1. Introduction
The World Health Organization (WHO) estimated that around two billion people were anemic in the world, which makes this disease one of the most common nutrition disorders [
1]. Anemia was defined as a hemoglobin (Hb) concentration below the thresholds given by WHO, United Nations Children’s Fund (UNICEF), United Nations University (UNU) [
2]. For children aged from 6 to 59 months of age and pregnant women, anemia is diagnosed when Hb is under 11 g/dL, under 11.5 g/dL for children aged 5–11, and under 12 g/dL for children aged 12–14 and non-pregnant females. Finally, for males aged 15 years and above, anemia is diagnosed when the level of Hb is under 13 g/dL. The main cause of anemia identified was iron deficiency (ID), which is defined by WHO as “a state in which there is insufficient iron to maintain the normal physiological function of tissues such as the blood, brain, and muscles” [
1]. ID is characterized by no mobilized iron stores and signs of a compromised supply of iron [
3]. ID was estimated to represent over than 60% of the anemia causes [
4,
5], especially among the younger population [
4,
6]. This nutritional deficiency—commonly defined as serum ferritin level on blood ≤30 µg/L [
7,
8]—has several consequences for human health, such as a delay in children’s mental and physical development, a decrease in work productivity, intelligence or cognitive capacity [
1,
9]. In some countries, ID and iron deficiency anemia (IDA) may also contribute to child, maternal, and perinatal mortality [
1,
9]. Among the overall population, the most concerned by this nutritional disease are children, adolescents, and women (pregnant and non-pregnant) in reproductive age [
4,
5,
10].
To reduce ID, the consumption of bioavailable iron-rich food—such as red meat—would be a logically feasible solution, since this food is the richest source of high absorbable iron (heme-iron) [
11]. A study revealed that an increase in red meat consumption twice a week compared to seldom intake would decrease 24% of child ID in Israel [
12]. Another study estimated an increase of 0.6% in serum ferritin in blood levels per 1g of red meat consumed [
13].
Since 1990, the Global Burden of Diseases (GBD) study, supported by the World Health Organization, has estimated the disability adjusted life years (DALY) associated with health effects of major diseases, injury, and risk factors. This metric takes into account mortality and morbidity and is expressed as the sum of the number of years of life lost (YLL) from premature death and the number of years lived with disability (YLD) [
14]. In addition to quantifying the impact of disease, the burden of diseases helps in risk-mitigating strategy: Several consumption patterns can be evaluated and compared by scenario analysis. In particular, in the study of Kassebaum on behalf of GBD 2013 Anemia Collaborators evaluated the global burden of anemia [
4]. This work estimated that, in 2013, anemia was responsible for 61.5 (41.0–88.7) millions of YLD in the world, from which 300,654 (200,463–434,060) YLD in France. However, this burden was estimated from hemoglobin levels, which makes scenarios of iron consumption impossible.
Regarding the separation of uncertainty—due to the lack of data and knowledge and variability associated with heterogeneity within populations—[
15,
16] of the inputs, it is important to identify which of them are driving the output of the risk model and to identify the needed data to increase the precision and the confidence of the estimated output [
17].
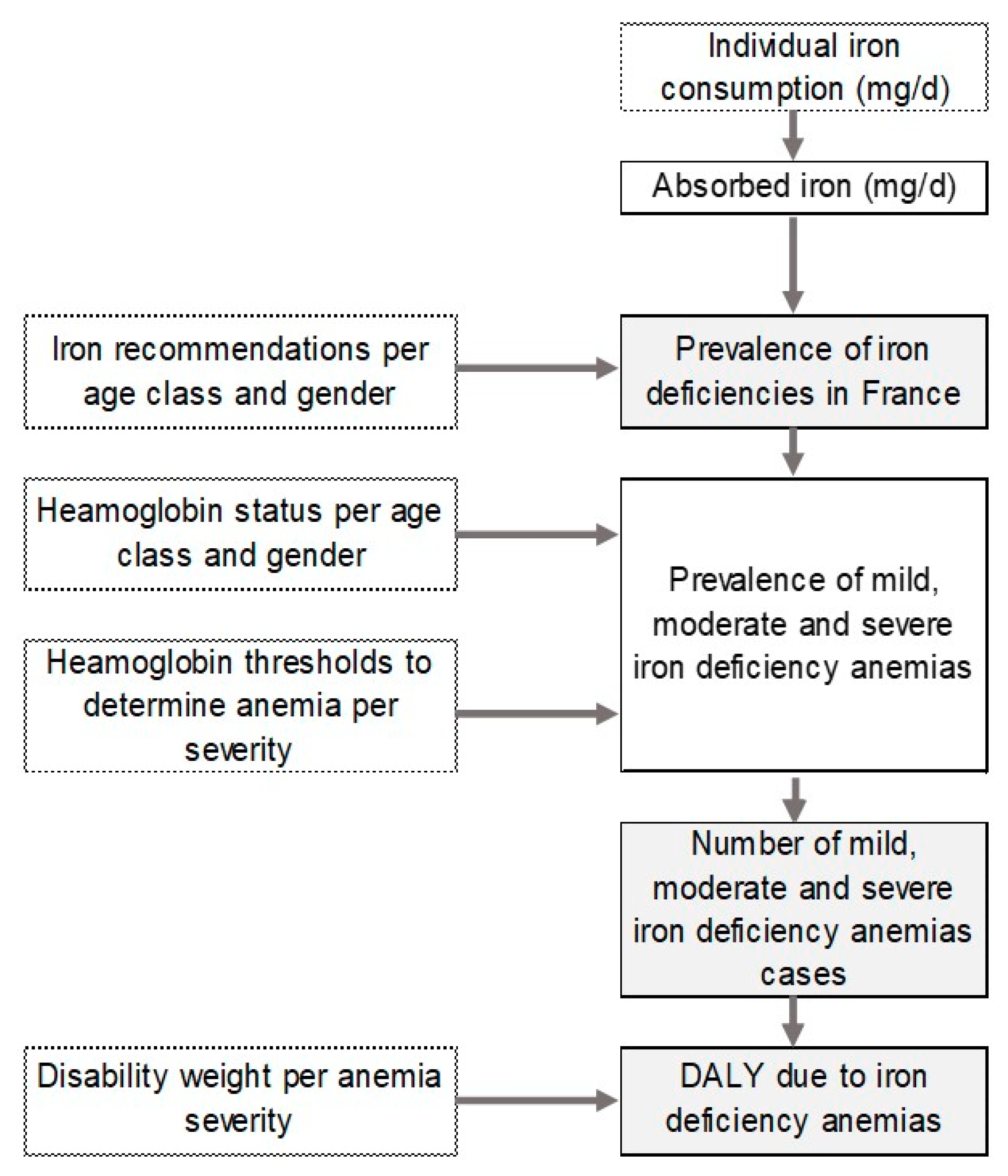
The objective of this study was to estimate the burden of disease in France due to ID, taking iron consumption into account. Based upon dietary surveys, iron recommendations and blood iron status of the French population, a probabilistic model was set up for both genders and for specific age classes to quantify the risk of ID and the consequent burden of disease due to IDA. Then, to reduce the burden, consumption scenario was built with ground beef intake as red meat is the richest source of high absorbable iron in developed countries.
3. Results
3.1. Prevalence and Number of Iron Deficiencies in France
The distributions of ID with current consumption of iron in France are shown in
Table 3. The mean number of ID cases is represented with its 95% confidence interval.
Among children, the most concerned with ID were children aged from 7 to 11, with 20% (95% CI = 16%–24%) and 31% (95% CI = 27%–36%) ID in this age class for males and females, respectively. Adolescent females were also more concerned with ID compared to adolescent males (
Table 3).
The higher impact of ID among females was also noted in adults’ age classes. Menstruating adult females aged from 18 to 24 were the most concerned with ID with 37% [95% CI = 33%–41%] of iron-deficient in this population group, corresponding to 1600 [95% CI = 1400–1700] IDs cases per 100,000 individuals. After this age class, the prevalence of ID decreases with increasing age.
3.2. Number of Iron Deficiency Anemias
In France, only children aged from three to six, older adolescent females, adult females and males aged from 25 to 44 years and from 65 to 74 suffered from IDA [
25,
26]. The distributions of IDA with current consumption of iron in France are shown in
Table 4. The mean number of IDA cases is represented with its 95% confidence interval.
A total of 1290 [95% CI = 1230–1350] cases of IDA per 100,000 individuals per year was estimated in the French population.
Children aged from three to six, had almost the same number of IDA cases for males and females with 32 (95% CI = 21–45) and 33 (95% CI = 23–45) cases per 100,000 individuals per year, respectively. Among adolescents, only females aged from 15 to 17 are concerned with IDA. The number of IDA cases for this population was ten times higher than for females aged from three to six.
Adult females were significantly more concerned with IDA than males with 584 (95% CI = 558–612) IDA cases versus 237 (95% CI = 194–282) IDA cases per 100,000 individuals, respectively. The major number of cases concerned menstruating women aged from 15 to 17 with 404 (95% CI = 377–431) IDA cases per 100,000 individuals per year. The cases of IDA for menopaused females only concerned the last age class.
3.3. DALY Attributable to Iron Deficiency Anemias
The number of DALY per 100,000 individuals per year associated with IDA in France is given in
Table 4. The mean number of IDA DALY is represented with its 95% confidence interval.
The major contributors to the burden from IDA were menstruating females aged from 25 to 44 with 6.5 (95% CI = 4.2–9.0) DALY associated with IDA per 100,000 individuals per year. Young children aged from three to six, had a low burden with an equivalent number of DALYs (0.3 (95% CI = 0.1–0.5) DALY per 100,000 per year). Older adolescent females, aged from 15 to 17, contributed with 4.0 (95% CI = 2.1–5.9) DALY per 100,000 individuals per year.
The estimated number of DALY associated with IDA was 16 (95% CI = 11–20) per 100,000 French individuals per year, from which more than 80% of the DALY were attributable to menstruating females.
3.4. Consumption Scenarios
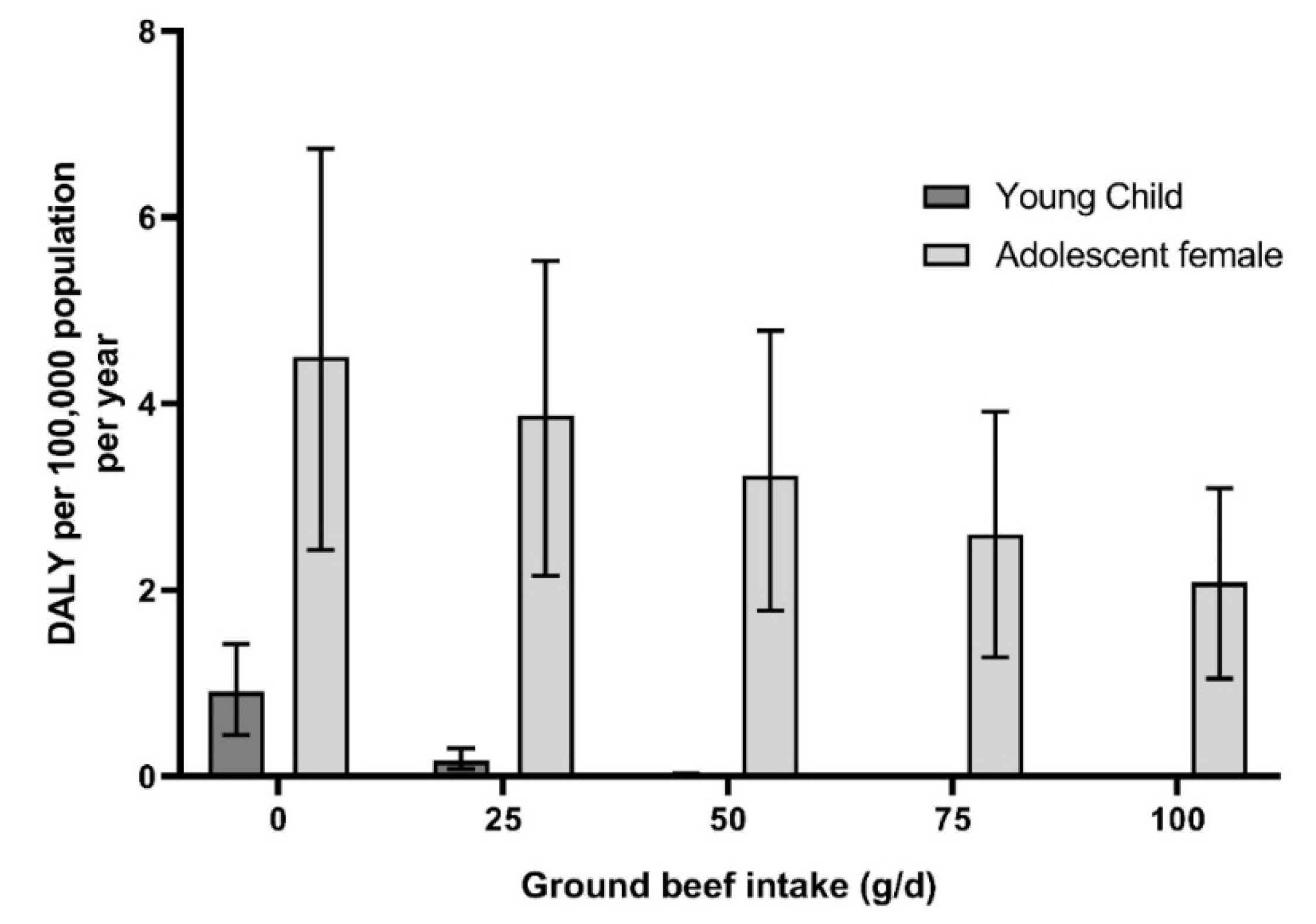
Based on the developed model, to estimate the effect of red meat intake on IDA burden of diseases, a consumption scenario for young children (three to six), older adolescent females (15–17), males (25–44; ≥60), adults menstruating females (≥18) and menstruated females (65–74) was generated. The results for young children and older adolescent females are presented in
Figure 2 and results for adult females are reported in
Figure 3.
For young children, the consumption of 50 g/d of ground beef, added to the iron consumption from other sources of iron without red meat, in current diet, would be enough to reduce the prevalence of ID to 0.2% (95% CI = 0%–1.9%) per 100,000 individuals per year and to decrease the burden of IDA close to zero DALY. For older adolescent females, the consumption of 100 g/d of red meat—which may represent a portion of red meat per day—added to the other sources of iron in current diet, would not be enough to eliminate ID and IDA. However, it would reduce the prevalence of ID to 22% (95% CI = 0%–90%) per 100,000 individuals per year and halve IDA burden when comparing with current consumption (mean red meat consumption of 18.2 g/d).
The burden of IDA in male adults was already low, but the consumption of 50 g/d or 100 g/d of red meat, in addition to the other sources of iron in current diet (without red meat), would decrease the current number of DALY from 0.8 [95% CI = 0.3–1.4] and 0.2 [95% CI = 0.1–0.4] per 100,000 individuals per year, respectively.
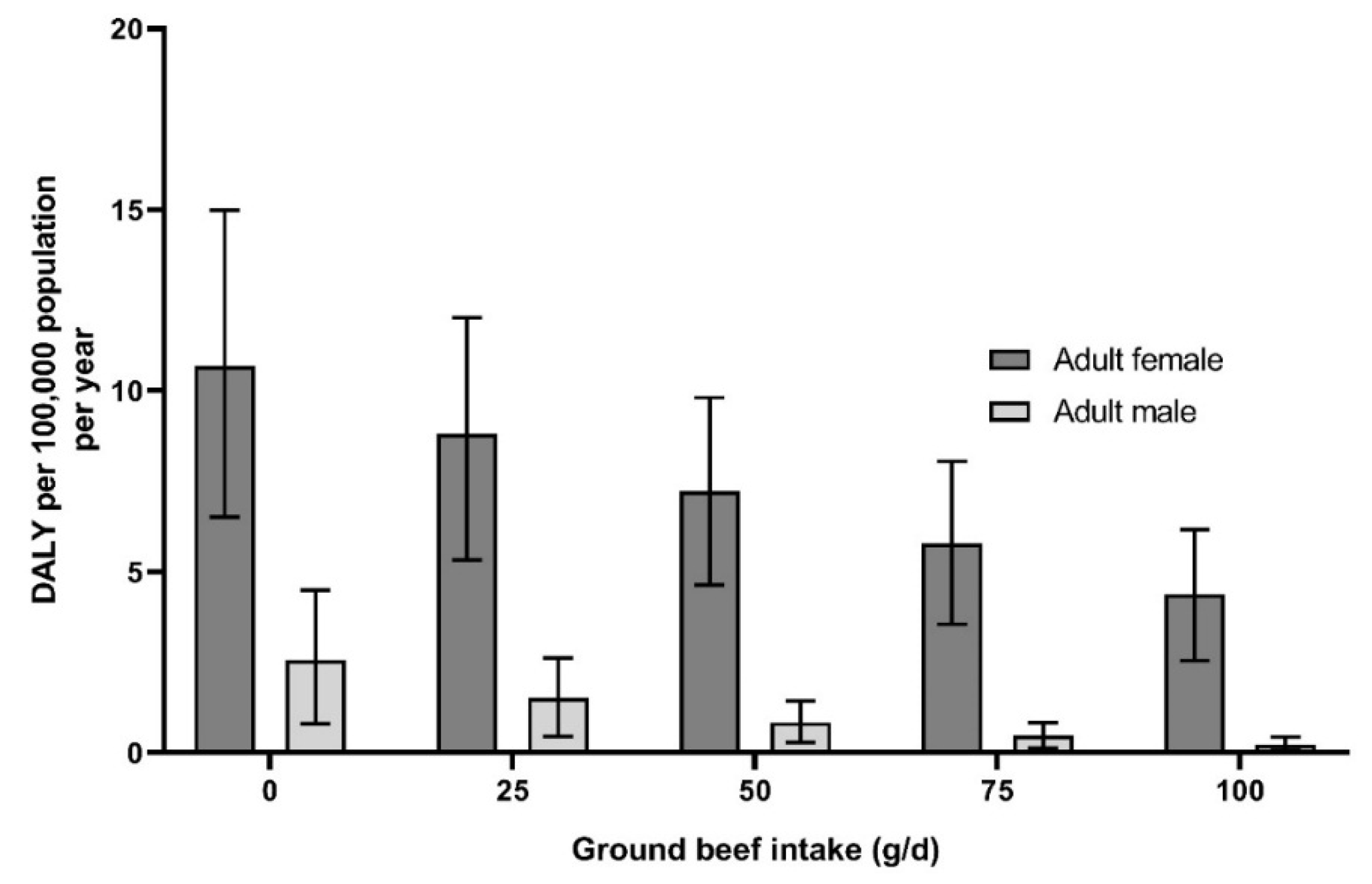
The burden of IDA in adult females aged over 18, were the highest in the population, especially for menstruating females (
Figure 3). The consumption of 50 g/d or 100 g/d of red meat, in addition to the other sources of iron in current diet (without red meat) would decrease the current number of DALY down to 7.2 (95% CI = 4.6–9.8) and 4.4 (95% CI = 2.5–6.2) per 100,000 individuals per year, respectively.
4. Discussion
The present study objective was to build an original probabilistic assessment model to estimate the burden of diseases associated with ID and subsequently IDA with the current iron consumption. A probabilistic risk assessment model was developed to estimate the prevalence of iron deficiencies, the number of cases and DALY in France from iron consumption.
Our results were in line with a previous study in France, from 2001, especially for young children [
25]. According to the study, 13.6% of young children aged from two to six were iron-deficient, which is not far from our estimations where 9% (95% CI = 6%–12%) of young boys and 9% (95% CI = 7%–13%) of young girls were iron-deficient. However, there is a missing population in this comparison. Due to the lack of consumption data, our estimations only included children aged from three to six. This estimation was also in line with iron deficiencies prevalence in Europe estimated between 7% and 18% for toddlers and young children [
32]. On the other hand, these results were higher than those found in France in a more recent study which found 3.2% (95% CI = 2.0%–5.1%) [
33], although the threshold for ID definition in this study was low with 10 or 12 µg/L—corresponding to the total depletion of iron storage. Indeed, the definition of ID was not the same because, with the data available, it was not possible to quantify the total depletion of iron, but the iron under the average requirement. For adolescents, it was estimated 15% (95% CI = 13%–18%) ID prevalence for males aged from 12 to 17 years old and 21% (95% CI = 17%–25%) and 44% (95% CI = 41%–47%) ID prevalence for adolescent females aged from 12 to 14 and from 15 to 17, respectively. This was in line with the estimations in Europe (between 0% and 43%) but was higher than iron deficiencies estimated for French adolescents (0% for males aged from 14 to 18, 3.1% for females aged from 11 to 15 and 15.4% for females aged from 14 to 18) [
24]. Nonetheless comparison was hard to establish because age classes were not the same as those in this study, the data were from 1988 and the definition of ID threshold was not the same [
34]. For the adult population, the most concerned with ID were menstruating adult females. This is mainly because iron losses are higher than for males and menopausal females, then, iron needs are higher for menstruating females (1.41 mg/day) compared to other adults’ needs (0.97 mg/day). In addition, iron consumption by adult menstruating females (mean 11 mg/d, sd 4 mg/d) was lower than by adult males (mean 14 mg/d, sd 5 mg/d). The values estimated in our study were similar to those measured in blood of French adults in ENNS study (for serum ferritin ≤30 µg/L) [
35].
The estimated number of IDA cases was 1290 (95% CI = 1130–1350) IDA per 100,000 individuals per year (
Table 4) with 584 (95% CI = 558–612) cases per 100,000 people for adult women per year. This corresponded to 797,200 (95% CI = 759,900–836,900) for the French population per year. The major contributors were menstruating females aged from 15 to 17. Indeed, twenty-two percent of older adolescent females were identified with IDA in our study, which was higher than the results found in 1994 in France (7.4% for adolescents aged from 14 to 18) [
24,
34]. The relevance of this comparison is somewhat questionable as there is a substantial time difference between the two studies: 2007 versus 1994. For adult females, it was estimated 1.7% (95% CI = 1.6%–1.8%) of IDA in France which was lower than results obtained in the SUpplementation en VItamines et Minéraux AntioXydants (SU.VI.MAX) study (4.4%) [
36]. However, the latter study only included individuals aged from 35 to 60 years old.
To go further than the estimation of the prevalence and the number of cases, we have taken into account morbidity with the use of the composite metric DALY [
37,
38], which is the most used in risk and benefit assessment studies [
30,
39]. Here, only morbidity was considered, because there is no existing data about IDA fatalities in France. Three levels of IDA severity were taken into account: Mild, moderate, and severe. The sequelae (
Table 2) of the different levels of IDA were assumed to be the same whatever the sub-population, and were based on the health status definitions from the GBD study [
29]. This assumption may induce an underestimation of the IDA burden for children and adolescents. Indeed, GBD health status does not take into account possible disabilities such as neurodevelopment delay due to ID and IDA which may induce impaired learning abilities, memory skills, and behavioral issues [
40,
41]. The majority of the studies evaluating the beneficial effect of iron supplementation were carried out in children under three years old. However, this age is considered under our first age class. After this age, some studies found a beneficial effect of iron treatment in older anemic children on intelligence quotient, but not in non-anemic [
42]. Moreover, there was no improvement in other disabilities, such as academic achievement, memory, or motor development [
42]. Therefore, experts remain cautious about these conclusions and more studies are needed to conclude about this effect. The estimated DALY of IDA cases was 16 (95% CI = 11–20) per 100,000 people per year (
Table 4) which corresponds to 9580 (95% CI = 7050–12,250) DALY for the French population per year. These values were lower than, but of the same order of magnitude as the estimation by GBD’s study which reported 35 DALY per 100,000 French population in 2007 [
43]. The major contributors to the burden were females aged from 25 to 44 and no longer adolescent girls aged from 15 to 17. This was due to the higher prevalence of moderate and severe anemia cases in the adult age class. However, our estimations were underestimated because children under three years old and pregnant females, which are particularly vulnerable populations, were excluded from the study [
4,
5].
The quantification of variability and uncertainties, as recommended by international organizations [
44], took into account the fitted distribution of iron intake and disability weight. For the first input cited, uncertainty and variability were quantified separately. However, for the second input cited, this separation was not possible. Even if some classify it as only variability [
45]—the confidence interval representing the variability of the severity of the disability—we decided to classify it as only uncertainty as done by the majority of the previous studies [
46,
47]. The variability of the iron needs and hemoglobin status were also taken into account in the study.
Nonetheless, despite the inherent uncertainty and variability described above, the results obtained in this study can be interpreted as showing that some differences in the burden of disease were observed, such as between males and females, or between menopausal and menstruating females.
The use of DALY metric also enabled to make consumption scenarios for concerned populations. Due to the richest source of heme-iron—which is the form of iron most absorbable by humans—brought by red meat consumption [
11], ground beef was taken as a food item in intake scenarios. In addition, consumption of red meat was found to increase the level of serum ferritin in the blood [
12,
13]. It was estimated that for young children, 50 g/d of ground beef—corresponding to 1.3 mg of iron—added to the other sources of iron already present in current diet (without red meat), would be enough to almost eliminate the IDA burden. For females aged over 15 years old and adult males, the consumption of 100 g/d of ground beef—corresponding to 2.6 mg of iron—added to the other sources of iron already present in current diet (without red meat) would not be enough to eliminate IDA burden (
Figure 2;
Figure 3). These results were in line with French Pediatric Society recommendations of eating 100–150 g/d of meat for children under six years old who stopped increasing milk consumption and twice a day by children over seven years and adolescents [
10], since beef meat, which has the highest level of heme-iron, is not the only meat consumed. The amount required to suppress IDA for adults is above the French Agency for Food, Environmental and Occupational Health and Safety (ANSES) recommendations, especially for adult women, which is to consume less than 500 g per week of red meat [
48]. This recommendation was largely based on the conclusions of the World Cancer Research Found/Imperial College of London and the WHO, which classified red meat as “probably carcinogenic to humans” for colorectal cancer [
49,
50]. In addition, a recent study of our team determined that the consumption of over 65 g/d of red meat would increase the risk of cardiovascular disease for the most concerned populations (adult population, especially elderly) [
51]. Indeed, heme-iron, is suspected to be the main component in the mechanism associated with colorectal cancer [
52,
53] and cardiovascular disease [
54,
55,
56]. These latter health effects were not considered to be of concern for children and adolescents for whom current epidemiological data were available [
57], but more studies and meta-analysis are needed to confirm this lack of association.
Furthermore, the intake scenario in this study does not consider the substitution and the acceptability of red meat. Indeed, when the individual increases the consumption of one food item, he/she may reduce the consumption of other foods. In addition, some population group will not accept to consume more red meat due to organoleptic reasons, beliefs, or ethics (e.g., vegetarian diet). In these cases, other sources of iron can be considered to reduce ID and IDA. The consumption of iron-rich sources such as white beans (7.97 mg of iron per 100 g), breakfast cereals (7.03 mg of iron per 100 g), or lentils (6.51 mg of iron per 100 g) [
31] would be a possible solution, especially for adult populations with a risk of colorectal and cardiovascular disease. Nevertheless, the quantity consumed of these other sources of iron, which are in form of non heme-iron, should be higher than that needed for red meat, because the degree of absorption is lower than for heme-iron products. Otherwise, some other heme-iron containing products, such as fish and poultry have a lower proportion of iron in the food compared to red meat. Some studies show that the vegetarian and vegan population presented a higher risk of iron deficiencies [
58,
59,
60]. However, there are large variations of non heme-iron absorption (0.7%–22.9%). Indeed, when blood levels had low serum and plasma ferritin concentrations, the absorption of iron increased [
61]. In addition, dietary enhancers (e.g., ascorbic acid, alcohol) and inhibitors (e.g., calcium, tannins, and polyphenols) influence the absorption of non heme-iron [
62].
Another possible solution for ID decrease is iron supplementation. It was observed that early iron supplementation of low birth weight infants would reduce the prevalence of behavioral problems and linear growth [
3]. Another study showed that iron supplementation with vitamin C of IDA children aged from 6 to 12 in Turkey, increased the intelligence quotient by 4.8 points [
63]. It was shown to improve learning and memory in non-anemic ID adolescent girls, in adults with IDA, and that iron supplementation can partially reverse the effects on cognitive performance.