The Role of Gut Microbiota in Anxiety, Depression, and Other Mental Disorders as Well as the Protective Effects of Dietary Components
Abstract
1. Introduction
2. Gut Microbiota and Mental Disorders
2.1. Anxiety
2.2. Depression
2.3. Bipolar Disorder
2.4. Autism Spectrum Disorder
2.5. Schizophrenia
2.6. Other Mental Disorders
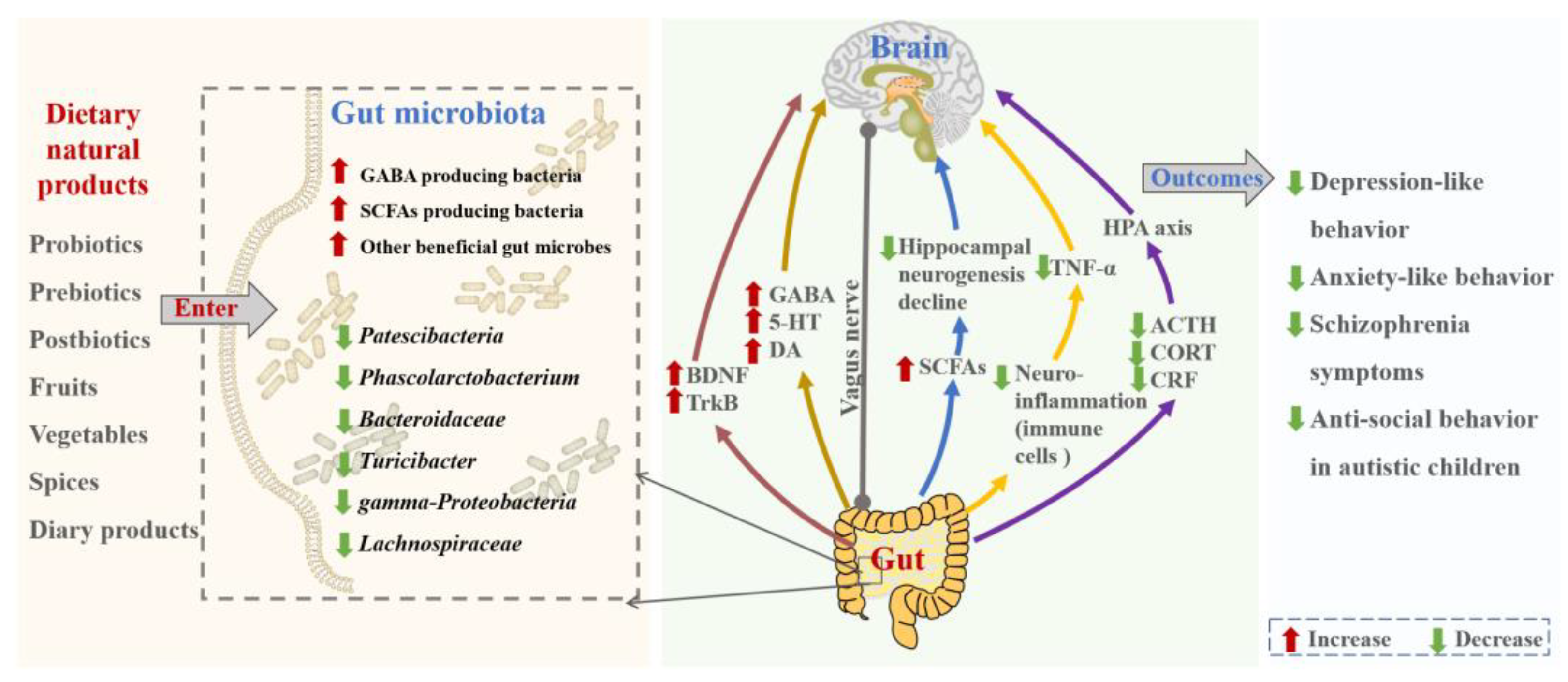
3. Effects and Mechanisms of Dietary Components on Mental Disorders through Modulating Gut Microbiota
3.1. Probiotics
3.2. Prebiotics and Postbiotics
3.3. Dairy Products
3.4. Spices
3.5. Other Natural Products
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Lund, C.; Brooke-Sumner, C.; Baingana, F.; Baron, E.C.; Breuer, E.; Chandra, P.; Haushofer, J.; Herrman, H.; Jordans, M.; Kieling, C.; et al. Social determinants of mental disorders and the Sustainable Development Goals: A systematic review of reviews. Lancet Psychiatry 2018, 5, 357–369. [Google Scholar] [CrossRef]
- Ferrari, A.J.; Santomauro, D.F.; Herrera, A.M.M.; Shadid, J.; Ashbaugh, C.; Erskine, H.E.; Charlson, F.J.; Degenhardt, L.; Scott, J.G.; McGrath, J.J.; et al. Global, regional, and national burden of 12 mental disorders in 204 countries and territories, 1990-2019: A systematic analysis for the Global Burden of Disease Study 2019. Lancet Psychiatry 2022, 9, 137–150. [Google Scholar] [CrossRef]
- Pan, K.Y.; Kok, A.A.L.; Eikelenboom, M.; Horsfall, M.; Jorg, F.; Luteijn, R.A.; Rhebergen, D.; van Oppen, P.; Giltay, E.J.; Penninx, B. The mental health impact of the COVID-19 pandemic on people with and without depressive, anxiety, or obsessive-compulsive disorders: A longitudinal study of three Dutch case-control cohorts. Lancet Psychiatry 2021, 8, 121–129. [Google Scholar] [CrossRef] [PubMed]
- Toubasi, A.A.; AbuAnzeh, R.B.; Abu Tawileh, H.B.; Aldebei, R.H.; Alryalat, S.A.S. A meta-analysis: The mortality and severity of COVID-19 among patients with mental disorders. Psychiatry Res. 2021, 299, 113856. [Google Scholar] [CrossRef]
- Cao, S.Y.; Zhao, C.N.; Xu, X.Y.; Tang, G.Y.; Corke, H.; Gan, R.Y.; Li, H.B. Dietary plants, gut microbiota, and obesity: Effects and mechanisms. Trends Food Sci. Technol. 2019, 92, 194–204. [Google Scholar] [CrossRef]
- Li, H.Y.; Zhou, D.D.; Gan, R.Y.; Huang, S.Y.; Zhao, C.N.; Shang, A.; Xu, X.Y.; Li, H.B. Effects and mechanisms of probiotics, prebiotics, synbiotics, and postbiotics on metabolic diseases targeting gut microbiota: A narrative review. Nutrients 2021, 13, 3211. [Google Scholar] [CrossRef]
- Luo, M.; Zhou, D.D.; Shang, A.; Gan, R.Y.; Li, H.B. Influences of food contaminants and additives on gut microbiota as well as protective effects of dietary bioactive compounds. Trends Food Sci. Technol. 2021, 113, 180–192. [Google Scholar] [CrossRef]
- Tao, J.; Li, S.; Gan, R.Y.; Zhao, C.N.; Meng, X.; Li, H.B. Targeting gut microbiota with dietary components on cancer: Effects and potential mechanisms of action. Crit. Rev. Food Sci. Nutr. 2020, 60, 1025–1037. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.J.; Li, S.; Gan, R.Y.; Zhou, T.; Xu, D.P.; Li, H.B. Impacts of gut bacteria on human health and diseases. Int. J. Mol. Sci. 2015, 16, 7493–7519. [Google Scholar] [CrossRef]
- Forssten, S.D.; Ouwehand, A.C.; Griffin, S.M.; Patterson, E. One giant leap from mouse to man: The microbiota-gut-brain axis in mood disorders and translational challenges moving towards human clinical trials. Nutrients 2022, 14, 568. [Google Scholar] [CrossRef]
- Wu, S.X.; Li, J.; Zhou, D.D.; Xiong, R.G.; Huang, S.Y.; Saimaiti, A.; Shang, A.; Li, H.B. Possible effects and mechanisms of dietary natural products and nutrients on depression and anxiety: A narrative review. Antioxidants 2022, 11, 2132. [Google Scholar] [CrossRef]
- Xiong, R.G.; Li, J.; Cheng, J.; Wu, S.X.; Huang, S.Y.; Zhou, D.D.; Saimaiti, A.; Shang, A.; Tang, G.Y.; Li, H.B.; et al. New insights into the protection of dietary components on anxiety, depression, and other mental disorders caused by contaminants and food additives. Trends Food Sci. Technol. 2023, 138, 44–56. [Google Scholar] [CrossRef]
- Generoso, J.S.; Giridharan, V.V.; Lee, J.; Macedo, D.; Barichello, T. The role of the microbiota-gut-brain axis in neuropsychiatric disorders. Braz. J. Psychiatry 2021, 43, 293–305. [Google Scholar] [CrossRef] [PubMed]
- Ortega, M.A.; Álvarez-Mon, M.A.; García-Montero, C.; Fraile-Martínez, Ó.; Monserrat, J.; Martinez-Rozas, L.; Rodríguez-Jiménez, R.; Álvarez-Mon, M.; Lahera, G. Microbiota-gut-brain axis mechanisms in the complex network of bipolar disorders: Potential clinical implications and translational opportunities. Mol. Psychiatry 2023. Advance online publication. [Google Scholar] [CrossRef] [PubMed]
- Godos, J.; Currenti, W.; Angelino, D.; Mena, P.; Castellano, S.; Caraci, F.; Galvano, F.; Del Rio, D.; Ferri, R.; Grosso, G. Diet and mental health: Review of the recent updates on molecular mechanisms. Antioxidants 2020, 9, 346. [Google Scholar] [CrossRef] [PubMed]
- Kennedy, P.J.; Murphy, A.B.; Cryan, J.F.; Ross, P.R.; Dinan, T.G.; Stanton, C. Microbiome in brain function and mental health. Trends Food Sci. Technol. 2016, 57, 289–301. [Google Scholar] [CrossRef]
- Bhatia, N.Y.; Jalgaonkar, M.P.; Hargude, A.B.; Sherje, A.P.; Oza, M.J.; Doshi, G.M. Gut-brain axis and neurological disorders-how microbiomes affect our mental health. CNS Neurol. Disord. Drug Targets 2023, 22, 1008–1030. [Google Scholar] [CrossRef]
- Hao, Z.; Meng, C.; Li, L.; Feng, S.; Zhu, Y.; Yang, J.; Han, L.; Sun, L.; Lv, W.; Figeys, D.; et al. Positive mood-related gut microbiota in a long-term closed environment: A multiomics study based on the “Lunar Palace 365” experiment. Microbiome 2023, 11, 88. [Google Scholar] [CrossRef]
- Liu, L.; Wang, H.; Chen, X.; Zhang, Y.; Zhang, H.; Xie, P. Gut microbiota and its metabolites in depression: From pathogenesis to treatment. EBioMedicine 2023, 90, 104527. [Google Scholar] [CrossRef]
- Asher, G.N.; Gerkin, J.; Gaynes, B.N. Complementary therapies for mental health disorders. Med. Clin. N. Am. 2017, 101, 847–864. [Google Scholar] [CrossRef]
- Lakhan, S.E.; Vieira, K.F. Nutritional therapies for mental disorders. Nutr. J. 2008, 7, 2. [Google Scholar] [CrossRef] [PubMed]
- Amini, S.; Jafarirad, S.; Abiri, B. Vitamin D, testosterone and depression in middle-aged and elderly men: A systematic review. Crit. Rev. Food Sci. Nutr. 2023, 63, 5194–5205. [Google Scholar] [CrossRef] [PubMed]
- Dobersek, U.; Teel, K.; Altmeyer, S.; Adkins, J.; Wy, G.; Peak, J. Meat and mental health: A meta-analysis of meat consumption, depression, and anxiety. Crit. Rev. Food Sci. Nutr. 2023, 63, 3556–3573. [Google Scholar] [CrossRef] [PubMed]
- Fusar-Poli, L.; Gabbiadini, A.; Ciancio, A.; Vozza, L.; Signorelli, M.S.; Aguglia, E. The effect of cocoa-rich products on depression, anxiety, and mood: A systematic review and meta-analysis. Crit. Rev. Food Sci. Nutr. 2022, 62, 7905–7916. [Google Scholar] [CrossRef] [PubMed]
- Musazadeh, V.; Zarezadeh, M.; Faghfouri, A.H.; Keramati, M.; Jamilian, P.; Jamilian, P.; Mohagheghi, A.; Farnam, A. Probiotics as an effective therapeutic approach in alleviating depression symptoms: An umbrella meta-analysis. Crit. Rev. Food Sci. Nutr. 2022, in press. [Google Scholar] [CrossRef]
- Pferschy-Wenzig, E.M.; Pausan, M.R.; Ardjomand-Woelkart, K.; Röck, S.; Ammar, R.M.; Kelber, O.; Moissl-Eichinger, C.; Bauer, R. Medicinal plants and their impact on the gut microbiome in mental health: A systematic review. Nutrients 2022, 14, 2111. [Google Scholar] [CrossRef]
- Yılmaz, C.; Gökmen, V. Neuroactive compounds in foods: Occurrence, mechanism and potential health effects. Food Res. Int. 2020, 128, 108744. [Google Scholar] [CrossRef]
- Hepsomali, P.; Groeger, J.A. Diet, sleep, and mental health: Insights from the UK biobank study. Nutrients 2021, 13, 2573. [Google Scholar] [CrossRef]
- Reuter, M.; Zamoscik, V.; Plieger, T.; Bravo, R.; Ugartemendia, L.; Rodriguez, A.B.; Kirsch, P. Tryptophan-rich diet is negatively associated with depression and positively linked to social cognition. Nutr. Res. 2021, 85, 14–20. [Google Scholar] [CrossRef]
- Kim, C.S.; Shin, G.E.; Cheong, Y.; Shin, D.M.; Chun, W.Y. Experiencing social exclusion changes gut microbiota composition. Transl. Psychiatry 2022, 12, 254. [Google Scholar] [CrossRef]
- Yuan, X.M.; Chen, B.Q.; Duan, Z.L.; Xia, Z.Q.; Ding, Y.; Chen, T.; Liu, H.Z.; Wang, B.S.; Yang, B.L.; Wang, X.Y.; et al. Depression and anxiety in patients with active ulcerative colitis: Crosstalk of gut microbiota, metabolomics and proteomics. Gut Microbes 2021, 13, 1987779. [Google Scholar] [CrossRef]
- Jiang, H.Y.; Zhang, X.; Yu, Z.H.; Zhang, Z.; Deng, M.; Zhao, J.H.; Ruan, B. Altered gut microbiota profile in patients with generalized anxiety disorder. J. Psychiatr. Res. 2018, 104, 130–136. [Google Scholar] [CrossRef] [PubMed]
- Jiang, H.Y.; Pan, L.Y.; Zhang, X.; Zhang, Z.; Zhou, Y.Y.; Ruan, B. Altered gut bacterial-fungal interkingdom networks in patients with current depressive episode. Brain Behav. 2020, 10, e016772020-10. [Google Scholar] [CrossRef]
- Valles-Colomer, M.; Falony, G.; Darzi, Y.; Tigchelaar, E.F.; Wang, J.; Tito, R.Y.; Schiweck, C.; Kurilshikov, A.; Joossens, M.; Wijmenga, C.; et al. The neuroactive potential of the human gut microbiota in quality of life and depression. Nat. Microbiol. 2019, 4, 623–632. [Google Scholar] [CrossRef] [PubMed]
- Lin, P.; Ding, B.; Feng, C.; Yin, S.; Zhang, T.; Qi, X.; Lv, H.; Guo, X.; Dong, K.; Zhu, Y.; et al. Prevotella and Klebsiella proportions in fecal microbial communities are potential characteristic parameters for patients with major depressive disorder. J. Affect. Disord. 2017, 207, 300–304. [Google Scholar] [CrossRef]
- Chen, Z.; Li, J.; Gui, S.; Zhou, C.; Chen, J.; Yang, C.; Hu, Z.; Wang, H.; Zhong, X.; Zeng, L.; et al. Comparative metaproteomics analysis shows altered fecal microbiota signatures in patients with major depressive disorder. Neuroreport 2018, 29, 417–425. [Google Scholar] [CrossRef]
- Li, D.; Sun, T.; Tong, Y.; Le, J.; Yao, Q.; Tao, J.; Liu, H.; Jiao, W.; Mei, Y.; Chen, J.; et al. Gut-microbiome-expressed 3β-hydroxysteroid dehydrogenase degrades estradiol and is linked to depression in premenopausal females. Cell Metab. 2023, 35, 685–694.e685. [Google Scholar] [CrossRef]
- McIntyre, R.S.; Subramaniapillai, M.; Shekotikhina, M.; Carmona, N.E.; Lee, Y.; Mansur, R.B.; Brietzke, E.; Fus, D.; Coles, A.S.; Iacobucci, M.; et al. Characterizing the gut microbiota in adults with bipolar disorder: A pilot study. Nutr. Neurosci. 2021, 24, 173–180. [Google Scholar] [CrossRef] [PubMed]
- Evans, S.J.; Bassis, C.M.; Hein, R.; Assari, S.; Flowers, S.A.; Kelly, M.B.; Young, V.B.; Ellingrod, V.E.; McInnis, M.G. The gut microbiome composition associates with bipolar disorder and illness severity. J. Psychiatr. Res. 2017, 87, 23–29. [Google Scholar] [CrossRef] [PubMed]
- Painold, A.; Morkl, S.; Kashofer, K.; Halwachs, B.; Dalkner, N.; Bengesser, S.; Birner, A.; Fellendorf, F.; Platzer, M.; Queissner, R.; et al. A step ahead: Exploring the gut microbiota in inpatients with bipolar disorder during a depressive episode. Bipolar Disord. 2019, 21, 40–49. [Google Scholar] [CrossRef]
- Coello, K.; Hansen, T.H.; Sorensen, N.; Munkholm, K.; Kessing, L.V.; Pedersen, O.; Vinberg, M. Gut microbiota composition in patients with newly diagnosed bipolar disorder and their unaffected first-degree relatives. Brain Behav. Immun. 2019, 75, 112–118. [Google Scholar] [CrossRef] [PubMed]
- Dilmore, A.H.; McDonald, D.; Nguyen, T.T.; Adams, J.B.; Krajmalnik-Brown, R.; Elijah, E.; Dorrestein, P.C.; Knight, R. The fecal microbiome and metabolome of Pitt Hopkins syndrome, a severe autism spectrum disorder. mSystems 2021, 6, e01006212021. [Google Scholar] [CrossRef]
- Hua, X.; Zhu, J.; Yang, T.; Guo, M.; Li, Q.; Chen, J.; Li, T. The gut microbiota and associated metabolites are altered in sleep disorder of children with autism spectrum disorders. Front. Psychiatry 2020, 11, 855. [Google Scholar] [CrossRef] [PubMed]
- Kandeel, W.A.; Meguid, N.A.; Bjørklund, G.; Eid, E.M.; Farid, M.; Mohamed, S.K.; Wakeel, K.E.; Chirumbolo, S.; Elsaeid, A.; Hammad, D.Y. Impact of Clostridium bacteria in children with autism spectrum disorder and their anthropometric measurements. J. Mol. Neurosci. 2020, 70, 897–907. [Google Scholar] [CrossRef] [PubMed]
- Plaza-Díaz, J.; Gómez-Fernández, A.; Chueca, N.; Torre-Aguilar, M.J.; Gil, Á.; Perez-Navero, J.L.; Flores-Rojas, K.; Martín-Borreguero, P.; Solis-Urra, P.; Ruiz-Ojeda, F.J.; et al. Autism spectrum disorder (ASD) with and without mental regression is associated with changes in the fecal microbiota. Nutrients 2019, 11, 337. [Google Scholar] [CrossRef] [PubMed]
- Manchia, M.; Fontana, A.; Panebianco, C.; Paribello, P.; Arzedi, C.; Cossu, E.; Garzilli, M.; Montis, M.A.; Mura, A.; Pisanu, C.; et al. Involvement of gut microbiota in schizophrenia and treatment resistance to antipsychotics. Biomedicines 2021, 9, 875. [Google Scholar] [CrossRef]
- Zhu, C.; Zheng, M.; Ali, U.; Xia, Q.; Wang, Z.; Chenlong; Yao, L.; Chen, Y.; Yan, J.; Wang, K.; et al. Association between abundance of Haemophilus in the gut microbiota and negative symptoms of schizophrenia. Front. Psychiatry 2021, 12, 685910. [Google Scholar] [CrossRef] [PubMed]
- Li, S.; Song, J.; Ke, P.; Kong, L.; Lei, B.; Zhou, J.; Huang, Y.; Li, H.; Li, G.; Chen, J.; et al. The gut microbiome is associated with brain structure and function in schizophrenia. Sci. Rep. 2021, 11, 9743. [Google Scholar] [CrossRef]
- Nguyen, T.T.; Kosciolek, T.; Daly, R.E.; Vázquez-Baeza, Y.; Swafford, A.; Knight, R.; Jeste, D.V. Gut microbiome in schizophrenia: Altered functional pathways related to immune modulation and atherosclerotic risk. Brain. Behav. Immun. 2021, 91, 245–256. [Google Scholar] [CrossRef]
- Li, S.; Zhuo, M.; Huang, X.; Huang, Y.; Zhou, J.; Xiong, D.; Li, J.; Liu, Y.; Pan, Z.; Li, H.; et al. Altered gut microbiota associated with symptom severity in schizophrenia. PeerJ 2020, 8, e95742020. [Google Scholar] [CrossRef]
- Zhang, X.; Pan, L.Y.; Zhang, Z.; Zhou, Y.Y.; Jiang, H.Y.; Ruan, B. Analysis of gut mycobiota in first-episode, drug-naïve Chinese patients with schizophrenia: A pilot study. Behav. Brain Res. 2020, 379, 112374. [Google Scholar] [CrossRef]
- Zhu, F.; Ju, Y.; Wang, W.; Wang, Q.; Guo, R.; Ma, Q.; Sun, Q.; Fan, Y.; Xie, Y.; Yang, Z.; et al. Metagenome-wide association of gut microbiome features for schizophrenia. Nat. Commun. 2020, 11, 1612. [Google Scholar] [CrossRef]
- Fan, Y.; Støving, R.K.; Berreira Ibraim, S.; Hyötyläinen, T.; Thirion, F.; Arora, T.; Lyu, L.; Stankevic, E.; Hansen, T.H.; Déchelotte, P.; et al. The gut microbiota contributes to the pathogenesis of anorexia nervosa in humans and mice. Nat. Microbiol. 2023, 8, 787–802. [Google Scholar] [CrossRef]
- Gao, F.; Guo, R.; Ma, Q.; Li, Y.; Wang, W.; Fan, Y.; Ju, Y.; Zhao, B.; Gao, Y.; Qian, L.; et al. Stressful events induce long-term gut microbiota dysbiosis and associated post-traumatic stress symptoms in healthcare workers fighting against COVID-19. J. Affect. Disord. 2022, 303, 187–195. [Google Scholar] [CrossRef]
- Malan-Muller, S.; Valles-Colomer, M.; Foxx, C.L.; Vieira-Silva, S.; van den Heuvel, L.L.; Raes, J.; Seedat, S.; Lowry, C.A.; Hemmings, S.M.J. Exploring the relationship between the gut microbiome and mental health outcomes in a posttraumatic stress disorder cohort relative to trauma-exposed controls. Eur. Neuropsychopharmacol. 2022, 56, 24–38. [Google Scholar] [CrossRef]
- Wang, L.J.; Li, S.C.; Li, S.W.; Kuo, H.C.; Lee, S.Y.; Huang, L.H.; Chin, C.Y.; Yang, C.Y. Gut microbiota and plasma cytokine levels in patients with attention-deficit/hyperactivity disorder. Transl. Psychiatry 2022, 12, 76. [Google Scholar] [CrossRef]
- Malan-Müller, S.; Valles-Colomer, M.; Palomo, T.; Leza, J.C. The gut-microbiota-brain axis in a Spanish population in the aftermath of the COVID-19 pandemic: Microbiota composition linked to anxiety, trauma, and depression profiles. Gut Microbes 2023, 15, 2162306. [Google Scholar] [CrossRef]
- Huang, E.; Kang, S.; Park, H.; Park, S.; Ji, Y.; Holzapfel, W.H. Differences in anxiety levels of various murine models in relation to the gut microbiota composition. Biomedicines 2018, 6, 113. [Google Scholar] [CrossRef]
- Wu, J.; Chai, T.; Zhang, H.; Huang, Y.; Perry, S.W.; Li, Y.; Duan, J.; Tan, X.; Hu, X.; Liu, Y.; et al. Changes in gut viral and bacterial species correlate with altered 1,2-diacylglyceride levels and structure in the prefrontal cortex in a depression-like non-human primate model. Transl. Psychiatry 2022, 12, 74. [Google Scholar] [CrossRef]
- Goo, N.; Bae, H.J.; Park, K.; Kim, J.; Jeong, Y.; Cai, M.; Cho, K.; Jung, S.Y.; Kim, D.H.; Ryu, J.H. The effect of fecal microbiota transplantation on autistic-like behaviors in Fmr1 KO mice. Life Sci. 2020, 262, 118497. [Google Scholar] [CrossRef]
- Penninx, B.; Pine, D.S.; Holmes, E.A.; Reif, A. Anxiety disorders. Lancet 2021, 397, 914–927. [Google Scholar] [CrossRef]
- Ericsson, A.C.; Hart, M.L.; Kwan, J.; Lanoue, L.; Bower, L.R.; Araiza, R.; Lloyd, K.C.K.; Franklin, C.L. Supplier-origin mouse microbiomes significantly influence locomotor and anxiety-related behavior, body morphology, and metabolism. Commun. Biol. 2021, 4, 716. [Google Scholar] [CrossRef]
- Malhi, G.S.; Mann, J.J. Depression. Lancet 2018, 392, 2299–2312. [Google Scholar] [CrossRef]
- Tan, X.; Zhang, L.; Wang, D.; Guan, S.; Lu, P.; Xu, X.; Xu, H. Influence of early life stress on depression: From the perspective of neuroendocrine to the participation of gut microbiota. Aging 2021, 13, 25588–25601. [Google Scholar] [CrossRef]
- Winter, G.; Hart, R.A.; Charlesworth, R.P.G.; Sharpley, C.F. Gut microbiome and depression: What we know and what we need to know. Rev. Neurosci. 2018, 29, 629–643. [Google Scholar] [CrossRef]
- Gu, Y.; Zheng, L.; Kumari, S.; Zhang, Q.; Liu, L.; Meng, G.; Wu, H.; Bao, X.; Yao, Z.; Sun, S.; et al. The relationship between Helicobacter pylori infection and depressive symptoms in the general population in China: The TCLSIH cohort study. Helicobacter 2019, 24, e126322019. [Google Scholar] [CrossRef]
- Liu, Q.; Meng, X.; Li, Y.; Zhao, C.N.; Tang, G.Y.; Li, S.; Gan, R.Y.; Li, H.B. Natural products for the prevention and management of Helicobacter pylori infection. Compr. Rev. Food. Sci. Food Saf. 2018, 17, 937–952. [Google Scholar] [CrossRef]
- Medina-Rodriguez, E.M.; Watson, J.; Reyes, J.; Trivedi, M.; Beurel, E. Th17 cells sense microbiome to promote depressive-like behaviors. Microbiome 2023, 11, 92. [Google Scholar] [CrossRef]
- Liu, Y.; Wang, H.; Gui, S.; Zeng, B.; Pu, J.; Zheng, P.; Zeng, L.; Luo, Y.; Wu, Y.; Zhou, C.; et al. Proteomics analysis of the gut-brain axis in a gut microbiota-dysbiosis model of depression. Transl. Psychiatry 2021, 11, 568. [Google Scholar] [CrossRef]
- Vieta, E.; Berk, M.; Schulze, T.G.; Carvalho, A.F.; Suppes, T.; Calabrese, J.R.; Gao, K.; Miskowiak, K.W.; Grande, I. Bipolar disorders. Nat. Rev. Dis. Primers 2018, 4, 18008. [Google Scholar] [CrossRef]
- Aizawa, E.; Tsuji, H.; Asahara, T.; Takahashi, T.; Teraishi, T.; Yoshida, S.; Koga, N.; Hattori, K.; Ota, M.; Kunugi, H. Bifidobacterium and Lactobacillus counts in the gut microbiota of patients with bipolar disorder and healthy controls. Front. Psychiatry 2019, 9, 730. [Google Scholar] [CrossRef] [PubMed]
- Lord, C.; Brugha, T.S.; Charman, T.; Cusack, J.; Dumas, G.; Frazier, T.; Jones, E.J.H.; Jones, R.M.; Pickles, A.; State, M.W.; et al. Autism spectrum disorder. Nat. Rev. Dis. Primers 2020, 6, 5. [Google Scholar] [CrossRef] [PubMed]
- Marder, S.R.; Cannon, T.D. Schizophrenia. N. Engl. J. Med. 2019, 381, 1753–1761. [Google Scholar] [CrossRef]
- Liang, Y.; Shi, X.; Shen, Y.; Huang, Z.; Wang, J.; Shao, C.; Chu, Y.; Chen, J.; Yu, J.; Kang, Y. Enhanced intestinal protein fermentation in schizophrenia. BMC Med. 2022, 20, 67. [Google Scholar] [CrossRef]
- Zheng, P.; Zeng, B.; Liu, M.; Chen, J.; Pan, J.; Han, Y.; Liu, Y.; Cheng, K.; Zhou, C.; Wang, H.; et al. The gut microbiome from patients with schizophrenia modulates the glutamate-glutamine-GABA cycle and schizophrenia-relevant behaviors in mice. Sci. Adv. 2019, 5, eaau8317. [Google Scholar] [CrossRef]
- Hata, T.; Miyata, N.; Takakura, S.; Yoshihara, K.; Asano, Y.; Kimura-Todani, T.; Yamashita, M.; Zhang, X.T.; Watanabe, N.; Mikami, K.; et al. The gut microbiome derived from anorexia nervosa patients impairs weight gain and behavioral performance in female mice. Endocrinology 2019, 160, 2441–2452. [Google Scholar] [CrossRef]
- Bundgaard-Nielsen, C.; Lauritsen, M.B.; Knudsen, J.K.; Rold, L.S.; Larsen, M.H.; Hindersson, P.; Villadsen, A.B.; Leutscher, P.D.C.; Hagstrøm, S.; Nyegaard, M.; et al. Children and adolescents with attention deficit hyperactivity disorder and autism spectrum disorder share distinct microbiota compositions. Gut Microbes 2023, 15, 2211923. [Google Scholar] [CrossRef]
- Gu, F.; Wu, Y.; Liu, Y.; Dou, M.; Jiang, Y.; Liang, H. Lactobacillus casei improves depression-like behavior in chronic unpredictable mild stress-induced rats by the BDNF-TrkB signal pathway and the intestinal microbiota. Food Funct. 2020, 11, 6148–6157. [Google Scholar] [CrossRef]
- Xu, J.; Tang, M.; Wu, X.; Kong, X.; Liu, Y.; Xu, X. Lactobacillus rhamnosus zz-1 exerts preventive effects on chronic unpredictable mild stress-induced depression in mice via regulating the intestinal microenvironment. Food Funct. 2022, 13, 4331–4343. [Google Scholar] [CrossRef]
- Kambe, J.; Watcharin, S.; Makioka-Itaya, Y.; Inoue, R.; Watanabe, G.; Yamaguchi, H.; Nagaoka, K. Heat-killed Enterococcus fecalis (EC-12) supplement alters the expression of neurotransmitter receptor genes in the prefrontal cortex and alleviates anxiety-like behavior in mice. Neurosci. Lett. 2020, 720, 134753. [Google Scholar] [CrossRef]
- Liu, Q.F.; Kim, H.M.; Lim, S.; Chung, M.J.; Lim, C.Y.; Koo, B.S.; Kang, S.S. Effect of probiotic administration on gut microbiota and depressive behaviors in mice. DARU J. Pharm. Sci. 2020, 28, 181–189. [Google Scholar] [CrossRef]
- Dandekar, M.P.; Palepu, M.S.K.; Satti, S.; Jaiswal, Y.; Singh, A.A.; Dash, S.P.; Gajula, S.N.R.; Sonti, R. Multi-strain probiotic formulation reverses maternal separation and chronic unpredictable mild stress-generated anxiety- and depression-like phenotypes by modulating gut microbiome-brain activity in rats. ACS Chem. Neurosci. 2022, 13, 1948–1965. [Google Scholar] [CrossRef] [PubMed]
- Tian, P.; Chen, Y.; Qian, X.; Zou, R.; Zhu, H.; Zhao, J.; Zhang, H.; Wang, G.; Chen, W. Pediococcus acidilactici CCFM6432 mitigates chronic stress-induced anxiety and gut microbial abnormalities. Food Funct. 2021, 12, 11241–11249. [Google Scholar] [CrossRef] [PubMed]
- Ding, Y.; Bu, F.; Chen, T.; Shi, G.; Yuan, X.; Feng, Z.; Duan, Z.; Wang, R.; Zhang, S.; Wang, Q.; et al. A next-generation probiotic: Akkermansia muciniphila ameliorates chronic stress-induced depressive-like behavior in mice by regulating gut microbiota and metabolites. Appl. Microbiol. Biotechnol. 2021, 105, 8411–8426. [Google Scholar] [CrossRef] [PubMed]
- Liu, Z.; Li, L.; Ma, S.; Ye, J.; Zhang, H.; Li, Y.; Sair, A.T.; Pan, J.; Liu, X.; Li, X.; et al. High-dietary fiber intake alleviates antenatal obesity-induced postpartum depression: Roles of gut microbiota and microbial metabolite short-chain fatty acid involved. J. Agric. Food Chem. 2020, 68, 13697–13710. [Google Scholar] [CrossRef]
- Tian, P.; Zhu, H.; Qian, X.; Chen, Y.; Wang, Z.; Zhao, J.; Zhang, H.; Wang, G.; Chen, W. Consumption of butylated starch alleviates the chronic restraint stress-induced neurobehavioral and gut barrier deficits through reshaping the gut microbiota. Front. Immunol. 2021, 12, 755481. [Google Scholar] [CrossRef] [PubMed]
- Mika, A.; Gaffney, M.; Roller, R.; Hills, A.; Bouchet, C.A.; Hulen, K.A.; Thompson, R.S.; Chichlowski, M.; Berg, B.M.; Fleshner, M. Feeding the developing brain: Juvenile rats fed diet rich in prebiotics and bioactive milk fractions exhibit reduced anxiety-related behavior and modified gene expression in emotion circuits. Neurosci. Lett. 2018, 677, 103–109. [Google Scholar] [CrossRef]
- Zhang, Y.; Guo, M.; Zhang, H.; Wang, Y.; Li, R.; Liu, Z.; Zheng, H.; You, C. Lactiplantibacillus plantarum ST-III-fermented milk improves autistic-like behaviors in valproic acid-induced autism spectrum disorder mice by altering gut microbiota. Front. Nutr. 2022, 9, 1005308. [Google Scholar] [CrossRef]
- Bidô, R.C.A.; Pereira, D.E.; Alves, M.D.C.; Dutra, L.M.G.; Costa, A.; Viera, V.B.; Araújo, W.J.; Leite, E.L.; Oliveira, C.J.B.; Alves, A.F.; et al. Mix of almond baru (Dipteryx alata Vog.) and goat whey modulated intestinal microbiota, improved memory and induced anxiolytic like behavior in aged rats. J. Psychiatr. Res. 2023, 164, 98–117. [Google Scholar] [CrossRef]
- Zhang, F.; Zhou, Y.; Chen, H.; Jiang, H.; Zhou, F.; Lv, B.; Xu, M. Curcumin alleviates DSS-induced anxiety-like behaviors via the microbial-brain-gut axis. Oxid. Med. Cell. Longev. 2022, 2022, 6244757. [Google Scholar] [CrossRef]
- Xia, J.; Gu, L.; Guo, Y.; Feng, H.; Chen, S.; Jurat, J.; Fu, W.; Zhang, D. Gut microbiota mediates the preventive effects of dietary capsaicin against depression-like behavior induced by lipopolysaccharide in mice. Front. Cell. Infect. Microbiol. 2021, 11, 627608. [Google Scholar] [CrossRef]
- Wei, D.; Zhao, Y.; Zhang, M.; Zhu, L.; Wang, L.; Yuan, X.; Wu, C. The volatile oil of Zanthoxylum bungeanum pericarp improved the hypothalamic-pituitary-adrenal axis and gut microbiota to attenuate chronic unpredictable stress-induced anxiety behavior in rats. Drug Des. Dev. Ther. 2021, 15, 769–786. [Google Scholar] [CrossRef]
- Bell, L.; Whyte, A.; Duysburgh, C.; Marzorati, M.; Van den Abbeele, P.; Le Cozannet, R.; Fança-Berthon, P.; Fromentin, E.; Williams, C. A randomized, placebo-controlled trial investigating the acute and chronic benefits of American Ginseng (Cereboost®) on mood and cognition in healthy young adults, including in vitro investigation of gut microbiota changes as a possible mechanism of action. Eur. J. Nutr. 2022, 61, 413–428. [Google Scholar] [CrossRef] [PubMed]
- Zhao, F.; Guan, S.; Fu, Y.; Wang, K.; Liu, Z.; Ng, T.B. Lycium barbarum polysaccharide attenuates emotional injury of offspring elicited by prenatal chronic stress in rats via regulation of gut microbiota. Biomed. Pharmacother. 2021, 143, 112087. [Google Scholar] [CrossRef] [PubMed]
- Han, S.K.; Kim, J.K.; Park, H.S.; Shin, Y.J.; Kim, D.H. Chaihu-Shugan-San (Shihosogansan) alleviates restraint stress-generated anxiety and depression in mice by regulating NF-κB-mediated BDNF expression through the modulation of gut microbiota. Chin. Med. 2021, 16, 77. [Google Scholar] [CrossRef] [PubMed]
- Hao, W.; Wu, J.; Yuan, N.; Gong, L.; Huang, J.; Ma, Q.; Zhu, H.; Gan, H.; Da, X.; Deng, L.; et al. Xiaoyaosan improves antibiotic-induced depressive-like and anxiety-like behavior in mice through modulating the gut microbiota and regulating the NLRP3 inflammasome in the colon. Front. Pharmacol. 2021, 12, 619103. [Google Scholar] [CrossRef]
- Chen, P.; Hei, M.; Kong, L.; Liu, Y.; Yang, Y.; Mu, H.; Zhang, X.; Zhao, S.; Duan, J. One water-soluble polysaccharide from Ginkgo biloba leaves with antidepressant activities via modulation of the gut microbiome. Food Funct. 2019, 10, 8161–8171. [Google Scholar] [CrossRef]
- Zheng, Y.; Yu, Z.; Zhang, W.; Sun, T. Lactobacillus rhamnosus probio-m9 improves the quality of life in stressed adults by gut microbiota. Foods 2021, 10, 2384. [Google Scholar] [CrossRef]
- Lee, H.J.; Hong, J.K.; Kim, J.K.; Kim, D.H.; Jang, S.W.; Han, S.W.; Yoon, I.Y. Effects of probiotic NVP-1704 on mental health and sleep in healthy adults: An 8-week randomized, double-blind, placebo-controlled trial. Nutrients 2021, 13, 2660. [Google Scholar] [CrossRef]
- Ma, T.; Jin, H.; Kwok, L.Y.; Sun, Z.; Liong, M.T.; Zhang, H. Probiotic consumption relieved human stress and anxiety symptoms possibly via modulating the neuroactive potential of the gut microbiota. Neurobiol. Stress 2021, 14, 100294. [Google Scholar] [CrossRef]
- Tian, P.; Chen, Y.; Zhu, H.; Wang, L.; Qian, X.; Zou, R.; Zhao, J.; Zhang, H.; Qian, L.; Wang, Q.; et al. Bifidobacterium breve CCFM1025 attenuates major depression disorder via regulating gut microbiome and tryptophan metabolism: A randomized clinical trial. Brain Behav. Immun. 2022, 100, 233–241. [Google Scholar] [CrossRef] [PubMed]
- Reininghaus, E.Z.; Platzer, M.; Kohlhammer-Dohr, A.; Hamm, C.; Mörkl, S.; Bengesser, S.A.; Fellendorf, F.T.; Lahousen-Luxenberger, T.; Leitner-Afschar, B.; Schöggl, H.; et al. PROVIT: Supplementary probiotic treatment and vitamin B7 in depression-a randomized controlled trial. Nutrients 2020, 12, 3422. [Google Scholar] [CrossRef] [PubMed]
- Johnstone, N.; Milesi, C.; Burn, O.; van den Bogert, B.; Nauta, A.; Hart, K.; Sowden, P.; Burnet, P.W.J.; Cohen Kadosh, K. Anxiolytic effects of a galacto-oligosaccharides prebiotic in healthy females (18-25 years) with corresponding changes in gut bacterial composition. Sci. Rep. 2021, 11, 8302. [Google Scholar] [CrossRef] [PubMed]
- Talbott, S.M.; Talbott, J.A.; Stephens, B.J.; Oddou, M.P. Effect of coordinated probiotic/prebiotic/phytobiotic supplementation on microbiome balance and psychological mood state in healthy stressed adults. Funct. Foods Health Dis. 2019, 9, 265–275. [Google Scholar] [CrossRef]
- Grimaldi, R.; Gibson, G.R.; Vulevic, J.; Giallourou, N.; Castro-Mejía, J.L.; Hansen, L.H.; Leigh Gibson, E.; Nielsen, D.S.; Costabile, A. A prebiotic intervention study in children with autism spectrum disorders (ASDs). Microbiome 2018, 6, 133. [Google Scholar] [CrossRef]
- Tarutani, S.; Omori, M.; Ido, Y.; Yano, M.; Komatsu, T.; Okamura, T. Effects of 4G-beta-D-Galactosylsucrose in patients with depression: A randomized, double-blinded, placebo-controlled, parallel-group comparative study. J. Psychiatr. Res. 2022, 148, 110–120. [Google Scholar] [CrossRef]
- Cannavale, C.N.; Mysonhimer, A.R.; Bailey, M.A.; Cohen, N.J.; Holscher, H.D.; Khan, N.A. Consumption of a fermented dairy beverage improves hippocampal-dependent relational memory in a randomized, controlled cross-over trial. Nutr. Neurosci. 2023, 26, 265–274. [Google Scholar] [CrossRef]
- Zhang, X.; Chen, S.; Zhang, M.; Ren, F.; Ren, Y.; Li, Y.; Liu, N.; Zhang, Y.; Zhang, Q.; Wang, R. Effects of fermented milk containing lacticaseibacillus paracasei strain shirota on constipation in patients with depression: A randomized, double-blind, placebo-controlled trial. Nutrients 2021, 13, 2238. [Google Scholar] [CrossRef]
- Park, M.; Choi, J.; Lee, H.J. Flavonoid-rich orange juice intake and altered gut microbiome in young adults with depressive symptom: A randomized controlled study. Nutrients 2020, 12, 1815. [Google Scholar] [CrossRef]
- Zhou, H.; Zhang, S.; Zhang, X.; Zhou, H.; Wen, T.; Wang, J. Depression-like symptoms due to Dcf1 deficiency are alleviated by intestinal transplantation of Lactobacillus murine and Lactobacillus reuteri. Biochem. Biophys. Res. Commun. 2022, 593, 137–143. [Google Scholar] [CrossRef]
- Slykerman, R.F.; Hood, F.; Wickens, K.; Thompson, J.M.D.; Barthow, C.; Murphy, R.; Kang, J.; Rowden, J.; Stone, P.; Crane, J.; et al. Effect of Lactobacillus rhamnosus hn001 in pregnancy on postpartum symptoms of depression and anxiety: A randomised double-blind placebo-controlled trial. EBioMedicine 2017, 24, 159–165. [Google Scholar] [CrossRef]
- Aslam, H.; Green, J.; Jacka, F.N.; Collier, F.; Berk, M.; Pasco, J.; Dawson, S.L. Fermented foods, the gut and mental health: A mechanistic overview with implications for depression and anxiety. Nutr. Neurosci. 2020, 23, 659–671. [Google Scholar] [CrossRef] [PubMed]
- Munawar, N.; Ahmad, A.; Anwar, M.A.; Muhammad, K. Modulation of gut microbial diversity through non-pharmaceutical approaches to treat schizophrenia. Int. J. Mol. Sci. 2022, 23, 2625. [Google Scholar] [CrossRef]
- Xiong, R.G.; Zhou, D.D.; Wu, S.X.; Huang, S.Y.; Saimaiti, A.; Yang, Z.J.; Shang, A.; Zhao, C.N.; Gan, R.Y.; Li, H.B. Health benefits and side effects of short-chain fatty acids. Foods 2022, 11, 2863. [Google Scholar] [CrossRef] [PubMed]
- Huang, J.; Kang, D.; Zhang, F.; Yang, Y.; Liu, C.; Xiao, J.; Long, Y.; Lang, B.; Peng, X.; Wang, W.; et al. Probiotics plus dietary fiber supplements attenuate olanzapine-induced weight gain in drug-naïve first-episode schizophrenia patients: Two randomized clinical trials. Schizophr. Bull. 2022, 48, 850–859. [Google Scholar] [CrossRef] [PubMed]
- Tang, C.F.; Wang, C.Y.; Wang, J.H.; Wang, Q.N.; Li, S.J.; Wang, H.O.; Zhou, F.; Li, J.M. Short-chain fatty acids ameliorate depressive-like behaviors of high fructose-fed mice by rescuing hippocampal neurogenesis decline and blood-brain barrier damage. Nutrients 2022, 14, 1882. [Google Scholar] [CrossRef]
- Leo, A.; De Caro, C.; Mainardi, P.; Tallarico, M.; Nesci, V.; Marascio, N.; Striano, P.; Russo, E.; Constanti, A.; De Sarro, G.; et al. Increased efficacy of combining prebiotic and postbiotic in mouse models relevant to autism and depression. Neuropharmacology 2021, 198, 108782. [Google Scholar] [CrossRef]
- Yu, B.; Zhu, Q.; Meng, G.; Gu, Y.; Zhang, Q.; Liu, L.; Wu, H.; Xia, Y.; Bao, X.; Shi, H.; et al. Habitual yoghurt consumption and depressive symptoms in a general population study of 19,596 adults. Eur. J. Nutr. 2018, 57, 2621–2628. [Google Scholar] [CrossRef]
- Liu, Q.; Meng, X.; Li, Y.; Zhao, C.N.; Tang, G.Y.; Li, H.B. Antibacterial and antifungal activities of spices. Int. J. Mol. Sci. 2017, 18, 1283. [Google Scholar] [CrossRef]
- Zheng, J.; Zhou, Y.; Li, Y.; Xu, D.P.; Li, S.; Li, H.B. Spices for prevention and treatment of cancers. Nutrients 2016, 8, 495. [Google Scholar] [CrossRef]
- Xu, X.Y.; Meng, X.; Li, S.; Gan, R.Y.; Li, Y.; Li, H.B. Bioactivity, health benefits, and related molecular mechanisms of curcumin: Current progress, challenges, and perspectives. Nutrients 2018, 10, 1553. [Google Scholar] [CrossRef] [PubMed]
- Yang, Z.J.; Huang, S.Y.; Zhou, D.D.; Xiong, R.G.; Zhao, C.N.; Fang, A.P.; Zhang, Y.J.; Li, H.B.; Zhu, H.L. Effects and mechanisms of curcumin for the prevention and management of cancers: An updated review. Antioxidants 2022, 11, 1481. [Google Scholar] [CrossRef] [PubMed]
- Rees, J.; Radavelli Bagatini, S.; Lo, J.; Hodgson, J.M.; Christophersen, C.T.; Daly, R.M.; Magliano, D.J.; Shaw, J.E.; Sim, M.; Bondonno, C.P.; et al. Association between fruit and vegetable intakes and mental health in the australian diabetes obesity and lifestyle cohort. Nutrients 2021, 13, 1447. [Google Scholar] [CrossRef] [PubMed]
- Robinette, L.M.; Hatsu, I.E.; Johnstone, J.M.; Tost, G.; Bruton, A.M.; Leung, B.M.Y.; Odei, J.B.; Orchard, T.; Gracious, B.L.; Arnold, L.E. Fruit and vegetable intake is inversely associated with severity of inattention in a pediatric population with ADHD symptoms: The MADDY Study. Nutr. Neurosci. 2023, 26, 572–581. [Google Scholar] [CrossRef] [PubMed]


| Study Type | Participants | Changes of Gut Microbiota in Mental Diseases | Ref. |
|---|---|---|---|
| Anxiety | |||
| Case-control study | 14 adult individuals with social exclusion and 25 HCs | ↓ Firmicutes/Bacteroidetes and Faecalibacterium spp. | [30] |
| Prospective observational study | 129 patients with active UC, 49 patients with depression and anxiety (non-UC), and 62 HCs | ↓ Prevotella_9, Lachnospira ↑ Lactobacillales, Sellimonas, and Streptococcus | [31] |
| Cross-sectional study | 40 GAD patients and 36 HCs | ↑ Fusobacteria, Bacteroidetes spp. ↓ Firmicutes spp., Lachnospira, and Butyricicoccus | [32] |
| Depression | |||
| Cross-sectional study | 24 CDE patients and 16 HCs | ↑ Akkermansia, Clostridium_sensu_stricto_1, UBA1819 ↓ Dialister, Fusicatenibacter, and Lachnospira | [33] |
| Cohort study | 1054 samples | ↓ Dialister, Coprococcus spp. | [34] |
| Cross-sectional study | 60 MDD patients and 60 HCs | ↑ phylum Firmicutes, genera Prevotella and Klebsiella ↓ Bacteroidetes | [35] |
| Cross-sectional study | 10 MDD patients and 10 HCs | ↑ Firmicutes, Actinobacteria ↓ Bacteroidetes, Proteobacteria | [36] |
| - | 91 premenopausal females with depression and 98 HCs | ↑ Klebsiella aerogenes | [37] |
| Bipolar disorder | |||
| Cross-sectional study | 23 BD patients and 23 HCs | ↑ Clostridiaceae and Collinsella | [38] |
| Cross-sectional study | 115 BD patients and 64 HCs | ↓ Faecalibacterium | [39] |
| Cross-sectional study | 32 BD patients and 10 HCs | ↑ phylum Actinobacteria and Coriobacteria ↓ Ruminococcaceae and Faecalibacterium | [40] |
| Cross-sectional study | 113 BD patients, 39 unaffected first-degree relatives, and 77 HCs | ↑ Flavonifractor | [41] |
| Autism spectrum disorder | |||
| Cross-sectional study | 39 PTHS children and 46 unaffected family members | ↑ Clostridium bolteae | [42] |
| Cross-sectional case-control study | ASD children with (n = 60) or without (n = 60) sleep disorder | ↓ Faecalibacterium and Agathobacter | [43] |
| Cross-sectional study | 30 ASD children and 30 neurotypical controls | ↑ Clostridium paraputri, Clostridium bolteae, and Clostridium perfringens | [44] |
| Cross-sectional case-control study | 48 ASD children and 57 HCs | ↑ Actinobacteria, Proteobacteria and Bacilli | [45] |
| Schizophrenia | |||
| Cross-sectional study | 38 schizophrenia patients and 20 HCs | ↓ Acetanaerobacterium, Haemophilus, and Turicibacter | [46] |
| Cross-sectional study | 42 patients with acute schizophrenia, 40 patients with schizophrenia in remission, and 44 HCs | ↑ Haemophilus ↓ Coprococcus | [47] |
| Cross-sectional study | 38 schizophrenia patients and 38 NCs | ↑ Veillonella ↓ Ruminococcus and Roseburia | [48] |
| Cross-sectional study | 48 schizophrenia patients and 48 NCs | ↑ Lachnospiraceae | [49] |
| Cross-sectional study | 82 schizophrenia patients and 80 NCs | ↑ Collinsella, Lactobacillus, and Succinivibrio ↓ Adlercreutzia, Anaerostipes, and Ruminococcus | [50] |
| Cross-sectional study | 10 schizophrenia patients and 16 HCs | ↑ Proteobacteria ↓ Faecalibacterium and Lachnospiraceae | [51] |
| Metagenome-wide association study | 90 medication-free schizophrenia patients and 81 NCs | ↑ Lactobacillus fermentum, Enterococcus faecium, and Alkaliphilus oremlandii | [52] |
| Anorexia nervosa | |||
| Cohort study | 77 females with anorexia nervosa and 70 HCs | ↑ Erysipelatoclostridium ramosum, Enterocloster bolteae ↓ Eisenbergiella, butyrate-producing bacterium | [53] |
| Posttraumatic stress disorder | |||
| Longitudinal investigation | 71 FHWs and 104 SHWs | ↑ Bacteroides eggerthii ↓ Eubacterium hallii group uncultured bacterium | [54] |
| Case-control study | 79 PTSD participants and 58 TECs | ↑ Mitsuokella, Odoribacter, and Catenibacterium | [55] |
| Attention deficit hyperactivity disorder | |||
| Case-control study | 41 ADHD children and 39 HCs | ↑ Agathobacter, Anaerostipes, and Lachnospiraceae | [56] |
| Others | |||
| Cross-sectional study | 198 individuals | Anxiety: ↓ Simpson’s diversity PTSD, depression, and trait anxiety: ↓ Fusicatenibacter saccharivorans | [57] |
| Study Type | Animals | Changes of Gut Microbiota in Mental Diseases | Ref. |
|---|---|---|---|
| Anxiety | |||
| In vivo | BALB/c, Orient C57BL/6N, Taconic C57BL/6N, and Taconic C57BL/6J mice | ↓ Firmicutes | [58] |
| Depression | |||
| In vivo | Female depression-like macaques | ↑ family Paraprevotella ↓ families Streptococcaceae, Gemella | [59] |
| In vivo | C57BL/6J female mice | ↑ Klebsiella aerogenes | [37] |
| Autism spectrum disorder | |||
| In vivo | Fmr1 KO mice on a C57BL/6J background | ↓ Akkermansia muciniphila | [60] |
| Study Type | Subjects | Methods | Alterations of the Gut Microbiota | Ref. |
|---|---|---|---|---|
| Probiotics | ||||
| In vivo | Male Sprague–Dawley rats | L. casei for 3 weeks | ↑ Blautia and Roseburia ↓ Prevotella | [78] |
| In vivo | Male C57BL/6 mice | L. rhamnosus zz-1 for 6 weeks | ↑ Lachnospiraceae NK4A136 group, Bacteroides, and Muribaculum | [79] |
| In vivo | Male C57BL/6 J mice | Diet supplemented with 0.125% heat-killed EC-12 | ↑ Butyricicoccus and Enterococcus | [80] |
| In vivo | Male ICR mice | Mixture of L. plantarum LP3, L. rhamnosus LR5, B. lactis BL3, B. breve BR3, and P. pentosaceus PP1 for 8 weeks | ↑ Actinobacteria, Cyanobacteria, and S24-7_unclassified | [81] |
| In vivo | Sprague–Dawley rats | Mixture of B. coagulans unique IS-2, L. plantarum UBLP-40, L. rhamnosus UBLR-58, B. lactis UBBLa-70, B. breve UBBr-01, and B. infantis UBBI-01 for 6 weeks | ↑ Firmicutes/Bacteroides | [82] |
| In vivo | Male C57BL/6 mice | Pediococcus acidilactici CCFM6432 for 5 weeks | ↑ Bifidobacterium ↓ Escherichia-shigella | [83] |
| In vivo | Male C57BL/6 mice | Akkermansia muciniphila for 3 weeks | ↑ Verrucomicrobia and Akkermansia ↓ Helicobacter, Lachnoclostridium, and Candidatus_Saccharimonas | [84] |
| Prebiotics and postbiotics | ||||
| In vivo | Female C57BL/6J mice | Inulin (37 g/1000 kcal) for 20 weeks | ↑ Lactobacillus, Prevotella, and Lactobacillus | [85] |
| In vivo | Male BALB/c mice | SCFA-acylated starches (20 w/v) for 3 weeks | ↑ Odoribacter and Oscillibacter | [86] |
| Dairy products | ||||
| In vivo | Juvenile (PND 24), male Fischer 344 rats | GOS (21.23 g/kg), PDX (6.58 g/kg), lactoferrin (1.86 g/kg) and whey protein concentrate MFGM-10 (15.9 g/kg) | ↑ Lactobacillus spp. | [87] |
| In vivo | ICR mice | 400 μL L. plantarum ST-III-fermented milk in the morning and evening for 2 weeks | ↑ family Lachnospiraceae and genus Kineothrix | [88] |
| In vivo | 40 elderly male Wistar rats | 2000 mg of almond baru+ 2000 mg of goat milk whey/kg for 10 weeks | ↑ Gastranaerophilales and Ruminococcaceae ↓ Clostridia_UCG-014 | [89] |
| Spices | ||||
| In vivo | C57BL/6 mice | Curcumin (100 mg/kg/d) for 8 d | ↑ Bacteroidetes, Muribaculaceae_unclassified ↓ Deinococcus-Thermus, Bacteroides, and Ruminococcaceae_unclassified | [90] |
| In vivo | Male C57BL/6 mice | Diet supplement with 0.005% capsaicin for 4 months | ↑ Ruminococcus, Prevotella, and Allobaculum | [91] |
| In vivo | Male Sprague–Dawley rats | VOZB (50, 100 and 200 mg/kg/d) by an intragastric gavage for 14 d | ↑ Bacteroidales_S24-7_group, Lactobacillaceae, and Prevotellaceae ↓ Lachnospiraceae | [92] |
| Medicinal herbs | ||||
| In vitro | Simulator of the human intestinal microbial ecosystem | Cereboost® (200 mg/d) for 3 weeks | ↑ Lactobacillus and Akkermansia muciniphila | [93] |
| In vivo | Sprague–Dawley rats | LBP (40 mg/kg) for 14 d | ↑ Firmicutes ↓ Turicibacter | [94] |
| In vivo | Male C57BL/6 mice | CSS (1.0 g/kg/d) for 5 d | ↑ Lactobacillaceae, Prevotellaceae, and AC160630_f ↓ gamma-Proteobacteria | [95] |
| In vivo | Male C57BL/6 mice | Xiaoyaosan (0.658 g/kg/d) for 14 d | ↑ Lachnospiraceae ↓ Bacteroidaceae | [96] |
| In vivo | Male BALB/c mice | GPS (300 mg/kg in PBS) for 4 weeks | ↑ Prevotellaceae, Erysipelotrichaceae, and Family_XIII | [97] |
| Study Type | Participants | Methods | Alterations of the Gut Microbiota | Ref. |
|---|---|---|---|---|
| Probiotics | ||||
| Double-blind placebo RCT | 12 postgraduate student volunteers | L. rhamnosus Probio-M9 for 21 d | ↑ Barnesiella and Akkermansia | [98] |
| Double-blind placebo RCT | 156 healthy adults with subclinical symptoms of depression, anxiety, and insomnia | Two 500 mg capsules for 8 weeks | ↑ Bifidobacteriaceae and Lactobacillacea ↓ Enterobacteriaceae | [99] |
| Double-blind placebo RCT | 103 stressed adults | L. plantarum P-8 for 12 weeks | ↑ Bifidobacterium adolescentis, Bifidobacterium longum and Fecalibacterium prausnitzii ↓ Roseburia faecis and Fusicatenibacter saccharivorans | [100] |
| Double-blind placebo RCT | 45 patients with MDD | Bifidobacterium breve CCFM1025 powder for 4 weeks | ↑ Desulfovibrio and Faecalibaculum | [101] |
| Monocentric, placebo RCT | 82 depressed individuals | Mixture of 9 probiotics for 28 d | ↓ Ruminococcus gauvreauii and Coprococcus 3 | [102] |
| Prebiotics and postbiotics | ||||
| Double-blind placebo RCT | 64 healthy females | GOS prebiotic for 28 d | ↑ Bifidobacterium | [103] |
| Double-blind placebo RCT | 33 healthy subjects | Natural multi-ingredient targeted mental wellness supplement for 4 weeks | ↑ Lactobacillus and Bifidobacterium | [104] |
| Double-blind placebo RCT | 30 autistic children | B-GOS® for 6 weeks | ↑ Coprococcus spp., Dorea formicigenerans, and Oribacterium spp. | [105] |
| Double-blind placebo RCT | 22 patients with depression | LS for 24 weeks | No significant change | [106] |
| Dairy products | ||||
| Cross-over RCT | 26 healthy adults | A dairy-based fermented beverage for 4 weeks | ↑ Lactobacillus ↓ Phascolarctobacterium | [107] |
| Double-blind placebo RCT | 82 depressive patients with constipation | Fermented dairy beverage for 9 weeks | ↑ Adlercreutzia, Megasphaera, and Veillonella ↓ Rikenellaceae_RC9_gut_group, Sutterella, and Oscillibacter | [108] |
| Fruits | ||||
| RCT | 40 participants | Flavonoid-rich orange juice for 8 weeks | ↑ Lachnospiraceae_uc, Bifidobacterium_uc, and Eubacterium_g4 | [109] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Xiong, R.-G.; Li, J.; Cheng, J.; Zhou, D.-D.; Wu, S.-X.; Huang, S.-Y.; Saimaiti, A.; Yang, Z.-J.; Gan, R.-Y.; Li, H.-B. The Role of Gut Microbiota in Anxiety, Depression, and Other Mental Disorders as Well as the Protective Effects of Dietary Components. Nutrients 2023, 15, 3258. https://doi.org/10.3390/nu15143258
Xiong R-G, Li J, Cheng J, Zhou D-D, Wu S-X, Huang S-Y, Saimaiti A, Yang Z-J, Gan R-Y, Li H-B. The Role of Gut Microbiota in Anxiety, Depression, and Other Mental Disorders as Well as the Protective Effects of Dietary Components. Nutrients. 2023; 15(14):3258. https://doi.org/10.3390/nu15143258
Chicago/Turabian StyleXiong, Ruo-Gu, Jiahui Li, Jin Cheng, Dan-Dan Zhou, Si-Xia Wu, Si-Yu Huang, Adila Saimaiti, Zhi-Jun Yang, Ren-You Gan, and Hua-Bin Li. 2023. "The Role of Gut Microbiota in Anxiety, Depression, and Other Mental Disorders as Well as the Protective Effects of Dietary Components" Nutrients 15, no. 14: 3258. https://doi.org/10.3390/nu15143258
APA StyleXiong, R.-G., Li, J., Cheng, J., Zhou, D.-D., Wu, S.-X., Huang, S.-Y., Saimaiti, A., Yang, Z.-J., Gan, R.-Y., & Li, H.-B. (2023). The Role of Gut Microbiota in Anxiety, Depression, and Other Mental Disorders as Well as the Protective Effects of Dietary Components. Nutrients, 15(14), 3258. https://doi.org/10.3390/nu15143258







