Effect of Pre-Conditioning Temperature and Method of Curing on the Shear Bond Strength of Dual-Cure Composite Cements to Dentin
Abstract
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
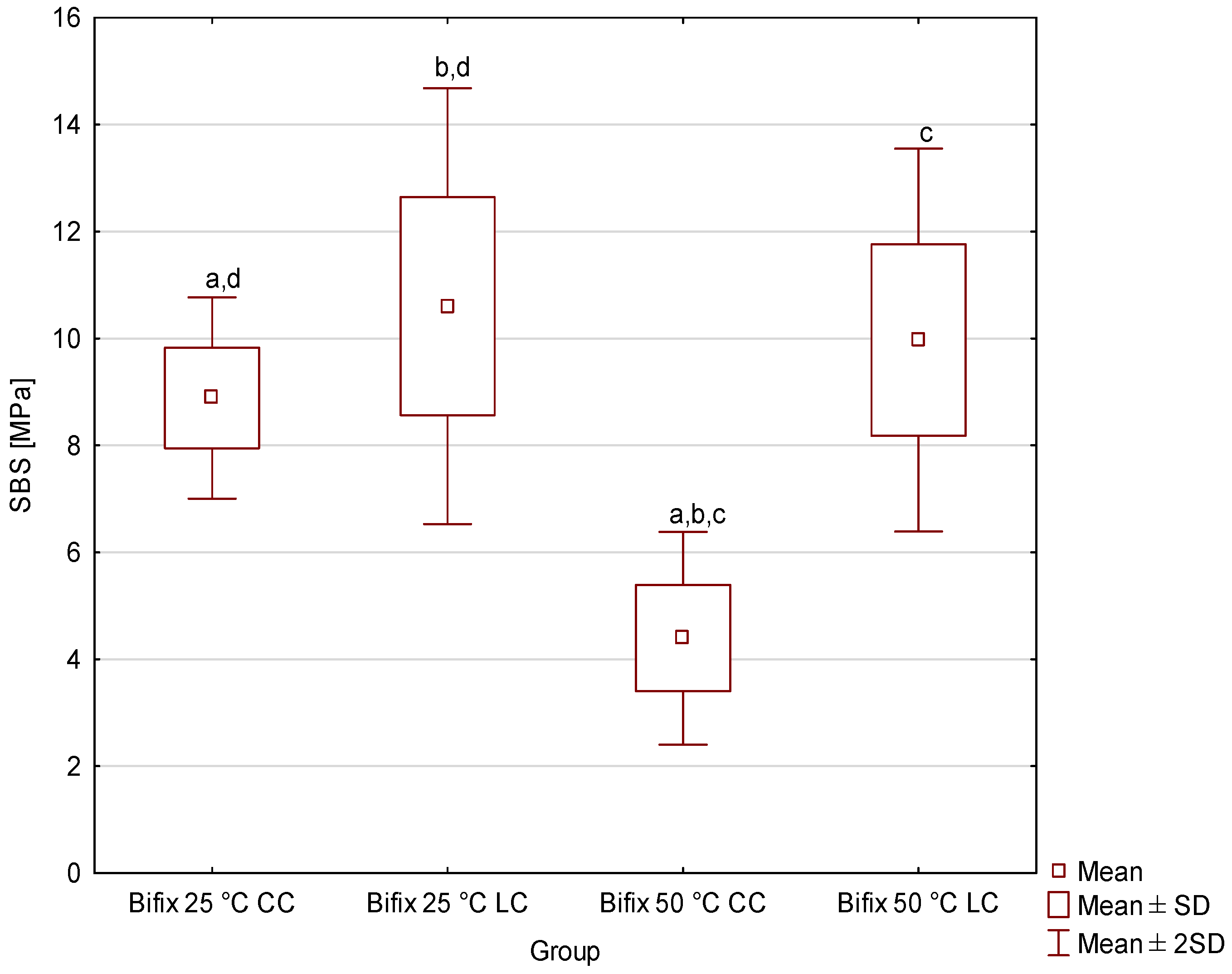
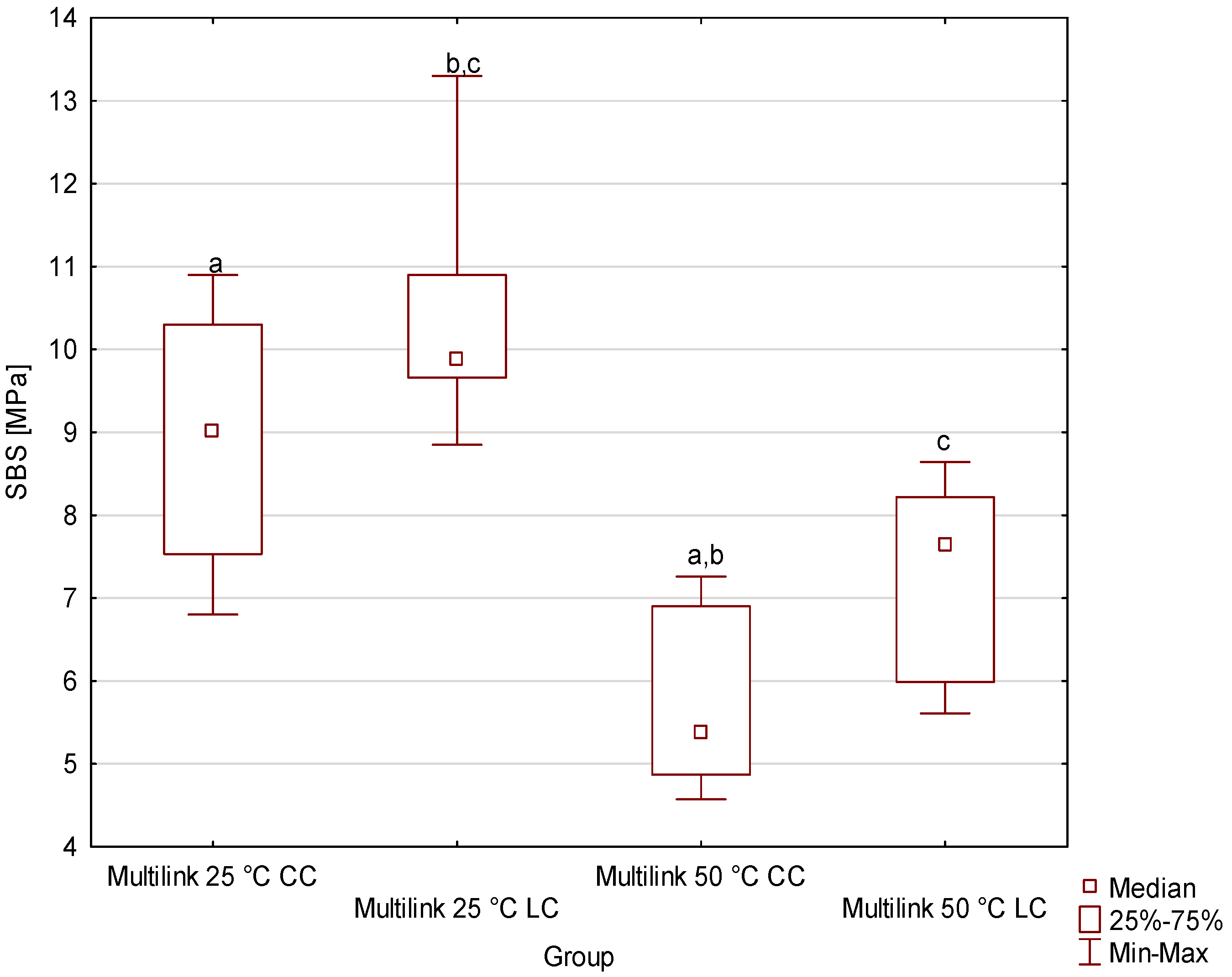
- The storage temperature of dual composite cements significantly affects their bond strength to dentin. Cements with benzoyl peroxide as an initiator, when stored at 50 °C, exhibited lower shear bond strength (SBS) than those stored at 25 °C, confirming their sensitivity to adverse thermal conditions.
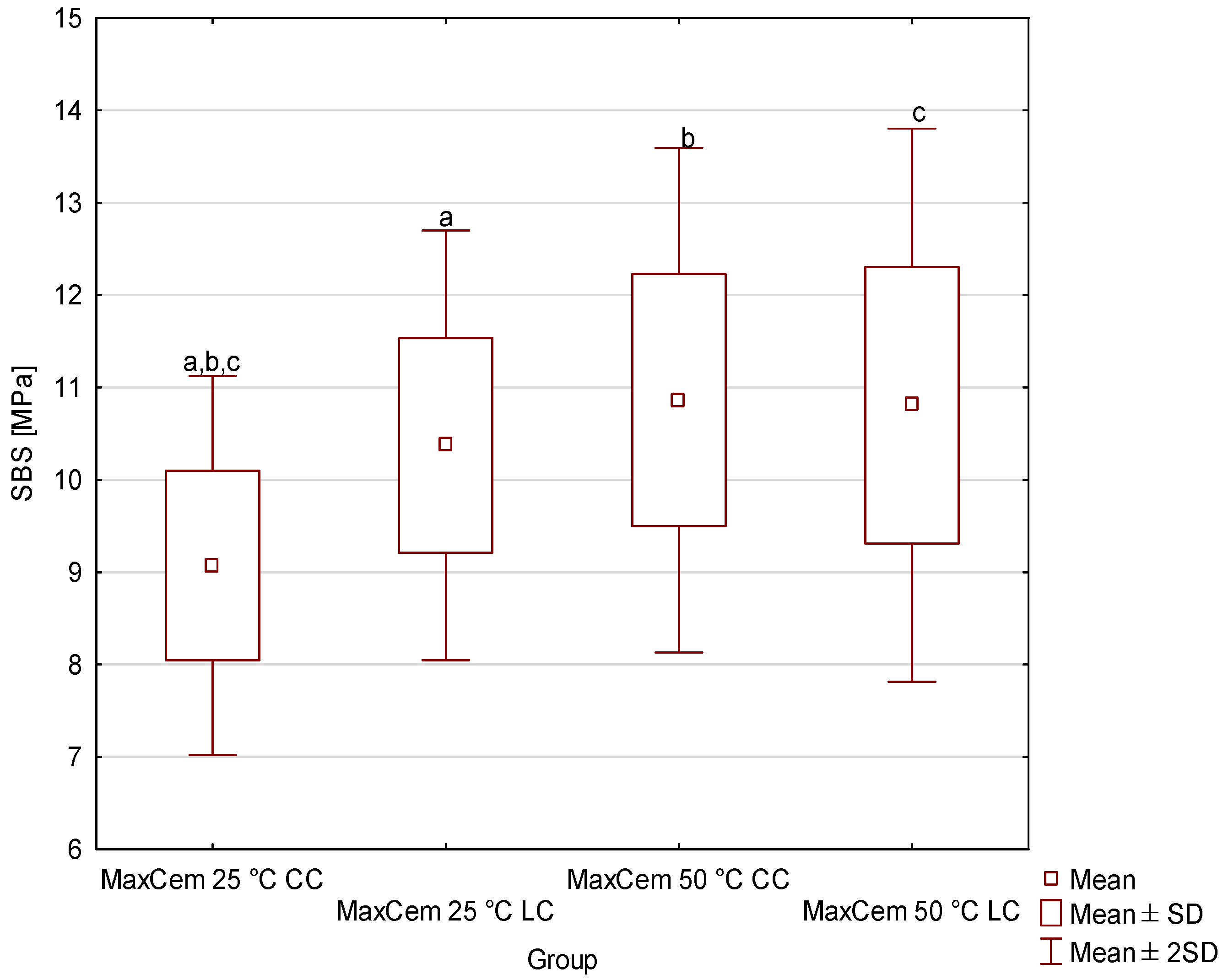
- Despite the lack of statistical significance, light-activated cements (LC) consistently demonstrated numerically higher shear bond strength (SBS) than chemically cured cements (CC) across all storage temperatures. This pattern suggests that light activation may play a key role in ensuring optimal bond strength of the material to dentin.
- MaxCem Elite exhibited the highest temperature stability due to its proprietary redox initiator system.
- The analysis of the results indicates that both the type of activation and the chemical composition of the cement determine its behavior under elevated temperature conditions.
- In clinical practice, it is recommended to store cements under conditions in accordance with the manufacturer’s instructions and to use light activation wherever possible to increase the durability of the bond with tooth tissues.
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Strazzi-Sahyon, H.B.; Hadis, M.A.; dos Santos, P.H.; Palin, W.M. The effect of photoinitiator type and filler load on physicochemical and mechanical properties of experimental light-cured resin cements through lithium disilicate ceramics of different shades and thicknesses. Dent. Mater. 2024, 40, 1452–1463. [Google Scholar] [CrossRef]
- Attar, N.; Tam, L.E. Mechanical and physical properties of contemporary dental luting agents. J. Prosthet. Dent. 2003, 89, 127–134. [Google Scholar] [CrossRef]
- Guimarães, R.C.C.; de Oliveira, D.; Rocha, M.G.; Roulet, J.F.; Geraldeli, S.; Sinhoreti, M.A.C. Effect of glass-ceramic thickness on the degree of conversion, polymerization shrinkage stress, and bond strength of resin cements. Int. J. Adhes. Adhes. 2024, 136, 103871. [Google Scholar] [CrossRef]
- Souza, G.; Braga, R.R.; Cesar, P.F.; Lopes, G.C. Correlation between clinical performance and degree of conversion of resin cements: A literature review. J. Appl. Oral Sci. 2015, 23, 358–368. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.-Y.; Cho, C.-B.; Koak, J.-Y.; Yang, S.-E. The effect of zirconia thickness and curing time on shear bond strength of dual-cure resin cement. Dent. Mater. J. 2016, 35, 132–137. [Google Scholar] [CrossRef] [PubMed]
- Arrais, C.A.G.; Giannini, M.; Rueggeberg, F.A.; Waller, J.L.; de Góes, M.F. Effect of curing mode on the polymerization characteristics of dual-cured resin cement systems. J. Dent. 2008, 36, 418–426. [Google Scholar] [CrossRef]
- Hofmann, N.; Papsthart, G.; Hugo, B.; Klaiber, B. Comparison of photo-activation versus chemical or dual-curing of resin-based luting cements regarding flexural strength, modulus and surface hardness. J. Oral Rehabil. 2001, 28, 1022–1028. [Google Scholar] [CrossRef]
- Aldhafyan, M.; Silikas, N.; Watts, D.C. Influence of curing modes on conversion and shrinkage of dual-cure resin cements. Dent. Mater. 2022, 38, 318–327. [Google Scholar] [CrossRef]
- D’Alessandro, C.; Baena, E.; Josic, U.; Maravic, T.; Mancuso, E.; Ceballos, L.; Mazzoni, A.; Blatz, M.B.; Breschi, L.; Mazzitelli, C. Tack-cure vs. conventional polymerization methods: A systematic review on resin composite cements’ properties. J. Dent. 2025, 160, 105917. [Google Scholar] [CrossRef]
- Patussi, A.F.C.; Ramacciato, J.C.; da Silva, J.G.R.; Nascimento, V.R.P.; Campos, D.E.S.; de Araújo Ferreira Muniz, I.; de Souza, G.M.; Lima, R.B.W. Preheating of dental composite resins: A scoping review. J. Esthet. Restor. Dent. 2023, 35, 646–656. [Google Scholar] [CrossRef]
- Maucoski, C.; Guarneri, J.A.G.; Farrar, P.; Price, R.B. Influence of temperature and primer application on setting time and degree of conversion of a dual-cure self-adhesive cement. J. Dent. 2025, 160, 105859. [Google Scholar] [CrossRef] [PubMed]
- Lemon, D.J.; Chen, W.; Smith, T.; Ford, A.F.; Moffett, S.X.; Hoyle, J.T.; Hamlin, N.J.; Hwang, Y.Y. The effect of simulated field storage conditions on dental restorative materials for military field use. Mil. Med. 2020, 185, e831–e838. [Google Scholar] [CrossRef] [PubMed]
- Hondrum, S.O. Storage stability of dental luting agents. J. Prosthet. Dent. 1999, 81, 467–472. [Google Scholar] [CrossRef] [PubMed]
- Sadr, A.; Ghasemi, A.; Shimada, Y.; Tagami, J. Effects of storage time and temperature on the properties of two self-etching systems. J. Dent. 2007, 35, 218–225. [Google Scholar] [CrossRef]
- Loher, H.; Behr, M.; Hintereder, U.; Rosentritt, M.; Handel, G. The impact of cement mixing and storage errors on the risk of failure of glass–ceramic crowns. Clin. Oral Investig. 2009, 13, 217–222. [Google Scholar] [CrossRef]
- Giełzak, J.; Szczesio-Włodarczyk, A.; Bociong, K. Effect of storage temperature on selected strength parameters of dual-cured composite cements. J. Funct. Biomater. 2023, 14, 487. [Google Scholar] [CrossRef]
- Deb, S.; Di Silvio, L.; Mackler, H.E.; Millar, B.J. Pre-warming of dental composites. Dent. Mater. 2011, 27, e51–e59. [Google Scholar] [CrossRef]
- Ayub, K.V.; Santos, G.C., Jr.; Rizkalla, A.S.; Bohay, R.; Pegoraro, L.F.; Rubo, J.H.; Santos, M.J. Effect of preheating on microhardness and viscosity of four resin composites. J. Can. Dent. Assoc. 2014, 80, e12. [Google Scholar]
- Muñoz, C.A.; Bond, P.R.; Sy-Muñoz, J.; Tan, D.; Peterson, J. Effect of pre-heating on depth of cure and surface hardness of light polymerized resin composites. Am. J. Dent. 2008, 21, 215–222. [Google Scholar]
- Morais, A.; Santos, A.; Giannini, M.; Reis, A.F.; Rodrigues, J.A.; Arrais, C.A. Effect of pre-heated dual-cured resin cements on the bond strength of indirect restorations to dentin. Braz. Oral Res. 2012, 26, 170–176. [Google Scholar] [CrossRef]
- ISO 11405:2015; Dentistry—Testing of Adhesion to Tooth Structure. International Organization for Standardization: Geneva, Switzerland, 2015.
- Pires Lopes, L.C.P.; Suga Terada, R.S.; Tsuzuki, F.M.; Giannini, M.; Hirata, R. Heating and preheating of dental restorative materials—A systematic review. Clin. Oral Investig. 2020, 24, 4225–4235. [Google Scholar] [CrossRef] [PubMed]
- França, F.A.; de Oliveira, M.; Rodrigues, J.A.; de Galvão Arrais, C.A. Pre-heated dual-cured resin cements: Analysis of the degree of conversion and ultimate tensile strength. Braz. Oral Res. 2011, 25, 174–179. [Google Scholar] [CrossRef] [PubMed]
- Lima, M.O.; Catelan, A.; Marchi, G.M.; Lima, D.A.; Martins, L.R.; Aguiar, F.H. Influence of pre-heating and ceramic thickness on physical properties of luting agents. J. Appl. Biomater. Funct. Mater. 2018, 16, 252–259. [Google Scholar] [CrossRef] [PubMed]
- Alizadeh Oskoee, P.; Nooroloyouni, A.; Pornaghi Azar, F.; Sajjadi, S.; Oskoee, J.S.; Pirzadeh Ashraf, A. Effect of resin cement preheating on the push-out bond strength of fiber post to root canal dentin. J. Dent. Res. Dent. Clin. Dent. Prospect. 2015, 9, 233–238. [Google Scholar] [CrossRef]
- Zaman, F.; Beezer, A.E.; Mitchell, J.C.; Clarkson, Q.; Elliott, J.; Davis, A.F.; Willson, R.J. The stability of benzoyl peroxide by isothermal microcalorimetry. Int. J. Pharm. 2001, 227, 133–137. [Google Scholar] [CrossRef]
- Cantoro, A.; Goracci, C.; Papacchini, F.; Mazzitelli, C.; Fadda, G.M.; Ferrari, M. Effect of pre-cure temperature on the bonding potential of self-etch and self-adhesive resin cements. Dent. Mater. 2007, 23, 561–567. [Google Scholar] [CrossRef]
- Cantoro, A.; Goracci, C.; Carvalho, C.A.; Coniglio, I.; Ferrari, M. Bonding potential of self-adhesive luting agents used at different temperatures to lute composite onlays. J. Dent. 2009, 37, 454–461. [Google Scholar] [CrossRef]
- Klaisiri, A.; Thamrongananskul, N. Effect of storage temperatures on the shear bond strength of three resin cements to dentin. J. Dent. Assoc. Thai. 2019, 69, 33–41. [Google Scholar]
- Ozer, F.; Ovecoglu, H.S.; Daneshmehr, L.; Sinmazisik, G.; Kashyap, K.; Iriboz, E.; Blatz, M.B. Effect of storage temperature on the shelf life of self-adhesive resin cements. J. Adhes. Dent. 2015, 17, 545–550. [Google Scholar] [CrossRef]
- Brauer, G.M.; Petrianyk, N.; Termini, D.J.; Davis, R.D. Storage stability of dental composites. J. Dent. Res. 1979, 58, 1791–1800. [Google Scholar] [CrossRef]
- David-Pérez, M.; Ramírez-Suárez, J.P.; Latorre-Correa, F.; Agudelo-Suárez, A.A. Degree of conversion of resin-cements (light-cured/dual-cured) under different thicknesses of vitreous ceramics: Systematic review. J. Prosthodont. Res. 2022, 66, 385–394. [Google Scholar] [CrossRef]
- The elite of self-adhesive resin cements. Br. Dent. J. 2015, 219, 592. [CrossRef]
- Maravić, T.; Mazzitelli, C.; Mancuso, E.; Del Bianco, F.; Josić, U.; Cadenaro, M.; Breschi, L.; Mazzoni, A. Resin composite cements: Current status and a novel classification proposal. J. Esthet. Restor. Dent. 2023, 35, 1085–1097. [Google Scholar] [CrossRef] [PubMed]
- Ferracane, J.L.; Stansbury, J.W.; Burke, F.J.T. Self-adhesive resin cements—Chemistry, properties and clinical considerations. J. Oral Rehabil. 2011, 38, 295–314. [Google Scholar] [CrossRef] [PubMed]
- Pongprueksa, P.; Miletic, V.; De Munck, J.; Brooks, N.R.; Meersman, F.; Nies, E.; Van Meerbeek, B.; Van Landuyt, K.L. Effect of evaporation on the shelf life of a universal adhesive. Oper. Dent. 2014, 39, 500–507. [Google Scholar] [CrossRef] [PubMed]
- Iliev, G.; Hardan, L.; Kassis, C.; Bourgi, R.; Cuevas-Suárez, C.E.; Lukomska-Szymanska, M.; Mancino, D.; Haikel, Y.; Kharouf, N. Shelf life and storage conditions of universal adhesives: A literature review. Polymers 2021, 13, 2708. [Google Scholar] [CrossRef]

| Cement | Polymer Matrix/Monomers | Fillers/Initiators | Filler Content |
|---|---|---|---|
| Multilink Automix (Ivoclare Vivadent) | Dimethacrylates (22–26%) HEMA (6–7%) Benzoyl peroxide (<1%) Stabilizers Pigments | Ytterbium trifluoride | Not specified in SDS |
| EnaCem HF (Micerdent) | Tetramethylene dimethacrylate (2.5–10%) Dibenzoyl peroxide (<2.5%) Diphenyl (2,4,6-trimethylbenzoyl)phosphine oxide (<2.5%) | Not specified in SDS | Not specified in SDS |
| MaxCem Elite (Kerr) | 1,6-hexanediyl bismethacrylate (5–10%) 2-hydroxy-1,3-propanediyl bismethacrylate (5–10%) 7,7,9 (or 7,9,9)-trimethyl-4,13-dioxo-3,14-dioxa-5,12-diazahexadecane-1,16-diyl bismethacrylate (1–5%) 3-trimethoxysilylpropyl methacrylate (1–5%) | Barium aluminoborosilicate glass (30–60%) Ytterbium fluoride (10–30%) Fumed silica (1–5%) | Not specified in SDS |
| Bifix Hybrid Abutment (VOCO) | Urethanedimethacrylate (5–10%) Glycerindimethacrylate (5–10%) BIS-GMA (5–10%) Acidic adhesive monomer (5–10%) Hydroxypropyl methacrylate (2.5–5%) Benzoyl peroxide (≤2.5%) Catalyst, unspecified (1–2.5%), Initiator, unspecified | Not specified in SDS | Not specified in SDS |
| Material | Type/Characteristics | Manufacturer (Country) | Application Procedure |
|---|---|---|---|
| 37% phosphoric acid (Blue Etch) | Etching gel for enamel and dentin | Arkona Dental, Nasutów, Poland | Applied to the dentin surface for 15 s, rinsed thoroughly with water, and gently air-dried, leaving a slightly moist surface |
| Solo Bond Plus | Single-component, light-curing etch-and rinse adhesive system | VOCO GmbH, Cuxhaven, Germany | A uniform layer was applied and rubbed for approximately 20 s, gently air-thinned, and light-cured for 10 s using an LED unit (≥1000 mW/cm2) |
| Bifix Hybrid Abutment | Dual-cure composite cement | VOCO GmbH, Cuxhaven, Germany | The cement was applied onto the dentin surface covered with an adhesive layer; the element was seated, excess cement removed, left for 90 s, and then light-cured for 20 s (LC) or allowed to self-polymerize (CC) |
| MaxCem Elite | Self-adhesive dual-cure composite cement | Kerr, Orange, CA, USA | The cement was applied without prior adhesive use; the element was positioned, excess cement removed, left for 90 s, and then light-cured for 20 s (LC) or allowed to self-polymerize (CC) |
| EnaCem HF | Dual-cure composite cement | Micerium, Avegno, Italy | The cement was applied onto the dentin surface pretreated with an adhesive, left for 90 s, and then light-cured for 20 s (LC) or allowed to self-polymerize (CC) |
| Multilink Automix | Dual-cure composite cement | Ivoclar Vivadent, Schaan, Liechtenstein | The cement was applied onto the dentin surface covered with an adhesive layer, excess cement removed, left for 90 s, and light-cured for 20 s (LC) or allowed to self-polymerize (CC) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.
Share and Cite
Giełzak, J.; Szczesio-Włodarczyk, A.; Bociong, K. Effect of Pre-Conditioning Temperature and Method of Curing on the Shear Bond Strength of Dual-Cure Composite Cements to Dentin. Materials 2026, 19, 718. https://doi.org/10.3390/ma19040718
Giełzak J, Szczesio-Włodarczyk A, Bociong K. Effect of Pre-Conditioning Temperature and Method of Curing on the Shear Bond Strength of Dual-Cure Composite Cements to Dentin. Materials. 2026; 19(4):718. https://doi.org/10.3390/ma19040718
Chicago/Turabian StyleGiełzak, Joanna, Agata Szczesio-Włodarczyk, and Kinga Bociong. 2026. "Effect of Pre-Conditioning Temperature and Method of Curing on the Shear Bond Strength of Dual-Cure Composite Cements to Dentin" Materials 19, no. 4: 718. https://doi.org/10.3390/ma19040718
APA StyleGiełzak, J., Szczesio-Włodarczyk, A., & Bociong, K. (2026). Effect of Pre-Conditioning Temperature and Method of Curing on the Shear Bond Strength of Dual-Cure Composite Cements to Dentin. Materials, 19(4), 718. https://doi.org/10.3390/ma19040718








