Eccentric Exercise for Achilles Tendinopathy: A Narrative Review and Clinical Decision-Making Considerations
Abstract
1. Background
2. Historical Perspective
3. Continuum Model of Tendinopathy
4. Proposed Mechanisms of Action
4.1. Pathological Changes with Tendinopathy
4.2. Possible Explanations for Improvement with Eccentrics
5. Clinical Efficacy of Eccentric Exercise for Achilles Tendinopathy
5.1. Eccentric Exercise Versus Control
5.2. Eccentric Exercise Versus other Forms of Exercise
5.3. Eccentric Exercise Versus Orthoses or Therapeutic Modalities
5.4. Multimodal Treatment Approaches with or Without Eccentric Exercise
6. Clinical Decision-Making Considerations
6.1. Patient Presentation
6.2. Reasons for Integrating Eccentric Exercise
6.3. Reasons for not Integrating Eccentric Exercise
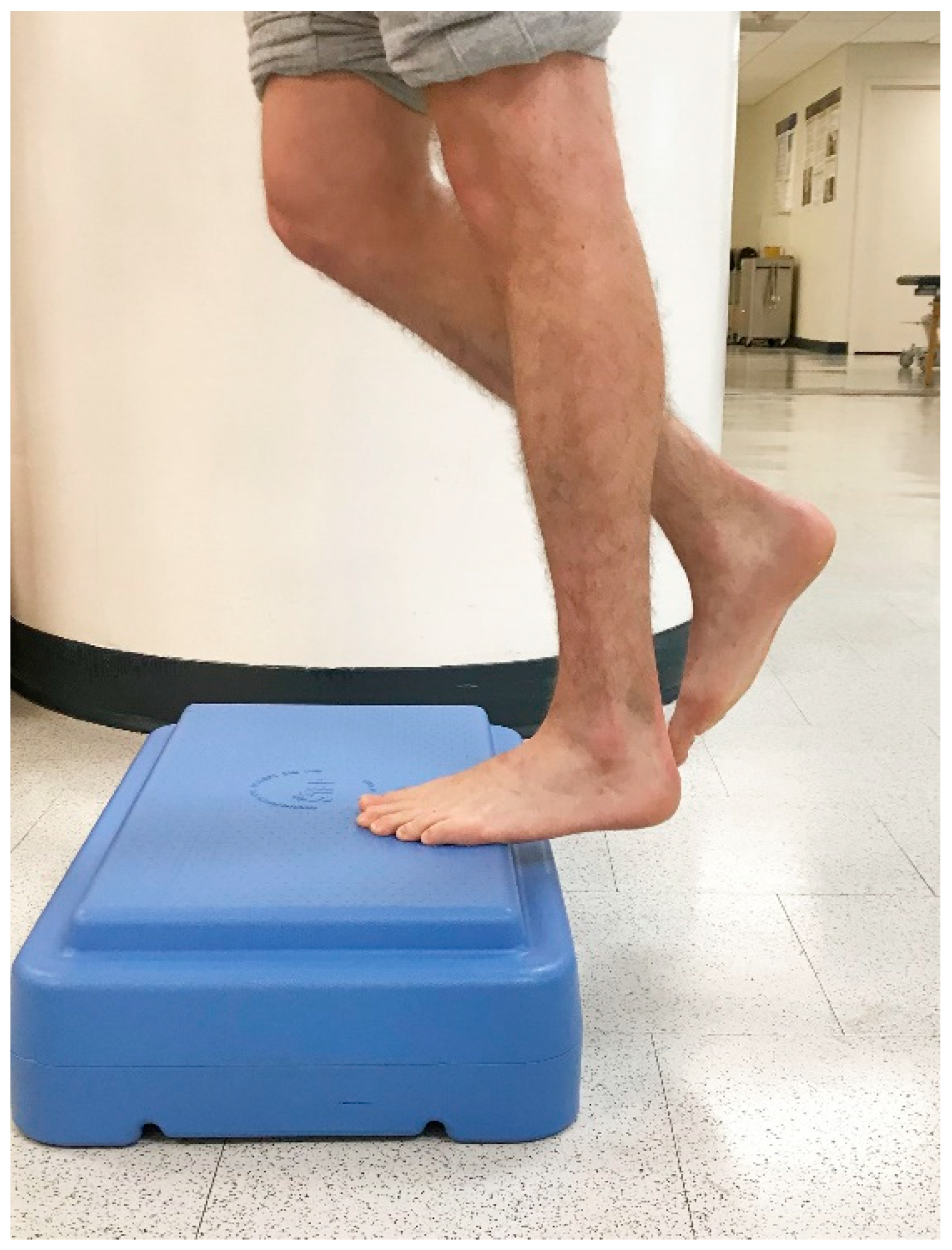
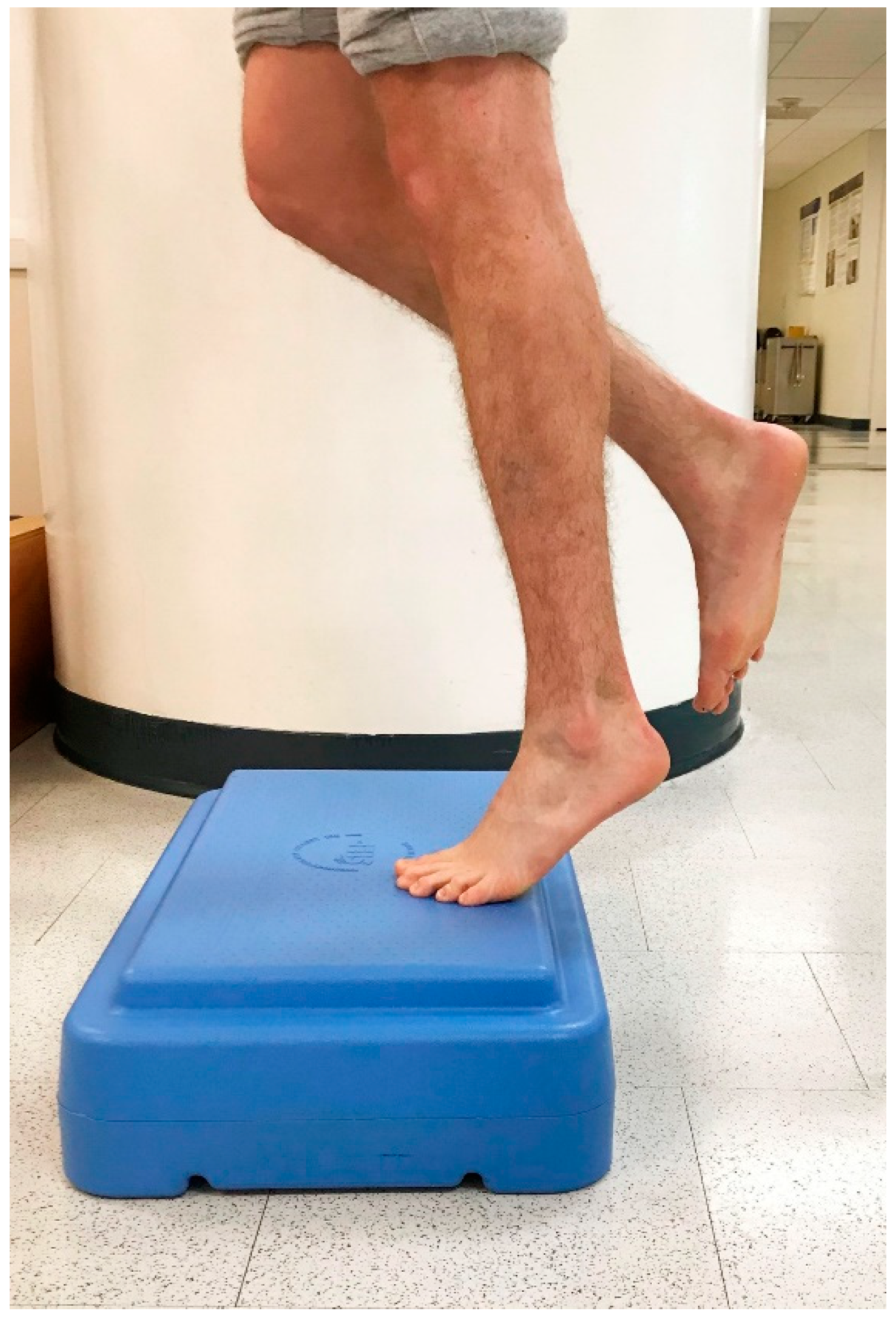
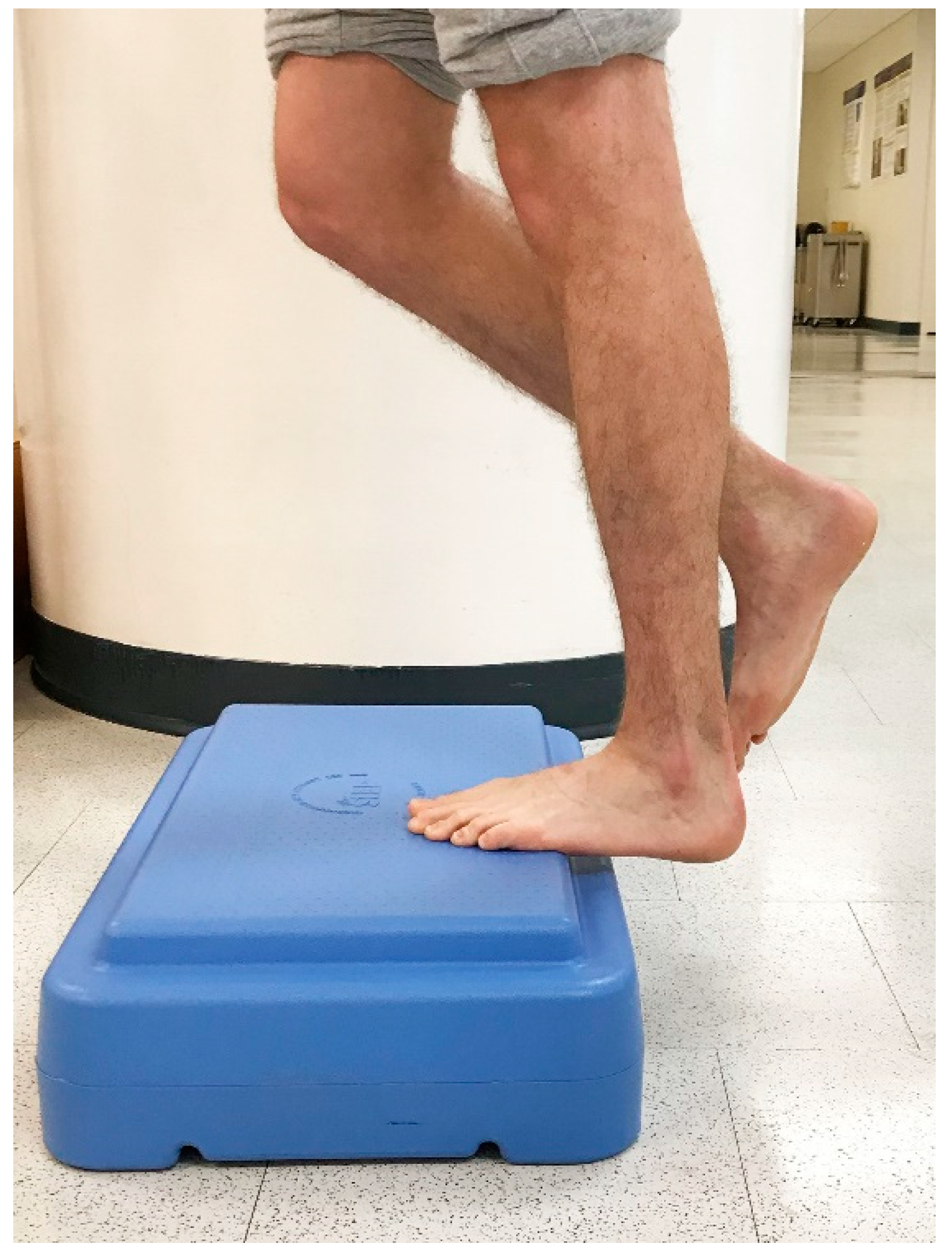
6.4. Clinical Suggestions for Incorporating Eccentric Exercise
7. Discussion
Author Contributions
Funding
Conflicts of Interest
References
- Albers, I.S.; Zwerver, J.; Diercks, R.L.; Dekker, J.H.; Akker-Scheek, I.V.D. Incidence and prevalence of lower extremity tendinopathy in a Dutch general practice population: A cross sectional study. BMC Musculoskelet. Disord. 2016, 17, 565. [Google Scholar] [CrossRef]
- Lopes, A.D.; Hespanhol Junior, L.C.; Yeung, S.S.; Costa, L.O. What are the main running-related musculoskeletal injuries? A systematic review. Sports Med. 2012, 42, 891–905. [Google Scholar] [CrossRef]
- Cook, J.L.; Purdam, C.R. The challenge of managing tendinopathy in competing athletes. Br. J. Sports Med. 2014, 48, 506–509. [Google Scholar] [CrossRef]
- Ceravolo, M.L.; Gaida, J.E.; Keegan, R.J. Quality-of-life in achilles tendinopathy: An exploratory study. Clin. J. Sport Med. 2018. [Google Scholar] [CrossRef]
- Martin, R.L.; Chimenti, R.; Cuddeford, T.; Houck, J.; Matheson, J.W.; McDonough, C.M.; Paulseth, S.; Wukich, D.K.; Carcia, C.R. Achilles pain, stiffness, and muscle power deficits: Midportion achilles tendinopathy revision 2018: Clinical practice guidelines linked to the international classification of functioning, disability and health from the orthopaedic section of the american physical therapy association. J. Orthop. Sports Phys. Ther. 2018, 48, A1–A38. [Google Scholar]
- Murphy, M.C.; Travers, M.J.; Chivers, P.; Debenham, J.R.; Docking, S.I.; Rio, E.K.; Gibson, W. Efficacy of heavy eccentric calf training for treating mid-portion Achilles tendinopathy: A systematic review and meta-analysis. Br. J. Sports Med. 2019. [Google Scholar] [CrossRef]
- Stanish, W.D.; Rubinovich, R.M.; Curwin, S. Eccentric Exercise in Chronic Tendinitis. Clin. Orthop. Relat. Res. 1986, 208, 65–68. [Google Scholar] [CrossRef]
- Alfredson, H.; Pietilä, T.; Jonsson, P.; Lorentzon, R. Heavy-Load Eccentric Calf Muscle Training for the Treatment of Chronic Achilles Tendinosis. Am. J. Sports Med. 1998, 26, 360–366. [Google Scholar] [CrossRef]
- Mafi, N.; Lorentzon, R.; Alfredson, H. Superior short-term results with eccentric calf muscle training compared to concentric training in a randomized prospective multicenter study on patients with chronic achilles tendinosis. Knee Surg. Sports Traumatol. Arthrosc. 2001, 9, 42–47. [Google Scholar] [CrossRef]
- Silbernagel, K.G.; Thomee, R.; Thomeé, P.; Karlsson, J. Eccentric overload training for patients with chronic Achilles tendon pain —A randomised controlled study with reliability testing of the evaluation methods. Scand. J. Med. Sci. Sports 2001, 11, 197–206. [Google Scholar] [CrossRef]
- Silbernagel, K.G.; Brorsson, A.; Lundberg, M. The majority of patients with achilles tendinopathy recover fully when treated with exercise alone: A 5-year follow-up. Am. J. Sports Med. 2011, 39, 607–613. [Google Scholar] [CrossRef]
- Silbernagel, K.G.; Thomee, R.; Eriksson, B.I.; Karlsson, J. Continued sports activity, using a pain-monitoring model, during rehabilitation in patients with achilles tendinopathy: A randomized controlled study. Am. J. Sports Med. 2007, 35, 897–906. [Google Scholar] [CrossRef]
- Habets, B.; Van Cingel, R.E.H.; Backx, F.J.G.; Huisstede, B.M.A. Alfredson versus Silbernagel exercise therapy in chronic midportion Achilles tendinopathy: Study protocol for a randomized controlled trial. BMC Musculoskelet. Disord. 2017, 18, 296. [Google Scholar] [CrossRef]
- Kingma, J.J.; de Knikker, R.; Wittink, H.M.; Takken, T. Eccentric overload training in patients with chronic achilles tendinopathy: A systematic review. Br. J. Sports Med. 2007, 41, e3. [Google Scholar] [CrossRef]
- Malliaras, P.; Barton, C.J.; Reeves, N.D.; Langberg, H. Achilles and patellar tendinopathy loading programmes: A systematic review comparing clinical outcomes and identifying potential mechanisms for effectiveness. Sports Med. 2013, 43, 267–286. [Google Scholar] [CrossRef]
- Cook, J.L.; Purdam, C.R. Is tendon pathology a continuum? A pathology model to explain the clinical presentation of load-induced tendinopathy. Br. J. Sports Med. 2009, 43, 409–416. [Google Scholar] [CrossRef]
- Cook, J.L.; Rio, E.; Purdam, C.R.; Docking, S.I. Revisiting the continuum model of tendon pathology: What is its merit in clinical practice and research? Br. J. Sports Med. 2016, 50, 1187–1191. [Google Scholar] [CrossRef]
- Maffulli, N.; Wong, J.; Almekinders, L.C. Types and epidemiology of tendinopathy. Clin. Sports Med. 2003, 22, 675–692. [Google Scholar] [CrossRef]
- Arya, S.; Kulig, K. Tendinopathy alters mechanical and material properties of the achilles tendon. J. Appl. Physiol. (1985) 2010, 108, 670–675. [Google Scholar] [CrossRef]
- Leung, J.L.; Griffith, J.F. Sonography of chronic achilles tendinopathy: A case-control study. J. Clin. Ultrasound 2008, 36, 27–32. [Google Scholar] [CrossRef]
- Alfredson, H.; Ohberg, L.; Forsgren, S. Is vasculo-neural ingrowth the cause of pain in chronic achilles tendinosis? an investigation using ultrasonography and colour doppler, immunohistochemistry, and diagnostic injections. Knee Surg. Sports Traumatol. Arthrosc. 2003, 11, 334–338. [Google Scholar] [CrossRef]
- Öhberg, L.; Lorentzon, R.; Alfredson, H. Neovascularisation in Achilles tendons with painful tendinosis but not in normal tendons: An ultrasonographic investigation. Knee Surg. Sports Traumatol. Arthrosc. 2001, 9, 233–238. [Google Scholar] [CrossRef]
- Corrigan, P.; Cortes, D.H.; Pontiggia, L.; Silbernagel, K.G. The degree of tendinosis is related to symptom severity and physical activity levels in patients with midportion achilles tendinopathy. Int. J. Sports Phys. Ther. 2018, 13, 196–207. [Google Scholar] [CrossRef]
- Tompra, N.; van Dieen, J.H.; Coppieters, M.W. Central pain processing is altered in people with achilles tendinopathy. Br. J. Sports Med. 2016, 50, 1004–1007. [Google Scholar] [CrossRef]
- Plinsinga, M.L.; van Wilgen, C.P.; Brink, M.S.; Vuvan, V.; Stephenson, A.; Heales, L.J.; Mellor, R.; Coombes, B.K.; Vicenzino, B.T. Patellar and achilles tendinopathies are predominantly peripheral pain states: A blinded case control study of somatosensory and psychological profiles. Br. J. Sports Med. 2018, 52, 284–291. [Google Scholar] [CrossRef]
- Öhberg, L.; Lorentzon, R.; Alfredson, H.; Maffulli, N. Eccentric training in patients with chronic Achilles tendinosis: Normalised tendon structure and decreased thickness at follow up. Br. J. Sports Med. 2004, 38, 8–11. [Google Scholar] [CrossRef]
- Öhberg, L.; Alfredson, H. Effects on neovascularisation behind the good results with eccentric training in chronic mid-portion Achilles tendinosis? Knee Surg. Sports Traumatol. Arthrosc. 2004, 12, 465–470. [Google Scholar] [CrossRef]
- de Jonge, S.; Tol, J.L.; Weir, A.; Waarsing, J.H.; Verhaar, J.A.; de Vos, R.J. The tendon structure returns to asymptomatic values in nonoperatively treated achilles tendinopathy but is not associated with symptoms: A prospective study. Am. J. Sports Med. 2015, 43, 2950–2958. [Google Scholar] [CrossRef]
- Drew, B.T.; Smith, T.O.; Littlewood, C.; Sturrock, B. Do structural changes (eg, collagen/matrix) explain the response to therapeutic exercises in tendinopathy: A systematic review. Br. J. Sports Med. 2014, 48, 966–972. [Google Scholar] [CrossRef]
- Rio, E.; Moseley, L.; Purdam, C.; Samiric, T.; Kidgell, D.; Pearce, A.J.; Jaberzadeh, S.; Cook, J. The pain of tendinopathy: Physiological or pathophysiological? Sports Med. 2014, 44, 9–23. [Google Scholar] [CrossRef]
- Hagglund, M.; Walden, M.; Ekstrand, J. Lower reinjury rate with a coach-controlled rehabilitation program in amateur male soccer: A randomized controlled trial. Am. J. Sports Med. 2007, 35, 1433–1442. [Google Scholar] [CrossRef]
- Silbernagel, K.G.; Crossley, K.M. A Proposed Return-to-Sport Program for Patients with Midportion Achilles Tendinopathy: Rationale and Implementation. J. Orthop. Sports Phys. Ther. 2015, 45, 876–886. [Google Scholar] [CrossRef]
- Rio, E.; Kidgell, D.; Moseley, G.L.; Gaida, J.; Docking, S.; Purdam, C.; Cook, J. Tendon neuroplastic training: Changing the way we think about tendon rehabilitation: A narrative review. Br. J. Sports Med. 2016, 50, 209–215. [Google Scholar] [CrossRef]
- Stackhouse, S.K.; Taylor, C.M.; Eckenrode, B.J.; Stuck, E.; Davey, H. Effects of Noxious Electrical Stimulation and Eccentric Exercise on Pain Sensitivity in Asymptomatic Individuals. PmR 2016, 8, 415–424. [Google Scholar] [CrossRef]
- Slater, H.; Thériault, E.; Ronningen, B.O.; Clark, R.; Nosaka, K. Exercise-induced mechanical hypoalgesia in musculotendinous tissues of the lateral elbow. Man. Ther. 2010, 15, 66–73. [Google Scholar] [CrossRef]
- Hirschmüller, A.; Frey, V.; Konstantinidis, L.; Baur, H.; Dickhuth, H.-H.; Südkamp, N.P.; Helwig, P. Prognostic Value of Achilles Tendon Doppler Sonography in Asymptomatic Runners. Med. Sci. Sports Exerc. 2012, 44, 199–205. [Google Scholar] [CrossRef]
- Jhingan, S.; Perry, M.; O’Driscoll, G.; Lewin, C.; Teatino, R.; Malliaras, P.; Maffulli, N.; Morrissey, D. Thicker Achilles tendons are a risk factor to develop Achilles tendinopathy in elite professional soccer players. Muscle Ligaments Tendons J. 2011, 1, 51–56. [Google Scholar]
- Beyer, R.; Kongsgaard, M.; Hougs Kjaer, B.; Ohlenschlaeger, T.; Kjaer, M.; Magnusson, S.P. Heavy slow resistance versus eccentric training as treatment for achilles tendinopathy: A randomized controlled trial. Am. J. Sports Med. 2015, 43, 1704–1711. [Google Scholar] [CrossRef]
- Herrington, L.; McCulloch, R. The role of eccentric training in the management of Achilles tendinopathy: A pilot study. Phys. Ther. Sport 2007, 8, 191–196. [Google Scholar] [CrossRef]
- Horstmann, T.; Jud, H.M.; Fröhlich, V.; Muendermann, A.; Grau, S. Whole-Body Vibration Versus Eccentric Training or a Wait-and-See Approach for Chronic Achilles Tendinopathy: A Randomized Clinical Trial. J. Orthop. Sports Phys. Ther. 2013, 43, 794–803. [Google Scholar] [CrossRef]
- Petersen, W.; Welp, R.; Rosenbaum, D. Chronic achilles tendinopathy: A prospective randomized study comparing the therapeutic effect of eccentric training, the AirHeel brace, and a combination of both. Am. J. Sports Med. 2007, 35, 1659–1667. [Google Scholar] [CrossRef]
- Rompe, J.D.; Nafe, B.; Furia, J.P.; Maffulli, N. Eccentric loading, shock-wave treatment, or a wait-and-see policy for tendinopathy of the main body of tendo achillis: A randomized controlled trial. Am. J. Sports Med. 2007, 35, 374–383. [Google Scholar] [CrossRef]
- Tumilty, S.; Mani, R.; Baxter, G.D. Photobiomodulation and eccentric exercise for achilles tendinopathy: A randomized controlled trial. Lasers Med. Sci. 2016, 31, 127–135. [Google Scholar] [CrossRef]
- Yu, J.; Park, D.; Lee, G. Effect of Eccentric Strengthening on Pain, Muscle Strength, Endurance, and Functional Fitness Factors in Male Patients with Achilles Tendinopathy. Am. J. Phys. Med. Rehabil. 2013, 92, 68–76. [Google Scholar] [CrossRef]
- Rio, E.; Kidgell, D.; Purdam, C.; Gaida, J.; Cook, J.; Gaida, J.; Moseley, L.; Pearce, A.J. Isometric exercise induces analgesia and reduces inhibition in patellar tendinopathy. Br. J. Sports Med. 2015, 49, 1277–1283. [Google Scholar] [CrossRef]
- Jayaseelan, D.J.; Weber, M.J.; Jonely, H. Potential Nervous System Sensitization in Patients with Persistent Lower Extremity Tendinopathies: 3 Case Reports. J. Orthop. Sports Phys. Ther. 2019, 49, 272–279. [Google Scholar] [CrossRef]
- Masci, L.; Spang, C.; Van Schie, H.T.M.; Alfredson, H. How to diagnose plantaris tendon involvement in midportion Achilles tendinopathy - clinical and imaging findings. BMC Musculoskelet. Disord. 2016, 17, 565. [Google Scholar] [CrossRef]
- Spang, C.; Alfredson, H.; Docking, S.I.; Masci, L.; Andersson, G. The plantaris tendon: A narrative review focusing on anatomical features and clinical importance. Bone Jt. J. 2016, 98-B, 1312–1319. [Google Scholar] [CrossRef]
- Stephen, J.M.; Marsland, D.; Masci, L.; Calder, J.D.F.; Daou, H.E. Differential motion and compression between the plantaris and achilles tendons: A contributing factor to midportion achilles tendinopathy? Am. J. Sports Med. 2018, 46, 955–960. [Google Scholar] [CrossRef]
- Romero-Morales, C.; Martín-Llantino, P.J.; Calvo-Lobo, C.; López-López, D.; Sánchez-Gómez, R.; De-La-Cruz-Torres, B.; Rodríguez-Sanz, D. Ultrasonography Features of the Plantar Fascia Complex in Patients with Chronic Non-Insertional Achilles Tendinopathy: A Case-Control Study. Sensors 2019, 19, 2052. [Google Scholar] [CrossRef]
- Morales, C.R.; Llantino, P.J.M.; Lobo, C.C.; Gómez, R.S.; López, D.L.; Galeano, H.P.; Sanz, D.R. Ultrasound evaluation of extrinsic foot muscles in patients with chronic non-insertional Achilles tendinopathy: A case-control study. Phys. Ther. Sport 2019, 37, 44–48. [Google Scholar] [CrossRef]
| First Author | Participants | Primary Eccentric Intervention Group | Comparison(s) | Frequency and Duration of Therapy |
|---|---|---|---|---|
| Beyer [38] | n = 47 (25 Exp, 22 Comp) Exp mean age: 48 ± 2.0; Comp mean age: 48 ± 2.0 Primary diagnosis: mid-portion Achilles tendinopathy | Unilateral eccentric exercise | Heavy slow resistance exercise | Exp: 3 × 15 repetitions per exercise; 2×/day; 7 days/week; 12 weeks Comp: 3–4 sets per exercise; 3×/week; 12 weeks total; (gradual increase in load and decrease in reps over 12 weeks) |
| Herrington [39] | n = 25 (13 Exp, 12 Comp) Exp mean age: 37 ± 9.26; Comp mean age: 36.6 ± 7.14 Primary diagnosis: Achilles tendinopathy | Eccentric exercise, DFM, US, and stretching to gastrocnemius and soleus | DFM, US, and stretching to gastrocnemius and soleus | Exp: eccentric exercise 2×/day; 7 days/week; 12 weeks total; DFM, US, and stretching followed same protocol as comp Comp: DFM and US 1×/week; 6 weeks; 6 sessions total; stretching daily; 12 weeks total |
| Horstmann [40] | n = 54 (18 Exp, 22 Comp, 14 controls) Exp mean age: 45.7 ± 8.5; Comp mean age: 46 ± 6.9; control mean age: 44.4 ± 7.7 Primary diagnosis: chronic Achilles tendinopathy | Unilateral eccentric exercise | (1) Comp: whole body vibration training (2) control | Exp: 3 × 15 repetitions per exercise; 12 weeks total; 36 total sessions Comp: 4–7 min per training session; 12 weeks total; 36 total session |
| Petersen [41] | n = 100 (37 Exp, 35 Comp, 28 combinations) Exp mean age: 42.1 ± 11.0; Comp mean age: 42.6 ± 10.7; combination mean age: 43 ± 12 Primary diagnosis: Chronic Achilles tendinopathy | Eccentric exercise | (1) AirHeel Brace (2) combination of experimental and comparison groups | Exp: 3 × 15 repetitions per exercise; 3×/day; 7 days/week; 12 weeks Comp: Participants instructed to wear the AirHeel brace during the daytime for 12 weeks Combination: Followed Exp and combination protocols |
| Rompe [42] | n = 75 (25 per group) Exp mean age: 48.1 ± 9.9; Comp mean age: 51.2 ± 10.3; control mean age: 46.4 ± 11.4 Primary diagnosis: Mid-portion Achilles tendinopathy | Eccentric exercise | (1) Shock wave Therapy (2) Control | Exp: 3 × 15 repetitions per exercise; 2×/day; 7 days/week; 12 weeks total Comp: 1×/week; 3 consecutive weeks; 3 sessions total |
| Tumilty [43] | n = 80 (20 per group) group 1 mean age: 47.2 ± 8.5; group 2 mean age: 46.2 ± 10.9; group 3 mean age: 47.7 ± 10.1; group 4 mean age: 48.5 ± 9.3 Primary diagnosis: Achilles tendinopathy | Exp group 1: Laser + eccentric exercise regime 1 Exp group 2: Laser + eccentric exercise regime 2 | Comp group 1: Placebo + eccentric exercise regime 1 Comp group 2: Placebo + eccentric exercise regime 2 | Exp group 1: laser therapy to Achilles tendon for 90 s, 2x/week, for 4 weeks; eccentric exercise 2x/day; 7 days/week; 12 weeks total Exp group 2: laser therapy to Achilles tendon for 90 s, 2×/week, for 4 weeks; eccentric exercise 2×/day; 2 days/week; 12 weeks total Comp group 1: Placebo laser therapy for 4 weeks; eccentric exercise 2×/day; 7 days/week; 12 weeks total Comp group 2: Placebo laser therapy for 4 weeks; eccentric exercise 2×/day; 2 days/week; 12 weeks total |
| Yu [44] | n = 32 (16 per group) Exp mean age: 20.14 ± 1.84; Comp mean age: 20.40 ± 1.27 Primary diagnosis: Achilles tendinopathy | Eccentric exercise | Concentric exercise | Exp: 3 × 15 repetitions per exercise; 50 min/session; 3 days/week; 8 weeks total Comp: 3 × 15 repetitions per concentric strengthening exercise; 5 × 10” hold per stretch; 50 min/session; 3 days/week; 8 weeks total |
| First Author | Outcome Timeline | Outcome(s) Utilized | Results † |
|---|---|---|---|
| Beyer [38] | Baseline, after 12-week intervention, 52-week follow-up | (1) VAS | Eccentric-running: 49 ± 5.5, 20 ± 5.7, 12 ± 4.2 HSR-running: 54 ± 5.4, 17 ± 4.1, 5 ± 2.6 Eccentric-heel raises: 19 ± 5.0, 12 ± 3.6, 6 ± 2.6 HSR-heel raises: 29 ± 5.5, 7 ± 2.4, 5 ± 2.5 No statistically significant differences between groups at 52 weeks for VAS while running (p = 0.71) or during heel raises (p = 0.77). |
| Herrington [39] | Baseline, 4 weeks, 8 weeks, and 12 weeks | (1) VISA-A | Eccentric % change between time points: 30.4, 15.8 *, 5.6, 51.8 * (0–12 week % change) Comparison: 9.7, 12.8, 9.4, 31.9 * (0–12 week % change) The eccentric group demonstrated significantly higher (F = 5.21, p = 0.014) VISA-A scores than the comparison group over the 12-week period |
| Horstmann [40] | Baseline, after 12-week intervention | (1) VAS | Eccentric group impact of pain on household responsibilities: 13.0 ± 17.7, 5.5 ± 15.8 * Eccentric group impact of pain on recreation: 21.9 ± 23.0, 9.4 ± 16.9 * Eccentric group impact of pain on social activities: 9.4 ± 15.8, 1.0 ± 2.0 * Eccentric group impact of pain on running training: 76.3 ± 27.3, 24.7 ± 30.3 * Vibration group impact of pain on household responsibilities: 8.4 ± 19.7, 3.8 ± 6.2 Vibration group impact of pain on recreation: 27.2±27.3, 15.8 ± 21.3 * Vibration group impact of pain on social activities: 5.8 ± 12.9, 3.3 ± 7.0 * Eccentric group impact of pain on running training: 60.2 ± 35.0, 35.3 ± 34.7 * Control group impact of pain on household responsibilities: 16.0 ± 28.1, 10.2 ± 26.5 Control group impact of pain on recreation: 29.7 ± 30.0, 19.8 ± 26.2 Control group impact of pain on social activities: 7.2 ± 17.1, 9.9 ± 16.9 Control group impact of pain on running training: 63.9 ± 33.6, 51.0 ± 38.1 Eccentric exercise and vibration groups had significant improvements in outcomes, as compared to wait-and-see control. Eccentric group performed better in pain reduction than vibration group. |
| Petersen [41] | Baseline, 6 weeks, 12 weeks, 52-week follow-up | (1) VAS | Eccentric-ADLs: 20% reduction after 6 weeks *, 60% reduction after 12 weeks *, 30% reduction at 1 year * Eccentric-walking: 25% reduction after 6 weeks, 71% reduction after 12 weeks, 45% reduction at 1 year * Eccentric-sports activities: 51% reduction at 1 year * AirHeel brace-ADLs: 41% reduction after 6 weeks *, 35% reduction after 12 weeks, 27% reduction at 1 year * AirHeel brace-walking: 43% reduction after 6 weeks *, 50% reduction after 12 weeks, 46% reduction at 1 year * AirHeeel brace-sports activities: 47% reduction at 1 year * Combination-ADLs: 22% reduction after 6 weeks *, 56% reduction after 12 weeks *, 53% reduction at 1 year * Combination-walking: 36% reduction after 6 weeks *, 56% reduction after 12 weeks, 64% reduction at 1 year * Combination-sports activities: 74% reduction at 1 year * No significant between group differences seen at 1 year |
| Rompe [42] | Baseline, 4-month follow-up | (1) NRS | Eccentric group: 7.03 ± 0.8. 3.6 ± 2.3 Shockwave therapy group: 6.8 ± 0.9, 4.0 ± 2.2 Control group: 7.9 ± 0.6, 5.9 ± 1.8 No statistically significant difference between eccentric and SWT group (p = 0.494). Statistically significant differences between eccentric and control groups (p < 0.001) * and SWT and control groups (p < 0.001) * |
| Tumilty [43] | Baseline, 4 weeks, 12 weeks | (1) NPRS (pain) | Eccentric exercise regimen 1 + Laser: 8.3, 4.5 *, 2.9 * Eccentric exercise regimen 2 + Laser: 7.8, 2.4 *, 0.05 * Eccentric exercise regimen 1 + Placebo: 7.4, 4.9 *, 2.5 * Eccentric exercise regimen 2 + Placebo: 8.6, 3.5 *, 2.3 * Group 4 had statistically significant improvement in pain at 12-week follow-up. Otherwise, no significant changes in pain. |
| Yu [44] | Baseline, after 8-week intervention | (1) VAS | Eccentric: 5.72 ± 0.89, 2.16 ± 0.42 * Concentric: 5.72 ± 0.79, 3.26 ± 0.78 * Statistically significant changes between eccentric and concentric group in favor of eccentric |
| First Author | Outcome Timeline | Outcome(s) Utilized | Results † |
|---|---|---|---|
| Beyer [38] | Baseline, after 12-week intervention, 52-week follow-up | (1) VISA-A | Eccentric: 58 ± 3.9, 72 ± 3.7, 84 ± 3.5 HSR: 54 ± 3.2, 76 ± 3.7, 89 ± 2.8 No statistically significant differences between groups at 52 weeks (p = 0.62). |
| Herrington [39] | Baseline, 4 weeks, 8 weeks, and 12 weeks | (2) VISA-A | Eccentric % change between time points: 30.4 *, 15.8 *, 5.6, 51.8 * (0–12 week % change) Comparison: 9.7, 12.8, 9.4, 31.9 * (0–12 week % change) The eccentric group demonstrated significantly higher (F = 5.21, p = 0.014) VISA-A scores than the comparison group over the 12-week period |
| Petersen [41] | Baseline, 6 weeks, 12 weeks, 52-week follow-up | (1) AOFAS (2) SF-36 | Eccentric AOFAS: 10% improvement at 1 year * Eccentric SF-36: 76.1 ± 21.6, 85.0 ± 16.4, 87.7 ± 12.2 * AirHeel brace AOFAS: 10% improvement at 1 year * AirHeel brace SF-36: 76.3 ± 19.8, 84.2 ± 14.4, 88.0 ± 13.0 * Combination AOFAS: 12% improvement at 1 year * Combination SF-36: 71.8 ± 24.0, 83.6 ± 21.8, 89.3 ± 17.9 * No statistically significant differences between groups |
| Rompe [42] | Baseline, 4-month follow-up | (1) VISA-A | Eccentric group: 50.6 ± 11.5, 75.6 ± 18.7 Shockwave therapy group: 50.3 ± 11.7, 70.4 ± 16.3 Control group: 48.2 ± 9.0, 55.0 ± 12.9 No statistically significant difference between eccentric and SWT group (p = 0.259). Statistically significant differences between eccentric and control groups (p < 0.001) * and SWT and control groups (p < 0.001) * |
| Tumilty [43] | Baseline, 4 weeks, 12 weeks | (1) VISA-A | Eccentric exercise regimen 1 + Laser: 59.9, 77.9 *, 88.6 * Eccentric exercise regimen 2 + Laser: 57.5, 81.1 *, 99.0 * Eccentric exercise regimen 1 + Placebo: 56.7, 74.7 *, 80.4 * Eccentric exercise regimen 2 + Placebo: 56.8, 77.8 *, 87.6 * Eccentric exercise regimen 2 + laser showed statistically significant improvements as compared with all other groups at 12 weeks |
| Yu [44] | Baseline, after 8-week intervention | (1) Biodex total Balance index | Eccentric: 36.38 ± 8.51, 8.0 ± 5.39 * Concentric: 29.0 ± 16.02, 22.50 ± 7.52 Statistically significant changes between eccentric and concentric group in favor of eccentric |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jayaseelan, D.J.; Mischke, J.J.; Strazzulla, R.L. Eccentric Exercise for Achilles Tendinopathy: A Narrative Review and Clinical Decision-Making Considerations. J. Funct. Morphol. Kinesiol. 2019, 4, 34. https://doi.org/10.3390/jfmk4020034
Jayaseelan DJ, Mischke JJ, Strazzulla RL. Eccentric Exercise for Achilles Tendinopathy: A Narrative Review and Clinical Decision-Making Considerations. Journal of Functional Morphology and Kinesiology. 2019; 4(2):34. https://doi.org/10.3390/jfmk4020034
Chicago/Turabian StyleJayaseelan, Dhinu J., John J. Mischke, and Raymond L. Strazzulla. 2019. "Eccentric Exercise for Achilles Tendinopathy: A Narrative Review and Clinical Decision-Making Considerations" Journal of Functional Morphology and Kinesiology 4, no. 2: 34. https://doi.org/10.3390/jfmk4020034
APA StyleJayaseelan, D. J., Mischke, J. J., & Strazzulla, R. L. (2019). Eccentric Exercise for Achilles Tendinopathy: A Narrative Review and Clinical Decision-Making Considerations. Journal of Functional Morphology and Kinesiology, 4(2), 34. https://doi.org/10.3390/jfmk4020034





