Abstract
Excess weight (EW) in children has become a severe public health problem. The present study aimed to describe the main lifestyle characteristics and their possible association with nutritional status in a group of schoolchildren enrolled in the GENYAL study, where 221 children in the first or second grade of primary education (6–9 years old) were included. Anthropometric (BMI and bioimpedance), dietary intake (twice-repeated 24 h food record), and physical activity (twice-repeated 24 h physical activity questionnaire) data were collected. Logistic and linear regressions, with p-values adjusted for multiple tests by Bonferroni’s method and with sex and age as covariates, were applied. The prevalence of EW was 19%, 25.4%, and 32.2%, according to Orbegozo Foundation, IOFT, and WHO criteria, respectively. The results showed a significant association between schoolchildren’s nutritional status and energy balance, defined as the ratio of estimated energy intake to estimated energy expenditure (%), (β = −1.49 (−1.9–1.07), p < 0.01) and KIDMED Mediterranean Diet Quality Index score (β = −0.19 (95% IC −0.38–0), p = 0.04), and between the availability of TV or other technological devices in their room and the child’s BMI (β = 1.15 (95% IC 0.20–2.10), p = 0.017) and their fat mass (β = 3.28 (95% IC 0.69–5.87), p = 0.013). The number of dairy servings/day had a protective effect against EW (OR = 0.48 (0.29–0.75), p adjusted = 0.05)). Studying lifestyle factors associated with obesity is essential for developing tools and strategies for obesity prevention in children.
1. Introduction
In line with the WHO European Childhood Obesity Surveillance Initiative, one in three European children aged six to nine were overweight or obese in 2015 [1]. This fact confirms that pediatric excess body weight has become a significant public health problem worldwide.
Notwithstanding the unexpected plateau in childhood obesity rates observed in developed countries [2], Spain continues to have one of the highest European rates [3], as some national researches reveal, such as the ALADINO study (2019) that estimated a rate of childhood overweight prevalence of 23.3% (24.7% girls, 21.9% boys) and an obesity rate of 17.3% (15.0% girls, 19.4% boys) [4].
Cardiovascular diseases, type 2 diabetes mellitus, dyslipidemia, hypertension, and non-alcoholic fatty liver disease, which are associated with premature adult mortality, are non-communicable diseases linked to obesity and their most frequent comorbidities [5]. The severity of obesity is directly related to the risk of cardio-metabolic diseases, particularly among children [6]. Regardless of the multifactorial obesity aetiology, genetic susceptibility plays a specific role. It is dramatically influenced by a permissive and obesogenic environment that begins in the mother’s womb and continues throughout childhood and adolescence [6]. It has been widely known that dietary and physical activity habits are essential health determinants [7] and can act as critical modulators in the prevention and treatment of obesity [8]. Hence, they are essential in the search for tools that might contribute to obesity prevention at an early age, improving the expectations of quality of life and longevity.
Dietary patterns in Spanish children have been getting worse in recent decades. Food consumption has approached westernized countries characterized by an excessive caloric intake, poor nutritional quality food, and low adherence to the typical Mediterranean diet (MD) [9]. Likewise, it has been observed that a high rate of 9–12-year-old Spanish children does not achieve the daily recommendation of practising at least 60 min of moderate- to vigorous-intensity physical activity [10].
Many studies have been conducted worldwide on the association between nutritional and physical activity factors and excess weight in schoolchildren, underlining the need for more research in this area [11,12,13,14,15]. Nevertheless, in Spain, only several studies were conducted, such as The ALADINO study [4] and the EsNuPi study [16], the two most complete national studies on the prevalence of pediatric obesity, but they were descriptive and cross-sectional studies. Other national studies, such as The THAO Child Health Program [17] and the POIBC study [18], included nutritional intervention, but were carried out outside the social context of Madrid. The GENYAL study is a cluster-randomized clinical trial with a 5-year follow-up intervention, based on nutritional education, annual anthropometric measurement evaluations, and data collection from questionnaires developed in Madrid (Spain), which will increase knowledge in this area.
Thus, the objective of this study was to describe the main lifestyle characteristics (diet and exercise) and their possible association with nutritional status in a group of schoolchildren (6–9 years old) enrolled in the GENYAL study (Madrid, Spain) for the prevention of childhood obesity.
2. Materials and Methods
2.1. Study Population and Design
A cross-sectional study was carried out in the context of the project “GENYAL study for the prevention of childhood obesity”. It is an observational and a 5-year intervention study whose main objective is to design and validate a predictive model to identify those children who would benefit most from actions to reduce the risk of obesity and its complications, considering both environmental and genetic factors involved. Given the large number of endpoints and associations analyzed, and the absence of initial guesses for the variability for many of them, it was not possible to conduct a rigorous and univocal estimation of the sample size. Given the available resources, we decided to use the most significant sample possible. This work was approved by the Research Ethics Committee of the IMDEA Food Foundation with PI number: IM024. The methodology used complies with the Declaration of Helsinki (1964) and its modifications. The project has been coded as Clinical Trial (www.clinicaltrials.gov, accessed on 29 October 2018) with the number NCT03419520. This study began in March 2017, and the initial assessment results have been analyzed here.
The Consejería de Educación e Investigación de la Comunidad de Madrid was responsible for selecting six primary schools in the city of Madrid (Spain), two in the north, two in the centre, and two in the south. This selection was based on the number of students per school and the socioeconomic level of the neighbourhoods, achieving a representative selection of the average income of the city households. The sample size calculation could not be defined due to the characteristics and design of this study, where we had no previous data for the variability of the outcomes in the population, with this being a study of exploratory character.
In order to participate, the school-aged children had to be studying the 1st or 2nd grade of primary education, attend the centre on the evaluation days, and not expect a change of school in the forthcoming years. The signed informed consent was collected by at least one of the parents of all participating children.
2.2. Anthropometric Data
The evaluations were taken by trained dietitians using a standardized protocol, following the guidelines proposed by the International Society for the Advancement of Kinanthropometry [19]. For all the parameters, an average of 2–3 measurements were made depending on the magnitude of the differences in each record.
The children were evaluated barefoot, with shorts and an undershirt on. Height was measured using a stadiometer with millimetric accuracy (Leicester-Biología Tecnología Médica SL, Barcelona, Spain). Body weight and fat mass (FM) were determined using a bioimpedance with electrodes for hands and feet (BF511, Omron Healthcare Co., Ltd., Kyoto, Japan). Based on these data, other derived variables of interest were calculated. The body mass index (BMI) was calculated as weight (kg)/height (m)2 and classified according to percentiles of the Faustino Orbegozo Foundation [20], the International Obesity Task Force (IOTF) [21], and the World Health Organization (WHO) growth standards [22].
2.3. Dietary Data
To obtain a dietary data compilation, a twice-repeated 24 h food record was completed over two non-consecutive days (one weekday and one weekend day), following the European Food Safety Authority guidelines [23]. The dietary data transformation to macro and micronutrients was done through the DIAL software (Alce Ingeniería, Madrid, España). The energy balance (%EB) was calculated as total energy intake (TEI) (kcal/day)/total energy expended (TEE) (kcal/day) × 100 (where TEI was obtained from the DIAL software, and TEE was estimated from the WHO equation [24] that establishes a basal expenditure based on the weight, age, and sex of each individual and then, this basal expenditure is multiplied by an Individual Physical Activity Coefficient (IPAC)). When the EB > 110%, it was considered overfeeding, between 90–110% remains in equilibrium, and <90% insufficient intake.
Data were also recorded from the children’s food consumption habits since birth and their parents’ habits. The “KIDMED Mediterranean Diet Quality Index” was utilized to evaluate their adhesion to the Mediterranean eating pattern. This questionnaire included 16 dichotomous questions with an affirmative or negative answer, obtaining a final score which ranged from 0 to 12. The questions included were (Q1) takes a fruit or fruit juice every day; (Q2) has a second fruit every day; (Q3) has fresh or cooked vegetables regularly once a day; (Q4) has fresh or cooked vegetables more than once a day; (Q5) consumes fish regularly (at least 2–3 times per week); (Q6) goes more than once a week to a fast-food (hamburger) restaurant; (Q7) likes pulses and eats them more than once a week; (Q8) consumes pasta or rice almost every day (5 or more times per week); (Q9) has cereals or grains (bread, etc.) for breakfast; (Q10) consumes nuts regularly (at least 2–3 times per week); (Q11) uses olive oil at home; (Q12) skips breakfast; (Q13) has a dairy product for breakfast (yoghurt, milk, etc.); (Q14) has commercially baked goods or pastries for breakfast; (Q15) takes two yoghurts and/or some cheese (40 g) daily; and (Q16) takes sweets and candy several times every day. Questions denoting a negative connotation concerning the Mediterranean diet were assigned a value of −1 (questions Q6, Q12, and Q16), and those with a positive aspect +1. The sums of the values from the administered test were classified into three levels: (1) >8, optimal Mediterranean diet; (2) 4–7, improvement needed to adjust intake to Mediterranean patterns; and (3) ≤3, low diet quality [25].
2.4. Physical Activity Data
A twice-repeated 24 h physical activity questionnaire (a weekday and a weekend day) was collected [26]. The parents had to specify the time that their children spent during 24 h on a weekday and 24 h on a weekend day doing different activities, including resting hours and activities with a variable level of intensity (very light, light, moderate, and intense). According to the activity coefficient defined by the WHO [27], the time spent doing different activities was multiplied, added, and divided by 24, obtaining the Individual Physical Activity Coefficient (IPAC). Firstly, the weekend day IPAC was multiplied by 2 and the weekday IPAC by 5. Then, the mean physical activity per individual was obtained by adding both results and dividing by 7. An equivalence between the IPAC and the Physical Activity Coefficient (PAC) was made according to sex, following the Institute of Medicine methodology [28]. To conclude, participants were classified for their PAC into very active, active, low active, and sedentary subjects. In order to estimate if children achieved the recommendation to do more than 60 min/day of active and moderate sports activities [29], the total active weekly hours (TAWH) were calculated considering the time invested in vigorous and moderate extra-curricular activities and two additional curricular hours.
2.5. Statistical Analyses
Descriptive analyses were performed by computing the class’s absolute and relative frequencies for the categorical variables. The mean, median, standard deviation, interquartile range, maximum, and minimum were calculated for the quantitative variables. The Shapiro–Wilk test (p > 0.05) was used to assess the normality of data. To check the homogeneity between groups, a t-test was used for quantitative variables with normal distribution and a Mann–Whitney U test in the opposite case. Chi-Square or Fischer exact tests were used for categorical variables.
The associations between anthropometric, physical activity, and nutritional data were established through logistic and linear regressions/ANOVA adjusted by sex and age. No variable selection approaches were used (e.g., stepwise), and for each association tested, a new regression model was developed with the two involved variables included (one as predictor and the other as outcome) plus the two adjustment variables as additional predictors. The p-values were corrected by means of the Bonferroni method. This correction was motivated by computational simplicity and the small number of tests performed. The multiple comparison analysis included a total of 50 variables from different categories included in the study (nutritional, anthropometric, socio-sanitary, etc.). The overweight and obesity categories were unified in some analyses as a single category called excess weight (EW). Statistical analyses between the study variables and nutritional status were performed with BMI as a continuous variable and as a BMI category according to IOTF criteria as a categorical variable, including underweight, average weight, and overweight. Statistical tests were two-tailed with a 5% level of significance. R Statistical Software 3.1 (www.r-projet.org) (accessed on 29 October 2018) was used to perform the statistical analysis.
3. Results
A total of 569 schoolchildren from the 6 contacted schools were included, and 39.36% of the parents signed the informed consent form. Among the 224 children included, 3 did not attend the evaluation day, so the final sample consisted of 221 (48.0% girls and 52.0% boys) with a mean age of 6.75 ± 0.73 years. The descriptive anthropometric, physical and leisure activities, and intake characteristics of schoolchildren according to sex are summarized in Table 1.

Table 1.
Sample characteristics by sex.
According to the WHO criteria, 32.2% of the students evaluated had EW (18.1% overweight, 14.1% obesity). These figures were higher than when the IOFT standard (25.4%) or the national criteria of the Orbegozo Foundation (19.0%) were applied. The percentages of mean values of nutrient intake over the total caloric value were 44.48% in carbohydrates, 20.15% simple sugars, 18.16% fibre, 16.55% protein, 38.96% of fats, 13.28% SFA, 17.22% MFA, and 4.84% PFA. Boys were more likely to dedicate weekly to active physical activities than girls.
The main dietary characteristics of schoolchildren according to their nutritional status are summarized in Table 2. Eleven underweight children (five percent) were found in the sample following the IOTF criteria. Given the small sample size, they could not be treated independently.

Table 2.
Main diet characteristics of the schoolchildren in accordance with nutritional status (IOTF criteria).
Regarding schoolchildren’s energy balance (EB), calculated as TEI (kcal/day)/TEE (kcal/day) × 100, 38.8% of the children were overfeeding, while 28.9% were classified as having insufficient intake. When the relationship between the %EB (independent variable) and schoolchildren’s BMI and FM (dependent variables) was evaluated, it was found to be an inverse and significant association (β = −1.49 (−1.9–1.07), p = 1.53 × 105 (p < 0.01) and β = −3.46 (−4.62–2.29), p = 1.24 × 108 (p < 0.01), respectively).
Nevertheless, the intake of macronutrients, fibre, simple sugars, and lipid percentage were not associated with the child’s nutritional status.
The number of servings per day for the different food groups considered according to the schoolchildren’s nutritional status is presented in Figure 1. The number of dairy servings/day showed a protective effect against EW (OR = 0.48 (0.29–0.75), p adjusted = 0.05).
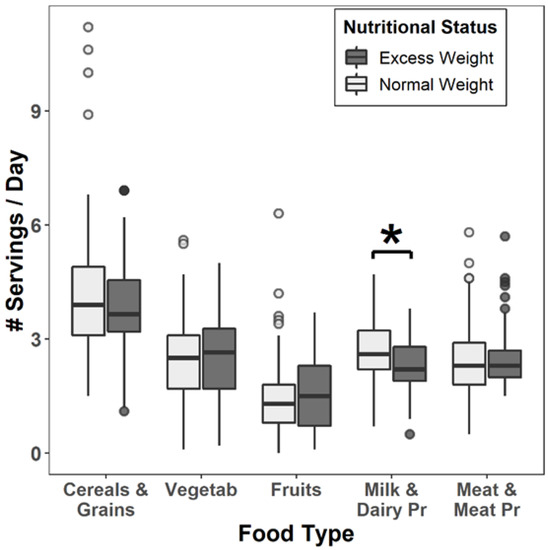
Figure 1.
Amount of servings/day for the different food groups according to the schoolchildren’s nutritional status. (* p = 0.039 Difference between the number of milk and dairy products servings/day according to nutritional status. Data adjusted by age and sex).
About 80.0% of the children had 5 or more meals daily, and 90.0% had breakfast regularly. Nonetheless, only 24.0% of the total schoolchildren had a breakfast considered as a well-balanced one (fruits, dairy, and cereal products). Neither the number of meals made per day nor the consumption of a quality breakfast showed an association with EW in schoolchildren.
Concerning the KIDMED questionnaire, more than 50.0% of the children needed to improve their diet and 7.50% had a very low-quality diet. The total score obtained in the KIDMED questionnaire was inversely associated with the schoolchildren’s BMI (β = −0.19 (95% IC −0.38–0), p = 0.04) and FM (β = −0.65 (−1.15–0.14), p = 0.01).
Finally, when other factors were considered, such as if the children received breastfeeding, its length of time, or the age of Beikost (defined as an infant’s first non-liquid food) beginning, neither of them was associated with the nutritional status. Table 3 describes the primary schoolchildren’s physical activity characteristics and sleep length according to their nutritional status.

Table 3.
Physical activity and sleep length of the schoolchildren in accordance with nutritional status.
According to the Individual Physical Activity Coefficient (IPAC), 55.6% of the children were classified as sedentary or low-active subjects. Moreover, the coefficient was lower during weekends (1.52 ± 0.13 at the weekend and 1.61 ± 0.12 during the week, p < 0.001). At the same time, only 40.0% of the total achieved the daily recommendation of practising at least 60 min of moderate- to vigorous-intensity physical activity [20].
In addition, 22.0% of children spend more than two hours of TV time a day (television, playing video games, computer…), mainly during the weekend. Likewise, 15.2% had a TV or other technological devices in their room. Concerning relation to this, a direct and significant association was observed between the availability of these devices and the child’s BMI (β = 1.15 (95% IC 0.20–2.10) p = 0.017) and their FM β = 3.28 (95% IC 0.69–5.87) p = 0.013. Only the relationship between the %EB and schoolchildren’s BMI (p < 0.01) and FM (p < 0.01) maintained significance after multiple comparison analyses.
4. Discussion
Detecting harmful dietary and sedentary habits could be advantageous in developing effective nutritional and educational intervention strategies towards obesity prevention [8]. The results of the anthropometric evaluation showed that a fourth of the children who participated in the study presented excess weight. These results parallel those obtained in the ALADINO study in 2019 [4].
The child’s energy balance (TEI (kcal/day)/TEE (kcal/day)) showed a paradoxical inverse association with the BMI in the same way described previously [30,31,32]. It has been known that the weight status of children can lead to under- and over-reporting of a child’s dietary and physical activity behaviour by parents. This results from social desirability and sociocultural biases when being overweight is seen as a desirable trait or if the prevalence is high and being overweight is considered “normal” relative to other children [33].
In this work, the diet’s distribution of proteins and fats and the simple sugar contribution were far from the recommendation, and they fell short of total carbohydrates [34]. This has been previously observed in different national children surveys [35] and in the EsNuPi study [16]. These data reflect that the diet in children must be improved. Excess protein in the diet has previously been associated with obesity and other metabolic risks at an early age and higher BMI later in childhood [36]. It maintains the same trend in terms of excess fat [37]. Nevertheless, these aspects of the diet were not associated with the schoolchildren’s nutritional status categories or with the BMI and FM in this study.
Significant differences were observed between the hours dedicated to practising physical activity weekly (TAWH) between boys and girls, observing that the boys spent the most time practising. These results have been observed in other studies [11,14]. In the ALADINO 2019 study, this same trend was observed. In addition, boys carried out more extracurricular sports activities than girls, reflecting an inequitable distribution between genders in sports since childhood [4].
The intake of calcium from dairy and the presence of peptides and bioactive components with a potential effect on satiety and weight control [38,39] could explain the significant association found between the number of daily portions of dairy consumed and the BMI of the children in the study. According to the latest reviews on the subject, milk and dairy products are not consistently associated or are inversely associated with obesity and indicators of adiposity in children [40]. For this reason, policies that intend to increase dairy consumption could be crucial to preventing “weight excess” in children and adults. Breakfast is often described as the most important meal of the day, and its omission has been related to adiposity among children and adolescents [41]. Although practically all the children had breakfast regularly in this study, only one out of four consumed a well-balanced breakfast. Unlike other studies [15,42], this one did not identify an association between this kind of breakfast consumption and obesity. The different methodologies employed to characterize a healthy breakfast could explain the varied results.
The Mediterranean diet is considered a model of a healthy diet. It is likely because its composition is rich in vegetables, fruits, legumes, whole cereals, and many sources of fibre and antioxidants. The score obtained in the KIDMED questionnaire confirmed the distancing of the Spanish children from the MD pattern described in previous studies [43] and is similar to the results reported by the ALADINO 2019 study [4]. This fact is considered one of the reasons why Spain is among the European countries with the highest prevalence of childhood obesity [44]. However, in the EsNupi study [16], a main dietary pattern was observed related to the Mediterranean diet, with high consumption of cereals, fruits, vegetables, milk, and dairy products. On the plus side, this result showed the association of this diet with a lower prevalence of obesity [45].
In this study, 22.0% of children spent more than two hours of TV time a day (television, playing video games, computer…), mainly during the weekend. In the ALADINO 2019 study, the percentage was higher, and the same trend was observed towards greater inactivity and passive leisure on the screen during weekends [4]. The connection observed in this study between the availability of TV and other devices in the child’s room and excess weight could be related to increased meal frequency and food intake or to less time that children are under adult supervision. Unfortunately, these aspects were not covered in this study. Similarly, it could avoid the performing of active leisure time [46,47]. Moreover, in other studies, total screen time has been directly related to excess weight in children [11].
The inverse relationship between sleep length and BMI has been described in children and adolescents. Recent studies associate it with a higher intake and a lower energy expenditure due to the hormonal pathways involved in the appetite for partial sleep deprivation [48]. In this study, the children who presented obesity had less average sleep length; however, the differences were not significant. It was observed that children with obesity performed more physical activity through the calculated variables (IPAC and TAWH) than children with average weight and who were overweight. The results did not obtain statistical significance. In the ALADINO 2019 study, contrary data was obtained. Children with average weight were the most active [4].
We can identify some limitations in this study. Firstly, the use of dietary and physical activity questionnaires has been criticized. Nevertheless, in the absence of better tools with a low cost and high throughput to estimate the intake, consumption records can offer valuable information, although they should be interpreted cautiously. A second limitation is the sample size (n = 221). Nevertheless, it is essential to consider that this study is framed as an intervention study of 5 years follow-up.
On the other hand, the lack of sample size calculation is one of the weak aspects of our study. Due to the nature of the study as a clinical trial, the large number of variables used, and the duration of 5 years, a statistically robust sample size could not be implemented. Furthermore, the “Consejería de Educación e Investigación de la Comunidad de Madrid” was responsible for the selection of six representative schools of the Community of Madrid (CM) (Spain), considering the number of students per centre and the average and socioeconomic level of the districts and neighbourhoods. Therefore, the selection was representative of the average income of the CM households. The lack of other confounding factors, such as sociodemographic variables of the characteristics of the families or genetics variables, is considered a limitation of this study. Nevertheless, in the GENYAL study, these variables were collected and will be evaluated within other studies with framed objectives on this subject.
From a statistical point of view, using a simple conservative Bonferroni correction that controls the family-wise error rate can lead to an increased rate of false negatives compared to other methods. However, given the small number of tests performed, this should not be a significant issue.
By contrast, it is worth highlighting the homogeneity of the population in terms of distribution by sex, as well as its representativeness since six schools from three different areas of the CM participated, which allows us to have a better knowledge of the situation throughout the Community and not from a specific school or area.
5. Conclusions
In conclusion, the results obtained in this study reflect that a high prevalence of excess weight was associated with the intake of dairy servings, the distancing of the Mediterranean diet pattern, and the presence of TV or other devices in children’s rooms. The control of these aspects could be an important point to guide families in lifestyle improvement. However, the small sample size of this study requires that its results be corroborated in future studies with larger sample sizes.
Author Contributions
Conceptualization, H.M.-P. and V.L.-K.; methodology, V.L.-K. and H.M.-P.; formal analysis, G.C.; investigation, H.M.-P., E.A.-A. and V.L.-K.; resources, H.M.-P., E.A.-A. and V.L.-K.; data curation, H.M.-P., E.A.-A., G.C. and V.L.-K.; writing—original draft preparation, H.M.-P., V.L.-K.; writing—review and editing, H.M.-P., E.A.-A., V.L.-K.; supervision, A.R.d.M., G.R. and V.L.-K.; funding acquisition, A.R.d.M. and G.R. All authors have read and agreed to the published version of the manuscript.
Funding
This research was supported by Conserjería de Educación, Universidades y Ciencia de la Comunidad de Madrid, Dirección General de Educación Infantil, Primaria y Secundaria.
Institutional Review Board Statement
The study was conducted in accordance with the Declaration of Helsinki and approved by the Ethics Committee of the IMDEA Food Foundation (protocol code: IMD-024 and date of approval: 29 March 2016).
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
Not applicable.
Acknowledgments
The authors would like to acknowledge the help of all the teachers and head teachers of Juan Zaragüeta, Fernando El Católico, Fernández Moratín, La Rioja, Concepción Arenal y Rosa Luxemburgo schools; and, especially, for the families and children volunteers who participated in the investigation.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Nutrition—EU Science Hub—European Commission. EU Science Hub. Available online: https://ec.europa.eu/jrc/en/research-topic/nutrition (accessed on 12 July 2021).
- Townsend, N.; Rutter, H.; Foster, C. Evaluating the evidence that the prevalence of childhood overweight is plateauing. Pediatr. Obes. 2012, 7, 343–346. [Google Scholar] [CrossRef] [PubMed]
- Childhood Obesity Surveillance Initiative (COSI) Factsheet. Highlights 2015-17 (2018). Available online: http://www.euro.who.int/en/health-topics/disease-prevention/nutrition/activities/who-european-childhood-obesity-surveillance-initiative-cosi/cosi-publications/childhood-obesity-surveillance-initiative-cosi-factsheet.-highlights-2015-17-2018 (accessed on 12 July 2021).
- Resumen de la Cuarta Ronda COSI (2015–2017) de la Oficina Regional Para Europa de la OMS y Cmparación con los Resultados de ALADINO 2019. Agencia Española de Consumo, Seguridad Alimentaria y Nutrición. Ministerio de Sanidad, Servicios Sociales e Igualdad. 2021. Available online: https://www.aesan.gob.es/AECOSAN/docs/documentos/nutricion/observatorio/RESULTADOS_4_INFORME_COSI_2105_2017_NAOS.pdf (accessed on 7 October 2022).
- Kunwar, R.; Minhas, S.; Mangla, V. Is obesity a problem among school children? Indian J. Public Health 2018, 62, 153. [Google Scholar] [PubMed]
- Styne, D.M.; Arslanian, S.A.; Connor, E.L.; Farooqi, I.S.; Murad, M.H.; Silverstein, J.H.; Yanovski, J.A. Pediatric Obesity—Assessment, Treatment, and Prevention: An Endocrine Society Clinical Practice Guideline. J. Clin. Endocrinol. Metab. 2017, 102, 709–757. [Google Scholar] [CrossRef] [PubMed]
- Hill, J. Physical activity and obesity. Lancet 2004, 363, 182. [Google Scholar] [CrossRef]
- Verduci, E.; Di Profio, E.; Fiore, G.; Zuccotti, G. Integrated Approaches to Combatting Childhood Obesity. Ann. Nutr. Metab. 2022, 78 (Suppl. S2), 8–19. [Google Scholar] [CrossRef]
- Bach-Faig, A.; Bo, A.P.; Castell, G.S. Hábitos Alimentarios y Estilos de Vida en Niños/as y Adolescentes. In Libro Blanco de la Nutrición Infantil en España; Prensas de la Universidad de Zaragoza: Zaragoza, España, 2015; pp. 315–324. [Google Scholar]
- Fundación para la Investigación Nutricional (FIN). Informe 2016: Actividad Física en Niños y Adolescentes en España. 2016. Available online: https://www.observatoriodelainfancia.es/oia/esp/documentos_ficha.aspx?id=5056 (accessed on 24 July 2022).
- Paduano, S.; Greco, A.; Borsari, L.; Salvia, C.; Tancredi, S.; Pinca, J.; Midili, S.; Tripodi, A.; Borella, P.; Marchesi, I. Physical and Sedentary Activities and Childhood Overweight/Obesity: A Cross-Sectional Study among First-Year Children of Primary Schools in Modena, Italy. Int. J. Environ. Res. Public Health 2021, 18, 3221. [Google Scholar] [CrossRef]
- Paduano, S.; Borsari, L.; Salvia, C.; Arletti, S.; Tripodi, A.; Pinca, J.; Borella, P. Risk Factors for Overweight and Obesity in Children Attending the First Year of Primary Schools in Modena, Italy. J. Community Health 2020, 45, 301–309. [Google Scholar] [CrossRef]
- Zhu, X.; Haegele, J.A.; Tang, Y.; Wu, X. Prevalence and Demographic Correlates of Overweight, Physical Activity, and Screen Time Among School-Aged Children in Urban China: The Shanghai Study. Asia Pac. J. Public Health 2018, 30, 118–127. [Google Scholar] [CrossRef]
- Gerber, M.; Lang, C.; Beckmann, J.; du Randt, R.; Long, K.Z.; Müller, I.; Nienaber, M.; Probst-Hensch, N.; Steinmann, P.; Pühse, U.; et al. Physical Activity, Sedentary Behaviour, Weight Status, and Body Composition among South African Primary Schoolchildren. Int. J. Environ. Res. Public Health. 2022, 19, 11836. [Google Scholar] [CrossRef]
- Gracia-Arnaiz, M.; Kraemer, F.B.; Demonte, F.C. Acting against obesity: A cross-cultural analysis of prevention models in Spain, Argentina and Brazil. Crit. Rev. Food Sci. Nutr. 2022, 62, 2192–2204. [Google Scholar] [CrossRef]
- Estudio EsNuPi 2022. Available online: https://www.estudioesnupi.org/ (accessed on 16 December 2022).
- Qué es el Programa Thao? Programa Thao-Salud Infantil. 2016. Available online: https://programathao.com/que-es/ (accessed on 16 December 2022).
- Gómez, S.F.; Casas, R.; Palomo, V.T.; Pujol, A.M.; Fitó, M.; Schroder, H. Study protocol: Effects of the THAO-child health intervention program on the prevention of childhood obesity—The POIBC study. BMC Pediatr. 2014, 14, 215. [Google Scholar] [CrossRef] [PubMed]
- Stewart, A.; Marfell-Jones, M. International Society for Advancement of Kinanthropometry. In International Standards for Anthropometric Assessment; International Society for the Advancement of Kinanthropometry: Lower Hutt, New Zealand, 2011. [Google Scholar]
- Fernández, C.; Lorenzo, H.; Vrotsou, K.; Aresti, U.; Rica, I.; Sánchez, E. Estudio de Crecimiento de Bilbao. Curvas y Tablas de Crecimiento. Estudio Transversal; Fundación Faustino Orbegozo Eizaguirre: Bilbao, Spain, 2011. [Google Scholar]
- Cole, T.J.; Lobstein, T. Extended international (IOTF) body mass index cut-offs for thinness, overweight and obesity. Pediatr. Obes. 2012, 7, 284–294. [Google Scholar] [CrossRef] [PubMed]
- WHO. Growth Reference Data for 5–19 Years 2018. Available online: http://www.who.int/growthref/en/ (accessed on 22 February 2022).
- European Food Safety Authority. General principles for the collection of national food consumption data in the view of a pan-European dietary survey. EFSA J. 2009, 7, 1435. [Google Scholar] [CrossRef]
- FAO. Energy and Protein Requirements. Available online: http://www.fao.org/docrep/003/aa040e/aa040e00.htm (accessed on 28 August 2022).
- Serra-Majem, L.; Ribas, L.; Ngo, J.; Ortega, R.M.; García, A.; Pérez-Rodrigo, C.; Aranceta, J. Food, youth and the Mediterranean diet in Spain. Development of KIDMED, Mediterranean Diet Quality Index in children and adolescents. Public Health Nutr. 2004, 7, 931–935. [Google Scholar] [CrossRef]
- Ortega, R.; Requejo, A.; López-Sobaler, A. Modelos de Cuestionario de Actividad. In Nutriguía Manual de Nutrición Clínica en Atención Primaria. 2006; Editorial Médica Panamericana: Madrid, Spain, 2015; p. 468. [Google Scholar]
- WHO. Physical Status: The Use and Interpretation of Anthropometry. 2018. Available online: http://www.who.int/childgrowth/publications/physical_status/en/ (accessed on 22 February 2022).
- Institute of Medicine of the National Academies. Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein, and Amino Acids. 2002. Available online: https://www.nap.edu/catalog/10490/dietary-reference-intakes-for-energy-carbohydrate-fiber-fat-fatty-acids-cholesterol-protein-and-amino-acids (accessed on 22 February 2022).
- WHO. Physical Activity and Young People. 2018. Available online: http://www.who.int/dietphysicalactivity/factsheet_young_people/en/ (accessed on 16 July 2022).
- Murakami, K.; Livingstone, M.B.E.; Okubo, H.; Sasaki, S. Younger and older ages and obesity are associated with energy intake underreporting but not overreporting in Japanese boys and girls aged 1–19 years: The National Health and Nutrition Survey. Nutr. Res. 2016, 36, 1153–1161. [Google Scholar] [CrossRef]
- Schoeller, D.A.; Thomas, D.; Archer, E.; Heymsfield, S.B.; Blair, S.N.; Goran, M.I.; Hill, J.O.; Atkinson, R.L.; Corkey, B.E.; Foreyt, J.; et al. Self-report–based estimates of energy intake offer an inadequate basis for scientific conclusions. Am. J. Clin. Nutr. 2013, 97, 1413–1415. [Google Scholar] [CrossRef]
- Wallace, A.; Kirkpatrick, S.I.; Darlington, G.; Haines, J. Accuracy of Parental Reporting of Preschoolers’ Dietary Intake Using an Online Self-Administered 24-h Recall. Nutrients 2018, 10, 987. [Google Scholar] [CrossRef]
- Koning, M.; de Jong, A.; de Jong, E.; Visscher, T.L.S.; Seidell, J.C.; Renders, C.M. Agreement between parent and child report of physical activity, sedentary and dietary behaviours in 9–12-year-old children and associations with children’s weight status. BMC Psychol. 2018, 6, 14. [Google Scholar] [CrossRef]
- Navia Lomban, B.; Ortega Anta, R.M. Ingestas Recomendadas de Energía y Nutrientes. In NutriguíaR Manual de Nutrición Clínica. 2a; Editorial Médica Panamericana: Madrid, Spain, 2015; pp. 3–26. [Google Scholar]
- Anibes. Available online: http://www.fen.org.es/anibes/es/distribucion_de_macronutrientes (accessed on 10 September 2022).
- Arnesen, E.K.; Thorisdottir, B.; Lamberg-Allardt, C.; Bärebring, L.; Nwaru, B.; Dierkes, J.; Ramel, A.; Åkesson, A. Protein intake in children and growth and risk of overweight or obesity: A systematic review and meta-analysis. Food Nutr. Res. 2022, 21, 66. [Google Scholar] [CrossRef]
- Naude, C.E.; Visser, M.E.; Nguyen, K.A.; Durao, S.; Schoonees, A. Effects of total fat intake on bodyweight in children. Cochrane Database Syst. Rev. 2018, 7, CD012960. [Google Scholar] [CrossRef]
- Wadolowska, L.; Ulewicz, N.; Sobas, K.; Wuenstel, J.W.; Slowinska, M.A.; Niedzwiedzka, E.; Czlapka-Matyasik, M. Dairy-Related Dietary Patterns, Dietary Calcium, Body Weight and Composition: A Study of Obesity in Polish Mothers and Daughters, the MODAF Project. Nutrients 2018, 10, 90. [Google Scholar] [CrossRef] [PubMed]
- Koca, T.; Akcam, M.; Serdaroglu, F.; Dereci, S. Breakfast habits, dairy product consumption, physical activity, and their associations with body mass index in children aged 6–18. Eur. J. Pediatr. 2017, 176, 1251–1257. [Google Scholar] [CrossRef] [PubMed]
- Dougkas, A.; Barr, S.; Reddy, S.; Summerbell, C.D. A critical review of the role of milk and other dairy products in the development of obesity in children and adolescents. Nutr. Res. Rev. 2019, 32, 106–127. [Google Scholar] [CrossRef] [PubMed]
- Blondin, S.A.; Anzman-Frasca, S.; Djang, H.C.; Economos, C.D. Breakfast consumption and adiposity among children and adolescents: An updated review of the literature. Pediatr. Obes. 2016, 11, 333–348. [Google Scholar] [CrossRef] [PubMed]
- Rosato, V.; Edefonti, V.; Parpinel, M.; Milani, G.P.; Mazzocchi, A.; Decarli, A.; Agostoni, C.; Ferraroni, M. Energy Contribution and Nutrient Composition of Breakfast and Their Relations to Overweight in Free-living Individuals: A Systematic Review. Adv. Nutr. 2016, 7, 455–465. [Google Scholar] [CrossRef]
- García Cabrera, S.; Herrera Fernández, N.; Rodríguez Hernández, C.; Nissensohn, M.; Román-Viñas, B.; Serra-Majem, L. KIDMED test; prevalence of low adherence to the Mediterranean Diet in children and young: A systematic review. Nutr. Hosp. 2015, 32, 2390–2399. [Google Scholar]
- Commission on Ending Childhood Obesity. Report of the Commission on Ending Childhood Obesity. 2017. Available online: https://apps.who.int/iris/handle/10665/259349 (accessed on 16 December 2022).
- Schröder, H.; Mendez, M.A.; Ribas-Barba, L.; Covas, M.-I.; Serra-Majem, L. Mediterranean diet and waist circumference in a representative national sample of young Spaniards. Int. J. Pediatr. Obes. 2010, 5, 516–519. [Google Scholar] [CrossRef]
- Pérez-Farinós, N.; Villar-Villalba, C.; Sobaler, A.M.L.; Dal Re Saavedra, M.Á.; Aparicio, A.; Santos Sanz, S.; Robledo de Dios, T.; Castrodeza-Sanz, J.J.; Ortega Anta, R.M. The relationship between hours of sleep, screen time and frequency of food and drink consumption in Spain in the 2011 and 2013 ALADINO: A cross-sectional study. BMC Public Health 2017, 17, 33. [Google Scholar] [CrossRef]
- Domingues-Montanari, S. Clinical and psychological effects of excessive screen time on children. J. Paediatr. Child Health 2017, 53, 333–338. [Google Scholar] [CrossRef]
- Felső, R.; Lohner, S.; Hollódy, K.; Erhardt, É.; Molnár, D. Relationship between sleep duration and childhood obesity: Systematic review including the potential underlying mechanisms. Nutr. Metab. Cardiovasc. Dis. 2017, 27, 751–761. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).