Comparison of Performance in the Six-Minute Walk Test (6MWT) between Overweight/Obese and Normal-Weight Children and Association with Haemodynamic Parameters: A Cross-Sectional Study in Four Primary Schools
Abstract
1. Introduction
2. Materials and Methods
2.1. Population Selection
2.2. Anthropometric and Haemodynamic Measurements
2.3. 6MWT
2.4. Laboratory Measurements
2.5. Questionnaires
2.6. Food Frequency Questionnaire (FFQ)
2.7. Physical Activity Questionnaire
2.8. Statistics
3. Results
Linear Regressions
4. Discussion
Limitations of the Study
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Wang, Y.; Lim, H. The Global Childhood Obesity Epidemic and the Association between Socio-Economic Status and Childhood Obesity. Int. Rev. Psychiatry 2012, 24, 176–188. [Google Scholar] [CrossRef]
- Buoncristiano, M.; Spinelli, A.; Williams, J.; Nardone, P.; Rito, A.I.; García-Solano, M.; Grøholt, E.K.; Gutiérrez-González, E.; Klepp, K.I.; Starc, G.; et al. Childhood Overweight and Obesity in Europe: Changes from 2007 to 2017. Obes. Rev. 2021, 22, e13226. [Google Scholar] [CrossRef]
- Fryar, C.D.; Carroll, M.D.; Afful, J. Prevalence of Overweight, Obesity, and Severe Obesity among Children and Adolescents Aged 2–19 Years: United States, 1963–1965 through 2017–2018. Health E-Stats 2020, 1–3. [Google Scholar] [CrossRef]
- McPhee, P.G.; Singh, S.; Morrison, K.M. Childhood Obesity and Cardiovascular Disease Risk: Working toward Solutions. Can. J. Cardiol. 2020, 36, 1352–1361. [Google Scholar] [CrossRef]
- Umer, A.; Kelley, G.A.; Cottrell, L.E.; Giacobbi, P.; Innes, K.E.; Lilly, C.L. Childhood Obesity and Adult Cardiovascular Disease Risk Factors: A Systematic Review with Meta-Analysis. BMC Public Health 2017, 17, 683. [Google Scholar] [CrossRef]
- Bonafini, S.; Giontella, A.; Tagetti, A.; Montagnana, M.; Benati, M.; Danese, E.; Minuz, P.; Maffeis, C.; Antoniazzi, F.; Fava, C. Markers of Subclinical Vascular Damages Associate with Indices of Adiposity and Blood Pressure in Obese Children. Hypertens. Res. 2019, 42, 400–410. [Google Scholar] [CrossRef]
- Paduano, S.; Greco, A.; Borsari, L.; Salvia, C.; Tancredi, S.; Pinca, J.; Midili, S.; Tripodi, A.; Borella, P.; Marchesi, I. Physical and Sedentary Activities and Childhood Overweight/Obesity: A Cross-Sectional Study among First-Year Children of Primary Schools in Modena, Italy. Int. J. Environ. Res. Public Health 2021, 18, 3221. [Google Scholar] [CrossRef]
- Ding, C.; Fan, J.; Yuan, F.; Feng, G.; Gong, W.; Song, C.; Ma, Y.; Chen, Z.; Liu, A. Association between Physical Activity, Sedentary Behaviors, Sleep, Diet, and Adiposity among Children and Adolescents in China. Obes. Facts 2022, 15, 26–35. [Google Scholar] [CrossRef]
- Rousham, E.K.; Goudet, S.; Markey, O.; Griffiths, P.; Boxer, B.; Carroll, C.; Petherick, E.S.; Pradeilles, R. Unhealthy Food and Beverage Consumption in Children and Risk of Overweight and Obesity: A Systematic Review and Meta-Analysis. Adv. Nutr. 2022, 13, 1669–1696. [Google Scholar] [CrossRef]
- Barnett, T.A.; Kelly, C.A.S.; Young, D.R.; Perry, C.K.; Pratt, C.A.; Edwards, N.M.; Rao, G.; Vos, M.B. Sedentary Behaviors in Today’s Youth: Approaches to the Prevention and Management of Childhood Obesity a Scientific Statement from the American Heart Association. Circulation 2018, 138, E142–E159. [Google Scholar] [CrossRef]
- ATS Committee on Proficiency Standards for Clinical Pulmonary Function Laboratories. ATS Statement: Guidelines for the Six-Minute Walk Test. Am. J. Respir Crit. Care Med. 2002, 166, 111–117. [Google Scholar] [CrossRef]
- Ingle, L.; Cleland, J.G.; Clark, A.L. The Long-Term Prognostic Significance of 6-Minute Walk Test Distance in Patients with Chronic Heart Failure. BioMed Res. Int. 2014, 2014, 505969. [Google Scholar] [CrossRef]
- Miyamoto, S.; Nagaya, N.; Satoh, T.; Kyotani, S.; Sakamaki, F.; Fujita, M.; Nakanishi, N.; Miyatake, K. Clinical Correlates and Prognostic Significance of Six-Minute Walk Test in Patients with Primary Pulmonary Hypertension: Comparison with Cardiopulmonary Exercise Testing. Am. J. Respir Crit. Care Med. 2000, 161, 487–492. [Google Scholar] [CrossRef]
- Salazar, G.; Vásquez, F.; Concha, F.; Leyton, B.; Kain, J. The Influence of Body Composition on the Six-Minute Walk Test in Chilean Preschool and School Children. Nutr. Hosp. 2022, 39, 27–32. [Google Scholar] [CrossRef]
- D’silva, C.; Vaishali, K.; Venkatesan, P. Six-Minute Walk Test-Normal Values of School Children Aged 7–12 y in India: A Cross-Sectional Study. Indian J. Pediatr. 2012, 79, 597–601. [Google Scholar] [CrossRef]
- Ulrich, S.; Hildenbrand, F.F.; Treder, U.; Fischler, M.; Keusch, S.; Speich, R.; Fasnacht, M. Reference Values for the 6-Minute Walk Test in Healthy Children and Adolescents in Switzerland. BMC Pulm. Med. 2013, 13, 49. [Google Scholar] [CrossRef]
- De Faria Santarém, G.C.; De Cleva, R.; Santo, M.A.; Bernhard, A.B.; Gadducci, A.V.; D’Andrea Greve, J.M.; Silva, P.R.S. Correlation between Body Composition and Walking Capacity in Severe Obesity. PLoS ONE 2015, 10, e0130268. [Google Scholar] [CrossRef]
- Makni, E.; Hachana, Y.; Elloumi, M. Allometric Association between Six-Minute Walk Distance and Both Body Size and Shape in Young Obese Girls. Children 2023, 10, 658. [Google Scholar] [CrossRef]
- Ekman, M.J.; Klintenberg, M.; Björck, U.; Norström, F. Six-Minute Walk Test before and after a Weight Reduction Program in Obese Subjects. Obesity 2013, 21, E236–E243. [Google Scholar] [CrossRef]
- de Souza, S.A.F.; Faintuch, J.; Fabris, S.M.; Nampo, F.K.; Luz, C.; Fabio, T.L.; Sitta, I.S.; de Batista Fonseca, I.C. Six-Minute Walk Test: Functional Capacity of Severely Obese before and after Bariatric Surgery. Surg. Obes. Relat. Dis. 2009, 5, 540–543. [Google Scholar] [CrossRef]
- Morinder, G.; Mattsson, E.; Sollander, C.; Marcus, C.; Larsson, U.E. Six-Minute Walk Test in Obese Children and Adolescents: Reproducibility and Validity. Physiother. Res. Int. 2009, 14, 91–104. [Google Scholar] [CrossRef]
- Schutte, R.; Thijs, L.; Asayama, K.; Boggia, J.; Li, Y.; Hansen, T.W.; Liu, Y.P.; Kikuya, M.; Björklund-Bodegård, K.; Ohkubo, T.; et al. Double Product Reflects the Predictive Power of Systolic Pressure in the General Population: Evidence from 9937 Participants. Am. J. Hypertens. 2013, 26, 665–672. [Google Scholar] [CrossRef]
- Yazdani, B.; Kleber, M.E.; Yücel, G.; Delgado, G.E.; Benck, U.; Krüger, B.; März, W.; Krämer, B.K. Association of Double Product and Pulse Pressure with Cardiovascular and All-Cause Mortality in the LURIC Study. J. Clin. Hypertens. 2020, 22, 2332–2342. [Google Scholar] [CrossRef]
- Giontella, A.; Bonafini, S.; Tagetti, A.; Bresadola, I.; Minuz, P.; Gaudino, R.; Cavarzere, P.; Ramaroli, D.A.; Marcon, D.; Branz, L.; et al. Relation between Dietary Habits, Physical Activity, and Anthropometric and Vascular Parameters in Children Attending the Primary School in the Verona South District. Nutrients 2019, 11, 1070. [Google Scholar] [CrossRef]
- Cole, T.J.; Bellizzi, M.C.; Flegal, K.M.; Dietz, W.H. Establishing a Standard Definition for Child Overweight and Obesity Worldwide: International Survey. BMJ 2000, 320, 1240–1243. [Google Scholar] [CrossRef]
- Valerio, G.; Maffeis, C.; Saggese, G.; Ambruzzi, M.A.; Balsamo, A.; Bellone, S.; Bergamini, M.; Bernasconi, S.; Bona, G.; Calcaterra, V.; et al. Diagnosis, Treatment and Prevention of Pediatric Obesity: Consensus Position Statement of the Italian Society for Pediatric Endocrinology and Diabetology and the Italian Society of Pediatrics. Ital. J. Pediatr. 2018, 44, 88. [Google Scholar] [CrossRef] [PubMed]
- Stergiou, G.S.; Yiannes, N.G.; Rarra, V.C. Validation of the Omron 705 IT Oscillometric Device for Home Blood Pressure Measurement in Children and Adolescents: The Arsakion School Study. Blood Press. Monit. 2006, 11, 229–234. [Google Scholar] [CrossRef]
- Lurbe, E.; Agabiti-Rosei, E.; Cruickshank, J.K.; Dominiczak, A.; Erdine, S.; Hirth, A.; Invitti, C.; Litwin, M.; Mancia, G.; Pall, D.; et al. 2016 European Society of Hypertension Guidelines for the Management of High Blood Pressure in Children and Adolescents. J. Hypertens. 2016, 34, 1887–1920. [Google Scholar] [CrossRef] [PubMed]
- Lockyer, M.G.; Fu, K.; Edwards, R.M.; Collymore, L.; Thomas, J.; Hill, T.; Devaraj, S. Evaluation of the Nova StatStrip Glucometer in a Pediatric Hospital Setting. Clin. Biochem. 2014, 47, 840–843. [Google Scholar] [CrossRef] [PubMed]
- Rapi, S.; Bazzini, C.; Tozzetti, C.; Sbolci, V.; Modesti, P.A. Point-of-Care Testing of Cholesterol and Triglycerides for Epidemiologic Studies: Evaluation of the Multicare-in System. Transl. Res. 2009, 153, 71–76. [Google Scholar] [CrossRef] [PubMed]
- Sarter, B.; Kelsey, K.S.; Schwartz, T.A.; Harris, W.S. Blood Docosahexaenoic Acid and Eicosapentaenoic Acid in Vegans: Associations with Age and Gender and Effects of an Algal-Derived Omega-3 Fatty Acid Supplement. Clin. Nutr. 2015, 34, 212–218. [Google Scholar] [CrossRef] [PubMed]
- Bonafini, S.; Giontella, A.; Tagetti, A.; Bresadola, I.; Gaudino, R.; Cavarzere, P.; Ramaroli, D.A.; Branz, L.; Marcon, D.; Pietrobelli, A.; et al. Fatty Acid Profile and Desaturase Activities in 7–10-Year-Old Children Attending Primary School in Verona South District: Association between Palmitoleic Acid, SCD-16, Indices of Adiposity, and Blood Pressure. Int. J. Mol. Sci. 2020, 21, 3899. [Google Scholar] [CrossRef] [PubMed]
- Johnston, D.T.; Deuster, P.A.; Harris, W.S.; Macrae, H.; Dretsch, M.N. Red Blood Cell Omega-3 Fatty Acid Levels and Neurocognitive Performance in Deployed U.S. Servicemembers. Nutr. Neurosci. 2013, 16, 30–38. [Google Scholar] [CrossRef] [PubMed]
- Rockett, H.R.; Breitenbach, M.; Frazier, A.L.; Witschi, J.; Wolf, A.M.; Field, A.E.; Colditz, G.A. Validation of a Youth/Adolescent Food Frequency Questionnaire. Prev. Med. 1997, 26, 808–816. [Google Scholar] [CrossRef] [PubMed]
- Manios, Y.; Androutsos, O.; Moschonis, G.; Birbilis, M.; Maragkopoulou, K.; Giannopoulou, A.; Argyri, E.; Kourlaba, G. Criterion Validity of the Physical Activity Questionnaire for Schoolchildren (PAQ-S) in Assessing Physical Activity Levels: The Healthy Growth Study. J. Sports Med. Phys. Fit. 2013, 53, 235–253. [Google Scholar]
- Nystoriak, M.A.; Bhatnagar, A. Cardiovascular Effects and Benefits of Exercise. Front. Cardiovasc. Med. 2018, 5, 135. [Google Scholar] [CrossRef] [PubMed]
- Niebauer, J.; Börjesson, M.; Carre, F.; Caselli, S.; Palatini, P.; Quattrini, F.; Serratosa, L.; Emilio Adami, P.; Biffi, A.; Pressler, A.; et al. Recommendations for Participation in Competitive Sports of Athletes with Arterial Hypertension: A Position Statement from the Sports Cardiology Section of the European Association of Preventive Cardiology (EAPC). Eur. Heart J. 2018, 39, 3664–3671. [Google Scholar] [CrossRef] [PubMed]
- Mancia, G.; Kreutz, R.; Brunström, M.; Burnier, M.; Grassi, G.; Januszewicz, A.; Muiesan, M.L.; Tsioufis, K.; Agabiti-Rosei, E.; Algharably, E.A.E.; et al. 2023 ESH Guidelines for the Management of Arterial Hypertension The Task Force for the Management of Arterial Hypertension of the European Society of Hypertension: Endorsed by the International Society of Hypertension (ISH) and the European Renal Association (ERA). J. Hypertens. 2023, 41, 1874–2071. [Google Scholar] [CrossRef]
- Schultz, M.G.; Otahal, P.; Cleland, V.J.; Blizzard, L.; Marwick, T.H.; Sharman, J.E. Exercise-Induced Hypertension, Cardiovascular Events, and Mortality in Patients Undergoing Exercise Stress Testing: A Systematic Review and Meta-Analysis. Am. J. Hypertens. 2013, 26, 357–366. [Google Scholar] [CrossRef]
- Laurent, S.; Boutouyrie, P. The Structural Factor of Hypertension. Circ. Res. 2015, 116, 1007–1021. [Google Scholar] [CrossRef]
- Cote, A.T.; Harris, K.C.; Panagiotopoulos, C.; Sandor, G.G.S.; Devlin, A.M. Childhood Obesity and Cardiovascular Dysfunction. J. Am. Coll. Cardiol. 2013, 62, 1309–1319. [Google Scholar] [CrossRef] [PubMed]
- Dourado, V.Z.; McBurnie, M.A. Allometric Scaling of 6-Min Walking Distance by Body Mass as a Standardized Measure of Exercise Capacity in Healthy Adults. Eur. J. Appl. Physiol. 2012, 112, 2503–2510. [Google Scholar] [CrossRef] [PubMed]
- Beriault, K.; Carpentier, A.C.; Gagnon, C.; Ménard, J.; Baillargeon, J.P.; Ardilouze, J.L.; Langlois, M.F. Reproducibility of the 6-Minute Walk Test in Obese Adults. Int. J. Sports Med. 2009, 30, 725–727. [Google Scholar] [CrossRef] [PubMed]
- Provencher, S.; Chemla, D.; Hervé, P.; Sitbon, O.; Humbert, M.; Simonneau, G. Heart Rate Responses during the 6-Minute Walk Test in Pulmonary Arterial Hypertension. Eur. Respir. J. 2006, 27, 114–120. [Google Scholar] [CrossRef] [PubMed]
- Itagi, A.H.; Jayalakshmi, M.; Yunus, G. Effect of Obesity on Cardiovascular Responses to Submaximal Treadmill Exercise in Adult Males. J. Fam. Med. Prim. Care 2020, 9, 4673. [Google Scholar] [CrossRef] [PubMed]
- Cavuoto, L.A.; Maikala, R.V. Obesity and the Role of Short Duration Submaximal Work on Cardiovascular and Cerebral Hemodynamics. PLoS ONE 2016, 11, e0153826. [Google Scholar] [CrossRef]
- Moore, S.M.; Berrones, A.J.; Clasey, J.L.; Abel, M.G.; Fleenor, B.S. Arterial Hemodynamics Are Impaired at Rest and Following Acute Exercise in Overweight Young Men. Vasc. Med. 2016, 21, 497–505. [Google Scholar] [CrossRef]
- Bunsawat, K.; Ranadive, S.M.; Lane-Cordova, A.D.; Yan, H.; Kappus, R.M.; Fernhall, B.; Baynard, T. The Effect of Acute Maximal Exercise on Postexercise Hemodynamics and Central Arterial Stiffness in Obese and Normal-Weight Individuals. Physiol. Rep. 2017, 5, e13226. [Google Scholar] [CrossRef]
- Huang, Z.; Chen, G.; Wang, X.; Zang, Y.; Yue, Q.; Cai, Z.; Ding, X.; Chen, Z.; Cai, Z.; Wu, K.; et al. The Effect of Acute Aerobic Exercise on Arterial Stiffness in Individuals with Different Body Fat Percentages: A Cross-Sectional Study. Front. Cardiovasc. Med. 2023, 9, 1072191. [Google Scholar] [CrossRef]
- Arias Téllez, M.J.; Soto-Sánchez, J.; Weisstaub, S.G. Condición Física, Riesgo Cardiometabólico y Frecuencia Cardiaca de Recuperación En Escolares Chilenos. Nutr. Hosp. 2018, 35, 44–49. [Google Scholar] [CrossRef]
- Thielecke, F.; Blannin, A. Omega-3 Fatty Acids for Sport Performance—Are They Equally Beneficial for Athletes and Amateurs? A Narrative Review. Nutrients 2020, 12, 3712. [Google Scholar] [CrossRef]
- Mozaffarian, D.; Katan, M.B.; Ascherio, A.; Stampfer, M.J.; Willett, W.C. Trans Fatty Acids and Cardiovascular Disease. N. Engl. J. Med. 2006, 354, 1601–1613. [Google Scholar] [CrossRef]
| Characteristics | Normal-Weight (NW) n = 194 | Overweight/Obese (OW&OB) n = 100 | p-Value |
|---|---|---|---|
| Age, yr | 8.7 ± 0.7 | 8.6 ± 0.7 | 0.143 |
| Male, % | 48.5 | 53.0 | |
| Anthropometric and Body Composition (via impedenzometry) | |||
| BMI, kg/m2 | 16.30 ± 1.7 | 21.8 ± 3.1 | <0.001 |
| BMI, percentile for age | 46.7 ± 26.2 | 93.6 ± 3.8 | <0.001 |
| Waist/height | 0.43 ± 0.06 | 0.51 ± 0.08 | <0.001 |
| Waist/hip | 0.85 ± 0.08 | 1.00 ± 0.96 | <0.001 |
| BSA, m2 | 1.06 ± 0.11 | 1.27 ± 0.14 | <0.001 |
| FAT mass, kg | 15.7 ± 5.1 | 12.9 ± 6.1 | <0.001 |
| FAT-FREE mass, kg | 37.5 ± 25.0 | 29.5 ± 5.2 | <0.001 |
| FFM/FM | 31.3 ± 6.3 | 2.7 ± 1.1 | <0.001 |
| TBW, kg | 27.5 ± 18.4 | 21.9 ± 3.1 | <0.001 |
| 6MWT distance, m | 554.6 ± 2.6 | 535.7 ± 53.8 | 0.007 |
| Pre-6MWT Haemodynamic Measurements | |||
| SBP, mmHg | 109.1 ± 10.5 | 113.4 ± 8.2 | <0.001 |
| z-SBP | 0.86 ± 0.91 | 1.13 ± 0.76 | 0.010 |
| DBP, mmHg | 66.1 ± 7.8 | 67.8 ± 7.8 | 0.092 |
| z-DBP | 0.64 ± 0.71 | 0.72 ± 0.76 | 0.316 |
| HR, bpm | 80.3 ± 11.5 | 80.6 ± 11.8 | 0.818 |
| RPP, mmHg * bpm | 8797.6 ± 1750.3 | 9157.4 ± 1657.3 | 0.043 |
| SatO2 | 98.8 ± 0.60 | 98.6 ± 1.5 | 0.228 |
| Post-6MWT Haemodynamic Measurements | |||
| SBP, mmHg | 119.3 ± 12.2 | 126.4 ± 11.1 | <0.001 |
| z-SBP | 1.8 ± 1.1 | 2.4 ± 1.0 | <0.001 |
| DBP, mmHg | 68.2 ± 7.0 | 69.6 ± 7.8 | 0.143 |
| z-DBP | 0.81 ± 0.63 | 0.89 ± 0.70 | 0.414 |
| HR, bpm | 86.6 ± 13.0 | 95.4 ± 17.2 | 0.004 |
| RPP, mmHg * bpm | 10,366.5 ± 2103.4 | 11,593.0 ± 2405.3 | <0.001 |
| SatO2 % | 98.8 ± 0.44 | 98.4 ± 0.9 | <0.001 |
| Delta (Post–Pre-6MWT) Haemodynamic Measurements | |||
| Delta PAS | 10.15 ± 9.80 | 13.0 ± 11.17 | 0.032 |
| Delta PAD | 1.09 ± 8.32 | 1.85 ± 7.45 | 0.792 |
| Delta HR | 6.32 ± 12.14 | 10.76 ± 11.56 | 0.003 |
| Delta RPP | 1574.5 ± 1927.4 | 2436.3 ± 2042.0 | <0.001 |
| Delta SatO2 | 0.05 ± 0.44 | 0.17 ± 1.58 | 0.519 |
| Physical Activity (from the PAQ-C Questionnaire) | |||
| Sedentary activity, MET * min/week | 3591.2 ± 3919 | 2968.7 ± 4154.1 | 0.236 |
| Intense physical activity, MET * min/week | 1606.3 ± 1367.8 | 1766.2 ± 2697 ± 0 | 0.591 |
| Post-6MWT SBP | Post-6MWT Z-SBP | Post-6MWT DBP | Post-6MWT Z-DBP | Post-6MWT HR | Post-6MWT RPP | Post-6MWT SatO2 | 6MWT Distance | |
|---|---|---|---|---|---|---|---|---|
| BMI, kg/m2 | 0.361 ** | 0.318 ** | 0.209 ** | 0.145 * | 0.228 ** | 0.345 ** | −0.313 ** | −0.212 ** |
| z-BMI | 0.324 ** | 0.291 ** | 0.161 ** | 0.123 * | 0.189 ** | 0.294 ** | −0.267 ** | −0.192 ** |
| Waist/height | 0.175 ** | 0.160 ** | 0.120 * | 0.094 | 0.150* | 0.193 ** | 0.081 | −0.089 |
| Waist/hip | 0.023 | 0.012 | −0.09 | −0.006 | 0.017 | 0.018 | 0.128 | −0.058 |
| BSA, m2 | 0.480 ** | 0.352 ** | 0.205 ** | 0.046 | 0.165 ** | 0.354 ** | −0.234 ** | −0.120 * |
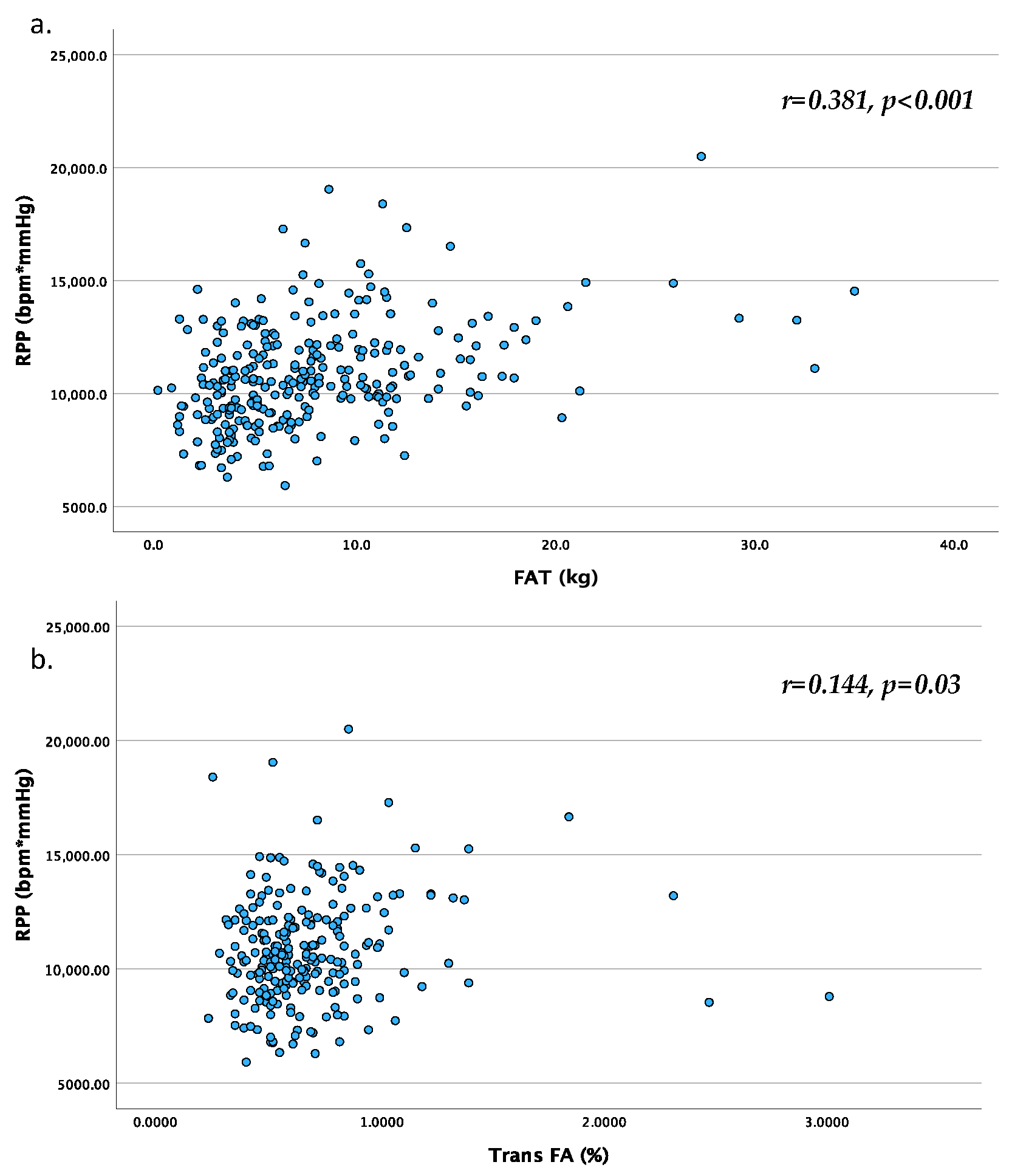
| FAT, kg | 0.393 ** | 0.163 ** | 0.241 ** | 0.163 ** | 0.252 ** | 0.381 ** | −0.354 ** | −0.194 ** |
| FFM, kg | 0.375 ** | 0.247 ** | 0.099 | −0.047 | 0.062 | 0.236 ** | −0.034 | −0.036 |
| FFM/FM | −0.305 ** | −0.288 ** | −0.157 ** | −0.120 * | −0.113 | −0.232 ** | 0.149 | 0.114 |
| TBW, kg | 0.402 ** | 0.262 ** | 0.094 | −0.070 | 0.060 | 0.239 ** | −0.088 | −0.071 |
| Post-6MWT SBP | Post-6MWT Z-SBP | Post-6MWT DBP | Post-6MWT Z-DBP | Post-6MWT HR | Post-6MWT RPP | Post-6MWT SatO2 | 6MWT Distance | |
|---|---|---|---|---|---|---|---|---|
| Healthy Pattern | 0.063 | 0.049 | −0.002 | −0.031 | 0.031 | 0.056 | 0.052 | 0.052 |
| Unhealthy Pattern | 0.066 | 0.047 | 0.067 | 0.054 | 0.009 | 0.029 | −0.039 | −0.039 |
| Sedentary Activity (MET * min/week) | 0.079 | 0.088 | −0.039 | −0.032 | −0.038 | 0.009 | 0.083 | 0.083 |
| Intense Physical Activity (MET * min/week) | −0.012 | 0.001 | −0.081 | −0.066 | 0.039 | 0.031 | −0.007 | −0.007 |
| Post-6MWT SBP | Post-6MWT Z-SBP | Post-6MWT DBP | Post-6MWT Z-DBP | Post-6MWT HR | Post-6MWT RPP | Post-6MWT SatO2 | 6MWT Distance | |
|---|---|---|---|---|---|---|---|---|
| Omega 6 FA, % | 0.002 | −0.016 | −0.026 | −0.033 | 0.028 | 0.019 | −0.005 | −0.059 |
| Omega 3 FA, % | 0.027 | −0.023 | 0.111 | 0.089 | 0.016 | 0.019 | −0.043 | 0.159 * |
| Omega 9 FA, % | 0.061 | 0.098 | −0.020 | 0.002 | 0.011 | 0.038 | −0.121 | −0.073 |
| Saturated FA, % | −0.085 | −0.084 | −0.021 | −0.019 | −0.06 | −0.088 | 0.098 | 0.055 |
| Trans FA, % | 0.143 * | 0.142 * | 0.232 | 0.031 | 0.101 | 0.144 * | −0.095 | 0.140 * |
| Glucose, mg/dL | 0.061 | 0.050 | −0.029 | −0.030 | −0.072 | −0.031 | −0.023 | −0.033 |
| Triglycerides mg/dL | 0.111 | 0.115 | 0.238 ** | 0.242 ** | 0.080 | 0.112 | −0.250 * | 0.046 |
| Cholesterol mg/dL | −0.135 | −0.096 | −0.071 | 0.003 | −0.113 | −0.153 * | 0.197 | 0.066 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Giontella, A.; Tagetti, A.; Bonafini, S.; Marcon, D.; Cattazzo, F.; Bresadola, I.; Antoniazzi, F.; Gaudino, R.; Cavarzere, P.; Montagnana, M.; et al. Comparison of Performance in the Six-Minute Walk Test (6MWT) between Overweight/Obese and Normal-Weight Children and Association with Haemodynamic Parameters: A Cross-Sectional Study in Four Primary Schools. Nutrients 2024, 16, 356. https://doi.org/10.3390/nu16030356
Giontella A, Tagetti A, Bonafini S, Marcon D, Cattazzo F, Bresadola I, Antoniazzi F, Gaudino R, Cavarzere P, Montagnana M, et al. Comparison of Performance in the Six-Minute Walk Test (6MWT) between Overweight/Obese and Normal-Weight Children and Association with Haemodynamic Parameters: A Cross-Sectional Study in Four Primary Schools. Nutrients. 2024; 16(3):356. https://doi.org/10.3390/nu16030356
Chicago/Turabian StyleGiontella, Alice, Angela Tagetti, Sara Bonafini, Denise Marcon, Filippo Cattazzo, Irene Bresadola, Franco Antoniazzi, Rossella Gaudino, Paolo Cavarzere, Martina Montagnana, and et al. 2024. "Comparison of Performance in the Six-Minute Walk Test (6MWT) between Overweight/Obese and Normal-Weight Children and Association with Haemodynamic Parameters: A Cross-Sectional Study in Four Primary Schools" Nutrients 16, no. 3: 356. https://doi.org/10.3390/nu16030356
APA StyleGiontella, A., Tagetti, A., Bonafini, S., Marcon, D., Cattazzo, F., Bresadola, I., Antoniazzi, F., Gaudino, R., Cavarzere, P., Montagnana, M., Pietrobelli, A., Maffeis, C., Minuz, P., & Fava, C. (2024). Comparison of Performance in the Six-Minute Walk Test (6MWT) between Overweight/Obese and Normal-Weight Children and Association with Haemodynamic Parameters: A Cross-Sectional Study in Four Primary Schools. Nutrients, 16(3), 356. https://doi.org/10.3390/nu16030356







