Elimination Diets in Lactating Mothers of Infants with Food Allergy
Abstract
1. Introduction
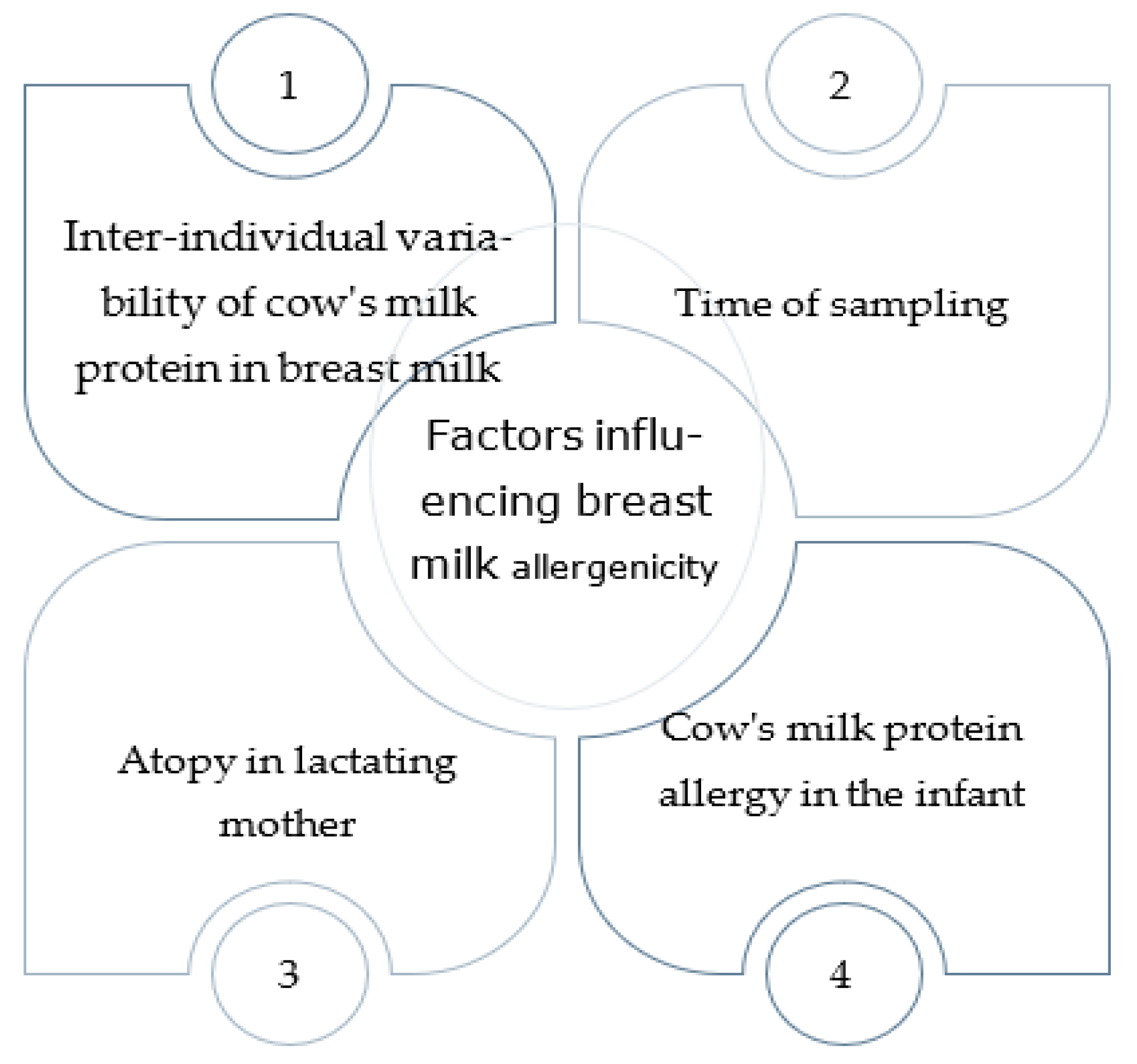
2. Transfer of Food Allergens into Human Milk
3. Management of Suspected IgE-Mediated FAs in Exclusively Breastfed Infants
4. Management of Suspected Non-IgE-Mediated FAs in Exclusively Breastfed Infants
4.1. Gastrointestinal Clinical Manifestations and Eczema in Exclusively Breastfed Infants
4.2. Food-Protein-Induced Allergic Proctocolitis in Exclusively Breastfed Infants
4.3. Food-Protein-Induced Enterocolitis Syndrome in Exclusively Breastfed Infants
4.4. Food Protein Enteropathy and Gastritis in Exclusively Breastfed Infants
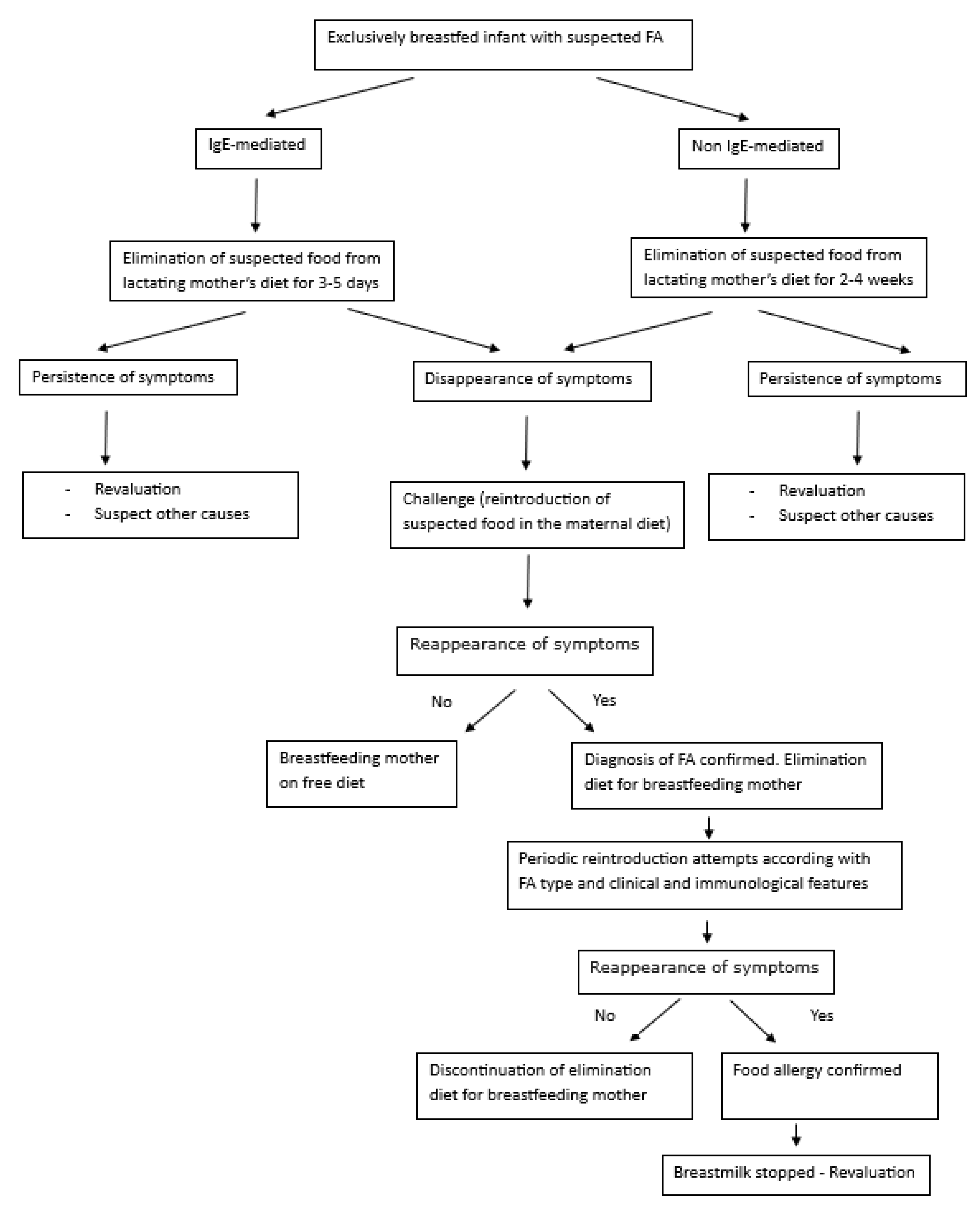
5. Management of a Suspected Food Allergy in Exclusively Breastfed Infants
6. Conclusions
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| FA | food allergy |
| CMPA | cow’s milk protein allergy |
| CM | cow’s milk |
| EAACI | European Association of Allergy and Immunology |
| EHF | extensively hydrolyzed formula |
| AAF | amino acid formula |
| FPIAP | food-protein-induced allergic proctocolitis |
| FPIES | food-protein-induced enterocolitis syndrome |
| OFC | oral food challenge |
| FPE | food protein enteropathy |
References
- Luyt, D.; Ball, H.; Makwana, N.; Green, M.R.; Bravin, K.; Nasser, S.M.; Clark, A.T. Standards of Care Committee (SOCC) of the British Society for Allergy and Clinical Immunology (BSACI). BSACI guideline for the diagnosis and management of cow’s milk allergy. Clin. Exp. Allergy 2014, 44, 642–672. [Google Scholar] [CrossRef] [PubMed]
- Nowak-Węgrzyn, A.; Chehade, M.; Groetch, M.E.; Spergel, J.M.; Wood, R.A.; Allen, K.; Atkins, D.; Bahna, S.; Barad, A.V.; Berin, C.; et al. International consensus guidelines for the diagnosis and management of food protein-induced enterocolitis syndrome: Executive summary Workgroup Report of the Adverse Reactions to Foods Committee, American Academy of Allergy, Asthma & Immunology. J. Allergy Clin. Immunol. 2017, 139, 1111–1126.e4. [Google Scholar] [CrossRef] [PubMed]
- Dupont, C.; Chouraqui, J.P.; Linglart, A.; Bocquet, A.; Darmaun, D.; Feillet, F.; Frelut, M.-L.; Girardet, J.-P.; Hankard, R.; Rozé, J.-C.; et al. Committee on Nutrition of the French Society of Pediatrics. Nutritional management of cow’s milk allergy in children: An update. Arch. Pediatr. 2018, 25, 236–243. [Google Scholar] [CrossRef] [PubMed]
- Meyer, R.; Chebar Lozinsky, A.; Fleischer, D.M.; Vieira, M.C.; Du Toit, G.; Vandenplas, Y.; Dupont, C.; Knibb, R.; Uysal, P.; Cavkaytar, O.; et al. Diagnosis and management of Non-IgE gastrointestinal allergies in breastfed infants—An EAACI Position Paper. Allergy 2020, 75, 14–32. [Google Scholar] [CrossRef] [PubMed]
- Mennini, M.; Fiocchi, A.G.; Cafarotti, A.; Montesano, M.; Mauro, A.; Villa, M.P.; Di Nardo, G. Food protein-induced allergic proctocolitis in infants: Literature review and proposal of a management protocol. World Allergy Organ. J. 2020, 13, 100471. [Google Scholar] [CrossRef] [PubMed]
- McWilliam, V.; Netting, M.J.; Volders, E.; Palmer, D.J.; WAO DRACMA Guideline Group World Allergy Organization (WAO). Diagnosis and Rationale for Action against Cow’s Milk Allergy (DRACMA) guidelines update—X–Breastfeeding a baby with cow’s milk allergy. World Allergy Organ. J. 2023, 16, 100830. [Google Scholar] [CrossRef]
- Vandenplas, Y.; Broekaert, I.; Domellöf, M.; Indrio, F.; Lapillonne, A.; Pienar, C.; Ribes-Koninckx, C.; Shamir, R.; Szajewska, H.; Thapar, N.; et al. An ESPGHAN position paper on the diagnosis, management and prevention of cow’s milk allergy. J. Pediatr. Gastroenterol. Nutr. 2024, 78, 386–413. [Google Scholar] [CrossRef] [PubMed]
- Jarvinen, K.M.; Makinen-Kiljunen, S.; Suomalainen, H. Cow’s milk challenge through human milk evokes immune responses in infants with cow’s milk allergy. J. Pediatr. 1999, 135, 506–512. [Google Scholar] [CrossRef]
- Host, A.; Husby, S.; Hansen, L.G.; Osterballe, O. Bovine B-lactoglobulin in human milk from atopic and non-atopic mothers. Relationship to maternal intake of homogenized and unhomogenized milk. Clin. Exp. Allergy 1990, 20, 383–387. [Google Scholar] [CrossRef]
- Sorva, R.; Makinen-Kiljunen, S.; Juntunen-Backman, K. B-Lacto-globulin secretion in human milk varies widely after cow’s milk ingestion in mothers of infants with cow’s milk allergy. J. Allergy Clin. Immunol. 1994, 93, 787–792. [Google Scholar] [CrossRef]
- Axelsson, I.; Jakobsson, I.; Lindberg, T.; Benediktsson, B. Bovine beta-lactoglobulin in the human milk: A longitudinal study during the whole lactation period. Acta Paediatr. Scand. 1986, 75, 702–707. [Google Scholar] [CrossRef]
- Fukushima, Y.; Kawata, Y.; Onda, T.; Kitagawa, M. Consumption of cow milk and egg by lactating women and the presence of B-lactoglobulin and ovalbumin in breast milk. Am. J. Clin. Nutr. 1997, 65, 30–35. [Google Scholar] [CrossRef] [PubMed]
- Matangkasombut, P.; Padungpak, S.; Thaloengsok, S.; Kamchaisatian, W.; Sasisakulporn, C.; Jotikasthira, W.; Benjaponpitak, S.; Manuyakorn, W. Detection of β-lactoglobulin in human breast-milk 7 days after cow milk ingestion. Paediatr. Int. Child. Health 2017, 37, 199–203. [Google Scholar] [CrossRef] [PubMed]
- Coscia, A.; Orrù, S.; Di Nicola, P.; Giuliani, F.; Rovelli, I.; Peila, C.; Martano, C.; Chiale, F.; Bertino, E. Cow’s milk proteins in human milk. J. Biol. Regul. Homeost. Agents 2012, 26, 39–42. [Google Scholar]
- Kilshaw, P.; Cant, A. The passage of maternal dietary proteins into human breast milk. Int. Arch. Allergy Appl. Immunol. 1984, 75, 8–15. [Google Scholar] [CrossRef]
- Hirose, J.; Ito, S.; Hirata, N.; Kido, S.; Kitabatake, N.; Narita, H. Occurrence of the major food allergen, ovomucoid, in human breast milk as an immune complex. Biosci. Biotechnol. Biochem. 2001, 65, 1438–1440. [Google Scholar] [CrossRef] [PubMed]
- Troncone, R.; Scarcella, A.; Donatiello, A.; Cannataro, P.; Tarabuso, A.; Auricchio, S. Passage of gliadin into human breast milk. Acta Paediatr. Scand. 1987, 76, 453–456. [Google Scholar] [CrossRef] [PubMed]
- Chirdo, F.G.; Rumbo, M.; Anon, M.C.; Fossati, C.A. Presence of high levels of non-degraded gliadin in breast milk from healthy mothers. Scand. J. Gastroenterol. 1998, 33, 1186–1192. [Google Scholar] [PubMed]
- Schocker, F.; Scharf, A.; Kull, S.; Jappe, U. Detection of the Peanut Allergens Ara h 2 and Ara h 6 in Human Breast Milk: Development of 2 Sensitive and Specific Sandwich ELISA Assays. Int. Arch. Allergy Immunol. 2017, 174, 17–25. [Google Scholar] [CrossRef]
- Vadas, P.; Wai, Y.; Burks, W.; Perelman, B. Detection of peanut allergens in breast milk of lactating women. JAMA 2001, 285, 1746–1748. [Google Scholar] [CrossRef]
- Schocker, F.; Baumert, J.; Kull, S.; Petersen, A.; Becker, W.M.; Jappe, U. Prospective investigation on the transfer of Ara h 2, the most potent peanut allergen, in human breast milk. Pediatr. Allergy Immunol. Off. Publ. Eur. Soc. Pediatr. Allergy Immunol. 2016, 27, 348–355. [Google Scholar] [CrossRef] [PubMed]
- Verhasselt, V. Neonatal tolerance under breastfeeding influence. Curr. Opin. Immunol. 2010, 22, 623–630. [Google Scholar] [CrossRef]
- Picariello, G.; Addeo, F.; Ferranti, P.; Nocerino, R.; Paparo, L.; Passariello, A.; Dallas, D.C.; Robinson, R.C.; Barile, D.; Canani, R.B. Antibody-independent identification of bovine milk-derived peptides in breast-milk. Food Funct. 2016, 7, 3402. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Dekker, P.M.; Boeren, S.; Wijga, A.H.; Koppelman, G.H.; Vervoort, J.J.M.; Hettinga, K.A. Maternal Allergy and the Presence of Nonhuman Proteinaceous Molecules in Human Milk. Nutrients 2020, 12, 1169. [Google Scholar] [CrossRef] [PubMed]
- Rajani, P.S.; Martin, H.; Groetch, M.; Järvinen, K.M. Presentation and Management of Food Allergy in Breastfed Infants and Risks of Maternal Elimination Diets. J. Allergy Clin. Immunol. Pract. 2019, 8, 52–67. [Google Scholar] [CrossRef] [PubMed]
- Jakobsson, I.; Lindberg, T.; Benediktsson, B.; Hansson, B.J. Dietary bovine beta-lactoglobulin is transferred to human milk. Acta Paediatr. Scand. 1985, 74, 342–345. [Google Scholar] [CrossRef] [PubMed]
- Schocker, F.; Jappe, U. Breastfeeding: Maternally Transferred Allergens in Breast Milk: Protective or Sensitizing? Mol. Nutr. Food Res. 2022, 66, e2200066. [Google Scholar] [CrossRef] [PubMed]
- Metcalfe, J.R.; Marsh, J.A.; D’Vaz, N.; Geddes, D.T.; Lai, C.T.; Prescott, S.L.; Palmer, D.J. Effects of maternal dietary egg intake during early lactation on human milk ovalbumin concentration: A randomized controlled trial. Clin. Exp. Allergy 2016, 46, 1605–1613. [Google Scholar] [CrossRef] [PubMed]
- Palmer, D.J.; Gold, M.S.; Makrides, M. Effect of maternal egg consumption on breast milk ovalbumin concentration. Clin. Exp. Allergy 2008, 38, 1186–1191. [Google Scholar] [CrossRef]
- Blom, W.M.; Vlieg-Boerstra, B.J.; Kruizinga, A.G.; van der Heide, S.; Houben, G.F.; Dubois, A.E.J. Threshold dose distributions for 5 major allergenic foods in children. J. Allergy Clin. Immunol. 2013, 131, 172–179. [Google Scholar] [CrossRef]
- Høst, A. Frequency of cow’s milk allergy in childhood. Ann. Allergy Asthma Immunol. 2002, 89 (Suppl. S1), 33–37. [Google Scholar] [CrossRef] [PubMed]
- ESPGHAN Committee on Nutrition; Agostoni, C.; Braegger, C.; Decsi, T.; Kolacek, S.; Koletzko, B.; Michaelsen, K.F.; Mihatsch, W.; Moreno, L.A.; Puntis, J.; et al. Breast-feeding: A commentary by the ESPGHAN committee of nutrition. J. Pediatr. Gastroenterol. Nutr. 2009, 49, 112–125. [Google Scholar] [PubMed]
- Koletzko, S.; Niggemann, B.; Arato, A.; Dias, J.A.; Heuschkel, R.; Husby, S.; Mearin, M.L.; Papadopoulou, A.; Ruemmele, F.M.; Staiano, A.; et al. Diagnostic approach and management of cow’s-milk protein allergy in infants and children: ESPGHAN GI Committee practical guidelines. J. Pediatr. Gastroenterol. Nutr. 2012, 55, 221–229. [Google Scholar] [CrossRef] [PubMed]
- Munblit, D.; Perkin, M.R.; Palmer, D.J.; Allen, K.J.; Boyle, R.J. Assessment of evidence about common infant symptoms and cow’s milk allergy. JAMA Pediatr. 2020, 174, 599–608. [Google Scholar] [CrossRef] [PubMed]
- Mousan, G.; Kamat, D. Cow’s Milk Protein Allergy. Clin. Pediatr. 2016, 55, 1054–1063. [Google Scholar] [CrossRef]
- Arima, T.; Campos-Alberto, E.; Funakoshi, H.; Inoue, Y.; Tomiita, M.; Kohno, Y.; Shimojo, N. Immediate systemic allergic reaction in an infant to fish allergen ingested through breast milk. Asia Pac. Allergy 2016, 6, 257–259. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Monti, G.; Marinaro, L.; Libanore, V.; Peltran, A.; Muratore, M.C.; Silvestro, L. Anaphylaxis due to fish hypersensitivity in an exclusively breastfed infant. Acta Paediatr. 2006, 95, 1514–1515. [Google Scholar] [CrossRef]
- Des Roches, A.; Paradis, L.; Singer, S.; Seidman, E. An allergic reaction to peanut in an exclusively breastfed infant. Allergy 2005, 60, 2667. [Google Scholar] [CrossRef]
- De Boissieu, D.; Matarazzo, P.; Rocchiccioli, F.; Dupont, C. Multiple food allergy: A possible diagnosis in breastfed infants. Acta Paediatr. 1997, 86, 10426. [Google Scholar] [CrossRef]
- Isolauri, E.; Tahvanainen, A.; Peltola, T.; Arvola, T. Breast-feeding of allergic infants. J. Pediatr. 1999, 134, 2732. [Google Scholar] [CrossRef]
- Lifschitz, C.H.; Hawkins, H.K.; Guerra, C.; Byrd, N. Anaphylactic shock due to cow’s milk protein hypersensitivity in a breast-fed infant. J. Pediatr. Gastroenterol. Nutr. 1988, 7, 1414. [Google Scholar] [CrossRef]
- Gamirova, A.; Berbenyuk, A.; Levina, D.; Peshko, D.; Simpson, M.R.; Azad, M.B.; Järvinen, K.M.; Brough, H.A.; Genuneit, J.; Greenhawt, M.; et al. Food Proteins in Human Breast Milk and Probability of IgE-Mediated Allergic Reaction in Children During Breastfeeding: A Systematic Review. J. Allergy Clin. Immunol. Pract. 2022, 10, 1312–1324.e8. [Google Scholar] [CrossRef] [PubMed]
- Jakobsson, I.; Lindberg, T. A prospective study of cow’s milk protein intolerance in Swedish infants. Acta Paediatr. Scand. 1979, 68, 853–859. [Google Scholar] [CrossRef]
- Høst, A.; Husby, S.; Østerballe, O. A prospective study of cow’s milk allergy in exclusively breast-fed infants. Acta Paediatr. Scand. 1988, 77, 663–670. [Google Scholar] [CrossRef] [PubMed]
- Jarvinen, K.M.; Suomalainen, H. Development of cow’s milk allergy in breast-fed infants. Clin. Exp. Allergy 2001, 31, 978–987. [Google Scholar] [CrossRef]
- De Greef, E.; Hauser, B.; Devreker, T.; Veereman-Wauters, G.; Vandenplas, Y. Diagnosis and management of cow’s milk protein allergy in infants. World J. Pediatr. 2012, 8, 19–24. [Google Scholar] [CrossRef] [PubMed]
- American Academy of Pediatrics; Committee on Nutrition. Hypoallergenic infant formulas. Pediatrics 2000, 106, 346–349. [Google Scholar] [CrossRef]
- Giampietro, P.G.; Kjellman, N.I.; Oldaeus, G.; Wouters-Wesseling, W.; Businco, L. Hypoallergenicity of an extensively hydrolyzed whey formula. Pediatr. Allergy Immunol. 2001, 12, 83–86. [Google Scholar] [CrossRef] [PubMed]
- Sorea, S.; Dabadie, A.; Bridoux-Henno, L.; Balancon-Morival, M.; Jouan, H.; Le Gall, E. Hemorrhagic colitis in exclusively breast-fed infants. Arch. Pediatr. 2003, 10, 772–775. [Google Scholar] [CrossRef]
- Ravelli, A.; Villanacci, V.; Chiappa, S.; Bolognini, S.; Manenti, S.; Fuoti, M. Dietary protein-inducedproctocolitis in childhood. Am. J. Gastroenterol. 2008, 103, 2605–2612. [Google Scholar] [CrossRef]
- Xanthacos, S.A.; Schwimmer, J.B.; Melin-Aldana, H.; Rothenberg, M.E.; Witte, D.P.; Cohen, M.B. Prevalence and outcome of allergic colitis in healthy infants with rectal bleeding: A prospective cohort study. J. Pediatr. Gastroenterol. Nutr. 2005, 41, 16–22. [Google Scholar] [CrossRef]
- Arvola, T.; Ruuska, T.; Keränen, J.; Hyöty, H.; Salminen, S.; Isolauri, E. Rectal bleeding in infancy: Clinical, allergological, and microbiological examination. Pediatrics 2006, 117, e760–e768. [Google Scholar] [CrossRef] [PubMed]
- Elizur, A.; Cohen, M.; Goldberg, M.R.; Rajuan, N.; Cohen, A.; Leshno, M.; Katz, Y. Cow’s milk associated rectal bleeding: A population based prospective study. Pediatr. Allergy Immunol. 2012, 23, 766–770. [Google Scholar] [CrossRef] [PubMed]
- Sampson, H.A.; Aceves, S.; Bock, S.A.; James, J.; Jones, S.; Lang, D.; Nadeau, K.; Nowak-Wegrzyn, A.; Oppenheimer, J.; Perry, T.T.; et al. Food allergy: A practice parameter update-2014. J. Allergy Clin. Immunol. 2014, 134, 1016–1025. [Google Scholar] [CrossRef] [PubMed]
- Nowak-Węgrzyn, A.; Katz, Y.; Mehr, S.S.; Koletzko, S. Non-IgE-mediated gastrointestinal food allergy. J. Allergy Clin. Immunol. 2015, 135, 1114–1124. [Google Scholar] [CrossRef] [PubMed]
- Miceli Sopo, S.; Monaco, S.; Bersani, G.; Romano, A.; Fantacci, C. Proposal for management of the infant with suspected food protein-induced allergic proctocolitis. Pediatr. Allergy Immunol. 2017, 29, 215–218. [Google Scholar] [CrossRef] [PubMed]
- Martin, V.M.; Virkud, Y.V.; Seay, H.; Hickey, A.; Ndahayo, R.; Rosow, R.; Southwick, C.; Elkort, M.; Gupta, B.; Kramer, E.; et al. Prospective Assessment of Pediatrician-Diagnosed Food Protein–Induced Allergic Proctocolitis by Gross or Occult Blood. J. Allergy Clin. Immunol. Pract. 2020, 8, 1692–1699.e1. [Google Scholar] [CrossRef] [PubMed]
- Buyuktiryaki, B.; Celik, I.K.; Erdem, S.B.; Capanoglu, M.; Civelek, E.; Guc, B.U.; Guvenir, H.; Cakir, M.; Misirlioglu, E.D.; Akcal, O.; et al. Risk Factors Influencing Tolerance and Clinical Features of Food Protein–induced Allergic Proctocolitis. J. Pediatr. Gastroenterol. Nutr. 2020, 70, 574–579. [Google Scholar] [CrossRef] [PubMed]
- Cetinkaya, P.G.; Kahveci, M.; Karaatmaca, B.; Esenboga, S.; Sahiner, U.M.; Sekerel, B.E.; Soyer, O. Predictors for late tolerance development in food protein-induced allergic proctocolitis. Allergy Asthma Proc. 2020, 41, E11–E18. [Google Scholar] [CrossRef]
- Kaya, A.; Toyran, M.; Civelek, E.; Misirlioglu, E.; Kirsaclioglu, C.; Kocabas, C.N. Characteristics and prognosis of allergic proctocolitis in infants. J. Pediatr. Gastroenterol. Nutr. 2015, 61, 69. [Google Scholar] [CrossRef]
- Labrosse, R.; Graham, F.; Caubet, J.C. Non-IgE-Mediated Gastrointestinal Food Allergies in Children: An Update. Nutrients 2020, 12, 2086. [Google Scholar] [CrossRef] [PubMed]
- Barni, S.; Mori, F.; Giovannini, M.; Liotti, L.; Mastrorilli, C.; Pecoraro, L.; Saretta, F.; Castagnoli, R.; Arasi, S.; Caminiti, L.; et al. Allergic Proctocolitis: Literature Review and Proposal of a Diagnostic-Therapeutic Algorithm. Life 2023, 13, 1824. [Google Scholar] [CrossRef] [PubMed]
- Gelsomino, M.; Sinatti, D.; Miceli Sopo, S. Non-allergic benign infantile proctocolitis: A neglected nosographic entity. BMJ Case Rep. 2021, 14, e244918. [Google Scholar] [CrossRef] [PubMed]
- Fox, V.L. Gastrointestinal bleeding in infancy and childhood. Gastroenterol. Clin. N. Am. 2000, 29, 37–66. [Google Scholar] [CrossRef] [PubMed]
- Nowak-Wegrzyn, A.; Berin, M.C.; Mehr, S. Food Protein-Induced Enterocolitis Syndrome. J. Allergy Clin. Immunol. Pract. 2020, 8, 24–35. [Google Scholar] [CrossRef] [PubMed]
- Leonard, S.A.; Nowak-Wegrzyn, A. Manifestations, diagnosis, and management of food protein-induced enterocolitis syndrome. Pediatr. Ann. 2013, 42, 135–140. [Google Scholar] [CrossRef] [PubMed]
- Miceli Sopo, S.; Monaco, S.; Greco, M.; Scala, G. Chronic food protein-induced enterocolitis syndrome caused by cow’s milk proteins passed through breast milk. Int. Arch. Allergy Immunol. 2014, 164, 207–209. [Google Scholar] [CrossRef] [PubMed]
- Monti, G.; Castagno, E.; Liguori, S.A.; Lupica, M.M.; Tarasco, V.; Viola, S.; Tovo, P.A. Food protein-induced enterocolitis syndrome by cow’s milk proteins passed through breast milk. J. Allergy Clin. Immunol. 2011, 127, 679–680. [Google Scholar] [CrossRef]
- Tan, J.; Campbell, D.; Mehr, S. Food protein-induced enterocolitis syndrome in an exclusively breast-fed infant—An uncommon entity. J. Allergy Clin. Immunol. 2012, 129, 873. [Google Scholar] [CrossRef]
- Boyce, J.A.; Assa’ad, A.; Burks, A.W.; Jones, S.M.; Sampson, H.A.; Wood, R.A.; Plaut, M.; Cooper, S.F.; Fenton, M.J.; Arshad, S.H.; et al. Guidelines for the diagnosis and management of food allergy in the United States: Report of the NIAID-sponsored expert panel. J. Allergy Clin. Immunol. 2010, 126, S1–S58. [Google Scholar] [CrossRef]
- Baldo, F.; Bevacqua, M.; Corrado, C.; Nisticò, D.; Cesca, L.; Declich, V.; Dall’amico, R.; Barbi, E. FPIES in exclusively breastfed infants: Two case reports and review of the literature. Ital. J. Pediatr. 2020, 46, 144. [Google Scholar] [CrossRef] [PubMed]
- Lake, A.M.; Whitington, P.F.; Hamilton, S.R. Dietary protein-induced colitis in breast-fed infants. J. Pediatr. 1982, 101, 906–910. [Google Scholar] [CrossRef] [PubMed]
- Higuchi, R.; Booka, M.; Suzuki, H.; Tsuno, H. Protein-losing enteropathy and erythema caused by egg allergy in a breast-fed infant. Pediatr. Int. 2016, 58, 422–424. [Google Scholar] [CrossRef] [PubMed]
- Kondo, M.; Fukao, T.; Omoya, K.; Kawamoto, N.; Aoki, M.; Teramotoet, T.; Kaneko, H.; Kondo, N. Protein-losing enteropathy associated with egg allergy in a 5-month-old boy. J. Investig. Allergol. Clin. Immunol. 2008, 18, 63–66. [Google Scholar]
- Vandenplas, Y.; Quenon, M.; Renders, F.; Dab, I.; Loeb, H. Milk-sensitive eosinophilic gastroenteritis in a 10-day-old boy. Eur. J. Pediatr. 1990, 149, 244–245. [Google Scholar] [CrossRef] [PubMed]
- Hwang, J.B.; Kang, Y.N.; Won, K.S. Protein losing enteropathy in severe atopic dermatitis in an exclusively breast-fed infant. Pediatr. Dermatol. 2009, 26, 638–639. [Google Scholar] [CrossRef] [PubMed]
- Venter, C.; Roth-Walter, F.; Vassilopoulos, E.; Hicks, A. Dietary management of IgE and non-IgE-mediated food allergies in pediatric patients. Pediatr. Allergy Immunol. 2024, 35, e14100. [Google Scholar] [CrossRef]
- Fox, A.; Brown, T.; Walsh, J.; Venter, C.; Meyer, R.; Nowak-Wegrzyn, A.; Levin, M.; Spawls, H.; Beatson, J.; Lovis, M.-T.; et al. An update to the milk allergy in primary care guideline. Clin. Transl. Allergy 2019, 9, 40. [Google Scholar] [CrossRef]
| Guidelines/Recommendations | Year of Publication | Advice Regarding Breastfed Infants |
|---|---|---|
| BSACI guideline for the diagnosis and management of cow’s milk allergy [1] | 2014 | Breast milk is advisable for most infants with CMA. Therefore, breastfeeding should be encouraged, usually with no dietary dairy restrictions unless the infant shows symptoms while being breastfed. Nonetheless, small amounts of cow’s milk proteins found in breast milk can elicit symptoms in exclusively breastfed infants never receiving cow’s milk. |
| International consensus guidelines for the diagnosis and management of food-protein-induced enterocolitis syndrome [2] | 2017 | Dietary elimination of offending triggers must not be recommended in lactating mothers if the infant is thriving and remains asymptomatic. In the case of symptomatic FPIES occurring in an exclusively breastfed infant, the trigger food or foods should be eliminated from the mother’s diet if reactions occur after breastfeeding or if the infant fails to thrive. Do not routinely recommend avoiding products with precautionary allergen labels in patients with FPIES. |
| Committee on Nutrition of the French Society of Pediatrics [3] | 2018 | Breast milk is preferable for all infants, including those with CMA. Milk and dairy products should be removed from the mother’s diet if the child is diagnosed with CMA when breastfed. |
| Diagnosis and management of non-IgE gastrointestinal allergies in breastfed infants—An EAACI Position Paper [4] | 2019 | Maternal elimination diets for 2–4 weeks with symptom improvement or resolution, followed by reintroduction with symptom deterioration, remains the cornerstone for diagnosis. does not apply in the case of a convincing history of FPIES or severe associated symptoms. The symptoms are present when reintroduction does not occur. International FPIES guidelines do not recommend routine allergen avoidance in breastfeeding mothers unless a child presents with symptoms while breastfeeding. In such cases, avoidance may be necessary. FPIAP: treatment, if required, is based on strict exclusion of the culprit food in the mother’s diet, usually cow’s milk, but other dietary antigens may also need to be eliminated. FPE: When food protein is suspected, a maternal elimination diet should be implemented, followed by reintroduction. |
| WAO food-protein-induced allergic proctocolitis in infants: literature review and proposal of a management protocol [5] | 2020 | In breastfeeding infants, it is vital to support the beneficial role of breastfeeding. Yet, cow’s milk proteins should be eliminated from the maternal diet. Clinical bleeding typically resolves within 1 to 2 weeks of eliminating the offending protein from the mother’s diet. |
| WAO DRACMA guideline group [6] | 2023 | In the current clinical practice recommendations, a 2–4-week trial of maternal cow’s milk dietary elimination is advised for the following: (a) IgE-mediated cow’s milk allergy, if the infant is symptomatic while breastfeeding alone; (b) Non-IgE-mediated associated symptoms, if the history and examination strongly point at cow’s milk allergy; (c) Infants with moderate to severe eczema/atopic dermatitis not responding to topical steroids and sensitized to cow’s milk protein. There should be a clear plan to reintroduce cow’s milk into the maternal diet at home for 1 week in order to determine a cause–effect relationship between the cow’s milk elimination and the resolution of symptoms. Then, there is a subsequent reoccurrence of infant symptoms upon maternal cow’s milk reintroduction. The evidence base to support avoiding cow’s milk in the mother’s diet so as to treat a breastfed infant with cow’s milk allergy is limited due to a lack of high-quality, adequately powered, randomized controlled trials. |
| An ESPGHAN position paper on the diagnosis, management, and prevention of cow milk allergy [7] | 2024 | CMA in exclusively breastfed infants is a rare condition. Dietary restrictions in breastfeeding mothers are usually not needed. Therefore, in exclusively breastfed infants with chronic symptoms of CMA dietary restrictions should only be considered in rare and specific circumstances. Clinical trials do not consistently support the exclusion of CM from the maternal or infant diet to manage common symptoms in infants without demonstrated CMA. Up to 20% of breastfed infants show spontaneous resolution of symptoms, such as rectal bleeding, without changing their mothers’ diets. Breastfeeding with a maternal elimination diet for CM may be considered for 2 to 4 weeks. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gelsomino, M.; Liotti, L.; Barni, S.; Mori, F.; Giovannini, M.; Mastrorilli, C.; Pecoraro, L.; Saretta, F.; Castagnoli, R.; Arasi, S.; et al. Elimination Diets in Lactating Mothers of Infants with Food Allergy. Nutrients 2024, 16, 2317. https://doi.org/10.3390/nu16142317
Gelsomino M, Liotti L, Barni S, Mori F, Giovannini M, Mastrorilli C, Pecoraro L, Saretta F, Castagnoli R, Arasi S, et al. Elimination Diets in Lactating Mothers of Infants with Food Allergy. Nutrients. 2024; 16(14):2317. https://doi.org/10.3390/nu16142317
Chicago/Turabian StyleGelsomino, Mariannita, Lucia Liotti, Simona Barni, Francesca Mori, Mattia Giovannini, Carla Mastrorilli, Luca Pecoraro, Francesca Saretta, Riccardo Castagnoli, Stefania Arasi, and et al. 2024. "Elimination Diets in Lactating Mothers of Infants with Food Allergy" Nutrients 16, no. 14: 2317. https://doi.org/10.3390/nu16142317
APA StyleGelsomino, M., Liotti, L., Barni, S., Mori, F., Giovannini, M., Mastrorilli, C., Pecoraro, L., Saretta, F., Castagnoli, R., Arasi, S., Klain, A., Giudice, M. M. d., & Novembre, E. (2024). Elimination Diets in Lactating Mothers of Infants with Food Allergy. Nutrients, 16(14), 2317. https://doi.org/10.3390/nu16142317









