Activation of Nrf2 by Natural Bioactive Compounds: A Promising Approach for Stroke?
Abstract
1. Introduction
2. Nrf2 and Its Regulation
3. Natural Compounds as Modulator of Nrf2 Pathway in Stroke Animal Models
3.1. Tea Bioactive Compounds
3.2. Citrus Bioactive Compounds
3.3. Spice Bioactive Compounds
3.4. Fruit Bioactive Compounds
3.5. Other Dietary Bioactive Compounds
3.6. Ginseng Bioactive Compounds
3.7. Salvia Miltiorrhiza Bioactive Compounds
3.8. Ginkgo biloba Bioactive Compounds
3.9. Bioactive Compounds of Chuanxiong Rhizome
3.10. Gastrodia elata Blume Bioactive Compounds
3.11. Other Plant-Derived Bioactive Compounds
3.12. Studies with a Combination of Bioactive Compounds
4. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Abbreviations
| 4-HNE | 4-hydroxynonenal |
| 8-OHdG | 8-hydroxy-2′-deoxyguanosine |
| α-LA | Alpha-lipoic acid |
| βTrCP | β-transducin repeat-containing protein |
| ABPPk | Achyranthes bidentata polypeptide k |
| Ahr | Aryl hydrocarbon receptor |
| AMPK | Monophosphate-activated protein kinase |
| AP-1 | Activator protein 1 |
| AQP4 | Aquaporin 4 |
| ARE | Antioxidant Response Element |
| BACH1 | BTB domain and CNC homolog 1 |
| BDNF | Brain-Derived Neurotrophic Factor |
| BBB | Blood Brain Barrier |
| CAT | Catalase |
| CBP | CREB-binding protein |
| CECs | Cerebral endothelial cells |
| CL | Corilagin |
| CGA | Chlorogenic acid |
| COX2 | Cyclooxygenase 2 |
| CREB | Cyclic AMP-responsive element binding protein |
| D3T | 3H-1,2-dithiole-3-thione |
| DATS | Diallyl trisulfide |
| DCFH-DA | Dichlorofluorescin-Diacetate |
| DGMI | Diterpene ginkgolides meglumine injection |
| DHC | Dihydrocapsaicin |
| DMF | Dimethyl fumarate |
| DTMF | 5,3′-dihydroxy-3,7,4′-trimethoxyflavone |
| EC | (-)-epicatechin |
| EGCG | (-)-Epigallocatechin-3-gallate |
| FA | Forsythiaside A |
| FGF | Fibroblast growth factor |
| GA | Ginkgolides A |
| GAS | Gastrodin |
| GB | Ginkgolides B |
| GC | Ginkgolides C |
| GLGZG | Gualou Guizhi granule |
| GPx | Glutathione peroxidase |
| GSH | Glutathione |
| GSK-3β | Glycogen Synthase Kinase-3β |
| GSSG | Oxidized glutathione |
| GST | Glutathione S-transferase |
| H2O2 | Hydrogen peroxide |
| HHC | Hexahydrocurcumin |
| HLJDD | Huang-Lian-Jie-Du-Decoction |
| HO-1 | Heme oxygenase 1 |
| HQO-1 | NAD(P)H quinine oxidoreductase |
| HSYA | Hydroxysafflor yellow A |
| ICAM-1 | Intercellular Adhesion Molecule 1 |
| ICH | Intracerebral hemorrhage |
| IL | Interleukin |
| iNOS | inducible nitric oxide synthase |
| I/R | Ischemia/Reperfusion |
| KBA | 11-Keto-β-boswellic acid |
| Keap1 | Kelch- like ECH- associated protein 1 |
| LPS | Lipopolysaccharide |
| LyA | Lyciumamide A |
| LTC | Longxuetongluo capsule |
| MAPK | Mitogen-Activated Protein Kinase |
| MAPK/ERK | MAPK/extracellular signal-related kinase |
| MCA | Middle Cerebral Artery |
| MCAO | MCA Occlusion |
| MDA | Malondialdehyde |
| miRNAs | MicroRNAs |
| MMP | Metalloproteinase |
| Nar | Naringenin |
| Nef | Neferine |
| NF-κB | Nuclear factor kappa-light-chain-enhancer of activated B cells |
| NGF | Nerve Growth Factor |
| NO | Nitric oxide |
| Nob | Nobiletin |
| NOX | NADPH oxidase |
| Nom | Nomilin |
| NQO1 | NAD(P)H quinone oxidoreductase 1 |
| Nrf2 | Nuclear factor erythroid 2-related factor 2 |
| NSCs | Neural stem cells |
| O2 | Oxygen |
| OGD | Oxygen Glucose Deprivation |
| PARP-1 | Poly [ADP-ribose] polymerase 1 |
| PB | Procyanidin B2 |
| PCA | Protocatechualdehyde |
| PCGE | phenolic components of Gastrodia elata Blume |
| PKC | Protein Kinase C |
| PI3K | Phosphoinositide 3-kinases |
| pMCAO | Permanent MCAO |
| pdMCAO | Permanent distal MCAO |
| PPARγ | Peroxisome proliferator activated receptor gamma |
| RA | Rosmarinic acid |
| Rg1 | Ginsenoside Rg1 |
| ROS | Reactive Oxygen Species |
| SAAG | Safflower extract and aceglutamide |
| SAC | S-allyl cysteine |
| SAH | Subarachnoid hemorrhage |
| Sch A | Schizandrin A |
| SEI | Senkyunolide I |
| SLI | Salvianolate lyophilized injection |
| sMAF | small musculoaponeurotic fibrosarcoma oncogene homologue |
| SOD | Superoxide dismutase |
| Swe | Swertiamarin |
| TGs | Total glycosides |
| THSWD | Tao Hong Si Wu decoction |
| TLB | Trilobatin |
| TMP | Tetramethylpyrazine |
| TNF | Tumor necrosis factor |
| tPA | Tissue plasminogen activator |
| TSA | Tanshinone IIA |
| VEGF | Vascular Endothelial Growth Factor |
| VEGFR2 | Vascular Endothelial Growth Factor Receptor 2 |
| WT | Wildtype |
| XN | Xanthohumol |
| XST | Xueshuantong injection |
| ZO-1 | Zonulin 1 |
References
- Hankey, G.J. Stroke. Lancet 2017, 389, 641–654. [Google Scholar] [CrossRef]
- Benjamin, E.J.; Virani, S.S.; Callaway, C.W.; Chamberlain, A.M.; Chang, A.R.; Cheng, S.; Chiuve, S.E.; Cushman, M.; Delling, F.N.; Deo, R.; et al. Heart Disease and Stroke Statistics—2018 Update: A Report from the American Heart Association. Circulation 2018, 137, e67–e492. [Google Scholar] [CrossRef] [PubMed]
- Thiebaut, A.M.; Gauberti, M.; Ali, C.; Martinez De Lizarrondo, S.; Vivien, D.; Yepes, M.; Roussel, B.D. The role of plasminogen activators in stroke treatment: Fibrinolysis and beyond. Lancet Neurol. 2018, 17, 1121–1132. [Google Scholar] [CrossRef]
- Brouwers, H.B.; Goldstein, J.N. Therapeutic Strategies in Acute Intracerebral Hemorrhage. Neurotherapeutics 2011, 9, 87–98. [Google Scholar] [CrossRef]
- Sun, M.-S.; Jin, H.; Sun, X.; Huang, S.; Zhang, F.-L.; Guo, Z.-N.; Yang, Y. Free Radical Damage in Ischemia-Reperfusion Injury: An Obstacle in Acute Ischemic Stroke after Revascularization Therapy. Oxidative Med. Cell. Longev. 2018, 2018, 1–17. [Google Scholar] [CrossRef]
- Qu, J.; Chen, W.; Hu, R.; Feng, H. The Injury and Therapy of Reactive Oxygen Species in Intracerebral Hemorrhage Looking at Mitochondria. Oxidative Med. Cell. Longev. 2016, 2016, 1–9. [Google Scholar] [CrossRef]
- Chamorro, Á.; Dirnagl, U.; Urra, X.; Planas, A.M. Neuroprotection in acute stroke: Targeting excitotoxicity, oxidative and nitrosative stress, and inflammation. Lancet Neurol. 2016, 15, 869–881. [Google Scholar] [CrossRef]
- Zhang, R.; Xu, M.; Wang, Y.; Xie, F.; Zhang, G.; Qin, X. Nrf2—A Promising Therapeutic Target for Defensing Against Oxidative Stress in Stroke. Mol. Neurobiol. 2017, 54, 6006–6017. [Google Scholar] [CrossRef]
- Lautié, E.; Russo, O.; Ducrot, P.; Boutin, J.A. Unraveling Plant Natural Chemical Diversity for Drug Discovery Purposes. Front. Pharmacol. 2020, 11, 397. [Google Scholar] [CrossRef]
- Guo, Z. The modification of natural products for medical use. Acta Pharm. Sin. B 2017, 7, 119–136. [Google Scholar] [CrossRef]
- Hayes, J.; Dinkova-Kostova, A.T. The Nrf2 regulatory network provides an interface between redox and intermediary metabolism. Trends Biochem. Sci. 2014, 39, 199–218. [Google Scholar] [CrossRef] [PubMed]
- Itoh, K.; Wakabayashi, N.; Katoh, Y.; Ishii, T.; Igarashi, K.; Engel, J.D.; Yamamoto, M. Keap1 represses nuclear activation of antioxidant responsive elements by Nrf2 through binding to the amino-terminal Neh2 domain. Genome Res. 1999, 13, 76–86. [Google Scholar] [CrossRef] [PubMed]
- Kobayashi, A.; Kang, M.-I.; Okawa, H.; Ohtsuji, M.; Zenke, Y.; Chiba, T.; Igarashi, K.; Yamamoto, M. Oxidative Stress Sensor Keap1 Functions as an Adaptor for Cul3-Based E3 Ligase To Regulate Proteasomal Degradation of Nrf2. Mol. Cell. Biol. 2004, 24, 7130–7139. [Google Scholar] [CrossRef] [PubMed]
- Yamamoto, M.; Kensler, T.W.; Motohashi, H. The KEAP1-NRF2 System: A Thiol-Based Sensor-Effector Apparatus for Maintaining Redox Homeostasis. Physiol. Rev. 2018, 98, 1169–1203. [Google Scholar] [CrossRef]
- Cuadrado, A.; Rojo, A.I.; Wells, G.; Hayes, J.; Cousin, S.P.; Rumsey, W.L.; Attucks, O.C.; Franklin, S.; Levonen, A.-L.; Kensler, T.W.; et al. Therapeutic targeting of the NRF2 and KEAP1 partnership in chronic diseases. Nat. Rev. Drug Discov. 2019, 18, 295–317. [Google Scholar] [CrossRef]
- Sivandzade, F.; Prasad, S.; Bhalerao, A.; Cucullo, L. NRF2 and NF-κB interplay in cerebrovascular and neurodegenerative disorders: Molecular mechanisms and possible therapeutic approaches. Redox Biol. 2019, 21, 101059-017. [Google Scholar] [CrossRef]
- Wardyn, J.D.; Ponsford, A.H.; Sanderson, C.M. Dissecting molecular cross-talk between Nrf2 and NF-κB response pathways. Biochem. Soc. Trans. 2015, 43, 621–626. [Google Scholar] [CrossRef]
- Tonelli, C.; Chio, I.I.C.; Tuveson, D. Transcriptional Regulation by Nrf2. Antioxid. Redox Signal. 2018, 29, 1727–1745. [Google Scholar] [CrossRef]
- Dhakshinamoorthy, S.; Jain, A.K.; Bloom, D.A.; Jaiswal, A.K. Bach1 Competes with Nrf2 Leading to Negative Regulation of the Antioxidant Response Element (ARE)-mediated NAD(P)H:Quinone Oxidoreductase 1 Gene Expression and Induction in Response to Antioxidants. J. Biol. Chem. 2005, 280, 16891–16900. [Google Scholar] [CrossRef]
- Niture, S.K.; Khatri, R.; Jaiswal, A.K. Regulation of Nrf2-an update. Free Radic. Biol. Med. 2014, 66, 36–44. [Google Scholar] [CrossRef]
- Huang, Y.; Li, W.; Su, Z.-Y.; Kong, A.-N. The complexity of the Nrf2 pathway: Beyond the antioxidant response. J. Nutr. Biochem. 2015, 26, 1401–1413. [Google Scholar] [CrossRef]
- Tavakkoli, A.; Iranshahi, M.; Hasheminezhad, S.H.; Hayes, A.W.; Karimi, G. The neuroprotective activities of natural products through the Nrf2 upregulation. Phytother. Res. 2019, 33, 2256–2273. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Zhang, P.; Tang, Z. Animal models of transient ischemic attack: A review. Acta Neurol. Belg. 2020, 120, 267–275. [Google Scholar] [CrossRef]
- Sommer, C.J. Ischemic stroke: Experimental models and reality. Acta Neuropathol. 2017, 133, 245–261. [Google Scholar] [CrossRef]
- McCabe, C.; Arroja, M.M.; Reid, E.; Macrae, I.M. Animal models of ischaemic stroke and characterisation of the ischaemic penumbra. Neuropharmacology 2018, 134, 169–177. [Google Scholar] [CrossRef] [PubMed]
- Marbacher, S.; Grüter, B.; Schöpf, S.; Croci, D.; Nevzati, E.; D’Alonzo, D.; Lattmann, J.; Roth, T.; Bircher, B.; Wolfert, C.; et al. Systematic Review of In Vivo Animal Models of Subarachnoid Hemorrhage: Species, Standard Parameters, and Outcomes. Transl. Stroke Res. 2018, 10, 250–258. [Google Scholar] [CrossRef] [PubMed]
- Khan, N.; Mukhtar, H. Tea Polyphenols in Promotion of Human Health. Nutrients 2018, 11, 39. [Google Scholar] [CrossRef]
- Li, R.; Li, X.; Wu, H.; Yang, Z.; Fei, L.; Zhu, J. Theaflavin attenuates cerebral ischemia/reperfusion injury by abolishing miRNA-128-3p-mediated Nrf2 inhibition and reducing oxidative stress. Mol. Med. Rep. 2019, 20, 4893–4904. [Google Scholar] [CrossRef]
- Khoubnasabjafari, M.; Ansarin, K.; Jouyban, A. Reliability of malondialdehyde as a biomarker of oxidative stress in psychological disorders. BioImpacts 2015, 5, 123–127. [Google Scholar] [CrossRef]
- Bai, Q.; Lyu, Z.; Yang, X.; Pan, Z.; Lou, J.; Dong, T. Epigallocatechin-3-gallate promotes angiogenesis via up-regulation of Nfr2 signaling pathway in a mouse model of ischemic stroke. Behav. Brain Res. 2017, 321, 79–86. [Google Scholar] [CrossRef]
- Leonardo, C.C.; Mendes, M.; Ahmad, A.S.; Doré, S. Efficacy of prophylactic flavan-3-ol in permanent focal ischemia in 12-mo-old mice. Am. J. Physiol. Circ. Physiol. 2015, 308, H583–H591. [Google Scholar] [CrossRef] [PubMed]
- Silva-Palacios, A.; Ostolga-Chavarría, M.; Zazueta, C.; Konigsberg, M. Nrf2: Molecular and epigenetic regulation during aging. Ageing Res. Rev. 2018, 47, 31–40. [Google Scholar] [CrossRef] [PubMed]
- Zhang, H.; Davies, K.J.A.; Forman, H.J. Oxidative stress response and Nrf2 signaling in aging. Free Radic. Biol. Med. 2015, 88, 314–336. [Google Scholar] [CrossRef] [PubMed]
- Schmidlin, C.J.; Dodson, M.B.; Madhavan, L.; Zhang, D.D. Redox regulation by NRF2 in aging and disease. Free Radic. Biol. Med. 2019, 134, 702–707. [Google Scholar] [CrossRef] [PubMed]
- Lan, X.; Han, X.; Li, Q.; Wang, J. (-)-Epicatechin, a Natural Flavonoid Compound, Protects Astrocytes Against Hemoglobin Toxicity via Nrf2 and AP-1 Signaling Pathways. Mol. Neurobiol. 2016, 54, 7898–7907. [Google Scholar] [CrossRef]
- Cai, Z.-Y.; Li, X.-M.; Liang, J.-P.; Xiang, L.-P.; Wang, K.-R.; Shi, Y.-L.; Yang, R.; Shi, M.; Ye, J.-H.; Lu, J.-L.; et al. Bioavailability of Tea Catechins and Its Improvement. Molecules 2018, 23, 2346. [Google Scholar] [CrossRef]
- Clifford, M.N.; Van Der Hooft, J.J.J.; Crozier, A. Human studies on the absorption, distribution, metabolism, and excretion of tea polyphenols. Am. J. Clin. Nutr. 2013, 98, 1619S–1630S. [Google Scholar] [CrossRef]
- Zou, Z.; Xi, W.; Hu, Y.; Nie, C.; Zhou, Z. Antioxidant activity of Citrus fruits. Food Chem. 2016, 196, 885–896. [Google Scholar] [CrossRef]
- Shi, Y.-S.; Zhang, Y.; Liu, B.; Li, C.-B.; Wu, J.; Li, Y. Nomilin protects against cerebral ischemia-reperfusion induced neurological deficits and blood-brain barrier disruption via the Nrf2 pathway. Food Funct. 2019, 10, 5323–5332. [Google Scholar] [CrossRef]
- Kalyanaraman, B.; Darley-Usmar, V.; Davies, K.E.; Dennery, P.A.; Forman, H.J.; Grisham, M.B.; Mann, G.E.; Moore, K.; Roberts, L.J.; Ischiropoulos, H. Measuring reactive oxygen and nitrogen species with fluorescent probes: Challenges and limitations. Free Radic. Biol. Med. 2012, 52, 1–6. [Google Scholar] [CrossRef]
- Wang, K.; Chen, Z.; Huang, J.; Huang, L.; Luo, N.; Liang, X.; Liang, M.; Xie, W. Naringenin prevents ischaemic stroke damage via anti-apoptotic and anti-oxidant effects. Clin. Exp. Pharmacol. Physiol. 2017, 44, 862–871. [Google Scholar] [CrossRef] [PubMed]
- Singh, B.; Singh, J.P.; Kaur, A.; Singh, N. Phenolic composition, antioxidant potential and health benefits of citrus peel. Food Res. Int. 2020, 132, 109114. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Zhang, X.; Zhang, C.; Bai, X.; Zhang, J.; Zhao, X.; Chen, L.; Wang, L.; Zhu, C.; Cui, L.; et al. Nobiletin promotes antioxidant and anti-inflammatory responses and elicits protection against ischemic stroke in vivo. Brain Res. 2016, 1636, 130–141. [Google Scholar] [CrossRef] [PubMed]
- Rahman, I.; Kode, A.; Biswas, S.K. Assay for quantitative determination of glutathione and glutathione disulfide levels using enzymatic recycling method. Nat. Protoc. 2006, 1, 3159–3165. [Google Scholar] [CrossRef]
- Bora, H.; Kamle, M.; Mahato, D.K.; Tiwari, P.; Kumar, P. Citrus Essential Oils (CEOs) and Their Applications in Food: An Overview. Plants 2020, 9, 357. [Google Scholar] [CrossRef]
- Barrera-Sandoval, A.M.; Osorio, E.; Cardona-Gómez, G.P. Microglial-targeting induced by intranasal linalool during neurological protection postischemia. Eur. J. Pharmacol. 2019, 857, 172420. [Google Scholar] [CrossRef]
- Cai, Y.; Zhang, S.; Wang, Q.; Sun, H.; Zhou, M.; Hu, S.; Xiang, Z. A Rapid, Selective and Sensitive UPLC-MS/MS Method for Quantification of Nomilin in Rat Plasma and Its Application in a Pharmacokinetic Study. Planta Med. 2015, 82, 224–229. [Google Scholar] [CrossRef]
- Kanaze, F.I.; Bounartzi, M.I.; Georgarakis, M.; Niopas, I. Pharmacokinetics of the citrus flavanone aglycones hesperetin and naringenin after single oral administration in human subjects. Eur. J. Clin. Nutr. 2006, 61, 472–477. [Google Scholar] [CrossRef]
- Erlund, I.; Silaste, M.L.; Alfthan, G.; Rantala, M.; Kesaniemi, Y.A.; Aro, A. Plasma concentrations of the flavonoids hesperetin, naringenin and quercetin in human subjects following their habitual diets, and diets high or low in fruit and vegetables. Eur. J. Clin. Nutr. 2002, 56, 891–898. [Google Scholar] [CrossRef]
- Goh, J.X.H.; Tan, L.T.-H.; Goh, J.K.; Chan, K.G.; Pusparajah, P.; Lee, L.-H.; Goh, B.-H. Nobiletin and Derivatives: Functional Compounds from Citrus Fruit Peel for Colon Cancer Chemoprevention. Cancers 2019, 11, 867. [Google Scholar] [CrossRef] [PubMed]
- Yang, Z.; Kuboyama, T.; Tohda, C. A Systematic Strategy for Discovering a Therapeutic Drug for Alzheimer’s Disease and Its Target Molecule. Front. Pharmacol. 2017, 8. [Google Scholar] [CrossRef] [PubMed]
- Singh, S.P.; Wahajuddin, M.; Tewari, D.; Patel, K.; Jain, G.K. Permeability determination and pharmacokinetic study of nobiletin in rat plasma and brain by validated high-performance liquid chromatography method. Fitotereapia 2011, 82, 1206–1214. [Google Scholar] [CrossRef] [PubMed]
- Shi, F.; Zhao, Y.; Firempong, C.K.; Xu, X. Preparation, characterization and pharmacokinetic studies of linalool-loaded nanostructured lipid carriers. Pharm. Biol. 2016, 54, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Jiang, T.A. Health Benefits of Culinary Herbs and Spices. J. AOAC Int. 2019, 102, 395–411. [Google Scholar] [CrossRef]
- Shi, H.; Jing, X.; Wei, X.; Perez, R.G.; Ren, M.; Zhang, X.; Lou, H. S-allyl cysteine activates the Nrf2-dependent antioxidant response and protects neurons against ischemic injuryin vitroandin vivo. J. Neurochem. 2015, 133, 298–308. [Google Scholar] [CrossRef]
- Silva-Islas, C.A.; Chanez-Cardenas, M.E.; Barrera-Oviedo, D.; Ortiz-Plata, A.; Pedraza-Chaverri, J.; Maldonado, P.D. Diallyl Trisulfide Protects Rat Brain Tissue against the Damage Induced by Ischemia-Reperfusion through the Nrf2 Pathway. Antioxidants 2019, 8, 410. [Google Scholar] [CrossRef]
- Janyou, A.; Wicha, P.; Jittiwat, J.; Suksamrarn, A.; Tocharus, C.; Tocharus, J. Dihydrocapsaicin Attenuates Blood Brain Barrier and Cerebral Damage in Focal Cerebral Ischemia/Reperfusion via Oxidative Stress and Inflammatory. Sci. Rep. 2017, 7, 10556. [Google Scholar] [CrossRef]
- Cui, H.Y.; Zhang, X.J.; Yang, Y.; Zhang, C.; Zhu, C.H.; Miao, J.Y.; Chen, R. Rosmarinic acid elicits neuroprotection in ischemic stroke via Nrf2 and heme oxygenase 1 signaling. Neural Regen. Res. 2018, 13, 2119–2128. [Google Scholar] [CrossRef]
- Li, W.; Suwanwela, N.C.; Patumraj, S. Curcumin by down-regulating NF-kB and elevating Nrf2, reduces brain edema and neurological dysfunction after cerebral I/R. Microvasc. Res. 2016, 106, 117–127. [Google Scholar] [CrossRef]
- Wicha, P.; Tocharus, J.; Janyou, A.; Jittiwat, J.; Changtam, C.; Suksamrarn, A.; Tocharus, C. Hexahydrocurcumin protects against cerebral ischemia/reperfusion injury, attenuates inflammation, and improves antioxidant defenses in a rat stroke model. PLoS ONE 2017, 12, e0189211. [Google Scholar] [CrossRef]
- Chang, S.K.; Alasalvar, C.; Shahidi, F. Superfruits: Phytochemicals, antioxidant efficacies, and health effects—A comprehensive review. Crit. Rev. Food Sci. Nutr. 2018, 59, 1580–1604. [Google Scholar] [CrossRef] [PubMed]
- Gao, K.; Liu, M.; Ding, Y.; Yao, M.; Zhu, Y.; Zhao, J.; Cheng, L.; Bai, J.; Wang, F.; Cao, J.; et al. A phenolic amide (LyA) isolated from the fruits of Lycium barbarum protects against cerebral ischemia-reperfusion injury via PKCepsilon/Nrf2/HO-1 pathway. Aging 2019, 11, 12361–12374. [Google Scholar] [CrossRef] [PubMed]
- Yang, Z.; Weian, C.; Susu, H.; Hanmin, W. Protective effects of mangiferin on cerebral ischemia–reperfusion injury and its mechanisms. Eur. J. Pharmacol. 2016, 771, 145–151. [Google Scholar] [CrossRef]
- Nassiri-Asl, M.; Hosseinzadeh, H. Review of the Pharmacological Effects ofVitis vinifera(Grape) and its Bioactive Constituents: An Update. Phytother. Res. 2016, 30, 1392–1403. [Google Scholar] [CrossRef] [PubMed]
- Narayanan, S.V.; Dave, K.R.; Saul, I.; Perez-Pinzon, M.A. Resveratrol Preconditioning Protects Against Cerebral Ischemic Injury via Nuclear Erythroid 2–Related Factor 2. Stroke 2015, 46, 1626–1632. [Google Scholar] [CrossRef]
- Sies, H. Polyphenols and health: Update and perspectives. Arch. Biochem. Biophys. 2010, 501, 2–5. [Google Scholar] [CrossRef]
- Zhang, L.; Wang, Y.; Li, D.; Ho, C.-T.; Li, J.; Wan, X. The absorption, distribution, metabolism and excretion of procyanidins. Food Funct. 2016, 7, 1273–1281. [Google Scholar] [CrossRef]
- Wu, S.; Yue, Y.; Li, J.; Li, Z.; Li, X.; Niu, Y.; Xiang, J.; Ding, H. Procyanidin B2 attenuates neurological deficits and blood-brain barrier disruption in a rat model of cerebral ischemia. Mol. Nutr. Food Res. 2015, 59, 1930–1941. [Google Scholar] [CrossRef]
- Semwal, D.K.; Semwal, R.B.; Combrinck, S.; Viljoen, A. Myricetin: A Dietary Molecule with Diverse Biological Activities. Nutrients 2016, 8, 90. [Google Scholar] [CrossRef]
- Wu, S.; Yue, Y.; Peng, A.; Zhang, L.; Xiang, J.; Cao, X.; Ding, H.; Yin, S. Myricetin ameliorates brain injury and neurological deficits via Nrf2 activation after experimental stroke in middle-aged rats. Food Funct. 2016, 7, 2624–2634. [Google Scholar] [CrossRef]
- Liu, D.; Wang, H.; Zhang, Y.; Zhang, Z. Protective Effects of Chlorogenic Acid on Cerebral Ischemia/Reperfusion Injury Rats by Regulating Oxidative Stress-Related Nrf2 Pathway. Drug Des. Dev. Ther. 2020, 14, 51–60. [Google Scholar] [CrossRef] [PubMed]
- Shahidi, F.; De Camargo, A.C. Tocopherols and Tocotrienols in Common and Emerging Dietary Sources: Occurrence, Applications, and Health Benefits. Int. J. Mol. Sci. 2016, 17, 1745. [Google Scholar] [CrossRef] [PubMed]
- Shang, J.; Yan, H.; Jiao, Y.; Ohta, Y.; Liu, X.; Li, X.; Morihara, R.; Nakano, Y.; Fukui, Y.; Shi, X.; et al. Therapeutic Effects of Pretreatment with Tocovid on Oxidative Stress in Postischemic Mice Brain. J. Stroke Cerebrovasc. Dis. 2018, 27, 2096–2105. [Google Scholar] [CrossRef] [PubMed]
- Kuo, P.-C.; Yu, I.-C.; Scofield, B.A.; Brown, D.A.; Curfman, E.T.; Paraiso, H.C.; Chang, F.-L.; Yen, J.-H. 3 H -1,2-Dithiole-3-thione as a novel therapeutic agent for the treatment of ischemic stroke through Nrf2 defense pathway. Brain Behav. Immun. 2017, 62, 180–192. [Google Scholar] [CrossRef]
- Zhao, X.; Sun, G.; Ting, S.-M.; Song, S.; Zhang, J.; Edwards, N.J.; Aronowski, J. Cleaning up after ICH: The role of Nrf2 in modulating microglia function and hematoma clearance. J. Neurochem. 2014, 133, 144–152. [Google Scholar] [CrossRef] [PubMed]
- Desmawati, D.; Sulastri, D. Phytoestrogens and Their Health Effect. Open Access Maced. J. Med. Sci. 2019, 7, 495–499. [Google Scholar] [CrossRef]
- Miao, Z.-Y.; Xia, X.; Che, L.; Song, Y.-T. Genistein attenuates brain damage induced by transient cerebral ischemia through up-regulation of Nrf2 expression in ovariectomized rats. Neurol. Res. 2018, 40, 1–7. [Google Scholar] [CrossRef]
- Guo, M.; Lu, H.; Qin, J.; Qu, S.; Wang, W.; Guo, Y.; Liao, W.; Song, M.; Chen, J.; Wang, Y. Biochanin A Provides Neuroprotection Against Cerebral Ischemia/Reperfusion Injury by Nrf2-Mediated Inhibition of Oxidative Stress and Inflammation Signaling Pathway in Rats. Med. Sci. Monit. 2019, 25, 8975–8983. [Google Scholar] [CrossRef]
- Jiao, Y.; Cao, Y.; Lu, X.; Wang, J.; Saitgareeva, A.; Kong, X.; Song, C.; Li, J.; Tian, K.; Zhang, S.; et al. Xanthohumol protects neuron from cerebral ischemia injury in experimental stroke. Mol. Biol. Rep. 2020, 47, 2417–2425. [Google Scholar] [CrossRef]
- Salehi, B.; Yılmaz, Y.B.; Antika, G.; Tumer, T.B.; Mahomoodally, M.F.; Lobine, D.; Akram, M.; Riaz, M.; Capanoglu, E.; Contreras, M.D.M.; et al. Insights on the Use of α-Lipoic Acid for Therapeutic Purposes. Biomolecules 2019, 9, 356. [Google Scholar] [CrossRef]
- Lv, C.; Maharjan, S.; Wang, Q.; Sun, Y.; Han, X.; Wang, S.; Mao, Z.; Xin, Y.; Zhang, B. α-Lipoic Acid Promotes Neurological Recovery After Ischemic Stroke by Activating the Nrf2/HO-1 Pathway to Attenuate Oxidative Damage. Cell. Physiol. Biochem. 2017, 43, 1273–1287. [Google Scholar] [CrossRef] [PubMed]
- Valentová, K.; Vrba, J.; Bancirova, M.; Ulrichová, J.; Křen, V. Isoquercitrin: Pharmacology, toxicology, and metabolism. Food Chem. Toxicol. 2014, 68, 267–282. [Google Scholar] [CrossRef]
- Dai, Y.; Zhang, H.; Zhang, J.; Yan, M. Isoquercetin attenuates oxidative stress and neuronal apoptosis after ischemia/reperfusion injury via Nrf2-mediated inhibition of the NOX4/ROS/NF-κB pathway. Chem. Interact. 2018, 284, 32–40. [Google Scholar] [CrossRef]
- Baliga, M.S.; Dsouza, J.J. Amla (Emblica officinalis Gaertn), a wonder berry in the treatment and prevention of cancer. Eur. J. Cancer Prev. 2011, 20, 225–239. [Google Scholar] [CrossRef] [PubMed]
- Ding, Y.; Ren, D.; Xu, H.; Liu, W.; Liu, T.; Li, L.; Li, J.; Li, Y.; Wen, A. Antioxidant and pro-angiogenic effects of corilagin in rat cerebral ischemia via Nrf2 activation. Oncotarget 2017, 8, 114816–114828. [Google Scholar] [CrossRef] [PubMed]
- Zhang, S.; Xu, S.; Duan, H.; Zhu, Z.; Yang, Z.; Cao, J.; Zhao, Y.; Huang, Z.; Wu, Q.; Duan, J. A novel, highly-water-soluble apigenin derivative provides neuroprotection following ischemia in male rats by regulating the ERK/Nrf2/HO-1 pathway. Eur. J. Pharmacol. 2019, 855, 208–215. [Google Scholar] [CrossRef]
- Hu, L.; Chen, W.; Tian, F.; Yuan, C.; Wang, H.; Yue, H. Neuroprotective role of fucoxanthin against cerebral ischemic/reperfusion injury through activation of Nrf2/HO-1 signaling. Biomed. Pharmacother. 2018, 106, 1484–1489. [Google Scholar] [CrossRef]
- Ben Salem, M.; Affes, H.; Ksouda, K.; Dhouibi, R.; Sahnoun, Z.; Hammami, S.; Zeghal, K.M. Pharmacological Studies of Artichoke Leaf Extract and Their Health Benefits. Plant Foods Hum. Nutr. 2015, 70, 441–453. [Google Scholar] [CrossRef]
- Li, Q.; Tian, Z.; Wang, M.; Kou, J.; Wang, C.; Rong, X.; Li, J.; Xie, X.; Pang, X. Luteoloside attenuates neuroinflammation in focal cerebral ischemia in rats via regulation of the PPARγ/Nrf2/NF-κB signaling pathway. Int. Immunopharmacol. 2019, 66, 309–316. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Wang, G.; Yi, J.; Xu, Y.; Duan, S.; Li, T.; Sun, X.-G.; Dong, L. The effect of monascin on hematoma clearance and edema after intracerebral hemorrhage in rats. Brain Res. Bull. 2017, 134, 24–29. [Google Scholar] [CrossRef]
- Liu, L.; Anderson, G.A.; Fernandez, T.G.; Doré, S. Efficacy and Mechanism of Panax Ginseng in Experimental Stroke. Front. Mol. Neurosci. 2019, 13, 294. [Google Scholar] [CrossRef] [PubMed]
- Liu, L.; Vollmer, M.K.; Fernandez, V.M.; Dweik, Y.; Kim, H.; Doré, S. Korean Red Ginseng Pretreatment Protects Against Long-Term Sensorimotor Deficits After Ischemic Stroke Likely Through Nrf2. Front. Cell. Neurosci. 2018, 12, 74. [Google Scholar] [CrossRef] [PubMed]
- Liu, L.; Kelly, M.G.; Wierzbicki, E.L.; Escober-Nario, I.C.; Vollmer, M.K.; Doré, S. Nrf2 Plays an Essential Role in Long-Term Brain Damage and Neuroprotection of Korean Red Ginseng in a Permanent Cerebral Ischemia Model. Antioxidants 2019, 8, 273. [Google Scholar] [CrossRef]
- Liu, L.; Vollmer, M.K.; Ahmad, A.S.; Fernandez, V.M.; Lee, D.; Doré, S. Pretreatment with Korean red ginseng or dimethyl fumarate attenuates reactive gliosis and confers sustained neuroprotection against cerebral hypoxic-ischemic damage by an Nrf2-dependent mechanism. Free Radic. Biol. Med. 2019, 131, 98–114. [Google Scholar] [CrossRef] [PubMed]
- Liu, L.; Vollmer, M.K.; Kelly, M.G.; Fernandez, V.M.; Fernandez, T.G.; Kim, H.; Doré, S. Reactive Gliosis Contributes to Nrf2-Dependent Neuroprotection by Pretreatment with Dimethyl Fumarate or Korean Red Ginseng Against Hypoxic-Ischemia: Focus on Hippocampal Injury. Mol. Neurobiol. 2020, 57, 105–117. [Google Scholar] [CrossRef] [PubMed]
- Chu, S.-F.; Zhang, Z.; Zhou, X.; He, W.-B.; Chen, C.; Luo, P.; Liu, D.-D.; Ai, Q.-D.; Gong, H.-F.; Wang, Z.-Z.; et al. Ginsenoside Rg1 protects against ischemic/reperfusion-induced neuronal injury through miR-144/Nrf2/ARE pathway. Acta Pharmacol. Sin. 2018, 40, 13–25. [Google Scholar] [CrossRef] [PubMed]
- Guo, H.; Adah, D.; James, P.B.; Liu, Q.; Li, G.; Ahmadu, P.; Chai, L.; Wang, S.; Liu, Y.; Hu, L.-M. Xueshuantong Injection (Lyophilized) Attenuates Cerebral Ischemia/Reperfusion Injury by the Activation of Nrf2–VEGF Pathway. Neurochem. Res. 2018, 43, 1096–1103. [Google Scholar] [CrossRef]
- Wang, J.; Xu, J.; Gong, X.; Yang, M.; Zhang, C.; Li, M. Biosynthesis, Chemistry, and Pharmacology of Polyphenols from Chinese Salvia Species: A Review. Molecules 2019, 24, 155. [Google Scholar] [CrossRef]
- Su, C.-Y.; Ming, Q.-L.; Rahman, K.; Han, T.; Qin, L.-P. Salvia miltiorrhiza: Traditional medicinal uses, chemistry, and pharmacology. Chin. J. Nat. Med. 2015, 13, 163–182. [Google Scholar] [CrossRef]
- Guo, C.; Wang, S.; Duan, J.; Jia, N.; Zhu, Y.; Ding, Y.; Guan, Y.; Wei, G.; Yin, Y.; Xi, M.; et al. Protocatechualdehyde Protects Against Cerebral Ischemia-Reperfusion-Induced Oxidative Injury Via Protein Kinase Cε/Nrf2/HO-1 Pathway. Mol. Neurobiol. 2017, 54, 833–845. [Google Scholar] [CrossRef]
- Cai, M.; Guo, Y.; Wang, S.; Wei, H.; Sun, S.; Zhao, G.; Dong, H. Tanshinone IIA Elicits Neuroprotective Effect Through Activating the Nuclear Factor Erythroid 2-Related Factor-Dependent Antioxidant Response. Rejuvenation Res. 2017, 20, 286–297. [Google Scholar] [CrossRef] [PubMed]
- Wang, F.; He, Q.; Wang, J.; Yuan, Q.; Guo, H.; Chai, L.; Wang, S.; Hu, L.; Zhang, Y. Neuroprotective effect of salvianolate lyophilized injection against cerebral ischemia in type 1 diabetic rats. BMC Complement. Altern. Med. 2017, 17, 258. [Google Scholar] [CrossRef] [PubMed]
- Tian, J.; Liu, Y.; Chen, K.; Tian, Y.L.A.K.C.J. Ginkgo biloba Extract in Vascular Protection: Molecular Mechanisms and Clinical Applications. Curr. Vasc. Pharmacol. 2017, 15, 532–548. [Google Scholar] [CrossRef] [PubMed]
- Zhang, W.; Song, J.; Yan, R.; Li, L.; Xiao, Z.-Y.; Zhou, W.-X.; Wang, Z.-Z.; Xiao, W.; Du, G.-H. Diterpene ginkgolides protect against cerebral ischemia/reperfusion damage in rats by activating Nrf2 and CREB through PI3K/Akt signaling. Acta Pharmacol. Sin. 2018, 39, 1259–1272. [Google Scholar] [CrossRef]
- Liu, Q.; Jin, Z.; Xu, Z.; Yang, H.; Li, L.; Li, G.; Li, F.; Gu, S.; Zong, S.; Zhou, J.; et al. Antioxidant effects of ginkgolides and bilobalide against cerebral ischemia injury by activating the Akt/Nrf2 pathway in vitro and in vivo. Cell Stress Chaperon 2019, 24, 441–452. [Google Scholar] [CrossRef]
- Zhao, J.-J.; Song, J.-Q.; Pan, S.-Y.; Wang, K. Treatment with Isorhamnetin Protects the Brain Against Ischemic Injury in Mice. Neurochem. Res. 2016, 41, 1939–1948. [Google Scholar] [CrossRef]
- Chen, Z.; Zhang, C.; Gao, F.; Fu, Q.; Fu, C.; He, Y.; Zhang, J. A systematic review on the rhizome of Ligusticum chuanxiong Hort. (Chuanxiong). Food Chem. Toxicol. 2018, 119, 309–325. [Google Scholar] [CrossRef]
- Chang, C.-Y.; Kao, T.-K.; Chen, W.-Y.; Ou, Y.-C.; Li, J.-R.; Liao, S.-L.; Raung, S.-L.; Chen, C.-J. Tetramethylpyrazine inhibits neutrophil activation following permanent cerebral ischemia in rats. Biochem. Biophys. Res. Commun. 2015, 463, 421–427. [Google Scholar] [CrossRef]
- Li, J.; Yu, J.; Ma, H.; Yang, N.; Li, L.; Zheng, D.-D.; Wu, M.-X.; Zhao, Z.-L.; Qi, H. Intranasal Pretreatment withZ-Ligustilide, the Main Volatile Component ofRhizoma Chuanxiong, Confers Prophylaxis against Cerebral Ischemia via Nrf2 and HSP70 Signaling Pathways. J. Agric. Food Chem. 2017, 65, 1533–1542. [Google Scholar] [CrossRef]
- Hu, Y.; Duan, M.; Liang, S.; Wang, Y.; Feng, Y. Senkyunolide I protects rat brain against focal cerebral ischemia–reperfusion injury by up-regulating p-Erk1/2, Nrf2/HO-1 and inhibiting caspase 3. Brain Res. 2015, 1605, 39–48. [Google Scholar] [CrossRef]
- Zhan, H.-D.; Zhou, H.-Y.; Sui, Y.-P.; Du, X.-L.; Wang, W.-H.; Dai, L.; Sui, F.; Huo, H.-R.; Jiang, T.-L. The rhizome of Gastrodia elata Blume—An ethnopharmacological review. J. Ethnopharmacol. 2016, 189, 361–385. [Google Scholar] [CrossRef] [PubMed]
- Peng, Z.; Wang, S.; Chen, G.; Cai, M.; Liu, R.; Deng, J.; Liu, J.; Zhang, T.; Tan, Q.; Hai, C. Gastrodin Alleviates Cerebral Ischemic Damage in Mice by Improving Anti-oxidant and Anti-inflammation Activities and Inhibiting Apoptosis Pathway. Neurochem. Res. 2015, 40, 661–673. [Google Scholar] [CrossRef] [PubMed]
- Luo, L.; Kim, S.-W.; Lee, H.-K.; Kim, I.-D.; Lee, H.; Lee, J.-K. Gastrodin exerts robust neuroprotection in the postischemic brain via its protective effect against Zn2+-toxicity and its anti-oxidative effects in astrocytes. Anim. Cells Syst. 2018, 22, 429–437. [Google Scholar] [CrossRef] [PubMed]
- Shi, A.; Xiang, J.; He, F.; Zhu, Y.; Zhu, G.; Lin, Y.; Zhou, N. The Phenolic Components of Gastrodia elata improve Prognosis in Rats after Cerebral Ischemia/Reperfusion by Enhancing the Endogenous Antioxidant Mechanisms. Oxidative Med. Cell. Longev. 2018, 2018, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Liu, X.-C.; Wu, C.-Z.; Hu, X.-F.; Wang, T.-L.; Jin, X.-P.; Ke, S.-F.; Wang, E.; Wu, G. Gastrodin Attenuates Neuronal Apoptosis and Neurological Deficits after Experimental Intracerebral Hemorrhage. J. Stroke Cerebrovasc. Dis. 2020, 29, 104483. [Google Scholar] [CrossRef] [PubMed]
- Nowak, A.; Zaklos-Szyda, M.; Blasiak, J.; Nowak, A.; Zhang, Z.; Zhang, B. Potential of Schisandra chinensis (Turcz.) Baill. in Human Health and Nutrition: A Review of Current Knowledge and Therapeutic Perspectives. Nutrients 2019, 11, 333. [Google Scholar] [CrossRef]
- Zhou, F.; Wang, M.; Ju, J.; Wang, Y.; Liu, Z.; Zhao, X.; Yan, Y.; Yan, S.; Luo, X.; Fang, Y. Schizandrin A protects against cerebral ischemia-reperfusion injury by suppressing inflammation and oxidative stress and regulating the AMPK/Nrf2 pathway regulation. Am. J. Transl. Res. 2019, 11, 199–209. [Google Scholar]
- Tao, H.; Wu, X.; Cao, J.; Peng, Y.; Wang, A.; Pei, J.; Ulrih, N.P.; Wang, S.; Wang, Y. Rhodiola species: A comprehensive review of traditional use, phytochemistry, pharmacology, toxicity, and clinical study. Med. Res. Rev. 2019, 39, 1779–1850. [Google Scholar] [CrossRef]
- Hu, J.; Han, J.; Xiao, Q.; Lin, Y.-H.; Zheng, Z.-Z.; He, Z.-D.; Chen, L.-D. Neuroprotective effects of salidroside on focal cerebral ischemia/reperfusion injury involves the nuclear erythroid 2-related factor 2 pathway. Neural Regen. Res. 2015, 10, 1989–1996. [Google Scholar] [CrossRef]
- Zhang, X.; Lai, W.; Ying, X.; Xu, L.; Chu, K.; Brown, J.; Chen, L.; Hong, G. Salidroside Reduces Inflammation and Brain Injury After Permanent Middle Cerebral Artery Occlusion in Rats by Regulating PI3K/PKB/Nrf2/NFkappaB Signaling Rather than Complement C3 Activity. Inflammation 2019, 42, 1830–1842. [Google Scholar] [CrossRef]
- Wang, F.; Li, R.; Tu, P.; Chen, J.; Zeng, K.; Jiang, Y. Total Glycosides of Cistanche deserticola Promote Neurological Function Recovery by Inducing Neurovascular Regeneration via Nrf-2/Keap-1 Pathway in MCAO/R Rats. Front. Pharmacol. 2020, 11, 236. [Google Scholar] [CrossRef]
- Yen, T.-L.; Chen, R.-J.; Jayakumar, T.; Lu, W.-J.; Hsieh, C.-Y.; Hsu, M.; Yang, C.H.; Chang, C.-C.; Lin, Y.-K.; Lin, K.H.; et al. Andrographolide stimulates p38 mitogen-activated protein kinase–nuclear factor erythroid-2-related factor 2–heme oxygenase 1 signaling in primary cerebral endothelial cells for definite protection against ischemic stroke in rats. Transl. Res. 2016, 170, 57–72. [Google Scholar] [CrossRef] [PubMed]
- Ma, T.; Shi, Y.L.; Wang, Y.L. Forsythiaside A protects against focal cerebral ischemic injury by mediating the activation of the Nrf2 and endoplasmic reticulum stress pathways. Mol. Med. Rep. 2019, 20, 1313–1320. [Google Scholar] [CrossRef]
- Ding, Y.; Chen, M.; Wang, M.; Li, Y.; Wen, A. Posttreatment with 11-Keto-β-Boswellic Acid Ameliorates Cerebral Ischemia–Reperfusion Injury: Nrf2/HO-1 Pathway as a Potential Mechanism. Mol. Neurobiol. 2015, 52, 1430–1439. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.; Wei, W.; Lan, X.; Liu, N.; Li, Y.; Ma, H.; Sun, T.; Peng, X.; Zhuang, C.; Yu, J.Q. Neuroprotective Effect of Swertiamain on Cerebral Ischemia/Reperfusion Injury by Inducing the Nrf2 Protective Pathway. ACS Chem. Neurosci. 2019, 10, 2276–2286. [Google Scholar] [CrossRef] [PubMed]
- Wu, C.; Chen, J.; Yang, R.; Duan, F.; Li, S.; Chen, X. Mitochondrial protective effect of neferine through the modulation of nuclear factor erythroid 2-related factor 2 signalling in ischaemic stroke. Br. J. Pharmacol. 2019, 176, 400–415. [Google Scholar] [CrossRef]
- Gao, Y.; Xu, X.; Chang, S.; Wang, Y.; Xu, Y.; Ran, S.; Huang, Z.; Li, P.; Li, J.; Zhang, L.; et al. Totarol prevents neuronal injury in vitro and ameliorates brain ischemic stroke: Potential roles of Akt activation and HO-1 induction. Toxicol. Appl. Pharmacol. 2015, 289, 142–154. [Google Scholar] [CrossRef] [PubMed]
- Xie, Y.Z.; Zhang, X.J.; Zhang, C.; Yang, Y.; He, J.N.; Chen, Y.X. Protective effects of leonurine against ischemic stroke in mice by activating nuclear factor erythroid 2-related factor 2 pathway. CNS Neurosci. Ther. 2019, 25, 1006–1017. [Google Scholar] [CrossRef]
- Wu, G.; Zhu, L.; Yuan, X.; Chen, H.; Xiong, R.; Zhang, S.; Cheng, H.; Shen, Y.; An, H.; Li, T.; et al. Britanin Ameliorates Cerebral Ischemia–Reperfusion Injury by Inducing the Nrf2 Protective Pathway. Antioxid. Redox Signal. 2017, 27, 754–768. [Google Scholar] [CrossRef]
- Chen, Z.; Mao, X.; Liu, A.; Gao, X.; Chen, X.; Ye, M.; Ye, J.; Liu, P.; Xu, S.; Liu, J.; et al. Osthole, a Natural Coumarin Improves Cognitive Impairments and BBB Dysfunction After Transient Global Brain Ischemia in C57 BL/6J Mice: Involvement of Nrf2 Pathway. Neurochem. Res. 2015, 40, 186–194. [Google Scholar] [CrossRef]
- Gao, J.; Chen, N.; Li, N.; Xu, F.; Wang, W.; Lei, Y.; Shi, J.; Gong, Q. Neuroprotective effects of trilobatin, a novel naturally-occurring Sirt3 agonist from Lithocarpus polystachyus Rehd., mitigates cerebral ischemia/reperfusion injury: Involvement of TLR4/NF-kappaB and Nrf2/Keap-1 signaling. Antioxid. Redox Signal. 2020, 33, 117–143. [Google Scholar]
- Cheng, Q.; Shen, Y.T.; Cheng, Z.H.; Shao, Q.; Wang, C.P.; Sun, H.L.; Zhang, Q. Achyranthes bidentata polypeptide k suppresses neuroinflammation in BV2 microglia through Nrf2-dependent mechanism. Ann. Transl. Med. 2019, 7, 575. [Google Scholar] [CrossRef]
- Kwon, Y.-W.; Cheon, S.Y.; Park, S.Y.; Song, J.; Lee, J.-H. Tryptanthrin Suppresses the Activation of the LPS-Treated BV2 Microglial Cell Line via Nrf2/HO-1 Antioxidant Signaling. Front. Cell. Neurosci. 2017, 11, 277. [Google Scholar] [CrossRef] [PubMed]
- Lee, D.-S.; Lee, M.; Sung, S.H.; Jeong, G.-S. Involvement of heme oxygenase-1 induction in the cytoprotective and neuroinflammatory activities of Siegesbeckia Pubescens isolated from 5,3′-dihydroxy-3,7,4′-trimethoxyflavone in HT22 cells and BV2 cells. Int. Immunopharmacol. 2016, 40, 65–72. [Google Scholar] [CrossRef] [PubMed]
- Hong, Q.; Yang, Y.; Wang, Z.; Xu, L.; Yan, Z. Longxuetongluo capsule alleviates lipopolysaccharide-induced neuroinflammation by regulating multiple signaling pathways in BV2 microglia cells. J. Chin. Med. Assoc. JCMA 2020, 83, 255–265. [Google Scholar] [CrossRef]
- Zhang, Y.; Fan, L.; Li, H.; Wang, X.; Xu, W.; Chu, K.; Lin, Y. Gualou Guizhi Granule Protects Against Oxidative Injury by Activating Nrf2/ARE Pathway in Rats and PC12 Cells. Neurochem. Res. 2018, 43, 1003–1009. [Google Scholar] [CrossRef]
- Xu, H.; Liu, W.; Liu, T.; Su, N.; Guo, C.; Feng, X.; Dou, F.; Ding, Y.; Shi, L.; Wen, A. Synergistic neuroprotective effects of Danshensu and hydroxysafflor yellow A on cerebral ischemia-reperfusion injury in rats. Oncotarget 2017, 8. [Google Scholar] [CrossRef]
- Zhang, J.; Zhou, R.; Xiang, C.; Fan, F.; Gao, J.; Zhang, Y.; Tang, S.; Xu, H.; Yang, H. Enhanced thioredoxin, glutathione and Nrf2 antioxidant systems by safflower extract and aceglutamide attenuate cerebral ischaemia/reperfusion injury. J. Cell. Mol. Med. 2020, 24, 4967–4980. [Google Scholar] [CrossRef]
- Wang, F.-J.; Wang, S.-X.; Chai, L.-J.; Zhang, Y.; Guo, H.; Hu, L.-M. Xueshuantong injection (lyophilized) combined with salvianolate lyophilized injection protects against focal cerebral ischemia/reperfusion injury in rats through attenuation of oxidative stress. Acta Pharmacol. Sin. 2017, 39, 998–1011. [Google Scholar] [CrossRef]
- Li, L.; Yang, N.; Nin, L.; Zhao, Z.; Chen, L.; Yu, J.; Jiang, Z.; Zhong, Z.; Zeng, D.; Qi, H.; et al. Chinese herbal medicine formula Tao Hong Si Wu decoction protects against cerebral ischemia–reperfusion injury via PI3K/Akt and the Nrf2 signaling pathway. J. Nat. Med. 2014, 69, 76–85. [Google Scholar] [CrossRef]
- Zhang, Q.; Wang, J.; Zhang, C.; Liao, S.; Li, P.; Xu, D.; Lv, Y.; Yang, M.; Kong, L. The components of Huang-Lian-Jie-Du-Decoction act synergistically to exert protective effects in a rat ischemic stroke model. Oncotarget 2016, 7, 80872–80887. [Google Scholar] [CrossRef]


| Natural Compound | Sources | Experimental Model | Tested Doses and Administration | Results | Nrf2 Mechanism | Ref. |
|---|---|---|---|---|---|---|
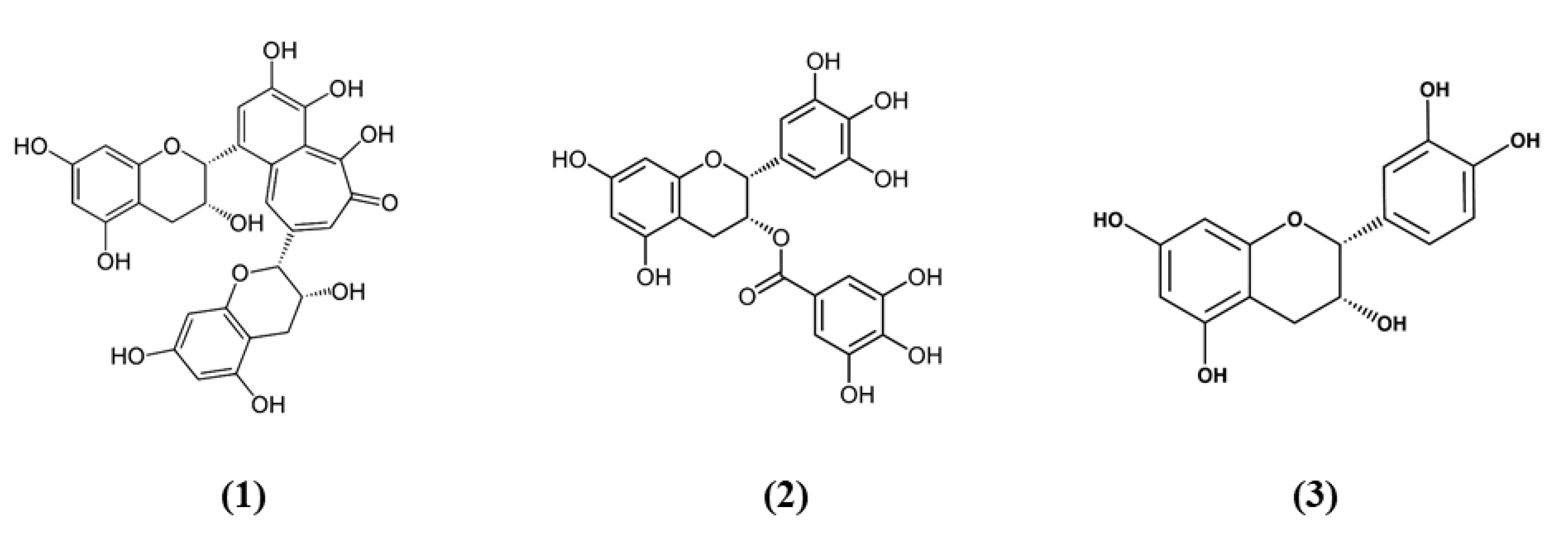
| Theaflavin | Black tea | In vivo: Rats subjected to tMCAO; In vitro: Primary rat NSCs exposed to OGD | In vivo: 10, 50 mg/kg i.v. 2 h after MCAO, daily for a week; In vitro: 2 and 10 µM for 2 h before OGD. | In vivo: ↓ infarct volume and oxidative stress; ↑ memory and learning. In vitro: ↓ apoptosis and oxidative stress; ↑ proliferation. | ↓ miRNA-128-3p ↑ Nrf2 and downstream antioxidant enzymes | [28] |
| (-)-Epigallocatechin-3-gallate | Green tea | Mice subjected to tMCAO | 50 mg/kg i.p at the end of surgery and daily for a week | ↓ infarct volume; ↑ neurologic function and angiogenesis. | ↑ ERK/Nrf2 | [30] |
| (-)-epicatechin | Green tea | WT and Nrf−/− mice subjected to pdMCAO | 15 mg/kg by gavage 90 min before pdMCAO | ↓ infarct volume | - | [31] |
| (-)-epicatechin | Green tea | Mouse WT and Nrf−/− astrocytes treated with hemoglobin | 10 µM before or after hemoglobin treatment | ↓ oxidative stress and AP-1 | ↑ Nrf2/SOD1 | [35] |
| Nomilin | Citrus fruits | In vivo: Rats subjected to tMCAO; In vitro: SH-SY5Y cells exposed to OGD | In vivo: 50 mg/kg orally 2 h before MCAO (for neurobehavioral tests: 2 h before tests every day for 6 days); In vitro: 0.1, 0.25, 0.5, 1, 2, 4, 8 μM for 12 h after OGD | In vivo: ↓ infarct volume, brain edema, BBB disruption, and oxidative stress; ↑ neurological score. In vitro: ↓ apoptosis and oxidative stress | ↑ Nrf2 and antioxidant enzymes | [39] |
| Naringenin | Citrus fruits | In vivo: Rats subjected to MCAO; In vitro: rat cortical neurons exposed to OGD | In vivo: 80 μM i.p. after MCAO; In vitro: 20, 40, and 80 μM after OGD. | In vivo: ↓ brain edema and apoptosis; ↑ neurological score. In vitro: ↓ apoptosis and oxidative stress; ↑ proliferation. | ↑ antioxidant enzymes | [41] |
| Nobiletin | Citrus peel | Rats subjected to pMCAO | 10 and 25 mg/kg i.p. daily starting 3 days before MCAO induction and a dose after | ↓ brain edema, infarct volume, oxidative stress, and inflammation; ↑ neurological score. | ↑ Nrf2 and antioxidant enzymes | [43] |
| Linalool | Citrus peel and citrus essential oils | In vivo: rats subjected to tMCAO; In vitro: rat primary astrocyte and microglial cultures treated with glutamate | In vivo: 25 mg/kg intranasal daily for one month In vitro: 100 nM for 24 h | In vivo: ↓ infarct volume and inflammation; ↑ neurological score. In vitro: ↓ inflammation. | - | [46] |
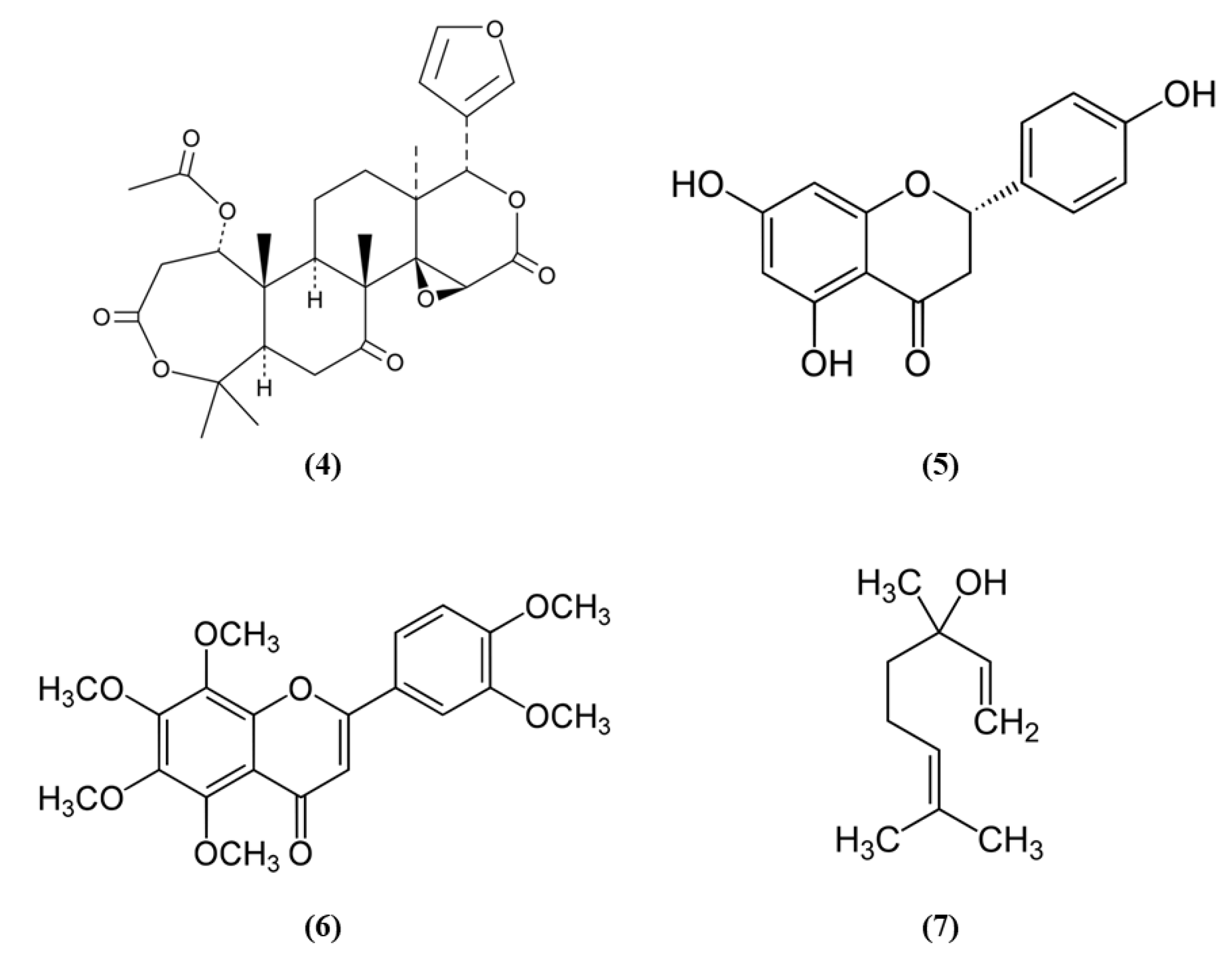
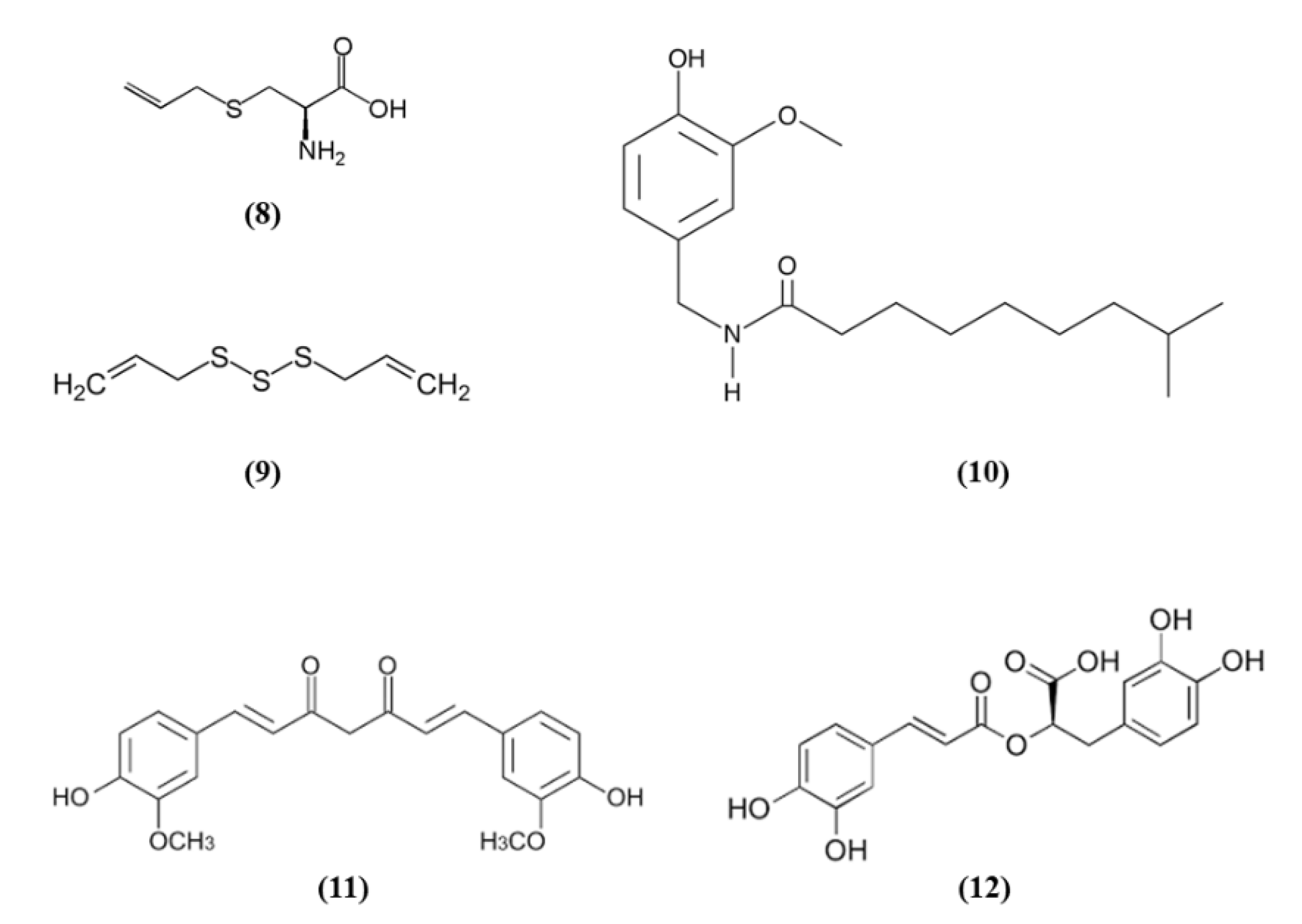
| S-allyl cysteine | Garlic | In vivo: WT and Nrf2−/− mice subjected to tMCAO; In vitro: rat cortical neurons exposed to OGD | In vivo: 300 mg/kg i.p. 30 min before MCAO; In vitro: 10, 25, and 50 µM pre-treated for 2 h before OGD and also after OGD. | In vivo: ↓ infarct volume, JNK, and p38; ↑ neurological score. In vitro: ↓ JNK and p38; ↑ cell viability. | ↑ Nrf2 and downstream antioxidant enzymes | [55] |
| Diallyl trisulfide | Garlic | In vivo: rats subjected to tMCAO | 15 mg/kg, i.p. 4 doses once a day. The first dose 5 min before the onset of reperfusion | ↓ brain damage, infarct volume, oxidative stress, and MMP9; ↑ motor function. | ↑ Nrf2 and downstream antioxidant enzymes | [56] |
| Dihydrocapsaicin | Chili peppers | Rats subjected to tMCAO | 2.5, 5 and 10 mg/kg i.p. 15 min previous cerebral reperfusion | ↓ neurological deficits, infarct area, BBB damage, inflammation, and oxidative stress | ↑ Nrf2 and antioxidant enzymes | [57] |
| Rosmarinic acid | Rosemary and Lamiaceae herbs | Mice subjected to tMCAO | 10, 20, or 40 mg/kg i.p. at reperfusion | ↓ apoptosis, infarct volume, and oxidative stress; ↑ neurological function | ↑ PI3K/Akt ↑ Nrf2 and antioxidant enzymes | [58] |
| Curcumin | Turmeric | Rats subjected to tMCAO | 300 mg/kg i.p. 30 min after occlusion. | ↓ BBB disruption, brain edema, infarct volume, inflammation, and oxidative stress; ↑ neurological function | ↑ Nrf2 | [59] |
| Hexahydrocurcumin | Turmeric | Rats subjected to MCAO | 10, 20, and 40 mg/kg i.p. at reperfusion onset | ↓ infarct volume, apoptosis inflammation, and oxidative stress; ↑ neurological function | ↑ Nrf2 and antioxidant enzymes | [60] |
| Lyciumamide A | Lycium barbarum | In vivo: Rats subjected to tMCAO; In vitro: differentiated SH-SY5Y cells exposed to OGD | In vivo: 40 mg/kg i.p.at the end of MCAO surgery In vitro: 10, 20, 40 µM for 8 h before OGD | In vivo: ↓ infarct volume and oxidative stress; ↑ neurologic function. In vitro: ↓ apoptosis and oxidative stress. | ↑ PKCε/Nrf2/antioxidant enzymes | [62] |
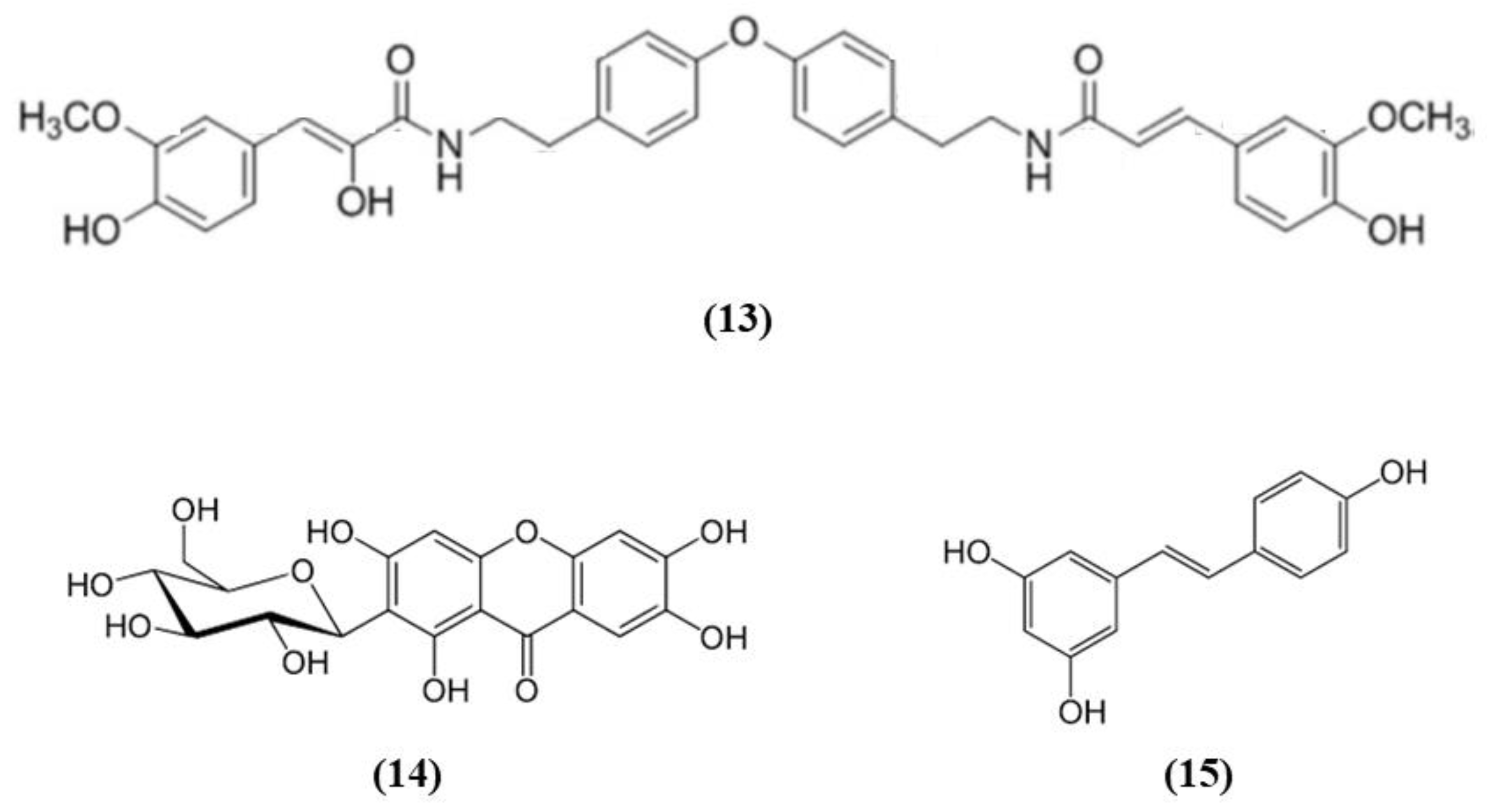
| Mangiferin | Mango and papaya | Rats subjected to tMCAO | 25, 50, and 100 mg/kg i.g. daily for 3 days before the MCAO | ↓ infarct volume, brain edema, inflammation, and oxidative stress; ↑ neurologic function. | ↑ Nrf2 and antioxidant enzymes | [63] |
| Resveratrol | Grape | In vitro: rat astrocytes In vivo: WT and Nrf2−/− rats subjected to tMCAO | In vitro: 25 μmol/L for 2 h In vivo: 10 mg/kg i.p. 48 h before occlusion | In vivo: ↓ infarct volume. In vitro: ↑ antioxidant enzyme. | ↑ Nrf2/NQO1 | [65] |
| Procyanidin B2 | Cocoa, apples, grapes | Rats subjected to tMCAO | To evaluate the effect on infarct size and brain edema: 40, 20, or 10 mg/kg i.g 3 h after MCAO. For BBB permeability and other evaluations: 40 mg/kg i.g. once a day, the first 3 h after MCAO. To evaluate neurological function: 40 mg/kg i.g. daily, the first a day after MCAO. | ↓ infarct volume, brain edema, BBB disruption, and oxidative stress; ↑ neurologic function. | ↑ Nrf2 and downstream antioxidant enzymes | [68] |
| Myricetin | Vegetables, berries, tea, wine | In vivo: Rats subjected to tMCAO; In vitro: SH-SY5Y cells exposed to OGD | In vivo: 20, 10, 5 mg/kg i.g. 2 h before and every day after MCAO. In vitro: 10, 3.3, 1, 0.33, 0.1 nM for 3 h before OGD | In vivo: ↓ infarct volume and oxidative stress; ↑ neurologic function. In vitro: ↓ apoptosis and oxidative stress. | ↑ Nrf2 and antioxidant enzymes | [70] |
| Chlorogenic acid | Coffea species | Rats subjected to I/R (common carotid arteries occlusion) | In vivo: 500, 100, 20 mg/kg orally | ↓ infarct volume, brain edema, apoptosis, and oxidative stress; ↑ neurologic function. | ↑ Nrf2 and antioxidant enzymes | [71] |
| Tocovid | Edible oils | Mice subjected to tMCAO | 200 mg/kg orally daily for 1 month as pre-treatment | ↓ infarct volume, apoptosis, and oxidative stress | ↑ Nrf2 | [73] |
| 3H-1,2-dithiole-3-thione | Cruciferous vegetables | In vivo: WT and Nrf2−/− mice subjected to tMCAO; In vitro: mouse microglial cell line BV2 and primary WT and Nrf2−/− microglia treated with LPS | In vivo: 50 mg/kg i.p. 3 h post reperfusion In vitro: 100 µM | ↓ infarct volume, brain edema, BBB disruption, immune cell infiltration, microglia activation, and oxidative stress; ↑ neurologic function and survival. | ↑ Nrf2/HO-1 | [74] |
| Sulforaphane | Cruciferous vegetables | In vivo: Nrf−/− and WT mice and rats subjected to autologous blood injection In vitro: microglia | In vivo: 5 mg/kg i.p. 30 min and a day after ICH In vitro: 1–10 µM | In vivo: ↑ hematoma clearance; In vitro: ↓ oxidative stress ↑ red blood cell phagocytosis | ↑ Nrf2 | [75] |
| Genistein | Soybeans | Ovariectomized rats subjected to tMCAO | 10 mg/kg i.p. once a day two weeks before MCAO | ↓ infarct volume, neuronal damage, and oxidative stress; ↑ neurologic function. | ↑ Nrf2/NQO1 | [77] |
| Biochanin A | Soybeans | Rats subjected to tMCAO | 10, 20 and 40 mg/kg i.p. for 2 weeks before MCAO | ↓ infarct volume, brain edema, inflammation and oxidative stress; ↑ neurologic function. | ↑ Nrf2 and antioxidant enzymes | [78] |
| Xanthohumol | Humulus lupulus | In vivo: Rats subjected to tMCAO; In vitro: rat primary cortical neurons exposed to OGD. | In vivo: 0.4 mg/kg i.p. 10 min before MCAO In vitro: 0.5 μg/mL for 10 min before OGD | In vivo: ↓ infarct volume, neuronal damage, apoptosis, and oxidative stress; ↑ neurologic function and survival rate. In vitro: ↓ apoptosis and oxidative stress | ↑ Nrf2 and downstream antioxidant enzymes | [79] |
| Alpha-lipoic acid | red meat and vegetables | In vivo: Rats subjected to tMCAO; In vitro: rat cortical neurons exposed to OGD | In vivo: 10, 20, 40, and 80 mg/kg i.v. after reperfusion In vitro: 1, 10 and 100 μM for 1 h before 24 h OGD. | In vivo: ↓ infarct volume, brain edema, and oxidative stress; ↑ neurologic function. In vitro: ↓ oxidative stress; ↑ cell viability | ↑ Nrf2 and antioxidant enzymes | [81] |
| Isoquercetin | medicinal and dietary plants | In vivo: Rats subjected to tMCAO; In vitro: primary culture of rat hippocampal neurons exposed to OGD | In vivo: 5, 10, and 20 mg/kg by gavage after MCAO once a day for 3 days; | In vivo: ↓ infarct volume, brain edema, apoptosis, and oxidative stress; ↑ neurologic function. In vitro: ↓ oxidative stress and apoptosis; ↑ cell viability | ↑ Nrf2 ↓ NOX4/ROS/NF-κB | [83] |
| Corilagin | Phyllanthus emblica | In vivo: Rats subjected to tMCAO; In vitro: rat primary cortical neurons exposed to OGD | In vivo: 30 mg/kg i.p. once a day for a week, the first 3 h after MCAO. In vitro: 10, 25, and 50 µM pretreatment for 2 h before OGD and for other 24 h after OGD | In vivo: ↓ infarct volume, apoptosis, and oxidative stress; ↑ neurologic function and angiogenesis. In vitro: ↑ cell viability | ↑ Nrf2 and antioxidant enzymes | [85] |
| 6″-O-succinylapigenin | In vivo: Rats subjected to tMCAO; In vitro: HT-22 cells exposed to OGD | In vivo: 20, 40, and 60 mg/kg i.p. immediately post occlusion In vitro: 1, 5, or 10 μM 24 h pre-incubation or 5 μM apigenin | In vivo: ↓ infarct volume and oxidative stress; ↑ neurologic function. In vitro: ↑ cell viability | ↑ antioxidant enzymes | [86] | |
| Luteoloside | Artichoke and other plants | Rats subjected to tMCAO | 20, 40, and 80 mg/kg i.p. immediately and 12 h after MCAO | ↓ cerebral edema, infarct volume, and inflammation; ↑ neurologic function. | ↑ Nrf2 | [89] |
| Monascin | red yeast rice | Rats subjected to intracerebral 32 hemorrhage model | 1, 5, and 10 mg/kg/day i.g. 6 h after ICH and twice a day for 1, 3, or 7 days. | ↓ BBB permeability, cerebral edema, and hematoma; ↑ neurologic function. | ↑ Nrf2 | [90] |
| Fucoxanthin | Edible brown seaweeds | In vivo: Rats subjected to tMCAO; In vitro: rat primary cortical neurons exposed to OGD | In vivo: 30, 60, and 90 mg/kg i.g. 1 h before MCAO In vitro: 5, 10 and 20 μM before OGD | In vivo: ↓ infarct volume, brain edema, apoptosis, and oxidative stress; ↑ neurologic function. In vitro: ↓ apoptosis and oxidative stress | ↑ Nrf2 and antioxidant enzymes | [87] |
| Korean red ginseng | Panax ginseng | WT and Nrf2−/− mice subjected to pdMCAO | 100 mg/kg once daily by gavage for 7 days before pdMCAO | ↓ infarct volume, reactive astrogliosis ↑ neurologic function | ↑ downstream antioxidant enzymes | [92] |
| Korean red ginseng | Panax ginseng | WT and Nrf2−/− mice subjected to pdMCAO | 100 mg/kg once a day by gavage for a week before pdMCAO | ↓ infarct volume, reactive astrogliosis, and microgliosis | - | [93] |
| Korean red ginseng | Panax ginseng | WT and Nrf2−/− mice subjected to cerebral hypoxia-ischemia (HI) | 100 mg/kg orally for a week before HI | ↓ neurological deficits, infarct volume, brain edema, inflammation, and reactive gliosis. | ↑ Nrf2 and downstream antioxidant enzymes | [94] |
| Korean red ginseng | Panax ginseng | WT and Nrf2−/− mice subjected to cerebral hypoxia-ischemia (HI) | 100 mg/kg orally for a week before HI | ↓ infarct volume, brain edema, hippocampal CA1 neuronal degeneration, and reactive gliosis. | ↑ downstream antioxidant enzymes | [95] |
| Ginsenoside Rg1 | Panax ginseng | In vitro: pheochromocytoma PC12 cells exposed to OGD; In vivo: rats subjected to tMCAO | In vitro: 0.01, 0.1, 1, and 10 μM after OGD In vivo: 20 mg/kg | In vivo: ↓ infarct volume and oxidative stress. In vitro: ↓ oxidative stress; ↑ cell viability | ↓ miR-144; ↑ Nrf2 and downstream antioxidant enzymes | [96] |
| Xueshuantong | Panax notoginseng | Rats subjected to tMCAO | 25, 50, and 100 mg/kg i.p. 1 h after the onset of reperfusion in MCAO rats and for 3 or 7 days. | ↓ oxidative stress. ↑ neuronal function and angiogenesis | ↑ Nrf2 and downstream antioxidant enzymes | [97] |
| Protocatechualdehyde | Salvia miltiorrhiza | In vivo: Rats subjected to tMCAO; In vitro: differentiated SH-SY5Y cells exposed to OGD | In vivo: 40 mg/kg i.v. 1 h before starting reperfusion In vitro: range 10 to 100 μM for 6 h previous OGD. | In vivo: ↓ infarct volume and oxidative stress. ↑ neurological function. In vitro: ↓ oxidative stress; ↑ cell viability | ↑ PKCε/Nrf2/HO-1 | [100] |
| TanshinoneIIA | Salvia miltiorrhiza | WT and Nrf2−/− mice subjected to tMCAO | 25 mg/kg i.p. 10 min after reperfusion | ↓ infarct volume, apoptosis, and oxidative stress. ↑ neurological function. | ↑ Nrf2 and downstream antioxidant enzymes | [101] |
| Salvianolate lyophilized injection | Salvia miltiorrhiza | Streptozotocin-induced diabetic rats subjected to tMCAO | 5.25, 10.5, and 21 mg/kg i.v. 3 h after tMCAO induction and then daily for 14 days. | ↓ neuronal damage, glucose uptake, and inflammation. | ↑ Nrf2 and downstream antioxidant enzymes | [102] |
| Diterpene ginkgolides meglumine injection | Ginkgo biloba | In vivo: rats subjected to tMCAO In vitro: PC12 cells exposed to OGD | In vivo: 1, 3, and 10 mg/kg i.v. at the start of reperfusion and 12 h after In vitro: 10 µmol/L for each ginkgolide A, B, or C or 1, 10, and 20 µg/mL DGMI for 24 h after OGD | In vivo: ↓ infarct volume and brain edema. ↑ neurological function. In vitro: ↑ cell viability | ↑ Akt/Nrf2 | [104] |
| Ginkgolide A, ginkgolide B, ginkgolide K and bilobalide | Ginkgo biloba | In vivo: rats subjected to tMCAO In vitro: SH-SY5Y cells exposed to OGD | In vivo: 1, 2, and 4 mg/kg i.p. 2 h after reperfusion twice a day. In vitro: 25 mg/L after OGD for 6 h | In vivo: ↓ infarct volume. In vitro: ↓ oxidative stress; ↑ cell viability | ↑ Akt/Nrf2 and antioxidant enzymes | [105] |
| Isorhamnetin | Ginkgo biloba and other plants | Mice subjected to tMCAO | 5 mg/kg i.p. at the starting of reperfusion, and after 24 h | ↓ infarct volume, brain edema, apoptosis, BBB disruption, oxidative stress, and inflammation. ↑ sensimotor function. | ↑ Nrf2/HO-1 | [106] |
| Tetramethylpyrazine | Rhizoma Chuanxiong | Rats subjected to pMCAO | 20 mg/kg i.p. 30 min before and an hour after the occlusion. | ↓ inflammatory cell infiltration, neuronal loss activation of circulating neutrophils | ↑ Nrf2/HO-1 | [108] |
| Z-ligustilide | Rhizoma Chuanxiong | Rats subjected to tMCAO | 15 mg/kg intranasal route for 3 days before MCAO | ↓ infarct volume, brain edema, and BBB disruption. ↑ neurological function. | ↑ NQO1 | [109] |
| Senkyunolide I | Rhizoma Chuanxiong | Rats subjected to tMCAO | 36 and 72 mg/kg i.v. 15 min after MCAO | ↓ infarct volume, brain edema, oxidative stress, and apoptosis. ↑ neurological function. | ↑ Erk1/2 ↑ Nrf2 and antioxidant enzymes | [110] |
| Gastrodin | Gastrodia elata Blume | Mice subjected to tMCAO | 10, 50, and 100 mg/kg i.p. at the starting of cerebral reperfusion | ↓ infarct volume, apoptosis, inflammation, and oxidative stress; ↑ neurologic function. | ↑ Akt/Nrf2 and downstream antioxidant enzymes | [112] |
| Gastrodin | Gastrodia elata Blume | In vivo: Rats subjected to tMCAO; In vitro: C6 astroglial cells treated with Zn2+ | In vivo: 20, 40, and 80 mg/kg i.p. at 1 or 6 h after MCAO In vitro: 50, 100, or 250 μM pretreatment or cotreatment | In vivo: ↓ infarct volume; ↑ neurologic function. In vitro: ↓ oxidative stress; ↑ cell viability | ↑ Nrf2 | [113] |
| Phenolic components of Gastrodia elata Blume | Gastrodia elata Blume | In vivo: rats subjected to tMCAO; In vitro: Primary human astrocytes HA-1800 and SH-SY5Y cells exposed to H2O2 | In vivo: 4 and 40 mg/kg intragastric once per day for a week before MCAO until the sacrifice. In vitro: 15, 25, or 50 μg/mL for 24 h before H2O2 treatment or 25 μg/mL for 1–48 h before H2O2 | In vivo: ↓ pathological lesions; ↑ motor and cognitive function. In vitro: ↑ cell viability | ↑ Nrf2 and downstream antioxidant enzymes | [114] |
| Gastrodin | Gastrodia elata Blume | In vivo: rats subjected to intracerebral hemorrhage model In vitro: rat primary cortical neuron exposed to hemolysate | In vivo: 100 mg/kg i.p. 2 h, a day, and 2 days after surgery In vitro: 10, 100, and 300 µM for 24 h or 100 µM for 0, 12, 24, 48, and 72 h | In vivo: ↓ brain edema, oxidative stress, and apoptosis; ↑ neurological function. In vitro: ↑ cell viability | ↑ Nrf2 and downstream antioxidant enzymes | [115] |
| Schizandrin A | Schisandra chinensis | In vivo: rats subjected to tMCAO; In vitro: differentiated SH-SY5Y cells exposed to OGD | In vivo: 20, 40, and 80 mg/kg i.v. before reperfusion In vitro: range 5 to 100 μM for 6 h pretreatment | In vivo: ↓ infarct volume, inflammation, and oxidative stress; ↑ neurological function. In vitro: ↓ inflammation and oxidative stress ↑ cell viability | ↑ AMPK/Nrf2 and downstream antioxidant enzymes | [117] |
| Salidroside | Rhodiola crenulata | Rats subjected to tMCAO | 15 and 30 mg/kg i.p. once before MCAO and once after reperfusion | ↓ infarct volume and oxidative stress; ↑ neurologic function. | ↑ Nrf2 and downstream antioxidant enzymes | [119] |
| Salidroside | Rhodiola rosea | Rats subjected to pMCAO | 25, 50, and 100 mg/kg i.p. for a week after MCAO | ↓ infarct volume and inflammation; ↑ neurologic function. | ↑ PI3K/PKB/Nrf2/NFκB | [120] |
| Total glycosides | Cistanche deserticola | Rats subjected to tMCAO | 280 mg/kg i.g. daily after MCAO for 2 weeks | ↓ infarct volume and oxidative stress; ↑ neurologic function, BBB integrity, angiogenesis, and neuronal remodeling. | ↑ Nrf2 and downstream antioxidant enzymes | [121] |
| Andrographolide | Andrographis paniculata | In vitro: primary mouse cerebral endothelial cells exposed to OGD In vivo: rats subjected to tMCAO | In vitro: 10 µM for 6 h before OGD In vivo: 0.1 mg/kg, i.p. immediately after MCAO | In vitro: ↓ cell death In vivo: ↓ free radical formation, BBB disruption, and infarct volume. | ↑ p38/Nrf2/HO-1 | [122] |
| Forsythiaside A | Forsythia suspensa | Rats subjected to tMCAO | 50 mg/kg i.p. for a week after MCAO | ↓ apoptosis, endoplasmic reticulum stress, and oxidative stress; ↑ neurologic function, survival rate. | ↑ Nrf2 and downstream antioxidant enzymes | [123] |
| 11-Keto-β-boswellic acid | Boswellia serrata | In vivo: rats subjected to tMCAO; In vitro: rat primary astrocytes exposed to OGD | In vivo: 25 mg/kg i.p. 1 h after reperfusion In vitro: 10, 30, and 50 µM for 24 h after OGD | In vivo: ↓ infarct volume, apoptosis, and oxidative stress. ↑ neurologic function In vitro: ↓ cell death and oxidative stress | ↑ Nrf2 and downstream antioxidant enzymes | [124] |
| Swertiamarin | Gentiana macrophylla Pall | In vivo: mice subjected to tMCAO; In vitro: rat primary hippocampal neurons exposed to OGD | In vivo: 25, 100, and 400 mg/kg i.p. daily for a week before MCAO In vitro: 0.1, 1, and 10 µM for 24 h after OGD | In vivo: ↓ infarct volume, apoptosis, and oxidative stress. ↑ neurologic function In vitro: ↓ cell death and oxidative stress | ↑ Nrf2 and downstream antioxidant enzymes | [125] |
| Neferine | Nelumbo nucifera Gaertn | In vivo: rats subjected to pMCAO; In vitro: PC12 cells exposed to tert-butyl hydroperoxide | In vivo: 12.5, 25, and 50 mg/kg i.g. In vitro: 1–10 µM for 24 h as pre- or post-treatment; | In vivo: ↓ infarct volume, oxidative stress and mitochondrial dysfunction. ↑ neurologic function In vitro: ↓ cell death, mitochondrial dysfunction, and oxidative stress | p62/Keap1/Nrf2 | [126] |
| Totarol | Podocarpus totara | In vivo: rats subjected to tMCAO; In vitro: primary rat cerebellar granule cells and cortical neurons exposed to OGD or glutamate | In vivo: 0.1, 1, and 10 µg/kg i.v. at 2 h, 4 h and 6 h after MCAO In vitro: 5 µM pretreatment for 24 h | In vivo: ↓ infarct volume and oxidative stress. ↑ neurologic function In vitro: ↓ neurotoxicity and oxidative stress | ↑ Akt and downstream antioxidant enzymes | [127] |
| Leonurine | Herba leonuri | WT and Nrf2−/− mice subjected to pMCAO | 5, 10, and 15 mg/kg 2 h i.p. after pMCAO | ↓ infarct volume and oxidative stress. ↑ neurologic function | ↑ Nrf2 and downstream antioxidant enzymes | [128] |
| Britanin | Inula lineariifolia | In vivo: rats subjected to tMCAO In vitro: rat cortical neurons exposed to OGD | In vivo: 25 and 50 mg/kg i.g. at the start of MCAO and dosed twice after reperfusion for 8 h; 25 mg/kg once at 2 h before occlusion, at the onset of occlusion, at reperfusion or 4 h after reperfusion In vitro: 1, 2.5, and 5 µM for 6 h before or after OGD | In vivo: ↓ infarct volume and oxidative stress. ↑ neurologic function In vitro: ↓ neurotoxicity and oxidative stress | ↓ Keap1-mediated ubiquitination of Nrf2 ↑ Nrf2 and downstream antioxidant enzymes | [129] |
| Osthole | Cnidium monnieri | In vivo: Mice subjected to global cerebral ischemia In vitro: HT22 murine hippocampal neuronal cells | In vivo: 25, 50, and 100 mg/kg i.p. 30 min before ischemia and after reperfusion In vitro: 25, 50, and 100 µM for 24 h | In vivo: ↓ BBB disruption and oxidative stress. ↑ cognitive function In vitro: ↑ Nrf2 | ↑ Nrf2 | [130] |
| Trilobatin | Lithocarpus polystachyus | In vivo: Rats subjected to tMCAO; In vitro: Primary rat astrocytes and cortical neurons exposed to OGD | In vivo: 5, 10, and 20 mg/kg by gavage at reperfusion onset twice a day for 3 days; to evaluate the time window: 20 mg/kg at 1, 2, 3, 4, and 6 h after MCAO. To discover the effect of TLB on functional recovery after MCAO: 5, 10, and 20 mg/kg at the onset reperfusion twice daily for 28 days after MCAO In vitro: astrocytes: 12.5, 25, 50 μM for 48 h after OGD. Neurons: 6.25, 12.5, 25, 50 μM for 24 h after OGD. | In vivo: ↓ cerebral edema, infarct volume, inflammation, and oxidative stress. ↑ neurological function In vitro: ↓ oxidative stress and inflammation | ↑ Nrf2 and downstream antioxidant enzymes | [131] |
| Achyranthes bidentata polypeptide k | Achyranthes bidentata Bl. | BV2 cells exposed to LPS | 0.008, 0.04, 0.2, 1, and 5 µg/mL for 30 min before LPS treatment | ↓ inflammation | ↑ Nrf2/HO-1 | [132] |
| Tryptanthrin | P. tinctorium | BV2 cells exposed to LPS | 0.1–20 µM for one hour before LPS treatment | ↓ inflammation | ↑ Nrf2/HO-1 | [133] |
| 5,3′-dihydroxy-3,7,4′-trimethoxyflavone | Siegesbeckia pubescens | Mouse hippocampal HT22 and microglia BV2 cells exposed respectively to glutamate and LPS | 20 µM | ↓ oxidative stress and inflammation | ↑ Nrf2/HO-1 | [134] |
| Longxuetongluo capsule | Dracaena cochinchinensis | BV2 microglial cells exposed to OGD or LPS | 0.5, 1 and 2 µg/mL | ↑ cell viability; ↓ inflammation | ↑ Nrf2/HO-1 | [135] |
| Gualou Guizhi Granule | Composed of 104 compounds | In vivo: Rats subjected to tMCAO; In vitro: PC12 cells exposed H2O2 | In vivo: 3 g/kg i.g. daily for a week after MCAO In vitro: 100, 200, 300 µg/mL for 24 h before H2O2 | In vivo: ↓ oxidative stress In vitro: ↓ oxidative stress | ↑ Nrf2/NQO1 and downstream antioxidant enzymes | [136] |
| Danshensu and hydroxysafflor yellow A (HSYA) | Danshensu: Salvia miltiorrhiza. HSYA: Carthamus tinctorius L. | In vivo: Rats subjected to tMCAO; In vitro: Primary culture of rat cortical neurons exposed to OGD | In vivo: Danshensu group: 15 mg/kg; HSYA group: 6 mg/kg; Danshensu+HSYA group: 7.5 mg/kg Danshensu plus 3 mg/kg HSYA; i.p. In vitro: 80 μM Danshensu, 80 μM HSYA, and 40 μM Danshensu+40 μM HSYA for 24 h after OGD | In vivo: ↓ infarct volume, apoptosis, inflammation, and oxidative stress; ↑ neurological function In vitro: ↑ cell viability | ↑ Nrf2 and downstream antioxidant enzymes | [137] |
| Safflower extract and aceglutamide | safflower extract: Carthamus tinctorius | In vivo: rats subjected to tMCAO; In vitro: differentiated PC12 cells exposed to H2O2 | In vivo: 2.5 mL/kg SAAG; 1.25 g/kg SA; 75 mg/kg AG; i.p. In vitro: 20 µl/mL SAAG; 0.6 mg/mL AG; 10 mg/mL SA; pretreated for 24 h | In vivo: ↓ infarct rate, inflammation, apoptosis, and oxidative stress; ↑ neurologic function. In vitro: ↓ oxidative stress; ↑ cell viability | ↑ Nrf2 and downstream antioxidant enzymes | [138] |
| Salvianolate lyophilized injection and Xueshuantong injection | Salvia miltiorrhiza and Panax notoginsen, respectively | Rats subjected to tMCAO | SLI: 21 mg/kg; XST: 100 mg/kg; combination: 100 mg/kg XST and 21 mg/kg SLI; i.v. 3 h after MCAO and daily for 3 days | ↓ infarct volume, glia activation and oxidative stress; ↑ body weights, neurobehavioral deficits, regional cerebral blood flow | ↑ Nrf2 and downstream antioxidant enzymes | [139] |
| Tao Hong Si Wu decoction | Radix Rehmanniae Praeparata, Radix Angelicae Sinensis, Rhizoma Ligustici Chuanxiong, Radix Paeoniae Alba, Semen Prunus and Flos Carthami Tinctorii | Iv vivo: rats subjected to tMCAO; In vitro: PC12 cells exposed to OGD | In vivo: 0.5, 1, and 1.5 mg/kg for 7 days In vitro: 0.25, 0.5, and 1 mg/mL | In vivo: ↓ infarct volume; ↑ neurologic function. In vitro: ↑ cell viability | ↑ PI3K/Akt/Nrf2 and downstream antioxidant enzymes | [140] |
| Berberine, baicalin and jasminoidin | Huang-Lian-Jie-Du-Decoction | Rats subjected to tMCAO | 20 mg/kg (Berberine 8.6 mg/kg, baicalin 6.8 mg/kg and jasminoidin 4.6 mg/kg) i.g. for 7 days | ↓ infarct volume, oxidative stress, inflammation, and apoptosis; ↑ neurologic function | ↑ Nrf2 and downstream antioxidant enzymes | [141] |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gugliandolo, A.; Bramanti, P.; Mazzon, E. Activation of Nrf2 by Natural Bioactive Compounds: A Promising Approach for Stroke? Int. J. Mol. Sci. 2020, 21, 4875. https://doi.org/10.3390/ijms21144875
Gugliandolo A, Bramanti P, Mazzon E. Activation of Nrf2 by Natural Bioactive Compounds: A Promising Approach for Stroke? International Journal of Molecular Sciences. 2020; 21(14):4875. https://doi.org/10.3390/ijms21144875
Chicago/Turabian StyleGugliandolo, Agnese, Placido Bramanti, and Emanuela Mazzon. 2020. "Activation of Nrf2 by Natural Bioactive Compounds: A Promising Approach for Stroke?" International Journal of Molecular Sciences 21, no. 14: 4875. https://doi.org/10.3390/ijms21144875
APA StyleGugliandolo, A., Bramanti, P., & Mazzon, E. (2020). Activation of Nrf2 by Natural Bioactive Compounds: A Promising Approach for Stroke? International Journal of Molecular Sciences, 21(14), 4875. https://doi.org/10.3390/ijms21144875




