1. Introduction
Kingdom Fungi is diverse and includes different types of organisms such as molds, yeasts, mushrooms, polypores, plant parasitic rusts, and smuts, totalizing more than 120,000 described species and between 2.2 and 5.1 million estimated species [
1,
2]. This group includes saprotrophic, pathogenic, parasitic, commensal, and symbiotic organisms that can be found in the most variable ecosystems, from marine or freshwater to terrestrial environments [
1,
3,
4]. Their morphological traits aligned with exceptional metabolic diversity enable them to occupy numerous ecological niches and to create a panoply of interactions with other organisms [
1,
4].
Due to their unique but diverse characteristics, fungi are an essential component for the well-functioning of the ecosystems and have diversified roles in them. In terrestrial environments, fungi are crucial for soil fertility, decomposing organic matter and facilitating carbon and nitrogen flow, as well as for supporting plant species development [
5]. Furthermore, microscopic fungi are an important food source for soil invertebrates and some of the macroscopic ones are eatable and valuable for humans’ and animals’ diets [
4]. Furthermore, the observed diverse interaction skills and ability to produce different primary and secondary metabolites turn fungi into an interesting group for the pharmaceutical industry [
6]. Most of the plant endophytic fungi produce compounds with both harmful and beneficial effects on plants, which, when extracted, may have agricultural or even medicinal value [
6,
7]. For example, some secondary metabolites, such as alkaloids, may help a plant to resist to pests, to repel herbivores, and to adapt to changes in climatic conditions [
6]. Others can be used as antibiotics (e.g., penicillin or cephalosporin), anticancer agents (e.g., illudin or paclitaxel), immunomodulatory substances (e.g., cyclosporine or mycophenolic acid), or antiviral agents (e.g., stachyflin), for example [
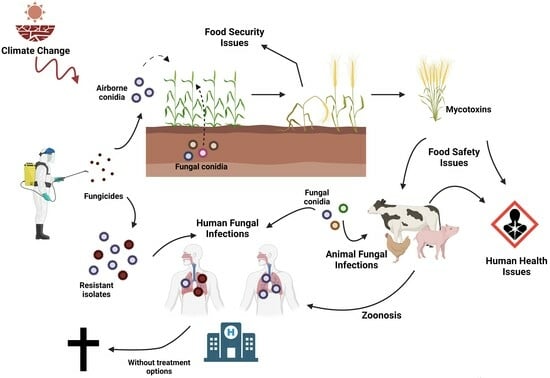
7]. Therefore, fungal metabolites comprise a panoply of promising compounds and applications, but also potential harmful implications, in particular regarding mycotoxins in human and animal health [
6,
7,
8], (
Figure 1).
The most important mycotoxins are aflatoxins, fumonisins, ochratoxin A (OTA), deoxynivalenol (DON), zearalenone (ZEN), and ergot alkaloids which are mainly produced by
Aspergillus,
Penicillium,
Fusarium,
Stachybotrys, and
Claviceps species [
9,
10].
Mycotoxin contamination of food and feed may result in acute or chronic consequences such as carcinogenic, teratogenic, immunosuppressive, or estrogenic issues in humans and animals [
9], which comprises a food safety concern. In this way, the European Commission set the maximum levels in raw materials, feed and processed food [
11], which means that all the products containing mycotoxins above the thresholds are strongly devalued or even banned from being sold, which also affects the global economy. Furthermore, mycotoxins can also be inhaled, being other route to cause adverse human health effects. Exposure by means of inhalation of molds may happen in indoor residential, school, and office environments [
12].Additionally, in certain conditions, fungi can directly or indirectly cause allergies [
13] and infections in humans [
14], as well as in crops, compromising their yields [
15,
16]. Thus, the contamination of edible plants and of the surrounding environment is another possible route affecting human and animal health. In this way, this review will explore the negative impact of fungi on human health, under the “One Health” perspective. The “One Health” concept connects the health of plants, humans, animals, and the environment in a unifying approach, aiming to balance and optimize them as only one. Its points of action include food security and safety, the integrity of ecosystems, fungal infections including zoonosis and antimicrobial resistance control, and the promotion of health [
17].
This review covers the most common mycological infestations of plants and animals with effects on human health either directly through dietary exposure or indirectly as environmental contaminants. Additionally, the subject of antifungal resistance induced by exposure to plant protection products will be explored and discussed, also under a “One Health” perspective.
2. Fungal Effects on Plant Health
Fungi are an important group of organisms that influence plant health, either by helping them to grow and to resist to some plant pathogens and herbivorous animals, or by harming them by causing diseases [
6]. The most relevant phytopathogenic fungi are the ones infecting agricultural crops and forestry trees with a high impact on human nutrition, life quality, and economy, as they may compromise production/yields and quality [
18]. In fact, 15 to 20% of crop losses are caused by plant diseases, of which over 70% correspond to fungal infections, including those of primary crops, resulting in high levels of direct economic losses [
15,
19].
There are several phytopathogenic species and strains in the world; however, their virulence depends on the host species and the susceptibility of the commercial varieties as well as on environmental conditions. One of the most important phytopathogenic fungal genera is
Fusarium, of which some species can produce mycotoxins or even cause diseases in humans also. For example,
Fusarium oxysporum causes “
Fusarium rot” in roots and seeds of rice [
20,
21], “
Fusarium wilt” in bananas [
22], tomato [
23] and watermelons [
24], and it is also a great producer of moniliformin [
25]. In wheat,
Fusarium graminearum causes “
Fusarium head blight” and is a great producer of DON, nivalenol, and fusarenone [
25]. In Delicious and Fuji apple trees,
Fusarium tricinctum causes a new disease that results in withering and death [
26], and produces moniliformin [
25]. In maize crops, in cooler temperate regions, several species of the
Fusarium genus (
F. graminearum,
F. culmorum,
F. cerealis, and
F. avenaceum) are usually detected to cause “
Gibberella ear rot” and contaminate grains with DON, nivalenol, fusarenone, ZEN, moniliformin, and T-2 toxin derivatives [
25,
27]. Also in maize, but in warmer temperate regions, the most frequently occurring species belong to
Fusarium fujikuroi complex species, such as
F. verticillioides,
F. proliferatum, and
F. subglutinans, causing “
Fusarium ear rot” contaminating maize grains with fumonisins, beauvericin, fusaproliferin, and moniliformin [
16,
18,
25,
27,
28] (
Table 1).
In 2020, the main crops produced worldwide were sugar cane and cereals, such as maize, rice, and wheat. Among the fruits, the most important crops were bananas and plantains, watermelons, and apples, while among the vegetables, the most important crop was tomato [
29]. As referred, among the many existent fungal genera, one is enough to cause disease and mycotoxin contamination in the most important crops, regardless of their type. In this way, phytopathogenic species have a huge impact on the global economy, decreasing crop yields and compromising food security, but also on human health, contaminating raw materials and products derived thereof, such as flours, breakfast cereals, tortillas, bread, and snack-like products, among others, with one or more mycotoxins [
16,
18,
30,
31,
32] and, therefore, compromising food safety.
Despite the global production of primary crops being raised up to 9.3 billion tons in 2020 [
29], phytopathogenic fungi diversity also increased and expanded, which constitutes a high risk to food security and global economy, as well as to global health and ecosystems [
19]. There are several reasons for the emergence of these fungal pathogens, including their high adaptive potential, the occurrence of climate and ecological changes, globalization and international commerce, and the broad use of antifungals in agriculture, compost, feedstock, commodities, and several other materials [
33]. Some common saprotrophic species, such as those from the genus
Aspergillus, are causing an emergent number of infections in plants and humans.
Post-harvest diseases together with the storage conditions of fruits, vegetables, and commodities are also worrisome, since annually, and depending on the product and country, 10% to 50% of production is lost due to microbial spoilage [
34] and may be contaminated with mycotoxins [
18]. Hence, currently, controlling the increasing presence and spreading of fungi and their mycotoxins’ production are priorities on field (before harvest) and after the harvest, including the storage period.
Fungal diseases are usually treated using chemical fungicides, which have a negative impact on ecosystems, food safety, and human health [
35]. Azoles are among the most frequent classes of fungicides used in agriculture, being present in around half of the cereal crops and vineyards of the European Union (EU) to control mildew and rust [
36]. Azoles are stable molecules that inhibit sterol 14α-demethylase enzymes, compromising ergosterol biosynthesis and cell structure, which preclude fungal growth [
37]. Their molecular stability allows them to remain active in water and soil for several months, as well as in fruits and vegetables, having adverse ecological effects [
35]. The increasing time of exposure of fungi to them enhances the pressure of positive selection of resistant strains [
35]. The emergence of resistant strains in crops is also a major concern to medical and scientific community, since azoles are used as a first-line therapy for a large number of fungal infections in humans [
35,
38,
39]. The most common azoles used in agriculture are epoxiconazole, difenoconazole, propiconazole, bromuconazole, and tebuconazole, while those in clinic are itraconazole, voriconazole, fluconazole, and posaconazole [
35,
38,
39]. These azoles have similar molecular structures, binding modes, and high levels of cross-resistance, meaning that there is a high risk of preclusion of fungal infection treatment in humans [
35,
38,
39].
To prevent and minimize the negative impact of using chemical fungicides, research on new and biological alternatives is increasing, including the use of bacteria, or other fungal species [
21,
23,
34] for the biocontrol of harmful fungal species. For example,
Bacillus spp. may be used to control “
Fusarium wilt” of tomatoes, caused by
F. oxysporum or
F. solani [
23], and “
Fusarium ear rot” in maize caused by
F. verticillioides [
40]. The use of fungal species as a sustainable option for biological control in agriculture relies on their high reproductive rates, short generation time, and capability to survive in the environment as parasites or saprotrophs [
34]. In fact, fungi as biocontrol agents are used against multiple organisms in agriculture, including to control insect pests. Some examples include
Metarhizium anisopliae,
Beauveria bassiana,
Aspergillus flavus, and
Metarhizium flavoviride, which may be used to control locust infestation [
15]. To manage fungal plant diseases, antagonist species may produce inhibitory metabolites, act as parasites on pathogenic fungi, induce the plant defense response against pathogens, promote plant growth (which reduces the effects of disease), or compete with pathogenic species [
34].
Trichoderma is one of the greatest fungal genera with the potential to control plant fungal diseases, comprising 25 biocontrol agents [
34]. For example,
Trichoderma viride and
T. harzianum effectively reduce
F. verticillioides growth and fumonisin production in vitro and
in planta [
40]. Other genera recognized as having significant potential are
Alternaria,
Aspergillus,
Candida,
Fusarium,
Penicillium,
Pichia,
Pythium,
Talaromyces, and
Verticillium, comprising five or more known antagonistic species [
34]. For example, some species of
Penicillium, namely
P. variabile,
P. dendriticum, and
P. duclauxii, were reported as antagonists of
Aspergillus niger, controlling its growth, which may be used as a biocontrol agent for onion “black rot” [
41]. Moreover, biocontrol antagonists are now also applied to control post-harvest diseases. One example is some
Trichoderma species used for the management of the post-harvest “crown rot” of banana caused by
Colletotrichum musae,
F. verticillioides, or
Lasiodiplodia theobromae [
34]. Another example is
Clonostachys rosae, which effectively reduces the sporulation of
F. verticillioides and
F. proliferatum on maize after and post-harvesting [
40].
Other agricultural practices for managing fungal diseases include the simultaneous use of biocontrol agents and synthetic fungicides [
34], crop rotation, the avoidance of excessive irrigation, and the use of resistant or tolerant plant varieties [
23]. In some cases, genetic engineering is also an alternative approach to controlling fungal diseases, e.g., introducing genes which encode proteins with antifungal activity into the plant genome. One example is the use of transgenic banana plants which express the rice thaumatin-like protein gene to resist
Fusarium wilt [
22].
3. Mycotoxin Effects on Animal and Human Health
The consumption of crop-based food and feed contaminated with mycotoxins constitutes a real concern to both animal and human health. The most relevant mycotoxins are mainly produced by
Fusarium,
Penicillium,
Aspergillus, or
Alternaria species. For example,
Alternaria alternata is a species that is considered to be vital in mycotoxin-contamination of fruits and vegetables [
42]. The most relevant mycotoxins harmful to human health are aflatoxins, OTA, fumonisins, ZEN, nivalenol, DON, and ergot alkaloids [
43].
In industrialized countries, the majority of the protein consumed
per capita is from animal sources, with 41% coming from terrestrial meat animals, 34% from milk, 15% from aquatic meat animals, and 10% coming from eggs [
44]. On the contrary, in developing countries, the main protein sources are cereals, followed by milk. Thus, since most of the ingested protein is from farming, the quality of crops and animal feed is an important aspect for human health.
In 2022, the DSM World Mycotoxin Survey reported that, worldwide, 57% of the commodities had more than one mycotoxin per sample, fumonisins and DON being the most prevalent, followed by ZEN and aflatoxins [
45]. Globally, this tendency has been seen in the last decade, with 52% to 74% of the commodity samples having DON and 53% to 70% having fumonisins [
45]. Furthermore, 75% to 93% of the samples from North American or South Asian countries, and China presented at least one mycotoxin existing in amounts beyond the stablished thresholds (500 ppm of fumonisins, 150 ppm of DON, 50 ppm of ZEN or T-2, 10 ppm of OTA and 2 ppm of aflatoxins) [
45]. This means that quality losses and economic costs, estimated by the US Food and Drug Administration (FDA) resulted in an annual mean of 932 million American dollars (USD) [
46].
Most of the animal feed is from commodities which may have been exposed to mycotoxin contamination. In fact, the incidences of mycotoxins and multi-mycotoxins in animal feed are high [
46]. Worldwide, most feed samples carry mycotoxins, namely fumonisins (B1-82%, B2-73%, and B3-62%), DON (71%), and/or ZEN (67%) [
45] The frequency by continents of the most relevant mycotoxins found in animal feed is presented in
Table 2).
Additionally, some emerging mycotoxins were also detected in most of the feed samples, namely beauvericin (71%) and enniatin (B1-67%, B-58%), that affects the immune system, and moniliformin (63%), that is genotoxic, immunosuppressive, causes heart damage, muscular weakness, and respiratory distress [
45].
As mycotoxins show resistance to both the digestive process and high and low temperatures, they can remain in meat and milk derivatives and be spread throughout the food chain [
43]. Exposure to mycotoxins can cause chronic and/or acute health problems, depending on factors as the type and dose of mycotoxins, time of exposure, individual health conditions, sex, and age [
9,
43]. Mycotoxicosis effects depend on the type of mycotoxin and on the route of exposure, which can occur via inhalation, ingestion, or skin absorption [
9]. For example, inhaling high concentrations of the T-2 toxin may result in human pulmonary edema or lung lesions, while its ingestion may cause direct damage to the intestinal mucosa [
9]. Thus, mycotoxins can directly affect the liver, kidneys, and nervous and immune systems, or, as aflatoxins and fumonisins do, interfere in protein synthesis, causing cancer [
9,
43].
In animals, the consumption of feed contaminated by mycotoxins has been observed via the loss of the body weight, decreased reproductivity, damage in vital organs, increased illness associated to immunosuppression, and even death [
9,
10]. One example of these situations occurred in 1960 in England where a massive number of turkeys died due to the consumption of peanuts contaminated with aflatoxins imported from Brazil [
9]. Mainly produced by
Aspergillus species, such as
A. niger and
A. flavus, aflatoxin B1 is also classified as a human carcinogen, mainly attacking the liver and immune system, and having been reported in the Philippines, Africa, and China as the cause of the increment in human gastrointestinal and hepatic neoplasms, as well as of weight loss in children [
9]. In fact, aflatoxins may be detected in several products and may come in other forms, such as aflatoxin M1, the hydroxylated metabolite of aflatoxin B1, that was reported in pasteurized milk, ultra-highly treated milk, milk powder, and some milk-based products [
9,
43]. Due to its importance, the maximum levels of AFM1 in raw milk are 50 ng/kg in the EU and 500 ng/kg in the United States (US) [
43]. One example of the terrible effect of aflatoxins on human health occurred in 1988, when 13 Chinese children in the northwestern state of Perak in peninsular Malaysia died due to an outbreak of acute hepatic encephalopathy caused by the consumption of aflatoxin-contaminated Chinese noodles [
47]. Another example occurred in 2004, in Kenya, where 125 individuals died and around 200 needed treatment after consuming maize contaminated with aflatoxins [
43]. Furthermore, in poultry and swine production settings, the occurrence of aflatoxins is high, with reported cases of aflatoxin B1 inhalation by workers, as well as the presence of
Aspergillus spp. conidia in the air [
48,
49,
50,
51,
52,
53].
Other
Aspergillus species are also mycotoxigenic; for example,
A. terreus produces territrems (neurotoxic), and
A. ochraceus produces OTA [
6,
9,
10]. In the same way, various mycotoxins may be present in feed contaminated with
Penicillium species, such as
P. verrucosum, including patulin, cyclopiazonic acid, and OTA [
54]. In animals, OTA can cause cancer, morphological defects, lesions on gastrointestinal, renal, and lymphoid tissues, blood clots, and a reduction in egg production [
9,
10]. In humans, OTA has teratogenic and genotoxic potential, is toxic to the liver and kidneys, and is an immunosuppressant, inducing apoptosis in lymphocytes and neuronal cells, and may be detected in human breast milk [
9,
10,
43].
On the other hand, fumonisins, DON, and ZEN are mainly produced by
Fusarium species. Fumonisin B1 is genotoxic, inducing chromosomal aberrations, is a cancer promoter, responsible for causing neural tube defects in human babies, and is linked with the high incidence of human esophageal carcinoma due to the consumption of fumonisin-contaminated maize [
9,
43]. In animals, fumonisins are also toxic to kidneys, the respiratory tract, and liver. For example, they cause porcine pulmonary edema, promote cancer activity, and are neurotoxic being responsible for the equine syndrome leukoencephalomalacia, defined by the liquefaction of the cerebral hemisphere of the brain [
9]. ZEN is relevant as an estrogenic mycotoxin with the potential to disrupt sex steroid hormone functions, being usually associated with feminizing syndromes or hyper-estrogenic activity in pigs, and having been found in 55.1% and 22.4% of endometrial tissues from women with endometrial adenocarcinoma and endometrial hyperplasia, respectively [
9,
43]. In turn, DON and T-2 toxin mainly affect bovine and poultry immune and digestive systems, and may be detected in eggs and milk. Animals intoxicated with these mycotoxins show several symptoms, e.g. food refusal, weight loss, vomiting, severe dermatitis, abortion, hemorrhage, abnormal feathering, lesions on the edges of the birds’ beaks, the inhibition of reproductive performance, and death [
9]. In general, monogastric farm animals, such as poultry and swine, are more susceptible to mycotoxins than ruminants because their rumen flora have the ability to convert mycotoxins in less carcinogenic metabolites or in compounds without biological action [
9,
10].
As previously mentioned, the same fungal species is able to produce different mycotoxins and more than one mycotoxigenic species may be detected in the same product. Therefore, Multi-mycotoxin occurrence is a frequent issue, since the co-occurrence of mycotoxins may result in synergistic effects. This happens when aflatoxins are present together with DON and T2 toxin, or OTA with fumonisins, or fumonisins with DON, for example [
9]. Furthermore, modified mycotoxins have been also reported in commodities. Modified mycotoxins have different structures, solubilities, polarities, and molecular masses that confer them less toxicity due to their lower absorption by animals and humans [
55]. However, potential conversions in their free form can increase bioavailability and thus involve higher risks to animal and human health. Therefore, it is important to detect and evaluate their stability during the feeds’ processing and digestion, as well as their toxicokinetic and toxicodynamic properties [
55].
Some good farming practices include carrying out proper fertilization, crop rotation, an integrated pest management plan, opting for pest- and disease-resistant/tolerant varieties, harvesting at the optimum maturity stage, and ensuring a grain’s physical integrity and good post-harvest management, namely controlling humidity, temperature, ventilation, insect and rodent presence, and sanitation [
55,
56,
57]. A combination of new strategies may also be used, such as bio-competitive fungi as biocontrol agents, varieties resistant to mycotoxins, antibody-mediated technology, or even nanomaterials for antifungal functions or the inhibition of mycotoxins [
55]. Additionally, some physical, thermal, and biological methods may be used, such as cleaning and aggressive sorting, non-ionizing and ionizing irradiation, or the use of microorganisms with detoxification activities [
55,
56,
57]. Other methods to control fungal and mycotoxin contamination have been studied, including ozone application, which inhibits fungal growth, cold plasma technology, which reduces and degrades mycotoxins in food and feed, pulsed light, radio frequency, and microwave for reducing mycotoxin contamination [
55]. However, it is important to keep in mind that, although there are several methods to prevent and control mycotoxins, it is impossible to eradicate both fungi and mycotoxins [
55]. Consequently, the aim should be to monitor and reduce them to nonharmful levels to human and animal health. In livestock production, it is important to choose high-quality feedstuffs and to perform mycotoxin monitorization [
55]. Moreover, the silage used for animals’ bedding, the feeding silos and feeders used should be routinely changed, cleaned, and climatized, with insect and rodent presence being duly controlled [
43,
55]. Additionally, some binding agents (inorganic or organic) or bio-transforming agents (e.g., bacteria, yeast, fungi, and enzymes that degrade mycotoxin molecules in non-toxic metabolites) may be used to control fungal proliferation and mycotoxin contamination [
43,
55,
56,
57].
4. Fungal Effects on Human Health
Fungal infections are among the most frequent causes of death worldwide [
58], accounting for more than 1,500,000 deaths per year and affecting over than 1,000,000,000 people in the world [
14]. Fungi cause health issues that can range from allergies to invasive infections, accounting, for example, for more than 10,000,000 of fungal asthma cases per year [
14].
Around 20–50%, of the fungal infections in humans, can be transmitted directly or indirectly by animals, including cryptococcosis, sporotrichosis, histoplasmosis, blastomycosis, paracoccidiomycosis and dermatophytosis. The last one is the most frequent zoonosis [
59], while sporotrichosis is described as the most prevalent and widespread subcutaneous infection worldwide [
60]. Dermatophytes can be transmitted to people from different sources; these sources can be anthropophilic fungi infecting humans almost exclusively, zoophilic fungi infecting animals and being transmitted to humans, or geophilic fungi, being found in the soil and infecting both humans and animals. Dermatophytosis is also known as ringworm or tinea, causing ~1,000,000,000 cases/year [
14], being a superficial and contagious infection of the skin, hair, and/or nails, caused by dermatophyte fungi belonging to
Trichophyton or
Microsporum genera, for example [
61].
Trichophyton is the genus more frequently identified as the etiological agent of dermatophytosis in humans [
61].
T. rubrum is an anthropophilic dermatophyte fungus, also having been reported in several studies as the etiological agent of deep and invasive disease in immunosuppressed patients [
60].
Thus, some fungal species are able to cause invasive fungal infections, which are difficult to diagnose, manage, and treat, with an estimated incidence of 6 cases per 100,000 persons per year, and are also associated with substantial morbidity and mortality worldwide [
60,
62]. These species belong to different genera, e.g.,
Cryptococcus,
Candida,
Aspergillus,
Histoplasma,
Fusarium,
Scedosporium,
Coccidioides, and
Paracoccidioides.
Lomentospora prolificans,
Talaromyces marneffei,
Pneumocystis jirovecii, and Mucorales, which are also frequently occurring species [
62].
The main species of the
Cryptococcus genus causing cryptococcosis in humans and other animals are
C. gattii, and
C. neoformans. C. neoformans mainly affects immunocompromised individuals, causing cryptococcal meningitis, a disease with very high mortality [
62]. Cryptococcal meningitis accounts for 152,000 cases of cryptococcal meningitis, resulting in 112,000 cryptococcal-related deaths worldwide [
14,
63].
C. gattii affects both immunocompromised and immunocompetent individuals, and may cause invasive disease, resulting in a mortality rate of 10% to 25%. Cryptococcosis is usually susceptible to fluconazole, amphotericin B and flucytosine, showing intrinsic resistance to echinocandins [
62].
The most common nosocomial fungal infections are caused by species generally considered to belong to the
Candida genus; five species account for around 90% of candidemia cases, namely
C. albicans,
Nakaseomyces glabrata (
C. glabrata),
C. tropicalis,
C. parapsilosis, and
Pichia kudriavzeveii (
C. krusei) [
62,
64]. However, their distribution varied in population-based studies conducted in different geographical areas [
62,
64,
65].
Candida albicans is the most frequently occurring species. Studies from Northern Europe and the USA reported a high number of cases caused by
N. glabrata, whereas studies from South America and countries from south Europe demonstrated a lower number of cases caused by
N. glabrata and a higher number of cases attributed to
C. parapsilosis [
65]. More recently,
C. auris emerged as a novel pathogen causing invasive candidiasis with high mortality, ranging from 29% to 53%, and has been reported in more than 35 countries, in all continents except Antarctica [
62,
64].
Candida albicans,
N. glabrata,
C. parapsilosis, and
C. tropicalis are usually present in the healthy human microbiome as commensals, but under certain circumstances they can cause superficial infections or invasive candidiasis. Mortality provoked by the presence of these fungi has been reported. It varies according to the fungal species. For instance, 20–50% was attributed to
C. albicans and
N. glabrata, 20–45% was due to
C. parapsilosis, and 26–60% was due to
C. tropicalis [
62].
P. kudriavzeveii is an opportunistic pathogenic yeast which can cause mucosal infections or invasive candidiasis, and also has a high mortality rate (44–67%).
Candida spp. are also associated to superficial infections, vaginal candidiasis being one of the most frequently occurring infections worldwide, affecting 70–75% of women and resulting in around 134,000,000 infections per year, mainly caused by
C. albicans [
14].
Worldwide, invasive candidiasis accounts for around 700,000 cases per year [
14], being usually treated with echinocandins and azoles [
14,
62]. In the last two decades, the
s proportion of invasive candidiasis caused by the
C. albicans decreased more than 10%, whereas the infections caused by other
Candida species known as being more resistant to antifungals increased [
58]. The rising numbers of these species are also due to prolonged prophylaxis or therapy with antifungal agents [
66]. One example of a species resistant to several or all e antifungal classes available is
C. auris, which is considered an emerging multidrug-resistant yeast, showing high rates of resistance to fluconazole (87–100%), moderate resistance rates to amphotericin B (8–35%), and low resistance to echinocandins (0–8%) [
62,
64]. Furthermore,
N. glabrata shows high minimum inhibitory concentrations (MIC) in response to azoles, and rising echinocandin resistance [
62].
C. tropicalis is azole-resistant, mainly to fluconazole and itraconazole, and this resistance usually ranges from 0% to 20%, with some reports of 40–80% [
10,
62]. The antifungal resistance of
C. parapsilosis and
P. kudriavzeveii is considered moderate, the latter being intrinsically resistant to fluconazole [
62]. Recently,
C. parapsilosis isolates resistant to fluconazole have emerged, causing outbreaks in several health institutions [
67].
The filamentous fungus more frequently isolated from patients with invasive fungal infections is
Aspergillus, accounting for about 300,000 cases of invasive aspergillosis per year worldwide [
14], with a high mortality rate of 45% to >99%, depending on if the patient is treated or not [
14,
39,
60,
68,
69]. Furthermore, also worldwide,
Aspergillus species cause around 3,000,000 cases of chronic pulmonary aspergillosis, and more than 1 million of deaths per year [
14,
39,
60,
68]. Some pulmonary pathologies are related to occupational exposure to
Aspergillus conidia that cause
Aspergillus-induced allergic and asthmatic lung diseases [
68]. An example of occupational disease caused by
Aspergillus is an onion farmer that developed hypersensitive pneumonitis caused by the inhalation of
A. niger while cleaning up onion peels with air compressors [
70].
Aspergillus genus is divided in several sections, of which the
Fumigati,
Circumdati,
Terrei,
Nidulantes,
Ornati,
Warcupi,
Candidi,
Restricti,
Usti, and
Flavipedes sections contain relevant species in clinics [
10]. Section
Fumigati includes the main etiologic agents of aspergillosis:
A. fumigatus sensu stricto—the major cause of aspergillosis—and its cryptic species
A. lentulus,
A. udagawae,
A. viridinutans,
A. thermomutatus,
A. novofumigatus, and
A. hiratsukae—responsible for 3% to 6% of those infections [
39].
A. fumigatus sensu stricto, due to its small conidia, high thermotolerance, rapid growth, and optimal temperature of 37 °C, can affect both the upper and the lower respiratory tract. The damage caused is due to the fungus itself and also due to the host’s inflammatory response, causing a range of health issues that can include an allergic reaction, colonization or semi-invasive disease, or even acute invasive aspergillosis, depending on the immune status of the host [
59,
62,
68]. Although invasive aspergillosis may be rare in immunocompetent individuals, in immunocompromised people it is a major cause of morbidity and mortality [
59,
62,
69]. Recently, two new forms of aspergillosis were reported: influenza-associated pulmonary aspergillosis (IAPA) and COVID-associated pulmonary aspergillosis (CAPA) [
69]. IAPA was reported in 19% of the patients admitted at the ICU with influenza infection and CAPA was reported in 10% of the mechanically ventilated patients with COVID-19 [
71,
72]. Aspergillosis is mainly treated with triazoles, especially voriconazole, which are responsible for a decrease of more than 50% in invasive aspergillosis mortality [
69]. However, the treatment of aspergillosis has been a concern since the appearance of
A. fumigatus resistant to azoles, causing a rise in mortality rates (47–88%) [
62]. The use of triazole prophylaxis, treatments with azoles, and azole agricultural fungicides cause the development of acquired resistance in
A. fumigatus isolates, leading to new challenges in the therapeutic management of these infections [
35,
36,
38,
68]. As the availability of antifungal drugs to treat fungal infections is limited, the rise in resistance rates may result in treatment failure and, consequently, in higher mortality rates [
39]. There are two predominant mutations in
A. fumigatus found in azole-naïve patients—TR34/L98H and TR46/Y121F/T298A (detected in the
cyp51A gene)—which are also detected in
A. fumigatus isolates found in the environment [
39]. Other
Aspergillus species a are also important pathogens, such as
A. terreus, which causes aspergillosis with a high frequency in Austria and that has been reported as resistant to several antifungals, especially to amphotericin B [
68]. Furthermore,
A. flavus,
A. nidulans,
A. sydowii, and
A. alabamensis are less susceptible to amphotericin B, while
A. niger,
A. tubingensis, and
A. calidoustus are less susceptible to azoles [
73]. Other species present intrinsic resistance to both azoles and amphotericin B, such as
A. fumigatiaffinis,
A. viridinulans, and
A. versicolor, while others are resistant to both caspofungin and amphotericin B, such as
A. persii, and
A. tetrazonus [
73]. In turn,
A. lentulus is intrinsically resistant to azoles, amphotericin B, and caspofungin, while
A. udagawae is resistant to voriconazole, and amphotericin B [
73]. Notably,
A. fumigatiaffinis,
A. viridinulans,
A. lentulus and
A. udagawae are all cryptic species within the
Fumigati section.
Dimorphic fungi, considered true pathogenic fungi, are a concern to humans’ health, being found in the environment in the mold form and changing to the yeast form inside the host, such as
Histoplasma spp.,
Paracoccidioides spp.,
Coccidioides spp.,
Blastomyces spp.,
Emergomyces spp., and
Talaromyces spp. Histoplasmosis is an example of a relevant disease in humans, caused by dimorphic fungi, mainly
Histoplasma capsulatum var. capsulatum, affecting the lungs and having the ability to disseminate in the body, through to the central nervous system, or blood, resulting in approximately 500,000 cases per year [
14] and 100,000 cases of disseminated histoplasmosis annually worldwide [
14,
59,
62].
Paracoccidioides species are also pathogenic dimorphic fungi, that can be inhaled or be introduced into the skin via injury, mainly affecting the lungs, mucous membranes, and skin. Paracoccidioidomycosis can disseminate to the lymph nodes and other organs of the reticuloendothelial system, having a mortality of 3–23% and being usually treated with itraconazole, amphotericin B, or cotrimoxazole [
62]. In the Americas, Africa, and Southeast Asia, histoplasmosis and paracoccidioidomycosis tend to be the most frequently detected endemic mycoses [
60]. In Latin America, about 10 million people are infected with
Paracoccidioides spp. per year [
60].
Coccidioides spp., mainly
C. immitis and
C. posadasii, are some of the most virulent fungal pathogens, with a global burden of ~25,000 cases [
14] causing invasive coccidioidomycosis with high mortality in immunocompromised patients, their antifungal resistance being of concern, with a high MIC for fluconazole [
62].
Blastomyces spp., mainly
B. dermatitidis and
B. gilchristii, can cause acute or chronic pulmonary infection, and more rarely hematogenous dissemination disease, being treated with itraconazole [
74,
75].
Emergomyces spp. infect essentially immunocompromised patients, causing pulmonary diseases and skin lesions, being treated using amphotericin B followed by itraconazole or only itraconazole, with some strains presenting a high MIC for fluconazole [
74,
75]. The only
Talaromyces species that is considered pathogenic is
T. marneffei, which mainly affects HIV patients, with a global estimated prevalence of ~8000 cases per year [
14] and can cause lymphadenopathy, hepatomegaly, splenomegaly, respiratory and gastrointestinal abnormalities, and skin lesions [
75]. Disseminated talaromycosis is fatal if untreated and the mortality rate is around 30% even with itraconazole administration [
74].
The large group of fungal genera belonging to the Mucorales order, including
Rhizopus,
Mucor,
Rhizomucor,
Absidia,
Lichtheimia,
Apophysomyces,
Cunninghamella, and
Saksenaea, can infect immunocompromised patients and patients with metabolic disorders, such as diabetes mellitus [
58]. Infection may occur via spore inhalation, ingestion or via skin and soft-tissue injuries, causing >10,000 cases of mucormicosis per year worldwide [
14]. Invasive mucormycosis is a very serious disease, with mortality rates ranging between 23% and 80% [
62]. The available treatments include surgery (tissue debridement) and antifungal administration. In general, Mucorales are susceptible to amphotericin B and isavuconazole, but show resistance to fluconazole, voriconazole, and echinocandins [
62].
Other fungi found in soil and water can cause implantation infections as cromoblastomycosis and species such as
Madurella spp.,
Falciformispora senegalensis,
Curvularia lunata,
Scedosporium spp.,
Lomentospora prolificans,
Zopfia rosatii,
Sarocladium spp. and
Fusarium spp., can cause eumycetoma, a serious deep tissue infection that results in amputation in up to 39% of the cases, with a special risk to farmers, namely the ones working under dry climates of Africa, Latin America, and Asia near the equator [
62]. The majority of fungal infections caused by environmental fungi are opportunistic and infect mainly immunocompromised people.
Lomentospora prolificans also causes invasive lomentosporiosis with mortality rates ranging from 50% to 71% and with high antifungal resistance as described in [
62]. In turn,
Scedosporium spp. cause invasive scedosporiosis, with mortality rates of 42–46%, usually showing reduced susceptibility to amphotericin B, itraconazole, isavuconazole, and echinocandins, being usually treated with voriconazole [
62]. In fact, infections caused by the emergent fungal
Scedosporium spp.,
Fusarium spp., and Mucorales show an increasing frequency and are more frequently isolated from invasive infections [
60]. For example,
Fusarium species are responsible for causing respiratory infections, keratitis, and invasive fusariosis that can reach, via hematogenous dissemination, the central nervous system, and other organs, as well, with a mortality rate of 43–67%, especially when caused by species belonging to the
F. solani complex [
62]. Worldwide, keratitis has an incidence of around 1,000,000 cases per year, mainly caused by
F. oxysporum [
14]. However,
Fusarium spp. cause fusariosis mainly in people who are subject to invasive surgery, organ transplantation, chronic steroid treatment, or aggressive cytotoxic therapy [
76]. Fusariosis treatment is difficult due to
Fusarium spp.’s innate resistance to most antifungals, such as echinocandins and polyenes [
62,
76].
Pneumocystis jirovecii is a different infectious agent, with only an intracellular life cycle, and with the ability to be transmitted from person to person, causing around 500,000 cases of pneumonia per year worldwide [
14,
62]. It is an opportunistic fungal pathogen transmitted via the air that can also affect healthy individuals but mostly affects immunocompromised patients, with highly variable mortality rates [
59,
62].
Despite all these potential pathogenic fungal species, it is important to keep in mind that some fungal species belong to the human mycobiome, and are defined by high interindividual and intraindividual variability [
77]. Although representing less than 0.1% of the microbiome, it maintains the microbial community structure, metabolic function, and host homeostasis, as well as being an essential source of antigens to immune system training and responses [
78,
79]. The composition of the human mycobiome changes substantially during its lifespan, having high interindividual and intraindividual variability, being shaped since birth, with the mother and the environment as sources, and then being influenced by factors such as diet, body weight, age, sex, and antibiotic and antifungal therapy [
78,
79]. The development of culture-independent methods allowed an understanding of the fungal genera/species found in different body sites and their association with disease. Specific organs that were previously thought to be sterile are now known to harbor a variety of fungi and other body sites that were thought to be colonized with a low variety of fungal species were found to have a wide range of species, sometimes in association with bacteria [
79,
80]. On the other hand, the identification of fungal species associated with different body sites needs to be complemented by a demonstration of their transient (a result of contact with the external fungal exposome) or resident status, the latter allowing recognition as real members of the mycobiota [
81].
The human mycobiome comprises the one found in oral cavity, gastrointestinal tract, respiratory tract, urogenital tract, and skin. The oral adult mycobiome includes a high number of fungal species, belonging mostly to
Candida,
Penicillium,
Cladosporium,
Aspergillus,
Alternaria,
Rhodotorula,
Malassezia, and
Cryptococcus genera [
79]. The gut mycobiome comprises approximately 400 fungal species, with the Ascomycota phylum covering 48% to 99% of all present species, while the Basidiomycota phylum covers 0.5% to 14%, followed by the phylum Mucoromycota [
79,
82]. The most common species belong to
Candida,
Saccharomyces,
Paecilomyces,
Cladosporium,
Aspergillus,
Penicillium,
Malassezia,
Cryptococcus,
Rhodotorula,
Mucor, and
Rhizopus genera [
78,
79]. The human respiratory tract mycobiome is mostly composed of
Saccharomyces cerevisiae,
Candida spp.,
Pichia jadinii,
Debaryomyces,
Cladosporium,
Aspergillus,
Alternaria, and
Penicillium species [
79,
82]. The genitourinary tract mycobiome comprises mainly Ascomycota and Basidiomycota species from 22 genera, with
C. albicans,
N. glabrata, and
S. cerevisiae being the most common species, while the human skin mycobiome includes at least 168 fungal genera, with the
Malassezia genus representing more than 57% of the microscopic colonizers on average [
79].
5. Fungal Effects in Animal Health
Fungi may affect animal health in several ways, being mycotoxin contamination, associated with agricultural components of their feed, and fungal infections the most relevant examples.
Some fungal species can infect both animals and humans, causing diseases, but are not transmitted between them. However, animals can transmit certain fungal diseases to humans, as previously mentioned.
Aspergillosis can truly affect several animal species, but certain avian species are even more susceptible.In fact, aspergillosis is one of the major causes of morbidity and mortality in birds in the wild (e.g., albatrosses and penguins) and in poultry production settings, which causes ecological damage and economic loses (e.g., in turkey production it can cost USD 11 million per year) [
10,
39,
83]. Only
A. fumigatus sensu stricto is responsible for up to 90% of deaths in birds with aspergillosis [
39]. Due to the constant travels between agricultural fields, and between natural environments and urban settings, birds substantially contribute to the dispersion of
Aspergillus spp.’ conidia, including azole-resistant strains [
39].
Aspergillus spp. also affect invertebrates, such as sea corals, honeybees (causing stonebrood disease throughout all larval stages), and reptiles (causing cutaneous and disseminated infections) [
10]. In horses,
A. fumigatus also causes disease, namely equine guttural pouch mycosis, while in cows, it causes mycotic pneumonia, gastroenteritis, mastitis, placentitis, and abortions [
10,
83]. Cats and dogs, mostly the immunocompromised ones, are also susceptible to aspergillosis, causing sinonasal, bronchopulmonary, and disseminated infections [
10,
59,
83].
Other opportunistic pathogens, such as Mucorales, also infect cattle, horses, birds, cats, and dogs, causing mucormycotic ruminitis, lymphadenitis and abortions in cows, mainly affecting the respiratory system and gastrointestinal tract in horses and birds, and enteritis or systemic mucormycosis in cats and dogs [
10,
58]. Mucorales also infect wild animals such as dolphins, bison, and seals [
58].
Dogs and cats are susceptible to other fungal diseases that can also affect humans but are not transmitted to them, which are caused by dimorphic soil-borne fungi. Some examples are coccidioidomycosis, histoplasmosis, and blastomycosis. Coccidioidomycosis is caused by
Coccidioides immitis or
C. posadasii, and may infect a panoply of susceptible animals species, but is mainly reported in pet dogs, resulting in subclinical to severe or disseminated infections [
10,
59,
75]. Histoplasmosis is caused by species belonging to the
Histoplasma capsulatum complex, resulting in infections in cats, dogs, primates, and equines that include skin and subcutaneous lymphatic system injury, or disseminated diseases [
10,
59,
75,
84]. Another example of fungal diseases in animals caused by dimorphic yeast is blastomycosis, caused by
Blastomyces dermatitidis, which highly affects dogs and, usually, is not transmitted to humans via direct contact with an infected animal, unless if there is injury, such as a bite [
59,
75]. Occasionally, blastomycosis can occur in other mammals such as cats and horses [
10,
75]. It may disseminate and affect various organs and systems [
85].
Some commensal fungi can also cause infections in animals if the host immune system is disturbed.
Candida spp., mainly
C. albicans, can cause mucosal oral and gastrointestinal candidiasis in chickens, horses, cattle, dogs, cats, and pigs, usually associated with antibiotic use or immunosuppression [
10,
58]. Additionally,
Malassezia spp., mainly
M. pachydermatis, which colonizes dogs’ external ear canal, lip, interdigital skin, anus, nose, and vagina, and can cause dermatitis and otitis externa [
59,
86].
M. pachydermatis can be transmitted to humans, but with a low incidence [
59].
Dermatophytosis is considered the most common zoonotic disease in the world, with cats as the major source of human infections, especially those colonized or infected with
Microsporum canis [
59]. Actually,
M. canis colonization is estimated to be in up to 36% of healthy dogs (affecting mostly puppies) and up to 54% of healthy cats [
59]. Other dermatophytes and animal hosts have also been reported, such as
Trichophyton benhamiae in guinea pig, rabbits, dogs, or cats [
61].
T. mentagrophytes and
Nannizia gypsea in cats and dogs,
T. verrucosum in cattle, and
T. equinum in horses are all zoophilic fungi [
59].
Another concerning zoonotic infection that may also infect dogs is the one caused by
Encephalitozoon cuniculi, a microsporidium, responsible for an important neurological disease in rabbits, starting in their kidneys and then spreading to the brain, [
59].
In the same way, cryptococcosis affects domestic animals, such as cats and birds, with possible subsequent hematogenous dissemination and tropism in the central nervous system [
59]. Cryptococcosis is caused by the inhalation of the encapsulated yeasts
Cryptococcus neoformans or
C. gattii, causing severe infections in both immunocompromised and immunocompetent individuals [
59,
87]. A large diversity of animals are affected by
C. neoformans, from lower invertebrates to higher mammals, most frequently infecting cats and affecting their respiratory tracts or causing subcutaneous granulomata or disseminated infections [
10,
58]. The same can occur in dogs, but usually the central nervous system is the most severely affected, while in dairy animals it causes mastitis and in horses respiratory causes infections [
10,
58].
C. gattii infects different animal species, such as marine mammals, ferrets, and llamas, but also cats and dogs, causing upper respiratory tract infections and subcutaneous masses. However, the central nervous system, lymphatic tissue, lungs, oral cavity, and eyes can also be affected [
10].
Another current fungal infection in animals is sporotrichosis, which in cats may vary from a subclinical to a systemic infection with the hematogenous dissemination of
Sporothrix schenckii (species complex) and can be easily transmitted to humans through cats’ scratches or bites [
88]. For example, in 2000, in Brazil more than 750 people were diagnosed with sporotrichosis, 83.4% of them reporting contact with infected cats, and 56% having suffered a cat scratch or bite [
88]. Other species have clinical relevance, such as
S. brasiliensis,
S. globosa, and
S. luriei, showing different responses to antifungals which means that antifungal susceptibility differs between species, as well as does the recommended treatment [
89].
In wild animal species, other panoplies of fungi can cause infections. Some examples include
Batrachochytrium dendrobatidis and
B. salamandrivorans infecting amphibians,
Pseudogymnoascus destructans causing white nose syndrome in bats, and melanized fungal species causing severe phaeohyphomycoses, chromoblastomycosis, and mycetoma in fish, amphibians, other cold-blooded vertebrates, and crustaceans [
10].
The options of treatment applied for the different animal diseases are mainly based on azole administration, which also promotes the emergence of azole-resistant strains of different species and can restrict the treatment options. The emergence of azole-resistant strains has been a problem since the last century because azoles have been the largest and most widely used class of antifungals [
90], with the increasing existence of species and strains with azole resistance being reported. For example, strains of several
Aspergillus species are resistant to different azoles [
35,
36,
37,
91], as well as are strains of
M. pachydermatis [
86]. There are also strains of
H. capsulatum reported as fluconazole-resistant [
90], and strains of
S. brasiliensis showing growing resistance to amphotericin B and itraconazole [
89]. Moreover, several fungal species have intrinsic resistance to specific antifungals.
6. Climate Change’s Influence on Fungi
Climate change has a significant role in fungal development, proliferation and distribution, pathogenicity, and the antifungal susceptibility pattern. Climate change effects on fungi lead to new environmental pressures that result in the emergence of novel pathogens in plants, animals, and humans, and consequently new fungal diseases, which may compromise production yields, public health, and wildlife biodiversity [
33,
92,
93,
94]. Species considered to be emergent pathogens are the ones which are causal agents of new diseases, showing changes in pathogenicity, exhibiting geographic expansion, showing an increasing incidence, and/or infecting novel hosts [
92]. Climate change also promotes the increase of frequency of natural disasters such as floods, hurricanes, and tsunamis, which contribute to the distribution, aerosolization, and proliferation of fungi and to the increase in fungal infections via traumatic wounds, caused by previously rare or unknown fungal species [
33]. For example, coccidioidomycosis incidence has increased after environmental disasters such as earthquakes, volcano eruptions, wildfires, and dust storms [
75]. These situations could be observed in 1977, when a severe dust storm dispersed
Coccidioides immitis from its endemic area in Bakersfield to Sacramento County, where it was rare, causing more than 100 infections [
33]. More recently, it was detected a cluster of cases of cutaneous mucormycosis (caused by
Apophysomyces trapeziformis) among Joplin tornado survivors [
95]. Furthermore, climate change, and in particular global warming, can favor heat-tolerant fungal species and increase the susceptibility of hosts to fungal pathogens [
33,
96]. Examples include the emergence of
C. auris in humans,
P. destructans in bats, and
B. dendrobatidis and
B. salamandrivorans in amphibians [
33,
93,
94].
Candida auris is hypothesized as being a completely new pathogenic fungal species that has an environmental reservoir [
97] and that emerged due to climate changes, in particular due to global warming [
58].
B. dendrobatidis and
B. salamandrivorans are emergent species that cause significant outbreaks in amphibians, since global warming is compromising their immune system and raising their susceptibility to these pathogens [
33,
94]. The predicted mean global temperature increase of around 2 °C to 5 °C in the next decades may cause strong selective pressure leading to a rise in heat-tolerant species and will decrease the temperature gradient between the environment and mammals, increasing the prevalence of fungal diseases [
96]. In the same way, higher day and night temperatures and milder winters can increase the proliferation and pathogenicity of foliar and other fungi [
92]. For example, a rise in temperature increases evaporation in certain forest environments, which promotes cloud formation and a decrease in daytime temperature via the blocking of the sun, while at night cloud cover serves as insulation to raise the night time temperature from its normal range, which may lead to chytridiomycosis proliferation in amphibians [
98]. Moreover, climate change can promote the emergence of new virulent fungal lineages and long-distance spore dispersal, as happens with the geographical expansion of
Fusarium wilt of bananas [
99]. Further,
Puccinia striiformis causing yellow stripe rust in wheat, existing originally in cooler regions, is now also reported in warmer regions, but with more aggressivity and thermotolerance [
33,
92]. Other example is
Fusarium head blight in cereal crops in cooler regions that is increasingly caused by
F. graminearum instead of
F. culmorum, resulting in higher yield losses, of up to 75%, and in mycotoxins contamination, affecting food safety and security [
33]. Thus, the substitution of species by other more thermotolerant and mycotoxigenic is predicted to come with climate change [
100]. For example, it is predicted that climate change promotes the substitution of
Penicillium species by aflatoxin-producing
Aspergillus species [
101], such as
A. flavus and
A. parasiticus which can persist in the most extreme climate warming conditions, having high optimum temperatures for producing aflatoxins [
100]. Additionally, extreme climatic conditions can promote mycotoxin production. This happened between 2003 and 2016, when high levels of aflatoxins were reported in maize from Italy and Serbia, in response to the extreme climatic events [
100]. The same happened in France in 2015, when 6% of maize fields was contaminated by aflatoxins, due to exceptionally hot and dry climatic conditions and the high prevalence of
A. flavus [
101]. In this way, climate change may be a real concern to agriculture in the future, making crops more susceptible to fungal and mycotoxin contamination, causing plants to be subjected to suboptimal climatic conditions and causing phytopathogenic and mycotoxigenic fungi to be subjected to optimal ones [
100]. Coffee cultivation is an example, with a predicted reduction of 50% of the production area and increase in mycotoxin contamination due to climate change [
101].
The prediction of where and when emergent fungal pathogens will appear is even more difficult with climate change acceleration [
92]. Moreover, the risk of emergence of new potential pathogenic species is a concern due to the few antifungals and fungicides available, which in association with the emergence of antifungal-resistant strains is a huge problem in the short and long term [
96]. In this way, reducing carbon emissions and controlling the exacerbation of climate change are important steps to control fungal species adaptation and pathogen emergence. Controlling the excessive use of antifungals and fungicides and the increasing efforts to develop vaccines are also the main actions to promote the reduction in fungal infections [
33,
96]. More epidemiological studies and mathematical models are also needed to predict the incidence of emergent pathogens in the long term [
92].