Changing Preference of One- Vs. Two-Stage Implant Placement in Partially Edentulous Individuals: An 18-Year Retrospective Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Subjects
2.2. Study Design
2.3. Methods
2.4. Statistical Analysis
3. Results
3.1. Implant Description and Distribution
3.1.1. One-Stage Surgery
3.1.2. Two-Stage Surgery
3.1.3. One- vs. Two-Stage Procedures
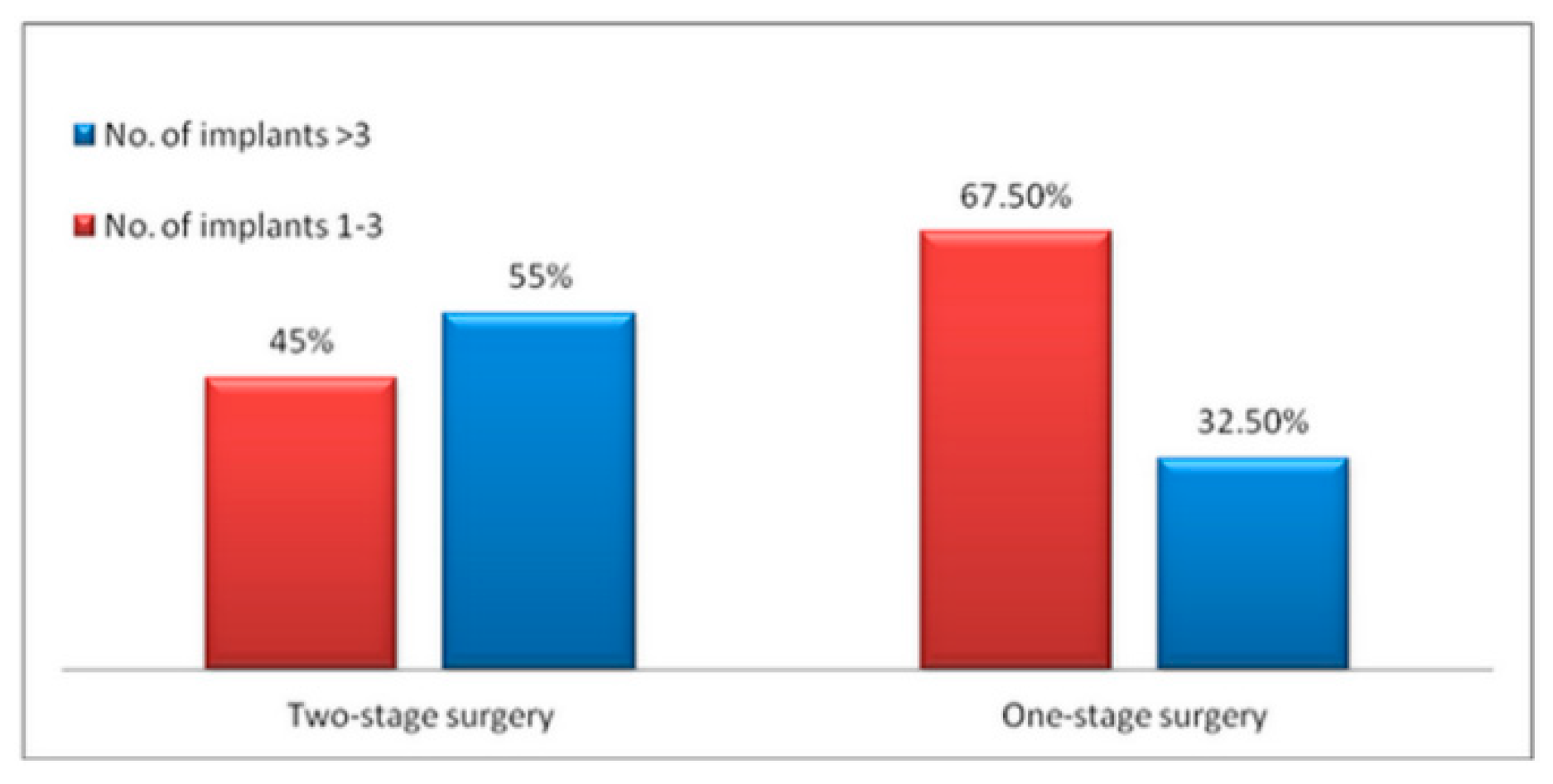
3.1.4. Selection of Surgical Approach
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Brånemark, P.I.; Hansson, B.O.; Adell, R.; Breine, U.; Lindström, J.; Hallén, O.; Ohmanet, A. Osseointegrated implants in the treatment of the edentulous jaw. Experience from a 10-year period. Scand. J. Plast. Reconstr. Surg. 1997, 16, 1–132. [Google Scholar]
- Esposito, M.; Grusovin, M.G.; Chew, Y.S.; Coulthard, P.; Worthington, H.V. Interventions for replacing missing teeth: 1- versus 2-stage implant placement. Cochrane Database Syst. Rev. 2009, 3, CD006698. [Google Scholar] [CrossRef] [PubMed]
- Albrektsson, T.; Brånemark, P.I.; Hansson, H.A.; Lindström, J. Osseointegrated titanium implants. Requirements for ensuring a long-lasting, direct bone-to-implant anchorage in man. Acta. Orthop. Scand. 1981, 52, 155–170. [Google Scholar] [CrossRef] [PubMed]
- Brunski, J.B.; Moccia, A.F.; Pollack, S.R.; Korostoff, E.; Trachtenberg, D.I. The influence of functional use of endosseous dental implants on the tissue-implant interface. I. Histological aspects. J. Dent. Res. 1979, 58, 1953–1969. [Google Scholar] [CrossRef]
- Buser, D.A.; Schroeder, A.; Sutter, F.; Lang, N.P. The new concept of ITI hollow-cylinder and hollow-screw implants: Part 2. Clinical aspects, indications, and early clinical results. Int. J. Oral Maxillofac. Implants 1988, 3, 173–181. [Google Scholar]
- Buser, D.; Weber, H.P.; Lang, N.P. Tissue integration of non-submerged implants. 1-year results of a prospective study with 100 ITI hollow-cylinder and hollow-screw implants. Clin. Oral Implants Res. 1990, 1, 33–40. [Google Scholar] [CrossRef]
- Buser, D.; Mericske-Stern, R.; Bernard, J.P.; Behneke, A.; Behneke, N.; Hirt, H.P.; Belser, U.C.; Lang, N.P. Long-term evaluation of non-submerged ITI implants. Part 1: 8-year life table analysis of a prospective multi-center study with 2359 implants. Clin. Oral Implants Res. 1997, 8, 161–172. [Google Scholar] [CrossRef]
- Ericsson, I.; Randow, K.; Nilner, K.; Petersson, A. Some clinical and radiographical features of submerged and non-submerged titanium implants. A 5-year follow-up study. Clin. Oral Implants Res. 1997, 8, 422–426. [Google Scholar] [CrossRef]
- Barber, H.D.; Seckinger, R.J.; Silverstein, K.; Abughazaleh, K. Comparison of soft tissue healing and osseointegration of IMZ implants placed in one-stage and two-stage techniques: A pilot study. Implant Dent. 1996, 5, 11–14. [Google Scholar] [CrossRef]
- Collaert, B.; De Bruyn, H. Comparison of Brånemark fixture integration and short-term survival using one-stage or two-stage surgery in completely and partially edentulous mandibles. Clin. Oral Implants Res. 1998, 9, 131–135. [Google Scholar] [CrossRef]
- Heydenrijk, K.; Raghoebar, G.M.; Meijer, H.J.A.; Van Der Reijden, W.A.; Van Winkelhoff, A.J.; Stegenga, B. Two-part implants inserted in a one-stage or a two-stage procedure. A prospective comparative study. J. Clin. Periodontol. 2002, 29, 901–909. [Google Scholar] [CrossRef] [PubMed]
- Cecchinato, D.; Olsson, C.; Lindhe, J. Submerged or non-submerged healing of endosseous implants to be used in the rehabilitation of partially dentate patients. A multicenter, randomized controlled clinical trial. J. Clin. Periodontol. 2004, 31, 299–308. [Google Scholar] [CrossRef]
- Becktor, J.P.; Isaksson, S.; Billström, C. A prospective multicenter study using two different surgical approaches in the mandible with turned brånemark implants: Conventional loading using fixed prostheses. Clin. Implant Dent. Relat. Res. 2007, 9, 179–185. [Google Scholar] [CrossRef] [PubMed]
- Cordaro, L.; Torsello, F.; Roccuzzo, M. Clinical outcome of submerged vs. non-submerged implants placed in fresh extraction sockets. Clin. Oral Implants Res. 2009, 20, 1307–1313. [Google Scholar] [CrossRef] [PubMed]
- Löe, H. The gingival index, the plaque index and the retention index systems. J. Periodontol. 1967, 38, 610–616. [Google Scholar] [CrossRef]
- Turkyilmaz, I.; Sennerby, L.; Tumer, C.; Yenigul, M.; Avci, M. Stability and marginal bone level measurements of unsplinted implants used for mandibular overdentures: A 1-year randomized prospective clinical study comparing early and conventional loading protocols. Clin. Oral Implants Res. 2006, 17, 501–505. [Google Scholar] [CrossRef]
- De Smet, E.; Jacobs, R.; Gijbels, F.; Naert, I. The accuracy and reliability of radiographic methods for the assessment of marginal bone level around oral implants. Dentomaxillofac. Radiol. 2002, 31, 176–181. [Google Scholar] [CrossRef]
- Batenburg, R.H.; Meijer, H.J.; Geraets, W.G.; van der Stelt, P.F. Radiographic assessment of changes in marginal bone around endosseous implants supporting mandibular overdentures. Dentomaxillofac. Radiol. 1998, 27, 221–224. [Google Scholar] [CrossRef]
- Batenburg, R.H.; Meijer, H.J.; Raghoebar, G.M.; Van Oort, R.P.; Boering, G. Mandibular overdentures supported by two Brånemark, IMZ or ITI implants. A prospective comparative preliminary study: One-year results. Clin. Oral Implants Res. 1998, 9, 374–383. [Google Scholar] [CrossRef]
- Cox, J.F.; Zarb, G.A. The longitudinal clinical efficacy of osseointegrated dental implants: A 3-year report. Int. J. Oral Maxillofac. Implants 1987, 2, 91–100. [Google Scholar]
- Ericsson, I.; Randow, K.; Glantz, P.O.; Lindhe, J.; Nilner, K. Clinical and radiographical features of submerged and nonsubmerged titanium implants. Clin. Oral Implants Res. 1994, 5, 185–189. [Google Scholar] [CrossRef] [PubMed]
- Bernard, J.P.; Belser, U.C.; Martinet, J.P.; Borgis, S.A. Osseointegration of Brånemark fixtures using a single-step operating technique. A preliminary prospective one-year study in the edentulous mandible. Clin. Oral Implants Res. 1995, 6, 122–129. [Google Scholar] [CrossRef] [PubMed]

| Surgical Technique | Patients, n | Age, y | Gender | Implant | Current Smokers (%) | |||
|---|---|---|---|---|---|---|---|---|
| Total | 111 | Male (%) | Female (%) | No. | Diameter (mm) | Length (mm) | ||
| One-stage | 52 * | 54 ± 14 | 44 | 56 | 140 | 4.3 ± 0.5 | 12 ± 1.4 | 15 |
| Two-stage | 74 * | 55 ± 13 | 42 | 58 | 253 | 4.05 ± 0.4 | 12.4 ± 1.6 | 23 |
| p | NS | NS | NS | NS | NS | NS | ||
| Surgical Technique | Mesial Marginal Bone Loss | p | Distal Marginal Bone Loss | p | Gingival Index at Last Follow-Up | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| Follow-Up ≤36 Months | Follow-Up >36 Months | Follow-Up ≤36 Months | Follow-Up >36 Months | 0 | 1 | 2 | 3 | |||
| One-stage | 1.1 ± 0.7 | 1.2 ± 1.4 | NS | 1 ± 0.8 | 1.3 ± 1.5 | NS | 71% | 28% | 0 | 0 |
| Two-stage | 0.9 ± 0.7 | 1 ± 1 | NS | 0.9 ± 0.7 | 1.1 ± 1.1 | NS | 70% | 30% | 0 | 0 |
| p | NS | NS | NS | NS | NS | |||||
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chaushu, L.; Naishlos, S.; Rosner, O.; Zenziper, E.; Glikman, A.; Lavi, D.; Kupershmidt, I.; Zelikman, H.; Chaushu, G.; Nissan, J. Changing Preference of One- Vs. Two-Stage Implant Placement in Partially Edentulous Individuals: An 18-Year Retrospective Study. Appl. Sci. 2020, 10, 7060. https://doi.org/10.3390/app10207060
Chaushu L, Naishlos S, Rosner O, Zenziper E, Glikman A, Lavi D, Kupershmidt I, Zelikman H, Chaushu G, Nissan J. Changing Preference of One- Vs. Two-Stage Implant Placement in Partially Edentulous Individuals: An 18-Year Retrospective Study. Applied Sciences. 2020; 10(20):7060. https://doi.org/10.3390/app10207060
Chicago/Turabian StyleChaushu, Liat, Sarit Naishlos, Ofir Rosner, Eran Zenziper, Ari Glikman, David Lavi, Irit Kupershmidt, Helena Zelikman, Gavriel Chaushu, and Joseph Nissan. 2020. "Changing Preference of One- Vs. Two-Stage Implant Placement in Partially Edentulous Individuals: An 18-Year Retrospective Study" Applied Sciences 10, no. 20: 7060. https://doi.org/10.3390/app10207060
APA StyleChaushu, L., Naishlos, S., Rosner, O., Zenziper, E., Glikman, A., Lavi, D., Kupershmidt, I., Zelikman, H., Chaushu, G., & Nissan, J. (2020). Changing Preference of One- Vs. Two-Stage Implant Placement in Partially Edentulous Individuals: An 18-Year Retrospective Study. Applied Sciences, 10(20), 7060. https://doi.org/10.3390/app10207060







