A Dengue Vaccine: Will It be Accepted and Is It Feasible? Lessons from Barranquilla, Colombia, and Merida, Venezuela
Abstract
1. Introduction
2. Materials and Methods
3. Results
3.1. Demographics
3.2. Colombia
3.3. Venezuela
4. Discussion
4.1. Overview
4.2. The Disease
4.3. Current Vaccination System
4.4. Study Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Villar, L.A.; Rojas, D.P.; Besada-Lombana, S.; Sarti, E. Epidemiological trends of dengue disease in Colombia (2000–2011): A systematic review. PLoS Negl. Trop. Dis. 2015, 9, e0003499. [Google Scholar] [CrossRef] [PubMed]
- Rico-Mendoza, A.; Porras-Ramírez, A.; Chang, A.; Encinales, L.; Lynch, R. Co-circulation of dengue, chikungunya, and Zika viruses in Colombia. Rev. Panam. Salud. Publica 2019, 43, e49. [Google Scholar] [CrossRef] [PubMed]
- San Martín, J.L.; Brathwaite, O.; Zambrano, B.; Solórzano, J.O.; Bouckenooghe, A.; Dayan, G.H.; Guzmán, M.G. The epidemiology of dengue in the Americas over the last three decades: A worrisome reality. Am. J. Trop. Med. Hyg. 2010, 82, 128–135. [Google Scholar] [CrossRef] [PubMed]
- Velasco-Salas, Z.I.; Sierra, G.M.; Guzmán, D.M.; Zambrano, J.; Vivas, D.; Comach, G.; Wilschut, J.C.; Tami, A. Dengue seroprevalence and risk factors for past and recent viral transmission in Venezuela: A comprehensive community-based study. Am. J. Trop. Med. Hyg. 2014, 91, 1039–1048. [Google Scholar] [CrossRef] [PubMed]
- Grillet, M.E.; Hernández-Villena, J.V.; Llewellyn, M.S.; Paniz-Mondolfi, A.E.; Tami, A.; Vincenti-Gonzalez, M.F.; Marquez, M.; Mogollon-Mendoza, A.C.; Hernandez-Pereira, C.E.; Plaza-Morr, J.D.; et al. Venezuela’s humanitarian crisis, resurgence of vector-borne diseases, and implications for spillover in the region. Lancet Infect. Dis. 2019, 19, E149–E161. [Google Scholar] [CrossRef]
- World Health Organization. Dengue vaccine: WHO position paper–September 2018. Wkly Epidemiol. Rec. 2019, 93, 457–476. [Google Scholar]
- World Health Organization. Dengue vaccine: WHO position paper–July 2016. Wkly Epidemiol. Rec. 2016, 91, 349–364. [Google Scholar]
- World Health Organization. Principles and Considerations for Adding a Vaccine to a National Immunization Programme; World Health Organization: Geneva, Switzerland, 2016. [Google Scholar]
- Torresi, J.; Tapia-Conyer, R.; Margolis, H. Preparing for dengue vaccine introduction: Recommendations from the 1st dengue v2V international meeting. PLoS Negl. Trop. Dis. 2013, 7, e2261. [Google Scholar] [CrossRef] [PubMed]
- Larson, H.J.; Hartigan-Go, K.; de Figueiredo, A. Vaccine confidence plummets in the Philippines following dengue vaccine scare: Why it matters to pandemic preparedness. Hum. Vaccin Immunother. 2018, 15, 625–627. [Google Scholar] [CrossRef] [PubMed]

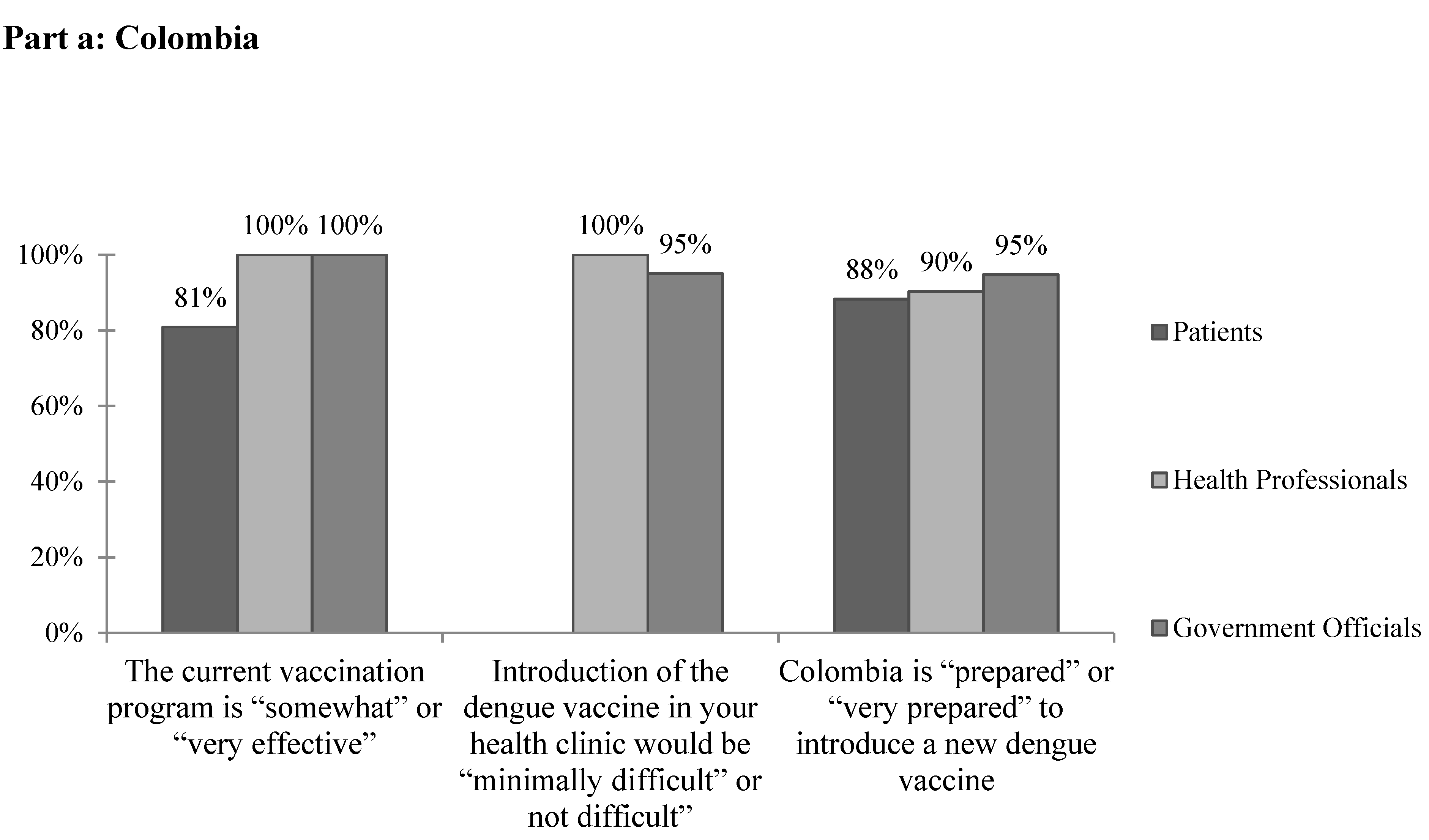
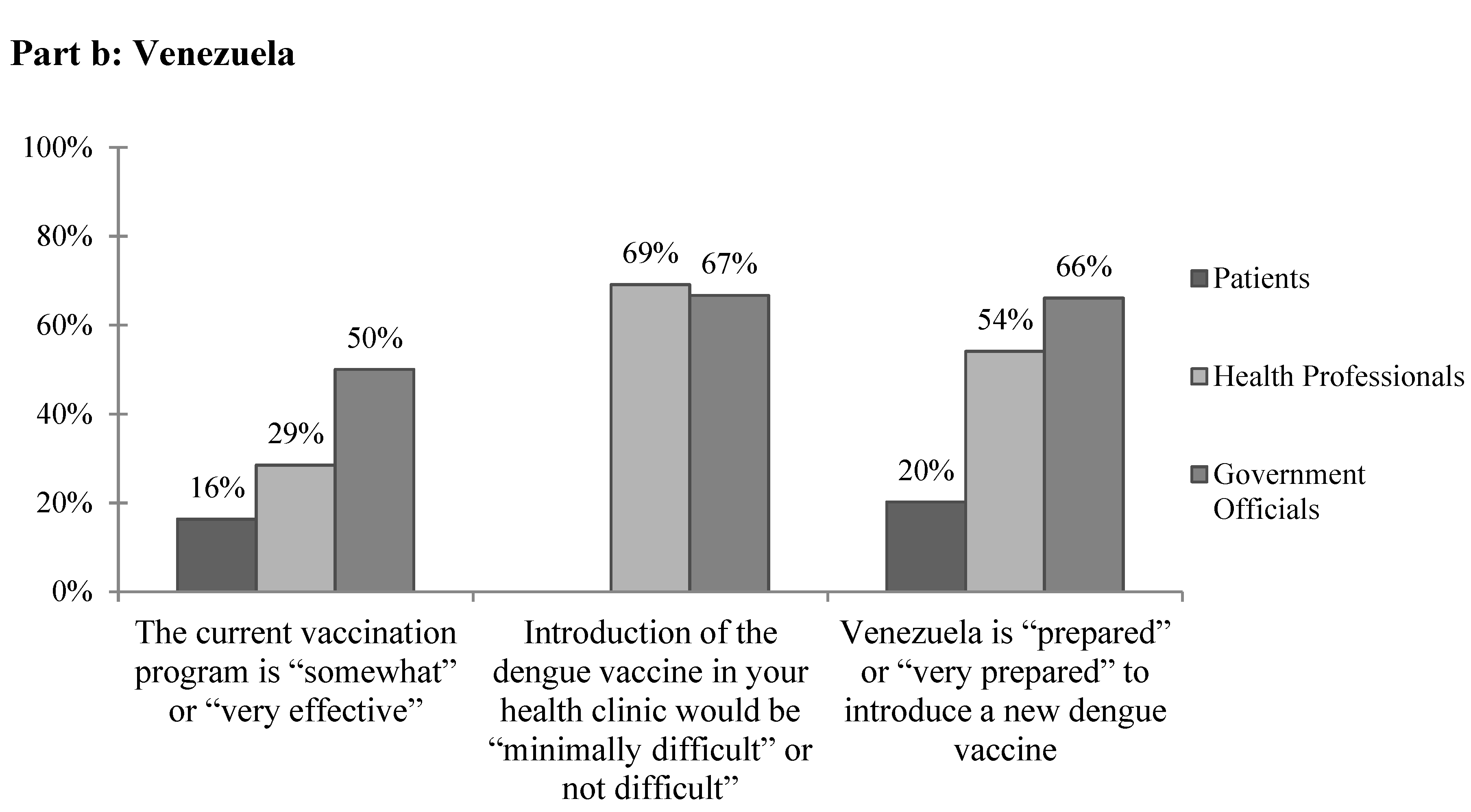
| Colombia | Patients (n = 191) | Health Professionals (n = 55) | Government Officials (n = 20) |
|---|---|---|---|
| Vaccines are beneficial in improving health. | 173 (90.6%) | 54 (98.2%) | 19 (95.0%) |
| Vaccines are safe. | 156 (81.7%) | 52 (94.5%) | 18 (90.0%) |
| A dengue vaccine would be useful in your community/country. | 167 (87.4%) | 54 (98.2%) | 19 (95.0%) |
| You would get a dengue vaccine. | 168 (88.0%) | 54 (98.2%) | 18 (90.0%) |
| You would vaccinate your child(ren) with the dengue vaccine | 156 (82.5%) | 53 (96.4%) | 18 (90.0%) |
| n = 189 | |||
| You would get vaccinated if you had to receive multiple doses. | NA | 48 (88.9%) | NA |
| You would get vaccinated if protection from illness was for less than two years. | 61 (32.3%) | 38 (69.1%) | NA |
| n = 189 | |||
| Dengue vaccines should be a standard vaccination. | 115 (61.2%) | 50 (90.9%) | 18 (90.0%) |
| n = 188 | |||
| As a provider, you would “very likely” recommend a dengue vaccine to your patients. | NA | 36 (65.5%) | NA |
| There will be political opposition to the dengue vaccine’s implementation. | 6 (3.2%) | NA | 6 (33.3%) |
| n = 190 | |||
| You would be willing to pay for the dengue vaccine | 88 (46.3%) n = 190 | NA | NA |
| Colombia | Health Professionals | Government Officials (n = 20) |
|---|---|---|
| Data collected are sent to a national database | 52 (94.5%) n = 55 | 18 (90.0%) |
| Surveillance data collected are serotype specific | 37 (71.3%) n = 52 | NA |
| Surveillance data are collected all year round (i.e., even during the dry season) | 53 (98.1%) n = 54 | 19 (95.0%) |
| There is currently a system in place to monitor/report: | ||
| Cases | NA | 19 (95.0%) |
| Lab test results | NA | 20 (100%) |
| Vaccine coverage | NA | 18 (90.0%) |
| Adverse events | NA | 16 (88.9%) n = 18 |
| Case outcomes | NA | 17 (94.4%) n = 18 |
| Data are collected equally from public and private healthcare facilities | NA | 14 (70.0%) |
| Surveillance data are collected equally from all areas of the country | NA | 14 (70%) |
| There are set national criteria in use for defining dengue (without warning signs, with warning signs, severe) | 53 (100%) n = 53 | 18 (90.0%) |
| For reported cases of dengue there is patient follow-up | 49 (94.2%) n = 52 | 18 (94.7%) n = 19 |
| Databases are electronic | 54 (98.2%) n = 55 | 19 (95.0%) |
| Vaccination plans are created each year | 42 (79.2%) n = 53 | 19 (95.0%) |
| Multiyear vaccination plans are created | 37 (72.5%) n = 51 | 13 (68.4%) n = 19 |
| Disease burden/vaccine needs are forecasted | 3 (6.1%) n = 49 | 9 (52.9%) n = 17 |
| Freezers and cold-chain supply are readily available | 51 (94.4%) n = 54 | 17 (85%) |
| Cold chain supply has never been broken | 23 (45.1%) n = 51 | NA |
| This healthcare facility performs dengue diagnostics | 52 (94.5%) n = 54 | … n = 16 |
| NS1 rapid | 37 (68.5%) | 3 (18.8%) |
| IgM rapid | 11 (20.4%) | 6 (37.5%) |
| IgG rapid | 8 (14.8%) | 6 (37.5%) |
| Neutralization assay | 0 (0%) | 0 (0%) |
| IgM ELISA | 12 (22.2%) | 9 (56.3%) |
| IgG ELISA | 9 (16.7%) | 7 (43.8%) |
| NS1 ELISA | 0 (0%) | 0 (0%) |
| PCR | 2 (3.7%) | 4 (25.0%) |
| Colombia | Health Professionals (n = 39) | Government Officials (n = 16) |
|---|---|---|
| Barriers to current vaccines | ||
| Financial | 1 (2.6%) | 7 (43.8%) |
| Political | 0 (0%) | 0 (0%) |
| Vaccine Availability | 0 (0%) | 0 (0%) |
| Lack of education/dissemination of knowledge | 0 (0%) | 0 (0%) |
| Other | 1 (2.6%) | 5 (31.3%) |
| None | 36 (92.3%) | 5 (31.3%) |
| Unknown | 1 (2.6%) | 0 (0%) |
| Barriers to implementing a dengue vaccine | ||
| Financial | 6 (17.6%) | 7 (63.6%) |
| Cultural | 5 (14.7%) | 4 (40.0%) |
| Political | 0 (0.0%) | 3 (27.3%) |
| Other | 0 (0.0%) | 4 (36.4%) |
| None | 21 (61.8%) | 0 (0.0%) |
| Unknown | 3 (8.8%) | 0 (0.0%) |
| Venezuela | Patients (n = 159) | Health Professionals (n = 142) | Government Officials (n = 6) |
|---|---|---|---|
| Vaccines are beneficial in improving health. | 151 (95.0%) | 133 (93.7%) | 6 (100%) |
| Vaccines are safe. | 141 (88.7%) | 121 (85.2%) | 4 (66.7%) |
| A dengue vaccine would be useful in your community/country. | 150 (95.5%) | 132 (94.3%) | 6 (100%) |
| n = 157 | n = 140 | ||
| You would get a dengue vaccine. | 150 (94.3%) | 132 (94.3%) | 5 (83.3%) |
| n = 140 | |||
| You would vaccinate your child(ren) with the dengue vaccine | 149 (94.9%) | 134 (94.4%) | 6 (100%) |
| n = 157 | |||
| You would get vaccinated if you had to receive multiple doses. | NA | 130 (92.2%) | NA |
| n = 141 | |||
| You would get vaccinated if protection from illness was for less than two years. | 146 (95.4%) | 125 (89.3%) | NA |
| n = 153 | n = 140 | ||
| Dengue vaccines should be a standard vaccination. | 147 (95.5%) | 127 (92.7%) | 6 (100%) |
| n = 154 | n = 137 | ||
| As a provider, you would “very likely” recommend a dengue vaccine to your patients. | NA | 118 (84.9%) | NA |
| n = 139 | |||
| There will be political opposition to the dengue vaccine’s implementation. | 24 (15.0%) | NA | 4 (66.7%) |
| n = 160 | |||
| You would be willing to pay for the dengue vaccine | 57 (35.8%) | NA | NA |
| Venezuela | Health Professionals | Government Officials (n = 6) |
|---|---|---|
| Data collected sent to a national database | 44 (32.8%) n = 134 | 6 (100%) |
| Surveillance data collected are serotype specific | 1 (0.7%) n = 138 | NA |
| Surveillance data are collected all year round (i.e., even during the dry season) | 91 (66.9%) n = 136 | 6 (100%) |
| There is currently a system in place to monitor/report: | ||
| Cases | NA | 6 (100%) |
| Lab test results | NA | 6 (100%) |
| Vaccine coverage | NA | 6 (100%) |
| Adverse events | NA | 6 (100%) |
| Case outcomes | NA | 6 (100%) |
| Data are collected equally from public and private healthcare facilities | NA | 5 (83.3%) |
| Surveillance data are collected equally from all areas of the country | NA | 3 (50.0%) |
| There are set national criteria in use for defining dengue (without warning signs, with warning signs, severe) | 120 (90.2%) n = 133 | 6 (100%) |
| For reported cases of dengue there is patient follow-up | 46 (34.3%) n = 134 | 5 (83.3%) |
| Databases are electronic | 10 (7.4%) | 3 (60.0%) |
| n = 135 | n = 5 | |
| Vaccination plans are created each year | 46 (33.3%) | 6 (100%) |
| n = 138 | ||
| Multiyear vaccination plans are created | 8 (15.4%) | 0 (0%) |
| n = 52 | ||
| Disease burden/vaccine needs are forecasted | 22 (16.5%) | 3 (50.0%) |
| n = 133 | ||
| Freezers and cold-chain supply are readily available | 30 (21.3%) | 5 (83.3%) |
| n = 141 | ||
| Cold chain supply has never been broken | 26 (19.1%) | NA |
| n = 136 | ||
| This healthcare facility performs dengue diagnostics | 98 (72.6%) n = 135 | ... |
| NS1 rapid | 17 (12.2%) | 0 (0%) |
| IgM rapid | 36 (25.9%) | 0 (0%) |
| IgG rapid | 25 (18.0%) | 0 (0%) |
| Neutralization assay | 0 (0%) | 0 (0%) |
| IgM ELISA | 80 (57.6%) | 6 (100%) |
| IgG ELISA | 9 (6.5%) | 0 (0%) |
| NS1 ELISA | 1 (0.7%) | 0 (0%) |
| PCR | 6 (4.3%) | 0 (0%) |
| Venezuela | Health Professionals (n = 139) | Government Officials (n = 6) |
|---|---|---|
| Barriers to current vaccines | ||
| Financial | 60 (43.2%) | 1 (16.7%) |
| Political | 71 (51.1%) | 3 (50.0%) |
| Vaccine Availability | 16 (11.5%) | 3 (50.0%) |
| Lack of education/dissemination of knowledge | 6 (4.3%) | 1 (16.7%) |
| Other | 7 (5.0%) | 2 (33.3%) |
| None | 3 (2.2%) | 0 (0%) |
| Unknown | 3 (2.2%) | 0 (0%) |
| Barriers to implementing a dengue vaccine | ||
| Financial | 37 (27.8%) | 5 (83.3%) |
| Political | 95 (71.4%) | 3 (50.0%) |
| Vaccine Availability | 1 (0.8%) | 1 (16.7%) |
| Lack of education/dissemination of knowledge | 6 (4.5%) | 0 (0%) |
| Other | 8 (6.0%) | 2 (33.3%) |
| None | 0 (0%) | 0 (0%) |
| Unknown | 0 (0%) | 0 (0%) |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
McMahon, E.; Encinales, L.; Navarro Encinales, C.; Vielma, S.; Pacheco, N.; Avendaño Echavez, L.G.; Acosta Rodríguez, S.; Calderon, M.; Encinales Sanabria, S.; Encinales Sanabria, L.; et al. A Dengue Vaccine: Will It be Accepted and Is It Feasible? Lessons from Barranquilla, Colombia, and Merida, Venezuela. Microorganisms 2019, 7, 458. https://doi.org/10.3390/microorganisms7100458
McMahon E, Encinales L, Navarro Encinales C, Vielma S, Pacheco N, Avendaño Echavez LG, Acosta Rodríguez S, Calderon M, Encinales Sanabria S, Encinales Sanabria L, et al. A Dengue Vaccine: Will It be Accepted and Is It Feasible? Lessons from Barranquilla, Colombia, and Merida, Venezuela. Microorganisms. 2019; 7(10):458. https://doi.org/10.3390/microorganisms7100458
Chicago/Turabian StyleMcMahon, Elizabeth, Liliana Encinales, Carlos Navarro Encinales, Silvana Vielma, Nelly Pacheco, Lil Geraldine Avendaño Echavez, Sandra Acosta Rodríguez, Milena Calderon, Silvia Encinales Sanabria, Lorena Encinales Sanabria, and et al. 2019. "A Dengue Vaccine: Will It be Accepted and Is It Feasible? Lessons from Barranquilla, Colombia, and Merida, Venezuela" Microorganisms 7, no. 10: 458. https://doi.org/10.3390/microorganisms7100458
APA StyleMcMahon, E., Encinales, L., Navarro Encinales, C., Vielma, S., Pacheco, N., Avendaño Echavez, L. G., Acosta Rodríguez, S., Calderon, M., Encinales Sanabria, S., Encinales Sanabria, L., Serrano Bernal, E., Gonzaléz Coba, A., Jiménez, D., Simon, G., & Chang, A. Y. (2019). A Dengue Vaccine: Will It be Accepted and Is It Feasible? Lessons from Barranquilla, Colombia, and Merida, Venezuela. Microorganisms, 7(10), 458. https://doi.org/10.3390/microorganisms7100458





