Outcomes of Transarterial Embolisation (TAE) vs. Transarterial Chemoembolisation (TACE) for Hepatocellular Carcinoma: A Systematic Review and Meta-Analysis
Simple Summary
Abstract
1. Introduction
2. Methods
2.1. Search Strategy
2.2. Inclusion and Exclusion Criteria
2.3. Study Outcomes
2.4. Data Extraction
2.5. Assessment of Methodological Quality
2.6. Statistical Analysis
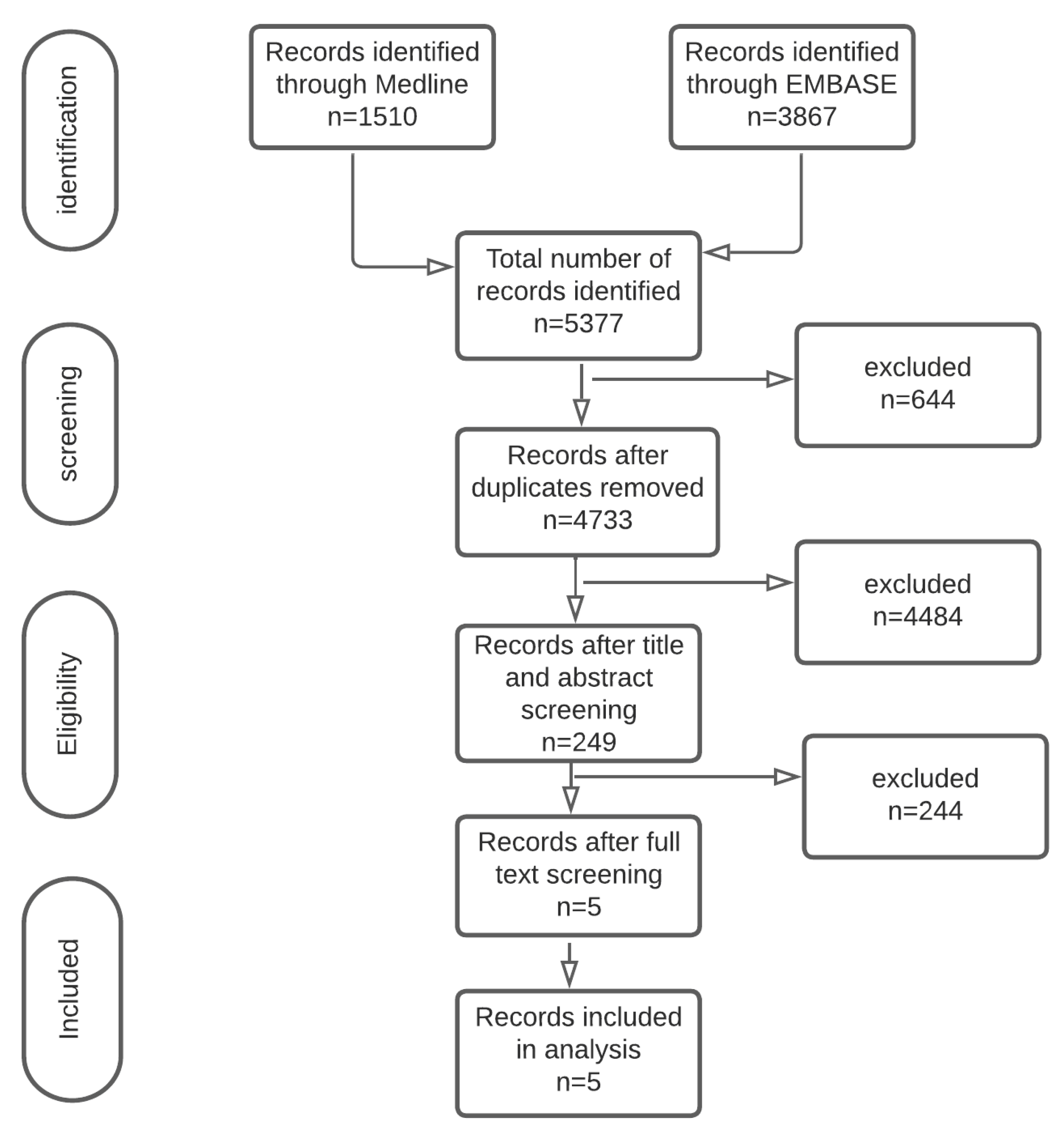
3. Results
Study Characteristics
4. Survival Outcomes
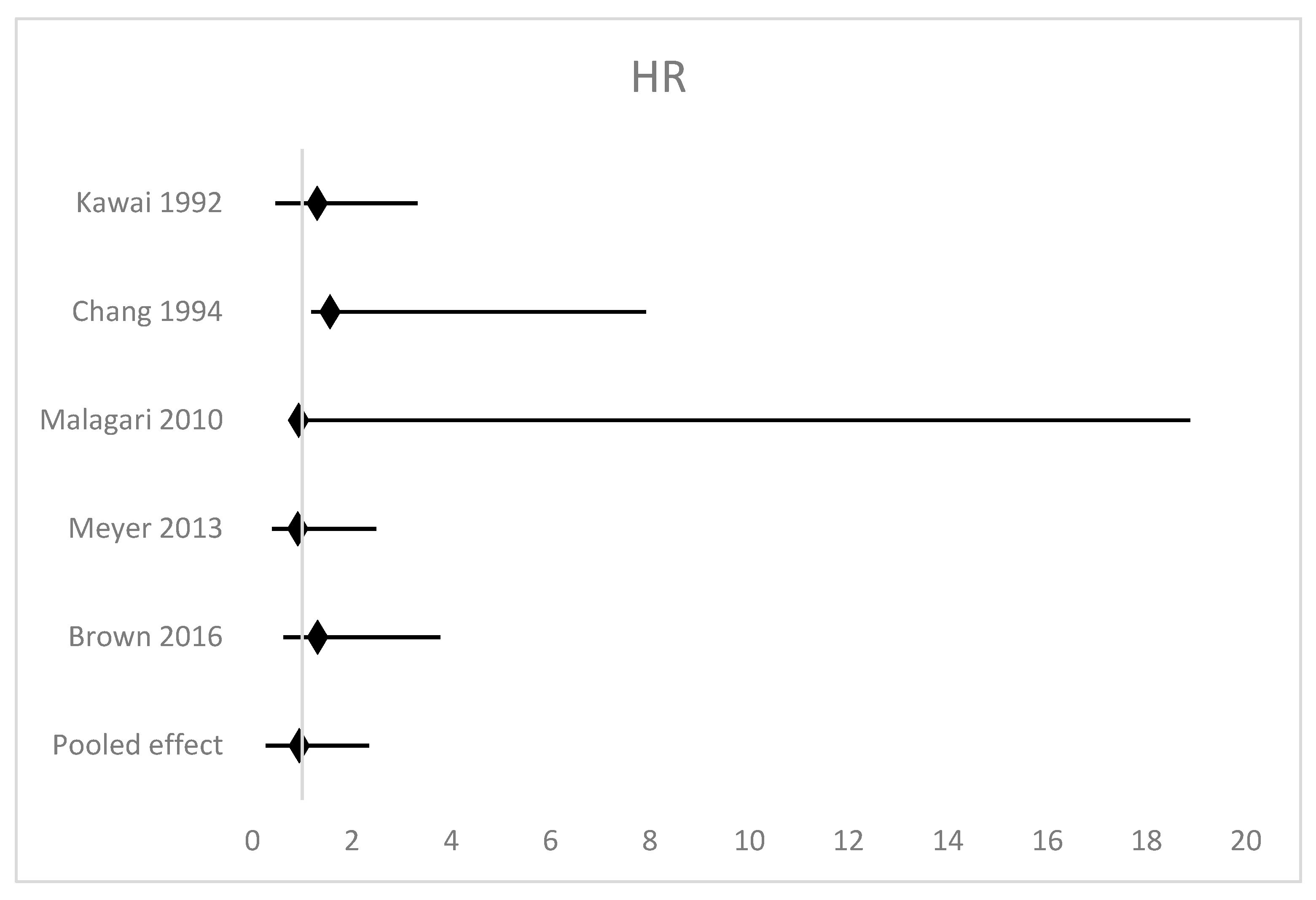
4.1. Overall Survival
4.2. Comparison by Number of Sessions
4.3. Progression-Free Survival
4.4. Comparison by Chemotherapeutic Agent
4.5. Adverse Events
4.6. Cholecystitis
4.7. Liver Abscess
4.8. Liver Failure
4.9. Abdominal Pain
4.10. Fever
5. Discussion
6. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Rawla, P.; Sunkara, T.; Muralidharan, P.; Raj, J.P. Update in global trends and aetiology of hepatocellular carcinoma. Contemp. Oncol. 2018, 22, 141–150. [Google Scholar] [CrossRef]
- Global Burden of Disease Liver Cancer Collaboration; Akinyemiju, T.; Abera, S.; Ahmed, M.; Alam, N.; Alemayohu, M.A.; Allen, C.; Al-Raddadi, R.; Alvis-Guzman, N.; Amoako, Y.; et al. The Burden of Primary Liver Cancer and Underlying Etiologies From 1990 to 2015 at the Global, Regional, and National Level: Results From the Global Burden of Disease Study 2015. JAMA Oncol. 2017, 3, 1683–1691. [Google Scholar] [CrossRef]
- Kamarajah, S.K.; Frankel, T.L.; Sonnenday, C.; Cho, C.S.; Nathan, H. Critical evaluation of the American Joint Commission on Cancer (AJCC) 8th edition staging system for patients with Hepatocellular Carcinoma (HCC): A Surveillance, Epidemiology, End Results (SEER) analysis. J. Surg. Oncol. 2018, 117, 644–650. [Google Scholar] [CrossRef]
- Kamarajah, S.K.; Bundred, J.R.; Littler, P.; Reeves, H.; Manas, D.M.; White, S.A. Treatment strategies for early stage hepatocellular carcinoma: A systematic review and network meta-analysis of randomised clinical trials. HPB 2021, 23, 495–505. [Google Scholar] [CrossRef]
- Qu, K.; Yan, Z.; Wu, Y.; Chen, Y.; Qu, P.; Xu, X.; Yuan, P.; Huang, X.; Xing, J.; Zhang, H.; et al. Transarterial chemoembolization aggravated peritumoral fibrosis via hypoxia-inducible factor-1alpha dependent pathway in hepatocellular carcinoma. J. Gastroenterol. Hepatol. 2015, 30, 925–932. [Google Scholar] [CrossRef]
- Tzao, C.; Lee, S.-C.; Tung, H.-J.; Hsu, H.-S.; Hsu, W.-H.; Sun, G.-H.; Yu, C.-P.; Jin, J.-S.; Cheng, Y.-L. Expression of hypoxia-inducible factor (HIF)-1alpha and vascular endothelial growth factor (VEGF)-D as outcome predictors in resected esophageal squamous cell carcinoma. Dis. Markers 2008, 25, 141–148. [Google Scholar] [CrossRef]
- Tsochatzis, E.A.; Fatourou, E.; O’Beirne, J.; Meyer, T.; Burroughs, A.K. Transarterial chemoembolization and bland embolization for hepatocellular carcinoma. World J. Gastroenterol. 2014, 20, 3069–3077. [Google Scholar] [CrossRef]
- Llovet, J.M.; Real, M.I.; Montaña, X.; Planas, R.; Coll, S.; Aponte, J.; Ayuso, C.; Sala, M.; Muchart, J.; Solà, R.; et al. Arterial embolisation or chemoembolisation versus symptomatic treatment in patients with unresectable hepatocellular carcinoma: A randomised controlled trial. Lancet 2002, 359, 1734–1739. [Google Scholar] [CrossRef]
- Meyer, T.; Kirkwood, A.; Roughton, M.; Beare, S.; Tsochatzis, E.; Yu, D.; Davies, N.; Williams, E.; Pereira, S.; Hochhauser, D.; et al. A randomised phase II/III trial of 3-weekly cisplatin-based sequential transarterial chemoembolisation vs embolisation alone for hepatocellular carcinoma. Br. J. Cancer 2013, 108, 1252–1259. [Google Scholar] [CrossRef]
- Malagari, K.; Pomoni, M.; Kelekis, A.; Pomoni, A.; Dourakis, S.; Spyridopoulos, T.; Moschouris, H.; Emmanouil, E.; Rizos, S.; Kelekis, D. Prospective randomized comparison of chemoembolization with doxorubicin-eluting beads and bland embolization with BeadBlock for hepatocellular carcinoma. Cardiovasc. Intervent. Radiol. 2010, 33, 541–551. [Google Scholar] [CrossRef]
- Facciorusso, A.; Mariani, L.; Sposito, C.; Spreafico, C.; Bongini, M.; Morosi, C.; Cascella, T.; Marchianò, A.; Camerini, T.; Bhoori, S.; et al. Drug-eluting beads versus conventional chemoembolization for the treatment of unresectable hepatocellular carcinoma. J. Gastroenterol. Hepatol. 2016, 31, 645–653. [Google Scholar] [CrossRef] [PubMed]
- Facciorusso, A.; Di Maso, M.; Muscatiello, N. Drug-eluting beads versus conventional chemoembolization for the treatment of unresectable hepatocellular carcinoma: A meta-analysis. Dig. Liver Dis. 2016, 48, 571–577. [Google Scholar] [CrossRef] [PubMed]
- Lo, C.K.; Mertz, D.; Loeb, M. Newcastle-Ottawa Scale: Comparing reviewers’ to authors’ assessments. BMC Med. Res. Methodol. 2014, 14, 45. [Google Scholar] [CrossRef] [PubMed]
- Stang, A. Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur. J. Epidemiol. 2010, 25, 603–605. [Google Scholar] [CrossRef]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gotzsche, P.C.; Ioannidis, J.P.A.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: Explanation and elaboration. BMJ 2009, 339, b2700. [Google Scholar] [CrossRef] [PubMed]
- Kamarajah, S.K.; Bundred, J.; Spence, G.; Kennedy, A.; Dasari, B.V.M.; Griffiths, E.A. Critical Appraisal of the Impact of Oesophageal Stents in the Management of Oesophageal Anastomotic Leaks and Benign Oesophageal Perforations: An Updated Systematic Review. World J. Surg. 2019, 44, 1173–1189. [Google Scholar] [CrossRef]
- Brown, K.T.; Do, R.K.; Gonen, M.; Covey, A.M.; Getrajdman, G.I.; Sofocleous, C.T.; Jarnagin, W.R.; D’Angelica, M.I.; Allen, P.J.; Erinjeri, J.P.; et al. Randomized Trial of Hepatic Artery Embolization for Hepatocellular Carcinoma Using Doxorubicin-Eluting Microspheres Compared With Embolization With Microspheres Alone. J. Clin. Oncol. 2016, 34, 2046–2053. [Google Scholar] [CrossRef]
- Chang, J.M.; Tzeng, W.S.; Pan, H.B.; Yang, C.F.; Lai, K.H. Transcatheter arterial embolization with or without cisplatin treatment of hepatocellular carcinoma. A randomized controlled study. Cancer 1994, 74, 2449–2453. [Google Scholar] [CrossRef]
- Kawai, S.; Okamura, J.; Ogawa, M.; Ohashi, Y.; Tani, M.; Inoue, J.; Kawarada, Y.; Kusano, M.; Kubo, Y.; Kuroda, C.; et al. Prospective and randomized clinical trial for the treatment of hepatocellular carcinoma--a comparison of lipiodol-transcatheter arterial embolization with and without adriamycin (first cooperative study). The Cooperative Study Group for Liver Cancer Treatment of Japan. Cancer Chemother. Pharmacol. 1992, 31, S1–S6. [Google Scholar]
- Facciorusso, A.; Bellanti, F.; Villani, R.; Salvatore, V.; Muscatiello, N.; Piscaglia, F.; Vendemiale, G.; Serviddio, G. Transarterial chemoembolization vs bland embolization in hepatocellular carcinoma: A meta-analysis of randomized trials. United Eur. Gastroenterol. J. 2017, 5, 511–518. [Google Scholar] [CrossRef]
- Guo, J.; Wang, W.; Zhang, Y.; Xu, L.; Kong, J. Comparison of initial tumor responses to transarterial bland embolization and drug-eluting beads-transarterial chemoembolization in the management of hepatocellular carcinoma: A propensity-score matching analysis. J. Gastrointest. Oncol. 2021, 12, 1838–1850. [Google Scholar] [CrossRef] [PubMed]
- Facciorusso, A.; Antonino, M.; Del Prete, V.; Neve, V.; Scavo, M.P.; Barone, M. Are hematopoietic stem cells involved in hepatocarcinogenesis? Hepatobiliary Surg. Nutr. 2014, 3, 199–206. [Google Scholar] [CrossRef] [PubMed]
- Sangro, B.; Salem, R. Transarterial chemoembolization and radioembolization. Semin. Liver Dis. 2014, 34, 435–443. [Google Scholar] [CrossRef] [PubMed]
- Lencioni, R.; de Baere, T.; Soulen, M.C.; Rilling, W.S.; Geschwind, J.F. Lipiodol transarterial chemoembolization for hepatocellular carcinoma: A systematic review of efficacy and safety data. Hepatology 2016, 64, 106–116. [Google Scholar] [CrossRef]
- Fako, V.; Martin, S.P.; Pomyen, Y.; Budhu, A.; Chaisaingmongkol, J.; Franck, S.; Lee, J.M.-F.; Ng, I.O.-L.; Cheung, T.-T.; Wei, X.; et al. Gene signature predictive of hepatocellular carcinoma patient response to transarterial chemoembolization. Int. J. Biol. Sci. 2019, 15, 2654–2663. [Google Scholar] [CrossRef]
- Arzumanyan, A.; Friedman, T.; Ng, I.O.; Clayton, M.M.; Lian, Z.; Feitelson, M.A. Does the hepatitis B antigen HBx promote the appearance of liver cancer stem cells? Cancer Res. 2011, 71, 3701–3708. [Google Scholar] [CrossRef]
- Zhang, W.; Xu, A.H.; Wang, W.; Wu, Y.H.; Sun, Q.L.; Shu, C. Radiological appearance of hepatocellular carcinoma predicts the response to trans-arterial chemoembolization in patients undergoing liver transplantation. BMC Cancer 2019, 19, 1041. [Google Scholar] [CrossRef]
- Granito, A.; Facciorusso, A.; Sacco, R.; Bartalena, L.; Mosconi, C.; Cea, U.V.; Cappelli, A.; Antonino, M.; Modestino, F.; Brandi, N.; et al. TRANS-TACE: Prognostic Role of the Transient Hypertransaminasemia after Conventional Chemoembolization for Hepatocellular Carcinoma. J. Pers. Med. 2021, 11, 1041. [Google Scholar] [CrossRef]
- Xue, T.C.; Jia, Q.A.; Ge, N.L.; Chen, Y.; Zhang, B.H.; Ye, S.L. Imbalance in systemic inflammation and immune response following transarterial chemoembolization potentially increases metastatic risk in huge hepatocellular carcinoma. Tumour. Biol. 2015, 36, 8797–8803. [Google Scholar] [CrossRef]
- Viedma-Martinez, M.; Villegas Romero, I. Skin Necrosis after Transarterial Chemoembolization. N. Engl. J. Med. 2022, 387, 2268. [Google Scholar] [CrossRef]
- Sidaway, P. HAIC-FO improves outcomes in HCC. Nat. Rev. Clin. Oncol. 2022, 19, 150. [Google Scholar] [CrossRef] [PubMed]
- Granito, A.; Forgione, A.; Marinelli, S.; Renzulli, M.; Ielasi, L.; Sansone, V.; Benevento, F.; Piscaglia, F.; Tovoli, F. Experience with regorafenib in the treatment of hepatocellular carcinoma. Therap. Adv. Gastroenterol. 2021, 14, 17562848211016959. [Google Scholar] [CrossRef] [PubMed]
- Stefanini, B.; Ielasi, L.; Chen, R.; Abbati, C.; Tonnini, M.; Tovoli, F.; Granito, A. TKIs in combination with immunotherapy for hepatocellular carcinoma. Expert Rev. Anticancer Ther. 2023, 23, 279–291. [Google Scholar] [CrossRef] [PubMed]
| # | Term | Results |
|---|---|---|
| Medline® | ||
| 1 | Carcinoma, Hepatocellular | 17,497 |
| 2 | Liver Neoplasms | 25,966 |
| 3 | HCC | 13,454 |
| 4 | Primary liver cancer | 408 |
| 5 | TACE | 1272 |
| 6 | Chemoembolisation, therapeutic | 1568 |
| 7 | Treatment embolization | 2 |
| 8 | Transarterial chemoembolisation | 38 |
| 9 | Transarterial chemoembolization | 38 |
| 10 | TAE | 399 |
| 11 | Transarterial embolisation | 16 |
| 12 | Bland embolisation | 1 |
| 13 | 1 OR 2 OR 3 OR 4 | 27,680 |
| 14 | 5 OR 6 OR 7 OR 8 OR 9 OR 10 OR 10 OR 11 | 2283 |
| 15 | 12 AND 13 | 1662 |
| 16 | Limit 14 to (English language and full text) | 1510 |
| Embase | ||
| 1 | Liver cell carcinoma | 148,941 |
| 2 | Liver tumor | 47,443 |
| 3 | Hepatocellular carcinoma | 167,582 |
| 4 | HCC | 86,079 |
| 5 | Primary Liver cancer | 3586 |
| 6 | TACE | 10,520 |
| 7 | Chemoembolisation | 15,880 |
| 8 | Transarterial chemoembolisation | 401 |
| 9 | Transarterial chemoembolization | 401 |
| 10 | Treatment embolisation | 10 |
| 11 | TAE | 3793 |
| 12 | Transarterial embolisation | 171 |
| 13 | Bland embolisation | 10 |
| 14 | 1 OR 2 OR 3 OR 4 | 205,638 |
| 15 | 5 OR 6 OR 7 OR 8 OR 9 OR 10 OR 11 OR 12 | 26,300 |
| 16 | 13 AND 14 | 17,081 |
| 17 | Limit 15 to (full text and English language | 3867 |
| Cochrane Library | ||
| 1 | Carcinoma, Hepatocellular | 5851 |
| 2 | Liver Neoplasms | 5958 |
| 3 | HCC | 4158 |
| 4 | Primary liver cancer | 8100 |
| 5 | TACE | 1389 |
| 6 | Chemoembolisation, therapeutic | 65 |
| 7 | Treatment embolization | 2063 |
| 8 | Transarterial chemoembolisation | 107 |
| 9 | Transarterial chemoembolization | 708 |
| 10 | TAE | 10,308 |
| 11 | Transarterial embolisation | 242 |
| 12 | Bland embolisation | 35 |
| 13 | 1 OR 2 OR 3 OR 4 | 16,338 |
| 14 | 5 OR 6 OR 7 OR 8 OR 9 OR 10 OR 10 OR 11 | 13,543 |
| 15 | 13 AND 14 | 83,651 |
| 16 | Limit 14 to (full text and English language) | 8710 |
| First Author | Patients, n | Country | Duration | Follow Up (Months) | Chemotherapy Drug | Chemotherapy Dose | Embolisation Agent | Embolisation Agent Size |
|---|---|---|---|---|---|---|---|---|
| Brown 2016 [17] | 101 | USA | 2007–2012 | 48 | Doxorubicin | <150 mg | LC bead | 100–300, 300–500, 500–700, 700–900 μm |
| Chang 1994 [18] | 46 | China | 1991–1993 | 28 | Cisplatin | 50 mg | Gelatin sponge | 1 × 1 mm |
| Kawai 1992 [19] | 289 | Japan | 1988–1989 | 36 | Adriamycin | 40 mg/m2 | Gelatin sponge | NA |
| Malagari 2010 [10] | 87 | Greece | 2005–2006 | 12 | Doxorubicin | <150 mg | DC bead | 100–300, 300–500 μm |
| Meyer 2013 [9] | 86 | UK | 2003–2009 | 36 | Cisplatin | 50 mg | PVA bead | 50–150 μm |
| Study Name | Random Sequence Generation | Allocation Concealment | Baseline Differences | Patient Blinding | Carer Blinding | Differing from Intended Treatment | Incomplete Outcome Data | Selective Outcome Reporting | Appropriate Outcome Assessment | Overall |
|---|---|---|---|---|---|---|---|---|---|---|
| Brown 2016 [17] | Low | Low | Low | Low | High | Low | Low | Low | Low | Low |
| Chang 1994 [18] | High | High | Low | Unclear | Low | Unclear | Low | Low | Low | Low |
| Kawai 1992 [19] | High | High | Unclear | Unclear | High | Unclear | Low | High | Low | High |
| Malagari 2010 [10] | High | High | Low | Unclear | High | Unclear | Low | High | Low | High |
| Meyer 2013 [9] | Low | High | Low | Unclear | Low | Low | Low | Low | Low | Low |
| Outcome | OR (95% CI) | p Value |
|---|---|---|
| Cholecystitis | 0.70 (0.12–4.06) | 0.7 |
| Liver abscess | 0.51 (0.10–2.58) | 0.4 |
| Liver failure | 1.01 (0.25–4.11) | 1.0 |
| Puncture site bleeding | 0.96 (0.19–4.93) | 1.0 |
| Emesis | 11.47 (4.22–31.16) | <0.001 |
| Gastro-intestinal bleed | 0.15 (0.01–7.44) | 0.3 |
| Leukopenia | 1.43 (0.79–2.57) | 0.3 |
| Anaemia | 2.68 (1.40–5.14) | 0.003 |
| Thrombocytopenia | 0.89 (0.47–1.68) | 0.7 |
| Abdominal Pain | 1.12 (0.71–1.78) | 0.6 |
| Fever | 0.68 (0.41–1.13) | 0.1 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lawson, A.; Kamarajah, S.K.; Parente, A.; Pufal, K.; Sundareyan, R.; Pawlik, T.M.; Ma, Y.T.; Shah, T.; Kharkhanis, S.; Dasari, B.V.M. Outcomes of Transarterial Embolisation (TAE) vs. Transarterial Chemoembolisation (TACE) for Hepatocellular Carcinoma: A Systematic Review and Meta-Analysis. Cancers 2023, 15, 3166. https://doi.org/10.3390/cancers15123166
Lawson A, Kamarajah SK, Parente A, Pufal K, Sundareyan R, Pawlik TM, Ma YT, Shah T, Kharkhanis S, Dasari BVM. Outcomes of Transarterial Embolisation (TAE) vs. Transarterial Chemoembolisation (TACE) for Hepatocellular Carcinoma: A Systematic Review and Meta-Analysis. Cancers. 2023; 15(12):3166. https://doi.org/10.3390/cancers15123166
Chicago/Turabian StyleLawson, Alexander, Sivesh K. Kamarajah, Alessandro Parente, Kamil Pufal, Ramanivas Sundareyan, Timothy M. Pawlik, Yuk Ting Ma, Tahir Shah, Salil Kharkhanis, and Bobby V. M. Dasari. 2023. "Outcomes of Transarterial Embolisation (TAE) vs. Transarterial Chemoembolisation (TACE) for Hepatocellular Carcinoma: A Systematic Review and Meta-Analysis" Cancers 15, no. 12: 3166. https://doi.org/10.3390/cancers15123166
APA StyleLawson, A., Kamarajah, S. K., Parente, A., Pufal, K., Sundareyan, R., Pawlik, T. M., Ma, Y. T., Shah, T., Kharkhanis, S., & Dasari, B. V. M. (2023). Outcomes of Transarterial Embolisation (TAE) vs. Transarterial Chemoembolisation (TACE) for Hepatocellular Carcinoma: A Systematic Review and Meta-Analysis. Cancers, 15(12), 3166. https://doi.org/10.3390/cancers15123166