Frontotemporal Transcranial Direct Current Stimulation Decreases Serum Mature Brain-Derived Neurotrophic Factor in Schizophrenia
Abstract
1. Introduction
2. Materials and Methods
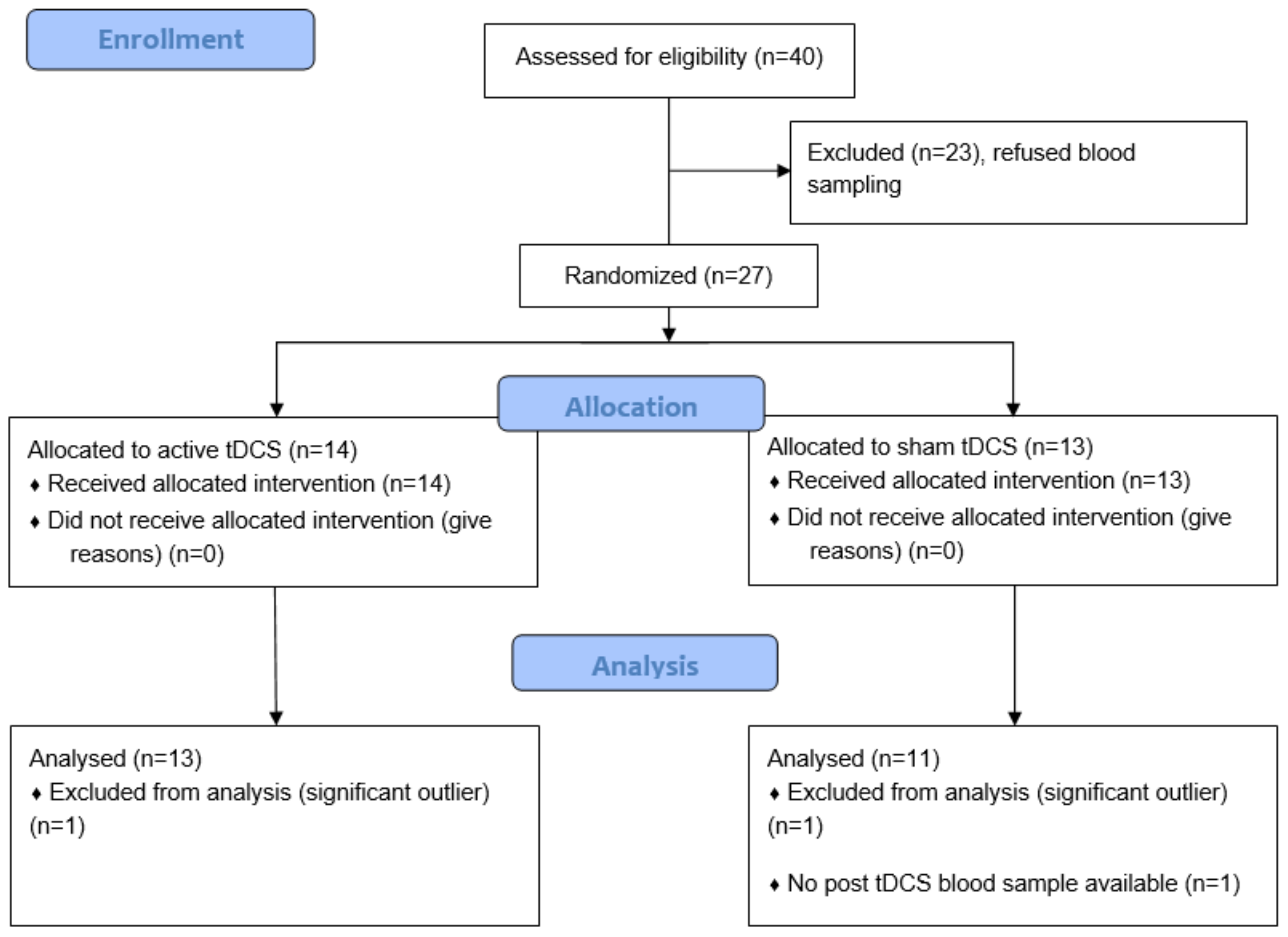
2.1. Study Design
2.2. Participants
2.3. tDCS Treatment
2.4. Measures of Serum BDNF
2.5. Statistical Analysis
3. Results
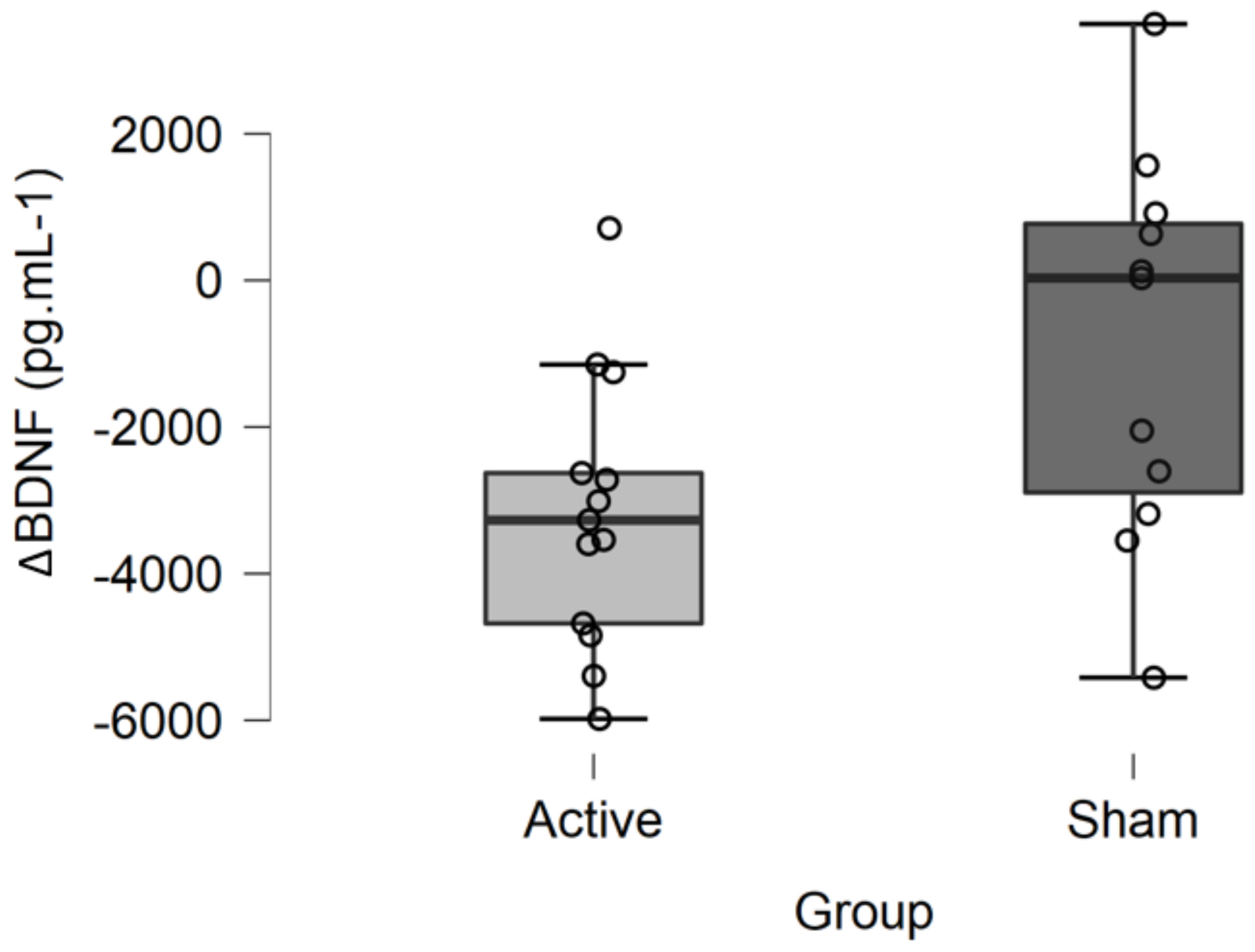
3.1. Effect of tDCS on mBDNF Levels
3.2. Tolerability and Blinding
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Mondino, M.; Sauvanaud, F.; Brunelin, J. A Review of the Effects of Transcranial Direct Current Stimulation for the Treatment of Hallucinations in Patients with Schizophrenia. J. ECT 2018, 34, 164–171. [Google Scholar] [CrossRef] [PubMed]
- Brunelin, J.; Mondino, M.; Gassab, L.; Haesebaert, F.; Gaha, L.; Suaud-Chagny, M.-F.; Saoud, M.; Mechri, A.; Poulet, E. Examining Transcranial Direct-Current Stimulation (TDCS) as a Treatment for Hallucinations in Schizophrenia. Am. J. Psychiatry 2012, 169, 719–724. [Google Scholar] [CrossRef] [PubMed]
- Fregni, F.; El-Hagrassy, M.M.; Pacheco-Barrios, K.; Carvalho, S.; Leite, J.; Simis, M.; Brunelin, J.; Nakamura-Palacios, E.M.; Marangolo, P.; Venkatasubramanian, G.; et al. Evidence-Based Guidelines and Secondary Meta-Analysis for the Use of Transcranial Direct Current Stimulation (TDCS) in Neurological and Psychiatric Disorders. Int. J. Neuropsychopharmacol. 2021, 24, 256–313. [Google Scholar] [CrossRef] [PubMed]
- Nitsche, M.A.; Paulus, W. Sustained Excitability Elevations Induced by Transcranial DC Motor Cortex Stimulation in Humans. Neurology 2001, 57, 1899–1901. [Google Scholar] [CrossRef]
- Keeser, D.; Meindl, T.; Bor, J.; Palm, U.; Pogarell, O.; Mulert, C.; Brunelin, J.; Möller, H.-J.; Reiser, M.; Padberg, F. Prefrontal Transcranial Direct Current Stimulation Changes Connectivity of Resting-State Networks during FMRI. J. Neurosci. 2011, 31, 15284–15293. [Google Scholar] [CrossRef]
- Fonteneau, C.; Redoute, J.; Haesebaert, F.; Le Bars, D.; Costes, N.; Suaud-Chagny, M.-F.; Brunelin, J. Frontal Transcranial Direct Current Stimulation Induces Dopamine Release in the Ventral Striatum in Human. Cereb. Cortex 2018, 28, 2636–2646. [Google Scholar] [CrossRef]
- Stagg, C.J.; Nitsche, M.A. Physiological Basis of Transcranial Direct Current Stimulation. Neuroscientist 2011, 17, 37–53. [Google Scholar] [CrossRef]
- Lu, B. BDNF and Activity-Dependent Synaptic Modulation. Learn. Mem. 2003, 10, 86–98. [Google Scholar] [CrossRef]
- Mowla, S.J.; Pareek, S.; Farhadi, H.F.; Petrecca, K.; Fawcett, J.P.; Seidah, N.G.; Morris, S.J.; Sossin, W.S.; Murphy, R.A. Differential Sorting of Nerve Growth Factor and Brain-Derived Neurotrophic Factor in Hippocampal Neurons. J. Neurosci. 1999, 19, 2069–2080. [Google Scholar] [CrossRef]
- Sasi, M.; Vignoli, B.; Canossa, M.; Blum, R. Neurobiology of Local and Intercellular BDNF Signaling. Pflug. Arch. Eur. J. Physiol. 2017, 469, 593–610. [Google Scholar] [CrossRef]
- Fritsch, B.; Reis, J.; Martinowich, K.; Schambra, H.M.; Ji, Y.; Cohen, L.G.; Lu, B. Direct Current Stimulation Promotes BDNF-Dependent Synaptic Plasticity: Potential Implications for Motor Learning. Neuron 2010, 66, 198–204. [Google Scholar] [CrossRef]
- Podda, M.V.; Cocco, S.; Mastrodonato, A.; Fusco, S.; Leone, L.; Barbati, S.A.; Colussi, C.; Ripoli, C.; Grassi, C. Anodal Transcranial Direct Current Stimulation Boosts Synaptic Plasticity and Memory in Mice via Epigenetic Regulation of Bdnf Expression. Sci. Rep. 2016, 6, 1–19. [Google Scholar] [CrossRef]
- Eskandari, Z.; Dadashi, M.; Mostafavi, H.; Armani Kia, A.; Pirzeh, R. Comparing the Efficacy of Anodal, Cathodal, and Sham Transcranial Direct Current Stimulation on Brain-Derived Neurotrophic Factor and Psychological Symptoms in Opioid-Addicted Patients. Basic Clin. Neurosci. 2019, 10, 641–650. [Google Scholar] [CrossRef]
- Hadoush, H.; Banihani, S.A.; Khalil, H.; Al-Qaisi, Y.; Al-Sharman, A.; Al-Jarrah, M. Dopamine, BDNF and Motor Function Postbilateral Anodal Transcranial Direct Current Stimulation in Parkinson’s Disease. Neurodegener. Dis. Manag. 2018, 8, 171–179. [Google Scholar] [CrossRef]
- Palm, U.; Fintescu, Z.; Obermeier, M.; Schiller, C.; Reisinger, E.; Keeser, D.; Pogarell, O.; Bondy, B.; Zill, P.; Padberg, F. Serum Levels of Brain-Derived Neurotrophic Factor Are Unchanged after Transcranial Direct Current Stimulation in Treatment-Resistant Depression. J. Affect. Disord. 2013, 150, 659–663. [Google Scholar] [CrossRef]
- Brunoni, A.R.; Padberg, F.; Vieira, E.L.M.; Teixeira, A.L.; Carvalho, A.F.; Lotufo, P.A.; Gattaz, W.F.; Benseñor, I.M. Plasma Biomarkers in a Placebo-Controlled Trial Comparing TDCS and Escitalopram Efficacy in Major Depression. Prog. Neuro-Psychopharmacol. Biol. Psychiatry 2018, 86, 211–217. [Google Scholar] [CrossRef]
- Goerigk, S.; Cretaz, E.; Sampaio-Junior, B.; Vieira, É.L.M.; Gattaz, W.; Klein, I.; Lafer, B.; Teixeira, A.L.; Carvalho, A.F.; Lotufo, P.A.; et al. Effects of TDCS on Neuroplasticity and Inflammatory Biomarkers in Bipolar Depression: Results from a Sham-Controlled Study. Prog. Neuro-Psychopharmacol. Biol. Psychiatry 2021, 105, 110119. [Google Scholar] [CrossRef]
- Wang, M.; Xie, Y.; Qin, D. Proteolytic Cleavage of ProBDNF to MBDNF in Neuropsychiatric and Neurodegenerative Diseases. Brain Res. Bull. 2020, 172–184. [Google Scholar] [CrossRef]
- Ambigapathy, G.; Zheng, Z.; Li, W.; Keifer, J. Identification of a Functionally Distinct Truncated BDNF MRNA Splice Variant and Protein in Trachemys scripta elegans. PLoS ONE 2013, 8, e67141. [Google Scholar] [CrossRef]
- Woo, N.H.; Teng, H.K.; Siao, C.-J.; Chiaruttini, C.; Pang, P.T.; Milner, T.A.; Hempstead, B.L.; Lu, B. Activation of P75 NTR by ProBDNF Facilitates Hippocampal Long-Term Depression. Nat. Neurosci. 2005, 8, 1069–1077. [Google Scholar] [CrossRef]
- Koshimizu, H.; Kiyosue, K.; Hara, T.; Hazama, S.; Suzuki, S.; Uegaki, K.; Nagappan, G.; Zaitsev, E.; Hirokawa, T.; Tatsu, Y.; et al. Multiple Functions of Precursor BDNF to CNS Neurons: Negative Regulation of Neurite Growth, Spine Formation and Cell Survival. Mol. Brain 2009, 2, 27. [Google Scholar] [CrossRef] [PubMed]
- Teng, H.K.; Teng, K.K.; Lee, R.; Wright, S.; Tevar, S.; Almeida, R.D.; Kermani, P.; Torkin, R.; Chen, Z.-Y.; Lee, F.S.; et al. ProBDNF Induces Neuronal Apoptosis via Activation of a Receptor Complex of P75NTR and Sortilin. J. Neurosci. 2005, 25, 5455–5463. [Google Scholar] [CrossRef] [PubMed]
- Rösch, H.; Schweigreiter, R.; Bonhoeffer, T.; Barde, Y.-A.; Korte, M. The Neurotrophin Receptor P75NTR Modulates Long-Term Depression and Regulates the Expression of AMPA Receptor Subunits in the Hippocampus. Proc. Natl. Acad. Sci. USA 2005, 102, 7362–7367. [Google Scholar] [CrossRef] [PubMed]
- Kowiański, P.; Lietzau, G.; Czuba, E.; Waśkow, M.; Steliga, A.; Moryś, J. BDNF: A Key Factor with Multipotent Impact on Brain Signaling and Synaptic Plasticity. Cell Mol. Neurobiol. 2018, 38, 579–593. [Google Scholar] [CrossRef] [PubMed]
- Pang, P.T.; Teng, H.K.; Zaitsev, E.; Woo, N.T.; Sakata, K.; Zhen, S.; Teng, K.K.; Yung, W.-H.; Hempstead, B.L.; Lu, B. Cleavage of ProBDNF by TPA/Plasmin Is Essential for Long-Term Hippocampal Plasticity. Science 2004, 306, 487–491. [Google Scholar] [CrossRef] [PubMed]
- Patterson, S.L.; Abel, T.; Deuel, T.A.S.; Martin, K.C.; Rose, J.C.; Kandel, E.R. Recombinant BDNF Rescues Deficits in Basal Synaptic Transmission and Hippocampal LTP in BDNF Knockout Mice. Neuron 1996, 16, 1137–1145. [Google Scholar] [CrossRef]
- Deinhardt, K.; Chao, M.V. Shaping Neurons: Long and Short Range Effects of Mature and ProBDNF Signalling upon Neuronal Structure. Neuropharmacology 2014, 76, 603–609. [Google Scholar] [CrossRef]
- Lommatzsch, M.; Zingler, D.; Schuhbaeck, K.; Schloetcke, K.; Zingler, C.; Schuff-Werner, P.; Virchow, J.C. The Impact of Age, Weight and Gender on BDNF Levels in Human Platelets and Plasma. Neurobiol. Aging 2005, 26, 115–123. [Google Scholar] [CrossRef]
- Ozan, E.; Okur, H.; Eker, C.; Eker, Ö.; Gönül, A.S.; Akarsu, N. The Effect of Depression, BDNF Gene Val66met Polymorphism and Gender on Serum BDNF Levels. Brain Res. Bull. 2010, 81, 61–65. [Google Scholar] [CrossRef]
- Fernandes, B.S.; Steiner, J.; Berk, M.; Molendijk, M.L.; Gonzalez-Pinto, A.; Turck, C.W.; Nardin, P.; Gonçalves, C.-A. Peripheral Brain-Derived Neurotrophic Factor in Schizophrenia and the Role of Antipsychotics: Meta-Analysis and Implications. Mol. Psychiatry 2015, 20, 1108–1119. [Google Scholar] [CrossRef]
- Nagappan, G.; Zaitsev, E.; Senatorov, V.V.; Yang, J.; Hempstead, B.L.; Lu, B. Control of Extracellular Cleavage of ProBDNF by High Frequency Neuronal Activity. Proc. Natl. Acad. Sci. USA 2009, 106, 1267–1272. [Google Scholar] [CrossRef]
- Gardner, D.M.; Murphy, A.L.; O’Donnell, H.; Centorrino, F.; Baldessarini, R.J. International Consensus Study of Antipsychotic Dosing. Am. J. Psychiatry 2010, 167, 686–693. [Google Scholar] [CrossRef] [PubMed]
- Brunelin, J.; Hasan, A.; Haesebaert, F.; Nitsche, M.A.; Poulet, E. Nicotine Smoking Prevents the Effects of Frontotemporal Transcranial Direct Current Stimulation (TDCS) in Hallucinating Patients with Schizophrenia. Brain Stimul. 2015, 8, 1225–1227. [Google Scholar] [CrossRef] [PubMed]
- Gaede, G.; Hellweg, R.; Zimmermann, H.; Brandt, A.U.; Dörr, J.; Bellmann-Strobl, J.; Zangen, A.; Paul, F.; Pfueller, C.F. Effects of Deep Repetitive Transcranial Magnetic Stimulation on Brain-Derived Neurotrophic Factor Serum Concentration in Healthy Volunteers. Neuropsychobiology 2014, 69, 112–119. [Google Scholar] [CrossRef]
- Schaller, G.; Sperling, W.; Richter-Schmidinger, T.; Mühle, C.; Heberlein, A.; Maihöfner, C.; Kornhuber, J.; Lenz, B. Serial Repetitive Transcranial Magnetic Stimulation (RTMS) Decreases BDNF Serum Levels in Healthy Male Volunteers. J. Neural. Transm. 2014, 121, 307–313. [Google Scholar] [CrossRef]
- Angelucci, F.; Oliviero, A.; Pilato, F.; Saturno, E.; Dileone, M.; Versace, V.; Musumeci, G.; Batocchi, A.P.; Tonali, P.A.; Lazzaro, V.D. Transcranial Magnetic Stimulation and BDNF Plasma Levels in Amyotrophic Lateral Sclerosis. NeuroReport 2004, 15, 717–720. [Google Scholar] [CrossRef]
- Lang, U.E.; Bajbouj, M.; Gallinat, J.; Hellweg, R. Brain-Derived Neurotrophic Factor Serum Concentrations in Depressive Patients during Vagus Nerve Stimulation and Repetitive Transcranial Magnetic Stimulation. Psychopharmacology 2006, 187, 56–59. [Google Scholar] [CrossRef]
- Zhao, X.; Li, Y.; Tian, Q.; Zhu, B.; Zhao, Z. Repetitive Transcranial Magnetic Stimulation Increases Serum Brain-Derived Neurotrophic Factor and Decreases Interleukin-1β and Tumor Necrosis Factor-α in Elderly Patients with Refractory Depression. J. Int. Med. Res. 2019, 47, 1848–1855. [Google Scholar] [CrossRef]
- Monte-Silva, K.; Kuo, M.-F.; Liebetanz, D.; Paulus, W.; Nitsche, M.A. Shaping the Optimal Repetition Interval for Cathodal Transcranial Direct Current Stimulation (TDCS). J. Neurophysiol. 2010, 103, 1735–1740. [Google Scholar] [CrossRef]
- Alonzo, A.; Brassil, J.; Taylor, J.L.; Martin, D.; Loo, C.K. Daily Transcranial Direct Current Stimulation (TDCS) Leads to Greater Increases in Cortical Excitability than Second Daily Transcranial Direct Current Stimulation. Brain Stimul. 2012, 5, 208–213. [Google Scholar] [CrossRef]
- Paulus, W. Transcranial Electric and Magnetic Stimulation. Brain Stimul. 2013, 116, 329–342. [Google Scholar]
- Stagg, C.J.; Antal, A.; Nitsche, M.A. Physiology of Transcranial Direct Current Stimulation. J. ECT 2018, 34, 144–152. [Google Scholar] [CrossRef] [PubMed]
- Green, M.J.; Matheson, S.L.; Shepherd, A.; Weickert, C.S.; Carr, V.J. Brain-Derived Neurotrophic Factor Levels in Schizophrenia: A Systematic Review with Meta-Analysis. Mol. Psychiatry 2011, 16, 960–972. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, A.O.; Kramer, S.; Hofman, N.; Flynn, J.; Hansen, M.; Martin, V.; Pillai, A.; Buckley, P.F. A Meta-Analysis of Brain-Derived Neurotrophic Factor Effects on Brain Volume in Schizophrenia: Genotype and Serum Levels. Neuropsychobiology 2021, 11, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Leßmann, V.; Brigadski, T. Mechanisms, Locations, and Kinetics of Synaptic BDNF Secretion: An Update. Neurosci. Res. 2009, 65, 11–22. [Google Scholar] [CrossRef]
- Vallence, A.M.; Ridding, M.C. Non-Invasive Induction of Plasticity in the Human Cortex: Uses and Limitations. Cortex 2014, 58, 261–271. [Google Scholar] [CrossRef]
- McClintock, S.M.; Martin, D.M.; Lisanby, S.H.; Alonzo, A.; McDonald, W.M.; Aaronson, S.T.; Husain, M.M.; O’Reardon, J.P.; Weickert, C.S.; Mohan, A.; et al. Neurocognitive Effects of Transcranial Direct Current Stimulation (TDCS) in Unipolar and Bipolar Depression: Findings from an International Randomized Controlled Trial. Depress. Anxiety 2020, 37, 261–272. [Google Scholar] [CrossRef]
- Strube, W.; Nitsche, M.A.; Wobrock, T.; Bunse, T.; Rein, B.; Herrmann, M.; Schmitt, A.; Nieratschker, V.; Witt, S.H.; Rietschel, M.; et al. BDNF-Val66Met-Polymorphism Impact on Cortical Plasticity in Schizophrenia Patients: A Proof-of-Concept Study. Int. J. Neuropsychopharmacol. 2015, 18, pyu040. [Google Scholar] [CrossRef]
- Grillo, R.W.; Ottoni, G.L.; Leke, R.; Souza, D.O.; Portela, L.V.; Lara, D.R. Reduced Serum BDNF Levels in Schizophrenic Patients on Clozapine or Typical Antipsychotics. J. Psychiatr. Res. 2007, 41, 31–35. [Google Scholar] [CrossRef]
- Bosse, K.E.; Maina, F.K.; Birbeck, J.A.; France, M.M.; Roberts, J.J.P.; Colombo, M.L.; Mathews, T.A. Aberrant Striatal Dopamine Transmitter Dynamics in Brain-Derived Neurotrophic Factor-Deficient Mice. J. Neurochem. 2012, 120, 385–395. [Google Scholar] [CrossRef]
- Filho, P.R.M.; Vercelino, R.; Cioato, S.G.; Medeiros, L.F.; de Oliveira, C.; Scarabelot, V.L.; Souza, A.; Rozisky, J.R.; Quevedo, A.d.S.; Adachi, L.N.S.; et al. Transcranial Direct Current Stimulation (TDCS) Reverts Behavioral Alterations and Brainstem BDNF Level Increase Induced by Neuropathic Pain Model: Long-Lasting Effect. Prog. Neuro-Psychopharmacol. Biol. Psychiatry 2016, 64, 44–51. [Google Scholar] [CrossRef]
- Klein, A.B.; Williamson, R.; Santini, M.A.; Clemmensen, C.; Ettrup, A.; Rios, M.; Knudsen, G.M.; Aznar, S. Blood BDNF Concentrations Reflect Brain-Tissue BDNF Levels across Species. Int. J. Neuropsychopharmacol. 2011, 14, 347–353. [Google Scholar] [CrossRef]
- Pan, W.; Banks, W.A.; Fasold, M.B.; Bluth, J.; Kastin, A.J. Transport of Brain-Derived Neurotrophic Factor across the Blood–Brain Barrier. Neuropharmacology 1998, 37, 1553–1561. [Google Scholar] [CrossRef]
- Sartorius, A.; Hellweg, R.; Litzke, J.; Vogt, M.; Dormannn, C.; Vollmayr, B.; Danker-Hopfe, H.; Gass, P. Correlations and Discrepancies between Serum and Brain Tissue Levels of Neurotrophins after Electroconvulsive Treatment in Rats. Pharmacopsychiatry 2009, 270–276. [Google Scholar] [CrossRef]
- Egan, M.F.; Kojima, M.; Callicott, J.H.; Goldberg, T.E.; Kolachana, B.S.; Bertolino, A.; Zaitsev, E.; Gold, B.; Goldman, D.; Dean, M.; et al. The BDNF Val66met Polymorphism Affects Activity-Dependent Secretion of BDNF and Human Memory and Hippocampal Function. Cell 2003, 112, 257–269. [Google Scholar] [CrossRef]
- Chen, Z.-Y.; Patel, P.D.; Sant, G.; Meng, C.-X.; Teng, K.K.; Hempstead, B.L.; Lee, F.S. Variant Brain-Derived Neurotrophic Factor (BDNF) (Met66) Alters the Intracellular Trafficking and Activity-Dependent Secretion of Wild-Type BDNF in Neuro-secretory Cells and Cortical Neurons. J. Neurosci. 2004, 24, 4401–4411. [Google Scholar] [CrossRef]
| Active Group (Mean ± SD) | Sham Group (Mean ± SD) | p-Value | |
|---|---|---|---|
| n total | 13 | 11 | |
| Age (years) | 33.08 ± 8.96 | 37.18 ± 9.38 | 0.285 |
| Illness duration (years) | 10.38 ± 9.51 | 14.73 ± 7.79 | 0.132 |
| Sex (n) | 6F/7M | 5F/6M | 0.973 |
| (%) | 46%/54% | 45%/55% | |
| Handedness (n) | 11R/1L/1 both | 9R/2L | 0.484 |
| Smokers (%) | 58% | 40% | 0.392 |
| Alcohol intake 1 (%) | 0% | 9% | 0.267 |
| Physical exercise 1 (%) | 8% | 9% | 0.902 |
| PANSS Total | 66.00 ± 14.89 | 69.78 ± 14.89 | 0.565 |
| PANSS Positive | 18.00 ± 4.81 | 19.44 ± 3.47 | 0.450 |
| PANSS Negative | 19.00 ± 5.63 | 17.33 ± 5.31 | 0.493 |
| PANSS General | 29.00 ± 5.31 | 33.00 ± 7.62 | 0.262 |
| mBDNF (pg·mL−1) | 16,510.80 ± 4346.98 | 13,257.50 ± 3274.58 | 0.054 |
| Antipsychotic dose (CPZeq) | 930.41 ± 415.13 | 1192.91 ± 449.45 | 0.151 |
| Molecule | |||
| Typical antipsychotics | 4 | 2 | 0.649 |
| Atypical antipsychotics | 12 | 11 | 1.000 |
| Clozapine | 4 | 4 | 1.000 |
| Antidepressants | 3 | 4 | 0.659 |
| Benzodiazepines | 5 | 2 | 0.386 |
| Anxiolytics | 3 | 6 | 0.206 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Adam, O.; Psomiades, M.; Rey, R.; Mandairon, N.; Suaud-Chagny, M.-F.; Mondino, M.; Brunelin, J. Frontotemporal Transcranial Direct Current Stimulation Decreases Serum Mature Brain-Derived Neurotrophic Factor in Schizophrenia. Brain Sci. 2021, 11, 662. https://doi.org/10.3390/brainsci11050662
Adam O, Psomiades M, Rey R, Mandairon N, Suaud-Chagny M-F, Mondino M, Brunelin J. Frontotemporal Transcranial Direct Current Stimulation Decreases Serum Mature Brain-Derived Neurotrophic Factor in Schizophrenia. Brain Sciences. 2021; 11(5):662. https://doi.org/10.3390/brainsci11050662
Chicago/Turabian StyleAdam, Ondine, Marion Psomiades, Romain Rey, Nathalie Mandairon, Marie-Francoise Suaud-Chagny, Marine Mondino, and Jerome Brunelin. 2021. "Frontotemporal Transcranial Direct Current Stimulation Decreases Serum Mature Brain-Derived Neurotrophic Factor in Schizophrenia" Brain Sciences 11, no. 5: 662. https://doi.org/10.3390/brainsci11050662
APA StyleAdam, O., Psomiades, M., Rey, R., Mandairon, N., Suaud-Chagny, M.-F., Mondino, M., & Brunelin, J. (2021). Frontotemporal Transcranial Direct Current Stimulation Decreases Serum Mature Brain-Derived Neurotrophic Factor in Schizophrenia. Brain Sciences, 11(5), 662. https://doi.org/10.3390/brainsci11050662






