Imaging-Based Anatomical Characterization of Aortic Aneurysms and Dissections: An Observational Study in a Tertiary Hospital in Bogotá, Colombia
Abstract
1. Introduction
2. Materials and Methods
3. Results
3.1. Aortic Aneurysm
3.2. Aortic Dissection
4. Discussion
4.1. General Clinical Aspects
4.2. Aortic Aneurysm: Clinical and Morphological Characteristics
4.3. Aortic Dissection: Profile and Patterns
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AA | Aortic Aneurysm |
| AD | Aortic Dissection |
| CTA | Computed Tomography Angiography |
| ICU | Intensive Care Unit |
| OR | Odds Ratio |
| CI | Confidence Interval |
| ROC | Receiver Operating Characteristic |
| VIF | Variance Inflation Factor |
References
- Tarazona, M.M.; Camacho, J.; Peláez, M.; Carreño, M.; Sandoval, N.; Umaña, J. Resultados del tratamiento quirúrgico de los aneurismas de aorta abdominal infrarrenal. Rev. Colomb. Cardiol. 2015, 22, 54–61. [Google Scholar] [CrossRef][Green Version]
- Cheung, K.; Boodhwani, M.; Chan, K.L.; Beauchesne, L.; Dick, A.; Coutinho, T. Thoracic aortic aneurysm growth: Role of sex and aneurysm etiology. J. Am. Heart Assoc. 2017, 6, e003792. [Google Scholar] [CrossRef] [PubMed]
- Pham, M.H.C.; Sigvardsen, P.E.; Fuchs, A.; Kühl, J.T.; Sillesen, H.; Afzal, S.; Nordestgaard, B.G.; Køber, L.V.; Kofoed, K.F. Aortic aneurysms in a general population cohort: Prevalence and risk factors in men and women. Eur. Heart J. Cardiovasc. Imaging 2024, 25, 1235–1243. [Google Scholar] [CrossRef] [PubMed]
- Nathan, D.P.; Xu, C.; Pouch, A.M.; Chandran, K.B.; Desjardins, B.; Gorman, J.H.; Fairman, R.M.; Gorman, R.C.; Jackson, B.M. Increased wall stress of saccular versus fusiform aneurysms of the descending thoracic aorta. Ann. Vasc. Surg. 2011, 25, 1129–1137. [Google Scholar] [CrossRef] [PubMed]
- Ullery, B.W.; Hallett, R.L.; Fleischmann, D. Epidemiology and contemporary management of abdominal aortic aneurysms. Abdom. Radiol. 2018, 43, 1032–1043. [Google Scholar] [CrossRef]
- Mathur, A.; Mohan, V.; Ameta, D.; Bhardwaj, G.; Haranahalli, P. Aortic aneurysm. J. Transl. Intern. Med. 2016, 4, 33–41. [Google Scholar] [CrossRef]
- Echeverry, E.J.; Gutiérrez, H.; Bustamante, M.E.; Borrero, Á.J.; Cadavid, E.A. Experience and results in surgery of type A aortic dissection during a decade in the Fundación Valle del Lili, Cali, Colombia. Rev. Colomb. Cardiol. 2012, 20, 325–330. Available online: https://www.sciencedirect.com/science/article/pii/S0120563313700779 (accessed on 18 August 2025).
- Alvarado, C.; Guzmán, F.; Vargas, F.; Barragán, R.; Arias, C.A. Síndromes aórticos agudos Acute aortic syndromes. Rev. Colomb. Cardiol. 2013, 20, 114–121. [Google Scholar]
- Higa, C.; Guetta, J.; Borracci, R.A.; Meribilhaa, R.; Marturano, M.P.; Marenchino, R.; Benzadón, M.N.; Comignani, P.; Botto, F.; Fuselli, J.J. Registro multicéntrico de disección aórtica aguda. Estudio RADAR. Resultados preliminares. Rev. Argent. Cardiol. 2009, 77, 354–360. Available online: http://www.scopus.com/inward/record.url?eid=2-s2.0-77952401367&partnerID=tZOtx3y1 (accessed on 18 August 2025).
- Braverman, A.C. Acute aortic dissection: Clinician update. Circulation 2010, 122, 184–188. [Google Scholar] [CrossRef]
- Sievers, H.H.; Rylski, B.; Czerny, M.; Baier, A.L.M.; Kreibich, M.; Siepe, M.; Beyersdorf, F. Aortic dissection reconsidered: Type, entry site, malperfusion classification adding clarity and enabling outcome prediction. Interact. Cardiovasc. Thorac. Surg. 2020, 30, 451–457. [Google Scholar] [CrossRef]
- Bojko, M.M.; Fleischman, F. Aortic Dissection: Diagnosis Aortic dissection Dissection diagnosis Dissection presentation Dissection symptoms. Cardiol. Clin. 2025, 43, 90033. [Google Scholar]
- Torres-España, N.F.; Solarte-Pineda, H.; Gómez-Vera, C.E.; Sepúlveda-Gallego, L.E.; Esparza-Albornoz, Á.S.; Gil-Guerrero, M.A. Evaluando la experiencia local: Primeros 50 casos de reparo endovascular de aneurismas aórticos en Manizales, Colombia. Rev. Colomb. Cirugía. 2022, 37, 434–447. [Google Scholar] [CrossRef]
- Goldfinger, J.Z.; Halperin, J.L.; Marin, M.L.; Stewart, A.S.; Eagle, K.A.; Fuster, V. Thoracic aortic aneurysm and dissection. J. Am. Coll. Cardiol. 2014, 64, 1725–1739. [Google Scholar] [CrossRef]
- Kent, K.C.; Zwolak, R.M.; Egorova, N.N.; Riles, T.S.; Manganaro, A.; Moskowitz, A.J.; Gelijns, A.C.; Greco, G. Analysis of risk factors for abdominal aortic aneurysm in a cohort of more than 3 million individuals. J. Vasc. Surg. 2010, 52, 539–548. [Google Scholar] [CrossRef] [PubMed]
- Aschner, P. Epidemiología de la diabétes en Colombia. Av. Diabetol. 2010, 26, 95–100. [Google Scholar] [CrossRef]
- Climent, E.; Benaiges, D.; Chillarón, J.J.; Flores-Le Roux, J.A.; Pedro-Botet, J. La diabetes mellitus como factor protector del aneurisma de aorta abdominal: Posibles mecanismos. Clínica Investig. Arterioscler. 2018, 30, 181–187. [Google Scholar] [CrossRef]
- Seriki, S.; Otoikhila, O. Age, smoking, hypertension, and aortic aneurysm: Interactions and risks. J. Cardiol. Cardiovasc. Med. 2022, 7, 001–005. [Google Scholar] [CrossRef]
- Jabagi, H.; Levine, D.; Gharibeh, L.; Camillo, C.; Castillero, E.; Ferrari, G.; Takayama, H.; Grau, J.B. Implications of Bicuspid Aortic Valve Disease and Aortic Stenosis/Insufficiency as Risk Factors for Thoracic Aortic Aneurysm. Rev. Cardiovasc. Med. 2023, 24, 178. [Google Scholar] [CrossRef]
- Martins, J.V.D.; Mendes, R.; Flumignan, R.L.G.; Nakano, L.C.U.; de Amorim, J.E.; Neto, H.J.G. The relationship between abdominal aortic aneurysm diametand its risk factors: A retrospective cohort study. J. Vasc. Bras. 2025, 24, e20230110. [Google Scholar]
- Poullis, M. Central vs. peripheral vascular factors determining risk of aortic dissection. Med. Hypotheses 2024, 182, 111235. [Google Scholar] [CrossRef]
- Landenhed, M.; Engström, G.; Gottsäter, A.; Caulfield, M.P.; Hedblad, B.; Newton-Cheh, C.; Melander, O.; Smith, J.G. Risk profiles for aortic dissection and ruptured or surgically treated aneurysms: A prospective cohort study. J. Am. Heart Assoc. 2015, 4, e001513. [Google Scholar] [CrossRef]

| Aneurysm | Dissection | ||||
|---|---|---|---|---|---|
| No. | % | No. | % | ||
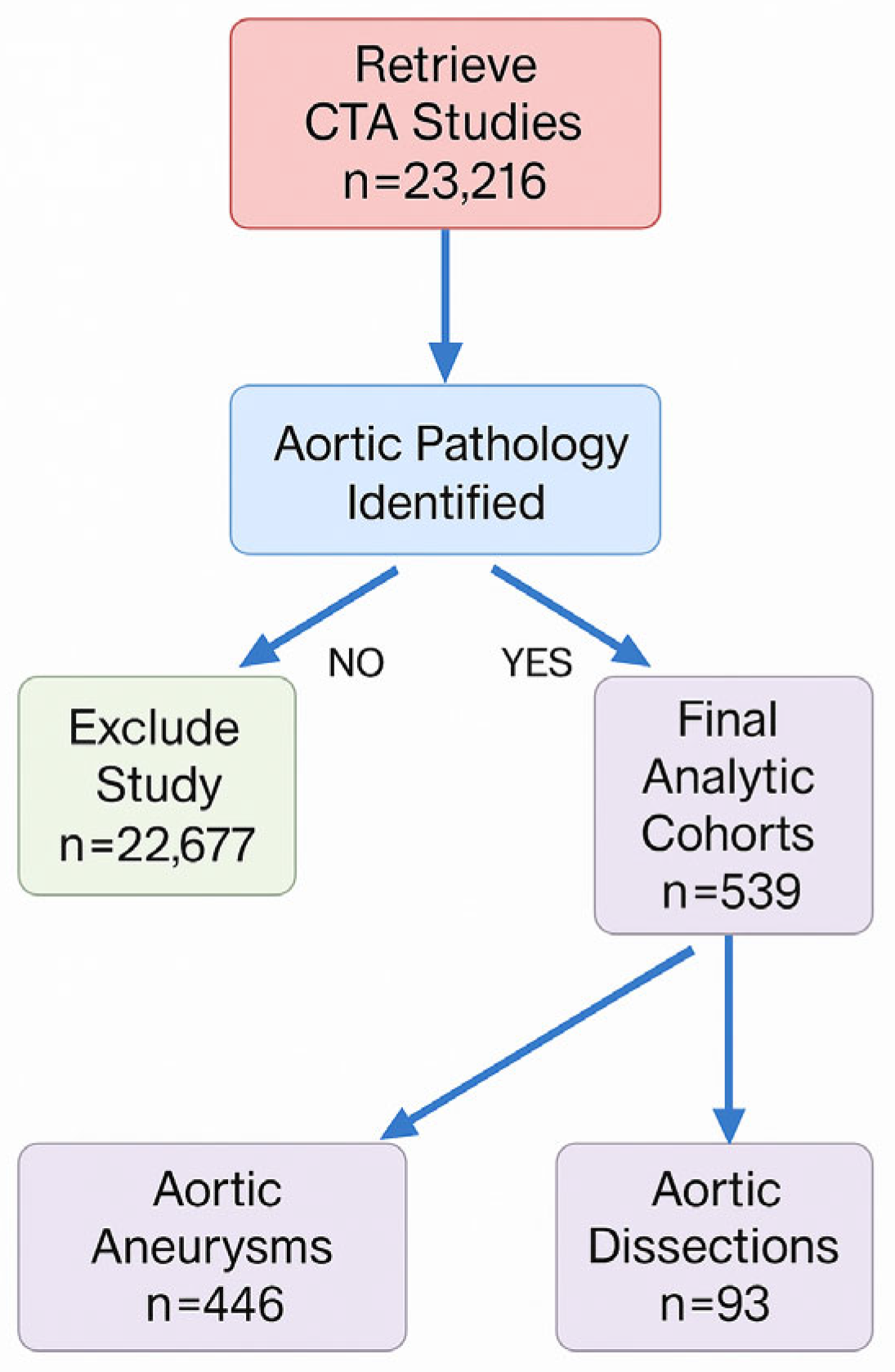
| Total patients | 446 | 100 | 93 | 100 | |
| Age | <50 years | 5 | 1.1 | 11 | 11.8 |
| 50–59 | 24 | 5.4 | 16 | 17.2 | |
| 60–69 | 103 | 23.1 | 22 | 23.7 | |
| 70–79 | 167 | 37.4 | 27 | 29.0 | |
| ≥80 | 143 | 32.1 | 17 | 18.3 | |
| Unspecified | 4 | 0.9 | 0 | 0.0 | |
| Sex | Male | 238 | 53.4 | 51 | 54.8 |
| Female | 208 | 46.6 | 42 | 45.2 | |
| Comorbidities | Hypertension | 332 | 74.4 | 74 | 79.6 |
| Diabetes mellitus | 53 | 11.9 | 12 | 12.9 | |
| Prior thoracic surgery | 3 | 0.7 | 8 | 8.6 | |
| Marfan syndrome | 0 | 0.0 | 1 | 1.1 | |
| Vasculitis | 2 | 0.4 | 0 | 0.0 | |
| Thoracic trauma | 0 | 0.0 | 1 | 1.1 | |
| Congenital heart disease | 3 | 0.7 | 1 | 1.1 | |
| No comorbidities | 87 | 19.5 | 21 | 22.6 |
| Nombre | Characteristic | p-Value | ||
|---|---|---|---|---|
| Diabetes and aneurysm location | Characteristic | Infrarenal aneurysm Yes | Infrarenal aneurysm No | 0.0153 |
| Diabetes: Yes | 37 (13.1%) | 9 (3.2%) | ||
| Diabetes: No | 246 (87.2%) | 153 (96.8%) | ||
| Thoracic surgery and location | Characteristic | Ascending aorta | Non-ascending aorta | 0.0660 |
| Thoracic Surgery: Yes | 7 (12.5%) | 23 (87.5%) | ||
| Thoracic Surgery: No | 49 (11.8%) | 366 (88.2%) | ||
| Sex and thoracic surgery | Characteristic | Surgery | No surgery | 1.06 × 10−6 |
| Male | 25 (10.5%) | 213 (89.5%) | ||
| Female | 5 (2.4%) | 202 (97.6%) | ||
| Sex and survival | Characteristic | Yes | No | 0.0956 |
| Male | 211 (88.7%) | 27 (11.3%) | ||
| Female | 193 (93.2%) | 14 (6.8%) | ||
| Hypertension and location | Characteristic | Infrarenal | Other locations | 0.0905 |
| Yes | 203 (61.3%) | 128 (38.7%) | ||
| No | 80 (70.2%) | 34 (29.8%) | ||
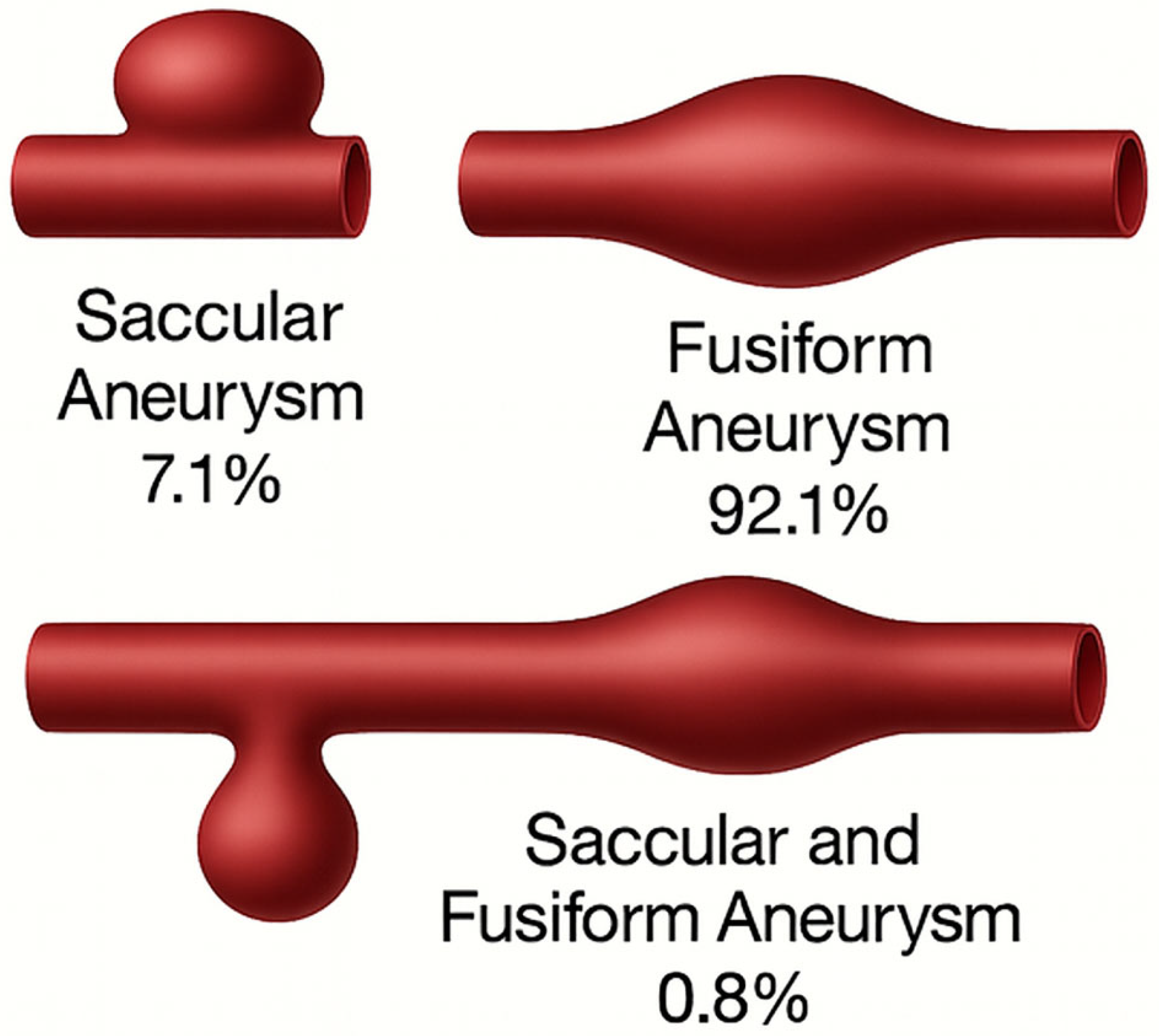
| Sex and aneurysm morphology | Characteristic | Saccular | Fusiform | 0.0267 |
| Male | 6 (4.0%) | 143 (96.0%) | ||
| Female | 14 (10.9%) | 114 (89.1%) | ||
| Location (infrarenal vs. other) and morphology | Characteristic | Saccular | Fusiform | 0.0162 |
| Infrarenal aorta | 9 (4.7%) | 182 (95.3%) | ||
| Other aortic segments | 11 (12.8%) | 75 (87.2%) | ||
| Location (arch vs. other) and morphology | Characteristic | Saccular | Fusiform | 1.57 × 10−15 |
| Aortic arch | 8 (72.7%) | 3 (27.3%) | ||
| Other aortic segments | 12 (4.5%) | 254 (95.5%) | ||
| Bicuspid aortic valve and location | Characteristic | Ascending aorta | Other aortic segments | 5.1 × 10−6 |
| Yes | 4 (100%) | 0 (0%) | ||
| No | 43 (11.6%) | 329 (88.4%) | ||
| Variable | Adjusted OR | 95% CI | p-Value |
|---|---|---|---|
| Age (per 5-year increment) | 1.23 | 1.01–1.48 | 0.036 |
| Maximum aortic diameter (per mm)–overall mortality | 1.02 | 1.01–1.03 | <0.001 |
| Maximum aortic diameter (per mm)–aneurysm-related death | 1.03 | 1.01–1.05 | <0.001 |
| Prior thoracic surgery | 2.78 | 0.99–7.83 | 0.053 |
| Age | Type I | Type II | Type III | Total |
|---|---|---|---|---|
| <55 years | 8 (8.6%) | 3 (3.2%) | 5 (5.4%) | 16 (17.2%) |
| 55–59 | 1 (1.1%) | 3 (3.2%) | 7 (7.5%) | 11 (11.8%) |
| 60–64 | 2 (2.2%) | 1 (1.1%) | 4 (4.3%) | 7 (7.5%) |
| 65–69 | 6 (6.5%) | 1 (1.1%) | 8 (8.6%) | 15 (16.1%) |
| 70–74 | 7 (7.5%) | 0 (0.0%) | 9 (9.7%) | 16 (17.2%) |
| 75–79 | 2 (2.2%) | 1 (1.1%) | 8 (8.6%) | 11 (11.8%) |
| ≥80 | 5 (5.4%) | 3 (3.2%) | 9 (9.7%) | 17 (18.3%) |
| Total | 31 (33.3%) | 12 (12.9%) | 50 (53.8%) | 93 (100%) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Published by MDPI on behalf of the Lithuanian University of Health Sciences. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bernal, R.M.L.; Duarte, A.C.V.; Chavarro, E.F.; Urbina, A.; Becerra, J.F.C.; Borda, S.; Falla, M.P.C.; Ardila, M.A.C.; Bayona, J.A.C. Imaging-Based Anatomical Characterization of Aortic Aneurysms and Dissections: An Observational Study in a Tertiary Hospital in Bogotá, Colombia. Medicina 2025, 61, 1558. https://doi.org/10.3390/medicina61091558
Bernal RML, Duarte ACV, Chavarro EF, Urbina A, Becerra JFC, Borda S, Falla MPC, Ardila MAC, Bayona JAC. Imaging-Based Anatomical Characterization of Aortic Aneurysms and Dissections: An Observational Study in a Tertiary Hospital in Bogotá, Colombia. Medicina. 2025; 61(9):1558. https://doi.org/10.3390/medicina61091558
Chicago/Turabian StyleBernal, Ricardo Miguel Luque, Angy Carolina Villamil Duarte, Ernesto Fajardo Chavarro, Adriana Urbina, Juan Fernando Cediel Becerra, Sergio Borda, María Paula Cerón Falla, María Andrea Calderón Ardila, and Jorge Alberto Carrillo Bayona. 2025. "Imaging-Based Anatomical Characterization of Aortic Aneurysms and Dissections: An Observational Study in a Tertiary Hospital in Bogotá, Colombia" Medicina 61, no. 9: 1558. https://doi.org/10.3390/medicina61091558
APA StyleBernal, R. M. L., Duarte, A. C. V., Chavarro, E. F., Urbina, A., Becerra, J. F. C., Borda, S., Falla, M. P. C., Ardila, M. A. C., & Bayona, J. A. C. (2025). Imaging-Based Anatomical Characterization of Aortic Aneurysms and Dissections: An Observational Study in a Tertiary Hospital in Bogotá, Colombia. Medicina, 61(9), 1558. https://doi.org/10.3390/medicina61091558







