Viral Loads and Disease Severity in Children with Rhinovirus-Associated Illnesses
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Definitions
2.2. Data Collection
2.3. Statistical Analysis
3. Results
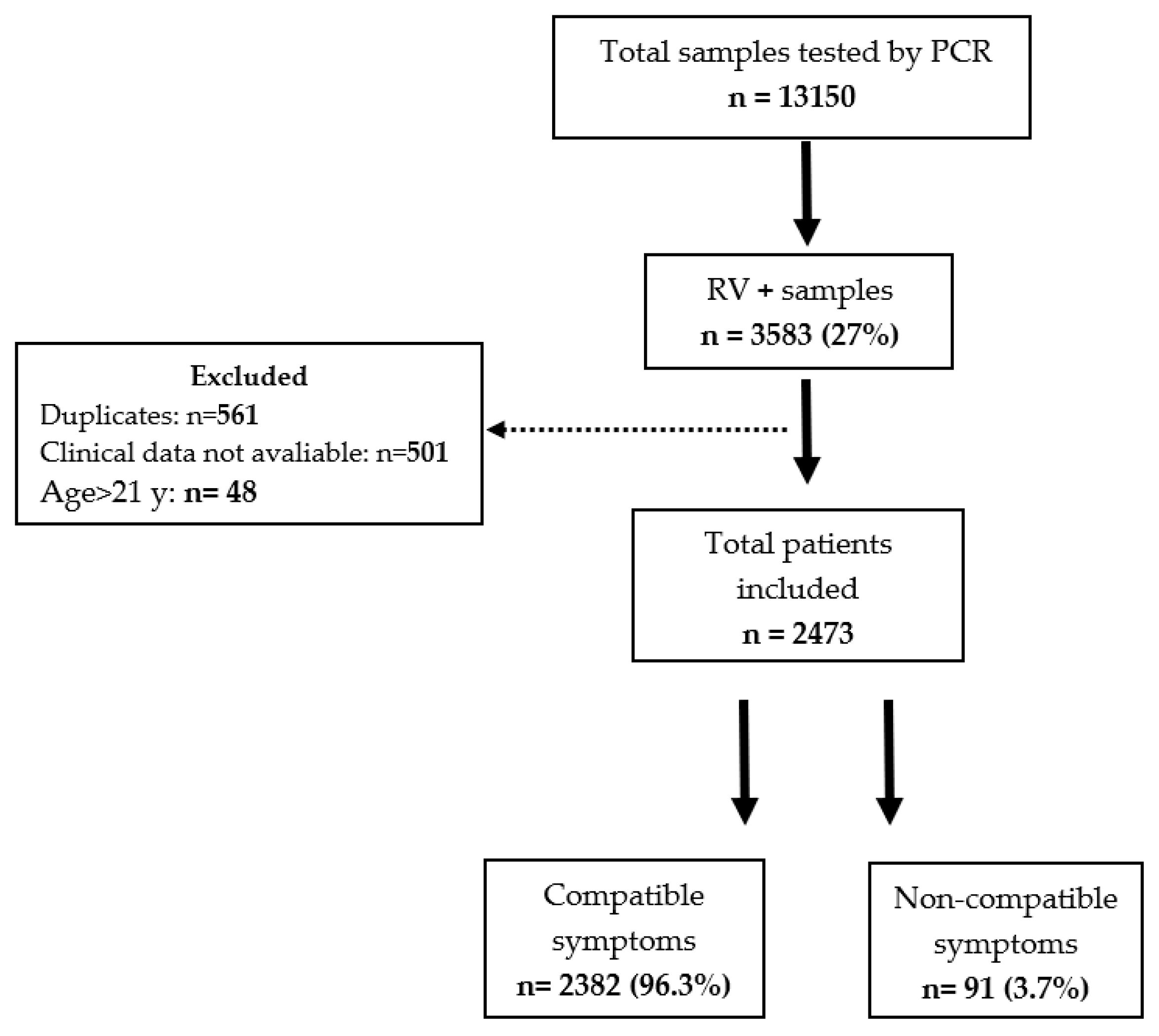
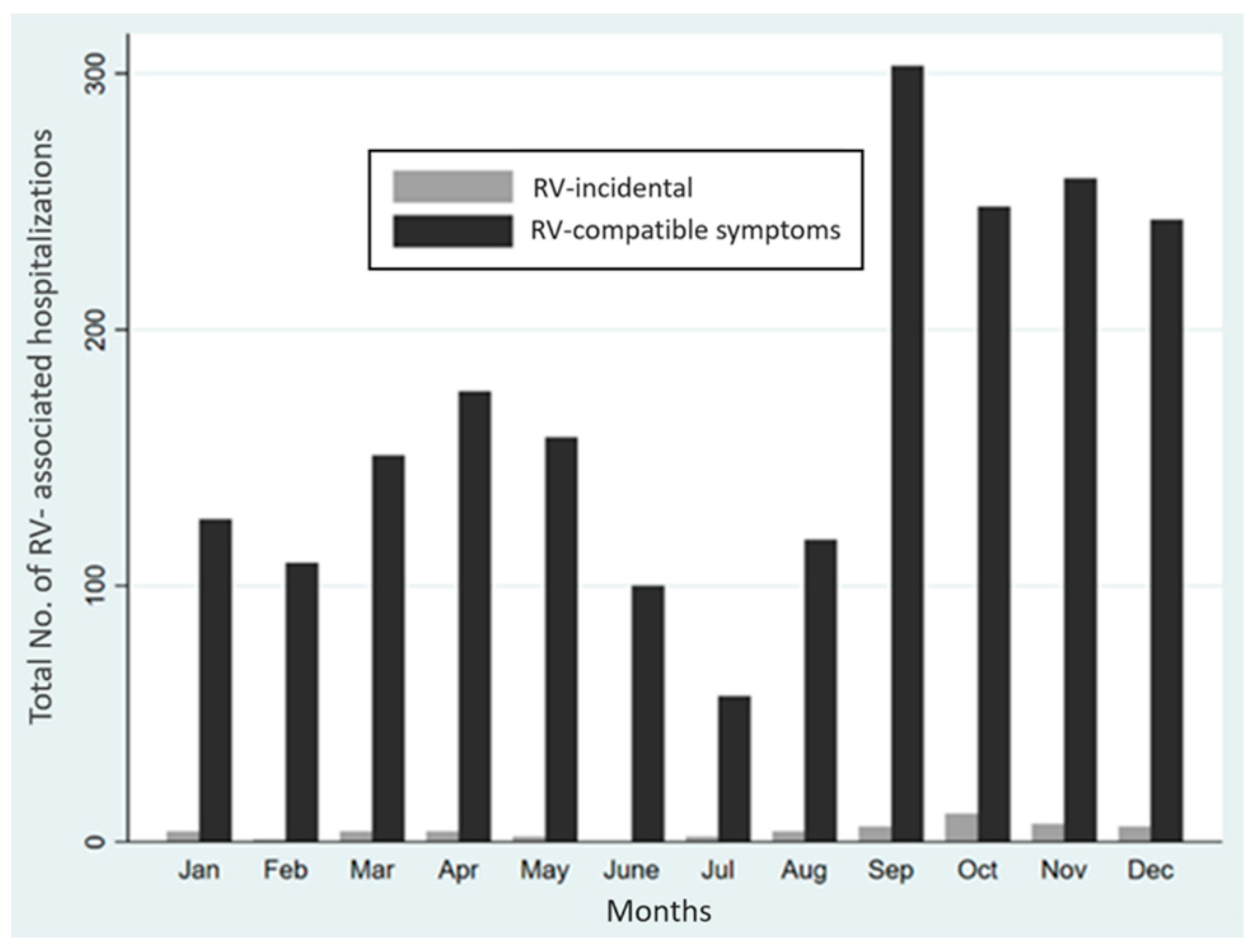
3.1. Study Patients, Diagnoses, and Seasonality of RV Infections
3.2. Demographic Characteristics and Underlying Diseases
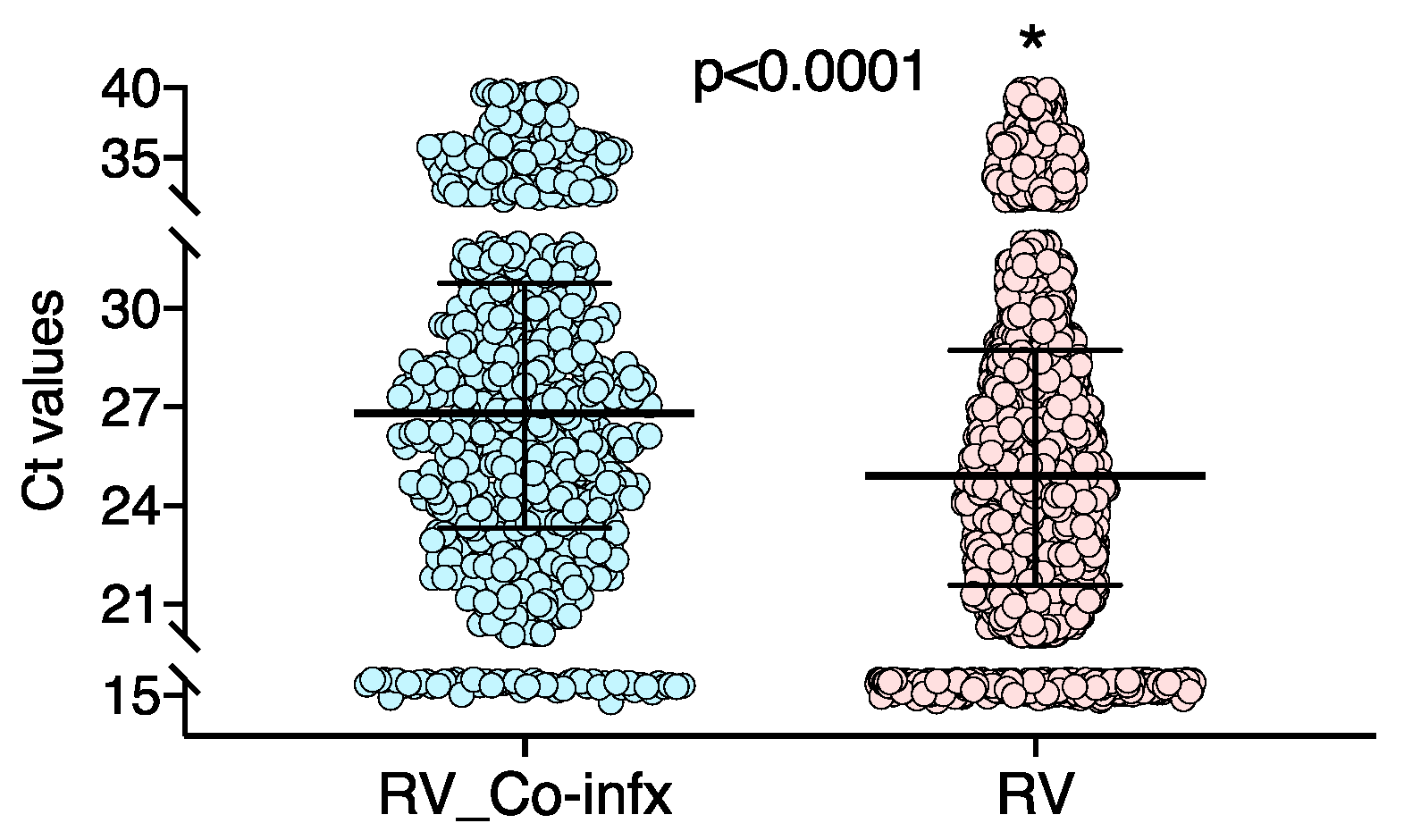
3.3. Viral and Bacterial Co-Infections
3.4. Disease Severity Parameters in Children with Compatible Symptoms and Incidental RV Detection
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Vandini, S.; Biagi, C.; Fischer, M.; Lanari, M. Impact of Rhinovirus Infections in Children. Viruses 2019, 11, 521. [Google Scholar] [CrossRef]
- Costa, L.F.; Queiróz, D.A.O.; Lopes da Silveira, H.; Bernardino Neto, M.; de Paula, N.T.; Oliveira, T.F.M.S.; Tolardo, A.L.; Yokosawa, J. Human Rhinovirus and Disease Severity in Children. Pediatrics 2014, 133, e312–e321. [Google Scholar] [CrossRef]
- Martin, E.K.; Kuypers, J.; Chu, H.Y.; Lacombe, K.; Qin, X.; Strelitz, B.; Bradford, M.; Jones, C.; Klein, E.J.; Englund, J.A. Molecular Epidemiology of Human Rhinovirus Infections in the Pediatric Emergency Department. J. Clin. Virol. 2015, 62, 25–31. [Google Scholar] [CrossRef]
- Gern, J.E. The ABCs of Rhinoviruses, Wheezing, and Asthma. J. Virol. 2010, 84, 7418–7426. [Google Scholar] [CrossRef]
- Miller, E.K.; Bugna, J.; Libster, R.; Shepherd, B.E.; Scalzo, P.M.; Acosta, P.L.; Hijano, D.; Reynoso, N.; Batalle, J.P.; Coviello, S.; et al. Human Rhinoviruses in Severe Respiratory Disease in Very Low Birth Weight Infants. Pediatrics 2012, 129, e60–e67. [Google Scholar] [CrossRef]
- Hartiala, M.; Lahti, E.; Forsström, V.; Vuorinen, T.; Ruuskanen, O.; Peltola, V. Characteristics of Hospitalized Rhinovirus-Associated Community-Acquired Pneumonia in Children, Finland, 2003–2014. Front. Med. (Lausanne) 2019, 6, 235. [Google Scholar] [CrossRef]
- Esposito, S.; Daleno, C.; Tagliabue, C.; Scala, A.; Tenconi, R.; Borzani, I.; Fossali, E.; Pelucchi, C.; Piralla, A.; Principi, N. Impact of Rhinoviruses on Pediatric Community-Acquired Pneumonia. Eur. J. Clin. Microbiol. Infect. Dis. 2012, 31, 1637–1645. [Google Scholar] [CrossRef] [PubMed]
- Brownlee, J.W.; Turner, R.B. New Developments in the Epidemiology and Clinical Spectrum of Rhinovirus Infections. Curr. Opin. Pediatr. 2008, 20, 67–71. [Google Scholar] [CrossRef] [PubMed]
- Jartti, T.; Söderlund-Venermo, M.; Hedman, K.; Ruuskanen, O.; Mäkelä, M.J. New Molecular Virus Detection Methods and Their Clinical Value in Lower Respiratory Tract Infections in Children. Paediatr. Respir. Rev. 2013, 14, 38–45. [Google Scholar] [CrossRef]
- Granados, A.; Goodall, E.C.; Luinstra, K.; Smieja, M.; Mahony, J. Comparison of Asymptomatic and Symptomatic Rhinovirus Infections in University Students: Incidence, Species Diversity, and Viral Load. Diagn. Microbiol. Infect. Dis. 2015, 82, 292–296. [Google Scholar] [CrossRef] [PubMed]
- Tomlinson, R.H.; Harrison, L.G.; Meals, E.A.; DeVincenzo, J.P. Do Asymptomatic Respiratory Viral Infections Occur? J. Clin. Virol. 2018, 102, 93–94. [Google Scholar] [CrossRef]
- Sundell, N.; Andersson, L.-M.; Brittain-Long, R.; Sundvall, P.-D.; Alsiö, Å.; Lindh, M.; Gustavsson, L.; Westin, J. PCR Detection of Respiratory Pathogens in Asymptomatic and Symptomatic Adults. J. Clin. Microbiol. 2019, 57. [Google Scholar] [CrossRef] [PubMed]
- Jansen, R.R.; Wieringa, J.; Koekkoek, S.M.; Visser, C.E.; Pajkrt, D.; Molenkamp, R.; de Jong, M.D.; Schinkel, J. Frequent Detection of Respiratory Viruses without Symptoms: Toward Defining Clinically Relevant Cutoff Values. J. Clin. Microbiol. 2011, 49, 2631–2636. [Google Scholar] [CrossRef] [PubMed]
- Peltola, V.; Waris, M.; Osterback, R.; Susi, P.; Ruuskanen, O.; Hyypiä, T. Rhinovirus Transmission within Families with Children: Incidence of Symptomatic and Asymptomatic Infections. J. Infect. Dis. 2008, 197, 382–389. [Google Scholar] [CrossRef] [PubMed]
- Moyer, K.; Wang, H.; Salamon, D.; Leber, A.; Mejias, A. Enterovirus D68 in Hospitalized Children: Sequence Variation, Viral Loads and Clinical Outcomes. PLoS ONE 2016, 11, e0167111. [Google Scholar] [CrossRef] [PubMed]
- Hung, H.-M.; Yang, S.-L.; Chen, C.-J.; Chiu, C.-H.; Kuo, C.-Y.; Huang, K.-Y.A.; Lin, T.-Y.; Hsieh, Y.-C.; Gong, Y.-N.; Tsao, K.-C.; et al. Molecular Epidemiology and Clinical Features of Rhinovirus Infections among Hospitalized Patients in a Medical Center in Taiwan. J. Microbiol. Immunol. Infect. 2019, 52, 233–241. [Google Scholar] [CrossRef]
- Chen, W.-J.; Arnold, J.C.; Fairchok, M.P.; Danaher, P.J.; McDonough, E.A.; Blair, P.J.; Garcia, J.; Halsey, E.S.; Schofield, C.; Ottolini, M.; et al. Epidemiologic, Clinical, and Virologic Characteristics of Human Rhinovirus Infection among Otherwise Healthy Children and Adults: Rhinovirus among Adults and Children. J. Clin. Virol. 2015, 64, 74–82. [Google Scholar] [CrossRef]
- Sánchez García, L.; Calvo, C.; Casas, I.; Pozo, F.; Pellicer, A. Viral Respiratory Infections in Very Low Birthweight Infants at Neonatal Intensive Care Unit: Prospective Observational Study. BMJ Paediatr. Open 2020, 4. [Google Scholar] [CrossRef]
- Comte, A.; Bour, J.-B.; Darniot, M.; Pitoiset, C.; Aho-Glélé, L.S.; Manoha, C. Epidemiological Characteristics and Clinical Outcomes of Human Rhinovirus Infections in a Hospitalized Population. Severity Is Independently Linked to RSV Coinfection and Comorbidities. J. Clin. Virol. 2020, 125, 104290. [Google Scholar] [CrossRef]
- Moesker, F.M.; van Kampen, J.J.A.; van Rossum, A.M.C.; de Hoog, M.; Koopmans, M.P.G.; Osterhaus, A.D.M.E.; Fraaij, P.L.A. Viruses as Sole Causative Agents of Severe Acute Respiratory Tract Infections in Children. PLoS ONE 2016, 11, e0150776. [Google Scholar] [CrossRef]
- Leotte, J.; Trombetta, H.; Faggion, H.Z.; Almeida, B.M.; Nogueira, M.B.; Vidal, L.R.; Raboni, S.M. Impact and Seasonality of Human Rhinovirus Infection in Hospitalized Patients for Two Consecutive Years. J. Pediatr. (Rio J) 2017, 93, 294–300. [Google Scholar] [CrossRef] [PubMed]
- Korppi, M.; Kotaniemi-Syrjänen, A.; Waris, M.; Vainionpää, R.; Reijonen, T.M. Rhinovirus-Associated Wheezing in Infancy: Comparison with Respiratory Syncytial Virus Bronchiolitis. Pediatr. Infect. Dis. J. 2004, 23, 995–999. [Google Scholar] [CrossRef] [PubMed]
- Miller, E.K.; Williams, J.V.; Gebretsadik, T.; Carroll, K.N.; Dupont, W.D.; Mohamed, Y.A.; Morin, L.-L.; Heil, L.; Minton, P.A.; Woodward, K.; et al. Host and Viral Factors Associated with Severity of Human Rhinovirus-Associated Infant Respiratory Tract Illness. J. Allergy Clin. Immunol. 2011, 127, 883–891. [Google Scholar] [CrossRef]
- Bergroth, E.; Aakula, M.; Elenius, V.; Remes, S.; Piippo-Savolainen, E.; Korppi, M.; Piedra, P.A.; Bochkov, Y.A.; Gern, J.E.; Camargo, C.A.; et al. Rhinovirus Type in Severe Bronchiolitis and the Development of Asthma. J. Allergy Clin. Immunol. Pr. 2020, 8, 588–595.e4. [Google Scholar] [CrossRef]
- Iwane, M.K.; Prill, M.M.; Lu, X.; Miller, E.K.; Edwards, K.M.; Hall, C.B.; Griffin, M.R.; Staat, M.A.; Anderson, L.J.; Williams, J.V.; et al. Human Rhinovirus Species Associated with Hospitalizations for Acute Respiratory Illness in Young US Children. J. Infect. Dis. 2011, 204, 1702–1710. [Google Scholar] [CrossRef] [PubMed]
- Annamalay, A.A.; Lanaspa, M.; Khoo, S.-K.; Madrid, L.; Acácio, S.; Zhang, G.; Laing, I.A.; Gern, J.; Goldblatt, J.; Bizzintino, J.; et al. Rhinovirus Species and Clinical Features in Children Hospitalised with Pneumonia from Mozambique. Trop. Med. Int. Health 2016, 21, 1171–1180. [Google Scholar] [CrossRef] [PubMed]
- Xiao, Q.; Zheng, S.; Zhou, L.; Ren, L.; Xie, X.; Deng, Y.; Tian, D.; Zhao, Y.; Fu, Z.; Li, T.; et al. Impact of Human Rhinovirus Types and Viral Load on the Severity of Illness in Hospitalized Children With Lower Respiratory Tract Infections. Pediatr. Infect. Dis. J. 2015, 34, 1187–1192. [Google Scholar] [CrossRef]
- Cox, D.W.; Khoo, S.-K.; Zhang, G.; Lindsay, K.; Keil, A.D.; Knight, G.; Gern, J.E.; Laing, I.A.; Bizzintino, J.; Le Souëf, P.N. Rhinovirus (RV) Is the Most Common Virus and RV-C the Most Common RV Species in Paediatric Intensive Care Respiratory Admissions. Eur. Respir. J. 2018, 52. [Google Scholar] [CrossRef] [PubMed]
- Heinonen, S.; Jartti, T.; Garcia, C.; Oliva, S.; Smitherman, C.; Anguiano, E.; de Steenhuijsen Piters, W.A.A.; Vuorinen, T.; Ruuskanen, O.; Dimo, B.; et al. Rhinovirus Detection in Symptomatic and Asymptomatic Children: Value of Host Transcriptome Analysis. Am. J. Respir. Crit. Care Med. 2016, 193, 772–782. [Google Scholar] [CrossRef]
- Jartti, T.; Bønnelykke, K.; Elenius, V.; Feleszko, W. Role of Viruses in Asthma. Semin Immunopathol. 2020, 42, 61–74. [Google Scholar] [CrossRef]
- Basnet, S.; Palmenberg, A.C.; Gern, J.E. Rhinoviruses and Their Receptors. Chest 2019, 155, 1018–1025. [Google Scholar] [CrossRef]
- Rovida, F.; Campanini, G.; Piralla, A.; Adzasehoun, K.M.G.; Sarasini, A.; Baldanti, F. Molecular Detection of Gastrointestinal Viral Infections in Hospitalized Patients. Diagn. Microbiol. Infect. Dis. 2013, 77, 231–235. [Google Scholar] [CrossRef] [PubMed]
- Jartti, T.; Gern, J.E. Role of Viral Infections in the Development and Exacerbation of Asthma in Children. J. Allergy Clin. Immunol. 2017, 140, 895–906. [Google Scholar] [CrossRef]
- Kennedy, J.L.; Turner, R.B.; Braciale, T.; Heymann, P.W.; Borish, L. Pathogenesis of Rhinovirus Infection. Curr. Opin. Virol. 2012, 2, 287–293. [Google Scholar] [CrossRef]
- Loughlin, D.W.; Coughlan, S.; De Gascun, C.F.; McNally, P.; Cox, D.W. The Role of Rhinovirus Infections in Young Children with Cystic Fibrosis. J. Clin. Virol. 2020, 129, 104478. [Google Scholar] [CrossRef] [PubMed]
- Van Piggelen, R.O.; van Loon, A.M.; Krediet, T.G.; Verboon-Maciolek, M.A. Human Rhinovirus Causes Severe Infection in Preterm Infants. Pediatr. Infect. Dis. J. 2010, 29, 364–365. [Google Scholar] [CrossRef]
- Seo, S.; Waghmare, A.; Scott, E.M.; Xie, H.; Kuypers, J.M.; Hackman, R.C.; Campbell, A.P.; Choi, S.-M.; Leisenring, W.M.; Jerome, K.R.; et al. Human Rhinovirus Detection in the Lower Respiratory Tract of Hematopoietic Cell Transplant Recipients: Association with Mortality. Haematologica 2017, 102, 1120–1130. [Google Scholar] [CrossRef] [PubMed]
- Campbell, A.P.; Guthrie, K.A.; Englund, J.A.; Farney, R.M.; Minerich, E.L.; Kuypers, J.; Corey, L.; Boeckh, M. Clinical Outcomes Associated with Respiratory Virus Detection before Allogeneic Hematopoietic Stem Cell Transplant. Clin. Infect. Dis. 2015, 61, 192–202. [Google Scholar] [CrossRef]
- Ahn, J.G.; Kim, D.S.; Kim, K.H. Clinical Characteristics and Cytokine Profiles of Children with Acute Lower Respiratory Tract Infections Caused by Human Rhinovirus. PLoS ONE 2018, 13, e0198624. [Google Scholar] [CrossRef]
- Chu, H.Y.; Englund, J.A.; Strelitz, B.; Lacombe, K.; Jones, C.; Follmer, K.; Martin, E.K.; Bradford, M.; Qin, X.; Kuypers, J.; et al. Rhinovirus Disease in Children Seeking Care in a Tertiary Pediatric Emergency Department. J. Pediatric Infect. Dis. Soc. 2016, 5, 29–38. [Google Scholar] [CrossRef]
- Takeyama, A.; Hashimoto, K.; Sato, M.; Sato, T.; Kanno, S.; Takano, K.; Ito, M.; Katayose, M.; Nishimura, H.; Kawasaki, Y.; et al. Rhinovirus Load and Disease Severity in Children with Lower Respiratory Tract Infections. J. Med. Virol. 2012, 84, 1135–1142. [Google Scholar] [CrossRef] [PubMed]
- Jartti, T.; Korppi, M. Rhinovirus-Induced Bronchiolitis and Asthma Development. Pediatr. Allergy Immunol. 2011, 22, 350–355. [Google Scholar] [CrossRef]
- Esposito, S.; Daleno, C.; Scala, A.; Castellazzi, L.; Terranova, L.; Sferrazza Papa, S.; Longo, M.R.; Pelucchi, C.; Principi, N. Impact of Rhinovirus Nasopharyngeal Viral Load and Viremia on Severity of Respiratory Infections in Children. Eur. J. Clin. Microbiol. Infect. Dis. 2014, 33, 41–48. [Google Scholar] [CrossRef]
- Miller, E.K.; Lu, X.; Erdman, D.D.; Poehling, K.A.; Zhu, Y.; Griffin, M.R.; Hartert, T.V.; Anderson, L.J.; Weinberg, G.A.; Hall, C.B.; et al. Rhinovirus-Associated Hospitalizations in Young Children. J. Infect. Dis. 2007, 195, 773–781. [Google Scholar] [CrossRef] [PubMed]
- To, K.K.W.; Lau, S.K.P.; Chan, K.-H.; Mok, K.-Y.; Luk, H.K.H.; Yip, C.C.Y.; Ma, Y.-K.; Sinn, L.H.Y.; Lam, S.H.Y.; Ngai, C.-W.; et al. Pulmonary and Extrapulmonary Complications of Human Rhinovirus Infection in Critically Ill Patients. J. Clin. Virol. 2016, 77, 85–91. [Google Scholar] [CrossRef]
- Nicholson, E.G.; Avadhanula, V.; Ferlic-Stark, L.; Patel, K.; Gincoo, K.E.; Piedra, P.A. The Risk of Serious Bacterial Infection in Febrile Infants 0–90 Days of Life With a Respiratory Viral Infection. Pediatr. Infect. Dis. J. 2019, 38, 355–361. [Google Scholar] [CrossRef] [PubMed]
| Diagnosis | N (%) |
|---|---|
| URTI | 680 (29.62) |
| Bronchiolitis | 483 (21.04) |
| Asthma exacerbation | 454 (19.80) |
| Pneumonia | 228 (9.93) |
| LRTI | 109 (4.74) |
| Respiratory failure | 160 (7.00) |
| Apnea | 5 (0.20) |
| Hypoxemia | 11 (0.47) |
| CF exacerbation | 46 (2.00) |
| Ventilator-associated pneumonia | 47 (2.04) |
| AOM/sinusitis | 26 (1.13) |
| Airway malacia exacerbation | 1 (0.04) |
| Other | 2 (0.09) |
| Diagnosis | N (%) |
|---|---|
| Cardiovascular | 24 (26.37) |
| GERD | 19 (20.87) |
| Neurological disorders | 13 (14.28) |
| Immunocompromised | 7 (7.70) |
| Kawasaki Disease | 6 (6.59) |
| Seizures | 5 (5.49) |
| Routine health examination | 4 (4.40) |
| Hematologic disease | 4 (4.40) |
| Syndromes | 2 (2.20) |
| Sepsis/shock | 2 (2.20) |
| Neuromuscular disorders | 1 (1.10) |
| Endocrine disorders | 1 (1.10) |
| Prematurity | 1 (1.10) |
| Surgery | 1 (1.10) |
| Trauma | 1 (1.10) |
| RV Symptoms Group (n = 2382) | RV Incidental Group (n = 91) | p Value | |
|---|---|---|---|
| Demographic Characteristics | |||
| Age, (months) | 14.35 (3.9–49.3) | 14.10 (3.8–38.1) | 0.844 |
| Sex, n (%) male | 1404 (58.94) | 55 (60.44) | 0.776 |
| Race or ethnic group, n (%) | 0.449 | ||
| White | 1320 (55.42) | 58 (63.74) | |
| Black or African American | 641 (26.91) | 19 (20.88) | |
| Biracial | 88 (7.89) | 5 (5.49) | |
| Other | 233 (9.78) | 9 (9.89) | |
| Underlying diseases, n (%) | 1886 (79.17) | 71 (78.02) | 0.031 |
| Asthma/atopy/allergy | 795 (42.15) | 13 (18.31) | 0.012 |
| Genetic syndromes | 256 (13.57) | 18 (25.35) | 0.096 |
| Prematurity | 251 (13.31) | 9 (12.68) | 0.774 |
| Gastrointestinal diseases | 82 (4.34) | 4 (5.63) | 0.734 |
| Congenital heart disease | 83 (4.40) | 10 (14.08) | 0.007 |
| Neurological disorders | 58 (3.08) | 3 (4.23) | 0.695 |
| Cystic fibrosis | 46 (2.44) | 0 (0.00) | - |
| Respiratory tract morbidity a | 55 (2.92) | 2 (2.82) | 0.891 |
| Immunodeficiencies | 35 (1.86) | 4 (5.63) | 0.070 |
| Hematologic disease | 23 (1.22) | 1 (1.41) | 0.943 |
| Other b | 202 (10.71) | 7 (9.86) | 0.735 |
| RV Symptoms Group (n = 2382) | RV Incidental Group (n = 91) | p Value | |
|---|---|---|---|
| Viral co-infections a | 532/2382 (22.33) | 10/91(10.99) | 0.010 |
| Adenovirus | 241 (10.12) | 8 (8.79) | 0.679 |
| RSV | 185 (7.77) | 0 (0) | 0.006 |
| Parainfluenza | 98 (4.12) | 1 (1.10) | 0.150 |
| hMPV | 53 (2.23) | 2 (2.20) | 0.986 |
| Influenza A | 9 (0.38) | 0 (0) | 0.557 |
| Influenza B | 6 (0.25) | 0 (0) | 0.632 |
| RV viral loads | 25.2 (22.05–29.04) | 25.6 (22.09–29.07) | 0.934 |
| Bacterial co-infections b | |||
| Blood culture | 21/1076 (1.95) | 3/39 (7.69) | 0.015 |
| Cerebrospinal fluid culture | 2/235 (0.85) | 1/13 (7.69) | 0.028 |
| Urine culture | 41/566(7.24) | 1/17 (5.88) | 0.831 |
| AL culture | 14/38 (34.84) | 3/3 (100) | 0.064 |
| Lower respiratory culture | 91/243 (37.44) | 3/4 (75) | 0.156 |
| Cystic fibrosis culture | 11/32 (34.38) | 0/0 (0) | - |
| Other cultures c | 45/212 (21.23) | 2/12 (16.67) | 0.706 |
| RV Symptoms Group (n = 2382) | RV Incidental Group (n = 91) | Odds Ratio (Upper-Lower CI) | p Value | |
|---|---|---|---|---|
| Hospitalization | 2048 (85.98) | 51 (56.4) | 4.80 (3.12–7.39) | 0.0001 |
| PICU | 743 (31.19) | 9 (9.89) | 4.13 (2.06–8.26) | 0.0001 |
| Length of stay a | 2.4 (1.5–4.7) | 1.7 (1–3.1) | 1.90 (1.14–3.17) | 0.013 |
| Length of stay in PICU b | 2.4 (1.4–4.7) | 1.6 (1.2–2.6) | 3.30 (0.82–13.32) | 0.093 |
| Suplemental oxygen | ||||
| Requirement, n (%) | 1278 (53.65) | 8 (8.79) | 12.01(5.78–24.92) | 0.0001 |
| Duration (days) c | 2 (1–4) | 2.5(1.5–6) | 0.95 (0.19–4.74) | 0.953 |
| Oxygen administration via | ||||
| Nasal Cannula | 736 (57.59) | 5 (62.50) | 1.71 (0.40–7.24) | 0.461 |
| NIV | 285 (22.30) | 0 (0) | - | - |
| Mechanical ventilation | 257 (20.11) | 3 (37.50) | 0.58 (0.13–2.45) | 0.461 |
| Hospitalization (OR, 95% CI) p-Value | PICU (OR, 95% CI) p-Value | Length of Stay (OR, 95% CI) p-Value | Supplemental Oxygen (OR, 95% CI) p-Value | |||||
|---|---|---|---|---|---|---|---|---|
| Age | 1.06 (1.03–1.09) | 0.0001 | 1.07 (1.05–1.09) | 0.0001 | 1.10 (1.08–1.13) | 0.0001 | 1.08 (1.06–1.10) | 0.0001 |
| Female | 0.90 (0.72–1.13) | 0.386 | 0.96 (0.80–1.14) | 0.662 | 0.98 (0.82–1.17) | 0.838 | 0.94 (0.80–1.11) | 0.494 |
| RV viral loads | 0.99 (0.97–1.01) | 0.319 | 0.97 (0.95–0.99) | 0.004 | 0.98 (0.96–1.00) | 0.090 | 0.99 (0.97–1.00) | 0.087 |
| RV viral co-infections a | 0.73 (0.57–0.95) | 0.021 | 1.2 (0.96–1.4) | 0.094 | 1.04 (0.84–1.29) | 0.682 | 1.11 (0.91–1.35) | 0.314 |
| Compatible symptoms | 4.99 (3.23–7.73) | 0.0001 | 3.9 (1.95–7.92) | 0.0001 | 2.03 (1.20–3.42) | 0.008 | 11.86 (5.68–24.76) | 0.0001 |
| Underlying diseases | 1.01 (0.98–1.04) | 0.650 | 0.98 (0.96–1.00) | 0.121 | 1.02 (1.00–1.04) | 0.030 | 0.98 (0.96–1.00) | 0.059 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sanchez-Codez, M.I.; Moyer, K.; Benavente-Fernández, I.; Leber, A.L.; Ramilo, O.; Mejias, A. Viral Loads and Disease Severity in Children with Rhinovirus-Associated Illnesses. Viruses 2021, 13, 295. https://doi.org/10.3390/v13020295
Sanchez-Codez MI, Moyer K, Benavente-Fernández I, Leber AL, Ramilo O, Mejias A. Viral Loads and Disease Severity in Children with Rhinovirus-Associated Illnesses. Viruses. 2021; 13(2):295. https://doi.org/10.3390/v13020295
Chicago/Turabian StyleSanchez-Codez, Maria I., Katherine Moyer, Isabel Benavente-Fernández, Amy L. Leber, Octavio Ramilo, and Asuncion Mejias. 2021. "Viral Loads and Disease Severity in Children with Rhinovirus-Associated Illnesses" Viruses 13, no. 2: 295. https://doi.org/10.3390/v13020295
APA StyleSanchez-Codez, M. I., Moyer, K., Benavente-Fernández, I., Leber, A. L., Ramilo, O., & Mejias, A. (2021). Viral Loads and Disease Severity in Children with Rhinovirus-Associated Illnesses. Viruses, 13(2), 295. https://doi.org/10.3390/v13020295






