Long COVID and Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS)—A Systemic Review and Comparison of Clinical Presentation and Symptomatology
Abstract
1. Introduction
2. Materials and Methods
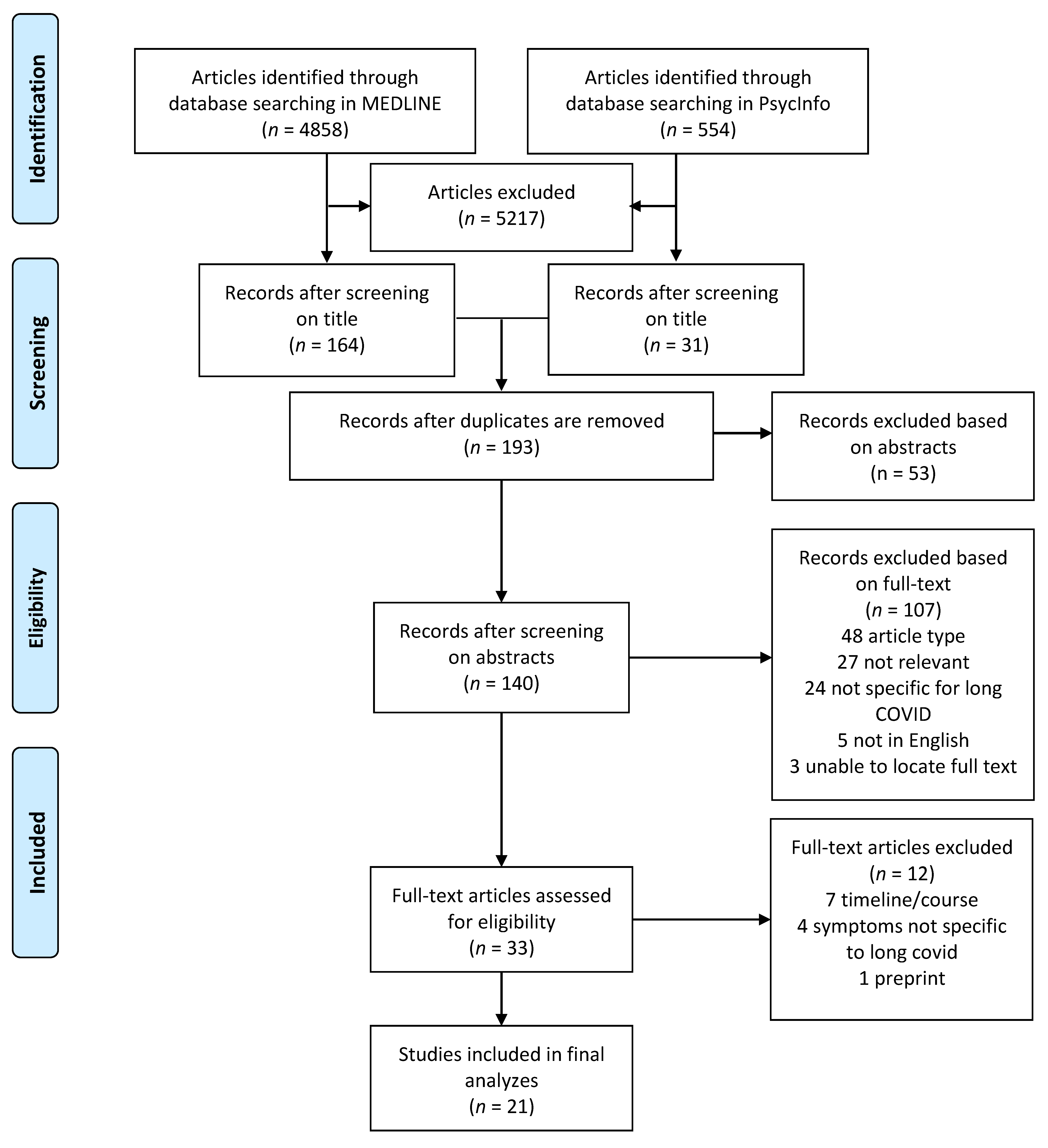
2.1. Search Strategy
2.2. Eligibility Criteria
2.3. Synthesis of Results
3. Results
4. Discussions
Limitations and Future Directions
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Pollard, C.A.; Morran, M.P.; Nestor-Kalinoski, A.L. The COVID-19 pandemic: A global health crisis. Physiol. Genom. 2020, 52, 549–557. [Google Scholar] [CrossRef]
- WHO. Weekly Epidemiological Update-9 March 2021 (Retrieved 17 March 2021). Available online: https://apps.who.int/iris/bitstream/handle/10665/340087/nCoV-weekly-sitrep9Mar21-eng.pdf?sequence=1 (accessed on 17 March 2021).
- CDC. COVID Data Tracker (Retrieved 17 March 2021). Available online: https://covid.cdc.gov/covid-data-tracker/#cases_casesper100klast7days (accessed on 17 March 2021).
- Zhou, F.; Yu, T.; Du, R.; Fan, G.; Liu, Y.; Liu, Z.; Xiang, J.; Wang, Y.; Song, B.; Gu, X.; et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: A retrospective cohort study. Lancet 2020, 395, 1054–1062. [Google Scholar] [CrossRef]
- Yuki, K.; Fujiogi, M.; Koutsogiannaki, S. COVID-19 pathophysiology: A review. Clin. Immunol. 2020, 215, 108427. [Google Scholar] [CrossRef]
- Tian, S.; Chang, Z.; Wang, Y.; Wu, M.; Zhang, W.; Zhou, G.; Zou, X.; Tian, H.; Xiao, T.; Xing, J.; et al. Clinical Characteristics and Reasons for Differences in Duration From Symptom Onset to Release From Quarantine Among Patients With COVID-19 in Liaocheng, China. Front. Med. 2020, 7, 210. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Huang, D.Q.; Zou, B.; Yang, H.; Hui, W.Z.; Rui, F.; Yee, N.; Liu, C.; Nerurkar, S.N.; Kai, J.; et al. Epidemiology of COVID-19: A systematic review and meta-analysis of clinical characteristics, risk factors, and outcomes. J. Med. Virol. 2021, 93, 1449–1458. [Google Scholar] [CrossRef] [PubMed]
- Di Gennaro, F.; Pizzol, D.; Marotta, C.; Antunes, M.; Racalbuto, V.; Veronese, N.; Smith, L. Coronavirus Diseases (COVID-19) Current Status and Future Perspectives: A Narrative Review. Int. J. Environ. Res. Public Health 2020, 17, 2690. [Google Scholar] [CrossRef]
- Somani, S.; Agnihotri, S.P. Emerging Neurology of COVID-19. Neurohospitalist 2020, 10, 281–286. [Google Scholar] [CrossRef] [PubMed]
- Mao, R.; Qiu, Y.; He, J.S.; Tan, J.Y.; Li, X.H.; Liang, J.; Shen, J.; Zhu, L.R.; Chen, Y.; Iacucci, M.; et al. Manifestations and prognosis of gastrointestinal and liver involvement in patients with COVID-19: A systematic review and meta-analysis. Lancet Gastroenterol. Hepatol. 2020, 5, 667–678. [Google Scholar] [CrossRef]
- Belluck, P. Many ‘Long Covid’ Patients had No Symptoms from Their Initial Infection (Retrieved 17 March 2021). Available online: https://www.nytimes.com/2021/03/08/health/long-covid-asymptomatic.html (accessed on 17 March 2021).
- NIH Launches New Initiative to Study “Long COVID” (Retrieved 17 March 2021). Available online: https://www.nih.gov/about-nih/who-we-are/nih-director/statements/nih-launches-new-initiative-study-long-covid (accessed on 17 March 2021).
- Sudre, C.H.; Murray, B.; Varsavsky, T.; Graham, M.S.; Penfold, R.S.; Bowyer, R.C.; Pujol, J.C.; Klaser, K.; Antonelli, M.; Canas, L.S.; et al. Attributes and predictors of long COVID. Nat. Med. 2021, 27, 626–631. [Google Scholar] [CrossRef]
- Nabavi, N. Long covid: How to define it and how to manage it. BMJ 2020, 370, m3489. [Google Scholar] [CrossRef]
- Aucott, J.N.; Rebman, A.W. Long-haul COVID: Heed the lessons from other infection-triggered illnesses. Lancet 2021, 397, 967–968. [Google Scholar] [CrossRef]
- Nath, A. Long-Haul COVID. Neurology 2020, 95, 559–560. [Google Scholar] [CrossRef]
- Garg, P.; Arora, U.; Kumar, A.; Wig, N. The “post-COVID” syndrome: How deep is the damage? J. Med. Virol. 2021, 93, 673–674. [Google Scholar] [CrossRef] [PubMed]
- Baig, A.M. Deleterious Outcomes in Long-Hauler COVID-19: The Effects of SARS-CoV-2 on the CNS in Chronic COVID Syndrome. ACS Chem. Neurosci. 2020, 11, 4017–4020. [Google Scholar] [CrossRef] [PubMed]
- Kalter, L.; WebMD Health News. Fauci Introduces New Acronym for Long COVID (Retrieved 17 March 2021). Available online: https://www.medscape.com/viewarticle/946419 (accessed on 17 March 2021).
- Soriano, V.; Ganado-Pinilla, P.; Sánchez-Santos, M.; Barreiro, P. Unveiling Long COVID-19 Disease. AIDS Rev. 2020, 22, 227–228. [Google Scholar] [CrossRef] [PubMed]
- Raveendran, A.V. Long COVID-19: Challenges in the diagnosis and proposed diagnostic criteria. Diabetes Metab. Syndr. 2021, 15, 145–146. [Google Scholar] [CrossRef]
- Carfì, A.; Bernabei, R.; Landi, F.; Gemelli Against COVID-19 Post-Acute Care Study Group. Persistent Symptoms in Patients After Acute COVID-19. JAMA 2020, 324, 603–605. [Google Scholar] [CrossRef]
- Mandal, S.; Barnett, J.; Brill, S.E.; Brown, J.S.; Denneny, E.K.; Hare, S.S.; Heightman, M.; Hillman, T.E.; Jacob, J.; Jarvis, H.C.; et al. ‘Long-COVID’: A cross-sectional study of persisting symptoms, biomarker and imaging abnormalities following hospitalisation for COVID-19. Thorax 2020, 10. [Google Scholar] [CrossRef]
- Altmann, D.M.; Boyton, R.J. Decoding the unknowns in long covid. BMJ 2021, 372, n132. [Google Scholar] [CrossRef] [PubMed]
- Bektas, A.; Schurman, S.H.; Franceschi, C.; Ferrucci, L. A public health perspective of aging: Do hyper-inflammatory syndromes such as COVID-19, SARS, ARDS, cytokine storm syndrome, and post-ICU syndrome accelerate short- and long-term inflammaging? Immun. Ageing I A 2020, 17, 23. [Google Scholar] [CrossRef]
- Datta, S.D.; Talwar, A.; Lee, J.T. A Proposed Framework and Timeline of the Spectrum of Disease Due to SARS-CoV-2 Infection: Illness Beyond Acute Infection and Public Health Implications. JAMA 2020, 324, 2251–2252. [Google Scholar] [CrossRef]
- #MEAction. Dr. Fauci Says POST-COVID Syndrome “Is Highly Suggestive of” Myalgic Encephalomyelitis (Retrieved 17 March 2021). Available online: https://www.meaction.net/2020/07/10/dr-anthony-fauci-says-that-post-covid-syndrome-is-highly-suggestive-of-myalgic-encephalomyelitis/ (accessed on 17 March 2021).
- Komaroff, A.L.; Bateman, L. Will COVID-19 Lead to Myalgic Encephalomyelitis/Chronic Fatigue Syndrome? Front. Med. 2021, 7, 606824. [Google Scholar] [CrossRef]
- Friedman, K.J.; Murovska, M.; Pheby, D.; Zalewski, P. Our Evolving Understanding of ME/CFS. Medicina 2021, 57, 200. [Google Scholar] [CrossRef]
- Pendergrast, T.; Brown, A.; Sunnquist, M.; Jantke, R.; Newton, J.L.; Strand, E.B.; Jason, L.A. Housebound versus nonhousebound patients with myalgic encephalomyelitis and chronic fatigue syndrome. Chronic Illn. 2016, 12, 292–307. [Google Scholar] [CrossRef]
- Bhui, K.S.; Dinos, S.; Ashby, D.; Nazroo, J.; Wessely, S.; White, P.D. Chronic fatigue syndrome in an ethnically diverse population: The influence of psychosocial adversity and physical inactivity. BMC Med. 2011, 9, 26. [Google Scholar] [CrossRef]
- Chu, L.; Valencia, I.J.; Garvert, D.W.; Montoya, J.G. Onset Patterns and Course of Myalgic Encephalomyelitis/Chronic Fatigue Syndrome. Front. Pediatr. 2019, 7, 12. [Google Scholar] [CrossRef] [PubMed]
- Tomas, C.; Newton, J.; Watson, S. A review of hypothalamic-pituitary-adrenal axis function in chronic fatigue syndrome. ISRN Neurosci. 2013, 2013, 784520. [Google Scholar] [CrossRef] [PubMed]
- Kerr, J.R. Epstein-Barr Virus Induced Gene-2 Upregulation Identifies a Particular Subtype of Chronic Fatigue Syndrome/Myalgic Encephalomyelitis. Front. Pediatr. 2019, 7, 59. [Google Scholar] [CrossRef] [PubMed]
- Chia, J.K.; Chia, A.Y. Chronic fatigue syndrome is associated with chronic enterovirus infection of the stomach. J. Clin. Pathol. 2008, 61, 43–48. [Google Scholar] [CrossRef]
- Brenu, E.W.; Hardcastle, S.L.; Atkinson, G.M.; van Driel, M.L.; Kreijkamp-Kaspers, S.; Ashton, K.J.; Staines, D.R.; Marshall-Gradisnik, S.M. Natural killer cells in patients with severe chronic fatigue syndrome. Auto Immun. Highlights 2013, 4, 69–80. [Google Scholar] [CrossRef]
- Landay, A.L.; Jessop, C.; Lennette, E.T.; Levy, J.A. Chronic fatigue syndrome: Clinical condition associated with immune activation. Lancet 1991, 338, 707–712. [Google Scholar] [CrossRef]
- Naviaux, R.K.; Naviaux, J.C.; Li, K.; Bright, A.T.; Alaynick, W.A.; Wang, L.; Baxter, A.; Nathan, N.; Anderson, W.; Gordon, E. Metabolic features of chronic fatigue syndrome. Proc. Natl. Acad. Sci. USA 2016, 113, E5472–E5480. [Google Scholar] [CrossRef]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gøtzsche, P.C.; Ioannidis, J.P.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: Explanation and elaboration. BMJ 2009, 339, b2700. [Google Scholar] [CrossRef] [PubMed]
- Butland, R.J.; Pang, J.; Gross, E.R.; Woodcock, A.A.; Geddes, D.M. Two-, six-, and 12-minute walking tests in respiratory disease. Br. Med. J. 1982, 284, 1607–1608. [Google Scholar] [CrossRef] [PubMed]
- Broadbent, S.; Coetzee, S.; Beavers, R. Effects of a short-term aquatic exercise intervention on symptoms and exercise capacity in individuals with chronic fatigue syndrome/myalgic encephalomyelitis: A pilot study. Eur. J. Appl. Physiol. 2018, 118, 1801–1810. [Google Scholar] [CrossRef] [PubMed]
- Vink, M.; Vink-Niese, A. Graded exercise therapy for myalgic encephalomyelitis/chronic fatigue syndrome is not effective and unsafe. Re-analysis of a Cochrane review. Health Psychol. Open 2018, 5, 2055102918805187. [Google Scholar] [CrossRef]
- Lim, E.J.; Son, C.G. Review of case definitions for myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS). J. Transl. Med. 2020, 18, 289. [Google Scholar] [CrossRef]
- Goërtz, Y.; Van Herck, M.; Delbressine, J.M.; Vaes, A.W.; Meys, R.; Machado, F.; Houben-Wilke, S.; Burtin, C.; Posthuma, R.; Franssen, F.; et al. Persistent symptoms 3 months after a SARS-CoV-2 infection: The post-COVID-19 syndrome? ERJ Open Res. 2020, 6, 00542–02020. [Google Scholar] [CrossRef] [PubMed]
- Huang, C.; Huang, L.; Wang, Y.; Li, X.; Ren, L.; Gu, X.; Kang, L.; Guo, L.; Liu, M.; Zhou, X.; et al. 6-month consequences of COVID-19 in patients discharged from hospital: A cohort study. Lancet 2021, 397, 220–232. [Google Scholar] [CrossRef]
- Moreno-Pérez, O.; Merino, E.; Leon-Ramirez, J.M.; Andres, M.; Ramos, J.M.; Arenas-Jiménez, J.; Asensio, S.; Sanchez, R.; Ruiz-Torregrosa, P.; Galan, I.; et al. Post-acute COVID-19 syndrome. Incidence and risk factors: A Mediterranean cohort study. J. Infect. 2021, 82, 378–383. [Google Scholar] [CrossRef]
- Taboada, M.; Cariñena, A.; Moreno, E.; Rodríguez, N.; Domínguez, M.J.; Casal, A.; Riveiro, V.; Diaz-Vieito, M.; Valdés, L.; Álvarez, J. Post-COVID-19 functional status six-months after hospitalization. J. Infect. 2021, 82, e31–e33. [Google Scholar] [CrossRef]
- Petersen, M.S.; Kristiansen, M.F.; Hanusson, K.D.; Danielsen, M.E.; Steig, B.Á.; Gaini, S.; Strøm, M.; Weihe, P. Long COVID in the Faroe Islands—a longitudinal study among non-hospitalized patients. Clin. Infect. Dis. 2020, ciaa1792. [Google Scholar] [CrossRef]
- Townsend, L.; Dowds, J.; O’Brien, K.; Sheill, G.; Dyer, A.H.; O’Kelly, B.; Hynes, J.P.; Mooney, A.; Dunne, J.; Cheallaigh, C.N.; et al. Persistent Poor Health Post-COVID-19 Is Not Associated with Respiratory Complications or Initial Disease Severity. Ann. Am. Thorac. Soc. 2021. [Google Scholar] [CrossRef]
- Weerahandi, H.; Hochman, K.A.; Simon, E.; Blaum, C.; Chodosh, J.; Duan, E.; Garry, K.; Kahan, T.; Karmen-Tuohy, S.L.; Karpel, H.C.; et al. Post-Discharge Health Status and Symptoms in Patients with Severe COVID-19. J. Gen. Intern. Med. 2021, 36, 738–745. [Google Scholar] [CrossRef] [PubMed]
- Townsend, L.; Dyer, A.H.; Jones, K.; Dunne, J.; Mooney, A.; Gaffney, F.; O’Connor, L.; Leavy, D.; O’Brien, K.; Dowds, J.; et al. Persistent fatigue following SARS-CoV-2 infection is common and independent of severity of initial infection. PLoS ONE 2020, 15, e0240784. [Google Scholar] [CrossRef] [PubMed]
- Halpin, S.J.; McIvor, C.; Whyatt, G.; Adams, A.; Harvey, O.; McLean, L.; Walshaw, C.; Kemp, S.; Corrado, J.; Singh, R.; et al. Postdischarge symptoms and rehabilitation needs in survivors of COVID-19 infection: A cross-sectional evaluation. J. Med. Virol. 2021, 93, 1013–1022. [Google Scholar] [CrossRef] [PubMed]
- Wong, A.W.; Shah, A.S.; Johnston, J.C.; Carlsten, C.; Ryerson, C.J. Patient-reported outcome measures after COVID-19: A prospective cohort study. Eur. Respir. J. 2020, 56, 2003276. [Google Scholar] [CrossRef] [PubMed]
- Le Bon, S.D.; Pisarski, N.; Verbeke, J.; Prunier, L.; Cavelier, G.; Thill, M.P.; Rodriguez, A.; Dequanter, D.; Lechien, J.R.; Le Bon, O.; et al. Psychophysical evaluation of chemosensory functions 5 weeks after olfactory loss due to COVID-19: A prospective cohort study on 72 patients. Eur. Arch. Otorhinolaryngol. 2021, 278, 101–108. [Google Scholar] [CrossRef]
- Woo, M.S.; Malsy, J.; Pöttgen, J.; Zai, S.S.; Ufer, F.; Hadjilaou, A.; Schmiedel, S.; Addo, M.M.; Gerloff, C.; Heesen, C.; et al. Frequent neurocognitive deficits after recovery from mild COVID-19. Brain Commun. 2020, 2, fcaa205. [Google Scholar] [CrossRef]
- Ortelli, P.; Ferrazzoli, D.; Sebastianelli, L.; Engl, M.; Romanello, R.; Nardone, R.; Bonini, I.; Koch, G.; Saltuari, L.; Quartarone, A.; et al. Neuropsychological and neurophysiological correlates of fatigue in post-acute patients with neurological manifestations of COVID-19: Insights into a challenging symptom. J. Neurol. Sci. 2021, 420, 117271. [Google Scholar] [CrossRef]
- Ludvigsson, J.F. Case report and systematic review suggest that children may experience similar long-term effects to adults after clinical COVID-19. Acta Paediatr. 2021, 110, 914–921. [Google Scholar] [CrossRef] [PubMed]
- Carroll, E.; Neumann, H.; Aguero-Rosenfeld, M.E.; Lighter, J.; Czeisler, B.M.; Melmed, K.; Lewis, A. Post-COVID-19 inflammatory syndrome manifesting as refractory status epilepticus. Epilepsia 2020, 61, e135–e139. [Google Scholar] [CrossRef] [PubMed]
- Novak, P. Post COVID-19 syndrome associated with orthostatic cerebral hypoperfusion syndrome, small fiber neuropathy and benefit of immunotherapy: A case report. Eneurologicalsci 2020, 21, 100276. [Google Scholar] [CrossRef]
- Koumpa, F.S.; Forde, C.T.; Manjaly, J.G. Sudden irreversible hearing loss post COVID-19. BMJ Case Rep. 2020, 13, e238419. [Google Scholar] [CrossRef] [PubMed]
- Alhiyari, M.A.; Ata, F.; Alghizzawi, M.I.; Bilal, A.B.I.; Abdulhadi, A.S.; Yousaf, Z. Post COVID-19 fibrosis, an emerging complicationof SARS-CoV-2 infection. IDCases 2020, 23, e01041. [Google Scholar] [CrossRef]
- Killion, L.; Beatty, P.E.; Salim, A. Rare cutaneous manifestation of COVID-19. BMJ Case Rep. 2021, 14, e240863. [Google Scholar] [CrossRef]
- Dyer, J.; Kolic, B. Public risk perception and emotion on Twitter during the Covid-19 pandemic. Appl. Netw. Sci. 2020, 5, 99. [Google Scholar] [CrossRef] [PubMed]
- Parikh, P.A.; Shah, B.V.; Phatak, A.G.; Vadnerkar, A.C.; Uttekar, S.; Thacker, N.; Nimbalkar, S.M. COVID-19 Pandemic: Knowledge and Perceptions of the Public and Healthcare Professionals. Cureus 2020, 12, e8144. [Google Scholar] [CrossRef]
- Bhagavathula, A.S.; Aldhaleei, W.A.; Rahmani, J.; Mahabadi, M.A.; Bandari, D.K. Knowledge and Perceptions of COVID-19 Among Health Care Workers: Cross-Sectional Study. JMIR Public Health Surveill. 2020, 6, e19160. [Google Scholar] [CrossRef]
- Yelin, D.; Wirtheim, E.; Vetter, P.; Kalil, A.C.; Bruchfeld, J.; Runold, M.; Guaraldi, G.; Mussini, C.; Gudiol, C.; Pujol, M.; et al. Long-term consequences of COVID-19: Research needs. Lancet Infect. Dis. 2020, 20, 1115–1117. [Google Scholar] [CrossRef]
- Cortinovis, M.; Perico, N.; Remuzzi, G. Long-term follow-up of recovered patients with COVID-19. Lancet 2021, 397, 173–175. [Google Scholar] [CrossRef]
- Subbaraman, N. US Health Agency Will Invest $1 Billion to Investigate ‘Long COVID’ (Retrieved 17 March 2021). Available online: https://www.nature.com/articles/d41586-021-00586-y (accessed on 17 March 2021).
- Committee on the Diagnostic Criteria for Myalgic Encephalomyelitis/Chronic Fatigue Syndrome; Board on the Health of Select Populations; Institute of Medicine. Beyond Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Redefining an Illness; National Academies Press (US): Washington, DC, USA, 2015. [Google Scholar]
- Fukuda, K.; Straus, S.E.; Hickie, I.; Sharpe, M.C.; Dobbins, J.G.; Komaroff, A. The chronic fatigue syndrome: A comprehensive approach to its definition and study. International Chronic Fatigue Syndrome Study Group. Ann. Intern. Med. 1994, 121, 953–959. [Google Scholar] [CrossRef]
- Carruthers, B.M.; van de Sande, M.I.; De Meirleir, K.L.; Klimas, N.G.; Broderick, G.; Mitchell, T.; Staines, D.; Powles, A.C.; Speight, N.; Vallings, R.; et al. Myalgic encephalomyelitis: International Consensus Criteria. J. Intern. Med. 2011, 270, 327–338. [Google Scholar] [CrossRef]
- Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (Retrieved 17 March 2021). Available online: https://www.tandfonline.com/doi/abs/10.1300/J092v11n01_02 (accessed on 17 March 2021).
- Rivera, M.C.; Mastronardi, C.; Silva-Aldana, C.T.; Arcos-Burgos, M.; Lidbury, B.A. Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: A Comprehensive Review. Diagnostics 2019, 9, 91. [Google Scholar] [CrossRef] [PubMed]
- Ortega-Hernandez, O.D.; Shoenfeld, Y. Infection, vaccination, and autoantibodies in chronic fatigue syndrome, cause or coincidence? Ann. N. Y. Acad. Sci. 2009, 1173, 600–609. [Google Scholar] [CrossRef] [PubMed]
- Arnett, S.V.; Alleva, L.M.; Korossy-Horwood, R.; Clark, I.A. Chronic fatigue syndrome—A neuroimmunological model. Med. Hypotheses 2011, 77, 77–83. [Google Scholar] [CrossRef] [PubMed]
- Oronsky, B.; Larson, C.; Hammond, T.C.; Oronsky, A.; Kesari, S.; Lybeck, M.; Reid, T.R. A Review of Persistent Post-COVID Syndrome (PPCS). Clin. Rev. Allergy Immunol. 2021, 1–9. [Google Scholar] [CrossRef]
- Doykov, I.; Hällqvist, J.; Gilmour, K.C.; Grandjean, L.; Mills, K.; Heywood, W.E. ‘The long tail of Covid-19’—The detection of a prolonged inflammatory response after a SARS-CoV-2 infection in asymptomatic and mildly affected patients. F1000Research 2020, 9, 1349. [Google Scholar] [CrossRef]
- Wood, E.; Hall, K.H.; Tate, W. Role of mitochondria, oxidative stress and the response to antioxidants in myalgic encephalomyelitis/chronic fatigue syndrome: A possible approach to SARS-CoV-2 ‘long-haulers’? Chronic Dis. Transl. Med. 2021, 7, 14–26. [Google Scholar] [CrossRef]
- Gupta, D. Almost A Third of People with ‘Mild’ COVID-19 Still Battle Symptoms Months Later, Study Finds (Retrieved 17 March 2021). Available online: https://www.cnn.com/2021/02/19/health/post-covid-syndrome-long-haulers-gupta-wellness/index.html (accessed on 17 March 2021).
- COVID Long-Haulers Plagued by Symptoms as Experts Seek Answers (Retrieved 17 March 2021). Available online: https://www.usnews.com/news/health-news/articles/2021-03-16/covid-long-haulers-plagued-by-symptoms-as-experts-seek-answers (accessed on 17 March 2021).
- Waldrop, T. Clinics Are Springing up around the Country for What Some Call a Potential Second Pandemic: Long Covid (Retrieved 17 March 2021). Available online: https://www.cnn.com/2021/02/22/health/long-covid-clinics/index.html (accessed on 17 March 2021).
- Ballering, A.; Hartman, T.O.; Rosmalen, J. Long COVID-19, persistent somatic symptoms and social stigmatisation. J. Epidemiol. Community Health 2021. [Google Scholar] [CrossRef]
- Ladds, E.; Rushforth, A.; Wieringa, S.; Taylor, S.; Rayner, C.; Husain, L.; Greenhalgh, T. Developing services for long COVID: Lessons from a study of wounded healers. Clin. Med. 2021, 21, 59–65. [Google Scholar] [CrossRef]
- Greenhalgh, T.; Knight, M. Long COVID: A Primer for Family Physicians. Am. Fam. Physician 2020, 102, 716–717. [Google Scholar]
- The Lancet. Facing up to long COVID. Lancet 2020, 396, 1861. [Google Scholar] [CrossRef]
- Iqbal, A.; Iqbal, K.; Ali, S.A.; Azim, D.; Farid, E.; Baig, M.D.; Arif, T.B.; Raza, M. The COVID-19 Sequelae: A Cross-Sectional Evaluation of Post-recovery Symptoms and the Need for Rehabilitation of COVID-19 Survivors. Cureus 2021, 13, e13080. [Google Scholar] [CrossRef] [PubMed]
- Wise, J. Long covid: WHO calls on countries to offer patients more rehabilitation. BMJ 2021, 372, n405. [Google Scholar] [CrossRef] [PubMed]
- Ouyang, L.; Gong, J. Mitochondrial-targeted ubiquinone: A potential treatment for COVID-19. Med. Hypotheses 2020, 144, 110161. [Google Scholar] [CrossRef] [PubMed]
- O’Connor, K.; Sunnquist, M.; Nicholson, L.; Jason, L.A.; Newton, J.L.; Strand, E.B. Energy envelope maintenance among patients with myalgic encephalomyelitis and chronic fatigue syndrome: Implications of limited energy reserves. Chronic Illn. 2019, 15, 51–60. [Google Scholar] [CrossRef] [PubMed]
| # of Patients | Patient Population | Location | Median Time at Assessment | Methodology | Key Findings | Other Findings | |
|---|---|---|---|---|---|---|---|
| Goertz et al. [44] | 2113 | Adult; hospitalized + nonhospitalized | Netherlands | 79 days after symptom onset | Online questionnaire | Fatigue (87%), dyspnea (71%), chest tightness (44%) | Headache, muscle pain, heart palpitations, cough, sore throat, etc. |
| Huang et al. [45] | 1733 | Adult; discharged from hospital | China | 186 days after symptom onset | Ambidirectional cohort; questionnaires, etc. | Fatigue/muscle weakness (63%), sleep difficulties (26%) | Anxiety/depression, hair loss, smell disorder, etc. |
| Mandal et al. [23] | 384 | Adult; discharged from hospital | U.K. | 54 days after discharge | Questionnaire | Fatigue (69%), Breathlessness (53%) | Cough (34%), depression (15%) |
| Moreno-Perez et al. [46] | 277 | Adult | Spain | 77 days after recovery/discharge | In-person evaluation and questionnaire | Dyspnea (34.4%), cough (21.3%), headache (17.8%) | |
| Taboada et al. [47] | 242 | Adult; discharged from hospital | Spain | 6 months after discharge | Structured interview | Decreased functional status (47.5%), dyspnea (10.4%) | |
| Petersen et al. [48] | 180 | Children + Adult | Faroe Islands | 125 days after symptom onset | Patient questionnaire | At least one symptom (53%) | Fatigue, loss of smell and taste, arthralgia, headache, myalgia, dyspnea, etc. |
| Townsend et al. [49] | 153 | Adult | Ireland | 75 days after diagnosis | Cross-sectional; Chalder Fatigue Scale, etc. | Fatigue (47%) | Decreased performance on six-minute-walk test (6MWT) |
| Weerahandi et al. [50] | 152 | Adult; discharged from hospital | U.S. | 37 days after discharge | Prospective cohort; PROMIS dyspnea characteristics instrument, etc. | Dyspnea (74.3%) | Worsened mental health |
| Carfi et al. [22] | 143 | Adult; discharged from hospital | Italy | 60.3 days after symptom onset | Questionnaire | Fatigue (53.1%), dyspnea (43.4%) | Joint pain, chest pain, etc. |
| Townsend et al. [51] | 128 | Adult | Ireland | 72 days after symptom onset | Chalder fatigue scale | Fatigue (52.3%) | |
| Halpin et al. [52] | 100 | Adult; discharged from hospital | U.K. | 48 days after discharge | Cross-sectional; telephone questionnaire | Fatigue (64%), breathlessness (50%), PTSD symptoms (31%) | Speech and swallowing dysfunction, continence, vocational difficulties |
| Wong et al. [53] | 78 | Adult; discharged from hospital | Canada | 3 months after symptom onset | Prospective cohort; questionnaire | Dyspnea (50%), cough (23%) | Anxiety, depression |
| Le Bon et al. [54] | 72 | Adult | Belgium | 37 days after symptom onset | Prospective cohort; “Sniffin’ Sticks” test battery | Olfactory dysfunction (37%), gustatory dysfunction (7%) | |
| Woo et al. [55] | 18 | Adult | Germany | 85 days after recovery | TICS-M, fatigue assessment scale, PHQ-9 | Cognitive deficits (78%) | Fatigue, mood swings |
| Ortelli et al. [56] | 12 | Adult; in neurorehabilitation | Italy | 9–13 weeks post COVID | Fatigue rating scale, Beck Depression Inventory, etc. | Neuromuscular fatigue, cognitive fatigue, apathy, executive dysfunction | |
| Ludvigsson [57] | 5 | Children | Sweden | 6–8 months after COVID onset | Parental report | Fatigue, dyspnea, heart palpitations/chest pain (all 100%) | Headaches, concentration difficulties, muscle weakness, dizziness, etc. |
| Carroll et al. [58] | 1 | Adult female | U.S. | 50 days after initial infection | Case report | Status epilepticus | |
| Novak [59] | 1 | Adult female | U.S. | 2.5 months after positive test | Case report | Fatigue, headache | |
| Koumpa et al. [60] | 1 | Adult male | U.K. | 55 days after symptom onset | Case report | Hearing loss | |
| Alhiyari et al. [61] | 1 | Adult | Qatar | 4 months after treatment | Case Report | Cough | |
| Killion et al. [62] | 1 | Child | Ireland | 3 months after hospital admission | Case report | Palmoplantar rash |
| ME/CFS Criteria | COVID Studies with Matching Symptoms | Non-ME/CFS Criteria Symptoms |
|---|---|---|
| Major criteria | ||
| Duration ≥6 months | Huang et al., Ludvigsson | |
| Fatigue | Goertz et al., Huang et al., Mandal et al., Petersen et al., Townsend et al., Weerahandi et al., Carfi et al., Townsend et al., Halpin et al., Woo et al., Ortelli et al., Ludvigsson, Novak | |
| Reduced daily activity | Huang et al., Taboada et al., Weerahandi et al., Halpin et al., Ludvigsson | |
| Post-exertional malaise | Huang et al., Townsend et al., Ludvigsson | |
| Minor criteria | ||
| Neurologic/Pain | ||
| Myalgia | Goertz et al., Huang et al., Petersen et al., Carfi et al. | |
| Muscle weakness | Huang et al. | |
| Motor disturbance | ||
| Generalized hyperalgesia (worsened pain, etc.) | Halpin et al. | |
| Joint pain | Goertz et al., Huang et al., Petersen et al., Carfi et al. | |
| Headaches | Goertz et al., Huang et al., Moreno-Perez et al., Petersen et al., Carfi et al., Novak | |
| Sleep difficulties | Huang et al., Mandal et al. | |
| Goertz et al., Huang et al., Petersen et al., Carfi et al., Le Bon et al. | Olfactory dysfunction | |
| Goertz et al., Huang et al., Petersen et al., Carfi et al., Le Bon et al. | Gustatory dysfunction | |
| Koumpa et al. | Auditory dysfunction | |
| Carroll et al. | Seizure | |
| Halpin et al. | Speech difficulties | |
| Neurocognitive/Psychiatric | ||
| Difficulty thinking/processing (brain fog, confusion, etc.) | Moreno-Perez et al., Woo et al., Ortelli et al., Ludvigsson | |
| Memory difficulties | Moreno-Perez et al., Halpin et al., Woo et al. | |
| Attention difficulties | Halpin et al., Woo et al., Ortelli et al., Ludvigsson | |
| Psychiatric (depression, anxiety, PTSD, etc.) | Huang et al., Mandal et al., Weerahandi et al., Halpin et al., Wong et al., Woo et al., Ortelli et al., Ludvigsson | |
| Hypersensitivity to noise/light | Woo et al. | |
| Tinnitus, double vision | ||
| Neuroendocrine | ||
| Thermostatic instability | Goertz et al. | |
| Anorexia (loss of appetite, weight loss, etc.) | Goertz et al., Huang et al., Petersen et al., Carfi et al., Halpin et al., Ludvigsson | |
| Autonomic Manifestations | ||
| Orthostatic intolerance (dizziness, etc.) | Goertz et al., Huang et al., Carfi et al. | |
| Cardiovascular (palpitations, chest pain, etc.) | Goertz et al., Huang et al., Carfi et al. | |
| Respiratory (dyspnea, etc.) | Goertz et al., Huang et al., Mandal et al., Moreno-Perez et al., Taboada et al., Petersen et al., Weerahandi et al., Carfi et al., Halpin et al., Wong et al., Ludvigsson | |
| Gastro-intestional (Nausea/vomiting, diarrhea, abdominal pain) | Goertz et al., Huang et al., Petersen et al., Carfi et al., Ludvigsson | |
| Gastro-urinary (Incontinence, etc.) | Halpin et al. | |
| Immune | ||
| Fever/Chills | Goertz et al., Petersen et al., Ludvigsson | |
| Flu-like symptoms (cough, etc.) | Goertz et al., Huang et al., Mandal et al., Moreno-Perez et al., Petersen et al., Carfi et al., Wong et al., Alhiyari et al. | |
| Susceptibility to virus | ||
| Sore throat (swallow problems, etc.) | Goertz et al., Huang et al., Petersen et al., Carfi et al., Halpin et al. | |
| Lymph node pain/tenderness | ||
| Sensitivity to chemicals, foods, medications, odors | ||
| Carfi et al. | Sicca Syndrome | |
| Others | ||
| Goertz et al. | Ear pain | |
| Goertz et al., Moreno-Perez et al., Carfi et al. | Eye problems (red eyes, etc.) | |
| Goertz et al., Huang et al., Moreno-Perez et al., Petersen et al., Ludvigsson, Killion et al. | Dermatological symptoms (rash, etc.) | |
| Huang et al. | Hair loss | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wong, T.L.; Weitzer, D.J. Long COVID and Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS)—A Systemic Review and Comparison of Clinical Presentation and Symptomatology. Medicina 2021, 57, 418. https://doi.org/10.3390/medicina57050418
Wong TL, Weitzer DJ. Long COVID and Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS)—A Systemic Review and Comparison of Clinical Presentation and Symptomatology. Medicina. 2021; 57(5):418. https://doi.org/10.3390/medicina57050418
Chicago/Turabian StyleWong, Timothy L., and Danielle J. Weitzer. 2021. "Long COVID and Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS)—A Systemic Review and Comparison of Clinical Presentation and Symptomatology" Medicina 57, no. 5: 418. https://doi.org/10.3390/medicina57050418
APA StyleWong, T. L., & Weitzer, D. J. (2021). Long COVID and Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS)—A Systemic Review and Comparison of Clinical Presentation and Symptomatology. Medicina, 57(5), 418. https://doi.org/10.3390/medicina57050418





