Breakfast in Canada: Prevalence of Consumption, Contribution to Nutrient and Food Group Intakes, and Variability across Tertiles of Daily Diet Quality. A Study from the International Breakfast Research Initiative
Abstract
:1. Introduction
- (1)
- To describe the context and prevalence of breakfast consumption in Canada;
- (2)
- To compare daily energy and nutrient intakes of breakfast consumers and non-consumers;
- (3)
- To describe the composition of breakfast and its contribution to daily nutrient intake and intake from key food groups; and
- (4)
- Among breakfast consumers, to compare energy, nutrient, and food group intakes at breakfast by tertiles of daily dietary quality.
2. Materials and Methods
2.1. Data Source and Analytical Sample
2.2. Dietary Quality
2.3. Food Group Intakes
2.4. Statistical Analysis
2.4.1. Prevalence and Context of Breakfast Consumption
2.4.2. Daily Energy and Nutrient Intakes of Breakfast Consumers and Non-Consumers
2.4.3. Breakfast Composition and Contribution of Breakfast to Daily Nutrient and Food Group Intake
2.4.4. Comparison of Energy, Nutrient, and Food Group Intakes at Breakfast by Tertiles of Daily Dietary Quality
3. Results
3.1. Prevalence and Context of Breakfast Consumption
3.2. Daily Intakes of Breakfast Consumers and Non-Consumers
3.3. Composition of Breakfast and Contribution of Breakfast to Daily Nutrient and Food Group Intakes
3.3.1. Energy and Nutrient Intakes at Breakfast
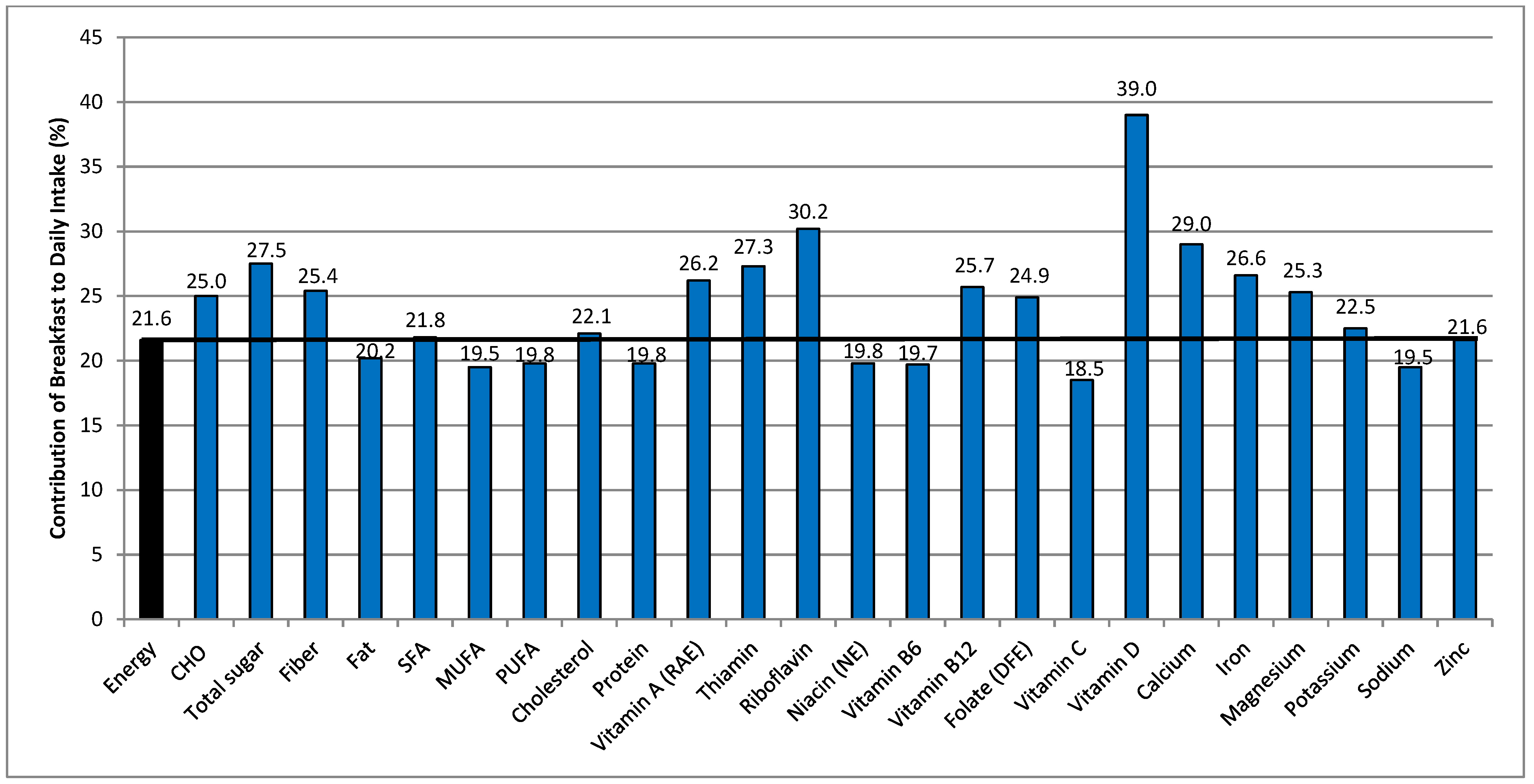
3.3.2. Contribution of Breakfast to Daily Nutrient Intakes
3.3.3. Contribution of Breakfast to Daily Food Group Intakes
3.3.4. Contribution of Breakfast to Daily Food Group Intakes
3.4. Energy, Nutrient, and Food Group Intakes at Breakfast by Tertiles of Daily Dietary Quality
4. Discussion
4.1. Prevalence and Context of Breakfast Consumption
4.2. Daily Intakes of Breakfast Consumers and Non-Consumers
4.3. Composition of Breakfast and Contribution of Breakfast to Daily Nutrient and Food Group Intakes
4.4. Energy, Nutrient, and Food Group Intakes at Breakfast by Tertiles of Daily Dietary Quality
4.5. Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Belloc, N.B.; Breslow, L. Relationship of physical health status and health practices. Prev. Med. 1972, 1, 409–421. [Google Scholar] [CrossRef]
- Gibney, M.J.; Barr, S.I.; Bellisle, F.; Drewnowski, A.; Fagt, S.; Livingstone, B.; Masset, G.; Varela Moreiras, G.; Moreno, L.A.; Smith, J.; et al. Breakfast in human nutrition: The International Breakfast Research Initiative. Nutrients 2018, 10, 559. [Google Scholar] [CrossRef] [PubMed]
- O’Neil, C.E.; Byrd-Bredbenner, C.; Hayes, D.; Jana, L.; Klinger, S.E.; Stephenson-Martin, S. The role of breakfast in health: Definition and criteria for a quality breakfast. J. Acad. Nutr. Diet. 2014, 114, S8–S26. [Google Scholar] [CrossRef] [PubMed]
- Barr, S.I.; DiFrancesco, L.; Fulgoni, V.L., III. Consumption of breakfast and the type of breakfast consumed are positively associated with nutrient intakes and adequacy of Canadian adults. J. Nutr. 2013, 143, 86–92. [Google Scholar] [CrossRef] [PubMed]
- Barr, S.I.; DiFrancesco, L.; Fulgoni, V.L., III. Breakfast consumption is positively associated with nutrient adequacy in Canadian children and adolescents. Br. J. Nutr. 2014, 112, 1373–1383. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- O’Neil, C.E.; Nicklas, T.A.; Fulgoni, V.L., III. Nutrient intake, diet quality, and weight measures in breakfast patterns consumed by children compared with breakfast skippers: NHANES 2001–2008. AIMS Public Health 2015, 2, 441–468. [Google Scholar] [CrossRef] [PubMed]
- O’Neil, C.E.; Nicklas, T.A.; Fulgoni, V.L. Nutrient intake, diet quality, and weight/adiposity parameters in breakfast patterns compared with no breakfast in adults: National Health and Nutrition Examination Survey 2001–2008. J. Acad. Nutr. Diet. 2014, 114, S27–S43. [Google Scholar] [CrossRef] [PubMed]
- Siega-Riz, A.M.; Popkin, B.M.; Carson, T. Differences in food patterns at breakfast by sociodemographic characteristics among a nationally representative sample of adults in the United States. Prev. Med. 2000, 30, 415–424. [Google Scholar] [CrossRef] [PubMed]
- Vereecken, C.; Dupuy, M.; Rasmussen, M.; Kelly, C.; Nansel, T.R.; Al Sabbah, H.; Baldassari, D.; Jordan, M.D.; Maes, L.; Niclasen, B.V.; et al. HBSC Eating & Dieting Focus Group. Breakfast consumption and its socio-demographic and lifestyle correlates in schoolchildren in 41 countries participating in the HBSC study. Int. J. Public Health 2009, 54 (Suppl. 2), 180–190. [Google Scholar] [CrossRef] [PubMed]
- Adolphus, K.; Lawton, C.L.; Champ, C.L.; Dye, L. The effects of breakfast and breakfast composition on cognition in children and adolescents: A systematic review. Adv. Nutr. 2016, 7, 590S–612S. [Google Scholar] [CrossRef] [PubMed]
- Brown, A.W.; Bohan Brown, M.M.; Allison, D.B. Belief beyond the evidence: Using the proposed effect of breakfast on obesity to show 2 practices that distort scientific evidence. Am. J. Clin. Nutr. 2013, 98, 1298–1308. [Google Scholar] [CrossRef] [PubMed]
- Cahill, L.E.; Chiuve, S.E.; Mekary, R.A.; Jensen, M.J.; Flint, A.J.; Hu, F.B.; Rimm, E.B. Prospective study of breakfast eating and incident coronary heart disease in a cohort of male U.S. health professionals. Circulation 2013, 128, 337–343. [Google Scholar] [CrossRef] [PubMed]
- Galioto, R.; Spitznagel, M.B. The effects of breakfast and breakfast composition on cognition in adults. Adv. Nutr. 2016, 7, 576S–589S. [Google Scholar] [CrossRef] [PubMed]
- Leidy, H.J.; Gwin, J.A.; Roenfeldt, C.A.; Zino, A.Z.; Shafer, R.S. Evaluating the intervention-based evidence surrounding the causal role of breakfast on markers of weight management, with specific focus on breakfast composition and size. Adv. Nutr. 2016, 7, 563S–575S. [Google Scholar] [CrossRef] [PubMed]
- Maki, K.C.; Phillips-Eakley, A.K.; Smith, K.N. The effects of breakfast consumption and composition on metabolic wellness with a focus on carbohydrate metabolism. Adv. Nutr. 2016, 7, 613S–621S. [Google Scholar] [CrossRef] [PubMed]
- Rosato, V.; Edefonti, V.; Parpinel, M.; Milani, G.P.; Mazzocchi, A.; Decarli, A.; Agostoni, C.; Ferraroni, M. Energy contribution and nutrient composition of breakfast and their relations to overweight in free-living individuals: A systematic review. Adv. Nutr. 2016, 7, 455–465. [Google Scholar] [CrossRef] [PubMed]
- St-Onge, M.P.; Ard, J.; Baskin, M.L.; Chiuve, S.E.; Johnson, H.M.; Kris-Etherton, P.; Varady, K.; American Heart Association Obesity Committee of the Council on Lifestyle and Cardiometabolic Health; Council on Cardiovascular Disease in the Young; Council on Clinical Cardiology; Stroke Council. Meal timing and frequency: Implications for cardiovascular disease prevention: A Scientific Statement from the American Heart Association. Circulation 2017, 135, e96–e121. [Google Scholar] [CrossRef] [PubMed]
- Health Canada. Canadian Community Health Survey, Cycle 2.2, Nutrition (2004): A Guide to Accessing and Interpreting the Data. 2006. Available online: https://www.canada.ca/en/health-canada/services/food-nutrition/food-nutrition-surveillance/health-nutrition-surveys/canadian-community-health-survey-cchs/canadian-community-health-survey-cycle-2-2-nutrition-2004-guide-accessing-interpreting-data-health-canada-2006.html (accessed on 20 June 2018).
- 2015 Canadian Community Health Survey-Nutrition. Reference Guide to Understanding and Using the Data. 2017. Available online: https://www.canada.ca/en/health-canada/services/food-nutrition/food-nutrition-surveillance/health-nutrition-surveys/canadian-community-health-survey-cchs/reference-guide-understanding-using-data-2015.html (accessed on 20 June 2018).
- Statistics Canada. Canadian Community Health Survey-Nutrition (CCHS). 2017. Available online: http://www23.statcan.gc.ca/imdb/p2SV.pl?Function=getSurvey&SDDS=5049 (accessed on 20 June 2018).
- Raper, N.; Perloff, B.; Ingwersen, L.; Steinfeldt, L.; Anand, J. An overview of USDA's dietary intake data system. J. Food Comp. Anal. 2004, 17, 545–555. [Google Scholar] [CrossRef]
- Statistics Canada. The Research Data Centres (RDC) Program. 2017. Available online: http://www.statcan.gc.ca/eng/rdc/index (accessed on 20 June 2018).
- Fulgoni, V.L., III; Keast, D.R.; Drewnowski, A. Development and validation of the Nutrient-Rich Foods Index: A tool to measure nutritional quality of foods. J. Nutr. 2009, 139, 1549–1554. [Google Scholar] [CrossRef] [PubMed]
- Palacios, C.; Gonzalez, L. Is vitamin D deficiency a major global public health problem? J. Steroid Biochem. Mol. Biol. 2014, 144, 138–145. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Holick, M.F.; Chen, T.C. Vitamin D deficiency: A worldwide problem with health consequences. Am. J. Clin. Nutr. 2008, 87, 1080S–1086S. [Google Scholar] [CrossRef] [PubMed]
- Government of Canada. Table of Daily Values. 2016. Available online: https://www.canada.ca/en/health-canada/services/technical-documents-labelling-requirements/table-daily-values.html (accessed on 20 June 2018).
- Government of Canada. Canadian Nutrient File (CNF)–Search by Food. 2018. Available online: https://food-nutrition.canada.ca/cnf-fce/index-eng.jsp (accessed on 20 June 2018).
- Government of Canada. Dietary Reference Intakes. Reference Values for Macronutrients. 2006. Available online: https://www.canada.ca/en/health-canada/services/food-nutrition/healthy-eating/dietary-reference-intakes/tables/reference-values-macronutrients-dietary-reference-intakes-tables-2005.html (accessed on 20 June 2018).
- Health Canada. Eating Well with Canada’s Food Guide. 2011. Available online: http://www.hc-sc.gc.ca/fn-an/alt_formats/hpfb-dgpsa/pdf/food-guide-aliment/print_eatwell_bienmang-eng.pdf (accessed on 20 June 2018).
- Health Canada. The Development and Use of a Surveillance Tool: The Classification of Foods in the Canadian Nutrient File according to Eating Well with Canada’s Food Guide. 2014. Available online: http://publications.gc.ca/collections/collection_2014/sc-hc/H164-158-2-2014-eng.pdf (accessed on 20 June 2018).
- Statistics Canada. The Research Data Centres Information and Technical Bulletin—Weighted Estimation and Bootstrap Variance Estimation for Analyzing Survey Data: How to Implement in Selected Software. 2014. Available online: http://www5.statcan.gc.ca/olc-cel/olc?ObjId=12-002-X201400111901&ObjType=47&lang=en (accessed on 20 June 2018).
- Horrace, W.; Schmidt, P. Multiple comparisons with the best, with economic applications. J. Appl. Economet. 2000, 15, 1–26. [Google Scholar] [CrossRef] [Green Version]
- Sanou, D.; O’Reilly, E.; Ngnie-Teta, I.; Batal, M.; Mondain, N.; Andrew, C.; Newbold, B.K.; Bourgeault, I.L. Acculturation and nutritional health of immigrants in Canada: A scoping review. J. Immigr. Minor. Health 2014, 16, 24–34. [Google Scholar] [CrossRef] [PubMed]
- Coppolino, A. Trends in Breakfast and Brunch Foods. Foodservice and Hospitality. Available online: http://www.foodserviceandhospitality.com/trends-in-breakfast-and-brunch-foods/ (accessed on 20 June 2018).
- Health Canada. Do Canadian Adolescents Meet Their Nutrient Requirements through Food Intake Alone? Catalogue Number H164-112/2-2012E-PDF. Available online: https://www.canada.ca/en/health-canada/services/food-nutrition/food-nutrition-surveillance/health-nutrition-surveys/canadian-community-health-survey-cchs/canadian-adolescents-meet-their-nutrient-requirements-through-food-intake-alone-health-canada-2012.html (accessed on 20 June 2018).
- Weaver, C.M. The role of nutrition on optimizing peak bone mass. Asia Pac. J. Clin. Nutr. 2008, 17 (Suppl. 1), 135–137. [Google Scholar] [CrossRef] [PubMed]
- Raaijmakers, L.G.M.; Bessems, K.M.H.H.; Kremers, S.P.J.; Van Assema, A. Breakfast consumption among children and adolescents in the Netherlands. Eur. J. Pub. Health 2010, 20, 318–324. [Google Scholar] [CrossRef]
- Tee, E.S.; Nurliyana, A.R.; Norimah, A.K.; Mohamed, H.J.B.J.; Tan, S.Y.; Appukutty, M.; Hopkins, S.; Thielecke, F.; Ong, M.K.; Ning, C.; et al. Breakfast consumption among Malaysian primary and secondary school children and relationship with body weight status-Findings from the My Breakfast Study. Asia Pac. J. Clin. Nutr. 2018, 27, 421–432. [Google Scholar] [CrossRef] [PubMed]
- US Department of Agriculture, Agricultural Research Service. Breakfast: Percentages of Selected Nutrients Contributed by Foods Eaten at Breakfast, by Gender and age. What We Eat in America, NHANES 2009–2010. 2012. Available online: http://www.ars.usda.gov/SP2UserFiles/Place/12355000/pdf/0910/Table_1_NIN_GEN_09.pdf (accessed on 20 June 2018).
- Institute of Medicine. Dietary Reference Intakes for Calcium and Vitamin D; The National Academies Press: Washington, DC, USA, 2011; Available online: https://www.nap.edu/catalog/13050/dietary-reference-intakes-for-calcium-and-vitamin-d (accessed on 20 June 2018).
- Whiting, S.J.; Langlois, K.A.; Vatanparast, H.; Greene-Finestone, L.S. The vitamin D status of Canadians relative to the 2011 Dietary Reference Intakes: An examination in children and adults with and without supplement use. Am. J. Clin. Nutr. 2011, 94, 128–135. [Google Scholar] [CrossRef] [PubMed]
- Government of Canada. Summary of Proposed Amendments Published in Canada Gazette, Part I: Nutrition Symbols, Other Labelling Provisions, Partially Hydrogenated Oils and Vitamin D. 2018. Available online: https://www.canada.ca/en/health-canada/proy/consultation-front-of-package-nutrition-labelling-cgi/summary-of-proposed-amendments.html (accessed on 12 July 2018).
- Garriguet, D. Overview of Canadians’ Eating Habits. Catalogue No. 82-620-MIE–No. 2. 2004. Available online: http://publications.gc.ca/Collection/Statcan/82-620-M/82-620-MIE2006002.pdf (accessed on 20 June 2018).
- Vatanparast, H.; Whiting, S.; Hossai, A.; Mirhosseini, N.; Merchant, A.T.; Szafron, M. National pattern of grain products consumption among Canadians in association with body weight status. BMC Nutr. 2017, 3, 59. [Google Scholar] [CrossRef]
- Marmot, M. Social determinants of health inequalities. Lancet 2005, 365, 1099–1104. [Google Scholar] [CrossRef] [Green Version]
- National Institutes of Health. Dietary supplement label database. Labeling Daily Values. 2018. Available online: https://www.dsld.nlm.nih.gov/dsld/dailyvalue.jsp (accessed on 20 June 2018).
- European Union. Regulation (EU) No. 1169/2011 of the European Parliament and of the Council of 25 October 2011. Available online: https://eur-lex.europa.eu/legal-content/EN/TXT/PDF/?uri=CELEX:32011R1169&from=EN (accessed on 20 June 2018).
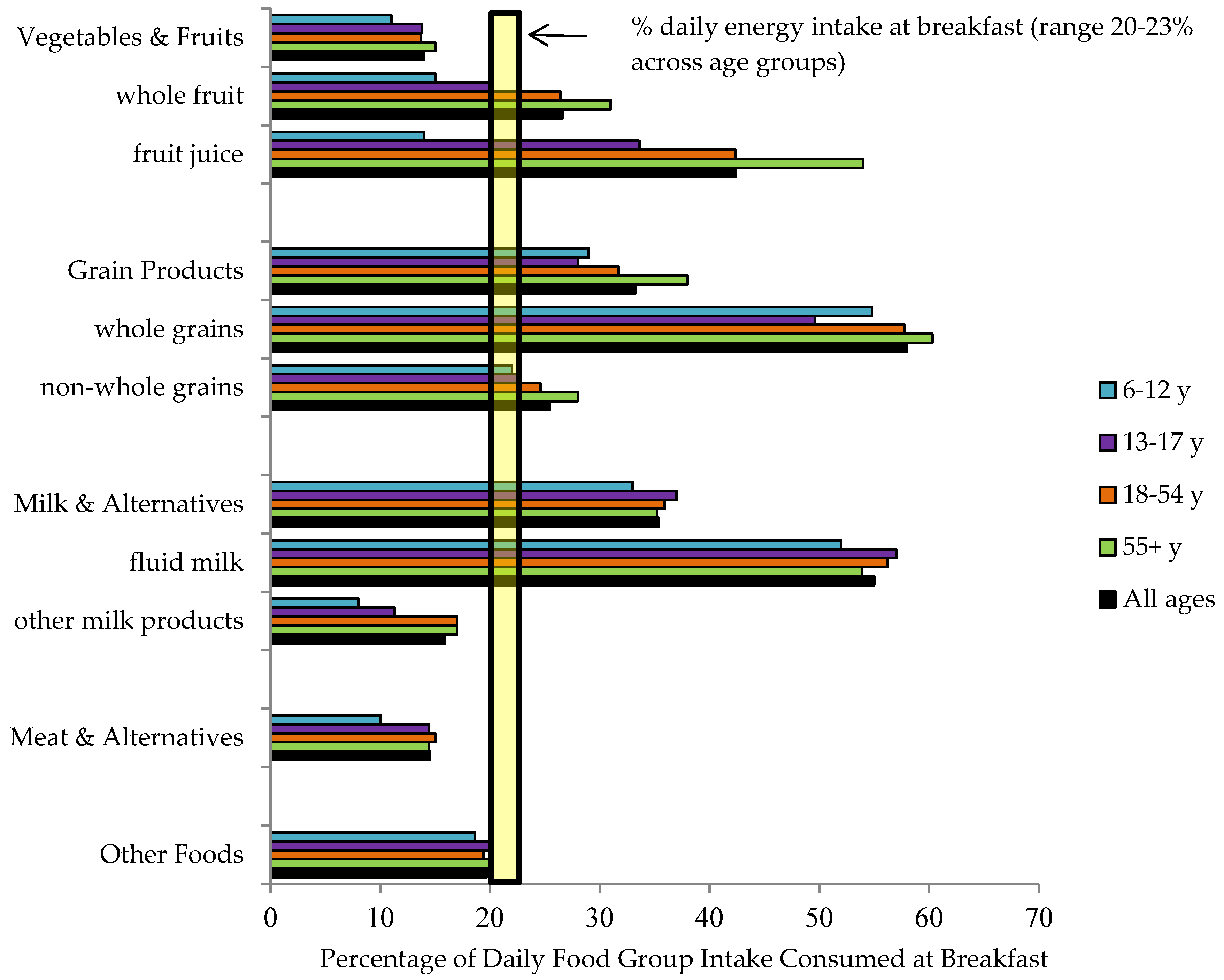
| Characteristic | Children/Teens (6–17 Years) | Adults (≥18 Years) | ||
|---|---|---|---|---|
| Breakfast (n = 3934) | No Breakfast (n = 423) | Breakfast (n = 12,550) | No Breakfast (n = 1380) | |
| Mean age (year) | 11.4 ± 0.06 | 13.9 ± 0.2 * | 49.7 ± 0.2 | 42.6 ± 0.9 * |
| Sex (% male) | 51.5 ± 1.0 | 47.3 ± 3.8 | 49.0 ± 0.3 | 58.2 ± 2.5 * |
| Ethnicity (% Caucasian) | 67.7 ± 1.4 | 65.8 ± 4.0 | 74.8 ± 1.0 | 74.1 ± 2.5 |
| Supplement use in past 30 day (% yes) | 36.6 ± 1.2 | 31.5 ± 4.4 | 48.1 ± 0.9 | 34.2 ± 2.4 * |
| Current smoker (% yes) 2 | 2.2 ± 0.4 | 7.6 ± 2.0 * | 16.5 ± 0.7 | 36.9 ± 2.6 * |
| Education (% university grad) 3 | 44.2 ± 1.5 | 31.6 ± 3.9 * | 39.4 ± 1.0 | 32.2 ± 2.7 * |
| Marital status (% married/cohabiting) | n/a | n/a | 65.2 ± 0.9 | 54.0 ± 2.8 * |
| Food secure (% yes) | 83.4 ± 1.0 | 80.8 ± 3.0 | 89.2 ± 0.5 | 82.8 ± 2.2 * |
| Body mass index (BMI; kg/m2) | n/a | n/a | 27.2 ± 0.1 | 28.0 ± 0.5 |
| BMI z-score for age and sex | 0.43 ± 0.04 | 0.54 ± 0.1 | n/a | n/a |
| Overweight/obese (% yes) 4 | 30.7 ± 1.3 | 39.0 ± 3.9 * | 60.9 ± 1.1 | 66.5 ± 3.2 |
| Urban residence (% yes) | 81.2 ± 1.2 | 80.0 ± 3.8 | 83.0 ± 0.8 | 79.5 ± 2.3 |
| Immigrant to Canada (% yes) | 10.4 ± 0.8 | 15.9 ± 3.5 | 28.3 ± 1.0 | 20.1 ± 2.2 * |
| Nutrient | All Ages | Children (6–12 Years) | Teens (13–17 Years) | Adults (18–54 Years) | Older Adults (55+ Years) | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| Breakfast (n = 16,484) | No Breakfast (n = 1803) | Breakfast (n = 2227) | No Breakfast (n = 104) | Breakfast (n = 1707) | No Breakfast (n = 319) | Breakfast (n = 6688) | No Breakfast (n = 963) | Breakfast (n = 5862) | No Breakfast (n = 417) | |
| Energy and Macronutrients | ||||||||||
| Energy (kcal) | 1896 ± 13 | 1760 ± 49 *** | 1854 ± 22 | 1661 ± 70 | 2102 ± 33 | 1791 ± 68 *** | 1980 ± 21 | 1801 ± 66 ** | 1740 ± 18 | 1649 ± 76 |
| CHO (g) | 231 ± 2 | 204 ± 5 *** | 256 ± 3 | 220 ± 11 *** | 275 ± 4 | 232 ± 11 | 234 ± 3 | 207 ± 7 ** | 211 ± 2 | 188 ± 9 ** |
| CHO (% energy) | 48.8 ± 0.2 | 46.8 ± 0.5 ** | 55.0 ± 0.3 | 53.2 ± 1.2 *** | 52.3 ± 0.4 | 50.9 ± 1.3 | 47.5 ± 0.3 | 46.6 ± 0.7 | 48.6 ± 0.2 | 45.3 ± 1.0 *** |
| Total sugars (g) | 91.1 ± 0.8 | 85.2 ± 3.2 | 113 ± 1.9 | 99.1 ± 7.0 | 118 ± 2.6 | 97.1 ± 6.6 | 89.8 ± 1.3 | 87.7 ± 4.3 | 82.8 ± 1.2 | 73.5 ± 4.6 * |
| Fiber (g) | 17.5 ± 0.2 | 12.1 ± 0.4 *** | 16.0 ± 0.2 | 11.2 ± 0.7 *** | 16.9 ± 0.3 | 12.7 ± 0.7 * | 17.8 ± 0.2 | 12.1 ± 0.4 *** | 17.6 ± 0.2 | 12.0 ± 0.8 *** |
| Fat (g) | 69.9 ± 0.7 | 66.6 ± 2.5 * | 64.0 ± 1.0 | 63.3 ± 3.5 *** | 76.8 ± 1.7 | 64.4 ± 3.0 | 74.2 ± 1.0 | 68.8 ± 3.5 * | 63.8 ± 1.0 | 61.5 ± 2.6 |
| Fat (% energy) | 31.9 ± 0.1 | 32.6 ± 0.4 | 30.1 ± 0.3 | 33.3 ± 1.2 *** | 31.6 ± 0.3 | 32.4 ± 1.1 | 32.5 ± 0.2 | 32.6 ± 0.6 | 31.5 ± 0.2 | 32.6 ± 0.9 |
| Saturates (g) | 23.0 ± 0.2 | 22.1 ± 0.9 | 23.1 ± 0.4 | 22.5 ± 1.9 | 26.6 ± 0.6 | 21.1 ± 1.2 | 24.0 ± 0.4 | 22.8 ± 1.2 | 20.8 ± 0.3 | 20.6 ± 1.3 |
| Monounsaturates (g) | 26.0 ± 0.3 | 25.2 ± 1.1 ** | 22.7 ± 0.4 | 22.7 ± 1.4 ** | 28.1 ± 0.7 | 24.0 ± 1.2 | 27.8 ± 0.4 | 26.3 ± 1.5 ** | 23.6 ± 0.4 | 22.8 ± 1.5 |
| Polyunsaturates (g) | 14.7 ± 0.2 | 13.4 ± 0.6 | 12.4 ± 0.3 | 12.5 ± 0.8 ** | 15.1 ± 0.4 | 13.5 ± 0.6 | 15.6 ± 0.3 | 13.8 ± 0.8 | 13.7 ± 0.2 | 12.5 ± 1.0 |
| Cholesterol (mg) | 266 ± 4 | 238 ± 12 | 211 ± 5 | 170 ± 15 | 270 ± 8 | 199 ± 16 * | 292 ± 7 | 252 ± 17 | 241 ± 4 | 217 ± 12 |
| Protein (g) | 79.2 ± 0.6 | 73.0 ± 2.3 | 69.0 ± 0.9 | 57.7 ± 3.2 | 83.4 ± 1.5 | 74.0 ± 6.9 | 85.2 ± 1.1 | 75.5 ± 3.2 | 71.7 ± 0.8 | 67.6 ± 3.0 |
| Protein (% energy) | 16.8 ± 0.1 | 16.7 ± 0.3 | 14.9 ± 0.1 | 13.5 ± 0.5 | 16.0 ± 0.2 | 16.6 ± 1.3 | 17.3 ± 0.1 | 16.8 ± 0.4 | 16.6 ± 0.1 | 17.1 ± 0.6 |
| Vitamins | ||||||||||
| Vitamin A (μg RAE) | 645 ± 9 | 553 ± 37 | 600 ± 20 | 402 ± 34 | 664 ± 18 | 548 ± 97 *** | 644 ± 13 | 567 ± 54 | 655 ± 15 | 530 ± 59 |
| Thiamin (mg) | 1.62 ± 0.01 | 1.32 ± 0.04 *** | 1.64 ± 0.03 | 1.27 ± 0.08 * | 1.83 ± 0.04 | 1.49 ± 0.10 ** | 1.68 ± 0.02 | 1.33 ± 0.05 | 1.49 ± 0.02 | 1.23 ± 0.07 ** |
| Riboflavin (mg) | 1.92 ± 0.01 | 1.70 ± 0.05 ** | 1.83 ± 0.03 | 1.39 ± 0.08 | 2.03 ± 0.04 | 1.51 ± 0.12 *** | 2.01 ± 0.02 | 1.73 ± 0.07 * | 1.80 ± 0.02 | 1.71 ± 0.08 |
| Niacin (mg NE) | 38.9 ± 0.3 | 36.6 ± 1.3 | 32.4 ± 0.4 | 26.9 ± 1.7 | 40.2 ± 0.8 | 37.6 ± 3.6 | 42.0 ± 0.6 | 38.3 ± 1.8 | 35.6 ± 0.4 | 32.5 ± 1.6 |
| Vitamin B6 (mg) | 1.67 ± 0.01 | 1.49 ± 0.06 | 1.40 ± 0.02 | 1.06 ± 0.09 | 1.67 ± 0.04 | 1.42 ± 0.16 ** | 1.78 ± 0.02 | 1.58 ± 0.08 | 1.57 ± 0.02 | 1.30 ± 0.09 |
| Vitamin B12 (μg) | 4.01 ± 0.06 | 3.99 ± 0.27 | 3.78 ± 0.19 | 2.68 ± 0.25 | 4.29 ± 0.14 | 2.90 ± 0.29 *** | 4.14 ± 0.09 | 4.20 ± 0.39 | 3.80 ± 0.09 | 3.88 ± 0.36 |
| Folate (μg DFE) | 450 ± 4 | 382 ± 12 *** | 446 ± 8 | 384 ± 29 | 492 ± 12 | 457 ± 44 | 478 ± 7 | 388 ± 14 *** | 400 ± 5 | 343 ± 22 * |
| Folic acid (μg) | 118 ± 2 | 106 ± 4 ** | 139 ± 3 | 123 ± 12 | 150 ± 5 | 148 ± 20 | 123 ± 3 | 104 ± 5) ** | 98 ± 2 | 96 ± 8 |
| Vitamin C (mg) | 103 ± 1.5 | 75 ± 5.8 *** | 117 ± 3.0 | 90.4 ± 13.5 *** | 119 ± 4.0 | 91.9 ± 12.4 * | 104 ± 2.6 | 78.3 ± 8.2 *** | 96.1 ± 2.1 | 60.4 ± 6.8 * |
| Vitamin D (μg) | 4.88 ± 0.07 | 3.98 ± 0.29 | 5.27 ± 0.12 | 3.97 ± 0.60 | 5.71 ± 0.18 | 4.17 ± 0.56 *** | 4.72 ± 0.11 | 3.65 ± 0.29 | 4.88 ± 0.11 | 4.82 ± 0.84 |
| Minerals and Electrolytes | ||||||||||
| Calcium (mg) | 818 ± 8 | 691 ± 30 | 936 ± 15 | 749 ± 50 | 1005 ± 22 | 771 ± 55 ** | 828 ± 12 | 705 ± 42 | 738 ± 10 | 623 ± 33 |
| Iron (mg) | 12.7 ± 0.1 | 10.1 0.3 *** | 12.6 ± 0.2 | 9.6 ± 0.6 *** | 13.8 ± 0.3 | 11.4 ± 1.0 *** | 13.0 ± 0.2 | 10.0 ± 0.3 *** | 11.9 ± 0.1 | 10.0 ± 0.6 |
| Magnesium (mg) | 308 ± 2 | 242 ± 7 *** | 254 ± 3 | 200 ± 11 ** | 297 ± 5 | 251 ± 24 ** | 322 ± 4 | 244 ± 8 *** | 302 ± 3 | 2399 ± 11 *** |
| Potassium (mg) | 2691 ± 19 | 2280 ± 63 ** | 2384 ± 30 | 1936 ± 123 | 2651 ± 45 | 2036 ± 120 *** | 2763 ± 30 | 2281 ± 73 ** | 2667 ± 27 | 2385 ± 146 |
| Sodium (mg) | 2751 ± 24 | 2556 ± 84 | 2586 ± 38 | 2283 ± 136 | 2993 ± 58 | 2455 ± 111 | 2904 ± 39 | 2646 ± 111 | 2513 ± 30 | 2372 ± 158 |
| Zinc (mg) | 10.5 ± 0.1 | 9.4 ± 0.3 | 9.1 ± 0.1 | 7.6 ± 0.5 | 10.9 ± 0.2 | 9.2 ± 0.8 * | 11.1 ± 0.2 | 9.6 ± 0.4 | 9.9 ± 0.2 | 9.3 ± 0.5 |
| Nutrient-Rich Foods (NRF) Index 9.3 Score 2 | ||||||||||
| NRF 9.3 | 524 ± 2 | 439 ± 7 *** | 516 ± 4 | 424 ± 16 * | 499 ± 4 | 429 ± 16 *** | 515 ± 3 | 433 ± 9 *** | 546 ± 3 | 463 ± 17 |
| Nutrient | All 6+ Years (n = 16,484) | Children 6–12 Years (n = 2227) | Teens 13–17 Years (n = 1707) | Adults 18–54 Years (n = 6688) | Adults 55+ Years (n = 5862) | p |
|---|---|---|---|---|---|---|
| Energy (kcal) | 389 ± 5 | 356 ± 8 L | 421 ± 10 H | 401 ± 8 | 374 ± 6 | <0.001 |
| CHO (g) | 54.6 ± 0.6 | 53.8 ± 1.2 L | 59.7 ± 1.5 H | 54.2 ± 1.0 | 54.5 ± 0.8 | <0.001 |
| (% energy) | 57.8 ± 0.3 | 60.8 ± 0.5 H | 58.6 ± 0.7 | 56.4 ± 0.5 L | 59.0 ± 0.4 | <0.001 |
| Total sugars (g) | 23.0 ± 0.3 | 24.9 ± 0.7 | 27.0 ± 0.8 H | 22.9 ± 0.6 | 22.0 ± 0.4 L | <0.001 |
| (% energy) | 26.4 ± 0.03 | 29.5 ± 0.1 H | 27.9 ± 0.1 | 26.1 ± 0.1 | 25.7 ± 0.1 L | <0.001 |
| Fiber (g) | 4.4 ± 0.1 | 3.4 ± 0.1 L | 3.8 ± 0.1 | 4.3 ± 0.1 | 4.9 ± 0.1 H | <0.001 |
| Fat (g) | 13.4 ± 0.3 | 10.6 ± 0.4 L | 14.1 ± 0.6 | 14.4 ± 0.5 H | 12.4 ± 0.4 | <0.001 |
| (% energy) | 27.3 ± 0.3 | 25 ± 0.5 L | 26.9 ± 0.6 | 28.2 ± 0.4 H | 26.5 ± 0.4 | <0.001 |
| Saturates (g) | 4.7 ± 0.1 | 4.3 ± 0.2 | 5.5 ± 0.2 H | 5.0 ± 0.2 | 4.2 ± 0.1 L | <0.001 |
| (% energy) | 9.9 ± 0.1 | 10.3 ± 0.2 | 10.4 ± 0.3 H | 10.1 ± 0.2 | 9.4 ± 0.2 L | 0.002 |
| Monounsaturates (g) | 4.9 ± 0.1 | 3.6 ± 0.1 L | 5.0 ± 0.2 | 5.3 ± 0.2 H | 4.4 ± 0.2 | <0.001 |
| Polyunsaturates (g) | 2.7 ± 0.1 | 1.8 ± 0.1 L | 2.6 ± 0.2 | 2.8 ± 0.1 H | 2.7 ± 0.1 | <0.001 |
| Cholesterol (mg) | 77.4 ± 2.7 | 50.7 ± 3.1 L | 81.4 ± 6.6 | 90.0 ± 4.8 H | 64.4 ± 2.9 | <0.001 |
| Protein (g) | 14.4 ± 0.2 | 12.5 ± 0.3 L | 15.4 ± 0.5 H | 15.4 ± 0.4 H | 13.2 ± 0.2 | <0.001 |
| (% energy) | 14.9 ± 0.1 | 14.2 ± 0.2 L | 14.5 ± 0.2 | 15.3 ± 0.2 H | 14.4 ± 0.2 | <0.001 |
| Vitamin A (μg RAE) | 149 ± 3 | 143 ± 4 | 180 ± 8 H | 156 ± 5 | 133 ± 4 L | <0.001 |
| Thiamin (mg) | 0.44 ± 0.01 | 0.43 ± 0.01 L | 0.50 ± 0.02 H | 0.43 ± 0.01 | 0.44 ± 0.01 | 0.01 |
| Riboflavin (mg) | 0.57 ± 0.01 | 0.52 ± 0.02 L | 0.62 ± 0.02 H | 0.59 ± 0.01 | 0.53 ± 0.01 | <0.001 |
| Niacin (mg NE) | 7.0 ± 0.1 | 5.6 ± 0.1 L | 7.1 ± 0.2 | 7.4 ± 0.2 H | 6.7 ± 0.1 | <0.001 |
| Vitamin B6 (mg) | 0.31 ± 0.01 | 0.30 ± 0.01 | 0.34 ± 0.01 | 0.31 ± 0.01 | 0.31 ± 0.01 | 0.1 |
| Vitamin B12 (μg) | 0.89 ± 0.02 | 1.00 ± 0.03 | 1.15 ± 0.05 H | 0.94 ± 0.03 | 0.72 ± 0.02 L | <0.001 |
| Folate (μg DFE) | 102.7 ± 1.4 | 95.1 ± 3.5 L | 110.1 ± 3.8 H | 107.2 ± 2.3 | 96.5 ± 2.0 | <0.001 |
| Folic acid (μg) | 30.1 ± 0.5 | 33.8 ± 1.7 | 36.7 ± 1.9 H | 30.6 ± 0.9 | 27.4 ± 0.8 L | <0.001 |
| Vitamin C (mg) | 21.2 ± 0.7 | 19.2 ± 1.2 | 22.0 ± 1.6 | 21.2 ± 1.2 | 21.6 ± 0.9 | 0.4 |
| Vitamin D (μg) | 1.67 ± 0.03 | 2.00 ± 0.07 | 2.22 ± 0.09 H | 1.65 ± 0.05 | 1.51 ± 0.04 L | <0.001 |
| Calcium (mg) | 225 ± 3 | 270 ± 7 | 282 ± 9 H | 224 ± 5 | 206 ± 4 L | <0.001 |
| Iron (mg) | 3.34 ± 0.04 | 3.47 ± 0.10 | 3.92 ± 0.16 H | 3.27 ± 0.06 L | 3.29 ± 0.07 | 0.001 |
| Magnesium (mg) | 77.3 ± 1.1 | 58.3 ± 1.3 L | 68.3 ± 2.1 | 78.5 ± 1.8 | 81.9 ± 1.7 H | <0.001 |
| Potassium (mg) | 580 ± 7 | 477 ± 10 L | 558 ± 15 | 590 ± 12 | 594 ± 9 H | <0.001 |
| Sodium (mg) | 494 ± 9 | 435 ± 12 L | 549 ± 22 H | 523 ± 15 | 453 ± 11 | <0.001 |
| Zinc (mg) | 2.03 ± 0.03 | 1.78 ± 0.04 L | 2.16 ± 0.08 H | 2.10 ± 0.05 | 1.97 ± 0.04 | <0.001 |
| Breakfast Intake | Children/teens 6–17 Years (n = 3934) | Adults 18+ Years (n = 12,550) | ||||||
|---|---|---|---|---|---|---|---|---|
| Tertile of NRF 9.3 Score | Tertile of NRF 9.3 Score | |||||||
| 1 (Low) | 2 (Middle) | 3 (High) | p3 | 1 (Low) | 2 (Middle) | 3 (High) | p3 | |
| Daily NRF 9.3 score 2 | 387 ± 3 | 512 ± 1 | 628 ± 2 | n/a | 389 ± 2 | 527 ± 1 | 665 ± 2 | n/a |
| Energy (kcal) | 386 ± 12 | 392 ± 11 | 368 ± 9 | 0.822 | 389 ± 10 | 400 ± 9 | 381 ± 10 | 0.351 |
| Energy (% of day) | 18.7 ± 0.0 L | 21.1 ± 0.1 H | 21.0 ± 0.0 | <0.001 | 20.0 ± 0.0 L | 21.6 ± 0.0 | 24.0 ± 0.0 H | 0.004 |
| Carbohydrate (g) | 53.0 ± 1.7 L | 59.4 ± 1.9 H | 56.0 ± 1.4 | 0.020 | 49.8 ± 1.1 L | 55.8 ± 1.2 | 57.4 ± 1.2 H | <0.001 |
| Total sugars (g) | 23.3 ± 0.9 L | 27.3 ± 1.1 H | 26.7 ± 0.7 | 0.003 | 20.0 ± 0.6 L | 23.5 ± 0.6 | 23.9 ± 0.6 H | <0.001 |
| Fiber (g) | 2.9 ± 0.1 L | 3.6 ± 0.2 | 4.1 ± 0.2 H | <0.001 | 3.2 ± 0.1 L | 4.4 ± 0.1 | 6.0 ± 0.2 H | <0.001 |
| Fat (g) | 13.9 ± 0.7 | 11.8 ± 0.5 | 10.4 ± 0.4 | 0.108 | 15.4 ± 0.6 H | 14.1 ± 0.6 | 11.4 ± 0.5 L | <0.001 |
| Saturates (g) | 5.4 ± 0.3 | 4.6 ± 0.2 | 4.0 ± 0.2 | 0.119 | 5.6 ± 0.2 H | 4.7 ± 0.2 | 3.7 ± 0.2 L | <0.001 |
| Monounsaturates (g) | 4.8 ± 0.2 | 4.1 ± 0.2 | 3.6 ± 0.2 | 0.081 | 5.7 ± 0.3 H | 5.2 ± 0.3 | 4.1 ± 0.2 L | <0.001 |
| Polyunsaturates (g) | 2.4 ± 0.2 | 2.1 ± 0.1 | 1.8 ± 0.1 | 0.491 | 2.8 ± 0.1 | 3.0 ± 0.1 H | 2.5 ± 0.1 L | 0.030 |
| Cholesterol (mg) | 72.1 ± 5.4 | 61.0 ± 4.9 | 56.1 ± 4.9 | 0.708 | 91.2 ± 5.4 H | 80.6 ± 5.4 | 67.9 ± 4.6 L | 0.039 |
| Protein (g) | 13.2 ± 0.5 | 13.4 ± 0.4 | 14.4 ± 0.4 | 0.131 | 14.2 ± 0.4 L | 14.4 ± 0.4 | 15.0 ± 0.4 H | 0.037 |
| Vitamin A (μg RAE) | 144 ± 7 L | 149 ± 6 | 181 ± 8 H | 0.019 | 129 ± 5 L | 146 ± 6 | 166 ± 6 H | <0.001 |
| Thiamin (mg) | 0.42 ± 0.02 L | 0.44 ± 0.02 | 0.52 ± 0.02 H | 0.033 | 0.38 ± 0.01 L | 0.43 ± 0.02 | 0.49 ± 0.01 H | <0.001 |
| Riboflavin (mg) | 0.51 ± 0.02 L | 0.55 ± 0.02 | 0.63 ± 0.02 H | <0.001 | 0.54 ± 0.01 L | 0.57 ± 0.01 | 0.59 ± 0.01 H | <0.001 |
| Niacin (mg NE) | 6.1 ± 0.2 | 6.2 ± 0.2 | 6.4 ± 0.2 | 0.265 | 7.0 ± 0.2 | 7.0 ± 0.2 L | 7.3 ± 0.2 H | 0.032 |
| Vitamin B6 (mg) | 0.25 ± 0.01 L | 0.34 ± 0.02 | 0.36 ± 0.01 H | <0.001 | 0.25 ± 0.01 L | 0.30 ± 0.01 | 0.38 ± 0.01 H | <0.001 |
| Vitamin B12 (μg) | 0.90 ± 0.04 L | 1.05 ± 0.05 | 1.22 ± 0.05 H | <0.001 | 0.78 ± 0.04 L | 0.84 ± 0.03 | 0.95 ± 0.03 H | <0.001 |
| Folate, DFE (μg) | 101.6 ± 4.6 | 106.4 ± 4.9 | 95.4 ± 3.8 | 0.436 | 101.6 ± 2.9 | 104.6 ± 2.7 | 102.8 ± 2.7 | 0.195 |
| Vitamin C (mg) | 16.2 ± 1.6 | 24.0 ± 2.0 | 20.7 ± 1.5 | 0.051 | 12.6 ± 1.0 L | 23.6 ± 1.6 | 27.8 ± 1.4 H | <0.001 |
| Vitamin D (μg) | 1.7 ± 0.1 L | 2.0 ± 0.1 | 2.5 ± 0.1 H | <0.001 | 1.3 ± 0.1 L | 1.7 ± 0.1 | 1.8 ± 0.1 H | <0.001 |
| Calcium (mg) | 221 ± 8 L | 274 ± 11 | 328 ± 10 H | <0.001 | 172 ± 6 L | 218 ± 6 | 262 ± 8 H | <0.001 |
| Iron (mg) | 3.1 ± 0.1 L | 3.8 ± 0.2 | 4.1 ± 0.1 H | <0.001 | 2.9 ± 0.1 L | 3.2 ± 0.1 | 3.8 ± 0.1 H | <0.001 |
| Magnesium (mg) | 51.9 ± 1.7 L | 62.6 ± 2.2 | 72.4 ± 2.4 H | <0.001 | 63.8 ± 2.0 L | 79.6 ± 2.5 | 96.1 ± 2.3 H | <0.001 |
| Potassium (mg) | 426 ± 14 L | 512 ± 16 | 590 ± 17 H | <0.001 | 488 ± 12 L | 592 ± 14 | 695 ± 15 H | <0.001 |
| Sodium (mg) | 540 ± 26 | 479 ± 16 | 424 ± 13 | 0.075 | 572 ± 19 H | 492 ± 14 | 423 ± 17 L | <0.001 |
| Zinc (mg) | 1.7 ± 0.1 L | 1.9 ± 0.1 | 2.2 ± 0.1 H | 0.003 | 1.8 ± 0.1 L | 2.0 ± 0.1 | 2.3 ± 0.1 H | <0.001 |
| Children/Teens 6–17 Years (n = 3934) | ||||||||
| Food Group 2 | Mean Food Group Intake (Servings or kcal 3) | p4 | Proportion Consuming Food Group (%) | p | ||||
| Tertile 1 | Tertile 2 | Tertile 3 | Tertile 1 | Tertile 2 | Tertile 3 | |||
| Vegetables and Fruit | 0.41 ± 0.0 L | 0.61 ± 0.04 | 0.61 ± 0.04 H | 0.006 | 28.4 ± 2.1 L | 36.8 ± 2.1 | 39.3 ± 2.1 H | <0.001 |
| Whole Fruit | 0.13 ± 0.02 L | 0.21 ± 0.02 | 0.29 ± 0.03 H | <0.001 | 13.2 ± 1.5 L | 18.1 ± 1.6 | 25.6 ± 2.0 H | <0.001 |
| Fruit Juice | 0.18 ± 0.02 L | 0.33 ± 0.03 H | 0.27 ± 0.03 | <0.001 | 10.2 ± 1.3 L | 17.5 ± 1.5 H | 14.6 ± 1.5 | 0.002 |
| Grain Products | 1.50 ± 0.07 | 1.56 ± 0.06 | 1.48 ± 0.05 | 0.430 | 83.0 ± 1.7 L | 89.0 ± 1.3 | 89.6 ± 1.3 H | 0.001 |
| Whole Grains | 0.23 ± 0.03 L | 0.45 ± 0.04 | 0.66 ± 0.05 H | <0.001 | 16.6 ± 1.6 L | 29.3 ± 1.9 | 43.2 ± 2.3 H | <0.001 |
| Non-Whole Grains | 1.26 ± 0.07 H | 1.11 ± 0.06 | 0.82 ± 0.05 L | 0.002 | 68.3 ± 2.0 H | 62.7 ± 2.0 | 50.8 ± 2.2 L | <0.001 |
| Milk and Alternatives | 0.46 ± 0.02 L | 0.57 ± 0.03 | 0.76 ± 0.03 H | <0.001 | 58.3 ± 2.2 L | 64.5 ± 2.1 | 78.4 ± 1.9 H | <0.001 |
| Fluid Milk | 0.35 ± 0.0 L | 0.49 ± 0.02 | 0.70 ± 0.03 H | <0.001 | 47.7 ± 2.1 L | 59.5 ± 2.1 | 75.3 ± 1.9 H | <0.001 |
| Other Milk Products | 0.11 ± 0.01 H | 0.08 ± 0.01 | 0.06 ± 0.01 L | 0.025 | 16.2 ± 1.6 H | 10.1 ± 1.1 | 9.9 ± 1.3 L | <0.001 |
| Meat and Alternatives | 0.20 ± 0.02 | 0.18 ± 0.02 | 0.17 ± 0.02 | 0.508 | 26.8 ± 2.0 | 24.9 ± 1.8 | 23.9 ± 2.0 | 0.580 |
| Other Foods | 61.8 ± 6.0 H | 48.0 ± 3.9 | 25.2 ± 2.0 L | 0.019 | 67.7 ± 2.1 H | 60.6 ± 2.1 | 49.5 ± 2.1 L | <0.001 |
| Adults 18+ years (n = 12,550) | ||||||||
| Food Group 2 | Mean Food Group Intake (Servings or kcal 3) | p4 | Proportion Consuming Food Group (%) | p | ||||
| Tertile 1 | Tertile 2 | Tertile 3 | Tertile 1 | Tertile 2 | Tertile 3 | |||
| Vegetables and Fruit | 0.42 ± 0.03 L | 0.72 ± 0.04 | 0.96 ± 0.04 H | <0.001 | 29.9 ± 1.4 L | 45.3 ± 1.6 | 56.2 ± 1.4 H | <0.001 |
| Whole Fruit | 0.18 ± 0.02 L | 0.37 ± 0.03 | 0.54 ± 0.03 H | <0.001 | 15.8 ± 1.0 L | 30.0 ± 1.5 | 41.5 ± 1.4 H | <0.001 |
| Fruit Juice | 0.16 ± 0.02 L | 0.26 ± 0.03 | 0.28 ± 0.03 H | <0.001 | 8.4 ± 1.0 L | 13.8 ± 1.2 | 13.9 ± 1.0 H | <0.001 |
| Grain Products | 1.49 ± 0.04 | 1.53 ± 0.04 | 1.47 ± 0.04 | 0.296 | 78.1 ± 1.2 L | 82.8 ± 1.2 | 83.4 ± 1.1 H | 0.003 |
| Whole Grains | 0.33 ± 0.02 L | 0.52 ± 0.03 | 0.68 ± 0.03 H | <0.001 | 20.0 ± 1.3 L | 32.2 ± 1.3 | 44.0 ± 1.5 H | <0.001 |
| Non-Whole Grains | 1.17 ± 0.04 H | 1.02 ± 0.04 | 0.79 ± 0.04 L | <0.001 | 60.6 ± 1.5 H | 55.3 ± 1.5 | 45.8 ± 1.4 L | <0.001 |
| Milk and Alternatives | 0.29 ± 0.01 L | 0.42 ± 0.02 | 0.50 ± 0.02 H | <0.001 | 50.1 ± 1.6 L | 62.1 ± 1.6 | 67.9 ± 1.4 H | <0.001 |
| Fluid Milk | 0.18 ± 0.01 L | 0.30 ± 0.02 | 0.38 ± 0.02 H | <0.001 | 40.5 ± 1.6 L | 53.5 ± 1.6 | 58.8 ± 1.4 H | <0.001 |
| Other Milk Products | 0.11 ± 0.01 | 0.11 ± 0.01 | 0.12 ± 0.01 | 0.452 | 17.0 ± 1.1 | 17.3 ± 1.3 | 17.5 ± 1.1 | 0.958 |
| Meat and Alternatives | 0.31 ± 0.02 | 0.32 ± 0.02 | 0.28 ± 0.01 | 0.835 | 36.6 ± 1.7 | 36.8 ± 1.5 | 36.9 ± 1.5 | 0.989 |
| Other Foods | 74.1 ± 3.9 H | 54.4 ± 3.9 | 37.8 ± 2.8 L | <0.001 | 74.2 ± 1.4 H | 67.1 ± 1.5 | 65.2 ± 1.4 L | <0.001 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Barr, S.I.; Vatanparast, H.; Smith, J. Breakfast in Canada: Prevalence of Consumption, Contribution to Nutrient and Food Group Intakes, and Variability across Tertiles of Daily Diet Quality. A Study from the International Breakfast Research Initiative. Nutrients 2018, 10, 985. https://doi.org/10.3390/nu10080985
Barr SI, Vatanparast H, Smith J. Breakfast in Canada: Prevalence of Consumption, Contribution to Nutrient and Food Group Intakes, and Variability across Tertiles of Daily Diet Quality. A Study from the International Breakfast Research Initiative. Nutrients. 2018; 10(8):985. https://doi.org/10.3390/nu10080985
Chicago/Turabian StyleBarr, Susan I., Hassan Vatanparast, and Jessica Smith. 2018. "Breakfast in Canada: Prevalence of Consumption, Contribution to Nutrient and Food Group Intakes, and Variability across Tertiles of Daily Diet Quality. A Study from the International Breakfast Research Initiative" Nutrients 10, no. 8: 985. https://doi.org/10.3390/nu10080985
APA StyleBarr, S. I., Vatanparast, H., & Smith, J. (2018). Breakfast in Canada: Prevalence of Consumption, Contribution to Nutrient and Food Group Intakes, and Variability across Tertiles of Daily Diet Quality. A Study from the International Breakfast Research Initiative. Nutrients, 10(8), 985. https://doi.org/10.3390/nu10080985





