A Systematic Review of Rehabilitation Interventions for Athletes with Chronic Ankle Instability
Abstract
1. Introduction
2. Materials and Methods
2.1. Design
2.2. Eligibility Criteria
2.2.1. Population
2.2.2. Interventions
2.2.3. Outcomes
2.2.4. Exclusion Criteria
2.3. Information Sources
2.4. Selection Process
2.5. Data Collection Process and Items
2.6. Methodological Quality
3. Results
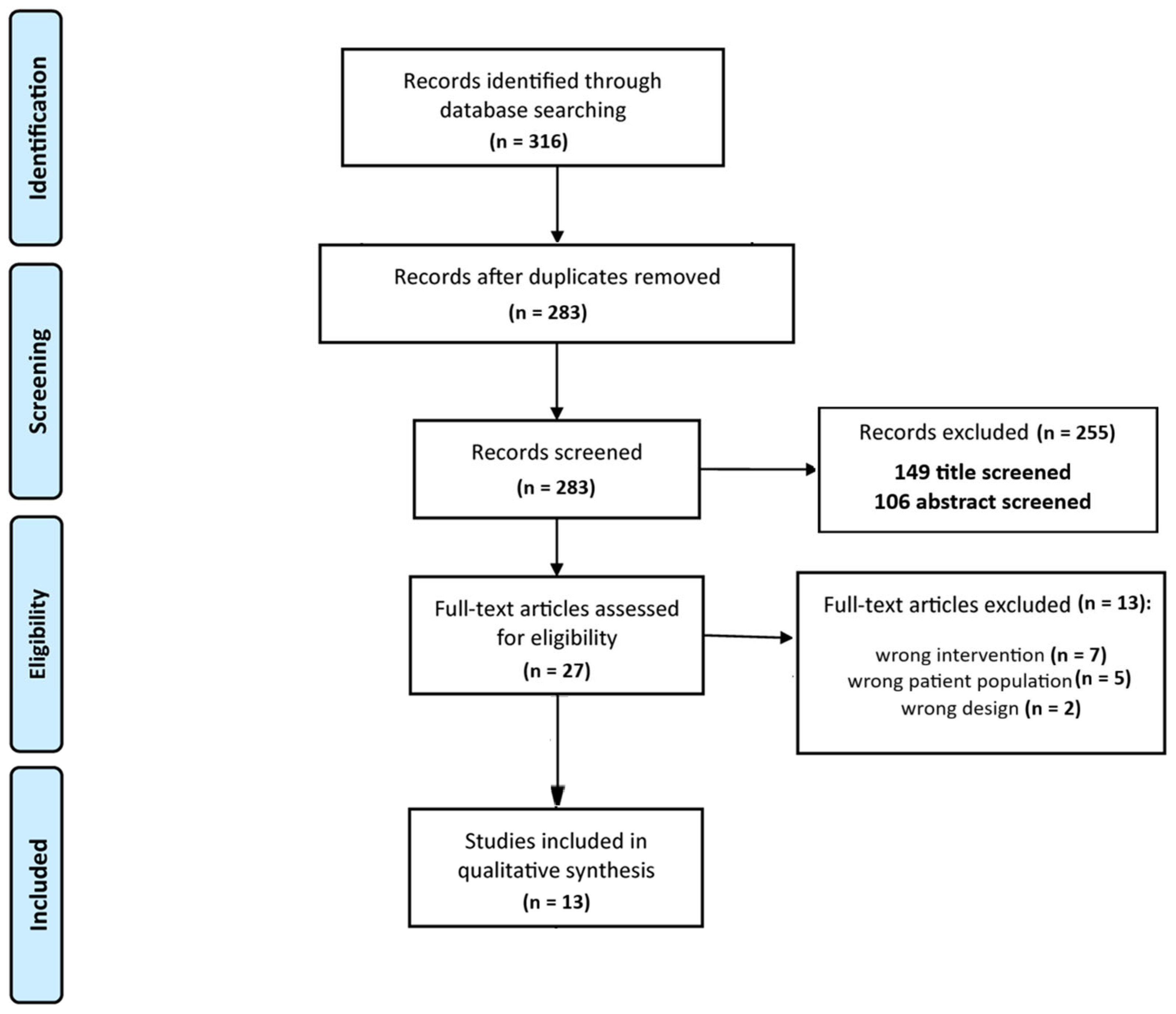
3.1. Study Inclusion
3.1.1. Characteristics and Quality of Included RCTs
3.1.2. Participants
3.1.3. Intervention Type
Balance Training (BT)
Plyometric Training and Other Interventions
3.2. Outcomes Measures
3.2.1. Dynamic Balance
3.2.2. Static Balance
3.2.3. Patient-Reported Outcomes
3.2.4. Kinematics Outcomes
3.2.5. Proprioception
3.2.6. Muscles Activity
3.2.7. Body-Composition Analysis
3.3. Summary of Results
3.4. NHMRC FORM Framework
4. Discussion
5. Limitations
6. Conclusions
7. Practical Implications
Supplementary Materials
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| CAI | The International Ankle Consortium |
| PRISMA | Preferred Reporting Items for Systematic Reviews and Meta-Analyses |
| RCT | Randomized Controll Trial |
| PICO | Population, Intervention, Comparison, and Outcome |
| BESS | Balance Error Scoring System |
| CAIT | Cumberland Ankle Instability Tool |
| DFROM | dorsifelxion ROM |
| FAAM | Foot and Ankle Ability Measure |
| FAAM-S | Foot and Ankle Ability Measure Sport |
| JPS | joint position sense |
| TSK | Tampa Scale for Kinesiophobia |
| SEBT | Star Excursion Balance Test |
| YBT | Y-Balance Test |
| BT | balance training |
| NMT | neuromuscular training combined |
| NFT | neurofeedback training |
| tDCS | transcranial direct current stimulation |
| IDFAI | The Identification of Functional Ankle Instability Questionnaire |
| HADS | The Hospital Anxiety and Depression Scale |
| DLS | double-limb squat |
| DLS-HL | double-limb squat with heel lift |
| sEMG | surface electromyography |
| DEXA | dual-energy X-ray absorptiometry |
References
- Lin, C.I.; Houtenbos, S.; Lu, Y.H.; Mayer, F.; Wippert, P.M. The epidemiology of chronic ankle instability with perceived ankle instability—A systematic review. J. Foot Ankle Res. 2021, 14, 41. [Google Scholar] [CrossRef]
- Whalan, M.; Lovell, R.; McCunn, R.; Sampson, J.A. The incidence and burden of time loss injury in Australian men’s sub-elite football (soccer): A single season prospective cohort study. J. Sci. Med. Sport 2019, 22, 42–47. [Google Scholar] [CrossRef]
- Deitch, J.R.; Starkey, C.; Walters, S.L.; Moseley, J.B. Injury risk in professional basketball players: A comparison of Women’s National Basketball Association and National Basketball Association athletes. Am. J. Sports Med. 2006, 34, 1077–1083. [Google Scholar] [CrossRef] [PubMed]
- Tee, E.; Melbourne, J.; Sattler, L.; Hing, W. Evidence for rehabilitation interventions after acute lateral ankle sprains in athletes: A scoping review. J. Sport Rehabil. 2022, 31, 457–464. [Google Scholar] [CrossRef]
- Drakos, M.; Hansen, O.; Kukadia, S. Ankle instability. Foot Ankle Clin. 2022, 27, 371–384. [Google Scholar] [CrossRef]
- Xue, X.; Wang, Y.; Xu, X.; Li, H.; Li, Q.; Na, Y.; Tao, W.; Yu, L.; Jin, Z.; Li, H.; et al. Postural Control Deficits During Static Single-leg Stance in Chronic Ankle Instability: A Systematic Review and Meta-Analysis. Sports Health 2024, 16, 29–37. [Google Scholar] [CrossRef]
- Xue, X.; Ma, T.; Li, Q.; Song, Y.; Hua, Y. Chronic ankle instability is associated with proprioception deficits: A systematic review and meta-analysis. J. Sport Health Sci. 2021, 10, 182–191. [Google Scholar] [CrossRef] [PubMed]
- Guo, Y.; Cheng, T.; Yang, Z.; Huang, Y.; Li, M.; Wang, T. A systematic review and meta-analysis of balance training in patients with chronic ankle instability. Syst. Rev. 2024, 13, 64. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Tang, Y.; Liang, P.; Pan, J.; Zhang, C.; Ren, H.; Cheng, S.; Kong, P.W. Effects of Ankle Orthoses, Taping, and Insoles on Postural Stability of Individuals with Chronic Ankle Instability: A Systematic Review. Healthcare 2023, 11, 2570. [Google Scholar] [CrossRef]
- Gribble, P.A.; Delahunt, E.; Bleakley, C.; Caulfield, B.; Docherty, C.; Fourchet, F.; Fong, D.T.-P.; Hertel, J.; Hiller, C.E.; Kaminski, T.W.; et al. Selection criteria for patients with chronic ankle instability in controlled research: A position statement of the International Ankle Consortium. Br. J. Sports Med. 2014, 48, 585–591. [Google Scholar] [CrossRef] [PubMed]
- Xu, Y.; Song, B.; Ming, A.; Zhang, C.; Ni, G. Chronic ankle instability modifies proximal lower extremity biomechanics during sports maneuvers that may increase the risk of ACL injury: A systematic review. Front. Physiol. 2022, 13, 1036267. [Google Scholar] [CrossRef]
- Khalaj, N.; Vicenzino, B.; Heales, L.J.; Smith, M.D. Is chronic ankle instability associated with impaired muscle strength? Ankle, knee and hip muscle strength in individuals with chronic ankle instability: A systematic review with meta-analysis. Br. J. Sports Med. 2020, 54, 839–847. [Google Scholar] [CrossRef] [PubMed]
- Miklovic, T.M.; Donovan, L.; Protzuk, O.A.; Kang, M.S.; Feger, M.A. Acute lateral ankle sprain to chronic ankle instability: A pathway of dysfunction. Phys. Sportsmed. 2018, 46, 116–122. [Google Scholar] [CrossRef]
- Selva-Sarzo, F.; Sánchez Romero, E.A.; Cuenca-Zaldívar, J.N.; García-Haba, B.; Akiyama, C.; Sillevis, R.; Fernández-Carnero, S. Effects on perceived pain and somatosensory function after transcutaneous neuromodulation in patients with chronic low back pain: A quasi-experimental study with a crossover intervention. Front. Pain Res. 2025, 6, 1525964. [Google Scholar] [CrossRef]
- Hertel, J.; Corbett, R.O. An updated model of chronic ankle instability. J. Athl. Train. 2019, 54, 572–588. [Google Scholar] [CrossRef] [PubMed]
- Picot, B.; Hardy, A.; Terrier, R.; Tassignon, B.; Lopes, R.; Fourchet, F. Which functional tests and self-reported questionnaires can help clinicians make valid return to sport decisions in patients with chronic ankle instability? A narrative review and expert opinion. Front. Sports Act. Living 2022, 4, 902886. [Google Scholar] [CrossRef]
- Hall, E.A.; Docherty, C.L.; Simon, J.; Kingma, J.J.; Klossner, J.C. Strength-training protocols to improve deficits in participants with chronic ankle instability: A randomized controlled trial. J. Athl. Train. 2015, 50, 36–44. [Google Scholar] [CrossRef]
- Smith, B.I.; Docherty, C.L.; Simon, J.; Klossner, J.; Schrader, J. Ankle strength and force sense after a progressive, 6-week strength-training program in people with functional ankle instability. J. Athl. Train. 2012, 47, 282–288. [Google Scholar] [CrossRef] [PubMed]
- Linens, S.W.; Ross, S.E.; Arnold, B.L. Wobble board rehabilitation for improving balance in ankles with chronic instability. Clin. J. Sport Med. 2016, 26, 76–82. [Google Scholar] [CrossRef]
- Wright, C.J.; Linens, S.W.; Cain, M.S. A randomized controlled trial comparing rehabilitation efficacy in chronic ankle instability. J. Sport Rehabil. 2017, 26, 238–249. [Google Scholar] [CrossRef]
- Eils, E.; Rosenbaum, D. A multi-station proprioceptive exercise program in patients with ankle instability. Med. Sci. Sports Exerc. 2001, 33, 1991–1998. [Google Scholar] [CrossRef]
- O’Driscoll, J.; Delahunt, E. Neuromuscular training to enhance sensorimotor and functional deficits in subjects with chronic ankle instability: A systematic review and best evidence synthesis. Sports Med. Arthrosc. Rehabil. Ther. Technol. 2011, 3, 19. [Google Scholar] [CrossRef]
- Loudon, J.K.; Santos, M.J.; Franks, L.; Liu, W. The effectiveness of active exercise as an intervention for functional ankle instability: A systematic review. Sports Med. 2008, 38, 553–563. [Google Scholar] [CrossRef] [PubMed]
- Cruz, A.L.; Oliveira, R.; Silva, A.G. Exercise-based interventions for physically active individuals with functional ankle instability: A systematic review of the literature. J. Sports Med. Phys. Fit. 2019, 59, 666–675. [Google Scholar] [CrossRef] [PubMed]
- Kim, K.; Choi, B.; Lim, W. The efficacy of virtual reality assisted versus traditional rehabilitation intervention on individuals with functional ankle instability: A pilot randomized controlled trial. Disabil. Rehabil. Assist. Technol. 2019, 14, 276–280. [Google Scholar] [CrossRef]
- Hertel, J. Functional Anatomy, Pathomechanics, and Pathophysiology of Lateral Ankle Instability. J. Athl. Train. 2002, 37, 364–375. [Google Scholar]
- Bialosky, J.E.; Beneciuk, J.M.; Bishop, M.D.; Coronado, R.A.; Penza, C.W.; Simon, C.B.; George, S.Z. Unraveling the Mechanisms of Manual Therapy: Modeling an Approach. J. Orthop. Sports Phys. Ther. 2018, 48, 8–18. [Google Scholar] [CrossRef]
- Boutelle, K.E.; Rickert, K.D.; Carroll, A.N.; Pennock, A.T.; Manhard, C.E.; Edmonds, E.W. Intermediate-term outcomes in adolescent recurrent ankle instability managed with a modified Broström-Gould procedure augmented with distal fibular periosteum incorporation. J. Pediatr. Orthop. 2023, 43, e199–e203. [Google Scholar] [CrossRef]
- Matsui, K.; Burgesson, B.; Takao, M.; Stone, J.; Guillo, S.; Glazebrook, M. Minimally invasive surgical treatment for chronic ankle instability: A systematic review. Knee Surg. Sports Traumatol. Arthrosc. 2016, 24, 1040–1048. [Google Scholar] [CrossRef] [PubMed]
- Law, M.; Stewart, D.; Pollock, N.; Letts, L.; Bosch, J.; Westmorland, M. Critical Review Form–Quantitative Studies; Occupational Therapy Evidence-Based Practice Research Group, McMaster University: Hamilton, ON, Canada, 1998. [Google Scholar]
- Cain, M.S.; Ban, R.J.; Chen, Y.P.; Geil, M.D.; Goerger, B.M.; Linens, S.W. Four-Week Ankle-Rehabilitation Programs in Adolescent Athletes With Chronic Ankle Instability. J. Athl. Train. 2020, 55, 801–810. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Ardakani, M.K.; Wikstrom, E.A.; Minoonejad, H.; Rajabi, R.; Sharifnezhad, A. Hop-Stabilization Training and Landing Biomechanics in Athletes With Chronic Ankle Instability: A Randomized Controlled Trial. J. Athl. Train. 2019, 54, 1296–1303. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Huang, P.Y.; Jankaew, A.; Lin, C.F. Effects of Plyometric and Balance Training on Neuromuscular Control of Recreational Athletes with Functional Ankle Instability: A Randomized Controlled Laboratory Study. Int. J. Environ. Res. Public Health 2021, 18, 5269. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Sierra-Guzmán, R.; Jiménez-Diaz, F.; Ramírez, C.; Esteban, P.; Abián-Vicén, J. Whole-Body-Vibration Training and Balance in Recreational Athletes With Chronic Ankle Instability. J. Athl. Train. 2018, 53, 355–363. [Google Scholar] [CrossRef]
- Cruz-Díaz, D.; Hita-Contreras, F.; Martínez-Amat, A.; Aibar-Almazán, A.; Kim, K.M. Ankle-Joint Self-Mobilization and CrossFit Training in Patients With Chronic Ankle Instability: A Randomized Controlled Trial. J. Athl. Train. 2020, 55, 159–168. [Google Scholar] [CrossRef]
- Lee, H.M.; Oh, S.; Kwon, J.W. Effect of Plyometric versus Ankle Stability Exercises on Lower Limb Biomechanics in Taekwondo Demonstration Athletes with Functional Ankle Instability. Int. J. Environ. Res. Public Health 2020, 17, 3665. [Google Scholar] [CrossRef]
- Anguish, B.; Sandrey, M.A. Two 4-Week Balance-Training Programs for Chronic Ankle Instability. J. Athl. Train. 2018, 53, 662–671. [Google Scholar] [CrossRef]
- Sepasgozar, S.S.; Khanmohammadi, R.; Shiravi, Z. Comparison of the effects of exergaming and balance training on dynamic postural stability during jump-landing in recreational athletes with chronic ankle instability. PLoS ONE 2024, 1, e0314686. [Google Scholar] [CrossRef]
- Wu, H.W.; Chang, Y.S.; Arefin, M.S.; You, Y.L.; Su, F.C.; Lin, C.F. Six-Week Remodeled Bike Pedal Training Improves Dynamic Control of Lateral Shuffling in Athletes With Functional Ankle Instability. Sports Health 2022, 14, 348–357. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Wu, J.; Liang, D.; Ruan, B.; Gao, Q. Effects of Different Intervention Methods on Postural Control in Athletes with Chronic Ankle Instability: A Randomized Controlled Trial. J. Sports Sci. Med. 2025, 24, 332–340. [Google Scholar] [CrossRef] [PubMed]
- Uzlaşır, S.; Özdıraz, K.Y.; Dağ, O.; Tunay, V.B. The effects of stroboscopic balance training on cortical activities in athletes with chronic ankle instability. Phys. Ther. Sport 2021, 50, 50–58. [Google Scholar] [CrossRef] [PubMed]
- Bagherian, S.; Rahnama, N.; Wikstrom, E.A. Corrective Exercises Improve Movement Efficiency and Sensorimotor Function but Not Fatigue Sensitivity in Chronic Ankle Instability Patients: A Randomized Controlled Trial. Clin. J. Sport Med. 2019, 29, 193–202. [Google Scholar] [CrossRef]
- Yalfani, A.; Azizian, M.; Gholami-Borujeni, B. Adding Neurofeedback Training to Neuromuscular Training for Rehabilitation of Chronic Ankle Instability: A 3-Arm Randomized Controlled Trial. Sports Health 2024, 16, 797–807. [Google Scholar] [CrossRef] [PubMed]
- Carcia, C.R.; Martin, R.L.; Drouin, J.M. Validity of the Foot and Ankle Ability Measure in athletes with chronic ankle instability. J. Athl. Train. 2008, 43, 179–183. [Google Scholar] [CrossRef]
- Hiller, C.E.; Refshauge, K.M.; Bundy, A.C.; Herbert, R.D.; Kilbreath, S.L. The Cumberland Ankle Instability Tool: A report of validity and reliability testing. Arch. Phys. Med. Rehabil. 2006, 87, 1235–1241. [Google Scholar] [CrossRef]
- Rahmati, N.; Moghadam, M.A.A.; Shairi,, M.R.; Paknejad, M.; Rahmati, Z.; Ghassami, M.; Ebrahimi, E.; Marufi, N.; Aghaee, H.N. Psychometric properties of the Tampa Scale for Kinesiophobia amongst Iranian patients with chronic persistent pain. J. Payesh. 2014, 13, 197–210. [Google Scholar]
- Bjelland, I.; Dahl, A.A.; Haug, T.T.; Neckelmann, D. The validity of the Hospital Anxiety and Depression Scale: An updated literature review. J. Psychosom. Res. 2002, 52, 69–77. [Google Scholar] [CrossRef]
- Sandrey, M.A.; Kent, T.E. The effects of eversion fatigue on frontal plane joint position sense in the ankle. J. Sport Rehabil. 2008, 17, 257–268. [Google Scholar] [CrossRef]
- Robbins, S.E.; Waked, W.E.; McClaran, J. Proprioception and stability: Foot position awareness as a function of age and footwear. Age Aging 1995, 24, 67–72. [Google Scholar] [CrossRef]
- Watanabe, K.; Koshino, Y.; Kawahara, D.; Akimoto, M.; Mishina, M.; Nakagawa, K.; Ishida, T.; Kasahara, S.; Samukawa, M.; Tohyama, H. Kinesiophobia, self-reported ankle function, and sex are associated with perceived ankle instability in college club sports athletes with chronic ankle instability. Phys. Ther. Sport 2023, 61, 45–50. [Google Scholar] [CrossRef] [PubMed]
- Caldemeyer, L.E.; Brown, S.M.; Mulcahey, M.K. Neuromuscular training for the prevention of ankle sprains in female athletes: A systematic review. Phys. Sportsmed. 2020, 48, 363–369. [Google Scholar] [CrossRef] [PubMed]
| Study | NHMRC Level | Items on Modified McMaster Critical Review Form | Raw Score | ||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 2 | 3 | 4a | 4b | 4c | 5a | 5b | 6a | 6b | 6c | 7a | 7b | 7c | 7d | 8 | Points | % | ||
| Cain [31] | Level II | Y | Y | RCT | 43 | Y | N/A | Y | Y | Y | NAD | Y | Y | Y | Y | Y | Y | 12 out of 13 | 92% |
| Ardakani [32] | Level II | Y | Y | RCT | 28 | Y | Y | Y | Y | Y | NAD | Y | Y | Y | Y | Y | Y | 13 out of 13 | 100% |
| Huang [33] | Level II | Y | Y | RCT | 30 | Y | Y | Y | Y | Y | NAD | Y | Y | Y | Y | Y | Y | 13 out of 13 | 100% |
| Sierra-Guzmán [34] | Level II | Y | Y | RCT | 50 | Y | Y | Y | Y | Y | NAD | Y | Y | Y | Y | Y | Y | 13 out of 13 | 100% |
| Cruz-Díaz [35] | Level II | Y | Y | RCT | 70 | Y | Y | Y | Y | Y | NAD | Y | Y | Y | Y | Y | Y | 13 out of 13 | 100% |
| Lee [36] | Level II | Y | Y | RCT | 14 | Y | N | Y | Y | Y | NAD | Y | Y | Y | N | N | Y | 10 out of 13 | 77% |
| Anguish [37] | Level II | Y | Y | RCT | 18 | Y | N/A | Y | Y | Y | NAD | Y | Y | Y | Y | Y | Y | 12 out of 13 | 92% |
| Sepasgozar [38] | Level II | Y | Y | RCT | 34 | Y | Y | Y | Y | Y | NAD | Y | Y | Y | N | Y | Y | 12 out of 13 | 92% |
| Wu [39] | Level II | Y | Y | RCT | 26 | Y | N/A | Y | Y | Y | NAD | Y | Y | Y | Y | Y | Y | 12 out of 13 | 92% |
| Zhang [40] | Level II | Y | Y | RCT | 36 | Y | Y | Y | Y | Y | NAD | Y | Y | Y | N | Y | Y | 12 out of 13 | 92% |
| Uzlaşır [41] | Level II | Y | Y | RCT | 39 | Y | Y | Y | Y | Y | NAD | Y | Y | Y | N | Y | Y | 12 out of 13 | 92% |
| Bagherian [42] | Level II | Y | Y | RCT | 40 | Y | Y | Y | Y | Y | NAD | Y | Y | Y | Y | Y | Y | 13 out of 13 | 100% |
| Yalfani [43] | Level II | Y | Y | RCT | 62 | Y | Y | Y | Y | Y | NAD | Y | Y | Y | N | Y | Y | 12 out of 13 | 92% |
| Study | Sample Size | Mean Age | Gender | Discipline | Injury | Intervention | Comparator/Control | Outcome Addressed | Follow Up |
|---|---|---|---|---|---|---|---|---|---|
| Cain [31] | 43 | G1: 16.42 ± 1.00; G2: 16.40 ± 0.97; G3: 16.20 ± 1.14; Controll: 16.45 ± 1.04 | F: 23; M: 20 | N/A | CAI | Stroboscopic balance trening | Combination with resistance-band/no intervention | Time-in-Balance-Test, Foot-Lift-Test, (SEBT), Side-Hoop-Test, Figure-8 Hop Test, FAAM, CAIT | 4–6 weeks |
| Ardakani [32] | 28 | G1: 22.78 ± 3.09; controll: 22.57 ± 2.76 | M: 28 | Basketball | CAI | Hop-Stabilization Training | No intervention | FAAM, FAAM-S, CAIT | 6 weeks |
| Huang [33] | 30 | G1: 23.20 ± 2.82; G2: 23.80 ± 4.13; Controll: 23.50 ± 3.00 | F: 23; M: 7 | N/A | CAI | Plyometric training, | Plyometric training + balance training/no intervention | Single-leg drop medial landing test, CAIT, JPS | 6 weeks |
| Sierra-Guzmán [34] | 50 | G1: 22.4 ± 2.6; G2: 21.8 ± 2.1; Controll: 23.6 ± 3.4 | F: 17; M: 33 | N/A | CAI | Wholebody–vibration (WBV) training | Stabilization training without vibration/no intervention | CAIT, BBS platform, SEBT, Body-Composition Analysis | 6 weeks |
| Cruz-Díaz [35] | 70 | G1: 29.16 ± 8.38; G2: 27.63 ± 7.42; Controll: 30.38 ± 9.86 | F: 30; M: 40 | CrossFit | CAI | CrossFit training, | CrossFit plus self-mobilization/no intervention | CAIT, SEBT, WBLT-DFROM | 12 weeks |
| Lee [36] | 14 | G1: 22.00 ± 1.73; G2: 23.57 ± 1.62 | M: 14 | Taekwondo | CAI | Plyometric training, | Stability exercises | YBT | 8 weeks |
| Anguish [37] | 18 | G1: 18.44 ± 1.87; G2: 18.33 ± 1.87 | F: 2; M: 16 | N/A | CAI | Progressive hop-to-stabilization balance (PHSB) | Single-limb balance (SLB) programme | SEBT, FAAM, FAAM-S, JPS | 4 weeks |
| Sepasgozar [38] | 34 | G1: 22; Controll: 24 | F: 11; M: 23 | N/A | CAI | Balance training | Exergaming | CAIT, platform, TSK | 4 weeks |
| Wu [39] | 26 | G1: 22.6 ± 62.47; G2: 22.86 ± 1.78 | F: 8; M: 18 | N/A | CAI | Remodeled bicycle pedal training | No intervention | CAIT, Lateral Shuffling Task, kinematic assessment, sEMG | 6 weeks |
| Zhang [40] | 36 | G1: 20.56 ± 1.67; G2: 20.78 ± 1.48; G3: 20.00 ± 1.00; G4: 19.78 ± 0.97 | F: 16; M: 20 | N/A | CAI | Transcranial direct current stimulation (tDCS), balance training, | tDCS/balance training | CAIT, BESS, YBT | 4 weeks |
| Uzlaşır [41] | 39 | G1: 19.08 ± 0.40; G2: 20.46 ± 0.51; Controll: 20.23 ± 0.39 | F: 19; M: 20 | N/A | CAI | Stroboscopic balance training program | Non-strobe/no intervention | FAAM, FAAM-S, IDFAI | 6 weeks |
| Bagherian [42] | 40 | G1: 21.2 ± 1.7; Controll: 20.9 ± 1.8 | M: 40 | N/A | CAI | Corrective exercise program | No intervention | FAAM, FAAM-S, squats, SEBT | 8 weeks |
| Yalfani [43] | 62 | G1: 22.14 ± 2.53; G2: 21.73 ± 2.60; Controll: 21.45 ± 3.21 | M: 62 | N/A | CAI | Neuromuscular training | Neurofeedback training + neuromuscular training/no training | JPS, FABQ, HADS, FAAM | 8 weeks |
| Study | Outcome Domain and Outcome Measures | |||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Static Balance | Dynamic Balance | Patient-Reported Outcomes | Kinematic Outcomes | Proprioception | Muscles Activity | Body-Composition Analysis | ||||||||||||||||||
| Time-in-Balance | Foot-Lift | BESS | Center of Pressure | SEBT | Single-Leg Drop Medial Landing | YBT | Platform | Side-Hop | Figure-8 Hop | Lateral Shuffling Task | FAAM | FAAM-S | CAIT | IDFAI | TSK | HADS | Cameras Infrared | WBLT-DFROM | Squat | JPS | Isokinetic Dynamometer | sEMG | Dual-Energy X-Ray Absorptiometry | |
| Cain | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | |||||||||||||||||
| Ardakani | ✓ | ✓ | ✓ | ✓ | ||||||||||||||||||||
| Huang | ✓ | ✓ | ✓ | |||||||||||||||||||||
| Sierra-Guzmán | ✓ | ✓ | ✓ | ✓ | ||||||||||||||||||||
| Cruz-Díaz | ✓ | ✓ | ✓ | |||||||||||||||||||||
| Lee | ✓ | ✓ | ||||||||||||||||||||||
| Anguish | ✓ | ✓ | ✓ | ✓ | ||||||||||||||||||||
| Sepasgozar | ✓ | ✓ | ✓ | ✓ | ||||||||||||||||||||
| Wu | ✓ | ✓ | ✓ | ✓ | ||||||||||||||||||||
| Zhang | ✓ | ✓ | ✓ | |||||||||||||||||||||
| Uzlaşır | ✓ | ✓ | ✓ | ✓ | ||||||||||||||||||||
| Bagherian | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ||||||||||||||||||
| Yalfani | ✓ | ✓ | ✓ | ✓ | ✓ | |||||||||||||||||||
| Study | Effect of Physiotherapy Interventions for the Management of | |||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Static Balance | Dynamic Balance | Patient-Reported Outcomes | Kinematic Outcomes | Proprioception | Muscles Activity | Body-Composition Analysis | ||||||||||||||||||
| Time-in-Balance | Foot-Lift | BESS | Center of Pressure | SEBT | Single-Leg Drop Medial Landing | YBT | Platform | Side-Hop | Figure-8 Hop | Lateral Shuffling Task | FAAM | FAAM-S | CAIT | IDFAI | TSK | HADS | Cameras Infrared | WBLT-DFROM | Squat | JPS | Isokinetic Dynamometer | sEMG | Dual-Energy X-Ray Absorptiometry | |
| Cain | (+) | (+) | (+) | (+) | (+) | (+) | (+) | |||||||||||||||||
| Ardakani | (+) | (+) | (+) | (+) | ||||||||||||||||||||
| Huang | (+) | (+) | (+) | |||||||||||||||||||||
| Sierra-Guzmán | (+) | (+) | (+) | (=) | ||||||||||||||||||||
| Cruz-Díaz | (+) | (+) | (+) | |||||||||||||||||||||
| Lee | (+) | (+) | ||||||||||||||||||||||
| Anguish | (+) | (+) | (+) | (+) | ||||||||||||||||||||
| Sepasgozar | (+) | (+) | (+) | (+) | ||||||||||||||||||||
| Wu | (+) | (+) | (+) | |||||||||||||||||||||
| Zhang | (+) | (=) | ||||||||||||||||||||||
| Uzlaşır | (+) | |||||||||||||||||||||||
| Bagherian | (+) | (+) | (+) | (+) | ||||||||||||||||||||
| Yalfani | (+) | (+) | (+) | |||||||||||||||||||||
| Component | Grade | Comments |
|---|---|---|
| A—Excellent Level II studies with a low risk of bias | Quantity: 13 studies Participants: 490 athletes with CAI Level II: 13 studies Level III-2: 0 study Level III-3: 0 study Level IV: 0 study |
| B—Good Most studies consistent and inconsistency may be explained | Similar time-point measurements Consistent results Heterogeneous interventions Various outcome measures |
| B—Good Substantial | Consistent outcome results: particularly improved functionality following interventions. All studies demonstrate statistical significance. Clinical significance should be considered with caution. No adverse events were reported. |
| B—Good Population/s studied in the body of evidence are similar to the target population for the guideline | The study population is similar to the target population. Age ranged from 16 to 30 years. All patients were athletes with CAI who were treated conservatively. The studies were conducted in eight different countries with different healthcare contexts. |
| C—Satisfactory Evidence provides some support for recommendation(s) but care should be taken in its application | These studies had high evidence and were of high methodological quality. Although overall there were positive results, the current evidence base is not homogeneous in terms of interventions delivered, and parameters and results measured for athletes with CAI. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.
Share and Cite
Skwiot, M. A Systematic Review of Rehabilitation Interventions for Athletes with Chronic Ankle Instability. J. Clin. Med. 2026, 15, 220. https://doi.org/10.3390/jcm15010220
Skwiot M. A Systematic Review of Rehabilitation Interventions for Athletes with Chronic Ankle Instability. Journal of Clinical Medicine. 2026; 15(1):220. https://doi.org/10.3390/jcm15010220
Chicago/Turabian StyleSkwiot, Marlena. 2026. "A Systematic Review of Rehabilitation Interventions for Athletes with Chronic Ankle Instability" Journal of Clinical Medicine 15, no. 1: 220. https://doi.org/10.3390/jcm15010220
APA StyleSkwiot, M. (2026). A Systematic Review of Rehabilitation Interventions for Athletes with Chronic Ankle Instability. Journal of Clinical Medicine, 15(1), 220. https://doi.org/10.3390/jcm15010220





