Functional Magnetic Resonance Imaging in the Final Stage of Creutzfeldt-Jakob Disease
Abstract
1. Introduction
2. Case Report
2.1. Clinical Course and Ancillary Findings
2.2. Coma Scale and fMRI
2.3. Anesthesiological Preparations and Procedures
2.4. MRI Parameters
3. Discussion
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Zerr, I.; Parchi, P. Sporadic Creutzfeldt-Jakob disease. Handb. Clin. Neurol. 2018, 153, 155–174. [Google Scholar] [CrossRef] [PubMed]
- Nakatani, E.; Kanatani, Y.; Kaneda, H.; Nagai, Y.; Teramukai, S.; Nishimura, T.; Zhou, B.; Kojima, S.; Kono, H.; Fukushima, M.; et al. Specific clinical signs and symptoms are predictive of clinical course in sporadic Creutzfeldt-Jakob disease. Eur. J. Neurol. 2016, 23, 1455–1462. [Google Scholar] [CrossRef] [PubMed]
- Kondziella, D.; Bender, A.; Diserens, K.; van Erp, W.; Estraneo, A.; Formisano, R.; Laureys, S.; Naccache, L.; Ozturk, S.; Rohaut, B.; et al. European Academy of Neurology guideline on the diagnosis of coma and other disorders of consciousness. Eur. J. Neurol. 2020. [Google Scholar] [CrossRef] [PubMed]
- Edlow, B.L.; Giacino, J.T.; Wu, O. Functional MRI and outcome in traumatic coma. Curr. Neurol. Neurosci. Rep. 2013, 13, 375. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Luo, L.; Zhou, Z.; Xu, K.; Zhang, L.; Liu, X.; Tan, X.; Zhang, J.; Ye, X.; Gao, J.; et al. Functional Connectivity of Anterior Insula Predicts Recovery of Patients With Disorders of Consciousness. Front. Neurol. 2018, 9, 1024. [Google Scholar] [CrossRef] [PubMed]
- Di Perri, C.; Bahri, M.A.; Amico, E.; Thibaut, A.; Heine, L.; Antonopoulos, G.; Charland-Verville, V.; Wannez, S.; Gomez, F.; Hustinx, R.; et al. Neural correlates of consciousness in patients who have emerged from a minimally conscious state: A cross-sectional multimodal imaging study. Lancet Neurol. 2016, 15, 830–842. [Google Scholar] [CrossRef]
- In, C.B.; Choi, Y.S.; Park, E.Y.; Chang, D.J.; Lee, S.K.; Choi, H.; Moon, H.S. Anesthetic management in patients suspected of Creutzfeldt-Jakob disease -A case report. Korean J. Anesthesiol. 2011, 61, 262–264. [Google Scholar] [CrossRef] [PubMed]
- Martuzzi, R.; Ramani, R.; Qiu, M.; Rajeevan, N.; Constable, R.T. Functional connectivity and alterations in baseline brain state in humans. NeuroImage 2010, 49, 823–834. [Google Scholar] [CrossRef] [PubMed]
- Golaszewski, S.M.; Siedentopf, C.M.; Baldauf, E.; Koppelstaetter, F.; Eisner, W.; Unterrainer, J.; Guendisch, G.M.; Mottaghy, F.M.; Felber, S.R. Functional magnetic resonance imaging of the human sensorimotor cortex using a novel vibrotactile stimulator. NeuroImage 2002, 17, 421–430. [Google Scholar] [CrossRef] [PubMed]
- Golaszewski, S.M.; Zschiegner, F.; Siedentopf, C.M.; Unterrainer, J.; Sweeney, R.A.; Eisner, W.; Lechner-Steinleitner, S.; Mottaghy, F.M.; Felber, S. A new pneumatic vibrator for functional magnetic resonance imaging of the human sensorimotor cortex. Neuroscience letters 2002, 324, 125–128. [Google Scholar] [CrossRef]
- Gallasch, E.; Golaszewski, S.M.; Fend, M.; Siedentopf, C.M.; Koppelstaetter, F.; Eisner, W.; Gerstenbrand, F.; Felber, S.R. Contact force- and amplitude-controllable vibrating probe for somatosensory mapping of plantar afferences with fMRI. J. Magn. Reson. Imaging JMRI 2006, 24, 1177–1182. [Google Scholar] [CrossRef] [PubMed]
- Marino, S.; Bonanno, L.; Giorgio, A. Functional connectivity in disorders of consciousness: Methodological aspects and clinical relevance. Brain Imaging Behav. 2016, 10, 604–608. [Google Scholar] [CrossRef] [PubMed]
- Renard, D.; Castelnovo, G.; Collombier, L.; Thouvenot, E.; Boudousq, V. FDG-PET in Creutzfeldt-Jakob disease: Analysis of clinical-PET correlation. Prion 2017, 11, 440–453. [Google Scholar] [CrossRef] [PubMed]
- Iwasaki, Y. Creutzfeldt-Jakob disease. Neuropathology 2017, 37, 174–188. [Google Scholar] [CrossRef] [PubMed]
- Hudetz, A.G.; Mashour, G.A. Disconnecting Consciousness: Is There a Common Anesthetic End Point? Anesth. Analg. 2016, 123, 1228–1240. [Google Scholar] [CrossRef] [PubMed]
- Alkire, M.T.; Hudetz, A.G.; Tononi, G. Consciousness and anesthesia. Science 2008, 322, 876–880. [Google Scholar] [CrossRef] [PubMed]
- Hudetz, A.G. Suppressing Consciousness: Mechanisms of general anesthesia. Sem. Anesth. Periop. Med. Pain 2006, 25, 196–204. [Google Scholar] [CrossRef]
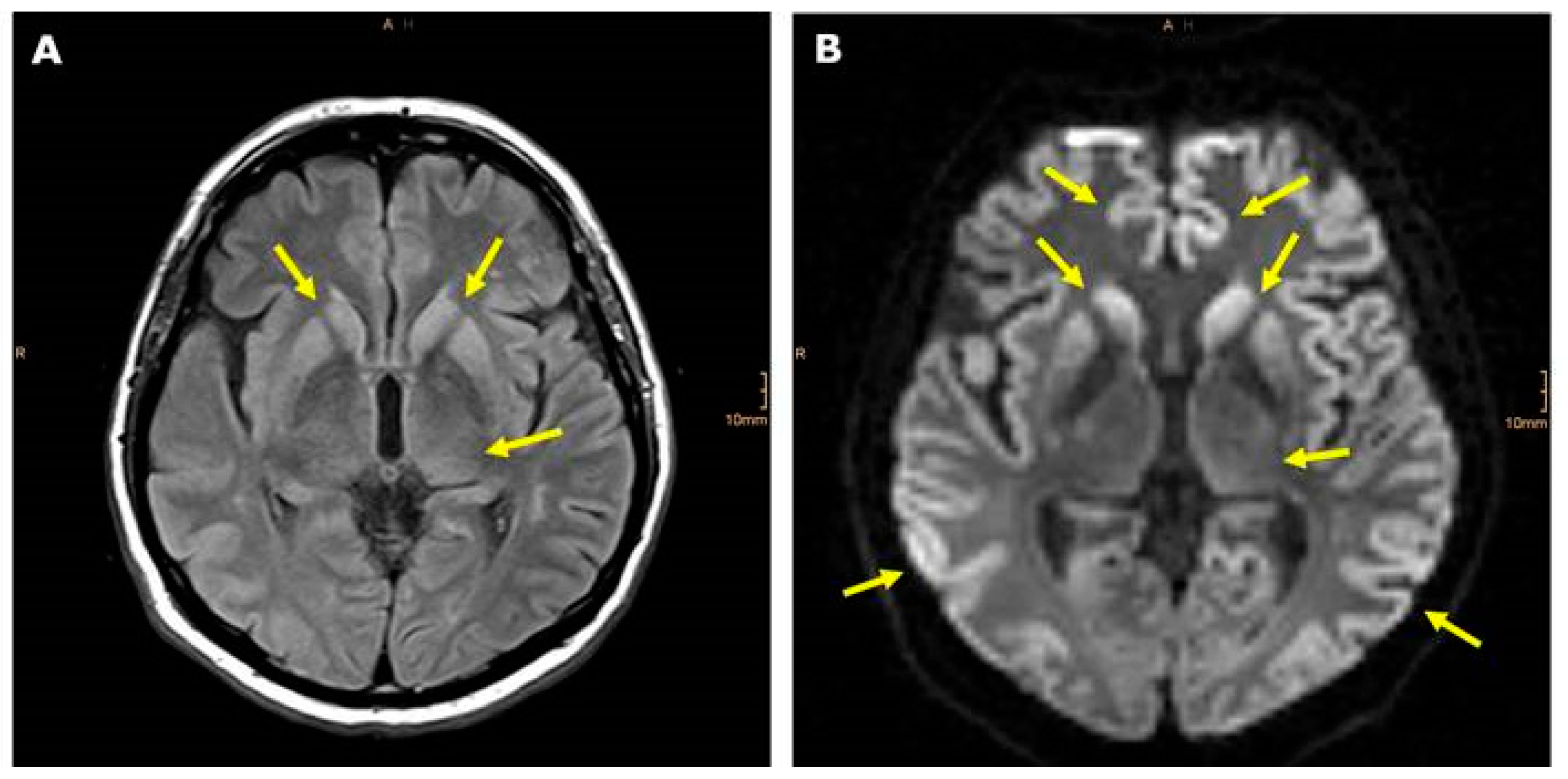
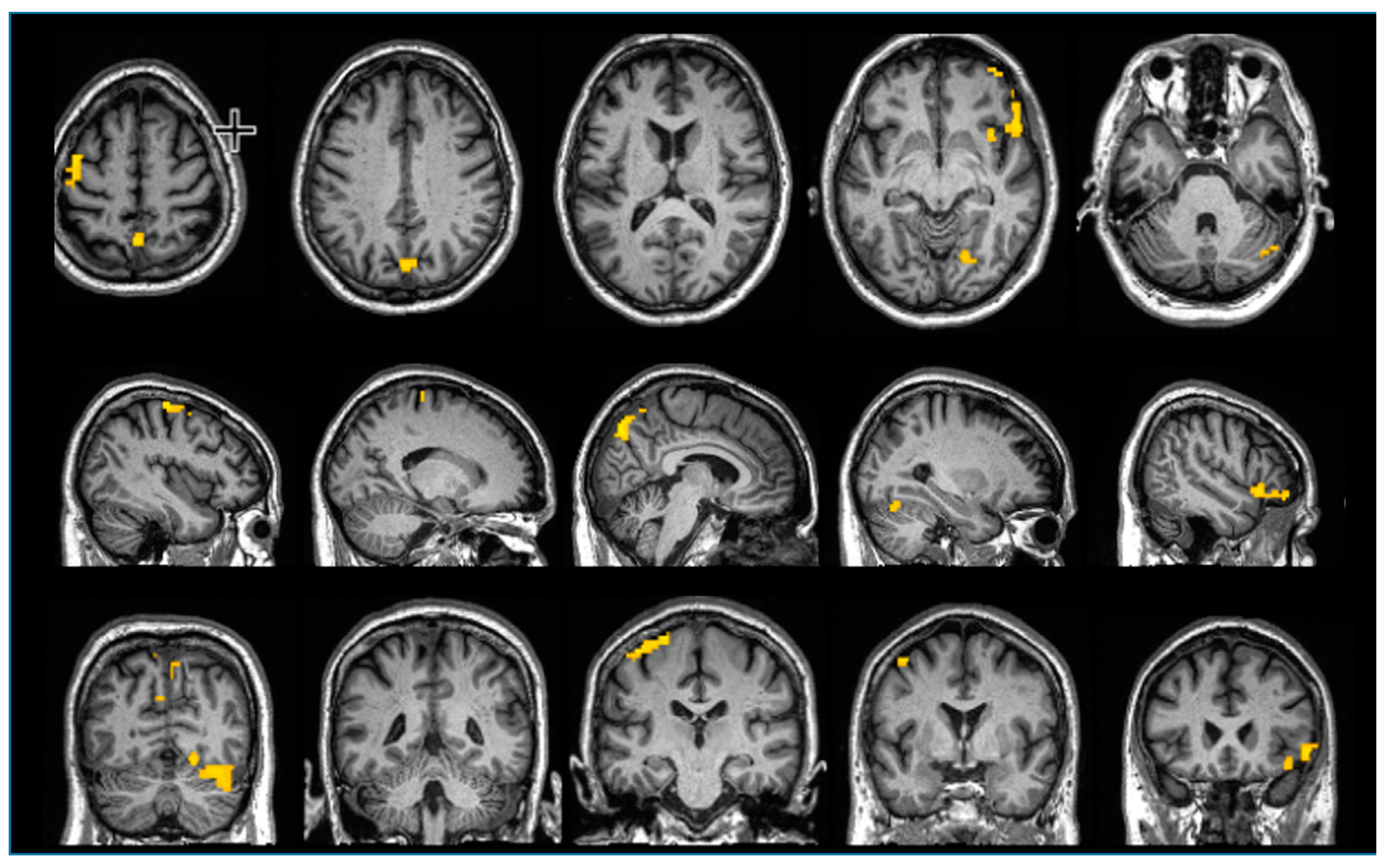
| Brain Region | Spongiform Changes | Prion IHC | Neuronal Loss | Astrogliosis | Microgliosis |
|---|---|---|---|---|---|
| Frontal cortex | ++ | + | ++ | +++ | +++ |
| Hippocampus | - | - | ++ | ++ | ++ |
| Temporal cortex | + | + | ++ | ++ | ++ |
| Parietal cortex | + | + | + | ++ | ++ |
| Occipital cortex | ++ | + | ++ | +++ | +++ |
| Basal ganglia | + | + | + | ++ | ++ |
| Thalamus | + | - | + | ++ | ++ |
| Cerebellum | + | + | + | + | + |
| Substantia nigra | - | - | - | + | + |
| Pons | - | - | + | + | + |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Golaszewski, S.M.; Wutzl, B.; Unterrainer, A.F.; Florea, C.; Schwenker, K.; Frey, V.N.; Kronbichler, M.; Rattay, F.; Nardone, R.; Hauer, L.; et al. Functional Magnetic Resonance Imaging in the Final Stage of Creutzfeldt-Jakob Disease. Diagnostics 2020, 10, 309. https://doi.org/10.3390/diagnostics10050309
Golaszewski SM, Wutzl B, Unterrainer AF, Florea C, Schwenker K, Frey VN, Kronbichler M, Rattay F, Nardone R, Hauer L, et al. Functional Magnetic Resonance Imaging in the Final Stage of Creutzfeldt-Jakob Disease. Diagnostics. 2020; 10(5):309. https://doi.org/10.3390/diagnostics10050309
Chicago/Turabian StyleGolaszewski, Stefan M., Bettina Wutzl, Axel F. Unterrainer, Cristina Florea, Kerstin Schwenker, Vanessa N. Frey, Martin Kronbichler, Frank Rattay, Raffaele Nardone, Larissa Hauer, and et al. 2020. "Functional Magnetic Resonance Imaging in the Final Stage of Creutzfeldt-Jakob Disease" Diagnostics 10, no. 5: 309. https://doi.org/10.3390/diagnostics10050309
APA StyleGolaszewski, S. M., Wutzl, B., Unterrainer, A. F., Florea, C., Schwenker, K., Frey, V. N., Kronbichler, M., Rattay, F., Nardone, R., Hauer, L., Sellner, J., & Trinka, E. (2020). Functional Magnetic Resonance Imaging in the Final Stage of Creutzfeldt-Jakob Disease. Diagnostics, 10(5), 309. https://doi.org/10.3390/diagnostics10050309






