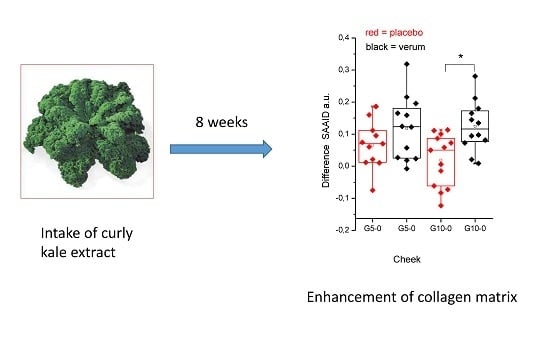
Influences of Orally Taken Carotenoid-Rich Curly Kale Extract on Collagen I/Elastin Index of the Skin
Abstract
:1. Introduction
2. Material and Methods
2.1. Subjects
2.2. Supplements
2.3. Study Protocol
2.4. Carotenoid Determination
2.5. Collagen I/Elastin Index SAAID
2.6. Statistics
3. Results
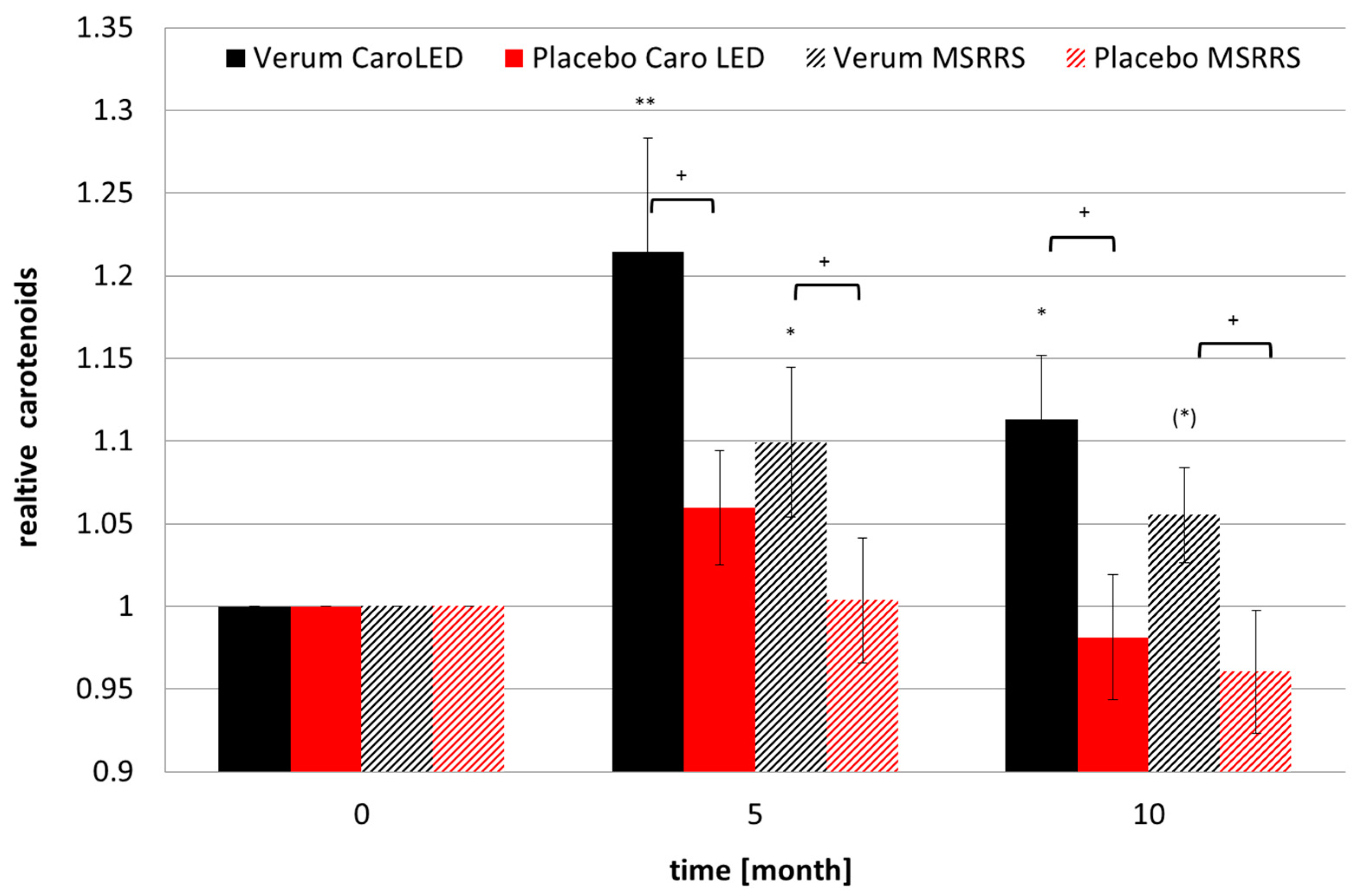
3.1. Carotenoids
3.2. SAAID
3.3. Correlations
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Fito, M.; Konstantinidou, V. Nutritional Genomics and the Mediterranean Diet’s Effects on Human Cardiovascular Health. Nutrients 2016, 8. [Google Scholar] [CrossRef] [PubMed]
- Li, S.; Zhu, Y.; Chavarro, J.E.; Bao, W.; Tobias, D.K.; Ley, S.H.; Forman, J.P.; Liu, A.; Mills, J.; Bowers, K.; et al. Healthful Dietary Patterns and the Risk of Hypertension Among Women With a History of Gestational Diabetes Mellitus: A Prospective Cohort Study. Hypertension 2016. [Google Scholar] [CrossRef]
- Sun, Y.; Li, Z.; Li, J.; Li, Z.; Han, J. A Healthy Dietary Pattern Reduces Lung Cancer Risk: A Systematic Review and Meta-Analysis. Nutrients 2016, 8. [Google Scholar] [CrossRef] [PubMed]
- Dias, I.H.; Polidori, M.C.; Li, L.; Weber, D.; Stahl, W.; Nelles, G.; Grune, T.; Griffiths, H.R. Plasma levels of HDL and carotenoids are lower in dementia patients with vascular comorbidities. J. Alzheimer’s Dis. 2014, 40, 399–408. [Google Scholar] [CrossRef]
- Polidori, M.C.; De Spirt, S.; Stahl, W.; Pientka, L. Conflict of evidence: Carotenoids and other micronutrients in the prevention and treatment of cognitive impairment. Biofactors 2012, 38, 167–171. [Google Scholar] [CrossRef] [PubMed]
- Xin, Y.J.; Yuan, B.; Yu, B.; Wang, Y.Q.; Wu, J.J.; Zhou, W.H.; Qiu, Z. Tet1-mediated DNA demethylation regulates neuronal cell death induced by oxidative stress. Sci. Rep. 2015, 5, 7645. [Google Scholar] [CrossRef] [PubMed]
- Varga, Z.V.; Giricz, Z.; Liaudet, L.; Hasko, G.; Ferdinandy, P.; Pacher, P. Interplay of oxidative, nitrosative/nitrative stress, inflammation, cell death and autophagy in diabetic cardiomyopathy. Biochim. Biophys. Acta 2015, 1852, 232–242. [Google Scholar] [CrossRef] [PubMed]
- Moretti, D.; Del Bello, B.; Allavena, G.; Corti, A.; Signorini, C.; Maellaro, E. Calpain-3 impairs cell proliferation and stimulates oxidative stress-mediated cell death in melanoma cells. PLoS ONE 2015, 10, e0117258. [Google Scholar] [CrossRef] [PubMed]
- Kandola, K.; Bowman, A.; Birch-Machin, M.A. Oxidative stress—A key emerging impact factor in health, ageing, lifestyle and aesthetics. Int. J. Cosmet. Sci. 2015, 37 (Suppl. S2), 1–8. [Google Scholar] [CrossRef] [PubMed]
- Khoubnasabjafari, M.; Ansarin, K.; Jouyban, A. Reliability of malondialdehyde as a biomarker of oxidative stress in psychological disorders. Bioimpacts 2015, 5, 123–127. [Google Scholar] [CrossRef] [PubMed]
- Mons, U.; Muscat, J.E.; Modesto, J.; Richie, J.P.J.; Brenner, H. Effect of smoking reduction and cessation on the plasma levels of the oxidative stress biomarker glutathione-Post-hoc analysis of data from a smoking cessation trial. Free Radic. Biol. Med. 2016, 91, 172–177. [Google Scholar] [CrossRef] [PubMed]
- Varadinova, M.G.; Valcheva-Traykova, M.L.; Boyadjieva, N.I. Effect of Circadian Rhythm Disruption and Alcohol on the Oxidative Stress Level in Rat Brain. Am. J. Ther. 2015, 23, 6. [Google Scholar] [CrossRef] [PubMed]
- Yoshida, A.; Shiotsu-Ogura, Y.; Wada-Takahashi, S.; Takahashi, S.S.; Toyama, T.; Yoshino, F. Blue light irradiation-induced oxidative stress in vivo via ROS generation in rat gingival tissue. J. Photochem. Photobiol. B 2015, 151, 48–53. [Google Scholar] [CrossRef] [PubMed]
- Grether-Beck, S.; Marini, A.; Jaenicke, T.; Krutmann, J. French Maritime Pine Bark Extract (Pycnogenol(R)) Effects on Human Skin: Clinical and Molecular Evidence. Skin Pharmacol. Physiol. 2016, 29, 13–17. [Google Scholar] [CrossRef] [PubMed]
- Schempp, C.M.; Ludtke, R.; Winghofer, B.; Simon, J.C. Effect of topical application of Hypericum perforatum extract (St. John’s wort) on skin sensitivity to solar simulated radiation. Photodermatol. Photoimmunol. Photomed. 2000, 16, 125–128. [Google Scholar] [CrossRef] [PubMed]
- Jung, S.; Darvin, M.E.; Chung, H.S.; Jung, B.; Lee, S.H.; Lenz, K.; Chung, W.S.; Yu, R.X.; Patzelt, A.; Lee, B.N.; et al. Antioxidants in Asian-Korean and caucasian skin: The influence of nutrition and stress. Skin Pharmacol. Physiol. 2014, 27, 293–302. [Google Scholar] [CrossRef] [PubMed]
- Fluhr, J.W.; Caspers, P.; van der Pol, J.A.; Richter, H.; Sterry, W.; Lademann, J.; Darvin, M.E. Kinetics of carotenoid distribution in human skin in vivo after exogenous stress: Disinfectant and wIRA-induced carotenoid depletion recovers from outside to inside. J. Biomed. Opt. 2011, 16, 035002. [Google Scholar] [CrossRef] [PubMed]
- Maeter, H.; Briese, V.; Gerber, B.; Darvin, M.E.; Lademann, J.; Olbertz, D.M. Case study: In vivo stress diagnostics by spectroscopic determination of the cutaneous carotenoid antioxidant concentration in midwives depending on shift work. Laser Phys. Lett. 2013, 10, 105701. [Google Scholar] [CrossRef]
- Darvin, M.E.; Sterry, W.; Lademann, J.; Patzelt, A. Alcohol consumption decreases the protection efficiency of the antioxidant network and increases the risk of sunburn in human skin. Skin Pharmacol. Physiol. 2013, 26, 45–51. [Google Scholar] [CrossRef] [PubMed]
- Vierck, H.B.; Darvin, M.E.; Lademann, J.; Reisshauer, A.; Baack, A.; Sterry, W.; Patzelt, A. The influence of endurance exercise on the antioxidative status of human skin. Eur. J. Appl. Physiol. 2012, 112, 3361–3367. [Google Scholar] [CrossRef] [PubMed]
- Darvin, M.; Patzelt, A.; Gehse, S.; Schanzer, S.; Benderoth, C.; Sterry, W.; Lademann, J. Cutaneous concentration of lycopene correlates significantly with the roughness of the skin. Eur. J. Pharm. Biopharm. 2008, 69, 943–947. [Google Scholar] [CrossRef] [PubMed]
- Darvin, M.; Zastrow, L.; Sterry, W.; Lademann, J. Effect of supplemented and topically applied antioxidant substances on human tissue. Skin Pharmacol. Physiol. 2006, 19, 238–247. [Google Scholar] [CrossRef] [PubMed]
- Darvin, M.; Lademann, J.; Magnussen, B.; Köcher, W. Multiple Spatially Resolved Reflection Spectroscopy for non-invasive determination of carotenoids in human skin. Laser Phys. Lett. 2016, 13, 095601. [Google Scholar] [CrossRef]
- Darvin, M.E.; Meinke, M.C.; Sterry, W.; Lademann, J. Optical methods for noninvasive determination of carotenoids in human and animal skin. J. Biomed. Opt. 2013, 18, 61230. [Google Scholar] [CrossRef] [PubMed]
- Palozza, P.; Serini, S.; Di Nicuolo, F.; Piccioni, E.; Calviello, G. Prooxidant effects of beta-carotene in cultured cells. Mol. Asp. Med. 2003, 24, 353–362. [Google Scholar] [CrossRef]
- Lambert, J.D.; Elias, R.J. The antioxidant and pro-oxidant activities of green tea polyphenols: A role in cancer prevention. Arch. Biochem. Biophys. 2010, 501, 65–72. [Google Scholar] [CrossRef] [PubMed]
- Zhang, P.; Omaye, S.T. DNA strand breakage and oxygen tension: Effects of beta-carotene, alpha-tocopherol and ascorbic acid. Food Chem. Toxicol. 2001, 39, 239–246. [Google Scholar] [CrossRef]
- Palozza, P.; Calviello, G.; Bartoli, G.M. Prooxidant activity of beta-carotene under 100% oxygen pressure in rat liver microsomes. Free Radic. Biol. Med. 1995, 19, 887–892. [Google Scholar] [CrossRef]
- Heinrich, U.; Tronnier, H.; Stahl, W.; Bejot, M.; Maurette, J.M. Antioxidant supplements improve parameters related to skin structure in humans. Skin Pharmacol. Physiol. 2006, 19, 224–231. [Google Scholar] [CrossRef] [PubMed]
- Gogly, B.; Godeau, G.; Gilbert, S.; Legrand, J.M.; Kut, C.; Pellat, B.; Goldberg, M. Morphometric analysis of collagen and elastic fibers in normal skin and gingiva in relation to age. Clin. Oral Investig. 1997, 1, 147–152. [Google Scholar] [PubMed]
- Yasui, T.; Yonetsu, M.; Tanaka, R.; Tanaka, Y.; Fukushima, S.; Yamashita, T.; Ogura, Y.; Hirao, T.; Murota, H.; Araki, T. In vivo observation of age-related structural changes of dermal collagen in human facial skin using collagen-sensitive second harmonic generation microscope equipped with 1250-nm mode-locked Cr:Forsterite laser. J. Biomed. Opt. 2013, 18, 31108. [Google Scholar] [CrossRef] [PubMed]
- Knott, A.; Reuschlein, K.; Lucius, R.; Stab, F.; Wenck, H.; Gallinat, S. Deregulation of versican and elastin binding protein in solar elastosis. Biogerontology 2009, 10, 181–190. [Google Scholar] [CrossRef] [PubMed]
- Sanchez, W.Y.; Obispo, C.; Ryan, E.; Grice, J.E.; Roberts, M.S. Changes in the redox state and endogenous fluorescence of in vivo human skin due to intrinsic and photo-aging, measured by multiphoton tomography with fluorescence lifetime imaging. J. Biomed. Opt. 2013, 18, 061217. [Google Scholar] [CrossRef] [PubMed]
- Koehler, M.J.; Preller, A.; Kindler, N.; Elsner, P.; Konig, K.; Buckle, R.; Kaatz, M. Intrinsic, solar and sunbed-induced skin aging measured in vivo by multiphoton laser tomography and biophysical methods. Skin Res. Technol. 2009, 15, 357–363. [Google Scholar] [CrossRef] [PubMed]
- Karagas, M.R.; Zens, M.S.; Nelson, H.H.; Mabuchi, K.; Perry, A.E.; Stukel, T.A.; Mott, L.A.; Andrew, A.S.; Applebaum, K.M.; Linet, M. Measures of cumulative exposure from a standardized sun exposure history questionnaire: A comparison with histologic assessment of solar skin damage. Am. J. Epidemiol. 2007, 165, 719–726. [Google Scholar] [CrossRef] [PubMed]
- Konig, K. Multiphoton microscopy in life sciences. J. Microsc. (Oxf.) 2000, 200, 83–104. [Google Scholar] [CrossRef]
- Konig, K. Clinical multiphoton tomography. J. Biophotonics 2008, 1, 13–23. [Google Scholar] [CrossRef] [PubMed]
- Sugata, K.; Osanai, O.; Sano, T.; Akiyama, M.; Fujimoto, N.; Tajima, S.; Takema, Y. Evaluation of unique elastic aggregates (elastic globes) in normal facial skin by multiphoton laser scanning tomography. Eur. J. Dermatol. 2015, 25, 138–144. [Google Scholar] [CrossRef] [PubMed]
- Koehler, M.J.; Konig, K.; Elsner, P.; Buckle, R.; Kaatz, M. In vivo assessment of human skin aging by multiphoton laser scanning tomography. Opt. Lett. 2006, 31, 2879–2881. [Google Scholar] [CrossRef] [PubMed]
- Darvin, M.E.; Richter, H.; Ahlberg, S.; Haag, S.F.; Meinke, M.C.; Le Quintrec, D.; Doucet, O.; Lademann, J. Influence of sun exposure on the cutaneous collagen/elastin fibers and carotenoids: Negative effects can be reduced by application of sunscreen. J. Biophotonics 2014, 7, 735–743. [Google Scholar] [CrossRef] [PubMed]
- Springer, S.; Zieger, M.; Bottcher, A.; Lademann, J.; Kaatz, M. Examination of wound healing after curettage by multiphoton tomography of human skin in vivo. Skin Res. Technol. 2017. [Google Scholar] [CrossRef] [PubMed]
- Adur, J.; Carvalho, H.F.; Cesar, C.L.; Casco, V.H. Nonlinear optical microscopy signal processing strategies in cancer. Cancer Inform. 2014, 13, 67–76. [Google Scholar] [CrossRef] [PubMed]
- Cicchi, R.; Kapsokalyvas, D.; De Giorgi, V.; Maio, V.; Van Wiechen, A.; Massi, D.; Lotti, T.; Pavone, F.S. Scoring of collagen organization in healthy and diseased human dermis by multiphoton microscopy. J. Biophotonics 2010, 3, 34–43. [Google Scholar] [CrossRef] [PubMed]
- Langton, A.K.; Halai, P.; Griffiths, C.E.; Sherratt, M.J.; Watson, R.E. The impact of intrinsic ageing on the protein composition of the dermal-epidermal junction. Mech. Ageing Dev. 2016, 156, 14–16. [Google Scholar] [CrossRef] [PubMed]
- Shirshin, E.A.; Gurfinkel, Y.I.; Priezzhev, A.V.; Fadeev, V.V.; Lademann, J.; Darvin, M.E. Two-photon autofluorescence lifetime imaging of human skin papillary dermis in vivo: Assessment of blood capillaries and structural proteins localization. Sci. Rep. (UK) 2017, 7, 1171. [Google Scholar] [CrossRef] [PubMed]
- Meinke, M.C.; Lohan, S.B.; Kocher, W.; Magnussen, B.; Darvin, M.E.; Lademann, J. Multiple spatially resolved reflection spectroscopy to monitor cutaneous carotenoids during supplementation of fruit and vegetable extracts in vivo. Skin Res. Technol. 2017. [Google Scholar] [CrossRef] [PubMed]
- Meinke, M.C.; Darvin, M.E.; Vollert, H.; Lademann, J. Bioavailability of natural carotenoids in human skin compared to blood. Eur. J. Pharm. Biopharm. 2010, 76, 269–274. [Google Scholar] [CrossRef] [PubMed]
- Meinke, M.C.; Friedrich, A.; Tscherch, K.; Haag, S.F.; Darvin, M.E.; Vollert, H.; Groth, N.; Lademann, J.; Rohn, S. Influence of dietary carotenoids on radical scavenging capacity of the skin and skin lipids. Eur. J. Pharm. Biopharm. 2013, 84, 365–373. [Google Scholar] [CrossRef] [PubMed]
- Fitzpatrick, T.B. The validity and practicality of sun-reactive skin types I through VI. Arch. Dermatol. 1988, 124, 869–871. [Google Scholar] [CrossRef] [PubMed]
- Andree, S.; Reble, C.; Helfmann, J. Spectral in vivo signature of carotenoids in visible light diffuse reflectance from skin in comparison to ex vivo absorption spectra. Photonics Lasers Med. 2013, 2, 3. [Google Scholar] [CrossRef]
- Darvin, M.E.; Gersonde, I.; Meinke, M.; Sterry, W.; Lademann, J. Non-invasive in vivo determination of the carotenoids beta-carotene and lycopene concentrations in the human skin using the Raman spectroscopic method. J. Phys. D Appl. Phys. 2005, 38, 2696–2700. [Google Scholar] [CrossRef]
- Lin, S.J.; Wu, R., Jr.; Tan, H.Y.; Lo, W.; Lin, W.C.; Young, T.H.; Hsu, C.J.; Chen, J.S.; Jee, S.H.; Dong, C.Y. Evaluating cutaneous photoaging by use of multiphoton fluorescence and second-harmonic generation microscopy. Opt. Lett. 2005, 30, 2275–2277. [Google Scholar] [CrossRef] [PubMed]
- Darvin, M.E.; Patzelt, A.; Knorr, F.; Blume-Peytavi, U.; Sterry, W.; Lademann, J. One-year study on the variation of carotenoid antioxidant substances in living human skin: Influence of dietary supplementation and stress factors. J. Biomed. Opt. 2008, 13, 044028. [Google Scholar] [CrossRef] [PubMed]
- Baillie, L.; Askew, D.; Douglas, N.; Soyer, H.P. Strategies for assessing the degree of photodamage to skin: A systematic review of the literature. Br. J. Dermatol. 2011, 165, 735–742. [Google Scholar] [CrossRef] [PubMed]
- Proksch, E.; Schunck, M.; Zague, V.; Segger, D.; Degwert, J.; Oesser, S. Oral intake of specific bioactive collagen peptides reduces skin wrinkles and increases dermal matrix synthesis. Skin Pharmacol. Physiol. 2014, 27, 113–119. [Google Scholar] [CrossRef] [PubMed]
- Manickavasagam, A.; Hirvonen, L.M.; Melita, L.N.; Chong, E.Z.; Cook, R.J.; Bozecc, L.; Festy, F. Multimodal optical characterisation of collagen photodegradation by femtosecond infrared laser ablation. Analyst 2014, 139, 6135–6143. [Google Scholar] [CrossRef] [PubMed]

| SAAID Cheek | SAAID | Carotenoids | |
|---|---|---|---|
| Forearm | CaroLED | ||
| SAAID forearm | |||
| Correlation according to Pearson | 0.504 ** | 1 | |
| Significance | <0.001 | ||
| N | 76 | 77 | |
| Carotenoids CaroLED | |||
| Correlation according to Pearson | 0.279 * | 0.295 ** | 1 |
| Significance | 0.014 | 0.008 | |
| N | 77 | 80 | 81 |
| Carotenoids MSRRS | |||
| Correlation according to Pearson | 0.328 ** | 0.225 * | 0.853 ** |
| Significance | 0.004 | 0.023 | <0.001 |
| N | 77 | 80 | 81 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Meinke, M.C.; Nowbary, C.K.; Schanzer, S.; Vollert, H.; Lademann, J.; Darvin, M.E. Influences of Orally Taken Carotenoid-Rich Curly Kale Extract on Collagen I/Elastin Index of the Skin. Nutrients 2017, 9, 775. https://doi.org/10.3390/nu9070775
Meinke MC, Nowbary CK, Schanzer S, Vollert H, Lademann J, Darvin ME. Influences of Orally Taken Carotenoid-Rich Curly Kale Extract on Collagen I/Elastin Index of the Skin. Nutrients. 2017; 9(7):775. https://doi.org/10.3390/nu9070775
Chicago/Turabian StyleMeinke, Martina C., Ceylan K. Nowbary, Sabine Schanzer, Henning Vollert, Jürgen Lademann, and Maxim E. Darvin. 2017. "Influences of Orally Taken Carotenoid-Rich Curly Kale Extract on Collagen I/Elastin Index of the Skin" Nutrients 9, no. 7: 775. https://doi.org/10.3390/nu9070775
APA StyleMeinke, M. C., Nowbary, C. K., Schanzer, S., Vollert, H., Lademann, J., & Darvin, M. E. (2017). Influences of Orally Taken Carotenoid-Rich Curly Kale Extract on Collagen I/Elastin Index of the Skin. Nutrients, 9(7), 775. https://doi.org/10.3390/nu9070775