A Comprehensive Examination of Percutaneous Endoscopic Gastrostomy and Its Association with Amyotrophic Lateral Sclerosis Patient Outcomes
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Inclusion Criteria
2.2. Calculation of Survival Duration
2.3. Temporal Disease Assessments
2.4. Clinical Impression of Mood
2.5. Gait
2.6. Statistical Analysis of Primary Results
2.7. Literature Meta-Analysis of PEG Usage in ALS
3. Results
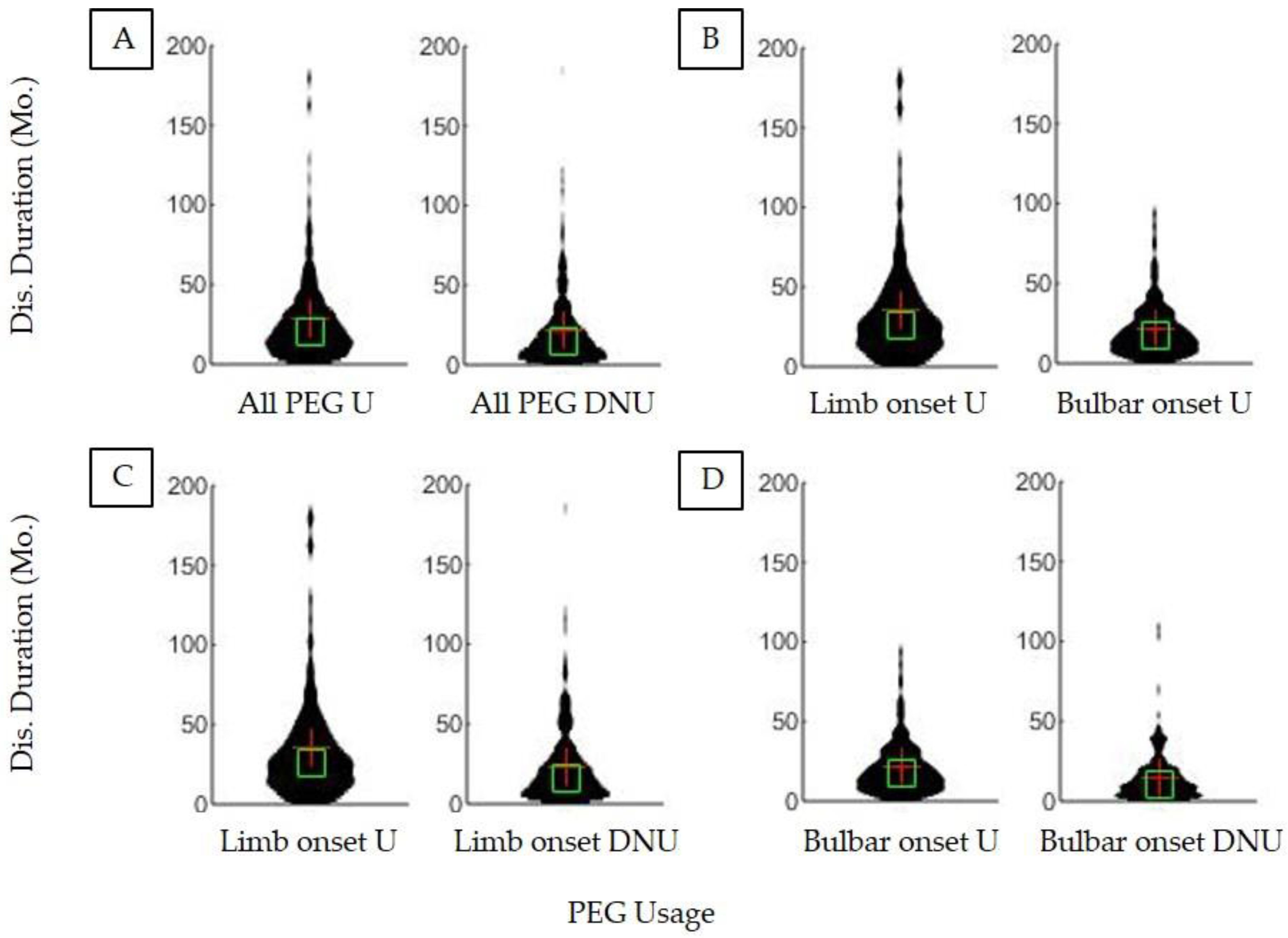
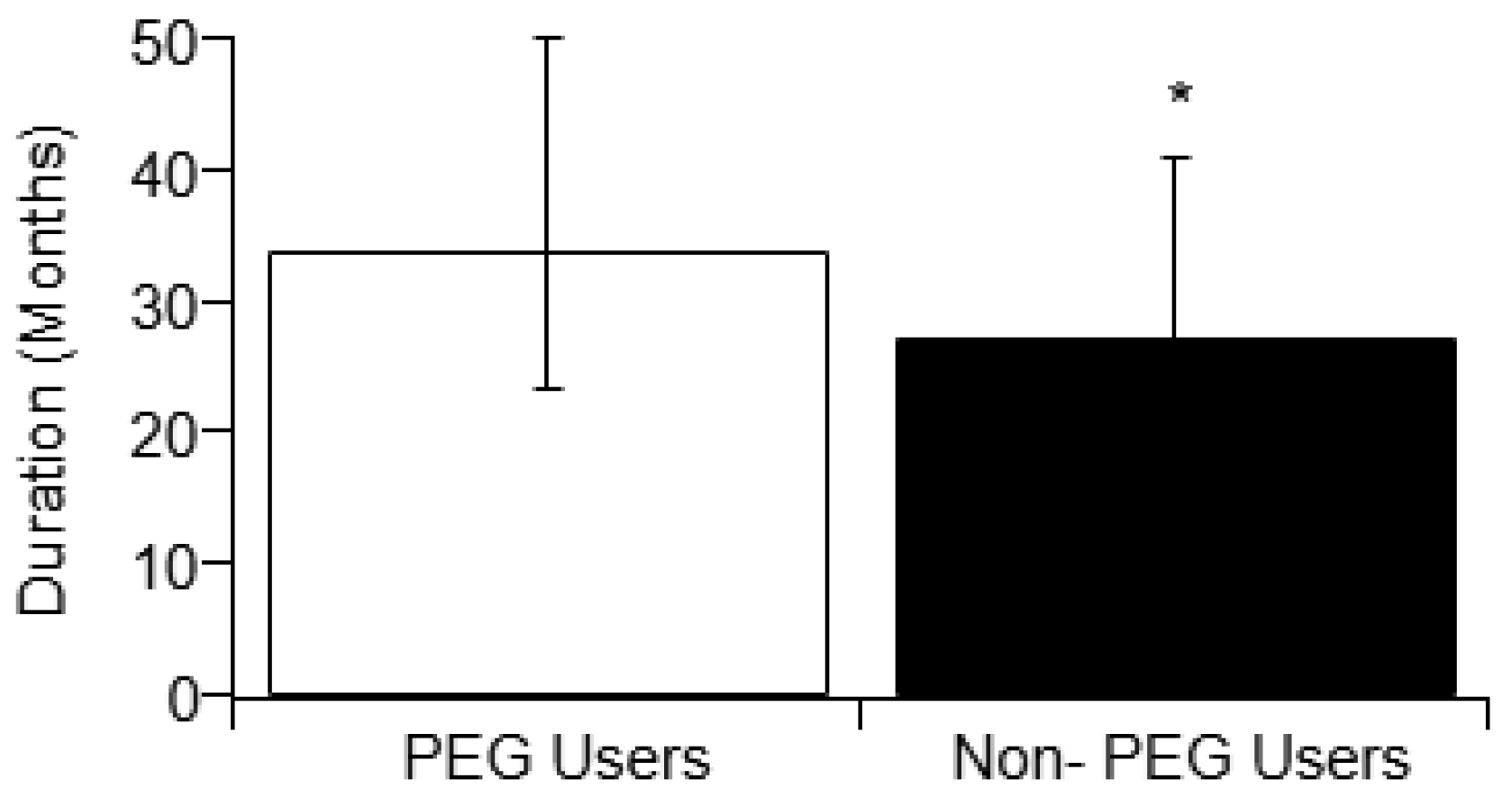
3.1. Assessment of Survival Duration
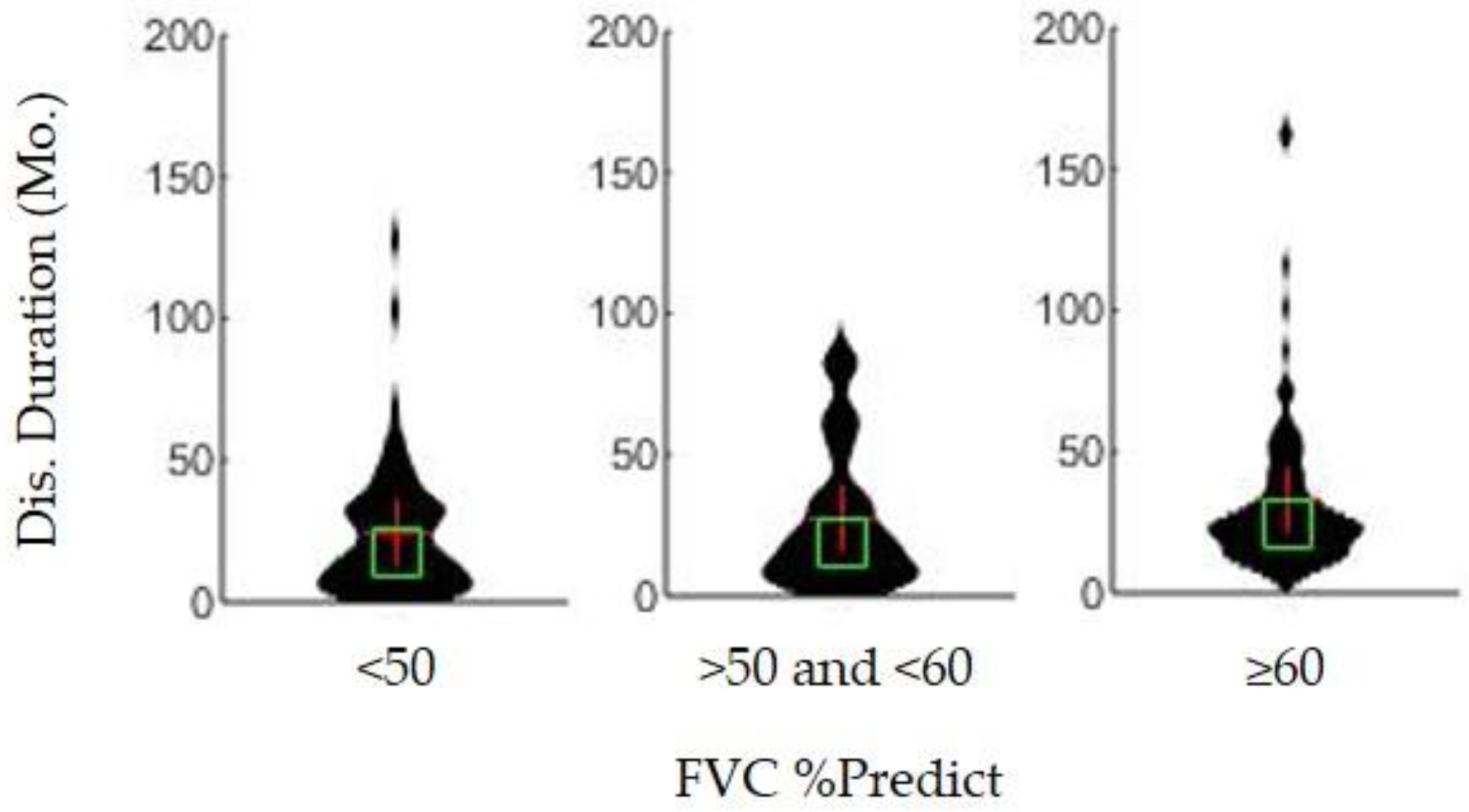
3.2. Assessment of FVC %Predict at PEG Placement
3.3. Timing of PEG Placement
3.4. Impact of PEG on Observed Patient Mood
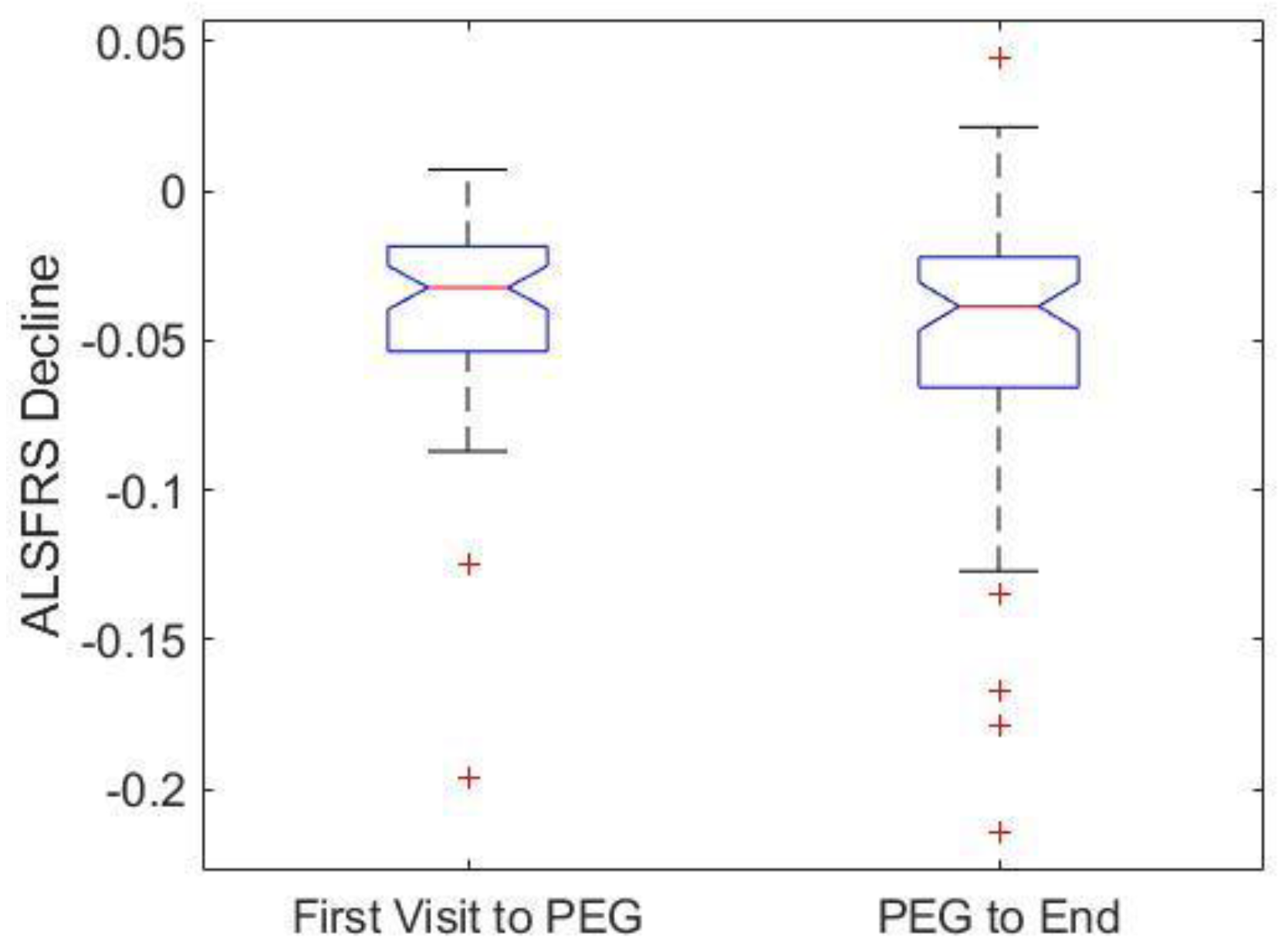
3.5. Impact of PEG on ALSFRS-R Decline
3.6. Impact of PEG on Body Weight and BMI
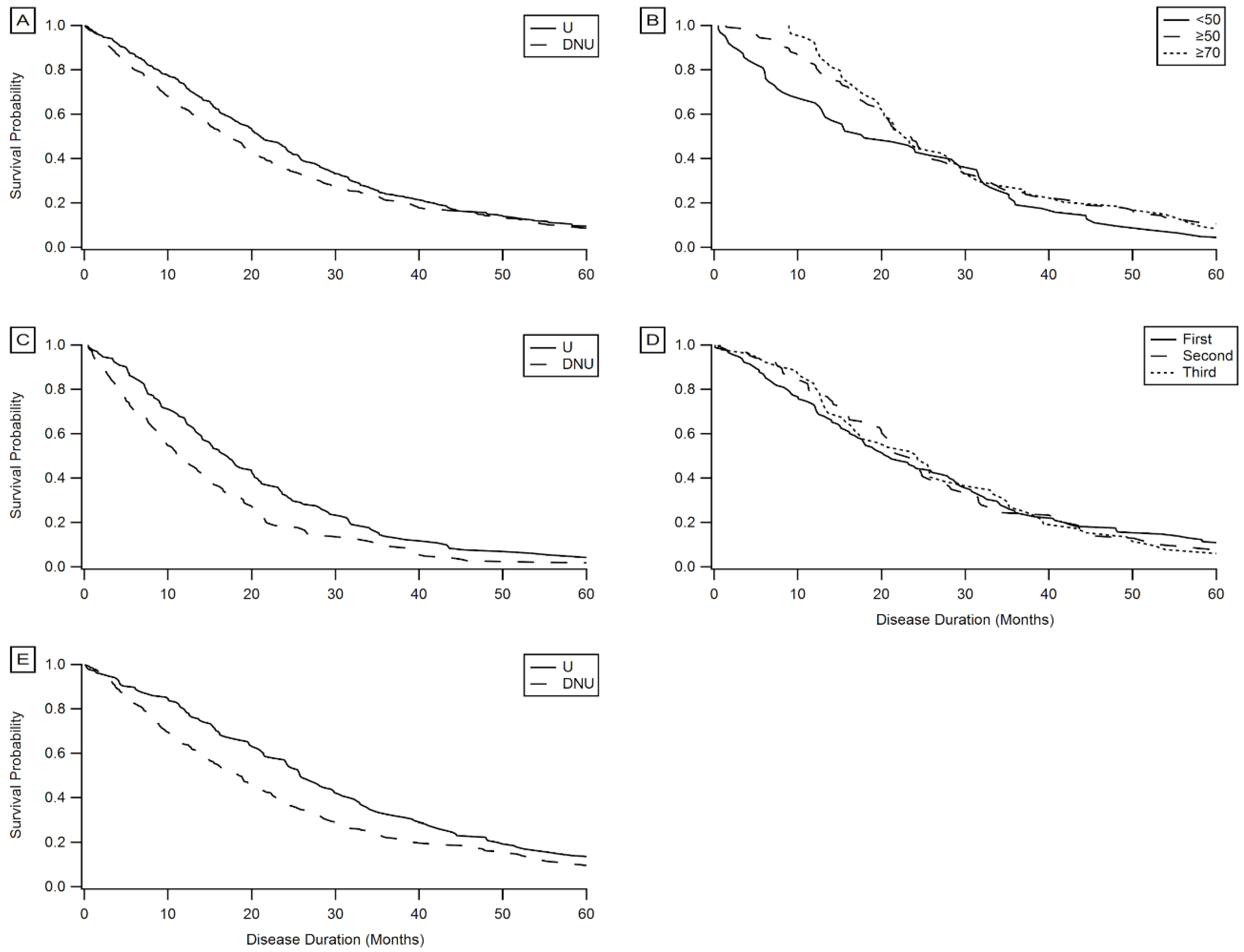
3.7. Kaplan–Meier Survival Analysis
3.8. Meta-Analysis of PEG Cohort Studies
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Czell, D.; Bauer, M.; Binek, J.; Schoch, O.D.; Weber, M. Outcomes of percutaneous endoscopic gastrostomy tube insertion in respiratory impaired amyotrophic lateral sclerosis patients under noninvasive ventilation. Respir. Care 2013, 58, 838–844. [Google Scholar] [PubMed]
- Yuruker, S.; Koca, B.; Karabicak, I.; Kuru, B.; Ozen, N. Percutaneous Endoscopic Gastrostomy: Technical Problems, Complications, and Management. Indian J. Surg. 2015, 77, 1159–1164. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rahnemai-Azar, A.A.; Rahnemaiazar, A.A.; Naghshizadian, R.; Kurtz, A.; Farkas, D.T. Percutaneous endoscopic gastrostomy: Indications, technique, complications and management. World J. Gastroenterol. 2014, 20, 7739–7751. [Google Scholar] [CrossRef] [PubMed]
- Sarkar, P.; Cole, A.; Scolding, N.J.; Rice, C.M. Percutaneous Endoscopic Gastrostomy Tube Insertion in Neurodegenerative Disease: A Retrospective Study and Literature Review. Clin. Endosc. 2017, 50, 270–278. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Spataro, R.F.L.; Piccoli, F.; La Bella, V. Percutaneous endoscopic gastrostomy in amyotrophic lateral sclerosis: Effect on survival. J. Neurol. Sci. 2011, 304, 44–48. [Google Scholar] [CrossRef]
- Kimyagarov, S.; Turgeman, D.; Fleissig, Y.; Klid, R.; Kopel, B.; Adunsky, A. Percutaneous endoscopic gastrostomy (PEG) tube feeding of nursing home residents is not associated with improved body composition parameters. J. Nutr. Health Aging 2013, 17, 162–165. [Google Scholar] [CrossRef]
- Limousin, N.; Blasco, H.; Corcia, P.; Gordon, P.H.; De Toffol, B.; Andres, C.; Praline, J. Malnutrition at the time of diagnosis is associated with a shorter disease duration in ALS. J. Neurol. Sci. 2010, 297, 36–39. [Google Scholar] [CrossRef]
- Ngo, S.; Steyn, F.; McCombe, P.; Ngo, S.; Steyn, F. Body mass index and dietary intervention: Implications for prognosis of amyotrophic lateral sclerosis. J. Neurol. Sci. 2014, 340, 5–12. [Google Scholar] [CrossRef] [Green Version]
- Nunes, G. Enteral feeding through endoscopic gastrostomy in amyotrophic lateral sclerosis patients. Nutr. Hosp. 2016, 33, 562. [Google Scholar] [CrossRef]
- Atassi, N.; Cudkowicz, M.E.; Schoenfeld, D.A. Advanced statistical methods to study the effects of gastric tube and non-invasive ventilation on functional decline and survival in amyotrophic lateral sclerosis. Amyotroph. Lateral Scler. 2011, 12, 272–277. [Google Scholar] [CrossRef] [Green Version]
- Cui, F.; Sun, L.; Xiong, J.; Li, J.; Zhao, Y.; Huang, X. Therapeutic effects of percutaneous endoscopic gastrostomy on survival in patients with amyotrophic lateral sclerosis: A meta-analysis. PLoS ONE 2018, 13, e0192243. [Google Scholar] [CrossRef] [PubMed]
- De Carvalho, M.; Gooch, C. The yin and yang of gastrostomy in the management of ALS Friend or foe? Am. Acad. Neurol. 2017, 89, 1–2. [Google Scholar]
- Bokuda, K.; Shimizu, T.; Imamura, K.; Kawata, A.; Watabe, K.; Hayashi, M.; Nakayama, Y.; Isozaki, E.; Nakano, I. Predictive factors for prognosis following unsedated percutaneous endoscopic gastrostomy in ALS patients. Muscle Nerve 2016, 54, 277–283. [Google Scholar] [CrossRef] [PubMed]
- Nagashima, K.; Furuta, N.; Makioka, K.; Fujita, Y.; Ikeda, M.; Ikeda, Y. An analysis of prognostic factors after percutaneous endoscopic gastrostomy placement in Japanese patients with amyotrophic lateral sclerosis. J. Neurol. Sci. 2017, 376, 202–205. [Google Scholar] [CrossRef] [PubMed]
- Castrillo-Viguera, C.; Grasso, D.L.; Simpson, E.; Shefner, J.; Cudkowicz, M.E. Clinical significance in the change of decline in ALSFRS-R. Amyotroph. Lateral Scler. 2010, 11, 178–180. [Google Scholar] [CrossRef] [PubMed]
- Cedarbaum, J.M.; Stambler, N.; Malta, E.; Fuller, C.; Hilt, D.; Thurmond, B.; Nakanishi, A. The ALSFRS-R: a revised ALS functional rating scale that incorporates assessments of respiratory function. J. Neurol. Sci. 1999, 169, 13–21. [Google Scholar] [CrossRef]
- Gordon, P.H.; Cheung, Y.K.; Kimura, F. Progression rate of ALSFRS-R at time of diagnosis predicts survival time in ALS. Neurology 2006, 67, 1314–1315. [Google Scholar] [CrossRef] [PubMed]
- Marin, B.; Couratier, P.; Arcuti, S.; Copetti, M.; Fontana, A.; Nicol, M.; Raymondeau, M.; Logroscino, G.; Preux, P.M. Stratification of ALS patients’ survival: a population-based study. J. Neurol. 2016, 263, 100–111. [Google Scholar] [CrossRef] [PubMed]
- Oliver, D.J.; Turner, M.R. Some difficult decisions in ALS/MND. Amyotroph. Lateral Scler. 2010, 11, 339–343. [Google Scholar] [CrossRef]
- Reich-Slotky, R.; Andrews, J.; Cheng, B.; Buchsbaum, R.; Levy, D.; Kaufmann, P.; Thompson, J.L.P. Body mass index (BMI) as predictor of ALSFRS-R score decline in ALS patients. Amyotroph. Lateral Scler. Front. Degener. 2013, 14, 212–216. [Google Scholar] [CrossRef]
- Mitchell, C.S.; Hollinger, S.K.; Goswami, S.D.; Polak, M.A.; Lee, R.H.; Glass, J.D. Antecedent disease is less prevalent in Amyotrophic Lateral Sclerosis. Neurodegener. Dis. 2015, 15, 109–113. [Google Scholar] [CrossRef] [PubMed]
- Hollinger, S.K.; Okosun, I.S.; Mitchell, C.S. Antecedent Disease and Amyotrophic Lateral Sclerosis: What Is Protecting Whom? Front. Neurol. 2016, 7, 47. [Google Scholar] [CrossRef]
- Pfohl, S.R.; Kim, R.B.; Coan, G.S.; Mitchell, C.S. Unraveling the Complexity of Amyotrophic Lateral Sclerosis Survival Prediction. Front. Aging Neurosci. 2018, 12, 36. [Google Scholar] [CrossRef]
- Coan, G.; Mitchell, C.S. An assessment of possible neuropathology and clinical relationships in 46 sporadic Amyotrophic Lateral Sclerosis patient autopsies. Neurodegener. Dis. 2015, 15, 301–312. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, C.S.; Cates, A.; Kim, R.B.; Hollinger, S.K. Undergraduate Biocuration: Developing Tomorrow’s Researchers While Mining Today’s Data. J. Undergrad. Neurosci. Educ. 2015, 14, A56–A65. [Google Scholar]
- Khamankar, N.; Coan, G.; Weaver, B.; Mitchell, C.S. Associative Increases in Amyotrophic Lateral Sclerosis Survival Duration With Non-invasive Ventilation Initiation and Usage Protocols. Front. Neurol. 2018, 9, 578. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bowen, G. An Analysis of Quality of Life (QoL) and Survival Impact in Amyotrophic Lateral Sclerosis (ALS) Patients. Bachelor Thesis, Biomedical Engineering, Georgia Institute of Technology, Atlanta, GA, USA, 2017. [Google Scholar]
- Procaccini, N.J.; Nemergut, E.C. Percutaneous Endoscopic Gastrostomy in the Patient with Amyotrophic Lateral Sclerosis: Risk vs Benefit? Pract. Gastroenterol. 2008, 60, 24–34. [Google Scholar]
- Burkhardt, C.C.N.; Sommacal, A.; Andersen, P.; Weber, M. Is survival improved by the use of NIV and PEG in amyotrophic lateral sclerosis (ALS)? A post-mortem study of 80 ALS patients. PLoS ONE 2017, 12, e0177555. [Google Scholar] [CrossRef]
- Chiò, A.; Galletti, R.; Finocchiaro, C.; Righi, D.; Ruffino, M.; Calvo, A.; Di, V.; Ghiglione, P.; Terreni, A.; Mutani, R. Percutaneous radiological gastrostomy: A safe and effective method of nutritional tube placement in advanced ALS. J. Neurol. Neurosurg. Psychiatry 2004, 75, 645–647. [Google Scholar] [CrossRef]
- Strong, M.R.A.; Rankin, R.N. Percutaneous gastrojejunostomy in amyotrophic lateral sclerosis. J. Neurol. Sci. 1999, 169, 128–132. [Google Scholar] [CrossRef]
- Mathus-Vliegen, L.L.L.; Merkus, M.P.; Tytgat, G.N.; Vianney de Jong, J.M. Percutaneous endoscopic gastrostomy in patients with amyotrophic lateral sclerosis and impaired pulmonary function. Gastrointest Endosc. 1994, 40, 463–469. [Google Scholar] [CrossRef]
- Forbes, R.B.; Colville, S.; Swingler, R.J. Scottish Motor Neurone Disease Research Group. Frequency, timing and outcome of gastrostomy tubes for amyotrophic lateral sclerosis/motor neurone disease--a record linkage study from the Scottish Motor Neurone Disease Register. J. Neurol. 2004, 251, 813–817. [Google Scholar] [CrossRef] [PubMed]
- Kurt, A.; Nijboer, F.; Matuz, T.; Kübler, A. Depression and anxiety in individuals with amyotrophic lateral sclerosis: Epidemiology and management. CNS Drugs 2007, 21, 279–291. [Google Scholar] [CrossRef] [PubMed]
- Lulé, D.; Häcker, S.; Ludolph, A.; Birbaumer, N.; Kübler, A. Depression and Quality of Life in Patients With Amyotrophic Lateral Sclerosis. Dtsch Arztebl Int. 2008, 105, 397–403. [Google Scholar]
- Bond, L.; Bernhardt, K.; Madria, P.; Sorrentino, K.; Scelsi, H.; Mitchell, C.S. A Metadata Analysis of Oxidative Stress Etiology in Preclinical Amyotrophic Lateral Sclerosis: Benefits of Antioxidant Therapy. Front. Mol. Neurosci. 2018, 12, 10. [Google Scholar] [CrossRef] [PubMed] [Green Version]

| ONSET TYPE | PEG User | PEG Non-User |
|---|---|---|
| Limb | 138 | 448 |
| Bulbar | 133 | 164 |
| Unclassifiable | 7 | 37 |
| Total | 278 | 649 |
| PEG Study | Sample Size | PEG Users | Non-Users | p Value | Disease Duration with PEG |
|---|---|---|---|---|---|
| Limousin, 2010 [7] | 63 | 33 | 30 | p = 0.02 | Significant Increase |
| Burkhardt, 2017 [29] | 71 | 46 | 25 | p < 0.01 | |
| Spataro, 2011 [5] | 150 | 76 | 74 | p = 0.05 | |
| Current study Bond, 2019 | 927 | 278 | 649 | p = 0.0001 | |
| Chiò, 2004 [30] | 50 | 25 | 25 | p = 0.004 | Significant Decrease |
| Strong, 1999 [31] | 366 | 73 | 293 | p = 0.001 | |
| Mathus-Vliegan, 1994 [32] | 68 | 13 | 10 | p = 0.6544 | Insignificant Increase |
| Forbes, 2004 [33] | 1226 | 142 | 1084 | p = 0.52 | |
| Aggregate Meta-Analysis | 1578 | 352 | 1226 | p = 0.0056 | Significant Increase |
| Parameter | Classification | Significant | p-Value |
|---|---|---|---|
| Disease Duration of PEG users vs. non-users | Limb Onset Bulbar Onset | Yes Yes | <<0.001 <<0.001 |
| Disease Duration of PEG users | Limb vs. bulbar onset | Yes | <<0.001 |
| ALSFRS-R decline in PEG Users vs. non-users | No | >0.05 | |
| Gait Score for PEG users | By PEG Placement Quartile | No | >0.05 |
| Body Mass Index (BMI) in PEG users | Prior to PEG Following PEG | Yes No | <0.05 >0.05 |
| Weight Change in PEG users | Prior to PEG Following PEG | Yes No | <0.05 >0.05 |
| Time of PEG Placement | By Placement Trimester By Placement Quartile | NoNo | >0.05 >0.05 |
| Clinical Impression of Mood (CIM) for PEG Users | By PEG Placement Quartile | No | >0.05 |
| FVC %predict for PEG users at PEG placement | 60% vs. <50% ≥50% vs <50% | Yes Yes | <0.05 <0.001 |
| Meta-Analysis Assessing Associative Benefit of PEG usage on ALS Patient Survival | Yes | <0.05 | |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bond, L.; Ganguly, P.; Khamankar, N.; Mallet, N.; Bowen, G.; Green, B.; Mitchell, C.S. A Comprehensive Examination of Percutaneous Endoscopic Gastrostomy and Its Association with Amyotrophic Lateral Sclerosis Patient Outcomes. Brain Sci. 2019, 9, 223. https://doi.org/10.3390/brainsci9090223
Bond L, Ganguly P, Khamankar N, Mallet N, Bowen G, Green B, Mitchell CS. A Comprehensive Examination of Percutaneous Endoscopic Gastrostomy and Its Association with Amyotrophic Lateral Sclerosis Patient Outcomes. Brain Sciences. 2019; 9(9):223. https://doi.org/10.3390/brainsci9090223
Chicago/Turabian StyleBond, Leila, Paulamy Ganguly, Nishad Khamankar, Nolan Mallet, Gloria Bowen, Braden Green, and Cassie S. Mitchell. 2019. "A Comprehensive Examination of Percutaneous Endoscopic Gastrostomy and Its Association with Amyotrophic Lateral Sclerosis Patient Outcomes" Brain Sciences 9, no. 9: 223. https://doi.org/10.3390/brainsci9090223
APA StyleBond, L., Ganguly, P., Khamankar, N., Mallet, N., Bowen, G., Green, B., & Mitchell, C. S. (2019). A Comprehensive Examination of Percutaneous Endoscopic Gastrostomy and Its Association with Amyotrophic Lateral Sclerosis Patient Outcomes. Brain Sciences, 9(9), 223. https://doi.org/10.3390/brainsci9090223