A Systematic Review of COVID-19 Epidemiology Based on Current Evidence
Abstract
1. Introduction
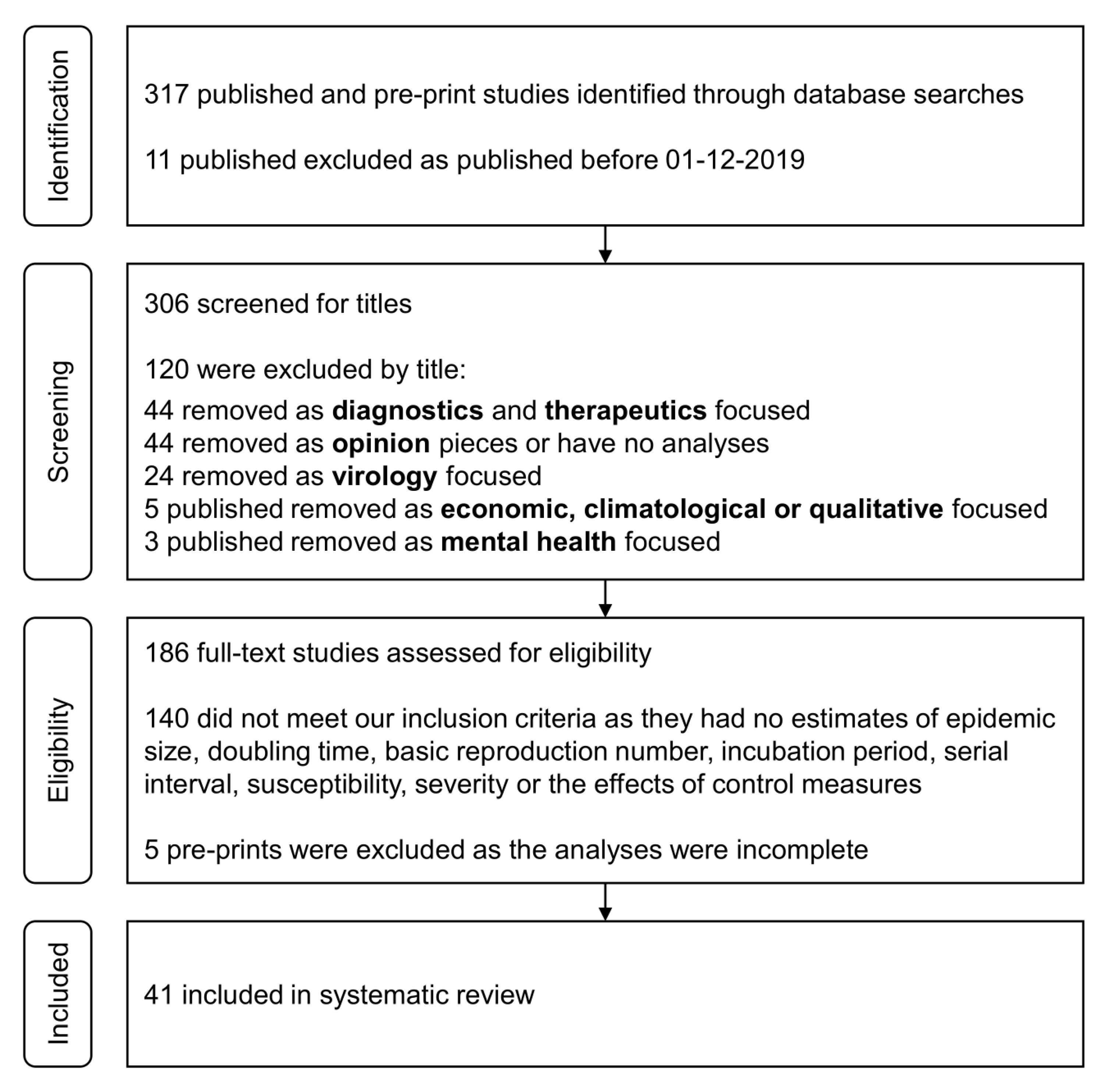
2. Materials and Methods
2.1. Inclusion Criteria
2.2. Literature Search
2.3. Additional Analysis
3. Results
3.1. Size of the Outbreak at Epicentre
3.2. Transmissibility of SARS-CoV-2
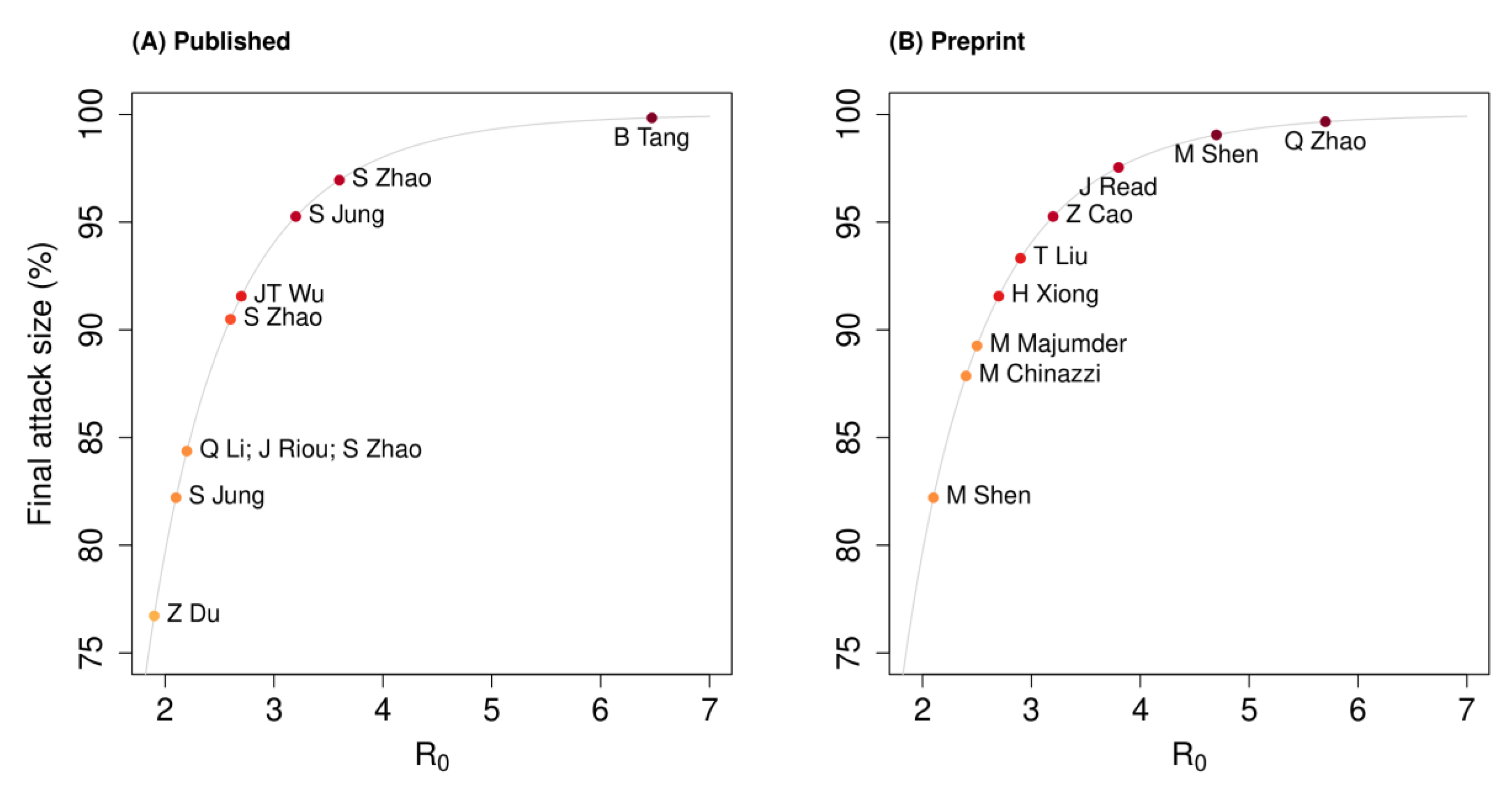
3.2.1. Basic Reproduction Number ()
3.2.2. Incubation Period
3.2.3. Serial Interval
3.3. Susceptibility
3.4. Severity
3.4.1. Descriptive Analysis
3.4.2. Modeling Studies: Estimates for China
3.4.3. Modeling Studies: Estimates for Outside China
3.5. Control Measures
3.5.1. Travel Restrictions
3.5.2. Non-Pharmaceutical Interventions and Quarantine
3.5.3. Airport Screening
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- BNO Tracking Coronavirus: Map, Data and Timeline. Available online: https://bnonews.com/index.php/2020/02/the-latest-coronavirus-cases/ (accessed on 18 March 2020).
- Guan, W.J.; Ni, Z.Y.; Hu, Y.; Liang, W.H.; Ou, C.Q.; He, J.X.; Liu, L.; Shan, H.; Lei, C.L.; Hui, D.S.C.; et al. Clinical Characteristics of Coronavirus Disease 2019 in China. N. Engl. J. Med. 2020. [Google Scholar] [CrossRef] [PubMed]
- Bai, Y.; Yao, L.; Wei, T.; Tian, F.; Jin, D.Y.; Chen, L.; Wang, M. Presumed Asymptomatic Carrier Transmission of COVID-19. JAMA 2020. [Google Scholar] [CrossRef] [PubMed]
- Chen, N.; Zhou, M.; Dong, X.; Qu, J.; Gong, F.; Han, Y.; Qiu, Y.; Wang, J.; Liu, Y.; Wei, Y.; et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: A descriptive study. Lancet 2020, 395, 507–513. [Google Scholar] [CrossRef]
- Cowling, B.J.; Leung, G.M. Epidemiological research priorities for public health control of the ongoing global novel coronavirus (2019-nCoV) outbreak. Euro Surveill. 2020, 25. [Google Scholar] [CrossRef] [PubMed]
- Kretzschmar, M. Measurement and Modeling: Infectious Disease Modeling. In International Encyclopedia of Public Health; Academic Press: Cambridge, MA, USA, 2017; pp. 579–585. ISBN 978-0-12-803708-9. [Google Scholar]
- Du, Z.; Wang, L.; Cauchemez, S.; Xu, X.; Wang, X.; Cowling, B.J.; Meyers, L.A. Risk for Transportation of 2019 Novel Coronavirus Disease from Wuhan to Other Cities in China. Emerg. Infect. Dis. 2020, 26. [Google Scholar] [CrossRef]
- Wu, J.T.; Leung, K.; Leung, G.M. Nowcasting and forecasting the potential domestic and international spread of the 2019-nCoV outbreak originating in Wuhan, China: A modelling study. Lancet 2020. [Google Scholar] [CrossRef]
- Nishiura, H.; Kobayashi, T.; Yang, Y.; Hayashi, K.; Miyama, T.; Kinoshita, R.; Linton, N.M.; Jung, S.M.; Yuan, B.; Suzuki, A.; et al. The Rate of Underascertainment of Novel Coronavirus (2019-nCoV) Infection: Estimation Using Japanese Passengers Data on Evacuation Flights. J. Clin. Med. 2020, 9, 419. [Google Scholar] [CrossRef]
- Li, Q.; Guan, X.; Wu, P.; Wang, X.; Zhou, L.; Tong, Y.; Ren, R.; Leung, K.S.M.; Lau, E.H.Y.; Wong, J.Y.; et al. Early Transmission Dynamics in Wuhan, China, of Novel Coronavirus-Infected Pneumonia. N. Engl. J. Med. 2020. [Google Scholar] [CrossRef]
- Cao, Z.; Zhang, Q.; Lu, X.; Pfeiffer, D.; Wang, L.; Song, H.; Pei, T.; Jia, Z.; Zeng, D.D. Incorporating Human Movement Data to Improve Epidemiological Estimates for 2019-nCoV. medRxiv 2020. [Google Scholar] [CrossRef]
- Chinazzi, M.; Davis, J.T.; Ajelli, M.; Gioannini, C.; Litvinova, M.; Merler, S.; Pastore y Piontti, A.; Rossi, L.; Sun, K.; Viboud, C.; et al. The effect of travel restrictions on the spread of the 2019 novel coronavirus (2019-nCoV) outbreak. medRxiv 2020. [Google Scholar] [CrossRef]
- Xiong, H.; Yan, H. Simulating the infected population and spread trend of 2019-nCov under different policy by EIR model. medRxiv 2020. [Google Scholar] [CrossRef]
- Zhao, Q.; Chen, Y.; Small, D.S. Analysis of the epidemic growth of the early 2019-nCoV outbreak using internationally confirmed cases. medRxiv 2020. [Google Scholar] [CrossRef]
- Zhao, S.; Musa, S.S.; Lin, Q.; Ran, J.; Yang, G.; Wang, W.; Lou, Y.; Yang, L.; Gao, D.; He, D.; et al. Estimating the Unreported Number of Novel Coronavirus (2019-nCoV) Cases in China in the First Half of January 2020: A Data-Driven Modelling Analysis of the Early Outbreak. J. Clin. Med. 2020, 9, 388. [Google Scholar] [CrossRef] [PubMed]
- Zhao, S.; Lin, Q.; Ran, J.; Musa, S.S.; Yang, G.; Wang, W.; Lou, Y.; Gao, D.; Yang, L.; He, D.; et al. Preliminary estimation of the basic reproduction number of novel coronavirus (2019-nCoV) in China, from 2019 to 2020: A data-driven analysis in the early phase of the outbreak. Int. J. Infect. Dis. 2020, 92, 214–217. [Google Scholar] [CrossRef] [PubMed]
- Riou, J.; Althaus, C.L. Pattern of early human-to-human transmission of Wuhan 2019 novel coronavirus (2019-nCoV), December 2019 to January 2020. Euro Surveill. 2020, 25. [Google Scholar] [CrossRef]
- Tang, B.; Wang, X.; Li, Q.; Bragazzi, N.L.; Tang, S.; Xiao, Y.; Wu, J. Estimation of the Transmission Risk of the 2019-nCoV and Its Implication for Public Health Interventions. J. Clin. Med. 2020, 9, 462. [Google Scholar] [CrossRef]
- Jung, S.M.; Akhmetzhanov, A.R.; Hayashi, K.; Linton, N.M.; Yang, Y.; Yuan, B.; Kobayashi, T.; Kinoshita, R.; Nishiura, H. Real-Time Estimation of the Risk of Death from Novel Coronavirus (COVID-19) Infection: Inference Using Exported Cases. J. Clin. Med. 2020, 9, 523. [Google Scholar] [CrossRef]
- Shen, M.; Peng, Z.; Xiao, Y.; Zhang, L. Modelling the epidemic trend of the 2019 novel coronavirus outbreak in China. bioRxiv 2020. [Google Scholar] [CrossRef]
- Read, J.M.; Bridgen, J.R.E.; Cummings, D.A.T.; Ho, A.; Jewell, C.P. Novel coronavirus 2019-nCoV: Early estimation of epidemiological parameters and epidemic predictions. medRxiv 2020. [Google Scholar] [CrossRef]
- Liu, T.; Hu, J.; Kang, M.; Lin, L.; Zhong, H.; Xiao, J.; He, G.; Song, T.; Huang, Q.; Rong, Z.; et al. Transmission dynamics of 2019 novel coronavirus (2019-nCoV). bioRxiv 2020. [Google Scholar] [CrossRef]
- Majumder, M.; Mandl, K.D. Early Transmissibility Assessment of a Novel Coronavirus in Wuhan, China (January 26, 2020). SSRN 2020. [Google Scholar] [CrossRef]
- Riley, S.; Fraser, C.; Donnelly, C.A.; Ghani, A.C.; Abu-Raddad, L.J.; Hedley, A.J.; Leung, G.M.; Ho, L.M.; Lam, T.H.; Thach, T.Q.; et al. Transmission dynamics of the etiological agent of SARS in Hong Kong: Impact of public health interventions. Science 2003, 300, 1961–1966. [Google Scholar] [CrossRef] [PubMed]
- Lipsitch, M.; Cohen, T.; Cooper, B.; Robins, J.M.; Ma, S.; James, L.; Gopalakrishna, G.; Chew, S.K.; Tan, C.C.; Samore, M.H.; et al. Transmission dynamics and control of severe acute respiratory syndrome. Science 2003, 300, 1966–1970. [Google Scholar] [CrossRef] [PubMed]
- Cauchemez, S.; Fraser, C.; Van Kerkhove, M.D.; Donnelly, C.A.; Riley, S.; Rambaut, A.; Enouf, V.; van der Werf, S.; Ferguson, N.M. Middle East respiratory syndrome coronavirus: Quantification of the extent of the epidemic, surveillance biases, and transmissibility. Lancet Infect. Dis. 2014, 14, 50–56. [Google Scholar] [CrossRef]
- Backer, J.A.; Klinkenberg, D.; Wallinga, J. Incubation period of 2019 novel coronavirus (2019-nCoV) infections among travellers from Wuhan, China, 20-28 January 2020. Euro Surveill. 2020, 25. [Google Scholar] [CrossRef]
- Linton, N.M.; Kobayashi, T.; Yang, Y.; Hayashi, K.; Akhmetzhanov, A.R.; Jung, S.M.; Yuan, B.; Kinoshita, R.; Nishiura, H. Incubation Period and Other Epidemiological Characteristics of 2019 Novel Coronavirus Infections with Right Truncation: A Statistical Analysis of Publicly Available Case Data. J. Clin. Med. 2020, 9, 538. [Google Scholar] [CrossRef]
- Ki, M.; Task Force for 2019-nCoV. Epidemiologic characteristics of early cases with 2019 novel coronavirus (2019-nCoV) disease in Republic of Korea. Epidemiol. Health 2020, e2020007. [Google Scholar] [CrossRef]
- Jiang, X.; Rayner, S.; Luo, M.H. Does SARS-CoV-2 has a longer incubation period than SARS and MERS? J. Med. Virol. 2020. [Google Scholar] [CrossRef]
- Lauer, S.A.; Grantz, K.H.; Bi, Q.; Jones, F.K.; Zheng, Q.; Meredith, H.; Azman, A.S.; Reich, N.G.; Lessler, J. The incubation period of 2019-nCoV from publicly reported confirmed cases: Estimation and application. medRxiv 2020. [Google Scholar] [CrossRef]
- Zhang, J.; Litvinova, M.; Wang, W.; Wang, Y.; Deng, X.; Chen, X.; Li, M.; Zheng, W.; Yi, L.; Chen, X.; et al. Evolving epidemiology of novel coronavirus diseases 2019 and possible interruption of local transmission outside Hubei Province in China: A descriptive and modeling study. medRxiv 2020. [Google Scholar] [CrossRef]
- Lau, E.H.; Hsiung, C.A.; Cowling, B.J.; Chen, C.H.; Ho, L.M.; Tsang, T.; Chang, C.W.; Donnelly, C.A.; Leung, G.M. A comparative epidemiologic analysis of SARS in Hong Kong, Beijing and Taiwan. BMC Infect. Dis. 2010, 10, 50. [Google Scholar] [CrossRef]
- Cowling, B.J.; Park, M.; Fang, V.J.; Wu, P.; Leung, G.M.; Wu, J.T. Preliminary epidemiological assessment of MERS-CoV outbreak in South Korea, May to June 2015. Euro Surveill. 2015, 20, 7–13. [Google Scholar] [CrossRef] [PubMed]
- Du, Z.; Wang, L.; Xu, X.; Wu, Y.; Cowling, B.J.; Meyers, L.A. The serial interval of COVID-19 from publicly reported confirmed cases. medRxiv 2020. [Google Scholar] [CrossRef]
- Nishiura, H.; Linton, N.M.; Akhmetzhanov, A.R. Serial interval of novel coronavirus (2019-nCoV) infections. medRxiv 2020. [Google Scholar] [CrossRef]
- Zhao, S.; Gao, D.; Zhuang, Z.; Chong, M.; Cai, Y.; Ran, J.; Cao, P.; Wang, K.; Lou, Y.; Wang, W.; et al. Estimating the serial interval of the novel coronavirus disease (COVID-19): A statistical analysis using the public data in Hong Kong from January 16 to February 15, 2020. medRxiv 2020. [Google Scholar] [CrossRef]
- Assiri, A.; McGeer, A.; Perl, T.M.; Price, C.S.; Al Rabeeah, A.A.; Cummings, D.A.; Alabdullatif, Z.N.; Assad, M.; Almulhim, A.; Makhdoom, H.; et al. Hospital outbreak of Middle East respiratory syndrome coronavirus. N. Engl. J. Med. 2013, 369, 407–416. [Google Scholar] [CrossRef]
- Wu, Z.; McGoogan, J.M. Characteristics of and Important Lessons from the Coronavirus Disease 2019 (COVID-19) Outbreak in China: Summary of a Report of 72314 Cases from the Chinese Center for Disease Control and Prevention. JAMA 2020. [Google Scholar] [CrossRef]
- Chen, H.; Guo, J.; Wang, C.; Luo, F.; Yu, X.; Zhang, W.; Li, J.; Zhao, D.; Xu, D.; Gong, Q.; et al. Clinical characteristics and intrauterine vertical transmission potential of COVID-19 infection in nine pregnant women: A retrospective review of medical records. Lancet 2020. [Google Scholar] [CrossRef]
- Zhu, H.; Wang, L.; Fang, Z.; Peng, S.; Zhang, L.; Chang, G.; Xia, S.; Zhou, W. Clinical analysis of 10 neonates born to mothers with 2019-nCoV pneumonia. Transl. Pediatr. 2020, 9, 51–60. [Google Scholar] [CrossRef]
- Huang, C.; Wang, Y.; Li, X.; Ren, L.; Zhao, J.; Hu, Y.; Zhang, L.; Fan, G.; Xu, J.; Gu, X.; et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 2020, 395, 497–506. [Google Scholar] [CrossRef]
- WHO. Summary of Probable SARS Cases with Onset of Illness from 1 November 2002 to 31 July 2003. Available online: https://www.who.int/csr/sars/country/table2004_04_21/en/ (accessed on 1 March 2020).
- WHO. Middle East Respiratory Syndrome Coronavirus (MERS-CoV). Available online: https://www.who.int/emergencies/mers-cov/en/ (accessed on 1 March 2020).
- Chen, Z.M.; Fu, J.F.; Shu, Q.; Chen, Y.H.; Hua, C.Z.; Li, F.B.; Lin, R.; Tang, L.F.; Wang, T.L.; Wang, W.; et al. Diagnosis and treatment recommendations for pediatric respiratory infection caused by the 2019 novel coronavirus. World J. Pediatr. 2020. [Google Scholar] [CrossRef]
- Wang, X.; Ma, Z.; Ning, Y.; Chen, C.; Chen, R.; Chen, Q.; Zhang, H.; Li, C.; He, Y.; Wang, T.; et al. Estimating the case fatality ratio of the COVID-19 epidemic in China. medRxiv 2020. [Google Scholar] [CrossRef]
- Mizumoto, K.; Kagaya, K.; Chowell, G. Early epidemiological assessment of the transmission potential and virulence of 2019 Novel Coronavirus in Wuhan City: China, 2019-2020. medRxiv 2020. [Google Scholar] [CrossRef]
- Wilson, N.; Kvalsvig, A.; Telfar Barnard, L.; Baker, M.G. Estimating the Case Fatality Risk of COVID-19 using Cases from Outside China. medRxiv 2020. [Google Scholar] [CrossRef]
- Mizumoto, K.; Kagaya, K.; Zarebski, A.; Chowell, G. Estimating the asymptomatic proportion of coronavirus disease 2019 (COVID-19) cases on board the Diamond Princess cruise ship, Yokohama, Japan, 2020. Eurosurveillance 2020, 25. [Google Scholar] [CrossRef] [PubMed]
- Tian, H.; Liu, Y.; Li, Y.; Kraemer, M.U.G.; Chen, B.; Wu, C.-H.; Cai, J.; Li, B.; Xu, B.; Yang, Q.; et al. Early evaluation of transmission control measures in response to the 2019 novel coronavirus outbreak in China. medRxiv 2020. [Google Scholar] [CrossRef]
- Koo, J.R.; Cook, A.R.; Park, M.; Sun, Y.; Sun, H.; Lim, J.T.; Tam, C.; Dickens, B.L. Interventions to mitigate early spread of SARS-CoV-2 in Singapore: A modelling study. Lancet Infect Dis 2020. [Google Scholar] [CrossRef]
- Quilty, B.J.; Clifford, S.; Flasche, S.; Eggo, R.M. Effectiveness of airport screening at detecting travellers infected with novel coronavirus (2019-nCoV). Euro Surveill. 2020, 25. [Google Scholar] [CrossRef]
- Gostic, K.; Gomez, A.C.R.; Mummah, R.O.; Kucharski, A.J.; Lloyd-Smith, J.O. Estimated effectiveness of traveller screening to prevent international spread of 2019 novel coronavirus (2019-nCoV). medRxiv 2020. [Google Scholar] [CrossRef]
| Author | Data | Estimates | Estimation Period | Doubling Time |
|---|---|---|---|---|
| Published (2020) | ||||
| Du et al. [7] | Number of confirmed cases outside China and travel data | 12,400 in Wuhan | By 22 Jan 2020 | 7.31 days |
| Wu et al. [8] | Number of confirmed cases outside China and travel data | 75,815 in Wuhan | By 25 Jan 2020 | 6.4 days |
| Nishiura et al. [9] | Proportion of asymptomatic cases among Japanese evacuated from Wuhan | 20,767 in Wuhan | By 29 Jan 2020 | - |
| Li et al. [10] | Case reports from Wuhan | - | By 22 Jan 2020 | 7.4 days |
| Preprint | ||||
| Cao et al. [11] | Number of confirmed cases in China and travel data | 18,556 in Wuhan | By 23 Jan 2020 | - |
| Chinazzi et al. [12] | Number of confirmed cases outside China and travel data | 58,956 in Wuhan | By 23 Jan 2020 | 4.6 days |
| Xiong et al. [13] | Number of confirmed cases in China | 49,093 in China | By 16 Feb 2020 | - |
| Q. Zhao et al. [14] | Number of confirmed cases outside China and travel data | − | By 23 Jan 2020 | 2.9 days |
| Author | Method | Estimates | Uncertainty | Estimation Period | |||
|---|---|---|---|---|---|---|---|
| Published (2020) | |||||||
| S. Zhao et al. [15] | Exponential growth model | 2.56 | 2.49 | – | 2.63 | 1–15 Jan 2020 | 95%CI |
| S. Zhao et al. [16] # | Exponential growth model | 2.24 | 1.96 | – | 2.55 | 10–24 Jan 2020 | 95%CI |
| S. Zhao et al. [16] ^ | Exponential growth model | 3.58 | 2.89 | – | 4.39 | 10–24 Jan 2020 | 95%CI |
| Riou et al. [17] | Stochastic simulations of outbreak trajectories | 2.2 | 1.4 | – | 3.8 | By 18 Jan 2020 | 90%HDI * |
| Li et al. [10] | Analysis of epidemiological data | 2.2 | 1.4 | – | 3.9 | By 22 Jan 2020 | 95%CI |
| Tang et al. [18] | SEIR model § | 6.47 | 5.71 | – | 7.23 | By 22 Jan 2020 | 95%CI |
| Du et al. [7] | Hierarchical model | 1.90 | 1.47 | – | 2.59 | By 22 Jan 2020 | 95%CI |
| Jung et al. [19] † | Epidemic growth model | 2.1 | 2 | – | 2.2 | By 24 Jan 2020 | 95%CI |
| Jung et al. [19] ‡ | Epidemic growth model | 3.2 | 2.7 | – | 3.7 | By 24 Jan 2020 | 95%CI |
| Wu et al. [8] | SEIR model | 2.68 | 2.47 | – | 2.86 | By 25 Jan 2020 | 95%CI |
| Preprint | |||||||
| Shen et al. [20] | SEIJR model §§ | 4.71 | 4.5 | – | 4.92 | On 12 Dec 2019 | 95%CI |
| Shen et al. [20] | SEIJR model | 2.08 | 1.99 | – | 2.18 | On 22 Jan 2020 | 95%CI |
| Read et al. [21] | SEIR model | 3.8 | 3.6 | – | 4.0 | By 22 Jan 2020 | 95%CI |
| Liu et al. [22] | Exponential growth model | 2.90 | 2.32 | – | 3.63 | By 23 Jan 2020 | 95%CI |
| Liu et al. [22] | MLE ¶ | 2.92 | 2.28 | – | 3.67 | By 23 Jan 2020 | 95%CI |
| Chinazziet al. [12] | GLEAM ** and SLIR ## | 2.4 | 2.2 | – | 2.6 | By 23 Jan 2020 | 90%CI |
| Q. Zhao et al. [14] | Exponential growth model | 5.7 | 3.4 | – | 9.2 | By 23 Jan 2020 | 95%CI |
| Cao et al. [11] | Geo-stratified debiasing estimation framework | 3.24 | By 23 Jan 2020 | ||||
| Majumder et al. [23] | Incidence Decay and Exponential Adjustment | 2.5 | 2.0 | – | 3.1 | By 26 Jan 2020 | Range |
| Xiong et al. [13] | EIR model (I = Identified) | 2.7 | By 16 Feb 2020 | ||||
| Comparison with SARS-CoV and MERS-CoV | |||||||
| SARS-CoV [24] | Hong Kong (2003) | 2.7 | 2.2 | – | 3.7 | Early phase | 95%CI |
| SARS-CoV [25] | Singapore (2003) | - | 2.2 | – | 3.6 | Early phase | Range |
| MERS-CoV [26] | South Korea (2012-2013) | 0.91 | 0.36 | – | 1.44 | 95%CI | |
| Author | Country/Region | Sample Size | Estimate | Uncertainty | |||
|---|---|---|---|---|---|---|---|
| Published (2020) | |||||||
| Li et al. [10] | Wuhan | 10 cases | 5.2 | 4.1 | – | 7.0 | 95% CI |
| Backer et al. [27] | Outside Wuhan | 88 cases | 6.4 | 5.6 | – | 7.7 | 95% CI |
| Linton et al. [28] | Wuhan | 158 cases | 5.6 | 5.0 | – | 6.3 | 95% CI |
| Linton et al. [28] | Outside Wuhan | 52 cases | 5.0 | 4.2 | – | 6.0 | 95% CI |
| Ki [29] | South Korea | 22 cases | 3.6 | 1.0 | – | 9.0 | Range |
| Jiang et al. [30] | Global | 50 cases | 4.9 | 4.4 | – | 5.5 | 95% CI |
| Guan et al. * [2] | China | 291 cases | 4.0 | 2.0 | – | 7.0 | IQR |
| Preprint | |||||||
| Lauer et al. [31] | Global (excl. Hubei) | 101 cases | 5.2 | 4.4 | – | 6.0 | 95% CI |
| Zhang et al. [32] | China (excl. Hubei) | 49 cases | 5.2 | 1.8 | – | 12.4 | 95% CI |
| Comparison with SARS-CoV and MERS-CoV | |||||||
| SARS-CoV (2003) [33] | Hong Kong | 4.4 | |||||
| MERS-CoV (2012-3) [26] | Global | 5.5 | 3.6 | – | 10.2 | 95% CI | |
| MERS-CoV (2015) [34] | South Korea | 6.7 | 6.1 | – | 7.3 | 95% CI | |
| Author | Country | Sample Size | Estimate | 95% CI | ||
|---|---|---|---|---|---|---|
| Published (2020) | ||||||
| Li et al. [10] | Wuhan | 6 pairs | 7.5 | 5.3 | – | 19.0 |
| Ki [29] | Korea | 7 pairs | 4.6 | 3.0 | – | 9.0 |
| Preprint | ||||||
| Du et al. [35] | China (excl. Hubei) | 468 pairs | 3.96 | 3.53 | – | 4.39 |
| Zhang et al. [32] | China (excl. Hubei) | 35 pairs | 5.1 | 1.3 | – | 11.6 |
| Nishiura et al. [36] | Global | 28 pairs | 4.0 | 3.1 | – | 4.9 |
| Nishiura et al. [36] | Global | 18 pairs | 4.6 | 3.5 | – | 5.9 |
| S. Zhao et al. [37] | Hong Kong | 21 pairs | 4.4 | 2.9 | – | 6.7 |
| Comparison with SARS-CoV and MERS-CoV | ||||||
| SARS-CoV (2003) [25] | Singapore | 8.4 | - | - | ||
| MERS-CoV (2013) [38] | Saudi Arabia | 7.6 | 2.5 | – | 23.1 | |
| MERS-CoV (2015) [34] | South Korea | 12.6 | 12.1 | – | 13.1 | |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Park, M.; Cook, A.R.; Lim, J.T.; Sun, Y.; Dickens, B.L. A Systematic Review of COVID-19 Epidemiology Based on Current Evidence. J. Clin. Med. 2020, 9, 967. https://doi.org/10.3390/jcm9040967
Park M, Cook AR, Lim JT, Sun Y, Dickens BL. A Systematic Review of COVID-19 Epidemiology Based on Current Evidence. Journal of Clinical Medicine. 2020; 9(4):967. https://doi.org/10.3390/jcm9040967
Chicago/Turabian StylePark, Minah, Alex R. Cook, Jue Tao Lim, Yinxiaohe Sun, and Borame L. Dickens. 2020. "A Systematic Review of COVID-19 Epidemiology Based on Current Evidence" Journal of Clinical Medicine 9, no. 4: 967. https://doi.org/10.3390/jcm9040967
APA StylePark, M., Cook, A. R., Lim, J. T., Sun, Y., & Dickens, B. L. (2020). A Systematic Review of COVID-19 Epidemiology Based on Current Evidence. Journal of Clinical Medicine, 9(4), 967. https://doi.org/10.3390/jcm9040967






