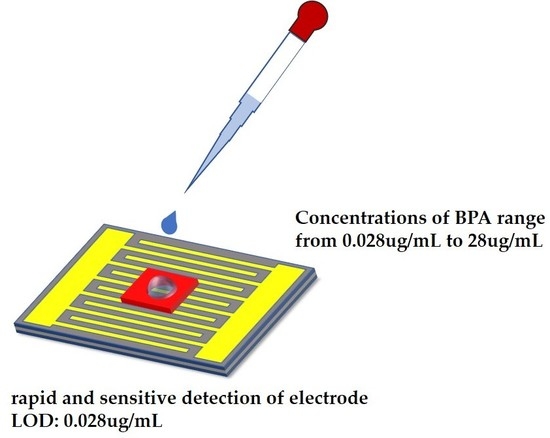
Rapid and Sensitive Detection of Bisphenol A Based on Self-Assembly
Abstract
1. Introduction
2. Materials and Methods
2.1. Materials and Reagents
2.2. Preparation of Interdigital Microelectrodes
2.3. Apparatus and Methods
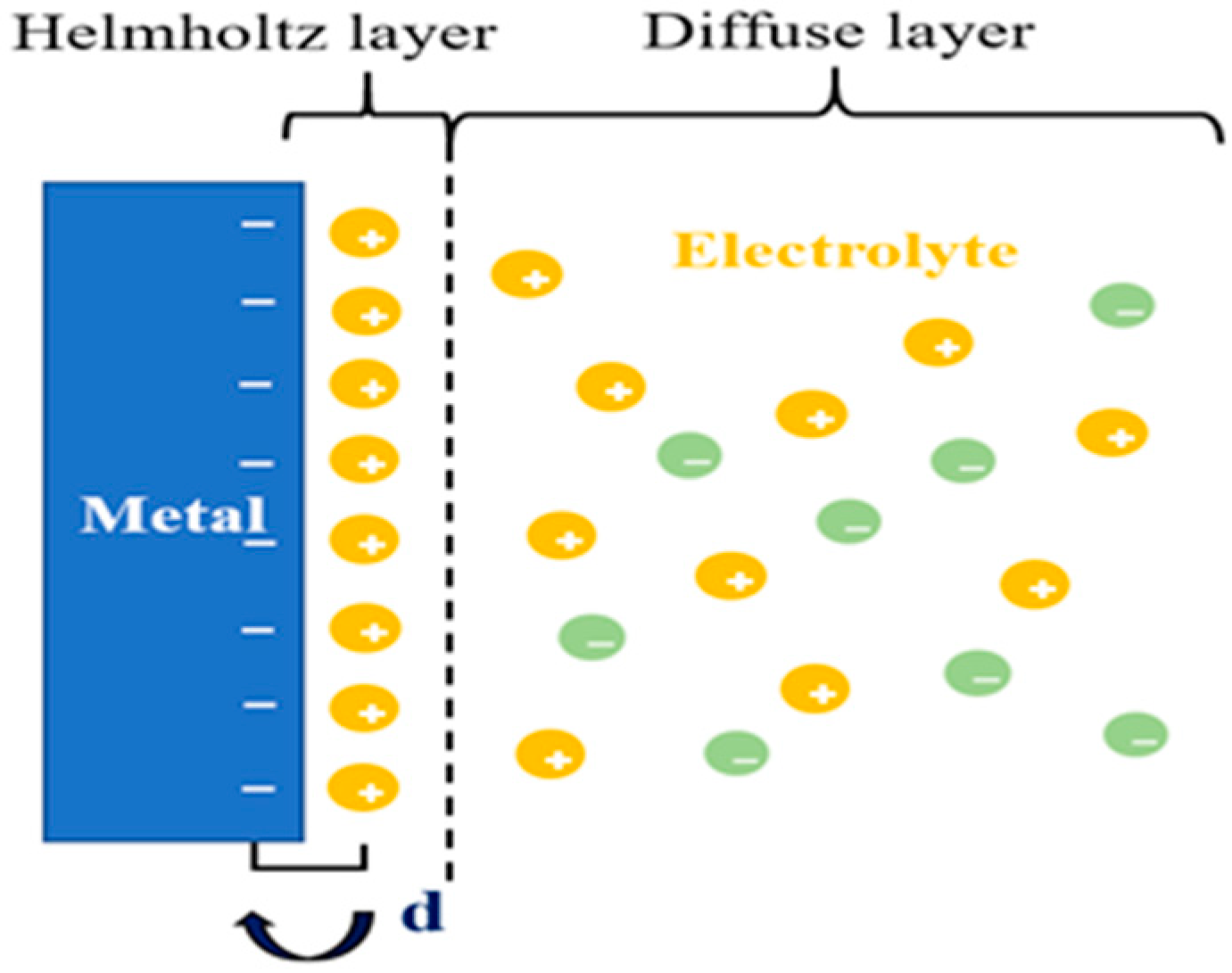
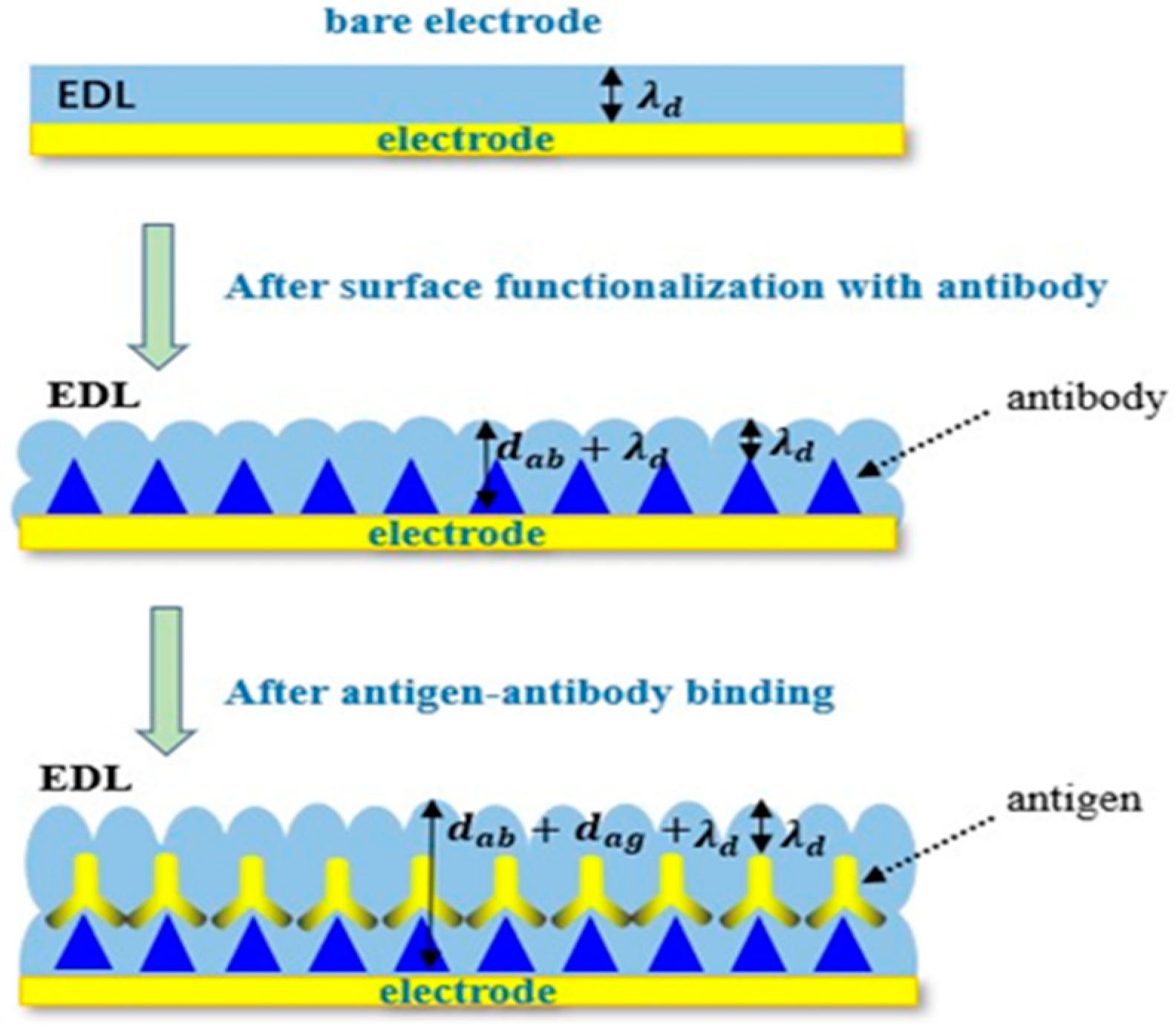
2.4. Electrical Double Layers
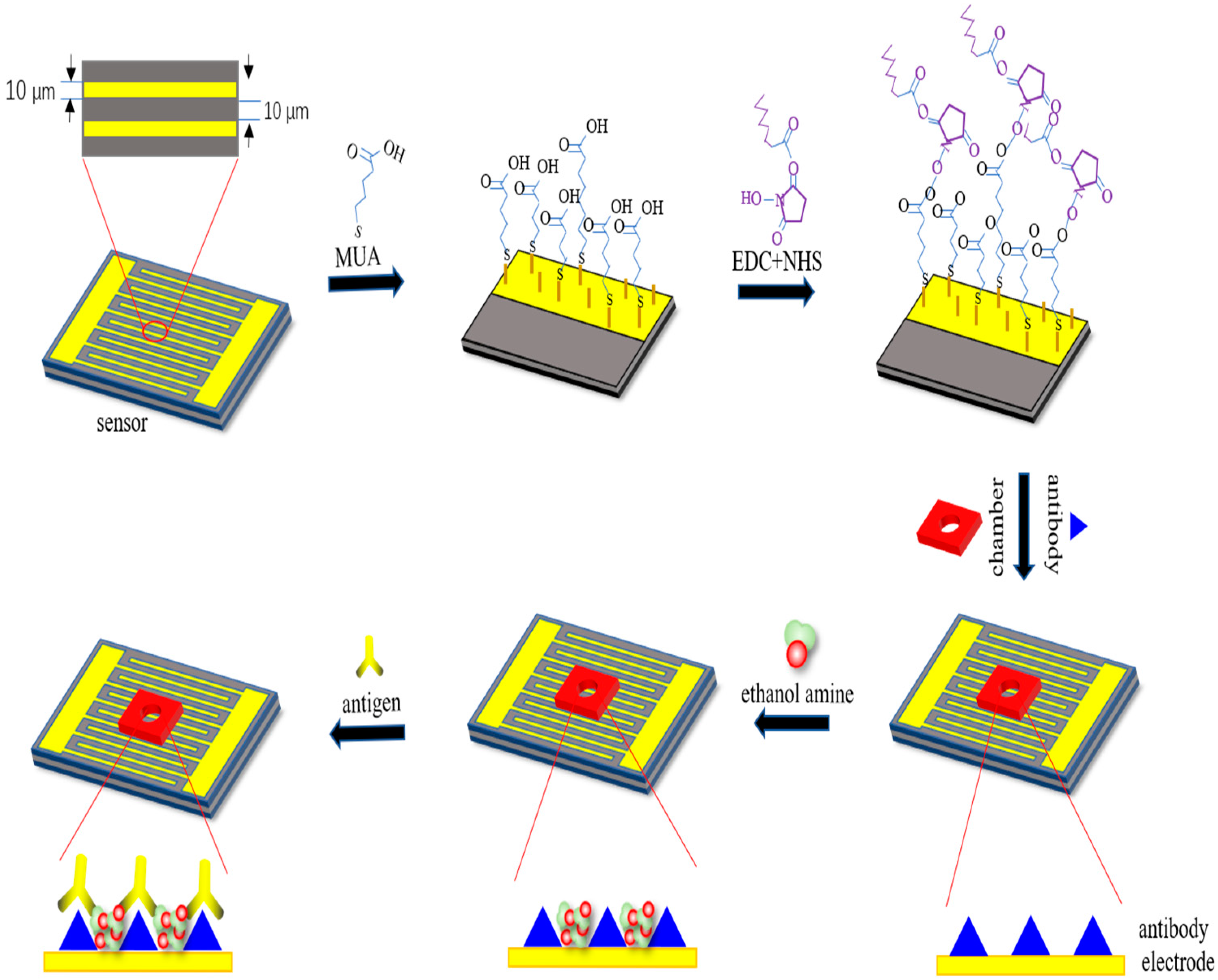
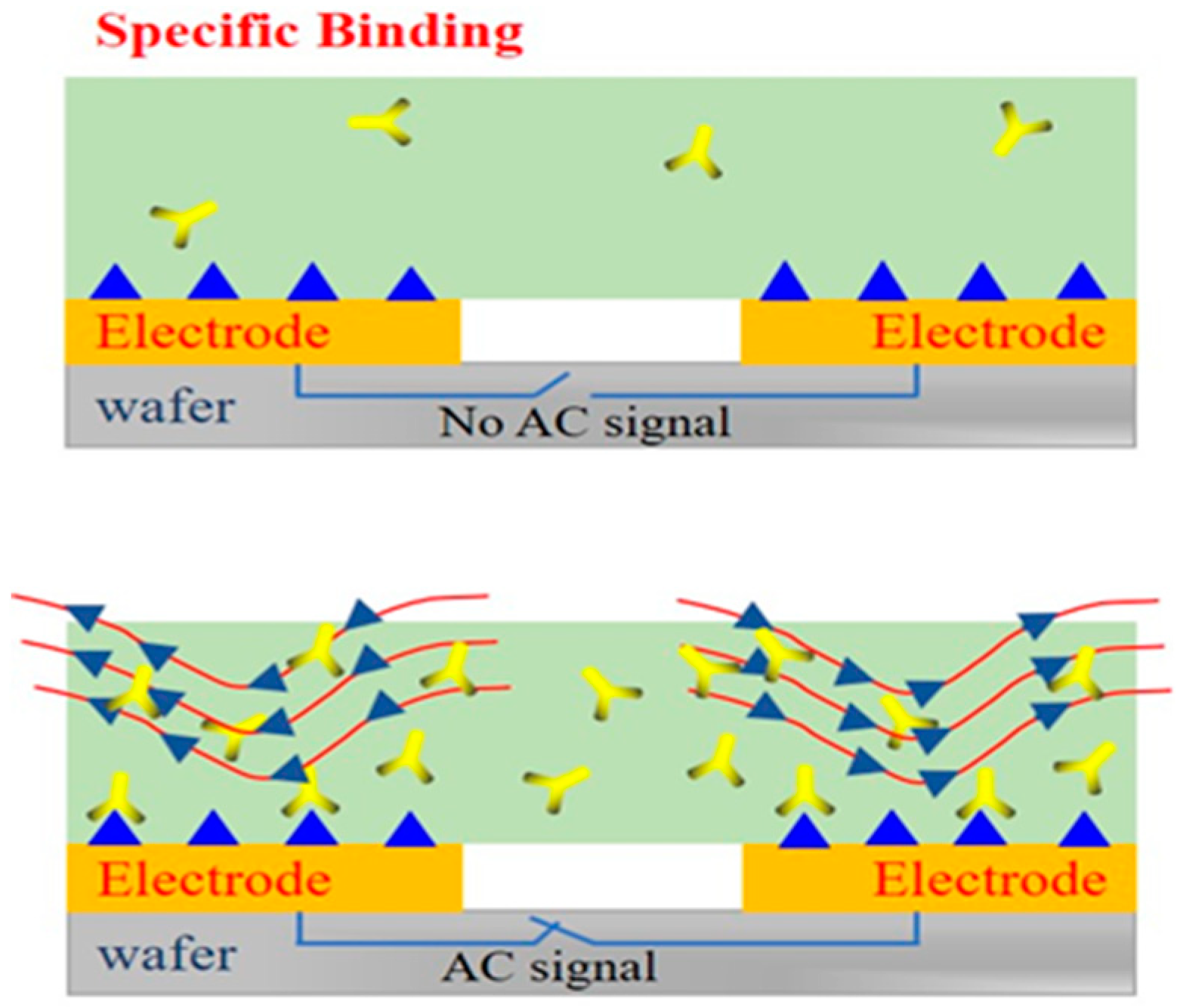
2.5. The Binding Mechanism of Interdigital Electrode Surface
3. Results and Discussions
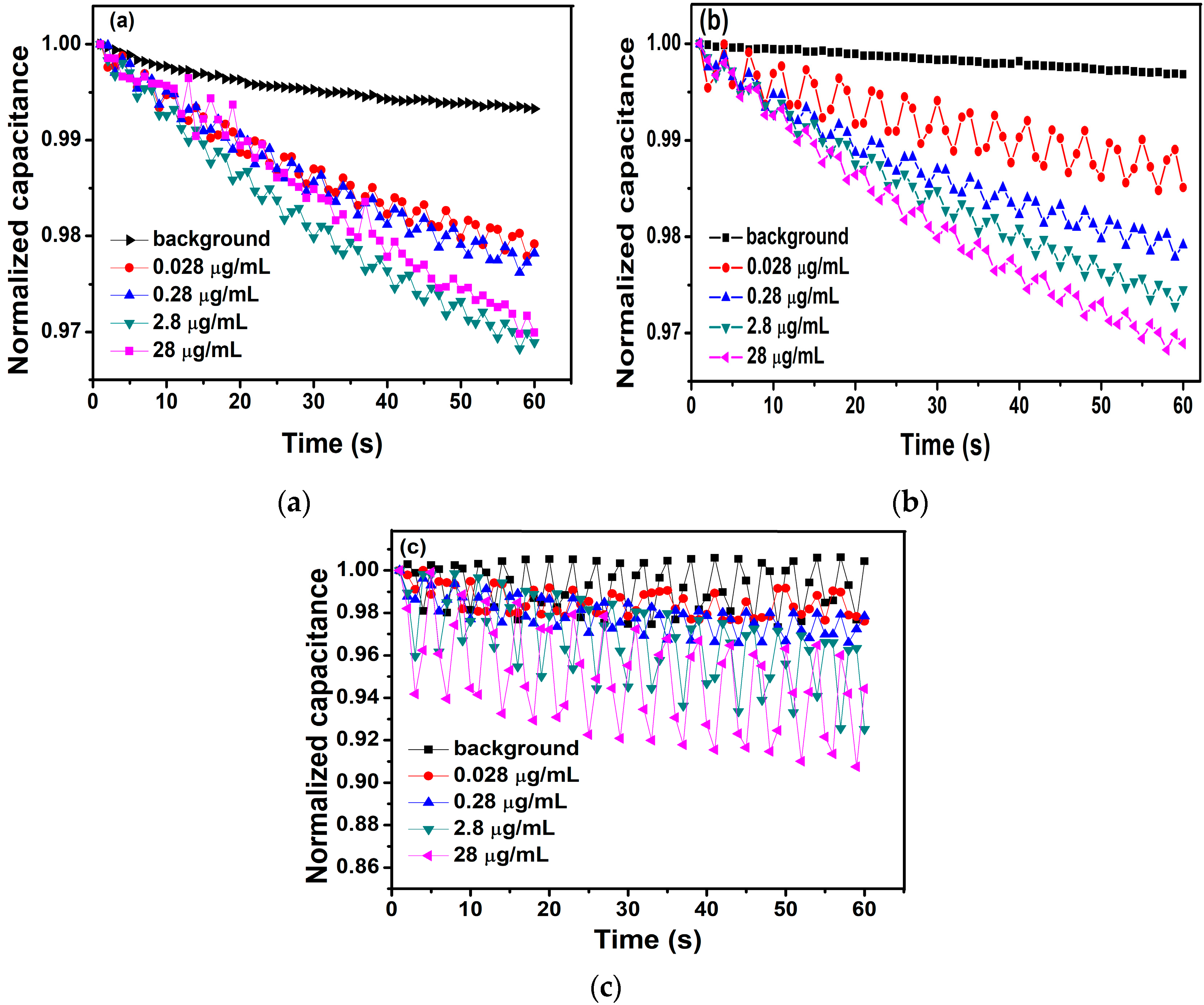
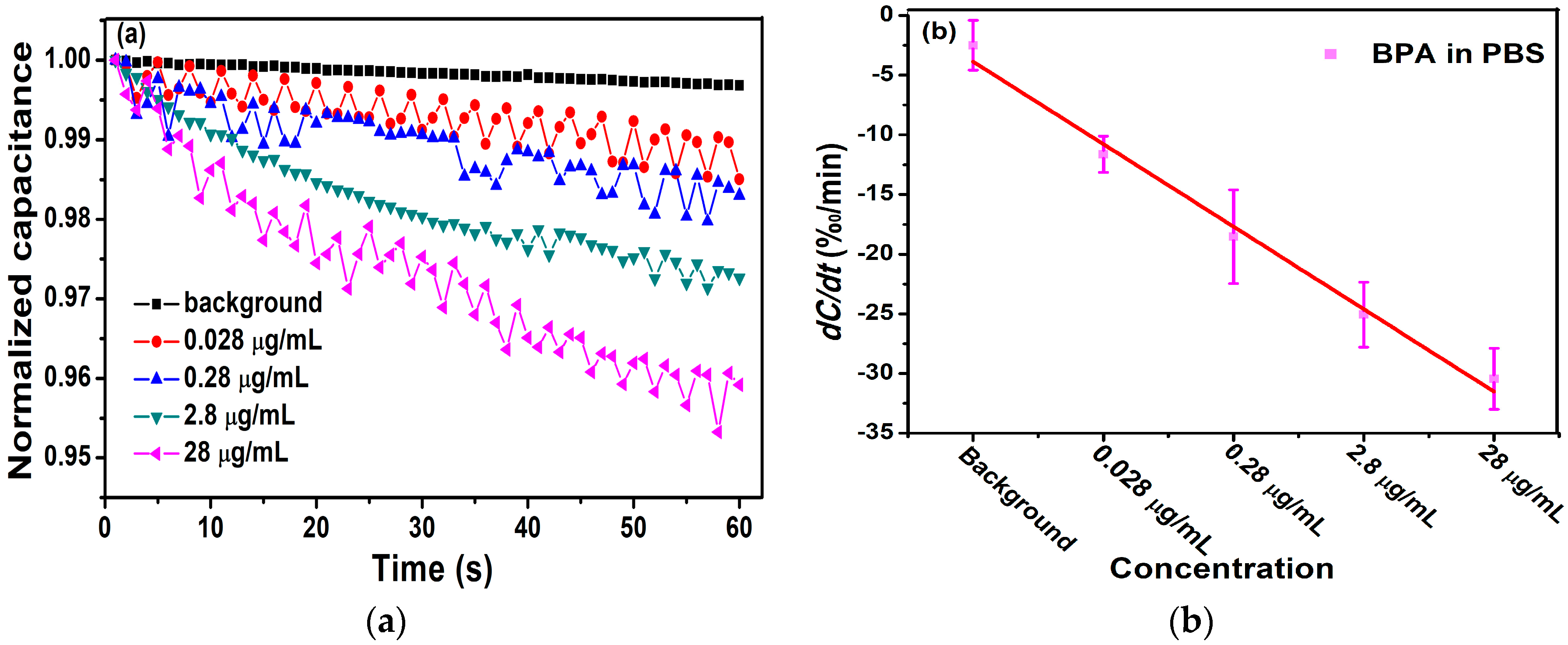
3.1. Detection of Antigen with 5.3 μg/L Antibody
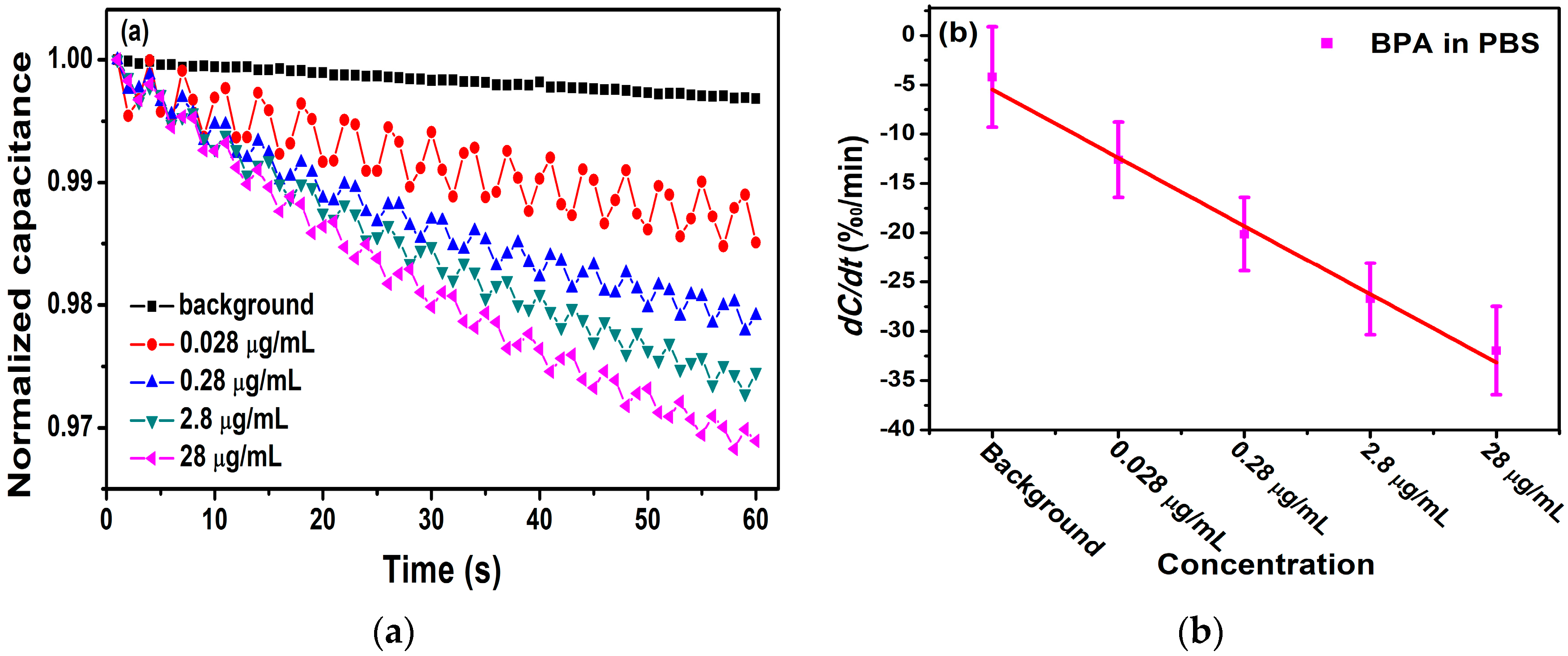
3.2. Detection of Antigen with 5.3 μg/mL Antibody
4. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Chevalier, N.; Brucker-Davis, F.; Lahlou, N.; Coquillard, P.; Pugeat, M.; Pacini, P.; Panaïa-Ferrari, P.; Wagner-Mahler, K.; Fénichel, P. A negative correlation between insulin-like peptide 3 and bisphenol A in human cord blood suggests an effect of endocrine disruptors on testicular descent during fetal development. Hum. Reprod. 2014, 30, 447–453. [Google Scholar] [CrossRef] [PubMed]
- Lang, I.A.; Galloway, T.S.; Scarlett, A.; Henley, W.E.; Depledge, M.; Wallace, R.B.; Melzer, D. Association of Urinary Bisphenol A Concentration With Medical Disorders and Laboratory Abnormalities in Adults. JAMA 2008, 300, 1303–1310. [Google Scholar] [CrossRef] [PubMed]
- Mei, Z.; Qu, W.; Deng, Y.; Chu, H.; Cao, J.; Xue, F.; Zheng, L.; El-Nezamic, H.S.; Wu, Y.; Chen, W. One-step signal amplified lateral flow strip biosensor for ultrasensitive and on-site detection of bisphenol A (BPA) in aqueous samples. Biosens. Bioelectron. 2013, 49, 457–461. [Google Scholar] [CrossRef] [PubMed]
- Apodaca, D.C.; Pernites, R.B.; Ponnapati, R.; Del Mundo, F.R.; Advincula, R.C. Electropolymerized Molecularly Imprinted Polymer Film: EIS Sensing of Bisphenol A. Macromol. 2011, 44, 6669–6682. [Google Scholar] [CrossRef]
- Soto, A.M.; Sonnenschein, C. Environmental causes of cancer: Endocrine disruptors as carcinogens. Nat. Rev. Endocrinol. 2010, 6, 363–370. [Google Scholar] [CrossRef]
- D’Antuono, A.; Dall’Orto, V.C.; Balbo, A.L.; Sobral, S.; Rezzano, I. Determination of bisphenol A in food-simulating liquids using LCED with a chemically modified electrode. J. Agric. Food Chem. 2001, 49, 1098–1101. [Google Scholar] [CrossRef]
- Nakazawa, H.; Yamaguchi, A.; Inoue, K.; Yamazaki, T.; Kato, K.; Yoshimura, Y.; Makino, T. In vitro assay of hydrolysis and chlorohydroxy derivatives of bisphenol A diglycidyl ether for estrogenic activity. Food Chem. Toxicol. 2002, 40, 1827–1832. [Google Scholar] [CrossRef]
- Fontana, A.R.; De Toro, M.M.; Altamirano, J.C. One-Step Derivatization and Preconcentration Microextraction Technique for Determination of Bisphenol A in Beverage Samples by Gas Chromatography−Mass Spectrometry. J. Agric. Food Chem. 2011, 59, 3559–3565. [Google Scholar] [CrossRef]
- Yin, W.; Wu, L.; Ding, F.; Li, Q.; Wang, P.; Li, J.; Lu, Z.; Han, H. Surface-imprinted SiO2@Ag nanoparticles for the selective detection of BPA using surface enhanced Raman scattering. Sensors Actuators B Chem. 2018, 258, 566–573. [Google Scholar] [CrossRef]
- Kubo, I.; Kanamatsu, T.; Furutani, S. Microfluidic device for enzyme-linked immunosorbent assay (ELISA) and its application to bisphenol a sensing Sens. Mater 2014, 26, 615–621. [Google Scholar]
- Gallo, P.; Pisciottano, I.D.M.; Fattore, M.; Rimoli, M.G.; Seccia, S.; Albrizio, S. A method to determine BPA, BPB, and BPF levels in fruit juices by liquid chromatography coupled to tandem mass spectrometry. Food Addit. Contam. Part A 2019, 36, 1871–1881. [Google Scholar] [CrossRef] [PubMed]
- Sheng, W.; Duan, W.; Shi, Y.; Chang, Q.; Zhang, Y.; Lu, Y.; Wang, S. Sensitive detection of bisphenol A in drinking water and river water using an upconversion nanoparticles-based fluorescence immunoassay in combination with magnetic separation. Anal. Methods 2018, 10, 5313–5320. [Google Scholar] [CrossRef]
- Xue, C.S.; Erika, G.; Jiří, H. Surface plasmon resonance biosensor for the ultrasensitive detection of bisphenol A. Anal. Bioanal. Chem. 2019, 411, 5655–5658. [Google Scholar] [CrossRef] [PubMed]
- Avila, M.; Zougagh, M.; Ríos, Á.; Escarpa, A. Molecularly imprinted polymers for selective piezoelectric sensing of small molecules. TrAC Trends Anal. Chem. 2008, 27, 54–65. [Google Scholar] [CrossRef]
- Brusnitsyn, D.V.; Medyantseva, E.P.; Varlamova, R.M.; Sitdikova, R.R.; Fattakhova, A.N.; Konovalova, O.A.; Budnikov, G.K. Carbon nanomaterials as electrode surface modifiers in development of amperometric monoamino oxidase biosensors. Inorg. Mater. 2016, 52, 1413–1419. [Google Scholar] [CrossRef]
- Vashist, S.K.; Zheng, D.; Al-Rubeaan, K.; Luong, J.H.; Sheu, F.-S. Advances in carbon nanotube based electrochemical sensors for bioanalytical applications. Biotechnol. Adv. 2011, 29, 169–188. [Google Scholar] [CrossRef]
- Ntsendwana, B.; Sampath, S.; Mamba, B.; Arotiba, O. Photoelectrochemical oxidation of p-nitrophenol on an expanded graphite–TiO2 electrode. Photochem. Photobiol. Sci. 2013, 12, 1091. [Google Scholar] [CrossRef]
- Ndlovu, T.; Arotiba, O.; Sampath, S.; Krause, R.; Mamba, B. Electroanalysis of copper as a heavy metal pollutant in water using cobalt oxide modified exfoliated graphite electrode. Phys. Chem. Earth Parts A/B/C 2012, 50, 127–131. [Google Scholar] [CrossRef]
- Liu, X.; Peng, Y.; Qu, X.; Ai, S.; Han, R.; Zhu, X. Multi-walled carbon nanotube-chitosan/poly(amidoamine)/DNA nanocomposite modified gold electrode for determination of dopamine and uric acid under coexistence of ascorbic acid. J. Electroanal. Chem. 2011, 654, 72–78. [Google Scholar] [CrossRef]
- Manivel, P.; Dhakshnamoorthy, M.; Balamurugan, A.; Ponpandian, N.; Mangalaraj, D.; Viswanathan, C.; N, P. Conducting polyaniline-graphene oxide fibrous nanocomposites: Preparation, characterization and simultaneous electrochemical detection of ascorbic acid, dopamine and uric acid. RSC Adv. 2013, 3, 14428. [Google Scholar] [CrossRef]
- Li, Z.; Nambiar, S.; Zheng, W.; Yeow, J. PDMS/single-walled carbon nanotube composite for proton radiation shielding in space applications. Mater. Lett. 2013, 108, 79–83. [Google Scholar] [CrossRef]
- Nazari, M.; Kashanian, S.; Rafipour, R.; Omidfar, K. Biosensor design using an electroactive label-based aptamer to detect bisphenol A in serum samples. J. Biosci. 2019, 44, 105. [Google Scholar] [CrossRef] [PubMed]
- Lee, E.-H.; Lee, S.K.; Kim, M.J.; Lee, S.-W. Simple and rapid detection of bisphenol A using a gold nanoparticle-based colorimetric aptasensor. Food Chem. 2019, 287, 205–213. [Google Scholar] [CrossRef]
- Inroga, F.A.D.; Rocha, M.O.; Lavayen, V.; Arguello, J. Development of a tyrosinase-based biosensor for bisphenol A detection using gold leaf–like microstructures. J. Solid State Electrochem. 2019, 23, 1659–1666. [Google Scholar] [CrossRef]
- Liu, Y.; Yao, L.; He, L.; Liu, N.; Piao, Y. Electrochemical Enzyme Biosensor Bearing Biochar Nanoparticle as Signal Enhancer for Bisphenol A Detection in Water. Sensors 2019, 19, 1619. [Google Scholar] [CrossRef] [PubMed]
- Peng, X.; Kang, L.; Pang, F.; Li, H.; Luo, R.; Luo, X.; Sun, F. A signal-enhanced lateral flow strip biosensor for ultrasensitive and on-site detection of bisphenol A. Food Agric. Immunol. 2018, 29, 216–227. [Google Scholar] [CrossRef]
- Liu, S.; Fu, Y.; Xiong, C.; Liu, Z.; Zheng, L.; Yan, F. Detection of Bisphenol A Using DNA-Functionalized Graphene Field Effect Transistors Integrated in Microfluidic Systems. ACS Appl. Mater. Interfaces 2018, 10, 23522–23528. [Google Scholar] [CrossRef]
- Li, S.; Cui, H.; Yuan, Q.; Wu, J.; Wadhwa, A.; Eda, S.; Jiang, H. AC electrokinetics-enhanced capacitive immunosensor for point-of-care serodiagnosis of infectious diseases. Biosens. Bioelectron. 2014, 51, 437–443. [Google Scholar] [CrossRef]
- Liu, X.; Yang, K.; Wadhwa, A.; Eda, S.; Li, S.; Wu, J. Development of an AC electrokinetics-based immunoassay system for on-site serodiagnosis of infectious diseases. Sens. Actuators A Phys. 2011, 171, 406–413. [Google Scholar] [CrossRef]
- Lian, M.; Islam, N.; Wu, J. AC electrothermal manipulation of conductive fluids and particles for lab-chip applications. IET Nanobiotechnology 2007, 1, 36–43. [Google Scholar] [CrossRef]
- Cheng, C.; Cui, H.; Wu, J.; Eda, S. A PCR-free point-of-care capacitive immunoassay for influenza A virus. Microchim. Acta 2017, 55, 53–1657. [Google Scholar] [CrossRef]
- Lin, X.; Cheng, C.; Terry, P.; Chen, J.; Cui, H.; Wu, J. Rapid and sensitive detection of bisphenol a from serum matrix. Biosens. Bioelectron. 2017, 91, 104–109. [Google Scholar] [CrossRef] [PubMed]
- Bertilsson, L.; Potje-Kamloth, K. Molecular interaction of DMMP and water vapor with mixed self-assembled mon01ayers studied by IR spectroscopy and SAW devices. 7rhin Solid Film. 1996, 284, 882–887. [Google Scholar] [CrossRef]
- Yang, X.; Shi, J.; Johnson, S.; Swanson, B. Molecular host siloxane thin films for surface acoustic wave chemical sensors. Sens. Actuators B Chem. 1997, 45, 79–84. [Google Scholar] [CrossRef]
- Helmholtz. On the modern development of Faraday’s conception of electricity. J. Franklin Inst. 1881, 44, 182–185. [Google Scholar]
- Grahame, D.C. The electrical double layer and the theory of electrocapillarity. Chem. Rev. 1947, 41, 441–501. [Google Scholar] [CrossRef]
- Berggren, C.; Bjarnason, B.; Johansson, G. Capacitive biosensors. Electroanalysis 2001, 13, 173–180. [Google Scholar] [CrossRef]
- Wu, J. Interactions of electrical fields with fluids: Laboratory-on-a-chip applications. IET Nanobiotechnology 2008, 2, 14. [Google Scholar] [CrossRef]
- Shi-Ping, S.; Zhi-Dong, M.A.; Wen-De, Z. Determination of Bisphenol A in Food Packaging Materials by Oscillopolarogaphic Method. J. Anal. Sci. 2002, 18, 490–492. [Google Scholar]
- Yan, X.; Zhou, C.; Yan, Y.; Zhu, Y. A Simple and Renewable Nanoporous Gold-based Electrochemical Sensor for Bisphenol A Detection. Electroanal. 2015, 27, 2718–2724. [Google Scholar] [CrossRef]
| Method | LOD | Reference |
|---|---|---|
| Carbon nanohorns/Nafion | 1.8 mol/L | Yilin Li (2014) |
| SDS-(bupy)P/CPE | 3.02 mol/L | Zhang Yanmei (2012) |
| Graphene modified SPCE | 4.99 mol/L | Ling Zhou (2014) |
| Strata® C18-E cartridge cleanup with detection by liquid chromatography coupled | 5.21 mol/L | Pasquale Gallo (2019) |
| Nanoparticles-based fluorescence immunoassay | 8.7 mol/L | Wei Sheng (2018) |
| Surface plasmon resonance (SPR) biosensor | 2.28 mol/L | Xue C S (2019) |
| Gold nanoparticle-based colorimetric aptasensor | 4.38 mol/L | Eun-Hee Lee (2019) |
| Electroactive label-based aptamer | 3.8 mol/L | Maryam Nazari (2019) |
| A tyrosinase-based biosensor | 7.7 mol/L | Filomeno A.D. Inroga (2019) |
| Electrochemical enzyme biosensor | 3.18 mol/L | Yang Liu (2019) |
| A signal-enhanced lateral flow strip biosensor | 4.38 mol/L | Xiayu Peng (2017) |
| DNA-functionalized graphene field effect transistors integrated in microfluidic systems. | 4.38 mol/L | Liu S (2018) |
| Self-assembly technology and AC electrokinetics effect | 1.22 mol/L | This work |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Luo, H.; Lin, X.; Peng, Z.; Song, M.; Jin, L. Rapid and Sensitive Detection of Bisphenol A Based on Self-Assembly. Micromachines 2020, 11, 41. https://doi.org/10.3390/mi11010041
Luo H, Lin X, Peng Z, Song M, Jin L. Rapid and Sensitive Detection of Bisphenol A Based on Self-Assembly. Micromachines. 2020; 11(1):41. https://doi.org/10.3390/mi11010041
Chicago/Turabian StyleLuo, Haoyue, Xiaogang Lin, Zhijia Peng, Min Song, and Lifeng Jin. 2020. "Rapid and Sensitive Detection of Bisphenol A Based on Self-Assembly" Micromachines 11, no. 1: 41. https://doi.org/10.3390/mi11010041
APA StyleLuo, H., Lin, X., Peng, Z., Song, M., & Jin, L. (2020). Rapid and Sensitive Detection of Bisphenol A Based on Self-Assembly. Micromachines, 11(1), 41. https://doi.org/10.3390/mi11010041