Changes in Bone Marrow Fat upon Dietary-Induced Weight Loss
Abstract
1. Introduction
2. Materials and Method
2.1. Study Population
2.2. Laboratory Methods
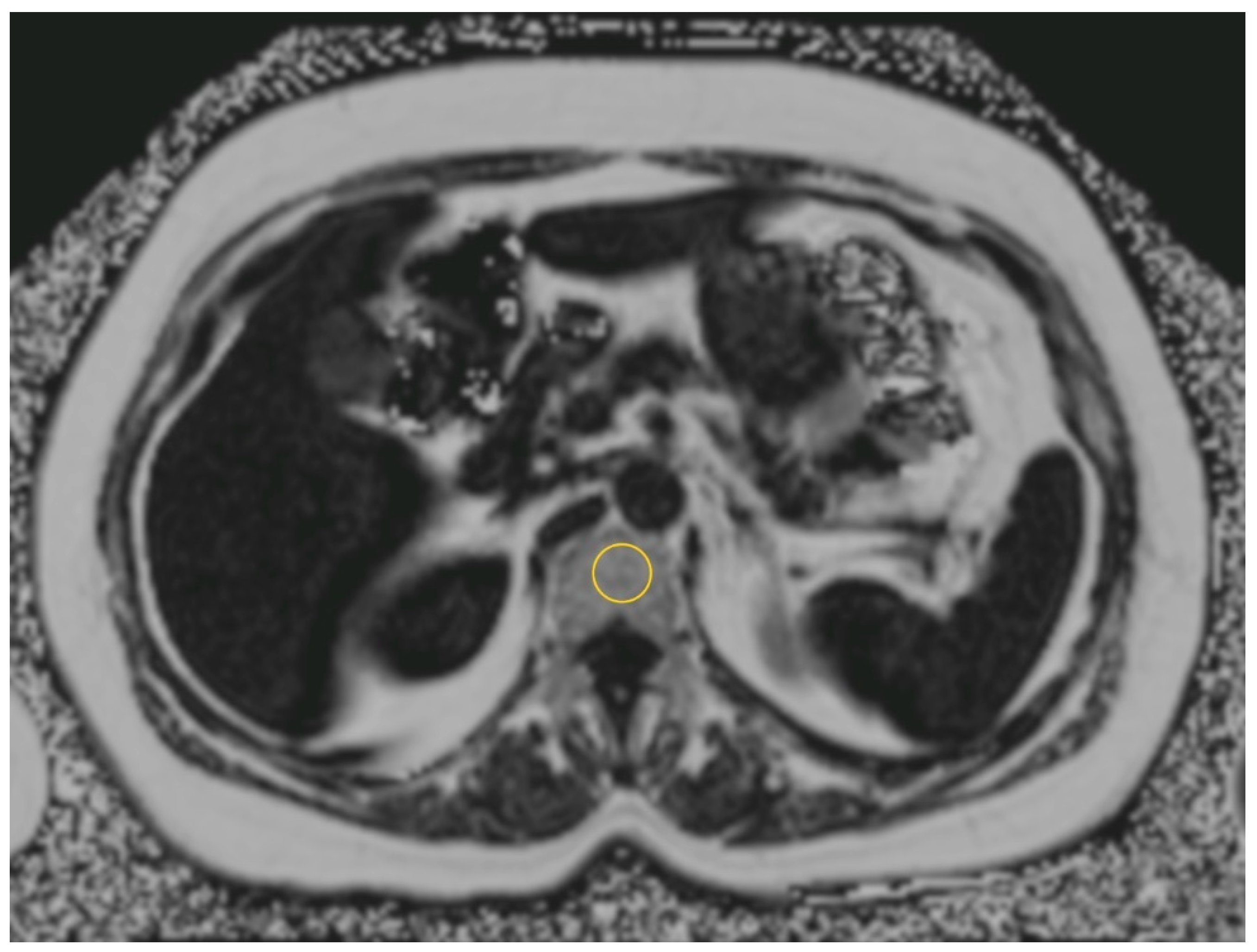
2.3. Imaging
2.4. Statistical Analyse
3. Results
3.1. Characteristics of the Study Population at Baseline
3.2. Correlations of Bone Marrow Fat in Comparison to Blood Biomarkers and Body Fat Volumes
3.3. Effects of Weight Loss on Bone Marrow Fat
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Lauby-Secretan, B.; Scoccianti, C.; Loomis, D.; Grosse, Y.; Bianchini, F.; Straif, K. Body fatness and cancer-viewpoint of the IARC working group. New Engl. J. Med. 2016, 375, 794–798. [Google Scholar] [CrossRef] [PubMed]
- Xu, H.; Zhang, Y.; Dong, H.; Pei, F.; Li, G.; Wu, D. To assess the association between vertebral marrow fat content and colorectal adenoma in postmenopausal women using magnetic resonance spectroscopy. Acta Radiol. 2016, 57, 1033–1039. [Google Scholar] [CrossRef] [PubMed]
- Chang, S.H.; Luo, S.; Thomas, T.S.; O’Brian, K.K.; Colditz, G.A.; Carlsson, N.P.; Carson, K.R. Obesity and the transformation of monoclonal gammopathy of undetermined significance to multiple myeloma: A population-based cohort study. J. Natl. Cancer Inst. 2017, 109. [Google Scholar] [CrossRef]
- Li, Q.; Wu, Y.; Kang, N. Marrow adipose tissue: Its origin, function, and regulation in bone remodeling and regeneration. Stem Cells Int. 2018, 2018, 11. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.; Leng, Y.; Gong, Y. Bone marrow fat and hematopoiesis. Front. Endocrinol. 2018, 9, 694. [Google Scholar] [CrossRef] [PubMed]
- Bertheau, R.C.; Lorbeer, R.; Nattenmuller, J.; Wintermeyer, E.; Machann, J.; Linkohr, B.; Peters, A.; Bamberg, F.; Schlett, C.L. Bone marrow fat fraction assessment in regard to physical activity: KORA FF4-3-T MR imaging in a population-based cohort. Eur. Radiol. 2020. [Google Scholar] [CrossRef]
- Horowitz, M.C.; Berry, R.; Holtrup, B.; Sebo, Z.; Nelson, T.; Fretz, J.A.; Lindskog, D.; Kaplan, J.L.; Ables, G.; Rodeheffer, M.S. Bone marrow adipocytes. Adipocyte 2017, 6, 193–204. [Google Scholar] [CrossRef]
- Morris, E.V.; Edwards, C.M. Adipokines, adiposity, and bone marrow adipocytes: Dangerous accomplices in multiple myeloma. J. Cell. Physiol. 2018, 233, 9159–9166. [Google Scholar] [CrossRef]
- Guerra, D.A.P.; Paiva, A.E.; Sena, I.F.G.; Azevedo, P.O.; Batista, M.L., Jr.; Mintz, A.; Birbrair, A. Adipocytes role in the bone marrow niche. Cytom. Part A J. Int. Soc. Anal. Cytol. 2018, 93, 167–171. [Google Scholar] [CrossRef]
- Morris, E.V.; Edwards, C.M. The role of bone marrow adipocytes in bone metastasis. J. Bone Oncol. 2016, 5, 121–123. [Google Scholar] [CrossRef]
- Masumoto, A.; Yonekura, S.; Haida, M.; Yanagimachi, N.; Hotta, T. Analysis of intramedullary cell density by MRI using the multiple spin-echo technique. Am. J. Hematol. 1997, 55, 134–138. [Google Scholar] [CrossRef]
- Trotter, T.N.; Gibson, J.T.; Sherpa, T.L.; Gowda, P.S.; Peker, D.; Yang, Y. Adipocyte-lineage cells support growth and dissemination of multiple myeloma in bone. Am. J. Pathol. 2016, 186, 3054–3063. [Google Scholar] [CrossRef] [PubMed]
- Kim, T.Y.; Schwartz, A.V.; Li, X.; Xu, K.; Black, D.M.; Petrenko, D.M.; Stewart, L.; Rogers, S.J.; Posselt, A.M.; Carter, J.T.; et al. Bone marrow fat changes after gastric bypass surgery are associated with loss of bone mass. J. Bone Miner. Res. Off. J. Am. Soc. Bone Miner. Res. 2017, 32, 2239–2247. [Google Scholar] [CrossRef] [PubMed]
- Ivaska, K.K.; Huovinen, V.; Soinio, M.; Hannukainen, J.C.; Saunavaara, V.; Salminen, P.; Helmio, M.; Parkkola, R.; Nuutila, P.; Kiviranta, R. Changes in bone metabolism after bariatric surgery by gastric bypass or sleeve gastrectomy. Bone 2017, 95, 47–54. [Google Scholar] [CrossRef] [PubMed]
- Schafer, A.L.; Li, X.; Schwartz, A.V.; Tufts, L.S.; Wheeler, A.L.; Grunfeld, C.; Stewart, L.; Rogers, S.J.; Carter, J.T.; Posselt, A.M.; et al. Changes in vertebral bone marrow fat and bone mass after gastric bypass surgery: A pilot study. Bone 2015, 74, 140–145. [Google Scholar] [CrossRef]
- Bredella, M.A.; Greenblatt, L.B.; Eajazi, A.; Torriani, M.; Yu, E.W. Effects of Roux-En-Y gastric bypass and sleeve gastrectomy on bone mineral density and marrow adipose tissue. Bone 2017, 95, 85–90. [Google Scholar] [CrossRef]
- Blom-Hogestol, I.K.; Mala, T.; Kristinsson, J.A.; Hauge, E.M.; Brunborg, C.; Gulseth, H.L.; Eriksen, E.F. Changes in bone marrow adipose tissue one year after Roux-En-Y gastric bypass: A prospective cohort study. J. Bone Miner. Res. Off. J. Am. Soc. Bone Miner. Res. 2019, 34, 1815–1823. [Google Scholar] [CrossRef]
- Osataphan, S.; Patti, M.E. Trim the gut, lose the weight-and the bone. J. Clin. Investig. 2019, 129, 2184–2186. [Google Scholar] [CrossRef]
- Vogt, L.J.; Steveling, A.; Meffert, P.J.; Kromrey, M.L.; Kessler, R.; Hosten, N.; Kruger, J.; Gartner, S.; Aghdassi, A.A.; Mayerle, J.; et al. Magnetic resonance imaging of changes in abdominal compartments in obese diabetics during a low-calorie weight-loss program. PLoS ONE 2016, 11, e0153595. [Google Scholar] [CrossRef]
- Cordes, C.; Dieckmeyer, M.; Ott, B.; Shen, J.; Ruschke, S.; Settles, M.; Eichhorn, C.; Bauer, J.S.; Kooijman, H.; Rummeny, E.J.; et al. MR-detected changes in liver fat, abdominal fat, and vertebral bone marrow fat after a four-week calorie restriction in obese women. J. Magn. Reson. Imaging JMRI 2015, 42, 1272–1280. [Google Scholar] [CrossRef]
- Schubel, R.; Graf, M.E.; Nattenmuller, J.; Nabers, D.; Sookthai, D.; Gruner, L.F.; Johnson, T.; Schlett, C.L.; von Stackelberg, O.; Kirsten, R.; et al. The effects of intermittent calorie restriction on metabolic health: Rationale and study design of the HELENA Trial. Contemp. Clin. Trials 2016, 51, 28–33. [Google Scholar] [CrossRef] [PubMed]
- Schubel, R.; Nattenmuller, J.; Sookthai, D.; Nonnenmacher, T.; Graf, M.E.; Riedl, L.; Schlett, C.L.; von Stackelberg, O.; Johnson, T.; Nabers, D.; et al. Effects of intermittent and continuous calorie restriction on body weight and metabolism over 50 wk: A randomized controlled trial. Am. J. Clin. Nutr. 2018, 108, 933–945. [Google Scholar] [CrossRef] [PubMed]
- Baum, T.; Rohrmeier, A.; Syvari, J.; Diefenbach, M.N.; Franz, D.; Dieckmeyer, M.; Scharr, A.; Hauner, H.; Ruschke, S.; Kirschke, J.S.; et al. Anatomical variation of age-related changes in vertebral bone marrow composition using chemical shift encoding-based water-fat magnetic resonance imaging. Front. Endocrinol. 2018, 9, 141. [Google Scholar] [CrossRef] [PubMed]
- Baum, T.; Yap, S.P.; Dieckmeyer, M.; Ruschke, S.; Eggers, H.; Kooijman, H.; Rummeny, E.J.; Bauer, J.S.; Karampinos, D.C. Assessment of whole spine vertebral bone marrow fat using chemical shift-encoding based water-fat MRI. J. Magn. Reson. Imaging JMRI 2015, 42, 1018–1023. [Google Scholar] [CrossRef]
- Kuhn, J.P.; Hernando, D.; Meffert, P.J.; Reeder, S.; Hosten, N.; Laqua, R.; Steveling, A.; Ender, S.; Schroder, H.; Pillich, D.T. Proton-density fat fraction and simultaneous R2* estimation as an MRI tool for assessment of osteoporosis. Eur. Radiol. 2013, 23, 3432–3439. [Google Scholar] [CrossRef]
- Idilman, I.S.; Tuzun, A.; Savas, B.; Elhan, A.H.; Celik, A.; Idilman, R.; Karcaaltincaba, M. Quantification of liver, pancreas, kidney, and vertebral body MRI-PDFF in non-alcoholic fatty liver disease. Abdom. Imaging 2015, 40, 1512–1519. [Google Scholar] [CrossRef]
- Kuhn, T.; Nonnenmacher, T.; Sookthai, D.; Schubel, R.; Quintana-Pacheco, D.A.; von Stackelberg, O.; Graf, M.E.; Johnson, T.; Schlett, C.L.; Kirsten, R.; et al. Anthropometric and blood parameters for the prediction of NAFLD among overweight and obese adults. BMC Gastroenterol. 2018, 18, 113. [Google Scholar] [CrossRef]
- Schubel, R.; Nonnenmacher, T.; Sookthai, D.; Gonzalez-Maldonado, S.; Sowah, S.A.; von Stackelberg, O.; Schlett, C.L.; Grafetstatter, M.; Nabers, D.; Johnson, T.; et al. Similar weight loss induces greater improvements in insulin sensitivity and liver function among individuals with NAFLD compared to individuals without NAFLD. Nutrients 2019, 11, 544. [Google Scholar] [CrossRef]
- Wald, D.; Teucher, B.; Dinkel, J.; Kaaks, R.; Delorme, S.; Boeing, H.; Seidensaal, K.; Meinzer, H.P.; Heimann, T. Automatic quantification of subcutaneous and visceral adipose tissue from whole-body magnetic resonance images suitable for large cohort studies. J. Magn. Reson. Imaging JMRI 2012, 36, 1421–1434. [Google Scholar] [CrossRef]
- Tornqvist, L.; Vartia, P.; Vartia, Y.O. How should relative changes be measured? Am. Stat. 1985, 39, 43–46. [Google Scholar]
- Jiang, Y.; Spurny, M.; Schubel, R.; Nonnenmacher, T.; Schlett, C.L.; von Stackelberg, O.; Ulrich, C.M.; Kaaks, R.; Kauczor, H.U.; Kuhn, T.; et al. Changes in pancreatic fat content following diet-induced weight loss. Nutrients 2019, 11, 912. [Google Scholar] [CrossRef] [PubMed]
- Yu, N.Y.; Wolfson, T.; Middleton, M.S.; Hamilton, G.; Gamst, A.; Angeles, J.E.; Schwimmer, J.B.; Sirlin, C.B. Bone marrow fat content is correlated with hepatic fat content in paediatric non-alcoholic fatty liver disease. Clin. Radiol. 2017, 72, 425.e9–425.e14. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Bredella, M.A.; Gill, C.M.; Gerweck, A.V.; Landa, M.G.; Kumar, V.; Daley, S.M.; Torriani, M.; Miller, K.K. Ectopic and serum lipid levels are positively associated with bone marrow fat in obesity. Radiology 2013, 269, 534–541. [Google Scholar] [CrossRef] [PubMed]
- Cawthorn, W.P.; Scheller, E.L.; Learman, B.S.; Parlee, S.D.; Simon, B.R.; Mori, H.; Ning, X.; Bree, A.J.; Schell, B.; Broome, D.T.; et al. Bone marrow adipose tissue is an endocrine organ that contributes to increased circulating adiponectin during caloric restriction. Cell Metab. 2014, 20, 368–375. [Google Scholar] [CrossRef] [PubMed]
- Tishinsky, J.M.; Robinson, L.E.; Dyck, D.J. Insulin-sensitizing properties of adiponectin. Biochimie 2012, 94, 2131–2136. [Google Scholar] [CrossRef] [PubMed]
- Ye, R.; Scherer, P.E. Adiponectin, driver or passenger on the road to insulin sensitivity? Mol. Metab. 2013, 2, 133–141. [Google Scholar] [CrossRef]
- Tishinsky, J.M.; Dyck, D.J.; Robinson, L.E. Lifestyle factors increasing adiponectin synthesis and secretion. Vitam. Horm. 2012, 90, 1–30. [Google Scholar]
- Baum, T.; Yap, S.P.; Karampinos, D.C.; Nardo, L.; Kuo, D.; Burghardt, A.J.; Masharani, U.B.; Schwartz, A.V.; Li, X.; Link, T.M. Does vertebral bone marrow fat content correlate with abdominal adipose tissue, lumbar spine bone mineral density, and blood biomarkers in women with type 2 diabetes mellitus? J. Magn. Reson. Imag. JMRI 2012, 35, 117–124. [Google Scholar] [CrossRef]
- Pham, T.T.; Ivaska, K.K.; Hannukainen, J.C.; Virtanen, K.A.; Lidell, M.E.; Enerback, S.; Makela, K.; Parkkola, R.; Piirola, S.; Oikonen, V.; et al. Human bone marrow adipose tissue is a metabolically active and insulin sensitive distinct fat depot. J. Clin. Endocrinol. Metab. 2020. [Google Scholar] [CrossRef]
- Scheller, E.L.; Khoury, B.; Moller, K.L.; Wee, N.K.; Khandaker, S.; Kozloff, K.M.; Abrishami, S.H.; Zamarron, B.F.; Singer, K. Changes in skeletal integrity and marrow adiposity during high-fat diet and after weight loss. Front. Endocrinol. 2016, 7, 102. [Google Scholar] [CrossRef]
- Lwin, S.T.; Olechnowicz, S.W.; Fowler, J.A.; Edwards, C.M. Diet-induced obesity promotes a myeloma-like condition in vivo. Leukemia 2015, 29, 507–510. [Google Scholar] [CrossRef] [PubMed]
- Ruan, J.; Trotter, T.N.; Nan, L.; Luo, R.; Javed, A.; Sanderson, R.D.; Suva, L.J.; Yang, Y. Heparanase inhibits osteoblastogenesis and shifts bone marrow progenitor cell fate in myeloma bone disease. Bone 2013, 57, 10–17. [Google Scholar] [CrossRef] [PubMed]
- Singhal, V.; Bredella, M.A. Marrow adipose tissue imaging in humans. Bone 2019, 118, 69–76. [Google Scholar] [CrossRef] [PubMed]
- Bredella, M.A.; Fazeli, P.K.; Miller, K.K.; Misra, M.; Torriani, M.; Thomas, B.J.; Ghomi, R.H.; Rosen, C.J.; Klibanski, A. Increased bone marrow fat in anorexia nervosa. J. Clin. Endocrinol. Metab. 2009, 94, 2129–2136. [Google Scholar] [CrossRef] [PubMed]
- Robinson, L.; Micali, N.; Misra, M. Eating disorders and bone metabolism in women. Curr. Opin. Pediatrics 2017, 29, 488–496. [Google Scholar] [CrossRef]
- Abella, E.; Feliu, E.; Granada, I.; Milla, F.; Oriol, A.; Ribera, J.M.; Sanchez-Planell, L.; Berga, L.I.; Reverter, J.C.; Rozman, C. Bone marrow changes in anorexia nervosa are correlated with the amount of weight loss and not with other clinical findings. Am. J. Clin. Pathol. 2002, 118, 582–588. [Google Scholar] [CrossRef]
- Fazeli, P.K.; Bredella, M.A.; Freedman, L.; Thomas, B.J.; Breggia, A.; Meenaghan, E.; Rosen, C.J.; Klibanski, A. Marrow fat and preadipocyte factor-1 levels decrease with recovery in women with anorexia nervosa. J. Bone Miner. 2012, 27, 1864–1871. [Google Scholar] [CrossRef]
- Patsch, J.M.; Li, X.; Baum, T.; Yap, S.P.; Karampinos, D.C.; Schwartz, A.V.; Link, T.M. Bone marrow fat composition as a novel imaging biomarker in postmenopausal women with prevalent fragility fractures. J. Bone Miner. Res. 2013, 28, 1721–1728. [Google Scholar] [CrossRef]
- Tang, A.; Tan, J.; Sun, M.; Hamilton, G.; Bydder, M.; Wolfson, T.; Gamst, A.C.; Middleton, M.; Brunt, E.M.; Loomba, R.; et al. Nonalcoholic fatty liver disease: MR imaging of liver proton density fat fraction to assess hepatic steatosis. Radiology 2013, 267, 422–431. [Google Scholar] [CrossRef]
- Heba, E.R.; Desai, A.; Zand, K.A.; Hamilton, G.; Wolfson, T.; Schlein, A.N.; Gamst, A.; Loomba, R.; Sirlin, C.B.; Middleton, M.S. Accuracy and the effect of possible subject-based confounders of magnitude-based MRI for estimating hepatic proton density fat fraction in adults, using MR spectroscopy as reference. J. Magn. Reson. Imag. JMRI 2016, 43, 398–406. [Google Scholar] [CrossRef]
- Gee, C.S.; Nguyen, J.T.; Marquez, C.J.; Heunis, J.; Lai, A.; Wyatt, C.; Han, M.; Kazakia, G.; Burghardt, A.J.; Karampinos, D.C.; et al. Validation of bone marrow fat quantification in the presence of trabecular bone using MRI. J. Magn. Reson. Imag. JMRI 2015, 42, 539–544. [Google Scholar] [CrossRef] [PubMed]

| Q1 | Q2 | Q3 | Q4 | |
|---|---|---|---|---|
| ≤2% | >2% to ≤4.5% | >4.5% to ≤7.5% | >7.5% | |
| n = 35 | n = 34 | n = 35 | n = 33 | |
| Women (n (%)) | 19 (54.3) | 14 (41.2) | 18 (51.4) | 17 (51.5) |
| Age (year) | 50.9 ± 6.4 | 50.8 ± 8.4 | 51.2 ± 7.9 | 47.3 ± 8.5 |
| Height (cm) | 171.4 ± 10.6 | 174.2 ± 9.8 | 173.8 ± 10.6 | 172.8 ± 7.9 |
| Weight (kg) | 94.8 ± 15.7 | 93.7 ± 14.4 | 93.9 ± 15.3 | 94.7 ± 14.4 |
| Waist circumference (cm) | 106.1 ± 12.0 | 104.9 ± 10.7 | 103.1 ± 10.8 | 103.5 ± 12.2 |
| BMI (kg/m2) | 32.2 ± 4.1 | 30.8 ± 3.6 | 31.0 ± 3.4 | 31.6 ± 3.6 |
| VAT (L) | 5.3 ± 2.2 | 4.8 ± 2.1 | 4.8 ± 2.0 | 4.7 ± 2.1 |
| SAT (L) | 13.1 ± 4.6 | 11.2 ± 2.9 | 12.1 ± 3.9 | 12.9 ± 4.1 |
| BMFC (%) | 43.9 ± 8.7 | 42.6 ± 8.3 | 44.6 ± 7.9 | 41.4 ± 10.2 |
| LFC (%) | 7.1 ± 4.4 | 8.8 ± 7.8 | 7.9 ± 6.5 | 7.4 ± 4.9 |
| ALT (U/L) | 25.0 ± 7.3 | 30.8 ± 13.9 | 26.6 ± 12.2 | 24.8 ± 9.9 |
| AST (U/L) | 21.7 ± 4.0 | 25.4 ± 6.8 | 22.3 ± 3.9 | 22.4 ± 5.2 |
| GGT (U/L) | 29.4 ± 14.0 | 25.5 ± 16.2 | 29.8 ± 19.7 | 24.3 ± 12.6 |
| Triglycerides (mg/dL) | 138.9 ± 65.7 | 135.0 ± 91.8 | 145.3 ± 94.2 | 109.4 ± 55.0 |
| Cholesterol (mg/dL) | 210.3 ± 33.9 | 201.9 ± 36.9 | 214.5 ± 36.5 | 203.3 ± 32.0 |
| HDL (mg/dL) | 53.5 ± 14.8 | 53.1 ± 14.5 | 56.3 ± 13.5 | 53.4 ± 15.3 |
| LDL (mg/dL) | 129.1 ± 26.2 | 120.2 ± 25.7 | 129.2 ± 26.8 | 128.0 ± 27.9 |
| Glucose (mg/dL) | 93.5 ± 8.0 | 93.2 ± 7.0 | 94.9 ± 6.9 | 91.9 ± 8.3 |
| Insulin (mU/L) | 14.9 ± 7.8 | 12.0 ± 6.9 | 10.9 ± 5.1 | 11.4 ± 5.6 |
| HbA1c (%) | 5.4 ± 0.4 | 5.5 ± 0.3 | 5.5 ± 0.3 | 5.5 ± 0.3 |
| HOMA-IR | 3.5 ± 1.9 | 2.8 ± 1.8 | 2.6 ± 1.2 | 2.6 ± 1.4 |
| CRP (ng/pL) | 7.0 ± 8.7 | 4.1 ± 5.5 | 3.8 ± 2.8 | 3.9 ± 3.8 |
| IFN-γ (ng/µL) | 16.6 ± 16.1 | 12.9 ± 12.9 | 17.5 ± 16.7 | 11.1 ± 7.8 |
| TNF-α (ng/µL) | 4.3 ± 2.7 | 4.0 ± 2.5 | 5.0 ± 2.6 | 4.2 ± 2.5 |
| IL-6 (ng/µL) | 2.0 ± 1.7 | 1.8 ± 3.5 | 1.3 ± 0.8 | 1.3 ± 1.1 |
| IL-8 (ng/µL) | 10.6 ± 4.4 | 14.2 ± 23.7 | 9.8 ± 4.8 | 10.6 ± 5.3 |
| LDH (U/L) | 197.3 ± 30.1 | 197.4 ± 26.8 | 192.7 ± 31.8 | 200.2 ± 28.3 |
| Adiponectin (ng/mL) | 15.6 ± 8.4 | 18.7 ± 11.4 | 16.9 ± 11.4 | 19.9 ± 13.7 |
| Leptin (ng/mL) | 29.2 ± 25.3 | 19.8 ± 20.3 | 21.5 ± 15.2 | 29.7 ± 29.4 |
| Erythrocytes (1/pl) | 4.8 ± 0.4 | 4.8 ± 0.5 | 4.9 ± 0.4 | 4.9 ± 0.3 |
| Leukocytes (1/nl) | 6.4 ± 1.5 | 6.1 ± 1.5 | 6.3 ± 1.3 | 6.3 ± 1.3 |
| Neutrophil granulocytes (%) | 58.9 ± 6.3 | 56.6 ± 8.1 | 57.7 ± 7.1 | 56.5 ± 9.2 |
| Lymphocytes (%) | 29.6 ± 6.2 | 30.6 ± 6.2 | 30.3 ± 7.1 | 31.5 ± 8.6 |
| Monocytes (%) | 6.1 ± 1.4 | 7.2 ± 2.0 | 6.6 ± 1.4 | 6.2 ± 1.5 |
| Thrombocytes (1/nl) | 239.2 ± 49.2 | 237.9 ± 50.6 | 240.5 ± 46.7 | 249.6 ± 60.5 |
| Bone Marrow Fat Content | ||||||
|---|---|---|---|---|---|---|
| Baseline | Week 12 | Week 50 | ||||
| rho | p-Value | rho | p-Value | rho | p-Value | |
| Weight | −0.21 | 0.0143* | 0.02 | 0.7999 | 0.05 | 0.592 |
| Waist circumference | −0.25 | 0.0041* | 0.06 | 0.5434 | - | - |
| BMI | −0.31 | 0.0003* | −0.12 | 0.177 | 0.01 | 0.8748 |
| VAT | −0.007 | 0.9394 | 0.18 | 0.045* | 0.19 | 0.032* |
| SAT | −0.20 | 0.0221* | −0.002 | 0.986 | 0.05 | 0.598 |
| LFC | 0.03 | 0.7228 | 0.17 | 0.0653 | 0.17 | 0.0699 |
| ALT | 0.10 | 0.237 | 0.25 | 0.0045* | 0.22 | 0.0159 |
| AST | 0.03 | 0.7087 | 0.15 | 0.0917 | 0.11 | 0.255 |
| GGT | 0.12 | 0.1872 | 0.28 | 0.0018* | 0.32 | 0.0004* |
| Triglycerides | 0.02 | 0.8556 | 0.09 | 0.3463 | 0.14 | 0.1216 |
| Cholesterol | 0.13 | 0.1314 | 0.18 | 0.0471* | 0.28 | 0.0024* |
| HDL | 0.21 | 0.0166* | 0.14 | 0.1165 | 0.23 | 0.0121* |
| LDL | 0.10 | 0.2473 | 0.14 | 0.1203 | 0.14 | 0.1399 |
| Glucose | 0.03 | 0.699 | 0.005 | 0.9596 | 0.09 | 0.3087 |
| Insulin | 0.04 | 0.6538 | 0.11 | 0.2432 | 0.12 | 0.1863 |
| HbA1c | 0.007 | 0.9388 | 0.06 | 0.5014 | 0.19 | 0.044* |
| HOMA-IR | 0.05 | 0.5945 | 0.10 | 0.2525 | 0.13 | 0.1641 |
| CRP | −0.10 | 0.2636 | 0.12 | 0.1725 | 0.10 | 0.2824 |
| INF-g | −0.03 | 0.7411 | 0.06 | 0.484 | −0.01 | 0.913 |
| TNF-a | −0.05 | 0.5489 | 0.01 | 0.8965 | −0.09 | 0.2886 |
| IL-6 | −0.12 | 0.1729 | −0.02 | 0.8467 | 0.03 | 0.7866 |
| IL-8 | 0.17 | 0.0528 | 0.07 | 0.4171 | 0.07 | 0.4803 |
| LDH | 0.25 | 0.0048* | 0.16 | 0.0746 | - | - |
| Adiponectin | 0.20 | 0.0194* | 0.21 | 0.0145* | - | - |
| Leptin | −0.02 | 0.8133 | 0.14 | 0.1191 | 0.07 | 0.4251 |
| Erythrocytes | −0.01 | 0.8797 | 0.03 | 0.7095 | 0.07 | 0.4519 |
| Leukocytes | −0.09 | 0.3155 | −0.009 | 0.9222 | −0.05 | 0.569 |
| Neutrophil granulocytes | 0.00 | 0.9855 | −0.08 | 0.3929 | −0.06 | 0.4887 |
| Lymphocytes | 0.03 | 0.7398 | 0.07 | 0.4235 | 0.05 | 0.6114 |
| Monocytes | −0.07 | 0.4249 | 0.03 | 0.7577 | 0.02 | 0.7993 |
| Thrombocytes | −0.09 | 0.3041 | −0.12 | 0.1895 | 0.05 | 0.5778 |
| Baseline Mean ± SD | Week 12 Mean ± SD | Loge Relative Change (Baseline–Week 12) Mean ± SEM | p-Value | Week 50 Mean ± SD | Loge Relative Change (Baseline–Week 50) Mean ± SEM | p-Value | ||
|---|---|---|---|---|---|---|---|---|
| Weight (kg) | Q1 | 94.8 ± 15.7 | 94.8 ± 15.6 | 0.0 ± 0.2 | <0.01* | 96.1 ± 16.1 | 1.3 ± 0.6 | <0.01* |
| Q2 | 93.7 ± 14.4 | 90.7 ± 14.0 | −3.2 ± 0.1 | 93.3 ± 13.9 | −1.3 ± 0.5 | |||
| Q3 | 93.9 ± 15.3 | 88.4 ± 14.4 | −6.1 ± 0.2 | 89.8 ± 15.8 | −4.4 ± 0.8 | |||
| Q4 | 94.7 ± 14.4 | 84.4 ± 12.8 | −11.5 ± 0.6 | 84.8 ± 14.2 | −11.2 ± 1.6 | |||
| BMFC (%) | Q1 | 43.9 ± 8.7 | 44.0 ± 8.5 | 0.7 ± 2.4 | <0.01* | 44.3 ± 7.5 | 1.4 ± 3.0 | 0.02 |
| Q2 | 42.6 ± 8.3 | 41.3 ± 8.2 | −3.5 ± 2.0 | 41.9 ± 7.5 | −1.2 ± 1.9 | |||
| Q3 | 44.6 ± 7.9 | 44.1 ± 8.3 | −1.4 ± 2.4 | 46.3 ± 8.4 | 1.8 ± 1.8 | |||
| Q4 | 41.4 ± 10.2 | 37.0 ± 10.8 | −12.7 ± 3.3 | 38.6 ± 9.7 | −6.9 ± 2.3 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Spurny, M.; Jiang, Y.; Sowah, S.A.; Schübel, R.; Nonnenmacher, T.; Bertheau, R.; Kirsten, R.; Johnson, T.; Hillengass, J.; Schlett, C.L.; et al. Changes in Bone Marrow Fat upon Dietary-Induced Weight Loss. Nutrients 2020, 12, 1509. https://doi.org/10.3390/nu12051509
Spurny M, Jiang Y, Sowah SA, Schübel R, Nonnenmacher T, Bertheau R, Kirsten R, Johnson T, Hillengass J, Schlett CL, et al. Changes in Bone Marrow Fat upon Dietary-Induced Weight Loss. Nutrients. 2020; 12(5):1509. https://doi.org/10.3390/nu12051509
Chicago/Turabian StyleSpurny, Manuela, Yixin Jiang, Solomon A. Sowah, Ruth Schübel, Tobias Nonnenmacher, Robert Bertheau, Romy Kirsten, Theron Johnson, Jens Hillengass, Christopher L. Schlett, and et al. 2020. "Changes in Bone Marrow Fat upon Dietary-Induced Weight Loss" Nutrients 12, no. 5: 1509. https://doi.org/10.3390/nu12051509
APA StyleSpurny, M., Jiang, Y., Sowah, S. A., Schübel, R., Nonnenmacher, T., Bertheau, R., Kirsten, R., Johnson, T., Hillengass, J., Schlett, C. L., von Stackelberg, O., Ulrich, C. M., Kaaks, R., Kauczor, H.-U., Kühn, T., & Nattenmüller, J. (2020). Changes in Bone Marrow Fat upon Dietary-Induced Weight Loss. Nutrients, 12(5), 1509. https://doi.org/10.3390/nu12051509






