The Role of Zinc in Selected Female Reproductive System Disorders
Abstract
1. Introduction
1.1. General Information
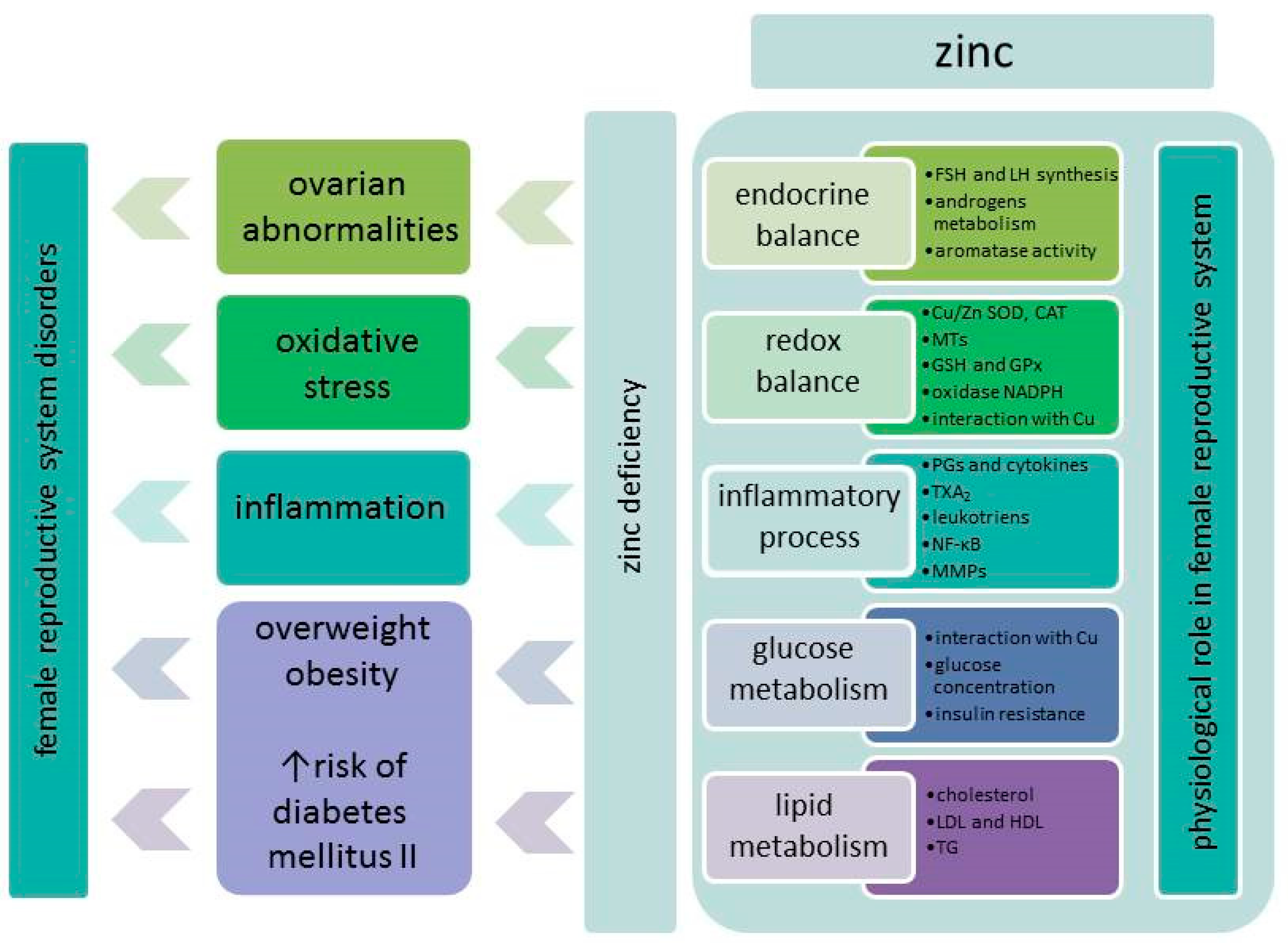
1.2. Role of Zinc in Female Reproductive System
2. Materials and Methods
3. Results and Discussion
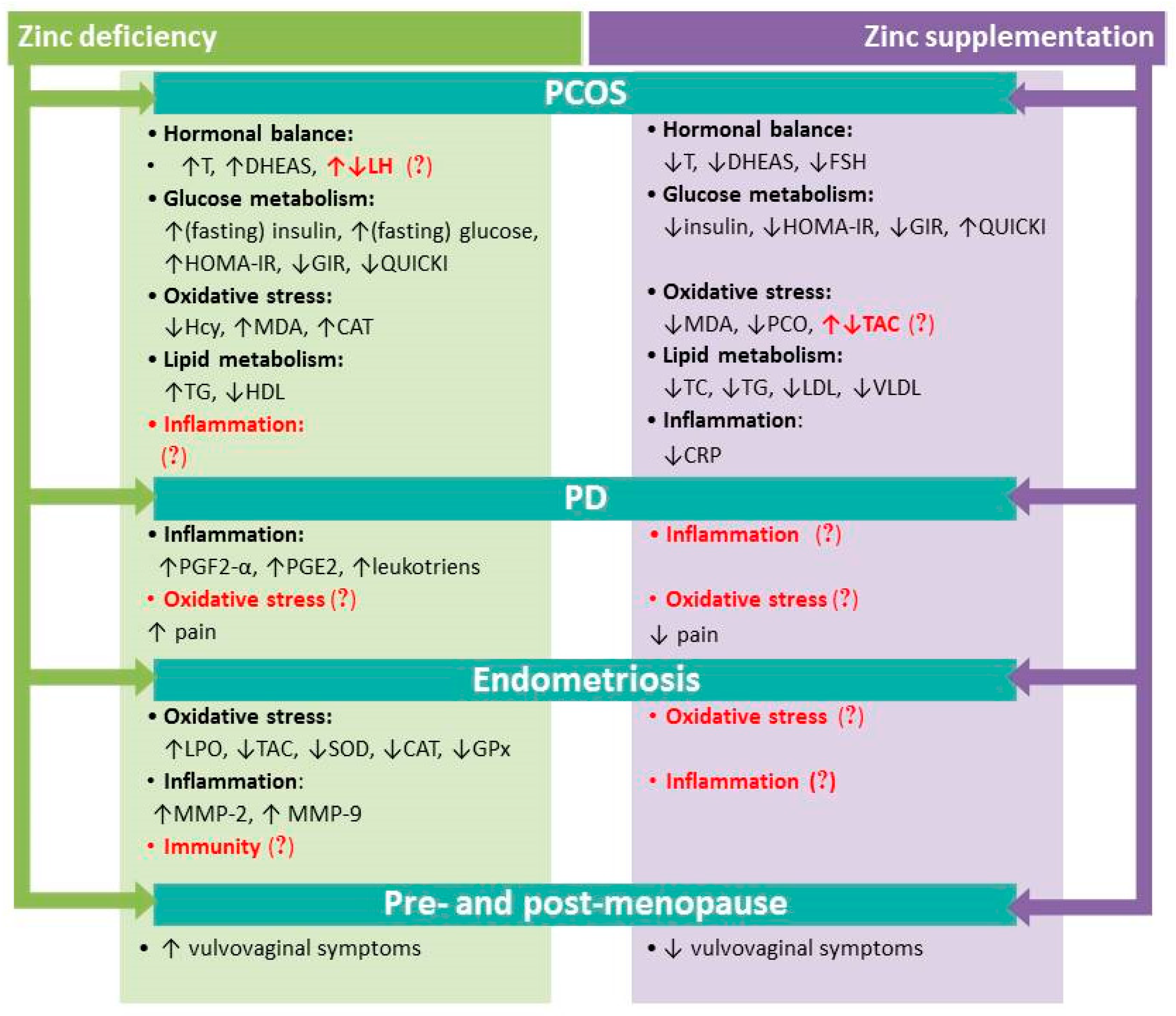
3.1. Zinc and Polycystic Ovary Syndrome (PCOS)
3.2. Zinc and Dysmenorrhea
3.3. Zinc and Endometriosis
3.4. Zinc in Pre- and Post-Menopause
4. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Chasapis, C.T.; Ntoupa, P.-S.A.; Spiliopoulou, C.A.; Stefanidou, M.E. Recent aspects of the effects of zinc on human health. Arch. Toxicol. 2020, 94, 1443–1460. [Google Scholar] [CrossRef] [PubMed]
- Kerns, K.C.; Zigo, M.; Sutovsky, P. Zinc: A Necessary Ion for Mammalian Sperm Fertilization Competency. Int. J. Mol. Sci. 2018, 19, 4097. [Google Scholar] [CrossRef] [PubMed]
- King, J.C.; Brown, K.H.; Gibson, R.S.; Krebs, N.F.; Lowe, N.M.; Siekmann, J.H.; Raiten, D.J. Biomarkers of Nutrition for Development (BOND)-Zinc Review. J. Nutr. 2016, 146, 858S–885S. [Google Scholar] [CrossRef] [PubMed]
- Livingstone, C. Zinc: Physiology, deficiency, and parenteral nutrition. Nutr. Clin. Pract. 2015, 30, 371–382. [Google Scholar] [CrossRef]
- Sandstead, H.H.; Au, W. Chapter 47—Zinc. In Handbook on the Toxicology of Metals, 3rd ed.; Norberg, G.F., Fowler, B.A., Norberg, M., Filberg, L.T., Eds.; Academic Press, Elsevier: Amsterdam, The Netherlands, 2007; pp. 925–945. [Google Scholar]
- Ebisch, I.M.; Thomas, C.; Peters, W.; Braat, D.; Steegers-Theunissen, R.P.M. The importance of folate, zinc and antioxidants in the pathogenesis and prevention of subfertility. Hum. Reprod. Update 2006, 13, 163–174. [Google Scholar] [CrossRef]
- Murarka, S.; Mishra, V.; Joshi, P.; Kumar, S. Role of zinc in reproductive biology—An overview. Austin J. Reprod. Med. Infertil. 2015, 2, 1009. [Google Scholar]
- World Health Organization (WHO); Food and Agricultural Organization (FAO). Vitamin and Mineral Requirements in Human Nutrition, 2nd ed.; WHO: Geneva, Switzerland, 2004. [Google Scholar]
- Institute of Medicine (IOM). Dietary Reference Intakes of Vitamin A, Vitamin K, Arsenic Boron, Chromium, Copper, Iodine, Iron, Manganese, Molybdenum, Nickel, Silicon, Vanadium, and Zinc; National Academy Press: Washington, WA, USA, 2002. [Google Scholar]
- European Food Safety Authority. Scientific opinion on dietary reference values of zinc (EFSA). EFSA Panel on dietetic products, nutrition and allergies (NDA). EFSA J. 2014, 12, 3844. [Google Scholar] [CrossRef]
- Brown, K.H.; Wuchler, S.E.; Peerson, J.M. The Importance of Zinc in Human Nutrition and Estimation of the Global Prevalence of Zinc Deficiency. Food Nutr. Bull. 2001, 22, 113–125. [Google Scholar] [CrossRef]
- Roohani, N.; Hurrell, R.; Kelishadi, R.; Schulin, R. Zinc and its importance for human health: An integrative review. J. Res. Med. Sci. 2013, 18, 144–157. [Google Scholar]
- World Heath Organization (WHO). Trace Elements in Human Nutrition and Health; WHO: Geneva, Switzerland, 1996. [Google Scholar]
- Bhowmik, D.; Bhattacharjee, C.; Kumar, S. A potential medicinal importance of zinc in human health and chronic disease. Int. J. Pharm. Biomed. Sci. 2010, 1, 5–11. [Google Scholar]
- Maret, W. Zinc and human disease. In Interrelations between Essential Metal Ions and Human Diseases; Sigel, A., Sigel, H., Sigel, R.K.O., Eds.; Springer: Dordrecht, The Netherlands, 2013; Volume 13, pp. 389–414. [Google Scholar] [CrossRef]
- Vallee, B.L.; Falchuk, K.H. The biochemical basis of zinc physiology. Physiol. Rev. 1993, 73, 79–118. [Google Scholar] [CrossRef] [PubMed]
- Kelleher, S.L.; McCormick, N.H.; Velasquez, V.; Lopez, V. Zinc in Specialized Secretory Tissues: Roles in the Pancreas, Prostate, and Mammary Gland12. Adv. Nutr. 2011, 2, 101–111. [Google Scholar] [CrossRef] [PubMed]
- Kanafchian, M.; Mahjoub, S.; Esmaeilzadeh, S.; Rahsepar, M.; Mousapour, A. Status of serum selenium and zinc in patients with the polycystic ovary syndrome with and without insulin resistance. Middle East Fertil. Soc. J. 2018, 23, 241–245. [Google Scholar] [CrossRef]
- Cummings, J.E.; Kovacic, J.P. The ubiquitous role of zinc in health and disease. J. Vet. Emerg. Crit. Care 2009, 19, 215–240. [Google Scholar] [CrossRef]
- Cicero, A.F.; Allkanjari, O.; Busetto, G.M.; Cai, T.; Larganà, G.; Magri, V.; Perlett, G.; Della Cuna, F.S.R.; Russo, G.I.; Stamatiou, K.; et al. Nutraceutical treatment and prevention of benign prostatic hyperplasia and prostate cancer. Arch. Ital. Urol. Androl. 2019, 91, 139–152. [Google Scholar] [CrossRef]
- Das, K.; Buchholz, N. Benign prostate hyperplasia and nutrition. Clin. Nutr. ESPEN 2019, 33, 5–11. [Google Scholar] [CrossRef]
- Ho, E.; Song, Y. Zinc and prostatic cancer. Curr. Opin. Clin. Nutr. Metab. Care 2009, 12, 640–645. [Google Scholar] [CrossRef]
- Ota, E.; Mori, R.; Middleton, P.; Tobe-Gai, R.; Mahomed, K.; Miyazaki, C.; Bhutta, Z.A. Zinc supplementation for improving pregnancy and infant outcome. Cochrane Database Syst. Rev. 2015, 2015, CD000230. [Google Scholar] [CrossRef]
- Wilson, R.L.; Grieger, J.A.; Bianco-Miotto, T.; Roberts, C.T. Association between Maternal Zinc Status, Dietary Zinc Intake and Pregnancy Complications: A Systematic Review. Nutrients 2016, 8, 641. [Google Scholar] [CrossRef]
- Bedwal, R.S.; Bahuguna, A. Zinc, copper and selenium in reproduction. Experientia 1994, 50, 626–640. [Google Scholar] [CrossRef]
- Wang, H.; Hu, Y.-F.; Hao, J.-H.; Chen, Y.-H.; Su, P.-Y.; Wang, Y.; Yu, Z.; Fu, L.; Xu, Y.-Y.; Zhang, C.; et al. Maternal zinc deficiency during pregnancy elevates the risks of fetal growth restriction: A population-based birth cohort study. Sci. Rep. 2015, 5, 11262. [Google Scholar] [CrossRef] [PubMed]
- Zheng, G.; Wang, L.; Guo, Z.; Sun, L.; Wang, L.; Wang, C.; Zuo, Z.; Qiu, H. Association of Serum Heavy Metals and Trace Element Concentrations with Reproductive Hormone Levels and Polycystic Ovary Syndrome in a Chinese Population. Biol. Trace Elem. Res. 2015, 167, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Aliyev, U.; Pehlivantürk-Kızılkan, M.; Düzçeker, Y.; Kanbur, N.; Aycan, Z.; Akgül, S.; Derman, O. Is There Any Association Between Hirsutism and Serum Zinc Levels in Adolescents? Biol. Trace Elem. Res. 2020, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Bizoń, A.; Słowiak, A.; Franik, G.; Biernacka-Bartnik, A.; Madej, P. Zinc, copper, sirtuin 1 concentration, and glucose metabolism parameters in the blood of women with polycystic ovary syndrome. Gynecol. Endocrinol. 2020, 1–4. [Google Scholar] [CrossRef] [PubMed]
- Prasad, A.S.; Mantzoros, C.S.; Beck, F.W.; Hess, J.W.; Brewer, G.J. Zinc status and serum testosterone levels of healthy adults. Nutrition 1996, 12, 344–348. [Google Scholar] [CrossRef]
- Cruz, K.J.C.; Cruz, K.J.C.; Morais, J.B.S.; Beserra, J.B.; Severo, J.S.; De Oliveira, A.R.S. Zinc and Oxidative Stress: Current Mechanisms. Antioxidants 2017, 6, 24. [Google Scholar] [CrossRef]
- Ronaghy, H.A.; Halsted, J.A. Zinc deficiency occurring in females. Report of two cases. Am. J. Clin. Nutr. 1975, 28, 831–836. [Google Scholar] [CrossRef]
- Favier, A.E. The role of zinc in reproduction. Hormonal mechanism. Biol. Trace Elem. Res. 1992, 32, 363–382. [Google Scholar] [CrossRef]
- Soltan, M.H.; Jenkins, D.M. Plasma copper and zinc concentrations and infertility. Br. J. Obstet. Gynaecol. 1983, 90, 457–459. [Google Scholar] [CrossRef]
- Ng, S.; Karunanithy, R.; Edirisinghe, W.; Roy, A.; Wong, P.; Ratnam, S. Human Follicular Fluid Levels of Calcium, Copper and Zinc. Gynecol. Obstet. Investig. 1987, 23, 129–132. [Google Scholar] [CrossRef]
- Menezo, Y.; Khatchadourian, C.; Gharib, A.; Hamidi, J.; Greenland, T.; Sarda, N. Regulation of S-adenosyl methionine synthesis in the mouse embryo. Life Sci. 1989, 44, 1601–1609. [Google Scholar] [CrossRef]
- Kong, B.Y.; Bernhardt, M.L.; Kim, A.M.; O’Halloran, T.V.; Woodruff, T.K. Zinc Maintains Prophase I Arrest in Mouse Oocytes Through Regulation of the MOS-MAPK Pathway1. Biol. Reprod. 2012, 87, 11. [Google Scholar] [CrossRef] [PubMed]
- Kim, A.M.; Vogt, S.; O’Halloran, T.V.; Woodruff, T.K. Zinc availability regulates exit from meiosis in maturing mammalian oocytes. Nat. Chem. Biol. 2010, 6, 674–681. [Google Scholar] [CrossRef] [PubMed]
- Kim, A.M.; Bernhardt, M.L.; Kong, B.Y.; Ahn, R.W.; Vogt, S.; Woodruff, T.K.; O’Halloran, T.V. Zinc Sparks Are Triggered by Fertilization and Facilitate Cell Cycle Resumption in Mammalian Eggs. ACS Chem. Biol. 2011, 6, 716–723. [Google Scholar] [CrossRef]
- Lisle, R.S.; Anthony, K.; Randall, M.A.; Diaz, F.J. Oocyte–cumulus cell interactions regulate free intracellular zinc in mouse oocytes. Reproduction 2013, 145, 381–390. [Google Scholar] [CrossRef][Green Version]
- Menezo, Y.; Pluntz, L.; Chouteau, J.; Gurgan, T.; Demirol, A.; Dalleac, A.; Benkhalifa, M. Zinc concentrations in serum and follicular fluid during ovarian stimulation and expression of Zn2+ transporters in human oocytes and cumulus cell. Reprod. Biomed. 2011, 22, 647–652. [Google Scholar] [CrossRef]
- Escobar-Morreale, H.F. Polycystic ovary syndrome: Definition, aetiology, diagnosis and treatment. Nat. Rev. Endocrinol. 2018, 14, 270–284. [Google Scholar] [CrossRef]
- Álvarez-Blasco, F.; Carretero, J.B.; Millán, J.L.S.; Escobar-Morreale, H.F. Prevalence and Characteristics of the Polycystic Ovary Syndrome in Overweight and Obese Women. Arch. Intern. Med. 2006, 166, 2081–2086. [Google Scholar] [CrossRef]
- Legro, R.S.; Arslanian, S.A.; Ehrmann, D.A.; Hoeger, K.M.; Murad, M.H.; Pasquali, R.; Welt, C. Diagnosis and Treatment of Polycystic Ovary Syndrome: An Endocrine Society Clinical Practice Guideline. J. Clin. Endocrinol. Metab. 2013, 98, 4565–4592. [Google Scholar] [CrossRef]
- Kurdoglu, Z.; Kurdoglu, M.; Demir, H.; Sahin, H. Serum trace elements and heavy metals in polycystic ovary syndrome. Hum. Exp. Toxicol. 2011, 31, 452–456. [Google Scholar] [CrossRef]
- Chakraborty, P.; Ghosh, S.; Goswami, S.; Kabir, S.N.; Chakravarty, B.; Jana, K. Altered Trace Mineral Milieu Might Play An Aetiological Role in the Pathogenesis of Polycystic Ovary Syndrome. Biol. Trace Elem. Res. 2013, 152, 9–15. [Google Scholar] [CrossRef] [PubMed]
- Li, M.; Tang, Y.; Lin, C.; Huang, Q.; Lei, D.; Hu, Y. Serum Macroelement and Microelement Concentrations in Patients with Polycystic Ovary Syndrome: A Cross-Sectional Study. Biol. Trace Elem. Res. 2016, 176, 73–80. [Google Scholar] [CrossRef] [PubMed]
- Özer, A.; Bakacak, M.; Kiran, H.; Ercan, O.; Kostu, B.; Pektas, M.K.; Kilinç, M.; Aslan, F. Increased oxidative stress is associated with insulin resistance and infertility in polycystic ovary syndrome. Ginekol. Pol. 2016, 87, 733–738. [Google Scholar] [CrossRef] [PubMed]
- Kulhan, M.; Nayki, U.A.; Ata, N.; Ulug, P.; Mertoglu, C. Assessment of the relationship between serum vitamin (A, B12, C, D, folate) and zinc levels and polycystic ovary syndrome. Arch. Med. Sci. Civiliz. Dis. 2017, 2, 62–69. [Google Scholar] [CrossRef]
- Farhood, I.G. Assessment of serum zinc level in patients with polycystic ovary syndrome. Iraqui J. Med 2017, 15, 39–47. [Google Scholar] [CrossRef]
- Sharif, M.E.; Adam, I.; Ahmed, M.A.; Rayis, D.A.; Hamdan, H.Z. Serum Level of Zinc and Copper in Sudanese Women with Polycystic Ovarian Syndrome. Biol. Trace Elem. Res. 2017, 180, 23–27. [Google Scholar] [CrossRef]
- Pourteymour, F.; Alipoor, B.; Sadagiani, M.M.; Ostadrahimi, A. Effect of zinc supplementation on cardiometabolic risk factors in women with polycystic ovary syndrome. J. Cardiovasc. Thorac. Res. 2010, 2, 11–20. [Google Scholar]
- Foroozanfard, F.; Jamilian, M.; Jafari, Z.; Khassaf, A.; Hosseini, A.; Khorammian, H.; Asemi, Z. Effects of Zinc Supplementation on Markers of Insulin Resistance and Lipid Profiles in Women with Polycystic Ovary Syndrome: A Randomized, Double-blind, Placebo-controlled Trial. Exp. Clin. Endocrinol. Diabetes 2015, 123, 215–220. [Google Scholar] [CrossRef]
- Jamilian, M.; Foroozanfard, F.; Bahmani, F.; Talaee, R.; Monavari, M.; Asemi, Z. Effects of Zinc Supplementation on Endocrine Outcomes in Women with Polycystic Ovary Syndrome: A Randomized, Double-Blind, Placebo-Controlled Trial. Biol. Trace Elem. Res. 2015, 170, 271–278. [Google Scholar] [CrossRef]
- Ebrahimi, F.A.; Foroozanfard, F.; Aghadavod, E.; Bahmani, F.; Asemi, Z. The Effects of Magnesium and Zinc Co-Supplementation on Biomarkers of Inflammation and Oxidative Stress, and Gene Expression Related to Inflammation in Polycystic Ovary Syndrome: A Randomized Controlled Clinical Trial. Biol. Trace Elem. Res. 2017, 184, 300–307. [Google Scholar] [CrossRef]
- Maktabi, M.; Jamilian, M.; Asemi, Z. Magnesium-Zinc-Calcium-Vitamin D Co-supplementation Improves Hormonal Profiles, Biomarkers of Inflammation and Oxidative Stress in Women with Polycystic Ovary Syndrome: A Randomized, Double-Blind, Placebo-Controlled Trial. Biol. Trace Elem. Res. 2017, 182, 21–28. [Google Scholar] [CrossRef] [PubMed]
- Marshall, J.C.; Dunaif, A. Should all women with PCOS be treated for insulin resistance? Fertil. Steril. 2012, 97, 18–22. [Google Scholar] [CrossRef] [PubMed]
- Dokras, A.; Bochner, M.; Hollinrake, E.; Markham, S.; VanVoorhis, B.; Jagasia, D.H. Screening Women With Polycystic Ovary Syndrome for Metabolic Syndrome. Obstet. Gynecol. 2005, 106, 131–137. [Google Scholar] [CrossRef] [PubMed]
- Wild, S.; Pierpoint, T.; McKeigue, P.; Jacobs, H. Cardiovascular disease in women with polycystic ovary syndrome at long-term follow-up: A retrospective cohort study. Clin. Endocrinol. 2000, 52, 595–600. [Google Scholar] [CrossRef]
- Cassar, S.; Teede, H.J.; Harrison, C.L.; Joham, A.E.; Moran, L.; Stepto, N.K. Biomarkers and insulin sensitivity in women with Polycystic Ovary Syndrome: Characteristics and predictive capacity. Clin. Endocrinol. 2014, 83, 50–58. [Google Scholar] [CrossRef]
- Beletate, V.; El Dib, R.; Atallah, Á.N. Zinc supplementation for the prevention of type 2 diabetes mellitus. Cochrane Database Syst. Rev. 2007, 1, CD005525. [Google Scholar] [CrossRef]
- Dunaif, A.; Xia, J.; Book, C.B.; Schenker, E.; Tang, Z. Excessive insulin receptor serine phosphorylation in cultured fibroblasts and in skeletal muscle. A potential mechanism for insulin resistance in the polycystic ovary syndrome. J. Clin. Invest. 1995, 96, 801–810. [Google Scholar] [CrossRef]
- Nestler, J.E. Role of hyperinsulinemia in the pathogenesis of the polycystic ovary syndrome and its clinical implications. Semin. Reprod. Endocrinol. 1997, 15, 111–122. [Google Scholar] [CrossRef]
- Baillargeon, J.-P.; Iuorno, M.J.; Nestler, J.E. Insulin Sensitizers for Polycystic Ovary Syndrome. Clin. Obstet. Gynecol. 2003, 46, 325–340. [Google Scholar] [CrossRef]
- De Leo, V.; La Marca, A.; Petraglia, F. Insulin-Lowering Agents in the Management of Polycystic Ovary Syndrome. Endocr. Rev. 2003, 24, 633–667. [Google Scholar] [CrossRef]
- Guler, I.; Himmetoglu, O.; Turp, A.; Erdem, A.; Erdem, M.; Onan, M.A.; Taskiran, C.; Taslipinar, M.Y.; Guner, H. Zinc and Homocysteine Levels in Polycystic Ovarian Syndrome Patients with Insulin Resistance. Biol. Trace Elem. Res. 2014, 158, 297–304. [Google Scholar] [CrossRef] [PubMed]
- Fassnacht, M.; Schlenz, N.; Schneider, S.B.; Wudy, S.A.; Allolio, B.; Arlt, W. Beyond Adrenal and Ovarian Androgen Generation: Increased Peripheral 5α-Reductase Activity in Women with Polycystic Ovary Syndrome. J. Clin. Endocrinol. Metab. 2003, 88, 2760–2766. [Google Scholar] [CrossRef] [PubMed]
- Vassiliadi, D.A.; Barber, T.M.; Hughes, B.A.; McCarthy, M.M.; Wass, J.A.H.; Franks, S.; Nightingale, P.; Tomlinson, J.W.; Arlt, W.; Stewart, P.M. Increased 5α-Reductase Activity and Adrenocortical Drive in Women with Polycystic Ovary Syndrome. J. Clin. Endocrinol. Metab. 2009, 94, 3558–3566. [Google Scholar] [CrossRef] [PubMed]
- Leake, A.; Chisholm, G.D.; Habib, F.K. The effect of zinc on the 5α-reduction of testosterone by the hyperplastic human prostate gland. J. Steroid Biochem. 1984, 20, 651–655. [Google Scholar] [CrossRef]
- Kambe, T.; Yamaguchi-Iwai, Y.; Sasaki, R.; Nagao, M. Overview of mammalian zinc transporters. Cell. Mol. Life Sci. 2004, 61, 49–68. [Google Scholar] [CrossRef]
- Walsh, S.W. Prostaglandins in Pregnancy. Glob. Libr. Women’s Med. 2009. [Google Scholar] [CrossRef]
- Amini, L.; Tehranian, N.; Movahedin, M.; Tehrani, F.R.; Ziaee, S. Antioxidants and management of polycystic ovary syndrome in Iran: A systematic review of clinical trials. Iran. J. Reprod. Med. 2015, 13, 1–8. [Google Scholar]
- González, F.; Rote, N.S.; Minium, J.; Kirwan, J. Reactive Oxygen Species-Induced Oxidative Stress in the Development of Insulin Resistance and Hyperandrogenism in Polycystic Ovary Syndrome. J. Clin. Endocrinol. Metab. 2006, 91, 336–340. [Google Scholar] [CrossRef]
- Latthe, P.; Latthe, M.; Say, L.; Gülmezoglu, A.M.; Khan, K.S. WHO systematic review of prevalence of chronic pelvic pain: A neglected reproductive health morbidity. BMC Public Health 2006, 6, 177. [Google Scholar] [CrossRef]
- Proctor, M.; Farquhar, C. Diagnosis and management of dysmenorrhoea. Br. Med. J. 2006, 332, 1134–1138. [Google Scholar] [CrossRef]
- French, L. Dysmenorrhea in adolescents: Diagnosis and treatment. Pediatr. Drugs 2008, 10, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Sharma, P.; Malhotra, C.; Taneja, D.K.; Saha, R. Problems related to menstruation amongst adolescent girls. Indian J. Pediatr. 2008, 75, 125–129. [Google Scholar] [CrossRef] [PubMed]
- Barcikowska, Z.; Rajkowska-Labon, E.; Grzybowska, M.E.; Hansdorfer-Korzon, R.; Zorena, K. Inflammatory Markers in Dysmenorrhea and Therapeutic Options. Int. J. Environ. Res. Public Health 2020, 17, 1191. [Google Scholar] [CrossRef] [PubMed]
- Harel, Z. Dysmenorrhea in Adolescents and Young Adults: Etiology and Management. J. Pediatr. Adolesc. Gynecol. 2006, 19, 363–371. [Google Scholar] [CrossRef]
- French, L. Dysmenorrhea. Am. Fam. Phys. 2005, 71, 285–291. [Google Scholar]
- Kelly, R.W.; Abel, M.H. Copper and Zinc Inhibit the Metabolism of Prostaglandin by the Human Uterus. Biol. Reprod. 1983, 28, 883–889. [Google Scholar] [CrossRef]
- Fong, L.Y.; Zhang, L.; Jiang, Y.; Farber, J.L. Dietary Zinc Modulation of COX-2 Expression and Lingual and Esophageal Carcinogenesis in Rats. J. Natl. Cancer Inst. 2005, 97, 40–50. [Google Scholar] [CrossRef]
- Wu, W.; Silbajoris, R.A.; Cao, N.; Bromberg, P.A.; Zhang, Q.; Peden, D.; Samet, J.M. Regulation of cyclooxygenase-2 expression by cAMP response element and mRNA stability in a human airway epithelial cell line exposed to zinc. Toxicol. Appl. Pharmacol. 2008, 231, 260–266. [Google Scholar] [CrossRef]
- Chuong, C.J.; Dawson, E.B. Zinc and copper levels in premenstrual syndrome. Fertil. Steril. 1994, 62, 313–320. [Google Scholar] [CrossRef]
- Prasad, A.S. Clinical, immunological, anti-inflammatory and antioxidant roles of zinc. Exp. Gerontol. 2008, 43, 370–377. [Google Scholar] [CrossRef]
- Hara, T.; Takeda, T.-A.; Takagishi, T.; Fukue, K.; Kambe, T.; Fukada, T. Physiological roles of zinc transporters: Molecular and genetic importance in zinc homeostasis. J. Physiol. Sci. 2017, 67, 283–301. [Google Scholar] [CrossRef] [PubMed]
- Eby, G.A. Zinc treatment prevents dysmenorrhea. Med. Hypoth. 2007, 69, 297–301. [Google Scholar] [CrossRef] [PubMed]
- Kashefi, F.; Khajehei, M.; Tabatabaeichehr, M.; Alavinia, S.M.; Asili, J. Comparison of the Effect of Ginger and Zinc Sulfate on Primary Dysmenorrhea: A Placebo-Controlled Randomized Trial. Pain Manag. Nurs. 2014, 15, 826–833. [Google Scholar] [CrossRef] [PubMed]
- Zekavat, O.R.; Karimi, M.Y.; Amanat, A.; Alipour, F. A randomised controlled trial of oral zinc sulphate for primary dysmenorrhoea in adolescent females. Aust. N. Z. J. Obstet. Gynaecol. 2015, 55, 369–373. [Google Scholar] [CrossRef]
- Sangestani, G.; Khatiban, M.; Marci, R.; Piva, I. The positive effects of zinc supplements on the improvement of primary dysmenorrhea and premenstrual symptoms: A double-blind, randomized, controlled trial. J. Midwifery Reprod. Health 2015, 3, 378–384. [Google Scholar] [CrossRef]
- Teimoori, B.; Ghasemi, M.; Hoseini, Z.S.A.; Razavi, M. The Efficacy of Zinc Administration in the Treatment of Primary Dysmenorrhea. Oman Med. J. 2016, 31, 107–111. [Google Scholar] [CrossRef]
- Farrah, A.M.; Halim, B.; Kaban, Y. Effectiveness of Zinc Supplementation in Treating Dysmenorrhea. Bali Med. J. 2017, 6, 34. [Google Scholar] [CrossRef]
- Giudice, L.C. Clinical practice. Endometriosis. N. Engl. J. Med. 2010, 362, 2389–2398. [Google Scholar] [CrossRef]
- Eskenazi, B.; Warner, M.L. Epidemiology of endometriosis. Obstet. Gynecol. Clin. N. Am. 1997, 24, 235–258. [Google Scholar] [CrossRef]
- D’Hooghe, T.M.; Hummelshoj, L. Multi-disciplinary centres/networks of excellence for endometriosis management and research: A proposal. Hum. Reprod. 2006, 21, 2743–2748. [Google Scholar] [CrossRef]
- Giudice, L.C.; Kao, L.C. Endometriosis. Lancet 2004, 364, 1789–1799. [Google Scholar] [CrossRef]
- Burney, R.O.; Giudice, L.C. Pathogenesis and pathophysiology of endometriosis. Fertil. Steril. 2012, 98, 511–519. [Google Scholar] [CrossRef] [PubMed]
- Singh, A.K.; Chattopadhyay, R.; Chakravarty, B.; Chaudhury, K. Altered circulating levels of matrix metalloproteinases 2 and 9 and their inhibitors and effect of progesterone supplementation in women with endometriosis undergoing in vitro fertilization. Fertil. Steril. 2013, 100, 127–134. [Google Scholar] [CrossRef] [PubMed]
- Messalli, E.M.; Schettino, M.T.; Mainini, G.; Ercolano, S.; Fuschillo, G.; Falcone, F.; Esposito, E.; Di Donna, M.C.; De Franciscis, P.; Torella, M. The possible role of zinc in the etiopathogenesis of endometriosis. Clin. Exp. Obstet. Gynecol. 2014, 41, 541–546. [Google Scholar]
- Lai, G.-L.; Yeh, C.-C.; Yeh, C.-Y.; Chen, R.-Y.; Fu, C.-L.; Chen, C.-H.; Tzeng, C.-R. Decreased zinc and increased lead blood levels are associated with endometriosis in Asian Women. Reprod. Toxicol. 2017, 74, 77–84. [Google Scholar] [CrossRef]
- Yılmaz, B.K.; Evliyaoğlu, Ö.; Yorganci, A.; Özyer, Ş.; Ustun, Y.E. Serum concentrations of heavy metals in women with endometrial polyps. J. Obstet. Gynaecol. 2019, 40, 541–545. [Google Scholar] [CrossRef]
- Wölfler, M.M.; Meinhold-Heerlein, I.M.; Henkel, C.; Rath, W.; Neulen, J.; Maass, N.; Bräutigam, K. Reduced hemopexin levels in peritoneal fluid of patients with endometriosis. Fertil. Steril. 2013, 100, 777–781. [Google Scholar] [CrossRef]
- Verit, F.F.; Erel, O.; Celik, N. Serum paraoxonase-1 activity in women with endometriosis and its relationship with the stage of the disease. Hum. Reprod. 2007, 23, 100–104. [Google Scholar] [CrossRef]
- Prieto, L.; Quesada, J.F.; Cambero, O.; Pacheco, A.; Pellicer, A.; Codoceo, R.; Garcia-Velasco, J.A. Analysis of follicular fluid and serum markers of oxidative stress in women with infertility related to endometriosis. Fertil. Steril. 2012, 98, 126–130. [Google Scholar] [CrossRef]
- Huang, H.; Hong, L.-H.; Tan, Y.; Sheng, J.-Z. Matrix metalloproteinase 2 is associated with changes in steroid hormones in the sera and peritoneal fluid of patients with endometriosis. Fertil. Steril. 2004, 81, 1235–1239. [Google Scholar] [CrossRef]
- Malvezzi, H.; Aguiar, V.G.; De Paz, C.C.P.; Tanus-Santos, J.E.; Penna, I.A.D.A.; Navarro, P.A. Increased Circulating MMP-2 Levels in Infertile Patients With Moderate and Severe Pelvic Endometriosis. Reprod. Sci. 2012, 20, 557–562. [Google Scholar] [CrossRef] [PubMed]
- de Sanctis, P.; Elmakky, A.; Farina, A.; Caramelli, E.; Seracchioli, R.; Mabrouk, M.; Mignemi, G.; Venturoli, S.; Villa, G.; Guerrini, M.; et al. Matrix metalloproteinase-3 mRNA: A promising peripheral blood marker for diagnosis of endometriosis. Gynecol. Obstet. Investig. 2011, 71, 118–123. [Google Scholar] [CrossRef] [PubMed]
- Mier-Cabrera, J.; Aburto, T.C.; Burrola-Méndez, S.; Jimenez, L.; Tolentino, M.C.; Casanueva, E.; Hernández-Guerrero, C. Women with endometriosis improved their peripheral antioxidant markers after the application of a high antioxidant diet. Reprod. Biol. Endocrinol. 2009, 7, 54. [Google Scholar] [CrossRef] [PubMed]
- Pollack, A.Z.; Louis, G.M.B.; Chen, Z.; Peterson, C.M.; Sundaram, R.; Croughan, M.S.; Sun, L.; Hediger, M.L.; Stanford, J.B.; Varner, M.W.; et al. Trace elements and endometriosis: The ENDO study. Reprod. Toxicol. 2013, 42, 41–48. [Google Scholar] [CrossRef]
- Singh, A.K.; Chattopadhyay, R.; Chakravarty, B.; Chaudhury, K. Markers of oxidative stress in follicular fluid of women with endometriosis and tubal infertility undergoing IVF. Reprod. Toxicol. 2013, 42, 116–124. [Google Scholar] [CrossRef]
- Oberweis, D.; Madelenat, P.; Nisolle, M.; Demanet, E. A pilot double-blind, randomized, placebo-controlled trial of the efficacy of trace elements in the treatment of endometriosis-related pain: Study design and methodology. Nutr. Diet. Suppl. 2016, 8, 1. [Google Scholar] [CrossRef]
- Takacs, P.; Kozma, B.; Erdodi, B.; Jakab, A.; Larson, K.; Poka, R. Zinc-containing Vaginal Moisturizer Gel Improves Postmenopausal Vulvovaginal Symptoms: A Pilot Study. J. Menopausal Med. 2019, 25, 63–68. [Google Scholar] [CrossRef]
- Takacs, P.; Damjanovich, P.; Sipos, A.G.; Kozma, B.; Gergely, A. The effect of oral zinc supplementation on cervicovaginal lavage fluid zinc level. Eur. J. Obstet. Gynecol. Reprod. Boil. 2020, 248, 106–109. [Google Scholar] [CrossRef]
- Yanagisawa, H. Zinc Deficiency and Clinical Practice—Validity of Zinc Preparations. Yakugaku Zasshi 2008, 128, 333–339. [Google Scholar] [CrossRef]
- Bednarek-Tupikowska, G.; Jodkowska, A.; Antonowicz-Juchniewicz, J. Zinc, cooper, manganese, and selenium status in pre-and postmenopausal women during sex hormone therapy. Adv. Clin. Exp. Med. 2010, 19, 337–345. [Google Scholar]
- Sunar, F.; Gormus, Z.I.; Baltaci, A.K.; Mogulkoc, R. The Effect of Low Dose Zinc Supplementation to Serum Estrogen and Progesterone Levels in Post-menopausal Women. Biol. Trace Elem. Res. 2008, 126, 11–14. [Google Scholar] [CrossRef] [PubMed]
| WHO/FAO | IOM | EFSA | |||||
|---|---|---|---|---|---|---|---|
| Age, Sex | RNI (mg/Day) | Age, Sex | RDA (mg/Day) | Age, Sex | PRI (mg/Day) | ||
| Higha | Moderateb | Lowc | |||||
| 0–6 months | 1.1d | 2.8e | 6.6f | 0–6 months | 2 (AI) | ||
| 7–12 months | 0.8d; 2.5g | 4.1 | 8.4 | 7–12 months | 3 | 7–11 months | 2.9 |
| 1–3 years | 2.4 | 4.1 | 8.3 | 1–3 years | 3 | 1–3 years | 4.3 |
| 4–6 years | 2.9 | 4.8 | 9.6 | 4–8 years | 5 | 4–6 years | 5.5 |
| 7–9 years | 3.3 | 5.6 | 11.2 | 9–13 years | 8 | 7–10 years | 7.4 |
| 11–14 years | 9.4 | ||||||
| 10–18 years | 14–18 years | 15–17 years | |||||
| Males | 5.1 | 8.6 | 17.1 | Males | 11 | Males | 12.5 |
| Females | 4.3 | 7.2 | 14.4 | Females | 9 | Females | 10.4 |
| ≥19 years | ≥19 years | ≥18 years | |||||
| Males | 4.2 | 7.0 | 14.0 | Males | 11 | Males | |
| 300h | 9.4 | ||||||
| 600h | 11.7 | ||||||
| 900h | 14.0 | ||||||
| 1200h | 16.3 | ||||||
| Females | 3.0 | 4.9 | 9.8 | Females | 8 | Females | |
| 300h | 7.5 | ||||||
| 600h | 9.3 | ||||||
| 900h | 11.0 | ||||||
| 1200h | 12.7 | ||||||
| Pregnancy | Pregnancy | Pregnancy | +1.6 | ||||
| 1st trimester | 3.4 | 5.5 | 11.0 | ||||
| 2nd trimester | 4.2 | 7.0 | 14.0 | 14–18 years | 12 | ||
| 3rd trimester | 6.0 | 10.0 | 20.0 | 19–50 years | 11 | ||
| Lactation | Lactation | Lactation | +2.6 | ||||
| 0–3 months | 5.8 | 9.5 | 19.0 | ||||
| 3–6 months | 5.3 | 8.8 | 17.5 | 14–18 years | 13 | ||
| 6–12 months | 4.3 | 7.2 | 14.4 | 19–50 years | 12 | ||
| Age (Years) | BMI (kg/m2) | Zinc (µg/dL) | Additional Information | Ref. | |||||
|---|---|---|---|---|---|---|---|---|---|
| Control | PCOS | Control | PCOS | Control | PCOS | Parameters | Control | PCOS | |
| 27.75 ± 5.45 (n = 30) | 24.25 ± 4.68 (n = 35) | 22.63 ± 3.08 | 21.72 ± 3.02 | 77 ± 19 | 92 ± 20b | T (ng/dL) DHEAS (µg/dL) | 45.8 ± 13.4 180.85 ± 80.45 | 83.24 ± 37.04c 307.81 ± 132.77c | [45] |
| 28.33 ± 0.87 (n = 46) | 28.93 ± 0.36 (n = 132) | 23.02 ± 0.17 | 23.57 ± 0.49 | 56 ± 6.7 | 60 ± 34.4 | LH (mIU/mL) | 7.39 ± 0.41 | 5.91 ± 0.39a | [46] |
| T (ng/dL) | 47 ± 24 | 149 ± 18c | |||||||
| fasting insulin (µIU/mL) | 8.12 ± 0.66 | 12.38 ± 0.83b | |||||||
| HOMA2-IR | 1.27 ± 0.37 | 2.21 ± 0.25c | |||||||
| manganese (µg/dL) | 13 ± 1.1 | 23 ± 2.2b | |||||||
| calcium (µg/dL) | 210 ± 11 | 300 ± 42a | |||||||
| 28.0 ± 5.9 (n = 33) | 25.4 ± 6.7 (n = 53) | 23.5 ± 4.9 | 27.4 ± 6.8a | 78.1 ± 14.7 | 66.3 ± 13.2c | HDL-C (mg/dL) | 52.4 ± 11.3 | 45.6 ± 8.9b | [47] |
| TG (mg/dL) | 79.3 ± 39.3 | 109.9 ± 60a | |||||||
| TG/HDL ratio | 1.6 ± 1 | 2.5 ± 1.7a | |||||||
| Hcy (µmol/L) | 10.5 ± 2.8 | 8.9 ± 2.3a | |||||||
| 29 (26–31) (n = 105) | 27.0 (25–30) (n = 96) | 20.45 (18.98–22.50) | 22.07 (19.72–25.03)c | 87.74 (79.21–96.63) | 82.37 (76.96–89.45)b | LH (mIU/mL) | 4.38 (3.14–5.61) | 9.80 (5.36–15.14)c | [27] |
| LH/FSH | 0.64 (0.46–0.81) | 1.51 (0.90–2.17)c | |||||||
| tT (ng/dL) | 33.98 (25.92–44.93) | 55.01 (44.06–69.98)c | |||||||
| DHEAS (µg/dL) | 270.94 (228.21–320.37) | 311.03 (269.96–348.59)c | |||||||
| SHGB (nmol/L) | 37.20 (28.90–57.81) | 16.74 (9.55–48.03)c | |||||||
| fasting insulin (µIU/mL) | 6.90 (5–8.60) | 10.35 (6.43–13.50)c | |||||||
| fasting glucose (mg/dL) | 83.52 (77.94–88.92) | 86.49 (80.82–92.12)a | |||||||
| GIR | 12.04 (9.42–15.65) | 8.61 (6.62–13.33)c | |||||||
| HOMA-IR | 1.44 (1–1.84) | 2.22 (1.35–2.97)c | |||||||
| QUICKI | 0.36 (0.35–0.38) | 0.34 (0.32–0.37)c | |||||||
| TG (mg/dL) | 7.54 (5–9.91) | 9.91 (7.1–14.74)c | |||||||
| HDL-C (mg/dL) | 56.5 (47.7–66.9) | 53.5 (45.4–60.8)a | |||||||
| 29.4 ± 8.8 (n = 53) | 26.2 ± 5.5 (n = 71) | 23.8 ± 4.7 | 26.9 ± 5.4 | 99.4 ± 19.9 | 84.4 ± 25.5a | glucose (mg/dL) | 78.5 ± 7.1 | 90.2 ± 6.1b | [48] |
| insulin (µIU/mL) | 9.7 ± 6.4 | 13.18 ± 8.9a | |||||||
| HOMA-IR | 1.88 ± 1.68 | 2.92 ± 2.15a | |||||||
| LH (mIU/mL) | 4.48 ± 2.03 | 7.95 ± 5.06c | |||||||
| tT (ng/dL) | 89 ± 34 | 155 ± 91c | |||||||
| freeT (ng/dL) | 146 ± 22 | 231 ± 54c | |||||||
| MDA (nmol/mL) | 3.1 ± 2.7 | 23.0 ± 13.8c | |||||||
| catalase (µg/mL) | 2302 ± 437.3 | 1875.7 ± 435.1a | |||||||
| GPx (µg/mL) | 3.2 ± 0.5 | 3.6 ± 0.4a | |||||||
| 33(30–37) (n = 559) | 30.0(28–33) (n = 578)c | 21.12 (19.72–23.34) | 22.01 (19.97–24.44)c | 646.23 (541.25–754.97) | 659.42 (560.82–771.16) | FSH (mIU/mL) | 7.90 (6.67–9.18) | 6.90 (6.01–8.16)c | [47] |
| LH (mIU/mL) | 3.68 (2.82–4.86) | 5.59 (3.91–9.84)c | |||||||
| copper (µg/dL) | 114.22 (98.34–138.79) | 126.19 (106.91–152.27)c | |||||||
| calcium (mg/dL) | 6.44 (5.76–7.04) | 6.2 (5.64–6.84)c | |||||||
| 25.34 ± 5.82 (n = 67) | 24.06 ± 6.12 (n = 65) | 25.27 ± 2.68 | 26.0 ± 4.52 | 89.22 ± 9.83 | 95.45 ± 10.94 | hirsutism score | 1.28 ± 1.73 | 8.32 ± 3.67a | [49] |
| insulin (µIU/mL) | 6.48 ± 2.34 | 10.71 ± 5.47a | |||||||
| HOMA-IR | 1.92 ± 0.58 | 2.37 ± 0.77a | |||||||
| 25.18 ± 3.1 (n = 40) | 25.48 ± 3.56 (n = 40) | 28.28 ± 8.33 | 28.34 ± 7.17 | 83.8 ± 10.11 | 75.31 ± 33.91 | prolactin (IU/mL) | 9.19 ± 2.2 | 15.07 ± 8.42c | [50] |
| LH (IU/mL) | 4.57 ± 1.8 | 6.48 ± 4.36a | |||||||
| 27.1 ± 4.8 (n = 50) | 26.9 ± 5.2 (n = 50) | 25.6 ± 5.7 | 28.4 ± 4.2b | 138 (98.2–192) | 123 (103.5–180.7) | Cu/Zn | 1.5 (0.9–1.8) | 1.1 (0.8–1.4)a | [51] |
| 29.17 ± 5.03 (n = 90) | 28.68 ± 5.08 (n = 60) | 27.92 ± 4.70 | 29.14 ± 5.57 | 108.31 ± 63.29 | 81.33 ± 24.28a | insulin (µIU/mL) | 11.80 ± 5.12 | 15.67 ± 7.88b | [18] |
| HOMA-IR | 2.46 ± 1.15 | 3.44 ± 2.11b | |||||||
| QUICKI | 0.339 ± 0.02 | 0.326 ± 0.03b | |||||||
| GIR | 8.63 ± 4.36 | 7.05 ± 4.77b | |||||||
| 15.21 ± 1.42 (n = 51) | 15.67 ± 1.58 (n = 34) | 23.0 ± 3.23 | 25.79 ± 4.80 | 101.72 ± 16.71 | 102.27 ± 10.41 | “idiopathic hirsutism" group | [28] | ||
| T (ng/dL) | 30.57 ± 10.61 | 54.71 ± 26.54a | |||||||
| DHEAS (µg/dL) | 273.43 ± 61.07 | 283.21 ± 142.87c | |||||||
| BMI < 25 | [29] | ||||||||
| 24 (18–39) (n = 55) | 20.94 (16.16–24.89) | 85.77 (58.97–107.57) | copper (µg/dL) | 80.21 (38.63–139.50) | |||||
| Cu/Zn | 0.96 (0.62–1.50) | ||||||||
| glucose (mg/dl) | 87 (75–98) | ||||||||
| glucose 120′ (mg/dL) | 92 (31–141) | ||||||||
| insulin (µIU/mL) | 4.71 (1.72–13.11) | ||||||||
| insulin 120′(µIU/mL) | 24.47 (8.36–90.46) | ||||||||
| HOMA-IR | 1.05 (0.36–2.88) | ||||||||
| SIRT1 (ng/mL) | 1.18 (0.81–30.87) | ||||||||
| BMI ≥ 25 | |||||||||
| 23 (17–38) (n = 21) | 31.14 (25.10–41.52) | 81.82 (59.60–109.99) | copper (µg/dL) | 94.82 (61.99–118.87) | |||||
| Cu/Zn | 1.06 (0.73–1.67) | ||||||||
| glucose (mg/dl) | 88 (79–116) | ||||||||
| glucose 120′ (mg/dL) | 113 (75–185) | ||||||||
| insulin (µIU/mL) | 10.32 (2.73–34.67) | ||||||||
| insulin 120′ (µIU/mL) | 52.2 (18.21–151.14) | ||||||||
| HOMA-IR | 2.17 (0.61–9.93) | ||||||||
| SIRT1 (ng/mL) | 1.09 (0.88–3.59) | ||||||||
| Type of Supplementation | Inclusion Criteria | Parameters | Placebo | Zinc Supplementation | Ref. | ||||
|---|---|---|---|---|---|---|---|---|---|
| Baseline | End of Trial | Change | Baseline | End of Trial | Change | ||||
| 220 mg of zinc sulfate (50 mg Zn) 8 weeks; | PCOS women 20–45 years Placebo group (n = 30) Zinc group (n = 35) | zinc (µg/dL) | 78.25 ± 0.87 | 79.30 ± 0.85 | 1.05 ± 0.70 | 76.11 ± 1.06 | 108.18 ± 1.77c | 32.06 ± 1.76c | [52] |
| insulin (µU/mL) | 17.93 ± 1.64 | 17.97 ± 1.56 | 0.04 ± 0.23 | 18.73 ± 1.41 | 16.19 ± 1.32c | −2.54 ± 0.40c | |||
| HOMA-IR | 4.16 ± 0.37 | 4.16 ± 0.36 | −0.003 ± 0.05 | 4.34 ± 0.31 | 3.71 ± 0.29c | −0.62 ± 0.09c | |||
| TC (mg/dL) | 196.0 ± 1.5 | 196.6 ± 1.5 | 0.66 ± 0.44 | 196.3 ± 1.7 | 194.8 ± 1.5b | −3.73 ± 1.81b | |||
| LDL-C (mg/dL) | 133.2 ± 4.5 | 134.04 ± 4.4a | 1.06 ± 0.48 | 132.77 ± 4.0 | 130.71 ± 3.7c | −5.84 ± 4.41 | |||
| TG (mg/dL) | 180.5 ± 9.3 | 180.4 ± 9.4 | −0.33 ± 0.44 | 182.9 ± 9.2 | 178.1 ± 8.5c | −11.46 ± 3.37b | |||
| T (ng/dL) | 90 ± 6 | 89 ± 6 | −1 ± 2 | 95 ± 6 | 88 ± 7a | −7 ± 3 | |||
| DHEAS (µg/dL) | 150 ± 14 | 147 ± 14 | −3 ± 1 | 156 ± 15 | 154 ± 14 | −19 ± 5b | |||
| 220 mg of zinc sulfate (50 mg Zn) 8 weeks; | PCOS women 18–40 years Placebo group (n = 26) Zinc group (n = 26) | zinc (mg/dL) | 101.0 ± 14.8 | 96.9 ± 10.9 | −4.1 ± 16.7 | 113.4 ± 21.3 | 129.0 ± 30.1a | 15.6 ± 21.8c | [53] |
| FPG (mg/dL) | 92.5 ± 7.1 | 93.0 ± 7.5 | 0.5 ± 6.0 | 99.8 ± 10.3 | 95.5 ± 8.0a | −4.3 ± 9.6a | |||
| insulin (µIU/mL) | 10.0 ± 8.3 | 11.5 ± 8.8 | 1.5 ± 8.4 | 10.4 ± 3.7 | 7.4 ± 2.0a | −3.0 ± 2.9b | |||
| HOMA-IR | 2.3 ± 1.9 | 2.6 ± 2.1 | 0.3 ± 1.9 | 2.6 ± 1.2 | 1.8 ± 0.8a | −0.8 ± 0.8b | |||
| HOMA-B | 36.4 ± 33.4 | 41.3 ± 33.4 | 4.9 ± 32.1 | 33.7 ± 11.4 | 23.1 ± 7.4a | −10.6 ± 9.5a | |||
| QUICKI | 0.35 ± 0.03 | 0.35 ± 0.04 | −0.004 ± 0.05 | 0.33 ± 0.02 | 0.35 ± 0.02a | 0.02 ± 0.02a | |||
| TG (mg/dL) | 108.7 ± 50.2 | 123.2 ± 61.3a | 14.5 ± 25.3 | 126.8 ± 56.2 | 111.2 ± 57.8 | −15.6 ± 40.3b | |||
| VLDL-C (mg/dL) | 21.7 ± 10.0 | 24.6 ± 12.3a | 2.9 ± 5.1 | 25.4 ± 11.2 | 22.2 ± 11.6 | −3.2 ± 8.1b | |||
| 220 mg of zinc sulfate (50 mg Zn) 8 weeks | PCOS women 18–40 years Placebo group (n = 24) Zinc group (n = 24) | zinc (mg/dL) | 102.66 ± 13.71 | 99.32 ± 10.31 | −3.34 ± 15.83 | 111.89 ± 20.9 | 128.87 ± 30.91 | 16.98 ± 22.3c | [54] |
| FSH (IU/L) | 7.16 ± 1.82 | 8.05 ± 1.84 | 0.89 ± 2.28 | 12.94 ± 8.52 | 11.87 ± 7.44 | −1.07 ± 5.16b | |||
| freeT (ng/dL) | 0.351 ± 0.186 | 0.341 ± 0.193 | −0.010 ± 0.096 | 0.265 ± 0.115 | 0.251 ± 0.109 | −0.014 ± 0.062a | |||
| 17-OHP (ng/mL) | 2.10 ± 1.23 | 1.92 ± 1.35 | −0.18 ± 1.78 | 1.13 ± 0.99 | 1.0 ± 0.61 | −0.13 ± 1.20c | |||
| TAC (nmol/L) | 718.2 ± 138.32 | 666.85 ± 135.7 | −51.35 ± 182.81 | 801.74 ± 210.59 | 781.66 ± 142.26 | −20.08 ± 156.82b | |||
| MDA (nmol/mL) | 4.96 ± 2.97 | 7.30 ± 4.37a | 2.34 ± 5.53 | 4.37 ± 1.04 | 4.28 ± 0.65 | −0.09 ± 1.31c | |||
| 250 mg of magnesium oxide + 220 mg of zinc sulfate (50 mg Zn) 12 weeks; twice a day | PCOS women 18–40 years Placebo group (n = 30) Zinc group (n = 30) | magnesium (mg/dL) | 1.81 ± 0.32 | 1.76 ± 0.31 | −0.05 ± 0.17 | 1.84 ± 0.29 | 2.05 ± 0.31 | 0.21 ± 0.24c | [55] |
| zinc (mg/dL) | 84.9 ± 11.6 | 84.3 ± 11.1 | −0.6 ± 3.9 | 80.4 ± 12.4 | 86.3 ± 13.4 | 6.6 ± 5.0c | |||
| hs-CRP (mg/L) | 5.1 ± 1.9 | 5.2 ± 1.9 | 0.1 ± 0.7 | 4.4 ± 2.6 | 2.8 ± 1.4 | −1.6 ± 2.4c | |||
| TAC (nmol/L) | 795 ± 132.5 | 793.5 ± 172.8 | −1.5 ± 141.5 | 712.7 ± 64 | 785.4 ± 73.1 | 60.7 ± 69.4c | |||
| PCO (nmol/mg protein) | 2.67 ± 0.64 | 2.70 ± 35 | 0.02 ± 0.07 | 2.59 ± 0.39 | 2.45 ± 0.41 | −0.14 ± 0.28b | |||
| 100 mg of Mg + 4 mg of Zn + 400 mg of Ca + 200 IU of Vit. D; 12 weeks; twice a day | PCOS women 18–40 years Placebo group (n = 30) Zinc group (n = 30) | magnesium (mg/dL) | 1.6 ± 0.3 | 1.5 ± 0.2 | −0.1 ± 0.3 | 1.5 ± 0.2 | 1.6 ± 0.2 | 0.1 ± 0.1b | [56] |
| zinc (mg/dL) | 101.0 ± 14.9 | 100.1 ± 13.6 | −0.9 ± 7.6 | 106.1 ± 17.9 | 109.1 ± 18.5 | 3.0 ± 8.8 | |||
| calcium (mg/dL) | 9.3 ± 0.5 | 9.3 ± 0.8 | −0.01 ± 0.6 | 9.5 ± 0.5 | 9.9 ± 0.5 | 0.4 ± 0.3c | |||
| 25-OH D (ng/mL) | 10.8 ± 4.6 | 10.9 ± 4.5 | 0.1 ± 0.5 | 10.1 ± 4.9 | 18.0 ± 10.3 | 7.9 ± 8.4c | |||
| tT (ng/dL) | 140 ± 90 | 150 ± 90 | 10 ± 40 | 160 ± 60 | 140 ± 50 | −20 ± 50a | |||
| mF-G scores | 12.6 ± 3.9 | 12.5 ± 3.9 | −0.1 ± 0.4 | 14.3 ± 3.8 | 11.9 ± 3.1 | −2.4 ± 1.2c | |||
| hs-CRP (mg/L) | 3.1 ± 2.1 | 3.3 ± 1.8 | 0.2 ± 0.8 | 3.7 ± 1.6 | 3.0 ± 1.2 | −0.7 ± 0.8c | |||
| TAC (nmol/L) | 881.6 ± 165.0 | 873.9 ± 189.3 | −7.7 ± 130.1 | 794.9 ± 59.3 | 841.5 ± 75.8 | 46.6 ± 66.5a | |||
| MDA (nmol/mL) | 2.2 ± 0.6 | 2.4 ± 0.9 | 0.2 ± 1.0 | 2.8 ± 0.2 | 2.4 ± 0.2 | −0.4 ± 0.3b | |||
| Type of Supplementation | Inclusion Criteria | Parameters | Placebo | Zinc | Ref. | |||
|---|---|---|---|---|---|---|---|---|
| Baseline | End of Trial | Baseline | End of Trial | p Value | ||||
| 30 mg of zinc (zinc gluconate) 4 days per menstrual cycle | Women with PD 17 years Zinc group (n = 1) | Muscle pain | Yes | No | [87] | |||
| Duration of menstrual bleeding | Normal | Normal | ||||||
| 14 mg of zinc (zinc acetate) as throat lozenges 2 days prior to and 1st day of menstrual cycle; 9 × day (total daily dose 126 mg) | Women with PD 23 years Zinc group (n = 1) | Muscle pain | Yes | No | ||||
| Menstrual cramp | Yes | No | ||||||
| Duration of menstrual bleeding | Normal | Normal | ||||||
| 60 mg of zinc (zinc gluconate) 3–4 days per menstrual cycle; twice a day per 3 cycles | Women with PD 49 years Zinc group (n = 1) | Muscle pain | Yes | No | ||||
| Menstrual cramp | Yes | No | ||||||
| Duration of menstrual bleeding | Long (8–9 days) | Normal (5 days) | ||||||
| 30 mg of zinc 1–2 days per menstrual cycle; | Women with PD 30 years Zinc group (n = 1) | Muscle pain | Yes | No | ||||
| Menstrual cramp | Yes | No | ||||||
| Duration of menstrual bleeding | Normal | Normal | ||||||
| 30 mg of zinc 3–5 days per menstrual cycle; 10 years | Women with PD 38 years Zinc group (n = 1) | Muscle pain | Yes | No | ||||
| Menstrual cramp | Yes | No | ||||||
| Duration of menstrual bleeding | Normal | Normal | ||||||
| 90 mg of zinc (220 mg of zinc sulfate) 4 days—from the day before to the third day of menstrual bleeding per 2 cycles | Women with PD 15–18 years Zinc group (n = 56) Control group – placebo (n = 46) Randomized Placebo-Controlled Trial | PVAS | [88] | |||||
| Severity of dysmenorrhea | 7.76 ± 1.30 | 8.01 ± 1.12 | ||||||
| 1st cycle | 7.13 ± 1.30 | 6.18 ± 1.70 | <0.001 | |||||
| 2nd cycle | 6.95 ± 1.67 | 3.12 ± 1.2 | <0.001 | |||||
| Diarrhea | ||||||||
| 1st cycle | 1 (2.2)* | 1 (1.9) | ||||||
| 2nd cycle | 1 (2.4)* | 2 (3.8) | ||||||
| Headache | ||||||||
| 1st cycle | 1 (1.19)* | |||||||
| 2nd cycle | ||||||||
| Heartburn | ||||||||
| 1st cycle | 1 (2.2)* | 1 (1.19)* | ||||||
| 2nd cycle | 1 (2.4)* | 1 (1.19)* | ||||||
| Duration of menstrual bleeding | 6.1 ± 1.02 | 6.7 ± 1.14 | ||||||
| 20 mg of zinc (50 mg of zinc sulfate) 4 days—from the first day to next three days of menstrual bleeding per 3 cycles | Women with PD 14–18 years Zinc group (n = 60) Control group—placebo (n = 60) DBRCT | VAS | [89] | |||||
| Pain duration | 5.47 ± 1.32 | |||||||
| 1st cycle | 4.62 ± 2.02 | 3.95 ± 1.52 | <0.05 | |||||
| 2nd cycle | 4.43 ± 1.76 | 3.22 ± 1.35 | <0.001 | |||||
| 3rd cycle | 4.42 ± 1.73 | 2.77 ± 1.47 | <0.001 | |||||
| Pain severity | 7.30 ± 2.43 | |||||||
| 1st cycle | 6.96 ± 1.56 | 6.60 ± 3.79 | ||||||
| 2nd cycle | 6.68 ± 1.79 | 5.01 ± 1.70 | <0.001 | |||||
| 3rd cycle | 6.58 ± 1.60 | 4.23 ± 1.69 | <0.001 | |||||
| 50 mg of zinc 4 days—before the menstruation twice a day per cycle | Women with PD 14–18 years Zinc group (n = 34) Control group—placebo (n = 32) DBRCT | VAS | [90] | |||||
| Severity of bleeding | 81.2 ± 71.2 | 78.9 ± 60.5 | 78.2 ± 54.1 | 64.3 ± 32.5 | <0.05 | |||
| Severity of dysmenorrhea | 56.3 ± 15.0 | 54.5 ± 18.1 | 64.9 ± 16.2 | 41.5 ± 22.3 | <0.01 | |||
| Muscular pain | 23* | 22* | 27* | 20* | <0.03 | |||
| Disability in daily activities | 29* | 26* | 27* | 10* | <0.001 | |||
| Weakness | 26* | 21* | 33* | 26* | <0.02 | |||
| 90 mg of zinc (220 mg of zinc sulfate) and 250 mg of mefenamic acid 6 days—three days before and three days after menstruation per 3 cycles | Women with PD 18–26 years Zinc group and mefenamic acid (n = 100) Control group—placebo and mefenamic acid (n = 100) DBRCT | VAS | [91] | |||||
| Mean pain | 5.8 ± 2.1 | 2.9 ± 2.6 | 5.3 ± 1.8 | 1.2 ± 1.9 | <0.001 | |||
| Dysmenorrhea | ||||||||
| Yes | 67* | 36* | <0.001 | |||||
| 30 mg of zinc 2 days before—and continuing until prior to the end of menstrual bleeding twice a day per 3 cycles. | Women with PD 17–25 years Zinc group (n = 34) | VAS | [92] | |||||
| Menstrual pain | 4.92 ± 1.80 | |||||||
| 1st cycle | 3.37 ± 2.04 | <0.001 | ||||||
| 2nd cycle | 3.30 ± 1.93 | <0.001 | ||||||
| 3rd cycle | 2.70 ± 2.03 | <0.001 | ||||||
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nasiadek, M.; Stragierowicz, J.; Klimczak, M.; Kilanowicz, A. The Role of Zinc in Selected Female Reproductive System Disorders. Nutrients 2020, 12, 2464. https://doi.org/10.3390/nu12082464
Nasiadek M, Stragierowicz J, Klimczak M, Kilanowicz A. The Role of Zinc in Selected Female Reproductive System Disorders. Nutrients. 2020; 12(8):2464. https://doi.org/10.3390/nu12082464
Chicago/Turabian StyleNasiadek, Marzenna, Joanna Stragierowicz, Michał Klimczak, and Anna Kilanowicz. 2020. "The Role of Zinc in Selected Female Reproductive System Disorders" Nutrients 12, no. 8: 2464. https://doi.org/10.3390/nu12082464
APA StyleNasiadek, M., Stragierowicz, J., Klimczak, M., & Kilanowicz, A. (2020). The Role of Zinc in Selected Female Reproductive System Disorders. Nutrients, 12(8), 2464. https://doi.org/10.3390/nu12082464





