Correction: Roncoroni, L. et al. A Low FODMAP Gluten-Free Diet Improves Functional Gastrointestinal Disorders and Overall Mental Health of Celiac Disease Patients: A Randomized Controlled Trial. Nutrients 2018, 10, 1023
Reference
- Roncoroni, L.; Bascuñán, K.A.; Doneda, L.; Scricciolo, A.; Lombardo, V.; Branchi, F.; Ferretti, F.; Dell’osso, B.; Montanari, V.; Bardella, M.T.; et al. A low FODMAP gluten-free diet improves functional gastrointestinal disorders and overall mental health of celiac disease patients: A randomized controlled trial. Nutrients 2018, 10, 8. [Google Scholar] [CrossRef] [PubMed]
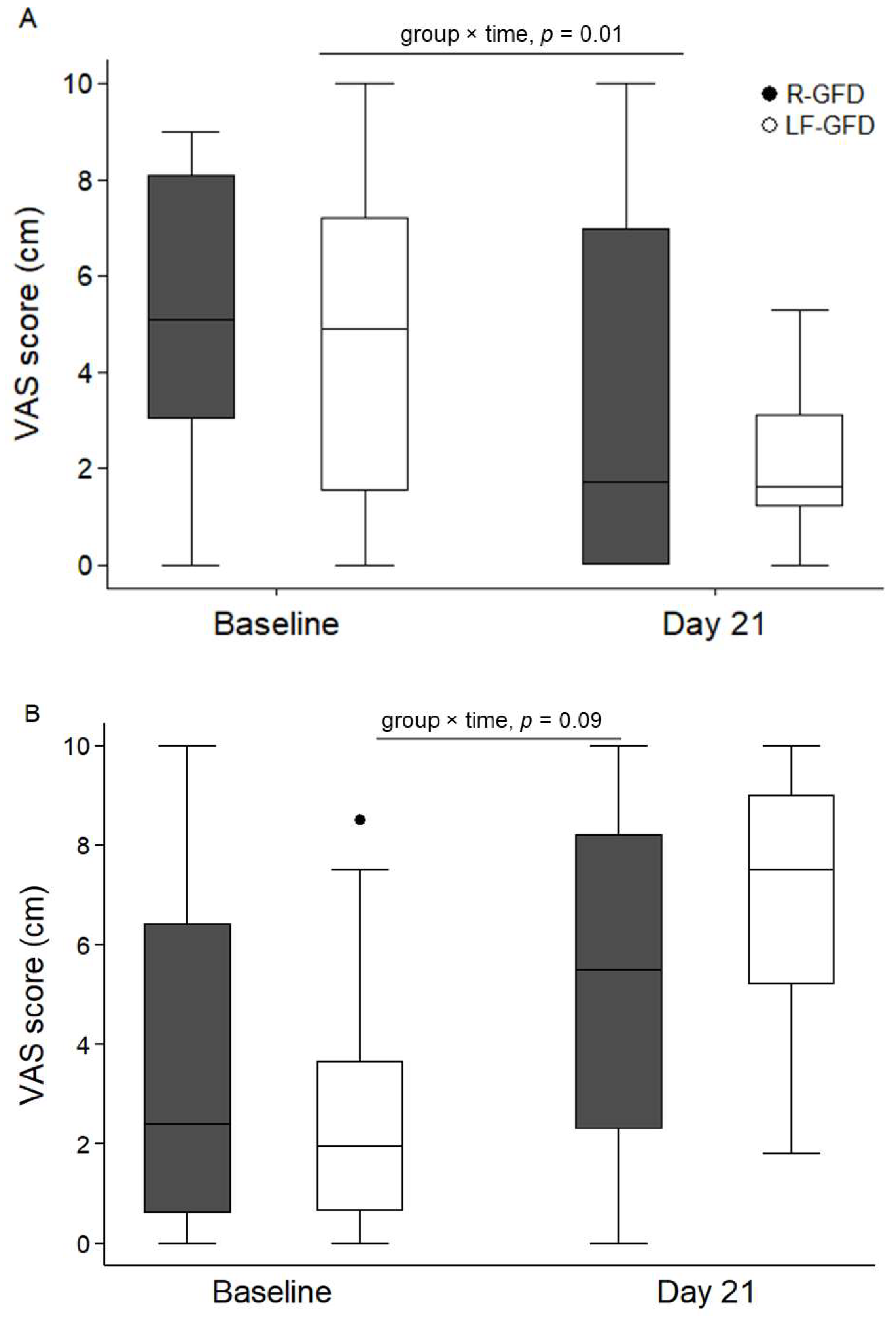
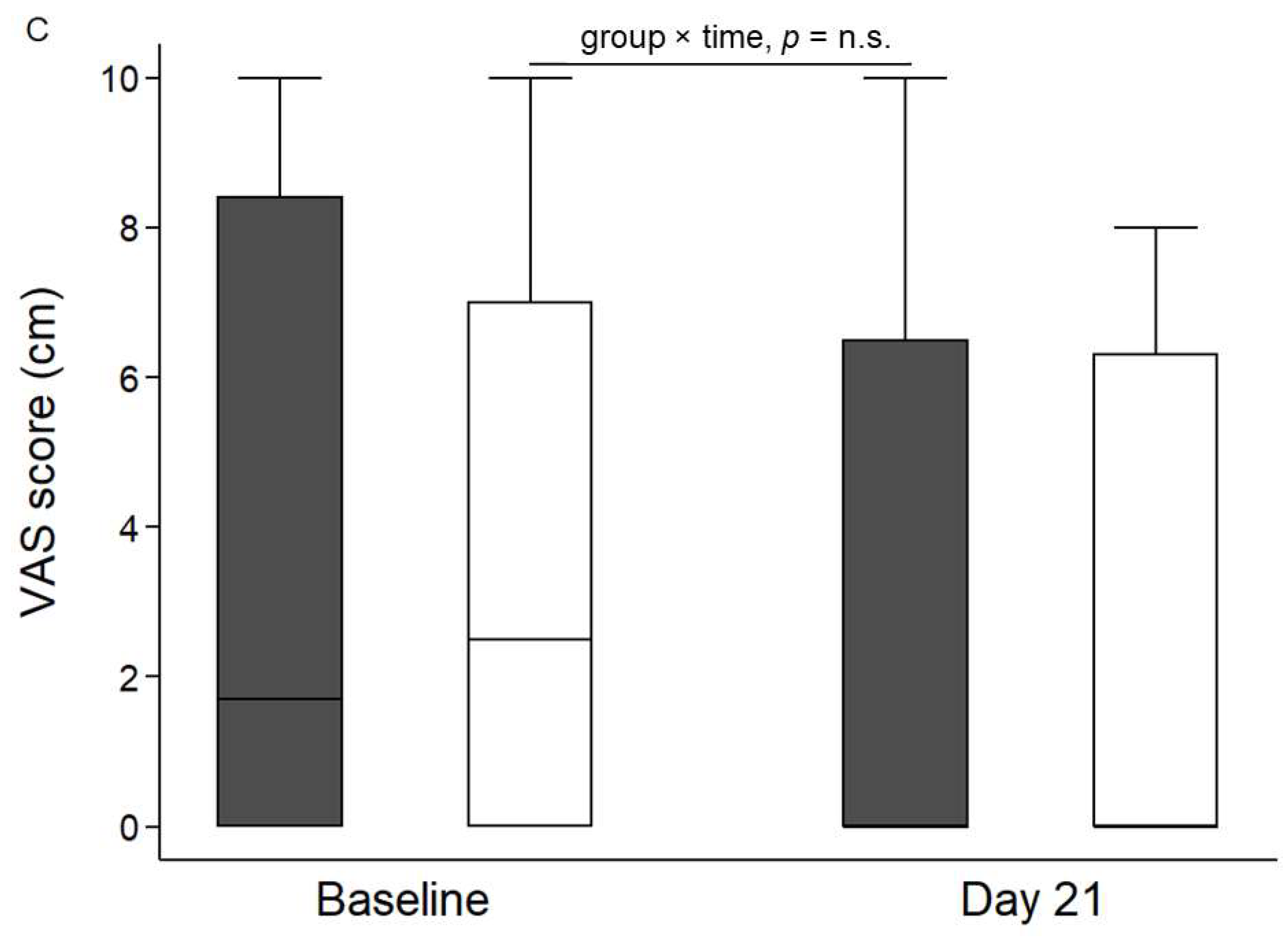
| Variable | Overall (n = 50) | R-GFD (n = 25) | LF-GFD (n = 25) | p Value † |
|---|---|---|---|---|
| Age, years | 41.1 ± 10.1 | 40.4 ± 10.1 | 41.9 ± 10.2 | 0.73 |
| Gender, female (%) | 44 (88) | 25 (100) | 22 (88) | 0.09 |
| BMI, kg/m2 | 22.5 ± 4.1 | 22.3 ± 3.6 | 22.1 ± 5.4 | 0.87 |
| Diarrhea, n (%) | 17 (34) | 6 (24) | 11 (44) | 0.18 |
| Constipation, n (%) | 16 (32) | 9 (36) | 7 (28) | 0.2 |
| Mixed symptoms, n (%) | 6 (12) | 4 (16) | 2 (8) | 0.36 |
| Non-specified, n (%) | 4 (8) | 3 (12) | 1 (4) | 0.29 |
| Dyspepsia, n (%) | 17 (34) | 8 (32) | 9 (36) | 0.95 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Roncoroni, L.; Bascuñán, K.A.; Doneda, L.; Scricciolo, A.; Lombardo, V.; Branchi, F.; Ferretti, F.; Dell’Osso, B.; Montanari, V.; Bardella, M.T.; et al. Correction: Roncoroni, L. et al. A Low FODMAP Gluten-Free Diet Improves Functional Gastrointestinal Disorders and Overall Mental Health of Celiac Disease Patients: A Randomized Controlled Trial. Nutrients 2018, 10, 1023. Nutrients 2019, 11, 566. https://doi.org/10.3390/nu11030566
Roncoroni L, Bascuñán KA, Doneda L, Scricciolo A, Lombardo V, Branchi F, Ferretti F, Dell’Osso B, Montanari V, Bardella MT, et al. Correction: Roncoroni, L. et al. A Low FODMAP Gluten-Free Diet Improves Functional Gastrointestinal Disorders and Overall Mental Health of Celiac Disease Patients: A Randomized Controlled Trial. Nutrients 2018, 10, 1023. Nutrients. 2019; 11(3):566. https://doi.org/10.3390/nu11030566
Chicago/Turabian StyleRoncoroni, Leda, Karla A. Bascuñán, Luisa Doneda, Alice Scricciolo, Vincenza Lombardo, Federica Branchi, Francesca Ferretti, Bernardo Dell’Osso, Valeria Montanari, Maria Teresa Bardella, and et al. 2019. "Correction: Roncoroni, L. et al. A Low FODMAP Gluten-Free Diet Improves Functional Gastrointestinal Disorders and Overall Mental Health of Celiac Disease Patients: A Randomized Controlled Trial. Nutrients 2018, 10, 1023" Nutrients 11, no. 3: 566. https://doi.org/10.3390/nu11030566
APA StyleRoncoroni, L., Bascuñán, K. A., Doneda, L., Scricciolo, A., Lombardo, V., Branchi, F., Ferretti, F., Dell’Osso, B., Montanari, V., Bardella, M. T., & Elli, L. (2019). Correction: Roncoroni, L. et al. A Low FODMAP Gluten-Free Diet Improves Functional Gastrointestinal Disorders and Overall Mental Health of Celiac Disease Patients: A Randomized Controlled Trial. Nutrients 2018, 10, 1023. Nutrients, 11(3), 566. https://doi.org/10.3390/nu11030566





