Protective Effects of Dioscorea batatas Flesh and Peel Extracts against Ethanol-Induced Gastric Ulcer in Mice
Abstract
1. Introduction
2. Materials and Methods
2.1. Preparation of Chinese Yam Extracts
2.2. Development of Ethanol-Induced Gastric Ulcer
2.3. Macroscopic Observation
2.4. Histological Analysis
2.5. Measurement of 8-Hydroxy-2’-Deoxyguanosine (8-OHdG) Level
2.6. Determination of Malondialdehyde (MDA) Level
2.7. Determination of Gastric Prostaglandin E2 (PGE2) Level
2.8. Determination of Catalase (CAT) and Superoxide Dismutase (SOD) Activities
2.9. Determination of Plasma Nitric Oxide (NO) and Cytokine Levels
2.10. Western Blot Analysis
3. Statistical Analysis
4. Results
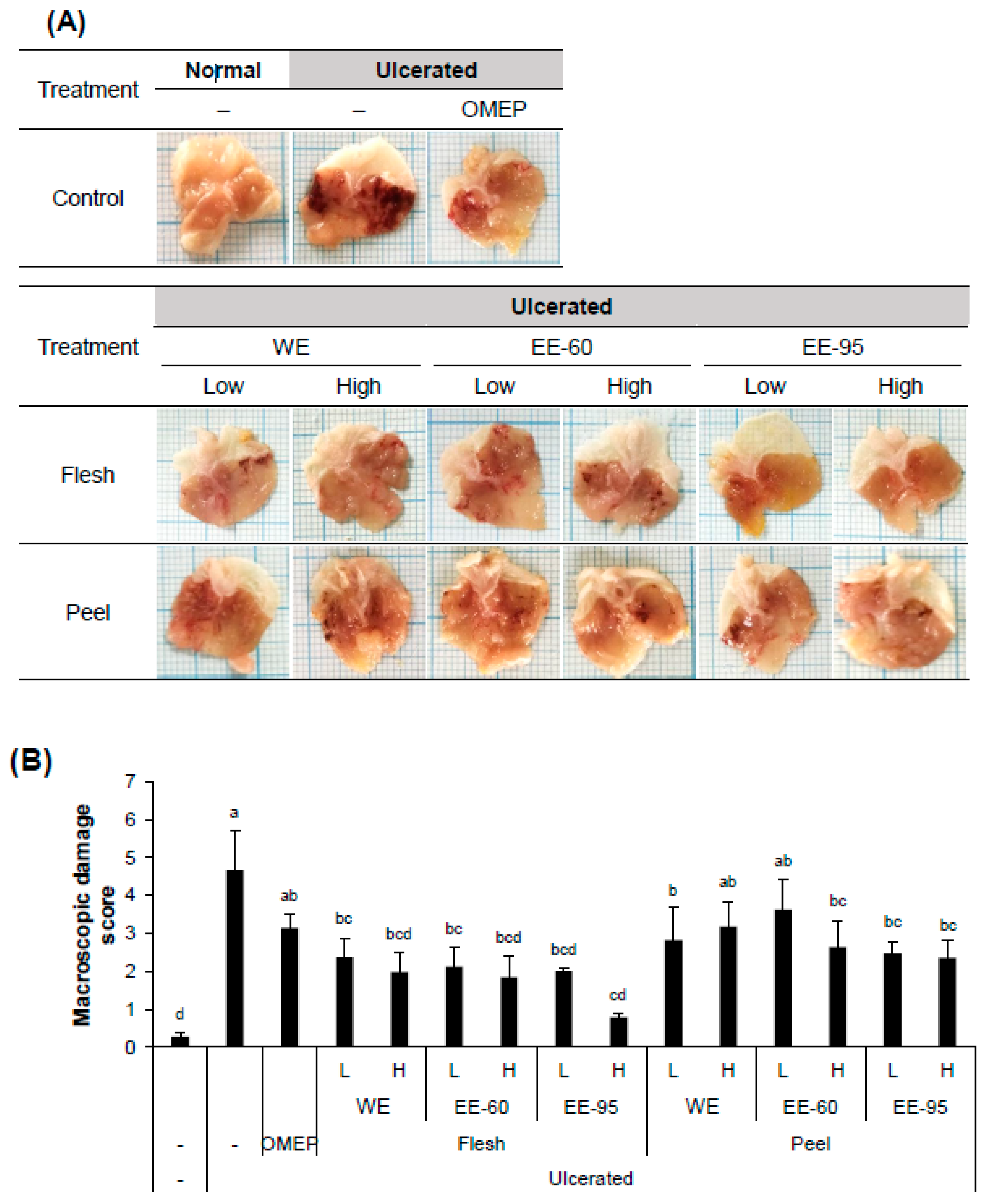
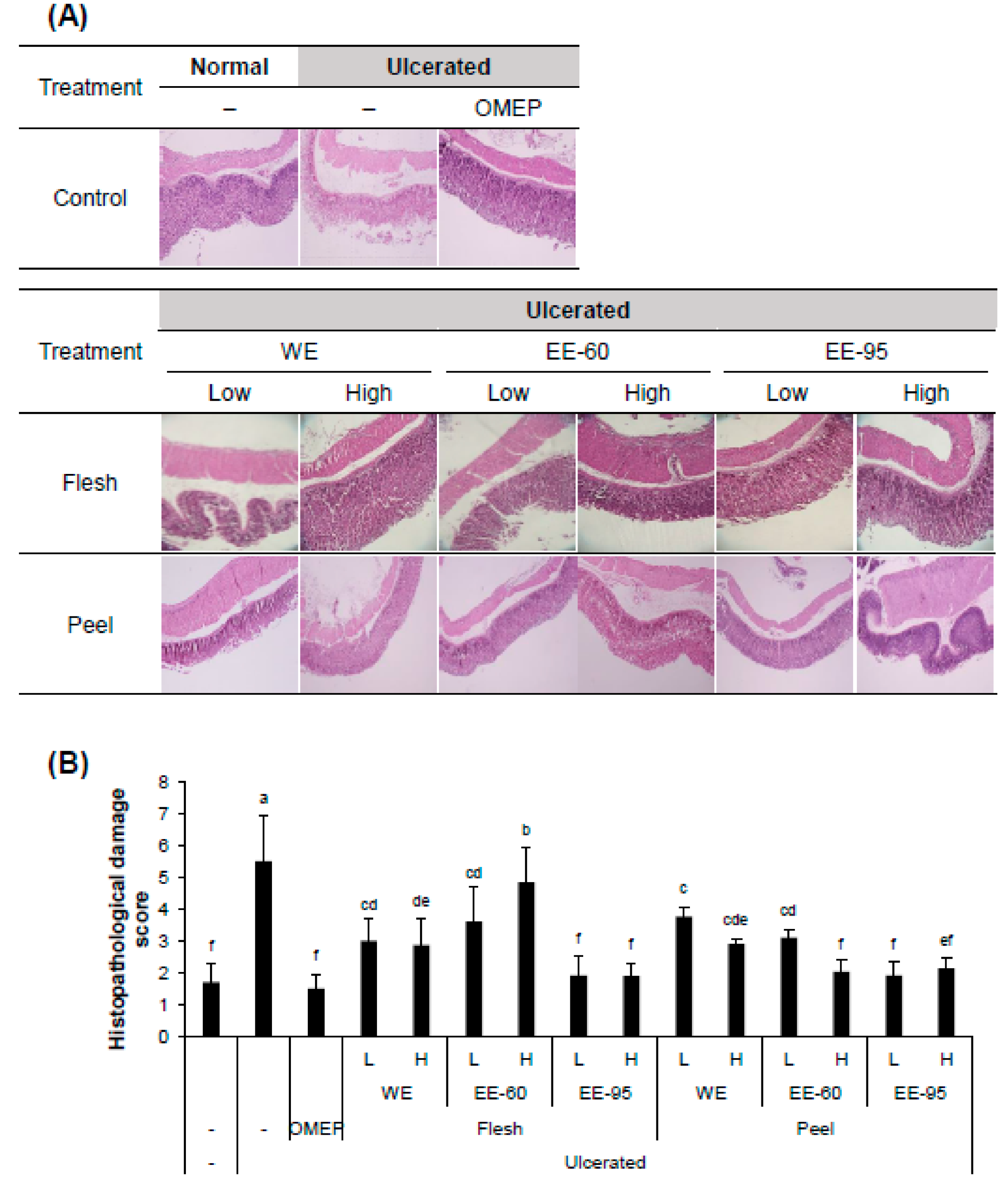
4.1. DBD Flesh and Peel Extracts Alleviated Acidified Ethanol-Induced Gastric Mucosal Damage
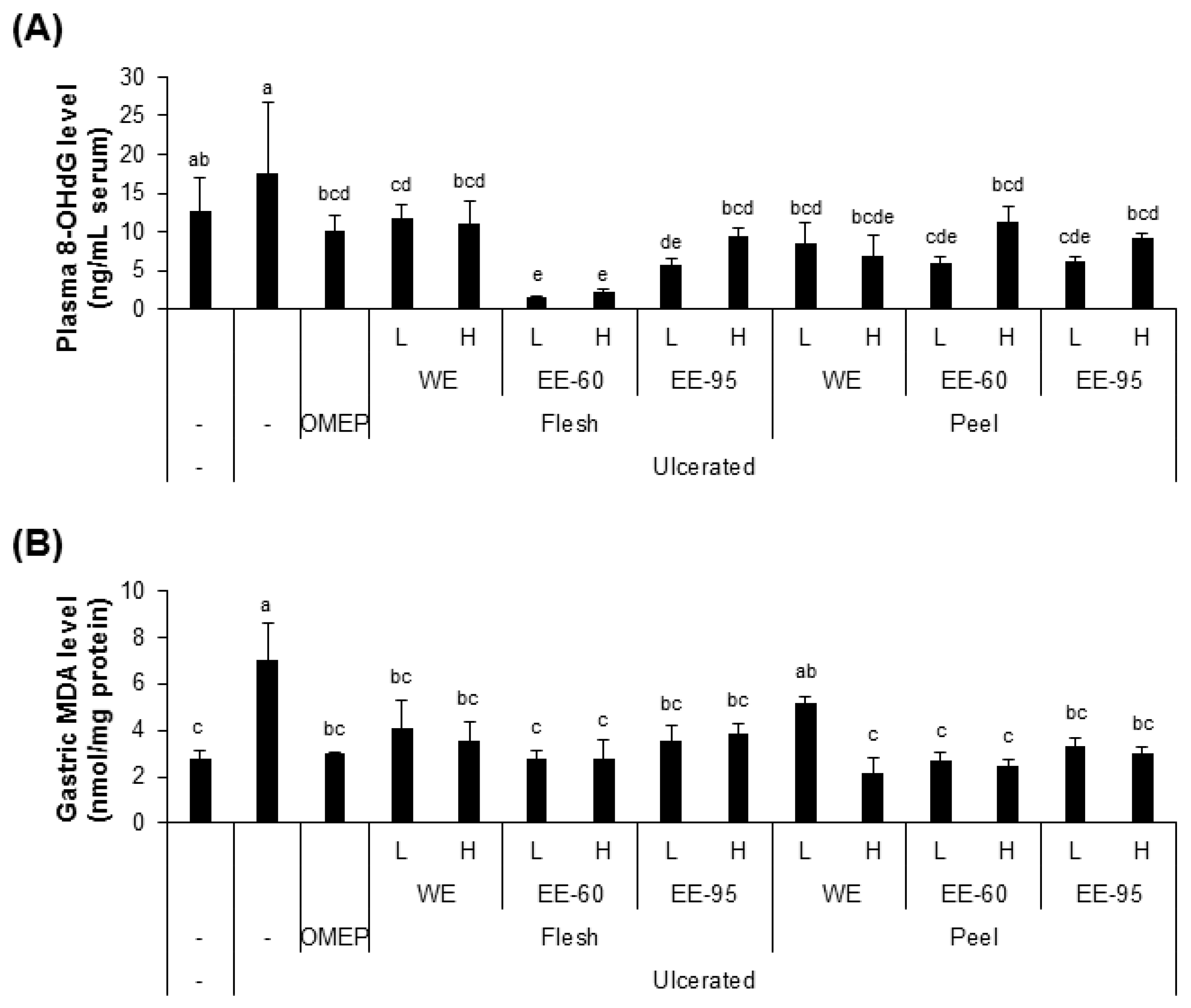
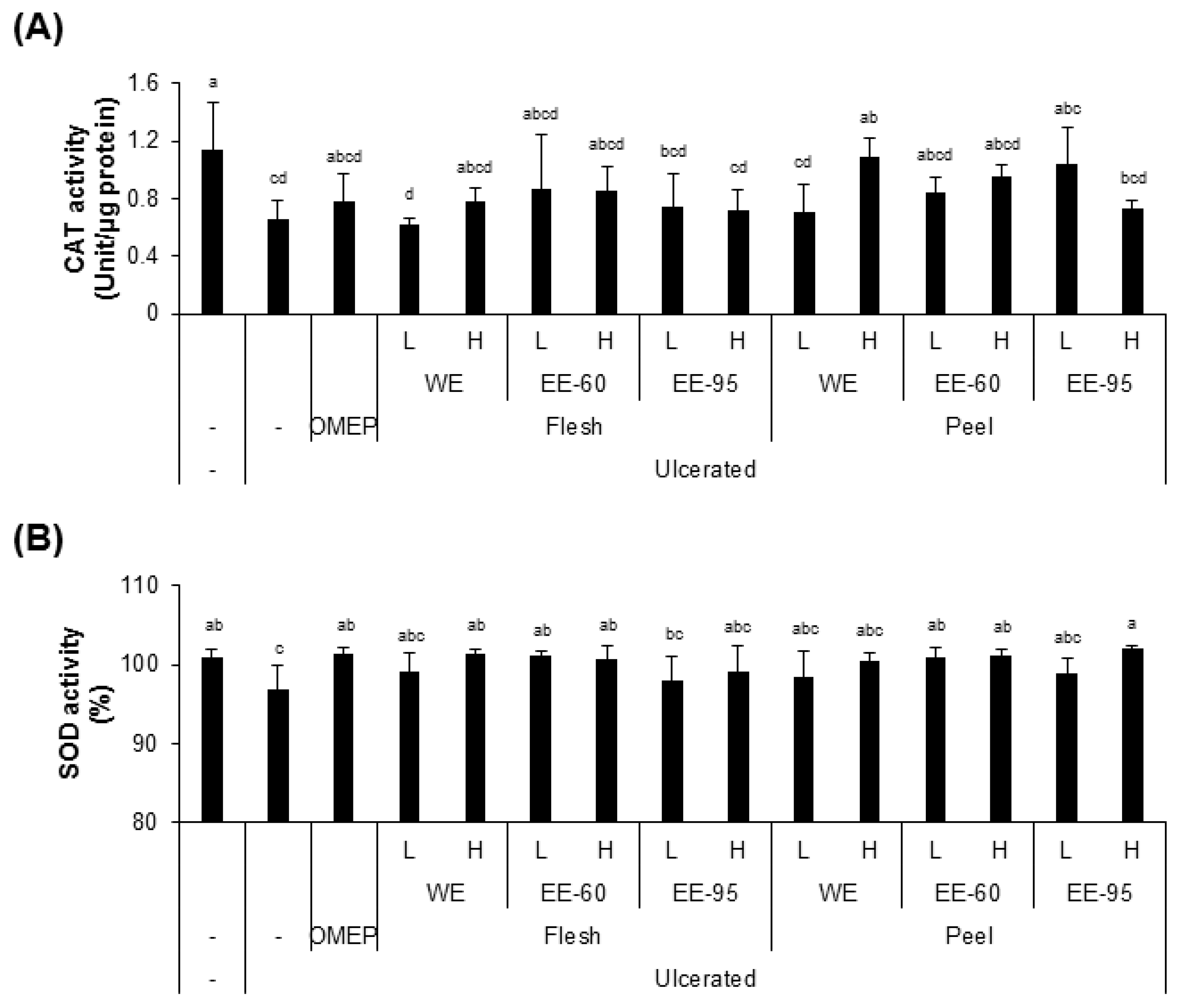
4.2. DBD Flesh and Peel Extracts Reduced Acidified Ethanol-Induced Oxidative Stress
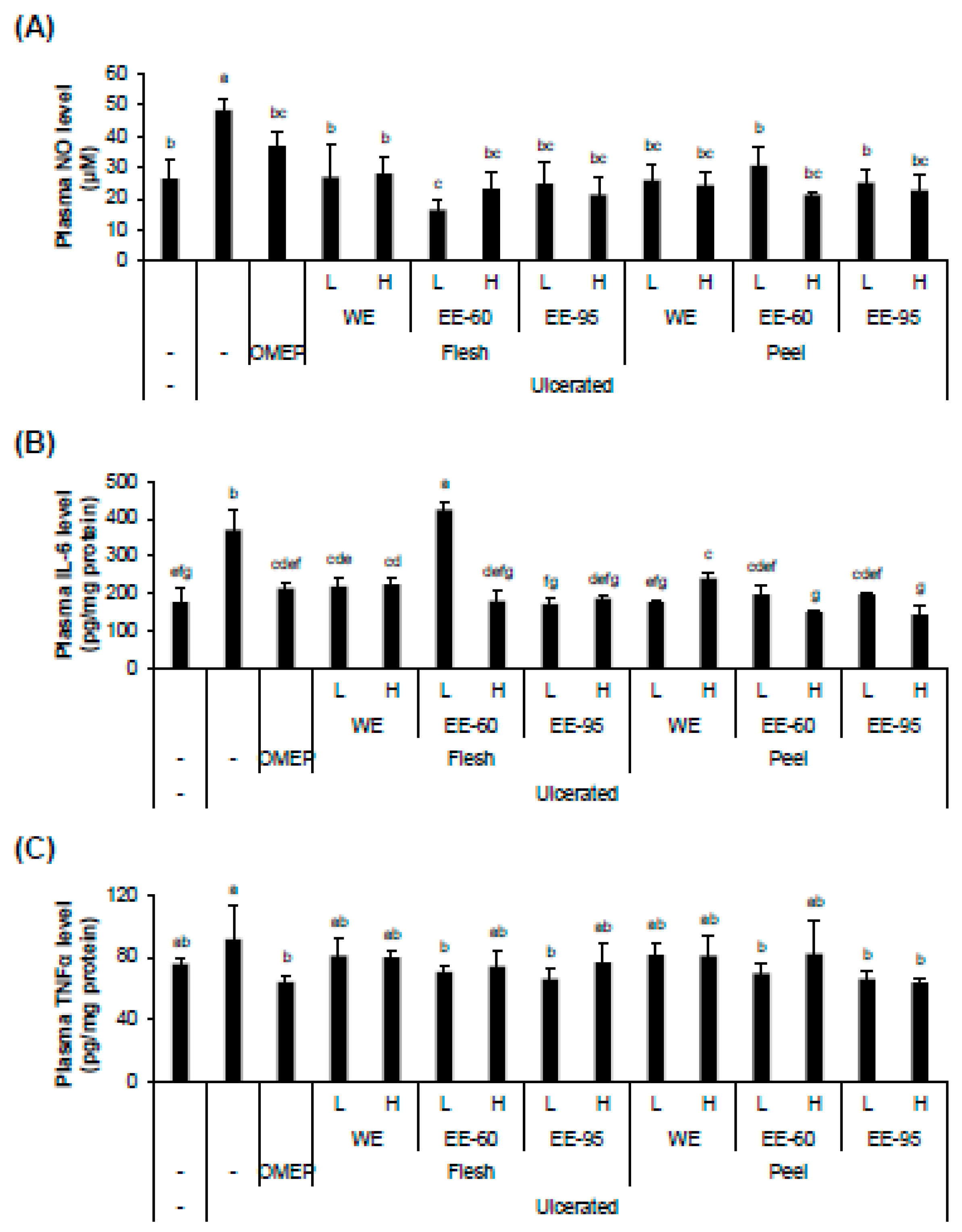
4.3. DBD Flesh and Peel Extracts Decreased Acidified Ethanol-Enhanced Production of Inflammatory Factors
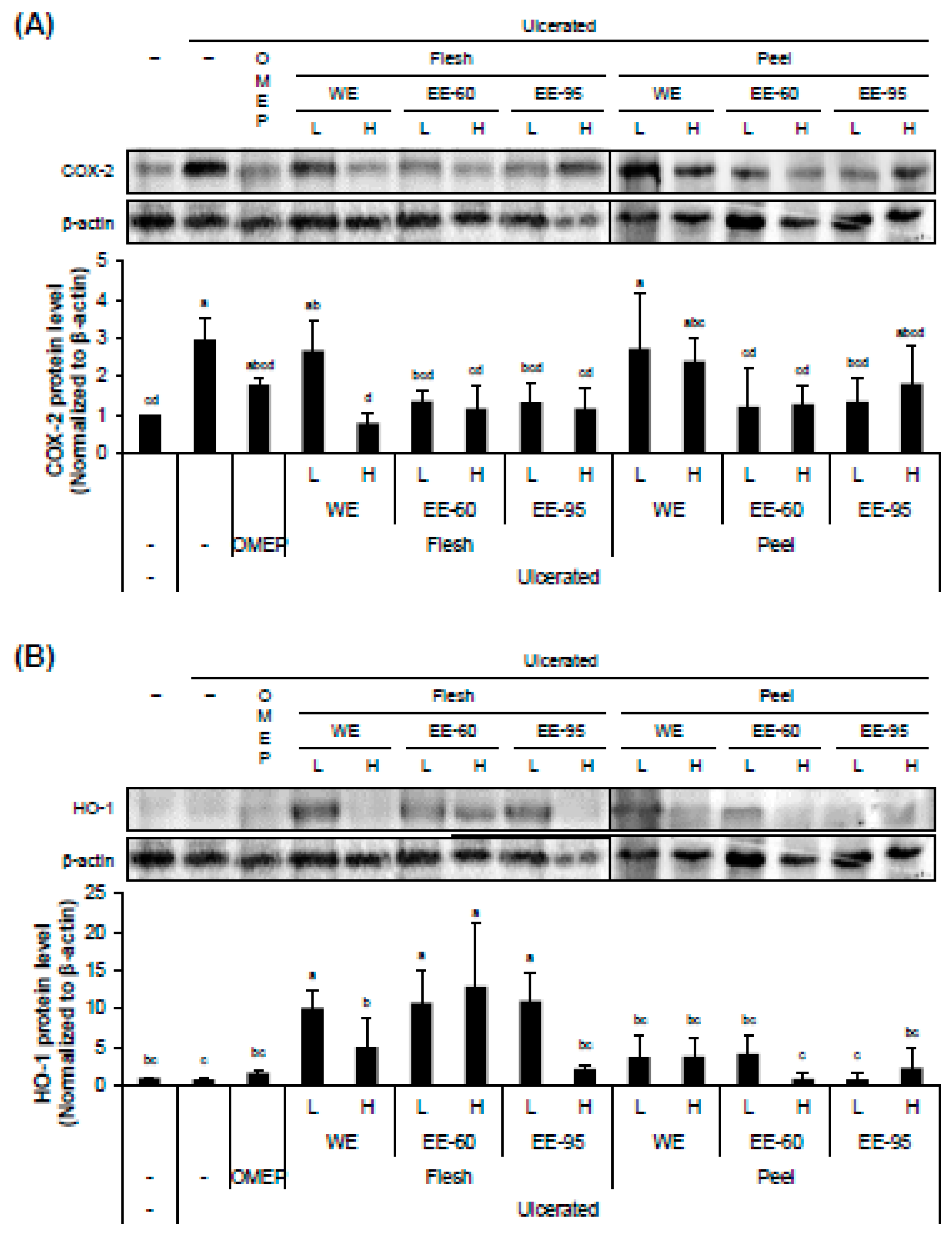
4.4. DBD Flesh and Peel Extracts Influenced the Expressions of an Inflammatory Marker COX-2 and an Antioxidant Enzyme HO-1 in Gastric Mucosa
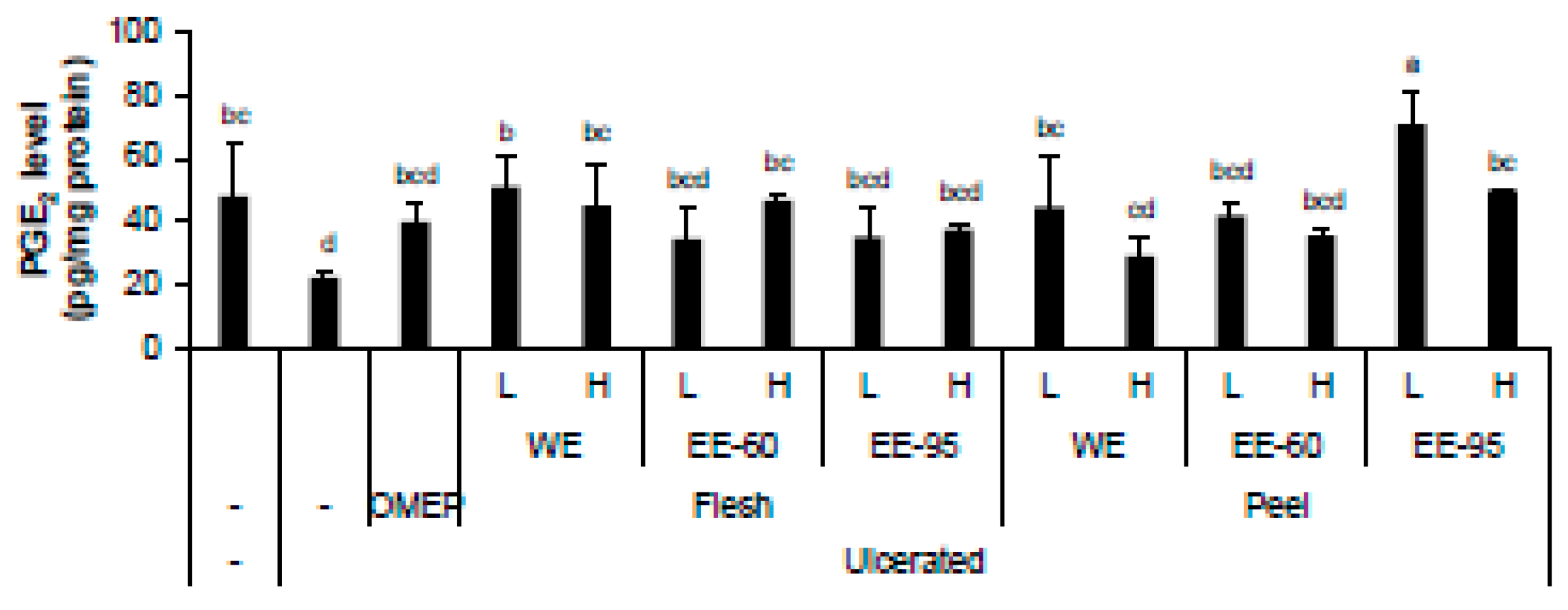
4.5. DBD Flesh and Peel Extracts Increased Acidified Ethanol-Lowered Level of PGE2 in Stomach Homogenate
5. Discussion
Author contributions
Acknowledgments
Conflicts of Interest
References
- Zabaleta, J. Multifactorial etiology of gastric cancer. Methods Mol. Biol. 2012, 863, 411–435. [Google Scholar] [PubMed]
- Cho, C.H.; Koo, M.W.; Garg, G.P.; Ogle, C.W. Stress-induced gastric ulceration: Its aetiology and clinical implications. Scand. J. Gastroenterol. 1992, 27, 257–262. [Google Scholar] [CrossRef] [PubMed]
- Tytgat, G.N. Etiopathogenetic principles and peptic ulcer disease classification. Dig. Dis. 2011, 29, 454–458. [Google Scholar] [CrossRef] [PubMed]
- Szelenyi, I.; Brune, K. Possible role of oxygen free radicals in ethanol-induced gastric mucosal damage in rats. Dig. Dis. Sci. 1988, 33, 865–871. [Google Scholar] [CrossRef] [PubMed]
- Oates, P.J.; Hakkinen, J.P. Studies on the mechanism of ethanol-induced gastric damage in rats. Gastroenterology 1988, 94, 10–21. [Google Scholar] [CrossRef]
- Chang, X.; Luo, F.; Jiang, W.; Zhu, L.; Gao, J.; He, H.; Wei, T.; Gong, S.; Yan, T. Protective activity of salidroside against ethanol-induced gastric ulcer via the MAPK/NF-kappaB pathway in vivo and in vitro. Int. Immunopharmacol. 2015, 28, 604–615. [Google Scholar] [CrossRef] [PubMed]
- Arab, H.H.; Salama, S.A.; Omar, H.A.; Arafa el, S.A.; Maghrabi, I.A. Diosmin protects against ethanol-induced gastric injury in rats: Novel anti-ulcer actions. PLoS ONE 2015, 10, e0122417. [Google Scholar] [CrossRef] [PubMed]
- Asnaashari, S.; Dastmalchi, S.; Javadzadeh, Y. Gastroprotective effects of herbal medicines (roots). Int. J. Food Prop. 2018, 21, 901–919. [Google Scholar] [CrossRef]
- Rozza, A.L.; Pellizzon, C.H. Essential oils from medicinal and aromatic plants: A review of the gastroprotective and ulcer-healing activities. Fundam. Clin. Pharmacol. 2013, 27, 51–63. [Google Scholar] [CrossRef] [PubMed]
- Awaad, A.S.; El-Meligy, R.M.; Soliman, G.A. Natural products in treatment of ulcerative colitis and peptic ulcer. J. Saudi Chem. Soc. 2013, 17, 101–124. [Google Scholar] [CrossRef]
- Geronikaki, A.A.; Gavalas, A.M. Antioxidants and inflammatory disease: Synthetic and natural antioxidants with anti-inflammatory activity. Comb. Chem. High Throughput Screen. 2006, 9, 425–442. [Google Scholar] [CrossRef] [PubMed]
- Zhang, H.; Tsao, R. Dietary polyphenols, oxidative stress and antioxidant and anti-inflammatory effects. Curr. Opin. Food Sci. 2016, 8, 33–42. [Google Scholar] [CrossRef]
- Wang, L.S.; Tu, Y.C.; Lian, T.W.; Hung, J.T.; Yen, J.H.; Wu, M.J. Distinctive antioxidant and antiinflammatory effects of flavonols. J. Agric. Food Chem. 2006, 54, 9798–9804. [Google Scholar] [CrossRef] [PubMed]
- Hou, W.C.; Lee, M.H.; Chen, H.J.; Liang, W.L.; Han, C.H.; Liu, Y.W.; Lin, Y.H. Antioxidant activities of dioscorin, the storage protein of yam (Dioscorea batatas Deene) tuber. J. Agric. Food Chem. 2001, 49, 4956–4960. [Google Scholar] [CrossRef] [PubMed]
- Jeon, J.R.; Lee, J.S.; Lee, C.H.; Kim, J.Y.; Kim, S.D.; Nam, D.H. Effect of ethanol extract of dried Chinese yam (Dioscorea batatas) flour containing dioscin on gastrointestinal function in rat model. Arch. Pharm. Res. 2006, 29, 348–353. [Google Scholar] [CrossRef] [PubMed]
- Jin, M.; Suh, S.J.; Yang, J.H.; Lu, Y.; Kim, S.J.; Kwon, S.; Jo, T.H.; Kim, J.W.; Park, Y.I.; Ahn, G.W.; et al. Anti-inflammatory activity of bark of Dioscorea batatas DECNE through the inhibition of iNOS and COX-2 expressions in RAW264.7 cells via NF-kappa B and ERK1/2 inactivation. Food Chem. Toxicol. 2010, 48, 3073–3079. [Google Scholar] [CrossRef] [PubMed]
- Hou, W.C.; Hsu, F.L.; Lee, M.H. Yam (Dioscorea batatas) tuber mucilage exhibited antioxidant activities in vitro. Planta Med. 2002, 68, 1072–1076. [Google Scholar] [CrossRef] [PubMed]
- Xu, T.; Zheng, L.; Xu, L.; Yin, L.; Qi, Y.; Xu, Y.; Han, X.; Peng, J. Protective effects of dioscin against alcohol-induced liver injury. Arch. Toxicol. 2014, 88, 739–753. [Google Scholar] [CrossRef] [PubMed]
- Zakarova, A.; Seo, J.Y.; Kim, H.Y.; Kim, J.H.; Shin, J.H.; Cho, K.M.; Lee, C.H.; Kim, J.S. Garlic Sprouting Is Associated with Increased Antioxidant Activity and Concomitant Changes in the Metabolite Profile. J. Agric. Food Chem. 2014, 62, 1875–1880. [Google Scholar] [CrossRef] [PubMed]
- Tabuchi, Y.; Sugiyama, N.; Horiuchi, T.; Furusawa, M.; Furuhama, K. Ebselen, a seleno-organic compound, protects against ethanol-induced murine gastric mucosal injury in both in vivo and in vitro systems. Eur. J. Pharmacol. 1995, 272, 195–201. [Google Scholar] [CrossRef]
- Biswas, K.; Bandyopadhyay, U.; Chattopadhyay, I.; Varadaraj, A.; Ali, E.; Banerjee, R.K. A novel antioxidant and antiapoptotic role of omeprazole to block gastric ulcer through scavenging of hydroxyl radical. J. Biol. Chem. 2003, 278, 10993–11001. [Google Scholar] [CrossRef] [PubMed]
- Seo, H.; Oh, J.; Hahn, D.; Kwon, C.S.; Lee, J.S.; Kim, J.S. Protective Effect of Glyceollins in a Mouse Model of Dextran Sulfate Sodium-Induced Colitis. J. Med. Food 2017, 20, 1055–1062. [Google Scholar] [CrossRef] [PubMed]
- Bito, T.; Misaki, T.; Yabuta, Y.; Ishikawa, T.; Kawano, T.; Watanabe, F. Vitamin B12 deficiency results in severe oxidative stress, leading to memory retention impairment in Caenorhabditis elegans. Redox. Biol. 2017, 11, 21–29. [Google Scholar] [CrossRef] [PubMed]
- Holcik, M.; Gordon, B.W.; Korneluk, R.G. The internal ribosome entry site-mediated translation of antiapoptotic protein XIAP is modulated by the heterogeneous nuclear ribonucleoproteins C1 and C2. Mol. Cell. Biol. 2003, 23, 280–288. [Google Scholar] [CrossRef] [PubMed]
- Franke, A.; Teyssen, S.; Singer, M.V. Alcohol-related diseases of the esophagus and stomach. Dig. Dis. 2005, 23, 204–213. [Google Scholar] [CrossRef] [PubMed]
- Kumar, S.; Das, G.; Shin, H.S.; Patra, J.K. Dioscorea spp. (A Wild Edible Tuber): A Study on Its Ethnopharmacological Potential and Traditional Use by the Local People of Similipal Biosphere Reserve, India. Front. Pharmacol. 2017, 8, 52. [Google Scholar] [CrossRef] [PubMed]
- Son, I.S.; Lee, J.S.; Lee, J.Y.; Kwon, C.S. Antioxidant and Anti-inflammatory Effects of Yam (Dioscorea batatas Decne.) on Azoxymethane-induced Colonic Aberrant Crypt Foci in F344 Rats. Prev. Nutr. Food Sci. 2014, 19, 82–88. [Google Scholar] [CrossRef] [PubMed]
- Dey, P.; Roy Chowdhuri, S.; Sarkar, M.P.; Chaudhuri, T.K. Evaluation of anti-inflammatory activity and standardisation of hydro-methanol extract of underground tuber of Dioscorea alata. Pharm. Biol. 2016, 54, 1474–1482. [Google Scholar] [CrossRef] [PubMed]
- Wallace, J.L. Prostaglandins, NSAIDs, and gastric mucosal protection: Why doesn’t the stomach digest itself? Physiol. Rev. 2008, 88, 1547–1565. [Google Scholar] [CrossRef] [PubMed]
- Lu, Y.L.; Chia, C.Y.; Liu, Y.W.; Hou, W.C. Biological activities and applications of dioscorins, the major tuber storage proteins of yam. J. Tradit. Complement. Med. 2012, 2, 41–46. [Google Scholar] [CrossRef]
- Go, H.K.; Rahman, M.M.; Kim, G.B.; Na, C.S.; Song, C.H.; Kim, J.S.; Kim, S.J.; Kang, H.S. Antidiabetic Effects of Yam (Dioscorea batatas) and Its Active Constituent, Allantoin, in a Rat Model of Streptozotocin-Induced Diabetes. Nutrients 2015, 7, 8532–8544. [Google Scholar] [CrossRef] [PubMed]
- Koo, H.J.; Park, H.J.; Byeon, H.E.; Kwak, J.H.; Um, S.H.; Kwon, S.T.; Rhee, D.K.; Pyo, S. Chinese yam extracts containing beta-sitosterol and ethyl linoleate protect against atherosclerosis in apolipoprotein E-deficient mice and inhibit muscular expression of VCAM-1 in vitro. J. Food Sci. 2014, 79, H719–H729. [Google Scholar] [CrossRef] [PubMed]
- Li, W.; Huang, H.; Niu, X.; Fan, T.; Mu, Q.; Li, H. Protective effect of tetrahydrocoptisine against ethanol-induced gastric ulcer in mice. Toxicol. Appl. Pharmacol. 2013, 272, 21–29. [Google Scholar] [CrossRef] [PubMed]
- Yoo, J.H.; Lee, J.S.; Lee, Y.S.; Ku, S.; Lee, H.J. Protective effect of bovine milk against HCl and ethanol-induced gastric ulcer in mice. J. Dairy Sci. 2018, 101, 3758–3770. [Google Scholar] [CrossRef] [PubMed]
- Li, W.F.; Hao, D.J.; Fan, T.; Huang, H.M.; Yao, H.; Niu, X.F. Protective effect of chelerythrine against ethanol-induced gastric ulcer in mice. Chem. Biol. Interact. 2014, 208, 18–27. [Google Scholar] [CrossRef] [PubMed]
- Kedika, R.R.; Souza, R.F.; Spechler, S.J. Potential anti-inflammatory effects of proton pump inhibitors: A review and discussion of the clinical implications. Dig. Dis. Sci. 2009, 54, 2312–2317. [Google Scholar] [CrossRef] [PubMed]
- El-Nezhawy, A.O.; Biuomy, A.R.; Hassan, F.S.; Ismaiel, A.K.; Omar, H.A. Design, synthesis and pharmacological evaluation of omeprazole-like agents with anti-inflammatory activity. Bioorg. Med. Chem. 2013, 21, 1661–1670. [Google Scholar] [CrossRef] [PubMed]
- Laine, L.; Takeuchi, K.; Tarnawski, A. Gastric mucosal defense and cytoprotection: Bench to bedside. Gastroenterology 2008, 135, 41–60. [Google Scholar] [CrossRef] [PubMed]
- Takeuchi, K.; Amagase, K. Roles of Cyclooxygenase, Prostaglandin E2 and EP Receptors in Mucosal Protection and Ulcer Healing in the Gastrointestinal Tract. Curr. Pharm. Des. 2018, 24, 2002–2011. [Google Scholar] [CrossRef] [PubMed]
- Zhao, W.; Zhu, F.; Shen, W.; Fu, A.; Zheng, L.; Yan, Z.; Zhao, L.; Fu, G. Protective effects of DIDS against ethanol-induced gastric mucosal injury in rats. Acta Biochim. Biophys. Sin. (Shanghai) 2009, 41, 301–308. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.J.; Lim, K.T. Inhibitory effect of 30-kDa phytoglycoprotein on expression of TNF-alpha and COX-2 via activation of PKCalpha and ERK 1/2 in LPS-stimulated RAW 264.7 cells. Mol. Cell. Biochem. 2008, 317, 151–159. [Google Scholar] [CrossRef] [PubMed]
- Jin, M.H.; Lu, Y.; Yang, J.H.; Jo, T.H.; Park, Y.I.; Lee, C.K.; Park, S.J.; Son, K.H.; Chang, H.W. Anti-inflammatory Activity of 6-Hydroxy-2,7-dimethoxy-1,4-henanthraquinone from Tuberous Roots of Yam (Dioscorea batatas) through Inhibition of Prostaglandin D-2 and Leukotriene C-4 Production in Mouse Bone Marrow-derived Mast Cells. Arch. Pharm. Res. 2011, 34, 1495–1501. [Google Scholar] [CrossRef] [PubMed]
| Group No. | Treatment 1) | Dose (mg/kg BW) | ||
|---|---|---|---|---|
| 1 | Normal | Vehicle | - | |
| 2 | Ulcerated 2) | Vehicle | - | |
| 3 | OMEP 3) | 20 | ||
| 4 | Flesh | WE 4) | 100 | |
| 5 | 200 | |||
| 6 | EE-60 5) | 100 | ||
| 7 | 200 | |||
| 8 | EE-95 6) | 100 | ||
| 9 | 200 | |||
| 10 | Peel | WE | 100 | |
| 11 | 200 | |||
| 12 | EE-60 | 100 | ||
| 13 | 200 | |||
| 14 | EE-95 | 100 | ||
| 15 | 200 | |||
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Byeon, S.; Oh, J.; Lim, J.S.; Lee, J.S.; Kim, J.-S. Protective Effects of Dioscorea batatas Flesh and Peel Extracts against Ethanol-Induced Gastric Ulcer in Mice. Nutrients 2018, 10, 1680. https://doi.org/10.3390/nu10111680
Byeon S, Oh J, Lim JS, Lee JS, Kim J-S. Protective Effects of Dioscorea batatas Flesh and Peel Extracts against Ethanol-Induced Gastric Ulcer in Mice. Nutrients. 2018; 10(11):1680. https://doi.org/10.3390/nu10111680
Chicago/Turabian StyleByeon, Siyul, Jisun Oh, Ji Sun Lim, Jeong Soon Lee, and Jong-Sang Kim. 2018. "Protective Effects of Dioscorea batatas Flesh and Peel Extracts against Ethanol-Induced Gastric Ulcer in Mice" Nutrients 10, no. 11: 1680. https://doi.org/10.3390/nu10111680
APA StyleByeon, S., Oh, J., Lim, J. S., Lee, J. S., & Kim, J.-S. (2018). Protective Effects of Dioscorea batatas Flesh and Peel Extracts against Ethanol-Induced Gastric Ulcer in Mice. Nutrients, 10(11), 1680. https://doi.org/10.3390/nu10111680





