida, K.; Saitoh, D.; Yamori, T.; et al. Abdominal Infection Suppresses the Number and Activity of Intrahepatic Natural Killer Cells and Promotes Tumor Growth in a Murine Liver Metastasis Model. Ann. Surg. Oncol. 2016, 23 (Suppl. 2), 257–265. [Google Scholar] [CrossRef]
- Bottaro, D.P.; Rubin, J.S.; Faletto, D.L.; Chan, A.M.; Kmiecik, T.E.; Vande Woude, G.F.; Aaronson, S.A. Identification of the hepatocyte growth factor receptor as the c-met proto-oncogene product. Science 1991, 251, 802–804. [Google Scholar] [CrossRef]
- Naldini, L.; Weidner, K.M.; Vigna, E.; Gaudino, G.; Bardelli, A.; Ponzetto, C.; Narsimhan, R.P.; Hartmann, G.; Zarnegar, R.; Michalopoulos, G.K.; et al. Scatter factor and hepatocyte growth factor are indistinguishable ligands for the MET receptor. EMBO J. 1991, 10, 2867–2878. [Google Scholar] [CrossRef] [PubMed]
- Takahashi, N.; Yamada, Y.; Furuta, K.; Honma, Y.; Iwasa, S.; Takashima, A.; Kato, K.; Hamaguchi, T.; Shimada, Y. Serum levels of hepatocyte growth factor and epiregulin are associated with the prognosis on anti-EGFR antibody treatment in KRAS wild-type metastatic colorectal cancer. Br. J. Cancer 2014, 110, 2716–2727. [Google Scholar] [CrossRef]
- Smyth, E.C.; Sclafani, F.; Cunningham, D. Emerging molecular targets in oncology: Clinical potential of MET/hepatocyte growth-factor inhibitors. OncoTarget Ther. 2014, 7, 1001–1014. [Google Scholar] [CrossRef] [PubMed]
- Nakamura, T.; Nishizawa, T.; Hagiya, M.; Seki, T.; Shimonishi, M.; Sugimura, A.; Tashiro, K.; Shimizu, S. Molecular cloning and expression of human hepatocyte growth factor. Nature 1989, 342, 440–443. [Google Scholar] [CrossRef] [PubMed]
- Zhen, R.; Yang, J.; Wang, Y.; Li, Y.; Chen, B.; Song, Y.; Ma, G.; Yang, B. Hepatocyte growth factor improves bone regeneration via the bone morphogenetic protein2mediated NFkappaB signaling pathway. Mol. Med. Rep. 2018, 17, 6045–6053. [Google Scholar] [CrossRef] [PubMed]
- Mosevoll, K.A.; Skrede, S.; Markussen, D.L.; Fanebust, H.R.; Flaatten, H.K.; Assmus, J.; Reikvam, H.; Bruserud, O. Inflammatory Mediator Profiles Differ in Sepsis Patients with and Without Bacteremia. Front. Immunol. 2018, 9, 691. [Google Scholar] [CrossRef] [PubMed]
- Glanemann, M.; Knobeloch, D.; Ehnert, S.; Culmes, M.; Seeliger, C.; Seehofer, D.; Nussler, A.K. Hepatotropic growth factors protect hepatocytes during inflammation by upregulation of antioxidative systems. World J. Gastroenterol. 2011, 17, 2199–2205. [Google Scholar] [CrossRef] [PubMed]
- Deutschman, C.S.; Haber, B.A.; Andrejko, K.; Cressman, D.E.; Harrison, R.; Elenko, E.; Taub, R. Increased expression of cytokine-induced neutrophil chemoattractant in septic rat liver. Am. J. Physiol. 1996, 271, R593–R600. [Google Scholar] [CrossRef]
- Knaus, W.A.; Draper, E.A.; Wagner, D.P.; Zimmerman, J.E. APACHE II: A severity of disease classification system. Crit. Care Med. 1985, 13, 818–829. [Google Scholar] [CrossRef]
- American College of Chest Physicians/Society of Critical Care Medicine Consensus Conference: Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. Crit. Care Med. 1992, 20, 864–874. [CrossRef]
- Brierley, J.D.; Gospodarowicz, M.K.; Wittekind, C. TNM Classification of Malignant Tumours; Oxford Wiley-Blackwell: Oxford, UK, 2016. [Google Scholar]
- Tsujimoto, H.; Ono, S.; Mochizuki, H.; Aosasa, S.; Majima, T.; Ueno, C.; Matsumoto, A. Role of macrophage inflammatory protein 2 in acute lung injury in murine peritonitis. J. Surg. Res. 2002, 103, 61–67. [Google Scholar] [CrossRef]
- Shinomiya, N.; Gao, C.F.; Xie, Q.; Gustafson, M.; Waters, D.J.; Zhang, Y.W.; Vande Woude, G.F. RNA interference reveals that ligand-independent met activity is required for tumor cell signaling and survival. Cancer Res. 2004, 64, 7962–7970. [Google Scholar] [CrossRef]
- Van der Bij, G.J.; Oosterling, S.J.; Beelen, R.H.; Meijer, S.; Coffey, J.C.; van Egmond, M. The perioperative period is an underutilized window of therapeutic opportunity in patients with colorectal cancer. Ann. Surg. 2009, 249, 727–734. [Google Scholar] [CrossRef]
- Tsujimoto, H.; Ono, S.; Ichikura, T.; Matsumoto, Y.; Yamamoto, J.; Hase, K. Roles of inflammatory cytokines in the progression of gastric cancer: Friends or foes? Gastric Cancer 2010, 13, 212–221. [Google Scholar] [CrossRef] [PubMed]
- Chochi, K.; Ichikura, T.; Kinoshita, M.; Majima, T.; Shinomiya, N.; Tsujimoto, H.; Kawabata, T.; Sugasawa, H.; Ono, S.; Seki, S.; et al. Helicobacter pylori Augments Growth of Gastric Cancers via the Lipopolysaccharide-Toll-like Receptor 4 Pathway whereas Its Lipopolysaccharide Attenuates Antitumor Activities of Human Mononuclear Cells. Clin. Cancer Res. 2008, 14, 2909–2917. [Google Scholar] [CrossRef] [PubMed]
- Sakamoto, N.; Tsujimoto, H.; Takahata, R.; Cao, B.; Zhao, P.; Ito, N.; Shimazaki, H.; Ichikura, T.; Hase, K.; Vande Woude, G.F.; et al. MET4 expression predicts poor prognosis of gastric cancers with Helicobacter pylori infection. Cancer Sci. 2017, 108, 322–330. [Google Scholar] [CrossRef]
- Kubo, Y.; Fukushima, S.; Inamori, Y.; Tsuruta, M.; Egashira, S.; Yamada-Kanazawa, S.; Nakahara, S.; Tokuzumi, A.; Miyashita, A.; Aoi, J.; et al. Serum concentrations of HGF are correlated with response to anti-PD-1 antibody therapy in patients with metastatic melanoma. J. Dermatol. Sci. 2019, 93, 33–40. [Google Scholar] [CrossRef]
- Yang, C.; Bork, U.; Scholch, S.; Kulu, Y.; Kaderali, L.; Bolstorff, U.L.; Kahlert, C.; Weitz, J.; Rahbari, N.N.; Reissfelder, C. Postoperative course and prognostic value of circulating angiogenic cytokines after pancreatic cancer resection. Oncotarget 2017, 8, 72315–72323. [Google Scholar] [CrossRef]
- Christensen, J.G.; Burrows, J.; Salgia, R. c-Met as a target for human cancer and characterization of inhibitors for therapeutic intervention. Cancer Lett. 2005, 225, 1–26. [Google Scholar] [CrossRef]
- Mizuno, S.; Nakamura, T. HGF-MET cascade, a key target for inhibiting cancer metastasis: The impact of NK4 discovery on cancer biology and therapeutics. Int. J. Mol. Sci. 2013, 14, 888–919. [Google Scholar] [CrossRef]
- Kim, K.H.; Kim, H. Progress of antibody-based inhibitors of the HGF-cMET axis in cancer therapy. Exp. Mol. Med. 2017, 49, e307. [Google Scholar] [CrossRef] [PubMed]




| Patients | |||||
|---|---|---|---|---|---|
| (n = 16) | |||||
| Age | 71.0 ± 9.4 | ||||
| Male/Female | 9/7 | ||||
| Diagnosis | |||||
| Colonic perforation | 14 | 88% | |||
| SMAO | 2 | 13% | |||
| APACH II score | 11.7 ± 3.4 | ||||
| Duration of SIRS (days) | 3.4 ± 2.4 | ||||
| Length of stay in hospital (days) | 27.4 ± 23.8 | ||||
| Duration of SIRS (days) | 1.8 ± 2.6 | ||||
| 30-day mortality | 3 | 19% | |||
| With PIC | Without PIC | p-Value | ||||
|---|---|---|---|---|---|---|
| (n = 44) | (n = 74) | |||||
| Age | 70.9 ± 8.7 | 71.4 ± 8.6 | 0.48 | |||
| Male/Female | 38/6 | 60/14 | 0.46 | |||
| Tumor location | ||||||
| Upper | 10 | 23% | 4 | 5% | 0.01 | |
| Middle | 20 | 45% | 33 | 45% | ||
| Lower | 14 | 32% | 37 | 50% | ||
| Fields of lymphadenectomy | ||||||
| 2-field | 22 | 50% | 53 | 72% | 0.02 | |
| 3-field | 22 | 50% | 21 | 28% | ||
| Neoadjuvant therapy | ||||||
| No | 25 | 57% | 31 | 42% | 0.12 | |
| Yes | 19 | 43% | 43 | 58% | ||
| Chemotherapy | 19 | 42 | ||||
| Chemoradiation | 0 | 1 | ||||
| Tumor depth | ||||||
| pT1-pT2 | 17 | 39% | 34 | 46% | 0.44 | |
| pT3-pT4 | 27 | 61% | 40 | 54% | ||
| Nodal metastasis | ||||||
| pN0-N1 | 35 | 80% | 53 | 72% | 0.34 | |
| pN2-N3 | 9 | 20% | 21 | 28% | ||
| pStage | ||||||
| 1 | 12 | 27% | 22 | 30% | 0.23 | |
| 2 | 10 | 23% | 15 | 20% | ||
| 3 | 18 | 41% | 36 | 49% | ||
| 4 | 4 | 9% | 1 | 1% | ||
| Infectious complications * | ||||||
| Anastomotic leakage | 23 | 52% | - | |||
| Pneumonia | 14 | 32% | - | |||
| Empyema | 4 | 9% | - | |||
| ARDS | 2 | 5% | - | |||
| UTI | 2 | 5% | - | |||
| Others | 4 | 9% | - | |||
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tsujimoto, H.; Horiguchi, H.; Matsumoto, Y.; Takahata, R.; Shinomiya, N.; Yamori, T.; Miyazaki, H.; Ono, S.; Saitoh, D.; Kishi, Y.; et al. A Potential Mechanism of Tumor Progression during Systemic Infections Via the Hepatocyte Growth Factor (HGF)/c-Met Signaling Pathway. J. Clin. Med. 2020, 9, 2074. https://doi.org/10.3390/jcm9072074
Tsujimoto H, Horiguchi H, Matsumoto Y, Takahata R, Shinomiya N, Yamori T, Miyazaki H, Ono S, Saitoh D, Kishi Y, et al. A Potential Mechanism of Tumor Progression during Systemic Infections Via the Hepatocyte Growth Factor (HGF)/c-Met Signaling Pathway. Journal of Clinical Medicine. 2020; 9(7):2074. https://doi.org/10.3390/jcm9072074
Chicago/Turabian StyleTsujimoto, Hironori, Hiroyuki Horiguchi, Yusuke Matsumoto, Risa Takahata, Nariyoshi Shinomiya, Takao Yamori, Hiromi Miyazaki, Satoshi Ono, Daizoh Saitoh, Yoji Kishi, and et al. 2020. "A Potential Mechanism of Tumor Progression during Systemic Infections Via the Hepatocyte Growth Factor (HGF)/c-Met Signaling Pathway" Journal of Clinical Medicine 9, no. 7: 2074. https://doi.org/10.3390/jcm9072074
APA StyleTsujimoto, H., Horiguchi, H., Matsumoto, Y., Takahata, R., Shinomiya, N., Yamori, T., Miyazaki, H., Ono, S., Saitoh, D., Kishi, Y., & Ueno, H. (2020). A Potential Mechanism of Tumor Progression during Systemic Infections Via the Hepatocyte Growth Factor (HGF)/c-Met Signaling Pathway. Journal of Clinical Medicine, 9(7), 2074. https://doi.org/10.3390/jcm9072074






