Malaria: The Past and the Present
Abstract
1. Introduction
2. Discovery of Malaria
3. The Development of Diagnostic Tests for Proving Malaria through History
4. Malaria Treatment through History
4.1. Malaria in Europe
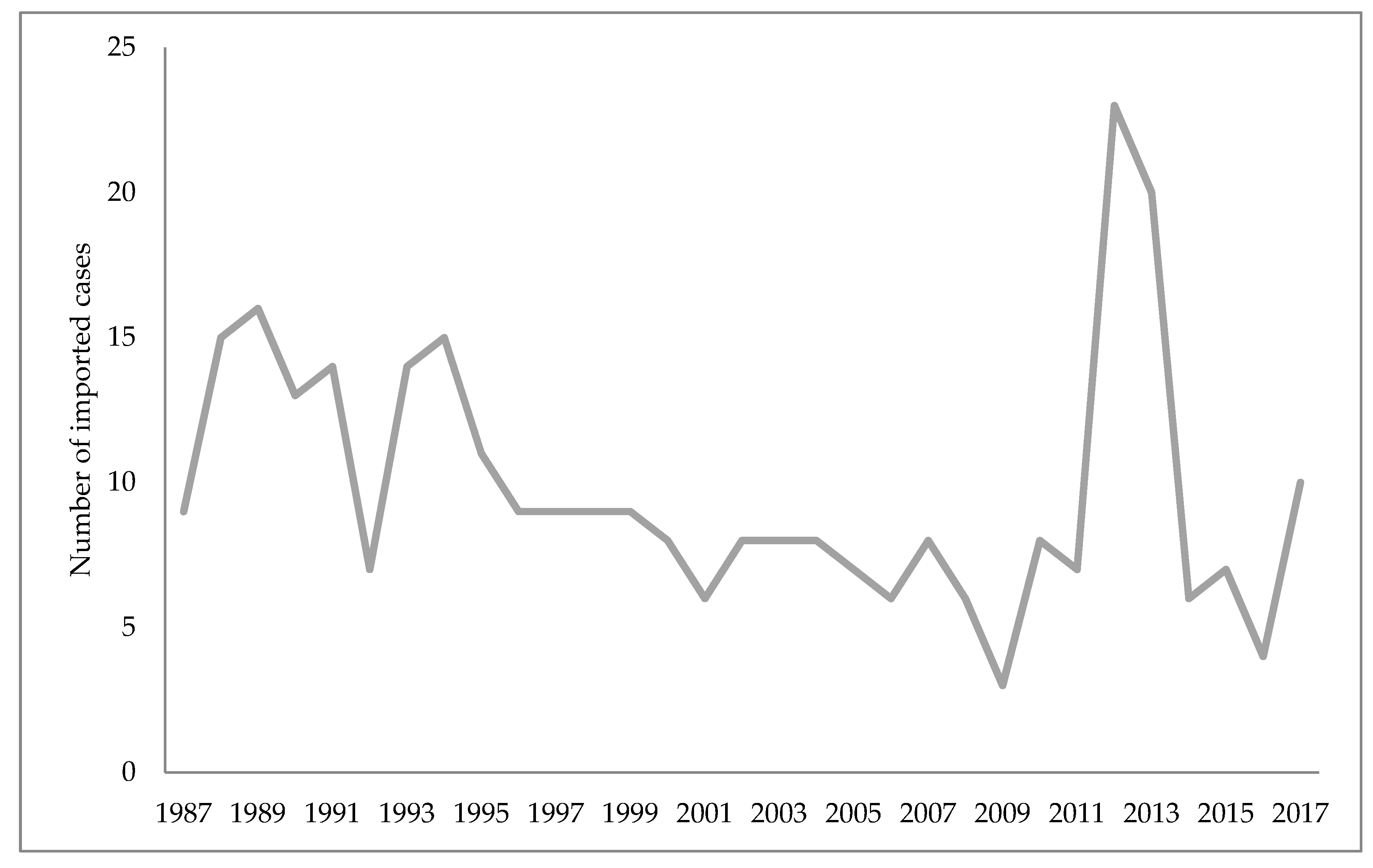
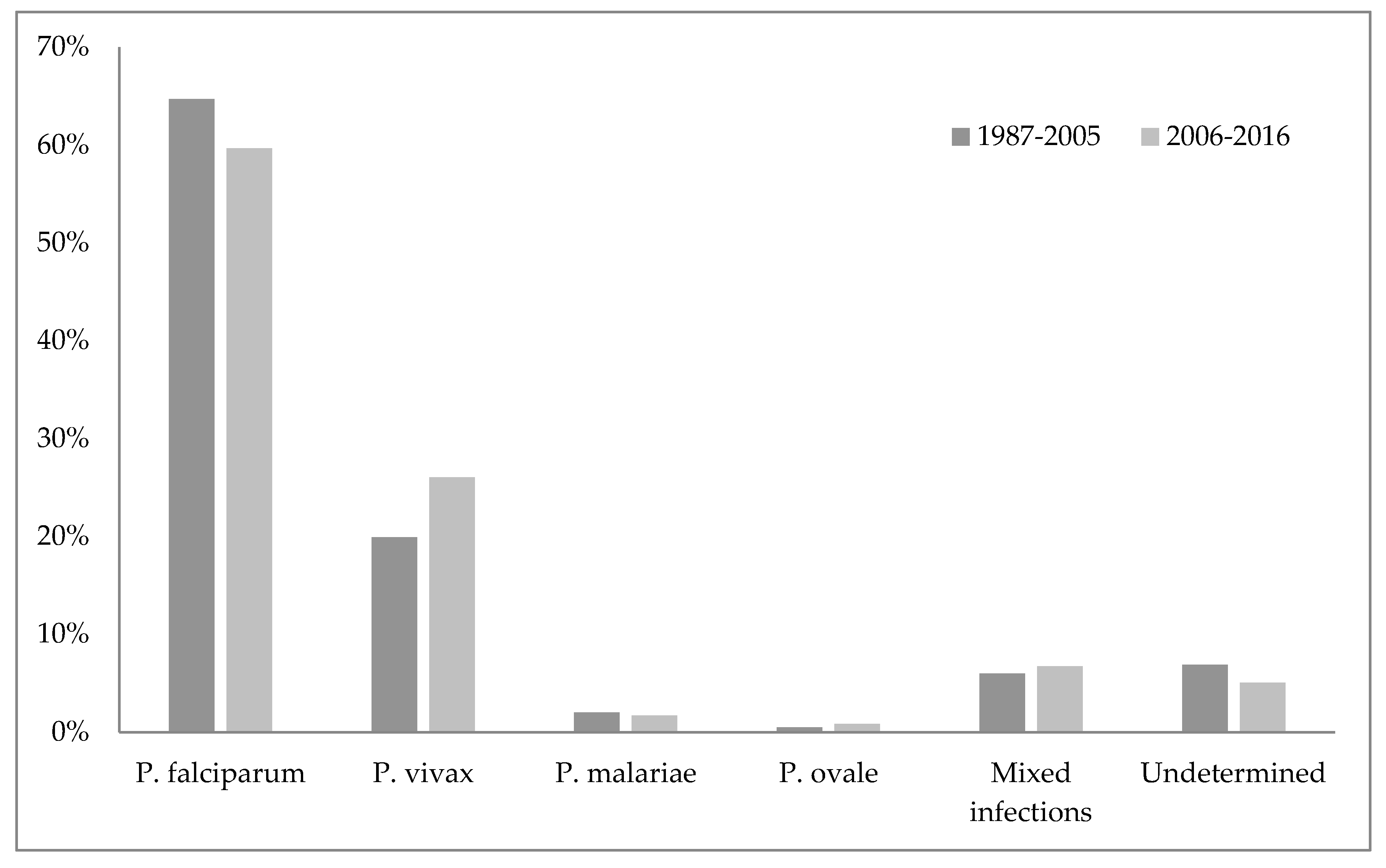
4.2. Malaria in Croatia
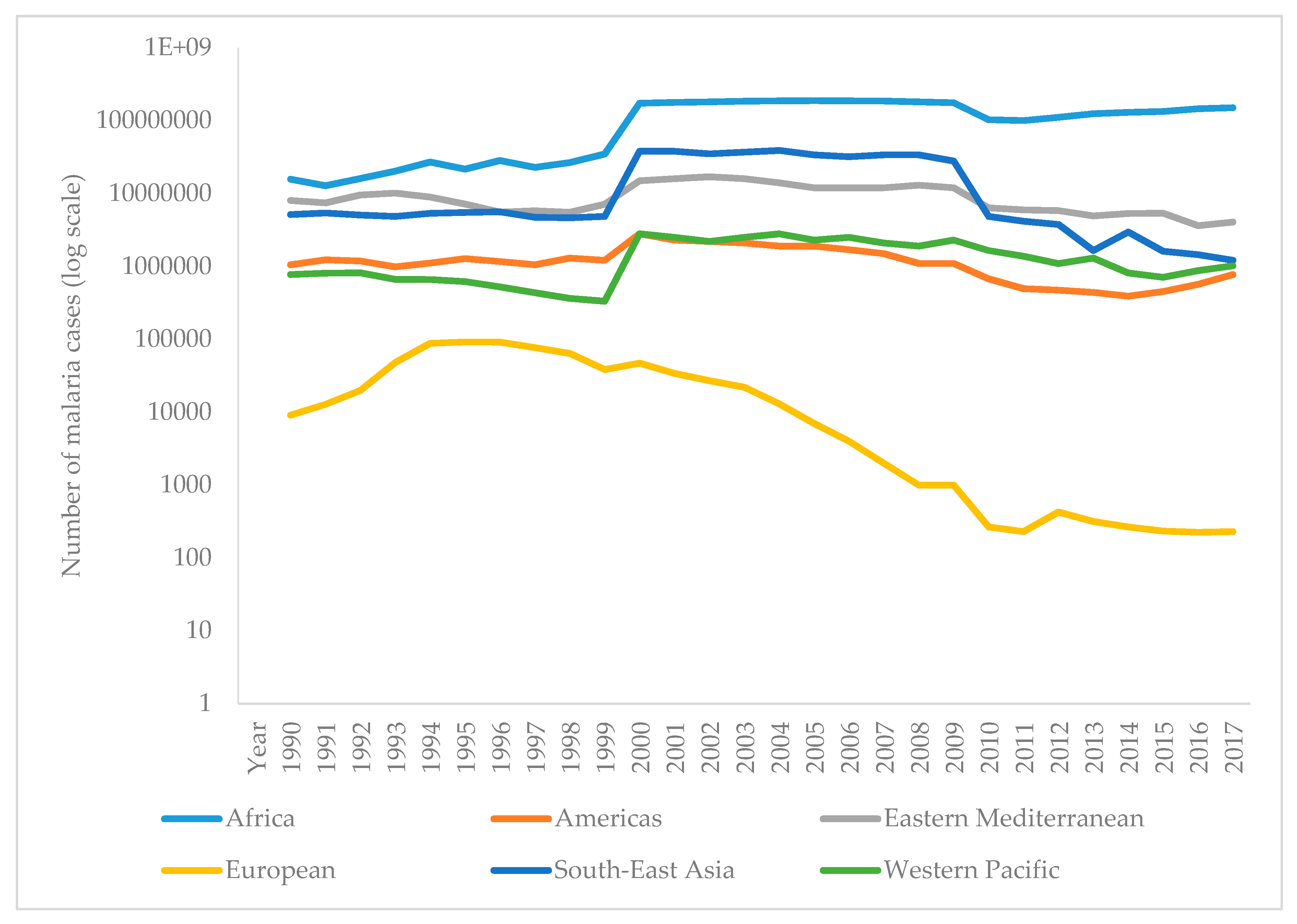
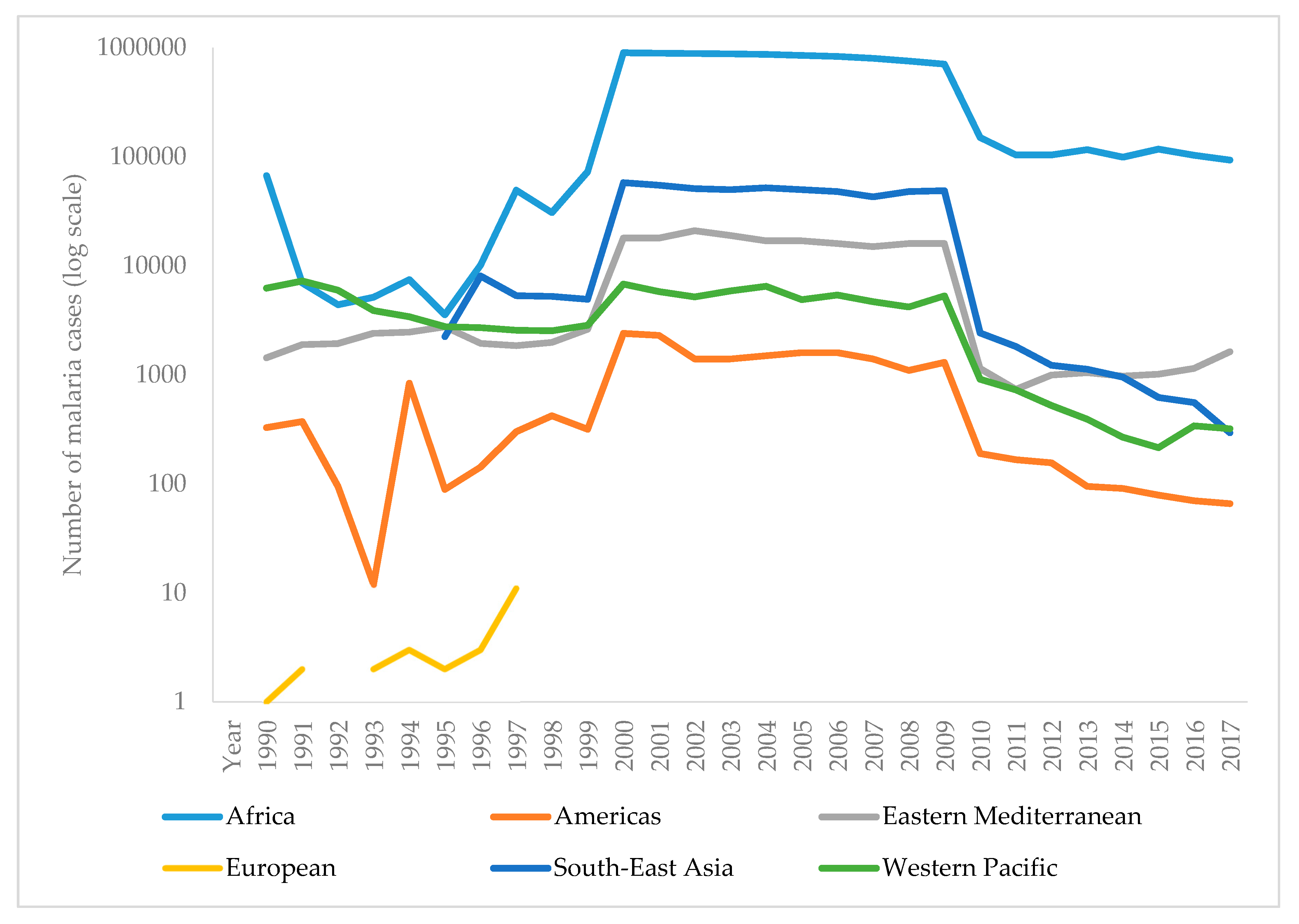
5. Malaria Trends in the World
6. Conclusions
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| ACT | Artemisinin-based combination therapy |
| CNS | Central nervous system |
| DDT | Dichlorodiphenyltrichloroethane |
| ELISA | Enzyme-linked immunosorbent assay |
| FDA | Food and Drug Administration |
| IFA | Immunofluorescence test |
| ITN | Insecticide-treated bed nets |
| PCR | Polymerase chain reaction |
| PfHRP2 | Plasmodium falciparum histidine-rich protein 2 |
| RDT | Rapid diagnostic tests |
| WHO | World Health Organization |
References
- World Health Organization. World Malaria Report 2018; WHO: Geneva, Switzerland, 2018. [Google Scholar]
- White, N.J.N.; Pukrittayakamee, S.; Hien, T.T.T.; Faiz, M.A.; Mokuolu, O.A.O.; Dondorp, A.A.M. Malaria. Lancet 2014, 383, 723–735. [Google Scholar] [CrossRef]
- Pan American Health Organization; World Health Organization. Epidemiological Alert, Increase of Malaria in the Americas; PAHO: Washington, DC, USA, 2018. [Google Scholar]
- Dhiman, S. Are malaria elimination efforts on right track? An analysis of gains achieved and challenges ahead. Infect. Dis. Poverty 2019, 8, 14. [Google Scholar] [CrossRef] [PubMed]
- Walker, N.; Nadjm, B.; Whitty, C. Malaria. Medicine 2017, 42, 52–58. [Google Scholar] [CrossRef]
- Antinori, S.; Galimberti, L.; Milazzo, L.; Corbellino, M. Biology of human malaria plasmodia including Plasmodium knowlesi. Mediterr. J. Hematol. Infect. Dis. 2012, 4, e2012013. [Google Scholar] [CrossRef] [PubMed]
- Ashley, E.A.; Pyae Phyo, A.; Woodrow, C.J. Malaria. Lancet 2018, 391, 1608–1621. [Google Scholar] [CrossRef]
- Singh, B.; Daneshvar, C. Human Infections and Detection of Plasmodium knowlesi. Clin. Microbiol. Rev. 2013, 26, 165–184. [Google Scholar] [CrossRef] [PubMed]
- Vuk, I.; Rajic, Z.; Zorc, B. Malaria and antimalarial drugs. Farm Glas 2008, 64, 51–60. [Google Scholar]
- Soulard, V.; Bosson-Vanga, H.; Lorthiois, A.; Roucher, C.; Franetich, J.-F.; Zanghi, G.; Bordessoulles, M.; Tefit, M.; Thellier, M.; Morosan, S.; et al. Plasmodium falciparum full life cycle and Plasmodium ovale liver stages in humanized mice. Nat. Commun. 2015, 6, 7690. [Google Scholar] [CrossRef]
- Josling, G.A.; Llinás, M. Sexual development in Plasmodium parasites: Knowing when it’s time to commit. Nat. Rev. Genet. 2015, 13, 573–587. [Google Scholar] [CrossRef]
- Blut, A. Untergruppe “Bewertung Blutassoziierter Krankheitserreger.” Malaria. Transfus. Med. Hemother. 2009, 36, 48–60. [Google Scholar] [CrossRef]
- Cowman, A.; Healer, J.; Marapana, D.; Marsh, K. Malaria, Biology and Disease. Cell 2016, 167, 610–624. [Google Scholar] [CrossRef] [PubMed]
- Cartwright, F.; Biddis, M. Disease and History; Naklada Ljevak: Zagreb, Croatia, 2006. [Google Scholar]
- Lehrer, S. Vitezi Medicine; Prosveta: Beograd, Serbia, 1981. [Google Scholar]
- Moss, W.; Shah, S.; Morrow, R. The History of Malaria and its Control. Int. Encycl. Public Health 2008, 389–398. [Google Scholar] [CrossRef]
- Dugacki, V. Dr. Rudolf Battara operation in Nin in 1902, the first systematic battle attempt against malaria in Croatia. Med. Jaderina 2005, 35, 33–40. [Google Scholar]
- Jovic, S. Istorija Medicine i Zdravstvene Kulture na tlu Dansnje Vojvodine 1718–1849 II; dio. Matica srpska, Srpska akademija nauka i umetnosti: Novi Sad, Serbia, 1998. [Google Scholar]
- Tan, S.Y.; Ahana, A. Charles Laveran (1845–1922), Nobel laureate pioneer of malaria. Singap. Med. J. 2009, 50, 657–658. [Google Scholar]
- Saifi, M.A.; Siddiqui, M.I.; Al-Khalifa, M.S. Malaria: Patterns of relapse and resistance. J. King Saud Univ. Sci. 2010, 22, 31–36. [Google Scholar] [CrossRef]
- Chu, C.S.; White, N.J. Management of relapsing Plasmodium vivax malaria. Expert Rev. Anti-Infect. Ther. 2016, 14, 885. [Google Scholar] [CrossRef] [PubMed]
- Murphy, S.C.; Shott, J.P.; Parikh, S.; Etter, P.; Prescott, W.R.; Stewart, V.A. Malaria diagnostics in clinical trials. Am. J. Trop. Med. Hyg. 2013, 89, 824–839. [Google Scholar] [CrossRef] [PubMed]
- Tangpukdee, N.; Duangdee, C.; Wilairatana, P.; Krudsood, S. Malaria diagnosis, a brief review. Korean J. Parasitol. 2009, 47, 93–102. [Google Scholar] [CrossRef] [PubMed]
- Trampuz, A.; Jereb, M.; Muzlovic, I.; Prabhu, R.M. Clinical review, Severe malaria. Crit. Care 2003, 7, 315–323. [Google Scholar] [CrossRef] [PubMed]
- She, R.C.; Rawlins, M.L.; Mohl, R.; Perkins, S.L.; Hill, H.R.; Litwin, C.M. Comparison of Immunofluorescence Antibody Testing and Two Enzyme Immunoassays in the Serologic Diagnosis of Malaria. J. Travel Med. 2007, 14, 105–111. [Google Scholar] [CrossRef] [PubMed]
- Oh, J.S.; Kim, J.S.; Lee, C.H.; Nam, D.H.; Kim, S.H.; Park, D.W.; Lee, C.K.; Lim, C.S.; Park, G.H. Evaluation of a malaria antibody enzyme immunoassay for use in blood screening. Mem. Inst. Oswaldo Cruz 2008, 103, 75–78. [Google Scholar] [CrossRef] [PubMed]
- Kakkilaya, B. Rapid Diagnosis of Malaria. Lab. Med. 2003, 34, 602–608. [Google Scholar] [CrossRef]
- Abba, K.; Kirkham, A.J.; Olliaro, P.L.; Deeks, J.J.; Donegan, S.; Garner, P.; Takwoingi, Y. Rapid diagnostic tests for diagnosing uncomplicated non-falciparum or Plasmodium vivax malaria in endemic countries. Cochrane Database Syst. Rev. 2014, 12. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Guidelines for the Treatment of Malaria, 3rd ed.; WHO: Geneva, Switzerland, 2015. [Google Scholar]
- World Health Organization. Malaria Rapid Diagnostic Test Performance, Results of WHO Product Testing of Malaria RDTs, Round 8 (2016–2018); WHO: Geneva, Switzerland, 2018. [Google Scholar]
- Ranadive, N.; Kunene, S.; Darteh, S.; Ntshalintshali, N.; Nhlabathi, N.; Dlamini, N.; Chitundu, S.; Saini, M.; Murphy, M.; Soble, A. Limitations of Rapid Diagnostic Testing in Patients with Suspected Malaria, A Diagnostic Accuracy Evaluation from Swaziland, a Low-Endemicity Country Aiming for Malaria Elimination. Clin. Infect. Dis. 2017, 64, 1221. [Google Scholar] [CrossRef] [PubMed]
- Berhane, A.; Russom, M.; Bahta, I.; Hagos, F.; Ghirmai, M.; Uqubay, S. Rapid diagnostic tests failing to detect Plasmodium falciparum infections in Eritrea, an investigation of reported false negative RDT results. Malar. J. 2017, 16, 105. [Google Scholar] [CrossRef] [PubMed]
- Kozycki, C.T.; Umulisa, N.; Rulisa, S.; Mwikarago, E.I.; Musabyimana, J.P.; Habimana, J.P.; Karema, C.; Krogstad, D.J. False-negative malaria rapid diagnostic tests in Rwanda: Impact of Plasmodium falciparum isolates lacking hrp2 and declining malaria transmission. Malar. J. 2017, 16, 123. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. False-negative RDT results and implications of new reports of P. falciparum histidine-rich protein 2/3 gene deletions. WHO 2017. [Google Scholar] [CrossRef]
- Murray, C.K.; Gasser, R.A.; Magill, A.J.; Miller, R.S. Update on Rapid Diagnostic Testing for Malaria. Clin. Microbiol. Rev. 2008, 21, 97–110. [Google Scholar] [CrossRef]
- Mathison, B.A.; Pritt, B.S. Update on Malaria Diagnostics and Test Utilization. J. Clin. Microbiol. 2017, 55, 2009–2017. [Google Scholar] [CrossRef]
- Rougemont, M.; Van Saanen, M.; Sahli, R.; Hinrikson, H.P.; Bille, J.; Jaton, K. Detection of Four Plasmodium Species in Blood from Humans by 18S rRNA Gene Subunit-Based and Species-Specific Real-Time PCR Assays. J. Clin. Microbiol. 2004, 42, 5636–5643. [Google Scholar] [CrossRef]
- Hsu, E. The history of qing hao in the Chinese materia medica. Trans. R. Soc. Trop. Med. Hyg. 2006, 100, 505–508. [Google Scholar] [CrossRef] [PubMed]
- Achan, J.; O Talisuna, A.; Erhart, A.; Yeka, A.; Tibenderana, J.K.; Baliraine, F.N.; Rosenthal, P.J.; D’Alessandro, U. Quinine, an old anti-malarial drug in a modern world: Role in the treatment of malaria. Malar. J. 2011, 10, 144. [Google Scholar] [CrossRef] [PubMed]
- Meshnick, S.R.; Dobson, M.J. The History of Antimalarial Drugs. In Antimalarial Chemotherapy, Mechanisms of Action, Resistance, and New Directions in Drug Discovery; Rosenthal, P., Ed.; Humana Press: Totowa NJ, USA, 2001; p. 396. [Google Scholar]
- World Health Organization. Antimalarial Drug Combination Therapy. Report of a WHO Technical Consultation; WHO: Geneva, Switzerland, 2001. [Google Scholar]
- Guo, Z. Artemisinin anti-malarial drugs in China. Acta Pharm. Sin. B 2016, 6, 115–124. [Google Scholar] [CrossRef] [PubMed]
- Ray, D. Organochlorine and Pyrethroid Insecticides. Compr. Toxicol. 2010, 13, 445–457. [Google Scholar] [CrossRef]
- Flannery, E.L.; Chatterjee, A.K.; Winzeler, E.A. Antimalarial drug discovery—Approaches and progress towards new medicines. Nat. Rev. Microbiol. 2013, 11, 849–862. [Google Scholar] [CrossRef] [PubMed]
- Zhao, X.; Smith, D.L.; Tatem, A.J. Exploring the spatiotemporal drivers of malaria elimination in Europe. Malar. J. 2016, 15, 122. [Google Scholar] [CrossRef] [PubMed]
- Karunamoorthi, K. Malaria vaccine, a future hope to curtail the global malaria burden. Int. J. Prev. Med. 2014, 5, 529–538. [Google Scholar]
- Moreno, A.; Joyner, C. Malaria vaccine clinical trials, what’s on the horizon. Curr. Opin. Immunol. 2015, 35, 98–106. [Google Scholar] [CrossRef]
- Coelho, C.H.; Doritchamou, J.Y.A.; Zaidi, I.; Duffy, P.E. Advances in malaria vaccine development, report from the 2017 malaria vaccine symposium. NPJ Vaccines 2017, 2, 34. [Google Scholar] [CrossRef]
- Mahmoudi, S.; Keshavarz, H. Efficacy of phase 3 trial of RTS, S/AS01 malaria vaccine, The need for an alternative development plan. Hum. Vaccines Immunother. 2017, 13, 2098–2101. [Google Scholar] [CrossRef]
- Rénia, L.; Goh, Y.S.; Peng, K.; Mauduit, M.; Snounou, G. Assessing Malaria Vaccine Efficacy. In Towards Malaria Elimination: A Leap Forw; Manguin, S., Dev, V., Eds.; IntechOpen: London, UK, 2018; pp. 339–362. [Google Scholar] [CrossRef]
- Draper, S.J.; Sack, B.K.; King, C.R.; Nielsen, C.M.; Rayner, J.C.; Higgins, M.K.; Long, C.A.; Seder, R.A. Malaria Vaccines, Recent Advances and New Horizons. Cell Host Microbe 2018, 24, 43–56. [Google Scholar] [CrossRef] [PubMed]
- Clinical Trials Register—Clinical Trials for Malaria 2019. Available online: https://www.clinicaltrialsregister.eu/ctr-search/search?query=Malaria (accessed on 30 April 2019).
- Crompton, P.D.; Pierce, S.K.; Miller, L.H. Advances and challenges in malaria vaccine development. J. Clin. Investig. 2010, 120, 4168–4178. [Google Scholar] [CrossRef] [PubMed]
- Arama, C.; Troye-Blomberg, M. The path of malaria vaccine development, challenges and perspectives. J. Intern. Med. 2014, 275, 456–466. [Google Scholar] [CrossRef] [PubMed]
- Kisalu, N.K.; Idris, A.H.; Weidle, C.; Flores-Garcia, Y.; Flynn, B.J.; Sack, B.K.; Murphy, S.; Schön, A.; Freire, E.; Francica, J.R.; et al. A human monoclonal antibody prevents malaria infection by targeting a new site of vulnerability on the parasite. Nat. Med. 2018, 24, 408–416. [Google Scholar] [CrossRef] [PubMed]
- Claudia, F. Malaria vaccine–is it still required? Are vaccine alternatives enough to achieve malaria control? Asian Pac. J. Trop. Biomed. 2014, 4, S541–S544. [Google Scholar] [CrossRef]
- Greenwood, B.; Targett, G. Malaria vaccines and the new malaria agenda. Clin. Microbiol. Infect. 2011, 17, 1600–1607. [Google Scholar] [CrossRef] [PubMed]
- Hoffman, S.L.; Vekemans, J.; Richie, T.; Duffy, P. The March Toward Malaria Vaccines. Am. J. Prev. Med. 2015, 49, S319–S333. [Google Scholar] [CrossRef]
- Shingadia, D. Treating malaria in the UK. Paediatr. Child Health 2014, 24, 232–235. [Google Scholar] [CrossRef]
- Kremsner, P.G.; Krishna, S. Antimalarial combinations. Lancet 2004, 364, 285–294. [Google Scholar] [CrossRef]
- Price, R.N.; Douglas, N.M. Artemisinin combination therapy for malaria, beyond good efficacy. Clin. Infect. Dis. 2009, 49, 1638–1640. [Google Scholar] [CrossRef]
- Nabudere, H.; Upunda, G.L.; Juma, M. Policy brief on improving access to artemisinin-based combination therapies for malaria in the East African community. Int. J. Technol. Assess Health Care 2010, 26, 255–259. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Sallares, R. Malaria and Rome: A History of Malaria in Ancient Italy; Oxford University Press: Oxford, UK, 2002. [Google Scholar]
- Micallef, M.J. The Roman fever, observations on the understanding of malaria in the ancient Roman world. Med. J. Aust. 2016, 205, 501–503. [Google Scholar] [CrossRef] [PubMed]
- Jugoslavenski Leksikografski Zavod. Medical Encycolpedia; Jugoslavenski Leksikografski Zavod: Zagreb, Yugoslavia, 1969; p. 374. [Google Scholar]
- Trausmiller, O. Malarija i civilizacija. Priroda 1936, 3, 76–83. [Google Scholar]
- Odolin, S.; Gautret, P.; Parola, P. Epidemiology of imported malaria in the mediterranean region. Mediterr. J. Hematol. Infect. Dis. 2012, 4, e2012031. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Fact Sheet—History of Malaria Elimination in the European Region; WHO: Geneva, Switzerland, 2016. [Google Scholar]
- Mlinaric, D. Eco-historical area of the istrian borderland as a framework of the development of endemic diseases. Vjesn. Istar. Arh. 2010, 17, 155–177. [Google Scholar]
- Radosevic, M. Health conditions in the municipality of Medulin through history. In Municipality of Medulin Monograph; Bader, A., Ed.; Opcina Medulin: Medulin, Croatia, 2013; pp. 314–325. [Google Scholar]
- Rudetic, I. Malaria. In Istarska Enciklopedija; Bertosa, M., Matijasic, R., Eds.; Leksikografski Zavod Miroslav Krleza: Zagreb, Croatia, 2005; p. 544. [Google Scholar]
- Bakic, J. Seven centuries of the prevention of spreading of the infectious diseases into Croatia—Overview of the 60th anniversary of establishment of modern pest control in Croatia. Hrvat. Cas. Zavod Javno Zdr. 2011, 7, 1–17. [Google Scholar]
- Bakic, J. Trust worthy facts on first medically-entomological laboratory and introduction of Gambusia holbrooki into Croatia. Hrvat. Cas. Zavod Javno Zdr. 2006, 2, 20–25. [Google Scholar]
- Nezic, E. Ribica gambuzija u borbi protiv malarije. Croat. J. Fish. 1938, 1, 62–66. [Google Scholar]
- Mulic, R.; Aljinovic, L.; Gizdic, Z.; Petri, N.M. Malaria in Republic of Croatia, past, present and future. Lijec. Vjesn. 2000, 122, 51–55. [Google Scholar]
- Fortis, A. Put Po Dalmaciji; Globus: Zagreb, Croatia, 1984. [Google Scholar]
- Wokaunn, M.; Juric, I.; Vrbica, Z. Between stigma and dawn of medicine, the last leprosarium in Croatia. Croat. Med. J. 2006, 47, 759–766. [Google Scholar]
- Tomasic, P. Malarija i blagostanje čovjeka. Priroda 1947, 4, 126–130. [Google Scholar]
- Skenderovic, R. Health Reforms Introduced by Maria Theresa in Provincial Slavonia and Generale Normativum Sanitatis of 1770. Scr. Slavon. 2005, 5, 115–143. [Google Scholar]
- Von Taube, F.W. Slavonija i Srijem 1777./1778; Drzavni Arhiv u Osijeku: Osijek, Croatia, 2012. [Google Scholar]
- Holzer, A. Asaniranje domacih predjela malarije. Liecnicki Viest. 1877, 4, 56–59. [Google Scholar]
- Majcen, V. The film funds of the school of national health (Andrija Stampar) at the Croatian film-library within the Croatian archive. Arh. Vjesn. 1987, 30, 71–88. [Google Scholar]
- Miletic-Medved, M.; Bozikov, J.; Uzarević, Z. Branko Cvjetanovic i Branimir Richter—Suradnici Andrije Stampara. Anal. Zavoda Za Znan. Umjetnicki Rad Osijeku 2012, 28, 103–113. [Google Scholar]
- Piperaki, E.T.; Daikos, G.L. Malaria in Europe, emerging threat or minor nuisance? Clin. Microbiol. Infect. 2016, 22, 487–493. [Google Scholar] [CrossRef]
- Mulic, R. Malaria in Croatia, from eradication until today. Malar. J. 2012, 11, P135. [Google Scholar] [CrossRef]
- Peric, D.; Skrobonja, I.; Skrobonja, A.; Peric, D.; Skrobonja, I.; Skrobonja, A. Malaria in Croatia in the period between 1987 to 2006. Lijec. Vjesn. 2009, 131, 192–195. [Google Scholar]
- Stevanovic, R.; Capak, K.; Brkic, K. Croatian Health Statistics Yearbook 2017; Croatian Institute of Public Health: Zagreb, Croatia, 2018. [Google Scholar]
- Talapko, J. Optimizacija metoda za uništavanje komaraca, ali i zaštite okoline. Prav. Vjesn. 1986, 2, 353–356. [Google Scholar]
- Tucak, A.; Dimitrijevic, M.; Gucunski, D.; Konstantinovic, B.; Miljus, B.; Grgic, Z.; Balog, Z.; Paulus, R.; Talapko, J. Multicentricni Program Istraživanja Ekologije Komaraca na Podrucju Sjeveroistocne Slavonije; Sveuciliste u Osijeku, Znanstvena Jedinica za Klinicko-Medicinska Istraživanja Opce bolnice Osijek: Osijek, Croatia, 1985. [Google Scholar]
- World Health Organization. World Malaria Report 2010; WHO: Geneva, Switzerland, 2010. [Google Scholar]
- Patouillard, E.; Griffin, J.; Bhatt, S.; Ghani, A.; Cibulskis, R. Global investment targets for malaria control and elimination between 2016 and 2030. BMJ Glob. Health 2017, 2, e000176. [Google Scholar] [CrossRef]
- World Health Organization. Global Report on Insecticide Resistance in Malaria Vectors, 2010–2016; WHO: Geneva, Switzerland, 2018. [Google Scholar]
- Alonso, P.; Noor, A.M. The global fight against malaria is at crossroads. Lancet 2017, 390, 2532–2534. [Google Scholar] [CrossRef]
| Advantages | Disadvantages | |
|---|---|---|
| Direct methods | ||
| Microscopic analysis | Fast test, cheap | Required much experience as well as equipment |
| Rapid diagnostic tests | Quick and simple | Less sensitive and accurate, price |
| Molecular tests | Correct determination of type, highly sensitive and accurate | Price, long-term in a large number of cases |
| Indirect methods | ||
| Indirect immunofluorescence | Specific, sensitive | Long time to perform, subjective evaluation of results |
| ELISA | Correct determination of type, specific, sensitive | Long time to perform, price |
| Medication Name | Year of Discovery/Synthesis | Origin | Usage | Mechanism of Action | Side Effects | Advantages/Disadvantages |
|---|---|---|---|---|---|---|
| Quinine | 1600 | Cinchona tree, South America | Resistance to chloroquine, prophylaxis and treatment of malaria | Inhibition of DNA and RNA synthesis | Headache, abortion, or congenital malformations if taken during pregnancy | Toxic, less effective than other medication |
| Chloroquine | 1934 | Synthesized by German scientist Hans Andersag | Most powerful remedy for the prophylaxis and treatment of malaria | Inhibition of DNA and RNA synthesis | Gastrointestinal disturbances, headache, skin irritation | Developed resistance of most strains of P. falciparum to the medication |
| Primaquine | 1953 | The 8-aminoquinoline derivative | Infections with P. vivax and P. ovale, prophylaxis and treatment of malaria | Interferes in transport chain of electrons and destroys parasite mitochondria | Anorexia, nausea, anemia, headaches, contraindicated in pregnancy and children under 4 years of age | Prevent relapse in P. vivax and P. ovale infection |
| Doxycycline | 1960 | Pfizer Inc. New York | Prophylaxis in areas with chloroquine resistance and against mefloquine resistant P. falciparum | Inhibition of protein synthesis by binding to 30S ribosomal subunit | Gastrointestinal disorders, nausea, vomiting, photosensitivity | Effective and cheap, use for treatment and prophylaxis in all malarious areas |
| Mefloquine | 1971 | USA army and WHO | Multiresistant P. falciparum strains, prophylaxis and treatment of malaria | Damage to parasite membrane | Gastrointestinal disorders, CNS disorder, contraindicated in pregnancy and patients with epilepsy | Partial resistance, brain damage |
| Proguanil (chloroguanide) | 1953 | Biguanide derivate | Prophylaxis in infections with P. falciparum | Inhibition of DNA synthesis | Digestive problems only in large doses | The least toxic antimalarial drug |
| Pyrimethamine | 1953 | Pyrimidine derivatives | For tissue parasites, prophylaxis and treatment of malaria | Folic acid antagonist | Gastrointestinal disorders, neuropathy, in high doses also megaloblastic anemia | Rapid development of resistance |
| Atovaquone/proguanil | 2000 | Ubiquinone analog | For the prophylaxis and treatment of malaria | Inhibition of cytochrome bc1 in Plasmodium | Nausea, vomiting, diarrhea, headache, dizziness, anxiety, difficulty falling asleep, rash, fever | Most commonly used, fewer side effects and more expensive than mefloquine, P. falciparum resistance |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Talapko, J.; Škrlec, I.; Alebić, T.; Jukić, M.; Včev, A. Malaria: The Past and the Present. Microorganisms 2019, 7, 179. https://doi.org/10.3390/microorganisms7060179
Talapko J, Škrlec I, Alebić T, Jukić M, Včev A. Malaria: The Past and the Present. Microorganisms. 2019; 7(6):179. https://doi.org/10.3390/microorganisms7060179
Chicago/Turabian StyleTalapko, Jasminka, Ivana Škrlec, Tamara Alebić, Melita Jukić, and Aleksandar Včev. 2019. "Malaria: The Past and the Present" Microorganisms 7, no. 6: 179. https://doi.org/10.3390/microorganisms7060179
APA StyleTalapko, J., Škrlec, I., Alebić, T., Jukić, M., & Včev, A. (2019). Malaria: The Past and the Present. Microorganisms, 7(6), 179. https://doi.org/10.3390/microorganisms7060179






