Plasma Proteins and Platelets Modulate Neutrophil Clearance of Malaria-Related Hemozoin Crystals
Abstract
1. Introduction
2. Material and Methods
2.1. Isolation of Human Blood Neutrophils
2.2. Fluorescence Microscopy of Hemozoin Uptake
2.3. Uptake of Hemozoin in Neutrophils Using Flow Cytometry
2.4. Preparation and Stimulation of Neutrophils with Platelet-Poor Plasma
2.5. Morphological and Ultrastructural Analysis by Electron Microscopy
2.6. Statistical Analysis
3. Results
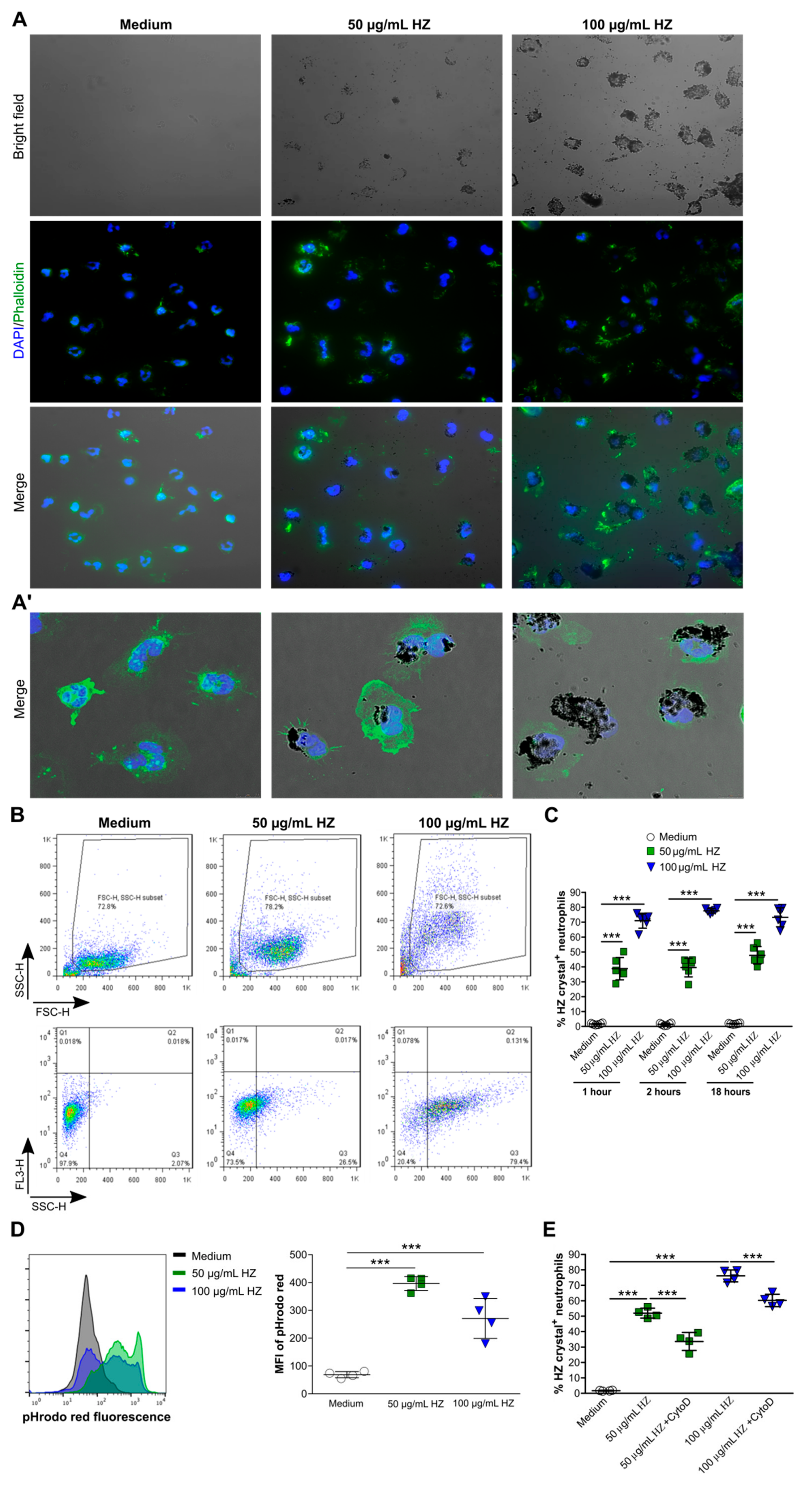
3.1. Neutrophils Took up Hemozoin Crystals under Serum/Plasma-Free Condition
3.2. Hemozoin Uptake Caused Nuclei Enlargement and Vesicle Formation but not NET Release
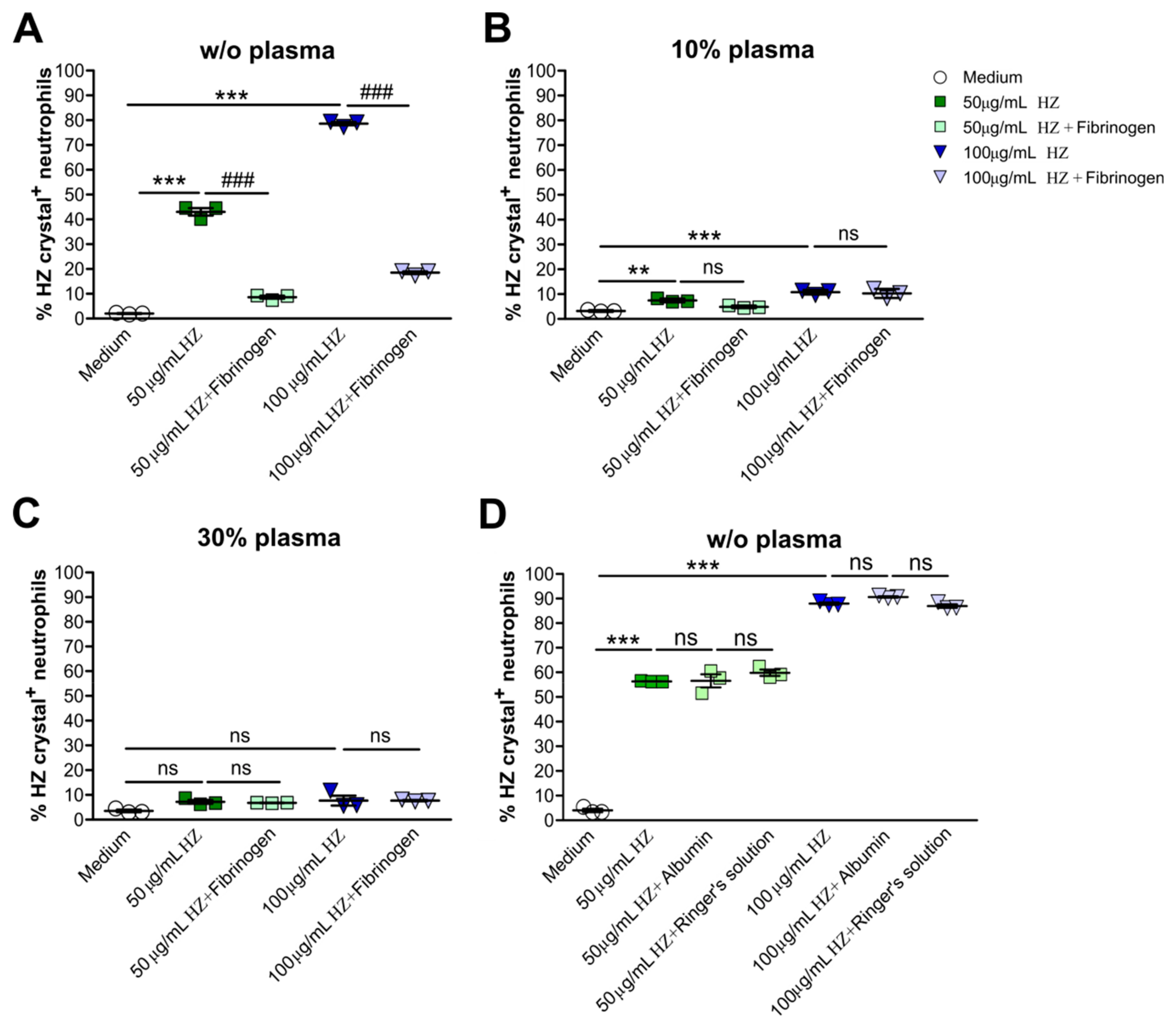
3.3. Human Plasma Impaired Hemozoin Uptake in Neutrophils
3.4. Fibrinogen Altered the Uptake of Hemozoin by Human Neutrophils
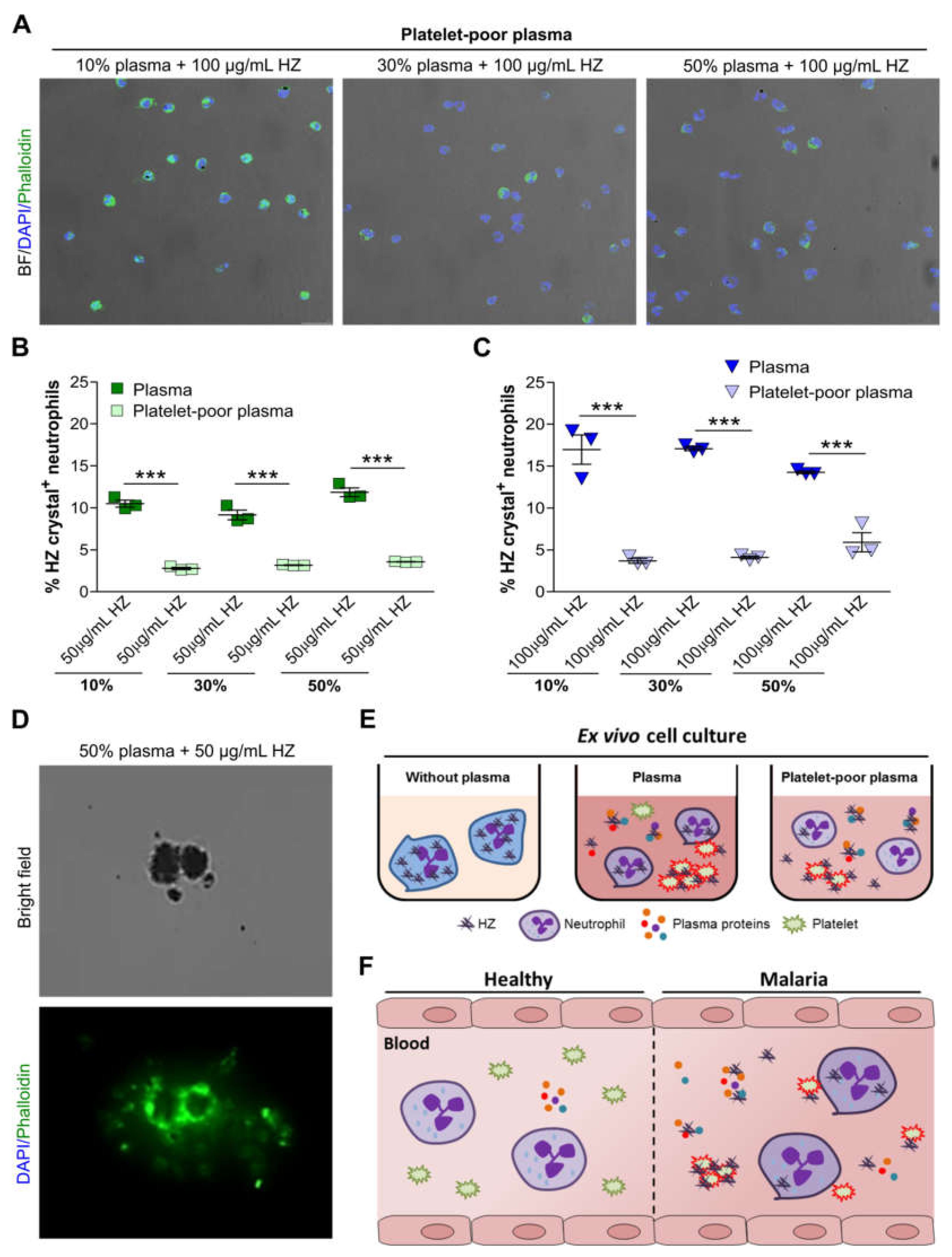
3.5. Removal of Platelets from Plasma Further Impaired HZ Uptake by Human Neutrophils
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- World Health Organization. World Malaria Report 2018. Available online: https://www.who.int/malaria/publications/world-malaria-report-2018/en/ (accessed on 28 November 2019).
- Coronado, L.M.; Nadovich, C.T.; Spadafora, C. Malarial hemozoin: From target to tool. Biochim. Biophys. Acta 2014, 1840, 2032–2041. [Google Scholar] [CrossRef]
- Polimeni, M.; Valente, E.; Ulliers, D.; Opdenakker, G.; Van den Steen, P.E.; Giribaldi, G.; Prato, M. Natural haemozoin induces expression and release of human monocyte tissue inhibitor of metalloproteinase-1. PLoS ONE 2013, 8, e71468. [Google Scholar] [CrossRef] [PubMed]
- Shio, M.T.; Eisenbarth, S.C.; Savaria, M.; Vinet, A.F.; Bellemare, M.J.; Harder, K.W.; Sutterwala, F.S.; Bohle, D.S.; Descoteaux, A.; Flavell, R.A.; et al. Malarial hemozoin activates the NLRP3 inflammasome through Lyn and Syk kinases. PLoS Pathog. 2009, 5, e1000559. [Google Scholar] [CrossRef]
- Gazzinelli, R.T.; Kalantari, P.; Fitzgerald, K.A.; Golenbock, D.T. Innate sensing of malaria parasites. Nat. Rev. Immunol. 2014, 14, 744–757. [Google Scholar] [CrossRef] [PubMed]
- Oakley, M.S.; Gerald, N.; McCutchan, T.F.; Aravind, L.; Kumar, S. Clinical and molecular aspects of malaria fever. Trends Parasitol. 2011, 27, 442–449. [Google Scholar] [CrossRef]
- Amulic, B.; Cazalet, C.; Hayes, G.L.; Metzler, K.D.; Zychlinsky, A. Neutrophil function, From mechanisms to disease. Annu. Rev. Immunol. 2012, 30, 459–489. [Google Scholar] [CrossRef]
- Wickramasinghe, S.N.; Phillips, R.E.; Looareesuwan, S.; Warrell, D.A.; Hughes, M. The bone marrow in human cerebral malaria, Parasite sequestration within sinusoids. Br. J. Haematol. 1987, 66, 295–306. [Google Scholar] [CrossRef]
- Leoratti, F.M.; Trevelin, S.C.; Cunha, F.Q.; Rocha, B.C.; Costa, P.A.; Gravina, H.D.; Tada, M.S.; Pereira, D.B.; Golenbock, D.T.; Antonelli, L.R.; et al. Neutrophil paralysis in Plasmodium vivax malaria. PLoS Negl. Trop. Dis. 2012, 6, e1710. [Google Scholar] [CrossRef]
- Mohammed, A.O.; Elghazali, G.; Mohammed, H.B.; Elbashir, M.I.; Xu, S.; Berzins, K.; Venge, P. Human neutrophil lipocalin, A specific marker for neutrophil activation in severe Plasmodium falciparum malaria. Acta Trop. 2003, 87, 279–285. [Google Scholar] [CrossRef]
- Boeltz, S.; Munoz, L.E.; Fuchs, T.A.; Herrmann, M. Neutrophil Extracellular Traps Open the Pandora’s Box in Severe Malaria. Front. Immunol. 2017, 8, 874. [Google Scholar] [CrossRef]
- Baker, V.S.; Imade, G.E.; Molta, N.B.; Tawde, P.; Pam, S.D.; Obadofin, M.O.; Sagay, S.A.; Egah, D.Z.; Iya, D.; Afolabi, B.B.; et al. Cytokine-associated neutrophil extracellular traps and antinuclear antibodies in Plasmodium falciparum infected children under six years of age. Malar. J. 2008, 7, 41. [Google Scholar] [CrossRef] [PubMed]
- Kho, S.; Minigo, G.; Andries, B.; Leonardo, L.; Prayoga, P.; Poespoprodjo, J.R.; Kenangalem, E.; Price, R.N.; Woodberry, T.; Anstey, N.M.; et al. Circulating Neutrophil Extracellular Traps and Neutrophil Activation Are Increased in Proportion to Disease Severity in Human Malaria. J. Infect. Dis. 2019, 219, 1994–2004. [Google Scholar] [CrossRef] [PubMed]
- Knackstedt, S.L.; Georgiadou, A.; Apel, F.; Abu-Abed, U.; Moxon, C.A.; Cunnington, A.J.; Raupach, B.; Cunningham, D.; Langhorne, J.; Kruger, R.; et al. Neutrophil extracellular traps drive inflammatory pathogenesis in malaria. Sci. Immunol. 2019, 4, eaaw0336. [Google Scholar] [CrossRef] [PubMed]
- Lyke, K.E.; Diallo, D.A.; Dicko, A.; Kone, A.; Coulibaly, D.; Guindo, A.; Cissoko, Y.; Sangare, L.; Coulibaly, S.; Dakouo, B.; et al. Association of intraleukocytic Plasmodium falciparum malaria pigment with disease severity, clinical manifestations, and prognosis in severe malaria. Am. J. Trop. Med. Hyg. 2003, 69, 253–259. [Google Scholar] [CrossRef]
- Kassa, F.A.; Shio, M.T.; Bellemare, M.J.; Faye, B.; Ndao, M.; Olivier, M. New inflammation-related biomarkers during malaria infection. PLoS ONE 2011, 6, e26495. [Google Scholar] [CrossRef]
- Barrera, V.; Skorokhod, O.A.; Baci, D.; Gremo, G.; Arese, P.; Schwarzer, E. Host fibrinogen stably bound to hemozoin rapidly activates monocytes via TLR-4 and CD11b/CD18-integrin, A new paradigm of hemozoin action. Blood 2011, 117, 5674–5682. [Google Scholar] [CrossRef]
- Nakazawa, D.; Kumar, S.V.; Marschner, J.; Desai, J.; Holderied, A.; Rath, L.; Kraft, F.; Lei, Y.; Fukasawa, Y.; Moeckel, G.W.; et al. Histones and Neutrophil Extracellular Traps Enhance Tubular Necrosis and Remote Organ Injury in Ischemic AKI. J. Am. Soc. Nephrol. 2017, 28, 1753–1768. [Google Scholar] [CrossRef]
- Desai, J.; Foresto-Neto, O.; Honarpisheh, M.; Steiger, S.; Nakazawa, D.; Popper, B.; Buhl, E.M.; Boor, P.; Mulay, S.R.; Anders, H.J. Particles of different sizes and shapes induce neutrophil necroptosis followed by the release of neutrophil extracellular trap-like chromatin. Sci. Rep. 2017, 7, 15003. [Google Scholar] [CrossRef]
- Honarpisheh, M.; Foresto-Neto, O.; Desai, J.; Steiger, S.; Gomez, L.A.; Popper, B.; Boor, P.; Anders, H.J.; Mulay, S.R. Phagocytosis of environmental or metabolic crystalline particles induces cytotoxicity by triggering necroptosis across a broad range of particle size and shape. Sci. Rep. 2017, 7, 15523. [Google Scholar] [CrossRef]
- Omoigberale, A.I.; Abiodun, P.O.; Famodu, A.A. Fibrinolytic activity in children with Plasmodium falciparum malaria. East Afr. Med. J. 2005, 82, 103–105. [Google Scholar] [CrossRef]
- Munoz, L.E.; Bilyy, R.; Biermann, M.H.; Kienhofer, D.; Maueroder, C.; Hahn, J.; Brauner, J.M.; Weidner, D.; Chen, J.; Scharin-Mehlmann, M.; et al. Nanoparticles size-dependently initiate self-limiting NETosis-driven inflammation. Proc. Natl. Acad. Sci. USA 2016, 113, E5856–E5865. [Google Scholar] [CrossRef]
- Schwarzer, E.; Bellomo, G.; Giribaldi, G.; Ulliers, D.; Arese, P. Phagocytosis of malarial pigment haemozoin by human monocytes, A confocal microscopy study. Parasitology 2001, 123, 125–131. [Google Scholar] [CrossRef]
- Schwarzer, E.; De Matteis, F.; Giribaldi, G.; Ulliers, D.; Valente, E.; Arese, P. Hemozoin stability and dormant induction of heme oxygenase in hemozoin-fed human monocytes. Mol. Biochem. Parasitol. 1999, 100, 61–72. [Google Scholar] [CrossRef]
- Schwarzer, E.; Turrini, F.; Ulliers, D.; Giribaldi, G.; Ginsburg, H.; Arese, P. Impairment of macrophage functions after ingestion of Plasmodium falciparum-infected erythrocytes or isolated malarial pigment. J. Exp. Med. 1992, 176, 1033–1041. [Google Scholar] [CrossRef] [PubMed]
- Dasari, P.; Reiss, K.; Lingelbach, K.; Baumeister, S.; Lucius, R.; Udomsangpetch, R.; Bhakdi, S.C.; Bhakdi, S. Digestive vacuoles of Plasmodium falciparum are selectively phagocytosed by and impair killing function of polymorphonuclear leukocytes. Blood 2011, 118, 4946–4956. [Google Scholar] [CrossRef] [PubMed]
- Tyberghein, A.; Deroost, K.; Schwarzer, E.; Arese, P.; Van den Steen, P.E. Immunopathological effects of malaria pigment or hemozoin and other crystals. Biofactors 2014, 40, 59–78. [Google Scholar] [CrossRef] [PubMed]
- Cunnington, A.J.; de Souza, J.B.; Walther, M.; Riley, E.M. Malaria impairs resistance to Salmonella through heme- and heme oxygenase-dependent dysfunctional granulocyte mobilization. Nat. Med. 2011, 18, 120–127. [Google Scholar] [CrossRef]
- Vieira, O.V.; Botelho, R.J.; Grinstein, S. Phagosome maturation, Aging gracefully. Biochem. J. 2002, 366, 689–704. [Google Scholar] [CrossRef]
- Olliaro, P.; Lombardi, L.; Frigerio, S.; Basilico, N.; Taramelli, D.; Monti, D. Phagocytosis of hemozoin (native and synthetic malaria pigment), and Plasmodium falciparum intraerythrocyte-stage parasites by human and mouse phagocytes. Ultrastruct. Pathol. 2000, 24, 9–13. [Google Scholar] [CrossRef][Green Version]
- Nordenfelt, P.; Tapper, H. Phagosome dynamics during phagocytosis by neutrophils. J. Leukoc. Biol. 2011, 90, 271–284. [Google Scholar] [CrossRef]
- Botelho, R.J.; Tapper, H.; Furuya, W.; Mojdami, D.; Grinstein, S. Fc gamma R-mediated phagocytosis stimulates localized pinocytosis in human neutrophils. J. Immunol. 2002, 169, 4423–4429. [Google Scholar] [CrossRef] [PubMed]
- Kuhn, D.A.; Vanhecke, D.; Michen, B.; Blank, F.; Gehr, P.; Petri-Fink, A.; Rothen-Rutishauser, B. Different endocytotic uptake mechanisms for nanoparticles in epithelial cells and macrophages. Beilstein J. Nanotechnol. 2014, 5, 1625–1636. [Google Scholar] [CrossRef] [PubMed]
- Rejman, J.; Oberle, V.; Zuhorn, I.S.; Hoekstra, D. Size-dependent internalization of particles via the pathways of clathrin- and caveolae-mediated endocytosis. Biochem. J. 2004, 377, 159–169. [Google Scholar] [CrossRef] [PubMed]
- Lisman, T. Platelet-neutrophil interactions as drivers of inflammatory and thrombotic disease. Cell Tissue Res. 2018, 371, 567–576. [Google Scholar] [CrossRef] [PubMed]
- O’Sullivan, J.M.; O’Donnell, J.S. Platelets in malaria pathogenesis. Blood 2018, 132, 1222–1224. [Google Scholar] [CrossRef] [PubMed]
- Von Hundelshausen, P.; Koenen, R.R.; Sack, M.; Mause, S.F.; Adriaens, W.; Proudfoot, A.E.; Hackeng, T.M.; Weber, C. Heterophilic interactions of platelet factor 4 and RANTES promote monocyte arrest on endothelium. Blood 2005, 105, 924–930. [Google Scholar] [CrossRef]
- Pervushina, O.; Scheuerer, B.; Reiling, N.; Behnke, L.; Schroder, J.M.; Kasper, B.; Brandt, E.; Bulfone-Paus, S.; Petersen, F. Platelet factor 4/CXCL4 induces phagocytosis and the generation of reactive oxygen metabolites in mononuclear phagocytes independently of Gi protein activation or intracellular calcium transients. J. Immunol. 2004, 173, 2060–2067. [Google Scholar] [CrossRef]
- Assinger, A.; Laky, M.; Schabbauer, G.; Hirschl, A.M.; Buchberger, E.; Binder, B.R.; Volf, I. Efficient phagocytosis of periodontopathogens by neutrophils requires plasma factors, platelets and TLR2. J. Thromb. Haemost. 2011, 9, 799–809. [Google Scholar] [CrossRef]
- Peters, M.J.; Dixon, G.; Kotowicz, K.T.; Hatch, D.J.; Heyderman, R.S.; Klein, N.J. Circulating platelet-neutrophil complexes represent a subpopulation of activated neutrophils primed for adhesion, phagocytosis and intracellular killing. Br. J. Haematol. 1999, 106, 391–399. [Google Scholar] [CrossRef]
- Hurley, S.M.; Kahn, F.; Nordenfelt, P.; Morgelin, M.; Sorensen, O.E.; Shannon, O. Platelet-Dependent Neutrophil Function Is Dysregulated by M Protein from Streptococcus pyogenes. Infect. Immun. 2015, 83, 3515–3525. [Google Scholar] [CrossRef]
- Selak, M.A. Neutrophil elastase potentiates cathepsin G-induced platelet activation. Thromb. Haemost. 1992, 68, 570–576. [Google Scholar] [PubMed]
- Sambrano, G.R.; Huang, W.; Faruqi, T.; Mahrus, S.; Craik, C.; Coughlin, S.R. Cathepsin G activates protease-activated receptor-4 in human platelets. J. Biol. Chem. 2000, 275, 6819–6823. [Google Scholar] [CrossRef] [PubMed]
- Mihara, K.; Ramachandran, R.; Renaux, B.; Saifeddine, M.; Hollenberg, M.D. Neutrophil elastase and proteinase-3 trigger G protein-biased signaling through proteinase-activated receptor-1 (PAR1). J. Biol. Chem. 2013, 288, 32979–32990. [Google Scholar] [CrossRef] [PubMed]


© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lautenschlager, S.d.O.S.; Kim, T.; Bidóia, D.L.; Nakamura, C.V.; Anders, H.-J.; Steiger, S. Plasma Proteins and Platelets Modulate Neutrophil Clearance of Malaria-Related Hemozoin Crystals. Cells 2020, 9, 93. https://doi.org/10.3390/cells9010093
Lautenschlager SdOS, Kim T, Bidóia DL, Nakamura CV, Anders H-J, Steiger S. Plasma Proteins and Platelets Modulate Neutrophil Clearance of Malaria-Related Hemozoin Crystals. Cells. 2020; 9(1):93. https://doi.org/10.3390/cells9010093
Chicago/Turabian StyleLautenschlager, Sueli de Oliveira Silva, Tehyung Kim, Danielle Lazarim Bidóia, Celso Vataru Nakamura, Hans-Joachim Anders, and Stefanie Steiger. 2020. "Plasma Proteins and Platelets Modulate Neutrophil Clearance of Malaria-Related Hemozoin Crystals" Cells 9, no. 1: 93. https://doi.org/10.3390/cells9010093
APA StyleLautenschlager, S. d. O. S., Kim, T., Bidóia, D. L., Nakamura, C. V., Anders, H.-J., & Steiger, S. (2020). Plasma Proteins and Platelets Modulate Neutrophil Clearance of Malaria-Related Hemozoin Crystals. Cells, 9(1), 93. https://doi.org/10.3390/cells9010093






