Manual Material Handling Training: The Effect of Self-Observation, Hetero-Observational and Intrinsic Feedback on Workers’ Knowledge and Behaviour
Abstract
1. Introduction
2. Materials and Methods
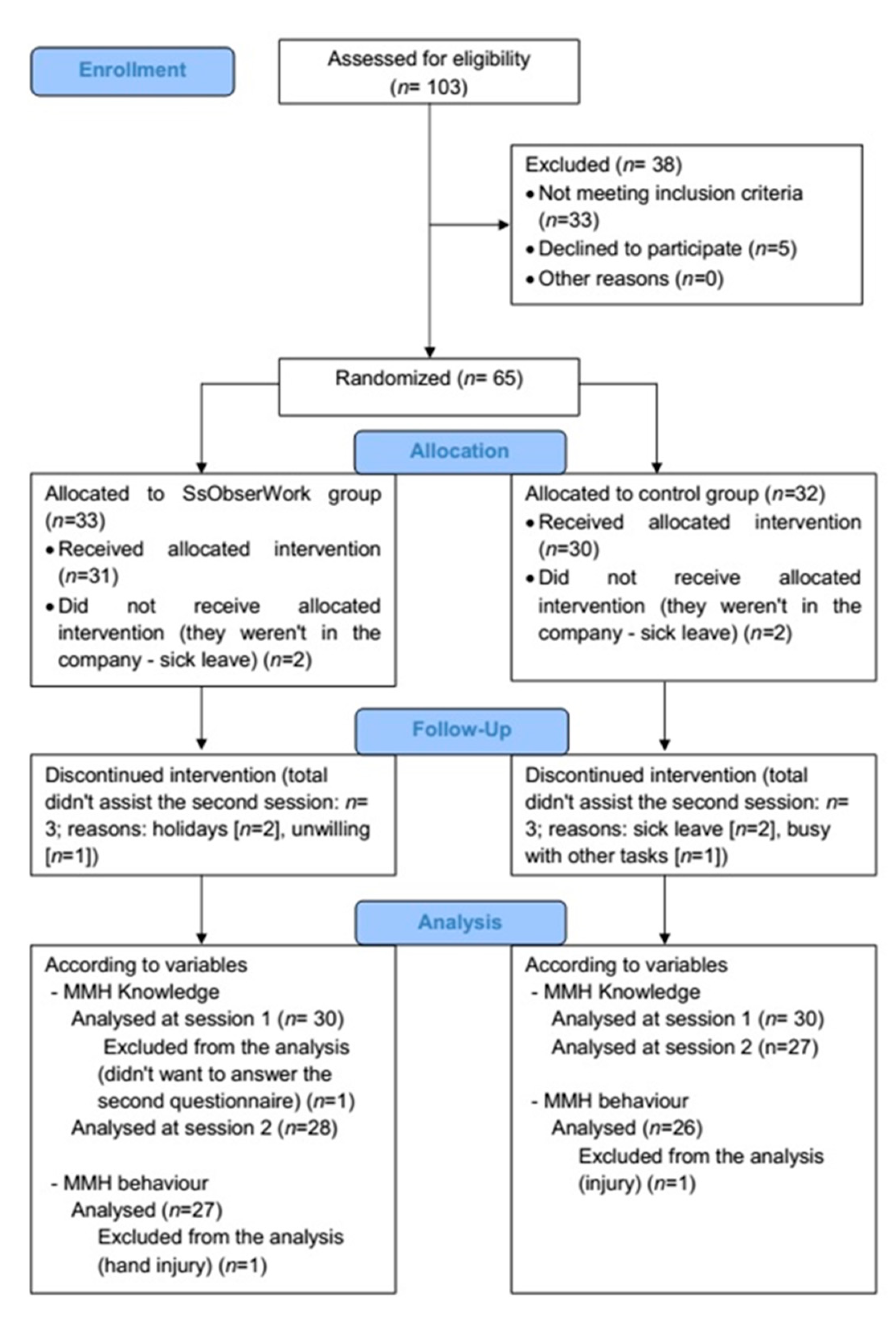
2.1. Study Design
2.2. Participants and Procedure
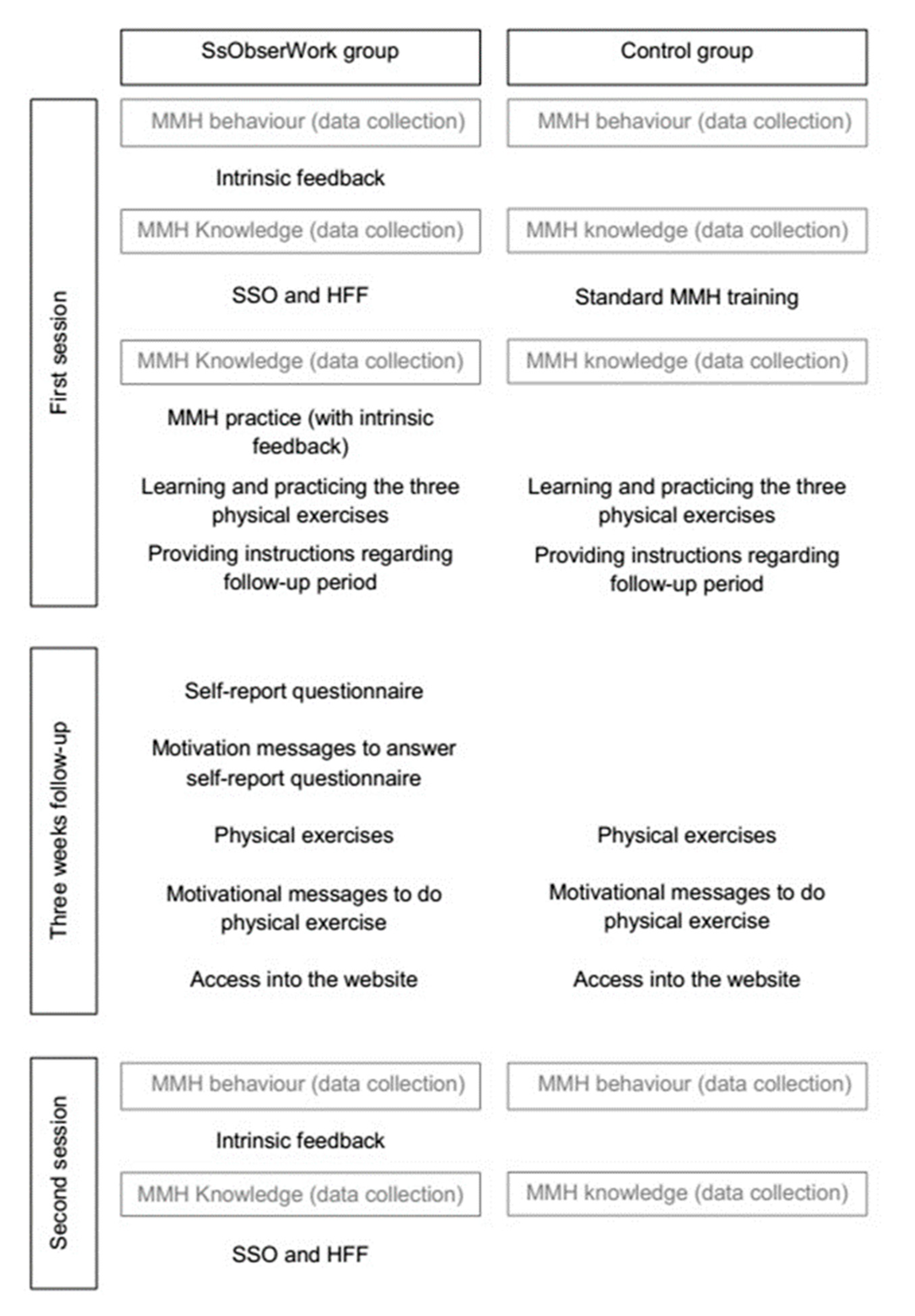
2.3. Intervention
2.4. Measures
2.5. Data Management
2.6. Statistical Analysis
3. Results
3.1. Baseline Characteristics of Participants
3.2. MMH Knowledge
3.3. MMH Behaviour
3.4. Supplementary Analysis
4. Discussion
Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
| Components | |
| Systematic self-observation (SSO) | After the MMH performance and recording, the SSO was done. It consisted of observing their own MMH performance by using a self-observation instrument that guides the observation and direct worker’s attention towards error detection or emphasise positive behaviours. |
| Hetero-observational feedback and feedforward (HFF) | It was provided during the SSO by the technician. It contributed to the worker’s direct attention towards qualitative information, such as whether what they do is recommended or not, and what and how to change (feedforward). |
| Self-report questionnaire | Through an ad hoc on-line questionnaire, workers self-reported aspects related to MMH tasks and physical exercise that they did every day (workplace and daily life) during the three-week follow-up. The questions were focused on frequency of MMH, implementation of technique learned, and performing of the physical exercises taught. The questionnaire had to be completed once a day by using a mobile phone. The aim was to complement the self-observation implemented during face-to-face sessions, by doing it every day. |
| Intrinsic feedback | Immediately after the MMH performance, workers had to recall and indicate how each body part was generally positioned during the MMH (for each phase) by using the self-observation instrument. The aim was to make workers aware of the importance of paying attention to the proprioceptive information and correcting oneself. Intrinsic feedback is also promoted during MMH practice. |
| Physical exercise | Three exercises were taught during the first session. These three exercises were chosen because are highly associated with the MMH movement pattern. These exercises train to adopt a neutral back and help to fit the body. The exercises were abdominal hollowing, hip hinge, and half -squat (at least 10 repetitions of each exercise had to be performed per day). |
| Motivational text messages | Motivational text messages were sent every day to their mobile phones and were used to reinforce and remind workers to adopt and implement what they had learned. There were two types of text messages: (a) Those used to motivate to do the three physical exercises. The message content was adapted to each worker according to their stage of change in physical exercise. Every day, the content was different. (b) Those used to remind workers to complete the self-report questionnaire. The text messages were sent every day in a strategic time of the day (when the worker was out of work) and a questionnaire link was attached in the text message. |
| Formative Activities | |
| MMH practice | Activity done in the first session. It was carried out after the SSO. Workers could practice and experience the MMH technique taught. Workers had to move a box and other things (e.g., a 5-litre bottle of water). By practicing the MMH technique, intrinsic feedback was potentiated and workers could identify benefits and resolve the barriers that were identified. It contributed to raise self-efficacy perception. |
| Physical exercise practice | The technician showed and taught how to perform each physical exercise. While workers had to perform each exercise, the technician corrected all the mistakes in order to make sure that workers would perform each exercise at home properly. |
| Didactic Material | |
| Self-observation instrument | It guided the observation and directed the worker’s attention towards each body part involved in the MMH task. |
| Website and informative triptych | Both sources provided all the information to eliminate any type of barrier related to forgetting how to do all exercises and the MMH technique. The website provided audio-visual information (videos), and on the other hand, the triptych provided written information with pictures. |
Appendix B
| Before and after the First Session | At the Beginning of the First and the Second Session | ||||||||
|---|---|---|---|---|---|---|---|---|---|
| Outcome (Criteria Position) | Groups Depending on Number of Days | Differences between Groups | Differences between Groups | ||||||
| Mean | SD | χ2 | P-value | Mean | SD | χ2 | p-Value | ||
| Feet | 1 to 5 days | 1.75 | 0.5 | 0.757 | 0.685 | 1.00 | 1.15 | 0.86 | 0.649 |
| 6 to 10 days | 1.28 | 0.95 | 1.00 | 1.29 | |||||
| 11 to 15 days | 1.33 | 0.98 | 0.42 | 1.44 | |||||
| Knees joint | 1 to 5 days | −0.25 | 0.50 | 2.942 | 0.230 | - | - | 0.48 | 0.787 |
| 6 to 10 days | 0.42 | 0.79 | 0.14 | 1.07 | |||||
| 11 to 15 days | 0.58 | 1.08 | 0.33 | 1.15 | |||||
| Back | 1 to 5 days | 0.50 | 0.58 | 0.297 | 0.862 | −0.55 | 0.50 | 1.32 | 0.517 |
| 6 to 10 days | 1.14 | 1.46 | 1.00 | 1.29 | |||||
| 11 to 15 days | 0.58 | 0.99 | 0.25 | 1.21 | |||||
| Elbows joint | 1 to 5 days | 2.25 | 0.96 | 0.709 | 0.701 | 0–75 | 1.71 | 0.886 | 0.642 |
| 6 to 10 days | 1.14 | 1.34 | 0.86 | 1.21 | |||||
| 11 to 15 days | 1.17 | 1.53 | 1.25 | 1.22 | |||||
| Load position | 1 to 5 days | 0.25 | 0.50 | 2.267 | 0.322 | 0.25 | 0.50 | 2.064 | 0.356 |
| 6 to 10 days | 0.58 | 1.16 | −0.14 | 0.38 | |||||
| 11 to 15 days | - | - | 0.50 | 1.24 | |||||
| Outcome (Criteria Position) | Groups Depending on Number of Days | Differences between Groups | |||||
|---|---|---|---|---|---|---|---|
| Mean | SD | χ2 | p-Value | F | p-Value | ||
| Feet | 0 days | 37.8 | 26.2 | 4.40 | 0.221 | ||
| 1 to 5 days | 19.5 | 22.9 | |||||
| 6 to 10 days | 5.6 | 53.2 | |||||
| 11 to 15 days | 11.6 | 27.8 | |||||
| Knees joint | 0 days | 6.4 | 22.7 | 0.178 | 0.911 | ||
| 1 to 5 days | 16.8 | 33.6 | |||||
| 6 to 10 days | 16.8 | 20.8 | |||||
| 11 to 15 days | 11.4 | 25.9 | |||||
| Back | 0 days | 11.7 | 19.6 | 1.23 | 0.745 | ||
| 1 to 5 days | 4.4 | 15.8 | |||||
| 6 to 10 days | 2.7 | 15.9 | |||||
| 11 to 15 days | 8.8 | 17.2 | |||||
| Elbows joint | 0 days | 17.7 | 34.7 | 1.71 | 0.635 | ||
| 1 to 5 days | 52.6 | 34.7 | |||||
| 6 to 10 days | 32.4 | 49.9 | |||||
| 11 to 15 days | 33.1 | 36.6 | |||||
| Load position | 0 days | 18.1 | 17.9 | 0.88 | 0.831 | ||
| 1 to 5 days | 12.3 | 15.5 | |||||
| 6 to 10 days | 16.4 | 31.9 | |||||
| 11 to 15 days | 7.7 | 16.7 | |||||
| Interaction between back tilt and move around | 0 days | 7.1 | 8.2 | 1.93 | 0.587 | ||
| 1 to 5 days | 3.0 | 6.4 | |||||
| 6 to 10 days | 2.3 | 5.0 | |||||
| 11 to 15 days | 6.4 | 8.8 | |||||
References
- Bruce, P.; Bernard, M.D. Musculoskeletal Disorders and Workplace Factors; DHHS (NIOSH) Publication No. 97B141.; National Institute for Occupational Safety and Health: Cincinnati, OH, USA, 1997. [Google Scholar]
- Goncharenko, I.M.; Komleva, N.E.; Chekhonatsky, A.A. Lower back pain at workplace: Prevalence and risk factors. Russ Open Med. J. 2020, 9, e0207. [Google Scholar] [CrossRef]
- The Council of European Communities. Council Directive 90/269/EEC. The minimum health and safety requirements for the manual handling of loads where there is a risk particularly of back injury to workers (fourth individual directive within the meaning of article 16 (1) of Directive 89/391/EEC). Off. J. L 1990, 156, 9. [Google Scholar]
- van der Beek, A.J.; Dennerlein, J.T.; Huysmans, M.A.; Mathiassen, S.E.; Burdorf, A.; van Mechelen, W.; van Dieën, J.H.; Frings-Dresen, M.H.W.; Holtermann, A.; Janwantanakul, P.; et al. A research framework for the development and implementation of interventions preventing work-related musculoskeletal disorders. Scand. J. Work Environ. Health 2017, 43, 526–539. [Google Scholar] [CrossRef] [PubMed]
- Denis, D.; Gonella, M.; Comeau, M.; Lauzier, M. Why Doesn’t Training Based on Safe Handling Techniques Work? A Critical Review of the Literature; IRSST—Communications and Knowledge Transfer Division: Montréal, QC, Canada, 2019; ISBN 9782897970574. [Google Scholar]
- Denis, D.; Gonella, M.; Comeau, M.; Lauzier, M. Questioning the value of manual material handling training: A scoping and critical literature review. Appl. Ergon. 2020, 89, 103186. [Google Scholar] [CrossRef] [PubMed]
- Hogan, D.A.; Greiner, B.A.; O’Sullivan, L. The effect of manual handling training on achieving training transfer, employees’s behaviour change and subsequent reduction of work-related musculoskeletal disorders: A systematic review. Ergonomics 2014, 57, 93–107. [Google Scholar] [CrossRef] [PubMed]
- Yehoyakim, M.; Bellefeuille, S.; Côté, J.N.; Plamondon, A. Relationship between leg and back strength with inter-joint coordination of females during lifting. Int. J. Ind. Ergon. 2016, 56, 32–40. [Google Scholar] [CrossRef]
- Bayram, M. Safety training and competence, employee participation and involvement, employee satisfaction, and safety performance: An empirical study on occupational health and safety management system implementing manufacturing firms. Alphanumeric J. 2019, 7, 301–318. [Google Scholar] [CrossRef]
- Dowrick, P.W. Self-modeling: Expanding the theories of learning. Psychol. Sch. 2012, 49, 30–41. [Google Scholar] [CrossRef]
- Garcia, I.; James, R.W.; Bischof, P.; Baroffio, A. Self-observation and peer feedback as a faculty development approach for problem-based learning tutors: A program evaluation. Teach. Learn. Med. 2017, 29, 313–325. [Google Scholar] [CrossRef]
- Seok, S.; DaCosta, B.; McHenry-Powell, M.; Heitzman-Powell, L.S.; Ostmeyer, K. A systematic review of evidence-based video modeling for students with emotional and behavioral disorders. Educ. Sci. 2018, 8, 170. [Google Scholar] [CrossRef]
- Marques, P.G.; Corrêa, U.C. The effect of learner’s control of self-observation strategies on learning of front crawl. Acta Psychol. 2016, 164, 151–156. [Google Scholar] [CrossRef] [PubMed]
- Garcia-Marques, P.; Alves-Thon, R.; Espanhol, J.; Tani, G.; Cesar-Corrêa, U. The intermediate learner’s choice of self-as-a-model strategies and the eight-session practice in learning of the front crawl swim. Kinesiology 2017, 49, 57–64. [Google Scholar] [CrossRef][Green Version]
- Brouwer, N.; Besselink, E.; Oosterheert, I. The power of video feedback with structured viewing guides. Teach. Teach. Educ. 2017, 66, 60–73. [Google Scholar] [CrossRef]
- Major, L.; Watson, S. Using video to support in-service teacher professionals development: The state of the field, limitations and possibilities. Technol. Pedagog. Inf. 2018, 27, 49–68. [Google Scholar] [CrossRef]
- Taieb-Maimon, M.; Cwikel, J.; Shapira, B.; Orenstein, I. The effectiveness of a training method using self-modeling webcam photos for reducing musculoskeletal risk among office workers using computers. Appl. Ergon. 2012, 43, 376–385. [Google Scholar] [CrossRef]
- Backåberg, S.; Rask, M.; Gummesson, C.; Brunt, D. Video-based feedback combined with reflective enquiry—An interactive model for movement awareness among nursing students. Nord. J. Digit. Lit. 2015, 10, 246–264. [Google Scholar]
- Backåberg, S.; Gummesson, C.; Brunt, D.; Rask, M. Is that a really my movement?—Students’ experiences of a video-supported interactive learning model for movement awareness. Int. J. Qual. Stud. Health. 2015, 10, 28474. [Google Scholar] [CrossRef]
- Schmidt, R.A.; Lee, T.D. Motor Learning and Performance. Principles to Application, 6th ed.; Human Kinetics: Champaign, IL, USA, 2020; ISBN 9781492571186. [Google Scholar]
- Giannousi, M.; Mountaki, F.; Kioumourtzoglou, E. The effects of verbal and visual feedback on performance and learning freestyle swimming in novice swimmers. Kinesiology 2017, 49, 65–73. [Google Scholar] [CrossRef]
- Shiffman, S.; Stone, A.A.; Hufford, M.R. Ecological momentary assessment. Annu. Rev. Clin. Psycho. 2008, 4, 1–32. [Google Scholar] [CrossRef]
- Portell, M.; Anguera, M.T.; Hernández-Mendo, A.; Jonsson, G.K. Quantifying biopsychosocial aspects in everyday contexts: An integrative methodological approach form the behavioral sciences. Psychol. Res. Behav. Manag. 2015, 8, 153–160. [Google Scholar] [CrossRef][Green Version]
- Batink, T.; Bakker, J.; Vaessen, T.; Kasanova, Z.; Collip, D.; van Os, J.; Wichers, M.; Germeys, I.; Peeters, F. Acceptance and commitment therapy in daily life training: A feasibility study of an mHealth intervention. JMIR Mhealth Uhealth 2016, 4, e103. [Google Scholar] [CrossRef]
- Reynolds, B.M.; Robles, T.F.; Repetti, R.L. Measurement reactivity and fatigue effects in daily diary research with families. Dev. Psychol. 2016, 52, 442–456. [Google Scholar] [CrossRef] [PubMed]
- Otte, F.W.; Davids, K.; Millar, S.K.; Klatt, S. When and how to provide feedback and instructions to athletes?—How sport psychology and pedagogy insights can improve coaching interventions to enhance self-regulation in training. Front. Psychol. 2020, 11, 1444. [Google Scholar] [CrossRef]
- Anguera, M.T.; Blanco-Villaseñor, A.; Losada, J.L.; Sánchez-Algarra, P.; Onwuegbuzie, A.J. Revisiting the difference between mixed methods and multimethods: Is it all in the name? Qual. Quant. 2018, 52, 2757–2770. [Google Scholar] [CrossRef]
- Portell, M.; Anguera, M.T.; Chacón-Moscoso, S.; Sanduvete-Chaves, S. Guidelines for reporting evaluations based on observational methodology. Psicothema 2015, 27, 283–289. [Google Scholar] [CrossRef] [PubMed]
- Anguera, M.T.; Portell, M.; Chacón-Moscoso, S.; Sanduvete-Chaves, S. Indirect observation in everyday contexts: Concepts and methodological guidelines within a mixed methods framework. Front. Psychol. 2018, 9, 1–20. [Google Scholar] [CrossRef]
- Chacón-Moscoso, S.; Anguera, M.T.; Sanduvete-Chaves, S.; Losada, J.L.; Lozano-Lozano, J.A.; Portell, M. Methodological quality checklist for studies based on observational methodology (MQCOM). Psicothema 2019, 31, 458–464. [Google Scholar] [CrossRef] [PubMed]
- Chacón-Moscoso, S.; Sanduvete-Chaves, S.; Anguera, M.T.; Losada, J.L.; Portell, M.; Lozano-Lozano, J.A. Preliminary checklist for reporting observational studies in sports areas: Content validity. Front. Psychol. 2018, 9, 291. [Google Scholar] [CrossRef]
- Janz, N.K.; Becker, M.H. The health belief model: A decade later. Health Educ. Quart. 1984, 11, 1–74. [Google Scholar] [CrossRef]
- Prochaska, J.O.; DiClemente, C.C.; Norcross, J.C. In search of how people change. Applications to addictive behaviors. Health Psychol. 1992, 47, 1102–1114. [Google Scholar] [CrossRef]
- Kuorinka, I.; Jonsson, B.; Kilbom, A.; Vinterberg, H.; Biering-Sørensen, F.; Andersson, G.; Jørgensen, K. Standarised Nordic questionnaires for the analysis of musculoskeletal symptoms. Appl. Ergon. 1987, 18, 233–237. [Google Scholar] [CrossRef]
- Ware, J.E.; Kosinski, M.; Turner-Bowker, D.M.; Gandek, B. User’s Manual for the SF-12v2 Health Survey (with a Supplement Documenting SF-12 Health Survey); QualityMetric Incorporated: Lincoln, RI, USA, 2009. [Google Scholar]
- Schaufeli, W.; Bakker, A. Utrecht Work Engagement Scale (Preliminary Manual); Utrecht University, Occupational Health Psychology Unit: Utrecht, The Netherlands, 2003. [Google Scholar]
- Marcus, B.H.; Selby, V.C.; Niaura, R.S.; Rossi, J.S. Self-efficacy and the stages of exercise behavior change. Res. Q. Exerc. Sport 1992, 63, 60–66. [Google Scholar] [CrossRef]
- Portell, M.; Sene-Mir, A.M.; Anguera, M.T.; Jonsson, G.K.; Losada, J.L. Support system for the assessment and intervention during the manual material handling training at the workplace: Contributions from the systematic observation. Front. Psychol. 2019, 10, 1–18. [Google Scholar] [CrossRef] [PubMed]
- Bakeman, R.; Quera, V.; Gnisci, A. Observer agreement for timed-event sequential data: A comparison of time-based and event-based algorithms. Behav. Res. Methods 2009, 41, 137–147. [Google Scholar] [CrossRef]
- Gabín, B.; Camerino, O.; Anguera, M.T.; Castañer, M. Lince: Multiplatform sport analysis software. Procedia Soc. Behav. Sci. 2012, 46, 4692–4694. [Google Scholar] [CrossRef]
- Cliff, N. Dominance statistics: Ordinal analyses to answer ordinal questions. Psychol. Bull. 1993, 114, 494–509. [Google Scholar] [CrossRef]
- Romano, J.; Kromrey, J.D.; Coraggio, J.; Skowronek, J.; Devine, L. Exploring methods for evaluating group differences on the NSSE and other surveys: Are the t-test and Cohen’s d indices the most appropriate choices? In Proceedings of the Annual Meeting of the Southern Association for Institutional Research, Arlington, VA, USA, 14–17 October 2006. [Google Scholar]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences, 2nd ed.; Lawrence Erlbaum Associates: New York, NY, USA, 1988. [Google Scholar]
- Magnusson, M.S. T-Pattern detection and analysis (TPA) with THEMETM: A mixed methods approach. Front. Psychol. 2020, 10, 2663. [Google Scholar] [CrossRef] [PubMed]
- Magnusson, M.S. T-Patterns, external memory and mass-societies in proteins and humans: In an eye-blink the naked ape became a string-controlled citizen. Physiol. Behav. 2020, 227, 113146. [Google Scholar] [CrossRef]
- Casarrubea, M.; Jonsson, G.K.; Faulisi, F.; Sorbera, F.; Di Giovanni, G.; Benigno, A.; Crescimanno, G.; Magnusson, M.S. T-pattern analysis for the study of temporal structure of animal and human behavior: A comprensive review. J. Neurosci. Meth. 2015, 239, 34–46. [Google Scholar] [CrossRef]
- Diana, B.; Zurloni, V.; Elia, M.; Cavalera, C.; Realdon, O.; Jonsson, G.K.; Anguera, M.T. T-Pattern analysis and cognitive load manipulation to detect low-stake lies: An exploratory study. Front. Psychol. 2018, 9, 1–16. [Google Scholar] [CrossRef]
- Kim, H.K.; Zhang, Y. Estimation of lumbar spinal loading and trunk muscle forces during asymmetric lifting tasks: Application of whole-body musculoskeletal modelling in OpenSim. Ergonomics 2017, 60, 563–576. [Google Scholar] [CrossRef]
- Linnerooth, P.J.N.; Houlihan, D.; Lenz, M.A.; Buchanan, J. A comparison of covert and videotape modeling strategies for training complex mechanical assembly tasks. J. Cogn. Eng. Decis. Mak. 2014, 8, 203–218. [Google Scholar] [CrossRef]
| SsObserWork Group | Control Group | |
|---|---|---|
| Sex: N (%) | ||
| Men | 12 (38.7) | 14 (46.7) |
| Women | 19 (61.3) | 16 (53.3) |
| Age: N (%) | ||
| 18 to 28 years | - | 2 (6.7) |
| 29 to 39 years | 12 (38.7) | 10 (33.3) |
| 40 to 50 years | 11 (35.5) | 7 (23.3) |
| +50 years | 8 (25.8) | 11 (36.7) |
| Years working in the company: N (%) | ||
| Less than one year | 1 (3.2) | 2 (6.7) |
| 1 to 5 years | 7 (22.6) | 7 (23.3) |
| 5 to 10 years | 7 (22.6) | 7 (23.3) |
| More than 10 years | 16 (51.6) | 14 (46.7) |
| Musculoskeletal disorders in the last 12 months: N (%) | ||
| Suffered pain or discomfort at any body part | 30 (96.8) | 21 (70) |
| Suffered lower back pain or discomfort a | 16 (53.3) | 15 (71.4) |
| Stage of change in physical exercise: N (%) | ||
| Precontemplation | 3 (9.7) | 3 (10) |
| Contemplation | 2 (6.5) | 6 (20) |
| Preparation | 14 (45.2) | 12 (40) |
| Action | - | - |
| Maintenance | 12 (38.7) | 9 (30) |
| Self-perceived health status: M (SD) | ||
| Physical Component Summary | 50.69 (7.01) | 49.47 (7.78) |
| Mental Component Summary | 50.18 (5.89) | 50.20 (6.07) |
| Work engagement: M (SD) | ||
| Vigor | 4.51 (1.11) | 4.69 (0.95) |
| Dedication | 3.90 (1.67) | 3.97 (1.49) |
| Absorption | 4.09 (1.36) | 4.17 (1.44) |
| Total score | 4.19 (1.26) | 4.29 (1.16) |
| Before and after the First Session a | At the Beginning of the First and the Second Session b | |||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Outcome (Criteria Position) | SsObserWork Group | Control Group | Differences between Groups | Effect Size | SsObserWork Group | Control Group | Differences between Groups | Effect Size | ||||||
| Mean | SD | Mean | SD | U c | p-Value | δ d | Mean | SD | Mean | SD | U | p-Value | δ | |
| Feet | 1.33 | 1.06 | 1.53 | 0.78 | −0.514 | 0.607 | −0.06 | 0.68 | 1.31 | 0.44 | 1.31 | −0.635 | 0.525 | 0.09 |
| Knees joint | 0.37 | 0.85 | 0.73 | 1.08 | −1.547 | 0.122 | −0.20 | 0.25 | 0.97 | 0.63 | 1.36 | −1.406 | 0.160 | −0.20 |
| Back | 0.63 | 1.03 | 0.10 | 0.61 | −2.113 | 0.035 * | 0.24 | 0.25 | 1.21 | −0.48 | 1.40 | −2.032 | 0.042 * | 0.29 |
| Elbows joint | 1.47 | 1.31 | 1.03 | 1.22 | −1.482 | 0.138 | 0.22 | 1.11 | 1.26 | 0.52 | 1.42 | −1.579 | 0.114 | 0.24 |
| Load position | 0.47 | 0.97 | 0.80 | 1.19 | −0.988 | 0.323 | −0.12 | 0.36 | 1.03 | 0.30 | 0.91 | −0.010 | 0.992 | 0.00 |
| SsObserWork Group a | Control Group b | Differences between Groups | Effect Size | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Mean | SD | Median | Mean | SD | Median | U c/t d | P-value | δ e/d f | |
| Feet | 15.34 | 33.89 | 0.00 | 6.22 | 27.41 | 0.00 | −1.884 c | 0.060 | 0.27 e |
| Knees joint | 12.69 | 24.42 | 9.79 | 1.45 | 15.04 | −2.49 | 2.025 d | 0.049 * | 0.55 f |
| Back | 7.21 | 16.37 | 3.72 | −5.89 | 16.01 | −6.78 | −2.615 c | 0.009 ** | 0.42 e |
| Elbows joint | 33.58 | 38.33 | 11.29 | 9.11 | 31.13 | 4.04 | −2.313 c | 0.021 * | 0.37 e |
| Load position | 11.86 | 20.23 | 9.55 | 4.29 | 21.66 | −2.72 | −1.619 c | 0.105 | 0.26 e |
| Interaction between back tilt and move around | 5.10 | 7.53 | 2.87 | 3.08 | 17.00 | 0.17 | −2.366 c | 0.018* | 0.38 e |
| First Session | Second Session | Differences between Sessions | ||||
|---|---|---|---|---|---|---|
| N | % | N | % | χ2 | p-Value | |
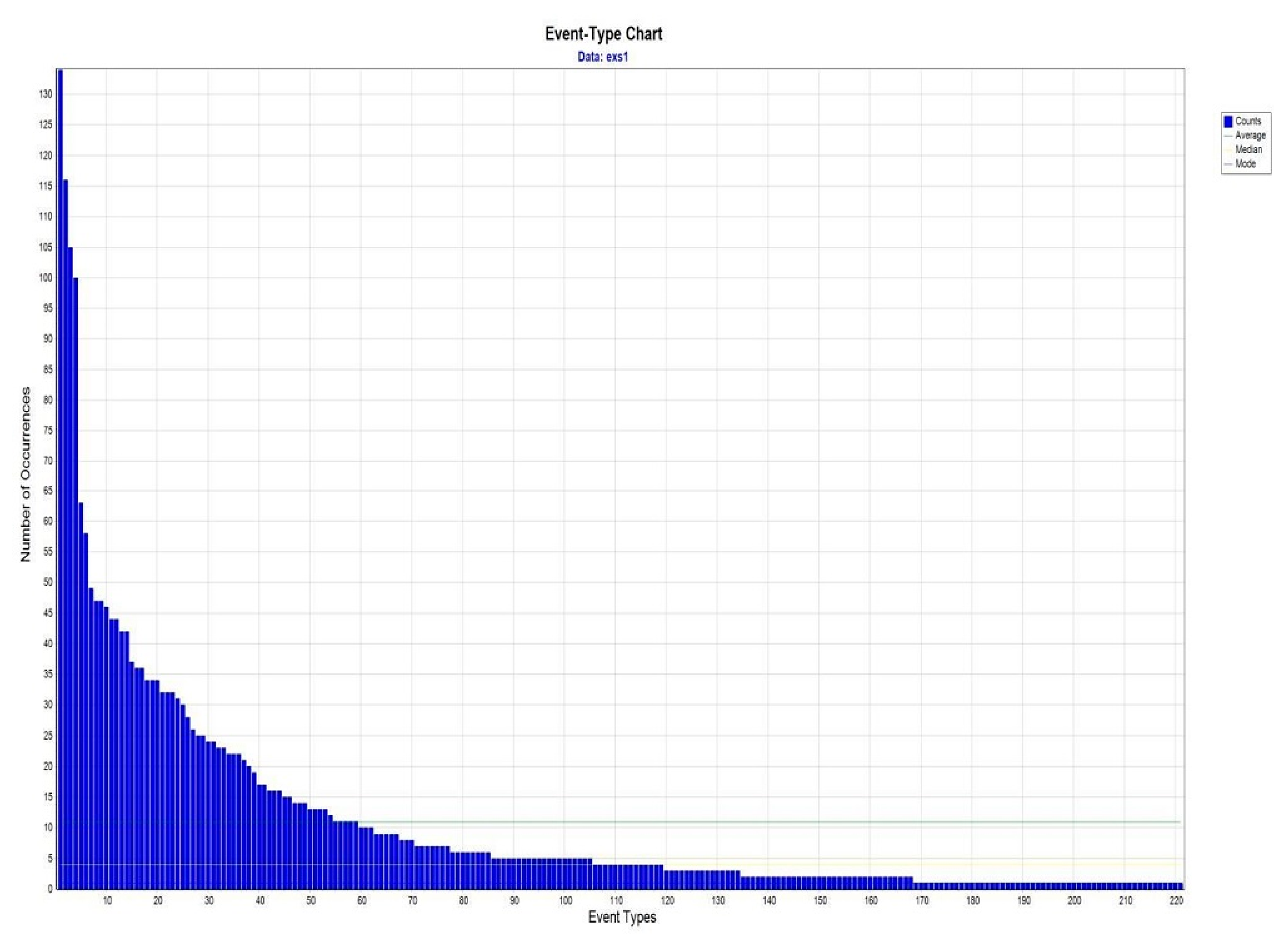
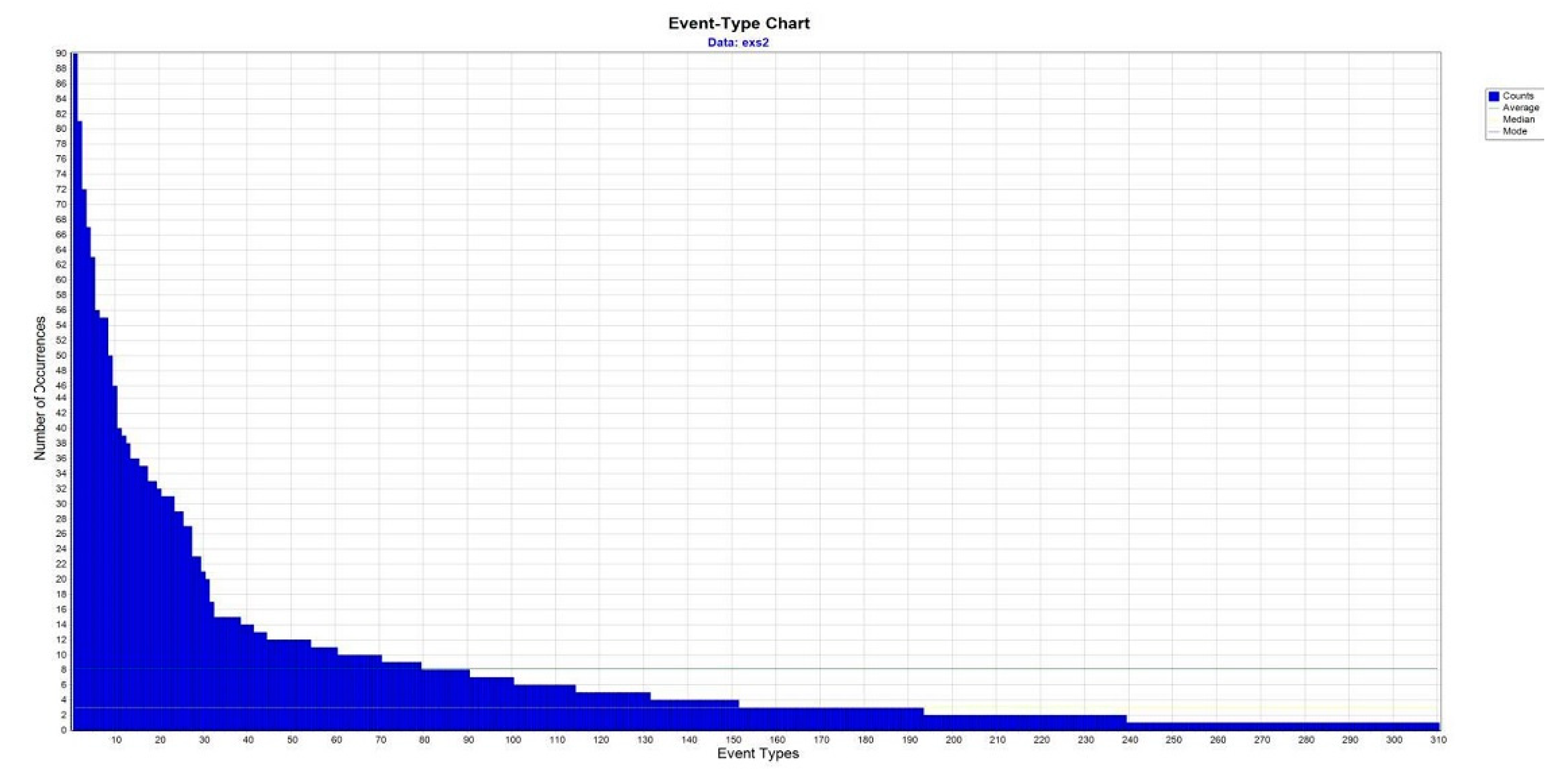
| Event types | 221 | 310 | ||||
| Event types with RBP | 20.9 | 28.4 | 37.769 | <0.0005 ** | ||
| T-pattern detected | 3414 | 446 | ||||
| T-patterns included RBP | 84 | 100 | 83.080 | <0.0005 ** | ||
| T-patterns (all events included with RBP) | 14 | 100 | 1602.296 | <0.0005 ** | ||
| T-patterns included RBP, RLP, REJP | 7 | 50 | 713.756 | <0.0005 ** | ||
| First Session | Second Session | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| N | Mean | SD | Min-Max | % | N | Mean | SD | Min-Max | % | |
| T-pattern different | 90 | . | . | . | . | 9 | . | . | . | . |
| Length | . | 2.848 | 0.733 | 2–4 | . | . | 2.333 | 0.5 | 2–3 | . |
| Level | . | 1.778 | 0.667 | 1–3 | . | . | 1.333 | 0.5 | 1–2 | . |
| Occurrences | . | 37.933 | 10.351 | 23–84 | . | . | 49.556 | 10.725 | 37–64 | . |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sene-Mir, A.M.; Portell, M.; Anguera, M.T.; Chacón-Moscoso, S. Manual Material Handling Training: The Effect of Self-Observation, Hetero-Observational and Intrinsic Feedback on Workers’ Knowledge and Behaviour. Int. J. Environ. Res. Public Health 2020, 17, 8095. https://doi.org/10.3390/ijerph17218095
Sene-Mir AM, Portell M, Anguera MT, Chacón-Moscoso S. Manual Material Handling Training: The Effect of Self-Observation, Hetero-Observational and Intrinsic Feedback on Workers’ Knowledge and Behaviour. International Journal of Environmental Research and Public Health. 2020; 17(21):8095. https://doi.org/10.3390/ijerph17218095
Chicago/Turabian StyleSene-Mir, Anna M., Mariona Portell, M. Teresa Anguera, and Salvador Chacón-Moscoso. 2020. "Manual Material Handling Training: The Effect of Self-Observation, Hetero-Observational and Intrinsic Feedback on Workers’ Knowledge and Behaviour" International Journal of Environmental Research and Public Health 17, no. 21: 8095. https://doi.org/10.3390/ijerph17218095
APA StyleSene-Mir, A. M., Portell, M., Anguera, M. T., & Chacón-Moscoso, S. (2020). Manual Material Handling Training: The Effect of Self-Observation, Hetero-Observational and Intrinsic Feedback on Workers’ Knowledge and Behaviour. International Journal of Environmental Research and Public Health, 17(21), 8095. https://doi.org/10.3390/ijerph17218095





