Use of Clopidogrel, Prasugrel, or Ticagrelor and Patient Outcome after Acute Coronary Syndrome in Austria from 2015 to 2017
Abstract
1. Introduction
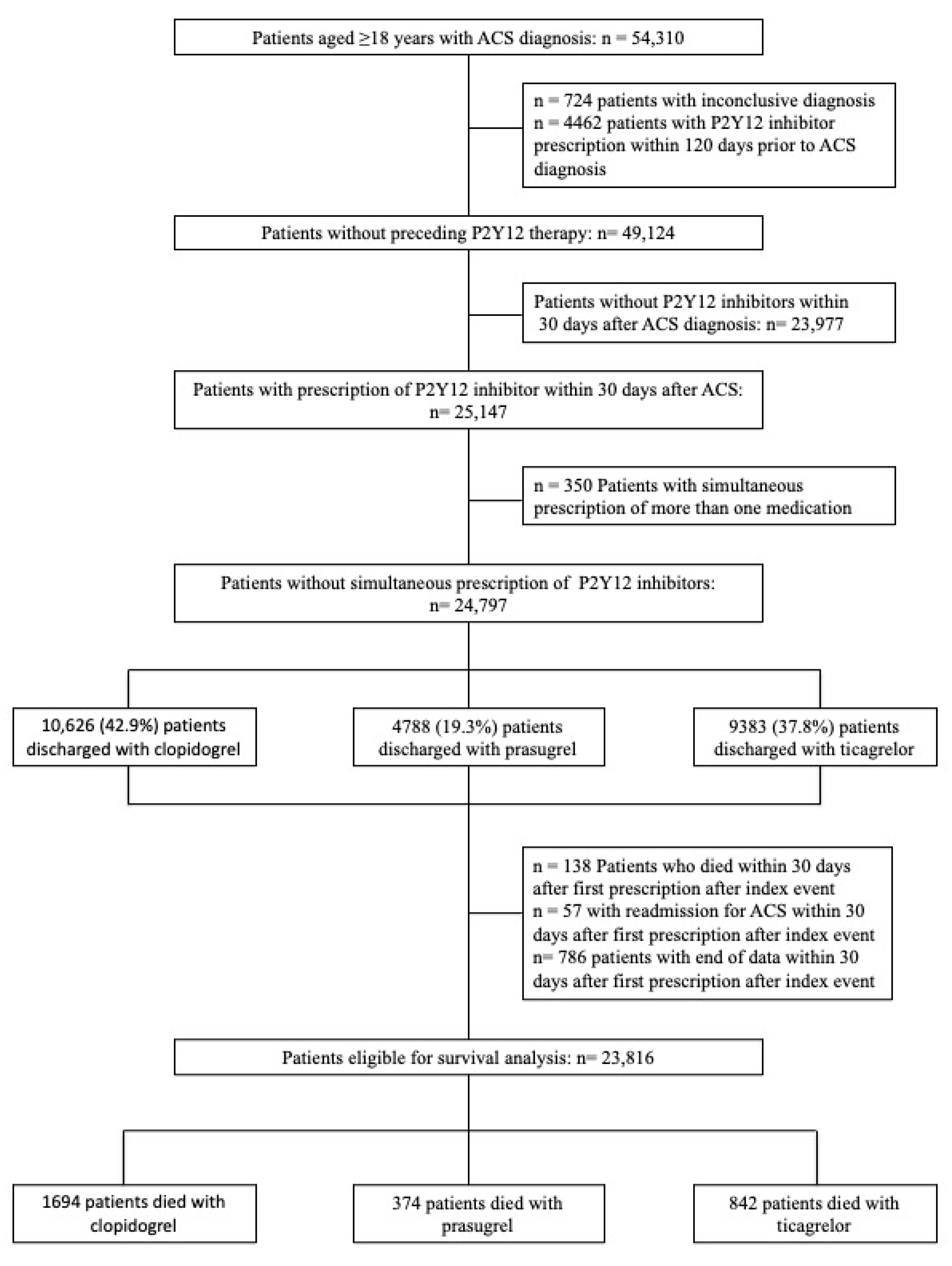
2. Materials and Methods
2.1. Data Preparation
2.2. Statistical Methods
3. Results
3.1. Drug Survival of P2Y12 Inhibitor Therapy
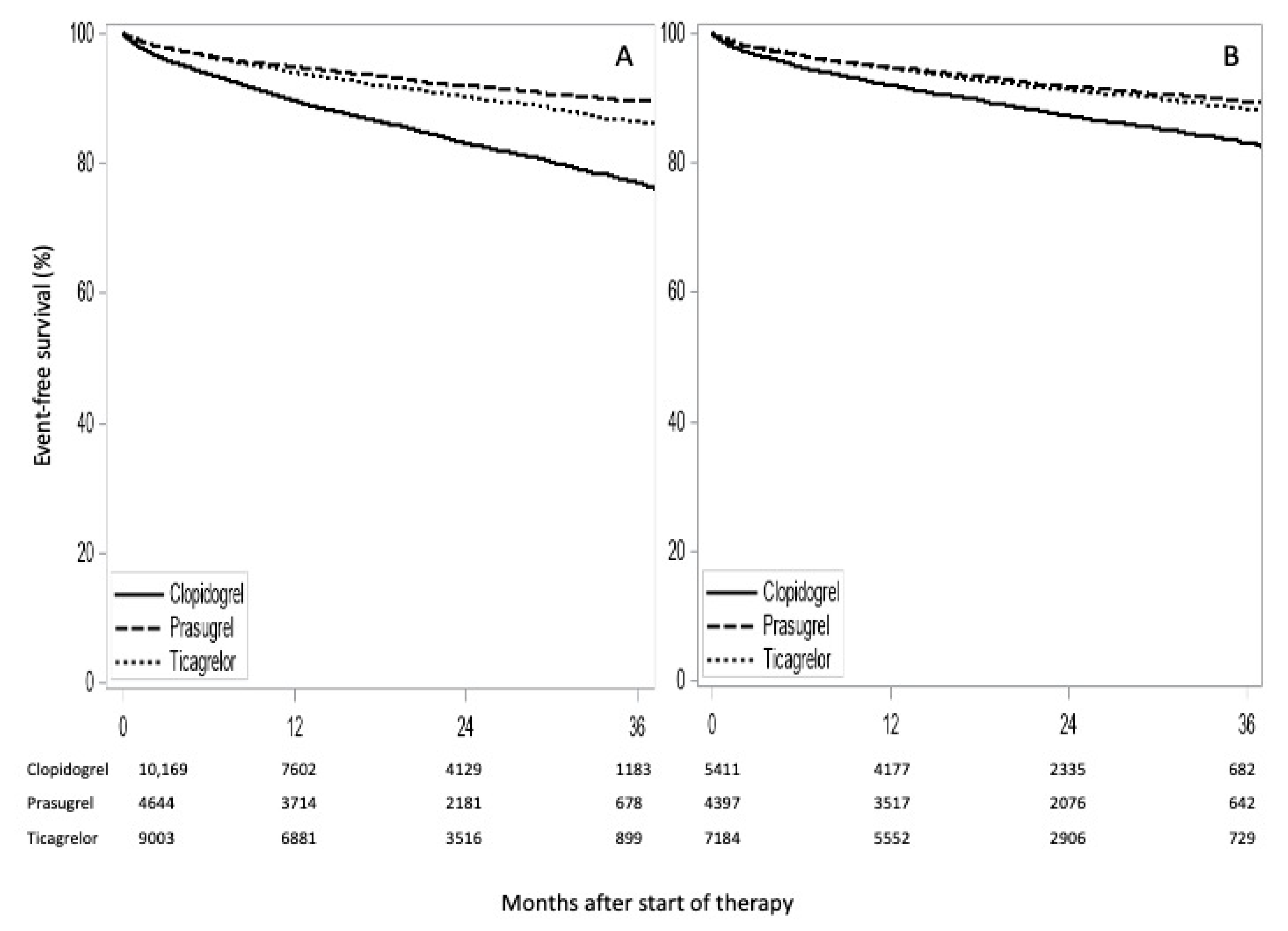
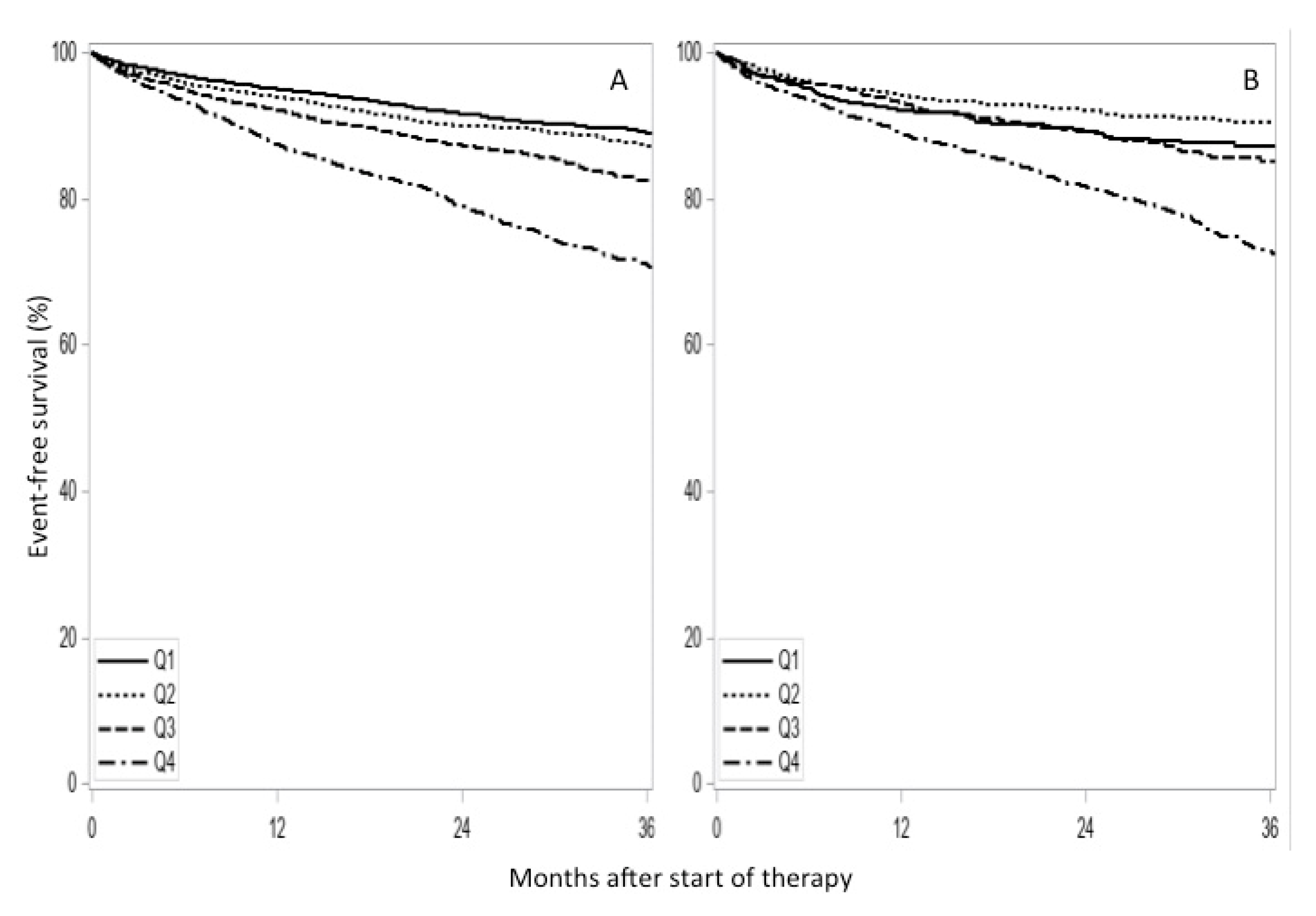
3.2. P2Y12 Inhibitor Therapy and Clinical Outcome
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Tu, J.V.; Naylor, C.D.; Austin, P. Temporal changes in the outcomes of acute myocardial infarction in Ontario, 1992–1996. CMAJ 1999, 161, 1257–1261. [Google Scholar] [PubMed]
- Valgimigli, M.; Bueno, H.; Byrne, R.A.; Collet, J.P.; Costa, F.; Jeppsson, A.; Jüni, P.; Kastrati, A.; Kolh, P.; Mauri, L.; et al. 2017 ESC focused update on dual antiplatelet therapy in coronary artery disease developed in collaboration with EACTS: The Task Force for dual antiplatelet therapy in coronary artery disease of the European Society of Cardiology (ESC) and of the European Association for Cardio-Thoracic Surgery (EACTS). Eur. Heart J. 2018, 39, 213–260. [Google Scholar] [PubMed]
- Gorog, D.A.; Geisler, T. Platelet Inhibition in Acute Coronary Syndrome and Percutaneous Coronary Intervention: Insights from the Past and Present. Thromb. Haemost. 2020, 120, 565–578. [Google Scholar] [CrossRef] [PubMed]
- Wiviott, S.D.; Braunwald, E.; McCabe, C.H.; Montalescot, G.; Ruzyllo, W.; Gottlieb, S.; Neumann, F.J.; Ardissino, D.; De Servi, S.; Murphy, S.A.; et al. Prasugrel versus clopidogrel in patients with acute coronary syndromes. N. Engl. J. Med. 2007, 357, 2001–2015. [Google Scholar] [CrossRef]
- Wallentin, L.; Becker, R.C.; Budaj, A.; Cannon, C.P.; Emanuelsson, H.; Held, C.; Horrow, J.; Husted, S.; James, S.; Katus, H.; et al. Ticagrelor versus Clopidogrel in Patients with Acute Coronary Syndromes. N. Engl. J. Med. 2009, 361, 1045–1057. [Google Scholar] [CrossRef] [PubMed]
- O’Gara, P.T.; Kushner, F.G.; Ascheim, D.D.; Casey, D.E.; Chung, M.K.; De Lemos, J.A.; Ettinger, S.M.; Fang, J.C.; Fesmire, F.M.; Franklin, B.A.; et al. 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction: Executive summary: A report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Circulation 2013, 127, 529–555. [Google Scholar] [CrossRef]
- Windecker, S.; Kolh, P.; Alfonso, F.; Collet, J.; Cremer, J.; Falk, V.; Filippatos, G.; Hamm, C.; Head, S.J.; Jüni, P.; et al. 2014 ESC/EACTS Guidelines on myocardial revascularization: The Task Force on Myocardial Revascularization of the European Society of Cardiology (ESC) and the European Association for Cardio-Thoracic Surgery (EACTS)Developed with the special contribution of the European Association of Percutaneous Cardiovascular Interventions (EAPCI). Eur. Heart J. 2014, 35, 2541–2619. [Google Scholar]
- Green, A.; Pottegård, A.; Broe, A.; Diness, T.G.; Emneus, M.; Hasvold, P.; Gislason, G.H. Initiation and persistence with dual antiplatelet therapy after acute myocardial infarction: A Danish nationwide population-based cohort study. BMJ Open 2016, 6, e010880. [Google Scholar] [CrossRef]
- Berger, P.B. Optimal duration of clopidogrel use after implantation of drug-eluting stents-still in doubt. N. Engl. J. Med. 2010, 362, 1441–1443. [Google Scholar] [CrossRef]
- Alexopoulos, D.; Xanthopoulou, I.; Deftereos, S.; Hamilos, M.; Sitafidis, G.; Kanakakis, I.; Pentara, I.; Vavouranakis, M.; Davlouros, P.; Hahalis, G.; et al. Contemporary antiplatelet treatment in acute coronary syndrome patients undergoing percutaneous coronary intervention: One-year outcomes from the GReek AntiPlatelet Registry (GRAPE). J. Thromb. Haemost. 2016, 14, 1146–1154. [Google Scholar] [CrossRef]
- Yudi, M.B.; Clark, D.J.; Farouque, O.; Eccleston, D.; Andrianopoulos, N.; Duffy, S.J.; Brennan, A.; Lefkovits, J.; Ramchand, J.; Yip, T.; et al. Clopidogrel, prasugrel or ticagrelor in patients with acute coronary syndromes undergoing percutaneous coronary intervention. Intern. Med. J. 2016, 46, 559–565. [Google Scholar] [CrossRef]
- Boggon, R.; van Staa, T.P.; Timmis, A.; Hemingway, H.; Ray, K.K.; Begg, A.; Emmas, C.; Fox, K.A.A. Clopidogrel discontinuation after acute coronary syndromes: Frequency, predictors and associations with death and myocardial infarction--a hospital registry-primary care linked cohort (MINAP-GPRD). Eur. Heart J. 2011, 32, 2376–2386. [Google Scholar] [CrossRef] [PubMed]
- D’Ascenzo, F.; Moretti, C.; Bianco, M.; Bernardi, A.; Taha, S.; Cerrato, E.; Omedè, P.; Montefusco, A.; Frangieh, A.H.; Lee, C.W.; et al. Meta-Analysis of the Duration of Dual Antiplatelet Therapy in Patients Treated with Second-Generation Drug-Eluting Stents. Am. J. Cardiol. 2016, 117, 1714–1723. [Google Scholar] [CrossRef] [PubMed]
- Yu, J.; Mehran, R.; Grinfeld, L.; Xu, K.; Nikolsky, E.; Brodie, B.R.; Witzenbichler, B.; Kornowski, R.; Dangas, G.D.; Lansky, A.J.; et al. Sex-based differences in bleeding and long term adverse events after percutaneous coronary intervention for acute myocardial infarction: Three year results from the HORIZONS-AMI trial. Catheter. Cardiovasc. Interv. 2015, 85, 359–368. [Google Scholar] [CrossRef] [PubMed]
- Jneid, H.; Fonarow, G.C.; Cannon, C.P.; Hernandez, A.F.; Palacios, I.F.; Maree, A.O.; Wells, Q.; Boszkurt, B.; LaBresh, K.A.; Liang, L.; et al. Sex differences in medical care and early death after acute myocardial infarction. Circulation 2008, 118, 2803–2810. [Google Scholar] [CrossRef]
- Radovanovic, D.; Erne, P.; Urban, P.; Bertel, O.; Rickli, H.; Gaspoz, J.M. Gender differences in management and outcomes in patients with acute coronary syndromes: Results on 20,290 patients from the AMIS Plus Registry. Heart 2007, 93, 1369–1375. [Google Scholar] [CrossRef] [PubMed]
- Schupke, S.; Neumann, F.J.; Menichelli, M.; Mayer, K.; Bernlochner, I.; Wöhrle, J.; Richardt, G.; Liebetrau, C.; Witzenbichler, B.; Antoniucci, D.; et al. Ticagrelor or Prasugrel in Patients with Acute Coronary Syndromes. N. Engl. J. Med. 2019, 381, 1524–1534. [Google Scholar] [CrossRef]
- De Filippo, O.; Cortese, M.; Raposeiras-Roubin, S.; Abu-Assi, E.; Kinnaird, T.; Ariza-Solé, A.; Manzano-Fernández, S.; Templin, C.; Velicki, L.; Xanthopoulou, I.; et al. Real-World Data of Prasugrel vs. Ticagrelor in Acute Myocardial Infarction: Results from the RENAMI Registry. Am. J. Cardiovasc. Drugs 2019, 19, 381–391. [Google Scholar] [CrossRef]
- Larmore, C.; Effron, M.B.; Molife, C.; DeKoven, M.; Zhu, Y.; Lu, J.; Karkare, S.; Lieu, H.D.; Lee, W.C.; Vetrovec, G.W. “Real-World” Comparison of Prasugrel with Ticagrelor in Patients with Acute Coronary Syndrome Treated with Percutaneous Coronary Intervention in the United States. Catheter. Cardiovasc. Interv. 2016, 88, 535–544. [Google Scholar] [CrossRef]
- Cirillo, P.; Di Serafino, L.; Patti, G.; Antonucci, E.; Calabrò, P.; Gresele, P.; Palareti, G.; Pengo, V.; Pignatelli, V.; Marcucci, R. Gender-Related Differences in Antiplatelet Therapy and Impact on 1-Year Clinical Outcome in Patients Presenting with ACS: The start antiplatelet registry. Angiology 2019, 70, 257–263. [Google Scholar] [CrossRef]
- Jimeno-Sanchez, J.; Fuertes-Ferre, G.; Ruiz-Aranjuelo, A.; Caballero-Jambrina, I.; Diarte-de Miguel, J.; Ortas-Nadal, M.R. Sex-specific differences in antithrombotic therapy and prognosis in patients with acute coronary syndrome treated with stent. Arch. Cardiol. Mex. 2019, 89, 330–338. [Google Scholar] [CrossRef]
- Stone, N.J.; Robinson, J.G.; Lichtenstein, A.H.; Merz, C.N.B.; Blum, C.B.; Eckel, R.H.; Goldberg, A.C.; Gordon, D.; Levy, D.; Lloyd-Jones, D.M.; et al. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J. Am. Coll. Cardiol. 2014, 63, 2889–2934. [Google Scholar] [CrossRef] [PubMed]
- Catapano, A.L.; Graham, I.; De Backer, G.; Wiklund, O.; Chapman, M.J.; Drexel, H.; Hoes, A.W.; Jennings, C.S.; Landmesser, U.; Pedersen, T.R.; et al. 2016 ESC/EAS Guidelines for the Management of Dyslipidaemias. Eur. Heart J. 2016, 37, 2999–3058. [Google Scholar] [CrossRef]
- Conrotto, F.; Bertaina, M.; Raposeiras-Roubin, S.; Kinnaird, T.; Ariza-Solé, A.; Manzano-Fernández, S.; Templin, C.; Velicki, L.; Xanthopoulou, I.; Cerrato, E.; et al. Prasugrel or ticagrelor in patients with acute coronary syndrome and diabetes: A propensity matched substudy of RENAMI. Eur. Heart J. Acute Cardiovasc. Care 2019, 8, 536–542. [Google Scholar] [CrossRef]
| Characteristics | Clopidogrel (n = 10626) | Prasugrel (n = 4788) | p-Value Clopi vs. Prasu | Ticagrelor (n = 9383) | p-Value Clopi vs. Tica |
|---|---|---|---|---|---|
| Age—median years (IQR) | 74 (64; 81) | 57 (51; 65) | p < 0.001 | 63 (54; 73) | p < 0.001 |
| Female sex—n (%) | 4103 (38.6) | 933 (19.5) | p < 0.001 | 2622 (27.9) | p < 0.001 |
| Cardiovascular medication—n (%) | 5585 (52.6) | 1481 (30.9) | p < 0.001 | 3880 (41.4) | p < 0.001 |
| HMG CoA reductase inhibitors—n (%) | 5926 (55.8) | 1961 (41.0) | p < 0.001 | 4579 (48.8) | p < 0.001 |
| Drugs for obstructive airway diseases—n (%) | 1026(9.7) | 247 (5.2) | p < 0.001 | 616(6.6) | p < 0.001 |
| Anti-diabetic medicines—n (%) | 1743 (16.4) | 506 (10.6) | p < 0.001 | 1278 (13.6) | p < 0.001 |
| NOAC—(%) | 1221 (11.5) | 9 (0.2) | p < 0.001 | 34 (0.4) | p < 0.001 |
| Clopidogrel | Prasugrel | p-Value Clopi vs. Prasu | Ticagrelor | p-Value Clopi vs. Tica | |
|---|---|---|---|---|---|
| Age | |||||
| Age 18–39 (n = 454) | 14.8% | 38.8% | p < 0.001 | 46.5% | p < 0.001 |
| Age 40–49 (n = 2374) | 16.2% | 37.4% | p < 0.001 | 46.5% | p < 0.001 |
| Age 50–59 (n = 5749) | 23.6% | 31.8% | p < 0.001 | 44.6% | p < 0.001 |
| Age 60–69 (n = 5963) | 37.8% | 20.9% | p < 0.001 | 41.3% | p < 0.001 |
| Age 70–79 (n = 6205) | 55.5% | 9.6% | p < 0.001 | 34.9% | p < 0.001 |
| Age 80–89 (n = 3532) | 75.3% | 1.5% | p < 0.001 | 23.2% | p < 0.001 |
| Age ≥ 90 (n = 520) | 88.5% | 0.2% | p < 0.001 | 11.3% | p < 0.001 |
| Calendar year | |||||
| 2015 (n = 8040) | 44.3% | 21.9% | p < 0.001 | 33.7% | p < 0.001 |
| 2016 (n = 8417) | 43.5% | 18.7% | p < 0.001 | 37.8% | p < 0.001 |
| 2017 (n = 8340) | 40.8% | 17.4% | p < 0.001 | 41.9% | p < 0.001 |
| Drug survival | |||||
| 6 months | 77.2% | 95.0% | p < 0.001 | 91.7% | p < 0.001 |
| 12 months | 47.1% | 52.9% | p < 0.001 | 47.7% | p < 0.001 |
| 18 months | 23.5% | 11.4% | p < 0.001 | 8.4% | p < 0.001 |
| 24 months | 17.3% | 6.8% | p < 0.001 | 5.1% | p < 0.001 |
| (n = 23816) | P2Y12 Inhibitors | Crude HR (95% CI) | Adjusted HR (95%CI) |
|---|---|---|---|
| Medication | prasugrel | 0.49 (0.44; 0.55) | 0.70 (0.61; 0.79) |
| ticagrelor | 0.57 (0.52; 0.62) | 0.70 (0.64; 0.77) | |
| clopidogrel | 1 | 1 | |
| Age (median 61 years) | 56–66 (2.Qu) | 1.01 (0.89; 1.16) | |
| (median 72 years) | 67–76 (3.Qu) | 1.44 (1.28; 1.60) | |
| (median 82 years) | ≥77 (4.Qu) | 2.18 (1.97; 2.41) | |
| (median 51 years) | 18–55 (1.Qu) | 1 | |
| Age, males | |||
| (median 61 years) | 56–66 (2.Qu) | 1.02 (0.88; 1.18) | |
| (median 72 years) | 67–76 (3.Qu) | 1.29 (1.12; 1.47) | |
| (median 82 years) | ≥77 (4.Qu) | 1.93 (1.69; 2.20) | |
| (median 51 years) | 18–55 (1.Qu) | 1 | |
| Age, females | |||
| (median 61 years) | 56–66 (2.Qu) | 0.63 (0.48; 0.84) | |
| (median 72 years) | 67–76 (3.Qu) | 0.93 (0.74; 1.17) | |
| (median 82 years) | ≥77 (4.Qu) | 1.31 (1.07; 1.61) | |
| (median 51 years) | 18–55 (1.Qu) | 1 | |
| Sex | male vs. female | 0.87 (0.80; 0.94) | |
| Sex, 18–55 years | male vs. female | 0.81 (0.67; 1.00) | |
| Sex, 56–66 years | male vs. female | 1.31 (1.02; 1.69) | |
| Sex, 67–76 years | male vs. female | 1.13 (0.93; 1.37) | |
| Sex, ≥77 years | male vs. female | 1.20 (1.10; 1.34) | |
| Cardiovascular medicines | yes vs. no | 1.41 (1.32; 1.52) | 1.18 (1.08; 1.29) |
| HMG CoA reductase inhibitors | yes vs. no | 1.20 (1.12; 1.29) | 0.98 (0.90; 1.07) |
| Drugs for obstructive airway diseases | yes vs. no | 1.57 (1.39; 1.77) | 1.36 (1.21; 1.54) |
| Anti-diabetic medicines | yes vs. no | 1.46 (1.33; 1.60) | 1.33 (1.21; 1.47) |
| Non-Vitamin K oral anticoagulant | yes vs. no | 1.40 (1.21; 1.65) | 0.93 (0.79; 1.09) |
| Calendar year | 2016 vs. 2015 | 1.01 (0.92; 1.01) | 1.01 (0.92; 1.10) |
| 2017 vs. 2015 | 1.14 (1.03; 1.27) | 1.17 (1.05; 1.30) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sheikh Rezaei, S.; Gleiss, A.; Reichardt, B.; Wolzt, M. Use of Clopidogrel, Prasugrel, or Ticagrelor and Patient Outcome after Acute Coronary Syndrome in Austria from 2015 to 2017. J. Clin. Med. 2020, 9, 3398. https://doi.org/10.3390/jcm9113398
Sheikh Rezaei S, Gleiss A, Reichardt B, Wolzt M. Use of Clopidogrel, Prasugrel, or Ticagrelor and Patient Outcome after Acute Coronary Syndrome in Austria from 2015 to 2017. Journal of Clinical Medicine. 2020; 9(11):3398. https://doi.org/10.3390/jcm9113398
Chicago/Turabian StyleSheikh Rezaei, Safoura, Andreas Gleiss, Berthold Reichardt, and Michael Wolzt. 2020. "Use of Clopidogrel, Prasugrel, or Ticagrelor and Patient Outcome after Acute Coronary Syndrome in Austria from 2015 to 2017" Journal of Clinical Medicine 9, no. 11: 3398. https://doi.org/10.3390/jcm9113398
APA StyleSheikh Rezaei, S., Gleiss, A., Reichardt, B., & Wolzt, M. (2020). Use of Clopidogrel, Prasugrel, or Ticagrelor and Patient Outcome after Acute Coronary Syndrome in Austria from 2015 to 2017. Journal of Clinical Medicine, 9(11), 3398. https://doi.org/10.3390/jcm9113398





