Current Use of Oral Anticoagulation Therapy in Elderly Patients with Atrial Fibrillation: Results from an Italian Multicenter Prospective Study—The ISNEP Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Data Measures
2.3. Statistical Analysis
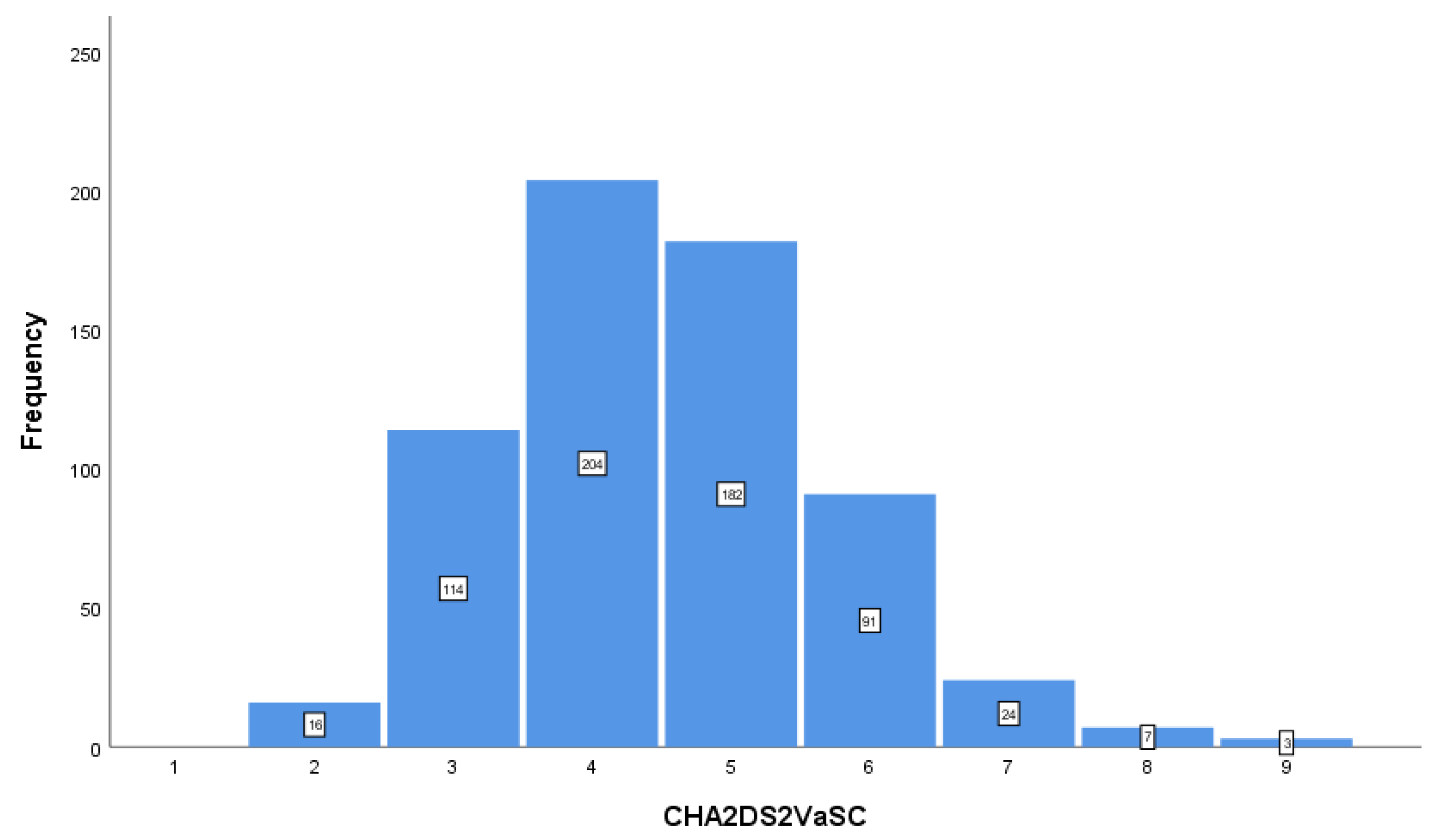
3. Results
4. Discussion
- -
- In elderly patients, there was still a significant portion of this population treated with VKAs;
- -
- The patients’ satisfaction with therapy was higher in the NOAC group.
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Informed Consent Statement
Conflicts of Interest
References
- Staerk, L.; Sherer, J.A.; Ko, D.; Benjamin, E.J.; Helm, R.H. Atrial fibrillation: Epidemiology, pathophysiology, and clinical outcomes. Circ. Res. 2017, 120, 1501–1517. [Google Scholar] [CrossRef] [PubMed]
- Krijthe, B.P.; Kunst, A.; Benjamin, E.; Lip, G.Y.; Franco, O.; Hofman, A.; Witteman, J.C.; Stricker, B.H.; Heeringa, J. Projections on the number of individuals with atrial fibrillation in the European Union, from 2000 to 2060. Eur. Heart J. 2013, 34, 2746–2751. [Google Scholar] [CrossRef] [PubMed]
- Hindricks, G.; Potpara, T.; Dagres, N.; Arbelo, E.; Bax, J.J.; Blomström-Lundqvist, C.; Boriani, G.; Castella, M.; Dan, G.A.; Dilaveris, P.E.; et al. ESC Scientific Document Group. 2020 ESC Guidelines for the diagnosis and management of atrial fibrillation developed in collaboration with the European Association for Cardio-Thoracic Surgery (EACTS): The Task Force for the diagnosis and management of atrial fibrillation of the European Society of Cardiology (ESC) Developed with the special contribution of the European Heart Rhythm Association (EHRA) of the ESC. Eur. Heart J. 2021, 42, 373–498. [Google Scholar] [PubMed]
- Granger, C.B.; Alexander, J.H.; McMurray, J.J.V.; Lopes, R.D.; Hylek, E.M.; Hanna, M.; Al-Khalidi, H.R.; Ansell, J.; Atar, D.; Ave-zum, A.; et al. Apixaban versus Warfarin in Patients with Atrial Fibrillation. N. Engl. J. Med. 2011, 365, 981–992 . [Google Scholar] [CrossRef]
- Giugliano, R.P.; Ruff, C.T.; Braunwald, E.; Murphy, S.A.; Wiviott, S.D.; Halperin, J.L.; Waldo, A.L.; Ezekowitz, M.D.; Weitz, J.I.; Špinar, J.; et al. Edoxaban versus warfarin in patients with atrial fibrillation. ENGAGE AF-TIMI 48 Trial. N. Engl. J. Med. 2013, 369, 2093–2104. [Google Scholar] [CrossRef] [PubMed]
- Patel, M.R.; Mahaffey, K.W.; Garg, J.; Pan, G.; Singer, D.E.; Hacke, W.; Breithardt, G.; Halperin, J.L.; Hankey, G.J.; Piccini, J.P.; et al. Rivaroxaban versus warfarin in patients with nonvalvular atrial fibrillation. ROCKET-AF Trial. N. Engl. J. Med. 2011, 365, 883–891. [Google Scholar] [CrossRef]
- Connolly, S.J.; Ezekowitz, M.D.; Yusuf, S.; Eikelboom, J.; Oldgren, J.; Parekh, A.; Pogue, J.; Reilly, P.A.; Themeles, E.; Varrone, J.; et al. Dabigatran versus Warfarin in Patients with Atrial Fibrillation. N. Engl. J. Med. 2009, 361, 1139–1151. [Google Scholar] [CrossRef]
- Barnett, K.; Mercer, S.W.; Norbury, M.; Watt, G.; Wyke, S.; Guthrie, B. Epidemiology of multimorbidity and implications for health care, research, and medical education: A cross-sectional study. Lancet 2012, 380, 37–43. [Google Scholar] [CrossRef]
- Patti, G.; Lucerna, M.; Pecen, L.; Siller-Matula, J.M.; Cavallari, I.; Kirchhof, P.; De Caterina, R. Thromboembolic Risk, Bleeding Outcomes and Effect of Different Antithrombotic Strategies in Very Elderly Patients With Atrial Fibrillation: A Sub-Analysis From the PREFER in AF (PREvention oF Thromboembolic Events-European Registry in Atrial Fibrillation). J. Am. Heart Assoc. 2017, 6, e005657. [Google Scholar] [CrossRef]
- Kato, E.T.; Goto, S.; Giugliano, R.P. Overview of oral antithrombotic treatment in elderly patients with atrial fibrillation. Ageing Res. Rev. 2018, 49, 115–124. [Google Scholar] [CrossRef]
- Polidori, M.C.; Alves, M.; Bahat, G.; Boureau, A.S.; Ozkok, S.; Pfister, R.; Pilotto, A.; Veronese, N.; Bo, M.; on behalf of the Special Interest Group “Cardiovascular Diseases” of the EuGMS. Atrial fibrillation: A geriatric perspective on the 2020 ESC guidelines. Eur. Geriatr. Med. 2022, 13, 5–18. [Google Scholar] [CrossRef] [PubMed]
- Proietti, M.; Camera, M.; Gallieni, M.; Gianturco, L.; Gidaro, A.; Piemontese, C.; Pizzetti, G.; Redaelli, F.; Scimeca, B.; Tadeo, C.S.; et al. Use and Prescription of Direct Oral Anticoagulants in Older and Frail Patients with Atrial Fibrillation: A Multidisciplinary Consensus Document. J. Pers. Med. 2022, 12, 469. [Google Scholar] [CrossRef] [PubMed]
- Eikelboom, J.W.; Connolly, S.J.; Healey, J.S.; Yang, S.; Yusuf, S.; Wallentin, L.; Oldgren, J.; Ezekowitz, M.; Alings, M.; Kaatz, S.; et al. Risk of bleeding with 2 doses of dabigatran compared with warfarin in older and younger patients with atrial fibrillation: An analysis of the randomized evaluation of long-term anticoagulant therapy (RE-LY) trial. Circulation 2011, 123, 2363–2372. [Google Scholar] [CrossRef]
- Hori, M.; Matsumoto, M.; Tanahashi, N.; Momomura, S.-I.; Uchiyama, S.; Goto, S.; Izumi, T.; Koretsune, Y.; Kajikawa, M.; Kato, M.; et al. Rivaroxaban vs. warfarin in Japanese patients with non-valvular atrial fibrillation in relation to age. Circ. J. 2014, 78, 1349–1356. [Google Scholar] [CrossRef] [PubMed]
- Halvorsen, S.; Atar, D.; Yang, H.; De Caterina, R.; Erol, C.; Garcia, D.; Granger, C.B.; Hanna, M.; Held, C.; Husted, S.; et al. Efficacy and safety of apixaban compared with warfarin according to age for stroke prevention in atrial fibrillation: Observations from the ARISTOTLE trial. Eur. Heart J. 2014, 35, 1864–1872. [Google Scholar] [CrossRef] [PubMed]
- Halperin, J.L.; Hankey, G.J.; Wojdyla, D.M.; Piccini, J.P.; Lokhnygina, Y.; Patel, M.R.; Breithardt, G.; Singer, D.E.; Becker, R.C.; Hacke, W.; et al. Efficacy and safety of rivaroxaban compared with warfarin among elderly patients with nonvalvular atrial fibrillation in the Rivaroxaban Once Daily, Oral, Direct Factor Xa Inhibition Compared With Vitamin K Antagonism for Prevention of Stroke and Embolism Trial in Atrial Fibrillation (ROCKET AF). Circulation 2014, 130, 138–146. [Google Scholar]
- Kato, E.T.; Giugliano, R.P.; Ruff, C.T.; Koretsune, Y.; Yamashita, T.; Kiss, R.G.; Nordio, F.; Murphy, S.A.; Kimura, T.; Jin, J.; et al. Efficacy and safety of edoxaban in elderly patients with atrial fibrillation in the ENGAGE AF–TIMI 48 Trial. J. Am. Heart Assoc. 2016, 5, e003432. [Google Scholar] [CrossRef]
- Cockcroft, D.W.; Gault, H. Prediction of creatinine clearance from serum creatinine. Nephron 1976, 16, 31–41. [Google Scholar] [CrossRef]
- Yamashita, T.; Suzuki, S.; Inoue, H.; Akao, M.; Atarashi, H.; Ikeda, T.; Okumura, K.; Koretsune, Y.; Shimizu, W.; Tsutsui, H.; et al. Two-year outcomes of more than 30 000 elderly patients with atrial fibrillation: Results from the All Nippon AF In the Elderly (ANAFIE) Registry. Eur. Heart J. Qual. Care Clin. Outcomes 2021, 8, 202–213. [Google Scholar] [CrossRef]
- Blacher, J.; Sorbets, E.; Meynier, D.G.; Huberman, J.-P.; Gauthier, J.; Cohen, S.; Hoffman, O. Determinants of Antithrombotic Treatment for Atrial Fibrillation in Octogenarians: Results of the OCTOFA Study. Clin. Drug Investig. 2019, 39, 891–898. [Google Scholar] [CrossRef]
- Collins, P.; Lewin, A.; Irving, N.V.; Sylvester, K.; Fanikos, J.; Goldhaber, S.Z.; Connors, J.M. Atrial Fibrillation Patients on Warfarin and Their Transition to Direct Oral Anticoagulants. Crit. Pathways Cardiol. A J. Evid.-Based Med. 2020, 20, 103–107. [Google Scholar] [CrossRef] [PubMed]
- Shen, N.-N.; Wu, Y.; Wang, N.; Kong, L.-C.; Zhang, C.; Wang, J.-L.; Gu, Z.-C.; Chen, J. Direct Oral Anticoagulants vs. Vitamin-K Antagonists in the Elderly With Atrial Fibrillation: A Systematic Review Comparing Benefits and Harms Between Observational Studies and Randomized Controlled Trials. Front. Cardiovasc. Med. 2020, 7, 132. [Google Scholar] [CrossRef]
- Silverio, A.; Di Maio, M.; Prota, C.; De Angelis, E.; Radano, I.; Citro, R.; Carrizzo, A.; Ciccarelli, M.; Vecchione, C.; Capodanno, D.; et al. Safety and efficacy of non-vitamin K antagonist oral anticoagulants in elderly patients with atrial fibrillation: Systematic review and meta-analysis of 22 studies and 440 281 patients. Eur. Heart J.-Cardiovasc. Pharmacother. 2019, 7, f20–f29. [Google Scholar] [CrossRef]
- Lafarge, L.; Khayi, F.; Bel-Kamel, A.; Charhon, N.; Sarfati, L.; Falquet, B.; Ducher, M.; Bourguignon, L. Time in therapeutic range of oral Vitamin K antagonists in hospitalized elderly patients. Drugs Aging 2018, 35, 569–574. [Google Scholar] [CrossRef] [PubMed]
- Hernandez, I.; He, M.; Brooks, M.M.; Saba, S.; Gellad, W.F. Adherence to Anticoagulation and Risk of Stroke Among Medicare Beneficiaries Newly Diagnosed with Atrial Fibrillation. Am. J. Cardiovasc. Drugs 2019, 20, 199–207. [Google Scholar] [CrossRef] [PubMed]
- Monelli, M.; Molteni, M.; Cassetti, G.; Bagnara, L.; De Grazia, V.; Zingale, L.; Zilli, F.; Bussotti, M.; Totaro, P.; De Maria, B.; et al. Non-vitamin K oral anticoagulant use in the elderly: A prospective real-world study—Data from the REGIstry of patients on Non-vitamin K oral Anticoagulants (REGINA). Vasc. Health Risk Manag. 2019, 15, 19–25. [Google Scholar] [CrossRef]
- Kimachi, M.; Furukawa, T.A.; Kimachi, K.; Goto, Y.; Fukuma, S.; Fukuhara, S. Direct oral anticoagulants versus warfarin for preventing stroke and systemic embolic events among atrial fibrillation patients with chronic kidney disease. Cochrane Database Syst. Rev. 2017, 2017, CD011373. [Google Scholar] [CrossRef]
| Overall Population (N = 641) | NOAC (N = 596) | VKA (N = 45) | p | |
|---|---|---|---|---|
| Age, years | 85 (82–87) | 85 (82–87) | 86 (82–88) | 0.384 |
| Male sex, N (%) | 275 (42.9) | 259 (43.5) | 16 (35.6) | 0.302 |
| Weight, kg | 71.0 ± 12.4 | 71.1 ± 12.4 | 68.5 ± 12.2 | 0.167 |
| Height, cm | 164.7 ± 77.1 | 164.8 ± 8.7 | 164.0 ± 10.0 | 0.557 |
| BMI, kg/m2 | 25.5 ± 3.7 | 25.5 ± 3.7 | 24.8 ± 3.2 | 0.209 |
| SAP, mmHg | 140 (130–154) | 140 (130–154) | 135 (125–155) | 0.493 |
| DAP, mmHg | 80 (75–90) | 85 (75–90) | 80 (70–80) | <0.001 |
| Diabetes, N (%) | 200 (31.2) | 191 (32.0) | 9 (20.0) | 0.093 |
| Dyslipidemia, N (%) | 258 (40.2) | 239 (40.1) | 19 (42.2) | 0.780 |
| Smoking status, N (%) | ||||
| Never | 447 (69.7) | 412 (69.1) | 35 (77.8) | 0.049 |
| Previous | 123 (19.2) | 113 (19.0) | 10 (22.2) | |
| Active | 71 (11.1) | 71 (11.9) | 0 | |
| Paroxysmal AF, N (%) | 96 (15.0) | 93 (15.6) | 3 (6.7) | 0.268 |
| Persistent AF, N (%) | 41 (6.4) | 38 (6.4) | 3 (6.7) | |
| Permanent AF, N (%) | 504 (78.6) | 465 (78.0) | 39 (86.7) | |
| CAD, N (%) | 181 (28.2) | 171 (28.7) | 10 (22.2) | 0.353 |
| HF, N (%) | 198 (30.9) | 188 (31.5) | 10 (22.2) | 0.192 |
| LVEF, N (%) | ||||
| ≥50% | 468 (73.0) | 439 (73.7) | 29 (64.4) | 0.406 |
| 40–49% | 140 (21.8) | 127 (21.3) | 13 (28.9) | |
| <40% | 33 (5.1) | 30 (5.0) | 3 (6.7) | |
| Prior stroke/TIA, N (%) | 91 (14.2) | 77 (12.9) | 14 (31.1) | <0.001 |
| PAD, N (%) | 123 (19.2) | 115 (19.3) | 8 (17.8) | 0.803 |
| eGFR, mL/min | 50.0 (41.5–66.0) | 51 (42–67) | 45 (39–55) | 0.003 |
| Liver disease, N (%) | 7 (1.1) | 6 (1.0) | 1 (2.2) | 0.449 |
| Concomitant medications | ||||
| Non-dihydropyridine CCB, N (%) | 58 (9.0) | 54 (9.1) | 4 (8.9) | 0.969 |
| Antiarrhythmic drugs, N (%) | 101 (15.8) | 90 (15.1) | 11 (24.4) | 0.097 |
| ACEi, N (%) | 280 (43.7) | 265 (44.5) | 15 (33.3) | 0.147 |
| Beta-blockers, N (%) | 481 (75.0) | 451 (75.7) | 30 (66.7) | 0.178 |
| Sartans, N (%) | 156 (24.3) | 140 (23.5) | 16 (35.6) | 0.069 |
| Ranolazine, N (%) | 16 (2.5) | 16 (2.7) | 0 | 0.266 |
| Statins, N (%) | 312 (48.7) | 296 (49.7) | 16 (35.6) | 0.068 |
| Prior bleeding, N (%) | 31 (4.8) | 28 (4.7) | 3 (6.7) | 0.553 |
| Chronic use of antiplatelet agents or NSAIDs, N (%) | 45 (7.0) | 39 (6.5) | 6 (13.3) | 0.086 |
| Overall Population (N = 641) | NOAC (N = 596) | VKA (N = 45) | p | |
|---|---|---|---|---|
| Duration of OAT since initiation, months | 36 (17–45) | 36 (17–42) | 36 (13–81) | 0.189 |
| History of anemia during OAT, N (%) | 36 (5.6) | 34 (5.7) | 2 (4.4) | 0.723 |
| History of GI bleeding during OAT, N (%) | 16 (2.5) | 14 (2.3) | 2 (4.4) | 0.385 |
| History of major bleeding during OAT, N (%) | 13 (2.0) | 12 (2.0) | 1 (2.2) | 0.924 |
| History of minor bleeding during OAT, N (%) | 43 (6.7) | 38 (6.4) | 5 (11.1) | 0.221 |
| History of severe thrombocytopenia during OAT, N (%) | 2 (0.3) | 2 (0.3) | 0 | 0.697 |
| History of stroke during OAT, N (%) | 6 (0.9) | 1 (0.2) | 5 (11.1) | <0.001 |
| History of TIA during OAT, N (%) | 16 (2.5) | 11 (1.8) | 5 (11.1) | <0.001 |
| History of ACS during OAT, N (%) | 17 (2.7) | 13 (2.2) | 4 (8.9) | 0.007 |
| Overall Population (N = 641) | NOAC (N = 596) | VKA (N = 45) | p | |
|---|---|---|---|---|
| The patient is informed about drug–drug and food–drug interactions | 529 (82.5) | 492 (82.6) | 37 (82.2) | 0.189 |
| The patient reports significant side effects from OAT | 20 (3.1) | 16 (2.7) | 4 (8.9) | 0.021 |
| The patient reports ecchymosis | 68 (10.6) | 55 (9.2) | 13 (28.9) | <0.001 |
| The patient reports epistaxis | 17 (2.7) | 12 (2.0) | 5 (11.1) | <0.001 |
| The patient reports bleeding | 22 (3.4) | 20 (3.4) | 2 (4.4) | 0.699 |
| OAT initiation improved the patient’s quality of life | ||||
| No | 72 (11.2) | 62 (10.4) | 10 (22.2) | <0.001 |
| Low | 72 (11.2) | 60 (10.1) | 12 (26.7) | |
| Enough | 276 (43.1) | 260 (43.6) | 16 (35.6) | |
| Complete | 221 (34.5) | 214 (35.9) | 7 (15.6) | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
De Stefano, F.; Benassi, A.; Cappelletti, A.M.; Donatelli, F.; Regazzoli, D.; Tolaro, S.; Perego, F.; Silverio, A.; Scatteia, A.; Guarini, P.; et al. Current Use of Oral Anticoagulation Therapy in Elderly Patients with Atrial Fibrillation: Results from an Italian Multicenter Prospective Study—The ISNEP Study. J. Pers. Med. 2022, 12, 1419. https://doi.org/10.3390/jpm12091419
De Stefano F, Benassi A, Cappelletti AM, Donatelli F, Regazzoli D, Tolaro S, Perego F, Silverio A, Scatteia A, Guarini P, et al. Current Use of Oral Anticoagulation Therapy in Elderly Patients with Atrial Fibrillation: Results from an Italian Multicenter Prospective Study—The ISNEP Study. Journal of Personalized Medicine. 2022; 12(9):1419. https://doi.org/10.3390/jpm12091419
Chicago/Turabian StyleDe Stefano, Francesco, Alberto Benassi, Alberto Maria Cappelletti, Francesco Donatelli, Damiano Regazzoli, Salvatore Tolaro, Francesca Perego, Angelo Silverio, Alessandra Scatteia, Pasquale Guarini, and et al. 2022. "Current Use of Oral Anticoagulation Therapy in Elderly Patients with Atrial Fibrillation: Results from an Italian Multicenter Prospective Study—The ISNEP Study" Journal of Personalized Medicine 12, no. 9: 1419. https://doi.org/10.3390/jpm12091419
APA StyleDe Stefano, F., Benassi, A., Cappelletti, A. M., Donatelli, F., Regazzoli, D., Tolaro, S., Perego, F., Silverio, A., Scatteia, A., Guarini, P., Dellegrottaglie, S., Mariani, S., Pezzella, E., Galasso, G., Caiazza, F., & on behalf of ISNEP Investigators. (2022). Current Use of Oral Anticoagulation Therapy in Elderly Patients with Atrial Fibrillation: Results from an Italian Multicenter Prospective Study—The ISNEP Study. Journal of Personalized Medicine, 12(9), 1419. https://doi.org/10.3390/jpm12091419







