A Physiologic Approach to Hemodynamic Monitoring and Optimizing Oxygen Delivery in Shock Resuscitation
Abstract
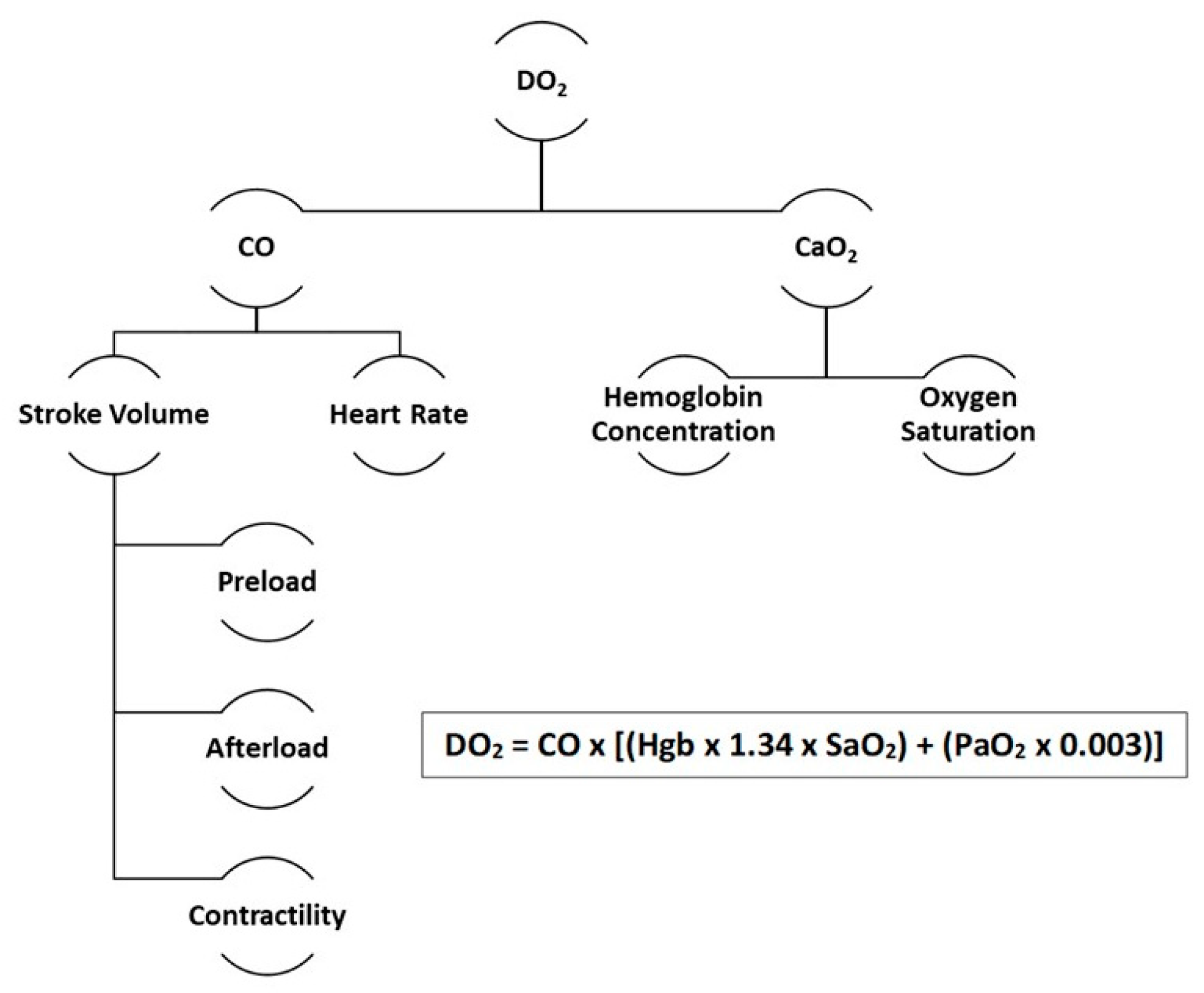
1. Introduction
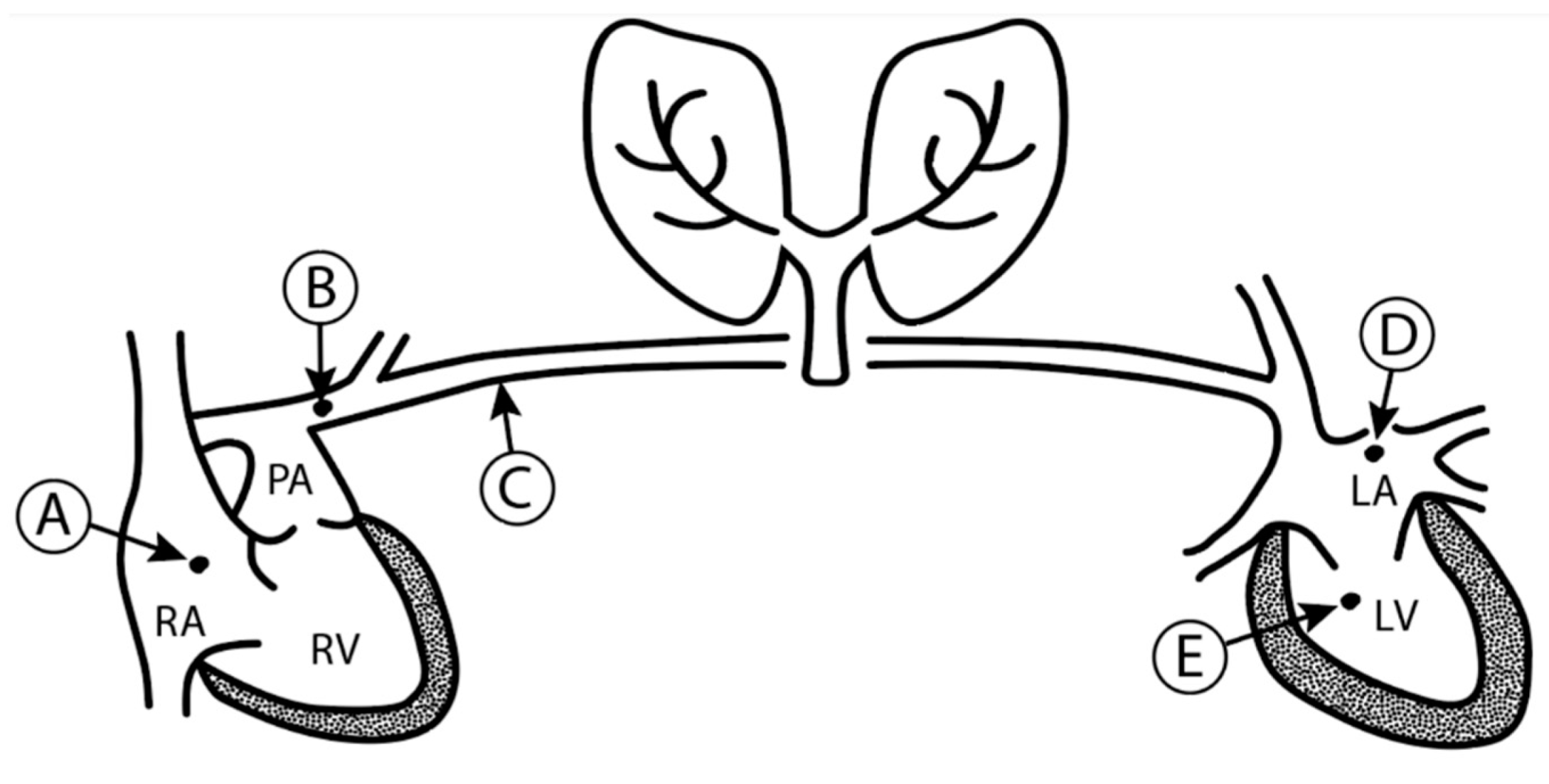
2. Measuring Preload
2.1. Left Ventricular End-Diastolic Volume and Pressure
2.2. Pulmonary Capillary Wedge Pressure and Left Atrial Pressure
2.3. Central Venous Pressure and Right Atrial Pressure
3. Determining Fluid Responsiveness
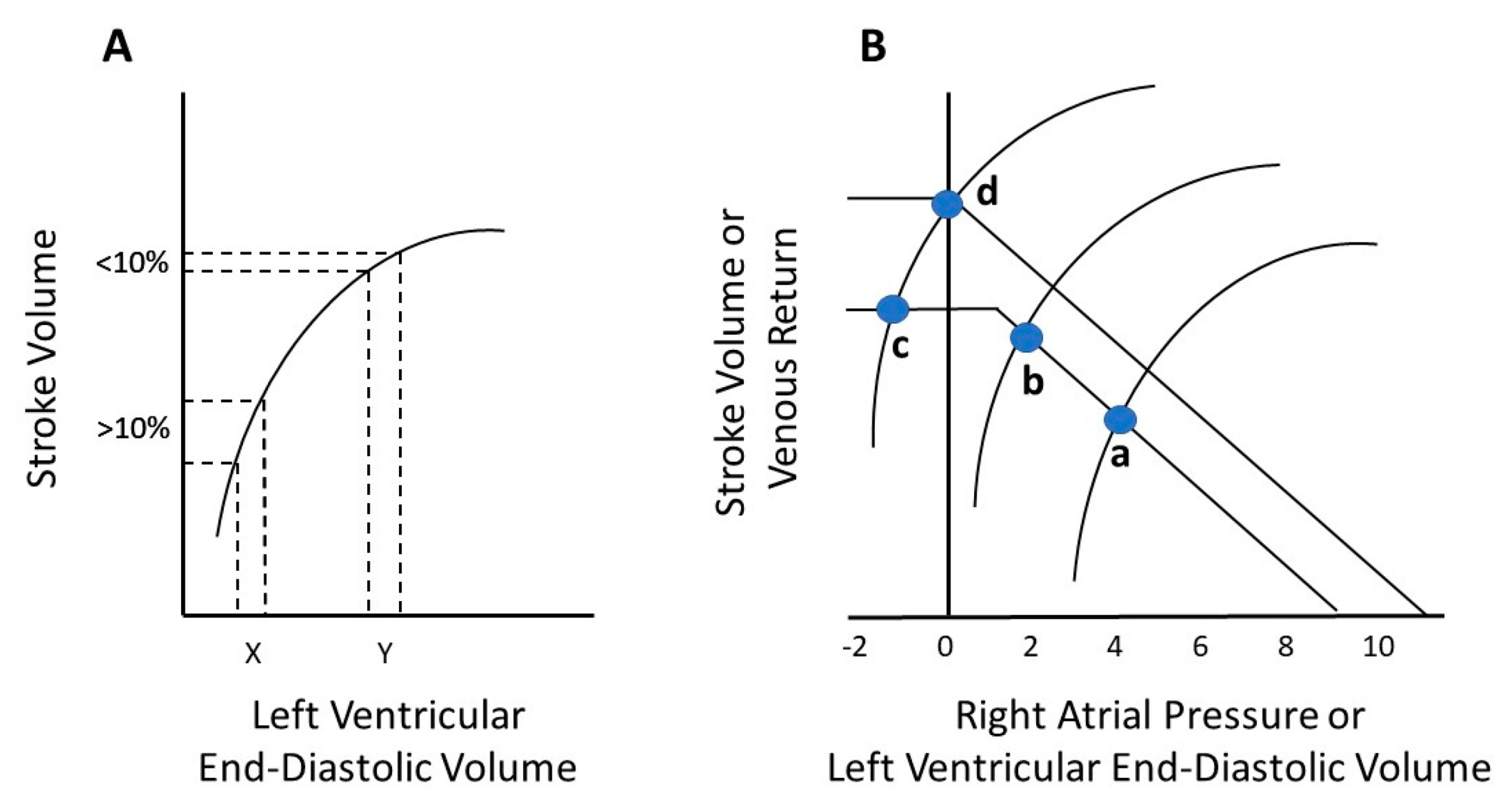
3.1. The Frank–Starling Law and Guyton’s Venous Return
3.2. The Classical Fluid Bolus
3.3. The 5-2-0 Rule
3.4. Inferior Vena Cava (IVC) Collapsibility
3.5. Passive Leg Raise (PLR)
3.6. Stroke Volume Variation (SVV) and Pulse Pressure Variation (PPV)
4. Measuring Stroke Volume and Cardiac Output
4.1. Indicator Dilution Methods
4.2. Arterial Waveform/Pulse Contour Analysis
4.3. Transthoracic (TTE) and Transesophageal Echocardiography (TEE)
4.4. Bioimpedance and Bioreactance
4.5. Transcutaneous/Transesophageal Doppler
5. Optimizing Afterload
6. Improving Contractility
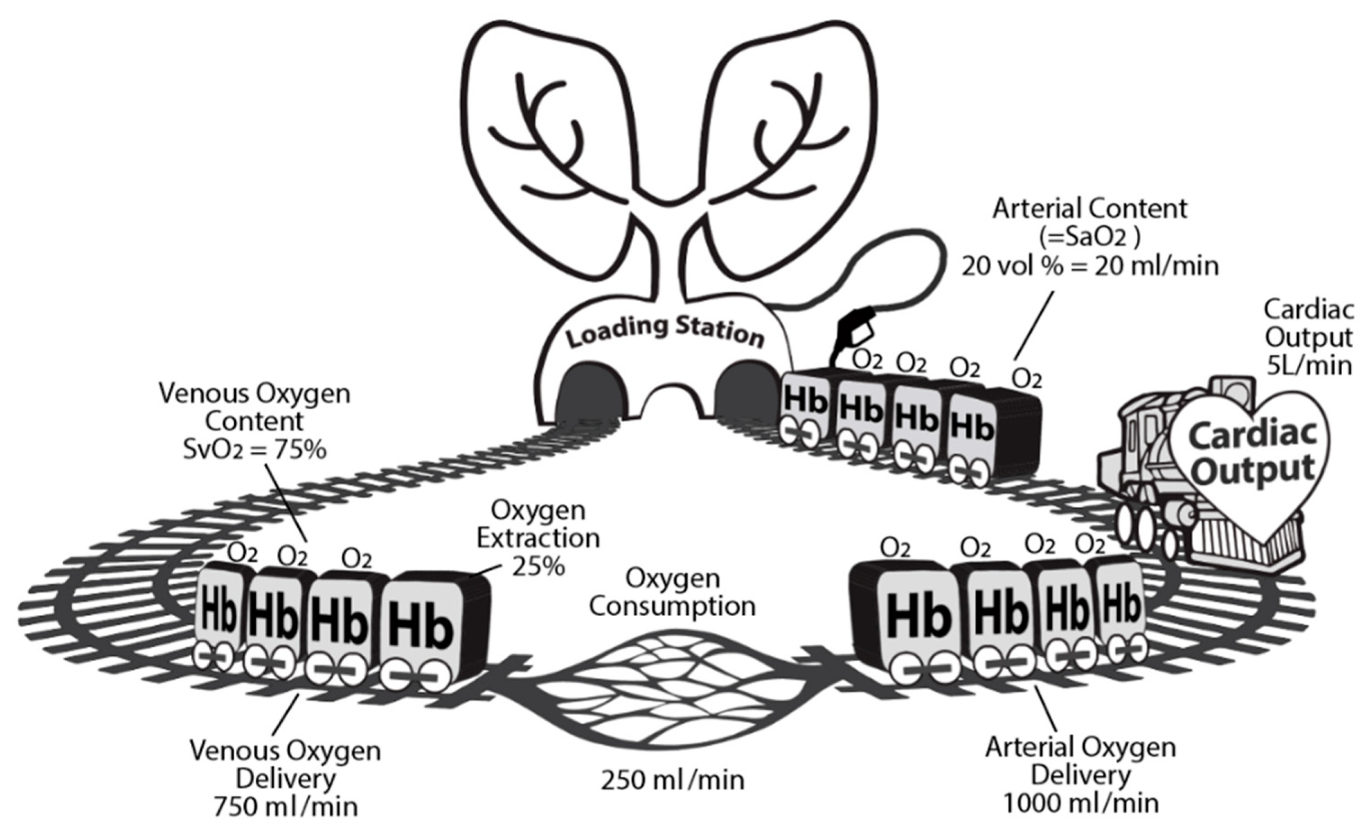
7. Increasing Arterial Oxygen Content
8. Targeting Contractility and Hemoglobin Guided by SvO2 or ScvO2
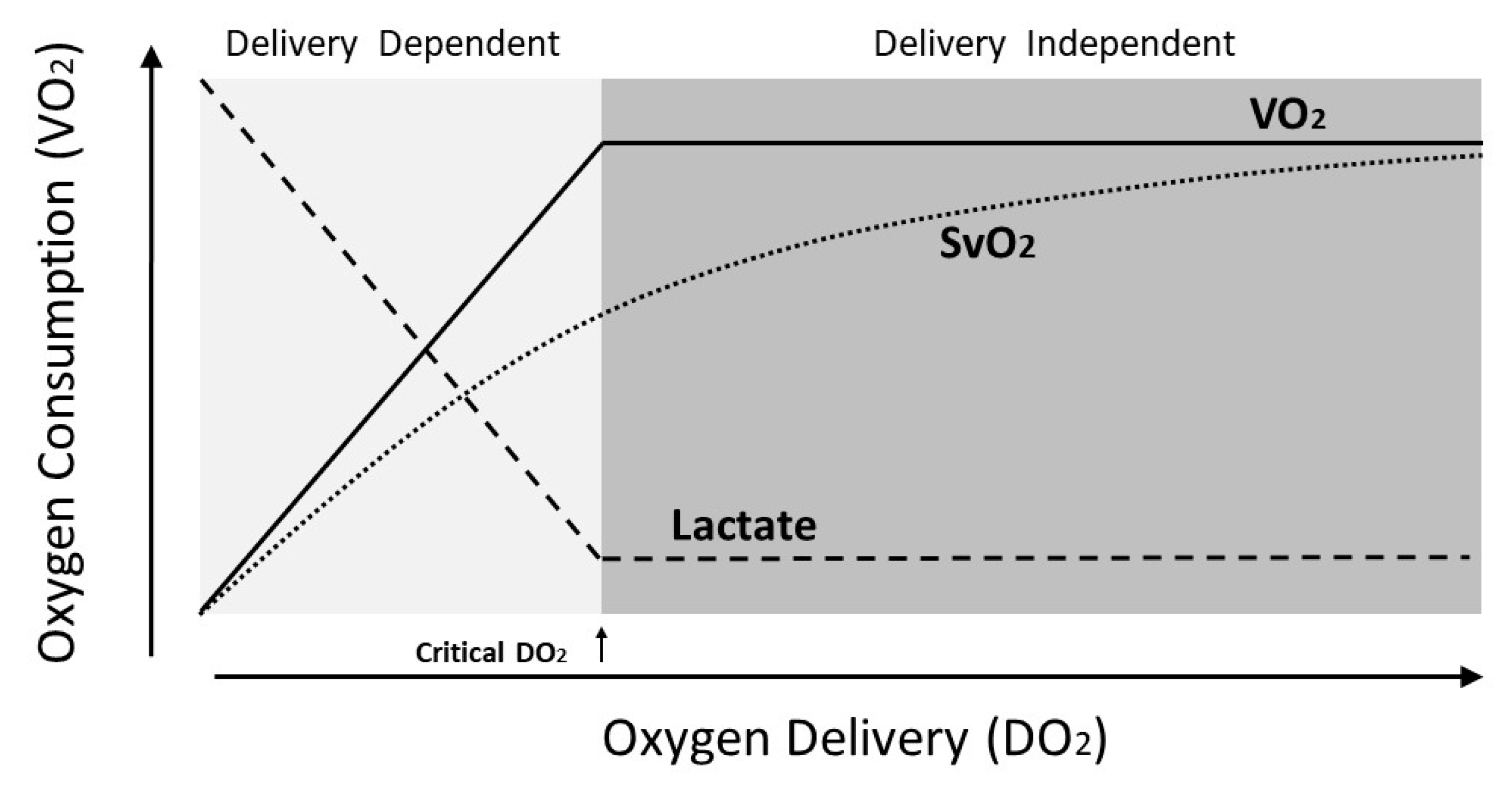
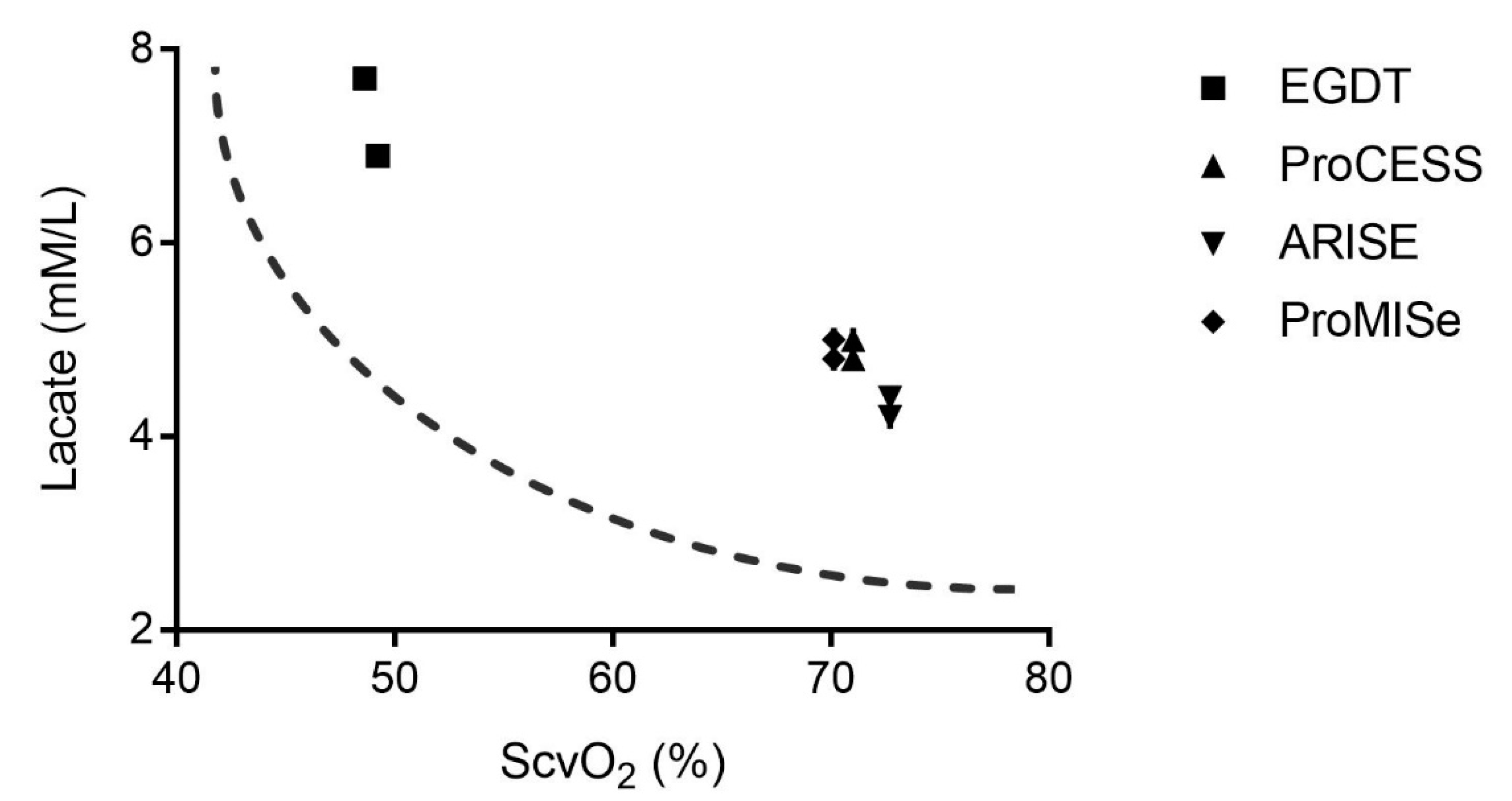
9. SvO2 and Lactate as Indicators of Shock and Resuscitation Endpoints
10. Liberal versus Restrictive Fluids or Vasopressors
11. Putting It All Together
Case Example
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Weil, M.H.; Gazmuri, R.J. Shock: New developments in the management of shock. Appl. Cardiopulm. Pathophysiol. 1991, 4, 103–107. [Google Scholar] [PubMed]
- Kalantari, K.; Chang, J.N.; Ronco, C.; Rosner, M.H. Assessment of intravascular volume status and volume responsiveness in critically ill patients. Kidney Int. 2013, 83, 1017–1028. [Google Scholar] [CrossRef] [PubMed]
- Bentzer, P.; Griesdale, D.E.; Boyd, J.; MacLean, K.; Sirounis, D.; Ayas, N.T. Will This Hemodynamically Unstable Patient Respond to a Bolus of Intravenous Fluids? JAMA 2016, 316, 1298–1309. [Google Scholar] [CrossRef]
- Shujaat, A.; Bajwa, A.A. Optimization of preload in severe sepsis and septic shock. Crit. Care Res. Pract. 2012, 2012, 761051. [Google Scholar] [CrossRef]
- Monnet, X.; Marik, P.; Teboul, J.L. Passive leg raising for predicting fluid responsiveness: A systematic review and meta-analysis. Intensive Care Med. 2016, 42, 1935–1947. [Google Scholar] [CrossRef]
- Abbas, A.E.; Fortuin, F.D.; Schiller, N.B.; Appleton, C.P.; Moreno, C.A.; Lester, S.J. Echocardiographic determination of mean pulmonary artery pressure. Am. J. Cardiol. 2003, 92, 1373–1376. [Google Scholar] [CrossRef]
- Hollenberg, S.M. Hemodynamic monitoring. Chest 2013, 143, 1480–1488. [Google Scholar] [CrossRef]
- Suess, E.M.; Pinsky, M.R. Hemodynamic Monitoring for the Evaluation and Treatment of Shock: What Is the Current State of the Art? Semin. Respir. Crit. Care Med. 2015, 36, 890–898. [Google Scholar] [CrossRef]
- Rhodes, A.; Cusack, R.J.; Newman, P.J.; Grounds, R.M.; Bennett, E.D. A randomised, controlled trial of the pulmonary artery catheter in critically ill patients. Intensive Care Med. 2002, 28, 256–264. [Google Scholar] [CrossRef]
- Richard, C.; Warszawski, J.; Anguel, N.; Deye, N.; Combes, A.; Barnoud, D.; Boulain, T.; Lefort, Y.; Fartoukh, M.; Baud, F.; et al. Early use of the pulmonary artery catheter and outcomes in patients with shock and acute respiratory distress syndrome: A randomized controlled trial. JAMA 2003, 290, 2713–2720. [Google Scholar] [CrossRef]
- Marik, P.E.; Baram, M.; Vahid, B. Does central venous pressure predict fluid responsiveness? A systematic review of the literature and the tale of seven mares. Chest 2008, 134, 172–178. [Google Scholar] [CrossRef]
- Sequeira, V.; van der Velden, J. Historical perspective on heart function: The Frank-Starling Law. Biophys. Rev. 2015, 7, 421–447. [Google Scholar] [CrossRef] [PubMed]
- Lopes, M.R.; Auler, J.O., Jr.; Michard, F. Volume management in critically ill patients: New insights. Clinics (Sao Paulo) 2006, 61, 345–350. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Guyton, A.C. Determination of cardiac output by equating venous return curves with cardiac response curves. Physiol. Rev. 1955, 35, 123–129. [Google Scholar] [CrossRef]
- Glassford, N.J.; Martensson, J.; Eastwood, G.M.; Jones, S.L.; Tanaka, A.; Wilkman, E.; Bailey, M.; Bellomo, R.; For the Global Observational Evaluations in the ICU (GLOBE-ICU) Investigators. Defining the characteristics and expectations of fluid bolus therapy: A worldwide perspective. J. Crit. Care 2016, 35, 126–132. [Google Scholar] [CrossRef]
- American Thoracic Society. Evidence-based colloid use in the critically III: American Thoracic Society Consensus Statement. Am. J. Respir. Crit. Care Med. 2004, 170, 1247–1259. [Google Scholar] [CrossRef]
- Annane, D.; Siami, S.; Jaber, S.; Martin, C.; Elatrous, S.; Declere, A.D.; Preiser, J.C.; Outin, H.; Troche, G.; Charpentier, C.; et al. Effects of fluid resuscitation with colloids vs. crystalloids on mortality in critically ill patients presenting with hypovolemic shock: The CRISTAL randomized trial. JAMA 2013, 310, 1809–1817. [Google Scholar] [CrossRef]
- Rhodes, A.; Evans, L.E.; Alhazzani, W.; Levy, M.M.; Antonelli, M.; Ferrer, R.; Kumar, A.; Sevransky, J.E.; Sprung, C.L.; Nunnally, M.E.; et al. Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016. Intensive Care Med. 2017, 43, 304–377. [Google Scholar] [CrossRef]
- Weil, M.H.; Henning, R.J. New concepts in the diagnosis and fluid treatment of circulatory shock: Thirteenth annual Becton, Dickinson and Company Oscar Schwidetsky Memorial Lecture. Anesth. Analg. 1979, 58, 124–132. [Google Scholar] [CrossRef]
- Weekes, A.J.; Tassone, H.M.; Babcock, A.; Quirke, D.P.; Norton, H.J.; Jayarama, K.; Tayal, V.S. Comparison of serial qualitative and quantitative assessments of caval index and left ventricular systolic function during early fluid resuscitation of hypotensive emergency department patients. Acad. Emerg. Med. 2011, 18, 912–921. [Google Scholar] [CrossRef] [PubMed]
- Yanagawa, Y.; Nishi, K.; Sakamoto, T.; Okada, Y. Early diagnosis of hypovolemic shock by sonographic measurement of inferior vena cava in trauma patients. J. Trauma Acute Care Surg. 2005, 58, 825–829. [Google Scholar] [CrossRef]
- Porter, T.R.; Shillcutt, S.K.; Adams, M.S.; Desjardins, G.; Glas, K.E.; Olson, J.J.; Troughton, R.W. Guidelines for the use of echocardiography as a monitor for therapeutic intervention in adults: A report from the American Society of Echocardiography. J. Am. Soc. Echocardiogr. 2015, 28, 40–56. [Google Scholar] [CrossRef]
- Chopra, S.; Thompson, J.; Shahangian, S.; Thapamagar, S.; Moretta, D.; Gasho, C.; Cohen, A.; Nguyen, H.B. Precision and consistency of the passive leg raising maneuver for determining fluid responsiveness with bioreactance non-invasive cardiac output monitoring in critically ill patients and healthy volunteers. PLoS ONE 2019, 14, e0222956. [Google Scholar] [CrossRef] [PubMed]
- Michard, F. Changes in arterial pressure during mechanical ventilation. Anesthesiology 2005, 103, 419–428. [Google Scholar] [CrossRef] [PubMed]
- Pinsky, M.R. Heart lung interactions during mechanical ventilation. Curr. Opin. Crit. Care 2012, 18, 256–260. [Google Scholar] [CrossRef] [PubMed]
- Marik, P.E.; Cavallazzi, R.; Vasu, T.; Hirani, A. Dynamic changes in arterial waveform derived variables and fluid responsiveness in mechanically ventilated patients: A systematic review of the literature. Crit. Care Med. 2009, 37, 2642–2647. [Google Scholar] [CrossRef] [PubMed]
- McGee, W.T. A simple physiologic algorithm for managing hemodynamics using stroke volume and stroke volume variation: Physiologic optimization program. J. Intensive Care Med. 2009, 24, 352–360. [Google Scholar] [CrossRef]
- Mesquida, J.; Kim, H.K.; Pinsky, M.R. Effect of tidal volume, intrathoracic pressure, and cardiac contractility on variations in pulse pressure, stroke volume, and intrathoracic blood volume. Intensive Care Med. 2011, 37, 1672–1679. [Google Scholar] [CrossRef]
- Reuter, D.A.; Huang, C.; Edrich, T.; Shernan, S.K.; Eltzschig, H.K. Cardiac output monitoring using indicator-dilution techniques: Basics, limits, and perspectives. Anesth. Analg. 2010, 110, 799–811. [Google Scholar] [CrossRef]
- Montenij, L.J.; de Waal, E.E.; Buhre, W.F. Arterial waveform analysis in anesthesia and critical care. Curr. Opin. Anaesthesiol. 2011, 24, 651–656. [Google Scholar] [CrossRef]
- Saugel, B.; Bendjelid, K.; Critchley, L.A.; Rex, S.; Scheeren, T.W. Journal of Clinical Monitoring and Computing 2016 end of year summary: Cardiovascular and hemodynamic monitoring. J. Clin. Monit. Comput. 2017, 31, 5–17. [Google Scholar] [CrossRef] [PubMed]
- Peyton, P.J.; Chong, S.W. Minimally invasive measurement of cardiac output during surgery and critical care: A meta-analysis of accuracy and precision. Anesthesiology 2010, 113, 1220–1235. [Google Scholar] [CrossRef]
- Feissel, M.; Michard, F.; Mangin, I.; Ruyer, O.; Faller, J.P.; Teboul, J.L. Respiratory changes in aortic blood velocity as an indicator of fluid responsiveness in ventilated patients with septic shock. Chest 2001, 119, 867–873. [Google Scholar] [CrossRef] [PubMed]
- Vincent, J.L.; Rhodes, A.; Perel, A.; Martin, G.S.; Della Rocca, G.; Vallet, B.; Pinsky, M.R.; Hofer, C.K.; Teboul, J.L.; de Boode, W.P.; et al. Clinical review: Update on hemodynamic monitoring—A consensus of 16. Crit. Care 2011, 15, 229. [Google Scholar] [CrossRef] [PubMed]
- Keren, H.; Burkhoff, D.; Squara, P. Evaluation of a noninvasive continuous cardiac output monitoring system based on thoracic bioreactance. Am. J. Physiol. Heart Circ. Physiol. 2007, 293, H583–H589. [Google Scholar] [CrossRef] [PubMed]
- Squara, P.; Denjean, D.; Estagnasie, P.; Brusset, A.; Dib, J.C.; Dubois, C. Noninvasive cardiac output monitoring (NICOM): A clinical validation. Intensive Care Med. 2007, 33, 1191–1194. [Google Scholar] [CrossRef]
- Marque, S.; Cariou, A.; Chiche, J.D.; Squara, P. Comparison between Flotrac-Vigileo and Bioreactance, a totally noninvasive method for cardiac output monitoring. Crit. Care 2009, 13, R73. [Google Scholar] [CrossRef]
- Raval, N.Y.; Squara, P.; Cleman, M.; Yalamanchili, K.; Winklmaier, M.; Burkhoff, D. Multicenter evaluation of noninvasive cardiac output measurement by bioreactance technique. J. Clin. Monit. Comput. 2008, 22, 113–119. [Google Scholar] [CrossRef]
- Chong, S.W.; Peyton, P.J. A meta-analysis of the accuracy and precision of the ultrasonic cardiac output monitor (USCOM). Anaesthesia 2012, 67, 1266–1271. [Google Scholar] [CrossRef]
- Mulder, E.; Basit, S.; Oben, J.; van Kuijk, S.; Ghossein-Doha, C.; Spaanderman, M. Accuracy and precision of USCOM versus transthoracic echocardiography before and during pregnancy. Pregnancy Hypertens. 2019, 17, 138–143. [Google Scholar] [CrossRef]
- Van den Oever, H.L.; Murphy, E.J.; Christie-Taylor, G.A. USCOM (Ultrasonic Cardiac Output Monitors) lacks agreement with thermodilution cardiac output and transoesophageal echocardiography valve measurements. Anaesth. Intensive Care 2007, 35, 903–910. [Google Scholar] [CrossRef]
- Nguyen, H.B.; Banta, D.P.; Stewart, G.; Kim, T.; Bansal, R.; Anholm, J.; Wittlake, W.A.; Corbett, S.W. Cardiac index measurements by transcutaneous Doppler ultrasound and transthoracic echocardiography in adult and pediatric emergency patients. J. Clin. Monit. Comput. 2010, 24, 237–247. [Google Scholar] [CrossRef]
- Nguyen, H.B.; Losey, T.; Rasmussen, J.; Oliver, R.; Guptill, M.; Wittlake, W.A.; Corbett, S.W. Interrater reliability of cardiac output measurements by transcutaneous Doppler ultrasound: Implications for noninvasive hemodynamic monitoring in the ED. Am. J. Emerg. Med. 2006, 24, 828–835. [Google Scholar] [CrossRef] [PubMed]
- Dark, P.M.; Singer, M. The validity of trans-esophageal Doppler ultrasonography as a measure of cardiac output in critically ill adults. Intensive Care Med. 2004, 30, 2060–2066. [Google Scholar] [CrossRef] [PubMed]
- Monnet, X.; Rienzo, M.; Osman, D.; Anguel, N.; Richard, C.; Pinsky, M.R.; Teboul, J.L. Esophageal Doppler monitoring predicts fluid responsiveness in critically ill ventilated patients. Intensive Care Med. 2005, 31, 1195–1201. [Google Scholar] [CrossRef] [PubMed]
- Levy, M.M.; Evans, L.E.; Rhodes, A. The Surviving Sepsis Campaign Bundle: 2018 Update. Intensive Care Med. 2018, 44, 925–928. [Google Scholar] [CrossRef]
- Yancy, C.W.; Jessup, M.; Bozkurt, B.; Butler, J.; Casey, D.E., Jr.; Drazner, M.H.; Fonarow, G.C.; Geraci, S.A.; Horwich, T.; Januzzi, J.L.; et al. 2013 ACCF/AHA guideline for the management of heart failure: A report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. J. Am. Coll. Cardiol. 2013, 62, e147–e239. [Google Scholar] [CrossRef]
- Lindenfeld, J.; Abraham, W.T.; Maisel, A.; Zile, M.; Smart, F.; Costanzo, M.R.; Mehra, M.R.; Ducharme, A.; Sears, S.F.; Desai, A.S.; et al. Hemodynamic-GUIDEd Management of Heart Failure (GUIDE-HF). Am. Heart J. 2019, 214, 18–27. [Google Scholar] [CrossRef]
- Asfar, P.; Meziani, F.; Hamel, J.F.; Grelon, F.; Megarbane, B.; Anguel, N.; Mira, J.P.; Dequin, P.F.; Gergaud, S.; Weiss, N.; et al. High versus low blood-pressure target in patients with septic shock. N. Engl. J. Med. 2014, 370, 1583–1593. [Google Scholar] [CrossRef] [PubMed]
- Jakkula, P.; Pettila, V.; Skrifvars, M.B.; Hastbacka, J.; Loisa, P.; Tiainen, M.; Wilkman, E.; Toppila, J.; Koskue, T.; Bendel, S.; et al. Targeting low-normal or high-normal mean arterial pressure after cardiac arrest and resuscitation: A randomised pilot trial. Intensive Care Med. 2018, 44, 2091–2101. [Google Scholar] [CrossRef]
- Cattermole, G.N.; Leung, P.Y.; Ho, G.Y.; Lau, P.W.; Chan, C.P.; Chan, S.S.; Smith, B.E.; Graham, C.A.; Rainer, T.H. The normal ranges of cardiovascular parameters measured using the ultrasonic cardiac output monitor. Physiol. Rep. 2017, 5, e13195. [Google Scholar] [CrossRef] [PubMed]
- Rosenthal, G.; Hemphill, J.C., 3rd; Sorani, M.; Martin, C.; Morabito, D.; Obrist, W.D.; Manley, G.T. Brain tissue oxygen tension is more indicative of oxygen diffusion than oxygen delivery and metabolism in patients with traumatic brain injury. Crit. Care Med. 2008, 36, 1917–1924. [Google Scholar] [CrossRef]
- Helmerhorst, H.J.; Arts, D.L.; Schultz, M.J.; van der Voort, P.H.; Abu-Hanna, A.; de Jonge, E.; van Westerloo, D.J. Metrics of Arterial Hyperoxia and Associated Outcomes in Critical Care. Crit. Care Med. 2017, 45, 187–195. [Google Scholar] [CrossRef] [PubMed]
- ICU-ROX Investigators and the Australian and New Zealand Intensive Care Society Clinical Trials Group; Mackle, D.; Bellomo, R.; Bailey, M.; Beasley, R.; Deane, A.; Eastwood, G.; Finfer, S.; Freebairn, R.; King, V.; et al. Conservative Oxygen Therapy during Mechanical Ventilation in the ICU. N. Engl. J. Med. 2020, 382, 989–998. [Google Scholar] [CrossRef]
- Chu, D.K.; Kim, L.H.; Young, P.J.; Zamiri, N.; Almenawer, S.A.; Jaeschke, R.; Szczeklik, W.; Schunemann, H.J.; Neary, J.D.; Alhazzani, W. Mortality and morbidity in acutely ill adults treated with liberal versus conservative oxygen therapy (IOTA): A systematic review and meta-analysis. Lancet 2018, 391, 1693–1705. [Google Scholar] [CrossRef]
- Siemieniuk, R.A.C.; Chu, D.K.; Kim, L.H.; Guell-Rous, M.R.; Alhazzani, W.; Soccal, P.M.; Karanicolas, P.J.; Farhoumand, P.D.; Siemieniuk, J.L.K.; Satia, I.; et al. Oxygen therapy for acutely ill medical patients: A clinical practice guideline. BMJ 2018, 363, k4169. [Google Scholar] [CrossRef]
- Hebert, P.C.; Transfusion Requirements in Critical Care Investigators and the Canadian Critical Care Trials Group. Transfusion requirements in critical care (TRICC): A multicentre, randomized, controlled clinical study. Br. J. Anaesth. 1998, 81 (Suppl. 1), 25–33. [Google Scholar]
- Holst, L.B.; Haase, N.; Wetterslev, J.; Wernerman, J.; Aneman, A.; Guttormsen, A.B.; Johansson, P.I.; Karlsson, S.; Klemenzson, G.; Winding, R.; et al. Transfusion requirements in septic shock (TRISS) trial—Comparing the effects and safety of liberal versus restrictive red blood cell transfusion in septic shock patients in the ICU: Protocol for a randomised controlled trial. Trials 2013, 14, 150. [Google Scholar] [CrossRef] [PubMed]
- Roberson, R.S.; Bennett-Guerrero, E. Impact of red blood cell transfusion on global and regional measures of oxygenation. Mt. Sinai J. Med. 2012, 79, 66–74. [Google Scholar] [CrossRef] [PubMed]
- Reinhart, K.; Kuhn, H.J.; Hartog, C.; Bredle, D.L. Continuous central venous and pulmonary artery oxygen saturation monitoring in the critically ill. Intensive Care Med. 2004, 30, 1572–1578. [Google Scholar] [CrossRef] [PubMed]
- Hayden, R.A. What keeps oxygenation on track? Am. J. Nurs. 1992, 92, 32–40. [Google Scholar] [CrossRef] [PubMed]
- Van Beest, P.; Wietasch, G.; Scheeren, T.; Spronk, P.; Kuiper, M. Clinical review: Use of venous oxygen saturations as a goal—A yet unfinished puzzle. Crit. Care 2011, 15, 232. [Google Scholar] [CrossRef] [PubMed]
- Crowell, J.W.; Smith, E.E. Oxygen Deficit and Irreversible Hemorrhagic Shock. Am. J. Physiol. 1964, 206, 313–316. [Google Scholar] [CrossRef]
- Barbee, R.W.; Reynolds, P.S.; Ward, K.R. Assessing shock resuscitation strategies by oxygen debt repayment. Shock 2010, 33, 113–122. [Google Scholar] [CrossRef]
- Joshi, R.; de Witt, B.; Mosier, J.M. Optimizing oxygen delivery in the critically ill: The utility of lactate and central venous oxygen saturation (ScvO2) as a roadmap of resuscitation in shock. J. Emerg. Med. 2014, 47, 493–500. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, H.B.; Rivers, E.P.; Knoblich, B.P.; Jacobsen, G.; Muzzin, A.; Ressler, J.A.; Tomlanovich, M.C. Early lactate clearance is associated with improved outcome in severe sepsis and septic shock. Crit. Care Med. 2004, 32, 1637–1642. [Google Scholar] [CrossRef]
- Dugas, A.F.; Mackenhauer, J.; Salciccioli, J.D.; Cocchi, M.N.; Gautam, S.; Donnino, M.W. Prevalence and characteristics of nonlactate and lactate expressors in septic shock. J. Crit. Care 2012, 27, 344–350. [Google Scholar] [CrossRef]
- Wacharasint, P.; Nakada, T.A.; Boyd, J.H.; Russell, J.A.; Walley, K.R. Normal-range blood lactate concentration in septic shock is prognostic and predictive. Shock 2012, 38, 4–10. [Google Scholar] [CrossRef]
- Permpikul, C.; Tongyoo, S.; Viarasilpa, T.; Trainarongsakul, T.; Chakorn, T.; Udompanturak, S. Early Use of Norepinephrine in Septic Shock Resuscitation (CENSER). A Randomized Trial. Am. J. Respir. Crit. Care Med. 2019, 199, 1097–1105. [Google Scholar] [CrossRef]
- Myles, P.S.; Bellomo, R.; Corcoran, T.; Forbes, A.; Peyton, P.; Story, D.; Christophi, C.; Leslie, K.; McGuinness, S.; Parke, R.; et al. Restrictive Versus Liberal Fluid Therapy for Major Abdominal Surgery. N. Engl. J. Med. 2018, 378, 2263–2274. [Google Scholar] [CrossRef]
- Self, W.H.; Semler, M.W.; Bellomo, R.; Brown, S.M.; deBoisblanc, B.P.; Exline, M.C.; Ginde, A.A.; Grissom, C.K.; Janz, D.R.; Jones, A.E.; et al. Liberal Versus Restrictive Intravenous Fluid Therapy for Early Septic Shock: Rationale for a Randomized Trial. Ann. Emerg. Med. 2018, 72, 457–466. [Google Scholar] [CrossRef] [PubMed]
- Rivers, E.; Nguyen, B.; Havstad, S.; Ressler, J.; Muzzin, A.; Knoblich, B.; Peterson, E.; Tomlanovich, M.; For the Early Goal-Directed Therapy Collaborative Group. Early goal-directed therapy in the treatment of severe sepsis and septic shock. N. Engl. J. Med. 2001, 345, 1368–1377. [Google Scholar] [CrossRef] [PubMed]
- Yealy, D.M.; Kellum, J.A.; Huang, D.T.; Barnato, A.E.; Weissfeld, L.A.; Pike, F.; Terndrup, T.; Wang, H.E.; Hou, P.C.; LoVecchio, F.; et al. ProCESS: A randomized trial of protocol-based care for early septic shock. N. Engl. J. Med. 2014, 370, 1683–1693. [Google Scholar] [CrossRef] [PubMed]
- Peake, S.L.; Delaney, A.; Bailey, M.; Bellomo, R.; Cameron, P.A.; Cooper, D.J.; Higgins, A.M.; Holdgate, A.; Howe, B.D.; Webb, S.A.; et al. Goal-directed resuscitation for patients with early septic shock. N. Engl. J. Med. 2014, 371, 1496–1506. [Google Scholar] [CrossRef] [PubMed]
- Mouncey, P.R.; Osborn, T.M.; Power, G.S.; Harrison, D.A.; Sadique, M.Z.; Grieve, R.D.; Jahan, R.; Harvey, S.E.; Bell, D.; Bion, J.F.; et al. Trial of early, goal-directed resuscitation for septic shock. N. Engl. J. Med. 2015, 372, 1301–1311. [Google Scholar] [CrossRef]
- Nguyen, H.B.; Jaehne, A.K.; Jayaprakash, N.; Semler, M.W.; Hegab, S.; Yataco, A.C.; Tatem, G.; Salem, D.; Moore, S.; Boka, K.; et al. Early goal-directed therapy in severe sepsis and septic shock: Insights and comparisons to ProCESS, ProMISe, and ARISE. Crit. Care 2016, 20, 160. [Google Scholar] [CrossRef]
- The PRISM Investigators; Rowan, K.M.; Angus, D.C.; Bailey, M.; Barnato, A.E.; Bellomo, R.; Canter, R.R.; Coats, T.J.; Delaney, A.; Gimbel, E.; et al. Early, Goal-Directed Therapy for Septic Shock—A Patient-Level Meta-Analysis. N. Engl. J. Med. 2017, 376, 2223–2234. [Google Scholar] [CrossRef]
- Protti, A.; Masson, S.; Latini, R.; Fumagalli, R.; Romero, M.; Pessina, C.; Pasetti, G.; Tognoni, G.; Pesenti, A.; Gattinoni, L.; et al. Persistence of Central Venous Oxygen Desaturation during Early Sepsis Is Associated with Higher Mortality: A Retrospective Analysis of the ALBIOS Trial. Chest 2018, 154, 1291–1300. [Google Scholar] [CrossRef]
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Russell, A.; Rivers, E.P.; Giri, P.C.; Jaehne, A.K.; Nguyen, H.B. A Physiologic Approach to Hemodynamic Monitoring and Optimizing Oxygen Delivery in Shock Resuscitation. J. Clin. Med. 2020, 9, 2052. https://doi.org/10.3390/jcm9072052
Russell A, Rivers EP, Giri PC, Jaehne AK, Nguyen HB. A Physiologic Approach to Hemodynamic Monitoring and Optimizing Oxygen Delivery in Shock Resuscitation. Journal of Clinical Medicine. 2020; 9(7):2052. https://doi.org/10.3390/jcm9072052
Chicago/Turabian StyleRussell, Amy, Emanuel P. Rivers, Paresh C. Giri, Anja K. Jaehne, and H. Bryant Nguyen. 2020. "A Physiologic Approach to Hemodynamic Monitoring and Optimizing Oxygen Delivery in Shock Resuscitation" Journal of Clinical Medicine 9, no. 7: 2052. https://doi.org/10.3390/jcm9072052
APA StyleRussell, A., Rivers, E. P., Giri, P. C., Jaehne, A. K., & Nguyen, H. B. (2020). A Physiologic Approach to Hemodynamic Monitoring and Optimizing Oxygen Delivery in Shock Resuscitation. Journal of Clinical Medicine, 9(7), 2052. https://doi.org/10.3390/jcm9072052




