Sesamin: A Promising Therapeutic Agent for Ameliorating Symptoms of Diabetes
Abstract
:1. Introduction
2. Results
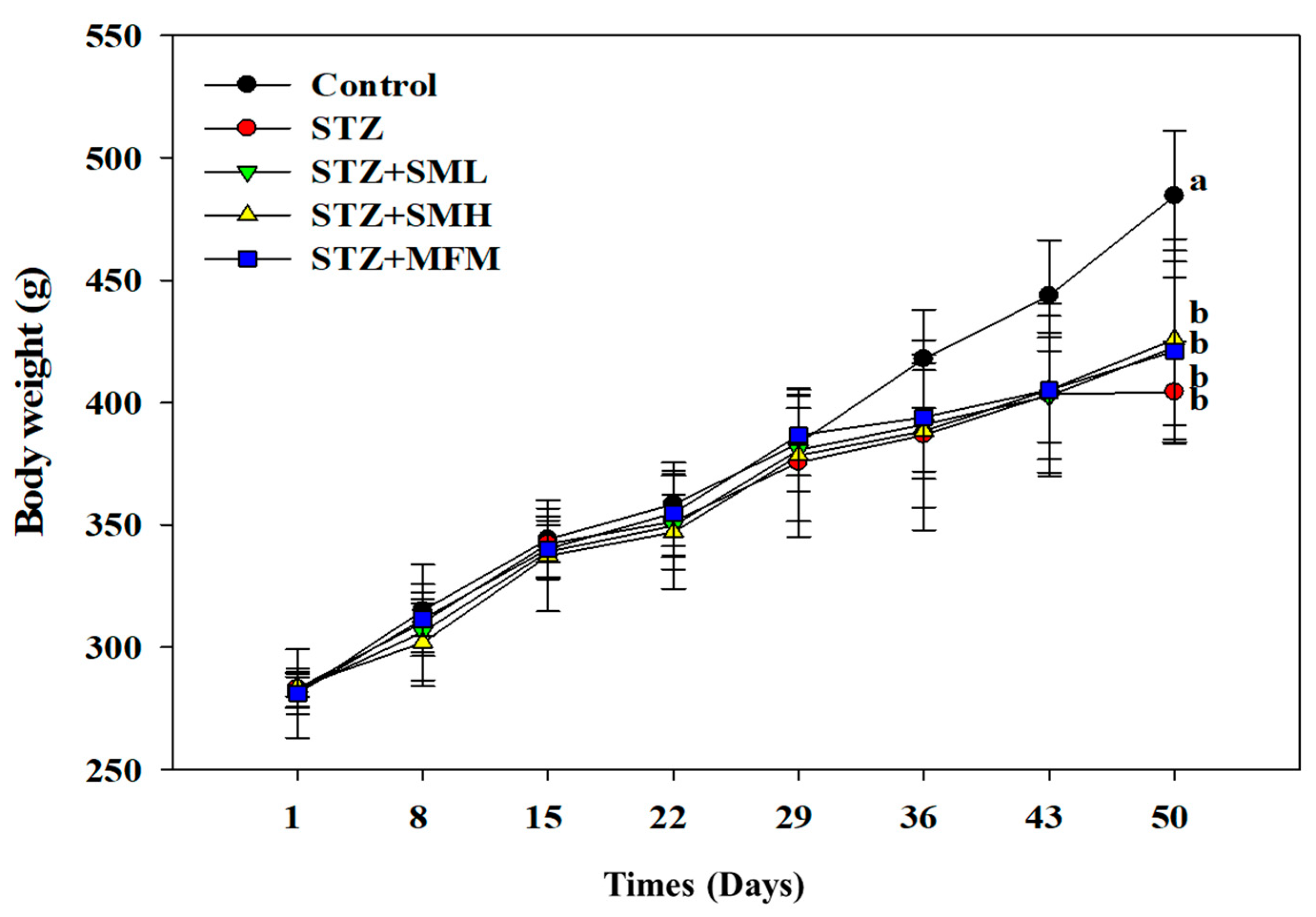
2.1. The Effect of Sesamin on the Body Weight of STZ-Induced Type 2 Diabetic Rats
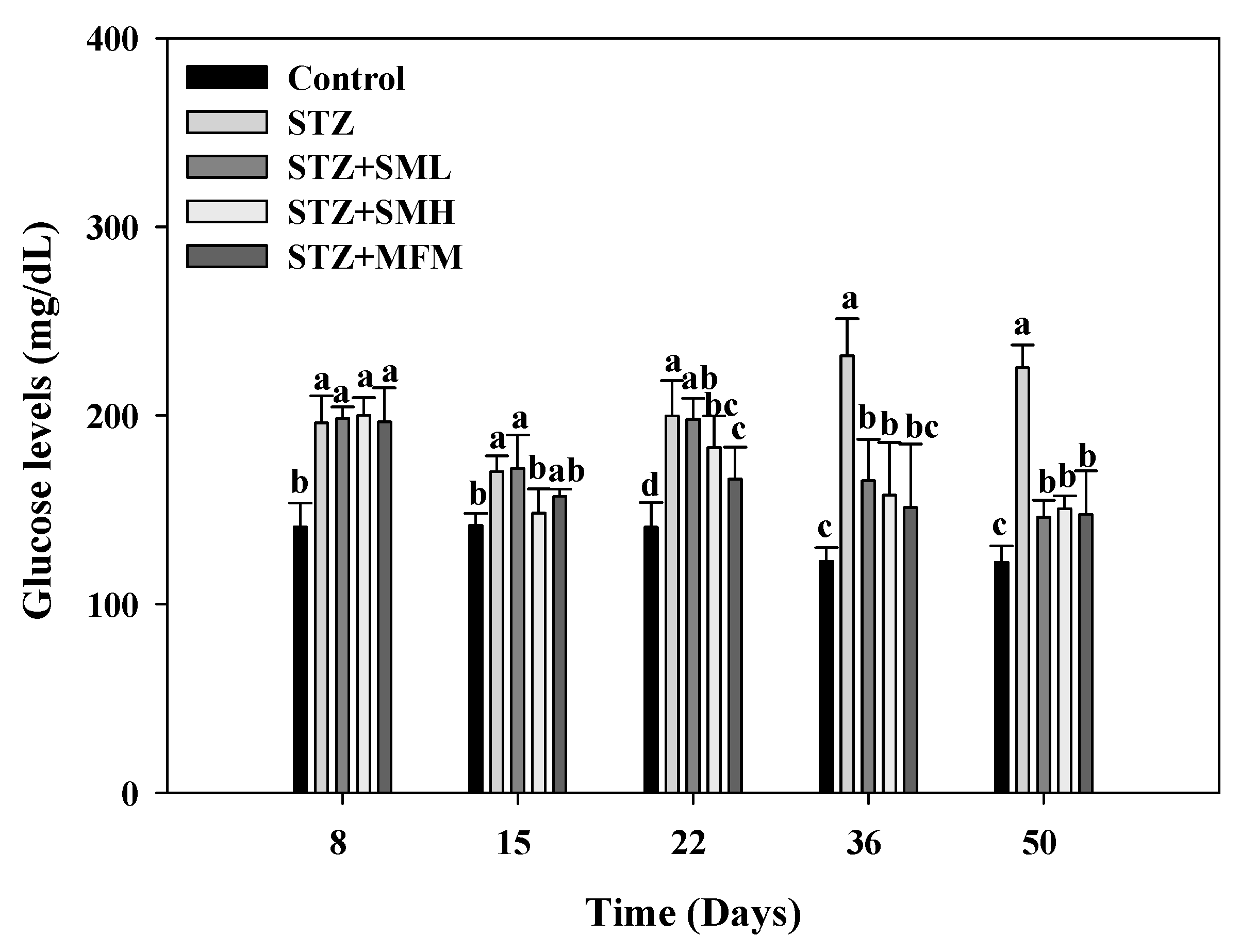
2.2. The Effect of Sesamin on the Blood Sugar Level in STZ-Induced Type 2 Diabetic Rats
2.3. The Effect of Sesamin on the Glycosylated Hemoglobin in STZ-Induced Type 2 Diabetic Rats
2.4. The Effect of Sesamin on Insulin Levels in STZ-Induced Type 2 Diabetic Rats
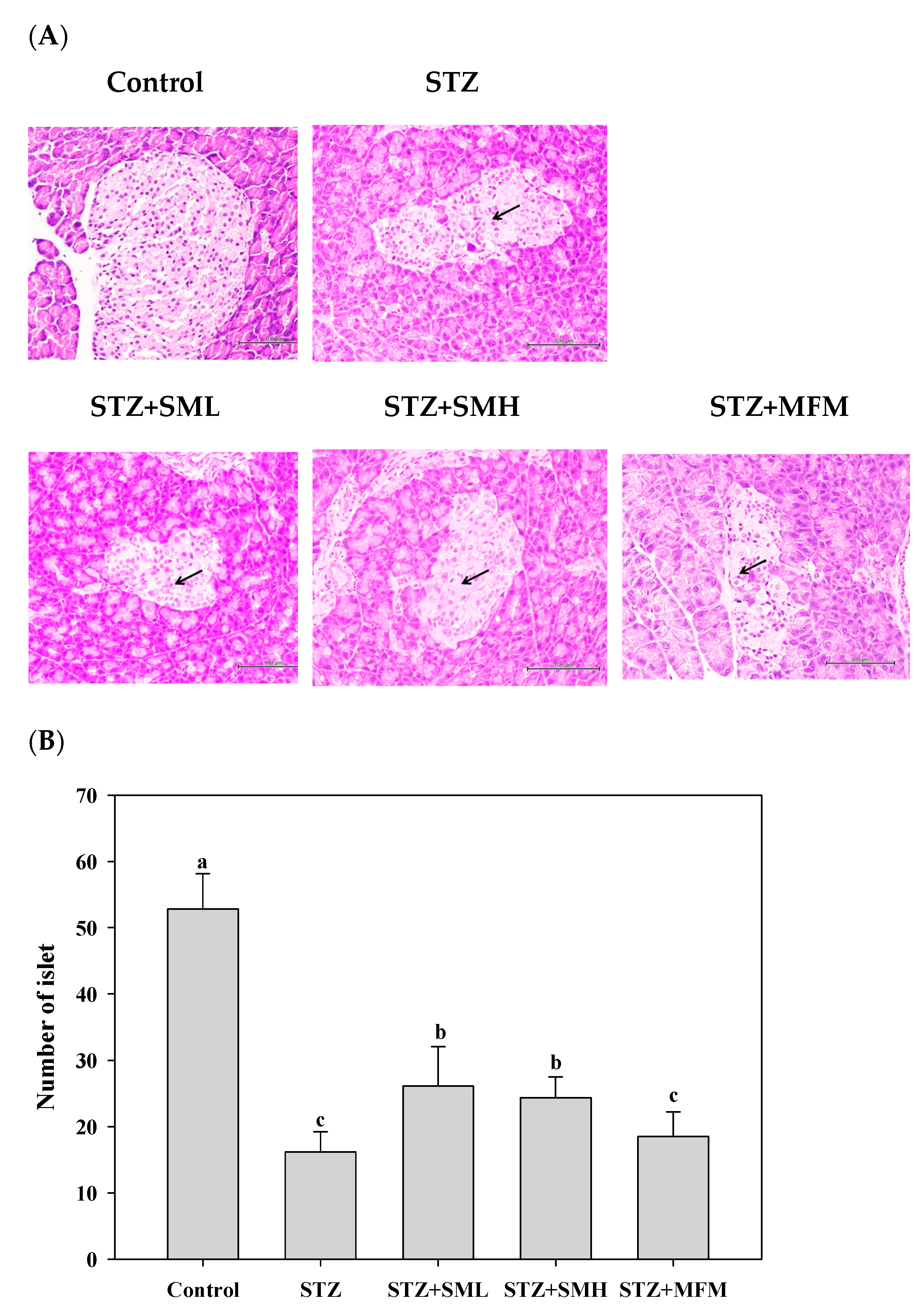
2.5. The Effect of Sesamin on the Pancreas of STZ-Induced Type 2 Diabetic Rats
2.6. The Effect of Sesamin on Serum Biochemical Values of STZ-Induced Type 2 Diabetic Rats
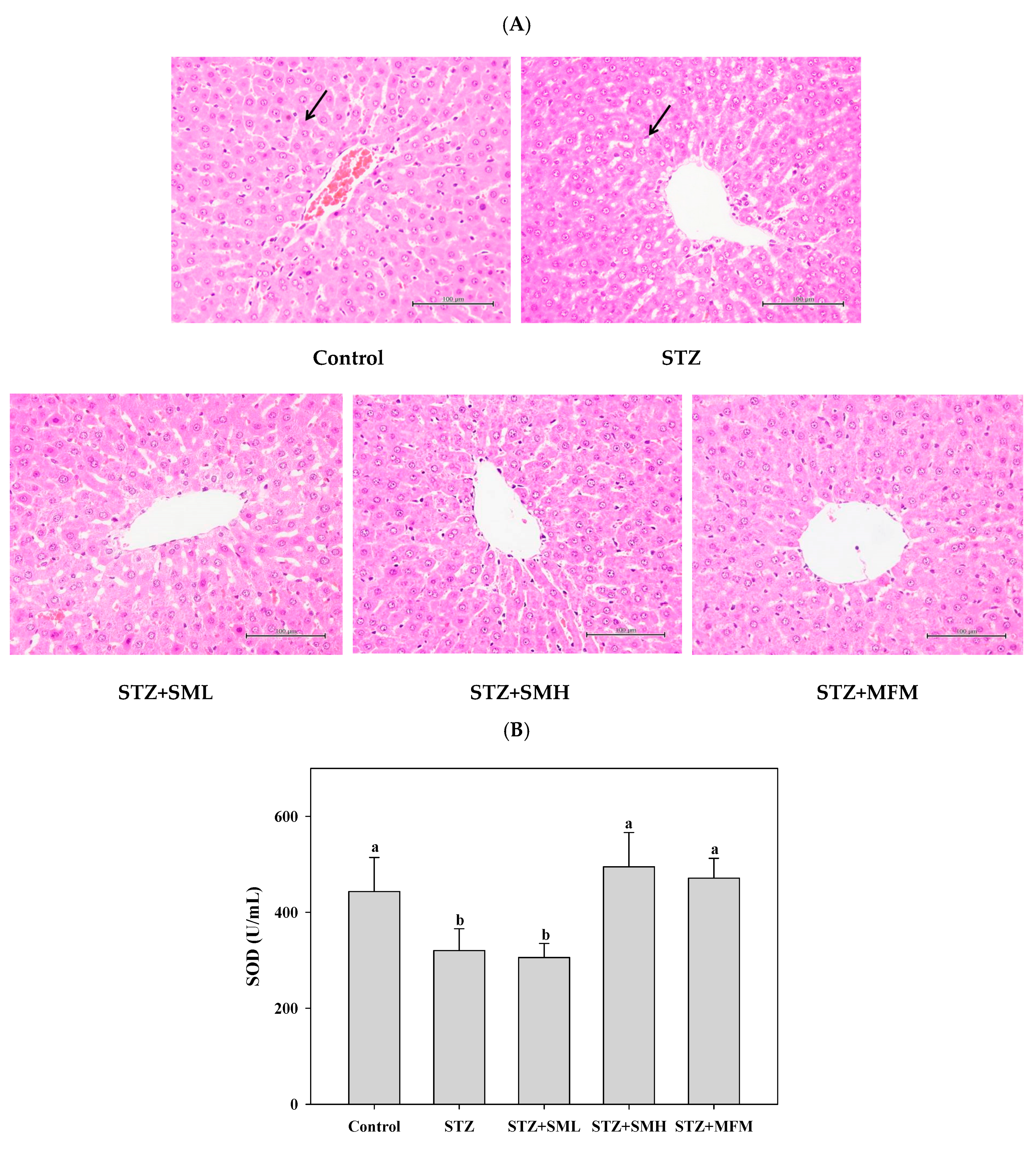
2.7. The Effect of Sesamin on the Liver of STZ-Induced Type 2 Diabetic Rats
3. Discussion
4. Materials and Methods
4.1. Animal Experiment and the Effect of Sesamin on the Body Weight
4.2. Blood Glucose Monitoring
4.3. Detection of Glycosylated Hemoglobin (HbA1c)
4.4. Determination of Serum Insulin Concentration
4.5. Determination of Plasma Triglycerides, Cholesterol, Amylase, HDL, ALT, and AST
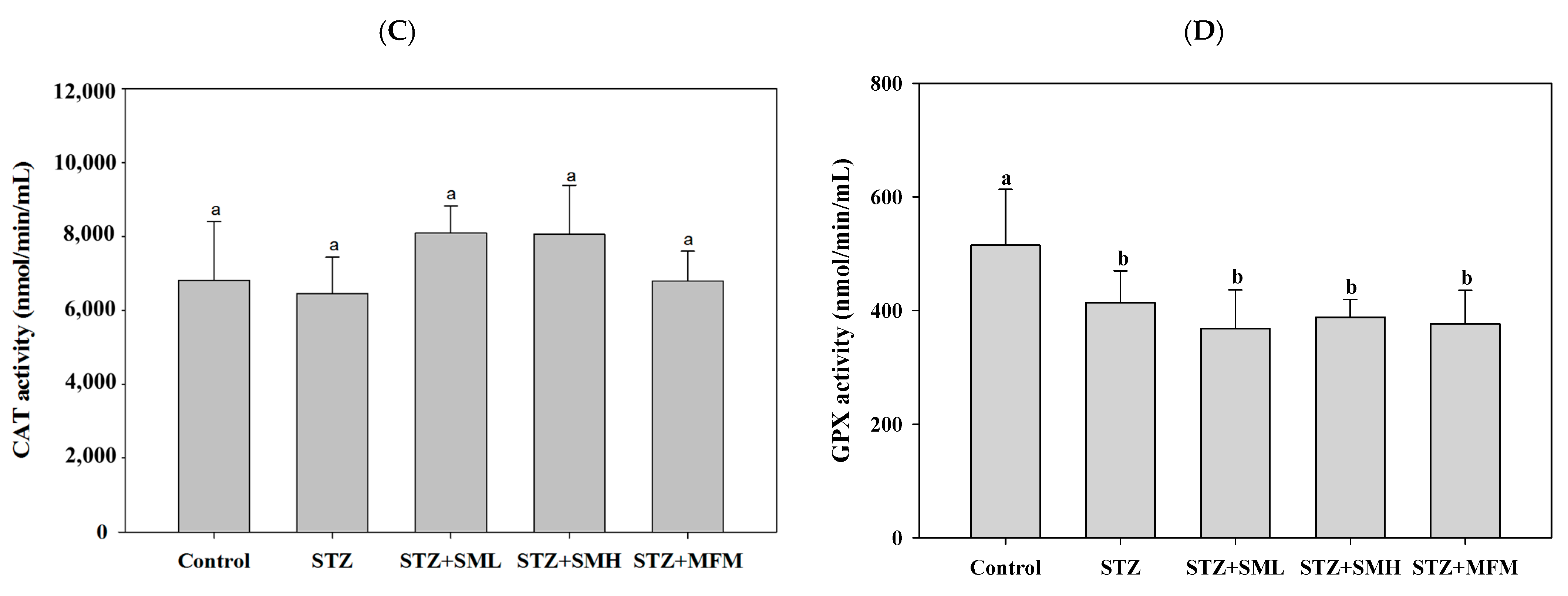
4.6. Antioxidant Enzyme Assay
4.6.1. Determination of Glutathione Peroxidase (Glutathione Peroxidase, GPx)
4.6.2. Determination of Superoxide Dismutase (SOD)
4.6.3. Determination of Catalase (CAT) Activity
4.7. Histological Studies
4.7.1. Tissue Embedding and Sectioning
4.7.2. Haematoxylin-Eosin (H&E) Staining
4.8. Statistical Analysis
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Sample Availability
References
- Diabetes. Available online: https://www.who.int/news-room/fact-sheets/detail/diabetes (accessed on 18 March 2023).
- Gouni-Berthold, I.; Krone, W. Diabetic Ketoacidosis and Hyperosmolar Hyperglycemic State. Med. Klin. 2006, 101 (Suppl. S1), 100–105. [Google Scholar]
- Whiting, D.R.; Guariguata, L.; Weil, C.; Shaw, J. IDF Diabetes Atlas: Global Estimates of the Prevalence of Diabetes for 2011 and 2030. Diabetes Res. Clin. Pract. 2011, 94, 311–321. [Google Scholar] [CrossRef] [PubMed]
- Bell, A.; Sherrell, Z. How Do Diabetes Rates Vary by Country? 2022. Available online: https://www.medicalnewstoday.com/articles/diabetes-rates-by-country (accessed on 18 March 2023).
- Li, H.; Chang, G.-Y.; Jiang, Y.-H.; Xu, L.; Shen, L.; Gu, Z.-C.; Lin, H.-W.; Shi, F.-H. System Dynamic Model Simulates the Growth Trend of Diabetes Mellitus in Chinese Population: Implications for Future Urban Public Health Governance. Int. J. Public Health 2022, 67, 1605064. [Google Scholar] [CrossRef] [PubMed]
- Namiki, M. Nutraceutical Functions of Sesame: A Review. Crit. Rev. Food Sci. Nutr. 2007, 47, 651–673. [Google Scholar] [CrossRef] [PubMed]
- Mahendra Kumar, C.; Singh, S.A. Bioactive Lignans from Sesame (Sesamum indicum L.): Evaluation of Their Antioxidant and Antibacterial Effects for Food Applications. J. Food Sci. Technol. 2015, 52, 2934–2941. [Google Scholar] [CrossRef] [PubMed]
- Andargie, M.; Vinas, M.; Rathgeb, A.; Möller, E.; Karlovsky, P. Lignans of Sesame (Sesamum indicum L.): A Comprehensive Review. Molecules 2021, 26, 883. [Google Scholar] [CrossRef]
- Kanu, P.; Bahsoon, J.; Kanu, J.; Kandeh, J. Nutraceutical Importance of Sesame Seed and Oil: A Review of the Contribution of Their Lignans. Sierra Leone J. Biomed. Res. 2010, 2, 4–16. [Google Scholar] [CrossRef]
- Wei, P.; Zhao, F.; Wang, Z.; Wang, Q.; Chai, X.; Hou, G.; Meng, Q. Sesame (Sesamum indicum L.): A Comprehensive Review of Nutritional Value, Phytochemical Composition, Health Benefits, Development of Food, and Industrial Applications. Nutrients 2022, 14, 4079. [Google Scholar] [CrossRef]
- Pathak, N.; Rai, A.K.; Kumari, R.; Bhat, K.V. Value Addition in Sesame: A Perspective on Bioactive Components for Enhancing Utility and Profitability. Pharmacogn. Rev. 2014, 8, 147–155. [Google Scholar] [CrossRef]
- Khatkar, A.; Sharma, K.K. Phenylpropanoids and Its Derivatives: Biological Activities and Its Role in Food, Pharmaceutical and Cosmetic Industries. Crit. Rev. Food Sci. Nutr. 2020, 60, 2655–2675. [Google Scholar] [CrossRef]
- Ciarcià, G.; Bianchi, S.; Tomasello, B.; Acquaviva, R.; Malfa, G.A.; Naletova, I.; La Mantia, A.; Di Giacomo, C. Vitamin E and Non-Communicable Diseases: A Review. Biomedicines 2022, 10, 2473. [Google Scholar] [CrossRef] [PubMed]
- Ma, X.; Wang, Z.; Zheng, C.; Liu, C. A Comprehensive Review of Bioactive Compounds and Processing Technology of Sesame Seed. Oil Crop Sci. 2022, 7, 88–94. [Google Scholar] [CrossRef]
- Orsavova, J.; Misurcova, L.; Ambrozova, J.; Vicha, R.; Mlcek, J. Fatty Acids Composition of Vegetable Oils and Its Contribution to Dietary Energy Intake and Dependence of Cardiovascular Mortality on Dietary Intake of Fatty Acids. Int. J. Mol. Sci. 2015, 16, 12871–12890. [Google Scholar] [CrossRef] [PubMed]
- Hirata, F.; Fujita, K.; Ishikura, Y.; Hosoda, K.; Ishikawa, T.; Nakamura, H. Hypocholesterolemic Effect of Sesame Lignan in Humans. Atherosclerosis 1996, 122, 135–136. [Google Scholar] [CrossRef] [PubMed]
- Phitak, T.; Pothacharoen, P.; Settakorn, J.; Poompimol, W.; Caterson, B.; Kongtawelert, P. Chondroprotective and Anti-Inflammatory Effects of Sesamin. Phytochemistry 2012, 80, 77–88. [Google Scholar] [CrossRef]
- Sohel, M.; Islam, M.N.; Hossain, M.A.; Sultana, T.; Dutta, A.; Rahman, M.S.; Aktar, S.; Islam, K.; Al Mamun, A. Pharmacological Properties to Pharmacological Insight of Sesamin in Breast Cancer Treatment: A Literature-Based Review Study. Int. J. Breast Cancer 2022, 2022, 2599689. [Google Scholar] [CrossRef]
- Peñalvo, J.L.; Hopia, A.; Adlercreutz, H. Effect of Sesamin on Serum Cholesterol and Triglycerides Levels in LDL Receptor-Deficient Mice. Eur. J. Nutr. 2006, 45, 439–444. [Google Scholar] [CrossRef]
- Majdalawieh, A.F.; Massri, M.; Nasrallah, G.K. A Comprehensive Review on the Anti-Cancer Properties and Mechanisms of Action of Sesamin, a Lignan in Sesame Seeds (Sesamum indicum). Eur. J. Pharmacol. 2017, 815, 512–521. [Google Scholar] [CrossRef]
- Xu, P.; Cai, F.; Liu, X.; Guo, L. Sesamin Inhibits Lipopolysaccharide-Induced Proliferation and Invasion through the P38-MAPK and NF-ΚB Signaling Pathways in Prostate Cancer Cells. Oncol. Rep. 2015, 33, 3117–3123. [Google Scholar] [CrossRef]
- Rosalina, R.; Weerapreeyakul, N. An Insight into Sesamolin: Physicochemical Properties, Pharmacological Activities, and Future Research Prospects. Molecules 2021, 26, 5849. [Google Scholar] [CrossRef]
- Nagarajan, S.; Lee, J.K. Therapeutic Effects of Sesamolin on Leukemia Induced by WEHI-3B in Model Mice. Appl. Biol. Chem. 2021, 64, 45. [Google Scholar] [CrossRef]
- Li, Q.-Z.; Zuo, Z.-W.; Liu, Y. Recent Status of Sesaminol and Its Glucosides: Synthesis, Metabolism, and Biological Activities. Crit. Rev. Food Sci. Nutr. 2022, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Grougnet, R.; Magiatis, P.; Laborie, H.; Lazarou, D.; Papadopoulos, A.; Skaltsounis, A.-L. Sesamolinol Glucoside, Disaminyl Ether, and Other Lignans from Sesame Seeds. J. Agric. Food Chem. 2012, 60, 108–111. [Google Scholar] [CrossRef] [PubMed]
- Majdalawieh, A.F.; Mansour, Z.R. Sesamol, a Major Lignan in Sesame Seeds (Sesamum indicum): Anti-Cancer Properties and Mechanisms of Action. Eur. J. Pharmacol. 2019, 855, 75–89. [Google Scholar] [CrossRef]
- Hong, L.; Yi, W.; Liangliang, C.; Juncheng, H.; Qin, W.; Xiaoxiang, Z. Hypoglycaemic and Hypolipidaemic Activities of Sesamin from Sesame Meal and Its Ability to Ameliorate Insulin Resistance in KK-Ay Mice. J. Sci. Food Agric. 2013, 93, 1833–1838. [Google Scholar] [CrossRef]
- Singh, R.B.; Mengi, S.A.; Xu, Y.-J.; Arneja, A.S.; Dhalla, N.S. Pathogenesis of Atherosclerosis: A Multifactorial Process. Exp. Clin. Cardiol. 2002, 7, 40–53. [Google Scholar]
- Ahmad, S.; ElSherbiny, N.M.; Jamal, M.S.; Alzahrani, F.A.; Haque, R.; Khan, R.; Zaidi, S.K.; AlQahtani, M.H.; Liou, G.I.; Bhatia, K. Anti-Inflammatory Role of Sesamin in STZ Induced Mice Model of Diabetic Retinopathy. J. Neuroimmunol. 2016, 295–296, 47–53. [Google Scholar] [CrossRef]
- Kong, P.; Chen, G.; Jiang, A.; Wang, Y.; Song, C.; Zhuang, J.; Xi, C.; Wang, G.; Ji, Y.; Yan, J. Sesamin Inhibits IL-1β-Stimulated Inflammatory Response in Human Osteoarthritis Chondrocytes by Activating Nrf2 Signaling Pathway. Oncotarget 2016, 7, 83720–83726. [Google Scholar] [CrossRef]
- Yan, L.-J. The Nicotinamide/Streptozotocin Rodent Model of Type 2 Diabetes: Renal Pathophysiology and Redox Imbalance Features. Biomolecules 2022, 12, 1225. [Google Scholar] [CrossRef]
- Li, X.; Gao, Y.; Li, S.; Yang, J. Effect of Sesamin on Pulmonary Vascular Remodeling in Rats with Monocrotaline-Induced Pulmonary Hypertension. Zhongguo Zhong Yao Za Zhi 2015, 40, 1355–1361. [Google Scholar]
- Noguchi, T.; Ikeda, K.; Sasaki, Y.; Yamamoto, J.; Yamori, Y. Effects of vitamin E and sesamin on hypertension and cerebral thrombogenesis in stroke-prone spontaneously hypertensive rats. Clin. Exp. Pharmacol. Physiol. 2004, 31, S24–S26. [Google Scholar] [CrossRef] [PubMed]
- Nakano, D.; Kwak, C.-J.; Fujii, K.; Ikemura, K.; Satake, A.; Ohkita, M.; Takaoka, M.; Ono, Y.; Nakai, M.; Tomimori, N.; et al. Sesamin Metabolites Induce an Endothelial Nitric Oxide-Dependent Vasorelaxation through Their Antioxidative Property-Independent Mechanisms: Possible Involvement of the Metabolites in the Antihypertensive Effect of Sesamin. J. Pharmacol. Exp. Ther. 2006, 318, 328–335. [Google Scholar] [CrossRef] [PubMed]
- Thuy, T.D.; Phan, N.N.; Wang, C.-Y.; Yu, H.-G.; Wang, S.-Y.; Huang, P.-L.; Do, Y.-Y.; Lin, Y.-C. Novel Therapeutic Effects of Sesamin on Diabetes-Induced Cardiac Dysfunction. Mol. Med. Rep. 2017, 15, 2949–2956. [Google Scholar] [CrossRef] [PubMed]
- Ananda, P.K.; Kumarappan, C.; Christudas, S.; Kalaichelvan, V. Effect of Biophytum Sensitivum on Streptozotocin and Nicotinamide-Induced Diabetic Rats. Asian Pac. J. Trop. Biomed. 2012, 2, 31–35. [Google Scholar] [CrossRef] [PubMed]
- Ramesh, B.; Saravanan, R.; Pugalendi, K.V. Influence of Sesame Oil on Blood Glucose, Lipid Peroxidation, and Antioxidant Status in Streptozotocin Diabetic Rats. J. Med. Food 2005, 8, 377–381. [Google Scholar] [CrossRef] [PubMed]
- Yargholi, A.; Najafi, M.H.; Zareian, M.A.; Hawkins, J.; Shirbeigi, L.; Ayati, M.H. The Effects of Sesame Consumption on Glycemic Control in Adults: A Systematic Review and Meta-Analysis of Randomized Clinical Trial. Evid. -Based Complement. Altern. Med. 2021, 2021, 2873534. [Google Scholar] [CrossRef]
- Bigoniya, P.; Nishad, R.; Singh, C.S. Preventive Effect of Sesame Seed Cake on Hyperglycemia and Obesity against High Fructose-Diet Induced Type 2 Diabetes in Rats. Food Chem. 2012, 133, 1355–1361. [Google Scholar] [CrossRef]
- Lei, H.; Han, J.; Wang, Q.; Guo, S.; Sun, H.; Zhang, X. Effects of Sesamin on Streptozotocin (STZ)-Induced NIT-1 Pancreatic β-Cell Damage. Int. J. Mol. Sci. 2012, 13, 16961–16970. [Google Scholar] [CrossRef]
- Eleazu, C.O.; Eleazu, K.C.; Chukwuma, S.; Essien, U.N. Review of the Mechanism of Cell Death Resulting from Streptozotocin Challenge in Experimental Animals, Its Practical Use and Potential Risk to Humans. J. Diabetes Metab. Disord. 2013, 12, 60. [Google Scholar] [CrossRef]
- Cerf, M.E. Beta Cell Dysfunction and Insulin Resistance. Front. Endocrinol. 2013, 4, 37. [Google Scholar] [CrossRef]
- Dworzański, J.; Strycharz-Dudziak, M.; Kliszczewska, E.; Kiełczykowska, M.; Dworzańska, A.; Drop, B.; Polz-Dacewicz, M. Glutathione Peroxidase (GPx) and Superoxide Dismutase (SOD) Activity in Patients with Diabetes Mellitus Type 2 Infected with Epstein-Barr Virus. PLoS ONE 2020, 15, e0230374. [Google Scholar] [CrossRef] [PubMed]
- Madi, M.; Babu, S.; Kumari, S.; Shetty, S.; Achalli, S.; Madiyal, A.; Bhat, M. Status of Serum and Salivary Levels of Superoxide Dismutase in Type 2 Diabetes Mellitus with Oral Manifestations: A Case Control Study. Ethiop. J. Health Sci. 2016, 26, 523. [Google Scholar] [CrossRef] [PubMed]
- Singhai, M.; Goyal, R.; Faizy, A. Glutathione Peroxidase Activity in Obese and Nonobese Diabetic Patients and Role of Hyperglycemia in Oxidative Stress. J. Midlife Health 2011, 2, 72. [Google Scholar] [CrossRef] [PubMed]
- Farbood, Y.; Ghaderi, S.; Rashno, M.; Khoshnam, S.E.; Khorsandi, L.; Sarkaki, A.; Rashno, M. Sesamin: A Promising Protective Agent against Diabetes-Associated Cognitive Decline in Rats. Life Sci. 2019, 230, 169–177. [Google Scholar] [CrossRef] [PubMed]
- Kong, X.; Wang, G.-D.; Ma, M.-Z.; Deng, R.-Y.; Guo, L.-Q.; Zhang, J.-X.; Yang, J.-R.; Su, Q. Sesamin Ameliorates Advanced Glycation End Products-Induced Pancreatic β-Cell Dysfunction and Apoptosis. Nutrients 2015, 7, 4689–4704. [Google Scholar] [CrossRef] [PubMed]
- Sharma, T.; Singh, I.; Singh, N.; Vardey, G.; Kumawat, M.; Ghalaut, V.; Shankar, V. Antioxidant Enzymes and Lipid Peroxidation in Type 2 Diabetes Mellitus Patients with and without Nephropathy. N. Am. J. Med. Sci. 2013, 5, 213. [Google Scholar] [CrossRef]
- Lubos, E.; Loscalzo, J.; Handy, D.E. Glutathione Peroxidase-1 in Health and Disease: From Molecular Mechanisms to Therapeutic Opportunities. Antioxid. Redox Signal 2011, 15, 1957–1997. [Google Scholar] [CrossRef]
- Hirano, T. Pathophysiology of Diabetic Dyslipidemia. J. Atheroscler. Thromb. 2018, 25, 771–782. [Google Scholar] [CrossRef]
- Lemieux, I.; Lamarche, B.; Couillard, C.; Pascot, A.; Cantin, B.; Bergeron, J.; Dagenais, G.R.; Després, J.-P. Total Cholesterol/HDL Cholesterol Ratio vs LDL Cholesterol/HDL Cholesterol Ratio as Indices of Ischemic Heart Disease Risk in Men. Arch. Intern. Med. 2001, 161, 2685. [Google Scholar] [CrossRef]
- Kwon, Y.H.; Kim, S.-K.; Cho, J.H.; Kwon, H.; Park, S.E.; Oh, H.-G.; Park, C.-Y.; Lee, W.-Y.; Oh, K.-W.; Park, S.-W.; et al. The Association between Persistent Hypertriglyceridemia and the Risk of Diabetes Development: The Kangbuk Samsung Health Study. Endocrinol. Metab. 2018, 33, 55. [Google Scholar] [CrossRef]
- Yadav, R.; Bhartiya, J.P.; Verma, S.K.; Nandkeoliar, M.K. The Evaluation of Serum Amylase in the Patients of Type 2 Diabetes Mellitus, with a Possible Correlation with the Pancreatic Functions. J. Clin. Diagn. Res. 2013, 7, 1291–1294. [Google Scholar] [CrossRef]
- Akanya, H.; Isa, U.; Adeyemi, H.; Ossamulu, I. Effect of Sesamum indicum (Linn) Seeds Supplemented Diets on Blood Glucose, Lipid Profiles and Serum Levels of Enzymes in Alloxan Induced Diabetic Rats. J. Appl. Life Sci. Int. 2015, 2, 134–144. [Google Scholar] [CrossRef] [PubMed]
- Mohammad Shahi, M.; Zakerzadeh, M.; Zakerkish, M.; Zarei, M.; Saki, A. Effect of Sesamin Supplementation on Glycemic Status, Inflammatory Markers, and Adiponectin Levels in Patients with Type 2 Diabetes Mellitus. J. Diet. Suppl. 2017, 14, 65–75. [Google Scholar] [CrossRef] [PubMed]
- Tai, T.-S.; Tien, N.; Shen, H.-Y.; Chu, F.-Y.; Wang, C.C.N.; Lu, C.-H.; Yu, H.-I.; Kung, F.-P.; Chuang, H.-H.; Lee, Y.-R.; et al. Sesamin, a Naturally Occurring Lignan, Inhibits Ligand-Induced Lipogenesis through Interaction with Liver X Receptor Alpha (LXR α) and Pregnane X Receptor (PXR). Evid.-Based Complement. Altern. Med. 2019, 2019, 9401648. [Google Scholar] [CrossRef] [PubMed]
- Majdalawieh, A.F.; Dalibalta, S.; Yousef, S.M. Effects of Sesamin on Fatty Acid and Cholesterol Metabolism, Macrophage Cholesterol Homeostasis and Serum Lipid Profile: A Comprehensive Review. Eur. J. Pharmacol. 2020, 885, 173417. [Google Scholar] [CrossRef] [PubMed]
- Jeon, C.Y.; Roberts, C.K.; Crespi, C.M.; Zhang, Z.-F. Elevated Liver Enzymes in Individuals with Undiagnosed Diabetes in the U.S. J. Diabetes Complicat. 2013, 27, 333–339. [Google Scholar] [CrossRef]
- Shrestha, N.; Bhatt, N.; Neopane, P.; Dahal, S.; Regmi, P.; Khanal, M.; Shrestha, R. Hepatic Involvement with Elevated Liver Enzymes in Nepalese Subjects with Type 2 Diabetes Mellitus. Int. J. Biochem. Res. Rev. 2017, 16, 1–8. [Google Scholar] [CrossRef]
- Ohaeri, O.C. Effect of Garlic Oil on the Levels of Various Enzymes in the Serum and Tissue of Streptozotocin Diabetic Rats. Biosci. Rep. 2001, 21, 19–24. [Google Scholar] [CrossRef]


| Group 1 | ALT 2 (U/L) | AST (U/L) | TG (mg/dL) | TC (mg/dL) | HDL (mg/dL) | Amylase (U/L) |
|---|---|---|---|---|---|---|
| Control | 39 ± 5 b2 | 126 ± 15 b | 75 ± 10.3 b | 72 ± 5.1 b | 21 ± 1.7 a | 1866 ± 129 a |
| STZ | 82 ± 11 a | 193 ± 32 a | 103 ± 9.8 a | 70 ± 2.9 b | 17 ± 2.5 b | 1423 ± 237 b |
| STZ + SML | 67 ± 12 b | 153 ± 27 b | 80 ± 8.2 b | 72 ± 5.3 b | 18 ± 2.2 ab | 1965 ± 391 a |
| STZ + SMH | 58 ± 14 b | 143 ± 24 b | 50 ± 6.7 c | 70 ± 2.6 b | 21 ± 2.3 a | 2124 ± 286 a |
| STZ + MFM | 57 ± 13 b | 122 ± 18 b | 68 ± 3.3 b | 80 ± 2.4 a | 21 ± 2.1 a | 1809 ± 154 a |
| No. | Group | Dose of Sample (mg/kg Body Weight/Day) | STZ (55 mg/kg Body Weight) | Animal Number |
|---|---|---|---|---|
| 1 | Control | - | - | 6 |
| 2 | Streptozotocin (STZ) | - | + | 6 |
| 3 | Sesamin low dose (SML) | 20 | + | 6 |
| 4 | Sesamin high dose (SMH) | 60 | + | 6 |
| 5 | Metformin (MFM) | 250 | + | 6 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Huang, S.-M.; Chuang, C.-H.; Rejano, C.J.F.; Tayo, L.L.; Hsieh, C.-Y.; Huang, S.K.-H.; Tsai, P.-W. Sesamin: A Promising Therapeutic Agent for Ameliorating Symptoms of Diabetes. Molecules 2023, 28, 7255. https://doi.org/10.3390/molecules28217255
Huang S-M, Chuang C-H, Rejano CJF, Tayo LL, Hsieh C-Y, Huang SK-H, Tsai P-W. Sesamin: A Promising Therapeutic Agent for Ameliorating Symptoms of Diabetes. Molecules. 2023; 28(21):7255. https://doi.org/10.3390/molecules28217255
Chicago/Turabian StyleHuang, Shu-Ming, Cheng-Hung Chuang, Christine Joyce F. Rejano, Lemmuel L. Tayo, Cheng-Yang Hsieh, Steven Kuan-Hua Huang, and Po-Wei Tsai. 2023. "Sesamin: A Promising Therapeutic Agent for Ameliorating Symptoms of Diabetes" Molecules 28, no. 21: 7255. https://doi.org/10.3390/molecules28217255
APA StyleHuang, S.-M., Chuang, C.-H., Rejano, C. J. F., Tayo, L. L., Hsieh, C.-Y., Huang, S. K.-H., & Tsai, P.-W. (2023). Sesamin: A Promising Therapeutic Agent for Ameliorating Symptoms of Diabetes. Molecules, 28(21), 7255. https://doi.org/10.3390/molecules28217255









