Predictive Parameters of Oral Health Quality of Life in Complete Mandibular Denture Wearers Stabilized by Mini-Implants: A Two-Year Follow-Up Study
Abstract
1. Introduction
2. Results
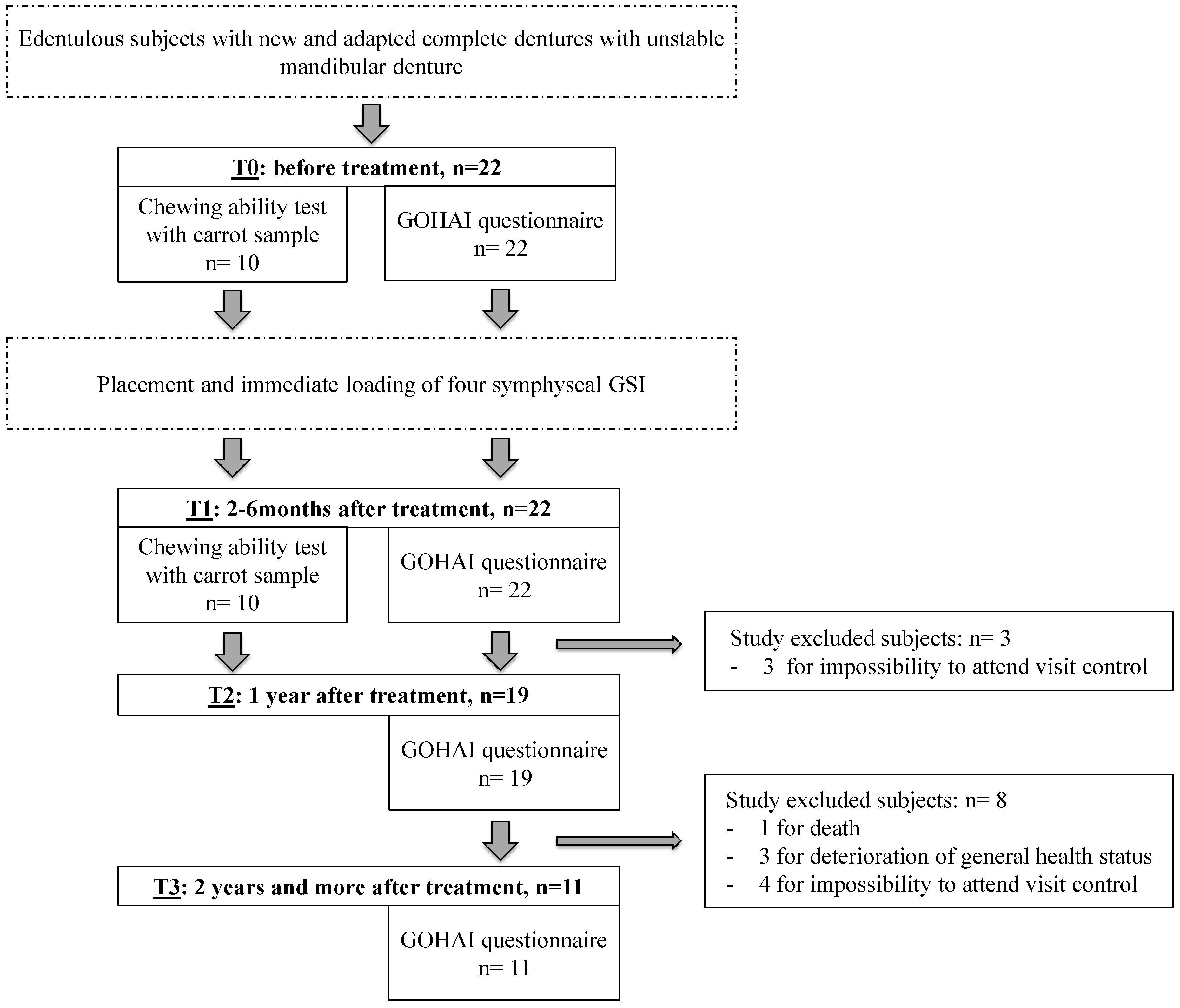
2.1. Study Sample
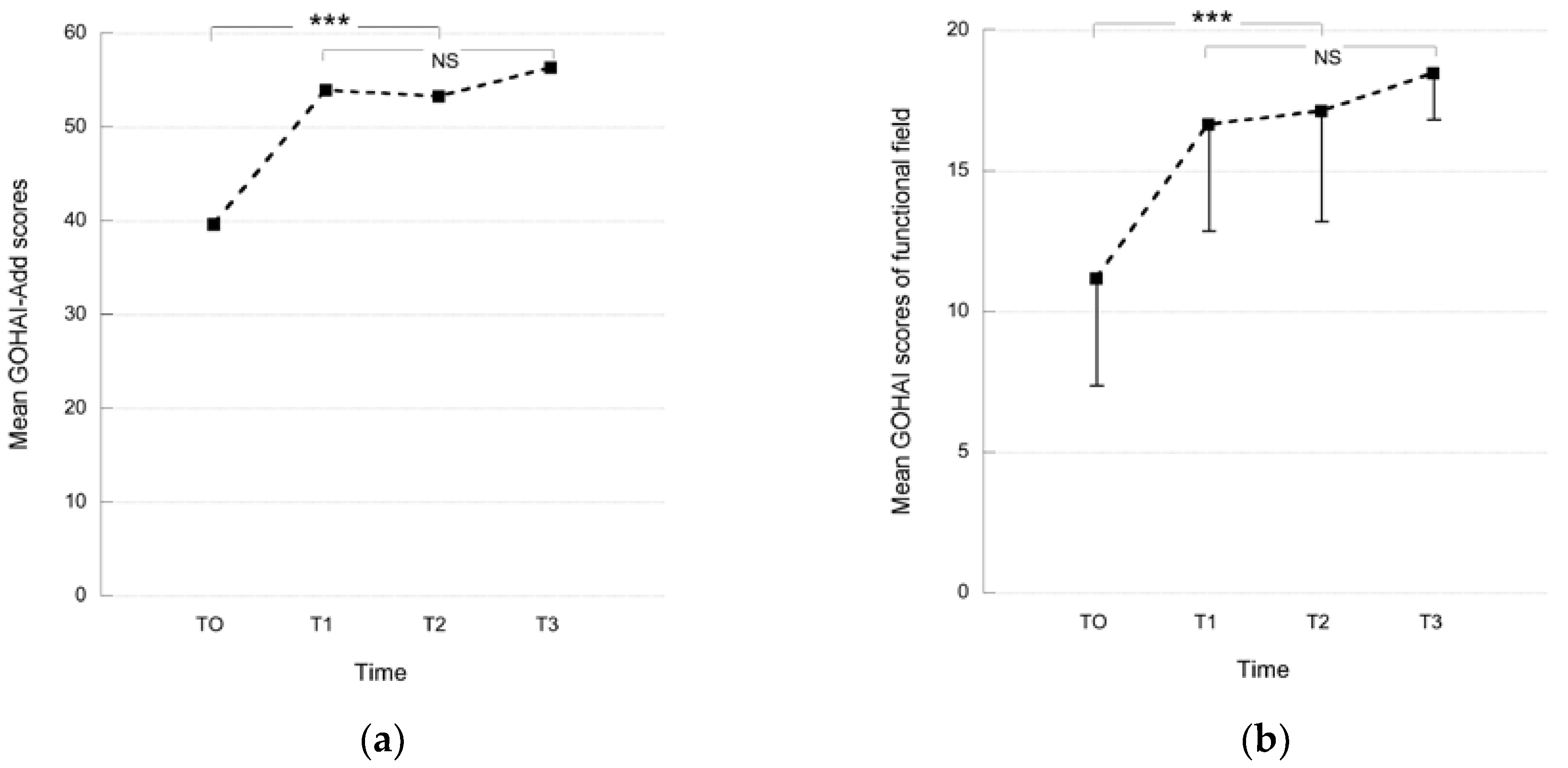
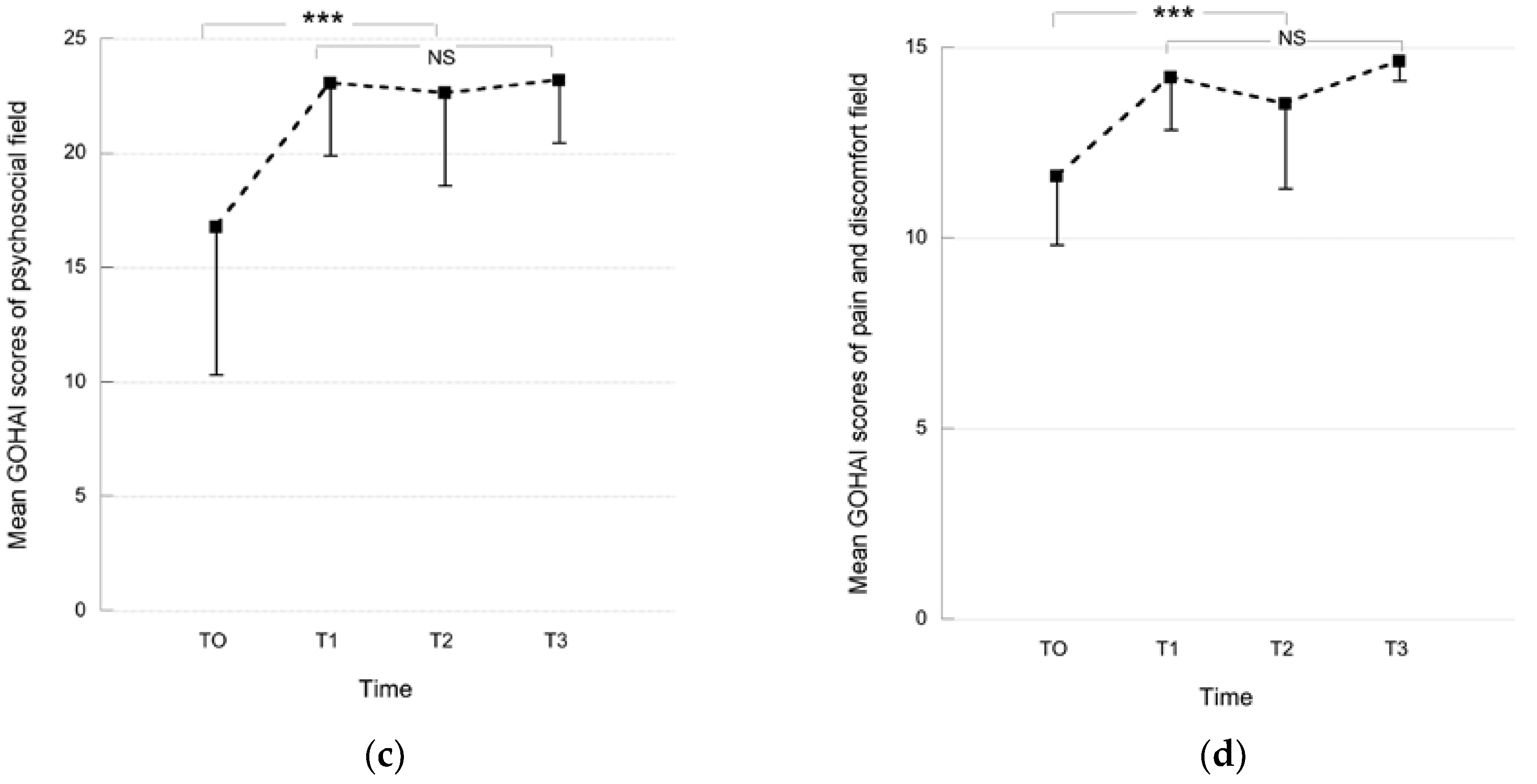
2.2. Influence of GSI Placement on Oral Health Related Quality of Life
2.2.1. Influence of Socio-Demographic Criteria on Oral Health Related Quality of Life
2.2.2. Influence of Chewing Ability on Oral Health Related Quality of Life
3. Discussion
4. Materials and Methods
4.1. Study Design
4.2. Study Sample
4.3. Experimental Design
4.4. Assessment Tools
4.4.1. Oral Health Related Quality of life
4.4.2. Chewing Ability
4.4.3. Statistical Analysis
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Thomason, J.M.; Feine, J.; Exley, C.; Moynihan, P.; Müller, F.; Naert, I.; Ellis, J.S.; Barclay, C.; Butterworth, C.; Scott, B.; et al. Mandibular two implant-supported overdentures as the first choice standard of care for edentulous patients-the York Consensus Statement. Br. Dent. J. 2009, 207, 185–186. [Google Scholar] [CrossRef] [PubMed]
- Feine, J.S.; Carlsson, G.E.; Awad, M.A.; Chehade, A.; Duncan, W.J.; Gizani, S.; Head, T.; Lund, J.P.; MacEntee, M.; Mericske-Stern, R.; et al. The McGill consensus statement on overdentures. Mandibular two-implant overdentures as first choice standard of care for edentulous patients. Montreal, Quebec, May 24–25, 2002. Int. J. Oral Maxillofac. Implants 2002, 17, 601–602. [Google Scholar] [PubMed]
- Huard, C.; Bessadet, M.; Nicolas, E.; Veyrune, J.L. Geriatric slim implants for complete denture wearers: Clinical aspects and perspectives. Clin. Cosmet. Investig. Dent. 2013, 5, 63–68. [Google Scholar] [PubMed]
- Christensen, G.J. The ‘mini’-implant has arrived. J. Am. Dent. Assoc. 2006, 137, 387–390. [Google Scholar] [CrossRef] [PubMed]
- Hjørting-Hansen, E. Glossary of Oral and Maxillofacial Implants; Quintessence Publishing Ltd.: London, UK, 2007; ISBN 978-3-938947-00-5. [Google Scholar]
- Preoteasa, E.; Meleşcanu-Imre, M.; Preoteasa, C.T.; Marin, M.; Lerner, H. Aspects of oral morphology as decision factors in mini-implant supported overdenture. Rom. J. Morphol. Embryol. 2010, 51, 309–314. [Google Scholar] [PubMed]
- Elsyad, M.A.; Gebreel, A.A.; Fouad, M.M.; Elshoukouki, A.H. The clinical and radiographic outcome of immediately loaded mini implants supporting a mandibular overdenture. A 3-year prospective study. J. Oral Rehabil. 2011, 38, 827–834. [Google Scholar] [CrossRef] [PubMed]
- Preoteasa, E.; Imre, M.; Preoteasa, C.T. A 3-year follow-up study of overdentures retained by mini-dental implants. Int. J. Oral Maxillofac. Implants 2014, 29, 1170–1176. [Google Scholar] [CrossRef] [PubMed]
- Scepanovic, M.; Calvo-Guirado, J.L.; Markovic, A.; Delgardo-Ruiz, R.; Todorovic, A.; Milicic, B.; Misic, T. A 1-year prospective cohort study on mandibular overdentures retained by mini dental implants. Eur. J. Oral Implantol. 2012, 5, 367–379. [Google Scholar] [PubMed]
- Enkling, N.; Saftig, M.; Worni, A.; Mericske-Stern, R.; Schimmel, M. Chewing efficiency, bite force and oral health-related quality of life with narrow diameter implants—a prospective clinical study: Results after one year. Clin. Oral Implants Res. 2017, 28, 476–482. [Google Scholar] [CrossRef] [PubMed]
- Mundt, T.; Schwahn, C.; Stark, T.; Biffar, R. Clinical response of edentulous people treated with mini dental implants in nine dental practices. Gerodontology 2015, 32, 179–187. [Google Scholar] [CrossRef] [PubMed]
- Griffitts, T.M.; Collins, C.P.; Collins, P.C. Mini dental implants: An adjunct for retention, stability, and comfort for the edentulous patient. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 2005, 100, e81–e84. [Google Scholar] [CrossRef] [PubMed]
- Elsyad, M.A. Patient satisfaction and prosthetic aspects with mini-implants retained mandibular overdentures. A 5-year prospective study. Clin. Oral Implants Res. 2016, 27, 926–933. [Google Scholar] [CrossRef] [PubMed]
- Tomasi, C.; Idmyr, B.O.; Wennström, J.L. Patient satisfaction with mini-implant stabilised full dentures. A 1-year prospective study. J. Oral Rehabil. 2013, 40, 526–534. [Google Scholar] [CrossRef] [PubMed]
- Batisse, C.; Bonnet, G.; Bessadet, M.; Veyrune, J.L.; Hennequin, M.; Peyron, M.A.; Nicolas, E. Stabilization of mandibular complete dentures by four mini implants: Impact on masticatory function. J. Dent. 2016, 50, 43–50. [Google Scholar] [CrossRef] [PubMed]
- Slade, G.D.; Spencer, A.J. Development and evaluation of the Oral Health Impact Profile. Community Dent. Health 1994, 11, 3–11. [Google Scholar] [PubMed]
- John, M.T.; Reissmann, D.R.; Čelebić, A.; Baba, K.; Kende, D.; Larsson, P.; Rener-Sitar, K. Integration of oral health-related quality of life instruments. J. Dent. 2016, 53, 38–43. [Google Scholar] [CrossRef] [PubMed]
- Preoteasa, E.; Marin, M.; Imre, M.; Lerner, H.; Preoteasa, C.T. Patients’ satisfaction with conventional dentures and mini implant anchored overdentures. Rev. Med. Chir. Soc. Med. Nat. Iasi. 2012, 116, 310–316. [Google Scholar]
- Awad, M.A.; Rashid, F.; Feine, J.S. The effect of mandibular 2-implant overdentures on oral health-related quality of life: An international multicentre study. Clin. Oral Implants Res. 2014, 25, 46–51. [Google Scholar] [CrossRef] [PubMed]
- Emami, E.; Heydecke, G.; Rompré, P.H.; de Grandmont, P.; Feine, J.S. Impact of implant support for mandibular dentures on satisfaction, oral and general health-related quality of life: A meta-analysis of randomized-controlled trials. Clin. Oral Implants Res. 2009, 20, 533–544. [Google Scholar] [CrossRef] [PubMed]
- Heydecke, G.; Locker, D.; Awad, M.A.; Lund, J.P.; Feine, J.S. Oral and general health-related quality of life with conventional and implant dentures. Community Dent. Oral Epidemiol. 2003, 31, 161–168. [Google Scholar] [CrossRef] [PubMed]
- Bonnet, G.; Batisse, C.; Segyo, J.W.; Veyrune, J.L.; Nicolas, E.; Bessadet, M. Influence of the renewal of removable dentures on oral health related quality of life. Springerplus 2016, 5, 2019. [Google Scholar] [CrossRef] [PubMed]
- Veyrune, J.L.; Opé, S.; Nicolas, E.; Woda, A.; Hennequin, M. Changes in mastication after an immediate loading implantation with complete fixed rehabilitation. Clin. Oral Investig. 2013, 17, 1127–1134. [Google Scholar] [CrossRef] [PubMed]
- De Souza, R.F.; Ribeiro, A.B.; Della Vecchia, M.P.; Costa, L.; Cunha, T.R.; Reis, A.C.; Albuquerque, R.F. Mini vs. standard implants for mandibular overdentures: A randomized trial. J. Dent. Res. 2015, 94, 1376–1384. [Google Scholar] [CrossRef] [PubMed]
- Jabbour, Z.; Emami, E.; de Grandmont, P.; Rompré, P.H.; Feine, J.S. Is oral health-related quality of life stable following rehabilitation with mandibular two-implant overdentures? Clin. Oral Implants Res. 2012, 23, 1205–1209. [Google Scholar] [CrossRef] [PubMed]
- Veyrune, J.L.; Lassauzay, C.; Nicolas, E.; Peyron, M.A.; Woda, A. Mastication of model products in complete denture wearers. Arch. Oral Biol. 2007, 52, 1180–1185. [Google Scholar] [CrossRef] [PubMed]
- Mishellany-Dutour, A.; Renaud, J.; Peyron, M.A.; Rimek, F.; Woda, A. Is the goal of mastication reached in young dentates, aged dentates and aged denture wearers? Br. J. Nutr. 2008, 99, 121–128. [Google Scholar] [CrossRef] [PubMed]
- Allen, P.F.; McMillan, A.S. A review of the functional and psychosocial outcomes of edentulousness treated with complete replacement dentures. J. Can. Dent. Assoc. 2003, 69, 662. [Google Scholar] [PubMed]
- Hutton, B.; Feine, J.; Morais, J. Is there an association between edentulism and nutritional state? J. Can. Dent. Assoc. 2002, 68, 182–187. [Google Scholar] [PubMed]
- Kurushima, Y.; Matsuda, K.; Enoki, K.; Ikebe, K.; Maeda, Y. Does case severity make a difference to clinical improvement following complete denture treatment? Int. J. Prosthodont. 2015, 28, 161–166. [Google Scholar] [CrossRef] [PubMed]
- Critchlow, S.B.; Ellis, J.S. Prognostic indicators for conventional complete denture therapy: A review of the literature. J. Dent. 2010, 38, 2–9. [Google Scholar] [CrossRef] [PubMed]
- Schimmel, M.; Christou, P.; Herrmann, F.; Müller, F. A two-colour chewing gum test for masticatory efficiency: Development of different assessment methods. J. Oral Rehabil. 2007, 34, 671–678. [Google Scholar] [CrossRef] [PubMed]
- Temizel, S.; Heinemann, F.; Dirk, C.; Bourauel, C.; Hasan, I. Clinical and radiological investigations of mandibular overdentures supported by conventional or mini-dental implants: A 2-year prospective follow-up study. J. Prosthet. Dent. 2017, 117, 239–246. [Google Scholar] [CrossRef] [PubMed]
- Tubert-Jeannin, S.; Riordan, P.J.; Morel-Papernot, A.; Porcheray, S.; Saby-Collet, S. Validation of an oral health quality of life index (GOHAI) in France. Community Dent. Oral Epidemiol. 2003, 31, 275–284. [Google Scholar] [CrossRef] [PubMed]
- Atchison, K.A.; Dolan, T.A. Development of the Geriatric Oral Health Assessment Index. J. Dent. Educ. 1990, 54, 680–687. [Google Scholar] [PubMed]
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Batisse, C.; Bonnet, G.; Veyrune, J.-L.; Nicolas, E.; Bessadet, M. Predictive Parameters of Oral Health Quality of Life in Complete Mandibular Denture Wearers Stabilized by Mini-Implants: A Two-Year Follow-Up Study. Materials 2017, 10, 1197. https://doi.org/10.3390/ma10101197
Batisse C, Bonnet G, Veyrune J-L, Nicolas E, Bessadet M. Predictive Parameters of Oral Health Quality of Life in Complete Mandibular Denture Wearers Stabilized by Mini-Implants: A Two-Year Follow-Up Study. Materials. 2017; 10(10):1197. https://doi.org/10.3390/ma10101197
Chicago/Turabian StyleBatisse, Cindy, Guillaume Bonnet, Jean-Luc Veyrune, Emmanuel Nicolas, and Marion Bessadet. 2017. "Predictive Parameters of Oral Health Quality of Life in Complete Mandibular Denture Wearers Stabilized by Mini-Implants: A Two-Year Follow-Up Study" Materials 10, no. 10: 1197. https://doi.org/10.3390/ma10101197
APA StyleBatisse, C., Bonnet, G., Veyrune, J.-L., Nicolas, E., & Bessadet, M. (2017). Predictive Parameters of Oral Health Quality of Life in Complete Mandibular Denture Wearers Stabilized by Mini-Implants: A Two-Year Follow-Up Study. Materials, 10(10), 1197. https://doi.org/10.3390/ma10101197




