How Should Patients with a Thoracolumbar Injury Classification and Severity Score of 4 Be Treated?
Abstract
1. Introduction
2. Materials and Methods
3. Results
3.1. Demographic Data
3.2. Radiological Outcomes
3.3. Statistical Analysis
4. Discussion
4.1. Background
4.2. Problem of TLICS Classification
4.3. Analysis of Our Results
4.4. Limitation and Strength of Current Study
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Behairy, Y. Unconventional fixation of thoracolumbar fractures using round hole bone plates and transpedicular Screws. Ann. Saudi Med. 2001, 21, 30–34. [Google Scholar] [PubMed]
- Aras, E.L.; Bunger, C.; Hansen, E.S.; Søgaard, R. Cost-effectiveness of surgical versus conservative treatment for thoracolumbar burst fracture. Spine 2016, 41, 337–343. [Google Scholar] [CrossRef]
- Leferink, V.; Zimmerman, K.; Veldhuis, E. Thoracolumbar spinal fractures: Radiological result of trans pedicular fixation combined with cancellous bone grafts in 183 patients. Eur. Spine J. 2001, 6, 517–523. [Google Scholar] [CrossRef] [PubMed]
- Nataraj, A.; Jack, A.S.; Ihsanullah, I.; Nomani, S.; Kortbeek, F.; Fox, R. Outcomes in thoracolumbar burst fractures with a Thoracolumbar Injury Classification Score (TLICS) of 4 treated with surgery versus initial conservative management. Clin. Spine Surg. 2018, 31, E317–E321. [Google Scholar] [CrossRef]
- Chokshi, J.J.; Shah, M. Outcomes of including fracture level in short-segment fixation for thoracolumbar fracture dislocation. Asian Spine J. 2019, 13, 56–60. [Google Scholar] [CrossRef]
- Alan, N.; Donohue, J.; Ozpinar, A.; Agarwal, N.; Kanter, A.S.; Okonkwo, D.O.; Hamilton, D.K. Load-sharing classification score as supplemental grading system in the decision-making process for patients with thoracolumbar injury classification and severity 4. Neurosurgery 2021, 89, 428–434. [Google Scholar] [CrossRef]
- Pneumaticos, S.G.; Karampinas, P.K.; Triantafilopoulos, G.; Koufos, S.; Polyzois, V.; Vlamis, J. Evaluation of TLICS for thoracolumbar fractures. Eur. Spine J. 2016, 25, 1123–1127. [Google Scholar] [CrossRef]
- Smith, C.J.; Abdulazeez, M.M.; ElGawady, M.; Mesfin, F.B. The effect of thoracolumbar injury classification in the clinical outcome of operative and non-operative treatments. Cureus 2021, 13, e12428. [Google Scholar]
- Thomas, K.C.; Bailey, C.S.; Dvorak, M.F.; Kwon, B.; Fisher, C. Comparison of operative and nonoperative treatment for thoracolumbar burst fractures in patients without neurological deficit: A systematic review. J. Neurosurg. Spine 2006, 4, 351–358. [Google Scholar] [CrossRef] [PubMed]
- Bakhsheshian, J.; Dahdaleh, N.S.; Fakurnejad, S.; Scheer, J.K.; Smith, Z.A. Evidence-based management of traumatic thoracolumbar burst fractures: A systematic review of nonoperative management. Neurosurg. Focus 2014, 37, E1. [Google Scholar] [CrossRef] [PubMed]
- Joaquim, A.F.; Ghizoni, E.; Tedeschi, H.; Batista, U.C.; Patel, A.A. Clinical results of patients with thoracolumbar spine trauma treated according to the thoracolumbar injury classification and severity score. J. Neurosurg. Spine 2014, 20, 562–567. [Google Scholar] [CrossRef]
- Rubery, P.T.; Brown, R.; Prasarn, M.; Small, J.; Conrad, B.; Horodyski, M.; Rechtine, G. Stabilization of 2-column thoracolumbar fractures with orthoses: A cadaver model. Spine 2013, 38, E270–E275. [Google Scholar] [CrossRef]
- van Leeuwen, P.J.; Bos, R.P.; Derksen, J.C.; de Vries, J. Assessment of spinal movement reduction by thoraco-lumbar-sacral orthoses. J. Rehabil. Res. Dev. 2000, 37, 395–403. [Google Scholar] [PubMed]
- Harry, N.H.; Steven, R.G.; Frank, J.E.; Gordon, R.B.; Richard, A.B. Rothman-Simeone the Spine, 6th ed.; Elsevier: Philadelphia, PA, USA, 2011; pp. 1372–1374. [Google Scholar]
- Dodwad, S.N.; Dodwad, S.J.; Wisneski, R.; Khan, S.N. Retrospective analysis of thoracolumbar junction injuries using the thoracolumbar injury severity and classification score, American Spinal Injury Association Class, injury severity score, age, sex, and length of hospitalization. J. Spinal Disord. Tech. 2015, 28, 410–416. [Google Scholar] [CrossRef]
- Park, H.J.; Lee, S.Y.; Park, N.H.; Shin, H.G.; Chung, E.C.; Rho, M.H.; Kim, M.S.; Kwon, H.J. Modified thoracolumbar injury classification and severity score (TLICS) and its clinical usefulness. Acta Radiol. 2016, 57, 74–81. [Google Scholar] [CrossRef] [PubMed]
- Vaccaro, A.R.; Lehman, R.A., Jr.; Hurlbert, R.J. A new classification of thoracolumbar injuries: The importance of injury morphology, the integrity of the posterior ligamentous complex, and neurologic status. Spine 2005, 30, 2325–2333. [Google Scholar] [CrossRef] [PubMed]
- Azhari, S.; Azimi, P.; Shahzadi, S.; Mohammadi, H.R.; Khayat Kashani, H.R. Decision-making process in patients with thoracolumbar and lumbar burst fractures with thoracolumbar injury severity and classification score less than four. Asian Spine J. 2016, 10, 136–142. [Google Scholar] [CrossRef] [PubMed]
- Abudou, M.; Chen, X.; Kong, X.; Wu, T. Surgical versus non-surgical treatment for thoracolumbar burst fractures without neurological deficit. Cochrane Database Syst. Rev. 2013, 6, CD005079. [Google Scholar] [CrossRef]
- Joaquim, A.F.; Fernandes, Y.B.; Cavalcante, R.A.; Fragoso, R.M.; Honorato, D.C.; Patel, A.A. Evaluation of the thoracolumbar injury classification system in thoracic and lumbar spinal trauma. Spine 2011, 36, 33–36. [Google Scholar] [CrossRef]
- Siebenga, J.; Leferink, V.J.; Segers, M.J.; Elzinga, M.J.; Bakker, F.C.; Haarman, H.J.T.M.; Rommens, P.M.; Duis, H.J.; Patka, P. Treatment of traumatic thoracolumbar spine fractures: A multicenter prospective randomized study of operative versus nonsurgical treatment. Spine 2006, 31, 2881–2890. [Google Scholar] [CrossRef]
- Wood, K.; Buttermann, G.; Mehbod, A.; Garvey, T.; Jhanjee, R.; Sechriest, V. Operative compared with nonoperative treatment of a thoracolumbar burst fracture without neurological deficit. A prospective, randomized study. J. Bone Joint Surg. Am. 2003, 85, 773–781. [Google Scholar] [CrossRef] [PubMed]
- Wood, K.B.; Buttermann, G.R.; Phukan, R.; Harrod, C.C.; Mehbod, A.; Shannon, B.; Bono, C.M.; Harris, M.B. Operative compared with nonoperative treatment of a thoracolumbar burst fracture without neurological deficit: A prospective randomized study with follow-up at sixteen to twenty-two years. J. Bone Jt. Surg. Am. 2015, 97, 3–9. [Google Scholar] [CrossRef] [PubMed]
- Mohamadi, A.; Googanian, A.; Ahmadi, A.; Kamali, A. Comparison of surgical or nonsurgical treatment outcomes in patients with thoracolumbar fracture with score 4 of TLICS: A randomized, single-blind, and single-central clinical trial. Medicine 2018, 97, e9842. [Google Scholar] [CrossRef] [PubMed]
- Hartmann, F.; Nusselt, T.; Mattyasovszky, S.; Maier, G.; Rommens, P.M.; Gercek, E. Misdiagnosis of thoracolumbar posterior ligamentous complex injuries and use of radiographic parameter correlations to improve detection accuracy. Asian Spine J. 2019, 13, 29–34. [Google Scholar] [CrossRef] [PubMed]
| Success Group (n = 18) | Failure Group (n = 26) | p | |
|---|---|---|---|
| Gender, male/female (n) † | 12/6 | 18/8 | 0.85 |
| Age (yr) ‡ | 48.6 ± 16.4 | 45.2 ± 12.8 | 0.46 |
| BMI (Kg/m2) ‡ | 23.7 ± 3.2 | 22.9 ± 3.5 | 0.46 |
| Initial VAS (score) § | 4.5 ± 1.2 | 4.4 ± 0.9 | 0.11 |
| Injury mechanism † | |||
| Traffic accident | 6 | 7 | 0.92 |
| Fall down | 9 | 13 | |
| Blunt trauma | 3 | 6 | |
| Level of fracture | |||
| T11 | 3 | 1 | |
| T12 | 3 | 3 | |
| L1 | 3 | 17 | |
| L2 | 9 | 5 |
| ASIA Impairment Scale | Success Group (n = 18) | Failure Group (n = 26) | |||
|---|---|---|---|---|---|
| Initial | Last F/U | Initial | Preoperative | Last F/U | |
| Grade A | 0 | 0 | 0 | 0 | 0 |
| Grade B | 0 | 0 | 0 | 0 | 0 |
| Grade C | 0 | 0 | 0 | 1 | 0 |
| Grade D | 2 | 2 | 4 | 11 | 5 |
| Grade E | 16 | 16 | 22 | 14 | 21 |
| Success Group (n = 18) | Failure Group (n = 26) | p | |
|---|---|---|---|
| Initial § | 4.5 ± 1.2 | 4.4 ± 0.9 | 0.11 |
| Before operative treatment | 6.5 ± 1.1 | ||
| Last follow-up § | 1.7 ± 1.1 | 1.9 ± 1.0 | 0.14 |
| Success Group (n = 18) | Failure Group (n = 26) | p | |
|---|---|---|---|
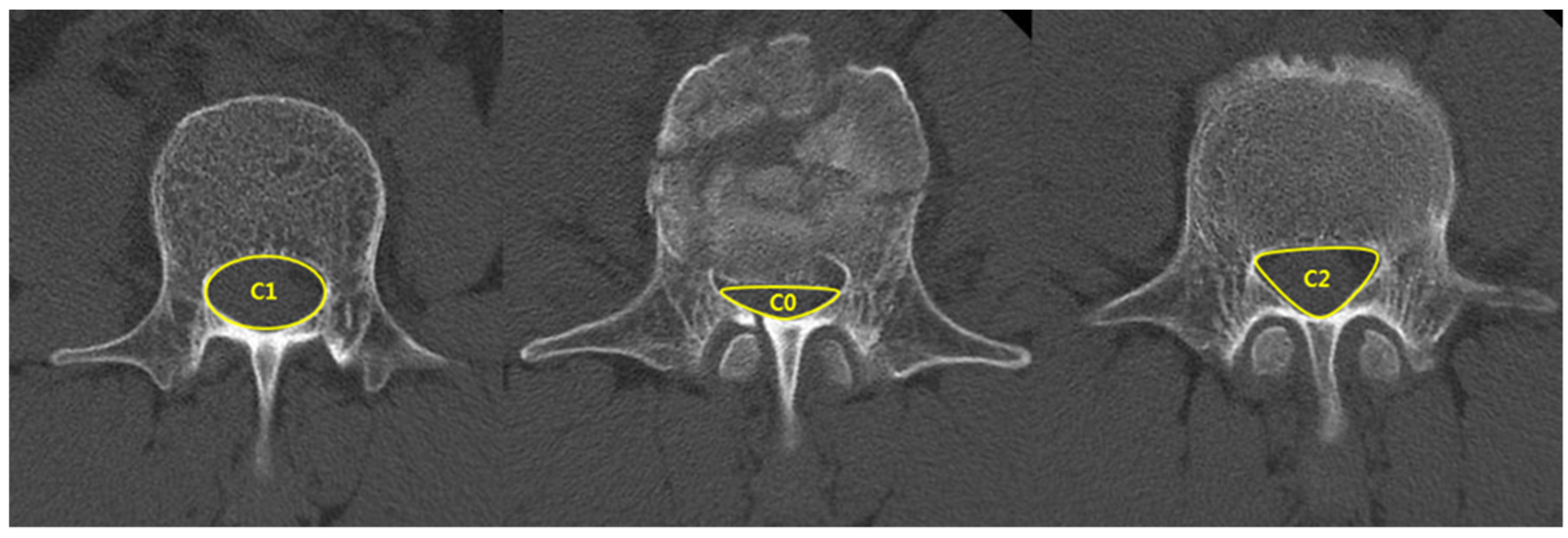
| Spinal canal compromise (%) ‡ | 27.9 ± 7.6 | 35.7 ± 13.3 | 0.03 |
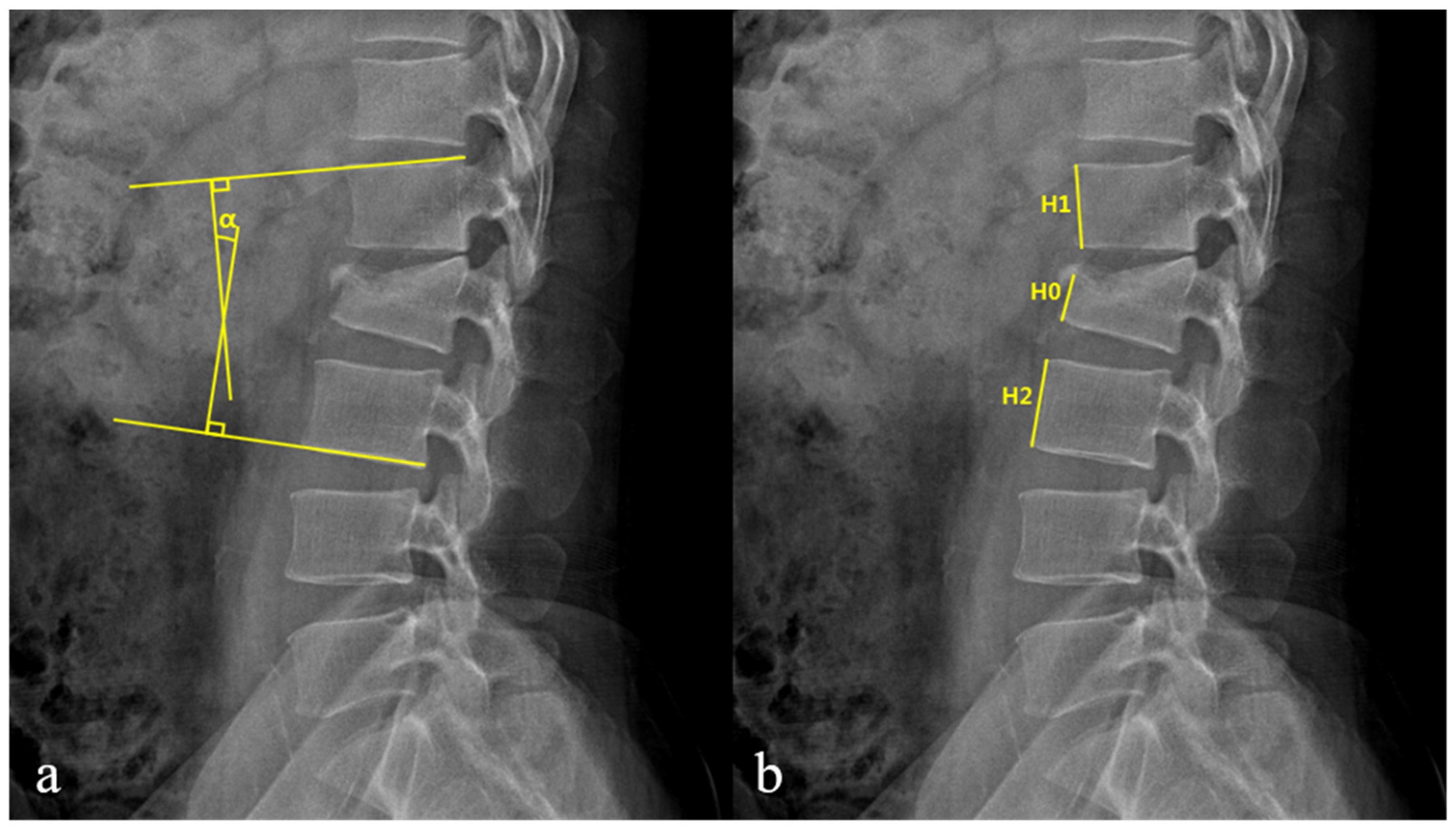
| Loss of vertebral body height (%) ‡ | 28.6 ± 7.8 | 34.1 ± 6.0 | 0.01 |
| Kyphotic angle (°) ‡ | 10.1 ± 6.2 | 13.9 ± 5.0 | 0.04 |
| Odd Ratio | 95% Confidence Interval | p | |
|---|---|---|---|
| Gender | 0.9 | 0.25 to 3.22 | 0.86 |
| Age | 0.98 | 0.94 to 1.03 | 0.45 |
| BMI | 0.93 | 0.77 to 1.12 | 0.45 |
| Initial VAS score | 0.84 | 0.45 to 1.18 | 0.13 |
| Spinal canal compromise | 1.26 | 1.00 to 1.42 | 0.04 |
| Loss of vertebral body height | 1.11 | 1.02 to 1.15 | 0.02 |
| Kyphotic angle | 1.33 | 1.01 to 1.47 | 0.04 |
| Odd Ratio | 95% Confidence Interval | p | |
|---|---|---|---|
| Spinal canal compromise | 1.316 | 1.01 to 1.41 | 0.03 |
| Loss of vertebral body height | 0.924 | 0.85 to 1.01 | 0.07 |
| Kyphotic angle | 1.416 | 1.02 to 1.55 | 0.03 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lee, N.-H.; Kim, S.-K.; Seo, H.-Y.; Park, E.T.; Jang, W.-Y. How Should Patients with a Thoracolumbar Injury Classification and Severity Score of 4 Be Treated? J. Clin. Med. 2021, 10, 4944. https://doi.org/10.3390/jcm10214944
Lee N-H, Kim S-K, Seo H-Y, Park ET, Jang W-Y. How Should Patients with a Thoracolumbar Injury Classification and Severity Score of 4 Be Treated? Journal of Clinical Medicine. 2021; 10(21):4944. https://doi.org/10.3390/jcm10214944
Chicago/Turabian StyleLee, Nam-Hun, Sung-Kyu Kim, Hyoung-Yeon Seo, Eric T. Park, and Won-Young Jang. 2021. "How Should Patients with a Thoracolumbar Injury Classification and Severity Score of 4 Be Treated?" Journal of Clinical Medicine 10, no. 21: 4944. https://doi.org/10.3390/jcm10214944
APA StyleLee, N.-H., Kim, S.-K., Seo, H.-Y., Park, E. T., & Jang, W.-Y. (2021). How Should Patients with a Thoracolumbar Injury Classification and Severity Score of 4 Be Treated? Journal of Clinical Medicine, 10(21), 4944. https://doi.org/10.3390/jcm10214944






