Factors Influencing Parental Awareness about Newborn Screening
Abstract
1. Introduction
2. Materials and methods
2.1. Sample
2.2. Questionnaires
2.3. Data Analysis
3. Results
3.1. Response Rate and Sample Characteristics
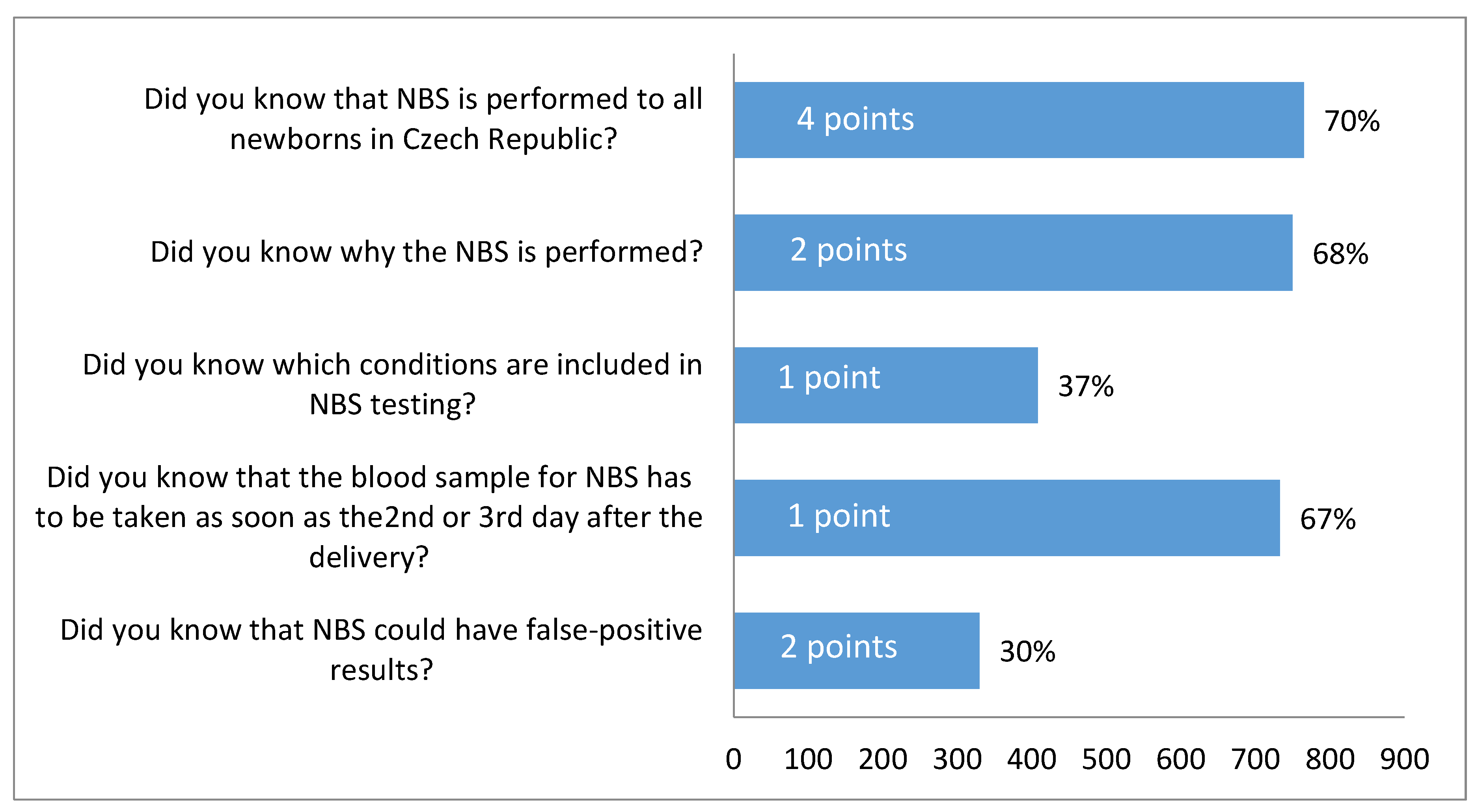
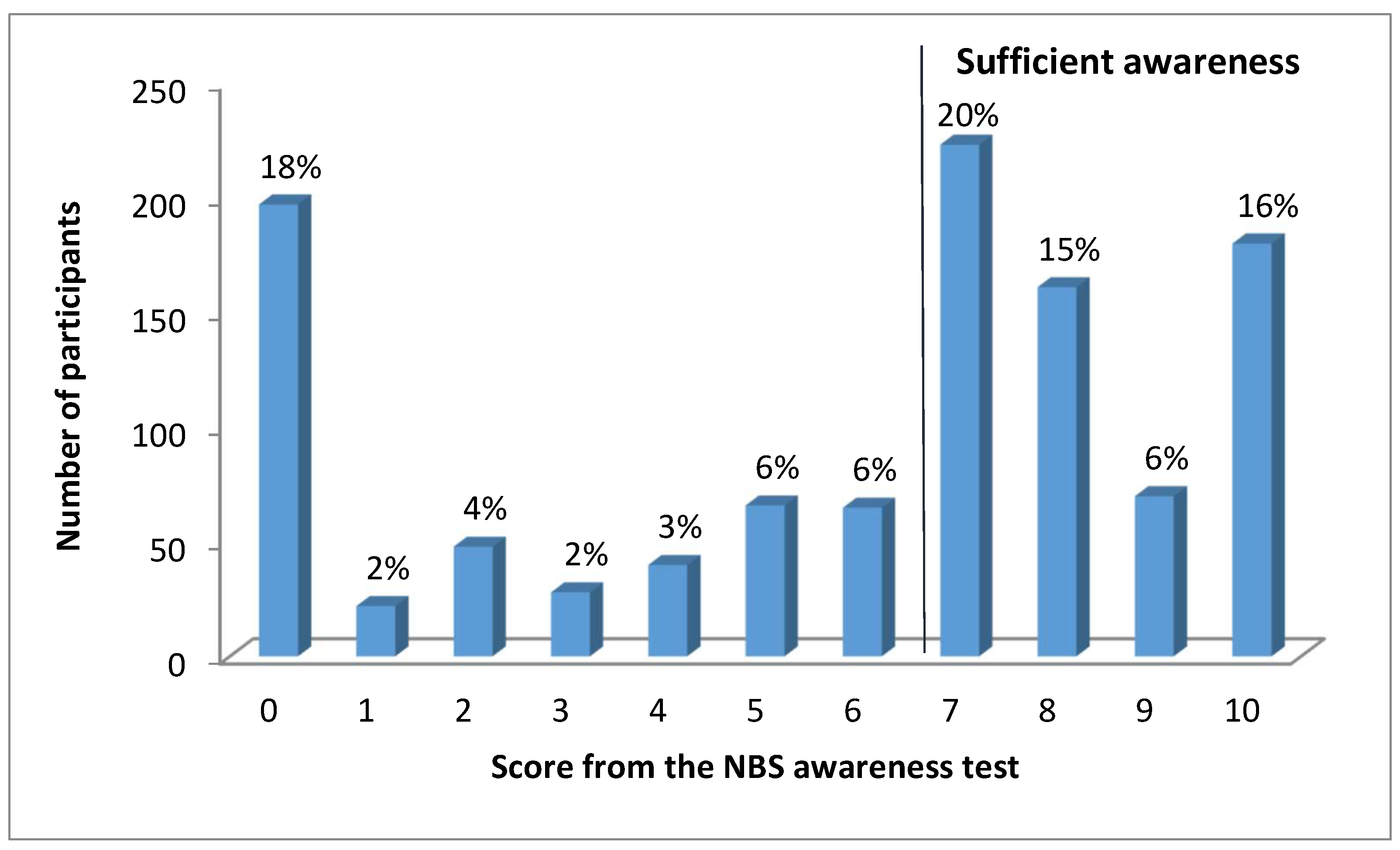
3.2. Awareness about NBS
3.3. Source of Information about NBS
3.4. Factors Associated with the Awareness about NBS
3.5. Analysis of the Free Text Comments about NBS Education and the NBS Programme
4. Discussion
Author Contributions
Funding
Conflicts of Interest
References
- Loeber, J.G.; Burgard, P.; Cornel, M.C.; Rigter, T.; Weinreich, S.S.; Rupp, K.; Hoffmann, G.F.; Vittozzi, L. Newborn screening programmes in Europe; arguments and efforts regarding harmonization. Part 1. From blood spot to screening result. J. Inherit. Metab. Dis. 2012, 35, 603–611. [Google Scholar] [CrossRef]
- Gurian, E.A.; Kinnamon, D.D.; Henry, J.J.; Waisbren, S.E. Expanded newborn screening for biochemical disorders: The effect of a false-positive result. Pediatrics 2006, 117, 1915–1921. [Google Scholar] [CrossRef]
- Tluczek, A.; Orland, K.M.; Nick, S.W.; Brown, R.L. Newborn screening: An appeal for improved parent education. J. Perinat. Neonatal Nurs. 2009, 23, 326–334. [Google Scholar] [CrossRef]
- DeLuca, J.M.; Kearney, M.H.; Norton, S.A.; Arnold, G.L. Parents’ experiences of expanded newborn screening evaluations. Pediatrics 2011, 128, 53–61. [Google Scholar] [CrossRef]
- Schmidt, J.L.; Castellanos-Brown, K.; Childress, S.; Bonhomme, N.; Oktay, J.S.; Terry, S.F.; Kyler, P.; Davidoff, A.; Greene, C. The impact of false-positive newborn screening results on families: A qualitative study. Genet. Med. 2012, 14, 76–80. [Google Scholar] [CrossRef]
- Burgard, P.; Rupp, K.; Lindner, M.; Haege, G.; Rigter, T.; Weinreich, S.S.; Loeber, J.G.; Taruscio, D.; Vittozzi, L.; Cornel, M.C.; et al. Newborn screening programmes in Europe; arguments and efforts regarding harmonization. Part 2. From screening laboratory results to treatment, follow-up and quality assurance. J. Inherit. Metab. Dis. 2012, 35, 613–625. [Google Scholar] [CrossRef]
- Etchegary, H.; Nicholls, S.G.; Tessier, L.; Simmonds, C.; Potter, B.K.; Brehaut, J.C.; Pullman, D.; Hayeems, R.; Zelenietz, S.; Lamoureux, M.; et al. Consent for newborn screening: parents’ and health-care professionals’ experiences of consent in practice. Eur. J. Hum. Genet. 2016, 24, 1530–1534. [Google Scholar] [CrossRef]
- Miller, F.A.; Hayeems, R.Z.; Carroll, J.C.; Wilson, B.; Little, J.; Allanson, J.; Bytautas, J.P.; Paynter, M.; Christensen, R.; Chaktraborty, P. Consent for newborn screening: The attitudes of health care providers. Public Health Genom. 2010, 13, 181–190. [Google Scholar] [CrossRef]
- Tluczek, A.; Koscik, R.L.; Farrell, P.M.; Rock, M.J. Psychosocial risk associated with newborn screening for cystic fibrosis: parents’ experience while awaiting the sweat-test appointment. Pediatrics 2005, 115, 1692–1703. [Google Scholar] [CrossRef]
- Davey, A.; French, D.P.; Dawkins, H.; O’Leary, P. New mother’s awareness of newborn screening, and their attitudes to the retention and use of screening samples for research purposes. Genom. Soc. Policy 2005, 1, 41–51. [Google Scholar] [CrossRef]
- Araia, M.H.; Wilson, B.J.; Chakraborty, P.; Gall, K.; Honeywell, C.; Milburn, J.; Ramsay, T.; Potter, B.K. Factors associated with knowledge of and satisfaction with newborn screening education: A survey of mothers. Genet. Med. 2012, 14, 963–970. [Google Scholar] [CrossRef] [PubMed]
- Backer, C.; Murphy, R.; Fox, J.R.E.; Ulph, F.; Calam, R. Young children’s experiences of living with a parent with bipolar disorder: Understanding the child’s perspective. Psychol. Psychother. 2017, 90, 212–228. [Google Scholar] [CrossRef] [PubMed]
- Guidelines for Newborn Bloodspot Screening and Follow-Up Care. Available online: http://www.mzcr.cz/Legislativa/dokumenty/vestnik-c6/2016_12065_3442_11.html (accessed on 27 July 2019).
- Newborn Blood Screening—Czech Official Web Pages. Available online: www.novorozeneckyscreening.cz (accessed on 12 September 2019).
- Act No. 372/2011 Coll., on Health Services and the Terms and Conditions for the Providing of Such Services (The Act on Healthcare Services). Available online: http://portal.gov.cz/app/zakony/zakonPar.jsp?page=0&idBiblio=75500&recShow=17&nr=372~2F2011&rpp=50#parCnt (accessed on 3 July 2015).
- Institute of Health Information and Statistics of the Czech Republic. Mother and Newborn 2013; Institute of Health Information and Statistics of the Czech Republic: Prague 2, Prague, Czech Republic, 2015. [Google Scholar]
- Suriadi, C.; Jovanovska, M.; Quinlivan, J.A. Factors affecting mothers’ knowledge of genetic screening. Aust. N. Z. J. Obstet. Gynaecol. 2004, 44, 30–34. [Google Scholar] [CrossRef] [PubMed]
- Davis, T.C.; Humiston, S.G.; Arnold, C.L.; Bocchini, J.A., Jr.; Bass, P.F., 3rd; Kennen, E.M.; Bocchini, A.; Kyler, P.; Lloyd-Puryear, M. Recommendations for effective newborn screening communication: Results of focus groups with parents, providers, and experts. Pediatrics 2006, 117, S326–S340. [Google Scholar] [CrossRef] [PubMed]
- Arnold, C.L.; Davis, T.C.; Frempong, J.O.; Humiston, S.G.; Bocchini, A.; Kennen, E.M.; Lloyd-Puryear, M. Assessment of newborn screening parent education materials. Pediatrics 2006, 117, S320–S325. [Google Scholar] [CrossRef] [PubMed]
- Lang, C.W.; Stark, A.P.; Acharya, K.; Ross, L.F. Maternal knowledge and attitudes about newborn screening for sickle cell disease and cystic fibrosis. Am. J. Med. Genet. A 2009, 149, 2424–2429. [Google Scholar] [CrossRef] [PubMed]
- Al-Sulaiman, A.; Kondkar, A.A.; Saeedi, M.Y.; Saadallah, A.; Al-Odaib, A.; Abu-Amero, K.K. Assessment of the Knowledge and Attitudes of Saudi Mothers towards Newborn Screening. Biomed. Res. Int. 2015, 2015, 718674. [Google Scholar] [CrossRef] [PubMed]
- Nicholls, S.G.; Southern, K.W. Parental information use in the context of newborn bloodspot screening. An exploratory mixed methods study. J. Community Genet. 2012, 3, 251–257. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Ulph, F.; Wright, S.; Dharni, N.; Payne, K.; Bennett, R.; Roberts, S.; Walshe, K.; Lavender, T. Provision of information about newborn screening antenatally: A sequential exploratory mixed-methods project. Health Technol. Assess. 2017, 21, 1–240. [Google Scholar] [CrossRef] [PubMed]
- Detmar, S.; Hosli, E.; Dijkstra, N.; Nijsingh, N.; Rijnders, M.; Verweij, M. Information and informed consent for neonatal screening: Opinions and preferences of parents. Birth 2007, 34, 238–244. [Google Scholar] [CrossRef] [PubMed]
- Moody, L.; Choudhry, K. Parental views on informed consent for expanded newborn screening. Health Expect. 2013, 16, 239–250. [Google Scholar] [CrossRef]
- Nicholls, S.G.; Southern, K.W. Informed choice for newborn blood spot screening in the United Kingdom: A survey of parental perceptions. Pediatrics 2012, 130, e1527–e1533. [Google Scholar] [CrossRef] [PubMed]
- Waisbren, S.E.; Albers, S.; Amato, S.; Ampola, M.; Brewster, T.G.; Demmer, L.; Eaton, R.B.; Greenstein, R.; Korson, M.; Larson, C.; et al. Effect of expanded newborn screening for biochemical genetic disorders on child outcomes and parental stress. JAMA 2003, 290, 2564–2572. [Google Scholar] [CrossRef] [PubMed]
- Tarini, B.A.; Christakis, D.A.; Welch, H.G. State newborn screening in the tandem mass spectrometry era: More tests, more false-positive results. Pediatrics 2006, 118, 448–456. [Google Scholar] [CrossRef] [PubMed]
- Goldenberg, A.J.; Comeau, A.M.; Grosse, S.D.; Tanksley, S.; Prosser, L.A.; Ojodu, J.; Botkin, J.R.; Kemper, A.R.; Green, N.S. Evaluating Harms in the Assessment of Net Benefit: A Framework for Newborn Screening Condition Review. Matern. Child Health J. 2016, 20, 693–700. [Google Scholar] [CrossRef] [PubMed]
- Howard, H.C.; Knoppers, B.M.; Cornel, M.C.; Wright Clayton, E.; Senecal, K.; Borry, P. Whole-genome sequencing in newborn screening? A statement on the continued importance of targeted approaches in newborn screening programmes. Eur. J. Hum. Genet. 2015, 23, 1593–1600. [Google Scholar] [CrossRef] [PubMed]
- Botkin, J.R.; Rothwell, E.; Anderson, R.A.; Rose, N.C.; Dolan, S.M.; Kuppermann, M.; Stark, L.A.; Goldenberg, A.; Wong, B. Prenatal Education of Parents About Newborn Screening and Residual Dried Blood Spots: A Randomized Clinical Trial. JAMA Pediatr. 2016, 170, 543–549. [Google Scholar] [CrossRef] [PubMed]
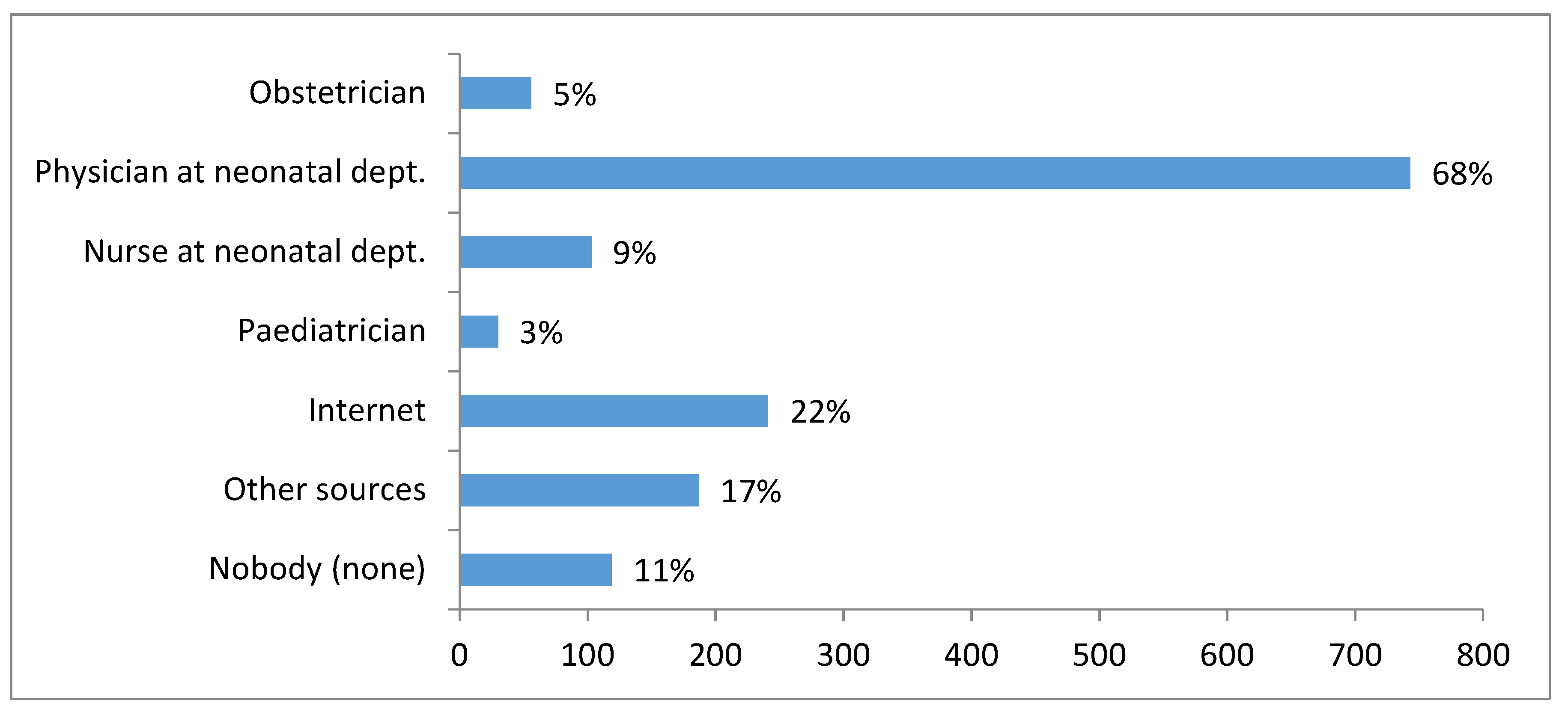
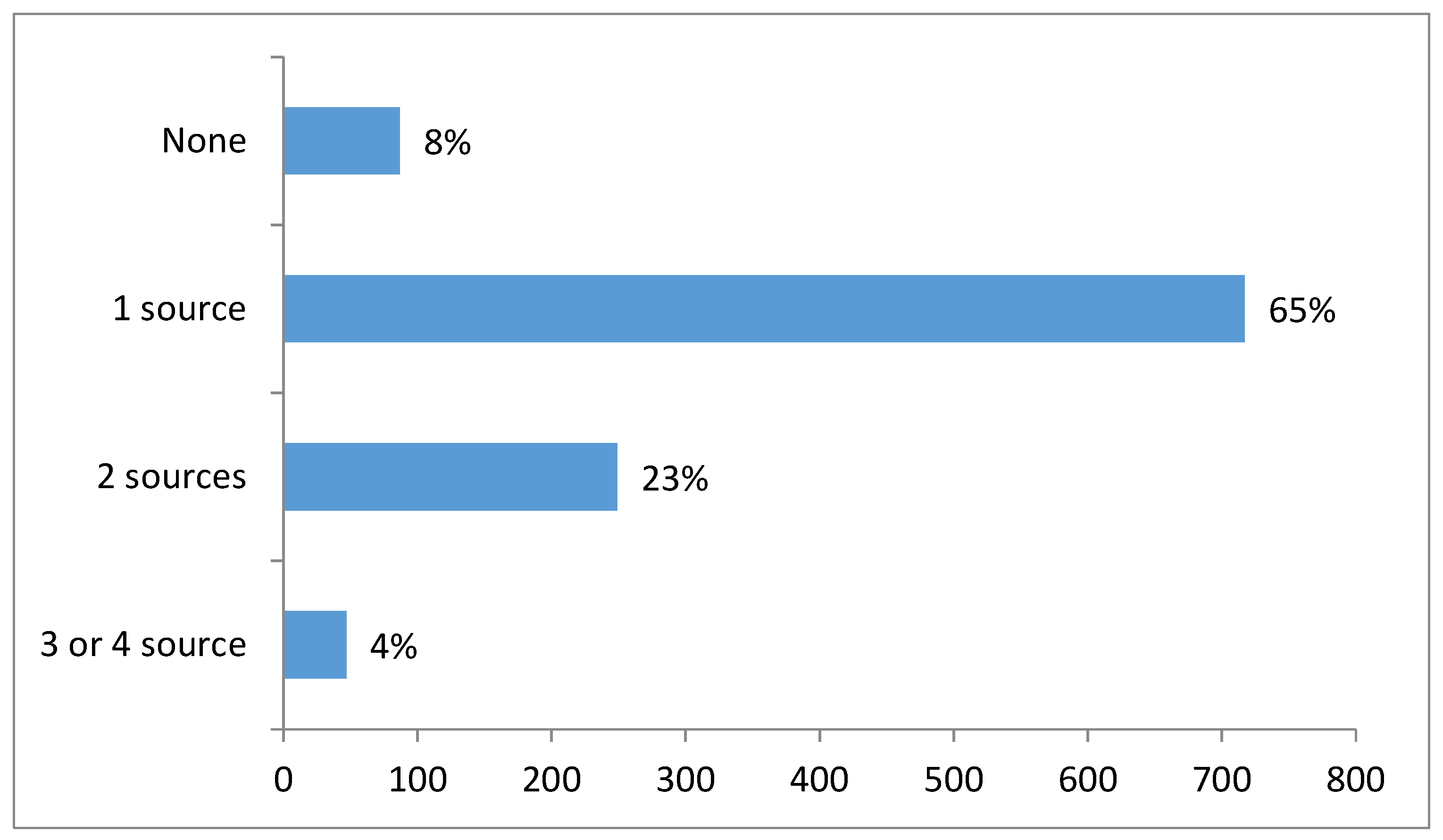
| n | This study | 95 % CI | National data a | |
|---|---|---|---|---|
| Age | ||||
| ≤29 | 345 | 31% | 28.3–33.7 | 45% |
| ≥30 | 755 | 69% | 66.3–71.7 | 55% |
| Education | ||||
| Secondary school or less | 126 | 12% | 10.1–13.9 | 32% |
| High school graduate | 442 | 40% | 37.1–42.9 | 39% |
| University degree | 532 | 48% | 45.1–51.0 | 29% |
| Parity | ||||
| Primiparous | 558 | 51% | 48.1–53.9 | 47% |
| Multiparous | 542 | 49% | 46.1–51.9 | 53% |
| Population of place of residence | ||||
| <500 | 128 | 12% | 10.1–13.9 | |
| 500–1000 | 67 | 6% | 4.6–7.4 | |
| 1000–5000 | 160 | 14% | 11.9–16.1 | |
| 5000–10,000 | 120 | 11% | 9.2–12.8 | |
| 10,000–50,000 | 174 | 16% | 13.8–18.2 | |
| 50,000–100,000 | 89 | 8% | 6.4–9.6 | |
| >100,000 | 110 | 10% | 8.2–11.8 | |
| >1 million (Prague) | 252 | 23% | 20.5–25.5 | |
| Current health status of participant | ||||
| Feeling healthy | 1002 | 91% | 89.3–92.7 | |
| With health complaints | 98 | 9% | 7.3–10.7 | |
| Complications during the pregnancy | ||||
| No | 869 | 79% | 76.6–84.4 | 85% |
| Yes | 231 | 21% | 18.6–23.4 | 15% |
| Child health status | ||||
| Healthy child | 1080 | 98% | 97.2–98.8 | 98% |
| Child with a long-term serious illness | 20 | 2% | 1.2–2.8 | 2% |
| Size of maternity hospital (number of births per year) | ||||
| Small (<1000 births/year) | 161 | 14.6% | 12.5–16.7 | 16.9% |
| Medium (1000–3000 births/year) | 463 | 42.1% | 39.2–45.0 | 42.3% |
| Large (>3000 births/year) | 473 | 43% | 40.1–45.9 | 39.9% |
| Home | 3 | 0.3% | 2.0–4.0 | 0.09% |
| n | Score from Questionnaire Evaluating Awareness about NBS | p | |||
|---|---|---|---|---|---|
| Mean | Median | Percentiles 25–75 | |||
| Age | 0.001 *** | ||||
| ≤29 | 345 | 5.27 | 7.00 | 1.00–8.00 | |
| ≥30 | 755 | 6.02 | 7.00 | 4.00–8.00 | |
| Education | N.S. | ||||
| Secondary school or less | 126 | 5.25 | 6.00 | 2.00–8.00 | |
| High school graduate | 442 | 5.69 | 7.00 | 2.00–8.00 | |
| University degree | 532 | 5.99 | 7.00 | 4.00–8.75 | |
| Parity | 0.001 *** | ||||
| Primiparous | 558 | 5.03 | 6.00 | 0.75–8.00 | |
| Multiparous | 542 | 6.56 | 7.00 | 5.00–9.00 | |
| Population of place of residence | N.S. | ||||
| <500 | 128 | 5.72 | 7.00 | 2.25–8.00 | |
| 500–1000 | 67 | 6.06 | 7.00 | 3.00–8.00 | |
| 1000–5000 | 160 | 5.70 | 7.00 | 2.25–8.00 | |
| 5000–10,000 | 120 | 5.18 | 7.00 | 1.25–8.00 | |
| 10,000–50,000 | 174 | 5.63 | 7.00 | 2.00–9.00 | |
| 50,000–100,000 | 89 | 5.90 | 7.00 | 2.50–10.00 | |
| >100,000 | 110 | 5.86 | 7.00 | 3.00–8.25 | |
| >1 million (Prague) | 252 | 6.11 | 7.00 | 4.00–9.00 | |
| Current health status of participants (self-reported) | N.S. | ||||
| Feeling healthy | 1002 | 5.80 | 7.00 | 3.00–8.00 | |
| With health complaints | 98 | 5.59 | 7.00 | 2.00–8.00 | |
| Complications during pregnancy | N.S. | ||||
| No | 869 | 5.79 | 7.00 | 3.00–8.00 | |
| Yes | 231 | 5.76 | 7.00 | 3.00–8.00 | |
| Child health status | 0.028 * | ||||
| Healthy child | 1080 | 5.81 | 7.00 | 3.00–8.00 | |
| Child with a long-term serious illness | 20 | 4.10 | 4.50 | 0.00–7.00 | |
| Size of maternity hospital (number of births per year) | 0.041 * | ||||
| Small (<1000 births/year) | 161 | 5.76 | 7.00 | 3.00–8.00 | |
| Medium (1000–3000 births/year) | 463 | 6.04 | 7.00 | 3.00–9.00 | |
| Large (>3000 births/year) | 473 | 5.53 | 7.00 | 2.00–8.00 | |
| Number of sources of information | 0.001 *** | ||||
| none | 87 | 1.11 | 0.00 | 0.00–1.00 | |
| One source | 717 | 5.78 | 7.00 | 3.00–8.00 | |
| ≥2 | 296 | 7.17 | 8.00 | 7.00–9.00 | |
| Obstetrician as the source of information | 0.001 *** | ||||
| Yes | 56 | 7.66 | 8.00 | 7.00–9.00 | |
| No | 1044 | 5.68 | 7.00 | 2.00–8.00 | |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Franková, V.; Dohnalová, A.; Pešková, K.; Hermánková, R.; O’Driscoll, R.; Ješina, P.; Kožich, V. Factors Influencing Parental Awareness about Newborn Screening. Int. J. Neonatal Screen. 2019, 5, 35. https://doi.org/10.3390/ijns5030035
Franková V, Dohnalová A, Pešková K, Hermánková R, O’Driscoll R, Ješina P, Kožich V. Factors Influencing Parental Awareness about Newborn Screening. International Journal of Neonatal Screening. 2019; 5(3):35. https://doi.org/10.3390/ijns5030035
Chicago/Turabian StyleFranková, Věra, Alena Dohnalová, Karolína Pešková, Renata Hermánková, Riona O’Driscoll, Pavel Ješina, and Viktor Kožich. 2019. "Factors Influencing Parental Awareness about Newborn Screening" International Journal of Neonatal Screening 5, no. 3: 35. https://doi.org/10.3390/ijns5030035
APA StyleFranková, V., Dohnalová, A., Pešková, K., Hermánková, R., O’Driscoll, R., Ješina, P., & Kožich, V. (2019). Factors Influencing Parental Awareness about Newborn Screening. International Journal of Neonatal Screening, 5(3), 35. https://doi.org/10.3390/ijns5030035





