Review of Advanced Medical Telerobots
Abstract
1. Introduction
1.1. Telerobotics General Context
- agility; precision; repeatability;
- automatic trajectory tracking and no-fly-zone generation;
- ability to satisfy constraints in position, and speed domains;
- real-time fusion of multimodal exteroceptive information;
- automatic recording of gestures made.
1.2. Introduction of Robotics in Medicine
1.3. History of Telerobotics in Medicine
1.4. The Motivations for Telerobotics in Medicine
1.5. The Critical Issue of Stability and Transparency of Telerobots
1.6. Outline of This Paper
2. Medical Telerobotic Topologies
2.1. Single-Leader Single-Follower Topology (SL/SF)
2.1.1. Sensory Augmentation through SL/SF Telerobotic Surgery
- the disturbing forces at the trocar and abdominal wall, the disturbing forces on the tool by nearby organs [136],
2.1.2. Motor Augmentation through SL/SF Telerobotic Surgery
2.2. Single-Leader Single-Follower Telerobotic Rehabilitation
2.3. Multilateral Teleoperation
2.3.1. Multi-Leader/Single-Follower (ML/SF)
2.3.2. Single-Leader/Multi-Follower (SL/MF)
2.3.3. Multi-Leader–Multi-Follower (ML/MF)
2.3.4. Trilateral Teleoperation
Human–Machine Shared Control (HMSC)
Dual-User Shared Teleoperation (DUST)
Dual-User Redundancy Control (DURC)
Section Vision
3. Autonomy Levels
- Bilateral teleoperation: features any exchange of position (and force) between the leader and the follower robots (only position exchanges were envisaged in [313]) and uses a SL/SF topology defined in Section 2.1;
- Shared control which can be split in two subcategories:
- Multi-user Shared Control: corresponds to architectures which include several operators sharing the control of the same telerobot;
- Supervisory Control, where some high-level information (parameters and/or offline programming) is sent to the follower robot to be reproduced with some degree of controlled autonomy, knowing that in main medical applications, there are no very long-distance constraints.
3.1. Bilateral Teleoperation
3.2. Shared Control
3.2.1. Task Decomposition Based Shared Control
3.2.2. Shared Authority Blending-Based Control
Linear Blending
Nonlinear Blending
Authority Blending with More than Two Users
3.2.3. Shared Control Synthesis
3.3. Traded Control
3.4. Supervisory Control
3.5. Discussion about Robotic Autonomy
4. Conclusions and Future Directions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Atashzar, S.F.; Naish, M.; Patel, R.V. Active Sensorimotor Augmentation in Robotics-Assisted Surgical Systems. In Mixed and Augmented Reality in Medicine; CRC Press: Boca Raton, FL, USA, 2018; pp. 61–81. [Google Scholar]
- Moorthy, K.; Munz, Y.; Dosis, A.; Hernandez, J.; Martin, S.; Bello, F.; Rockall, T.; Darzi, A. Dexterity enhancement with robotic surgery. Surg. Endosc. Other Interv. Tech. 2004, 18, 790–795. [Google Scholar] [CrossRef]
- Atashzar, S.F.; Patel, R.V. Teleoperation for Minimally Invasive Robotics-Assisted Surgery. In The Encyclopedia of Medical Robotics; World Scientific: Singapore, 2018; pp. 341–372. [Google Scholar]
- Shahbazi, M.; Atashzar, S.F.; Patel, R.V. A Systematic Review of Multilateral Teleoperation Systems. IEEE Trans. Haptics 2018, 11, 338–356. [Google Scholar] [CrossRef]
- Prasad, S.M.; Prasad, S.M.; Maniar, H.S.; Chu, C.; Schuessler, R.B.; Damiano, R.J., Jr. Surgical robotics: Impact of motion scaling on task performance. J. Am. Coll. Surg. 2004, 199, 863–868. [Google Scholar] [CrossRef]
- Bethea, B.T.; Okamura, A.M.; Kitagawa, M.; Fitton, T.P.; Cattaneo, S.M.; Gott, V.L.; Baumgartner, W.A.; Yuh, D.D. Application of haptic feedback to robotic surgery. J. Laparoendosc. Adv. Surg. Tech. 2004, 14, 191–195. [Google Scholar] [CrossRef]
- Atashzar, S.F.; Shahbazi, M.; Tavakoli, M.; Patel, R.V. A passivity-based approach for stable patient–robot interaction in haptics-enabled rehabilitation systems: Modulated time-domain passivity control. IEEE Trans. Control Syst. Technol. 2016, 25, 991–1006. [Google Scholar] [CrossRef]
- Peretti, A.; Amenta, F.; Tayebati, S.K.; Nittari, G.; Mahdi, S.S. Telerehabilitation: Review of the State-of-the-Art and Areas of Application. JMIR Rehabil. Assist. Technol. 2017, 4, e7. [Google Scholar] [CrossRef]
- Albakri, A. Haptic Teleoperation for Robotic-Assisted Surgery. Ph.D. Thesis, Université de Montpellier, Montpellier, France, 2015. [Google Scholar]
- Richa, R.; Bó, A.P.; Poignet, P. Towards robust 3D visual tracking for motion compensation in beating heart surgery. Med. Image Anal. 2011, 15, 302–315. [Google Scholar] [CrossRef] [PubMed]
- Yuen, S.G.; Kettler, D.T.; Novotny, P.M.; Plowes, R.D.; Howe, R.D. Robotic motion compensation for beating heart intracardiac surgery. Int. J. Robot. Res. 2009, 28, 1355–1372. [Google Scholar] [CrossRef] [PubMed]
- Konietschke, R.; Zerbato, D.; Richa, R.; Tobergte, A.; Poignet, P.; Fröhlich, F.A.; Botturi, D.; Fiorini, P.; Hirzinger, G. Integration of new features for telerobotic surgery into the MiroSurge system. Appl. Bionics Biomech. 2011, 8, 253–265. [Google Scholar] [CrossRef]
- Wong, W.K.; Yang, B.; Liu, C.; Poignet, P. A quasi-spherical triangle-based approach for efficient 3-D soft-tissue motion tracking. IEEE/ASME Trans. Mechatron. 2012, 18, 1472–1484. [Google Scholar] [CrossRef]
- Mathiassen, K.; Fjellin, J.E.; Glette, K.; Hol, P.K.; Elle, O.J. An Ultrasound Robotic System Using the Commercial Robot UR5. Front. Robot. AI 2016, 3, 1. [Google Scholar] [CrossRef]
- Krupa, A.; Folio, D.; Novales, C.; Vieyres, P.; Li, T. Robotized Tele-Echography: An Assisting Visibility Tool to Support Expert Diagnostic. Syst. J. IEEE 2014. [Google Scholar] [CrossRef]
- Sharifi, M.; Salarieh, H.; Behzadipour, S.; Tavakoli, M. Tele-echography of moving organs using an Impedance-controlled telerobotic system. Mechatronics 2017, 45, 60–70. [Google Scholar] [CrossRef]
- Santos, L.; Cortesao, R. Computed-Torque Control for Robotic-Assisted Tele-Echography Based on Perceived Stiffness Estimation. IEEE Trans. Autom. Sci. Eng. 2018, 15, 1337–1354. [Google Scholar] [CrossRef]
- Avgousti, S.; Panayides, A.S.; Jossif, A.P.; Christoforou, E.G.; Vieyres, P.; Novales, C.; Voskarides, S.; Pattichis, C.S. Cardiac ultrasonography over 4G wireless networks using a tele-operated robot. Healthc. Technol. Lett. 2016, 3, 212–217. [Google Scholar] [CrossRef] [PubMed]
- Seo, J.; Cho, J.H.; Lee, M.W.; Kim, T.; Par, H.; Kim, S.; Kim, C.; Kwon, O. Feasibility Evaluation of Mobile Internet based Robot-assisted Tele-echography System. In Proceedings of the 2018 15th International Conference on Ubiquitous Robots (UR), Jeju, Korea, 28 June–1 July 2018; pp. 53–56. [Google Scholar] [CrossRef]
- Byrn, J.C.; Schluender, S.; Divino, C.M.; Conrad, J.; Gurland, B.; Shlasko, E.; Szold, A. Three-dimensional imaging improves surgical performance for both novice and experienced operators using the da Vinci Robot System. Am. J. Surg. 2007, 193, 519–522. [Google Scholar] [CrossRef]
- Spinoglio, G.; Priora, F.; Bianchi, P.P.; Lucido, F.S.; Licciardello, A.; Maglione, V.; Grosso, F.; Quarati, R.; Ravazzoni, F.; Lenti, L.M. Real-time near-infrared (NIR) fluorescent cholangiography in single-site robotic cholecystectomy (SSRC): A single-institutional prospective study. Surg. Endosc. 2013, 27, 2156–2162. [Google Scholar] [CrossRef]
- Haber, G.P.; White, M.A.; Autorino, R.; Escobar, P.F.; Kroh, M.D.; Chalikonda, S.; Khanna, R.; Forest, S.; Yang, B.; Altunrende, F.; et al. Novel robotic da Vinci instruments for laparoendoscopic single-site surgery. Urology 2010, 76, 1279–1282. [Google Scholar] [CrossRef]
- Intuitive Surgical, Inc. Da Vinci by Intuitive: Enabling Surgical Care to Get Patients Back to What Matters; Intuitive Surgical, Inc.: Sunnyvale, CA, USA, 2020. [Google Scholar]
- Kwoh, Y.S.; Hou, J.; Jonckheere, E.A.; Hayati, S. A robot with improved absolute positioning accuracy for CT guided stereotactic brain surgery. IEEE Trans. Biomed. Eng. 1988, 35, 153–160. [Google Scholar] [CrossRef]
- Schäfer, M.; Stewart, K.; Pott, P. Industrial robots for teleoperated surgery—A systematic review of existing approaches. Curr. Dir. Biomed. Eng. 2019, 5, 153–156. [Google Scholar] [CrossRef]
- Taylor, R.H.; Kazanzides, P.; Fischer, G.S.; Simaan, N. Chapter Nineteen—Medical robotics and computer-integrated interventional medicine. In Biomedical Information Technology, 2nd ed.; Feng, D.D., Ed.; Biomedical Engineering, Academic Press: Cambridge, MA, USA, 2020; pp. 617–672. [Google Scholar] [CrossRef]
- Choi, P.J.; Oskouian, R.J.; Tubbs, R.S. Telesurgery: Past, Present, and Future. Cureus 2018, 10, e2716. [Google Scholar] [CrossRef]
- Lelevé, A.; McDaniel, T.; Rossa, C. Haptic Training Simulation. Front. Virtual Real. 2020, 1, 3. [Google Scholar] [CrossRef]
- Sung, G.T.; Gill, I.S. Robotic laparoscopic surgery: A comparison of the da Vinci and Zeus systems. Urology 2001, 58, 893–898. [Google Scholar] [CrossRef]
- Payne, T.N.; Dauterive, F.R. A comparison of total laparoscopic hysterectomy to robotically assisted hysterectomy: Surgical outcomes in a community practice. J. Minim. Invasive Gynecol. 2008, 15, 286–291. [Google Scholar] [CrossRef] [PubMed]
- De, S.; Rosen, J.; Dagan, A.; Hannaford, B.; Swanson, P.; Sinanan, M. Assessment of tissue damage due to mechanical stresses. Int. J. Robot. Res. 2007, 26, 1159–1171. [Google Scholar] [CrossRef]
- Kuo, C.H.; Dai, J.S. Robotics for minimally invasive surgery: A historical review from the perspective of kinematics. In International Symposium on History of Machines and Mechanisms; Springer: Berlin/Heidelberg, Germany, 2009; pp. 337–354. [Google Scholar]
- Tortora, G.; Dario, P.; Menciassi, A. Array of robots augmenting the kinematics of endocavitary surgery. IEEE/ASME Trans. Mechatron. 2014, 19, 1821–1829. [Google Scholar] [CrossRef]
- Staub, C.; Ono, K.; Mayer, H.; Knoll, A.; Ulbrich, H.; Bauernschmitt, R. Remote minimally invasive surgery–haptic feedback and selective automation in medical robotics. Appl. Bionics Biomech. 2011, 8, 221–236. [Google Scholar] [CrossRef]
- Westebring, E.P.; Goossens, R.H.M.; Jakimowicz, J.J.; Dankelman, J. Haptics in minimally invasive surgery—A review. Minim. Invasive Ther. Allied Technol. 2008, 17, 3–16. [Google Scholar] [CrossRef]
- Trejos, A.; Patel, R.; Naish, M. Force sensing and its application in minimally invasive surgery and therapy: A survey. Proc. Inst. Mech. Eng. Part C J. Mech. Eng. Sci. 2010, 224, 1435–1454. [Google Scholar] [CrossRef]
- Park, A.; Lee, G.; Seagull, F.J.; Meenaghan, N.; Dexter, D. Patients benefit while surgeons suffer: An impending epidemic. J. Am. Coll. Surg. 2010, 210, 306–313. [Google Scholar] [CrossRef]
- Kant, I.; de Jong, L.; van Rijssen-Moll, M.; Borm, P. A survey of static and dynamic work postures of operating room staff. Int. Arch. Occup. Environ. Health 1992, 63, 423–428. [Google Scholar] [CrossRef] [PubMed]
- Patkin, M.; Isabel, L. Ergonomics, engineering and surgery of endosurgical dissection. J. R. Coll. Surg. Edinb. 1995, 40, 120–132. [Google Scholar] [PubMed]
- Reiley, C.E.; Akinbiyi, T.; Burschka, D.; Chang, D.C.; Okamura, A.M.; Yuh, D.D. Effects of visual force feedback on robot-assisted surgical task performance. J. Thorac. Cardiovasc. Surg. 2008, 135, 196–202. [Google Scholar] [CrossRef] [PubMed]
- Wagner, C.R.; Howe, R.D. Force feedback benefit depends on experience in multiple degree of freedom robotic surgery task. IEEE Trans. Robot. 2007, 23, 1235–1240. [Google Scholar] [CrossRef]
- Sackier, J.; Wang, Y. Robotically assisted laparoscopic surgery. Surg Endosc 1994, 8, 63–66. [Google Scholar] [CrossRef] [PubMed]
- Taylor, R.H.; Funda, J.; Eldridge, B.; Gomory, S.; Gruben, K.; LaRose, D.; Talamini, M.; Kavoussi, L.; Anderson, J. A telerobotic assistant for laparoscopic surgery. IEEE Eng. Med. Biol. Mag. 1995, 14, 279–288. [Google Scholar] [CrossRef]
- Cornella, J.; Elle, O.J.; Ali, W.; Samset, E. Improving Cartesian position Accuraca of a telesurgical robot. In Proceedings of the 2008 IEEE International Symposium on Industrial Electronics, Cambridge, UK, 30 June–2 July 2008; pp. 1261–1266. [Google Scholar] [CrossRef]
- Marescaux, J.; Diana, M. Robotics and Remote Surgery: Next Step. In Robotics in General Surgery; Kim, K.C., Ed.; Springer: New York, NY, USA, 2014; pp. 479–484. [Google Scholar] [CrossRef]
- Francis, P.; Eastwood, K.W.; Bodani, V.; Price, K.; Upadhyaya, K.; Podolsky, D.; Azimian, H.; Looi, T.; Drake, J. Miniaturized Instruments for the da Vinci Research Kit: Design and Implementation of Custom Continuum Tools. IEEE Robot. Autom. Mag. 2017, 24, 24–33. [Google Scholar] [CrossRef]
- Iribarne, A.; Easterwood, R.; Chan, E.; Yang, J.; Soni, L.; Russo, M.; Smith, C.; Argenziano, M. The golden age of minimally invasive cardiothoracic surgery: Current and future perspectives. Future Cardiol. 2011, 7, 333–346. [Google Scholar] [CrossRef]
- Azizian, M.; Liu, M.; Khalaji, I.; DiMaio, S. The Da Vinci Surgical System. In Encyclopedia Of Medical Robotics; Patel, R.V., Ed.; World Scientific: Singapore, 2018; pp. 3–28. [Google Scholar] [CrossRef]
- Rosen, J.; Hannaford, B.; Satava, R.M. Surgical Robotics: Systems Applications and Visions; Springer: Berlin/Heidelberg, Germany, 2011. [Google Scholar]
- Lakhmani, S.G.; Wright, J.L.; Chen, J.Y. Chapter 1—Transparent interaction and human–robot collaboration for military operations. In Living with Robots; Pak, R., de Visser, E.J., Rovira, E., Eds.; Academic Press: Cambridge, MA, USA, 2020; pp. 1–19. [Google Scholar] [CrossRef]
- Fiani, B.; Quadri, S.; Farooqui, M. Impact of robot-assisted spine surgery on health care quality and neurosurgical economics: A systemic review. Neurosurg. Rev. 2020, 43, 17–25. [Google Scholar] [CrossRef]
- Longmore, S.; Naik, G.; Gargiulo, G. Laparoscopic robotic surgery: Current perspective and future directions. Robotics 2020, 9, 42. [Google Scholar] [CrossRef]
- Tamaki, A.; Rocco, J.W.; Ozer, E. The future of robotic surgery in otolaryngology—Head and neck surgery. Oral Oncol. 2020, 101, 104510. [Google Scholar] [CrossRef] [PubMed]
- Sheridan, T. Teleoperation, telerobotics and telepresence: A progress report. Control Eng. Pract. 1995, 3, 205–214. [Google Scholar] [CrossRef]
- Okamura, A. Methods for haptic feedback in teleoperated robot-assisted surgery. Ind. Robot 2004, 31, 499–508. [Google Scholar] [CrossRef] [PubMed]
- Anvari, M.; McKinley, C.; Stein, H. Establishment of the world’s first telerobotic remote surgical service: For provision of advanced laparoscopic surgery in a rural community. Ann. Surg. 2005, 241, 460–464. [Google Scholar] [CrossRef] [PubMed]
- Takács, A.; Jordán, S.; Nagy, D.A.; Tar, J.K.; Rudas, I.J.; Haidegger, T. Surgical robotics—Born in space. In Proceedings of the 2015 IEEE 10th Jubilee International Symposium on Applied Computational Intelligence and Informatics, Timisoara, Romania, 21–23 May 2015; pp. 547–551. [Google Scholar] [CrossRef]
- Hokayem, P.F.; Spong, M.W. Bilateral teleoperation: An historical survey. Automatica 2006, 42, 2035–2057. [Google Scholar] [CrossRef]
- Zaffino, P.; Moccia, S.; De Momi, E.; Spadea, M.F. A Review on Advances in Intra-operative Imaging for Surgery and Therapy: Imagining the Operating Room of the Future. Ann. Biomed. Eng. 2020. [Google Scholar] [CrossRef]
- Seifabadi, R.; Song, S.E.; Krieger, A.; Cho, N.B.; Tokuda, J.; Fichtinger, G.; Iordachita, I. Robotic system for MRI-guided prostate biopsy: Feasibility of teleoperated needle insertion and ex vivo phantom study. Int. J. Comput. Assist. Radiol. Surg. 2012, 7, 181–190. [Google Scholar] [CrossRef]
- Shang, W.; Su, H.; Li, G.; Fischer, G.S. Teleoperation system with hybrid pneumatic-piezoelectric actuation for MRI-guided needle insertion with haptic feedback. In Proceedings of the 2013 IEEE/RSJ International Conference on Intelligent Robots and Systems, Tokyo, Japan, 3–7 November 2013; pp. 4092–4098. [Google Scholar] [CrossRef]
- Chen, Y.; Godage, I.; Su, H.; Song, A.; Yu, H. Stereotactic Systems for MRI-Guided Neurosurgeries: A State-of-the-Art Review. Ann. Biomed. Eng. 2019, 47, 335–353. [Google Scholar] [CrossRef]
- Licona, A.R.; Liu, F.; Pinzon, D.; Torabi, A.; Boulanger, P.; Lelevé, A.; Moreau, R.; Pham, M.T.; Tavakoli, M. Applications of Haptics in Medicine. In Haptic Interfaces for Accessibility, Health, and Enhanced Quality of Life; McDaniel, T., Panchanathan, S., Eds.; Springer International Publishing: Cham, Switzerland, 2020; pp. 183–214. [Google Scholar] [CrossRef]
- Atashzar, S.F.; Polushin, I.G.; Patel, R.V. A small-gain approach for nonpassive bilateral telerobotic rehabilitation: Stability analysis and controller synthesis. IEEE Trans. Robot. 2016, 33, 49–66. [Google Scholar] [CrossRef]
- Yang, S.; MacLachlan, R.A.; Riviere, C.N. Manipulator design and operation of a six-degree-of-freedom handheld tremor-canceling microsurgical instrument. IEEE/ASME Trans. Mechatron. 2014, 20, 761–772. [Google Scholar] [CrossRef]
- Taylor, R.; Jensen, P.; Whitcomb, L.; Barnes, A.; Kumar, R.; Stoianovici, D.; Gupta, P.; Wang, Z.; Dejuan, E.; Kavoussi, L. A Steady-Hand Robotic System for Microsurgical Augmentation. Int. J. Robot. Res. 1999, 18, 1201–1210. [Google Scholar] [CrossRef]
- Bowyer, S.A.; Davies, B.L.; Rodriguez y Baena, F. Active Constraints/Virtual Fixtures: A Survey. IEEE Trans. Robot. 2014, 30, 138–157. [Google Scholar] [CrossRef]
- Li, M.; Ishii, M.; Taylor, R.H. Spatial motion constraints using virtual fixtures generated by anatomy. IEEE Trans. Robot. 2007, 23, 4–19. [Google Scholar] [CrossRef]
- Bettini, A.; Marayong, P.; Lang, S.; Okamura, A.M.; Hager, G.D. Vision-assisted control for manipulation using virtual fixtures. IEEE Trans. Robot. 2004, 20, 953–966. [Google Scholar] [CrossRef]
- Olivieri, E.; Barresi, G.; Caldwell, D.G.; Mattos, L.S. Haptic feedback for control and active constraints in contactless laser surgery: Concept, implementation, and evaluation. IEEE Trans. Haptics 2017, 11, 241–254. [Google Scholar] [CrossRef]
- Li, M.; Taylor, R.H. Spatial motion constraints in medical robot using virtual fixtures generated by anatomy. In Proceedings of the IEEE International Conference on Robotics and Automation, ICRA’04 2004, New Orleans, LA, USA, 26 April–1 May 2004; IEEE: Piscataway, NJ, USA, 2004; Volume 2, pp. 1270–1275. [Google Scholar]
- Urias, M.G.; Patel, N.; He, C.; Ebrahimi, A.; Kim, J.W.; Iordachita, I.; Gehlbach, P.L. Artificial intelligence, robotics and eye surgery: Are we overfitted? Int. J. Retin. Vitr. 2019, 5, 52. [Google Scholar] [CrossRef]
- Hanna, E.Y.; Holsinger, C.; DeMonte, F.; Kupferman, M. Robotic endoscopic surgery of the skull base: A novel surgical approach. Arch. Otolaryngol. Head Neck Surg. 2007, 133, 1209–1214. [Google Scholar] [CrossRef]
- Klodmann, J.; Schlenk, C.; Borsdorf, S.; Unterhinninghofen, R.; Albu-Schäffer, A.; Hirzinger, G. Robotic assistance systems for surgery: Current developments and focus of research. Der Chir. Z. Fur Alle Geb. Der Oper. Medizen 2020, 91, 533–543. [Google Scholar]
- Florez, J.M.; Szewczyk, J.; Morel, G. An impedance control strategy for a hand-held instrument to compensate for physiological motion. In Proceedings of the 2012 IEEE International Conference on Robotics and Automation, Saint Paul, MN, USA, 14–18 May 2012; IEEE: Piscataway, NJ, USA, 2012; pp. 1952–1957. [Google Scholar]
- Patel, V.; Krishnan, S.; Goncalves, A.; Chen, C.; Boyd, W.D.; Goldberg, K. Using intermittent synchronization to compensate for rhythmic body motion during autonomous surgical cutting and debridement. In Proceedings of the 2018 International Symposium on Medical Robotics (ISMR), Atlanta, GA, USA, 1–3 March 2018; IEEE: Piscataway, NJ, USA, 2018; pp. 1–6. [Google Scholar]
- Pandya, A.; Eslamian, S.; Ying, H.; Nokleby, M.; Reisner, L.A. A Robotic Recording and Playback Platform for Training Surgeons and Learning Autonomous Behaviors Using the da Vinci Surgical System. Robotics 2019, 8, 9. [Google Scholar] [CrossRef]
- Abdelaal, A.E.; Sakr, M.; Avinash, A.; Mohammed, S.K.; Bajwa, A.K.; Sahni, M.; Hor, S.; Fels, S.; Salcudean, S.E. Play Me Back: A Unified Training Platform for Robotic and Laparoscopic Surgery. IEEE Robot. Autom. Lett. 2019, 4, 554–561. [Google Scholar] [CrossRef]
- Wang, Z.; Majewicz Fey, A. Deep learning with convolutional neural network for objective skill evaluation in robot-assisted surgery. Int. J. Comput. Assist. Radiol. Surg. 2018, 13, 1959–1970. [Google Scholar] [CrossRef] [PubMed]
- Lawrence, D. Stability and transparency in bilateral teleoperation. IEEE Trans. Robot. Autom. 1993, 9, 624–637. [Google Scholar] [CrossRef]
- Hastrudi-Zaad, K.; Salcudean, S.E. On the use of local force feedback for transparent teleoperation. In Proceedings of the 1999 IEEE International Conference on Robotics and Automation (Cat. No.99CH36288C), Detroit, MI, USA, 10–15 May 1999; Volume 3, pp. 1863–1869. [Google Scholar] [CrossRef]
- Niemeyer, G.; Slotine, J.J. Stable adaptive teleoperation. IEEE J. Ocean. Eng. 1991, 16, 152–162. [Google Scholar] [CrossRef]
- Sun, D.; Naghdy, F.; Du, H. Application of wave-variable control to bilateral teleoperation systems: A survey. Annu. Rev. Control 2014, 38, 12–31. [Google Scholar] [CrossRef]
- Hannaford, B.; Jee-Hwan, R. Time-domain passivity control of haptic interfaces. IEEE Trans. Robot. Autom. 2002, 18, 1–10. [Google Scholar] [CrossRef]
- Atashzar, S.F.; Shahbazi, M.; Tavakoli, M.; Patel, R.V. A grasp-based passivity signature for haptics-enabled human-robot interaction: Application to design of a new safety mechanism for robotic rehabilitation. Int. J. Robot. Res. 2017, 36, 778–799. [Google Scholar] [CrossRef]
- Escobar-Castillejos, D.; Noguez, J.; Neri, L.; Magana, A.; Benes, B. A Review of Simulators with Haptic Devices for Medical Training. J. Med. Syst. 2016, 40. [Google Scholar] [CrossRef]
- MacLachlan, R.A.; Becker, B.C.; Tabarés, J.C.; Podnar, G.W.; Lobes, L.A., Jr.; Riviere, C.N. Micron: An actively stabilized handheld tool for microsurgery. IEEE Trans. Robot. 2011, 28, 195–212. [Google Scholar] [CrossRef]
- Wells, T.S.; Yang, S.; MacLachlan, R.A.; Lobes, L.A., Jr.; Martel, J.N.; Riviere, C.N. Hybrid position/force control of an active handheld micromanipulator for membrane peeling. Int. J. Med. Robot. Comput. Assist. Surg. 2016, 12, 85–95. [Google Scholar] [CrossRef]
- Rossa, C.; Fong, J.; Usmani, N.; Sloboda, R.; Tavakoli, M. Multiactuator haptic feedback on the wrist for needle steering guidance in brachytherapy. IEEE Robot. Autom. Lett. 2016, 1, 852–859. [Google Scholar] [CrossRef]
- Raitor, M.; Walker, J.M.; Okamura, A.M.; Culbertson, H. WRAP: Wearable, restricted-aperture pneumatics for haptic guidance. In Proceedings of the 2017 IEEE International Conference on Robotics and Automation (ICRA), Singapore, 29 May–3 June 2017; IEEE: Piscataway, NJ, USA, 2017; pp. 427–432. [Google Scholar]
- Atashzar, S.F.; Polushin, I.G.; Patel, R.V. Networked teleoperation with non-passive environment: Application to tele-rehabilitation. In Proceedings of the 2012 IEEE/RSJ International Conference on Intelligent Robots and Systems, Vilamoura, Portugal, 7–12 October 2012; IEEE: Piscataway, NJ, USA, 2012; pp. 5125–5130. [Google Scholar]
- Mehrtash, M.; Zhang, X.; Khamesee, M. Bilateral Magnetic Micromanipulation Using Off-Board Force Sensor. IEEE/ASME Trans. Mechatron. 2015, 20, 3223–3231. [Google Scholar] [CrossRef]
- Kasahara, Y.; Kawana, H.; Usuda, S.; Ohnishi, K. Telerobotic-assisted bone-drilling system using bilateral control with feed operation scaling and cutting force scaling. Int. J. Med. Robot. Comput. Assist. Surg. 2012, 8, 221–229. [Google Scholar] [CrossRef] [PubMed]
- Paul, H.A.; Bargar, W.L.; Mittlestadt, B.; Musits, B.; Taylor, R.H.; Kazanzides, P.; Zuhars, J.; Williamson, B.; Hanson, W. Development of a surgical robot for cementless total hip arthroplasty. Clin. Orthop. Relat. Res. 1992, 285, 57–66. [Google Scholar] [CrossRef]
- Siebert, W.; Mai, S.; Kober, R.; Heeckt, P.F. Technique and first clinical results of robot-assisted total knee replacement. Knee 2002, 9, 173–180. [Google Scholar] [CrossRef]
- Jakopec, M.; Harris, S.; y Baena, F.R.; Gomes, P.; Davies, B. Acrobot: A “hands-on” robot for total knee replacement surgery. In Proceedings of the 7th International Workshop on Advanced Motion Control (Cat. No.02TH8623), Maribor, Slovenia, 3–5 July 2002; IEEE: New York, NY, USA, 2002. [Google Scholar]
- Bonneau, E.; Taha, F.; Gravez, P.; Lamy, S. Surgicobot: Surgical Gesture Assistance Cobot For Maxillo-Facial Interventions. In Perspective in Image-Guided Surgery; World Scientific: Singapore, 2004; pp. 353–360. [Google Scholar] [CrossRef]
- Tian, W.; Wei, Y.; Han, X. The History and Development of Robot-Assisted Orthopedic Surgery. In Navigation Assisted Robotics in Spine and Trauma Surgery; Tian, W., Ed.; Springer: Singapore, 2020; pp. 1–3. [Google Scholar] [CrossRef]
- Talasaz, A.; Trejos, A.L.; Patel, R.V. The role of direct and visual force feedback in suturing using a 7-DOF dual-arm teleoperated system. IEEE Trans. Haptics 2016, 10, 276–287. [Google Scholar] [CrossRef] [PubMed]
- Kitagawa, M.; Dokko, D.; Okamura, A.M.; Yuh, D.D. Effect of sensory substitution on suture-manipulation forces for robotic surgical systems. J. Thorac. Cardiovasc. Surg. 2005, 129, 151–158. [Google Scholar] [CrossRef]
- Enayati, N.; De Momi, E.; Ferrigno, G. Haptics in robot-assisted surgery: Challenges and benefits. IEEE Rev. Biomed. Eng. 2016, 9, 49–65. [Google Scholar] [CrossRef]
- Tavakoli, M.; Patel, R.V.; Aziminejad, A. Haptics for Teleoperated Surgical Robotic Systems; New Frontiers in Robotics; World Scientific Publishing Company: Singapore, 2008. [Google Scholar]
- Wentink, B. Eye-hand coordination in laparoscopy-an overview of experiments and supporting aids. Minim. Invasive Ther. Allied Technol. 2001, 10, 155–162. [Google Scholar] [CrossRef]
- Sørensen, S.M.D.; Savran, M.M.; Konge, L.; Bjerrum, F. Three-dimensional versus two-dimensional vision in laparoscopy: A systematic review. Surg. Endosc. 2016, 30, 11–23. [Google Scholar] [CrossRef]
- Gao, Y.; Wang, S.; Li, J.; Li, A.; Liu, H.; Xing, Y. Modeling and evaluation of hand–eye coordination of surgical robotic system on task performance. Int. J. Med. Robot. Comput. Assist. Surg. 2017, 13, e1829. [Google Scholar] [CrossRef]
- Guthart, G.S.; Salisbury, J.K. The Intuitive/sup TM/telesurgery system: Overview and application. In Proceedings of the 2000 ICRA, Millennium Conference, IEEE International Conference on Robotics and Automation, Symposia Proceedings (Cat. No. 00CH37065), San Francisco, CA, USA, 24–28 April 2000; IEEE: Piscataway, NJ, USA, 2000; Volume 1, pp. 618–621. [Google Scholar]
- Taylor, R.H.; Menciassi, A.; Fichtinger, G.; Fiorini, P.; Dario, P. Medical robotics and computer-integrated surgery. In Springer Handbook of Robotics; Springer: Berlin/Heidelberg, Germany, 2016; pp. 1657–1684. [Google Scholar]
- Vitiello, V.; Lee, S.L.; Cundy, T.P.; Yang, G.Z. Emerging robotic platforms for minimally invasive surgery. IEEE Rev. Biomed. Eng. 2012, 6, 111–126. [Google Scholar] [CrossRef] [PubMed]
- Freschi, C.; Ferrari, V.; Melfi, F.; Ferrari, M.; Mosca, F.; Cuschieri, A. Technical review of the da Vinci surgical telemanipulator. Int. J. Med. Robot. Comput. Assist. Surg. 2013, 9, 396–406. [Google Scholar] [CrossRef] [PubMed]
- Intuitive Surgical, Inc. Da Vinci Vision: Enhancing Visualization; Intuitive Surgical, Inc.: Sunnyvale, CA, USA, 2020. [Google Scholar]
- Vitrani, M.A.; Poquet, C.; Morel, G. Applying virtual fixtures to the distal end of a minimally invasive surgery instrument. IEEE Trans. Robot. 2016, 33, 114–123. [Google Scholar] [CrossRef]
- Beasley, R.A.; Howe, R.D. Increasing accuracy in image-guided robotic surgery through tip tracking and model-based flexion correction. IEEE Trans. Robot. 2009, 25, 292–302. [Google Scholar] [CrossRef]
- Meccariello, G.; Faedi, F.; AlGhamdi, S. An experimental study about haptic feedback in robotic surgery: May visual feedback substitute tactile feedback? J. Robot. Surg. 2016, 10, 57–61. [Google Scholar] [CrossRef] [PubMed]
- Black, D.; Hosseinabadi, A.; Salcudean, S. 6-DOF Force Sensing for the Master Tool Manipulator of the da Vinci Surgical System. IEEE Robot. Autom. Lett. 2020, 5, 2264–2271. [Google Scholar] [CrossRef]
- Oude Vrielink, T.J.C.; Vitiello, V.; Mylonas, G.P. Chapter 3.3—Robotic surgery in cancer. In Bioengineering Innovative Solutions for Cancer; Ladame, S., Chang, J.Y., Eds.; Academic Press: Cambridge, MA, USA, 2020; pp. 245–269. [Google Scholar] [CrossRef]
- Cengiz, T.B.; Steele, S.R.; Gorgun, E. 9—Implementation of Novel Robotic Systems in Colorectal Surgery. In Handbook of Robotic and Image-Guided Surgery; Abedin-Nasab, M.H., Ed.; Elsevier: Amsterdam, The Netherlands, 2020; pp. 147–158. [Google Scholar] [CrossRef]
- Hungr, N.; Bricault, I.; Cinquin, P.; Fouard, C. Design and Validation of a CT- and MRI-Guided Robot for Percutaneous Needle Procedures. IEEE Trans. Robot. 2016, 32, 973–987. [Google Scholar] [CrossRef]
- Sigrist, R.; Rauter, G.; Riener, R.; Wolf, P. Augmented visual, auditory, haptic, and multimodal feedback in motor learning: A review. Psychon. Bull. Rev. 2013, 20, 21–53. [Google Scholar] [CrossRef]
- Black, D.; Hettig, J.; Luz, M.; Hansen, C.; Kikinis, R.; Hahn, H. Auditory feedback to support image-guided medical needle placement. Int. J. CARS 2017, 12, 1655–1663. [Google Scholar] [CrossRef]
- Mewes, A.; Hensen, B.; Wacker, F.; Hansen, C. Touchless interaction with software in interventional radiology and surgery: A systematic literature review. Int. J. Comput. Assist. Radiol. Surg. 2017, 12, 291–305. [Google Scholar] [CrossRef]
- Al Fayyadh, M.J.; Hassan, R.A.; Tran, Z.K.; Kempenich, J.W.; Bunegin, L.; Dent, D.L.; Willis, R.E. Immediate Auditory Feedback is Superior to Other Types of Feedback for Basic Surgical Skills Acquisition. J. Surg. Educ. 2017, 74, e55–e61. [Google Scholar] [CrossRef] [PubMed]
- Wottawa, C.R.; Genovese, B.; Nowroozi, B.N.; Hart, S.D.; Bisley, J.W.; Grundfest, W.S.; Dutson, E.P. Evaluating tactile feedback in robotic surgery for potential clinical application using an animal model. Surg. Endosc. 2016, 30, 3198–3209. [Google Scholar] [CrossRef] [PubMed]
- Judkins, T.N.; Oleynikov, D.; Stergiou, N. Real-time augmented feedback benefits robotic laparoscopic training. Stud. Health Technol. Inform. 2005, 119, 243. [Google Scholar]
- Van der Meijden, O.A.; Schijven, M.P. The value of haptic feedback in conventional and robot-assisted minimal invasive surgery and virtual reality training: A current review. Surg. Endosc. 2009, 23, 1180–1190. [Google Scholar] [CrossRef] [PubMed]
- Naidu, A.S.; Patel, R.V.; Naish, M.D. Low-cost disposable tactile sensors for palpation in minimally invasive surgery. IEEE/ASME Trans. Mechatron. 2016, 22, 127–137. [Google Scholar] [CrossRef]
- Wagner, C.R.; Howe, R.D.; Stylopoulos, N. The role of force feedback in surgery: Analysis of blunt dissection. In Haptic Interfaces for Virtual Environment and Teleoperator Systems, International Symposium on Citeseer; ASME: New York, NY, USA, 2002; p. 73. [Google Scholar]
- Ortmaier, T.; Deml, B.; Kübler, B.; Passig, G.; Reintsema, D.; Seibold, U. Robot assisted force feedback surgery. In Advances in Telerobotics; Springer: Berlin/Heidelberg, Germany, 2007; pp. 361–379. [Google Scholar]
- Lee, D.H.; Kim, U.; Gulrez, T.; Yoon, W.J.; Hannaford, B.; Choi, H.R. A laparoscopic grasping tool with force sensing capability. IEEE/ASME Trans. Mechatron. 2015, 21, 130–141. [Google Scholar]
- Anooshahpour, F.; Polushin, I.G.; Patel, R.V. Quasi-static modeling of the da Vinci instrument. In Proceedings of the 2014 IEEE/RSJ International Conference on Intelligent Robots and Systems, Chicago, IL, USA, 14–18 September 2014; IEEE: New York, NY, USA, 2014; pp. 1308–1313. [Google Scholar]
- Anooshahpour, F.; Polushin, I.G.; Patel, R.V. Tissue compliance determination using a da Vinci instrument. In Proceedings of the 2015 IEEE International Conference on Robotics and Automation (ICRA), Seattle, WA, USA, 26–30 May 2015; IEEE: New York, NY, USA, 2015; pp. 5344–5349. [Google Scholar]
- Anooshahpour, F.; Polushin, I.G.; Patel, R.V. Classical Preisach model of hysteretic behavior in a da Vinci instrument. In Proceedings of the 2016 IEEE International Conference on Advanced Intelligent Mechatronics (AIM); IEEE: New York, NY, USA, 2016; pp. 1392–1397. [Google Scholar]
- Sang, H.; Yun, J.; Monfaredi, R.; Wilson, E.; Fooladi, H.; Cleary, K. External force estimation and implementation in robotically assisted minimally invasive surgery. Int. J. Med. Robot. Comput. Assist. Surg. 2017, 13, e1824. [Google Scholar] [CrossRef]
- Haghighipanah, M.; Miyasaka, M.; Hannaford, B. Utilizing elasticity of cable-driven surgical robot to estimate cable tension and external force. IEEE Robot. Autom. Lett. 2017, 2, 1593–1600. [Google Scholar] [CrossRef]
- Li, Y.; Hannaford, B. Gaussian process regression for sensorless grip force estimation of cable-driven elongated surgical instruments. IEEE Robot. Autom. Lett. 2017, 2, 1312–1319. [Google Scholar] [CrossRef]
- Beccani, M.; Di Natali, C.; Sliker, L.J.; Schoen, J.A.; Rentschler, M.E.; Valdastri, P. Wireless tissue palpation for intraoperative detection of lumps in the soft tissue. IEEE Trans. Biomed. Eng. 2013, 61, 353–361. [Google Scholar] [CrossRef]
- Puangmali, P.; Althoefer, K.; Seneviratne, L.D.; Murphy, D.; Dasgupta, P. State-of-the-art in force and tactile sensing for minimally invasive surgery. IEEE Sens. J. 2008, 8, 371–381. [Google Scholar] [CrossRef]
- Trejos, A.L. A Sensorized Instrument for Minimally Invasive Surgery for the Measurement of Forces during Training and Surgery: Development and Applications. Ph.D. Thesis, University of Western Ontario, London, ON, Canada, 2012. [Google Scholar]
- Mitchell, B.; Koo, J.; Iordachita, I.; Kazanzides, P.; Kapoor, A.; Handa, J.; Hager, G.; Taylor, R. Development and application of a new steady-hand manipulator for retinal surgery. In Proceedings of the 2007 IEEE International Conference on Robotics and Automation, Roma, Italy, 10–14 April 2007; IEEE: New York, NY, USA, 2007; pp. 623–629. [Google Scholar]
- Üneri, A.; Balicki, M.A.; Handa, J.; Gehlbach, P.; Taylor, R.H.; Iordachita, I. New steady-hand eye robot with micro-force sensing for vitreoretinal surgery. In Proceedings of the 2010 3rd IEEE RAS & EMBS International Conference on Biomedical Robotics and Biomechatronics, Tokyo, Japan, 26–29 September 2010; IEEE: New York, NY, USA, 2010; pp. 814–819. [Google Scholar]
- Faroque, S.; Horan, B.; Adam, H.; Pangestu, M.; Joordens, M. Haptic technology for micro-robotic cell injection training systems—A review. Intell. Autom. Soft Comput. 2016, 22, 509–523. [Google Scholar] [CrossRef]
- Pillarisetti, A.; Pekarev, M.; Brooks, A.D.; Desai, J.P. Evaluating the effect of force feedback in cell injection. IEEE Trans. Autom. Sci. Eng. 2007, 4, 322–331. [Google Scholar] [CrossRef]
- Zareinejad, M.; Rezaei, S.; Abdullah, A.; Shiry Ghidary, S. Development of a piezo-actuated micro-teleoperation system for cell manipulation. Int. J. Med. Robot. Comput. Assist. Surg. 2009, 5, 66–76. [Google Scholar] [CrossRef] [PubMed]
- Kim, D.H.; Kim, B.; Kang, H. Development of a piezoelectric polymer-based sensorized microgripper for microassembly and micromanipulation. Microsyst. Technol. 2004, 10, 275–280. [Google Scholar] [CrossRef]
- Wang, Y.; Zheng, J.; Ren, G.; Zhang, P.; Xu, C. A flexible piezoelectric force sensor based on PVDF fabrics. Smart Mater. Struct. 2011, 20, 045009. [Google Scholar] [CrossRef]
- Quek, Z.F.; Schorr, S.B.; Nisky, I.; Provancher, W.R.; Okamura, A.M. Sensory substitution and augmentation using 3-degree-of-freedom skin deformation feedback. IEEE Trans. Haptics 2015, 8, 209–221. [Google Scholar] [CrossRef]
- Schorr, S.B.; Quek, Z.F.; Nisky, I.; Provancher, W.R.; Okamura, A.M. Tactor-induced skin stretch as a sensory substitution method in teleoperated palpation. IEEE Trans. Hum. Mach. Syst. 2015, 45, 714–726. [Google Scholar] [CrossRef]
- Tavakoli, M.; Aziminejad, A.; Patel, R.; Moallem, M. Methods and mechanisms for contact feedback in a robot-assisted minimally invasive environment. Surg. Endosc. Other Interv. Tech. 2006, 20, 1570–1579. [Google Scholar] [CrossRef]
- Griffin, J.A.; Zhu, W.; Nam, C.S. The Role of Haptic Feedback in Robotic-Assisted Retinal Microsurgery Systems: A Systematic Review. IEEE Trans. Haptics 2017, 10, 94–105. [Google Scholar] [CrossRef]
- Abiri, A.; Pensa, J.; Tao, A. Multi-Modal Haptic Feedback for Grip Force Reduction in Robotic Surgery. Sci. Rep. 2019, 9. [Google Scholar] [CrossRef] [PubMed]
- Shahbazi, M.; Talebi, H.A.; Patel, R.V. Networked dual-user teleoperation with time-varying authority adjustment: A wave variable approach. In Proceedings of the 2014 IEEE/ASME International Conference on Advanced Intelligent Mechatronics, Besacon, France, 8–11 July 2014; IEEE: New York, NY, USA, 2014; pp. 415–420. [Google Scholar]
- Arabagi, V.; Felfoul, O.; Gosline, A.H.; Wood, R.J.; Dupont, P.E. Biocompatible pressure sensing skins for minimally invasive surgical instruments. IEEE Sens. J. 2015, 16, 1294–1303. [Google Scholar] [CrossRef] [PubMed]
- Hill, K.O.; Meltz, G. Fiber Bragg grating technology fundamentals and overview. J. Light. Technol. 1997, 15, 1263–1276. [Google Scholar] [CrossRef]
- Ryu, S.C.; Dupont, P.E. FBG-based shape sensing tubes for continuum robots. In Proceedings of the 2014 IEEE International Conference on Robotics and Automation (ICRA), Hong Kong, China, 31 May–7 June 2014; IEEE: New York, NY, USA, 2014; pp. 3531–3537. [Google Scholar]
- Haslinger, R.; Leyendecker, P.; Seibold, U. A fiberoptic force-torque-sensor for minimally invasive robotic surgery. In Proceedings of the 2013 IEEE International Conference on Robotics and Automation, Karlsruhe, Germany, 6–10 May 2013; IEEE: New York, NY, USA, 2013; pp. 4390–4395. [Google Scholar]
- Müller, M.S.; Hoffmann, L.; Christopher Buck, T.; Walter Koch, A. Fiber Bragg grating-based force-torque sensor with six degrees of freedom. Int. J. Optomechatron. 2009, 3, 201–214. [Google Scholar] [CrossRef]
- Peirs, J.; Clijnen, J.; Reynaerts, D.; Van Brussel, H.; Herijgers, P.; Corteville, B.; Boone, S. A micro optical force sensor for force feedback during minimally invasive robotic surgery. Sen. Actuators A Phys. 2004, 115, 447–455. [Google Scholar] [CrossRef]
- Shahzada, K.S.; Yurkewich, A.; Xu, R.; Patel, R.V. Sensorization of a surgical robotic instrument for force sensing. Optical Fibers and Sensors for Medical Diagnostics and Treatment Applications XVI. Int. Soc. Opt. Photonics 2016, 9702, 97020U. [Google Scholar]
- Xu, R.; Yurkewich, A.; Patel, R.V. Curvature, torsion, and force sensing in continuum robots using helically wrapped FBG sensors. IEEE Robot. Autom. Lett. 2016, 1, 1052–1059. [Google Scholar] [CrossRef]
- Song, H.S.; Jeong, J.W.; Lee, J.J. Optical fiber Bragg grating (FBG) force reflection sensing system of surgical tool for minimally invasive surgery. In Proceedings of the 2014 9th IEEE Conference on Industrial Electronics and Applications, Hangzhou, China, 9–11 June 2014; IEEE: New York, NY, USA, 2014; pp. 478–482. [Google Scholar]
- Puangmali, P.; Liu, H.; Seneviratne, L.D.; Dasgupta, P.; Althoefer, K. Miniature 3-axis distal force sensor for minimally invasive surgical palpation. IEEE/Asme Trans. Mechatron. 2011, 17, 646–656. [Google Scholar] [CrossRef]
- Gafford, J.B.; Wood, R.J.; Walsh, C.J. Self-assembling, low-cost, and modular mm-scale force sensor. IEEE Sens. J. 2015, 16, 69–76. [Google Scholar] [CrossRef]
- Xu, R. Modeling, Sensorization and Control of Concentric-Tube Robots. Ph.D. Thesis, University of Western Ontario, London, ON, Canada, 2016. [Google Scholar]
- Shahbazi, M.; Atashzar, S.F.; Patel, R.V. A dual-user teleoperated system with virtual fixtures for robotic surgical training. In Proceedings of the 2013 IEEE International Conference on Robotics and Automation, Karlsruhe, Germany, 6–10 May 2013; IEEE: New York, NY, USA, 2013; pp. 3639–3644. [Google Scholar]
- Bowyer, S.A.; y Baena, F.R. Dissipative control for physical human–robot interaction. IEEE Trans. Robot. 2015, 31, 1281–1293. [Google Scholar] [CrossRef]
- Abbott, J.J.; Okamura, A.M. Stable Forbidden-Region Virtual Fixtures for Bilateral Telemanipulation. J. Dyn. Syst. Meas. Control 2005, 128, 53–64. [Google Scholar] [CrossRef]
- Ryu, J.H.; Preusche, C.; Hannaford, B.; Hirzinger, G. Time domain passivity control with reference energy following. IEEE Trans. Control Syst. Technol. 2005, 13, 737–742. [Google Scholar]
- Hashtrudi-Zaad, K.; Salcudean, S.E. Analysis of control architectures for teleoperation systems with impedance/admittance master and slave manipulators. Int. J. Robot. Res. 2001, 20, 419–445. [Google Scholar] [CrossRef]
- Haddadi, A.; Razi, K.; Hashtrudi-Zaad, K. Operator dynamics consideration for less conservative coupled stability condition in bilateral teleoperation. IEEE/ASME Trans. Mechatron. 2015, 20, 2463–2475. [Google Scholar] [CrossRef]
- Shahbazi, M.; Atashzar, S.F.; Tavakoli, M.; Patel, R.V. Position-force domain passivity of the human arm in telerobotic systems. IEEE/ASME Trans. Mechatron. 2018, 23, 552–562. [Google Scholar] [CrossRef]
- Quek, Z.F.; Schorr, S.B.; Nisky, I.; Okamura, A.M.; Provancher, W.R. Augmentation of stiffness perception with a 1-degree-of-freedom skin stretch device. IEEE Trans. Hum. Mach. Syst. 2014, 44, 731–742. [Google Scholar] [CrossRef]
- Schorr, S.B.; Quek, Z.F.; Romano, R.Y.; Nisky, I.; Provancher, W.R.; Okamura, A.M. Sensory substitution via cutaneous skin stretch feedback. In Proceedings of the 2013 IEEE International Conference on Robotics and Automation, Karlsruhe, Germany, 6–10 May 2013; IEEE: New York, NY, USA, 2013; pp. 2341–2346. [Google Scholar]
- Nisky, I.; Mussa-Ivaldi, F.A.; Karniel, A. A regression and boundary-crossing-based model for the perception of delayed stiffness. IEEE Trans. Haptics 2008, 1, 73–82. [Google Scholar] [CrossRef]
- Quek, Z.F.; Schorr, S.B.; Nisky, I.; Okamura, A.M.; Provancher, W.R. Sensory augmentation of stiffness using fingerpad skin stretch. In Proceedings of the 2013 World Haptics Conference (WHC), Daejeon, Korea, 14–17 April 2013; IEEE: New York, NY, USA, 2013; pp. 467–472. [Google Scholar]
- Rayman, R.; Primak, S.; Patel, R.; Moallem, M.; Morady, R.; Tavakoli, M.; Subotic, V.; Galbraith, N.; Van Wynsberghe, A.; Croome, K. Effects of latency on telesurgery: An experimental study. In International Conference on Medical Image Computing and Computer-Assisted Intervention; Springer: Berlin/Heidelberg, Germany, 2005; pp. 57–64. [Google Scholar]
- Rayman, R.; Croome, K.; Galbraith, N.; McClure, R.; Morady, R.; Peterson, S.; Smith, S.; Subotic, V.; Van Wynsberghe, A.; Patel, R.; et al. Robotic telesurgery: A real-world comparison of ground-and satellite-based internet performance. Int. J. Med. Robot. Comput. Assist. Surg. 2007, 3, 111–116. [Google Scholar] [CrossRef]
- Nguan, C.; Miller, B.; Patel, R.; Luke, P.P.; Schlachta, C.M. Pre-clinical remote telesurgery trial of a da Vinci telesurgery prototype. Int. J. Med. Robot. Comput. Assist. Surg. 2008, 4, 304–309. [Google Scholar] [CrossRef]
- Pressman, A.; Welty, L.J.; Karniel, A.; Mussa-Ivaldi, F.A. Perception of delayed stiffness. Int. J. Robot. Res. 2007, 26, 1191–1203. [Google Scholar] [CrossRef]
- Simsek, M.; Aijaz, A.; Dohler, M.; Sachs, J.; Fettweis, G. 5G-enabled tactile internet. IEEE J. Sel. Areas Commun. 2016, 34, 460–473. [Google Scholar] [CrossRef]
- Aijaz, A.; Dohler, M.; Aghvami, A.H.; Friderikos, V.; Frodigh, M. Realizing the tactile Internet: Haptic communications over next generation 5G cellular networks. IEEE Wirel. Commun. 2016, 24, 82–89. [Google Scholar] [CrossRef]
- Polushin, I.G.; Takhmar, A.; Patel, R.V. Projection-based force-reflection algorithms with frequency separation for bilateral teleoperation. IEEE/ASME Trans. Mechatron. 2014, 20, 143–154. [Google Scholar] [CrossRef]
- Ryu, J.H.; Kwon, D.S.; Hannaford, B. Stable teleoperation with time-domain passivity control. IEEE Trans. Robot. Autom. 2004, 20, 365–373. [Google Scholar] [CrossRef]
- Guo, J.; Liu, C.; Poignet, P. A Scaled Bilateral Teleoperation System for Robotic-Assisted Surgery with Time Delay. J. Intell. Robot. Syst. 2019, 95, 165–192. [Google Scholar] [CrossRef]
- Hao, S.; Hu, L.; Liu, P.X. Sliding Mode Control for a Surgical Teleoperation System via a Disturbance Observer. IEEE Access 2019, 7, 43383–43393. [Google Scholar] [CrossRef]
- Ye, Y.; Liu, P.X. Improving trajectory tracking in wave-variable-based teleoperation. IEEE/ASME Trans. Mechatron. 2009, 15, 321–326. [Google Scholar]
- Abbou, C.C.; Hoznek, A.; Salomon, L.; Olsson, L.E.; Lobontiu, A.; Saint, F.; Cicco, A.; Antiphon, P.; Chopin, D. Laparoscopic radical prostatectomy with a remote controlled robot. J. Urol. 2001, 165, 1964–1966. [Google Scholar] [CrossRef]
- Nia Kosari, S.; Rydén, F.; Lendvay, T.S.; Hannaford, B.; Chizeck, H.J. Forbidden region virtual fixtures from streaming point clouds. Adv. Robot. 2014, 28, 1507–1518. [Google Scholar] [CrossRef]
- Ren, J.; Patel, R.V.; McIsaac, K.A.; Guiraudon, G.; Peters, T.M. Dynamic 3-D virtual fixtures for minimally invasive beating heart procedures. IEEE Trans. Med. Imaging 2008, 27, 1061–1070. [Google Scholar]
- Abbott, J.J.; Hager, G.D.; Okamura, A.M. Steady-hand teleoperation with virtual fixtures. In Proceedings of the 12th IEEE International Workshop on Robot and Human Interactive Communication, Millbrae, CA, USA, 2 November 2003; IEEE: New York, NY, USA, 2003; pp. 145–151. [Google Scholar]
- Charles, S. Dexterity enhancement for surgery. In Computer-Integrated Surgery: Technology and Clinical Applications; MIT Press: Cambridge, MA, USA, 1996; pp. 467–471. [Google Scholar]
- Riviere, C.N.; Rader, R.S.; Thakor, N.V. Adaptive cancelling of physiological tremor for improved precision in microsurgery. IEEE Trans. Biomed. Eng. 1998, 45, 839–846. [Google Scholar] [CrossRef] [PubMed]
- Veluvolu, K.C.; Latt, W.T.; Ang, W.T. Double adaptive bandlimited multiple Fourier linear combiner for real-time estimation/filtering of physiological tremor. Biomed. Signal Process. Control 2010, 5, 37–44. [Google Scholar] [CrossRef]
- Veluvolu, K.C.; Ang, W.T. Estimation of physiological tremor from accelerometers for real-time applications. Sensors 2011, 11, 3020–3036. [Google Scholar] [CrossRef] [PubMed]
- Atashzar, S.F.; Shahbazi, M.; Samotus, O.; Tavakoli, M.; Jog, M.S.; Patel, R.V. Characterization of upper-limb pathological tremors: Application to design of an augmented haptic rehabilitation system. IEEE J. Sel. Top. Signal Process. 2016, 10, 888–903. [Google Scholar] [CrossRef]
- Gras, G.; Leibrandt, K.; Wisanuvej, P.; Giataganas, P.; Seneci, C.A.; Ye, M.; Shang, J.; Yang, G.Z. Implicit gaze-assisted adaptive motion scaling for highly articulated instrument manipulation. In Proceedings of the 2017 IEEE International Conference on Robotics and Automation (ICRA), Singapore, 29 May–3 June 2017; IEEE: New York, NY, USA, 2017; pp. 4233–4239. [Google Scholar]
- Wang, Y.; Veluvolu, K. Time-frequency decomposition of band-limited signals with BMFLC and Kalman filter. In Proceedings of the 2012 7th IEEE Conference on Industrial Electronics and Applications (ICIEA), Singapore, 18–20 July 2012; IEEE: New York, NY, USA, 2012; pp. 582–587. [Google Scholar]
- Wang, F.; Balakrishnan, V. Robust Kalman filters for linear time-varying systems with stochastic parametric uncertainties. IEEE Trans. Signal Process. 2002, 50, 803–813. [Google Scholar] [CrossRef]
- Reif, K.; Gunther, S.; Yaz, E.; Unbehauen, R. Stochastic stability of the discrete-time extended Kalman filter. IEEE Trans. Autom. Control 1999, 44, 714–728. [Google Scholar] [CrossRef]
- Taghirad, H.; Atashzar, S.; Shahbazi, M. Robust solution to three-dimensional pose estimation using composite extended Kalman observer and Kalman filter. IET Comput. Vis. 2012, 6, 140–152. [Google Scholar] [CrossRef]
- Bowthorpe, M.; Tavakoli, M.; Becher, H.; Howe, R. Smith predictor-based robot control for ultrasound-guided teleoperated beating-heart surgery. IEEE J. Biomed. Health Inform. 2013, 18, 157–166. [Google Scholar] [CrossRef]
- Tuna, E.E.; Franke, T.J.; Bebek, O.; Shiose, A.; Fukamachi, K.; Cavusoglu, M.C. Heart motion prediction based on adaptive estimation algorithms for robotic-assisted beating heart surgery. IEEE Trans. Robot. 2012, 29, 261–276. [Google Scholar] [CrossRef]
- Bebek, O.; Cavusoglu, M.C. Intelligent control algorithms for robotic-assisted beating heart surgery. IEEE Trans. Robot. 2007, 23, 468–480. [Google Scholar] [CrossRef]
- Liang, F.; Yu, Y.; Wang, H.; Meng, X. Heart motion prediction in robotic-assisted beating heart surgery: A nonlinear fast adaptive approach. Int. J. Adv. Robot. Syst. 2013, 10, 82. [Google Scholar] [CrossRef]
- Bowthorpe, M.; Tavakoli, M. Generalized predictive control of a surgical robot for beating-heart surgery under delayed and slowly-sampled ultrasound image data. IEEE Robot. Autom. Lett. 2016, 1, 892–899. [Google Scholar] [CrossRef]
- Vrooijink, G.J.; Denasi, A.; Grandjean, J.G.; Misra, S. Model predictive control of a robotically actuated delivery sheath for beating heart compensation. Int. J. Robot. Res. 2017, 36, 193–209. [Google Scholar] [CrossRef] [PubMed]
- Ortmaier, T.; Groger, M.; Boehm, D.H.; Falk, V.; Hirzinger, G. Motion estimation in beating heart surgery. IEEE Trans. Biomed. Eng. 2005, 52, 1729–1740. [Google Scholar] [CrossRef]
- Shahbazi, M.; Atashzar, S.F.; Ward, C.; Talebi, H.A.; Patel, R.V. Multimodal Sensorimotor Integration for Expert-in-the-Loop Telerobotic Surgical Training. IEEE Trans. Robot. 2018, 34, 1549–1564. [Google Scholar] [CrossRef]
- Liu, F.; Lelevé, A.; Eberard, D.; Redarce, T. A dual-user teleoperation system with online authority adjustment for haptic training. In Proceedings of the 2015 37th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), Milan, Italy, 25–29 August 2015; IEEE: New York, NY, USA, 2015; pp. 1168–1171. [Google Scholar]
- Liu, F.; Licona, A.R.; Lelevé, A.; Eberard, D.; Pham, M.T.; Redarce, T. An Energy-Based Approach for n-d.o.f. Passive Dual-User Haptic Training Systems. Robotica 2019, 38, 1155–1175. [Google Scholar] [CrossRef]
- Ruszkowski, A.; Schneider, C.; Mohareri, O.; Salcudean, S. Bimanual teleoperation with heart motion compensation on the da Vinci® Research Kit: Implementation and preliminary experiments. In Proceedings of the 2016 IEEE International Conference on Robotics and Automation (ICRA), Stockholm, Sweden, 16–21 May 2016; IEEE: New York, NY, USA, 2016; pp. 4101–4108. [Google Scholar]
- Yuen, S.G.; Perrin, D.P.; Vasilyev, N.V.; Pedro, J.; Howe, R.D. Force tracking with feed-forward motion estimation for beating heart surgery. IEEE Trans. Robot. 2010, 26, 888–896. [Google Scholar] [CrossRef]
- Atashzar, S.F.; Khalaji, I.; Shahbazi, M.; Talasaz, A.; Patel, R.V.; Naish, M.D. Robot-assisted lung motion compensation during needle insertion. In Proceedings of the 2013 IEEE International Conference on Robotics and Automation(ICRA), Karlsruhe, Germany, 6–10 May 2013; IEEE: New York, NY, USA, 2013; pp. 1682–1687. [Google Scholar] [CrossRef]
- Kim, Y.J.; Seo, J.H.; Kim, H.R.; Kim, K.G. Impedance and admittance control for respiratory-motion compensation during robotic needle insertion—A preliminary test. Int. J. Med. Robot. Comput. Assist. Surg. 2017, 13, e1795. [Google Scholar] [CrossRef]
- Gil, J.J.; Ugartemendia, A.; Diaz, I. Stability Analysis and User Perception of Haptic Rendering Combining Virtual Elastic, Viscous and Inertial Effects. Appl. Sci. 2020, 10, 8807. [Google Scholar] [CrossRef]
- Rosenberg, L.B. Virtual fixtures: Perceptual tools for telerobotic manipulation. In Proceedings of the IEEE Virtual Reality Annual International Symposium, Seattle, WA, USA, 18–22 September 1993; IEEE: New York, NY, USA, 1993; pp. 76–82. [Google Scholar]
- Jakopec, M.; y Baena, F.R.; Harris, S.J.; Gomes, P.; Cobb, J.; Davies, B.L. The hands-on orthopaedic robot “Acrobot”: Early clinical trials of total knee replacement surgery. IEEE Trans. Robot. Autom. 2003, 19, 902–911. [Google Scholar] [CrossRef]
- Powell, D.; O’Malley, M.K. The task-dependent efficacy of shared-control haptic guidance paradigms. IEEE Trans. Haptics 2012, 5, 208–219. [Google Scholar] [CrossRef] [PubMed]
- Huegel, J.C.; O’Malley, M.K. Progressive haptic and visual guidance for training in a virtual dynamic task. In Proceedings of the 2010 IEEE Haptics Symposium, Salt Lake City, UT, USA, 18–20 March 2009; IEEE: New York, NY, USA, 2010; pp. 343–350. [Google Scholar]
- Shahbazi, M.; Atashzar, S.F.; Talebi, H.A.; Patel, R.V. Novel Cooperative Teleoperation Framework: Multi-Master/Single-Slave System. IEEE/ASME Trans. Mechatron. 2015, 20, 1668–1679. [Google Scholar] [CrossRef]
- Atashzar, S.F.; Shahbazi, M.; Patel, R.V. Haptics-enabled interactive neurorehabilitation mechatronics: Classification, functionality, challenges and ongoing research. Mechatronics 2019, 57, 1–19. [Google Scholar] [CrossRef]
- Tavakoli, M.; Carriere, J.; Torabi, A. Robotics, Smart Wearable Technologies, and Autonomous Intelligent Systems for Healthcare During the COVID-19 Pandemic: An Analysis of the State of the Art and Future Vision. Adv. Intell. Syst. 2020, 2, 2000071. [Google Scholar] [CrossRef]
- Tiwari, K.; Kumar, S.; Tiwari, R. FOG Assisted Healthcare Architecture for Pre-Operative Support to Reduce Latency. Procedia Comput. Sci. 2020, 167, 1312–1324. [Google Scholar] [CrossRef]
- Bhaskar, S.; Bradley, S.; Sakhamuri, S.; Moguilner, S.; Chattu, V.K.; Pandya, S.; Schroeder, S.; Ray, D.; Banach, M. Designing Futuristic Telemedicine Using Artificial Intelligence and Robotics in the COVID-19 Era. Front. Public Health 2020, 8, 708. [Google Scholar] [CrossRef]
- Antón, D.; Kurillo, G.; Goñi, A.; Illarramendi, A.; Bajcsy, R. Real-time communication for Kinect-based telerehabilitation. Future Gener. Comput. Syst. 2017, 75, 72–81. [Google Scholar] [CrossRef]
- Dandanov, N.; Semov, P.; Ivanov, A.; Christoff, N.; Poulkov, V. Communication Framework for Tele-rehabilitation Systems with QoS Guarantee. MATEC Web Conf. 2017, 125, 03008. [Google Scholar] [CrossRef]
- Kosuge, K.; Ishikawa, J.; Furuta, K.; Sakai, M. Control of single-master multi-slave manipulator system using VIM. In Proceedings of the IEEE International Conference on Robotics and Automation, Cincinnati, OH, USA, 13–18 May 1990; IEEE: New York, NY, USA, 1990; pp. 1172–1177. [Google Scholar]
- Lee, D.; Spong, M.W. Bilateral teleoperation of multiple cooperative robots over delayed communication networks: Theory. In Proceedings of the 2005 IEEE International Conference on Robotics and Automation, Barcelona, Spain, 18–22 April 2005; IEEE: New York, NY, USA, 2005; pp. 360–365. [Google Scholar]
- Hwang, G.; Hashimoto, H. Development of a human-robot-shared controlled teletweezing system. IEEE Trans. Control Syst. Technol. 2007, 15, 960–966. [Google Scholar] [CrossRef]
- Lee, D.; Franchi, A.; Son, H.I.; Ha, C.; Bülthoff, H.H.; Giordano, P.R. Semiautonomous haptic teleoperation control architecture of multiple unmanned aerial vehicles. IEEE/ASME Trans. Mechatron. 2013, 18, 1334–1345. [Google Scholar] [CrossRef]
- Sun, D.; Naghdy, F.; Du, H. Stability control of force-reflected nonlinear multilateral teleoperation system under time-varying delays. J. Sens. 2016, 2016, 4316024. [Google Scholar] [CrossRef]
- Malysz, P.; Sirouspour, S. Cooperative teleoperation control with projective force mappings. In Proceedings of the 2010 IEEE Haptics Symposium, Waltham, MA, USA, 25–26 March 2010; IEEE: New York, NY, USA, 2010; pp. 301–308. [Google Scholar]
- Li, J.; Tavakoli, M.; Huang, Q. Stability of cooperative teleoperation using haptic devices with complementary degrees of freedom. IET Control Theory Appl. 2014, 8, 1062–1070. [Google Scholar] [CrossRef]
- Goldberg, K.; Chen, B.; Solomon, R.; Bui, S.; Farzin, B.; Heitler, J.; Poon, D.; Smith, G. Collaborative teleoperation via the internet. In Proceedings of the 2000 ICRA Millennium Conference IEEE International Conference on Robotics and Automation, Symposia Proceedings (Cat. No. 00CH37065), San Francisco, CA, USA, 24–28 April 2000; IEEE: New York, NY, USA, 2000; Volume 2, pp. 2019–2024. [Google Scholar]
- Chong, N.Y.; Kotoku, T.; Ohba, K.; Komoriya, K.; Tanie, K.; Oaki, J.; Hashimoto, H.; Ozaki, F.; Maeda, K.; Matsuhira, N. A collaborative multi-site teleoperation over an ISDN. Mechatronics 2003, 13, 957–979. [Google Scholar] [CrossRef]
- Passenberg, C.; Peer, A.; Buss, M. Model-mediated teleoperation for multi-operator multi-robot systems. In Proceedings of the 2010 IEEE/RSJ International Conference on Intelligent Robots and Systems, Taipei, Taiwan, 18–22 October 2010; IEEE: New York, NY, USA, 2010; pp. 4263–4268. [Google Scholar]
- Feth, D.; Peer, A.; Buss, M. Enhancement of multi-user teleoperation systems by prediction of dyadic haptic interaction. In Experimental Robotics; Springer: Berlin/Heidelberg, Germany, 2014; pp. 855–869. [Google Scholar]
- Chen, Z.; Pan, Y.J.; Gu, J. Integrated adaptive robust control for multilateral teleoperation systems under arbitrary time delays. Int. J. Robust Nonlinear Control 2016, 26, 2708–2728. [Google Scholar] [CrossRef]
- Sirouspour, S.; Setoodeh, P. Multi-operator/multi-robot teleoperation: An adaptive nonlinear control approach. In Proceedings of the 2005 IEEE/RSJ International Conference on Intelligent Robots and Systems, Edmonton, AB, Canada, 2–6 August 2005; IEEE: New York, NY, USA, 2005; pp. 1576–1581. [Google Scholar]
- Lo, W.t.; Liu, Y.; Elhajj, I.H.; Xi, N.; Wang, Y.; Fukuda, T. Cooperative teleoperation of a multirobot system with force reflection via internet. IEEE/ASME Trans. Mechatron. 2004, 9, 661–670. [Google Scholar] [CrossRef]
- Setoodeh, P.; Sirouspour, S.; Shahdi, A. Discrete-time multi-model control for cooperative teleoperation under time delay. In Proceedings of the 2006 IEEE International Conference on Robotics and Automation, Orlando, FL, USA, 15–19 May 2006; IEEE: New York, NY, USA, 2006; pp. 2921–2926. [Google Scholar]
- Li, Z.; Xia, Y.; Sun, F. Adaptive fuzzy control for multilateral cooperative teleoperation of multiple robotic manipulators under random network-induced delays. IEEE Trans. Fuzzy Syst. 2013, 22, 437–450. [Google Scholar] [CrossRef]
- Zhai, D.H.; Xia, Y. Adaptive fuzzy control of multilateral asymmetric teleoperation for coordinated multiple mobile manipulators. IEEE Trans. Fuzzy Syst. 2015, 24, 57–70. [Google Scholar] [CrossRef]
- Zhai, D.H.; Xia, Y. Multilateral telecoordinated control of multiple robots with uncertain kinematics. IEEE Trans. Neural Netw. Learn. Syst. 2017, 29, 2808–2822. [Google Scholar] [CrossRef]
- Sun, D.; Naghdy, F.; Du, H. Enhancing flexibility of the dual-master-dual-slave multilateral teleoperation system. In Proceedings of the 2015 IEEE Conference on Control Applications (CCA), Sydney, NSW, Australia, 21–23 September 2015; IEEE: New York, NY, USA, 2015; pp. 300–305. [Google Scholar]
- Kanno, T.; Yokokohji, Y. Multilateral teleoperation control over time-delayed computer networks using wave variables. In Proceedings of the 2012 IEEE Haptics Symposium (HAPTICS), Vancouver, BC, Canada, 4–7 March 2012; IEEE: New York, NY, USA, 2012; pp. 125–131. [Google Scholar]
- Panzirsch, M.; Artigas, J.; Ryu, J.H.; Ferre, M. Multilateral control for delayed teleoperation. In Proceedings of the 2013 16th International Conference on Advanced Robotics (ICAR), Montevideo, Uruguay, 25–29 November 2013; IEEE: New York, NY, USA, 2013; pp. 1–6. [Google Scholar]
- Van Quang, H.; Ryu, J.H. Stable multilateral teleoperation with time domain passivity approach. In Proceedings of the 2013 IEEE/RSJ International Conference on Intelligent Robots and Systems; IEEE: New York, NY, USA, 2013; pp. 5890–5895. [Google Scholar]
- Shahbazi, M.; Atashzar, S.F.; Tavakoli, M.; Patel, R.V. Robotics-Assisted Mirror Rehabilitation Therapy: A Therapist-in-the-Loop Assist-as-Needed Architecture. IEEE/ASME Trans. Mechatron. 2016, 21, 1954–1965. [Google Scholar] [CrossRef]
- Melis, A.P. The evolutionary roots of human collaboration: Coordination and sharing of resources. Ann. N. Y. Acad. Sci. 2013, 1299, 68–76. [Google Scholar] [CrossRef]
- Sirouspour, S. Modeling and control of cooperative teleoperation systems. IEEE Trans. Robot. 2005, 21, 1220–1225. [Google Scholar] [CrossRef]
- Buttolo, P.; Oboe, R.; Hannaford, B. Architectures for shared haptic virtual environments. Comput. Graph. 1997, 21, 421–429. [Google Scholar] [CrossRef]
- Shamaei, K.; Che, Y.; Murali, A.; Sen, S.; Patil, S.; Goldberg, K.; Okamura, A.M. A paced shared-control teleoperated architecture for supervised automation of multilateral surgical tasks. In Proceedings of the 2015 IEEE/RSJ International Conference on Intelligent Robots and Systems (IROS), Hamburg, Germany, 28 September–2 October 2015; IEEE: New York, NY, USA, 2015; pp. 1434–1439. [Google Scholar]
- Williams, R.L.; Harrison, F.W.; Soloway, D.L. Shared control of multiple-manipulator, sensor-based telerobotic systems. In Proceedings of the International Conference on Robotics and Automation, Albuquerque, NM, USA, 25 April 1997; IEEE: New York, NY, USA, 1997; Volume 2, pp. 962–967. [Google Scholar]
- Shahbazi, M.; Atashzar, S.F.; Patel, R.V. A framework for supervised robotics-assisted mirror rehabilitation therapy. In Proceedings of the 2014 IEEE/RSJ International Conference on Intelligent Robots and Systems, Chicago, IL, USA, 14–18 September 2014; IEEE: New York, NY, USA, 2014; pp. 3567–3572. [Google Scholar] [CrossRef]
- Shahbazi, M.; Atashzar, S.F.; Tavakoli, M.; Patel, R.V. Therapist-in-the-loop robotics-assisted mirror rehabilitation therapy: An assist-as-needed framework. In Proceedings of the 2015 IEEE International Conference on Robotics and Automation (ICRA), Seattle, WA, USA, 26–30 May 2015; IEEE: New York, NY, USA, 2015; pp. 5910–5915. [Google Scholar] [CrossRef]
- Rakhsha, R.; Constantinescu, D. Distributed haptic cooperation with passive multirate wave communications. In Proceedings of the 2012 IEEE Haptics Symposium (HAPTICS), Vancouver, BC, Canada, 4–7 March 2012; IEEE: New York, NY, USA, 2012; pp. 117–123. [Google Scholar]
- Lee, D.; Huang, K. Peer-to-peer control architecture for multiuser haptic collaboration over undirected delayed packet-switching network. In Proceedings of the 2010 IEEE International Conference on Robotics and Automation, Anchorage, AK, USA, 3–7 May 2010; IEEE: New York, NY, USA, 2010; pp. 1333–1338. [Google Scholar]
- Katsura, S.; Suzuyama, T.; Ohishi, K. A realization of multilateral force feedback control for cooperative motion. IEEE Trans. Ind. Electron. 2007, 54, 3298–3306. [Google Scholar] [CrossRef]
- Shahbazi, M.; Atashzar, S.F.; Talebi, H.A.; Patel, R.V. An expertise-oriented training framework for robotics-assisted surgery. In Proceedings of the 2014 IEEE international conference on robotics and automation (ICRA), Hong Kong, China, 31 May–7 June 2014; IEEE: New York, NY, USA, 2014; pp. 5902–5907. [Google Scholar]
- Carignan, C.R.; Olsson, P.A. Cooperative control of virtual objects over the internet using force-reflecting master arms. In Proceedings of the IEEE International Conference on Robotics and Automation, 2004 ICRA’04, New Orleans, LA, USA, 26 April–1 May 2004; IEEE: New York, NY, USA, 2004; Volume 2, pp. 1221–1226. [Google Scholar]
- Reed, K.; Peshkin, M.; Hartmann, M.J.; Grabowecky, M.; Patton, J.; Vishton, P.M. Haptically linked dyads: Are two motor-control systems better than one? Psychol. Sci. 2006, 17, 365–366. [Google Scholar] [CrossRef]
- Ganesh, G.; Takagi, A.; Osu, R.; Yoshioka, T.; Kawato, M.; Burdet, E. Two is better than one: Physical interactions improve motor performance in humans. Sci. Rep. 2014, 4, 3824. [Google Scholar] [CrossRef]
- Yano, H.; Iwata, H. Cooperative Work in Virtual Environment with Force Feed-back. Trans. Soc. Instrum. Control Eng. 1995, 31, 1495–1501. [Google Scholar] [CrossRef]
- Chebbi, B.; Lazaroff, D.; Bogsany, F.; Liu, P.X.; Ni, L.; Rossi, M. Design and implementation of a collaborative virtual haptic surgical training system. In Proceedings of the IEEE International Conference Mechatronics and Automation, Niagara Falls, ON, Canada, 29 July–1 August 2005; IEEE: New York, NY, USA, 2005; Volume 1, pp. 315–320. [Google Scholar]
- Gunn, C.; Hutchins, M.; Stevenson, D.; Adcock, M.; Youngblood, P. Using collaborative haptics in remote surgical training. In Proceedings of the First Joint Eurohaptics Conference and Symposium on Haptic Interfaces for Virtual Environment and Teleoperator Systems, World Haptics Conference, Pisa, Italy, 18–20 March 2005; IEEE: New York, NY, USA, 2005; pp. 481–482. [Google Scholar]
- Moghimi, S.; Sirouspour, S.; Malysz, P. Haptic-enabled collaborative training with generalized force and position mappings. In Proceedings of the 2008 Symposium on Haptic Interfaces for Virtual Environment and Teleoperator Systems, Reno, NE, USA, 13–14 March 2008; IEEE: New York, NY, USA, 2008; pp. 287–294. [Google Scholar]
- Khademian, B.; Hashtrudi-Zaad, K. Shared control architectures for haptic training: Performance and coupled stability analysis. Int. J. Robot. Res. 2011, 30, 1627–1642. [Google Scholar] [CrossRef]
- Shamaei, K.; Kim, L.; Okamura, A. Design and evaluation of a trilateral shared-control architecture for teleoperated training robots. In Proceedings of the Engineering in Medicine and Biology Society (EMBC), 2015 37th Annual International Conference of the IEEE, Milan, Italy, 25–29 August 2015; IEEE: New York, NY, USA, 2015; pp. 4887–4893. [Google Scholar] [CrossRef]
- Nudehi, S.S.; Mukherjee, R.; Ghodoussi, M. A shared-control approach to haptic interface design for minimally invasive telesurgical training. IEEE Trans. Control Syst. Technol. 2005, 13, 588–592. [Google Scholar] [CrossRef]
- Khademian, B.; Hashtrudi-Zaad, K. Dual-User Teleoperation Systems: New Multilateral Shared Control Architecture and Kinesthetic Performance Measures. IEEE/ASME Trans. Mechatron. 2012, 17, 895–906. [Google Scholar] [CrossRef]
- Khademian, B.; Hashtrudi-Zaad, K. A robust multilateral shared controller for dual-user teleoperation systems. In Proceedings of the 2008 Canadian Conference on Electrical and Computer Engineering, Niagara Falls, ON, Canada, 4–7 May 2008; IEEE: New York, NY, USA, 2008; pp. 1871–1876. [Google Scholar]
- Shahbazi, M.; Talebi, H.; Towhidkhah, F. A robust control architecture for dual user teleoperation system with time-delay. In Proceedings of the IECON 2010-36th Annual Conference on IEEE Industrial Electronics Society, Glendale, AZ, USA, 7–10 November 2010; IEEE: New York, NY, USA, 2010; pp. 1419–1423. [Google Scholar]
- Shahbazi, M.; Talebi, H.; Atashzar, S.; Towhidkhah, F.; Patel, R.; Shojaei, S. A new set of desired objectives for dual-user systems in the presence of unknown communication delay. In Proceedings of the 2011 IEEE/ASME International Conference on Advanced Intelligent Mechatronics (AIM), Budapest, Hungary, 3–7 July 2011; IEEE: New York, NY, USA, 2011; pp. 146–151. [Google Scholar]
- Shahbazi, M.; Atashzar, S.F.; Talebi, H.A.; Towhidkhah, F.; Yazdanpanah, M.J. A sliding-mode controller for dual-user teleoperation with unknown constant time delays. Robotica 2013, 31, 589. [Google Scholar] [CrossRef]
- Santacruz-Reyes, H.; Garcia-Valdovinos, L.G.; Jiménez-Hernández, H.; Salgado-Jiménez, T.; Garcia-Zarco, L.A. Higher order sliding mode based impedance control for dual-user bilateral teleoperation under unknown constant time delay. In Proceedings of the 2015 IEEE/RSJ International Conference on Intelligent Robots and Systems (IROS), Hamburg, Germany, 28 September–2 October 2015; IEEE: New York, NY, USA, 2015; pp. 5209–5215. [Google Scholar]
- Niemeyer, G.; Preusche, C.; Stramigioli, S.; Lee, D. Telerobotics. In Springer Handbook of Robotics; Springer: Berlin/Heidelberg, Germany, 2016; pp. 1085–1108. [Google Scholar]
- Groten, R.; Feth, D.; Goshy, H.; Peer, A.; Kenny, D.A.; Buss, M. Experimental analysis of dominance in haptic collaboration. In Proceedings of the RO-MAN 2009-The 18th IEEE International Symposium on Robot and Human Interactive Communication, Toyama, Japan, 27 September–2 October 2009; IEEE: New York, NY, USA, 2009; pp. 723–729. [Google Scholar]
- Li, Z.; Ding, L.; Gao, H.; Duan, G.; Su, C.Y. Trilateral teleoperation of adaptive fuzzy force/motion control for nonlinear teleoperators with communication random delays. IEEE Trans. Fuzzy Syst. 2012, 21, 610–624. [Google Scholar] [CrossRef]
- Shahbazi, M. Expert-in-the-Loop Multilateral Telerobotics for Haptics-Enabled Motor Function and Skills Development. Ph.D. Thesis, The University of Western Ontario, London, ON, Canada, 2017. [Google Scholar]
- Patel, R.V.; Shadpey, F. Control of Redundant Robot Manipulators: Theory and Experiments; Springer Science & Business Media: Berlin/Heidelberg, Germany, 2005; Volume 316. [Google Scholar]
- Culmer, P.R.; Jackson, A.E.; Makower, S.; Richardson, R.; Cozens, J.A.; Levesley, M.C.; Bhakta, B.B. A control strategy for upper limb robotic rehabilitation with a dual robot system. IEEE/ASME Trans. Mechatron. 2009, 15, 575–585. [Google Scholar] [CrossRef]
- Hamel, W.R.; Humphreys, H.C.; Nycz, A.; Park, J.k.; Noakes, M.W. Large scale multi-fingered end-effector teleoperation. In Proceedings of the 2009 IEEE/RSJ International Conference on Intelligent Robots and Systems, St. Louis, MO, USA, 10–15 October 2009; IEEE: New York, NY, USA, 2009; pp. 3304–3310. [Google Scholar]
- Malysz, P.; Sirouspour, S. Trilateral teleoperation control of kinematically redundant robotic manipulators. Int. J. Robot. Res. 2011, 30, 1643–1664. [Google Scholar] [CrossRef]
- Fotoohi, M.; Sirouspour, S.; Capson, D. Stability and performance analysis of centralized and distributed multi-rate control architectures for multi-user haptic interaction. Int. J. Robot. Res. 2007, 26, 977–994. [Google Scholar] [CrossRef]
- Yasrebi, N.; Constantinescu, D. Centralized multi-user multi-rate haptic cooperation using wave transformation. In Proceedings of the 2009 International Conference on Mechatronics and Automation, Changchun, China, 9–12 August 2009; IEEE: New York, NY, USA, 2009; pp. 3816–3821. [Google Scholar]
- Sankaranarayanan, G.; Hannaford, B. Experimental internet haptic collaboration using virtual coupling schemes. In Proceedings of the 2008 Symposium on Haptic Interfaces for Virtual Environment and Teleoperator Systems, Reno, NE, USA, 13–14 March 2008; IEEE: New York, NY, USA, 2008; pp. 259–266. [Google Scholar]
- Sankaranarayanan, G.; Hannaford, B. Experimental comparison of internet haptic collaboration with time-delay compensation techniques. In Proceedings of the 2008 IEEE International Conference on Robotics and Automation, Pasadena, CA, USA, 19–23 May 2008; IEEE: New York, NY, USA, 2008; pp. 206–211. [Google Scholar]
- Mitra, P.; Niemeyer, G. Dynamic proxy objects in haptic simulations. In Proceedings of the IEEE Conference on Robotics, Automation and Mechatronics 2004; IEEE: New York, NY, USA, 2004; Volume 2, pp. 1054–1059. [Google Scholar]
- Cheong, J.; Niculescu, S.I.; Annaswamy, A.; Srinivasan, M.A. Motion synchronization in virtual environments with shared haptics and large time delays. In Proceedings of the First Joint Eurohaptics Conference and Symposium on Haptic Interfaces for Virtual Environment and Teleoperator Systems, World Haptics Conference, Pisa, Italy, 18–20 March 2005; IEEE: New York, NY, USA, 2005; pp. 277–282. [Google Scholar]
- Sankaranarayanan, G.; Hannaford, B. Virtual coupling schemes for position coherency in networked haptic environments. In Proceedings of the The First IEEE/RAS-EMBS International Conference on Biomedical Robotics and Biomechatronics, BioRob 2006, Pisa, Italy, 20-22 February 2006; IEEE: New York, NY, USA, 2006; pp. 853–858. [Google Scholar]
- Glencross, M.; Jay, C.; Feasel, J.; Kohli, L.; Whitton, M.; Hubbold, R. Effective cooperative haptic interaction over the internet. In Proceedings of the 2007 IEEE Virtual Reality Conference, Charlotte, NC, USA, 10–14 March 2007; IEEE: New York, NY, USA, 2007; pp. 115–122. [Google Scholar]
- Li, Z.; Constantinescu, D. Networked haptic cooperation using remote dynamic proxies. In Proceedings of the 2009 Second International Conferences on Advances in Computer-Human Interactions, Cancun, Mexico, 1–7 February 2009; IEEE: New York, NY, USA, 2009; pp. 243–248. [Google Scholar]
- Li, Z.; Constantinescu, D. Remote dynamic proxies for wave-based peer-to-peer haptic interaction. In Proceedings of the World Haptics 2009-Third Joint EuroHaptics conference and Symposium on Haptic Interfaces for Virtual Environment and Teleoperator Systems, Salt Lake City, UT, USA, 18–20 March 2009; IEEE: New York, NY, USA, 2009; pp. 553–558. [Google Scholar]
- Li, Z.; Constantinescu, D. Comparison of power-and wave-based control of remote dynamic proxies for networked haptic cooperation. In Proceedings of the 2009 International Conference on Mechatronics and Automation, Changchun, China, 9–12 August 2009; IEEE: New York, NY, USA, 2009; pp. 66–71. [Google Scholar]
- Ryu, J.; Ha-Van, Q.; Jafari, A. Multilateral Teleoperation Over Communication Time Delay Using the Time-Domain Passivity Approach. IEEE Trans. Control. Syst. Technol. 2019. [Google Scholar] [CrossRef]
- Zakerimanesh, A.; Hashemzadeh, F.; Ghiasi, A.R. Dual-user nonlinear teleoperation subjected to varying time delay and bounded inputs. ISA Trans. 2017, 68, 33–47. [Google Scholar] [CrossRef]
- Wang, X.G.; Moallem, M.; Patel, R.V. An Internet-based distributed multiple-telerobot system. IEEE Trans. Syst. Man, Cybern. Part A Syst. Hum. 2003, 33, 627–634. [Google Scholar] [CrossRef]
- Chong, N.Y.; Kawabata, S.; Ohba, K.; Kotoku, T.; Komoriya, K.; Takase, K.; Tanie, K. Multioperator teleoperation of multirobot systems with time delay: Part I—Aids for collision-free control. Presence Teleoperators Virtual Environ. 2002, 11, 277–291. [Google Scholar] [CrossRef]
- Tumerdem, U.; Ohnishi, K. Multi-robot teleoperation under dynamically changing network topology. In Proceedings of the 2009 IEEE International Conference on Industrial Technology, Gippsland, VIC, Australia, 10–13 February 2009; IEEE: New York, NY, USA, 2009; pp. 1–6. [Google Scholar]
- Li, Y.; Patoglu, V.; O’Malley, M.K. Negative efficacy of fixed gain error reducing shared control for training in virtual environments. ACM Trans. Appl. Percept. 2009, 6, 1–21. [Google Scholar] [CrossRef]
- Hayati, S.; Lee, T.; Tso, K.; Backes, P.; Lloyd, J. A testbed for a unified teleoperated-autonomous dual-arm robotic system. In Proceedings of the IEEE International Conference on Robotics and Automation, Cincinnati, OH, USA, 13–8 May 1990; IEEE: New York, NY, USA, 1990; pp. 1090–1095. [Google Scholar]
- Backes, P.G. Supervised autonomous control, shared control, and teleoperation for space servicing. In Sixth Annual Workshop on Space Operations Applications and Research (SOAR 1992); NASA: Washington, DC, USA, 1993; Volume 2, pp. 720–731. [Google Scholar]
- Hayati, S.; Venkataraman, S.T. Design and implementation of a robot control system with traded and shared control capability. In Proceedings of the 1989 International Conference on Robotics and Automation, Scottsdale, AZ, USA, 14–19 May 1989; IEEE: New York, NY, USA, 1989; Volume 3, pp. 1310–1315. [Google Scholar] [CrossRef]
- Backes, P.G.; Tso, K.S. UMI: An interactive supervisory and shared control system for telerobotics. In Proceedings of the IEEE International Conference on Robotics and Automation, Cincinnati, OH, USA, 13–18 May 1990; IEEE: New York, NY, USA, 1990; pp. 1096–1101. [Google Scholar]
- Yang, G.Z.; Cambias, J.; Cleary, K.; Daimler, E.; Drake, J.; Dupont, P.E.; Hata, N.; Kazanzides, P.; Martel, S.; Patel, R.V.P.; et al. Medical robotics—Regulatory, ethical, and legal considerations for increasing levels of autonomy. Sci. Robot. 2017, 2, 8638–8639. [Google Scholar] [CrossRef]
- Reed, K.B.; Peshkin, M.; Hartmann, M.J.; Patton, J.; Vishton, P.M.; Grabowecky, M. Haptic cooperation between people, and between people and machines. In Proceedings of the 2006 IEEE/RSJ International Conference on Intelligent Robots and Systems, Beijing, China, 9–15 October 2006; IEEE: New York, NY, USA, 2006; pp. 2109–2114. [Google Scholar]
- Li, Z.; Xia, Y.; Wang, D.; Zhai, D.H.; Su, C.Y.; Zhao, X. Neural network-based control of networked trilateral teleoperation with geometrically unknown constraints. IEEE Trans. Cybern. 2015, 46, 1051–1064. [Google Scholar] [CrossRef]
- Panzirsch, M.; Artigas, J.; Tobergte, A.; Kotyczka, P.; Preusche, C.; Albu-Schaeffer, A.; Hirzinger, G.; Artigas, J.; Tobergte, A.; Kotyczka, P.; et al. A peer-to-peer trilateral passivity control for delayed collaborative teleoperation. In Proceedings of the International Conference on Human Haptic Sensing and Touch Enabled Computer Applications, Tampere, Finland, 13–15 June 2012; Springer: Berlin/Heidelberg, Germany, 2012; pp. 395–406. [Google Scholar]
- Ghorbanian, A.; Rezaei, S.M.; Khoogar, A.R.; Zareinejad, M.; Baghestan, K. A novel control framework for nonlinear time-delayed Dual-master/Single-slave teleoperation. ISA Trans. 2013, 52, 268–277. [Google Scholar] [CrossRef] [PubMed]
- Huang, P.; Lu, Z. Auxiliary asymmetric dual-user shared control method for teleoperation. In Proceedings of the 2015 12th International Conference on Ubiquitous Robots and Ambient Intelligence (URAI), Goyang, Korea, 28–30 October 2015; IEEE: New York, NY, USA, 2015; pp. 267–272. [Google Scholar]
- Malysz, P.; Sirouspour, S. A kinematic control framework for single-slave asymmetric teleoperation systems. IEEE Trans. Robot. 2011, 27, 901–917. [Google Scholar] [CrossRef]
- Sheridan, T.B.; Verplank, W.L.; Brooks, T.L. Human and Computer Control of Undersea Teleoperators; Techreport 780815025; MIT: Arlington, VA, USA, 1978. [Google Scholar]
- Conway, L.; Volz, R.A.; Walker, M.W. Teleautonomous systems: Projecting and coordinating intelligent action at a distance. IEEE Trans. Robot. Autom. 1990, 6, 146–158. [Google Scholar] [CrossRef]
- Nichols, K.; Okamura, A. A framework for multilateral manipulation in surgical tasks. IEEE Trans. Autom. Sci. Eng. 2016, 13, 68–77. [Google Scholar] [CrossRef]
- Abbink, D.A.; Carlson, T.; Mulder, M.; de Winter, J.C.F.; Aminravan, F.; Gibo, T.L.; Boer, E.R. A Topology of Shared Control Systems—Finding Common Ground in Diversity. IEEE Trans. Hum. Mach. Syst. 2018, 48, 509–525. [Google Scholar] [CrossRef]
- Sutherland, G.R.; McBeth, P.B.; Louw, D.F. NeuroArm: An MR compatible robot for microsurgery. Int. Congr. Ser. 2003, 1256, 504–508. [Google Scholar] [CrossRef]
- Park, S.; Jang, N.; Ihn, Y.; Yang, S.; Jeong, J.; Yim, S.; Oh, S.R.; Kim, K.; Hwang, D. A tele-operated microsurgical forceps-driver with a variable stiffness haptic feedback master device. IEEE Robot. Autom. Lett. 2020, 5, 1946–1953. [Google Scholar] [CrossRef]
- Salcudean, S. Control for teleoperation and haptic interfaces. In Control Problems in Robotics and Automation; Siciliano, B., Valavanis, K., Eds.; Springer: Berlin/Heidelberg, Germany, 1998; Volume 230, pp. 51–66. [Google Scholar] [CrossRef]
- Cassilly, R.; Diodato, M.D.; Bottros, M.; Damiano, R.J. Optimizing motion scaling and magnification in robotic surgery. Surgery 2004, 136, 291–294. [Google Scholar] [CrossRef]
- Zhang, Z.; Dequidt, J.; Back, J.; Liu, H.; Duriez, C. Motion Control of Cable-Driven Continuum Catheter Robot Through Contacts. IEEE Robot. Autom. Lett. 2019, 4, 1852–1859. [Google Scholar] [CrossRef]
- Cho, J.H.; Kristalny, M.; Seo, J.; Lee, H.J.; Kim, K.; Woo, H.S. Control of Delayed Bilateral Teleoperation System for Robotic Tele-Echography. In Proceedings of the 2019 International Conference on Robotics and Automation (ICRA), Montreal, QC, Canada, 20–24 May 2019; IEEE: New York, NY, USA, 2019; pp. 2714–2720. [Google Scholar] [CrossRef]
- Sartori, E.; Tadiello, C.; Secchi, C.; Muradore, R. Tele-echography using a two-layer teleoperation algorithm with energy scaling. In Proceedings of the IEEE International Conference on Robotics and Automation, Montreal, QC, Canada, 20–24 May 2019; IEEE: New York, NY, USA, 2019; pp. 1569–1575. [Google Scholar] [CrossRef]
- Ferraguti, F.; Preda, N.; Manurung, A.; Bonfè, M.; Lambercy, O.; Gassert, R.; Muradore, R.; Fiorini, P.; Secchi, C. An Energy Tank-Based Interactive Control Architecture for Autonomous and Teleoperated Robotic Surgery. IEEE Trans. Robot. 2015, 31, 1073–1088. [Google Scholar] [CrossRef]
- Baayoun, M.; Daher, N.; Liermann, M. Reduced order indirect self-tuning regulator for a novel pneumatic tele-operation system. Proc. Inst. Mech. Engineers. Part I J. Syst. Control Eng. 2020, 234, 370–383. [Google Scholar] [CrossRef]
- Cheng, L.; Tavakoli, M. A multilateral impedance-controlled system for haptics-enabled surgical training and cooperation in beating-heart surgery. Int. J. Intell. Robot. Appl. 2019, 3, 314–325. [Google Scholar] [CrossRef]
- Li, Z.; Zhao, S.; Duan, J.; Su, C.; Yang, C.; Zhao, X. Human Cooperative Wheelchair With Brain–Machine Interaction Based on Shared Control Strategy. IEEE/ASME Trans. Mechatron. 2017, 22, 185–195. [Google Scholar] [CrossRef]
- Selvaggio, M.; Fontanelli, G.A.; Ficuciello, F.; Villani, L.; Siciliano, B. Passive Virtual Fixtures Adaptation in Minimally Invasive Robotic Surgery. IEEE Robot. Autom. Lett. 2018, 3, 3129–3136. [Google Scholar] [CrossRef]
- Ma, X.; Wang, P.; Ye, M.; Chiu, P.W.Y.; Li, Z. Shared Autonomy of a Flexible Manipulator in Constrained Endoluminal Surgical Tasks. IEEE Robot. Autom. Lett. 2019, 4, 3106–3112. [Google Scholar] [CrossRef]
- Moustris, G.P.; Mantelos, A.I.; Tzafestas, C.S. Shared control for motion compensation in robotic beating heart surgery. In Proceedings of the 2013 IEEE International Conference on Robotics and Automation, Karlsruhe, Germany, 6–10 May 2013; IEEE: New York, NY, USA, 2013; pp. 5819–5824. [Google Scholar] [CrossRef]
- Cheng, L.; Tavakoli, M. Ultrasound image guidance and robot impedance control for beating-heart surgery. Control Eng. Pract. 2018, 81, 9–17. [Google Scholar] [CrossRef]
- Pandya, A.; Reisner, L.A.; King, B.; Lucas, N.; Composto, A.; Klein, M.; Ellis, R.D. A Review of Camera Viewpoint Automation in Robotic and Laparoscopic Surgery. Robotics 2014, 3, 310–329. [Google Scholar] [CrossRef]
- Mylonas, G.P.; Darzi, A.; Yang, G.Z. Gaze-contingent control for minimally invasive robotic surgery. Comput. Aided Surg. 2006, 11, 256–266. [Google Scholar] [CrossRef]
- Park, J.; Park, W.J.; Lee, C.; Kim, M.; Kim, S.; Kim, H.J. Endoscopic Camera Manipulation planning of a surgical robot using Rapidly-Exploring Random Tree algorithm. In Proceedings of the 2015 15th International Conference on Control, Automation and Systems (ICCAS), Busan, Korea, 13–16 October 2015; IEEE: New York, NY, USA, 2015; pp. 1516–1519. [Google Scholar] [CrossRef]
- Eslamian, S.; Reisner, L.A.; Pandya, A.K. Development and evaluation of an autonomous camera control algorithm on the da Vinci Surgical System. Int. J. Med. Robot. Comput. Assist. Surg. 2020, 16, e2036. [Google Scholar] [CrossRef]
- Mariani, A.; Colaci, G.; Da Col, T.; Sanna, N.; Vendrame, E.; Menciassi, A.; De Momi, E. An Experimental Comparison Towards Autonomous Camera Navigation to Optimize Training in Robot Assisted Surgery. IEEE Robot. Autom. Lett. 2020, 5, 1461–1467. [Google Scholar] [CrossRef]
- Stachaczyk, M.; Atashzar, S.F.; Dupan, S.; Vujaklija, I.; Farina, D. Toward Universal Neural Interfaces for Daily Use: Decoding the Neural Drive to Muscles Generalises Highly Accurate Finger Task Identification Across Humans. IEEE Access 2020, 8, 149025–149035. [Google Scholar] [CrossRef]
- Merletti, R.; Farina, D. Surface Electromyography: Physiology, Engineering, and Applications; John Wiley & Sons: Hoboken, NJ, USA, 2016. [Google Scholar]
- Gardner, M.; Mancero Castillo, C.S.; Wilson, S.; Farina, D.; Burdet, E.; Khoo, B.C.; Atashzar, S.F.; Vaidyanathan, R. A Multimodal Intention Detection Sensor Suite for Shared Autonomy of Upper-Limb Robotic Prostheses. Sensors 2020, 20, 6097. [Google Scholar] [CrossRef] [PubMed]
- Zhuang, K.Z.; Sommer, N.; Mendez, V.; Aryan, S.; Formento, E.; D’Anna, E.; Artoni, F.; Petrini, F.; Granata, G.; Cannaviello, G.; et al. Shared human-robot proportional control of a dexterous myoelectric prosthesis. Nat. Mach. Intell. 2019, 1, 400–411. [Google Scholar] [CrossRef]
- Fracczak, L.; Szaniewski, M.; Podsedkowski, L. Share control of surgery robot master manipulator guiding tool along the standard path. Int. J. Med. Robot. Comput. Assist. Surg. 2019, 15, e1984. [Google Scholar] [CrossRef]
- Gopinath, D.; Jain, S.; Argall, B.D. Human-in-the-Loop Optimization of Shared Autonomy in Assistive Robotics. IEEE Robot. Autom. Lett. 2017, 2, 247–254. [Google Scholar] [CrossRef]
- Javdani, S.; Admoni, H.; Pellegrinelli, S.; Srinivasa, S.S.; Bagnell, J.A. Shared autonomy via hindsight optimization for teleoperation and teaming. Int. J. Robot. Res. 2018, 37, 717–742. [Google Scholar] [CrossRef]
- Licona Rodriguez, A.R.; Lelevé, A.; Pham, M.T.; Eberard, D. A multi-trainee architecture for haptic hands-on training. In Proceedings of the IEEE/RSJ International Conference on Intelligent Robots and Systems, Macau, China, 3–8 November 2019; IEEE: New York, NY, USA, 2019. [Google Scholar]
- Sharifi, M.; Salarieh, H.; Behzadipour, S.; Tavakoli, M. Stable Nonlinear Trilateral Impedance Control for Dual-User Haptic Teleoperation Systems With Communication Delays. J. Dyn. Syst. Meas. Control 2017, 139, 121012. [Google Scholar] [CrossRef]
- Hashemzadeh, F.; Sharifi, M.; Tavakoli, M. Nonlinear trilateral teleoperation stability analysis subjected to time-varying delays. Control Eng. Pract. 2016, 56, 123–135. [Google Scholar] [CrossRef]
- Saeidi, H.; Opfermann, J.D.; Kam, M.; Raghunathan, S.; Leonard, S.; Krieger, A. A Confidence-Based Shared Control Strategy for the Smart Tissue Autonomous Robot (STAR). In Proceedings of the 2018 IEEE/RSJ International Conference on Intelligent Robots and Systems (IROS), Madrid, Spain, 1–5 October 2018; IEEE: New York, NY, USA, 2018; pp. 1268–1275. [Google Scholar] [CrossRef]
- Liu, F.; Lelevé, A.; Eberard, D.; Redarce, T. A Dual-User Teleoperation System with Adaptive Authority Adjustment for Haptic Training. In New Trends in Medical and Service Robots; Springer International Publishing: Cham, Switzerland, 2016; pp. 165–177. [Google Scholar]
- Motaharifar, M.; Taghirad, H.D.; Hashtrudi-Zaad, K.; Mohammadi, S.F. Control of Dual-User Haptic Training System With Online Authority Adjustment: An Observer-Based Adaptive Robust Scheme. IEEE Trans. Control. Syst. Technol. 2019, 1–12. [Google Scholar] [CrossRef]
- Stephens, T.K.; Kong, N.J.; Dockter, R.L.; O’Neill, J.J.; Sweet, R.M.; Kowalewski, T.M. Blended shared control utilizing online identification. Int. J. Comput. Assist. Radiol. Surg. 2018, 13, 769–776. [Google Scholar] [CrossRef] [PubMed]
- Kucukyilmaz, A.; Demiris, Y. Learning Shared Control by Demonstration for Personalized Wheelchair Assistance. IEEE Trans. Haptics 2018, 11, 431–442. [Google Scholar] [CrossRef] [PubMed]
- Nakajima, Y.; Nozaki, T.; Ohnishi, K. Heartbeat synchronization with haptic feedback for telesurgical robot. IEEE Trans. Ind. Electron. 2014, 61, 3753–3764. [Google Scholar] [CrossRef]
- Razi, K.; Hashtrudi-Zaad, K. Analysis of Coupled Stability in Multilateral Dual-User Teleoperation Systems. IEEE Trans. Robot. 2014, 30, 631–641. [Google Scholar] [CrossRef]
- Motaharifar, M.; Taghirad, H.D.; Hashtrudi-Zaad, K.; Mohammadi, S.F. Control Synthesis and ISS Stability Analysis of a Dual-User Haptic Training System Based on S-Shaped Function. IEEE/ASME Trans. Mechatron. 2019, 24, 1553–1564. [Google Scholar] [CrossRef]
- Abi-Farraj, F.; Pacchierotti, C.; Arenz, O.; Neumann, G.; Giordano, P.R. A Haptic Shared-Control Architecture for Guided Multi-Target Robotic Grasping. IEEE Trans. Haptics 2020, 13, 270–285. [Google Scholar] [CrossRef]
- Zeestraten, M.J.A.; Havoutis, I.; Calinon, S. Programming by Demonstration for Shared Control With an Application in Teleoperation. IEEE Robot. Autom. Lett. 2018, 3, 1848–1855. [Google Scholar] [CrossRef]
- Trautman, P. Breaking the Human-Robot Deadlock: Surpassing Shared Control Performance Limits with Sparse Human-Robot Interaction. In Proceedings of the Robotics: Science and Systems XIII, Cambridge, MA, USA, 12–16 July 2017; pp. 1–10. [Google Scholar]
- Jain, S.; Argall, B. Recursive Bayesian Human Intent Recognition in Shared-Control Robotics. In Proceedings of the 2018 IEEE/RSJ International Conference on Intelligent Robots and Systems (IROS), Madrid, Spain, 1–5 October 2018; IEEE: New York, NY, USA, 2018; pp. 3905–3912. [Google Scholar] [CrossRef]
- Xu, Y.; Ding, C.; Shu, X.; Gui, K.; Bezsudnova, Y.; Sheng, X.; Zhang, D. Shared control of a robotic arm using non-invasive brain–computer interface and computer vision guidance. Robot. Auton. Syst. 2019, 115, 121–129. [Google Scholar] [CrossRef]
- Music, S.; Hirche, S. Control sharing in human-robot team interaction. Annu. Rev. Control 2017, 44, 342–354. [Google Scholar] [CrossRef]
- Matijevic, J.R.; Zimmerman, W.F.; Dolinsky, S. The NASA/OAST Telerobot Testbed Architecture. In Proceedings of the NASA Conference on Space Telerobotics; Rodriguez, G., Seraji, H., Eds.; NASA: Washington, DC, USA, 1989. [Google Scholar]
- Ma, Q.; Kobayashi, E.; Suenaga, H.; Hara, K.; Wang, J.; Nakagawa, K.; Sakuma, I.; Masamune, K. Autonomous Surgical Robot with Camera-Based Markerless Navigation for Oral and Maxillofacial Surgery. IEEE/ASME Trans. Mechatron. 2020, 25, 1084–1094. [Google Scholar] [CrossRef]
- Lu, B.; Chu, H.; Huang, K.; Cheng, L. Vision-Based Surgical Suture Looping Through Trajectory Planning for Wound Suturing. IEEE Trans. Autom. Sci. Eng. 2019, 16, 542–556. [Google Scholar] [CrossRef]
- Watanabe, K.; Kanno, T.; Ito, K.; Kawashima, K. Single-Master Dual-Slave Surgical Robot with Automated Relay of Suture Needle. IEEE Trans. Ind. Electron. 2018, 65, 6343–6351. [Google Scholar] [CrossRef]
- Parasuraman, R.; Sheridan, T.B.; Wickens, C.D. A model for types and levels of human interaction with automation. IEEE Trans. Syst. Man, Cybern. Part A Syst. Humans 2000, 30, 286–297. [Google Scholar] [CrossRef] [PubMed]
- Tao, R.; Ocampo, R.; Fong, J.; Soleymani, A.; Tavakoli, M. Modeling and Emulating a Physiotherapist’s Role in Robot-Assisted Rehabilitation. Adv. Intell. Syst. 2020, 2, 1900181. [Google Scholar] [CrossRef]
- Atashzar, S.F.; Shahbazi, M.; Tavakoli, M.; Patel, R.V. A computational-model-based study of supervised haptics-enabled therapist-in-the-loop training for upper-limb poststroke robotic rehabilitation. IEEE/ASME Trans. Mechatron. 2018, 23, 563–574. [Google Scholar] [CrossRef]
- Najafi, M.; Sharifi, M.; Adams, K.; Tavakoli, M. Robotic assistance for children with cerebral palsy based on learning from tele-cooperative demonstration. Int. J. Intell. Robot. Appl. 2017, 1, 43–54. [Google Scholar] [CrossRef]
- Maaref, M.; Rezazadeh, A.; Shamaei, K.; Ocampo, R.; Mahdi, T. A bicycle cranking model for assist-as-needed robotic rehabilitation therapy using learning from demonstration. IEEE Robot. Autom. Lett. 2016, 1, 653–660. [Google Scholar] [CrossRef]
- Sheridan, T. Human-Robot Interaction. Hum. Factors 2016, 58, 525–532. [Google Scholar] [CrossRef]
- Ferrell, W.R.; Sheridan, T.B. Supervisory control of remote manipulation. IEEE Spectr. 1967, 4, 81–88. [Google Scholar] [CrossRef]
- Lopes, Y.; Trenkwalder, S.; Leal, A.; Dodd, T.; Groß, R. Supervisory control theory applied to swarm robotics. Swarm Intell. 2016, 10, 65–97. [Google Scholar] [CrossRef]
- Ficuciello, F.; Tamburrini, G.; Arezzo, A.; Villani, L.; Siciliano, B. Autonomy in surgical robots and its meaningful human control. Paladyn, J. Behav. Robot. 2019, 10, 30–43. [Google Scholar] [CrossRef]
- Shademan, A.; Decker, R.S.; Opfermann, J.D.; Leonard, S.; Krieger, A.; Kim, P.C.W. Supervised autonomous robotic soft tissue surgery. Sci. Transl. Med. 2016, 8, 337ra64. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Jin, P.; Liu, W.; Tian, W. Basic Principle of Robot-Assisted Orthopedic Surgery. In Navigation Assisted Robotics in Spine and Trauma Surgery; Tian, W., Ed.; Springer: Singapore, 2020; pp. 5–10. [Google Scholar] [CrossRef]
- Attanasio, A.; Scaglioni, B.; De Momi, E.; Fiorini, P.; Valdastri, P. Autonomy in Surgical Robotics. Annu. Rev. Control. Robot. Auton. Syst. 2020, 4. [Google Scholar] [CrossRef]
- Haidegger, T. Autonomy for surgical robots: Concepts and paradigms. IEEE Trans. Med. Robot. Bionics 2019, 1, 65–76. [Google Scholar] [CrossRef]
- Connor, M.J.; Dasgupta, P.; Ahmed, H.U.; Raza, A. Autonomous surgery in the era of robotic urology: Friend or foe of the future surgeon? Nat. Rev. Urol. 2020, 17, 643–649. [Google Scholar] [CrossRef] [PubMed]
- Doulgeris, J.J.; Gonzalez-Blohm, S.A.; Filis, A.K.; Shea, T.M.; Aghayev, K.; Vrionis, F.D. Robotics in Neurosurgery: Evolution, Current Challenges, and Compromises. Cancer Control 2015, 22, 352–359. [Google Scholar] [CrossRef]
- Chauhan, M.; Deshpande, N.; Caldwell, D.; Mattos, L. Design and Modeling of a Three-Degree-of-Freedom Articulating Robotic Microsurgical Forceps for Trans-Oral Laser Microsurgery. J. Med. Devices Trans. ASME 2019, 13. [Google Scholar] [CrossRef]
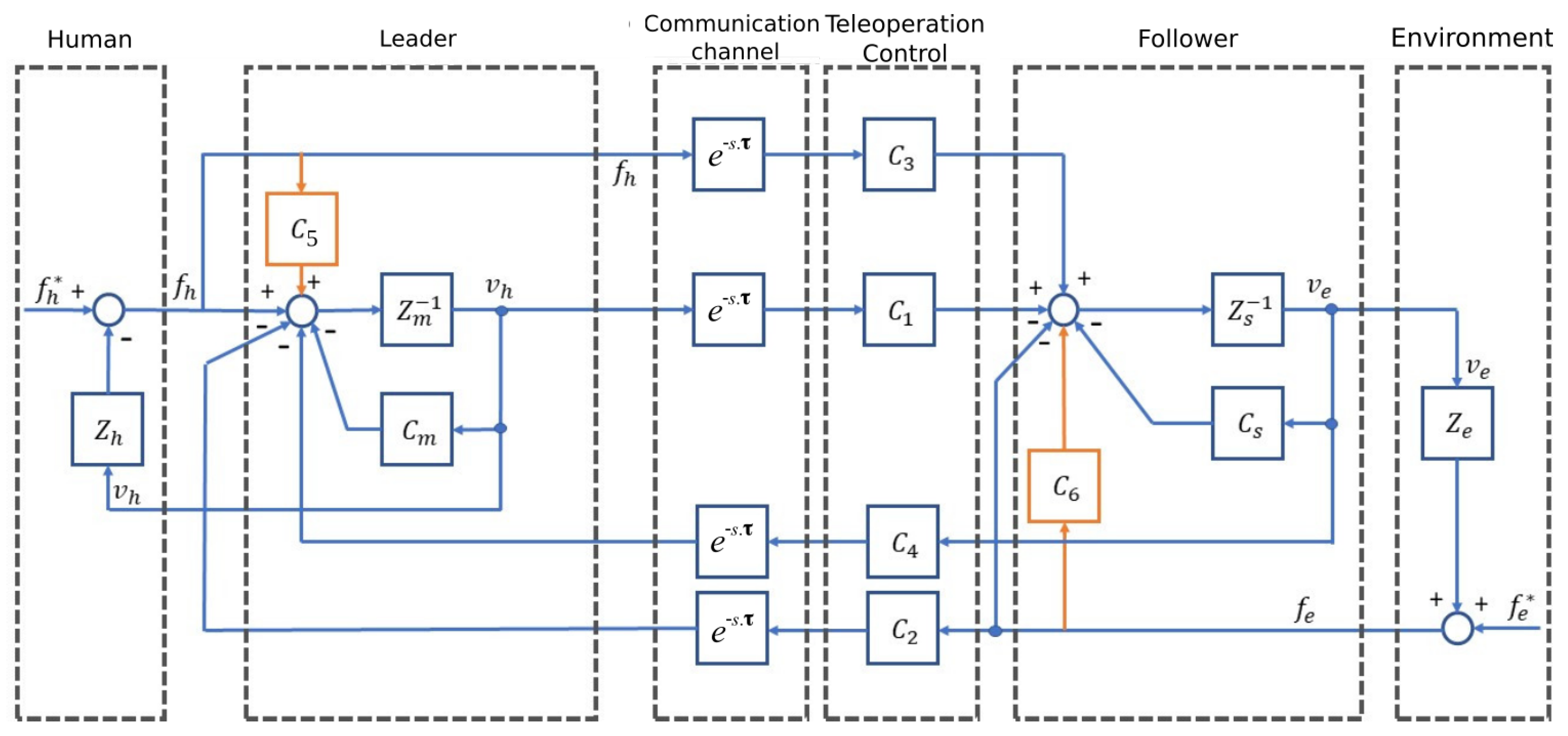
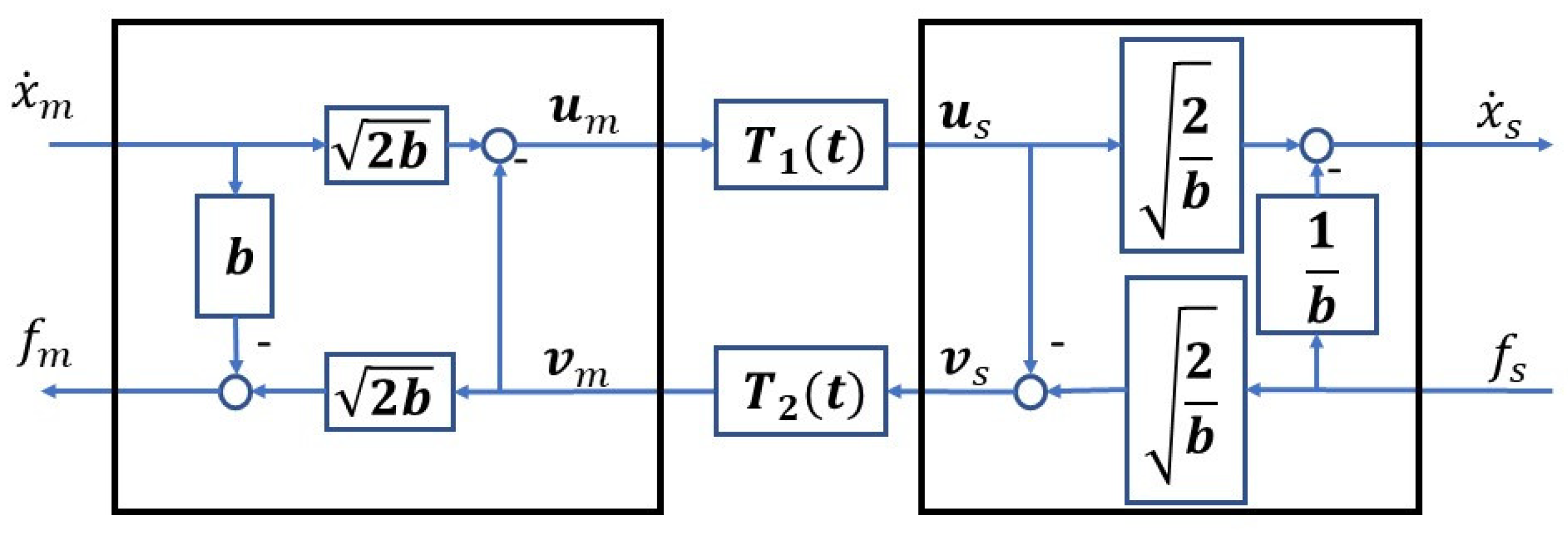
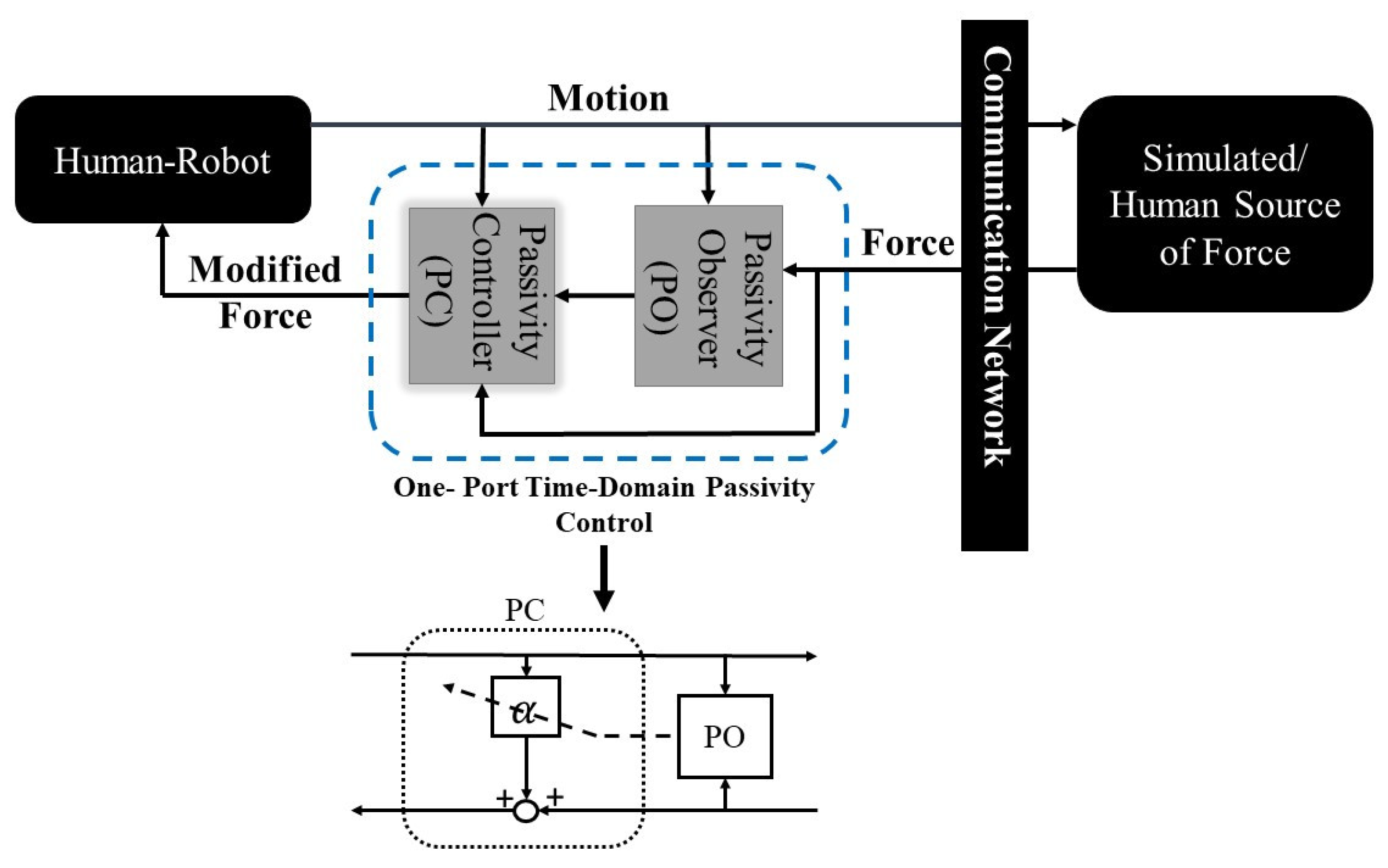
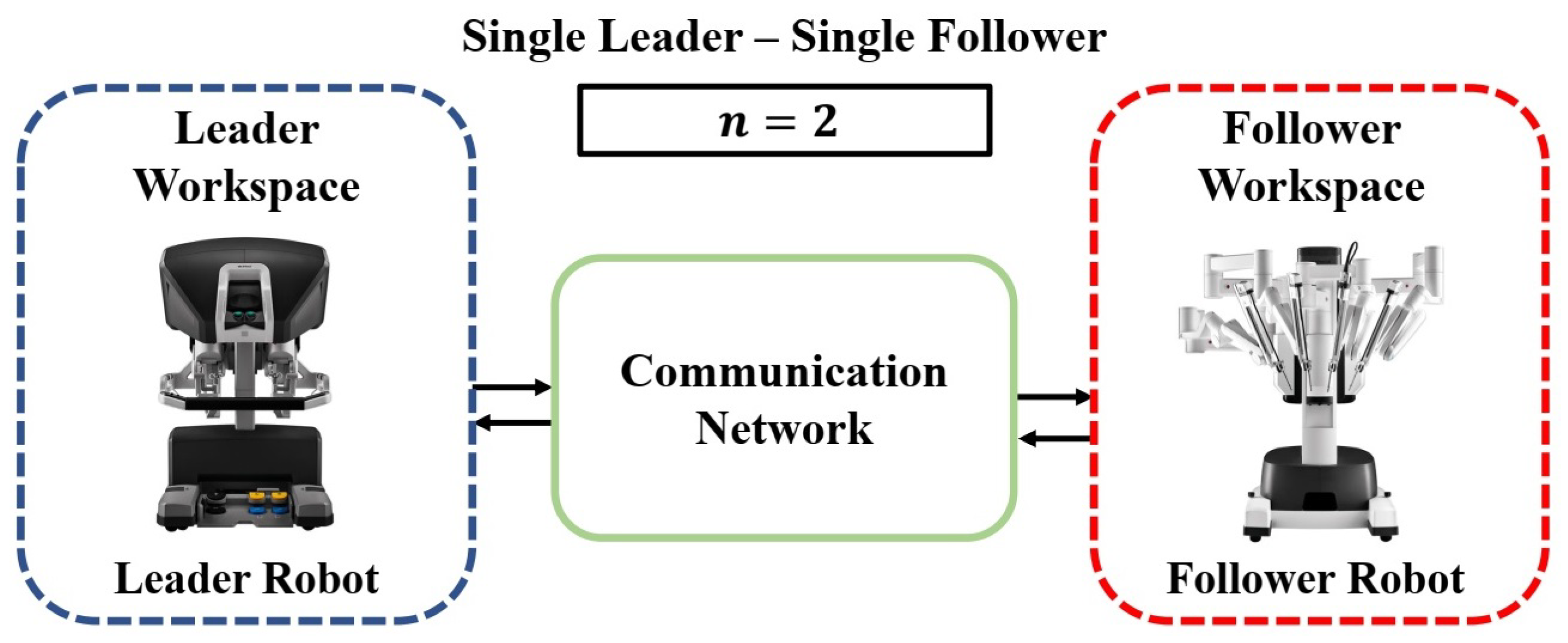

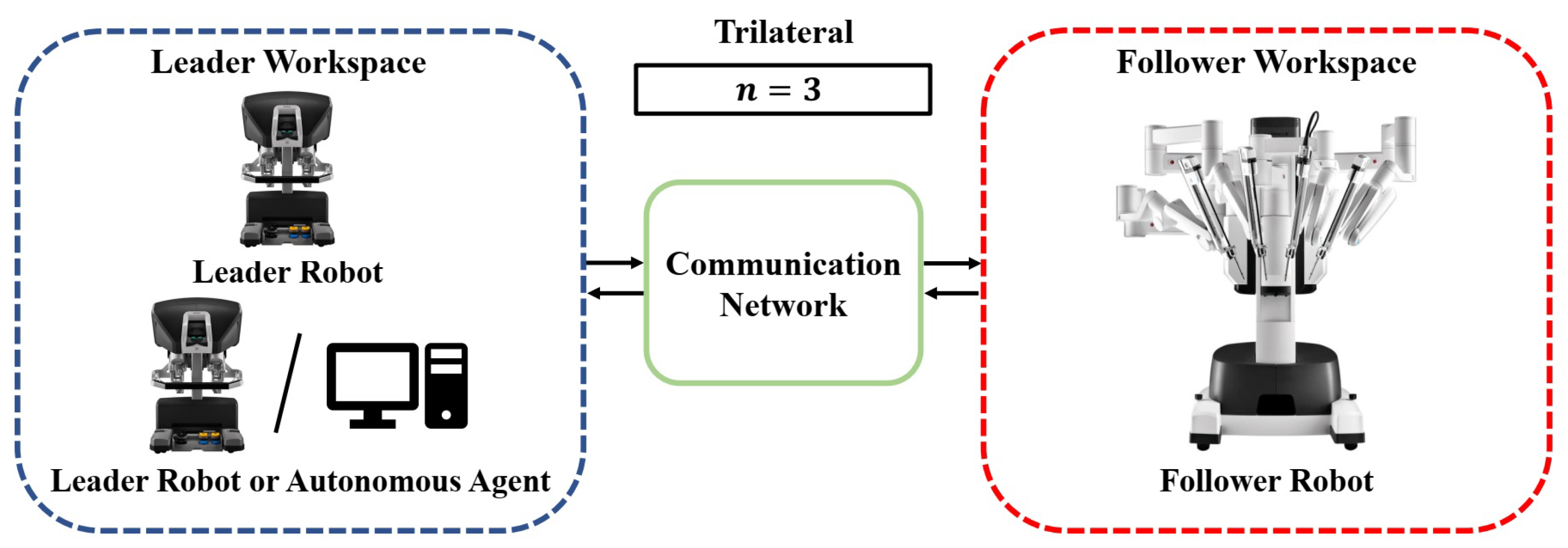
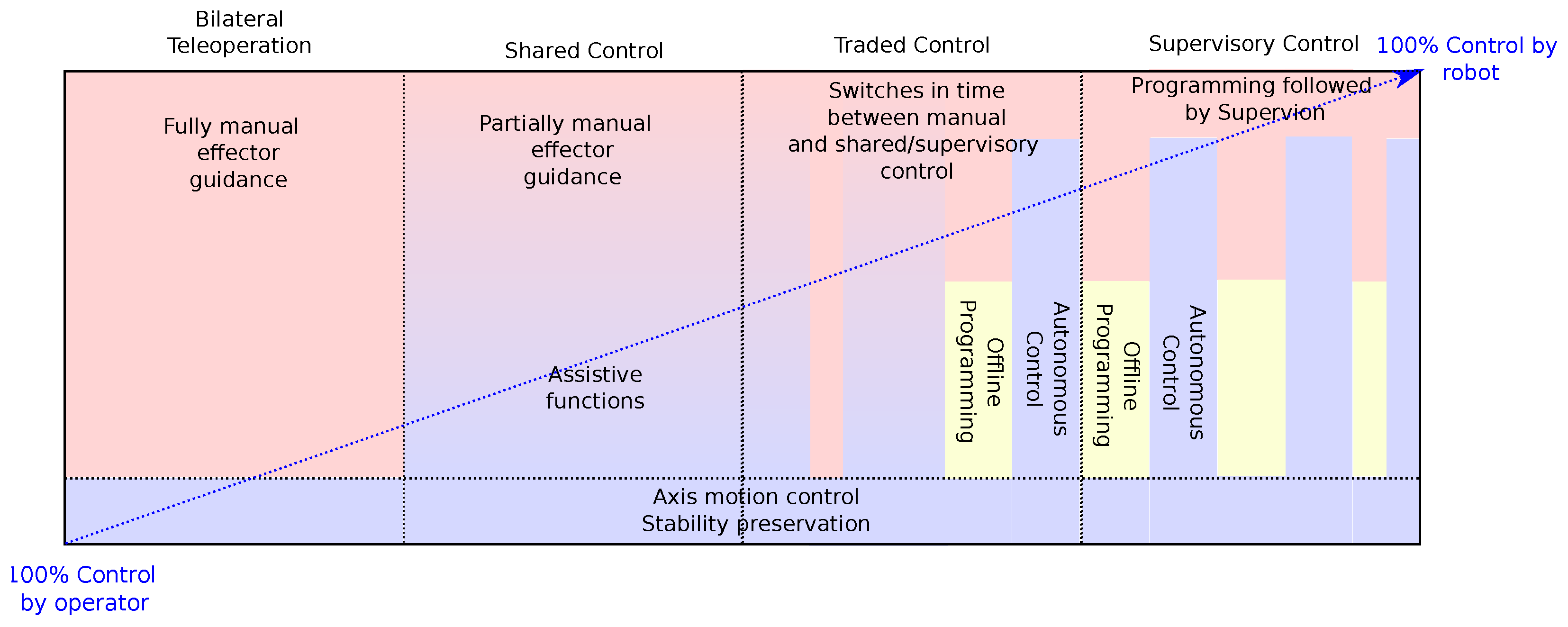
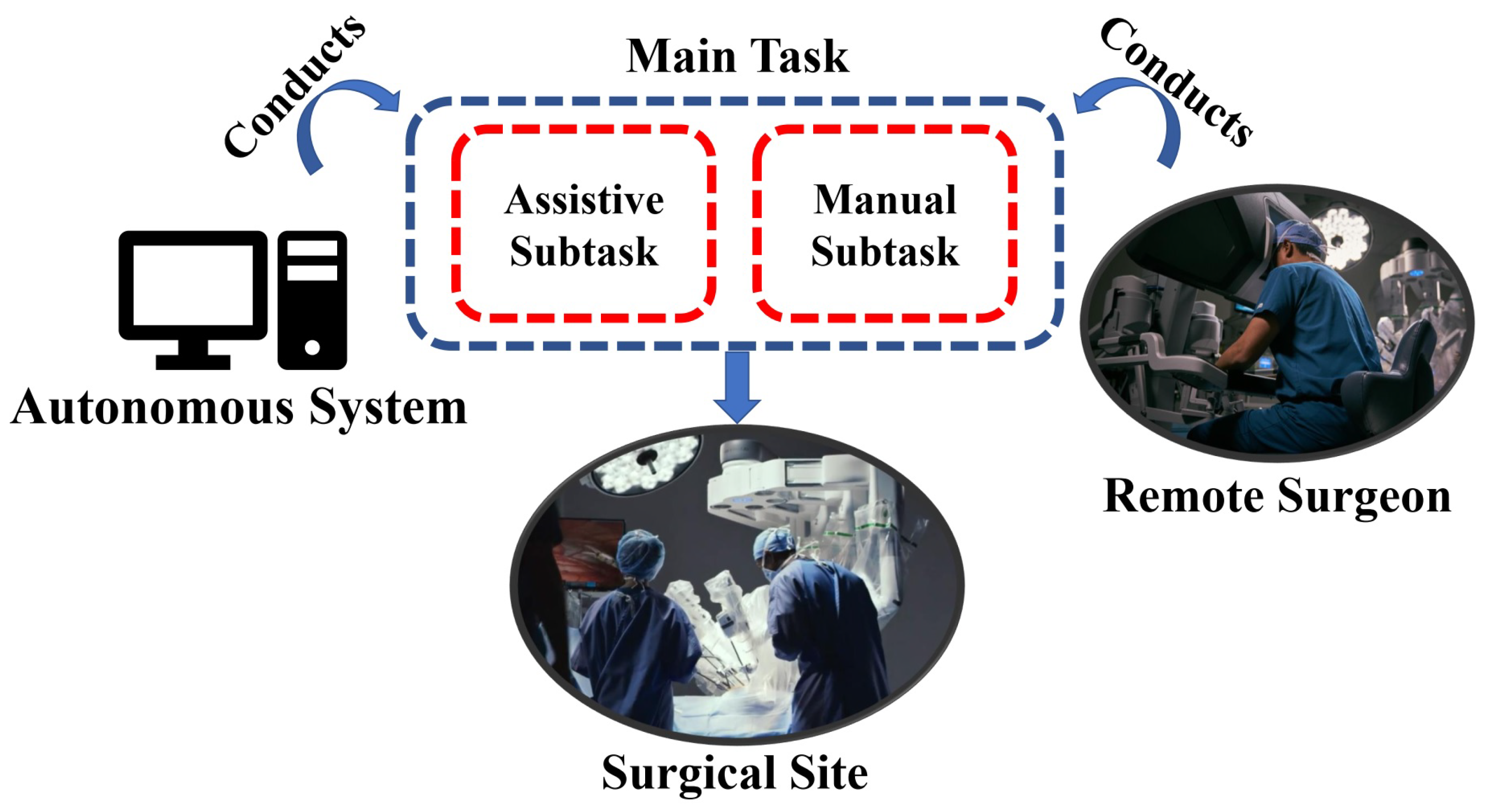
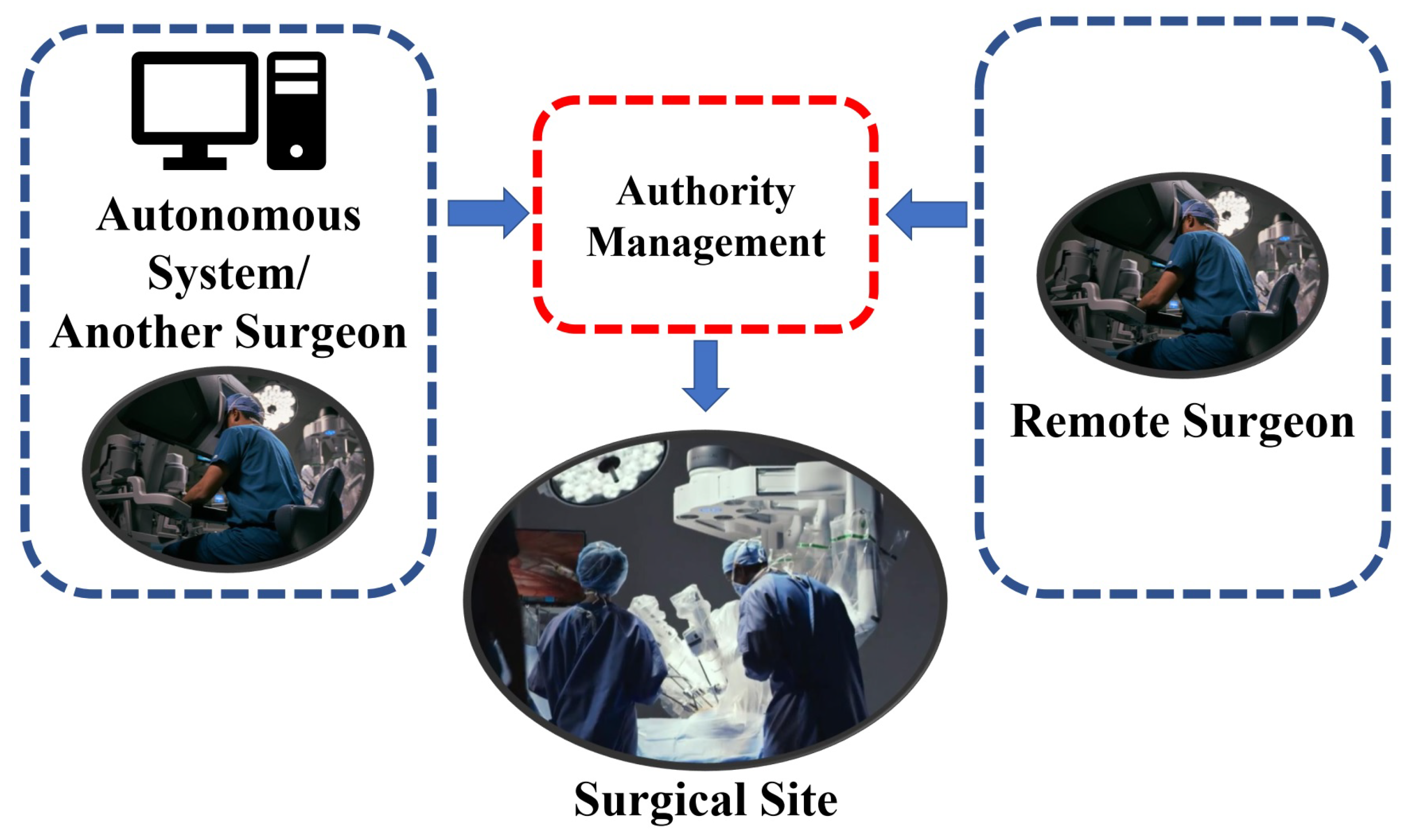
| Papers | Application | Task Level | Assistance | Haptic Feedback | Topology | Category | Solution |
|---|---|---|---|---|---|---|---|
| [313] | Surgical Manipulation (palpation) | High-level | Decision Making | ✓ | SL/SF | Task Decomposition | Dimension Reduction |
| [327] | Surgical Manipulation (dissection) | Low-level | Motion Control | ✗ | |||
| [326] | ✓ | Virtual Fixtures | |||||
| [328] | Surgical Manipulation (tracking) | ✗ | Motion Compensation | ||||
| [329,350] | Surgical Manipulation (tissue contact) | ✓ | |||||
| [16] | Tele-echography | ||||||
| [348] | Surgical Grasping | Authority Blending | Linear Blending | ||||
| [345] | Surgical Cutting | ||||||
| [325,340] | Assistive Rehabilitation | High-level | Decision Making | ✗ | |||
| [247] | Low-level | Motion Control | ✓ | Trilateral | Task Decomposition | Virtual Fixtures | |
| [349] | Authority Blending | Nonlinear Blending (virtual spring-damper) | |||||
| [206,208,268,269,308,343,344,347,351] | Surgical Training | Dual-user | Linear Blending | ||||
| [352] | Nonlinear Blending (cubic polynomials) | ||||||
| [218,324] | ML/SF | Linear Blending |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mehrdad, S.; Liu, F.; Pham, M.T.; Lelevé, A.; Atashzar, S.F. Review of Advanced Medical Telerobots. Appl. Sci. 2021, 11, 209. https://doi.org/10.3390/app11010209
Mehrdad S, Liu F, Pham MT, Lelevé A, Atashzar SF. Review of Advanced Medical Telerobots. Applied Sciences. 2021; 11(1):209. https://doi.org/10.3390/app11010209
Chicago/Turabian StyleMehrdad, Sarmad, Fei Liu, Minh Tu Pham, Arnaud Lelevé, and S. Farokh Atashzar. 2021. "Review of Advanced Medical Telerobots" Applied Sciences 11, no. 1: 209. https://doi.org/10.3390/app11010209
APA StyleMehrdad, S., Liu, F., Pham, M. T., Lelevé, A., & Atashzar, S. F. (2021). Review of Advanced Medical Telerobots. Applied Sciences, 11(1), 209. https://doi.org/10.3390/app11010209






