Aligning Patient’s Ideas of a Good Life with Medically Indicated Therapies in Geriatric Rehabilitation Using Smart Sensors
Abstract
1. Introduction
- Parkinson’s disease: The Gait Tutor (mHealth Technologies) is a commercially available medical device that includes a smartphone application and gait sensors. The device assesses gait quality in real time and gives voice instructions for a safe, effective, and steady gait. This enables gait rehabilitation for, e.g., Parkinson’s patients without the patients having to attend a clinical facility [14]. The accuracy and precision is as good as in professional gait labs [15].
- Cardiac rehabilitation: A system consisting in a wearable device and a smartphone application measures and reports instantaneous heart rates during intensive physical exercise. The smartphone application is connected to a web interface and a database at a medical station to monitor the prescribed exercises. The system enables patients to conduct their rehabilitation at home instead of a hospital [16]. It eliminates the need for self-reporting, which can be prone to bias.
- Pulmonary rehabilitation: A remote system for a multimodal sensors-based application provides a cost-effective rehabilitation at home. Patients who have chronic breathing difficulties can thereby track their progress and performance and receive exercise assignments and guidance [17].
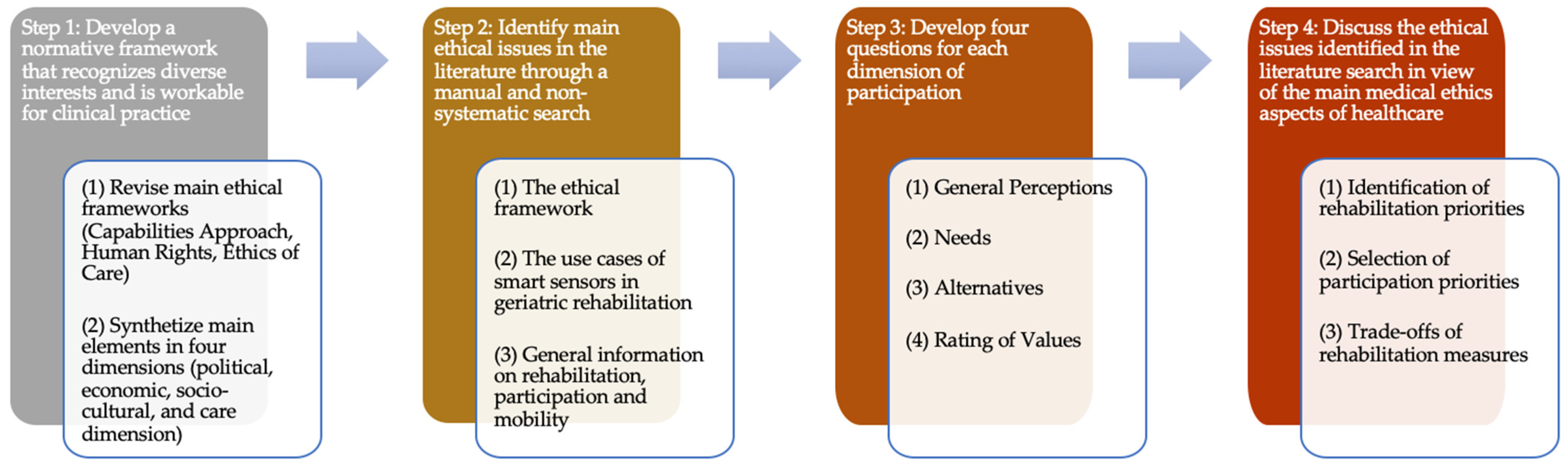
2. Materials and Methods
3. Results

3.1. Political Dimension
3.2. Economic Dimension
3.3. Socio-Cultural Dimension
3.4. Care Dimension
3.5. Assessing Patient’s Priorities

4. Discussion
4.1. Identification of Rehabilitation Priorities
4.2. Assessment of Alternative Forms of Participation
4.3. Ethical Implications for Privacy and Accessibility
4.4. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Mendes, J.J.A., Jr.; Vieira, M.E.M.; Pires, M.B.; Stevan, S.L., Jr. Sensor Fusion and Smart Sensor in Sports and Biomedical Applications. Sensors 2016, 16, 1569. [Google Scholar] [CrossRef]
- Belsi, A.; Papi, E.; McGregor, A.H. Impact of wearable technology on psychosocial factors of osteoarthritis management: A qualitative study. BMJ Open 2016, 6, e010064. [Google Scholar] [CrossRef][Green Version]
- Zwijsen, S.A.; Niemeijer, A.R.; Hertogh, C.M. Ethics of using assistive technology in the care for community-dwelling elderly people: An overview of the literature. Aging Ment. Health 2011, 15, 419–427. [Google Scholar] [CrossRef] [PubMed]
- Patel, S.; Park, H.; Bonato, P.; Chan, L.; Rodgers, M. A review of wearable sensors and systems with application in rehabilitation. J. Neuroeng. Rehabil. 2012, 9, 1–17. [Google Scholar] [CrossRef] [PubMed]
- McAdams, E.; Krupaviciute, A.; Géhin, C.; Grenier, E.; Massot, B.; Dittmar, A.; Rubel, P.; Fayn, J. Wearable sensor systems: The challenges. In Proceedings of the 2011 Annual International Conference of the IEEE Engineering in Medicine and Biology Society, Boston, MA, USA, 30 August–3 September 2011; pp. 3648–3651. [Google Scholar]
- Kluge, E.-H.W. Ethical issues in geriatric medicine: A unique problematic? Health Care Anal. 2002, 10, 379–390. [Google Scholar] [CrossRef]
- Spencer Hartmann Júnior, J.A.; Almeida de Farias Fernandes, A.L.; Araújo Pimentel de Medeiros, A.G.; Carvalho de Vasconcelos, C.A.; Lope de Amorim, L.L.; Ferreira Silveira de Queiroga, M.; Torres de Araújo, R.C. Hopelessness in the elderly: A systematic review. MOJ Gerontol. Geriatr. 2018, 3, 273–278. [Google Scholar] [CrossRef]
- Steger, F.; Rubeis, G. Selbstbestimmung und individualisierte Medizin. In Selbst-Oder Bestimmt; Lindner, J.F., Ed.; Nomos: Baden-Baden, Germany, 2017; pp. 27–44. [Google Scholar]
- Nussbaum, M.C. Frontiers of Justice: Disability, Nationality, Species Membership; The Belknap Press of Harvard University Press: Cambridge, MA, USA, 2006. [Google Scholar]
- Robeyns, I.; Byskov, M.F. The Capability Approach. Stanford Encyclopedia of Philosophy (Winter 2021 Edition). 2021. Available online: http://plato.stanford.edu/entries/capability-approach (accessed on 1 December 2021).
- Chan, M.; Estève, D.; Fourniols, J.-Y.; Escriba, C.; Campo, E. Smart wearable systems: Current status and future challenges. Artif. Intell. Med. 2012, 56, 137–156. [Google Scholar] [CrossRef] [PubMed]
- Penteridis, L.; D’Onofrio, G.; Sancarlo, D.; Giuliani, F.; Ricciardi, F.; Cavallo, F.; Greco, A.; Trochidis, I.; Gkiokas, A. Robotic and sensor technologies for mobility in older people. Rejuvenation Res. 2017, 20, 401–410. [Google Scholar] [CrossRef]
- do Nascimento, L.M.S.; Bonfati, L.V.; Freitas, M.L.B.; Mendes Junior, J.J.A.; Siqueira, H.V.; Stevan, S.L. Sensors and Systems for Physical Rehabilitation and Health Monitoring—A Review. Sensors 2020, 20, 4063. [Google Scholar] [CrossRef]
- Zoetewei, D.; Herman, T.; Brozgol, M.; Ginis, P.; Thumm, P.C.; Ceulemans, E.; Decaluwé, E.; Palmerini, L.; Ferrari, A.; Nieuwboer, A.; et al. Protocol for the DeFOG trial: A randomized controlled trial on the effects of smartphone-based, on-demand cueing for freezing of gait in Parkinson’s disease. Contemp. Clin. Trials Commun. 2021, 24, 100817. [Google Scholar] [CrossRef]
- Casamassima, F.; Ferrari, A.; Milosevic, B.; Ginis, P.; Farella, E.; Rocchi, L. A Wearable System for Gait Training in Subjects with Parkinson’s Disease. Sensors 2014, 14, 6229–6246. [Google Scholar] [CrossRef]
- Chung, H.; Lee, H.; Kim, C.; Hong, S.; Lee, J. Patient-provider interaction system for efficient home-based cardiac rehabilitation exercise. IEEE Access 2019, 7, 14611–14622. [Google Scholar] [CrossRef]
- Tey, C.-K.; An, J.; Chung, W.-Y. A novel remote rehabilitation system with the fusion of noninvasive wearable device and motion sensing for pulmonary patients. Comput. Math. Methods Med. 2017, 2017, 5823740. [Google Scholar] [CrossRef]
- Oosterlaken, I. Human Capabilities in Design for Values. In Handbook of Ethics, Values, and Technological Design: Sources, Theory, Values and Application Domains; van den Hoven, J., Vermaas, P.E., van de Poel, I., Eds.; Springer: Dordrecht, The Netherlands, 2015; pp. 221–250. [Google Scholar]
- Jacobs, N. Capability Sensitive Design for Health and Wellbeing Technologies. Sci. Eng. Ethics 2020, 26, 3363–3391. [Google Scholar] [CrossRef]
- Entwistle, V.A.; Watt, I.S. Treating patients as persons: A capabilities approach to support delivery of person-centered care. Am. J. Bioeth. 2013, 13, 29–39. [Google Scholar] [CrossRef] [PubMed]
- Nussbaum, M.C. Capabilities and Human Rights. Fordham Law Rev. 1997, 66, 273–300. [Google Scholar]
- Kittay, E. Loves Labor Revisited. Hypatia 2002, 17, 237–250. [Google Scholar] [CrossRef]
- Levasseur, M.; Routhier, S.; Clapperton, I.; Doré, C.; Gallagher, F. Social participation needs of older adults living in a rural regional county municipality: Toward reducing situations of isolation and vulnerability. BMC Geriatr. 2020, 20, 456. [Google Scholar] [CrossRef] [PubMed]
- Joshi, A.; Kale, S.; Chandel, S.; Pal, D. Likert Scale: Explored and Explained. Br. J. Appl. Sci. Technol. 2015, 7, 396–403. [Google Scholar] [CrossRef]
- Office of the High Commissioner for Human Rights. Guidelines for States on the Effective Implementation of the Right to Participate in Public Affairs; United Nations: Geneva, Switzerland, 2018. [Google Scholar]
- Nussbaum, M.C. The capabilities of people with cognitive disabilities. Metaphilosophy 2009, 40, 331–351. [Google Scholar] [CrossRef]
- Goodman, N.; Stokes, L.C. Reducing the cost of voting: An evaluation of internet voting’s effect on turnout. Br. J. Political Sci. 2020, 50, 1155–1167. [Google Scholar] [CrossRef]
- Steinvorth, U. The right to work and the right to develop one’s capabilities. Anal. Krit. 2009, 31, 101–113. [Google Scholar] [CrossRef]
- Timmermann, C. Contributive Justice: An Exploration of a Wider Provision of Meaningful Work. Soc. Justice Res. 2018, 31, 85–111. [Google Scholar] [CrossRef]
- Gheaus, A.; Herzog, L. The goods of work (other than money!). J. Soc. Philos. 2016, 47, 70–89. [Google Scholar] [CrossRef]
- International Covenant on Economic, Social and Cultural Rights. 1966. Available online: https://www.ohchr.org/en/professionalinterest/pages/cescr.aspx (accessed on 1 December 2021).
- Aloisi, A.; De Stefano, V. Essential jobs, remote work and digital surveillance: Addressing the COVID-19 pandemic panopticon. Int. Labour Rev. 2021. [Google Scholar] [CrossRef] [PubMed]
- Shaver, L. The right to science and culture. Wis. Law Rev. 2010, 121, 121–184. [Google Scholar] [CrossRef]
- Kittay, E.F. When caring is just and justice is caring: Justice and mental retardation. Public Cult. 2001, 13, 557–579. [Google Scholar] [CrossRef]
- Vallor, S. Carebots and caregivers: Sustaining the ethical ideal of care in the twenty-first century. Philos. Technol. 2011, 24, 251–268. [Google Scholar] [CrossRef]
- Karimi, M.; Brazier, J.; Basarir, H. The capability approach: A critical review of its application in health economics. Value Health 2016, 19, 795–799. [Google Scholar] [CrossRef] [PubMed]
- Yang, K.; Isaia, B.; Brown, L.J.; Beeby, S. E-Textiles for Healthy Ageing. Sensors 2019, 19, 4463. [Google Scholar] [CrossRef] [PubMed]
- Jecker, N.S. Age-related inequalities in health and healthcare: The life stages approach. Dev. World Bioeth. 2018, 18, 144–155. [Google Scholar] [CrossRef] [PubMed]
- Tijsen, L.M.; Derksen, E.W.; Achterberg, W.P.; Buijck, B.I. Challenging rehabilitation environment for older patients. Clin. Interv. Aging 2019, 14, 1451. [Google Scholar] [CrossRef]
- Pereira, A.; Folgado, D.; Nunes, F.; Almeida, J.; Sousa, I. Using Inertial Sensors to Evaluate Exercise Correctness in Electromyography-based Home Rehabilitation Systems. In Proceedings of the 2019 IEEE International Symposium on Medical Measurements and Applications (MeMeA), Istanbul, Turkey, 26–28 June 2019; pp. 1–6. [Google Scholar]
- Neuhauser, L.; Kreps, G.L.; Morrison, K.; Athanasoulis, M.; Kirienko, N.; Van Brunt, D. Using design science and artificial intelligence to improve health communication: ChronologyMD case example. Patient Educ. Couns. 2013, 92, 211–217. [Google Scholar] [CrossRef] [PubMed]
- Schicktanz, S.; Schweda, M. Aging 4.0? Rethinking the ethical framing of technology-assisted eldercare. Hist. Philos. Life Sci. 2021, 43, 93. [Google Scholar] [CrossRef]
- Sen, A. The Idea of Justice; Harvard University Press: Cambridge, MA, USA, 2009. [Google Scholar]
- Cirillo, D.; Catuara-Solarz, S.; Morey, C.; Guney, E.; Subirats, L.; Mellino, S.; Gigante, A.; Valencia, A.; Rementeria, M.J.; Chadha, A.S. Sex and gender differences and biases in artificial intelligence for biomedicine and healthcare. NPJ Digit. Med. 2020, 3, 1–11. [Google Scholar] [CrossRef]
- Schneider, I. Diskriminierungsgefahren und Regulationsansätze bei der medizinischen Nutzung von KI. Z. Med. Ethik 2021, 67, 327–350. [Google Scholar] [CrossRef]
- Chen, D.; Cai, Y.; Qian, X.; Ansari, R.; Xu, W.; Chu, K.-C.; Huang, M.-C. Bring gait lab to everyday life: Gait analysis in terms of activities of daily living. IEEE Internet Things J. 2019, 7, 1298–1312. [Google Scholar] [CrossRef]
- Appelboom, G.; Camacho, E.; Abraham, M.E.; Bruce, S.S.; Dumont, E.L.P.; Zacharia, B.E.; D’Amico, R.; Slomian, J.; Reginster, J.Y.; Bruyère, O.; et al. Smart wearable body sensors for patient self-assessment and monitoring. Arch. Public Health 2014, 72, 28. [Google Scholar] [CrossRef]
- Friedman, B.; Kahn, P.H.; Borning, A. Value sensitive design and information systems. In The Handbook of Information and Computer Ethics; Himma, K.E., Tavani, H.T., Eds.; John Wiley & Sons: Hoboken, NJ, USA, 2008; pp. 69–101. [Google Scholar]
- Essén, A. The two facets of electronic care surveillance: An exploration of the views of older people who live with monitoring devices. Soc. Sci. Med. 2008, 67, 128–136. [Google Scholar] [CrossRef]
- Bruce, C.R. Informed decision making for in-home use of motion sensor-based monitoring technologies. Gerontologist 2012, 52, 317–324. [Google Scholar] [CrossRef] [PubMed]
- Coughlin, J.F.; D’Ambrosio, L.A.; Reimer, B.; Pratt, M.R. Older adult perceptions of smart home technologies: Implications for research, policy & market innovations in healthcare. In Proceedings of the 2007 29th Annual International Conference of the IEEE Engineering in Medicine and Biology Society, Lyon, France, 23–26 August 2007; pp. 1810–1815. [Google Scholar]
- Cajamarca, G.; Herskovic, V.; Rossel, P.O. Enabling Older Adults’ Health Self-Management through Self-Report and Visualization—A Systematic Literature Review. Sensors 2020, 20, 4348. [Google Scholar] [CrossRef] [PubMed]
- Ienca, M.; Wangmo, T.; Jotterand, F.; Kressig, R.W.; Elger, B. Ethical design of intelligent assistive technologies for dementia: A descriptive review. Sci. Eng. Ethics 2018, 24, 1035–1055. [Google Scholar] [CrossRef] [PubMed]
- Vogler, B.S.; Schwab, G. Ethics of Wearable Medical and Fitness Devices. Available online: https://benediktsvogler.com/downloads/Ethics%20of%20wearable%20medical%20and%20fitness%20devices.pdf (accessed on 1 December 2021).


Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Timmermann, C.; Ursin, F.; Predel, C.; Steger, F. Aligning Patient’s Ideas of a Good Life with Medically Indicated Therapies in Geriatric Rehabilitation Using Smart Sensors. Sensors 2021, 21, 8479. https://doi.org/10.3390/s21248479
Timmermann C, Ursin F, Predel C, Steger F. Aligning Patient’s Ideas of a Good Life with Medically Indicated Therapies in Geriatric Rehabilitation Using Smart Sensors. Sensors. 2021; 21(24):8479. https://doi.org/10.3390/s21248479
Chicago/Turabian StyleTimmermann, Cristian, Frank Ursin, Christopher Predel, and Florian Steger. 2021. "Aligning Patient’s Ideas of a Good Life with Medically Indicated Therapies in Geriatric Rehabilitation Using Smart Sensors" Sensors 21, no. 24: 8479. https://doi.org/10.3390/s21248479
APA StyleTimmermann, C., Ursin, F., Predel, C., & Steger, F. (2021). Aligning Patient’s Ideas of a Good Life with Medically Indicated Therapies in Geriatric Rehabilitation Using Smart Sensors. Sensors, 21(24), 8479. https://doi.org/10.3390/s21248479





