AXIN1 in Plasma or Serum Is a Potential New Biomarker for Endometriosis
Abstract
1. Introduction
2. Results
2.1. Basal Characteristics
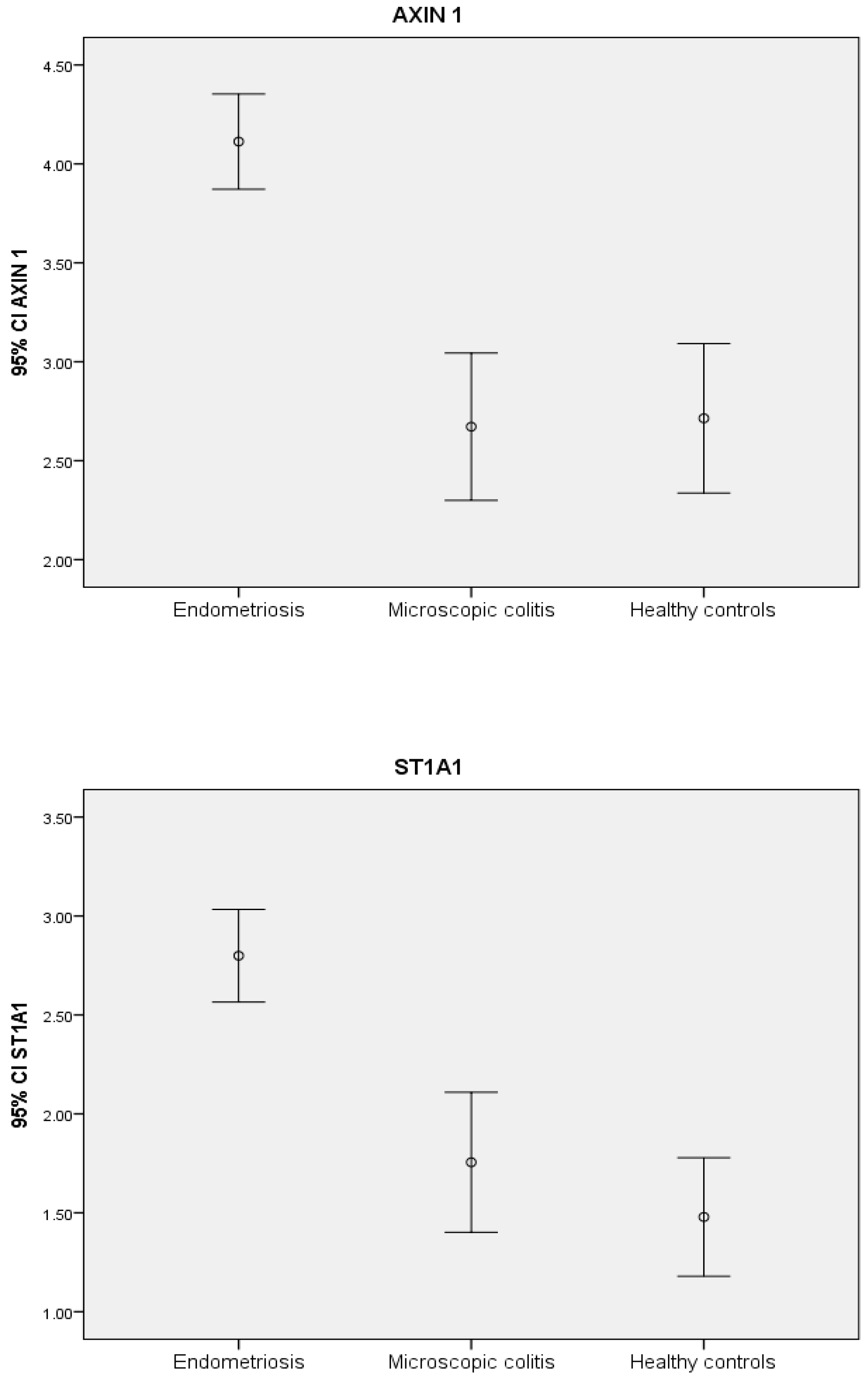
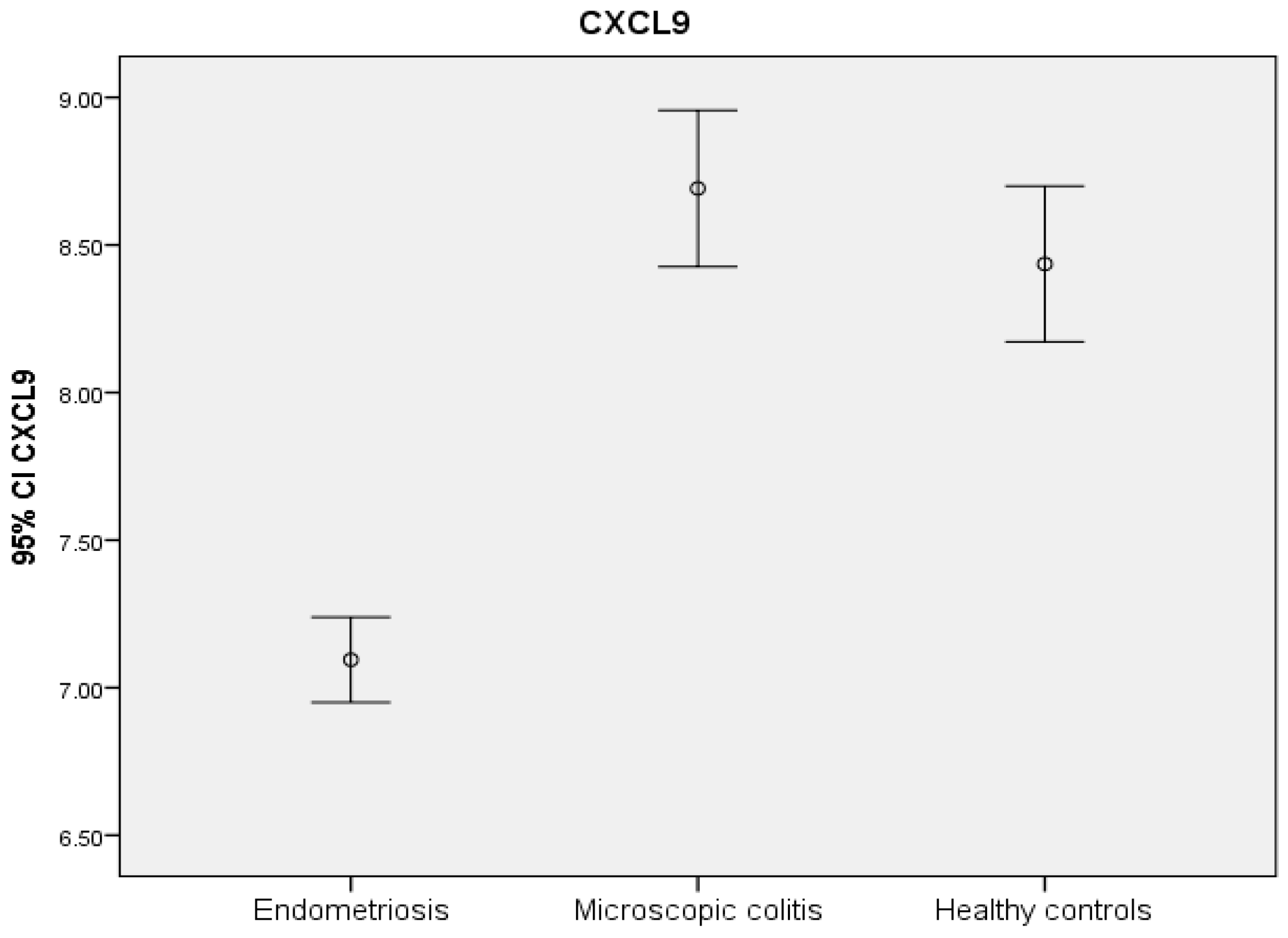
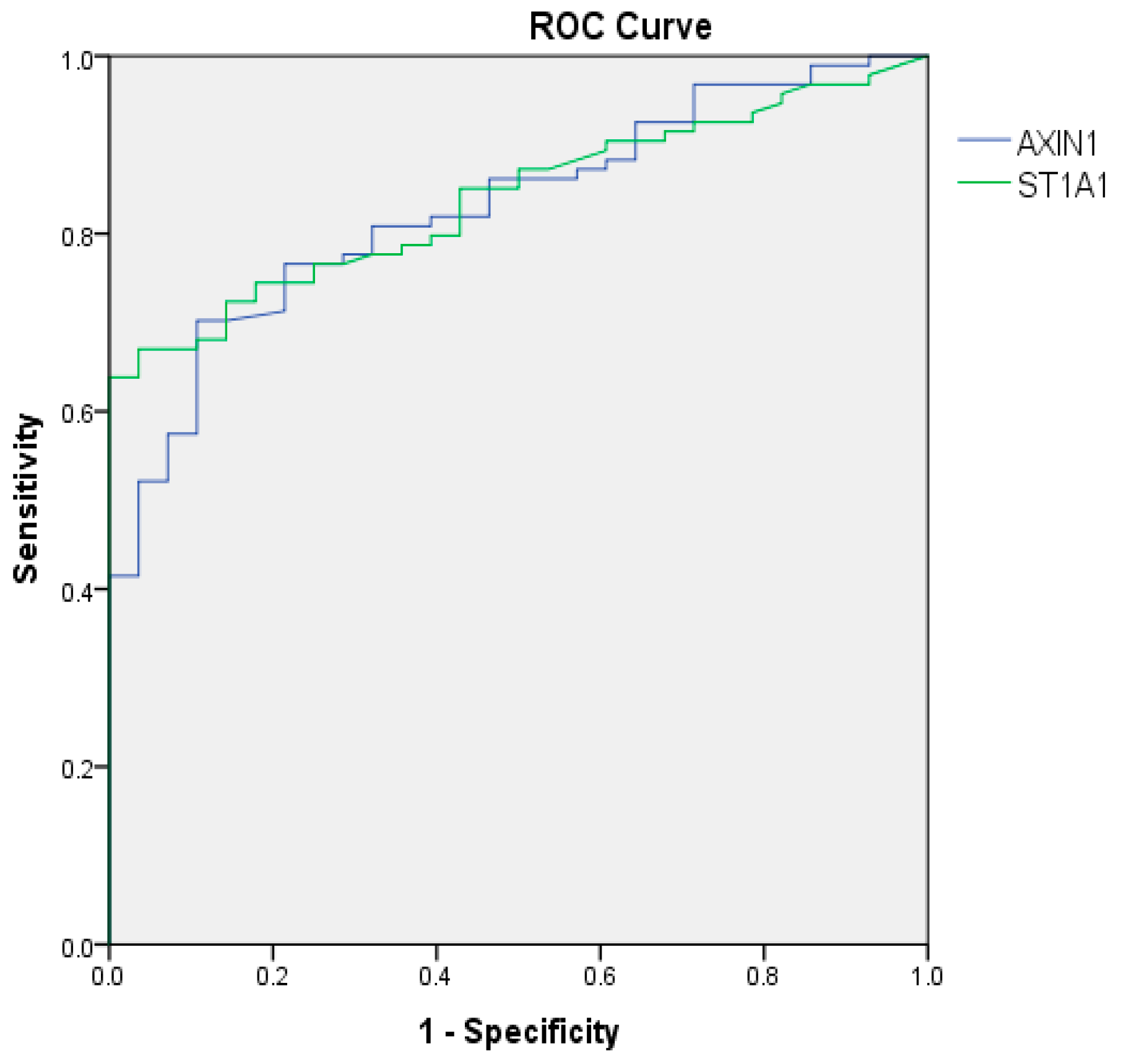
2.2. Protein Expression
2.3. Principal Component Analysis of Protein Expression
2.4. Gastrointestinal Symptoms and Protein Expression
3. Discussion
4. Methods
4.1. Patients
4.2. Controls
4.3. Study Design
4.4. The Visual Analogue Scale for Irritable Bowel Syndrome
4.5. Analytical Methods
4.6. Statistical Methods
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgements
Conflicts of Interest
References
- Giudice, L.C.; Kao, L.C. Endometriosis. Lancet 2004, 364, 1789–1799. [Google Scholar] [CrossRef]
- Nnoaham, K.E.; Hummelshoj, L.; Webster, P.; d’Hooghe, T.; de Cicco Nardone, F.; de Cicco Nardone, C.; Jenkinson, C.; Kennedy, S.H.; Zondervan, K.T. Impact of endometriosis on quality of life and work productivity: A multicenter study across ten countries. Fertil. Steril. 2011, 96, 366–373. [Google Scholar] [CrossRef]
- Fassbender, A.; Burney, R.O.; O, D.F.; D’Hooghe, T.; Giudice, L. Update on biomarkers for the detection of endometriosis. BioMed Res. Int. 2015, 2015, 130854. [Google Scholar] [CrossRef] [PubMed]
- Nisenblat, V.; Bossuyt, P.M.; Shaikh, R.; Farquhar, C.; Jordan, V.; Scheffers, C.S.; Mol, B.W.; Johnson, N.; Hull, M.L. Blood biomarkers for the non-invasive diagnosis of endometriosis. Cochrane Database Syst. Rev. 2016. [Google Scholar] [CrossRef] [PubMed]
- Halme, J.; Hammond, M.G.; Hulka, J.F.; Raj, S.G.; Talbert, L.M. Retrograde menstruation in healthy women and in patients with endometriosis. Obstet. Gynecol. 1984, 64, 151–154. [Google Scholar] [PubMed]
- Ahn, S.H.; Monsanto, S.P.; Miller, C.; Singh, S.S.; Thomas, R.; Tayade, C. Pathophysiology and immune dysfunction in endometriosis. BioMed Res. Int. 2015, 2015, 795976. [Google Scholar] [CrossRef]
- Roman, H.; Ness, J.; Suciu, N.; Bridoux, V.; Gourcerol, G.; Leroi, A.M.; Tuech, J.J.; Ducrotte, P.; Savoye-Collet, C.; Savoye, G. Are digestive symptoms in women presenting with pelvic endometriosis specific to lesion localizations? A preliminary prospective study. Hum. Reprod. 2012, 27, 3440–3449. [Google Scholar] [CrossRef]
- Seaman, H.E.; Ballard, K.D.; Wright, J.T.; de Vries, C.S. Endometriosis and its coexistence with irritable bowel syndrome and pelvic inflammatory disease: Findings from a national case-control study—Part 2. BJOG 2008, 115, 1392–1396. [Google Scholar] [CrossRef]
- Issa, B.; Onon, T.S.; Agrawal, A.; Shekhar, C.; Morris, J.; Hamdy, S.; Whorwell, P.J. Visceral hypersensitivity in endometriosis: A new target for treatment? Gut 2012, 61, 367–372. [Google Scholar] [CrossRef]
- Bellini, M.; Gambaccini, D.; Stasi, C.; Urbano, M.T.; Marchi, S.; Usai-Satta, P. Irritable bowel syndrome: A disease still searching for pathogenesis, diagnosis and therapy. World J. Gastroenterol. 2014, 20, 8807–8820. [Google Scholar] [CrossRef]
- Kikuchi, A. Roles of Axin in the Wnt signalling pathway. Cell. Signal. 1999, 11, 777–788. [Google Scholar] [CrossRef]
- Zhang, L.; Xiong, W.; Xiong, Y.; Liu, H.; Liu, Y. 17 beta-Estradiol promotes vascular endothelial growth factor expression via the Wnt/beta-catenin pathway during the pathogenesis of endometriosis. Mol. Hum. Reprod. 2016, 22, 526–535. [Google Scholar] [CrossRef] [PubMed]
- Matsuzaki, S.; Botchorishvili, R.; Pouly, J.L.; Canis, M. Targeting the Wnt/beta-catenin pathway in endometriosis: A potentially effective approach for treatment and prevention. Mol. Cell. Ther. 2014, 2, 36. [Google Scholar] [CrossRef]
- Gamage, N.U.; Tsvetanov, S.; Duggleby, R.G.; McManus, M.E.; Martin, J.L. The structure of human SULT1A1 crystallized with estradiol. An insight into active site plasticity and substrate inhibition with multi-ring substrates. J. Biol. Chem. 2005, 280, 41482–41486. [Google Scholar] [CrossRef] [PubMed]
- Hemmerich, S. Carbohydrate sulfotransferases: Novel therapeutic targets for inflammation, viral infection and cancer. Drug Discov. Today 2001, 6, 27–35. [Google Scholar] [CrossRef]
- Rizner, T.L. The Important Roles of Steroid Sulfatase and Sulfotransferases in Gynecological Diseases. Front. Pharmacol. 2016, 7, 30. [Google Scholar] [CrossRef] [PubMed]
- Borrelli, G.M.; Abrao, M.S.; Mechsner, S. Can chemokines be used as biomarkers for endometriosis? A systematic review. Hum. Reprod. 2014, 29, 253–266. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.H.; Farber, J.M. Localization of the gene for the human MIG cytokine on chromosome 4q21 adjacent to INP10 reveals a chemokine “mini-cluster”. Cytogenet. Cell. Genet. 1996, 74, 255–258. [Google Scholar] [CrossRef]
- Galleri, L.; Luisi, S.; Rotondi, M.; Romagnani, P.; Cobellis, L.; Serio, M.; Petraglia, F. Low serum and peritoneal fluid concentration of interferon-gamma-induced protein-10 (CXCL10) in women with endometriosis. Fertil. Steril. 2009, 91, 331–334. [Google Scholar] [CrossRef]
- Malutan, A.M.; Drugan, T.; Ciortea, R.; Bucuri, C.; Rada, M.P.; Mihu, D. Endometriosis-associated changes in serum levels of interferons and chemokines. Turk. J. Med. Sci. 2017, 47, 115–122. [Google Scholar] [CrossRef]
- Chung, H.W.; Wen, Y.; Chun, S.H.; Nezhat, C.; Woo, B.H.; Lake Polan, M. Matrix metalloproteinase-9 and tissue inhibitor of metalloproteinase-3 mRNA expression in ectopic and eutopic endometrium in women with endometriosis: A rationale for endometriotic invasiveness. Fertil. Steril. 2001, 75, 152–159. [Google Scholar] [CrossRef]
- Liu, H.; Wang, J.; Wang, H.; Tang, N.; Li, Y.; Zhang, Y.; Hao, T. The plasma and peritoneal fluid concentrations of matrix metalloproteinase-9 are elevated in patients with endometriosis. Ann. Clin. Biochem. 2016, 53, 599–605. [Google Scholar] [CrossRef] [PubMed]
- Van den Steen, P.E.; Husson, S.J.; Proost, P.; Van Damme, J.; Opdenakker, G. Carboxyterminal cleavage of the chemokines MIG and IP-10 by gelatinase B and neutrophil collagenase. Biochem. Biophys. Res. Commun. 2003, 310, 889–896. [Google Scholar] [CrossRef] [PubMed]
- Gomez-Lechon, M.J. Oncostatin M: Signal transduction and biological activity. Life Sci. 1999, 65, 2019–2030. [Google Scholar] [CrossRef]
- Beigel, F.; Friedrich, M.; Probst, C.; Sotlar, K.; Goke, B.; Diegelmann, J.; Brand, S. Oncostatin M mediates STAT3-dependent intestinal epithelial restitution via increased cell proliferation, decreased apoptosis and upregulation of SERPIN family members. PLoS ONE 2014, 9, e93498. [Google Scholar] [CrossRef] [PubMed]
- West, N.R.; Hegazy, A.N.; Owens, B.M.J.; Bullers, S.J.; Linggi, B.; Buonocore, S.; Coccia, M.; Gortz, D.; This, S.; Stockenhuber, K.; et al. Oncostatin M drives intestinal inflammation and predicts response to tumor necrosis factor-neutralizing therapy in patients with inflammatory bowel disease. Nat. Med. 2017, 23, 579–589. [Google Scholar] [CrossRef] [PubMed]
- Deshmane, S.L.; Kremlev, S.; Amini, S.; Sawaya, B.E. Monocyte chemoattractant protein-1 (MCP-1): An overview. J. Interferon Cytokine Res. 2009, 29, 313–326. [Google Scholar] [CrossRef]
- Young, V.J.; Brown, J.K.; Saunders, P.T.; Horne, A.W. The role of the peritoneum in the pathogenesis of endometriosis. Hum. Reprod. Update 2013, 19, 558–569. [Google Scholar] [CrossRef]
- Tulubas, F.; Oran, M.; Mete, R.; Turan, F.; Yilmaz, A.; Yildiz, Z.D.; Gurel, A. Investigation of serum macrophage migration inhibitor factor and monocyte chemotactic protein-1 levels in irritable bowel syndrome. Turk. J. Med. Sci. 2014, 44, 967–971. [Google Scholar] [CrossRef]
- Darkoh, C.; Comer, L.; Zewdie, G.; Harold, S.; Snyder, N.; Dupont, H.L. Chemotactic chemokines are important in the pathogenesis of irritable bowel syndrome. PLoS ONE 2014, 9, e93144. [Google Scholar] [CrossRef]
- Ahn, SH.; Singh, V.; Tayade, C. Biomarkers in endometriosis: Challenges and opportunities. Fertil. Steril. 2017, 107, 523–532. [Google Scholar] [CrossRef] [PubMed]
- Ferlita, A.; Battaglia, R.; Andronico, F.; Caruso, S.; Cianci, A.; Purello, M.; Pietro, C.D. Non-coding RNAs in endometrial pathophysiology. Int. J. Mol. Sci. 2018, 19, 2120. [Google Scholar] [CrossRef] [PubMed]
- Cioffi, M.; Esposito, K.; Vietri, M.T.; Gazzerro, P.; D’Auria, A.; Ardovino, I.; Puca, G.A.; Molinari, A.M. Cytokine pattern in postmenopause. Maturitas 2002, 41, 187–192. [Google Scholar] [CrossRef]
- Kim, O.Y.; Chae, J.S.; Paik, J.K.; Seo, H.S.; Jang, Y.; Cavaillon, J.M.; Lee, J.H. Effects of aging and menopause on serum interleukin-6 levels and peripheral blood mononuclear cell cytokine production in healthy nonobese women. Age 2012, 34, 415–425. [Google Scholar] [CrossRef] [PubMed]
- Grandi, G.; Xholli, A.; Napolitano, A.; Palma, F.; Cagnacci, A. Pelvic pain and quality of life of women with endometriosis during quadriphasic estradiol valerate/dienogest oral contraceprive: A patient-preference prospective 24-week pilot study. Reprod. Sci. 2015, 22, 626–632. [Google Scholar] [CrossRef] [PubMed]
- Caruso, S.; Iraci, M.; Cianci, S.; Fava, V.; Casella, E.; Cianci, A. Comparative, open-label prospective study on the quality of life and sexual function of women affected by endometriosis-associated pelvic pain on 2 mg dienogest/30 µg ethinyl estradiol continuous or 21/7 regimen oral contraceptive. J. Endocrinol. Invest. 2016, 39, 923–931. [Google Scholar] [CrossRef] [PubMed]
- Koh, K.K.; Yoon, B.K. Controversies regarding hormone therapy: Insights from inflammation and hemostasis. Cardiovasc. Res. 2006, 70, 22–30. [Google Scholar] [CrossRef]
- Roth, B.; Gustafsson, R.J.; Ohlsson, B. Auto-antibodies and their association with clinical findings in women diagnosed with microscopic colitis. PLoS ONE 2013, 8, e66088. [Google Scholar] [CrossRef]
- Berglund, G.; Elmstahl, S.; Janzon, L.; Larsson, S.A. The malmo diet and cancer study. Design and feasibility. J. Intern. Med. 1993, 233, 45–51. [Google Scholar] [CrossRef]
- Ohlsson, B.; Orho-Melander, M.; Nilsson, P.M. Higher levels of serum zonulin may rather be associated with increased risk of obesity and hyperlipidemia, than with gastrointestinal symptoms or disease manifestations. Int. J. Mol. Sci. 2017, 18. [Google Scholar] [CrossRef]
- Bengtsson, M.; Ohlsson, B.; Ulander, K. Development and psychometric testing of the visual analogue scale for irritable bowel syndrome (VAS-IBS). BMC Gastroenterol. 2007, 7, 16. [Google Scholar] [CrossRef] [PubMed]
- Assarsson, E.; Lundberg, M.; Holmquist, G.; Bjorkesten, J.; Thorsen, S.B.; Ekman, D.; Eriksson, A.; Rennel Dickens, E.; Ohlsson, S.; Edfeldt, G.; et al. Homogenous 96-plex PEA immunoassay exhibiting high sensitivity, specificity, and excellent scalability. PLoS ONE 2014, 9, e95192. [Google Scholar] [CrossRef] [PubMed]
- Lundberg, M.; Eriksson, A.; Tran, B.; Assarsson, E.; Fredriksson, S. Homogeneous antibody-based proximity extension assays provide sensitive and specific detection of low-abundant proteins in human blood. Nucleic Acids Res. 2011, 39, e102. [Google Scholar] [CrossRef] [PubMed]
- Olink Proteomics. Data Validation. Available online: https://www.olink.com/data-you-can-trust/validation (accessed on 30 October 2017).
| Characteristics | Endo | MC | HC | p-Value | p-Value |
|---|---|---|---|---|---|
| N = 94 | N = 47 | N = 28 | Endo vs. MC | Endo vs. HC | |
| Age (years) | 36.7 ± 7.4 | 59.4 ± 9.9 | 64.1 ± 5.5 | <0.001 | <0.001 |
| BMI (kg/m2) | 24.0 (21.8–26.2) | 23.9 (21.8–27.8) | 24.1 (20.8–25.7) | 0.718 | 0.490 |
| Smoking (n, %) | 14 (14.9) | 24 (51.1) | 6 (21.4) | <0.001 | 0.562 |
| Protein | Absolute Value | Absolute Value | Absolute Value | p-Value | p-Value |
|---|---|---|---|---|---|
| Endometriosis | MC | HC | Endometriosis vs. MC | Endometriosis vs. HC | |
| N = 94 | N = 47 | N = 28 | |||
| AXIN1 | 4.1 ± 1.2 | 2.7 ± 1.3 | 2.7 ± 1.0 | <0.001 | 0.001 |
| ST1A1 | 2.8 ± 1.1 | 1.8 ± 1.2 | 1.5 ± 0.8 | 0.001 | 0.010 |
| CXCL9 | 7.1 ± 0.7 | 8.7 ± 0.9 | 8.4 ± 0.7 | <0.001 | <0.001 |
| CD40 | 9.4 ± 0.6 | 9.2 ± 0.4 | 9.1 ± 0.4 | 0.007 | 0.020 |
| SIRT2 | 6.2 ± 1.4 | 4.9 ± 1.2 | 4.9 ± 1.1 | 0.001 | 0.018 |
| CD244 | 6.0 ± 0.4 | 5.8 ± 0.4 | 5.8 ± 0.4 | 0.002 | 0.131 |
| STAMBP | 4.6 ± 1.2 | 3.7 ± 0.9 | 3.7 ± 1.0 | 0.001 | 0.041 |
| NT3 | 1.9 ± 0.5 | 1.4 ± 0.3 | 1.6 ± 0.6 | 0.001 | 0.226 |
| MCP-1 | 8.6 ± 0.4 | 9.2 ± 0.6 | 9.1 ± 0.3 | 0.003 | 0.021 |
| MMP-10 | 8.6 ± 0.7 | 9.5 ± 0.9 | 9.2 ± 0.6 | 0.010 | 0.335 |
| CCL11 | 7.3 ± 0.4 | 8.3 ± 0.5 | 8.3 ± 0.5 | <0.001 | 0.030 |
| TGF-α | 0.8 ± 0.3 | 1.0 ± 0.2 | 0.9 ± 0.3 | <0.001 | 0.016 |
| OPG | 9.7 ±0.4 | 10.1 ± 0.5 | 10.0 ± 0.3 | 0.015 | 0.004 |
| CDCP1 | 2.0 ± 0.4 | 2.9 ± 0.7 | 3.0 ± 0.5 | 0.047 | 0.008 |
| Flt3l | 8.7 ± 0.4 | 9.2 ± 0.5 | 9.1 ± 0.5 | 0.023 | 0.055 |
| CXCL10 | 8.4 ± 0.9 | 9.3 ± 0.8 | 9.6 ± 1.0 | 0.041 | 0.015 |
| IL-18R1 | 7.2 ± 0.5 | 7.3 ± 0.6 | 7.3 ± 0.5 | 0.437 | 0.038 |
| HGF | 6.6 ± 0.4 | 7.1 ± 0.4 | 6.9 ± 0.4 | 0.017 | 0.740 |
| TNFRSF9 | 5.8 ± 0.4 | 6.3 ± 0.6 | 6.1 ± 0.5 | 0.013 | 0.338 |
| IL-10 | 3.5 ± 0.6 | 4.0 ± 0.6 | 3.8 ± 0.7 | 0.036 | 0.702 |
| IL-7 | 3.1 ± 0.8 | 3.1 ± 0.7 | 3.0 ± 0.7 | 0.047 | 0.047 |
| TNFSF14 | 2.5 ± 0.6 | 2.6 ± 0.4 | 2.3 ± 0.4 | 0.819 | 0.038 |
| EN-RAGE | 2.3 ± 1.1 | 1.9 ± 0.8 | 1.8 ± 0.5 | 0.017 | 0.013 |
| PCA Factors | Endo | MC | HC | p-Value | p-Value |
|---|---|---|---|---|---|
| N = 94 | N = 47 | N = 28 | Endo vs. MC | Endo vs. HC | |
| Factor 1 | −0.14 ± 0.61 | 0.35 ± 0.57 | 0.25 ± 0.49 | 0.381 | 0.777 |
| Factor 2 | 0.52 ± 0.92 | −0.63 ± 0.73 | −0.69 ± 0.57 | <0.001 | 0.001 |
| Factor 3 | −0.45 ± 0.72 | 0.60 ± 0.78 | 0.31 ± 0.66 | 0.068 | 0.966 |
| Factor 4 | 0.27 ± 0.84 | −0.39 ± 1.11 | −0.31 ± 0.99 | 0.372 | 0.931 |
| Protein | Abdominal Pain | Diarrhea | Constipation | Bloating and Flatulence | Vomiting and Nausea |
|---|---|---|---|---|---|
| OSM | r = 0.182, p = 0.083 | r = 0.235, p = 0.024 | r = 0.268, p = 0.010 | r = 0.238, p = 0.022 | |
| MCP1 | r = 0.291, p = 0.005 | ||||
| TNFRSF9 | r = 0.280, p = 0.007 | ||||
| CCL 11 | r = 0.215, p = 0.039 | ||||
| MMP10 | r = -0.229, p = 0.028 | ||||
| EN-RAGE | r = -0.228, p = 0.029 | ||||
| IL 5 | r = 0.237, p = 0.023 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ek, M.; Roth, B.; Engström, G.; Ohlsson, B. AXIN1 in Plasma or Serum Is a Potential New Biomarker for Endometriosis. Int. J. Mol. Sci. 2019, 20, 189. https://doi.org/10.3390/ijms20010189
Ek M, Roth B, Engström G, Ohlsson B. AXIN1 in Plasma or Serum Is a Potential New Biomarker for Endometriosis. International Journal of Molecular Sciences. 2019; 20(1):189. https://doi.org/10.3390/ijms20010189
Chicago/Turabian StyleEk, Malin, Bodil Roth, Gunnar Engström, and Bodil Ohlsson. 2019. "AXIN1 in Plasma or Serum Is a Potential New Biomarker for Endometriosis" International Journal of Molecular Sciences 20, no. 1: 189. https://doi.org/10.3390/ijms20010189
APA StyleEk, M., Roth, B., Engström, G., & Ohlsson, B. (2019). AXIN1 in Plasma or Serum Is a Potential New Biomarker for Endometriosis. International Journal of Molecular Sciences, 20(1), 189. https://doi.org/10.3390/ijms20010189






