Socio-Ecological Factors Associated with Dengue Risk and Aedes aegypti Presence in the Galápagos Islands, Ecuador
Abstract
1. Introduction
2. Materials and Methods
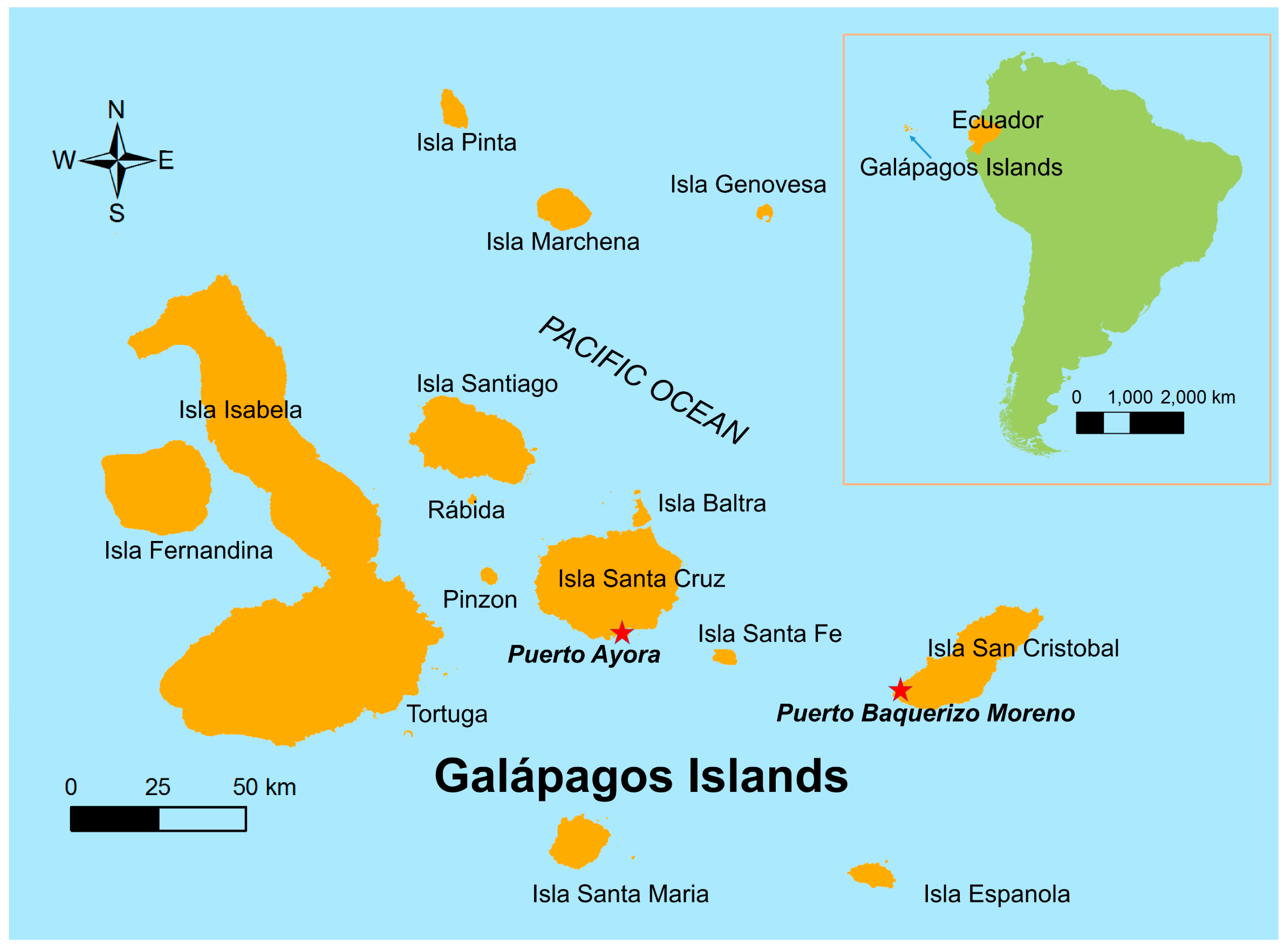
2.1. Study Site
2.2. Ethics Statement
2.3. Field Data Collection
2.4. Statistical Models
3. Results
3.1. Risk Perceptions and Practices
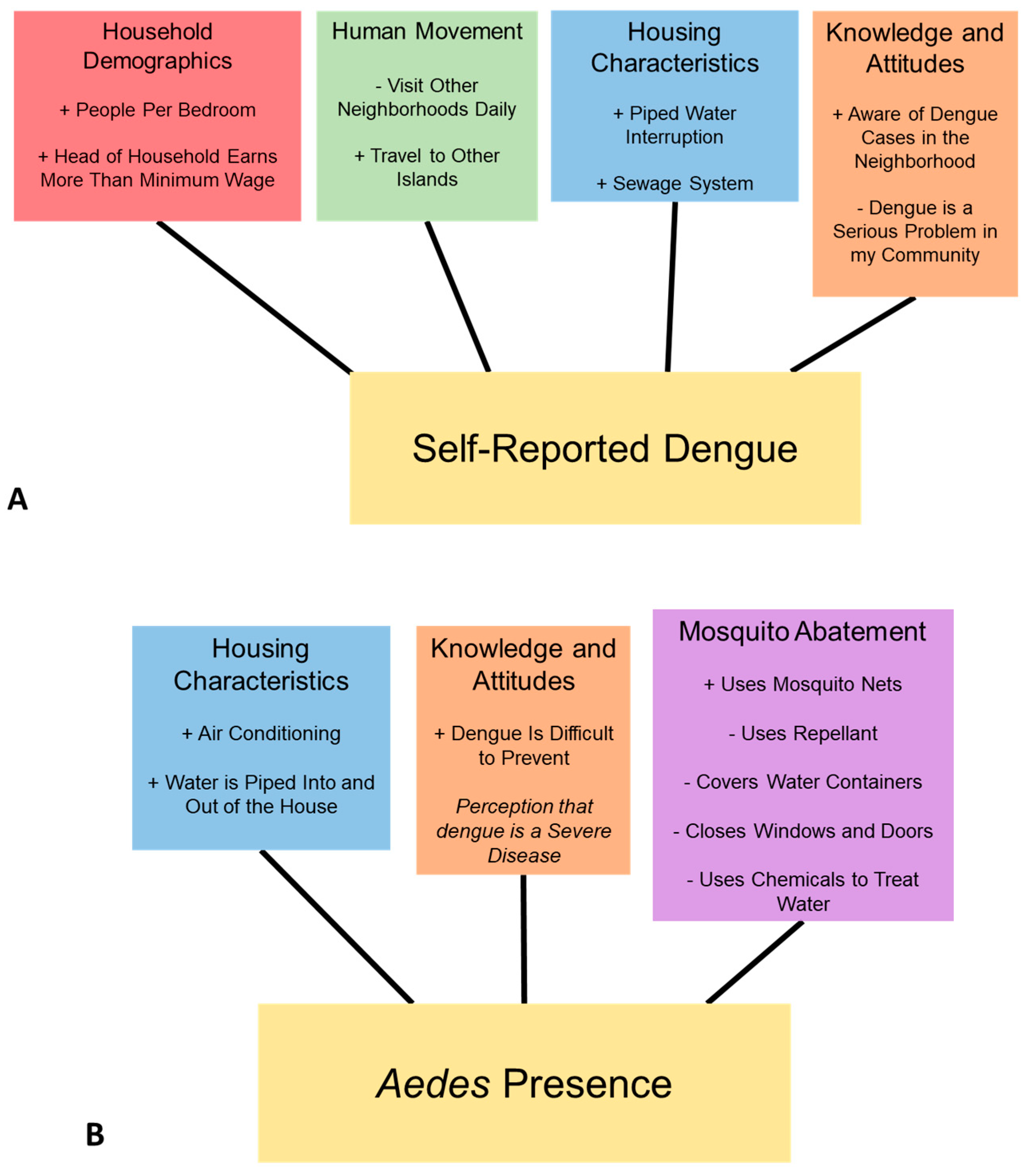
3.2. Model Selection Outcomes
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Bhatt, S.; Gething, P.W.; Brady, O.J.; Messina, J.P.; Farlow, A.W.; Moyes, C.L.; Drake, J.M.; Brownstein, J.S.; Hoen, A.G.; Sankoh, O.; et al. The global distribution and burden of dengue. Nature 2013, 496, 504–507. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Global Strategy for Dengue Prevention and Control 2012–2020. Available online: http://apps.who.int/iris/bitstream/10665/75303/1/9789241504034_eng.pdf (accessed on 13 February 2017).
- World Health Organization. Special Programme for Research and Training in Tropical Diseases. In Dengue: Guidelines for Diagnosis, Treatment, Prevention and Control; World Health Organization: Geneva, Switzerland, 2009. [Google Scholar]
- Gubler, D.J.; Meltzer, M. Impact of dengue/dengue hemorrhagic fever on the developing world. Adv. Virus Res. 1999, 53, 35–70. [Google Scholar] [PubMed]
- Stewart-Ibarra, A.M.; Ryan, S.J.; Kenneson, A.; King, C.A.; Abbott, M.; Barbachano-Guerrero, A.; Beltrán-Ayala, E.; Borbor-Cordova, M.J.; Cárdenas, W.B.; Cueva, C.; et al. The Burden of Dengue Fever and Chikungunya in Southern Coastal Ecuador: Epidemiology, Clinical Presentation, and Phylogenetics from the First Two Years of a Prospective Study. Am. J. Trop. Med. Hyg. 2018, 98, 1444. [Google Scholar] [CrossRef] [PubMed]
- Hemingway, J.; Ranson, H. Insecticide resistance in insect vectors of human disease. Annu. Rev. Entomol. 2000, 45, 371–391. [Google Scholar] [CrossRef] [PubMed]
- Liu, N. Insecticide resistance in mosquitoes: Impact, mechanisms, and research directions. Annu. Rev. Entomol. 2015, 60, 537–559. [Google Scholar] [CrossRef] [PubMed]
- Gonzalez, V.; Jurado, H. Guayaquil: Aedes aegypti, 1740–2007; Servicio Nacional para La Eradicaccion de Malaria (SNEM): Guayaquil, Ecuador, 2007.
- Alava, A.; Mosquera, C.; Vargas, W.; Real, J. Dengue en el Ecuador 1989–2002. Rev. Ecuat. Hig. Med. Trop. 2005, 42, 11–34. [Google Scholar]
- Gutierrez, E.; Real, J.; Alava, A.; Mosquera, C. Epidemia de Dengue Hemorragico en el Ecuador, 2003. Rev. Ecuat. Hig. Med. Trop. 2005, 42, 35–49. [Google Scholar]
- Alava, A.; Suarez, C.; Mosquera, C.; Vargas, I.; Montesdeoca, J. Dengue en el Ecuador: Consideraciones de laboratorio. Rev. Ecuat. Hig. Med. Trop. 1992, 40, 5–22. [Google Scholar]
- World Health Organization. 2002—Dengue/Dengue Hemorrhagic Fever in Ecuador. Available online: http://www.who.int/csr/don/2002_08_16/en/ (accessed on 13 February 2017).
- Feldstein, L.R.; Brownstein, J.S.; Brady, O.J.; Hay, S.I.; Johansson, M.A. Dengue on islands: A Bayesian approach to understanding the global ecology of dengue viruses. Trans. R. Soc. Trop. Med. Hyg. 2015, 109, 303–312. [Google Scholar] [CrossRef] [PubMed]
- González, J.A.; Montes, C.; Rodríguez, J.; Tapia, W. Rethinking the Galapagos Islands as a complex social-ecological system: Implications for conservation and management. Ecol. Soc. 2008, 13, 13. [Google Scholar] [CrossRef]
- National Institute of Statistics and Census (INEC). Proyección de la Población Ecuatoriana, por años Calendario, Según Regiones, Provincias y Sexo: Periodo 2010–2020. Available online: http://www.ecuadorencifras.gob.ec/documentos/web-inec/Poblacion_y_Demografia/Proyecciones_Poblacionales/proyeccion_cantonal_total_2010-2020.xlsx (accessed on 13 February 2017).
- El turismo en las Islas Galápagos creció un 6% en el 2014. Available online: http://www.eluniverso.com/noticias/2015/05/05/nota/4840906/turismo-islas-galapagos-crecio-6-2014 (accessed on 31 January 2017).
- Wikelski, M.; Foufopoulos, J.; Vargas, H.; Snell, H. Galápagos Birds and Diseases: Invasive Pathogens as Threats for Island Species. Ecol. Soc. 2004, 9. [Google Scholar] [CrossRef]
- Kilpatrick, A.M.; Daszak, P.; Goodman, S.J.; Rogg, H.; Kramer, L.D.; Cedeño, V.; Cunningham, A.A. Predicting Pathogen Introduction: West Nile Virus Spread to Galápagos. Conserv. Biol. 2006, 20, 1224–1231. [Google Scholar] [CrossRef] [PubMed]
- Eastwood, G.; Goodman, S.J.; Cunningham, A.A.; Kramer, L.D. Aedes taeniorhynchus Vectorial Capacity Informs A Pre-Emptive Assessment of West Nile Virus Establishment in Galápagos. Sci. Rep. 2013, 3, 1519. [Google Scholar] [CrossRef] [PubMed]
- Eastwood, G.; Kramer, L.D.; Goodman, S.J.; Cunningham, A.A. West Nile virus vector competency of Culex quinquefasciatus mosquitoes in the Galápagos Islands. Am. J. Trop. Med. Hyg. 2011, 85, 426–433. [Google Scholar] [CrossRef] [PubMed]
- Stewart Ibarra, A.M.; Luzadis, V.A.; Cordova, M.J.B.; Silva, M.; Ordoñez, T.; Ayala, E.B.; Ryan, S.J. A social-ecological analysis of community perceptions of dengue fever and Aedes aegypti in Machala, Ecuador. BMC Public Health 2014, 14, 1. [Google Scholar] [CrossRef] [PubMed]
- Stewart Ibarra, A.M.; Ryan, S.J.; Beltrán, E.; Mejía, R.; Silva, M.; Muñoz, Á. Dengue Vector Dynamics (Aedes aegypti) Influenced by Climate and Social Factors in Ecuador: Implications for Targeted Control. PLoS ONE 2013, 8, e78263. [Google Scholar] [CrossRef] [PubMed]
- Stoddard, S.T.; Forshey, B.M.; Morrison, A.C.; Paz-Soldan, V.A.; Vazquez-Prokopec, G.M.; Astete, H.; Reiner, R.C., Jr.; Vilcarromero, S.; Elder, J.P.; Halsey, E.S.; et al. House-to-house human movement drives dengue virus transmission. Proc. Natl. Acad. Sci. USA 2013, 110, 994–999. [Google Scholar] [CrossRef] [PubMed]
- Castro, M.; Sánchez, L.; Pérez, D.; Sebrango, C.; Shkedy, Z.; Van der Stuyft, P. The Relationship between Economic Status, Knowledge on Dengue, Risk Perceptions and Practices. PLoS ONE 2013, 8, e81875. [Google Scholar] [CrossRef] [PubMed]
- Braga, C.; Luna, C.F.; Martelli, C.M.; de Souza, W.V.; Cordeiro, M.T.; Alexander, N.; de Albuquerque, M.F.P.M.; SilveiraJúnior, J.C.; Marquesa, E.T. Seroprevalence and risk factors for dengue infection in socioeconomically distinct areas of Recife, Brazil. Acta Trop. 2010, 113. [Google Scholar] [CrossRef] [PubMed]
- Sinclair, B.J. CDF Checklist of Galapagos Flies; Charles Darwin Foundation: Galapagos, Ecuador, 2017. [Google Scholar]
- Bataille, A.; Cunningham, A.A.; Cedeño, V.; Patiño, L.; Constantinou, A.; Kramer, L.D.; Goodman, S.J. Natural colonization and adaptation of a mosquito species in Galápagos and its implications for disease threats to endemic wildlife. Proc. Natl. Acad. Sci. USA 2009, 106, 10230–10235. [Google Scholar] [CrossRef] [PubMed]
- Ministerio de Salud Publica. Registro Historico del Dengue en la Provincia de Galapagos; Ministerio Salud Publica (MSP): Quito, Ecuador, 2014; pp. 1–58.
- Trueman, M.; d’Ozouville, N. Characterizing the Galapagos terrestrial climate in the face of global climate change. Galapagos Res. 2010, 67, 26–37. [Google Scholar]
- Granda, L.M.; Salazar, G.C. Population and migration in Galapagos. In Galapagos Report 2011–2012; GNPS, GCREG, CDF and GC: Galapagos, Ecuador, 2013; pp. 44–51. [Google Scholar]
- Vazquez-Prokopec, G.M.; Galvin, W.A.; Kelly, R.; Kitron, U. A New, Cost-Effective, Battery-Powered Aspirator for Adult Mosquito Collections. J. Med. Entomol. 2009, 46, 1256–1259. [Google Scholar] [CrossRef] [PubMed]
- Focks, D.A. A Review of Entomological Sampling Methods and Indicators for Dengue Vectors; World Health Organization: Geneva, Switzerland, 2003. [Google Scholar]
- Barrera, R.; Amador, M.; Clark, G.G. Use of the pupal survey technique for measuring Aedes aegypti (Diptera: Culicidae) productivity in Puerto Rico. Am. J. Trop. Med. Hyg. 2006, 74, 290–302. [Google Scholar] [CrossRef] [PubMed]
- Manrique-Saide, P.; Che-Mendoza, A.; Rizzo, N.; Arana, B.; Pilger, D.; Lenhart, A.; Kroeger, A. Operational Guide for Assessing the Productivity of Aedes Aegypti Breeding Sites; World Health Organization: Geneva, Switzerland, 2011; pp. 1–30. [Google Scholar]
- R Core Team. R: A Language and Environment for Statistical Computing. Available online: https://www.R-project.org (accessed on 13 February 2017).
- Calcagno, V.; de Mazancourt, C. Glmulti: An R Package for Easy Automated Model Selection with (Generalized) Linear Models. J. Stat. Softw. 2010, 34, 1–29. [Google Scholar] [CrossRef]
- Morrison, A.C.; Zielinski-Gutierrez, E.; Scott, T.W.; Rosenberg, R. Defining challenges and proposing solutions for control of the virus vector Aedes aegypti. PLoS Med. 2008, 5, e68. [Google Scholar] [CrossRef] [PubMed]
- Stoddard, S.T.; Morrison, A.C.; Vazquez-Prokopec, G.M.; Soldan, V.P.; Kochel, T.J.; Kitron, U.; Elder, J.P.; Scott, T.W. The role of human movement in the transmission of vector-borne pathogens. PLoS Negl. Trop. Dis. 2009, 3, e481. [Google Scholar] [CrossRef] [PubMed]
- Stewart Ibarra, A.M.; Munoz, A.G.; Ryan, S.J.; Borbor, M.J.; Ayala, E.B.; Finkelstein, J.L.; Mejía, R.; Ordoñez, T.; Recalde-Coronel, G.C.; Rivero, K. Spatiotemporal clustering, climate periodicity, and social-ecological risk factors for dengue during an outbreak in Machala, Ecuador, in 2010. BMC Infect. Dis. 2014, 14, 610. [Google Scholar] [CrossRef] [PubMed]
- Barrera, R.; Delgado, N.; Jiménez, M.; Valero, S. Eco-epidemiological factors associated with hyperendemic dengue haemorrhagic fever in Maracay City, Venezuela. Dengue Bull. 2002, 26, 84–95. [Google Scholar]
- De Mattos Almeida, M.C.; Caiaffa, W.T.; Assunçao, R.M.; Proietti, F.A. Spatial vulnerability to dengue in a Brazilian urban area during a 7-year surveillance. J. Urban Health. 2007, 84, 334–345. [Google Scholar] [CrossRef] [PubMed]
- Bohra, A.; Andrianasolo, H. Application of GIS in modeling of dengue risk based on sociocultural data: Case of Jalore, Rajasthan, India. Dengue Bull. 2001, 25, 92–102. [Google Scholar]
- Chao, D.-Y.; Lin, T.H.; Chu, P.Y.; Chang, S.J.; Huang, J.H.; Chen, K.T.; King, C.C. Predisposing factors of dengue cases by random effect model in the largest dengue haemorrhagic fever epidemic in Taiwan in 1998. Dengue Bull. WHO 2000, 24, 46–52. [Google Scholar]
- Parks, W.; Lloyd, L. Planning Social Mobilization and Communication for Dengue Fever Prevention and Control; World Health Organization: Geneva, Switzerland, 2004. [Google Scholar]
- Kenneson, A.; Beltrán-Ayala, E.; Borbor-Cordova, M.J.; Polhemus, M.E.; Ryan, S.J.; Endy, T.P.; Stewart-Ibarra, A.M. Social-ecological factors and preventive actions decrease the risk of dengue infection at the household-level: Results from a prospective dengue surveillance study in Machala, Ecuador. PLoS Negl. Trop. Dis. 2017, 11, e0006150. [Google Scholar] [CrossRef] [PubMed]
- Ramos, M.M.; Mohammed, H.; Zielinski-Gutierrez, E.; Hayden, M.H.; Lopez, J.L.R.; Fournier, M.; Trujillo, A.R.; Burton, R.; Brunkard, J.M.; Anaya-Lopez, L.; et al. Epidemic Dengue and Dengue Hemorrhagic Fever at the Texas–Mexico Border: Results of a Household-based Seroepidemiologic Survey, December 2005. Am. J. Trop. Med. Hyg. 2008, 78, 364–369. [Google Scholar] [CrossRef] [PubMed]
- Guyot-Téphany, J.; Grenier, C.; Orellana, D. Usos, percepciones y manejo del agua en Galápagos. In Galapagos Report 2011–2012; GNPS, GCREG, CDF and GC: Puerto Ayora, Galapagos, Ecuador, 2013; pp. 67–75. [Google Scholar]
- Liu, J.; d’Ozouville, N. Water contamination in Puerto Ayora: Applied interdisciplinary research using Escherichia coli as an indicator bacteria. In Galapagos Report 2011–2012; GNPS, GCREG, CDF and GC: Puerto Ayora, Galapagos, Ecuador, 2013; pp. 76–83. [Google Scholar]
- Water Supply and Demand in Santa Cruz Island—Galapagos Archipelago. Available online: http://iwtc.info/wp-content/uploads/2015/03/33.pdf (accessed on 13 February 2017).
- Lowe, R.; Gasparrini, A.; Van Meerbeeck, C.J.; Lippi, C.A.; Mahon, R.; Trotman, A.R.; Rollock, L.; Hinds, A.Q.J.; Ryan, S.J.; Stewart-Ibarra, A.M. Nonlinear and delayed impacts of climate on dengue risk in Barbados: A modelling study. PLoS Med. 2018, 15, e1002613. [Google Scholar] [CrossRef] [PubMed]
- Toan, N.T.; Rossi, S.; Prisco, G.; Nante, N.; Viviani, S. Dengue epidemiology in selected endemic countries: Factors influencing expansion factors as estimates of underreporting. Trop. Med. Int. Health 2015, 20, 840–863. [Google Scholar] [CrossRef] [PubMed]
- Heydari, N.; Larsen, D.A.; Neira, M.; Ayala, E.B.; Fernandez, P.; Adrian, J.; Rochford, R.; Stewart-Ibarra, A.M. Household Dengue Prevention Interventions, Expenditures, and Barriers to Aedes aegypti Control in Machala, Ecuador. Int. J. Environ. Res. Public Health 2017, 14, 196. [Google Scholar] [CrossRef] [PubMed]
- Sistematizacion de Lecciones Aprendidas en Proyectos COMBI en Dengue en la Region de las Americas; Organización Panamericana de la Salud: Calle Blancos, Costa Rica, 2011; p. 101.
- Parks, W.; Lloyd, L.; Nathan, M.B.; Hosein, E.; Odugleh, A.; Clark, G.G.; Gubler, D.J.; Prasittisuk, C.; Palmer, K.; San Martín, J.L.; et al. International experiences in social mobilization and communication for dengue prevention and control. Dengue Bull. 2004, 28, S1–S7. [Google Scholar]
- Viet, T.L.; Choisy, M.; Bryant, J.E.; Trong, D.V.; Quang, T.P.; Horby, P.; Tran, H.N.; Thi Kieu, H.T.; Vu, T.N.; Van, K.N.; et al. A dengue outbreak on a floating village at Cat Ba Island in Vietnam. BMC Public Health 2015, 15. [Google Scholar] [CrossRef]
- Cao-Lormeau, V.-M.; Roche, C.; Aubry, M.; Teissier, A.; Lastere, S.; Daudens, E.; Mallet, H.-P.; Musso, D.; Aaskov, J. Recent Emergence of Dengue Virus Serotype 4 in French Polynesia Results from Multiple Introductions from Other South Pacific Islands. PLoS ONE 2011, 6, e29555. [Google Scholar] [CrossRef] [PubMed]
- Wilder-Smith, A.; Gubler, D.J. Geographic Expansion of Dengue: The Impact of International Travel. Med. Clin. N. Am. 2008, 92, 1377–1390. [Google Scholar] [CrossRef] [PubMed]
- Yactayo, S.; Staples, J.E.; Millot, V.; Cibrelus, L.; Ramon-Pardo, P. Epidemiology of Chikungunya in the Americas. J. Infect. Dis. 2016, 214, S441–S445. [Google Scholar] [CrossRef] [PubMed]
- Chen, L.H.; Hamer, D.H. Zika Virus: Rapid Spread in the Western Hemisphere. Ann. Intern. Med. 2016, 164, 613. [Google Scholar] [CrossRef] [PubMed]
| Parameter | PA | PB | p-Value | ||
|---|---|---|---|---|---|
| n | Percent or Mean (±SD) | n | Percent or Mean (±SD) | ||
| Human Movement | |||||
| Member of the household travels to the mainland 1 | 33 | 66% | 39 | 78% | 0.21 |
| Member of the household travels between islands 1 | 15 | 30% | 24 | 48% | 0.09 |
| Member of the household visits houses outside the neighborhood daily 1 | 9 | 18% | 10 | 20% | 1 |
| Demographics | |||||
| Number of people per bedroom in household 1,A | 41 | 2.07 (±1.37) | 47 | 1.86 (±1.25) | 0.45 |
| Head of household age is less than 37 years 1 | 13 | 36% | 7 | 18% | 0.08 |
| Head of household age is greater than 56 years 1 | 7 | 16% | 11 | 37% | 0.03 |
| Female head of household 1 | 28 | 56% | 12 | 24% | <0.01 |
| Head of household is employed 1 | 36 | 72% | 43 | 86% | 0.03 |
| More than 1 family sleeps on the property 1 | 25 | 53% | 12 | 26% | 0.01 |
| Head of household earns more than the minimum wage 1 | 12 | 24% | 14 | 28% | 0.82 |
| Head of household has a secondary level of education or higher 1 | 19 | 38% | 19 | 38% | 1 |
| Mosquito Abatement Practices | |||||
| Covers water containers 2 | 31 | 62% | 30 | 60% | 1 |
| Applies chemicals to standing water 2 | 5 | 10% | 18 | 36% | <0.01 |
| Eliminates standing water 2 | 2 | 4% | 26 | 52% | <0.01 |
| Disposes of trash on the property 2 | 6 | 12% | 21 | 42% | <0.01 |
| Fumigates house 2 | 9 | 18% | 14 | 28% | 0.34 |
| Applies repellent 2 | 4 | 8% | 13 | 26% | 0.03 |
| Closes windows and doors 2 | 0 | 0% | 14 | 28% | <0.01 |
| Cuts vegetation 2,B | 0 | 0% | 7 | 14% | 0.01 |
| Spreads burned diesel on floor/in puddles 2,B | 0 | 0% | 1 | 2% | 1 |
| Burns palosanto or insecticide coils 2,B | 0 | 0% | 2 | 4% | 0.5 |
| Uses bed nets | 2 | 4% | 27 | 54% | <0.01 |
| Housing Characteristics | |||||
| Poorly maintained patio 1,2 | 22 | 44% | 8 | 16% | <0.01 |
| Poor overall condition of house (old, unpainted, uncared for) 1,2,B | 2 | 4% | 0 | 0% | 0.5 |
| Good overall condition of house (new, well-maintained) 1,2 | 19 | 38% | 25 | 50% | 0.31 |
| Patio is shady (>50% shaded) 1,2,B | 2 | 4% | 6 | 12% | 0.27 |
| House is rented 1,2 | 12 | 24% | 10 | 20% | 0.81 |
| Uses air conditioning to ventilate the household 1,2 | 6 | 12% | 7 | 14% | 1 |
| No screens on windows and/or doors 1,2 | 9 | 18% | 14 | 28% | 0.34 |
| Lives near abandoned homes or vacant lots 1,2 | 32 | 64% | 44 | 88% | 0.01 |
| Household receives piped water from outside the home 1,2 | 11 | 22% | 18 | 36% | 0.19 |
| There are daily or weekly interruptions in the water supply 1,2 | 22 | 44% | 20 | 40% | 0.84 |
| Waste water disposal by a sewage system 1,2,B | 1 | 2% | 38 | 76% | <0.01 |
| Stores water apart in containers other than in a cistern or elevated water tank (sometimes or always) 1,2 | 42 | 84% | 28 | 56% | <0.01 |
| Knowledge and Attitudes | |||||
| Aware of cases of dengue in the community 1,2 | 21 | 42% | 27 | 54% | 0.32 |
| Considers dengue to be a severe disease 1,2,B | 43 | 86% | 49 | 98% | 0.06 |
| Knows that dengue is transmitted by a mosquito 1,2 | 47 | 94% | 47 | 94% | 1 |
| Considers dengue to be a serious problem in the community 1,2,B | 41 | 82% | 47 | 94% | 0.12 |
| Perception that it is difficult to prevent dengue 1,2 | 6 | 12% | 17 | 34% | 0.02 |
| Participated in dengue prevention campaigns 1,2,B | 6 | 12% | 5 | 10% | 1 |
| Source of dengue information: media (television, newspaper, radio) B | 46 | 92% | 48 | 96% | 0.67 |
| Source of dengue information: Ministry of Health outreach (community health meetings, in clinics/hospitals, fliers) | 28 | 56% | 38 | 74% | 0.09 |
| Source of dengue information: social networks (family, friends) B | 6 | 12% | 7 | 14% | 1 |
| Vector Indices | Total | PA | PB | p-Value | ||
|---|---|---|---|---|---|---|
| n | n | % | n | % | ||
| Houses inspected | 100 | 50 | 50 | |||
| Total containers with water | 248 | 119 | 129 | |||
| Houses with adult AA | 9 | 2 | 4.00% | 7 | 14.00% | 0.16 |
| Houses with containers with juvenile AA | 13 | 3 | 6.00% | 10 | 20.00% | 0.012 * |
| Total containers with juvenile AA | 16 | 3 | 2.50% | 13 | 10.10% | 0.019 * |
| Breteau index | 6 | 26 | ||||
| House index | 6 | 20 | ||||
| Factor | Estimate | SE | p-Value | OR (95% CI) | VIF |
|---|---|---|---|---|---|
| Intercept | −7.02 | 1.98 | <0.001 | ||
| People per bedroom | 1.28 | 0.39 | <0.001 | 3.60 (0.00–8.80) | 2.11 |
| Head of household earns more than minimum wage | 3.23 | 1.09 | <0.01 | 25.31 (0.00–301.64) | 2.08 |
| Visit other neighborhoods daily | −2.95 | 1.37 | 0.031 | 0.05 (0.00–0.53) | 1.49 |
| Travel to island | 3.16 | 1.06 | <0.01 | 23.57 (0.00–268.08) | 2.17 |
| Daily or weekly interruption in the piped water supply | 2.18 | 1.00 | 0.029 | 8.85 (0.00–84.26) | 1.96 |
| Aware of cases of dengue in the neighborhood | 2.54 | 1.16 | 0.028 | 11.85 (0.00–107.67) | 1.69 |
| Considers dengue to be a serious problem in the community | −2.90 | 1.42 | 0.041 | 0.06 (0.00–0.75) | 1.74 |
| Waste water disposal by a sewage system | 1.47 | 0.87 | 0.092 | 4.35 (0.00–29.21) | 1.47 |
| Factor | Estimate | SE | p-Value | OR (95% CI) | VIF |
|---|---|---|---|---|---|
| Intercept | −22.81 | 2815.28 | 0.994 | - | |
| Uses mosquito nets | 3.25 | 1.20 | 0.007 | 25.90 (2.47–271.24) | 2.07 |
| Uses repellant | −2.37 | 1.52 | 0.118 | 0.09 (0.01–1.83) | 1.67 |
| Covers water containers | −3.39 | 1.24 | 0.006 | 0.034 (0.003–0.38) | 2.19 |
| Closes windows and doors | −3.10 | 2.02 | 0.126 | 0.05 (0.001–2.38) | 1.85 |
| Uses chemicals to treat water | −2.89 | 1.52 | 0.057 | 0.06 (0.003–1.10) | 2.02 |
| Perception that dengue is a severe disease | 19.61 | 2815.28 | 0.994 | - | 1 |
| Air conditioning | 5.27 | 1.78 | 0.003 | 194.06 (5.98–6293.60) | 3.87 |
| Water is piped into and out of the house | 2.47 | 1.28 | 0.055 | 11.80 (0.95–146.11) | 2.27 |
| Dengue is difficult to prevent | 2.26 | 0.97 | 0.020 | 9.61 (1.42–64.95) | 1.35 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ryan, S.J.; Lippi, C.A.; Nightingale, R.; Hamerlinck, G.; Borbor-Cordova, M.J.; Cruz B, M.; Ortega, F.; Leon, R.; Waggoner, E.; Stewart-Ibarra, A.M. Socio-Ecological Factors Associated with Dengue Risk and Aedes aegypti Presence in the Galápagos Islands, Ecuador. Int. J. Environ. Res. Public Health 2019, 16, 682. https://doi.org/10.3390/ijerph16050682
Ryan SJ, Lippi CA, Nightingale R, Hamerlinck G, Borbor-Cordova MJ, Cruz B M, Ortega F, Leon R, Waggoner E, Stewart-Ibarra AM. Socio-Ecological Factors Associated with Dengue Risk and Aedes aegypti Presence in the Galápagos Islands, Ecuador. International Journal of Environmental Research and Public Health. 2019; 16(5):682. https://doi.org/10.3390/ijerph16050682
Chicago/Turabian StyleRyan, Sadie J., Catherine A. Lippi, Ryan Nightingale, Gabriela Hamerlinck, Mercy J. Borbor-Cordova, Marilyn Cruz B, Fernando Ortega, Renato Leon, Egan Waggoner, and Anna M. Stewart-Ibarra. 2019. "Socio-Ecological Factors Associated with Dengue Risk and Aedes aegypti Presence in the Galápagos Islands, Ecuador" International Journal of Environmental Research and Public Health 16, no. 5: 682. https://doi.org/10.3390/ijerph16050682
APA StyleRyan, S. J., Lippi, C. A., Nightingale, R., Hamerlinck, G., Borbor-Cordova, M. J., Cruz B, M., Ortega, F., Leon, R., Waggoner, E., & Stewart-Ibarra, A. M. (2019). Socio-Ecological Factors Associated with Dengue Risk and Aedes aegypti Presence in the Galápagos Islands, Ecuador. International Journal of Environmental Research and Public Health, 16(5), 682. https://doi.org/10.3390/ijerph16050682






