Physical Activity and Inhibitory Control: The Mediating Role of Sleep Quality and Sleep Efficiency
Abstract
1. Introduction
2. Methods
2.1. Participants
2.2. Demographic Information
2.3. International Physical Activity Questionnaire
2.4. Pittsburgh Sleep Quality Index Scale
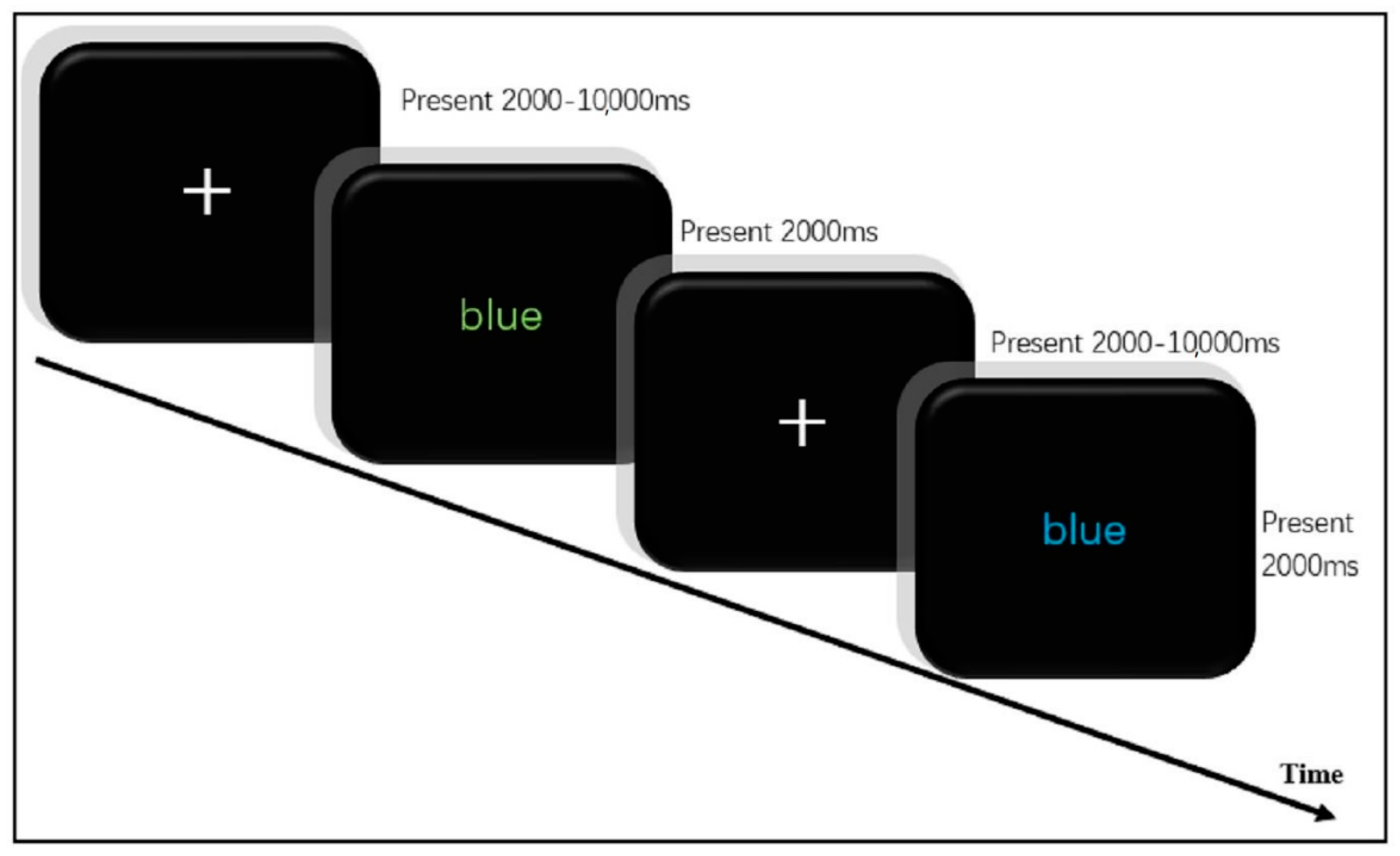
2.5. Measurement of Inhibitory Control Performance
2.6. Statistical Analysis
3. Results
3.1. Correlation Analysis
3.2. Multiple Mediation Model
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Erickson, K.I.; Hillman, C.; Stillman, C.M.; Ballard, R.M.; Bloodgood, B.; Conroy, D.E.; Macko, R.; Marquez, D.X.; Petruzzello, S.J.; Powell, K.E. Physical Activity, Cognition, and Brain Outcomes: A Review of the 2018 Physical Activity Guidelines. Med. Sci. Sports Exerc. 2019, 51, 1242–1251. [Google Scholar] [CrossRef]
- Garber, C.E.; Blissmer, B.; Deschenes, M.R.; Franklin, B.A.; Lamonte, M.J.; Lee, I.-M.; Nieman, D.C.; Swain, D.P. American College of Sports Medicine position stand. Quantity and quality of exercise for developing and maintaining cardiorespiratory, musculoskeletal, and neuromotor fitness in apparently healthy adults: Guidance for prescribing exercise. Med. Sci. Sports Exerc. 2011, 43, 1334–1359. [Google Scholar] [CrossRef]
- Verburgh, L.; Königs, M.; Scherder, E.J.; Oosterlaan, J.J. Physical exercise and executive functions in preadolescent children, adolescents and young adults: A meta-analysis. Br. J. Sports Med. 2014, 48, 973–979. [Google Scholar] [CrossRef]
- Li, J.W.; O’Connor, H.; O’Dwyer, N.; Orr, R. The effect of acute and chronic exercise on cognitive function and academic performance in adolescents: A systematic review. J. Sci. Med. Sport 2017, 20, 841–848. [Google Scholar] [CrossRef]
- Xue, Y.; Yang, Y.; Huang, T. Effects of chronic exercise interventions on executive function among children and adolescents: A systematic review with meta-analysis. Br. J. Sports Med. 2019, 53, 1397–1404. [Google Scholar] [CrossRef]
- Miyake, A.; Friedman, N.; Emerson, M.J.; Witzki, A.H.; Howerter, A.; Wager, T.D. The Unity and Diversity of Executive Functions and Their Contributions to Complex “Frontal Lobe” Tasks: A Latent Variable Analysis. Cogn. Psychol. 2000, 41, 49–100. [Google Scholar] [CrossRef]
- Lenroot, R.K.; Giedd, J.N. Brain development in children and adolescents: Insights from anatomical magnetic resonance imaging. Neurosci. Biobehav. Rev. 2006, 30, 718–729. [Google Scholar] [CrossRef]
- Whitford, T.J.; Rennie, C.J.; Grieve, S.M.; Clark, C.R.; Gordon, E.; Williams, L.M. Brain maturation in adolescence: Concurrent changes in neuroanatomy and neurophysiology. Hum. Brain Mapp. 2006, 28, 228–237. [Google Scholar] [CrossRef]
- Lebel, C.; Walker, L.; Leemans, A.; Phillips, L.; Beaulieu, C. Microstructural maturation of the human brain from childhood to adulthood. NeuroImage 2008, 40, 1044–1055. [Google Scholar] [CrossRef]
- Tamnes, C.K.; Herting, M.M.; Goddings, A.-L.; Meuwese, R.; Blakemore, S.-J.; Dahl, R.E.; Güroğlu, B.; Raznahan, A.; Sowell, E.R.; Crone, E.; et al. Development of the Cerebral Cortex across Adolescence: A Multisample Study of Inter-Related Longitudinal Changes in Cortical Volume, Surface Area, and Thickness. J. Neurosci. 2017, 37, 3402–3412. [Google Scholar] [CrossRef]
- Diamond, A.; Lee, K. Interventions Shown to Aid Executive Function Development in Children 4 to 12 Years Old. Science 2011, 333, 959–964. [Google Scholar] [CrossRef]
- Stillman, C.M.; Cohen, J.; Lehman, M.E.; Erickson, K.I. Mediators of Physical Activity on Neurocognitive Function: A Review at Multiple Levels of Analysis. Front. Hum. Neurosci. 2016, 10, 626. [Google Scholar] [CrossRef]
- Wong, M.L.; Lau, E.Y.Y.; Wan, J.H.Y.; Cheung, S.F.; Hui, C.H.; Mok, D.S.Y. The interplay between sleep and mood in predicting academic functioning, physical health and psychological health: A longitudinal study. J. Psychosom. Res. 2013, 74, 271–277. [Google Scholar] [CrossRef]
- King, A.C.; Oman, R.F.; Brassington, G.S.; Bliwise, D.L.; Haskell, W.L. Moderate-intensity exercise and self-rated quality of sleep in older adults. A randomized controlled trial. JAMA 1997, 277, 32–37. [Google Scholar] [CrossRef]
- Singh, N.A.; Clements, K.M.; Fiatarone, M.A. Sleep, Sleep Deprivation, and Daytime Activities–A Randomized Controlled Trial of the Effect of Exercise on Sleep. Sleep 1997, 20, 95–101. [Google Scholar] [CrossRef] [PubMed]
- Vanderlinden, J.; Boen, F.; Van Uffelen, J.G.Z. Effects of physical activity programs on sleep outcomes in older adults: A systematic review. Int. J. Behav. Nutr. Phys. Act. 2020, 17, 11. [Google Scholar] [CrossRef]
- Lins-Filho, O.L.; Pedrosa, R.P.; Gomes, J.M.; Moraes, S.L.D.; Vasconcelos, B.C.E.; Lemos, C.A.A.; Pellizzer, E.P. Effect of exercise training on subjective parameters in patients with obstructive sleep apnea: A systematic review and meta-analysis. Sleep Med. 2020, 69, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Lo, J.C.; Groeger, J.; Cheng, G.H.; Dijk, D.-J.; Chee, M.W. Self-reported sleep duration and cognitive performance in older adults: A systematic review and meta-analysis. Sleep Med. 2016, 17, 87–98. [Google Scholar] [CrossRef]
- Naismith, S.L.; Mowszowski, L.J. Sleep disturbance in mild cognitive impairment: A systematic review of recent findings. Curr. Opin. Psychiatry 2018, 31, 153–159. [Google Scholar] [CrossRef]
- Smithies, T.D.; Toth, A.J.; Dunican, I.C.; Caldwell, J.A.; Kowal, M.; Campbell, M.J. The Effect of Sleep Restriction on Cognitive Performance in Elite Cognitive Performers: A Systematic Review. Sleep 2021. [Google Scholar] [CrossRef]
- Benitez, A.; Gunstad, J. Poor sleep quality diminishes cognitive functioning independent of depression and anxiety in healthy young adults. Clin. Neuropsychol. 2012, 26, 214–223. [Google Scholar] [CrossRef]
- Horn, J.A. Human sleep, sleep loss and behavior. Implications for the prefrontal cortex and psychiatric behavior. Br. J. Psychiatry 1993, 162, 413–419. [Google Scholar] [CrossRef]
- Harrison, Y.; Horne, J.A. Sleep loss impairs short and novel language tasks having a prefrontal focus. J. Sleep Res. 1998, 7, 95–100. [Google Scholar] [CrossRef]
- Harrison, Y.; Horne, J.A.; Rothwell, A. Prefrontal Neuropsychological Effects of Sleep Deprivation in Young Adults—A Model for Healthy Aging? Sleep 2000, 23, 1067–1073. [Google Scholar] [CrossRef]
- Muzur, A.; Pace-Schott, E.F.; Hobson, J. The prefrontal cortex in sleep. Trends Cogn. Sci. 2002, 6, 475–481. [Google Scholar] [CrossRef]
- Wilckens, K.A.; Erickson, K.I.; Wheeler, M.E. Physical Activity and Cognition: A Mediating Role of Efficient Sleep. Behav. Sleep Med. 2018, 16, 569–586. [Google Scholar] [CrossRef]
- Falck, R.S.; Best, J.R.; Davis, J.C.; Liu-Ambrose, T. The independent associations of physical activity and sleep with cognitive function in older adults. J. Alzheimer’s Dis. 2018, 63, 1469–1484. [Google Scholar] [CrossRef] [PubMed]
- Cheval, B.; Maltagliati, S.; Sieber, S.; Beran, D.; Chalabaev, A.; Sander, D.; Cullati, S.; Boisgontier, M.P. Why Are Individuals with Diabetes Less Active? The Mediating Role of Physical, Emotional, and Cognitive Factors. Ann. Behav. Med. 2021. [Google Scholar] [CrossRef] [PubMed]
- Buysse, D.J.; Reynolds, C.F., III; Monk, T.H.; Berman, S.R.; Kupfer, D.J. The Pittsburgh Sleep Quality Index: A new instrument for psychiatric practice and research. Psychiatry Res. 1989, 28, 193–213. [Google Scholar] [CrossRef]
- Cui, J.; Zou, L.; Herold, F.; Yu, Q.; Jiao, C.; Zhang, Y.; Chi, X.; Müller, N.G.; Perrey, S.; Li, L.; et al. Does Cardiorespiratory Fitness Influence the Effect of Acute Aerobic Exercise on Executive Function? Front. Hum. Neurosci. 2020, 14, 569010. [Google Scholar] [CrossRef] [PubMed]
- Hu, L.T.; Bentler, P.M. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Struct. Equ. Model. Multidiscip. J. 1999, 6, 1–55. [Google Scholar] [CrossRef]
- Stillman, C.M.; Esteban-Cornejo, I.; Brown, B.; Bender, C.M.; Erickson, K.I. Effects of Exercise on Brain and Cognition Across Age Groups and Health States. Trends Neurosci. 2020, 43, 533–543. [Google Scholar] [CrossRef]
- Youngstedt, S.D. Effects of exercise on sleep. Clin. Sports Med. 2005, 24, 355–365. [Google Scholar] [CrossRef] [PubMed]
- Kalak, N.; Gerber, M.; Kirov, R.; Mikoteit, T.; Yordanova, J.; Pühse, U.; Holsboer-Trachsler, E.; Brand, S. Daily morning running for 3 weeks improved sleep and psychological functioning in healthy adolescents compared with controls. J. Adolesc. Health 2012, 51, 615–622. [Google Scholar] [CrossRef] [PubMed]
- Lang, C.; Brand, S.; Feldmeth, A.K.; Holsboer-Trachsler, E.; Pühse, U.; Gerber, M. Increased self-reported and objectively assessed physical activity predict sleep quality among adolescents. Physiol. Behav. 2013, 120, 46–53. [Google Scholar] [CrossRef] [PubMed]
- Kline, C.E. The bidirectional relationship between exercise and sleep: Implications for exercise adherence and sleep improvement. Am. J. Lifestyle Med. 2014, 8, 375–379. [Google Scholar] [CrossRef] [PubMed]
- Wendt, A.; da Silva, I.C.M.; Gonçalves, H.; Menezes, A.; Barros, F.; Wehrmeister, F.C. Short-term effect of physical activity on sleep health: A population-based study using accelerometry. J. Sport Health Sci. 2020, in press. [Google Scholar] [CrossRef]
- Bastien, C.H.; Fortier-Brochu, E.; Rioux, I.; LeBlanc, M.; Daley, M.; Morin, C.M. Cognitive performance and sleep quality in the elderly suffering from chronic insomnia: Relationship between objective and subjective measures. J. Psychosom. Res. 2003, 54, 39–49. [Google Scholar] [CrossRef]
- Foley, D.J.; Masaki, K.; White, L.; Larkin, E.K.; Monjan, A.; Redline, S. Sleep-disordered breathing and cognitive impairment in elderly Japanese-American men. Sleep 2003, 26, 596–599. [Google Scholar] [CrossRef]
- Blackwell, T.; Yaffe, K.; Ancoli-Israel, S.; Schneider, J.L.; Cauley, J.A.; Hillier, T.A.; Fink, H.A.; Stone, K.L. Poor sleep is associated with impaired cognitive function in older women: The study of osteoporotic fractures. J. Gerontol. Ser. A 2006, 61, 405–410. [Google Scholar] [CrossRef]
- Wilckens, K.A.; Erickson, K.I.; Wheeler, M.E. Age-Related Decline in Controlled Retrieval: The Role of the PFC and Sleep. Neural Plast. 2012, 2012, 624795. [Google Scholar] [CrossRef] [PubMed]
- Harrison, Y.; Horne, J.A. Long-term extension to sleep—Are we really chronically sleep deprived? Psychophysiology 1996, 33, 22–30. [Google Scholar] [CrossRef] [PubMed]
- Youngstedt, S.D.; Kripke, D.F. Long sleep and mortality: Rationale for sleep restriction. Sleep Med. Rev. 2004, 8, 159–174. [Google Scholar] [CrossRef]
- Monk, T.H.; Buysse, D.J.; Begley, A.E.; Billy, B.D.; Fletcher, M.E. Effects of a Two-Hour Change in Bedtime on the Sleep of Healthy Seniors. Chronobiol. Int. 2009, 26, 526–543. [Google Scholar] [CrossRef] [PubMed]
- Shrivastava, D.; Jung, S.; Saadat, M.; Sirohi, R.; Crewson, K. How to interpret the results of a sleep study. J. Community Hosp. Intern. Med. Perspect. 2014, 4, 24983. [Google Scholar] [CrossRef] [PubMed]
- Preacher, K.J.; Hayes, A.F. Asymptotic and resampling strategies for assessing and comparing indirect effects in multiple mediator models. Behav. Res. Methods 2008, 40, 879–891. [Google Scholar] [CrossRef] [PubMed]
- Zhao, X.; Lynch, J.G., Jr.; Chen, Q. Reconsidering Baron and Kenny: Myths and truths about mediation analysis. J. Consum. Res. 2010, 37, 197–206. [Google Scholar] [CrossRef]
- Landry, G.J.; Best, J.R.; Liu-Ambrose, T. Measuring sleep quality in older adults: A comparison using subjective and objective methods. Front. Aging Neurosci. 2015, 7, 166. [Google Scholar] [CrossRef]
- Lambiase, M.J.; Gabriel, K.P.; Kuller, L.H.; Matthews, K.A. Sleep and Executive Function in Older Women: The Moderating Effect of Physical Activity. J. Gerontol. Ser. A 2014, 69, 1170–1176. [Google Scholar] [CrossRef]
- Scullin, M.K.; Bliwise, D.L. Sleep, cognition, and normal aging: Integrating a half century of multidisciplinary research. Perspect. Psychol. Sci. 2015, 10, 97–137. [Google Scholar] [CrossRef]
- Hughes, J.M.; Song, Y.; Fung, C.H.; Dzierzewski, J.M.; Mitchell, M.N.; Jouldjian, S.; Josephson, K.R.; Alessi, C.A.; Martin, J.L. Measuring Sleep in Vulnerable Older Adults: A Comparison of Subjective and Objective Sleep Measures. Clin. Gerontol. 2018, 41, 145–157. [Google Scholar] [CrossRef] [PubMed]
- Okano, K.; Kaczmarzyk, J.R.; Dave, N.; Gabrieli, J.D.; Grossman, J.C. Sleep quality, duration, and consistency are associated with better academic performance in college students. NPJ Sci. Learn. 2019, 4, 16. [Google Scholar] [CrossRef] [PubMed]

| Males (n = 71) | Females (n = 109) | Total (n = 180) | |
|---|---|---|---|
| Demographic and Anthropometric Parameters | |||
| Age (years) | 20.31 ± 1.45 | 19.68 ± 1.64 | 19.93 ± 1.59 |
| BMI (kg/m2) | 21.66 ± 2.05 | 21.20 ± 2.55 | 21.37 ± 2.37 |
| International Physical Activity Questionnaire | |||
| MET-min/w | 4967.05 ± 1447.06 | 5171.22 ± 1556.39 | 5090.69 ± 1513.41 |
| Pittsburgh Sleep Quality Index | |||
| Subjective sleep quality | 0.68 ± 0.69 | 0.76 ± 0.79 | 0.73 ± 0.75 |
| Sleep time | 0.62 ± 0.70 | 0.54 ± 0.69 | 0.57 ± 0.69 |
| Sleep efficiency | 0.73 ± 0.72 | 0.68 ± 0.76 | 0.70 ± 0.74 |
| Sleep disorders | 0.80 ± 0.71 | 0.97 ± 0.55 | 0.91 ± 0.62 |
| Stroop Test | |||
| Congruent accuracy (%) | 95.00 ± 9.35 | 97.00 ± 5.80 | 96.00 ± 7.46 |
| Incongruent accuracy (%) | 95.00 ± 8.65 | 97.00 ± 4.70 | 96.00 ± 6.66 |
| Congruent reaction time (ms) | 899.98 ± 107.20 | 867.53 ± 135.39 | 875.47 ± 141.42 |
| Incongruent reaction time (ms) | 1000.18 ± 107.79 | 964.34 ± 148.10 | 973.07 ± 152.56 |
| Stroop effect (ms) | 100.21 ± 45.64 | 96.81 ± 47.13 | 98.15 ± 46.45 |
| MET-min/w | S1 | S2 | S3 | S4 | S5 | S6 | S7 | Acc.1 | Acc.2 | RT1 | RT2 | Stroop Effect | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| MET | - | ||||||||||||
| S1 | −0.425 *** | - | |||||||||||
| S2 | −0.033 | 0.068 | - | ||||||||||
| S3 | −0.006 | 0.082 | 0.107 | - | |||||||||
| S4 | −0.519 *** | 0.652 *** | 0.033 | 0.126 | - | ||||||||
| S5 | 0.180 ** | 0.100 | 0.186 ** | −0.106 | −0.008 | - | |||||||
| S6 | 0.153 ** | 0.060 | 0.125 | −0.210 ** | 0.081 | 0.331 *** | - | ||||||
| S7 | 0.058 | 0.047 | 0.289 *** | −0.039 | 0.002 | 0.198 ** | 0.412 *** | - | |||||
| Acc.1 | −0.018 | 0.057 | 0.064 | 0.074 | −0.023 | 0.103 | −0.019 | 0.136 | - | ||||
| Acc.2 | −0.056 | −0.032 | −0.016 | 0.116 | −0.062 | −0.002 | −0.106 | 0.017 | 0.486 *** | - | |||
| RT1 | 0.036 | 0.139 | 0.021 | −0.053 | 0.043 | 0.047 | 0.116 | 0.033 | −0.076 | −0.107 | - | ||
| RT2 | −0.101 | 0.419 *** | 0.036 | −0.006 | 0.252 *** | 0.060 | 0.142 | 0.032 | −0.027 | −0.109 | 0.938 *** | - | |
| Stroop effect | −0.386 *** | 0.831 *** | 0.045 | 0.125 | 0.611 *** | 0.045 | 0.098 | 0.003 | 0.125 | −0.026 | 0.008 | 0.355 *** | - |
| Model | χ2 | p | f | χ2/DF | NFI | IFI | CFI | RMSEA | SRMR |
|---|---|---|---|---|---|---|---|---|---|
| Initial model | 64.43 | 0.001 | 1 | 64.43 | 0.83 | 0.83 | 0.82 | 0.07 | 0.06 |
| Final model | 0.06 | 0.06 | 1 | 0.06 | 0.92 | 0.92 | 0.93 | 0.05 | 0.04 |
| Δχ2 | 64.37 |
| Route | Indirect Effects of Standardization | Average Indirect Effect | 95% Confidence Interval | p | |
|---|---|---|---|---|---|
| Lower Limit | Upper Limit | ||||
| Subjective Sleep Quality | 0.42 × 0.77 = 0.32 | 0.41 | 0.27 | 0.55 | 0.01 |
| Sleep Efficiency | 0.53 × 0.13 = 0.07 | 0.51 | 0.39 | 0.63 | 0.01 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Li, L.; Yu, Q.; Zhao, W.; Herold, F.; Cheval, B.; Kong, Z.; Li, J.; Mueller, N.; Kramer, A.F.; Cui, J.; et al. Physical Activity and Inhibitory Control: The Mediating Role of Sleep Quality and Sleep Efficiency. Brain Sci. 2021, 11, 664. https://doi.org/10.3390/brainsci11050664
Li L, Yu Q, Zhao W, Herold F, Cheval B, Kong Z, Li J, Mueller N, Kramer AF, Cui J, et al. Physical Activity and Inhibitory Control: The Mediating Role of Sleep Quality and Sleep Efficiency. Brain Sciences. 2021; 11(5):664. https://doi.org/10.3390/brainsci11050664
Chicago/Turabian StyleLi, Lin, Qian Yu, Wenrui Zhao, Fabian Herold, Boris Cheval, Zhaowei Kong, Jinming Li, Notger Mueller, Arthur F. Kramer, Jie Cui, and et al. 2021. "Physical Activity and Inhibitory Control: The Mediating Role of Sleep Quality and Sleep Efficiency" Brain Sciences 11, no. 5: 664. https://doi.org/10.3390/brainsci11050664
APA StyleLi, L., Yu, Q., Zhao, W., Herold, F., Cheval, B., Kong, Z., Li, J., Mueller, N., Kramer, A. F., Cui, J., Pan, H., Zhan, Z., Hui, M., & Zou, L. (2021). Physical Activity and Inhibitory Control: The Mediating Role of Sleep Quality and Sleep Efficiency. Brain Sciences, 11(5), 664. https://doi.org/10.3390/brainsci11050664








