Current Status of Animal-Assisted Interventions in Scientific Literature: A Critical Comment on Their Internal Validity
Simple Summary
Abstract
1. Introduction
2. Objectives
3. Analyzing Key Points That Affect the Internal Validity of AAIs
3.1. Classical Terms and Definitions of AAIs
3.2. Empirical Definition of AAI Studies
3.3. The Role of Animals within the Intervention Strategy
3.4. Mechanisms for Explaining Changes
3.5. Do Animal-Assisted Interventions Exist?
4. Proposals for Integrating AAIs
4.1. Improving the Definition, Classification, and Terms Used
“Animal-assisted interventions offer a generic label to bring together any programmed intervention (designed and evaluated) that takes advantage of the benefits of human–animal interaction as an enhancing or facilitating element. AAIs do not in themselves constitute a profession or discipline, but rather they are identified by including animals as support for any pre-existing professional role, such as performing psychotherapy, physiotherapy, education or even sociocultural animation; therefore, the professionals involved must comply with the legal and qualification requirements needed to perform these tasks. In all cases, the design of the intervention will assess the relevance, efficiency and ethical implications of including animals within the given anthrozoological and sociocultural context. The training and certification of the animals will depend on the tasks they are entrusted with, but they will always act under the supervision of qualified personnel to guarantee their well-being and the safety of all participants.”
4.2. Attending to Mechanisms of Change: How the HAI Can Improve Intervention Programs
4.3. Understanding AAIs from a Cultural Point of View
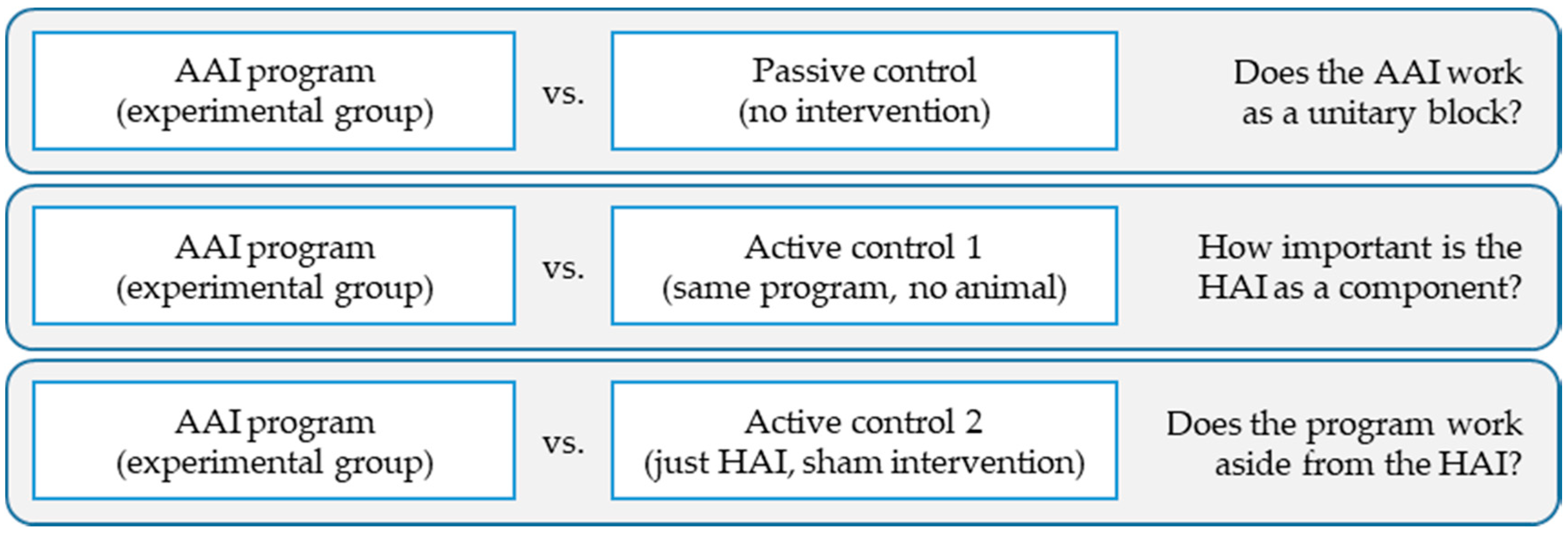
4.4. Improving Research on the Efficacy and Efficiency of AAIs
5. Conclusions
Funding
Acknowledgments
Conflicts of Interest
References
- Thew, K.; Marco, L.; Erdman, P.; Caro, B.I. Assessing Attitudes Towards Animal Assisted Therapy among Students and Faculty in American Psychological Association Accredited Programs. Human-Animal Interact. Bull. 2015, 3, 11–27. [Google Scholar]
- Black, A.F.; Chur-Hansen, A.; Winefield, H.R. Australian psychologists’ knowledge of and attitudes towards animal-assisted therapy. Clin. Psychol. 2011, 15, 69–77. [Google Scholar] [CrossRef]
- López-Cepero Borrego, J.; Perea-Mediavilla, M.A.; Tejada Roldán, A.; Sarasola-Sánchez-Serrano, J.L. Validación del Cuestionario de Actitudes ante las Intervenciones Asistidas por Perros (CAINTAP) en Estudiantes Universitarios del Sur de España: Beneficios y Temores Percibidos. Altern. Cuad. Trab. Soc. 2015, 22, 123–138. [Google Scholar] [CrossRef]
- Perea-Mediavilla, M.A.; López-Cepero, J.; Tejada-Roldán, A.; Sarasola, J.L. Intervenciones asistidas por animales y calidad de vida: Expectativas en estudiantes universitarios españoles. Escritos Psicol. 2014. [Google Scholar] [CrossRef]
- Berget, B.; Grepperud, S. Animal-Assisted Interventions for psychiatric patients: Beliefs in treatment effects among practitioners. Eur. J. Integr. Med. 2011, 3, 91–96. [Google Scholar] [CrossRef]
- Berget, B.; Grepperud, S.; Aasland, O.G.; Braastad, B.O. Animal-assisted interventions and psychiatric disorders: Knowledge and attitudes among general practitioners, psychiatrists, and psychologists. Soc. Anim. 2013, 21, 284–293. [Google Scholar] [CrossRef]
- Herzog, H. The impact of pets on human health and psychological well-being: Fact, fiction, or hypothesis? Curr. Dir. Psychol. Sci. 2011, 20, 236–239. [Google Scholar] [CrossRef]
- Herzog, H. Some We Love, Some We Hate, Some We Ate; Harper Collins: New York, NY, USA, 2011. [Google Scholar]
- Halm, M.A. The healing power of the human-animal connection. Am. J. Crit Care. 2008, 17, 373–376. [Google Scholar] [CrossRef]
- Marino, L. Construct Validity of Animal-Assisted Therapy and Activities: How Important Is the Animal in AAT? Anthrozoos 2012, 25, s139–s151. [Google Scholar] [CrossRef]
- Nimer, J.; Lundahl, B. Animal-Assisted Therapy: A Meta-Analysis. Anthrozoos 2007, 20, 225–238. [Google Scholar] [CrossRef]
- Souter, M.A.; Miller, M.D. Do animal-assisted activities effectively treat depression? a meta-analysis. Anthrozoos 2007, 20, 167–180. [Google Scholar] [CrossRef]
- Hu, M.; Zhang, P.; Leng, M.; Li, C.; Chen, L. Animal-assisted intervention for individuals with cognitive impairment: A meta-analysis of randomized controlled trials and quasi-randomized controlled trials. Psychiatry Res. 2018, 260, 418–427. [Google Scholar] [CrossRef] [PubMed]
- Zafra-Tanaka, J.H.; Pacheco-Barrios, K.; Tellez, W.A.; Taype-Rondan, A. Effects of dog-assisted therapy in adults with dementia: A systematic review and meta-analysis. BMC Psychiatry 2019, 19, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Charry-Sánchez, J.D.; Pradilla, I.; Talero-Gutiérrez, C. Effectiveness of Animal-Assisted Therapy in the Pediatric Population: Systematic Review and Meta-Analysis of Controlled Studies. J. Dev. Behav Pediatr. 2018, 39, 580–590. [Google Scholar] [CrossRef] [PubMed]
- Higgins, J.P.T.; Altman, D.G.; Gøtzsche, P.C.; Jüni, P.; Moher, D.; Oxman, A.D.; Savovic, J.; Schulz, K.F.; Weeks, L.; Sterne, J.C.C.; et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 2011, 343, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Slim, K.; Nini, E.; Forestier, D.; Kwiatkowski, F.; Panis, Y.; Chipponi, J. Methodological index for non-randomized studies (Minors): Development and validation of a new instrument. ANZ J. Surg. 2003, 73, 712–716. [Google Scholar] [CrossRef]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gøtzsche, P.C.; Ioannidis, J.P.A.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: Explanation and elaboration. BMJ 2009, 339. [Google Scholar] [CrossRef]
- Cooke, B.J.; Farrington, D.P. The Effectiveness of Dog-Training Programs in Prison: A Systematic Review and Meta-Analysis of the Literature. Prison J. 2016, 96, 854–876. [Google Scholar] [CrossRef]
- Virués-Ortega, J.; Pastor-Barriuso, R.; Castellote, J.M.; Población, A.; de Pedro-Cuesta, J. Effect of animal-assisted therapy on the psychological and functional status of elderly populations and patients with psychiatric disorders: A meta-analysis. Health Psychol. Rev. 2012, 6, 197–221. [Google Scholar] [CrossRef]
- López-Cepero, J. Animales de Compañía y Salud: Del Vínculo Humano-Animal Al Diseño de Intervenciones Asistidas Por Animales [Companion Animals and Health: From Human-Animal Bond to Designing Animal-Assisted Interventions]; Pirámide: Madrid, Spain, 2019. (In Spanish) [Google Scholar]
- Menna, L.F.; Santaniello, A.; Todisco, M.; Amato, A.; Borrelli, L.; Scandurra, C.; Fioretti, A. The human-animal relationship as the focus of animal-assisted interventions: A one health approach. Int. J. Environ. Res. Public Health 2019, 16, 3660. [Google Scholar] [CrossRef]
- Hediger, K.; Meisser, A.; Zinsstag, J. A One Health Research Framework for Animal-Assisted Interventions. Int. J. Environ. Res. Public Health 2019, 16, 640. [Google Scholar] [CrossRef]
- Pichot, T.; Coulter, M. Animal-Assisted Brief Therapy: A Solution-Focused Approach; Routledge: New York, NY, USA, 2006. [Google Scholar]
- Kruger, K.A.; Serpell, J.A. Animal-Assisted Interventions in Mental Health: Definitions and Theoretical Foundations. In Handbook on Animal-Assisted Therapy, 3rd ed.; Fine, A., Ed.; Elsevier Inc.: San Diego, CA, USA, 2010; pp. 33–48. [Google Scholar] [CrossRef]
- Lopez-Cepero, J.; Franco, L.R.; Mediavilla, M.A.P.; Piñero, N.B.; Roldán, A.T.; Picabia, A.B. Animal-assisted interventions: Review of current status and future challenges. Int. J. Psychol. Psychol. Ther. 2014, 14, 85–101. [Google Scholar]
- Delta Society. Standards of Practice; Delta Society: Bellevue, WA, USA, 1996. [Google Scholar]
- Gammonley, J.; Howie, A.R.; Kirwin, S.; Zapf, S.A.; Frye, J.; Freeman, G.; Stuart-Russell, R. Therapeutic Interventions; Delta Society: Bellevue, WA, USA, 1997. [Google Scholar]
- Jegatheesan, B.; Beetz, A.; Ormerod, E.; Johnson, R.; Fine, A.; Yamazaki, K.; Dudzik, C.; Garcia, R.M.; Winkle, M.; Choi, G. IAHAIO White Paper: The IAHAIO Definitions for Animal Assisted Intervention and Guidelines for Wellness of Animals Involved; International Association of Human-Animal Interaction Organizations: Seattle, WA, USA, 2014; pp. 1–10. [Google Scholar]
- Filan, S.L.; Llewellyn-Jones, R.H. Animal-assisted therapy for dementia: A review of the literature. Int. Psychogeriatr. 2006, 18, 597–611. [Google Scholar] [CrossRef] [PubMed]
- Hooker, S.D.; Freeman, L.H.; Stewart, P. Pet Therapy Research: A Historical Review. Holist. Nurs. Pract. 2002, 17, 17–23. [Google Scholar] [CrossRef] [PubMed]
- Greco, T.; Zangrillo, A.; Biondi-Zoccai, G.; Landoni, G. Meta-analysis: Pitfalls and hints. Hear. Lung Vessel. 2013, 5, 219–225. [Google Scholar] [CrossRef]
- Biondi-Zoccai, G.; Lotrionte, M.; Landoni, G.; Modena, M.G. The rough guide to systematic reviews and meta-analyses. HSR Proc. Intensive Care Cardiovasc. Anesth. 2011, 3, 161–173. [Google Scholar] [PubMed]
- Glenk, L.M. Current perspectives on therapy dog welfare in animal-assisted interventions. Animals 2017, 7, 7. [Google Scholar] [CrossRef] [PubMed]
- Gut, W.; Crump, L.; Zinsstag, J.; Hattendorf, J.; Hediger, K. The effect of human interaction on guinea pig behavior in animal-assisted therapy. J. Vet. Behav. 2018, 25, 56–64. [Google Scholar] [CrossRef]
- Wilkie, K.D.; Germain, S.; Theule, J. Evaluating the Efficacy of Equine Therapy Among At-risk Youth: A Meta-analysis. Anthrozoos 2016, 29, 377–393. [Google Scholar] [CrossRef]
- Maujean, A.; Pepping, C.A.; Kendall, E. A systematic review of randomized controlled trials of animal-assisted therapy on psychosocial outcomes. Anthrozoos 2015, 28, 23–36. [Google Scholar] [CrossRef]
- McNicholas, J.; Gilbey, A.; Rennie, A.; Ahmedzai, S.; Dono, J.A.; Ormerod, E. Pet ownership and human health: A brief review of evidence and issues. Br. Med. J. 2005, 331, 1252–1254. [Google Scholar] [CrossRef] [PubMed]
- Wesley, M.C.; Minatrea, N.B.; Watson, J.C. Animal-assisted therapy in the treatment of substance dependence. Anthrozoos 2009, 22, 137–148. [Google Scholar] [CrossRef]
- Kazdin, A.E. Methodological Standards and Strategies for Establishing the Evidence Base of Animal-Assisted Therapies, 4th ed.; Elsevier Inc.: Bellevue, CA, USA, 2015. [Google Scholar] [CrossRef]
- Wampold, B.E. How Important Are the Common Factors in Psychotherapy? An Update. World Psychiatry 2015, 14, 270–277. [Google Scholar] [CrossRef]
- Chandler, C.K. Animal-Assisted Therapy in Counseling, 3rd ed.; Routledge: New York, NY, USA, 2017. [Google Scholar]
- Jenkins, C.D.; Laux, J.M.; Ritchie, M.H.; Tucker-Gail, K. Animal-Assisted Therapy and Rogers’ Core Components Among Middle School Students Receiving Counseling Services: A Descriptive Study. J. Creat. Ment. Heal. 2014, 9, 174–187. [Google Scholar] [CrossRef]
- Bryan, J.L.; Quist, M.C.; Young, C.M.; Steers, M.L.N.; Foster, D.W.; Lu, Q. Canine comfort: Pet affinity buffers the negative impact of ambivalence over emotional expression on perceived social support. Pers. Individ. Dif. 2014, 68, 23–27. [Google Scholar] [CrossRef] [PubMed]
- Schneider, M.S.; Harley, L.P. How dogs influence the evaluation of psychotherapists. Anthrozoos 2006, 19, 128–142. [Google Scholar] [CrossRef]
- Virués-Ortega, J.; Buela-Casal, G. Psychophysiological effects of human-animal interaction theoretical issues and long-term interaction effects. J. Nerv. Ment. Dis. 2006, 194, 52–57. [Google Scholar] [CrossRef]
- Bradshaw, J. The Animals among Us: The New Science of Anthrozoology; Penguin Books: London, UK, 2017. [Google Scholar]
© 2020 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
López-Cepero, J. Current Status of Animal-Assisted Interventions in Scientific Literature: A Critical Comment on Their Internal Validity. Animals 2020, 10, 985. https://doi.org/10.3390/ani10060985
López-Cepero J. Current Status of Animal-Assisted Interventions in Scientific Literature: A Critical Comment on Their Internal Validity. Animals. 2020; 10(6):985. https://doi.org/10.3390/ani10060985
Chicago/Turabian StyleLópez-Cepero, Javier. 2020. "Current Status of Animal-Assisted Interventions in Scientific Literature: A Critical Comment on Their Internal Validity" Animals 10, no. 6: 985. https://doi.org/10.3390/ani10060985
APA StyleLópez-Cepero, J. (2020). Current Status of Animal-Assisted Interventions in Scientific Literature: A Critical Comment on Their Internal Validity. Animals, 10(6), 985. https://doi.org/10.3390/ani10060985




